HAY SPRINGS, Neb.тАФ The sun was just warming the horizon as Mark Pieper left his house near his cattle ranch on a crisp February morning.
It’s not unusual for the rancher to wake up early to tend to livestock, but at 5:45 a.m. this day his cattle wouldn’t come first. For the past 3┬╜ years, three days a week, Pieper has made an early-morning commute to get dialysis at the nearest hospital.
Pieper lives outside Hay Springs, which has 599 residents, according to a sign at the edge of town. He makes sure not to forget his chocolate-brown cowboy hat before starting up his pickup truck for the half-hour drive to Chadron.
That February morning was one of his last dialysis sessions there before the hospital shuttered the service at the end of March.
“I guess I’ll just bloat up and die in a month,” Pieper remembered thinking when he learned the center was closing, eliminating the only option near his home.
He needs dialysis to survive after cancer treatment damaged his kidneys.
Pieper and 16 other patients relied on Chadron Hospital for the life-sustaining therapy that filters waste and fluid from their blood тАФ a job their failing kidneys could no longer do. Treatment lasts about four hours.

The closure is just one example of the long decline of health care services in rural America, where people have higher rates of many chronic conditions but less access to care than elsewhere.
The Trump administration promised to address this problem, when it launched the $50 billion federal Rural Health Transformation Program in September. It may not be enough to stop the trend.
“[President Donald] Trump says he is going to help the rural health care,” Pieper said. Dialysis “is one thing that we really need here.”
Some patients have moved to live closer to care, including several nursing home residents. Their new facilities may be farther from their families.
Others are making long drives to dialysis centers. Pieper eventually found treatment in Scottsbluff, which, with about 14,000 residents, is the biggest city in the rural Panhandle region of western Nebraska. The hour-and-a-half drive will triple his time on the road to more than nine hours each week.
Jim Wright and his wife reduced their drive time тАФ but are spending more money тАФ by renting a small home near Rapid City, South Dakota, and living there on weekdays so he can get dialysis. Wright said he understands that rural hospitals face financial challenges.
“But we’re talking about something that’s lifesaving. It’s not a matter of, тАШOh, I would like to be there’” getting treatment, he said. “It’s a case that if you don’t, you die.”

An Influx of Money That’s Out of Reach
Jon Reiners, CEO of the independent, nonprofit Chadron Hospital, wrestled with the decision to end dialysis services. He and several patients said that the closure was announced as the $219 million the state will receive in first-year funding from the .
But the five-year program is aimed at exploring new, creative ways to improve rural health, not to help existing services stay afloat. States can use only up to 15% of their funding to pay providers for patient care.
At least 11 states тАФ Nebraska is not among them тАФ have mentioned using funding for rural dialysis programs, according to a ║┌┴╧│╘╣╧═Ї News review of applications. Their ideas include starting a mobile dialysis unit and helping people get treatment at home or in long-term care facilities.
Reiners said Chadron Hospital lost $1 million a year on its dialysis service due to low reimbursement rates that didn’t cover operational costs.

The facility is a critical access hospital, a designation that allows certain small, mostly rural hospitals to get increased reimbursement rates for their Medicare patients. While most of the affected patients were on Medicare, the critical access program doesn’t cover outpatient dialysis, Reiners said.
Reiners said the hospital worked for more than a year to find solutions, such as reaching out to four private companies to potentially take over the center. But he said they all passed after realizing they would lose money.
Nephrologist Mark Unruh said the dialysis closure in Chadron reflects a wider trend of staffing and funding challenges.
“You do end up in situations where you have people who are displaced like this, and it’s just sad,” said Unruh, chair of the Internal Medicine Department at the University of New Mexico.
People in rural America face significant disparities in kidney health and treatment, published in 2024 in the American Journal of Nephrology. They’re and face after diagnosis, according to data from the National Institutes of Health.
The best way to address this is to focus on prevention, Unruh said. He pointed to a that helps primary care doctors in rural and other underserved areas prevent end-stage renal failure.
Another idea, Unruh said, is boosting the rate of kidney transplantation for rural patients. He’s looking at whether it’s helpful to “fast-track” tests patients need to get approved for a transplant by scheduling all of them over a couple of days to limit travel time.
Unruh said the U.S. health system also needs to recruit more staff who can train patients and their caregivers to administer dialysis at home.
Exploring the Option of Home Dialysis
Rural dialysis patients are more likely than urban ones to get home dialysis, according to . In 2023, the rate was nearly 18% for rural patients and about 14% for urban ones.
One type of home dialysis requires surgery to get a catheter placed in the abdomen and . The other kind requires . The nearest facility to Chadron that offers training for the first option is in Scottsbluff. The nearest that offers training for the latter kind is three hours away in Cheyenne, Wyoming.
Pieper said doctors told him he’s not a candidate for home dialysis or a transplant. The Panhandle has a nonprofit, rural transit system, but its schedule won’t work for Pieper. He said that leaves him with no choice but to get treatment in Scottsbluff, a 200-mile round trip.
It takes Linda Simonson even longer тАФ more than four hours round trip тАФ to drive her husband, Alan, from their ranch to his treatment in Scottsbluff.
Linda sat in the waiting room with a yellow legal pad during one of Alan’s final treatments in Chadron. The paper was scrawled with phone numbers of politicians to call and driving distances to dialysis centers in the region. She said facilities closer to their ranch either don’t have room for new patients or lack good spots along the route to take a driving break in bad weather.
“It’s just unreal,” she said.
She said even if Alan took a bus, she’d have to ride along to support him during the trip and his treatment.
Jim and Carol Wright, the couple staying near Rapid City on weekdays, said they can’t afford to rent a second home forever. Their weekly commute is already taking a physical and emotional toll. They said they’ll eventually have to move to a bigger city, giving up the house they love in the scenic Nebraska National Forest.
Carol said she feels for the dialysis staffers in Chadron, who are wonderful.
“It just doesn’t seem right to sacrifice one unit that’s so vital,” she said while standing next to a pile of moving boxes stacked inside their rental.

The Wrights wrote letters to politicians and hospital leaders to share their concerns and ideas for keeping the unit open, including using the federal rural health funding.
Simonson said she spoke with aides for the governor and her state representatives but none of the leaders called her back.
“It feels like they don’t know that we exist at this end of the state,” she said.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/dialysis-unit-closes-rural-transformation-health-fund-nebraska/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2178069&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>It’s one of the many parts of the 25-bed rural hospital that need updating, former CEO Ron Wiens said.
He said the hospital, an essential service in its namesake town of nearly 800 residents in the state’s sprawling north-central high plains, needs at least $1 million for deferred maintenance, including a failing HVAC system. But the facility has struggled to make payroll each month and can’t afford to make all the fixes, Wiens said.
Built by farmers and ranchers in 1965, Big Sandy Medical Center began with nine beds. Today, a similar community effort тАФ donations and grants to plug financial holes each year тАФ keeps it afloat.
Wiens, who recently left his position at the hospital, said he wishes Big Sandy could get funding from Montana’s share of the $50 billion federal Rural Health Transformation Program to renovate the hospital and direct payments to help secure its future. The state received more than $233 million in its first-year award.
But the hospital may not get the kind of help he sought.
That’s because the five-year program focuses on new, creative ways to improve access to rural health care, not on directly funding services and renovations. And Montana is one of at least 10 states whose leaders say projects launched under the federal program could lead rural hospitals to cut services so they can continue to afford to offer emergency and other essential care.

Congressional Republicans created the fund as a last-minute sweetener to their One Big Beautiful Bill Act, signed into law last summer. The funding was intended to offset disproportionate fallout anticipated in rural communities from the law, which is expected to slash Medicaid spending .
includes programs to make it easier for rural residents to get medical care and live a healthy lifestyle. For example, it says funding can be used to start community gardens, train paramedics to make home visits, open school-based clinics, or bring mobile clinics to rural areas.
rural Montana hospitals can receive payments for implementing recommendations, “including right-sizing select inpatient services” to match demand. In some cases, it says, right-sizing might mean “downsizing.” The state says hospitals will have input and recommendations will be specific to each facility.
“That’s what has all the hospitals on pins and needles, words like restructuring, reducing inpatient beds. Everybody is going, тАШWhat is this going to look like?’” Wiens said.
The Montana Department of Public Health and Human Services declined to answer questions about how it will carry out its right-sizing efforts.
A Lifeline of Care
Big Sandy cattle rancher Shane Chauvet doesn’t want any services cut.
He credits Big Sandy Medical Center with saving his life after a flying piece of metal nearly cut off his arm during a windstorm a few years back.
“I looked over, saw it coming, and whack!” Chauvet recalled.
His wife drove him to the hospital, where they frantically pounded on the ER door while Chauvet’s blood pooled on the ground.
Because of the storm, staffers worked on Chauvet with no power and no ability to summon a helicopter. He was then taken by ambulance 80 miles through intense rain and hail to a larger hospital.
Chauvet understands the state’s plan doesn’t call for eliminating emergency care, but he worries that reducing other services would set off a downward spiral for the hospital and his town.

In Oklahoma, realigning clinical services could mean “shutting down service lines,” to the federal program. And in Wyoming, any facility that receives funding must agree to “reduce unprofitable, duplicative or nonessential service lines,” .
Monique McBride, business operations administrator at the Wyoming Department of Health, said the department interprets right-sizing as helping rural hospitals provide essential services тАФ such as emergency departments, ambulance services, and labor and delivery units тАФ while maintaining long-term, financial stability.
“This might involve limiting some elective procedures that could be done at lower cost in higher-volume facilities. The main distinction here is time-sensitive emergencies vs. тАШshoppable’ services,” she said.
A New Lease on Life?
Seven of the 10 states тАФ Nebraska, North Dakota, Tennessee, Kansas, Nevada, South Carolina, and Washington тАФ where rural hospital service cuts are on the table say they’ll help pay for hospitals to convert to Rural Emergency Hospitals. The recently created federal designation requires hospitals to halt inpatient services and offers enhanced payments to help them maintain emergency and outpatient care.
