This KHN story can be republished for free. (details)
brightcove.createExperiences();
A new pitch by Republican candidates to make the pill available without a prescription could have unintended financial consequences for women. KHN’s Mary Agnes Carey and Julie Rovner discuss.
MARY AGNES CAREY: Welcome to Health on the Hill, I’m Mary Agnes Carey. The health law’s provisions on contraception coverage have always been controversial. But now the issue is getting fresh attention in the midterm elections. KHN Senior Correspondent Julie Rovner joins me now with the latest. Hi, Julie.
JULIE ROVNER: Hi, MAC.
MARY AGNES CAREY: Democrats, as we know, have been talking a lot about contraception. This is an issue they are very comfortable with. But some of the new messaging is coming from the Republican side. Let’s take a look at this ad from Senate Republican candidate Cory Gardner.
CORY GARDNER (advertisement): What’s the difference between me and Mark Udall on contraception? I believe The Pill ought to be available over-the-counter, round the clock without a prescription, cheaper and easier for you. Mark Udall’s plan is different. He wants to keep government bureaucrats between you and your health care plan. That means more politics and more profits for drug companies. My plan means more rights, more freedom and more control for you, and that’s a big difference. I’m Cory Gardner and I approved this message.
MARY AGNES CAREY: Cory Gardner and some other Republican candidates in these tight Senate races are talking about birth control being sold over-the-counter. What’s happening there?
JULIE ROVNER: Well, it’s a very interesting turn of events. Of course, a number of women’s health groups, led by the American Congress of Obstetricians and Gynecologists, have also called for over-the-counter birth control, but there’s a little bit of a twist here in the way the Republicans are doing it.
What they are trying is to get out from under the issue of the Hobby Lobby case, the Supreme Court case, that said that religious employers don’t have to provide contraception, which, of course, is one of the requirements of the Affordable Care Act. The Republicans are caught between their religious, conservative base and women, who, of course, like this provision of the Affordable Care Act.
So by saying: “Let’s make it over-the-counter” that will take it out of insurance, and therefore you won’t have the issue with the religious conservatives and it sounds like it will be cheaper for women. Of course, under the Affordable Care Act, it’s no cost to women, so it might in fact end up being more expensive if you make it over-the-counter.
Now some of the Republicans are talking about making it over the counter, but reimbursable, but that of course puts it back into the insurance realm, which is a problem they were trying to get over in the first place.
MARY AGNES CAREY:ô But is this nuance about the idea that women might pay more, is that getting through to folks? I mean some of the estimates I have seen are something like $700 a year, for just the pill itself.
JULIE ROVNER: That’s right and remember we are just talking about the birth control pill. Only about a quarter of women who use contraception use the birth control pill. There’s been a push to use more longer acting forms of contraception, which are more expensive; that’s been a barrier and that was one of the goals of the Affordable Care Act to make all forms of contraception available and more affordable.
So not only would women have to perhaps pay this $600 a year, but it’s not clear who if anyone would cover the other forms of birth control things, like the IUD or implants.
Pretty much as far as the polls I’ve seen, I am not sure this is flying with women, whether or not they are sort of aware of it, I think a lot of these Republicans — Cory Gardner for example in Colorado, has in the past supported Personhood amendments, both in Colorado and at the federal level that could make some forms of birth control illegal. He is now saying that was a mistake, he doesn’t support that anymore, but there is some question as to why all of a sudden you see all these Republicans and it’s getting to be half-dozen or more Republicans who are making this an issue in their races, coming out, many of them cutting ads like Gardner saying, “I’m for women. I’m going to make birth control available over the counter.”
MARY AGNES CAREY: You also did a very interesting story recently looking at Catholic health plans that are now selling health insurance to non-Catholics, as well as Catholics. And they’re wrestling with this really interesting tension between meeting the demands in the Affordable Care Act on contraception coverage but also following Catholic Church teaching.
JULIE ROVNER: That’s right. And, you know, this is another sort of bit of fallout. The Hobby Lobby case was about for-profit insurers. There are another line of cases heading toward the Supreme Court from actual religious insurers mostly religious hospitals and universities saying, “We can’t have anything to do with contraceptive coverage, even to the extent of signing a form and sending it to the government saying we object to it.” They won’t even do that. They say that is a violation of their religious doctrine. On the other hand, you have many Catholic insurers who, as you point out, are selling not just to Catholics, although many of them do sell to Catholics.
But in New York, Fidelis, which is a Catholic insurer, was the second most popular plan on the New York health exchange. So they’re selling to non-Catholics. When they get into the market like that, they have to cover contraceptives. Partly because of the Affordable Care Act — in half the states, the states require it. So they have found ways over the years, these Catholic health insurers go back a good number of years, to basically farm that out to a third party, except that in court that’s exactly what some of these other Catholic institutions are saying they can’t do.
So, there’s now some questions looking within the Catholic Church about whether it’s okay, what these insurers have been doing. Because they’re not providing the insurance, but they’re certainly facilitating the insurance. They have to if they’re going to sell to people who are in the regular market.ô
MARY AGNES CAREY:ô ô And in your story, I think you quoted one of the bishops sort-of looking at one of these health plans, kind of questioning how they’re handling this coverage.
JULIE ROVNER:ô That’s right. There’s a bishop in Little Rock, Arkansas, which is where C.H.I., one of the largest Catholic hospital systems is going to start offering insurance. And they bought a private plan in Little Rock and that got the bishop down there wondering whether this is okay and how they’re going to handle this. He’s actually contacted the Vatican. Apparently, he’s heard back and apparently, they’re still talking. But that’s as much as we know about that.
