Each week, dozens of patients with diabetes come to him with deep wounds, severe infections and poor circulation — debilitating complications of a disease that has spiraled out of control. He works to save their limbs, but sometimes Armstrong and his team must resort to amputation to save the patient, a painful and life-altering measure he knows is nearly always preventable.
For decades now, the American medical establishment has known how to manage diabetes. Even as the number of people living with the illness continues to climb — today, estimated at more than 30 million nationwide — the prognosis for those with access to good health care has become far less dire. With the right medication, diet and lifestyle changes, patients can learn to manage their diabetes and lead robust lives.
Yet across the country, surgeons still perform tens of thousands of diabetic amputations each year. It’s a drastic procedure that stands as a powerful example of the consequences of being poor, uninsured and cut off from a routine system of quality health care.
“Amputations are an unnecessary consequence of this devastating disease,” said Armstrong, professor of surgery at Keck School of Medicine of USC. “It’s an epidemic within an epidemic. And it’s a problem that’s totally ignored.”
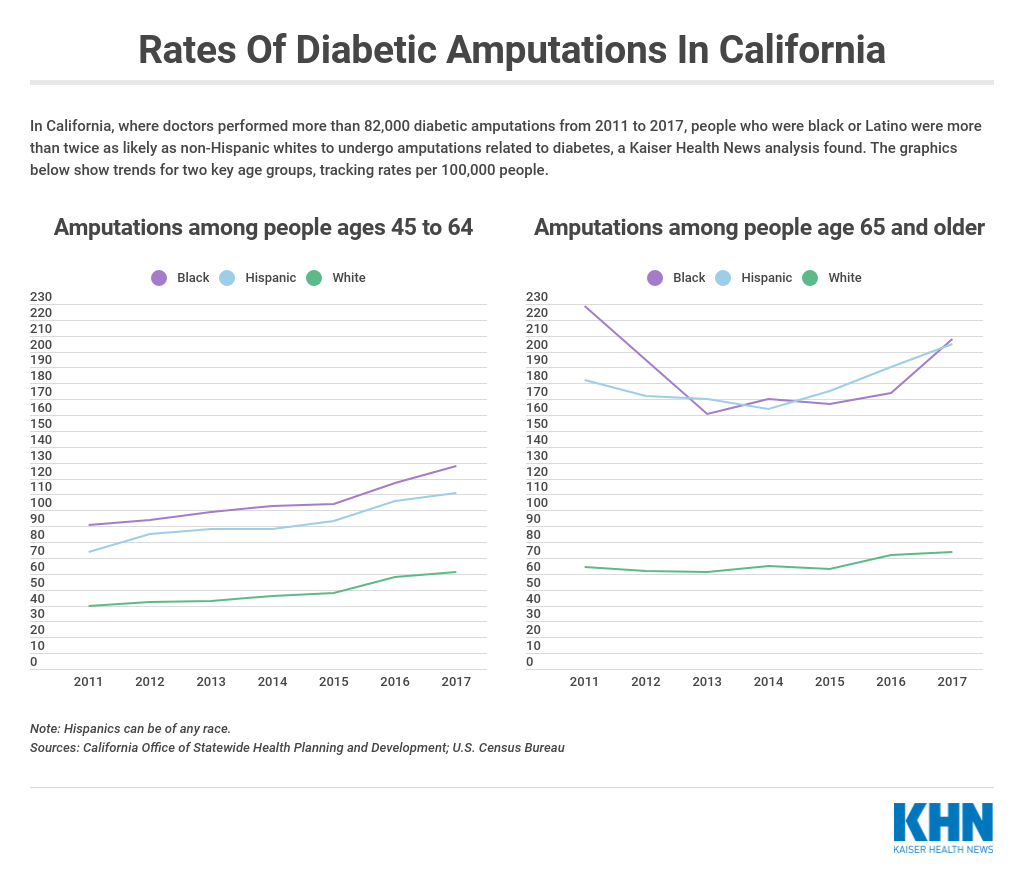
In California, where doctors performed more than 82,000 diabetic amputations from 2011 to 2017, people who were black or Latino were more than twice as likely as non-Hispanic whites to undergo amputations related to diabetes, a Kaiser Health News analysis found.
The pattern is not unique to California. Across the country, studies have shown that diabetic amputations vary significantly not just by race and ethnicity but also by income and geography. Diabetic patients living in communities that rank in the nation’s bottom quartile by income were nearly 39% more likely to undergo major amputations compared with people living in the highest-income communities, according to one .
A by UCLA researchers found that people with diabetes in poorer neighborhoods in Los Angeles County were twice as likely to have a foot or leg amputated than those in wealthier areas. The difference was more than tenfold in some parts of the county.
Amputations are considered a “mega-disparity” and dwarf nearly every other health disparity by race and ethnicity, said Dr. Dean Schillinger, a medical professor at the University of California-San Francisco. To begin with, people who are black or Latino are more at risk of diabetes than other groups ‚Äî a disparity often attributed to socioeconomic factors such as higher rates of poverty and lower levels of education. They also may live in environments with less access to healthy food or places to exercise.
Then, among those with the disease, blacks and Latinos often get diagnosed after the disease has taken hold and have more complications, such as amputations. “If you go into low-income African American neighborhoods, it is a war zone,” said Schillinger, former chief of the Diabetes Prevention and Control Program at the California Department of Public Health. “You see people wheeling themselves around in wheelchairs.”
Part of the outrage for researchers is that medical science has made so much headway in diabetes treatment. Nationwide, fewer than get amputations.
But for those who do, the consequences are profound. More than half of amputations in California from 2011 to 2017 occurred among people ages 45 to 64, according to the KHN analysis, meaning many people are left disabled and dependent on others for care during their prime working years.
From Mother To Son
Jackson Moss leaned back on his couch and raised his right leg. His wife, Bernadette, sprayed antiseptic on a gaping wound on the sole of his foot before dabbing it with Vaseline and rewrapping it with gauze.
A stocky man who used to deliver poultry, Moss, 47, said he had to stop working after his left leg was amputated below the knee about 10 years ago. Later, he lost part of his right foot. With Bernadette’s help, he is trying to save the rest of it.
“If I didn’t have my wife, I don’t know where I’d be,” said Moss, who wears a prosthesis on his left leg and uses a wheelchair. “I can’t get around good like I used to.”
Moss, who lives in Compton, embodies many of the characteristics of people most likely to get diabetic amputations. He is African American with a relatively low family income: about $30,000 a year from his Social Security disability check and his wife’s job with the county mental health department.
Moss has not always received regular medical care. His mother, who also had a leg amputated from diabetes, would take him to the doctor when he was a boy. But he stopped going as an adult. He didn’t have insurance during much of his 20s and 30s. Medical care just wasn’t a priority, he said, until about 25 years ago when his blood sugar shot up so high he passed out at home.

After he was diagnosed with Type 2 diabetes, he started seeing a physician more often. He tried to avoid sugar, as his doctor recommended, but bad habits die hard. “It takes a lot to eat right,” he said, “and it costs more.”
One day, about 10 years ago, he bumped his toe on the bed. He thought little of it until he developed an infected wound. A fever sent him to the hospital, where his lower leg was removed. A few years later, with his diabetes still poorly controlled, he lost the toes on his other foot.
In recent years, Moss and his wife said, health providers have sometimes ignored their concerns. They recalled trips to the emergency room when they had to convince doctors his fever came from a diabetes-related infection. “They wouldn’t take my word,” he said. The couple did not see it as discrimination, more like dismissiveness.
Now, Moss goes to a clinic run by Martin Luther King, Jr. Community Hospital, which serves a large Latino and black population in South Los Angeles. On a recent visit, his doctor asked if he was staying off the foot with the wound. “I just get up when I have to go to the restroom and to get in and out of the bed,” Moss responded.
Moss hopes someday he will be able to do more — get back to taking his grandsons to Chuck E. Cheese or playing dominoes with friends.
“I just sit here all day long,” he said.

