This story was produced in partnership with
At Swedish Medical Center’s Cherry Hill hospital, the “EMERGENCY” sign glows bright in the dusk above the emergency-room entrance. Some 18,000 people sought help here last year.
Right next to the sign, there’s another one on the building: “After-Hours Clinic.” Operated by Country Doctor Community Health Centers, this clinic — like Swedish’s ER — is open evenings and weekends.
This isn’t competition, but a partnership few would have predicted before the Affordable Care Act, also known as Obamacare. Swedish, a huge, specialty-oriented medical center, has plunked down startup money and a cheap lease to help tiny Country Doctor, whose two clinics were started by idealistic community activists in the late 1960s and early ’70s.
So what has brought these two very different organizations together? In a nutshell: the Affordable Care Act (ACA), with the rumbling disruptions in business-as-usual it has energized. It has changed incentives, brought insurance to people who never had it, and focused attention on unnecessary costs — for example, emergency-room visits for sore throats and ankle sprains.
Both sides see themselves benefiting from this partnership in ways that are part financial, part philosophical. Swedish gains a nonemergency after-hours alternative for patients; County Doctor creates another avenue for those who have had trouble accessing daytime care.
The ACA, by bringing insurance to more, makes the deal affordable for Country Doctor. And by signaling that doctors’ and hospitals’ future livelihood will be linked to value, not volume, the ACA has led Swedish to seek such a partner.
“Before the ACA, hospitals were kind of silos and the alternative providers were silos,” says Howard Springer, Swedish’s administrative director for accountable-care services. Now, for the first time, he says, the two have mutual incentives to cooperate.
The average person may not have read the ACA’s fine print or interpreted the writing on the wall as employers and governments increasingly refuse to play by the old fee-for-each-service rules. But many hospital and clinic leaders understand their world is heading in a new direction.
To make it financially, they’ll have to come together, one way or another, to provide a sort of health-care soup-to-nuts menu, each organization serving not just individual patients but the health of larger communities. This, both of these partners say, is new ground.
“We are not all things to all people,” Swedish’s Springer says. “We are illness-care providers, with a heavy emphasis on specialty care and inpatient care.”
Country Doctors’ clinics, by contrast, focus on primary care and low-income patients, says Dr. Rich Kovar, medical director for County Doctors’ clinics.
It just makes sense for Country Doctor and Swedish to each focus on what it does best, Kovar says. “This is not the solution to all our problems, but it’s the right direction.”
Care for communities
On one recent evening, Brian Stevens, a former sheet-metal fabricator, waits to be seen in the Country Doctor After-Hours Clinic, a bag of clothing and personal effects at his side.
Now homeless, Stevens, 44, does odd jobs for people, such as cleaning gutters and wrestling with climbing rosebushes. A few weeks before, he fell from a scaffold. At a hospital emergency room, he got an X-ray and was told he had no broken bones, and should see his primary-care doctor for follow-up care.
Even though he is newly insured by Medicaid, he couldn’t get in to see a doctor for the next two weeks, and he was hurting.
Another problem: He left his medications on the bus earlier that day.
Patients like Stevens are what Country Doctor does, says Dr. Rich Kovar, medical director for Country Doctor’s clinics.
These days, the clinics pay staff members and use electronic records. But their mission, Kovar says, hasn’t changed from their counterculture origins. Country Doctor began in an abandoned fire station with an all-volunteer staff, and what became Carolyn Downs Family Medical Center grew out of a community effort by the Seattle Black Panthers.
“Our specialty is people without insurance and on Medicaid. That’s what we do,” Kovar says.
Swedish, on the other hand, has been on a different track, building up its specialty centers and services, transforming its southern campus at Cherry Hill into a center for neurosurgery and cardiac care, beefing up its transplant program and building a showcase Orthopedic Institute at its First Hill campus.
Federal regulations have long required hospital emergency rooms to treat all, regardless of ability to pay. Many patients, unable to access care elsewhere because they lacked insurance or were at work during doctors’ hours, sought care in ERs for conditions such as coughs and bladder infections that could have been treated in a doctor’s office.
But as report after report has noted, the ER, with its high costs and lack of continuity for patients, is the wrong place for patients like Stevens, who may need social-services help as much as medical care.
