Oz, who heads the U.S. Centers for Medicare & Medicaid Services, there was approximately $3.5 billion of fraud in the hospice and home health care industry in Los Angeles County alone. “This administration under President [Donald] Trump is not going to tolerate taxpayer dollars being stolen because people aren’t paying attention anymore. We’re focused on this,” . He claimed the fraud was largely orchestrated by the “Russian, Armenian mafia” and said that most of the money spent on home and community-based services across California “might be fraudulent.”
However, CMS clarified that not all billing activities referenced by Oz were presumed to be improper. And a review of the most recent available data shows that there are hotbeds of health care fraud across the country and across practice areas, most of them allegedly perpetrated by health insurers and other domestic actors, and that California outperforms most other states in recovering fraud dollars.
As the temperature heats up in the conflict between the Trump administration and California, a handful of Republican state lawmakers have entered the fray, accusing Gov. Gavin Newsom in of allowing “rampant fraud.” Democratic state officials insist they aggressively combat fraud, and Newsom has filed a against Oz, calling language in the allegations “baseless and racially charged.”
“The Trump Administration is attempting to take the issue of fraud тАФ a very real, and national issue тАФ and weaponize it against Democratic states,” California Attorney General Rob Bonta said in an early February statement.
Oz said that he would halt “hundreds of millions of dollars” in payments to California if he didn’t get satisfactory answers from state officials. He and Vice President JD Vance announced in late February that they would delay about $260 million in Medicaid payments , another Democratic-led state, over fraud allegations there, and the state is now suing.
Oz has also launched social media campaigns alleging high-dollar public benefit fraud in Democratic-led Maine and New York. On March 17, he added a Republican-led state to his target list: Florida.
Georgetown University professor Andy Schneider, who served as a senior adviser primarily on Medicaid integrity issues during the Obama administration, said fraud has always been an issue across states, dating back decades. About $3.4 billion in Medicare and Medicaid fraud across the country was , according to the most recent report available. Insurers have paid the highest settlements in alleged health care fraud schemes.
“Bad actors trying to steal public health care funds have been around for a long time,” Schneider said.
How California Stacks Up
The federal government is responsible for Medicare, which primarily benefits older people, while Medicaid, which primarily serves people with lower incomes, is a joint federal-state program. Melissa Rumley, a spokesperson for the Department of Health and Human Services’ Office of Inspector General, said the office could not make state-by-state data on Medicare fraud available because the federal probes often cross jurisdictions.
States file annual reports on actions by Medicaid anti-fraud units that are jointly funded with the federal government and run by state attorneys general. They investigate fraud as well as abuse and neglect of Medicaid patients.
These reports provide a sense of the scale of Medicaid fraud across states. In fiscal 2024, states recovered , compared with $949 billion in total Medicaid spending, according to from the HHS Office of Inspector General. California recouped an outsize share, recovering more than 50% of all the criminal recoveries made by the anti-fraud units nationwide in fiscal 2024 even though the state made up only about 17% of enrollment.
California ranked fourth in the U.S. in 2024 in dollars recovered per Medicaid enrollee across civil and criminal investigations, behind the District of Columbia, Montana, and Delaware. It led all the most populous states, followed in order by Texas, Florida, and New York. (California and federal officials noted that state recovery data varies significantly year to year, often because of the length of investigations.)
Vulnerability of Hospice Care
One aspect of health care fraud that has been at the center of Oz’s attack on California is hospice fraud, which has plagued Republican and Democratic administrations.
The use of hospice, intended to provide care to patients expected to die within six months, increased by over 8% from fiscal 2020 to 2024, to about 1.84 million Medicare beneficiaries, significantly.
To combat fraud, the Biden administration in 2023 of hospices in California, Arizona, Nevada, and Texas. The Trump administration Ohio and Georgia.
CMS spokesperson Chris Krepich did not say specifically what criteria were used to choose which states to monitor, only that the decision was based on “activity typically indicative of hospice-related fraud.” As of June, the agency had revoked the Medicare enrollment of 122 hospices in the original four states, but Krepich said a breakdown by state was not available.
While Oz stated there was some $3.5 billion of fraud in the hospice and home health care industry in Los Angeles County alone, his agency clarified that the number is for overall Medicare billing related to hospice and home health services. Krepich said that “not all billing activity referenced in the remarks is presumed to be improper” and added that the agency could not identify the amount of fraudulent activity until an “evidence-based” investigation was completed.
That’s not to say there is no truth to allegations of hospice fraud.
A published in 2022 found “numerous indicators” of large-scale fraud in Los Angeles County, and a highlighted nearly 500 hospices within a 3-mile radius, including 89 companies registered to a single building in Van Nuys. that “hospice fraud has become an epidemic in California.” He noted that state officials have been aggressively combating it for years, including with .
In January, the state in Monterey County with hospice fraud. That follows hospice scam cases in and .
However, California public health officials are overdue in adopting that were supposed to be . The state’s Department of Public Health is currently revising the regulations, according to spokesperson Mark Smith.
In the interim, the state has revoked the licenses of more than 280 hospices over the past two years and is evaluating an additional 300 hospices, . California had licensed hospice agencies as of 2022, according to the state audit.
Civil Rights Complaint
Meanwhile, Newsom is pushing back on Oz. The governor filed his discrimination complaint with the at HHS, which oversees CMS. The office said it will first decide whether it has the authority to investigate, then, if so, will gather information through interviews and documents. However, the process seems designed to aid individuals who have lost a job to discrimination, or to correct a specific policy, and it is unclear whether there could be any real-world consequences.
The governor wants the agency to address “systematic bias from their leadership,” said Newsom spokesperson Marissa Saldivar.
Krepich said CMS “does not target communities, ethnic groups, or states” and bases its decisions on “confirmed investigative findings.” The allegations of organized fraud refer to “documented criminal cases,” Krepich said, providing a link to in which California residents were convicted of using the identities of foreign nationals to steal almost $16 million from Medicare.
It’s unclear what cases Oz was referring to when he spoke of the Russian and Armenian mafia.
Ciaran McEvoy, a spokesperson for the U.S. attorney’s office for the Central District of California, which includes Los Angeles County, said it doesn’t track whether hospice fraud defendants are alleged to be foreign nationals, but he pointed to the office’s online prosecution announcements. None alleged involvement by foreign influences or organized crime.
The state audit references by the U.S. Justice Department under President Barack Obama that an “Armenian-American organized crime enterprise” was behind a nationwide health care scam.
Federal officials at the time described an “international organized crime enterprise” based in Los Angeles and New York but with roots in Russia and Armenia. The scheme involved billing for unneeded medical treatments, not hospice fraud.
A revealed fraud schemes in which hospice operators recruited patients who were not actually terminally ill, then paid kickbacks to doctors who falsely certified these patients as dying so the hospices could bill Medicare. There was no mention of foreign involvement.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/hospice-fraud-medicaid-mehmet-oz-cms-california/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2166080&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Health officials are recommending diet and exercise as alternatives to heavily advertised weight loss drugs like Wegovy and Zepbound, advice experts say is unrealistic.
“Of course he tried eating well and everything, but now with the medications, it’s better тАФ a 100% change,” said Wilmer Cardenas of Santa Clara, who said his husband lost about 100 pounds over about two years using GLP-1s covered by Medi-Cal, California’s version of Medicaid.