‚ÄòThe Most Shameful Metric’
Amputations typically start with poorly controlled diabetes, a disease characterized by excess sugar in the blood. Untreated, it can lead to serious complications such as kidney failure and blindness.
People with diabetes often have reduced sensation in their feet, as well as poor circulation. of people with the most common form — Type 2 — develop foot ulcers or a break in the skin that can become infected.
Amputations occur after those infections rage out of control and enter the bloodstream or seep deeper into the tissue. People with diabetes often have a condition that makes it harder for blood to circulate and wounds to heal.
The circumstances that give rise to amputations are complex and often intertwined: Patients may avoid doctors because their family and friends do, or clinics are too far away. Some may delay medical visits because they don’t trust doctors or have limited insurance. Even when they seek treatment, some find it difficult to take medication as directed, adhere to dietary restrictions or stay off an infected foot.
Californians with diabetes who have a regular place to go for health care other than the emergency room are less likely to get amputations, according to an analysis conducted for Kaiser Health News by the UCLA Center for Health Policy Research. If they have a plan to control their diabetes, they also have less chance of amputation.
The analysis shows that many amputations could be avoided with better access to care and better disease management, said Ninez Ponce, director of the center.
“It’s the most shameful metric we have on quality of care,” Ponce said. “It is a health equity issue. We are a very rich state. We shouldn’t be seeing these diabetic amputations.”
An amputation often leads to a cascade of setbacks: more infections, more amputations, decreased mobility, social isolation. as many as three-quarters of people with diabetes who have had lower-limb amputations die within five years.

The health system bears surprisingly large costs for what remains a relatively uncommon problem. A single lower-limb amputation can cost more than $100,000. By far, government programs — Medicaid and Medicare — pay for the most amputations.
Experts say the best bet is to intervene well before they become necessary. People with diabetes are “very much in need of the simplest, basic, cost-effective, easy-to-implement treatments,” said Dr. Philip Goodney, director of the Center for the Evaluation of Surgical Care at Dartmouth.
Along with basic measures to control diabetes, regular foot exams are key. The Centers for Disease Control and Prevention estimates somewhere between 11% and 28% of people with diabetes get the recommended podiatric care, a yearly foot exam to check for loss of sensation and blood flow. Under federal rules governing Medicaid, the government program for low-income Americans, such care is optional and not covered by every state.
California includes it as an optional benefit, limiting access to such care. An by UCLA researchers estimated that the use of preventive podiatric services saved the Medi-Cal system ‚Äî California’s version of Medicaid ‚Äî up to $97 million in 2014, based on avoided hospital admissions and amputations, and that savings could be much greater if more patients had access.
Fighting For Jesse
Jesse Guerrero is 12, but already knows what diabetes ‚Äî and amputations ‚Äî can do to a family. He has seen how life changed since his mom, Patricia Zamora, had her first surgery. She had to stop working as a group home supervisor. They were evicted and eventually moved into his grandmother’s house in Pomona.
Now, they stay home a lot more than they used to. “I want her to get better so we can finally go places,” Jesse said.
First diagnosed with gestational diabetes, Zamora, 49, eventually was diagnosed with conventional Type 2. Though her mother has diabetes, she said, she didn’t understand the risks.
Her serious troubles started in 2014, when she stubbed her big toe and it turned black and purple. When she finally went to an ER, doctors said it had to be amputated. The next year, after another stumble and another infection, doctors removed the remaining toes on her right foot.


Now, she is fighting a third wound and risks losing the limb below her knee. She uses a scooter and wears a boot to keep the pressure off.
Many days, she wants to give up.
“But I can’t,” she said. “I have Jesse.”
His health is also a concern. Though only in middle school, Jesse is overweight, putting him at greater risk for Type 2 diabetes. She recently took away his PlayStation and signed him up for flag football so he would be more active.
Jesse, too, is scared.
“I don’t want to get my foot cut off,” he said. “I’d rather have a full life than a short one.”
The Gift Of Pain
As hospitals have seen the impacts — and cost — of amputations, some have made efforts to reduce them. Some, like Keck Hospital, have started limb preservation centers, which use cross-disciplinary teams and technology to treat wounds and help patients improve disease management.
Even with a team of specialists, however, saving a limb often depends on patients coming in early rather than waiting until their foot has become dangerously infected. But because their sensation is dulled, they often don’t appreciate the danger.
“How do you get someone to come in if they don’t have pain?” Armstrong said. “They need the gift of pain.”
One of Armstrong’s patients, Cirilo Delgado, has a wound on his heel that could cost him his lower leg. He already lost a toe.
Delgado, 41, knew diabetes ran in his family. His father, 68, has diabetes. His mother, who had diabetes and kidney failure, died at 67. His diabetic sister died at 35 of a heart attack, a possible complication of diabetes.
“I saw them die young,” he said. “I don’t want to be the next one.”
Like Moss, Delgado didn’t always have insurance. And he didn’t seek care for his diabetes until the symptoms got dire.
Delgado used to work at a dry cleaning shop but had to stop because he doesn’t have the balance he once did. His blood pressure fluctuates dangerously, and he needs dialysis three times a week for kidney failure. He has moved in with his father, a truck driver who stopped working to help care for him.
In November, doctors used a skin flap from his leg to try to heal his latest wound. He’s praying he doesn’t get another.
“I know there’s a prosthesis,” he said, “but it’s not the same as a limb.”
METHODOLOGY BOX:
Kaiser Health News analyzed 2011-17 data from California’s Office of Statewide Health Planning and Development (OSHPD) on diabetes patients discharged after lower-limb amputations. OSPHD grouped the amputations into these racial and ethnic categories: white, black, Hispanic and other; and these age groups: under 45, 45-64, 65 and over. To compare amputation rates across groups, KHN calculated crude rates using California population data for each year from the U.S. Census Bureau, and calculated the final age-adjusted rate for each racial/ethnic group using U.S. 2010 population distribution as weights.
California Healthline ethnic media editor Ngoc Nguyen and Kaiser Health News data editor Elizabeth Lucas contributed to this report.
This <a target="_blank" href="/public-health/diabetic-amputations-a-shameful-metric-of-inadequate-care/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=942727&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
It can be republished for free.
A record number of homeless people — 918 last year alone — are dying across Los Angeles County, on bus benches, hillsides, railroad tracks and sidewalks.
Deaths have jumped 76% in the past five years, outpacing the growth of the homeless population, according to a KHN analysis of the coroner’s data.
Health officials and experts have not pinpointed a single cause for the sharp increase in deaths, but they say rising substance abuse may be a major reason. The surge also reflects growth in the number of people who are chronically homeless and those who don’t typically use shelters, which means more people are living longer on the streets with serious physical and behavioral health issues, they say.
“It is a combination of people who are living for a long time in unhealthy situations and who have multiple health problems,” said Michael Cousineau, a professor at the Keck School of Medicine of the University of Southern California. “There are more complications, and one of those complications is a high mortality rate. It’s just a tragedy.”
Nearly 53,000 people were homeless in L.A. County last year, according to a of homeless residents, an increase of about 39% since 2014. The majority were not living in shelters.
The homeless population has also grown nationwide, but there is no national count of homeless deaths.
The Los Angeles County Department of Medical Examiner-Coroner considers someone homeless if that person doesn’t have an established residence, or if the body was found in an encampment, shelter or other location that suggests homelessness.
Based on that criteria, the coroner reported 3,612 deaths of homeless people in L.A. County from 2014 to 2018.
A detailed look at the numbers reveals a complex picture of where — and how — homeless people are dying.
One-third died in hospitals and even more died outside, in places such as sidewalks, alleyways, parking lots, riverbeds and on freeway on-ramps.
Male deaths outnumbered female deaths, but the percentage of homeless women who died increased faster than that of men. And although black people make up fewer than one-tenth of the county’s population, they accounted for nearly a quarter of the homeless deaths.
“We need to take action now,” said Rev. Andy Bales, CEO of the Union Rescue Mission, a homeless shelter on L.A.’s skid row. “Otherwise next year it’s going to be more than 1,000.”