The ACA, by fostering the notion that clinics, hospitals and doctors must think in terms of caring for communities, fueled concerns already afoot. Employers, looking for value, were complaining that uncompensated costs of inappropriate ER visits ballooned their insurance premiums, and the state’s Medicaid program was threatening to restrict payments if hospitals didn’t find ways to better connect patients with primary-care doctors and other services.
At Swedish’s Cherry Hill emergency room, nearly 19 percent of patients seen last year — more than 3,000 — were treated for nonemergency conditions.
“Vulnerable, homeless people — those patients are a huge expense to Swedish,” Kovar notes.
Country Doctor’s clinics, unlike hospital ERs, don’t have high overhead. Half of their patients have had no insurance — above even the 35 percent statewide average for community clinics.
Linda McVeigh, executive director of Country Doctor Community Health Centers, said her organization has long wanted to open such a night-and-weekend-hours clinic.
At about 62,000 patient visits last year, Country Doctor’s daytime clinics were nearing full capacity, and clinic providers often scrambled to find after-hours care for patients.
But after-hours care for people without insurance, cash or credit cards, McVeigh noted, has been virtually nonexistent. “Our poor triage nurses were hugely frustrated that they had nowhere to send people,” she said.
But before the ACA expanded Medicaid eligibility this year, she said, an after-hours clinic was not financially possible. The clinics, as Federally Qualified Health Centers, are focused on underserved patients and bound to take all, regardless of ability to pay. “My concern was that we would get all uninsured patients,” McVeigh said.
The Medicaid expansion makes that less likely. Unlike large medical centers, which often say they lose money on Medicaid reimbursements, Country Doctor’s leaders say they can operate very well on that amount.
Now, McVeigh is eager to bring more patients to the clinic, which opened quietly in December.
Because of federal regulations, Swedish ER staff members can’t simply say to patients with nonemergency conditions: “Hey, why don’t you go next door to Country Doctor?”
But Springer notes there is a “teachable moment” after a visit, when ER staff can explain to a patient that the next time they need a prescription refilled or their rash checked, they might go next door. And, he says, Swedish plans to promote the clinic in the neighborhood.
“My concern at this point is keeping us afloat for the next few months until we can get to a break-even point.” McVeigh says.
Kovar is enthusiastic about the partnership, but even so, he adds: “It’s a gamble. We’re betting the bank.”
“Every reason for us to be partners”
Up to now, major medical centers and community clinics haven’t formed partnerships in this town — or much of anywhere, actually, with very few exceptions.
“Before the Affordable Care Act, hospitals didn’t really partner or even know who the alternative-delivery providers were in their communities,” Springer said.
He recalls a question he put to chief financial officers of regional hospitals at a meeting in 2011: How many knew the name of the heads of their local community-clinic organizations? Not a single hand went up.
Since then, the ACA has changed the willingness and ability of both partners to form such a strange-bedfellows partnership, he said.
Both organizations are contributing. Country Doctor is providing staff, and Swedish, through its foundation, has given $200,000 to sustain the clinic through the startup, leased the building for $1 a year, and pledged to help advertise the clinic.
Kovar and Springer credit Dr. Ralph Pascualy, who heads the Swedish Medical Group representing Swedish medical providers, for seeing early on that Swedish was going to have to make a change.
“The business model had been working pretty well on fee-for-service,” Springer said. “That is not the model that is going to survive in the future.”
Pascualy and others realized that ACA aims to change incentives in health care, moving away from making money by simply doing more and more services — the fee-for-service model that Springer and others call a “volume-based” approach.
The new model, Springer said, will be more focused on value and accountability — meaning offering to provide efficient, cost-effective care to a whole group of people for a price that works for those who pay health-care bills, such as insurers or employers.
But to do that, Swedish calculated that it would have to “embrace and partner with other providers in the community,” Springer says, even though relationships may have been nonexistent or strained in the past.
“We’re trying to change it with this — this was intentional,” says Springer, who sees the model potentially rolling out more broadly.
“This is a kind of trust walk,” Springer says. “There is no reason for us to be competitors. There is every reason for us to be partners.”
şÚÁĎłÔąĎÍř News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/seattle-after-hours-clinic/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=32955&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>With about 16 percent of its residents uninsured, Washington state falls solidly in middie of the pack, with Texas having the highest percentage of residents without health insurance: more than 25 percent. Massachusetts, where a state health-insurance mandate has been in place for years, has the smallest percentage of uninsured residents at just under 5 percent.