California joined several other states in restricting an option they say is no longer affordable as they confront soaring pharmaceutical costs and steep Medicaid cuts under the Trump administration, among . Despite negotiated price reductions announced in November that would make the drugs available at a “dramatically lower cost to taxpayers” and enable Medicaid to cover them, states are going ahead with the cuts, which providers say may undermine patients’ health.
“It will be quite negative for our patients” because data shows people typically regain weight after stopping the drugs, said , medical director of the University of California-San Francisco Weight Management Program.
While California, , , and stopped covering adult GLP-1 prescriptions for obesity on Jan. 1, they continue to cover the drugs for other health issues, such as Type 2 diabetes, cardiovascular disease, and chronic kidney disease.
, , and Wisconsin are planning or considering restrictions, according to KFF’s .
That reverses a trend that saw 16 states covering the medications for obesity as of Oct. 1. Interest in providing the coverage “appears to be waning,” the survey found, likely due to the drugs’ cost and other state budget pressures. North Carolina pulled back GLP-1 coverage in October, but reinstated it in December, bowing to court orders despite a lingering budget shortfall.
Catherine Ferguson, vice president of federal advocacy for the American Diabetes Association and its affiliated Obesity Association, said it’s not clear how states will adjust to the White House plan to lower the cost of several of the most popular GLP-1s through TrumpRx, an online portal for discounted prescription drugs. The price of Wegovy, for example, will be $350 per month for consumers, versus the current list price of nearly $1,350, and Medicare and Medicaid programs will pay $245, according to the plan.
“Many states are facing budgetary challenges, such as deficits, and are working to address the impacts of the changes to Medicaid and SNAP,” Ferguson wrote, referring to the Supplemental Nutrition Assistance Program. “As more details become available for the Administration’s agreements, we will see how state Medicaid responds.”
The Department of Health and Human Services referred questions to the White House, which did not respond to requests for comment on states’ termination of Medicaid coverage for the weight loss drugs.
California projected its costs to cover GLP-1s for weight loss would have more than quadrupled over four years to if it didn’t end Medi-Cal coverage for that use. Medi-Cal has covered weight loss drugs since 2006, but use of GLP-1s soared only in recent years. By 2024, more than 645,000 prescriptions were covered by Medi-Cal across all uses of the medications. The California Department of Health Care Services could not readily provide a breakdown of whether the drugs were for weight loss or other conditions.
When asked whether the state would reconsider its plans in light of the announced price cuts, Department of Finance spokesperson H.D. Palmer said it had no plans to do so. California’s cut is written into .
California officials would not say how much it could save under the TrumpRx plan, citing federal and state restrictions on disclosing rebate information.
Health providers don’t expect the Trump administration’s negotiated price cuts to make much difference to consumers, because pharmaceutical companies already offer some discounts.
“The out-of-pocket costs will still be very cost-prohibitive for most, especially individuals with Medicaid insurance,” Thiara said.
is among the other states that ended their coverage Jan. 1. Officials with the New Hampshire Department of Health and Human Services did not respond to requests for comment.
About 1 in 8 adults are now taking a GLP-1 drug for obesity, disease, or both, up 6 percentage points from May 2024, according to released in November. Over half of users said their GLP-1s were difficult to afford, and many who had stopped the treatment cited the cost.
Public and private payers have been trying to wean patients off to save costs. California health officials said Medi-Cal members and their health care providers “other treatment options that can support weight loss, such as diet changes, increased activity or exercise, and counseling.” That echoes advice from the New Hampshire Medicaid program.
California Department of Health Care Services spokesperson Tessa Outhyse said in an email that the official advice to try those other approaches now “is not meant to dismiss any past efforts, but to encourage Medi-Cal members to take a renewed, proactive, and medically supported approach with their healthcare provider that may appropriately include these additional options.”
But that may be unrealistic, said , founding director of the Center for Clinical Nutrition at Keck School of Medicine of the University of Southern California.
“We definitely want patients to do their part with the diet and exercise, but unfortunately, and from a practical standpoint, that itself frequently is not enough,” Hong said, adding that usually by the time patients see doctors they have already failed at achieving results through those means.
Hong understands why Medicaid programs, as well as private providers, want to cut back on covering the drugs, which can cost per patient per year. However, they can produce twice the weight loss as the medications typically used previously, he said.
A school of medical thought supports patients’ gradually ending their use, but Hong said obesity is generally considered a chronic condition that requires indefinite treatment.
“Once they reach their target weight, a lot of people will try to see whether or not they can wean off,” Hong said. “We do see a lot of patients тАФ when they try to get off, unfortunately, then the weight comes back.”
Medi-Cal members under age 21 for purposes including weight loss, California officials said, citing a federal requirement.
Medi-Cal members are able to keep their GLP-1 coverage if they can demonstrate it is medically necessary for purposes other than weight loss, the department said. Members who are denied coverage can seek a hearing, the department said in to members.
Members will still be able to pay for the prescriptions and may be able to use various discounts to lower costs. Another option is new pills to treat obesity, which will be cheaper than their injectable counterparts. The a pill version of Wegovy on Dec. 22, which will likely run $149 per month for the lowest dosage, and similar weight loss pills are expected to be available in the first half of the year.
While Cardenas said his husband, Jeffer Jimenez, 37, uses GLP-1s primarily for weight loss, Jimenez’s prescription is for his diabetes, so the couple hoped to continue receiving coverage through Medi-Cal.
“He tried a thousand medications, pills, natural teas, exercise program, but it doesn’t work like the injections,” Cardenas said. “You need both.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/california-medicaid-medi-cal-glp1-weight-loss-drugs-ends-coverage-cost/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2135528&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The was created more than two decades ago in response to the Sept. 11, 2001, terrorist attacks on New York City’s World Trade Center and the Pentagon, and the deadly anthrax attacks that began days later. The fund has provided nearly $2.2 billion to over the past 17 years to ready health care systems for the next pandemic, cyberattack, or mass-casualty event.
Recently, that money has been used to combat the bird flu that has in the United States, killed at least one, and . The funds also have been used to respond to crises such as hurricanes, tornadoes, mass shootings, floods, and heat waves.
But the sent to Congress by Trump’s budget director, Russell Vought, proposes eliminating the program, saying the effort “has been wasteful and unfocused” and that cutting it would allow states and cities to “properly” fund their own preparedness plans. Any action is currently stalled by the government shutdown, which stems from a partisan dispute over expiring health care subsidies that affect many of the from Affordable Care Act marketplaces.
Red and blue states say the hospital preparedness funds are essential and could not be readily replaced with local funds. It’s an example of how the White House’s efforts to and natural disasters have imperiled state and municipal reliance on federal resources to meet community needs.
The program “is the main source of government funding for disaster preparedness among hospitals, EMS providers, and other parts of the health care system,” Texas Department of State Health Services spokesperson Chris Van Deusen said.
Texas received more than $20 million from the Hospital Preparedness Program this year, and Van Deusen said it’s unlikely the state could backfill any federal funding gap in the short term since the budget has been finalized through August 2027.
The funds help Texas’ health providers create disaster plans and test hospitals’ ability to boost their capacity in an emergency, he said, while enabling the distribution of medical resources and patient loads so hospitals aren’t overwhelmed during disasters. The program, along with state funding, supports the state’s , which responded to deadly floods this year and the Uvalde school shooting in 2022, among many other emergencies.