At least 15 additional states wrote that they’ll use the federal funding to right-size, evaluate, or adjust services тАФ which could mean adding or taking away services, or transitioning them to a telehealth or outpatient setting.
Brock Slabach, chief operations officer of the National Rural Health Association, said, “There’s a proper concern from rural hospital administrators that this funding is not going to where it was intended.”
He said cutting services that lose money could backfire in the long run. For example, he said, halting labor and delivery care might drive more people out of small towns, further reducing hospitals’ patient numbers and revenue.
The type of hospital services that states will assess matters, said Tony Shih, a senior adviser at the Commonwealth Fund, a nonprofit focused on making health care more equitable.
“If the end result is that high-margin services are taken away from local hospitals with nothing given back in return, it can be financially harmful,” he said.
Shih noted that states’ plans to add more outpatient care could prove beneficial for patients. It’ll take time to know which states help stabilize rural hospitals, he said.
Rural hospital leaders say they know which changes would keep their facilities open and that states shouldn’t suggest or mandate service cuts and other changes on their behalf.

Josh Hannes, who oversees rural health policy at the Colorado Hospital Association, said “top-down” directives won’t work.
He said the association’s members believe they can find efficiencies and are eager to collaborate. But “a state agency shouldn’t be making those determinations,” he said.
Hannes said members are worried Colorado’s plan to classify rural health facilities as a “hub, spoke, or telehealth node” will compel service reductions. The classification will help determine “which services are sustainable locally and which are best provided regionally or through telehealth,” .
Spokespeople for the Colorado and Oklahoma health departments said no facility will be forced to end services. But Oklahoma spokesperson Rachel Klein said some facilities might choose to do so as part of a broader effort to make sure they’re meeting community needs while remaining financially stable.
“A hospital might shift certain services to a nearby regional provider with higher patient volume and specialized staff while expanding other local services,” such as primary, outpatient, or community-based care, she said.
Wiens and Darrell Messersmith, CEO of Dahl Memorial Hospital in the southeastern Montana town of Ekalaka, said they worry the only way hospitals will get their share of funding is to cut services or become Rural Emergency Hospitals that don’t offer inpatient services.
“I would hate to see things shift toward a pack-and-ship facility,” Messersmith said. “Right now, we function quite well as an inpatient facility.”
Not all Montana health leaders are worried.
Ed Buttrey, president and CEO of the Montana Hospital Association, said he thinks his state’s plan could help rural hospitals become financially sustainable and survive Medicaid cuts. Buttrey is also a Republican state lawmaker.
Chauvet, the Big Sandy rancher, said his perspective on whether remote towns like his should have a hospital is forever changed because of his accident.
“I always would say, тАШOh, they’re nice to have,’ but now I look at the hospital and say, тАШThat’s essential to our community,’” he said.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/rural-emergency-hospitals-montana-rightsize-downsize-services-transformation-fund/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2172028&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But plans to spend those nine-digit awards aren’t all warmly received.
At least one group of Republican state lawmakers appears to have scuttled an initiative preapproved by federal officials. And at least one hospital association persuaded its state health leaders to alter who greenlights spending. Other critics are taking a more cautious approach.
That’s because the Centers for Medicare & Medicaid Services, which manages the five-year Rural Health Transformation Program, says states could lose money if they make major changes to the plans approved in their applications. Changes could also delay states’ ability to get projects rolling in time to show the agency that they’re meeting progress deadlines.
“During the application period, states were advised to only propose initiatives and state policy actions that the state deemed feasible,” said CMS spokesperson Catherine Howden, who noted that the agency will work with states case by case.
The recent pushback reflects “tension” over state plans тАФ which were approved by the federal government тАФ from state lawmakers and health leaders who want more input amid tight deadlines, said Carrie Cochran-McClain, chief policy officer of the National Rural Health Association, the largest organization representing rural hospitals and clinics.
Cochran-McClain said many states must pass a bill to allow federal dollars to be spent and added that because the program rolled out so quickly “there’s important work that still needs to be done in some states between the legislatures and the governors.”
State lawmakers want to have a say, she said, in “how the funding is being allocated тАФ how the implementation will go.”
Congressional Republicans created the program as a last-minute sweetener to include in their One Big Beautiful Bill Act, signed into law last summer. The funding was intended to offset concerns about the anticipated in rural communities from the law, which is expected to slash Medicaid spending by nearly $1 trillion over a decade.
CMS officials announced first-year funding тАФ ranging from $147 million for New Jersey to $281 million for Texas тАФ on Dec. 29, after scoring applications. Federal officials will begin evaluating progress in late summer and announce 2027 allocations at the end of October.
A chorus of critics say the program won’t make up for harm caused by Medicaid cuts.
The program is “a complete sham,” Sen. Ron Wyden (D-Ore.) said at a rural policy conference in February.
Medicaid, a joint federal-state program for low-income and disabled Americans, serves nearly , and many rural hospitals depend on it to stay afloat.
But the rural health program tilts toward seeding innovative projects and technologies, not shoring up rural hospital finances. States can use only up to 15% of their funding to pay providers for patient care.
That hasn’t stopped some federal officials and lawmakers from framing the program as a rural hospital rescue.
For example, the White House , “President Trump secured $50 billion in funding for rural hospitals.”
Now that applications have been approved, some state Republican lawmakers тАФ who are than Democrats are тАФ and hospital associations are upset that the political rhetoric doesn’t match what they see.
They’re also lobbing criticisms at specific aspects of their states’ plans, including the proposed projects, what’s not included, and the spending approval process.
In Wyoming, lawmakers didn’t just criticize an initiative from their state’s application. They moved to kill it.
State Rep. John Bear, a Republican, said he and other lawmakers declined to fund “BearCare,” a proposed state-sponsored health insurance plan that patients could use only after medical emergencies. But they did approve other aspects of the rural health program.
The Wyoming Department of Health won’t “proceed with BearCare without express legislative authority to do so,” said spokesperson Lindsay Mills.
While Wyoming lawmakers removed an initiative from their state’s rural health plan, a group in Ohio wants to add something.
Ohio Rep. Kellie Deeter and other Republican lawmakers to use the maximum allowed funding for provider payments тАФ 15% тАФ to support 13 independent, rural hospitals.
“We understand that the rural transformation fund is not designed to be given directly to prop up hospitals,” Deeter said. “We just want to capitalize on the mechanism of the fund that can be utilized for that purpose.”
Those hospitals “operate with very, very narrow margins, and it’s just difficult and, frankly, unsustainable,” she added.
Ken Gordon, a press secretary responding for the governor’s office and the state health department, said, “It’s still very early in this process, and many details are being worked out.”
State lawmakers around the country are also trying to ensure the federal program’s dollars benefit rural areas.
In North Dakota, Rep. Bill Tveit, a Republican who lives in a town with about 2,000 residents, that would have required the state to reserve its funding for programs located more than 35 miles from urban areas and small cities.
During a hearing, lawmakers appeared sympathetic to Tveit’s concerns but quickly shot down his idea.
State Sen. Brad Bekkedahl said the North Dakota health department already committed to prioritizing funding for the most pressing rural health needs. He also said he’s concerned any significant changes could cause the state to lose funding because CMS already reviewed and approved the plan.
Meanwhile, Republican lawmakers in Michigan and North Carolina have criticized their states’ definitions of “partially rural” or “rural,” saying that counties that include urban population centers could take money from lower-density counties, according to and .
Lawmakers aren’t the only ones speaking out.
The Colorado Hospital Association to state lawmakers denouncing how the state created its plan and two of its proposed initiatives.
“Not only were Colorado’s rural hospitals’ recommendations disregarded,” president and CEO Jeff Tieman wrote, but the plan includes ideas “they actively oppose and believe will harm the communities they serve.”
The department responded to one of the association’s concerns by adding rural health leaders to the .
Meanwhile, and Nebraska, some health groups are upset that their states’ plans lack specific funding streams for rural hospitals.
Lauren LaPine-Ray, who oversees rural health policy at the Michigan Health & Hospital Association, predicted the state’s rural hospitals will compete with other organizations, such as academic centers and health clinics, for funding. She said about 65% of the group’s rural members have never applied for a state grant before.
“The rural hospitals, the ones that really need the funding the most, will not be well equipped to apply for and pull down these dollars,” LaPine-Ray said.
Jed Hansen, executive director of the Nebraska Rural Health Association, said the federal funding won’t go to “rural hospitals, rural clinics, and rural providers in a meaningful way.”
“Rural Health Transformation will not save a single hospital in our state,” he said. “I don’t think it will save a hospital nationally.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/rural-transformation-fund-lawmakers-health-groups-resist-state-spending-plans/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2161929&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The state could tackle rural health issues long into the future by investing its awards from the Rural Health Transformation Program, the director of Wyoming’s health department, Stefan Johansson, told state lawmakers.
But it’s unclear whether the maneuver will pass muster with the federal government.
If approved, Wyoming’s Rural Health Transformation Perpetuity fund could provide $28.5 million for the state to spend every year, presented to lawmakers.
Wyoming would spend the money on scholarships for health students and incentive payments to help keep small hospitals and rural ambulance services afloat.
“I have lots of questions. It seems very clever,” said Kevin Bennett, director of the South Carolina Center for Rural and Primary Healthcare. “It’s a wild idea.”
Bennett said the big question is whether the federal Centers for Medicare & Medicaid Services, which manages the new program, will approve of Wyoming’s plan.
If it does, he said, “it’s really an interesting way to keep things going” тАФ one with potential benefits as well as risks.
Congressional Republicans created the Rural Health Transformation Program as a last-minute sweetener in their One Big Beautiful Bill Act last summer. The funding was intended to offset concerns about the anticipated in rural communities from the new law, which is expected to reduce Medicaid spending by nearly $1 trillion over the next decade.
Since 2010, 152 rural hospitals in the U.S. have , according to the Sheps Center for Health Services Research at the University of North Carolina. The guidelines for the federal rural health program say states can use only 15% of their funding for direct payments to providers, including hospitals.