Substance Abuse
Drugs and alcohol played a direct role in at least a quarter of the deaths of homeless people over the past five years, according to the analysis of the coroner’s data. It likely contributed to many more, including some whose deaths were related to liver and heart problems.
The coroner’s cause of death determination “doesn’t necessarily tell the whole story,” said Brian Elias, the county’s chief of coroner investigations, who called the increase “alarming.”
A person who is homeless may get an infection on top of a chronic disease on top of a substance abuse disorder ‚Äî and all of those together lead to bad outcomes. “It’s a house of cards,” said Dr. Coley King, a physician at the Venice Family Clinic.
Raymond Thill was just 46 when he died last year of what his wife, Sherry Thill, called complications related to alcoholism. The couple had been homeless for many years before moving into a small apartment in South Los Angeles shortly before his death.
Thill said her husband often drank vodka throughout the day and had been in and out of the hospital because of liver and other health problems. He tried rehab and she tried taking the alcohol away. Nothing worked, she said.
“His mind was set,” she said. “So I took care of him.”
In the end, Thill said, cirrhosis left her husband jaundiced, swollen and unable to keep food down.
King treated Raymond Thill and said he is convinced that Thill would have lived longer if he’d been off the streets earlier.
“This shouldn’t be happening,” especially when many deaths could have been prevented with better access to health care and housing, said David Snow, a sociology professor at the University of California-Irvine. “If you are on the streets, you are not getting the attention you need.”

‚ÄòReady For Bad Luck To Happen’
Homeless residents in Los Angeles also died from the same ailments as the general population — heart disease, cancer, lung disease, diabetes and infections. But they did so at a much younger age, said Dr. Paul Gregerson, who treats homeless residents as chief medical officer for JWCH Institute clinics in the Los Angeles area.
A stressful lifestyle, lack of healthy food and exposure to the weather contribute to an early death, he said. “If you are homeless, your body ages faster from living outside,” Gregerson said.
In Los Angeles County, the average age of death for homeless people was 48 for women and 51 for men. The for women in California in 2016 was 83 and 79 for men — among the best longevity statistics in the nation.
Over the five-year period in L.A. County, there also was a sharp increase in deaths of younger adults who were homeless. For instance, the deaths of adults under 45 more than doubled.

The data does not include information about mental illnesses, which Elias of the coroner’s office said could be a contributing factor in some of the deaths.
Stephen Rosenstein, 59, was walking across the street in Panorama City, an L.A. neighborhood, when a car struck and killed him one night early last year, said his sister, Cindy Garcia. He had spent years bouncing from the streets to shelters to board-and-care homes, she said.
Rosenstein had been diagnosed with schizophrenia and manic depression, Garcia said, and often resisted help ‚Äî behavior she attributed to his mental illness. “Most people would want to have a roof over your head,” she said. “He just fought it all the way.”
Rosenstein’s cause of death was listed as “traumatic injuries.” Deaths by trauma or violence were common among the homeless in the period analyzed: At least 800 people died from trauma, and of those, about 200 were shot or stabbed.
“They are ready for bad luck to happen,” King said.
This <a target="_blank" href="/mental-health/the-homeless-are-dying-in-record-numbers-on-the-streets-of-l-a/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=941824&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The efforts ‚Äî funded with roughly $8 million from the federal government’s Centers for Disease Control and Prevention ‚Äî are taking place at 50 facilities in those two states.
This novel approach recognizes that superbugs don’t remain isolated in one hospital or nursing home but move quickly through a community, said Dr. John Jernigan, who directs the CDC’s office on health care-acquired infection research.
“No health care facility is an island,” Jernigan said. “We all are in this complicated network.”
At least 2 million people in the U.S. become infected with an antibiotic-resistant bacterium each year, and about 23,000 die from those infections, according to the CDC.
People in hospitals are vulnerable to these bugs, and people in nursing homes are particularly vulnerable. Up to harbor drug-resistant organisms, though not all of them will develop an infection, said Dr. Susan Huang, who specializes in infectious diseases at the University of California-Irvine.
“Superbugs are scary and they are unabated,” Huang said. “They don’t go away.”
Some of the most common bacteria in health care facilities are methicillin-resistant Staphylococcus aureus, or MRSA, and carbapenem-resistant Enterobacteriaceae, or , often called “nightmare bacteria.” E. coli and Klebsiella pneumoniae are two common germs that can fall into this category when they become resistant to last-resort antibiotics known as . CRE bacteria cause an estimated 600 deaths each year, according to the CDC.
CREs have “basically spread widely” among health care facilities in the Chicago region, said , an infectious-diseases specialist at Rush University Medical Center, who is heading the CDC-funded effort there. “If MRSA is a superbug, this is the extreme ‚Äî the super superbug.”
Containing the dangerous bacteria has been a challenge for hospitals and nursing homes. As part of the CDC effort, doctors and health care workers in Chicago and Southern California are using the antimicrobial soap chlorhexidine, which to reduce infections when patients bathe with it. Though chlorhexidine is frequently used for bathing in hospital intensive care units and as a mouthwash for dental infections, it is used less commonly for bathing in nursing homes.
In Chicago, researchers are working with 14 nursing homes and long-term acute care hospitals, where staff are screening people for the CRE bacteria at admission and bathing them daily with chlorhexidine.
The Chicago project, which started in 2017 and ends in September, includes a campaign to promote handwashing and increased communication among hospitals about which patients carry the drug-resistant organisms.
The infection-control work was new to many nursing homes, which don’t have the same resources as hospitals, Lin said.
In fact, three-quarters of nursing homes in the U.S. received citations for infection-control problems over a four-year period, according to a Kaiser Health News analysis, and the facilities with repeat citations almost never were fined. Nursing home residents often are sent back to hospitals because of infections.
In California, health officials are closely watching the CRE bacteria, which are less prevalent there than elsewhere in the country, and they are trying to prevent CRE from taking hold, said Dr. Matthew Zahn, medical director of epidemiology at the Orange County Health Care Agency. “We don’t have an infinite amount of time,” he said. “Taking a chance to try to make a difference in CRE’s trajectory now is really important.”
The CDC-funded project in California is based in Orange County, where 36 hospitals and nursing homes are using the antiseptic wash along with an iodine-based nose swab. The goal is to prevent new people from getting drug-resistant bacteria and keep the ones who already have the bacteria on their skin or elsewhere from developing infections, said Huang, who is leading the project.
Huang kicked off the project by studying how patients move among different hospitals and nursing homes in Orange County, and discovered they do so far more than imagined. That prompted a key question: “What can we do to not just protect our patients but to protect them when they start to move all over the place?” she recalled.
Her previous research showed that patients with the MRSA bacteria who used chlorhexidine for bathing and as a mouthwash, and swabbed their noses with a nasal antibiotic, could reduce their risk of developing a MRSA infection by 30%. But all the patients in that study, published in February in the , already had been discharged from hospitals.
Now the goal is to target patients still in hospitals or nursing homes and extend the work to CRE. The traditional hospitals participating in the new project are focusing on patients in intensive care units and those who already carried drug-resistant bacteria, while the nursing homes and the long-term acute care hospitals perform the cleaning ‚Äî also called “decolonizing” ‚Äî on every resident.
One recent morning at Coventry Court Health Center, a nursing home in Anaheim, Calif., 94-year-old Neva Shinkle sat patiently in her wheelchair. Licensed vocational nurse Joana Bartolome swabbed her nose and asked if she remembered what it did.
“It kills germs,” Shinkle responded.
“That’s right ‚Äî it protects you from infection.”