MARY AGNES CAREY:ô ô Before I let you go, I want to touch on this recent court ruling that could affect access to abortion in Texas. What’s happening there?ô
JULIE ROVNER:ô This was a federal appeals court. It’s been a long-standing court fight over this Texas law, which has a lot of pieces to it. But this latest piece says that all abortion clinics basically have to meet the same standards as ambulatory surgical facilities. Most clinics in Texas don’t. So the result of this is that it’s going to close down, or force the closure, of all but seven clinics in the entire state of Texas.
Now obviously, this is only Texas that we’re talking about now, but this law has had an enormous amount of publicity. And the idea that abortion could become very, very, very difficult to obtain in Texas — it’s hard to tell if that might spread and concern women in other parts of the country.ô
MARY AGNES CAREY:ô ô It’s certainly something worth watching. Thanks so much, ô Julie Rovner, Kaiser Health News.ô
¤Öêü°å¿üë½ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFãan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/news/health-on-the-hill-contraception-women-voters-gop/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=329482&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Maryland Proton Treatment Center
Construction of the Maryland Proton Treatment Center is on schedule, and we plan to open our doors to patients next year.
We are very confident that the Maryland Proton Treatment Center will be successful. Our center is part of a highly developed, integrated system of hospitals in the region, all working together to ensure that cancer patients receive the care they need. This region has a very large population, and we see a real need here for this kind of innovative treatment approach. We will look to the scientific evidence, and what’s best for each particular patient, when deciding what treatments we use.
Many studies already show that proton treatment improves outcomes for different kinds of cancer. And there are more than 50 studies and trials now going on to see how best to use this treatment. This research will help us understand better how to use proton treatment most effectively. We remain confident that PBT can help many patients and are excited about how it improves patient’s lives.
It’s also important to emphasize that the proton treatment technology itself continues to improve rapidly. In particular, our center will use the latest proton approach, pencil beam scanning (PBS), which controls the radiation with extreme precision. PBS is a significant improvement over previous proton technologies.
— William F. Regine, executive director of the Maryland Proton Treatment Center and chair of radiation oncology at theô University of Maryland School of Medicine.
MedStar Georgetown University Hospital
MedStar Georgetown University Hospitalãs Lombardi Comprehensive Cancer Center is excited to be moving forward with construction of the D.C. area’s first proton therapy program.ô We have purchased the MEVION S250 proton therapy system which is the world’s smallest single room proton therapy system.ô The MEVION S250 gives the same precise non-invasive treatments as the larger, more expensive proton therapy systems but because of its smaller size, the MEVION S250 uses a reduced footprint, has improved reliability and offers more efficient patient access, all at lower cost to build and operate.
Adding proton therapy to our arsenal of cancer-fighting tools is a natural progression for MedStar Georgetown whose Lombardi Comprehensive Cancer Center just earned prestigious redesignation as a “comprehensive cancer center” by the National Cancer Institute (NCI) for the 21stô year.ô Adults and children who are patients in our well-established and renowned cancer center will benefit from the advantages of proton beam therapy over standard radiation in a cost effective way.ô Proton therapy is part of the cutting-edge care patients in this region have come to expect from us.
We are confident that payors will agree that proton therapy is an important treatment option for patients suffering with many forms of cancer.
We look forward to breaking ground on the proton beam project this fall with completion expected in a little over a year.
Johns Hopkins Medicine, Sibley Memorial Hospital
While we don’t know all the issues that resulted in the closure of the Indiana University facility, some of the issues might be related to its location; within an area with a relatively small population, thus lacking a large patient population to support the center. Additionally, the Indiana facility is in need of major upgrades to allow it to deliver proton therapy to patients in the most contemporary manner, and the high costs associated with this renovation may have influenced the decisions to close the center.
This closure does not affect the Sibley Hospital proton therapy project, which is proceeding.
¤Öêü°å¿üë½ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFãan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/hospitals-react-to-proton-therapy/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=329545&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This KHN story can be republished for free. (details)
Testifying before a House subcommittee, a key Obama administration official lays out the updates that HHS is making to the online marketplaces before enrollment begins in November. Mary Agnes Carey and Politico Pro’s Jennifer Haberkorn discuss.
MARY AGNES CAREY: Welcome to Health on the Hill, I’m Mary Agnes Carey. With the health law’s open enrollment season just months away, a key Obama administration official was on Capitol Hill today to discuss ongoing efforts to fix problems with healthcare.gov. Politico Pro’s Jennifer Haberkorn was at that hearing and joins us now. Thanks for being with us.
JENNIFER HABERKORN: Thanks for having me.

People wait in line to see a health care insurance adviser in Florida in March (Photo by Joe Raedle/Getty Images)
MARY AGNES CAREY: Andy Slavitt, who is principal deputy administrator for the Centers for Medicare & Medicaid Services, gave members of the House Ways and Means Health Subcommittee an update on the work that his agency has been doing to improve healthcare.gov. What did he say would be different when enrollment begins again in November?
JENNIFER HABERKORN: Andy Slavitt said that the application process is going to be a little more streamlined. There isn’t going to be much of a difference in consumers’ eyes in what they enter into the website. But it’s supposed to be easier for the information to get from point A, which is the consumer, to point B, the insurer. And that’s supposed to ease some of the problems that we saw last year — once the website was working, there was still some issues getting that information across. Consumers are also going to use it to re-enroll, which is obviously an issue that they did have to confront last year. This is people who are choosing a new plan, that looked ahead last year or are just trying to stay in their same plan as last year. We don’t know exactly yet what that’s going to look like, but it is an issue that the administration is going to have to confront because they’ll want those people to remain on the rolls in the second year of enrollment.