CMS officials on Dec. 29 after scoring states’ applications. States had until Jan. 30 to submit revised budgets and other documents that align with their grant awards. CMS has until March 1 to review and approve the updated material.
Wyoming тАФ the least populous state, with about 588,000 residents тАФ will receive $205 million in the program’s first year, $5 million more than it asked for.
States must spend each year’s grants by the end of the following fiscal year, . If they don’t, unused money will be . The final deadline for all spending is Oct. 1, 2032, with leftover funds being returned to the federal government.
Given those rules, “how do you square that with squirreling money away in an account?” state Rep. Ken Pendergraft, a Republican, asked during a hearing on Wyoming’s plan.
Johansson said that depositing the federal grants into the perpetuity fund counts as expending them.
He said that CMS called in December to specifically ask questions about the fund and that he believes the agency has formally approved it. But “the devil’s always in the details,” he said, as the state works with CMS during the budget review period.
Emails obtained by ║┌┴╧│╘╣╧═Ї News through public records requests show CMS told officials in some states in early November that the grant money can’t “fund an endowment, capital fund, or other vehicle resembling an investment fund with the purpose of generating income.”
Wyoming officials that the perpetuity fund won’t be making or keeping any profit.
“All program income from these investments will directly fund” rural health programs, they wrote.
CMS spokesperson Catherine Howden did not directly comment on whether Wyoming’s perpetuity idea is allowed. Instead, she said states must follow regulations related to the program and federal grants.
The Trump administration gave states a mandate to spend their money by fall 2032, but on projects that will continue to help rural patients even after the federal program ends.
The perpetuity fund would ensure just that, said Patrick Hardigan, dean of the College of Health Sciences at the University of Wyoming.
“Rather than spend out now,” Hardigan said, “we would have this available to help fund us over a longer time period.”
The state health department has already presented lawmakers with to create the perpetuity fund and approve other parts of its rural health plan.
The legislation says Wyoming would put 80% of this year’s award тАФ $164 million тАФ and 69.5% of the funding it receives over the next four years into the fund. The state treasurer’s office would invest the fund in equities, including stocks. The health department plans to spend 4% of the fund’s money тАФ in line with its expected return тАФ each year, .
About 41% of the annual fund distribution would be spent on incentive payments for qualifying small hospitals, the bill says. The assistance could include one-time grants, medical debt relief for patients, and ongoing payments to offset fixed costs. This funding could amount to 2.5% to 10% of these hospitals’ annual operating expenses, in Wyoming’s application.
Bennett said it’s unclear whether all those types of payments are allowed under the federal rules.
“I think that states will try to do a lot of creative things like this, and CMS will approve or not on a case-by-case basis,” he said.
The bill says around 27% of annual spending would go to incentive payments to encourage coordination or consolidation among rural ambulance services. The funding could be ongoing or grants that help pay for ambulances, communications equipment, and regional dispatch services.
But these incentives would come with . Hospitals and ambulance services could receive payments only if they reduce “unprofitable, duplicative or nonessential” services and participate in “cost-containment arrangements,” such as regional collaborations and shared services.
About 22% of the annual spending would provide scholarships to help Wyomingites afford nursing, behavioral health, emergency medical services, and physician education. In exchange, recipients would have to work in the state for five years.
The remaining spending, around 11%, would be for scholarships to help doctors in training afford medical school, residency programs, and fellowships if they agree to work in an “underserved” Wyoming county for five years. The state health department would prioritize scholarships for people pursuing family medicine, obstetrics, or other high-demand specialties.
Johansson told Wyoming lawmakers that CMS could claw back money if a future state legislature decides to spend the fund in ways not allowed under the federal rural health program. He said this “check and balance” could last for decades.
“I can’t predict the future,” Johansson said, but “I think they have the authority to go look at the appropriate use of those funds through their audit parameters.”
Other states proposed funds in their applications, but Wyoming’s appears unique, according to a ║┌┴╧│╘╣╧═Ї News review of state applications.
For example, Kentucky wants to create a rural health endowment to continue its work once the federal program ends. But it would be backed by charitable donations, not seed money and investments from the federal funding.
Several states mention putting some of their federal award money into what they call rural health “catalyst funds.” But these funds, sometimes augmented with private contributions, would be invested in rural health technology.
Bennett said he’s never heard of a state investing any other federal health grant the way Wyoming wants to.
He said that in setting aside significant portions of its Rural Health Transformation Program awards, Wyoming would have much less money for rural health care in the short term in exchange for an ongoing revenue stream that could last decades.
“Everything has trade-offs,” Bennett said.
The Wyoming House Appropriations Committee unanimously approved the bill on Feb. 12, sending the legislation to the House floor.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/wyoming-rural-health-transformation-funding-grants/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2151884&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But there are strings attached.
In late December, President Donald Trump’s administration announced how much all 50 states would get under its new Rural Health Transformation Program, assigning them to use the money to fix systemic problems that leave rural Americans without access to good health care. Now, the clock is ticking.
Within eight months, states must submit revised budgets, begin spending, and show the money is going to good use. Federal officials will begin reviewing state progress in late summer and announce 2027 funding levels by the end of October.
The money — divided into unique allocations for each state, ranging from $147 million for New Jersey to $281 million for Texas — represents the first $10 billion installment from the five-year, $50 billion program. Congress created the fund as a last-minute sweetener in Trump’s One Big Beautiful Bill Act last summer to offset the anticipated in rural communities from the statute’s nearly $1 trillion in Medicaid spending cuts over the next decade.
Federal officials crafted the fund to give states “space to be creative,” Mehmet Oz, administrator of the Centers for Medicare & Medicaid Services, said on a call with reporters after announcing the funding Dec. 29. “Some states will fail, and we will learn from that.”
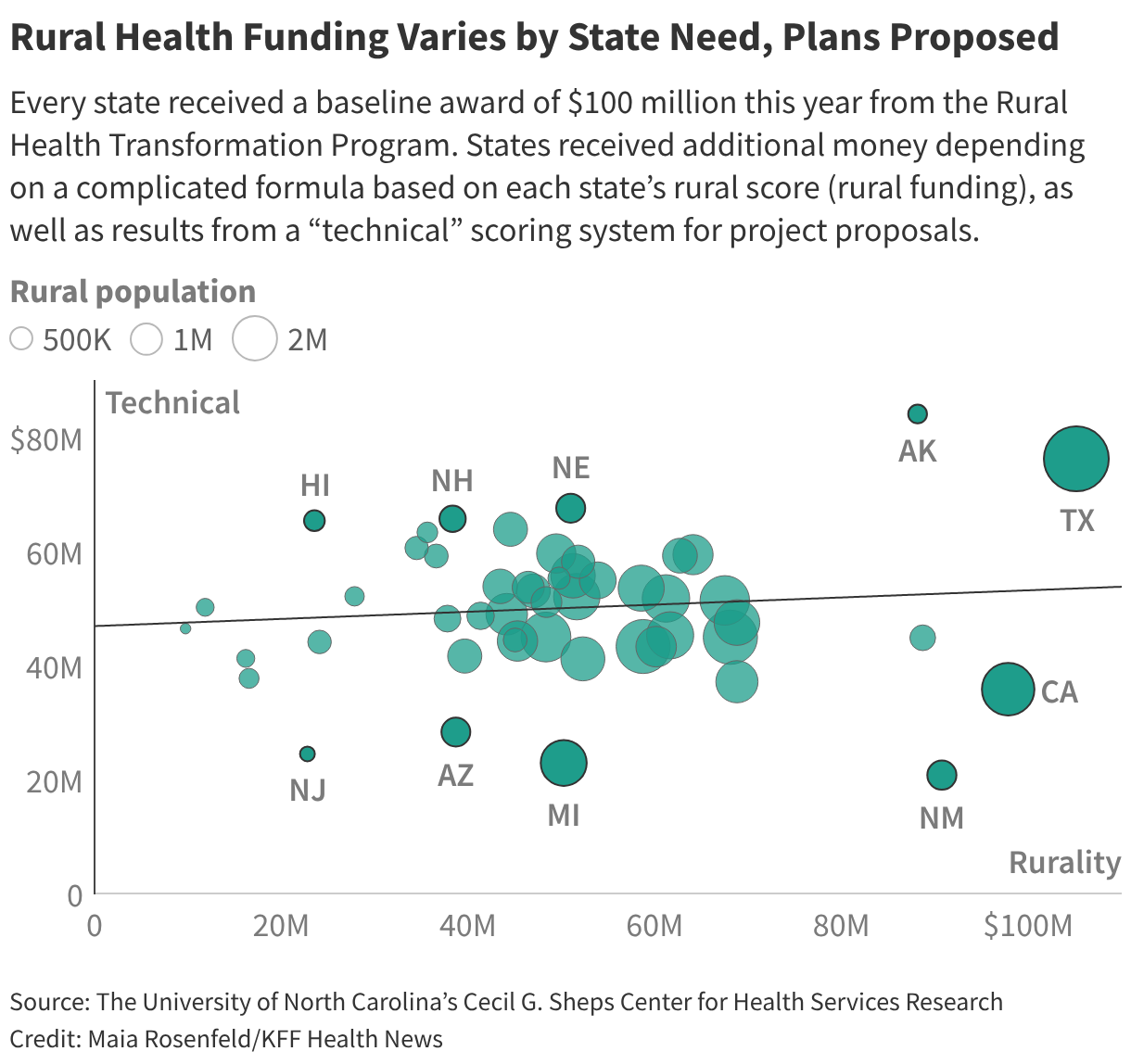
The money was divided according to a complicated formula.
In 2026, each state will receive an equal $100 million share for the first half of the money, plus additional funding from the second half. Oz’s staff steered payouts from the second portion based on each state’s rural score, as well as results from a “technical” scoring system for project proposals.
Within hours of the announcement, academics and researchers began to parse the awards to better understand why some states received more than others, including whether the awards reflected any partisanship or political favoritism.