Georgia, which received $13.5 million this year, “continues to monitor and plan for potential changes to future federal funding while ensuring health care preparedness efforts across Georgia remain strong and sustainable,” said public health spokesperson Eric Jens.
A California health official called the money vital to ensuring local health care systems can respond to emergencies beyond their usual capacity. The program is the only federal funding devoted to health care system preparedness for such catastrophes, said Department of Public Health spokesperson Robert Barsanti.
“Without this funding, California risks losing critical infrastructure for emergency response, weakening its ability to protect lives, maintain continuity of care, and meet federal preparedness benchmarks,” Barsanti said.
As the most populous state, California receives the most money тАФ nearly $29 million this year тАФ as it struggles with a massive budget deficit and fights a running rhetorical battle with Trump administration officials. The funds go to the state’s public health department; the California Emergency Medical Services Authority, which coordinates the state’s emergency medical system; health care associations; and about 60 local entities. Los Angeles County, with more than a quarter of the state’s population, received an additional $11 million, and the University of California system got $1.2 million.
Neither the White House, the Administration for Strategic Preparedness and Response, which administers the program under the U.S. Department of Health and Human Services, nor the Office of Management and Budget responded to repeated requests for comment about the May proposal to cut the Hospital Preparedness Program.
The Administration for Strategic Preparedness and Response has seen in employees over the past year, The New York Times reported тАФ part of the wider culling of federal workers under Trump.
Already, HHS has delayed the distribution of this year’s Hospital Preparedness Program funds by nearly three months. The funds were supposed to be available to states for use starting in July, but the bulk of the money was not released until late September. Health officials in the waning days of the Biden administration the funds for the nation’s response to the H5N1 bird flu.
The months-long delay “is yet another example of how changes and uncertainty at the federal level threaten critical public health programs in New York state,” said Department of Health spokesperson Cadence Acquaviva. Despite health officials’ best efforts, “delays or elimination of funding places New Yorkers at significant risk in the event of a disaster or emergency,” Acquaviva said.
New York state received nearly $14 million, and New York City more than $9 million.
Illinois Department of Public Health spokesperson Jim Leach said the medical system needs the federal funds to prepare for natural and human-caused disasters of every sort, “regardless of the ebb and flow of any single disease.”
Illinois and Chicago received a combined $15 million from the preparedness program.
During emergencies, the state’s federally funded crisis response program “turns hundreds of Illinois hospitals, EMS, and other health care facilities into a single, coordinated system,” Leach said, adding it saves both lives and taxpayer dollars. “If there is a natural disaster or an infectious disease outbreak, a state would not be able to react quickly enough without the HPP funds.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/hospital-preparedness-program-federal-disaster-funds-state-lifeline/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2107408&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>For more than a decade, the University of California-San Francisco researcher relied on federal grants without incident. But Thakur, a doctor and a scientist, suddenly found herself leading the charge for public health science against President Donald Trump’s political ideology.
Thakur, 45, a pulmonologist who also is medical director of the Zuckerberg San Francisco General Hospital Chest Clinic, is the lead plaintiff among six UC researchers who in June won against the efforts of several federal agencies to carry out Trump’s executive orders seeking to eliminate research grants deemed to focus on areas of diversity, equity, and inclusion. The administration has filed a notice of appeal, and the outcome, whether or not she and her colleagues prevail, could influence both the future of academic research and the health of those she’s spent her life trying to help.
“When this moment hit us, where science was really under attack and lives are at stake, it doesn’t surprise me that she stepped up,” said Margot Kushel, who directs the UCSF Action Research Center for Health Equity and has known Thakur for more than a decade through their work at the center and San Francisco General, the public county hospital.
“We don’t think our work should be political, to be honest,” Kushel said. “Saving people’s lives and making sure people don’t die doesn’t seem to me that it should be a partisan issue.”
Thakur said that after the abrupt funding cuts, she and the other researchers “felt pretty powerless and found that the class-action lawsuit was a way for us to join together and sort of take a stance.”
The suit was filed independently by the researchers and allowed them to show the harm inflicted not just on their own work “but more broadly on public health and public health research,” she said.
Thakur’s study, which received more than $1.3 million in funding from the Environmental Protection Agency and was set to run through November, explores the impact of increased wildfire smoke on low-income communities and communities of color, populations that already experience heightened pollution and other environmental health disparities. The goal is to find ways to help residents limit their smoke exposure, Thakur said, adding that the results could help people no matter their circumstances.
Preliminary findings show that smoke can trigger breathing emergencies among children days after exposure, knowledge that could lead to better treatment, and that smoke intensity may peak during just a few hours when protection is most needed, indicating the need for more precise and timely safety messaging.
Thakur said her studies on health equity and health disparities saw growing federal support during the covid pandemic and a national focus on racism spurred by the murder of George Floyd. The EPA had solicited the grant in 2021 for her and her team to research how climate change affects underserved communities.
Trump, in executive orders blocking federal funding for DEI programs, said they “use dangerous, demeaning, and immoral race- and sex-based preferences” that he said have “prioritized how people were born instead of what they were capable of doing.”
EPA Administrator Lee Zeldin that, in cooperation with the , the administration had canceled more than 400 grants topping $2 billion “to rein in wasteful federal spending.”
The order by U.S. District Judge Rita Lin in San Francisco temporarily blocking the grant terminations covered the EPA, as well as grants by the National Endowment for the Humanities and the National Science Foundation. Lin’s ruling was not a nationwide injunction of the sort restricted by the U.S. Supreme Court in .
The Trump administration agencies affected by the order have reinstated the UC grants as the lawsuit proceeds. The government filed a motion for a temporary stay on the order pending the outcome of its appeal, but a decision had not been issued as of publication.
The EPA declined to comment on the judge’s order blocking the attempted cancellation of the research funding, citing the ongoing litigation, and attorneys representing the government did not respond to requests for comment.
Thakur defends the need for research that spotlights disadvantaged communities. Her interest in health equity stems from childhood experiences. The daughter of immigrants from India, with a physician and an engineer as parents, she grew up relatively well-off in a mixed-income neighborhood in Phoenix. While she prospered, however, she had friends who couldn’t afford college or became pregnant as teenagers.
“I see my research being directed towards trying to understand how where you live and what you experience impacts your health,” Thakur said.
When the grants were suspended in April, the researchers were unable to finish identifying ways to help protect communities from wildfire smoke. Thakur had to dismiss a student intern and dip into discretionary funds to pay her postdoctoral fellow. At least three research papers that could have directly affected public health were in danger of going unpublished without the funding, she said.
The government reinstated her team’s grants about three weeks after the judge’s order, and Thakur is in the process of picking up the pieces. She’s hopeful that researchers can publish two of the three studies they were working on.
Thakur said she is now cautiously optimistic after experiencing “a roller coaster of emotions.” Putting together a project and conducting the research takes years, she said, so “to have all of that end suddenly, it brought me a range of emotions one thinks about when folks are experiencing grief. There’s denial, anger.”
But the Trump administration’s actions have already sapped morale in the field. Rebecca Sugrue, Thakur’s postdoctoral fellow and an expert in health equity and climate change, is rethinking her entire career path.