In a nearby room, senior project coordinator Raveena Singh from UC-Irvine talked with Caridad Coca, 71, who had recently arrived at the facility. She explained that Coca would bathe with the chlorhexidine rather than regular soap. “If you have some kind of open wound or cut, it helps protect you from getting an infection,” Singh said. “And we are not just protecting you, one person. We protect everybody in the nursing home.”
Coca said she had a cousin who had spent months in the hospital after getting MRSA. “Luckily, I’ve never had it,” she said.
Coventry Court administrator Shaun Dahl said he was eager to participate because people were arriving at the nursing home carrying MRSA or other bugs. “They were sick there and they are sick here,” Dahl said.
Results from the Chicago project are pending. Preliminary results of the Orange County project, which ends in May, show that it seems to be working, Huang said. After 18 months, researchers saw a 25% decline in drug-resistant organisms in nursing home residents, 34% in patients of long-term acute care hospitals and 9% in traditional hospital patients. The most dramatic drops were in CRE, though the number of patients with that type of bacteria was smaller.
The preliminary data also shows a promising ripple effect in facilities that aren’t part of the effort, a sign that the project may be starting to make a difference in the county, said Zahn of the Orange County Health Care Agency.
“In our community, we have seen an increase in antimicrobial-resistant infections,” he said. “This offers an opportunity to intervene and bend the curve in the right direction.”
This <a target="_blank" href="/health-industry/how-to-fight-scary-superbugs-cooperation-and-a-special-soap/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=934289&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Patients heavily sedated or shackled to gurneys for days while awaiting placement in a specialized psychiatric hospital, their symptoms exacerbated by the noise and chaos of emergency medicine. Long wait times in crowded ERs for people who show up with serious medical emergencies. High costs for taxpayers, insurers and families as patients languish longer than necessary in the most expensive place to get care.
“If you are living with schizophrenia or bipolar disorder, that is a really tough way to begin that road to recovery,” said Dr. Jack Rozel, president of the American Association for Emergency Psychiatry.
In pockets across the country, hospitals are trying something new to address the unique needs of psychiatric patients: opening emergency units specifically designed to help stabilize and treat patients and connect them to longer-term resources and care. These psychiatric ERs aim to address the growing number of patients with mental health conditions who end up hospitalized because traditional emergency rooms don’t have the time or expertise to treat the crisis.
The rate of ER visits involving psychoses, bipolar disorder, depression or anxiety from 2006 to 2013, according to the federal Agency for Healthcare Research and Quality. Roughly 1 in 8 emergency department visits now stem from mental illness or substance use disorders, the data show.
The psychiatric ERs, staffed with nurses, social workers and psychiatrists, work to treat and release patients in under 24 hours, much as traditional emergency rooms handle physical ailments. Those who are well enough to go home get discharged, while those who need more treatment are admitted to the hospital or transferred to an inpatient facility.
There are now roughly 100 such units across the country, said Dr. Scott Zeller, vice president of acute psychiatry at Vituity, a physician-led organization that provides staffing and consulting services to medical centers nationwide.
Zeller pioneered the approach while working as chief of psychiatric emergency services at John George Psychiatric Hospital in Alameda County, Calif. Over time, he transformed the center from a traditional ward where restraints were common into one that treated patients in a more supportive, living-room like setting. The results — in terms of both patient outcomes and cost-savings — made Zeller a believer.
He is helping design 10 , including in California, Florida, Illinois and Tennessee. Each is distinct, accepting patients in somewhat different circumstances and offering a slightly different range of services.
Patients who arrive at an emergency room for psychiatric or substance use disorders are more than twice as likely to be admitted than other patients, federal data show. And yet about 80 percent of the time, Zeller said, patients’ mental health crises can be resolved without a costly inpatient hospital stay. A patient may be having a psychotic episode because he fell off his medications, for example, or having drug-induced hallucinations.
“We need to treat people at the emergency level of care,” he said. “The vast majority of psychiatric emergencies can be resolved in less than 24 hours.”
Nowhere To Hide
Wearing a hospital gown, Rachel Diamond lay back in her recliner in a spacious room in a relatively new ward at Providence Little Company of Mary Medical Center San Pedro, a hospital near the Port of Los Angeles. Nearby, a few patients slept on identical recliners, draped in soft blankets. Others communed at a kitchen table over microwaved meals. A nurse walked through the locked unit with a rolling cart, dispensing medications.
Except for a nursing station in the middle of the room, the unit didn’t look much like a health care facility. The room was divided into men’s and women’s sides, with separate TVs. A few smaller rooms ‚Äî where patients could meet with a psychiatrist or social worker ‚Äî lined the unit’s edge.

Anya Price, interim clinical supervisor and a nurse, said the unit was designed to feel more like a home than a hospital. “We’re operating from an understanding that they’re coming here to get better,” Price said.
The open design of the unit, known as the “Outpatient Behavioral Health Center,” allows patients to move freely. Staff said it also helps reduce problems because they can quickly spot a patient who may be getting agitated. Dr. Herbert Harman, a psychiatrist and medical director for the facility, said violence and the need for restraints are rare.
The unit is in a building a short walk from the medical center emergency room. It opened in 2017 and accepts patients from emergency rooms across Los Angeles County once they are deemed stable medically. So far this year, its staff has treated about 400 patients, Price said.
One recent morning, the patients included a man in his 40s found on the railroad tracks after an alcohol binge, and a woman with a history of schizophrenia who said she was seeing spirits. Some were there on involuntary holds because authorities had decided they were at risk of hurting themselves or others because of their illness.



Diamond, 30, said she has been diagnosed with depression and anxiety and has landed in multiple ERs over the past decade when her symptoms spiked out of control. During those stays, she said, she often felt isolated and in the dark about her treatment. Doctors typically numbed her with medications and consigned her to a guarded room. “No one really talked to me,” said Diamond, who lives in Torrance, Calif. “It was like I was a caged animal.”
She had been living in a car and fighting with her boyfriend in late February when she decided she wanted to end her life. She tried jumping out of a moving car, and when that didn’t work, she grabbed a bottle of pills. She gets help for her mental health issues, but sometimes, she said, the stress becomes too much. This time, she was taken to a hospital emergency room in Torrance before being transferred to the San Pedro unit.
During her time in the behavioral health center — about 26 hours — she slept, received medications and met with nurses, a social worker and a psychiatrist. She said it was calmer than a regular ER, and the staff had time to talk, listen and help her through the worst of the crisis.
“I genuinely feel better enough to leave,” she said. “I haven’t been able to say that in a while.”
A Return On Investment
Zeller argues that the use of emergency psychiatric clinics is both humane and cost-effective. on the Alameda County model found such units can dramatically reduce how long patients spend in medical emergency rooms, and that about three-quarters of patients treated in the units can be discharged to the community rather than to inpatient care. That, Zeller said, can lessen the overwhelming demand for inpatient psychiatric beds and preserve available spots for those who truly require them. The model saves money for hospitals in part because the patients spend less time in emergency care.
“The return on investment is exponential,” he said.
In Montana, the Billings Clinic opened a psychiatric stabilization unit last April across the street from the traditional ER. Dr. Eric Arzubi, psychiatry department chair, said nearly 10 percent of the visits in the Billings Clinic emergency room involve people in psychiatric crisis. Since the new unit opened, wait times for psychiatric patients have dropped from about 10 hours to four hours, and fewer patients are being admitted to the inpatient unit. Arzubi said his staff isn’t trying to cure people of their mental illness but rather stabilize them and get them the care they need.
“Just like in the emergency room, you don’t get comprehensive care,” Arzubi said. “But you can stop the bleeding, you stabilize the patient and get them to the right level of care.”
In some cases, that means a transfer to an inpatient facility.