At first glance, total awards do not appear to favor states governed by either Republicans or Democrats. But teased out the amount awarded for each state’s technical score, which is the part determined by the discretion of agency officials.
The analysis was performed at the University of North Carolina’s Cecil G. Sheps Center for Health Services Research, which specializes in rural health. A ║┌┴╧│╘╣╧═Ї News review of the Sheps Center data found that states with Republican governors tended to receive more money for the parts of their application based on the technical score. Democratic-controlled states crowded the bottom quarter of those technical score awards.
Overall, though, the state awards reveal wild variation in how much money each state will get per rural resident, almost a hundredfold difference between the top and bottom.
In an emailed statement to , a spokesperson for Arizona’s Democratic Gov. Katie Hobbs accused the administration of shortchanging rural residents in the state, which was awarded $167 million this year from the program.
CMS spokesperson Chris Krepich said in an emailed statement to ║┌┴╧│╘╣╧═Ї News that “politics played no role in funding decisions.”
On the December call, Oz pushed states to start working on policy actions championed by the administration — such as approving presidential fitness tests and restricting food benefits — that could require legislative approval.
Half of states promised to mandate the presidential fitness test, Oz said. Many states also proposed food waivers under the Supplemental Nutrition Assistance Program, known as SNAP, which would limit low-nutrition items such as soda. He also said some states promised to teach health care professionals about nutrition. And others confirmed they will repeal certificate-of-need laws, which require companies to prove that new health facilities they want to open are necessary.
Krepich said CMS’ new Office of Rural Health Transformation is hiring program officers to serve as point people for three or four states. Many states are setting up their own offices to oversee the new funding.
Oz highlighted Alabama’s “big maternity initiative with robotics doing ultrasounds” and said states are tackling issues ranging from behavioral health to obesity.
A ║┌┴╧│╘╣╧═Ї News review of state “” and “” released by CMS shows that many states plan to address the workforce challenges in rural areas. Delaware, for example, plans to use its funding to create the state’s first four-year medical school with a rural primary care track.
A third of states said they want to improve electronic health records, and every state mentioned telehealth.
Many state legislatures to distribute the funding to their state offices. Meanwhile, state officials are hiring staff, , and .
“I’m excited about what’s next,” said Terry Scoggin, former interim chief executive of the Texas Organization of Rural & Community Hospitals, or TORCH. Texas was awarded the biggest allocation. The money will bolster a rural hospital funding bill Republican Texas Gov. Greg Abbott signed last year, Scoggin said.
More than two dozen cash-strapped rural hospitals in Texas to clinics since 2005, a nationwide trend that hit the Lone Star State particularly hard. The state has the largest rural population in the United States. Texas’ allocation amounts to about $66 per rural resident, . By contrast, Rhode Island was granted about $6,300 per rural resident.
Scoggin said he has “a ton of concerns” about companies taking the money instead of it helping rural hospitals and residents. “I was blown away about how many for-profit companies reached out.” The companies have also called rural hospitals and asked to work with them to apply for state money, he said.
The awards should be judged on how they benefit rural residents because “the stated goal of the program is to improve rural health,” said Paula Chatterjee, an assistant professor of medicine at the University of Pennsylvania who co-authored on the transformation fund.
Researchers at the Sheps Center conducted the analysis to estimate how much money states received from the technical score, which is the portion of funding based on the quality of their proposals and state policy actions that align with “Make America Healthy Again” priorities.
New Mexico won the least amount of technical funding, with less than 10% of its award based on the discretionary metrics. Alaska won the largest technical award, according to the Sheps Center data.
Texas, Nebraska, New Hampshire, and Hawaii rounded out the top five recipients of technical funding. In addition to New Mexico, the other lowest technical awards went to Michigan, New Jersey, Arizona, and California.
Mark Holmes, director of the Sheps Center, declined to comment on whether he saw any political bias in the awards but said the nuance in the final portion of discretionary awards based on technical scores is important because those dollars can be redistributed and potentially clawed back in future years.
“We can be fairly certain that every state will get at least a slightly, if not a vastly, different amount next year based on this re-pooling and reallocation piece,” Holmes said.
States now have a limited time to show they’re using the money effectively to secure future funding.
But they can’t start spending yet. CMS followed standard grant procedures and is requiring each state to submit revised budgets before they can draw down money, Krepich said.
States have until Jan. 30 to resubmit their budgets, and CMS then has 30 days to respond, according to the standard . Under that timing, some states may not have cash in hand until March.
“CMS is working closely with states to complete this process as efficiently as possible,” Krepich said.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/rural-health-transformation-state-distribution-technical-scores-variation-deadlines/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2141942&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Because they aren’t U.S. citizens, they would each need a visa.
West River and other companies used to pay up to $5,000 in fees to sponsor each H-1B visa for such workers.
The nonprofit hospital now has to pay $100,000 if it wants to hire one of the new applicants, who are all from the Philippines or Nigeria. Or it could spend money on an attorney to petition the government for an exemption from the new fee.
H-1B visas are for highly skilled foreign workers in fields тАФ such as the chronically understaffed rural health system тАФ that struggle to find enough American employees.
In September, President Donald Trump increased the visa fee to $100,000 for workers living outside the U.S. It doesn’t apply to foreign workers or students who were already in the U.S. on a visa.
His proclamation rails against the tech world’s use of H-1B workers, but the new fee applies to all fields.
“The health care industry wasn’t even considered. They’re going to be collateral damage, and to such an extreme degree that it was clearly not thought about at all,” said Eram Alam, a Harvard associate professor whose examines the history of foreign doctors in the U.S.
H-1B applicants will receive a fee exemption only in an “extraordinarily rare circumstance.”
The , two , and asked Homeland Security Secretary Kristi Noem to grant categorical exemptions for the health care industry. The new cost will disproportionally harm rural communities that already struggle to afford and recruit enough providers, the groups argued.
DHS officials directed inquiries to the White House, which did not answer questions about individual waiver timelines or the possibility of an exemption for the health care industry.
Instead, White House spokesperson Taylor Rogers sent a statement defending the new fee, saying it will “put American workers first.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/the-week-in-brief-rural-health-h1b-visa-fee/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2130398&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Not one U.S. citizen has applied.
West River Health Services in Hettinger, a town of about 1,000 residents in the southwestern part of the state, has four options, and none is good.
The hospital could fork over $100,000 for the Trump administration’s new H-1B visa fee and hire one of the more than 30 applicants from the Philippines or Nigeria. The fee is the equivalent of what some rural hospitals would pay two lab techs in a year, said Holzkamm, who is West River’s lab manager.
West River could ask the Department of Homeland Security to waive the fee. But it’s unclear how long the waiver process would take and if the government would grant one. The hospital could continue trying to recruit someone inside the U.S. for the job. Or, Holzkamm said, it could leave the position unfilled, adding to the workload of the current “skeleton crew.”
The U.S. health care system depends on foreign-born professionals to fill its ranks of doctors, nurses, technicians, and other health providers, particularly in chronically understaffed facilities in rural America.
But a new presidential proclamation aimed at the tech industry’s use of H-1B visas is making it harder for West River and other rural providers to hire those staffers.
“The health care industry wasn’t even considered. They’re going to be collateral damage, and to such an extreme degree that it was clearly not thought about at all,” said Eram Alam, a Harvard associate professor whose new book examines the history of foreign doctors in the U.S.
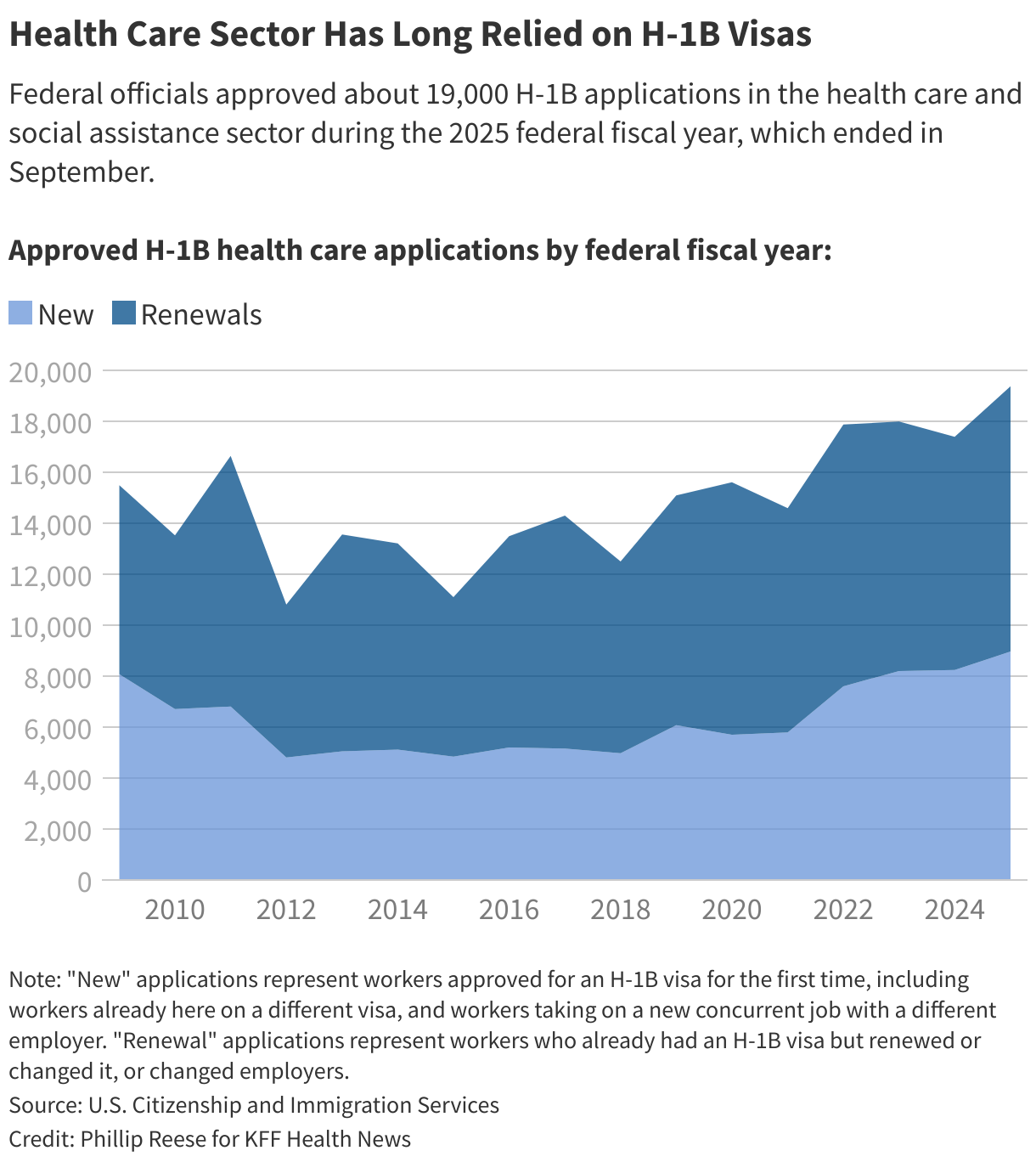
Elissa Taub, a Memphis, Tennessee-based attorney who assists hospitals with the H-1B application process, has been hearing concerns from her clients.