MARY AGNES CAREY: Typically these health law hearings are extremely combative with Republicans blasting the law and the officials that are implementing it. But the tone of today’s session seemed different. Was that your sense as well?
JENNIFER HABERKORN: Yeah, I definitely noticed that this year it was toned down. You definitely get a sense that the administration is at least trying to work with Congress a little bit more. Trying to tell them “We’re going to be transparent. We’re going to talk to you. We’re going to give you a heads up when there are problems.” I think we have yet to see whether that’s actually going to come to fruition, but Slavitt today was talking a lot about that and we saw the HHS Secretary Sylvia Mathews Burwell say the same thing earlier this week and she [may have] done the same thing in her conversations with Congress.ô
Slavitt interestingly did not make a promise today that the website was going to work seamlessly, but he did say that they’re doing all the ground work now to hopefully try to get a website that works properly.ô
MARY AGNES CAREY:ô I think one of his phrases was “improvement but not perfection.”
JENNIFER HABERKORN: Yeah, and I think that’s going to be the theme of what they talk about in the next few months. I think they’re very worried about promising too much. Because you know a year ago, the administration was saying this was going to work, and then we saw that it didn’t work, so I think they are very concerned about keeping expectations low.
MARY AGNES CAREY:ô Back to today’s Ways and Means hearing, IRS Commissioner John Koskinen was also there. He got a lot of questions from members, both Republicans and Democrats, about what happens if someone gets too large or too small or simply gets a subsidy in error. What happens then if that’s the case?
JENNIFER HABERKORNô Yeah, this is a big point. I think it’s going to be a significant protocol issue for the ACA over the next several months. Many of the members today were concerned that people were going to get a huge tax bill next year because they put their income in wrong, whether maliciously or not and got too large of a subsidy. That’s because if someone told an application counselor say last November that they made $40,000 so they would get a subsidy.ô But later they got a huge raise or got a new job and made $60,000. They would qualify for less of a subsidy. So if they didn’t tell the IRS about that, come April they are going to owe a significant amount of money in subsidies that they weren’t supposed to get.
And the concern is that people who don’t realize this are going to blame the tax repayment on Obamacare and it’s going to kind of drive home the Republican opposition to the law on the whole. So the IRS is saying that they are trying to notify consumers that if your income changes, you do have to notify them and that you do have to make sure that your subsidy gets changed. We still have to see whether that’s effective and whether people are actually doing that. I think this is going to come to a head next April when people are filing their taxes for the first time. One interesting thing to note, I think, is that if you get a subsidy you often can’t use the 1040EZ forms to file your taxes, which is what a lot of people use. And that might be a surprise to consumers in April.
MARY AGNES CAREY:ô How many Americans are affected by this? What happens, for example, for someone who currently has health care insurance? What happens when they file their taxes?
JENNIFER HABERKORN:ô Well, for the vast majority of people, you just have to check a box saying you have coverage. The IRS commissioner told the committee today that of the 150 million people who file tax returns, 125 million simply have to check that box that says “I have coverage,” and essentially it’s over for them.
That’s at least 25 million people, likely those who have complicated tax situations or a big income change to deal with this potential problem. And this is the first time this is going to take place, so we really don’t know how many people this could be an issue for when they go to their tax adviser.
MARY AGNES CAREY: You covered last year’s roll out of healthcare.gov, what do you think will be the same or different this fall?
JENNIFER HABERKORN: ô I think it really can’t be worse for this administration that it was last year. As you remember, it was really bad for them. The website didn’t work for two months. I don’t think we’re going to see the same thing this time. I think the administration is going to work hard to downplay expectations but to make sure the website is working.
And I think the message is going to be a little different. Last year, there was so much attention on the flaws of the website and it really did a lot to educate consumers that this Affordable Care Act exists. It will be interesting to see how the White House knows that people know about this again so that they sign up againand that they get the millions of people they want to enroll the second year for the first time to actually do so.
MARY AGNES CAREY:ô Thank you so much, Jennifer Haberkorn of Politico Pro.
¤Öêü°å¿üë½ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFãan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/health-on-the-hill-healthcare-gov-hearing-open-enrollment/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=329279&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
Letters to the Editor is a periodic KHN feature. We welcome all comments and will publish a selection. We will edit for space, and we require full names.
A recent story, Washington’s $10 Billion Search For Health Care’s Next Big Ideas (Hancock, 8/11), drew various reader responses:
Tony Hausner, independent health policy consultant; Silver Spring, Md.
I worked at Centers for Medicare & Medicaid Services Office of Research and Demostrations for many years. The model we used of carefully designed demonstration projects with well-designed comparison models and evaluation research paid off extremely well. It resulted in many major successes implemented into legislation, with incredible savings and extremely important advances in the programs. Some of the advances included prospective payment for hospitals, home health, managed care programs, hospices, and prenatal care programs, just to name a few. Much more of this is needed at CMS.
Michael A. Rie, MD, associate professor of anesthesiology at the University of Kentucky College of Medicine; Lexington, Ky.
You indicate that Premier Group Purchasing, a buying group, is pursuing innovation in efficiency and pricing in the drugs or equipment arena. Indeed, the American Society of Anesthesiologists and Premier are recent partners in a quality improvement project, and all ASA members are asked to [voluntarily contribute] their hospital drug quality issues to a database. There are legitimate reasons to be ethically concerned with a group purchasing organization (GPO) creating and owning such a database as the business model of GPOs under existing rule of law places the GPO at variance with the economic causation of chronic and increasing generic injectable drug shortages for all hospitalized patients and ambulatory patients and those requiring basic cancer chemotherapy.