Staff at the San Pedro unit decided soon after Chantelle Unique arrived that she would be one of those patients. Unique, who is 23, has been diagnosed with bipolar disorder and schizophrenia. She had been dancing on the roof and speaking gibberish when her mother called 911.
Unique said she has had a hard time in regular emergency rooms. “There are a million people,” she said. For most of a morning at the San Pedro facility, she sat calmly watching TV, talking to nurses and eating spaghetti. But at one point, she started pacing and yelling at other patients. Nurses and security guards quickly surrounded her and persuaded her to return to her recliner and take additional medication.
Finding an inpatient bed for a patient like Unique with more progressed mental illness is not always easy, said clinical social worker Mark Tawfik. But he’s committed to finding a way. “We have to make sure we find them adequate resources,” he said. “Otherwise, they will come right back.”
For Price, the clinical supervisor, even when a patient requires a transfer for more intensive care, there’s satisfaction in knowing that person is headed in the right direction. If Unique hadn’t been brought in, Price said, she would have been out in the community, lost to her delusions, putting herself at risk of accident or arrest.
In the unit, staff made sure she was safe, Price said, in addition to providing “a warm bed, some food and some compassion.”
This <a target="_blank" href="/health-industry/she-was-dancing-on-the-roof-and-talking-gibberish-a-special-kind-of-er-helped-her/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=931263&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But this homeless encampment off a Hollywood freeway ramp is often littered with needles and trash, and soaked in urine. Rats occasionally scamper through, and Millar fears the consequences.
“I worry about all those diseases,” said Millar, 43, who said she has been homeless most of her life.
Infectious diseases — some that ravaged populations in the Middle Ages — are resurging in California and around the country, and are hitting homeless populations especially hard.
Los Angeles recently experienced an outbreak of typhus — a disease spread by infected fleas on rats and other animals — in downtown streets. Officials briefly closed part of City Hall after reporting that rodents had invaded the building.
People have been infected with Shigella bacteria, which is spread through feces and causes the diarrheal disease shigellosis, as well as Bartonella quintana, which spreads through body lice and causes trench fever.
Hepatitis A, also spread primarily through feces, infected more than 1,000 people in Southern California in the past two years. The disease in New Mexico, Ohio and Kentucky, primarily among people who are homeless or use drugs.
Public health officials and politicians are using terms like “disaster” and “public health crisis” to describe the outbreaks, and they warn that these diseases can easily jump beyond the homeless population.
“Our homeless crisis is increasingly becoming a public health crisis,” California Gov. Gavin Newsom said in his State of the State speech in February, citing outbreaks of hepatitis A in San Diego County, syphilis in Sonoma County and typhus in Los Angeles County.
“Typhus,” he said. “A medieval disease. In California. In 2019.”
The diseases have flared as the nation’s has grown in the past two years: About 553,000 people were homeless at the end of 2018, and nearly one-quarter of homeless people live in California.
The diseases spread quickly and widely among people living outside or in shelters, fueled by sidewalks contaminated with human feces, crowded living conditions, weakened immune systems and limited access to health care.
“The hygiene situation is just horrendous” for people living on the streets, said Dr. Glenn Lopez, a physician with St. John’s Well Child & Family Center, who treats homeless patients in Los Angeles County. “It becomes just like a Third World environment where their human feces contaminate the areas where they are eating and sleeping.”
Those infectious diseases are not limited to homeless populations, Lopez warned. “Even someone who believes they are protected from these infections are not.”

At least one said she contracted typhus in City Hall last fall. And San Diego County officials warned in 2017 that diners at a well-known restaurant were at risk of hepatitis A.
There were 167 cases of typhus from Jan. 1, 2018, through Feb. 1 of this year, up from 125 in 2013 and 13 in 2008, according to the .
Typhus is a bacterial infection that can cause a high fever, stomach pain and chills but can be treated with antibiotics. Outbreaks are more common in overcrowded and trash-filled areas that attract rats.
The recent typhus outbreak began last fall, when health officials reported clusters of the flea-borne disease in downtown Los Angeles and Compton. They also have occurred in Pasadena, where the problems are likely due to people feeding stray cats carrying fleas.
Last month, the county announced another outbreak in downtown Los Angeles that infected nine people, six of whom were homeless. After city workers rodent droppings in City Hall, Los Angeles City Council President Herb Wesson briefly shut down his office to rip up the rugs, and he also called for an investigation and more cleaning.
Hepatitis A is caused by a virus usually transmitted when people come in contact with feces of infected people. Most people recover on their own, but the disease can be very serious for those with underlying liver conditions. There were 948 cases of hepatitis A in 2017 and 178 in 2018 and 2019, the state public health department said. Twenty-one as a result of the 2017-18 outbreak.
Typhus. A medieval disease. In California. In 2019.
Gov. Gavin Newsom
The infections around the country are not a surprise, given the lack of attention to housing and health care for the homeless and the dearth of bathrooms and places to wash hands, said Dr. Jeffrey Duchin, the health officer for , Wash.
“It’s a public health disaster,” he said.
In his area, Duchin said, he has seen shigellosis, trench fever and skin infections among homeless populations.
In New York City, where more of the homeless population lives in shelters rather than on the streets, there have not been the same outbreaks of hepatitis A and typhus, said Dr. Kelly Doran, an emergency medicine physician and assistant professor at NYU School of Medicine. But Doran said different infections occur in shelters, including tuberculosis, a disease that spreads through the air and typically infects the lungs.
The diseases sometimes get the “medieval” moniker because people in that era lived in squalid conditions without clean water or sewage treatment, said Dr. Jeffrey Klausner, a professor of medicine and public health at UCLA.
People living on the streets or in homeless shelters are vulnerable to such outbreaks because their weakened immune systems are worsened by stress, malnutrition and sleep deprivation. Many also have mental illness and substance abuse disorders, which can make it harder for them to stay healthy or get health care.