“I kind of came to the realization that all the expertise I had built up were the kind of things that were being deprioritized,” Sugrue said. She said she and other postdoctoral students and more junior members of the research team even had discussions about leaving academia: “тАШUnstable’ and тАШuncertain’ were words that were used a lot.”
The lasting damage is not lost on Thakur. If the grants ultimately disappear, universities won’t have the typical programs to train students or to support academic research, she said, adding that, “I think there are concerns that the sort of divestment from science and research in these particular areas will cause generations of impact.”
This article was produced by ║┌┴╧│╘╣╧═Ї News, which publishes , an editorially independent service of the .╠¤
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/california-researcher-leads-legal-challenge-against-trump-policy-disadvantaged-people/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2069182&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The funds come from nearly $200 million in federal fines imposed because of California’s lack of progress in hiring sufficient mental health staff. They are being used for hiring and retention bonuses, including an extra $20,000 for psychologists and psychiatric social workers тАФ roles with the highest vacancy rates тАФ and $5,000 boosts for psychiatrists and recreational therapists.
“I think it’s important to point out that this is the money that the state saved by not hiring people for these positions,” said Michael Bien, an attorney representing the roughly one-third of California prisoners with serious mental illness in a class action lawsuit. “And we know that not hiring caused suffering, harm, and even death.”
The cash is aimed at countering a scarcity of mental health workers and . State officials blame this dearth of workers for their chronic inability to meet hiring levels required by the long-running suit тАФ a failure that led a federal judge to hold top officials in contempt of court last year. The funds are being distributed after an appeals court in March, saying staffing shortages affect whether prisoners have access to “essential, even lifesaving, care.” The spending plan was jointly developed by attorneys representing prisoners and state officials.
Janet Coffman, a professor at the University of California-San Francisco Institute for Health Policy Studies, said planned improvements in working conditions should help with hiring, but she was skeptical of the impact of bonuses.
“What I don’t see is the sustained increases, the increases in salaries over the long term, which is what I think is probably more effective for retention than one-time bonuses,” Coffman said.
The state did not take that view. Its expert witness, labor economist Erica Greulich, testifying during the 2023 trial that led to the fines, said that higher salaries were unlikely to meaningfully increase hiring.
Facing a $12 billion deficit, Gov. Gavin Newsom in May proposed across state government that would “make it extremely difficult to fill chronically vacant mental health positions,” said Abdul Johnson, chief negotiator for the bargaining unit representing health and social service professionals in prisons and other agencies. He said he believes California should add longevity pay to retain veteran workers and pay more in areas with higher costs of living.
On the face of it, the salaries for mental health positions at California prisons are competitive with the private sector’s. For example, the range for is $133,932 to $162,372, while the in California ranged from $117,630 to $137,540 last year. The most recent state contract with prison psychiatrists already includes , on top of other sweeteners, with a state salary range topping $360,000, nearly $34,000 above the California mean salary.
But California prisons are competing for behavioral health workers amid a roughly 40% shortage of psychologists and psychiatrists in the state, and that shortfall is expected . For more than a year before the court’s contempt ruling, the vacancy rate for psychologists never fell below 35% тАФ the state is currently recruiting for nearly 300 such positions тАФ while vacancies among social workers ranged from 17% to 29%. The court ruling said the state oversaw “adequate” staffing for psychiatrists and recreation therapists but only periodically succeeded in reducing the vacancy rate below the 10% maximum allowed. Officials are in the process of adding several new positions that are eligible for the bonuses.
Further complicating the hiring push is that other organizations recruiting these professionals can offer more competitive packages, which can include signing bonuses and other perks, according to testimony during the 2023 trial.
The state is also adopting a new hybrid work policy that allows mental health staff to spend part of their time working remotely. The policy will let the state better compete with the private sector, particularly in the remote areas where many prisons are located, Coffman said.
Money from the fines will also go to improving a working environment that the appellate decision said “often took the form of windowless converted cells in old and unheated prisons.” One-time payments ranging from $50,000 to $300,000 are going to various prison mental health programs for things like new furniture and improvements to treatment and office spaces.
“Working in a prison is difficult and dangerous work,” Johnson said. “Our members constantly face threats, physical assaults, and extremely high caseloads.”
Angela Reinhold, a supervising psychiatric social worker at the California Correctional Institution in Tehachapi, said during the 2023 hearings that her office was in a closet, featuring furniture from “1970s at best.”
She compared her situation with that of a co-worker who had recently left for a safer, higher-paying job in the private sector.
“She’s very excited that she gets a bathroom with two-ply toilet paper, not to mention the other office equipment that’s state-of-the-art, and treatment space, and an office that has a view,” Reinhold said. “She’s not risking her safety with her patients, and she gets to telework three times a week.”
Alexandra David, chief of mental health at the California Medical Facility in Vacaville, described working in buildings without adequate heating or cooling, with leaky ceilings and flooded clinical offices.
“You know, it’s an old prison. There are smells and sometimes rodents,” David said during the same hearings.
The California Department of Corrections and Rehabilitation did not respond to requests for comment on the spending plan.
In what Bien characterized as a bid to avoid ill will, all prison mental health workers will benefit from the new expenditures, with current employees and new hires each receiving one-time $10,000 bonuses. All corrections department employees, not just mental health workers, are also eligible for $5,000 bonuses for referrals leading to new hires in understaffed areas. The state estimates that the bonuses will cost about $44 million, although the projection does not include the referral bonuses or bonuses paid to new employees hired during the year.
Future bonuses and other incentives are likely to depend on recommendations from a court-appointed receiver who is developing a long-term plan to bring the prison mental health system up to constitutional standards.
“We do think they have to do better with money, but money alone is not the answer here,” Bien said. “And so that’s why we’re trying to do these working-conditions things, as well as bonuses.”
This article was produced by ║┌┴╧│╘╣╧═Ї News, which publishes , an editorially independent service of the .╠¤
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/courts/california-prison-mental-health-conditions-staffing-shortages-bonuses/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2041223&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Enrollment is high because California goes beyond federal eligibility requirements, opening Medi-Cal to more low-income residents. The state also provides a broad range of benefits, such as vision, dental, and maternity care — some of which is largely paid for by federal dollars but which also affects state spending.
But lately, Medi-Cal has found itself in political crosshairs.
Democrats say the biggest threat to Medi-Cal is $880 billion in GOP budget cuts being mulled in Washington, D.C., which health experts say would require eligibility restrictions, such as work requirements, or program cuts to yield enough savings over a decade. Republicans argue that Medicaid costs have spiked due to fraud and abuse and they criticize state Democrats for making the benefit available to immigrants regardless of legal status.
In March, Gov. Gavin Newsom’s administration borrowed $3.4 billion to cover an unexpected overrun in Medi-Cal, and lawmakers in April appropriated an for the rest of the fiscal year. Although the Democratic governor , he has defended the state’s efforts to get more people covered. In 2022, California’s uninsured rate for residents under age 65 of 6.2%, according to the California Health Care Foundation.
As lawmakers debate funding for the safety net program, here’s what’s at stake for California’s largest health program.
Who’s Covered?
More than a third of Californians depend on Medi-Cal or the closely related Children’s Health Insurance Program to see a doctor, therapist, or dentist. They rely on the program to get medicine and access treatment. It can also be a lifeline for families by allowing people with disabilities and seniors to stay in their homes and providing . It also funds nursing care for seniors.