Another KHN article, Patients Seeking Cheaper Care Are Soliciting Bids From Doctors Online (Boodman, 8/5), drew the following reader reaction:
William Prentice, CEO, Ambulatory Surgery Center Association; Alexandria, Va.
In her article about the online medical site, Medibid, Sandra Boodman correctly observes that ambulatory surgery centers (ASCs) often provide a more affordable alternative to their hospital counterparts. Unfortunately, she also erroneously implies that ASCs adhere to lower safety standards than other health care providers. Today, there are approximately 5,300 Medicare-certified ASCs in the country. Each of these centers meets or exceeds the rigorous health and safety standards set by the Centers for Medicare & Medicaid Services. In addition, most of these ASCs also meet additional state and federal regulatory and licensing requirements, and are accredited by the very same organizations that accredit hospitals. ASCs also maintain extensive anti-infection programs based on protocols established by the Centers for Disease Control and Prevention, and other nationally and internationally recognized infection-control guidelines. Numerous medical experts have recognized ASCs as integral to improving quality in our health care system.
Readers shared a variety of thoughts regarding Expert Panel Recommends Sweeping Changes To Doctor Training System (Rovner, 7/29). Here’s one example that focuses on rural health care:
Jean R. Sumner, MD, Georgia Rural Medical Scholar Program; Wrightsville, Ga.
Excellent article and so true. As a rural physician you see bright capable students leave the area and never return here to practice. The present system trains physicians in urban areas, in large institutions and often fails to provide the unique skills needed to be successful in a rural practice.
Readers also responded to stories about Medicare issues relating to hospice and to observation care. Here’s a comment regarding Medicare Experiment Could Signal Sea Change For Hospice (Andrews, 7/29).
Patrice Nerone; Painesville Township, Ohio
I am greatly encouraged by the direction hospice and palliative medicine seem to be going, and hope to see it become a reality. I used to work in hospice and am very heartened that patients may not have to make a choice to end treatment while pursuing comfort measures at the end of life. I don’t believe it ever should have been a one-or-the-other situation to begin with. What most patients and families seemed to hear because of that policy was: “That’s it, throw in the towel, life is over” and many of them emotionally, spiritually, and physically did just that.
And here’s a response regarding FAQ: Hospital Observation Care Can Be Costly For Medicare Patients (Jaffe, 6/18).
Bob Olsen; Helena, Mont.
The description of “observation care” is okay, but overlooks that for years Medicare attempted to limit that care only to those cases in which diagnostic tests and active medical monitoring were required. This all changed specifically due to Medicare audit decisions that denied coverage for short hospital stays, and instead argued for observation care. The “2-midnight rule” is also contrived to overcome the confusion of when admission is reasonable. [But] there was no confusion before the Medicare program itself created the problem.
Another reader offered this comment in regard to Appeals Courts Split On Legality Of Subsidies For Affordable Care Act (Rovner, 7/22).
Dawn Prevete; Atlanta, Ga.
The confusion over who is entitled to subsidies is another example of the Affordable Care Act’s failings — an overly complicated construct that made a mess of what should have been a simple expansion of health care to all Americans. We could have gone with single-payer plan — think of Canada or France or Great Britain. Or, a heavily government-regulated nationwide private insurance option like the Swiss enjoy. In Switzerland, there are no narrow networks — every insured citizen can go to any doctor or hospital or specialist in their canon (equivalent to our states). Instead, we still have insurance risk pools — state by state and even county by county — leading to tremendous differences in cost, tiny networks of doctors and hospitals, and [other] complaints and headaches.
Readers also shared their ideas regarding recent stories about employer health plans. For instance, one reader had this response to More Employers Limit Health Plan Networks But Seek To Preserve Quality, Says Adviser (Carey, 8/13).
Budd N. Shenkin, MD, affiliated faculty at the Philip R. Lee Institute for Health Policy Studies; University of California, San Francisco
In supporting high-deductible health plans, Dr. Robert Galvin is simply mouthing the line of those who don’t care a fig about the ordinary person. These plans discriminate against the ordinary worker in favor of higher income people, as though health care were an ordinary [commodity] like a TV set. HDHPs ration by income. These plans are also anti-primary care. Primary care physicians should be the “health coaches” he talks about, yet patients are dissuaded from accessing them, which is directly against decided national health policy to strengthen primary care.
And here’s a comment regarding 16% Of Large Employers Plan To Offer Low-Benefit ‘Skinny’ Plans Despite ACA: Survey (Hancock, 8/13).
Joel R. Stegner; Edina, Minn.
¤Öêü°å¿üë½ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFãan independent source of health policy research, polling, and journalism. Learn more about .[It’s] not surprising that [skinny plans] are popular in Las Vegas, where so many people make bets hoping for good luck and lose their shirts. Bet on a skinny plan, and if things don’t go your way, you lose your health, all your money and your life. Your employer is happy to let you do something so stupid, as the house always wins.
This <a target="_blank" href="/health-industry/letters-to-the-editor-18/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=329122&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This KHN story can be republished for free. (details)
House members examined concerns raised in a GAO report about the healthcare.gov website during a subcommittee hearing Thursday. KHN’s Mary Agnes Carey and CQ Roll Call’s Melissa Attias discuss.
A transcript follows.
MARY AGNES CAREY:ô Welcome to Health On The Hill.ô I’m Mary Agnes Carey. After a rocky rollout, healthcare.gov may be headed for more trouble this fall. Federal investigators told Congress Thursday that sloppy oversight and poor planning led to cost overruns and technical problems at the website, and that significant risks remain for the fall enrollment period. A Centers for Medicare and Medicaid services official also testifying at a House hearing said that while the agency is working to improve the site,ô there will be bumps when enrollment resumes in November. CQ Roll Call’s Melissa Attias was at the hearing and joins us now. Thanks so much for being here.