One recent February afternoon, Saban Community Clinic physician assistant Negeen Farmand walked through homeless encampments in Hollywood carrying a backpack with medical supplies. She stopped to talk to a man sweeping the sidewalks. He said he sees “everything and anything” in the gutters and hopes he doesn’t get sick.
She introduced herself to a few others and asked if they had any health issues that needed checking. When she saw Millar, Farmand checked her blood pressure, asked about her asthma and urged her to come see a doctor for treatment of her , a viral infection spread through contaminated blood that can lead to serious liver damage.
“To get these people to come into a clinic is a big thing,” she said. “A lot of them are distrustful of the health care system.”
On another day, 53-year-old Karen Mitchell waited to get treated for a persistent cough by St. John’s Well Child & Family Center’s mobile health clinic. She also needed a tuberculosis test, as required by the shelter where she was living in Bellflower, Calif.
Mitchell, who said she developed alcoholism after a career in pharmaceutical sales, said she has contracted pneumonia from germs from other shelter residents. “Everyone is always sick, no matter what precautions they take.”
During the hepatitis A outbreak, public health officials administered widespread vaccinations, cleaned the streets with bleach and water and installed hand-washing stations and portable toilets near high concentrations of homeless people.
But health officials and homeless advocates said more needs to be done, including helping people access medical and behavioral health care and affordable housing.
“It really is unconscionable,” said Bobby Watts, CEO of the National Health Care for the Homeless Council, a policy and advocacy organization. “These are all preventable diseases.”
This <a target="_blank" href="/public-health/medieval-diseases-flare-as-unsanitary-living-conditions-proliferate/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=924299&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>These and other health and safety problems were detailed in two reports released Tuesday. The reports, produced by state Attorney General Xavier Becerra and California , found that the inadequate medical care, along with other health and safety risks, posed a serious danger to immigration detainees.
Becerra and Howle blamed the federal and local governments for failing to oversee the detention centers, allowing the health and safety violations to persist.
“Everyone in this country has constitutional rights, and everyone at the end of the day, child and adult, deserves to be treated in a humane way,” Becerra said at a news conference in San Francisco where he announced his findings.
U.S. Immigration and Customs Enforcement is committed to “ensuring all detainees are treated in a humane and professional manner,” spokeswoman Lori Haley countered in a written statement. “The safety, rights and health of detainees in ICE’s care are of paramount concern and all ICE detention facilities are subject to stringent, regular inspections.”
Haley’s statement didn’t discuss the specific findings in the reports.
Becerra described his as an initial look at conditions in the 10 California centers that housed immigration detainees in 2017, when his review began. The centers, overseen by ICE, hold people awaiting immigration hearings or deportation.
The federal centers have come under increased scrutiny as President Donald Trump has stepped up immigration enforcement, with reports of deaths, abuse and substandard medical care.
The reports landed on the same day as a on the detention of immigrants and family separation. During the hearing, Democrats questioned White House officials about the policy of taking children from their parents at the Mexican border.
Over the past three years, nearly 75,000 immigrant detainees were housed in the 10 California facilities. The immigrants, who stayed an average of more than 50 days, were held in civil, not criminal, detention.
The federal also examined detention facilities and revealed health and safety problems such as nooses in cells and “improper and overly restrictive segregation.” The inspector general also that the federal immigration agency’s own inspections are not consistent or thorough.
“The standards are so low for these detention centers, and they are not regulated the way that they should be,” said Angelica Salas, executive director of the Coalition for Humane Immigrant Rights.
In addition to one-day visits to all of the facilities, Becerra’s Department of Justice conducted more comprehensive investigations of three: the Yolo County Juvenile Detention Facility, Theo Lacey Facility in Orange County and the West County Detention Facility in Contra Costa County. Contra Costa County no longer to house immigrant detainees in the West County facility.
The department found a number of health and safety problems in the centers:
- Staff at the Yolo facility did not adequately address the mental health needs of detainees and overused psychotropic medications. One youth had been cutting himself but wasn’t put under a special watch.
- Providers conducted superficial medical examinations that failed to rule out serious injuries or health conditions, including one case in which a detainee complained of testicular pain.
- A shortage of bilingual medical staff compromised the confidentiality of medical care and made it more difficult to access care.
- Unqualified personnel, including detention officers, deputies and licensed vocational nurses, made medical decisions.
- Dental services were often delayed, including one case in which a detainee needed urgent care for a probable “tooth eruption.” Other detainees were denied fillings and root canal procedures.
Noheli Sandoval, 32, entered the U.S. in March from Venezuela seeking asylum, and spent four months at the West County Detention Facility in Richmond.
It wasn’t easy accessing medical services there, said Sandoval, who lives in Berkeley. “You have to be practically dying for them to treat you.”
To get dental care, you had to be in pain, and the waiting list for mental health help was months long, she added.
Becerra said the federal government is not ensuring its own standards are met. And while some of the facilities already have made changes, he said he will continue monitoring them to ensure they adequately address their shortcomings. He didn’t rule out legal action.
“Our work is not done,” Becerra said. “We are prepared to do whatever we must to make sure that the laws of this country and this state ‚Ķ are not only protected but enforced.”
A separate but equally damning report by the state auditor concluded that California cities that contract with ICE to house immigration detainees are not providing adequate oversight, putting the detainees’ health and safety at risk.
The report highlights health care at three detention centers: Adelanto Detention Facility in Adelanto, Mesa Verde Detention Facility in McFarland and Imperial Regional Detention Facility in Holtville.
Those cities subcontract with private businesses to manage and operate the detention facilities, but they provided “little or no oversight of the private operators and simply passed federal payments from ICE to these subcontractors,” Howle wrote in a letter to the legislature.
Most of the health concerns raised in her report occurred during an unannounced federal inspection in May at the Adelanto Detention Facility, where inspectors found that detainees had hung bedsheets, which could be used to attempt suicide. In 2017, a detainee died after staff found him hanging from his sheets. The report said there had been three other suicide attempts by hanging as well.
The inspection also revealed that medical providers at the Adelanto facility did not conduct face-to-face medical assessments of detainees in segregation, but instead performed “cursory walk-throughs.” Nor did the facility provide proper interpretation services for people seeking care, or adequate dental services. No detainees had received fillings in the last four years, the report said.
“The city takes the findings contained in the report seriously and appreciates the recommendations,” said Adelanto city spokeswoman Michelle Van Der Linden in an emailed statement. The city, she added, is in the process of forming a committee to oversee the operation of the facility.
The city of McFarland it will not renew its contract with ICE.
During the five-year period covered by the auditor, the cities did not review complaints or inspection reports, the report said.
These cities have done little “to ensure that they are living up to their responsibilities in ensuring the safety and well-being of the detainees there,” said Michael Kaufman, senior staff attorney of the ACLU of Southern California.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/mental-health/detention-centers-in-california-lack-oversight-and-proper-care-reports-find/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=922617&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Carol Marley wants everyone to know what a life-threatening cancer diagnosis looks like in America today.
Yes, it’s the chemotherapy that leaves you weak and unable to walk across the room. Yes, it’s the litany of tests and treatments ‚Äî the CT scans and MRIs and biopsies and endoscopies and surgeries and blood draws and radiation and doctor visits. Yes, it’s envisioning your funeral that torments you day and night.
But none of these is her most gnawing, ever-present concern.
That would be the convoluted medical bills that fill multiple binders, depleted savings accounts that destroy early retirement plans, and so, so many phone calls with insurers and medical providers.
“I have faith in God that that my cancer is not going to kill me,” said Marley, who lives in Round Rock, Texas. “I have a harder time believing that this is gonna get straightened out and isn’t gonna harm us financially. That’s the leap of faith that I’m struggling with.”
Coping with the financial fallout of cancer is exhausting. And nerve-wracking. But the worst part, Marley said, is that it’s unexpected. When she was diagnosed with pancreatic cancer last summer, she didn’t anticipate so many bills, or so many billing mistakes. After all, she is a hospital nurse with good, private insurance that allowed her access to high-quality doctors and medical centers.
Randall Marley, a computer systems engineer, said he frequently comes home from work to find his wife not feeling well and frustrated having spent a precious day of her recovery making phone calls to understand and dispute medical bills. One recent night she was in tears and “emotionally at a breaking point,” he said. “The hardest part of this is seeing the toll it’s taken on my wife.”

Piling On The Pain
More than 42 percent of the 9.5 million people diagnosed with cancer from 2000 to 2012 drained their life’s assets within two years, according to a study published last year in the Cancer patients are 2.65 times for bankruptcy than those without cancer, and that puts them at a higher risk for early death, according to .
But those statistics don’t convey the daily misery of a patient with a life-threatening disease trying to navigate the convoluted finances of U.S. health care, while simultaneously facing a roller coaster of treatment and healing.
Stephanie Wheeler, a professor at the University of North Carolina at Chapel Hill, said the number of bills coming from different providers can be overwhelming.
“It’s oftentimes multiple different bills that are rolling in over a period of several months and sometimes years,” said Wheeler, who has conducted with metastatic cancer patients. “As those bills start to accumulate it can be very stress-inducing.”
Given many patients cannot work during treatment, these bills may force even relatively well-to-do cancer patients to take out second mortgages, spend college savings or worry about leaving debt behind for their families, Wheeler said.
Carol Marley is a slight woman who dotes on her two dogs and is involved in her church. Her 88-year-old father, who has dementia, had moved in. She and Randall pride themselves on living frugally. They pay their credit card off every month and don’t have car payments.

Marley and her daughter, June Marley — a second-year college student — have health insurance through her employer, Ascension Health, a large, faith-based health care system with facilities across the nation. Her husband has separate insurance through his job.
They were hoping to retire early, buy an RV and drive around the country. Instead, they see their meticulous plans disappearing, even if Carol recovers. Their high-deductible insurance policy meant they had to spend $6,000 before their insurance started covering her treatment expenses. They hit their annual out-of-pocket maximum of $10,000 well before the year was over. But Carol Marley said she was prepared for that. “What I didn’t anticipate is the knock-down, drag-out fight that I would have to engage in to get people to see there were errors and address it.”
Since she’s unable to work, the family lost her nursing salary.
“Money is not coming in, and it’s going out by the thousands,” she said.
Coming To Terms With Diagnosis
Marley had treated cancer patients before. She had seen them come in with unexplained aches and leave with devastating diagnoses. Now it was her turn. Though she didn’t recognize it at the time, her symptoms were textbook. Fatigue. Back pain. Weight loss. In July, doctors told her she had pancreatic cancer.
Her first thought was that she was going to die. A nurse friend asked if she had her affairs in order. That’s because pancreatic cancer is usually discovered too late. Just 9 percent of patients are alive five years after diagnosis, compared with 90 percent of breast cancer patients. Marley knew she was lucky. Hers hadn’t spread. She might be able to undergo surgery. But first, four months of chemotherapy and five weeks of radiation.
The chemotherapy ‚Äî seven or eight rounds, she can’t quite remember ‚Äî drained her. “I couldn’t put words together in my head,” she said. She had muscle spasms and developed fevers that landed her in the emergency room.
As she became weaker, Marley realized she could no longer care for her father at home. On a recent morning in early January, Marley sat down with nurse from a memory care facility where a space had become available. Holding back tears, Marley told the nurse she knew this day would come. “I didn’t think it would be so soon, and I didn’t know under these circumstances.”
Becoming Her Own Patient Advocate
Later that same day, Marley’s energy was up. She adjusted the colorful scarf on her head, turned on her computer and pulled out a pen. Some days, Marley said, she spends hours trying to clarify and fix medical bills. “But I don’t do that frequently because it is so fruitless and it is stressful,” she said.
Often, she is just trying to figure out what different bills mean. “Even as a nurse, I feel like it’s impossible to understand,” she said. “I can’t make heads or tails of it.”
Sometimes there are errors.
Part of the problem, she contends, is that one insurance company covers visits with Ascension providers and hospitals and another company covers pharmacy claims and specialty drugs and providers outside of the Ascension network. Some of the bills, including one for $1,400 from an ER visit — were sent to the wrong insurer, she said.
Marley cited other issues. An $18,400 chemotherapy bill submitted with missing information and then denied because it arrived late. A $870 MRI bill denied because the provider said there had been no preauthorization.
“It’s not any one individual. It’s not any one system or provider,” she said. “The whole system is messed up. ‚Ķ There’s no recourse for me except to just keep making phone calls.”