But in one way, and not a good one, Washington nearly led the nation, a recent report revealed. From 2008 to 2011, the state’s increase in the number of residents without insurance was second-highest.
The latest numbers come from the U.S. Census Bureau’s recently released 2011 Small Area Health Insurance Estimates for counties and states.
Washington ranked ranked high in two other measures: the percentage of under-age-65 Hispanics without insurance, and the percentage of people under age 65 living at or below the poverty level without insurance.
Only Tennessee had a higher rate of growth in uninsured residents from 2008 to 2011.Ěý Some states stayed virtually the same, and some had decreases.
The Census Bureau’s report also looked at counties. In Washington, the county where the percentage of uninsured residents grew the most from 2008 to 2011 was San Juan with an increase of 4.3 percent. It was followed by Mason and Whatcom counties. King County had an increase of 2.5 percent.
şÚÁĎłÔąĎÍř News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/news/washington-ranks-2nd-in-nation-in-uninsured-growth/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=6185&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story was produced in partnership with
Critics say that Washington state’s rejection of individual health-insurance plans from five companies that applied to sell inside the newly created exchange marketplace will limit consumer choices and hurt continuity of care for those with low incomes.
When Washington state individual health-insurance plans from four companies to be sold inside its newly created , it also rejected efforts by five others.
Now, critics say that rejection will limit consumer choices and hurt continuity of care for those with low incomes.
The plans, targeted at uninsured individuals, are a central feature of the , which aims to offer insurance plans through state online exchanges, where customers can easily compare plans and perhaps qualify for free or subsidized premiums.
State Sen. Linda Evans Parlette, R-Wenatchee, said the state is moving in the wrong direction — away from the stated goal of insurance exchanges to “increase choice and competition for health insurance.”
Her colleague, Sen. Michael Baumgartner, R-Spokane, called the insurance office’s actions a “significant reduction in free-market competition.”
State Insurance Commissioner said some plans had trouble securing adequate networks of providers or meeting other commercial-market regulations, which he said can pose a significant challenge.
“I fully support competition in the market, but it’s also my responsibility to make sure that plans sold in Washington state comply with state and federal law,” Kreidler said. “It’s also critical that if consumers buy a plan, they’re actually able to use the benefits they’re promised.”
Other critics, including Alison Carl White, executive director of , a nonprofit that helps connect families with services, noted that three companies rejected for the have been approved for patients on Medicaid, the state-federal insurance plan for low-income people.
Because those companies won’t be allowed to sell commercial plans inside the exchange, low-income people, who are more likely to have fluctuating incomes, won’t be able to stay with the same insurance company if their income rises to the point they no longer qualify for Medicaid, she wrote in a . If they have to switch from Medicaid to a commercial plan inside the exchange, they may have to move to a new doctor and provider network.
“I don’t know about you, but I think insurance and health care are already pretty complicated,” White said. “The thought of having to switch my insurance plans when my income level changes would be overwhelming especially if I was new to having insurance, struggling to pay rent or feed my kids and make good parenting decisions.”
On Aug. 1, Kreidler’s office announced that 31 individual from four companies were approved to sell inside the exchange.
The approved companies were Group Health Cooperative, BridgeSpan Health Company (an affiliate of Cambia Health Solutions, the parent company of Regence BlueShield), Premera Blue Cross and its subsidiary, Lifewise Health Plan.
The rejected plans were Moda Health Plan (formerly ODS Health), Kaiser Foundation Health Plan of the Northwest, and three Medicaid plans: Coordinated Care Health, a subsidiary of Centene Corp.; Molina Healthcare of Washington; and Community Health Plan of Washington.
Because Lifewise is a subsidiary of Premera, noted Parlette, the Wenatchee legislator, consumers in 19 counties who want to shop inside the exchange will only be able to choose among plans from a single company.
Kreidler gave these reasons for the rejections:
• Molina didn’t allow access to certain providers, and had no approved retail pharmacy.
• Coordinated care had no pediatric hospital in its network, and no approved vision network.
• Community Health Plan of Washington was unable to adjust benefits to meet new cost-sharing requirements, Kreidler said. It also required people, even those in an urban area, to drive more than 47 miles to see a cardiologist and 123 miles to see a gastroenterologist.