“It’s not like there’s a surplus of American physicians or nurses waiting in the wings to fill in those positions,” she said.
Until recently, West River and other employers paid up to $5,000 each time they applied to sponsor an H-1B worker. The visas are reserved for highly skilled foreign workers.
The new $100,000 fee — part of a by President Donald Trump — applies to workers living outside the U.S. but not those who were already in the U.S. on a visa.
West River lab tech Kathrine Abelita is one of nine employees — six technicians and three nurses — at the hospital who are current or former H-1B visa holders. Abelita is from the Philippines and has worked at West River since 2018. She’s now a permanent U.S. resident.
“It’s going to be a big problem for rural health care,” she said of the new fee. She said most younger American workers want to live in urban areas.
Sixteen percent of registered nurses, 14% of physician assistants, and 14% of nurse practitioners and midwives who work in U.S. hospitals are immigrants, according to a . Nearly a quarter of physicians in the U.S. went to medical school outside the U.S. or Canada, according to .
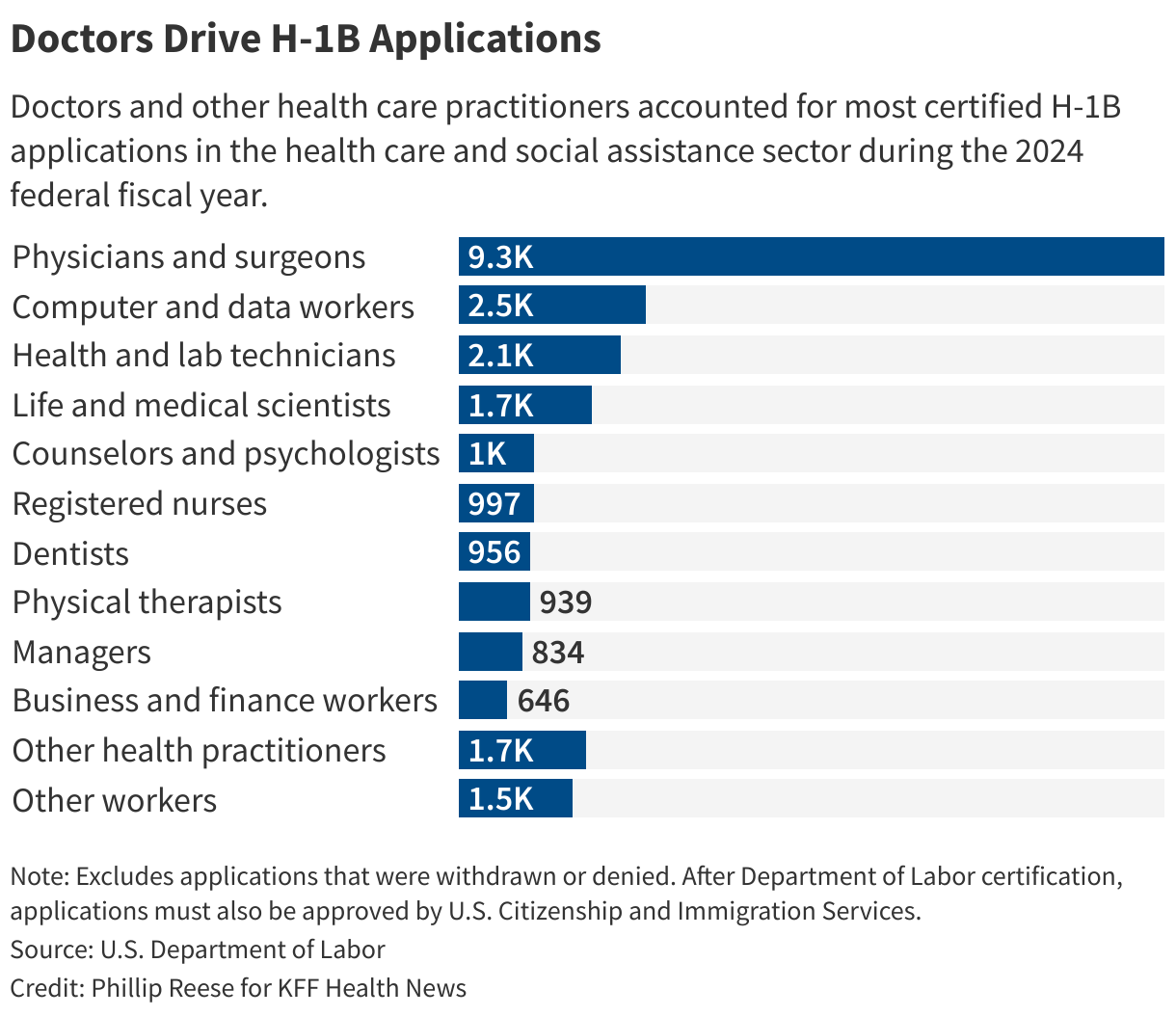
The , two , and have asked the administration to give the health care industry exemptions from the new fee. The new cost will disproportionally harm rural communities that already struggle to afford and recruit enough providers, the groups argue.
“A blanket exception for healthcare providers is the simplest path forward,” the National Rural Health Association and National Association of Rural Health Clinics wrote in a joint letter.
The proclamation allows fee exemptions for individuals, workers at specific companies, and those in entire industries when “in the national interest.” says the fee will be waived only in an “extraordinarily rare circumstance.” That includes showing that there is “no American worker” available for the position and that requiring a company to spend $100,000 would “significantly undermine” U.S. interests.
Taub called those standards “exceptionally high.”
Representatives of the NRHA and the American Medical Association, which organized a letter from the medical societies, said they’ve received no response after sending requests to Homeland Security Secretary Kristi Noem in late September and early October. The AHA declined to say whether it had heard back.
Homeland Security officials directed ║┌┴╧│╘╣╧═Ї News’ inquiries to the White House, which did not answer questions about individual waiver timelines or the possibility of a categorical exemption for the health care industry.
Instead, White House spokesperson Taylor Rogers sent a statement defending the new fee, saying it will “put American workers first.” Her comments echo Trump’s proclamation, which focuses on accusations that the tech industry is abusing the H-1B program by replacing American workers with lower-paid foreign ones. But the order applies to all trades.
Alam, the Harvard professor, said the U.S.’ reliance on international providers does raise legitimate concerns, such as about how it takes professionals away from lower-income countries facing even greater health concerns and staffing shortages than the U.S.
This decades-long dependency, she said, stems from population booms, medical schools’ historical exclusion of nonwhite men, and the “much, much cheaper” cost of importing providers trained abroad than expanding health education in the U.S.
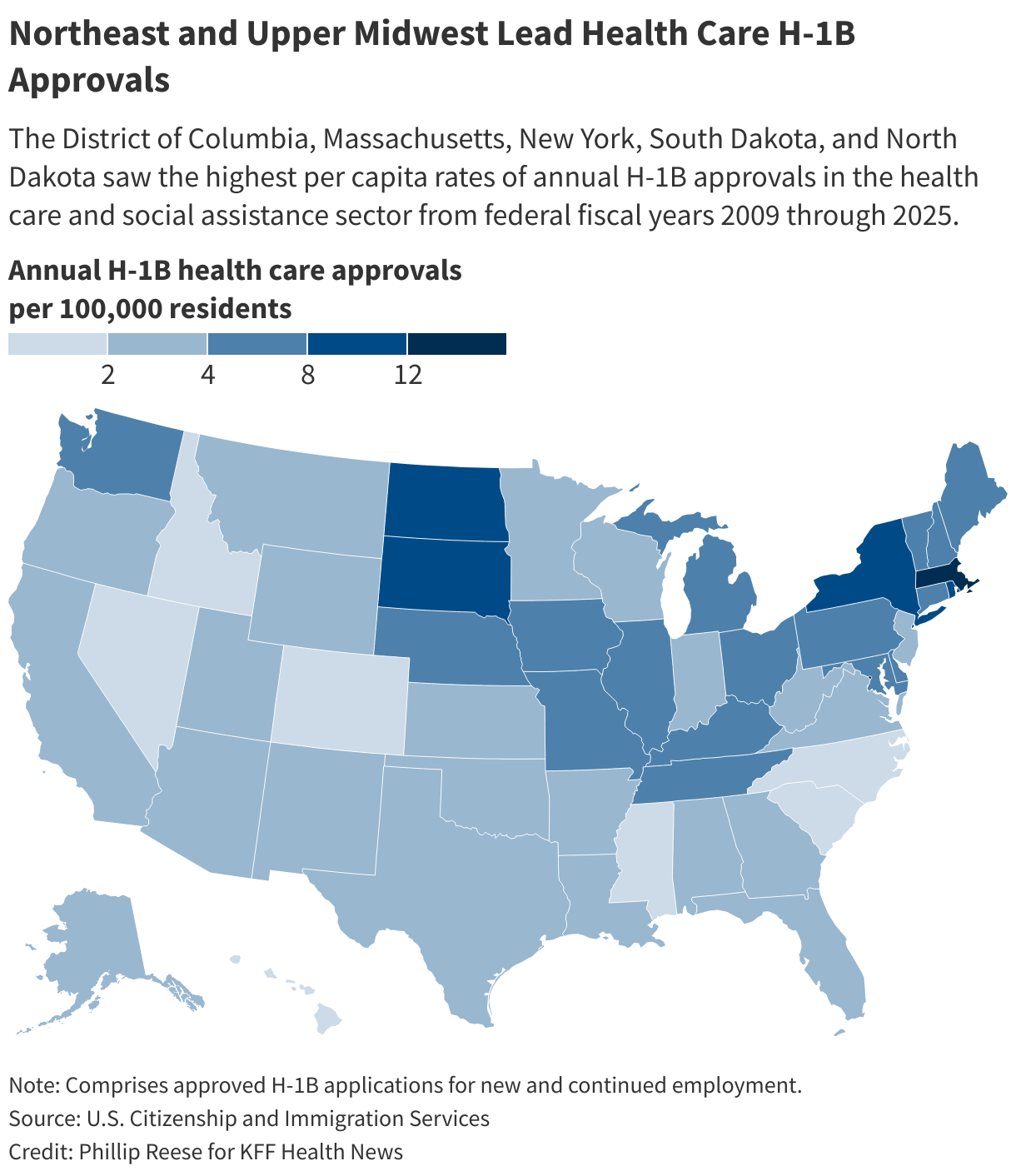
Internationally trained doctors tend to work in rural and urban areas that are poor and underserved, according to and .