On this particular afternoon, Marley has a long list of calls to make. One to figure out why she couldn’t access her insurance claims online. Another to a medical provider that urged her to pay $380, even though they acknowledged they owed her about $80 of that total.
Someone who answered the phone again suggested Marley pay the entire amount. “Once it’s posted to your account and it goes through,” the woman said, “we would send you a check.”
Marley shook her head. “I’m sure y’all are fine people over there, but I’m not trusting a refund to come,” she responded, reflecting on her experience as a consumer of cancer care. “The problem is, they want their money and they are going to get it one way or the other.”
As for her hospital bills, Ascension declined to comment, citing protected health information. But spokesman Nick Ragone said, “The matter at issue was favorably resolved.”
He did not say which issue was resolved.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/cancers-complications-confusing-bills-maddening-errors-and-endless-phone-calls/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=918921&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>“Two major public health issues are colliding,” said Dr. Sarah Kidd, a medical officer at the Centers for Disease Control and Prevention and lead author of a new report issued Thursday on the link between drugs and syphilis.
The report shows a large intersection between drug use and syphilis among women and heterosexual men. In those groups, reported use of methamphetamine, heroin and other injection drugs more than doubled from 2013 to 2017.
The data did not reveal the same increases in drug use among gay men with syphilis, the group with the highest rates of the disease.
Researchers said the results suggest that drug use — and the risky sexual behaviors associated with it — may be driving some of the increase in syphilis transmission among heterosexuals.
People who use drugs are more likely to engage in unsafe sexual behaviors, which put them at higher risk for sexually transmitted diseases, experts said. The CDC also saw increases in syphilis among heterosexuals during the crack cocaine epidemic of the 1980s and 1990s, and use of the drug was associated with higher syphilis transmission.
“The addiction takes over,” said Patricia Kissinger, an epidemiology professor at Tulane University School of Public Health and Tropical Medicine.
For example, people using drugs may avoid condoms, have multiple sex partners or exchange sex for drugs or money¬Ý‚Äî all significant risk factors for sexually transmitted diseases, said Dr. Sara Kennedy, medical director of Planned Parenthood Northern California.
“I think it’s impossible to eradicate syphilis and congenital syphilis unless we are simultaneously addressing the meth-use and IV-use epidemic,” Kennedy said.
Syphilis rates are setting records nationally. They jumped by 73 percent overall and 156 percent for women from 2013 to 2017. The highest rates were reported in Nevada, and Louisiana.
Syphilis¬Ý‚Äî which had been nearly eradicated before its resurgence in recent years¬Ý‚Äî is treatable with antibiotics, but if left untreated it can lead to organ damage and even death. , which occurs when a mother passes the disease to her unborn baby, can lead to premature birth and newborn deaths.
The study’s authors analyzed syphilis cases from 2013 to 2017 and determined which patients had also reported using drugs. They discovered methamphetamine was the biggest problem: More than one-third of women and one-quarter of heterosexual men with syphilis reported using methamphetamine within the previous year.
Substance use among both populations was highest in 13 Western states and lowest in the Northeast. In California, methamphetamine use by people with syphilis nearly doubled for women and heterosexual men from 2013 to 2017, according to the California Department of Public Health.
The intersecting epidemics of sexually transmitted infections and substance abuse make it harder to identify and treat people with syphilis because drug use makes people less likely to go to the doctor and to report their sexual partners, Kidd said.
Pregnant women also may be reluctant to seek prenatal care and get syphilis testing and treatment because of concerns their doctor will report the drug use.
To stem the transmission of syphilis, the CDC urges more collaboration between programs that address STDs and programs that treat substances abuse.
Drug use is an “incredibly huge contributing factor” to somebody getting an STD and transmitting it, said Jennifer Howell, sexual health program coordinator for the health district in Washoe County, Nev.
“Everybody needs to see that we are dealing with a lot of the same clients,” she said.
Fresno County has the highest rate of congenital syphilis in California. Its health department analyzed 25 cases of congenital syphilis in 2017 and determined that more than two-thirds of the mothers were using drugs, said Joe Prado, the county’s community health division manager.
The county has started offering STD testing for people entering inpatient drug treatment facilities, Prado said. “That’s our opportunity to get them screened,” he said.
Those who return for the results are offered incentives such as gift cards. The county also gives people in drug treatment a care package that contains condoms and education materials about sexually transmitted infections, Prado said.
The city of Long Beach sends a mobile clinic to drug treatment facilities, where it provides HIV testing, said Dr. Anissa Davis, the city’s health officer. She said Long Beach hopes to expand services to include screening for other sexually transmitted infections.
Although increased collaboration between drug treatment providers and STD clinics is essential, it’s not always easy because they traditionally have not worked together, said Kissinger of Tulane.
“The STI people are hyperfocused on STIs and the substance abuse people are focused on substance abuse,” she said. It is an “opportunity lost” if people in drug treatment aren’t screened for syphilis and other sexually transmitted infections, she added.
Fighting the rising rates of syphilis will also require more resources, said Dr. Jeffrey Klausner, a professor of medicine and public health at UCLA.
“The STD workforce has almost entirely disappeared,” he said. “While policies could be put in place that require syphilis testing, those policies also have to come with resources.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/two-crises-in-one-as-drug-use-rises-so-does-syphilis/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=918289&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Listen to KQED Politics and Government Reporter Katie Orr’s radio version of this story, which ran on .
Can’t see the audio player?
Gov. Gavin Newsom has proposed bold steps to ensure more Californians have health coverage, but a new report underscores that his success may depend in part on large-scale investments to expand the state’s health care workforce.
A coalition of health, labor and education leaders, in a released Monday, cited a dearth of health care workers in many regions of the state and recommended spending up to $3 billion over 10 years to address the shortfall. It’s not clear where that money would come from, though the report cited several possible sources.
The proposals of the group, the , include: creating more primary care and psychiatric residency slots; increasing the use of nurse practitioners; boosting scholarships for low-income students who agree to work in underserved areas; and expanding the supply — and training — of home care workers.
The commission also recommended building a more culturally and linguistically diverse pool of health care professionals to better match California’s demographics.
To meet the needs of an aging population, the commission recommended training home care workers and putting them on a more defined career path. In addition, the report focuses on shortages in mental health care, with proposals to create a new training program for psychiatric nurse practitioners and expand the use of mental health peer counselors.
“As we strive to get everyone covered ‚Ķ we need to have the providers there to actually provide the care,” said California Assemblyman Jim Wood, a commission member and chairman of the state Assembly Health Committee. “We need to realize that this is a growing state and our workforce is not growing proportionally.”
Health care providers simply aren’t working in the areas of greatest need, resulting in a two-tier system for the haves and have-nots, he said.
An estimated 7 million Californians live in shortage areas, and the problem is expected to worsen as older physicians retire, baby boomers age and more people live with chronic diseases. About 45 percent of psychiatrists and 37 percent of psychologists in the state are over 60 years old, according to research from the University of California-San Francisco.
Among the areas experiencing shortages are the San Joaquin Valley and the Inland Empire, as well as the state’s rural northern and Sierra regions, according to the commission.
The report comes less than a month after Newsom unveiled his ambitious health care agenda.
On his first day in office, the Democratic governor proposed extending Medicaid coverage to undocumented young adult immigrants, requiring all Californians to have health insurance, and supplementing federal health insurance subsidies with state money to help them pay for it. He also President Donald Trump and congressional leaders to amend federal law to allow California to move toward a single-payer health care system.
Wood said such policies would not be effective without enough providers in the places where they are needed. “Coverage isn’t care, and we can’t just say ‚ÄòEverybody’s got coverage’ and walk away,” he said. “If you don’t have access to physicians or dentists or mental health providers in your area, that is an empty promise.”
The in August 2017 by several health philanthropies hoping to forge a strategy to build the workforce needed by 2030. It consisted of two dozen representatives from hospitals, schools, businesses and labor, and was chaired by University of California President Janet Napolitano and Dignity Health president and CEO Lloyd Dean.
Some of the commission’s proposals would face challenges ‚Äî especially financial ones. Creating more residencies for primary care physicians and psychiatrists, for example, would cost an estimated $1.56 billion over a decade. And the state’s physicians are likely to oppose giving nurse practitioners more authority.
C. Dean Germano, CEO of Shasta Community Health Center in Redding, Calif., said his community has significant mental health needs and that health centers are often the first place many people go for treatment of depression or anxiety.
“We are sort of handicapped by not having the workforce on the primary care side or on the mental health side,” he said, adding that training students to work in underserved communities is the “golden ticket.”
In Los Angeles County, L.A. Care Health Plan is already working to expand the primary care workforce by offering full scholarships to certain medical school students and loan repayment for physicians recruited to practice in underserved areas.
Investing in more health care professionals — especially primary care providers — can help reduce the overall cost of health care, said Dr. David Carlisle, president and CEO of Charles R. Drew University of Medicine and Science in Los Angeles who served on the commission. The state is expected to need an in 2030.
“We shouldn’t be intimidated by the $3 billion price tag because, in many ways, we are paying for this already,” Carlisle said. “This is part of the reason why our health care system is so expensive ‚Äî because patients have to delay care until they are really sick.”
Wood said the estimated cost of the commission’s proposals is a small fraction of the state’s $201 billion annual budget. The report cited other possible funding sources, including philanthropic grants, education dollars, health plan contributions and federal dollars.
Gov. Newsom has “established a vision for how to pursue a pro-health agenda” in California, Carlisle said. “This report provides him with a road map.”
(Five organizations funded the project of the California Future Health Workforce Commission: the California Endowment, California Health Care Foundation, the California Wellness Foundation,¬ÝBlue Shield of California Foundation and the Gordon and Betty Moore Foundation. Kaiser Health News, which produces California Healthline, has received support from each of these organizations.)
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/aging/task-force-outlines-strategy-to-address-californias-shortfall-of-health-workers/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=915752&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>For Marques Martinez, that date was Nov. 15, 2016. Until then, he had used OxyContin, Xanax and nearly every other drug he could get his hands on, he said. He had been suspended from school for selling drugs. “I knew what I was doing was bad,” he said. “But I didn’t think there was another way.”
Two years ago, Martinez’s parents sent him to an in-patient treatment center and then enrolled him in this unusual high school, Interagency at Queen Anne, or IQA. Martinez, 17, learned about the school from an alumnus and knew it might be his last option. He was skeptical at first, but he knew one thing immediately: “I felt safe here.”
The Seattle public school campus, known as a recovery school, is designed for students learning to lead lives of sobriety while they earn their diplomas. The roughly 20 students attend classes in math, language arts and physical education, and they complete other courses online. They meet regularly with a counselor and attend daily support group meetings based on Alcoholics Anonymous programs.