The overwhelming majority of enrollees qualify because they earn 138% or less of the federal poverty level: for an individual person or $44,367 for a family of four. While that’s low for a state where the tops $96,000, it’s far more generous than , which is 18% of the federal poverty level, or Florida’s, at 26%.
Unlike Alabama or Florida, California extends coverage to low-income adults without dependents. The state also covers more people with disabilities who work, inmates, and other residents who wouldn’t qualify for the benefit program if California lawmakers hadn’t expanded the program beyond what the federal government requires.
According to , Medi-Cal covers about 7.3 million low-income families and an additional 5 million adults, most of whom don’t have dependents. An additional million people with disabilities rely on the program.
Medi-Cal also picks up the tab for 1.4 million residents 65 and older for benefits not covered by Medicare, such as long-term care and dental, hearing, and vision care.
The majority of adult Medi-Cal recipients under 65 work, according to of March 2024 census data. In California, about 42% of nondisabled adults on Medi-Cal work full time and an additional 20% work part time. Those not employed were most commonly caring for a family member, attending school, or ill.
Just over half of Medi-Cal recipients are Latino, about 16% white, 9% Asian or Pacific Islander, and 7% Black, according to . That differs from the nation as a whole, where about 40% of people under age 65 who use Medicaid are white, 30% Hispanic, 19% Black, and 1% Indigenous people.
Where Does the Money Come From?
The federal government pays for about 60% of the Medi-Cal program. Of its nearly $175 billion budget this fiscal year, Washington, D.C., is expected to contribute .
An additional $37.6 billion comes from the state’s general fund. The final $29.5 billion comes from other sources including hospital fees, a managed-care organization tax, tobacco tax revenue, and drug rebates.
California receives 50% in matching federal dollars for core services, such as coverage to children and low-income pregnant women. But it gets a 90% match for the roughly 5 million Californians it has added to rolls under the Medicaid expansion authorized by the Affordable Care Act.
Where Does It Go?
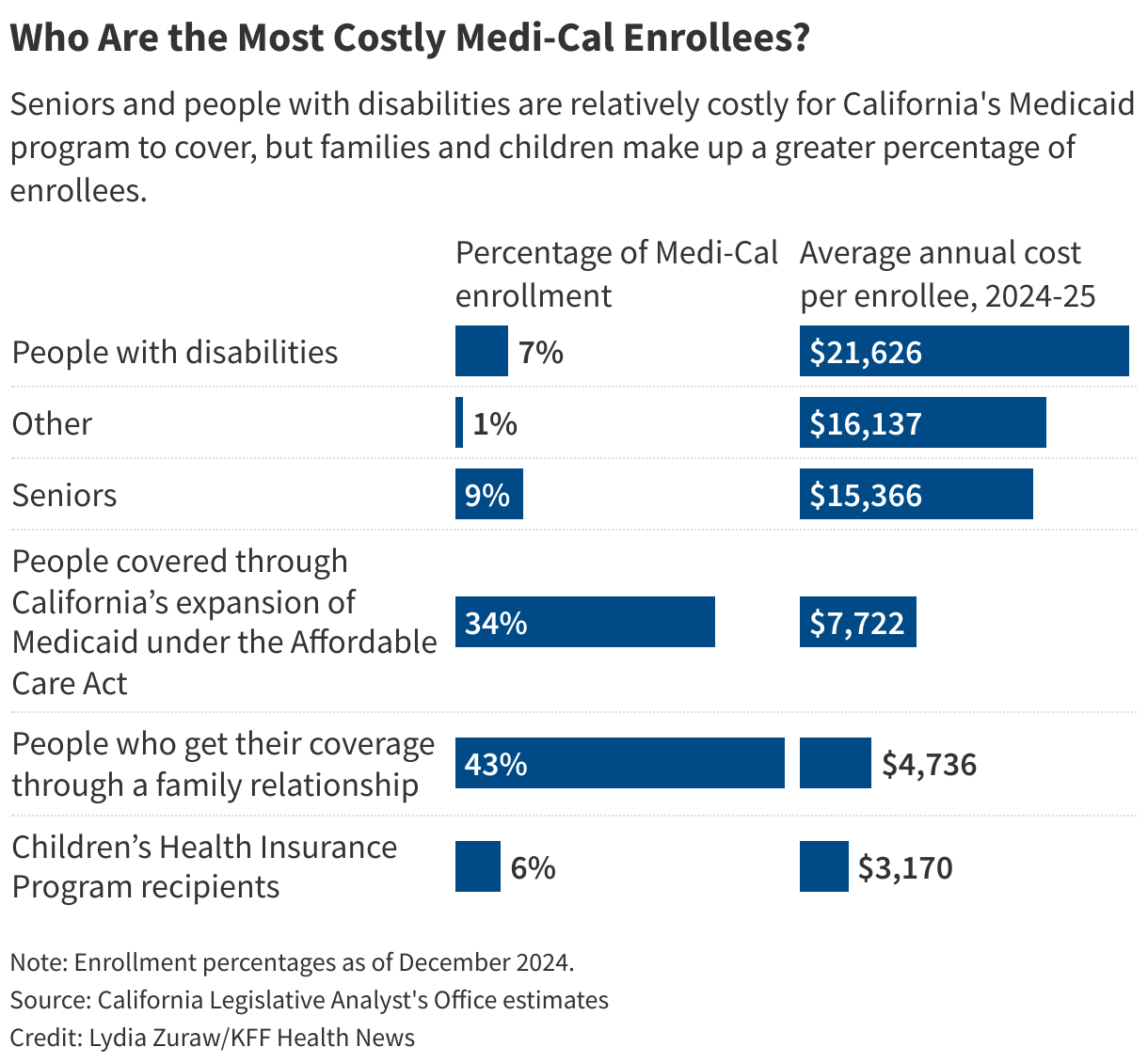
On average, Medi-Cal costs $8,000 per recipient, but costs vary widely, according to a by the California Legislative Analyst’s Office.
For instance, people with disabilities account for 7% of enrollees but 19% of Medi-Cal’s spending, with an average annual cost of $21,626.
Meanwhile, the cost to cover seniors averages roughly $15,000. And senior enrollment, at 1.4 million, has skyrocketed, increasing 40% since 2020 as lawmakers for how many assets people 65 and older could have and still qualify for the program.
California also foots much of the bill to cover immigrants without legal status — roughly $8.4 billion of the $9.5 billion, Department of Finance program budget manager Guadalupe Manriquez said during a .
What Could Get Cut?
President Donald Trump in March said that he would not “touch Social Security, Medicare, Medicaid” but focus on getting the “fraud out of there.” However, health experts say Medicaid services would be gutted if Congress follows through on massive spending reductions to pay to extend Trump’s tax cuts.
Congressional Republicans have discussed implementing work requirements for nondisabled adults, which could affect at least in California, the most of any state, according to an analysis by the Urban Institute.
Lawmakers also could roll back the under the Affordable Care Act, also known as Obamacare, which passed in 2010 and allowed more people to qualify for Medicaid based on income. California, 39 other states, and Washington, D.C., have chosen to adopt “Medicaid expansion,” in which the federal government pays for 90% of coverage for those enrollees.
Such a move would cost California billions each year if it opted to continue coverage for the roughly 5 million additional enrollees who have gained coverage under the expansion.