MELISSA ATTIAS:ô Thanks for having me.
MARY AGNES CAREY:ô I’d like to focus first on the report from the Government Accountability Office that detailed problems with healthcare.gov. Melissa I know you have covered a lot of these hearings. For you what were the key takeaways?
MELISSA ATTIAS:ô First GAO found that CMS did not employ effective planning or oversight as it developed healthcare.gov, which was the website for the federal exchange. And they said that happened even though there were things that increased the need for oversight and that there were risks.ô
The agency also found that the effort to meet project deadlines affected a number of CMS’s decisions. And they found that CMS delayed some things, — they delayed a readiness assessment for the federal exchange from March 2013 to September of that year, which meant that the website launched without CMS verifying that it met performance requirements. The agency also found that CMS saw significant performance issues with the contractor for the federal exchange at the time, which was CGI Federal, especially as the Oct. 1 open enrollment deadline neared, but that they took limited steps in response.ô
And GAO said that CMS awarded a new contract to another contractor, but that since then costs have risen and the backend system for the exchange still isn’t ready.
MARY AGNES CAREY: How did the administration respond to all of this?
MELISSA ATTIAS: Andy Slavitt, who is the principal deputy administrator at CMS — and he is just three weeks into the job — said that he agreed with recommendations that GAO made in the report for improvement. But he also said that the report wasn’t news to the people at this agency, and that they’ve had actions underway before the report came out. He also said the situation is vastly different from the rollout last fall, since the website is already up and running, and that officials are making improvements. But he said there will still be some bumps in the road.
MARY AGNES CAREY: So what is he talking about when he says bumps?
MELISSA ATTIAS: By bumps, he’s saying there are things in place to make the process smoother but that it won’t be perfect. For example, he said, it’s now very clear who can give work to the contractor and how that work gets approved, which was an issue identified in the report.ô He also said the new contractor has skin in the game to make sure it delivers.ô
MARY AGNES CAREY:ô Before healthcare.gov launched last year, CMS officials told the House Energy & Commerce Subcommittee on Oversight and Investigations ã that was the same panel that had the hearing today ã that the website was ready to go. The subcommittee chair, Tim Murphy, asked the GAO witness today if he had evidence that those officials knew the site wasn’t going to work and that they knew that when they testified last fall.
What was the response on that?
MELISSA ATTIAS:ô The top Democrat on the subcommittee, who is Diana DeGette of Colorado, really took pains to make sure this was clarified. The GAO witness said that files his agency reviewed suggest that people within CMS knew that the website would not work on Oct. 1. He said GAO found some indication that there were estimates in the spring of 2013 that the federal exchange would only be 65 percent complete by the deadline.
But he said he had no evidence that CMS Administrator Marilyn Tavenner or a former CMS official, Gary Cohen, knew that the site would not be ready ã or live in other words ã when they testified before the committee.
MARY AGNES CAREY:ô In some cases, federal and state officials have had difficulties verifying the identities of people who have enrolled in healthcare.gov and received subsidies to help defray the costs. An earlier GAO report found that the agency was able to get coverage and subsidies for fake applicants. And now we have this.
What does it all mean for the fall enrollment period?
MELISSA ATTIAS:ô I think it means that any problems with open enrollment are really going to be under the microscope as it gets underway.
Obviously, politically these issues that many Democrats want to move on from from last open enrollment and the problems saw there are going to keep coming up, also. As the investigations continue, we’re told to expect more reports, and we also have the November elections coming up. There’s always expected to be a lot of attention on the health law.
MARY AGNES CAREY:ô Sounds like we’re going to have lots to talk about. Thanks very much, Melissa Attias of CQ Roll Call.
MELISSA ATTIAS:ô Thanks.
¤Öêü°å¿üë½ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFãan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/news/health-on-the-hill-gao-energy-and-commerce-obamacare-website/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=317386&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
Letters to the Editor is a periodic KHN feature. We welcome all comments and will publish a selection. We will edit for space, and we require full names.
The recent story, The Latest In Medical Convenience: ER Appointments (Gorman and Colliver, 7/3), drew a number of responses. Here’s an example:
Judy Lay; Lomita, Calif.
This idea sounds fantastic. Having been a former ER registration clerk in a county and a private hospital, I know the grueling wait times for walk-ins, and I myself have brought home illnesses picked up in an urgent care waiting room. With technology in our hands and in our pockets this is an innovative way to harness its vast capabilities for the good.
Another reader offered this comment regarding What The Hobby Lobby Decision Means For Employersä»(6/30):
John Clark; Frisco, Texas
When you say that insurance companies can just pay for the contraceptives that Hobby Lobby doesn’t want to pay for you miss the very significant point that large employers are almost always self insured. They use third-party administrators to process the claims and re-insurance carriers to assume the abnormal claim risk, but, by and large, the claims are paid by the employer. In the case of smaller companies which are fully insured, the insurance companies will raise premiums to cover all of the claims that occur under the plans they sell. The disconnect between the money paid by the insured and the benefits the insurer provides isn’t true and lets one escape the fact that the employer IS, in fact, paying for these benefits.
Meanwhile, an insurance industry trade group offered this response to Proposal To Add Skimpier ãCopper’ Plans To Marketplace Raises Concerns (Andrews, 7/1).
Brendan Buck, vice president of communications for America’s Health Insurance Plans; Washington, D.C.