Nearly 1,000 H-1B providers were employed in rural areas this year, the two rural health organizations wrote in their letter to the Trump administration.
J-1 visas, the most common type held by foreign doctors during their residencies and other postgraduate training in the U.S., require them to return to their home country for two years before applying for an H-1B.
But a government program called the Conrad 30 Waiver Program allows up to 1,500 J-1 holders a year to remain in the U.S. and apply for an H-1B in exchange for working for three years in a provider shortage area, which includes many rural communities.
Trump’s proclamation says employers that sponsor H-1B workers already inside the U.S., such as doctors with these waivers, won’t have to pay the six-figure fee, a nuance clarified in guidance released about a month later.
But employers will have to pay the new fee when hiring doctors and others who apply while living outside the U.S.
Alyson Kornele, CEO of West River Health Services, said most of the foreign nurses and lab techs it hires are outside the U.S. when they apply.
Ivan Mitchell, CEO of Great Plains Health in North Platte, Nebraska, said most of his hospital’s H-1B physicians were inside the U.S. on other visas when they applied. But he said physical therapists, nurses, and lab techs typically apply from abroad.
Holzkamm said it took five to eight months to hire H-1B applicants at her lab before the new fee was introduced.

Bobby Mukkamala, a surgeon and the president of the American Medical Association, said Republican and Democratic lawmakers are concerned about the ramifications for rural health care.
They include Senate Majority Leader John Thune, who said he planned to reach out about possible exemptions.
“We want to make it easier, not harder, and less expensive, not more expensive, for people who need the workforce,” the Republican told ║┌┴╧│╘╣╧═Ї News in September.
Thune’s office did not respond to questions about whether the senator has heard from the administration regarding potential waivers for health workers.
The Trump administration is facing at least two lawsuits attempting to block the new fee. includes a company that recruits foreign nurses and a union that represents medical graduates. , by the U.S. Chamber of Commerce, mentions concerns about the physician shortage and health systems’ ability to afford the new fee.
Kornele said West River won’t be able to afford a $100,000 fee so it’s doubling down on local recruiting and retention.
But Holzkamm said she hasn’t been successful in finding lab techs from North Dakota colleges, even those who intern at the hospital. She said West River can’t compete with the salaries offered in bigger cities.
“It’s a bad cycle right now. We’re in a lot of trouble,” she said.
Phillip Reese is a data reporting specialist and an associate professor of journalism at California State University-Sacramento.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/h1b-visa-fee-rural-hospitals-foreign-worker-shortages-north-dakota/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2123805&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The Trump administration, which has promised “radical transparency,” that it plans to publish the “project summary” for states that win awards. Following the lead of federal regulators, many states are withholding their complete applications, and some have refused to release any details.
“Let’s be clear,” said Alan Morgan, chief executive of the National Rural Health Association. “The hospital CEOs, the clinic administrators, the community leaders: They’re going to want to know what their states are doing.” The NRHA’s members include struggling rural hospitals and clinics, which would benefit from the Trump administration’s Rural Health Transformation Program.
Morgan said his members are interested in what states propose, which of their ideas are approved or rejected, and their budget narratives, which detail how the money could be spent.
Improving rural health care is an “insanely complicated and difficult task,” Morgan said.
The five-year Rural Health Transformation Program was approved by Congress in a law — the One Big Beautiful Bill Act — that also drastically cuts Medicaid spending, on which rural providers heavily depend. It’s being watched closely because it’s a much-needed influx of funds — with a caveat from the Trump administration that the money be spent on transformational ideas, not just to prop up ailing rural hospitals.
The law says half of the $50 billion will be divided equally among all states with an approved application. The rest will be distributed through a points-based system. Of , $12.5 billion will be allotted based on each state’s rurality. The remaining $12.5 billion will go to states that on initiatives and policies that, in part, mirror the Trump administration’s “” objectives.
Health and Human Services Secretary Robert F. Kennedy Jr. has repeatedly promised to open the government to the American people. His agency has devoted to “radical transparency.”
“We’re working to make this the most transparent HHS in its 70-year history,” in written testimony to lawmakers in September.
Lawrence Gostin, a professor of public health law at Georgetown University, said HHS is “acting in a way that utterly lacks transparency” and that the public has the right to demand “greater openness and clarity.” Without transparency, the public cannot hold HHS accountable, he said.
Centers for Medicare & Medicaid Services spokesperson Catherine Howden said the agency will follow the federal regulations when releasing information about the rural health program.
Grant applications are “not released to the public during the merit review process,” Howden said, adding, “The purpose of this policy is to protect the integrity of evaluations, applicant confidentiality, and the competitive nature of the process.”
Democrats and many health care advocates are concerned politics will affect how much money states get.
“I am very concerned about retaliation,” said Rep. Nikki Budzinski (D-Ill.). Because Democrats control her state’s politics, “our application might not be as seriously considered as other states that have Republican leadership,” she added.
Illinois’ Democratic members of the U.S. House to CMS Administrator Mehmet Oz in November asking for “full and fair consideration” of their state application. Illinois officials have not yet released their state’s proposal to ║┌┴╧│╘╣╧═Ї News, which has a pending public records request.
Heather Howard, a professor of the practice at Princeton University, said she is “pleasantly surprised at how transparent the states have been.”
Howard directs the university’s State Health and Value Strategies program, which the rural health fund, and praised most states for publicly posting their project summaries.
“To me, it speaks to the intense interest in this program,” Howard said. Her team, reviewing about two dozen state summaries, found themes including expansion of home-based and mobile services, increased use of technology, and workforce development initiatives like scholarships, signing bonuses, and child care assistance for high-demand positions.
“I think it’s exciting,” Howard said. “What’s great here is the experimentation we’re going to learn from.”
Telerobotics appeared in Georgia’s and Alabama’s applications, she said, including a proposal to use robotic equipment for remote ultrasounds.
Another theme that “warms my heart,” Howard said, was the effort among states to create advisory groups or committees, including in Idaho, where work groups are expected to focus on technology, workforce development, tribal collaboration, and behavioral health.
All 50 states submitted applications to federal regulators by the Nov. 5 deadline and awards will be announced by the end of the year, according to CMS.