Republicans could also make it tougher for states such as California to continue to draw federal aid through provider taxes such as the MCO tax, something the first Trump administration proposed but later dropped. The tax on managed care plans brings in a year and was endorsed by voters in last fall, but the federal government has been complaining for years about how states levy such taxes on insurance plans and hospitals. If it restricts how states collect these taxes, it would likely cause a funding gap in California.
If federal cuts occur, Newsom officials acknowledge, the state couldn’t absorb the cost of existing programs. Republicans are pressuring Democrats who control the legislature to end Medi-Cal coverage of residents without legal status — something neither Newsom nor Democratic legislative leaders have expressed a willingness to do.
State leaders also could be faced with cutting such as dental care and optometry, trimming services aimed at enhancing recipients’ , or reducing payments to managed care plans that cover 94% of Medi-Cal recipients.
That’s what California lawmakers did during the Great Recession, cutting reimbursement rates to providers and eliminating benefits including eye and dental care for adults. The governor at the time, Republican Arnold Schwarzenegger, went a step further, chopping $61 million from counties’ Medi-Cal funding in a budget bloodletting that he said contained “.”
This article was produced by ║┌┴╧│╘╣╧═Ї News, which publishes , an editorially independent service of the .
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/aging/medi-cal-california-medicaid-funding-threats-congress-trump-gop-newsom/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2019404&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The unilateral termination is drawing protests from attorneys representing prisoners and the author of the state’s medical parole legislation, who say it unnecessarily puts this vulnerable population at risk. The move is the latest wrinkle in a long-running drive to free those deemed so ill that they are no longer a danger to society.
“We have concerns that they cannot meet the needs of the population for things like memory care, dementia, traumatic brain injury,” said Sara Norman, an attorney who represents the prisoners as part of a nearly three-decade-old federal . “These are not people who are in full command and control of their own surroundings, their memories тАФ they’re helpless.”
Caring for a prison population is a growing problem across the United States. It is twice as expensive to imprison older people than those younger, according to , and prisoners 55 and older are more than twice as likely to have cognitive difficulties as non-incarcerated older adults.
Medical parole is reserved for the sliver of California’s 90,000 prisoners who have a “significant and permanent condition” that leaves them “physically or cognitively debilitated or incapacitated” to the point they can’t care for themselves, . Prisoners who qualify тАФ excluded are those sentenced to death or life without parole тАФ can be placed in a community health care facility instead of state prison.
Attorneys said the roughly 20 parolees the state has returned to lockup need significant help performing basic functions of daily life, with some in wheelchairs or suffering from debilitating mental or physical disabilities. They say outside facilities have the capacity to provide more compassionate and humane care to very ill prisoners.
Kyle Buis, a California Correctional Health Care Services spokesperson, characterized the program as “on pause” as patients return to in-prison facilities and as officials anticipate increasing their use of the compassionate release program. Prisoners granted compassionate release have their sentences reduced and are released into society, while those on medical parole remain technically in custody.
“There were multiple considerations that went into this decision,” Buis said. “Our growing ability to support those with cognitive impairment inside of our facilities was one factor.” Democratic Gov. Gavin Newsom also cited “eliminating non-essential activities and contracts” to save money.
While now has a medical parole law, they are , according to the National Conference of State Legislatures. One common reason is eligibility. Texas, for instance, screened more than 2,600 prisoners in 2022 but approved just 58 people. Officials also often face procedural hurdles, according to the Vera Institute of Justice, a national nonprofit research and advocacy group.
Some states, however, have tried to expand medical parole programs. because an earlier version of the law proved too difficult to use, resulting in the release of just one person. New York has some of the nation’s for release but is among states struggling to find for parolees.
California’s first effort to free prisoners deemed so incapacitated that they are no longer dangerous began in 1997 with a little-used process that allowed corrections officials to seek the release of dying prisoners. But that program resulted in the release of just two prisoners in 2009. The medical parole program was officially created by a that took effect in 2011 and was expanded in 2014 to help reduce prison crowding so severe that federal judges ruled it was harming prisoners’ physical and mental health.
Nearly 300 prisoners had been granted medical parole since July 2014, . The average annual cost per medical parolee was between about $250,000 and $300,000 in 2023, Buis said. And despite when they started the program, he said, Medi-Cal тАФ California’s Medicaid program, which is partly funded by the federal government тАФ did not reimburse the state for their care because they were still considered incarcerated.
California has had a with its sole nursing home contractor for medical parolees. The state ended its contract with in Sylmar at the end of 2024, Newsom reported in January .
In 2021, prison officials said they were sending dozens of paralyzed and otherwise disabled prisoners back to state prisons and , blaming a federal rule change that barred any restrictions on prisoners in such facilities. The move came after state public health inspectors fined Golden Legacy for to the bed in violation of state and federal laws.
Golden Legacy did not return repeated telephone and email requests for comment. Buis said state officials “continuously monitored care at Golden Legacy, and we never had concern for the quality of care provided.”
Attorney Rana Anabtawi, who also represents prisoners in the class-action suit, toured Golden Legacy’s medical parole building with Norman in November and saw caregivers offering memory care patients special art classes and a “happy feet” dance party.
She felt it “was a much better place for our patients than being in prison тАФ there appeared to be regular programming aimed at engaging them, there were no officers walking around, the patient doors were open and unlocked, patients had general freedom of movement within their building.”
Over the past several years, the California Department of Corrections and Rehabilitation has built up its capacity to service those with severely compromised health. The state created two of its own memory care units in men’s prisons, a 30-bed unit in the California Health Care Facility in Stockton in 2019 and a 35-bed unit in the California Medical Facility in Vacaville in 2023. The Central California Women’s Facility in Chowchilla provides up to 24-hour skilled nursing care for women with life-limiting illnesses including dementia.
Yet Norman fears the in-prison facilities are a poor substitute.
“They’re nowhere near enough and they are inside prisons, so there’s a limit to how compassionate and humane they can be,” she said.
In addition to the 20 returned to state prisons when the contract expired, Buis said, one was paroled through the standard process, while 36 were recommended for compassionate release. Of those, 26 were granted compassionate release, eight were denied, and two died before they could be considered.
The use of compassionate release increased under passed in 2022 that , including by adding dementia patients. , 87 prisoners received compassionate release. By contrast, during the six years before the new law, just 53 were freed. Officials expect about 100 prisoners each year will qualify for compassionate release, Buis said.
Compassionate release would allow them to “sort of die with dignity,” said Daniel Landsman, vice president of policy for the criminal justice advocacy group FAMM, previously known as , and ensure “that the California prison system is not turning into a de facto hospice or skilled nursing facility.”
Mark Leno, who authored California’s medical parole law when he was a Democratic state senator, criticized prison officials for ending their use of the law without legislative approval and instead just terminating the Golden Legacy contract. He also railed against returning very ill patients to prisons, a decision he called “perfectly inhumane.”
“Is it just cruel punishment and retribution or is this thoughtful execution of the law put in place by the legislature?” he said.
This article was produced by ║┌┴╧│╘╣╧═Ї News, which publishes , an editorially independent service of the .╠¤
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/mental-health/california-medical-parole-critically-ill-prisoners/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2017736&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Senior U.S. District Judge Kimberly Mueller issued her order March 19, identifying Colette Peters as the nominated receiver. Peters, who was Oregon’s and , ran the for 30 months until President Donald Trump took office in January. During her tenure, she in Dublin, east of Oakland, that had become known as the “rape club.”