Your June 30th story … sends a troubling message that those who find current coverage options unaffordable are better left uninsured. Instead of writing these Americans off, our goal should be to find new ways to lower barriers to the important benefits that health plans provide. Indeed, the issue is not a choice between a new lower-premium plan or a platinum policy; it’s this new option or no coverage at all. The goal of a new catastrophic plan is to address the fundamental issue of affordability, and give those currently uninsured a pathway into the system. For younger and healthier Americans especially, a lower-premium plan option would not only help protect them from being bankrupted by a medical tragedy, but also provide access to important preventive care services that would be available with no out-of-pocket cost. The critics quoted may not believe consumers would be interested in a lower-tier plan, but we know with certainty that a market exists.
Another reader shared her personal experiences after reading In Unhealthy Eastern Tennessee, Limited Patient Options Bring Some Of The Country’s Cheapest Premiums (Rau, 7/8).
Kimberly K. Dorris; Scottsdale, Ariz.
¤Öêü°å¿üë½ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFãan independent source of health policy research, polling, and journalism. Learn more about .I could not agree more with Andy Figlestahler, the insurance broker who was quoted as saying that narrow network policies “should be in flashing letters: if they select E, buyer beware.” … I … purchased a Blue Cross Blue Shield of Arizona policy via the ACA Marketplace. … I was aware that there was a restricted hospital network with this plan, but there was no disclosure of a restricted physician network. In fact, the summary of the plan specifically said, “You Can See Any Specialist”! I specifically looked for my gynecologist and endocrinologist on the BCBSAZ web site, and both were listed as accepting PPOs. … I later found out that neither my gynecologist or endocrinologist – even though designated as accepting PPOs – is part of the “Alliance” PPO. I did an informal count of endocrinologists in my city of Scottsdale, Ariz. There are 22 on the BCBSAZ web site – and yet just *one* listed for the “Alliance” PPO. … For patients who wish to keep their current providers (which President Obama specifically promised we could do), this causes two issues. First, a $12,000 deductible applies for out-of-network services, vs. $6,000 in-network for my policy. Second, consumers can be charged the full rate for services, rather than the contractual discount rate.
This <a target="_blank" href="/aging/letters-to-the-editor-14/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=32477&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This KHN story can be republished for free. (details)
KHN’s Mary Agnes Carey and legal analyst Stuart Taylor discuss Monday’s ruling on the health law’s contraception mandate, examining what the decision could mean for future challenges to the law.
MARY AGNES CAREY: Welcome. I’m Mary Agnes Carey.ô
By a vote of 5 to 4, the Supreme Court has ruled that family-owned, closely held corporations do not have to comply with the health law’s contraception coverage requirements if they violate the owner’s religious views. Legal analyst Stuart Taylor Jr. joins us now to discuss the decision. Thanks for being with us.
STUART TAYLOR: Nice to be with you.
MARY AGNES CAREY: Why did the court rule this way?
STUART TAYLOR: Well, the court held that under an act of Congress passed in 1993, the Religious Freedom Restoration Act, the right is conferred on all religious groups, including, the court said in this case for the first time, for-profit corporations as well as churches and, say, nonprofit religious groups — they all get broad protection of their religious freedoms. And in a very detailed analysis of the various steps you go through under this law, first, can you invoke protection at all if you’re a for-profit corporation. The court said yes. Then, does it substantially burden your religious exercise. The court said yes, because these companies have objections to providing contraception coverage, and then they go on and say is this the government’s least restrictive means they could use to serve the need of the women who want the contraceptives, in this case. And the court said no; they have other ways they could to it. The government could pay for it or they could use an accommodation they are already using for nonprofit religious employers.
MARY AGNES CAREY: These companies, Hobby Lobby, which is a very well-known craft store, and Conestoga Wood Specialties, which is a cabinet maker, what were their arguments against the contraception mandate?
STUART TAYLOR: Unlike the Catholic groups that are also challenging the mandate, these groups have a religious objection only to what they call abortifacientsãthe morning after pill, certain kinds of IUDs that they think operate to induce abortion.
Now, it doesn’t induce abortion as the government describes abortifacient, but it does in the beliefs of these companies. And the government says they are entitled to their beliefs. So [companies] say: For us to help someone get that kind of contraception, violates our religious beliefs. We cannot do it without violating our religious beliefs. The government is trying to force us to do it against our religious beliefs, and that puts us in a terrible position, because the fines are enormous for not complying with this provision of the Affordable Care Act.
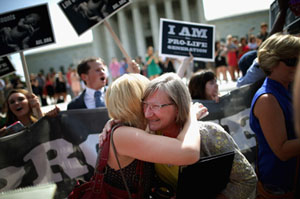
Anti-abortion advocates cheer in front of the Supreme Court after the decision in Burwell v. Hobby Lobby Stores (Photo by Chip Somodevilla/Getty Images).
For Hobby Lobby, which is a pretty [good-sized] company, it would be fines of $1.3 million a day, or $475 million a year, if it refuses to provide all federally approved contraceptive coverage, including these so-called abortifacients, and they say that’s an intolerable burden: We shouldn’t be put to that choice and the Religious Freedom Restoration Act exempts us from that choice.
MARY AGNES CAREY: What does this ruling mean for female employees of Hobby Lobby and similar companies that have objections to some forms of contraception coverage?
STUART TAYLOR Jr.: In this case, it’s not going to have much effect. In fact, the majority opinion says the effect of this on the women employed by Hobby Lobby and other companies involved in these cases would be precisely zero. And the reason is that the court says if the administration extends the same so-called accommodation to these religious employers who are for-profit companies then it’s already extended to nonprofit Catholic hospitals, nonprofit religious schools, nonprofit religious colleges, and nonprofits ã if it extends the same so-called “accommodation” to these for-profit companies, that it has already created for the nonprofit companies, then the women will get the coverage anyway through the same insurance companies that cover everything else.