• Kaiser had several health-savings account (HSA) plans that didn’t meet state and federal requirements.
• Moda wanted to charge the same rates for plans with different benefits. For example, it included pediatric dental benefits in some plans, but rates didn’t reasonably reflect difference in costs.
Kreidler’s office said some of the plans were new to the commercial market, “and it’s a big challenge to meet the criteria to enter that market.”
In Washington, about 1.2 million people, mostly children, are now covered by Medicaid. The state expects provisions of the Affordable Care Act will add nearly 330,000 more people, mostly adults, over the next few years.
Dr. Mario Molina, president and CEO of Molina, said Washington is the only one of nine states that has rejected Molina’s bid to sell inside an exchange.
Currently, Molina, which has operated in Washington since 2000, covers about 413,000 Medicaid patients in the state, and has a large network of providers, including a pharmacy network, Dr. Molina said.
About 10 to 15 percent each year fall off Medicaid because their incomes have risen, and should be eligible for subsidies inside the exchange, he said.
But now, they won’t be able to stay with Molina if they’re not on Medicaid. “People will have to change health plans, and in many cases, change doctors,” he said. That seems to run counter to the notion of promoting continuity of care and making the marketplace more competitive, he said.
Community Health Plan of Washington, which covers about 305,000 individuals and families through Medicaid plans, said the rejection was a surprise and would have negative consequences for the most vulnerable population.
In a statement, the company said its proposed “member-focused and innovative” plans were designed to address “the unique needs of lower-income individuals.” The plans offered unrestricted access to the First Choice Health Network, including a group of Community Health Centers with more than 100 primary-care centers.
“Unfortunately, the OIC seems unable to move away from an outdated model of commercial insurance, which the Affordable Care Act was intended to reform,” the company said.
Coordinated Care spokeswoman Sally Mildren said the company believes being able to sell inside the exchange is important to help low-income customers. But she said Coordinated Care will work closely with the insurance office in hopes of being able to get approval next year.
Kreidler said it’s not surprising there was a lot of confusion the first year of the new requirements. Now, both his office and the companies have a much clearer understanding of what’s needed, he said. For 2015, they’ll begin working with companies as early as March and April, he said.
“While I wish all of the companies who applied had succeeded, I had to hold everyone to the same standards,” Kreidler said. Many more companies have filed to sell outside the exchange, which the insurance office has until the end of September to approve or reject. Individuals who purchase insurance plans outside the exchange will not be eligible for the reduced premiums.
Carol M. Ostrom: costrom@seattletimes.com or 206-464-2249. On Twitter .Ěý
şÚÁĎłÔąĎÍř News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/washington-state-insurance-plan-exchange-marketplace-limits/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=27170&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story was produced in partnership with
For some people, individual insurance plans offered through Washington’s new online exchange marketplace may cost more than those available now, but they will cover much more, state Insurance Commissioner Mike Kreidler said Thursday.
And although people in some counties will have limited choices, as they do now, in most counties the 31 new plans available from four companies will offer a wide range of premiums and cost-sharing options.
The plans, which are being made available under the federal Affordable Care Act (ACA), sometimes called Obamacare, take effect in 2014. The state Thursday disclosed details of the exchange plans, the centerpiece of the ACA.
Targeted groups are mostly people who don’t have health insurance through employers or who have no coverage at all. The law provides subsidies for those buying these plans whose incomes fall below certain levels.
By law, the plans under the exchange cover a wider range of benefits than most individual plans today, including things rarely covered now, such as prescription drugs, and maternity and newborn care.
Not all companies that applied to sell new individual insurance plans inside Washington’s online exchange marketplace will be able to do so, Kreidler said. Five of the nine companies that applied were turned down because they weren’t able to guarantee access to doctors and hospitals, the insurance office said.
The insurance office also pared premiums overall by 1.8 percent, compared with what the companies originally requested, for a total savings of more than $10 million.
In King, Pierce and Snohomish counties, the companies with approved plans to be sold inside Washington’s Health Benefit Exchange are BridgeSpan Health Company (an affiliate of Cambia Health Solutions, the parent company of Regence BlueShield), Group Health Cooperative, Lifewise Health Plan of Washington and Premera Blue Cross.