Michael Bien, who represents prisoners with mental illness in the long-running prison lawsuit, said Peters is a good choice. Bien said Peters’ time in Oregon and Washington, D.C., showed that she “kind of buys into the fact that there are things we can do better in the American system.”
“We took strong objection to many things that happened under her tenure at the BOP, but I do think that this is a different job and she’s capable of doing it,” said Bien, whose firm women who were housed at the shuttered federal women’s prison.
California corrections officials called Peters “highly qualified” in a statement, while Gov. Gavin Newsom’s office did not immediately comment. Mueller gave the parties until March 28 to show cause why Peters should not be appointed.
Peters is not talking to the media at this time, Bien said. The judge said Peters is to be paid $400,000 a year, prorated for the four-month period.
About 34,000 people incarcerated in California prisons have been diagnosed with serious mental illnesses, representing more than a third of California’s prison population, who face harm because of the state’s noncompliance, Mueller said.
Appointing a receiver is a rare step taken when federal judges feel they have exhausted other options. A receiver took control of , and they have otherwise been used to govern prisons and jails only , mostly to combat poor conditions caused by overcrowding. Attorneys representing inmates have asked a judge to take over prison health care there.
Mueller’s appointment of a receiver comes nearly 20 years after a different federal judge of California’s prison medical system and installed a receiver, currently J. Clark Kelso, with broad powers to hire, fire, and spend the state’s money.
California officials initially said in August that they would not oppose a receivership for the mental health program provided that the receiver was also Kelso, saying then that federal control “has successfully transformed medical care” in California prisons. But Kelso withdrew from consideration in September, as did two subsequent candidates. Kelso said he could not act “zealously and with fidelity as receiver in both cases.”
Both cases have been running for so long that they are now overseen by a second generation of judges. The original federal judges, in a legal battle that reached the U.S. Supreme Court, more than a decade ago forced California to significantly in a bid to improve medical and mental health care for incarcerated people.
State officials in court filings defended their improvements over the decades. Prisoners’ attorneys countered that treatment remains poor, as evidenced in part by the system’s record-high suicide rate, topping 31 suicides per 100,000 prisoners, nearly double that in federal prisons.
“More than a quarter of the 30 class-members who died by suicide in 2023 received inadequate care because of understaffing,” prisoners’ attorneys wrote in January, citing the prison system’s own analysis. One prisoner did not receive mental health appointments for seven months “before he hanged himself with a bedsheet.”
They argued that the November passage of a ballot measure increasing criminal penalties for some drug and theft crimes is likely to increase the prison population and worsen staffing shortages.
California officials argued in January that Mueller isn’t legally justified in appointing a receiver because “progress has been slow at times but it has not stalled.”
Mueller has countered that she had no choice but to appoint an outside professional to run the prisons’ mental health program, given officials’ intransigence even after she held top officials in and levied fines topping $110 million in June. Those extreme actions, she said, only triggered more delays.
The 9th U.S. Circuit Court of Appeals on March 19 upheld Mueller’s contempt ruling but said she didn’t sufficiently justify calculating the fines by doubling the state’s monthly salary savings from understaffing prisons. It upheld the fines to the extent that they reflect the state’s actual salary savings but sent the case back to Mueller to justify any higher penalty.
Mueller had been set to begin additional civil contempt proceedings against state officials for their failure to meet two other court requirements: adequately staffing the prison system’s psychiatric inpatient program and improving suicide prevention measures. Those could bring additional fines topping tens of millions of dollars.
But she said her initial contempt order has not had the intended effect of compelling compliance. Mueller wrote as far back as July that additional contempt rulings would also be likely to be ineffective as state officials continued to appeal and seek delays, leading “to even more unending litigation, litigation, litigation.”
She went on to foreshadow her latest order naming a receiver in a preliminary order: “There is one step the court has taken great pains to avoid. But at this point,” Mueller wrote, “the court concludes the only way to achieve full compliance in this action is for the court to appoint its own receiver.”
This article was produced by ║┌┴╧│╘╣╧═Ї News, which publishes , an editorially independent service of the .╠¤
If you or someone you know may be experiencing a mental health crisis, contact the 988 Suicide & Crisis Lifeline by dialing or texting “988.”
This <a target="_blank" href="/courts/california-prison-mental-health-judge-receiver-takeover-suicide/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2004064&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Weeks later, a in San Francisco ended with the suspect’s vehicle crashing and sending six people, including a child, to the hospital.
The February crash was a reminder of how dangerous high-speed pursuits can be to the public. At least 30% of police vehicle chases include collisions, and up to nearly one-fifth bring injuries or deaths, according to research cited in a .
But balancing the public appetite for tougher law enforcement with the risks to public health these chases pose is challenging, and as cities nationwide wrestle with what trade-offs they’re willing to accept on either side, experts worry that lives are at risk.
Geoffrey Alpert, an authority on police pursuits, helped craft Oakland’s policy, which allows chases only if police believe a suspect has a gun or committed certain violent crimes. He thinks loosening guidelines would be a menace to public health.
“If you reverse and start chasing for these minor offenses, you’re signing death warrants. It’s extremely dangerous. That’s the reason why people went away from chasing everyone until the wheels fell off,” said Alpert, a criminology professor at the University of South Carolina.
Alpert said there is no convincing evidence that chases deter people from fleeing or lower crime rates. “This is a political decision; it’s not scientific,” he said of the Democratic governor’s drive to loosen these regulations.
The push toward more restrictive chase policies comes as a spike in traffic-related deaths has raised the public health alarm, leading to more local policies focused on road safety. New York City, for example, recently banned chasing drivers for traffic violations and other low-level offenses, reserving vehicle pursuits for suspected felonies or violent misdemeanors. Police Commissioner Jessica Tisch said such pursuits “can be both potentially dangerous and unnecessary.”
Similarly, Houston limited pursuits in 2023 after the Houston Chronicle reported on an increase in .
The Police Executive Research Forum, a national think tank on policing standards, recommended in 2023 that pursuits be allowed only when there has been a violent crime and the suspect is an imminent violent threat.
“You can get a suspect another day, but you can’t get a life back,” wrote Chuck Wexler, the group’s executive director.
Nearly 12,000 police pursuits were , the most recent data available. More than 400 bystanders were injured because of those chases. Of the 34 people who died, five were uninvolved bystanders.
Nationwide, more than 500 people died because of police pursuits in 2020, the first year of the covid pandemic, up from closer to 400 people a year from 2016 to 2019, according to federal data.
But federal statistics understate the danger.
The San Francisco Chronicle found that hundreds of people killed in chases from 2017 through 2021 in federal databases, increasing the number to more than 3,000 people over five years.
Alexis Piquero, a criminologist and previous director of the federal Bureau of Justice Statistics, said high-stakes trade-offs are involved in creating chase policies.
He said that while police chases are “dangerous because they are usually at high speeds or there’s a lot of people around,” he would allow police to chase someone fleeing a traffic stop or a shoplifter fleeing a store.
“If we loosen it to create more things that police can pursue, you also increase the likelihood that bad things could happen,” Piquero said. “What’s the risk-reward calculation that someone is willing to deal with?”