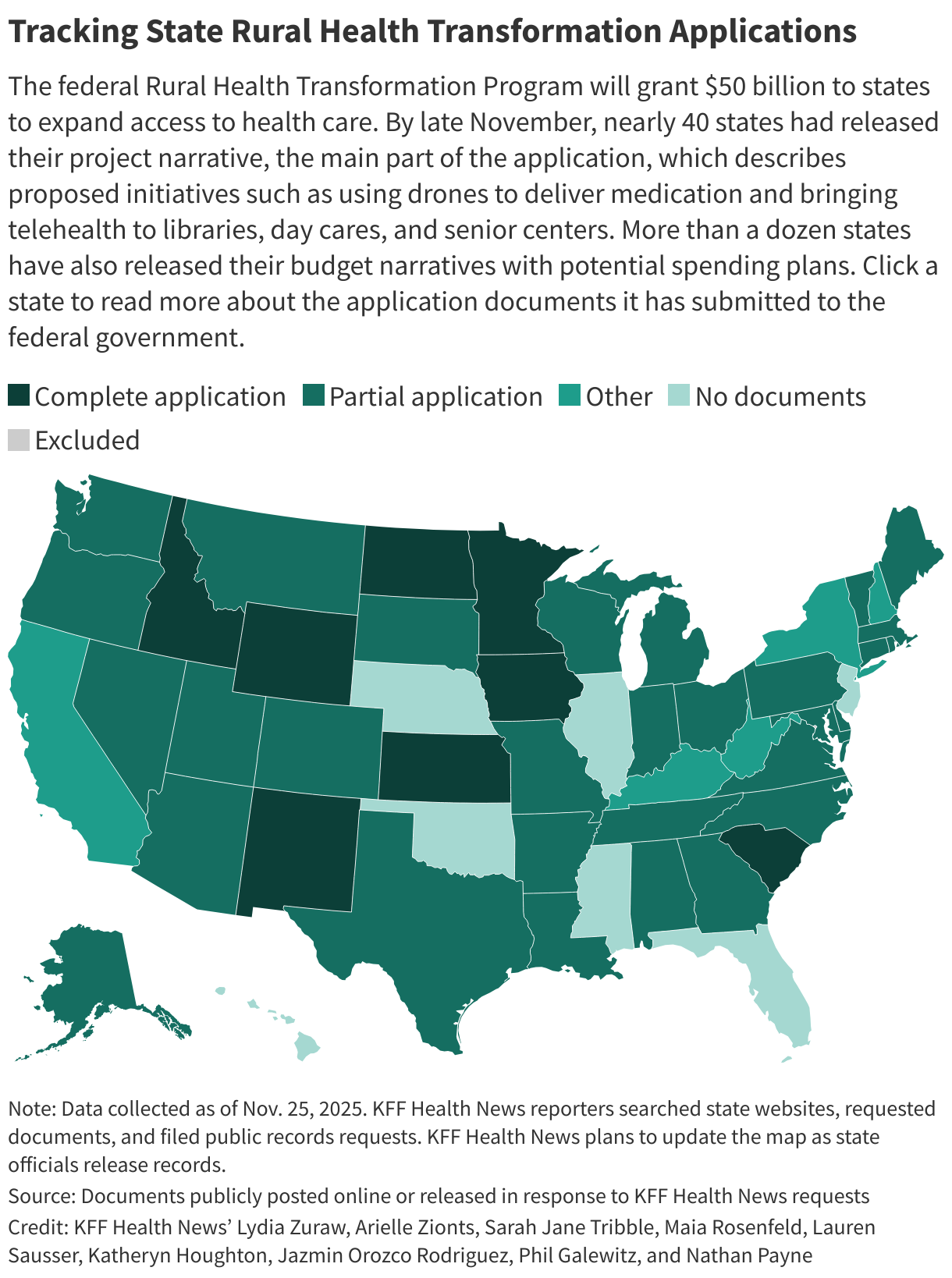
As of late November, nearly 40 states had released their project narrative, the main part of the application, which describes proposed initiatives, according to ║┌┴╧│╘╣╧═Ї News tracking. More than a dozen states have also released their budget narratives.
Also as of late November, only a handful of states — Idaho, Iowa, Kansas, Minnesota, New Mexico, North Dakota, South Carolina, and Wyoming — had released all parts of the application.
║┌┴╧│╘╣╧═Ї News filed public records requests for states’ complete applications. Some states have refused to release any of their application materials.
Nebraska, for example, rejected a public records request, saying its application materials are “proprietary or commercial information” that “would give advantage to business competitors.”
Kentucky shared its application summary but said the remainder of the application is a “preliminary draft” not subject to release under state laws.
Erika Engle, a spokesperson for Hawaii Gov. Josh Green, said the governor “is committed to transparency” but declined to share any of the state’s proposal.
Hawaii and other states are still processing formal public records requests.
The rural health program is part of the July law projected to reduce federal Medicaid spending in rural areas by 10 years.
Those cuts are expected to affect rural health facilities’ bottom lines, threatening their ability to stay open. A recent Commonwealth Fund report found that rural areas continue to to primary care. But the guidelines for the rural health program say states can use only 15% of their new funding to pay providers for patient care.
Between the Medicaid cuts and funding boost from the new program, “there’s real opportunity for national policy to impact rural, both in the negative and the positive potentially,” said Celli Horstman, a senior research associate at the New York-based policy think tank who co-authored the report.
Among the publicly available rural health transformation proposals, Democratic-leaning states show support, or are willing to adopt, some of the administration’s goals but will lose out on points from eschewing others.
For example, New Mexico said it would introduce legislation requiring students to take the Presidential Fitness Test and physicians to complete continuing education courses on nutrition. But it won’t prevent people from using their Supplemental Nutrition Assistance Program benefits to buy “non-nutritious” foods such as soda and candy.
Many states want to invest in technology, including telehealth, cybersecurity, and remote patient monitoring equipment. Other themes include increasing access to healthy food, improving emergency services, preventing and managing chronic illnesses, and enlisting community health workers and paramedics for home visits.
Specific proposals include:
- Arkansas wants to spend $5 million through its “FAITH” program — Faith-based Access, Interventions, Transportation, & Health — to enlist rural religious institutions to host education and preventive screening events. Congregations could also install walking circuits and fitness equipment.
- Alaska, which historically relied on dogsled teams to bring medication to remote areas, is looking to test the use of “unmanned aerial systems” to speed up pharmacy deliveries to such communities.
- Tennessee wants to increase access to healthy activities by spending money on parks, trails, and farmers markets.
- Maryland wants to start mobile markets and install refrigerators and freezers to improve access to fresh, healthy food that often spoils in rural areas with few grocery stores.
State Sen. Stephen Meredith, a Republican who represents part of western Kentucky, said he still expects rural hospitals to close despite his state’s rural health transformation program.
“I think we’re treating symptoms without curing the disease,” he said after listening to a presentation on Kentucky’s proposal at .
Morgan, whose organization represents rural hospitals likely to close, said the state’s ideas may sound good.
“You can craft a narrative that sounds wonderful,” he said. “But then translating the aspirational goals to a functioning program? That’s difficult.”
║┌┴╧│╘╣╧═Ї News staffers Phil Galewitz, Katheryn Houghton, Tony Leys, Jazmin Orozco Rodriguez, Maia Rosenfeld, Bram Sable-Smith, and Lauren Sausser contributed to this report.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/rural-health-transformation-program-cms-state-applications-transparency/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2123985&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Kopplin, a physician assistant who works with seniors, low-income people, and mental health patients in the rural Black Hills, shared her thoughts at a meeting hosted by state officials.
South Dakota’s leaders did a “good job of diving in” and asking questions to get “deeper at the root of the problem,” she said.
Kopplin later told ║┌┴╧│╘╣╧═Ї News how one of her rural patients recently missed two appointments because of a broken-down car and no access to public transportation.
Nationwide, health care workers like Kopplin and thousands of others тАФ from patient advocates to technology executives тАФ flocked to town halls or online portals during the seven weeks state leaders had to craft and submit their applications for the Rural Health Transformation Program to the federal Centers for Medicare & Medicaid Services. That deadline was Nov. 5.
“We will give $50 billion away by the end of the year,” CMS Administrator Mehmet Oz said Nov. 6 at a Milken Institute event in Washington. He said all 50 states had submitted applications.
The program will “allow us to right-size the health care system,” Oz said, adding that innovations from the rural work “will spill over to suburban and urban America as well.”
Among applications and summaries publicly shared by states, themes include workforce development, telehealth, and access to healthy food. In Kansas, leaders want to build a “Food is Medicine” program. Wyoming officials propose a new program called “BearCare,” a state-sponsored health insurance plan that patients could use only after medical emergencies.
But many health policy experts and Democrats are raising alarms that the Republican-backed program will become a “slush fund.” Critics worry it will fail to reach the small-town patients they say need it most, especially as states face nearly a trillion dollars in Medicaid spending reductions over the next decade. Medicaid, a joint federal-state program, serves nearly rural Americans.
“The status quo is tremendous distress in rural communities,” said Heather Howard, a professor of the practice at Princeton University and director of the university’s State Health and Value Strategies program, which is tracking the rural health fund. The new funding won’t be enough to offset the Medicaid losses, she said.
Congressional Republicans added the five-year, $50 billion Rural Health Transformation Program as a last-minute sweetener to President Donald Trump’s massive tax-and-spending legislation. The move helped win support for the One Big Beautiful Bill Act from conservative holdouts who worried that the Medicaid cuts in the bill would harm rural hospitals in their states.
In Montana, which hosted an online public forum before submitting its application, a nonprofit director pitched youth peer support as a way of battling high suicide rates. A registered nurse asked state leaders to “think maybe even bigger” and consider statewide universal health care.
And in Georgia, a technology-focused chain of primary care clinics that serves seniors proposed expanding its operations into that state in its online public comment. A rural grant writer asked for “safe and stable housing.”
The law says half of the $50 billion will be divided equally among all states with an approved application. The rest will be doled out according to a points-based system. Of , $12.5 billion will be allotted based on each state’s rurality. The remaining $12.5 billion will go to states that on initiatives and policies that, in part, mirror the Trump administration’s “” objectives.
Top Senate Democrats have raised alarms about the rural health program. They include Ron Wyden of Oregon and Tina Smith of Minnesota, who a federal watchdog agency to investigate the fairness and implementation of the fund. Taylor Harvey, a Wyden aide, said the Government Accountability Office has confirmed it will investigate.
According to , no less than a quarter of states with an approved application may share the second half of the funding each fiscal year, CMS spokesperson Catherine Howden said. The agency plans to publish summaries of approved state projects, .
A handful of conservative-leaning states тАФ including Texas, Arkansas, Louisiana, and Oklahoma тАФ have already instituted regulatory and legislative initiatives, such as prohibiting “non-nutritious” foods in benefit programs, that in the program application process.
Michael Chameides, a county supervisor in rural New York, said he fears the money could “be used in ways that would hurt certain states or reward certain states.” Chameides is also the communications and policy director with the Rural Democracy Initiative, a national advocacy organization that released last month.
Edwin Park, a research professor at Georgetown University’s Center for Children and Families, said federal lawmakers gave Oz and his agency “really excessive discretion” when awarding the money.
Federal administrators have added rules that aren’t within the statute that created the program, Park said. For example, its application guidelines say states cannot use more than 15% of their funding to pay providers for patient care тАФ payments that are expected to take a hit due to the Medicaid cuts.
Georgetown’s health policy experts and Democrats aren’t the only ones with concerns. and in Ohio worry the money will go to large health systems instead of smaller, independent hospitals that serve people within their rural communities.
CMS’ Oz repeated the idea of getting “big hospitals to adopt smaller institutions” at the Washington gathering after applications were filed. He used similar language at a rural health summit hosted by South Dakota-based Sanford Health. “How do we get big hospitals to adopt smaller hospitals? Not to take them over, but to keep them viable by giving them good telehealth services, specialty support, radiology support,” he said at the October event.