Three of those — Group Health, Premera and Lifewise (a Premera subsidiary) — also have been approved to sell individual plans outside the exchange, while six other insurers also have proposed plans. The insurance commissioner has until the end of September to review those plans.
Plans sold outside the exchange must cover the same essential benefits and have the same rules under the federal law, but insurers would not have to set them up to conform to the exchange’s technology and payment system requirements, said Rich Roesler of the insurance office.
Premera spokeswoman Melanie Coon said selling plans outside the exchange allows the company to offer existing customers an easy transition and specific support.
“It’s about customer care,” she said. “We don’t want to dump them into the exchange — we don’t want to lose them.”
The subsidies set up by the federal law to help eligible people pay for premiums are available only in plans purchased through the exchange, which will open for enrollment Oct. 1.
Citizens and legal immigrants who make up to $45,960 and families of four making up to $94,200 a year may be eligible for subsidies, which are scaled by income so people don’t pay more than a certain percentage of their income.
New rules under the ACA also limit out-of-pocket costs in most plans to $6,350 for individuals and $12,700 for families, including deductibles but not premiums.
Plans can no longer have annual or lifetime coverage caps for essential health services.
People with very low incomes also may qualify for a cost-sharing subsidy to help them with deductibles, co-payment, coinsurance and other out-of-pocket costs.
How much people pay for insurance will depend on their age, where they live, whether or not they smoke, and the plan they select. All plans will be offered in at least three different levels of premium and cost-sharing, so consumers can compare.
The lower-level “bronze” plans approved by the insurance office have smaller premiums, but consumers will pay higher cost-sharing percentages. “Gold” plans have larger premiums but smaller cost-sharing requirements.
To illustrate, the insurance office looked at premiums for the lowest-priced plan to be sold inside the exchange at each of the three levels, before subsidies, for three different hypothetical shoppers.
For example, a single 40-year-old non-tobacco user in King County could pay premiums ranging from $213 a month to $351.
A 21-year-old single non-tobacco user could pay from $166 to $274, and a similar 60-year-old from $451 to $744 a month.
In some counties, those under age 30 also could choose a “catastrophic” limited-coverage plan offered by Group Health that would be less expensive than some others.
Earlier this year, the insurance office said it was surprised the proposed rates were not much higher than current similar plans even when the plans offered more extensive coverage.
Kreidler said he thinks many companies came in with reasonable prices because they wanted to attract healthy people, not just those who must buy because they have lots of health expenses.
But for people who have lost employer-sponsored coverage, said Dr. Roger Stark, health-care analyst at the Washington Policy Center, these new rates will be a substantial increase in expense. “Even with the subsidies, people are going to pay more,” he said.
For many people, the premium is what counts, and coverage limits aren’t always apparent — at least while they’re healthy.
Many people who have bought individual plans in the past don’t realize the extent of coverage gaps, Kreidler said. “Your financial exposure could be huge,” he said. “None of us is immune to bad luck, cancer or being in a major accident.”
Comparing existing individual plans and the new plans is difficult. Current plans often limit coverage in ways the new ones can’t, or require consumers to shoulder more of the costs.
So the actuaries in the insurance office took the most popular 2013 plans that were closest to the new ones offered on the exchange, and re-priced them as if they had the same level of coverage. They priced the plans for a 21-year-old, a 40-year-old and a 60-year-old.
In almost all case the old plans, if they had coverage that closely matched the plans approved Thursday, would be much more expensive.
The differences weren’t much for the 21-year-old, but rose with each age group and were most stark for the hypothetical 60-year-old.
For example, the 2013 Regence “Evolve Core 1500” plan with a $2,500 deductible, which covers 32,811 people currently, costs $488 for that 60-year-old.
But if that plan’s coverage were the same as the new “BridgeSpan Exchange Silver” with a $3,000 deductible, and a premium of $638, it would cost $887, the office’s actuaries concluded.
Kreidler said creating and reviewing completely new plans was a scramble for both the companies and his office. “It’s been a learning process with these very new plans, how best to meet the requirements of state and federal law … and price them appropriately.”
Some companies that wanted to offer plans in the exchange were new to the commercial market and weren’t able to guarantee access to certain providers and hospitals.
Kreidler said his office will work with them to help them get ready for plans in 2015.