After three people were killed in two years in Oakland as a result of collisions during pursuits, the in December 2022, adding a speed limit on chases. Pursuits dropped from 130 that year to 38 in the first seven months of 2024. The number of captured suspects and recovered firearms fell, too. But while there were no further deaths, the number of injuries to both suspects and bystanders remained static as of July.
By contrast, the California Highway Patrol last year was involved in more than 500 pursuits in Oakland, . They resulted in 155 felony arrests, according to the CHP. Beauchamp did not mention that they also led to 62 collisions, 19 of them involving injuries тАФ a dozen of those to uninvolved third parties, the CHP said in response to an inquiry from ║┌┴╧│╘╣╧═Ї News.
“Police pursuits are dangerous, and we recognize that. That is why we need active supervision and active management during police pursuits,” he said. “But let me be clear: When a criminal flees from the police, it is the community that is suffering, and it is the criminal that is putting people in jeopardy.”
In late January, President Donald Trump Washington, D.C., police officers sentenced to prison for their role in a fatal police chase that killed a 20-year-old on a moped. “They arrested the two officers and put them in jail for going after a criminal,” Trump said in announcing clemency for the officers.
Support for law and order has been gaining ground in progressive parts of the nation. New Jersey in 2022 in response to a surge in car thefts. Washington state lawmakers last year allowed police to pursue of violating the law, instead of only those suspected of specific crimes. Milwaukee loosened its policies and in accidents and injuries.

Even San Francisco shares that sentiment. Less than a year before the February police chase that sent several bystanders to the hospital, voters changed the city’s pursuit policy to allow police to chase committed or is likely to commit a felony or violent misdemeanor.
But for Mark Priano and his family, the drive to change these policies is personal. He had no idea that police in Chico were chasing a teenage driver joyriding with two friends in her mother’s car that dark night in January 2002. The Prianos were headed with their 15-year-old daughter, Kristie, to her high school basketball game.
“We got T-boned. Never saw it coming,” Priano said. “They blew right through the fifth stop sign and she ran right into us going close to 60 miles an hour.”
Kristie died.
Her parents twice tried unsuccessfully to change California law to limit pursuits to when an “,” an effort known as , and started an who have lost loved ones to police chases.
Kristie’s father is still frustrated that the safeguards proposed in their daughter’s name never became law.
“To this day,” Priano said, “pursuits continue to kill innocent victims.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/news/california-police-chase-pursuit-policy-law-order-safety-bystanders/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1991231&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Officials said they began distributing more than 2 million pieces of personal protective equipment in late May, four months before the first human case was confirmed in the state. They said they began ramping up coordination with local health officials in April after bird flu was first detected in cattle in the U.S. Bird flu has now been confirmed at more than in central California, and traces were recently detected at a wastewater sampling site in Los Angeles County. Bird flu was also recently detected in in Sacramento County.
California is putting a number of lessons from the covid-19 pandemic to use, such as coordinating emergency response with local health officials and tracking infectious diseases through wastewater surveillance, as the state tries to limit the spread of bird flu to humans. It’s striving to maintain an adequate emergency stockpile to withstand the first wave of any new public health disaster without hemorrhaging the state budget.
“We are far better prepared to respond to a pandemic than we were in 2020,” said Amy Palmer, a spokesperson for the Governor’s Office of Emergency Services.
For instance, before the coronavirus struck in 2020, the state’s emergency supplies stockpile was barely big enough to crowd two basketball courts.
By the time California ramped up its pandemic response, it had enough personal protective equipment and other disaster supplies to fill 52 football fields. California spent $15.6 billion on direct pandemic response during the covid crisis years, much of it provided by the federal government.
Today, the stockpile fits into about 12┬╜ football fields, though it can seesaw from month to month.
According to the state, the current stockpile includes 101 million face masks, 26 million more than the 90-day supply recommended by .
That includes 88 million N95 masks, more than the emergency services agency said was needed last year. The high-efficiency masks are considered crucial to protect against airborne viruses such as covid-19.
Although the state is building up its stockpile, Palmer could not say if the additional masks are related to fears of bird flu, only that planners are always working “to keep pace with the current risk environment.”
The state’s goal, Palmer said, is to have “an initial supply during emergencies to allow us the time to secure resources,” whether through the federal government or by buying more.
There is no indication of spread between humans in the recent California bird flu cases, and health officials say public risk remains low. Human transmission of bird flu is among several worst-case scenarios for a new pandemic, alongside the possibility of a resurgent mutant coronavirus; wider international spread of mpox, Marburg virus, or Ebola; or an entirely new virus for which there initially is no immunity or vaccine.
Yet, health officials nationwide have struggled to track bird flu transmission. And California has a history of swinging back and forth on preparedness.
Republican Gov. Arnold Schwarzenegger in California’s pandemic preparedness in 2006 in response to an earlier threat from bird flu. That included three mobile hospitals that could immediately be deployed during disasters.
Gov. Jerry Brown, a Democrat, in 2011 as state finances went bust. By the time covid struck, the state released 21 million N95 masks, some so old they were date.
Now hospitals are required to maintain their own three-month supply of masks, gowns, and other personal protective equipment under a passed in 2020. California’s also uniquely requires hospitals and other high-risk workplaces to follow precautions such as using negative pressure isolation rooms and the highest level of protective equipment until more is known about a new pathogen.
“It is difficult to overstate the level of unpreparedness exhibited by hospitals both in and outside of California in dealing with the 2020 outbreak of COVID-19,” according to a legislative analysis. “Harrowing images of nurses walking the corridors of hospitals in makeshift masks and garbage bags became commonplace.”
California Hospital Association spokesperson Jan Emerson-Shea said hospitals “continuously prepare to respond to all types of disasters, including outbreaks of transmissible viruses.”
In addition, Palmer said California has five mobile hospitals acquired from the federal government, though they got during the pandemic. She said they have to be maintained, such as making sure pulse oximeters have working batteries.
But, once again, the current deficit has the state trying to strike a balance.
While lawmakers rejected most of Democratic Gov. Gavin Newsom’s $300 million proposed cut to public health funding, the state slashed funding for its stockpile of personal protective equipment by one-third a year ago after it determined that no additional covid-related purchases were necessary, according to the Department of Finance. California eliminated funding this year for eight 53-foot-long trailers that would have moved stockpiled items between warehouses. It’s also cutting nearly $40 million over the next four years from its $175 million disaster stockpile budget.
The state’s preparedness wasn’t good enough for , which gathered more than 1 million signatures to put a ballot measure before voters in November. would have increased taxes on people with incomes over $5 million and used that money for pandemic prevention and response.
But after one of its key financial supporters, former cryptocurrency executive Sam Bankman-Fried, was convicted of defrauding customers and investors. In exchange for initiative backers dropping the measure, to broaden the scope of the California Initiative to Advance Precision Medicine, which was created to focus on developing new medicines and therapies, to include technologies for preventing another pandemic.
“By harnessing the power of precision medicine, California is moving to the forefront of pandemic preparedness and prevention,” Newsom said at the time.
Rodger Butler, a spokesperson for the state Health and Human Services Agency, said it’s unclear if the precision medicine initiative will receive additional funding.
This article was produced by ║┌┴╧│╘╣╧═Ї News, which publishes , an editorially independent service of the .╠¤
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/california-bird-flu-farmworkers-ppe-stockpile/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1939864&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>