Recent research shows that recovery schools — also known as sober schools — help keep their students off drugs and in class.
A 2017 by Vanderbilt University associate professor Andy Finch and other researchers showed that students in recovery schools were significantly more likely than those not in such schools to report being off drugs and alcohol six months after they were first surveyed. And the average reported absences among the 134 recovery school students in the study was lower than the other students.
Recovery schools first appeared in the late 1970s and now about 40 exist nationwide, including in Minnesota, Texas and Massachusetts. More are likely to open as opioid overdoses continue to climb, said Finch, who is co-founder of the . “There has been a gap in adolescent treatment for many, many years,” he said. “The schools are one of the programs that fill in that gap.”
Finch said about 85 percent of the recovery schools are public or have some source of public funding, while some are private campuses or part of treatment centers. New sober schools are planned in New York, Delaware and Oregon, Finch said.
Starting any school can be complicated, but recovery schools have extra layers of complexity. They have to recruit their students, impose policies specific to them and fund the services they need.
Advocates and school officials in Delaware had hoped to start a public recovery school this year but couldn’t get the funding they needed, said Don Keister, who helps run , an advocacy group he co-founded after his son died of a heroin overdose. Keister said a local school district offered to provide the space and the equipment but didn’t have the estimated $2 million needed to cover staff costs.
“There is a real need,” he said. “In Delaware, we don’t have any real help for adolescents.”
Nationally, illicit drug use among middle and high school students is at record lows. Still, nearly 1 in 5 10th-graders reported using an illegal drug in the previous 30 days, according to the annual nationwide survey.



Like Martinez, many of the Interagency at Queen Anne students go there straight from treatment programs. They say they encounter less temptation than at traditional high schools. “There, people offer you drugs every day,” said 15-year-old Coltrane Fisher, who regularly used heroin, cocaine and other illegal drugs before coming to the school last March.
The success of recovery high schools is partly due to the fact that the students are among sober peers, as well as teachers and counselors who all support their sobriety.
“Unless these kids get engaged with other young people in recovery, they don’t stand a chance,” said Seth Welch, a recovery support counselor at Interagency Queen Anne. “This becomes their new community.”
But the going is not always easy.
Teachers at IQA say they believe the environment has been critical to the students’ success, but it is sometimes a challenge to work there. Some students are way behind in their credits, and they don’t always respond well to authority. “The more we push them, the more they push back,” said one of the teachers, Phyllis Coletta.
Sometimes classwork must be set aside, Coletta said. On a recent school day, one of the newer students was so upset that she spent most of the day crying, clutching a blanket. Coletta hugged her and they took a long walk.
“Mental health and sobriety come first,” Coletta said.

Interagency at Queen Anne, which opened in late 2014, is part of a network of alternative public school campuses called Interagency Academy, which also serves homeless and incarcerated youths.
At first, the campus drew opposition from a group of elementary school parents who feared the students would sell drugs in the neighborhood. But Melinda Leonard, the former vice principal who helped found the school, said those fears have now given way to community support.
“The campus is the most sober school in the school district,” Leonard said.
Students at the school sign a sobriety pledge and agree to random drug testing. They aren’t kicked out for relapsing, but Welch, the support counselor, works to get them back into treatment if they begin actively using again.
Since the school opened, 21 students have graduated. Welch and the teachers help students plan for the future. Martinez, for example, will graduate this month and is taking community college courses.
On a recent morning, language arts teacher Heidi Lally played a song from the hit musical “Dear Evan Hansen” about loneliness and anxiety in high school. She encouraged the students to write about the song in terms of their recovery.
One student wrote, “I’ve had suicidal thoughts and attempts and these lyrics made me remember those times.” Another wrote, “Shadows crowd me / I’m lost / but what’s the cost to end this feeling.”
For Coltrane Fisher, the cost was hitting rock bottom. He began smoking marijuana at age 12 and then moved on to other drugs. Last year, he stopped going to school and didn’t come home for days on end. “Nobody grows up thinking you are going to become an addict,” he said. “It just happens.”

Fisher’s mother, Lisa Luengo, said she didn’t realize the extent of what was happening. “He derailed quickly and very deeply,” said Luengo, a community college teacher. She sent Fisher to a rehab program in Utah before enrolling him here.
Luengo knows the school is right for her son, even though she believes it is weaker academically than other schools. “If he was in a different school setting, he would crumble,” she said. “The school is giving him a future.”
Fisher agreed. “I can accomplish nothing in my life if I am not sober,” he said, “and I would not be sober if not for that school.”
This <a target="_blank" href="/mental-health/students-with-addictions-immersed-in-the-sober-life-at-recovery-high-schools/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=910579&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>