MARY AGNES CAREY: So these accommodations, the justices suggested, for example, number one, the government can pay for it. Or, they could put into play some accommodations that are already there for religiously affiliated employers, which is having the insurers cover it.
STUART TAYLOR Jr.: Yes, and that’s a tricky little thing that would apply in this case and not many others. And what makes it work is that the cost of providing the contraceptive coverage is really about zero, whether it’s the employers paying for it or whether it’s the insurance company that’s paying for it because they save money on the other end, because they don’t have the child birth expenses, which are larger than contraceptive coverage. So nobody’s really paying out much money. It’s a matter of who’s got the symbolic function of providing the coverage.
This accommodation that’s already been given to nonprofit employers basically says: OK, all you have to do is certify that you have a religious objection to providing this coverage and then the government will require that your insurance company provide the coverage at no cost to you. And that’s what’s being done already in some cases — and what the court now says they can do in the cases of company, for-profit companies like Hobby Lobby.ô
MARY AGNES CAREY:ô There are many other non-profit employers like Catholic hospitals that have said even these accommodations, these other arrangements, are going to violate their religious beliefs. So what does this mean for them?ô ô
STUART TAYLOR:ô That’s right, and the reason they say it violates their religious beliefs is that they are required, at least by the regulation to certify to the insurance companies that they have this religious objection, then that triggers the insurance companies obligation to provide it. So these companies are saying, yeah, but if we have to certify and then it gets provided that means we are doing what we object to doing, which is providing a link in the chain of causation that leads to women using contraceptives.ô
Burwell v. Hobby Lobby Stores
- Supreme Court Limits Contraceptive Mandate For Certain Employers
- What The Hobby Lobby Decision Means For Employers
- FAQ: High Court’s Hobby Lobby Ruling Cuts Into Contraceptive Mandate
- Court Ruling Geared To ‘Closely Held’ Firms, But What Is That?
- Hobby Lobby Decision May Not Be The Last Word On Birth Control Coverage
So it’s a little peculiar because the court has said that Hobby Lobby and its co-plaintiffs who do not object to the certification can be covered by this, but at least technically the possibility remains that the court would eventually decide that you cannot require, say, Catholic organizations that object to providing the coverage to object to certifying that they won’t provide the coverage to do so.
MARY AGNES CAREY:ô Does this ruling mean that privately held for for-profit corporations can ignore other requirements of the health law if they find those requirements objectionable on religious grounds?
STUART TAYLOR:ô Justice Ginsburg’s long and eloquent dissent implied that, but the majority and more specifically Justice Kennedy who provided a concurring opinion say that no that wouldn’t really do that, it’s not nearly as broad as Justice Ginsburg says it is. The quote is Justice Kennedy says: The Court’s opinion does not have the breadth and sweep ascribed to it by the respectful and powerful dissent of Justice Ginsburg’s. So you have a disagreement between the dissent and at least some of the majority of whether this is going to be a far reaching decision or whether it’s going to be one that covers this case and not too many other cases.
MARY AGNES CAREY:ô What did Justice Ginsburg mean in her dissent when she called the ruling a decision of startling breadth?
STUART TAYLOR:ô She meant that, she went on to say, that it says: The court holds that commercial enterprises, including corporations, can opt out of any law, except tax laws, they judge incompatible with their sincerely held religious beliefs.
It would be a decision of startling breadth if the court had said that. But as the majority and Justice Kennedy’s concurrence both say: No, no, no, Justice Ginsburg. It isn’t nearly as broad as you’re saying it is.
And, by the way, this kind of dialogue is fairly common when dissenters, in order to emphasize what terrible things could happen as the result of a decision they don’t like, they tend to read it as broadly as possible to make it sound worse, and then the majority tends to say: Oh, no, it’s not that broad. And you never really find out how broad it is until the next case comes along.
MARY AGNES CAREY:ô What does today’s decision mean for other litigants who are challenging the contraception mandate because they say it violates their religious freedom?
STUART TAYLOR:ô I think most of them are going to win their cases if they can make it clear that their religious objections are sincere. I think most of them can, or they don’t file lawsuits.
It should be clear: A public company, certainly a big public company, would not be able to pull off a sincere religious objection of this kind, because the bigger a company gets, the less likely it is that all of the people who have an ownership or management interest in it are of the same religion and share the same objections. So this is, by its nature, this sort of logic is confined to family-owned companies, or maybe companies owned by a small group of like-minded religious people who say their religion is very important to the way they operate their businesses.
Hobby Lobby is quite a big company, for example, but still we’re not talking about General Motors or Ford or McDonald’s or any companies like that.
MARY AGNES CAREY:ô That you so much legal analyst Stuart Taylor.
STUART TAYLOR:ô Thank you.
¤Öêü°å¿üë½ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFãan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/hobby-lobby-legal-issues-stuart-taylor/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=33398&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This KHN story can be republished for free. (details)
Medicare has identified 761 hospitals that are in line to be penalized for high rates of infections and complications this fall. Some of these hospitals may avoid the penalties in the fall after federal officials factor into their analysis an additional year of infections.
Below are the 175 hospitals that are most likely to be penalized because their preliminary scores are nine or above on a scale of 1 to 10. You can download the complete . You can also read the KHN story, KHN explanation of how the penalty program works,ô and look at the KHN analysis.
Source: Centers for Medicare & Medicaid Services
<< Main Story: More Than 750 Hospitals Face Medicare Crackdown On Patient Injuries
¤Öêü°å¿üë½ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFãan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/aging/patient-injuries-hospitals-most-likely-to-be-penalized/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=33542&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The Congressional Budget Office will no longer evaluate the fiscal implications of some parts of the Affordable Care Act, partly because of all the changes made during implementation. KHN’s Mary Agnes Carey and The Fiscal Times’ Eric Pianin discuss.