Sanford owns or manages dozens of hospitals and hundreds of clinics and long-term care centers, as well as a health insurance company. The system reported about $81 million in operating income during the first six months of fiscal year 2025, according to .
Last year, Sanford opened a “command center” for its systemwide telehealth initiative. It launched a telehealth expansion in 2021 and offers virtual care for 78 medical specialties, Sanford President and CEO Bill Gassen said.
“We’ve tried to imagine, what if that number doubles?” Gassen said. The startup costs for telehealth are high, he said, and the rural fund could be a unique opportunity “for us to make virtual care available to more patients, to more communities, to more hospitals and health systems across the country.”
Gassen, who is set to chair the American Hospital Association in 2027, said Sanford leaders have met with state and federal officials, including Oz, whom he’s known for years, and Chris Klomp, a top deputy at CMS and a senior adviser to Health and Human Services Secretary Robert F. Kennedy Jr.
The word “telehealth” appears 36 times in the rural health program’s 124-page application guidelines. But Don Robbins Jr., chief executive of a small hospital on the Illinois-Kentucky border, chuckled at the idea of using the funding for that purpose.
Robbins, whose 25-bed Massac Memorial Hospital averages five to seven patients in its beds each day, said his hospital does not regularly offer telehealth. Even if it did, he said, patients living more than a mile outside of town couldn’t use it because they don’t have a good internet connection.
The small hospital reported a $31,314 loss in September, Robbins said. “I think if we get anything out of it,” Robbins said of the rural health program, “we’ll be lucky.”
Kopplin, the physician assistant who attended the South Dakota meeting, is cautiously optimistic about the rural health fund. She views it as a wonderful chance for states to test out ideas and learn from what works and what doesn’t.
But “in a lot of ways this bill is going to be a band-aid approach” for rural health, she said. “It’s not really going to fix the problem.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/states-competing-rural-health-transformation-program-cms/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2113931&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>“It’s going to be the biggest infusion of federal dollars into rural health care in American history.”Robert F. Kennedy Jr. on Sept. 4, 2025, in a Senate hearing

At a September Senate hearing, Health and Human Services Secretary Robert F. Kennedy Jr. boasted about a rural health initiative within President Donald Trump’s “.”
“It’s going to be the biggest infusion of federal dollars into rural health care in American history,” responding to criticism from Sen. Bernie Sanders (I-Vt.). Sanders said the law would harm patients and rural hospitals.
Kennedy was referring to the law’s five-year, $50 billion Rural Health Transformation Program, HHS spokesperson Emily Hilliard said. GOP lawmakers have made similar claims about the program.
The fund was added to the bill at the last minute to secure support from Republican lawmakers who represent rural states. Some were concerned about how the bill’s Medicaid cuts would harm rural America, where have stopped offering inpatient services or been shuttered completely since 2010, according to the Cecil G. Sheps Center for Health Services Research at the University of North Carolina.
“The transformation fund was really talked about in the context of saving rural hospitals that would be facing these significant Medicaid cuts,” said Carrie Cochran-McClain, chief policy officer at the National Rural Health Association. Medicaid is the joint state-federal health insurance program that primarily covers low-income people and those with disabilities.
So is Kennedy right in his description of the rural health fund as a historic cash infusion, or does it fail to acknowledge critical context?
The Rural Health Transformation Program
Trump’s tax and spending law is expected to reduce federal Medicaid spending in rural areas by at least $137 billion by 2034, according to an , a health information nonprofit that includes ║┌┴╧│╘╣╧═Ї News. The the law will increase the overall number of uninsured patients by 10 million by 2034.
Rural health facilities disproportionately rely on Medicaid reimbursement to stay afloat. In 2023, 40.6% of children and 18.3% of adults under age 65 from rural areas and small towns , according to the Center for Children and Families at Georgetown University. In metro areas, the rates were 38.2% and 16.3%, respectively.
The Trump administration argues that rural hospitals cannot rely on “legacy” funding sources like Medicaid and Medicare due to the programs’ reimbursement structure, which ties payments to the number of services provided, a model that’s not financially sustainable for rural facilities with typically low patient volumes.
“Distinct from these other programs, the Rural Health Transformation Program is designed to provide a flexible source of investment” to promote innovation, efficiency, and sustainability, the White House .
Here’s how it works. States can propose projects spearheaded by state agencies, health care providers, consultants, and vendors aimed at various purposes, such as improving technology, access to care, and workforce recruitment.
States can use only 15% of their transformation program funding for provider payments and can direct money to non-rural areas, .
Half of the $50 billion will be evenly divided among states whose applications are approved тАФ regardless of their rural and overall populations тАФ according to the “” for the program.
The other half will be awarded based on “the transformative possibilities” of states’ grant proposals; how much they’ve committed to aligning their health policies with the Trump administration’s; and data on their rural population, rural health facilities, uncompensated care, and other measurements.
The application deadline is Nov. 5.
The Big Picture
Michael Meit, director of the Center for Rural Health and Research at East Tennessee State University, said the rural health community is excited about the innovations the new program might foster, but he’d “love for it to happen in the absence of these cuts that are going to devastate our rural health system.”
“It’s not going to fill the hole,” Meit said.
KFF estimates that the rural health fund’s five-year, $50 billion investment is a little over of federal funding in rural areas that will be spread over 10 years. According to that analysis, Medicaid cuts over that period would tally at least $137 billion in rural areas.
That number doesn’t account for other reductions stemming from the same law, such as cuts to the ACA Marketplaces or the health system revenue loss expected from an increase in the number of people without insurance.
These factors are important to note because the rural health program is a temporary initiative, while reductions in federal spending are long-term.
Another issue is the difference in the program’s spirit. The rural health fund is focused on transforming the rural health care system тАФ not providing continued funding to keep facilities open or making up for lost Medicaid funds. Even if the money triggers successful innovations, there are doubts that those will happen in time to prevent rural health facilities from closing.
“There’s a real misperception that somehow these funds are going to be able to save rural America or save rural hospitals,” Cochran-McClain said.
Joseph Antos, a health policy expert and senior fellow emeritus at the conservative-leaning American Enterprise Institute, said Kennedy’s comment is something “politicians say when they want to ignore the rest of the policies.”
“What they wanted was to say that they were creating a new program,” Antos said. “Well, this is a very inefficient way to distribute a relatively very small amount of money to hospitals that will incur much larger bad debt over the coming years, thanks to the cuts in Medicaid.”
One Caveat
Experts said that when viewed outside of mandatory programs like Medicare and Medicaid, the $50 billion rural health fund does appear to be unrivaled, especially for a limited, five-year program.
Several mentioned the Hill-Burton Act as another program that significantly boosted rural health care. The law provided loans and grants that , many of which were in rural areas, from 1946 to 1997, according to the Health Resources and Services Administration.
Incomplete funding data makes it difficult to account for inflation, said Kelsey Moran, an assistant professor and health economist at the University of Miami.
But that, during the life of the program, it spent $47 billion in 2024 dollars when using the Consumer Price Index, or $109 billion when using the CPI’s medical care index. The medical index has a higher inflation rate because health prices have risen more than overall prices.
Our Ruling
Kennedy said the rural health fund is “going to be the biggest infusion of federal dollars into rural health care in American history.”
The statement contains an element of truth because the new program could be the most significant one-time investment in rural health funding.
But it ignores critical facts and context that create a different impression.
Federal contributions to rural areas from Medicaid and Medicare easily dwarf this program’s $50 billion mark. The new fund offers states flexibility in how they can allocate resources, meaning there’s no guarantee that all the new funding will go to rural Americans’ health care. The program comes at the same time rural areas are expected to lose far more from Medicaid cuts and an increase in uninsured patients than what the rural health fund infusion can backfill.
Experts say the rural health fund’s cash infusion is canceled out by other parts of Trump’s tax and spending law that call for cuts and policy changes.
We rate this statement Mostly False.
Our Sources
“,” CBS News, Sept. 4, 2025.
“$50B Rural Health тАШSlush Fund’ Faces Questions, Skepticism,” ║┌┴╧│╘╣╧═Ї News, July 21, 2025.
“,” Cecil G. Sheps Center for Health Services Research at the University of North Carolina-Chapel Hill, accessed Sept. 15, 2025.
“,” Roll Call, June 20, 2025.
“,” KFF, Sept. 23, 2025.
“,” Congressional Budget Office, July 21, 2025.
“,” Georgetown University Center for Children and Families, Jan. 15, 2025.
“,” The White House, undated.
, government document published on Sept. 15, 2025.
“,” Congressional Budget Office, March 5, 2024.
“,” Congressional Budget Office, March 20, 2025.
“,” HRSA, accessed Sept. 16, 2025.
“,” working paper by Kelsey Moran updated on Sept. 15, 2025.
Phone interview with Matthew Fiedler, a senior fellow in economic studies at the Center on Health Policy at The Brookings Institution, Sept. 24, 2025.
Phone interview with Gbenga Ajilore, chief economist, and Allison Orris, director of Medicaid policy at the Center on Budget and Policy Priorities, Sept. 24, 2025.
Phone interview with Larry Levitt, executive vice president for health policy at KFF, Sept. 24, 2025.
Phone interview with Joseph Antos, a health policy expert and senior fellow emeritus at the American Enterprise Institute, Sept. 23, 2025.
Phone interview with Carrie Cochran-McClain, chief policy officer at the National Rural Health Association, Sept. 17, 2025.
Phone interview with Kelsey Moran, assistant professor in the Department of Health Management and Policy at the University of Miami, Sept. 15, 2025.
Phone interview with Alana Knudson, director of the NORC Walsh Center for Rural Health Analysis at the University of Chicago, Sept. 12, 2025.
Phone interview with Michael Meit, director of the Center for Rural Health and Research at East Tennessee State University, Sept. 11, 2025.
This <a target="_blank" href="/rural-health/fact-check-rfk-jr-misses-mark-calling-rural-health-transformation-program-historic-cash-infusion/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2100987&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>