The insurance office estimates that about 477,400 people in Washington will qualify for subsidies, and the state’s target for enrollment is about 130,000 people by Jan. 1.
People can buy insurance for 2014 until March 31, 2014. After that, if they aren’t insured or exempt under the federal rules, they must pay a penalty on their income tax.
The board of the Health Benefit Exchange must review the approved plans before they become final. A decision is expected Aug. 21.

Carol M. Ostrom: costrom@seattletimes.com or 206-464-2249. On Twitter .
şÚÁĎłÔąĎÍř News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/washington-state-obamacare-health-plans-marketplace-exchange/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=27100&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story was produced in partnership with
At the headquarters of Public Health — Seattle & King County in downtown Seattle, those leading the county’s effort to get people to sign up for insurance under the new federal health-care law are conspiring around a table.

Chris Brown is a navigator specialist with Washington Health Benefit Exchange (Photo by Elllen M. Banner/Seattle Times).
Maybe they could get singer Dave Matthews to urge everyone to get covered, one suggests. Macklemore, sighs a young woman, intoning in a hushed, reverent voice the name of the rising star of Seattle rap and social justice.
For the growing campaign to enroll the uninsured in health insurance as part of the monumental health-care overhaul, signing up healthy young adults — the “young invincibles” — is crucial to success.
But so far, all the brainstorming, like the rest of a flurry of activity around the state, has been largely invisible as the clock ticks toward Oct. 1.
That’s when most uninsured people in Washington will be able to sign up for insurance under the Affordable Care Act (ACA), aka “ObamaCare,” no matter what their health status or pre-existing conditions. And nearly three-quarters of them will qualify for free or subsidized insurance, according to state estimates.
With an influx of federal money — $150 million in grants — and the help of a network of groups and community organizations in every county, a new agency, the  in Olympia, is building the advertising, training and technological infrastructure to support a massive sign-up effort.
Under the law, most individuals, except those specifically , must have health insurance by March 31, 2014, or pay a penalty on their income tax. A similar requirement for businesses to provide employee coverage has been delayed for a year.
About 80 percent of adults in Washington are now insured through private or government programs, including employer-sponsored plans, Medicare and Medicaid, military and veterans’ programs and individual plans, according to the state’s Office of the Insurance Commissioner.
For most people, there will be few new changes. Many elements of the federal law, such as free preventive care and guaranteed coverage for children with pre-existing conditions, have already gone into effect.
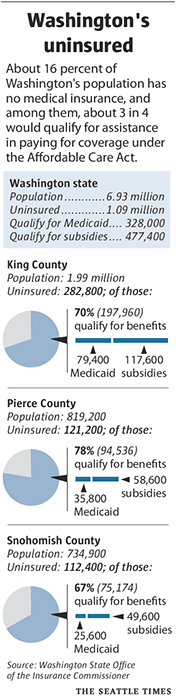
But about 20 percent of adult state residents under age 65 — about 1 million people — are uninsured . (If the state’s entire population is considered, the uninsured make up about 16 percent of the total).
In King County, nearly 300,000 adults have no health insurance, according to the insurance office’s calculations.
U.S. citizens with very low incomes will be able to qualify for Medicaid, the state-federal insurance program. Eligibility has been substantially broadened, and state officials estimate an additional 250,000 adults will qualify .
For those with higher incomes, including legal immigrants here for five years or more, there will be sliding-scale subsidies to help pay private insurance premiums.
The penalty for going bare is $95 per adult or 1 percent of family income, whichever is greater.
The other penalty is being uninsured in the face of a serious, costly health problem.
Progress in the state
Washington state is ahead of many states in setting up key provisions of the ACA: an online insurance-change marketplace and instant-enrollment tool known here as the  (motto: “Click. Compare. Covered.”).
Political leaders in the state made leaps of faith early on, even hiring some key people before the U.S. Supreme Court blessed the act last year.
“We are going to lead the nation in getting our exchange up and running,” Gov. Jay Inslee vowed at a recent meeting.
Despite all this effort, questions continue to dog the organizers.
What if we build a system and they don’t come?
Are subsidies enough to get people to sign up — in particular, those healthy young adults, whose participation and premiums are necessary for a financially healthy marketplace?
What if people simply skip the insurance and pay the penalty?
On the other hand, if lots of people sign up, will they be able to find doctors?