MARY AGNES CAREY:ô Welcome to Health on the Hill, I’m Mary Agnes Cary. One of the Obama administration’s major selling points of the sweeping 2010 health care law was a Congressional Budget Office (CBO) analysis that the measure would expand coverage for millions of people, while reducing the federal deficit over the next decade. But recently the CBO said it could no longer evaluate the fiscal implications of all of the law’s provisions, in part because the administration has made so many changes during implementation. Eric Pianin of The Fiscal Times is with us now to discuss this development. Thanks so much for being here, Eric.
ERIC PIANIN:ô It’s my pleasure.
MARY AGNES CAREY:ô As you and I both know from covering the health care law together, the CBO had made this estimate that the law would save something around $120 billion over the next decade. But given this recent announcement what does this mean for the CBO’s ability to analyze these provisions on how much money they’ll save.
ERIC PIANIN:ô I think you’re right, I think the CBO consistently in recent years has projected that overall it would have a positive impact on the deficit, maybe bring it down by $120 billion over ten years or so. And when Republicans made a big push to try to repeal Obamacare, the CBO warned that it could add $210 billion to the deficit, so that was the flip side. But very interestingly in April, very quietly in a footnote to a very complicated report, the CBO signaled for the first time that while it could point to areas or programs in the Affordable Care Act that would bring down the deficit long term they couldn’t make a blanket assertion that the law taken together with all of its component parts would have that impact. They backed away. In a sense, they backed down, from that earlier projection.
MARY AGNES CAREY:ô Eric, there are some parts of the law the CBO can track and others that they can’t. Can you explain?
ERIC PIANIN:ô Well, I think that’s right. In terms of the insurance coverage and subsidy program to help poor people obtain insurance, the CBO can track that and has pretty good handle on its long-term budgetary impact. For other programs, like for the example, the employer mandate and a series of other policy initiatives, and segments of the program that have been temporarily put on hold or delayed, it’s much harder for them to track that.
MARY AGNES CAREY:ô You’ve been a budget reporter for a long time. Have you ever seen the CBO do this before? Come out and basically say, we just can’t score some elements.
ERIC PIANIN:ô I can’t recall anything quite like this. And I am kind of surprised by the way they did it, so quietly, in terms of a footnote. It wasn’t like, a little announcement or a separate box in one of their complicated reports — say, “Oh, by the way, we can’t do this anymore.” It was something that they — in a sense, slipped in — my guess feeling that experts who are following this issue very closely, they would immediately pick up on it.
But for the rest of us who don’t follow it in an incremental stage, it was kind of a surprise.
MARY AGNES CAREY:ô You mentioned politics a minute ago. What are the political ramifications of this?
ERIC PIANIN:ô I think from the Republican standpoint, this is just one more example of [bait and switch], in which the administration promised one thing and is delivering something else.
This isn’t the administration’s estimates. This is the independent Congressional Budget Office doing this, so I guess if [the White House Office of Management and Budget] made a pronouncement like that, it would be even more controversial. But I sense that this will be just like one more argument by the Republicans that this is a terribly flawed program that needs to be changed or done away with, according to some.
MARY AGNES CAREY:ô Do you think it will be an issue in the midterms or the presidential [campaign], or that it wouldn’t get that kind of legs?
ERIC PIANIN:ô It’s not clear. I think that maybe in some races and some venues it might be brought up as another example. And I don’t think we’ve heard the last of it. I’m sure members of Congress are bombarding Doug Elmendorf, the head of the CBO, with letters demanding explanations. My guess is we’re going to be hearing more about this at least on the Hill or in a budget context.
It’s something I’m sure the administration is worried about, because it was a great arguing point for the Affordable Care Act. Maybe this program wasn’t working. Maybe we had a terrible rollout, but in the end, ten years from now, this is going to be a good thing for the budget.
MARY AGNES CAREY:ô Thanks so much, Eric Pianin of The Fiscal Times.
ERIC PIANIN: My pleasure.
¤Öêü°å¿üë½ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFãan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/news/hoth-cbo-will-not-evaluate-some-health-law-money-after-changes/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=11392&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
Letters to the Editor is a periodic KHN feature. We welcome all comments and will publish a selection. We will edit for space, and we require full names.
The recent story, The Latest In Medical Convenience: ER Appointments (Gorman and Colliver, 7/3), drew a number of responses. Here’s an example:
Judy Lay; Lomita, Calif.
¤Öêü°å¿üë½ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFãan independent source of health policy research, polling, and journalism. Learn more about .This idea sounds fantastic. Having been a former ER registration clerk in a county and a private hospital, I know the grueling wait times for walk-ins, and I myself have brought home illnesses picked up in an urgent care waiting room. With technology in our hands and in our pockets this is an innovative way to harness its vast capabilities for the good. Another reader offered this comment regarding What The Hobby Lobby Decision Means For Employers (6/30): John Clark; Frisco, Texas Meanwhile, an insurance industry trade group offered this response to Proposal To Add Skimpier ‘Copper’ Plans To Marketplace Raises Concerns (Andrews, 7/1). Brendan Buck, vice president of communications for America’s Health Insurance Plans; Washington, D.C. Another reader shared her personal experiences after reading In Unhealthy Eastern Tennessee, Limited Patient Options Bring Some Of The Country’s Cheapest Premiums (Rau, 7/8). Kimberly K. Dorris; Scottsdale, Ariz.
This <a target="_blank" href="/health-industry/letters-to-the-editor-16/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=33471&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>