And what happens to those who are left out?
What’s happening now
For now, organizers in Washington haven’t made much noise about the Oct. 1 enrollment opening.
Other states have jumped out with advertising, including online  in Oregon that feature folk singers. Other states’ ads use Super Bowl “competition” themes and cartoons.
Everyone agrees the new law needs some fanfare. Only 62 percent of Americans know that individuals can get subsidies to help pay premiums, and two-thirds of those uninsured say they don’t understand how the federal law might affect them, according to a Kaiser Family Foundation  in March. (KHN is an editorially independent program of the foundation.)
The state’s exchange — which holds the advertising purse strings — is holding off until Sept. 3, when a hotline will go live.
In the meantime, Public Health — Seattle & King County, like other lead agencies in counties across the state, is working with a wider network of community groups and agencies to get the word out.
All around the state, these groups are making plans for “outreach events” at festivals, in libraries, farmers markets, community-college campuses, community centers and more.
They’ll visit with people in food-bank lines, piggyback on state programs for the unemployed and arrange sit-downs with immigrant communities.
And, of course, they will try to reach those key young people at ballgames and rock concerts and through messages from their heroes and confidantes. Oh, and their mothers, who were voted most trusted by that age group in focus-group polls.
After Labor Day, the effort in King County and elsewhere will go into high gear — in English, Vietnamese, Laotian, Mandarin, Amharic, Arabic, Korean, Spanish, Russian, Swahili, Punjabi and more.
Oct. 1 unveiling
On Oct. 1, the shiny new part of this new system will go live: the , an online tool to help the uninsured “shopper” compare health plans and enroll in either private insurance or Medicaid.
Four “” of plans from different insurance companies — ranging from the minimum “bronze” level to “platinum” — require individuals to pay from 40 percent to 10 percent of costs. But all plans must cover 10 “.”
Behind the screen, 60 percent of that $150 million grant the state received has gone toward setting up the complex interfaces needed to hook up the state system with federal agencies, including and the .
The goal is that once a person fills out the application to be insured — a process that might take up to an hour — the healthplanfinder will spit out answers within seconds.
Private insurance brokers will continue to help people find insurance, but community agencies may be more likely to reach those who might qualify for assistance.
In King County, for example, about 28 percent of uninsured adults will qualify for Medicaid (now named Apple Health); 42 percent will qualify for subsidies.
Possible hurdles
If past experience is any guide, not everyone who qualifies for subsidies — even for free insurance — will sign up.
Even explaining the concept of insurance can be difficult, especially for people who haven’t had any in the past, or who come from countries where the concept is foreign. What’s this cost-sharing thing? Deductible? Premium?
Then there’s getting those healthy young people to sign up. What happens if they don’t? By law, the program must be financially self-sustaining by Jan. 1, 2015.
A recent analysis in  estimated that the federal law will leave about 503,000 Washington residents without insurance. “It will do little to alter racial disparities in coverage,” wrote the authors.
That’s one side of the coin.
The other: What if everyone signs up and wants care right now?
Adding hundreds of thousands of adults to the ranks of the insured, even over years, means the term “doctor shortage” enters the conversation.
“There already are significant shortages of primary-care providers in rural areas in Washington state, and it’s going to be get a lot worse,” says Dr. Roger Rosenblatt, vice chair of the Department of Family Medicine at the University of Washington and associate director of the UW’s Rural/Underserved Opportunities Program.
As part of the federal law, family-practice doctors and pediatricians will now receive Medicare rates for seeing Medicaid patients, which the state hopes will help open some doors.
But Rudy Vasquez, director of managed-care operations at Sea Mar Community Health Centers in Seattle, cautions: “Coverage alone is not going to cut it.”
Access to specialty care, Vasquez and others warn, will continue to be a problem for Medicaid patients.
Even so, the prospect of movement on health insurance has mobilized and encouraged many, advocates say.
“I have never seen communities come together so quickly,” Vasquez says.
Maybe, just maybe, the county public-health organizers hope, it will include Macklemore. “Do you know him?” someone asks.
Carol M. Ostrom: costrom@seattletimes.com or 206-464-2249. On Twitter @costrom.
şÚÁĎłÔąĎÍř News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/washington-state-young-invincibles-marketplace-exchange/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=26584&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>