This story comes from our partner
The U.S. Department of Health and Human Services has turned down Texas’ request to run a family planning program that excludes certain providers — namely Planned Parenthood — saying it’s a violation of the federal Social Security Act.
But in the same breath, federal officials approved the state’s request for a waiver to expand Texas’ Medicaid managed care program statewide, and to establish funding pools to help providers recoup the costs of uncompensated care.
Gov. Rick Perry called the decisions out of Washington “one step forward” and “two steps back.”Â
“I am concerned the Obama Administration is playing politics by holding women’s health care hostage because of Texas’ pro-life policies,” he said in a statement, “sacrificing the health of millions of Texas women in the name of their pro-abortion agenda.”
In one letter sent to the Texas Health and Human Services Commission on Monday, Cindy Mann, director of the Center for Medicaid and CHIP Services, said the state’s request to circumvent federal rules — namely the Social Security Act — by restricting family planning providers in the Medicaid Women’s Health Program was not acceptable. The state’s request was in keeping with lawmakers’ efforts last legislative session to try to force Planned Parenthood, which provides abortions at some of its facilities, but in none affiliated with the Women’s Health Program, out of business.
“We want to be very clear [that] Medicaid does not pay for abortions and will not pay for abortions,” Mann said in a phone interview. “…We indicated to the state today [that] their proposal violates the longstanding law.”
Mann said the agency would extend Texas’ existing Women’s Health Program through March while state and federal officials try to determine how to proceed.
“We’re very much interested in continuing discussions with them on having a longstanding renewal of the family planning demonstration program,” Mann said. “…The issue here is not whether Medicaid funding is involved but whether the state can restrict access to a qualified health provider simply because they provide other services Medicaid doesn’t pay for.”
In a second letter sent to Texas officials on Monday, Marilyn Tavenner, the acting administrator of the federal agency, said the feds had approved Texas’ request for a waiver to expand its STAR and STAR+PLUS Medicaid managed care programs, and to create funding mechanisms to help keep safety net hospitals afloat and transform the state’s health system.Â
Tom Suehs, HHSC’s executive commissioner, said in a statement that his agency is disappointed with the family planning decision, “which is inconsistent with federal law that gives states the authority to establish qualifications for Medicaid providers.”
In better news, he said, the managed care waiver “will allow us to replace an archaic federal Medicaid funding system with one built around local solutions.”
He added: “These reforms will allow us to ensure the best, most efficient use of Medicaid funding and improve services for Texans.”
şÚÁĎłÔąĎÍř News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/news/texas-tribune-waivers/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=27560&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story was produced in collaboration with
Gov. Rick Perry routinely attacks federal health care reform, calling it a massive overreach that intrudes into the lives of every American. But in the presidential contender’s early days on the campaign trail, he’s revealed little about what his own “Perrycare” could look like — or how much changing American health care will figure into his candidacy.

(Photo by Gage Skidmore via Flickr)
Political strategists say don’t hold your breath: Republican candidates talk very little about health care in primary campaigns because the issue isn’t a top priority for their voters, and because anything beyond hammering “Obamacare” could become a target for critics. They don’t expect Perry to roll out the specifics in stump speeches unless he makes it to the general election, where Democrats could try to hit him on Texas’ low spending on mental health and Medicaid, and the state’s poor rate of insurance coverage. Â
On Wednesday night, the governor’s camp released an early sketch of what his health care plan could entail. Perry spokesman Mark Miner said the first thing the governor would do as president is work with Congress to repeal “Obamacare.” Then he would “start over,” first by working to stabilize the country’s economy for employers, then by trying to “free states from federal mandates and empower them to develop innovative solutions.” Finally, he would attempt to lower skyrocketing health care costs “through the proven, market-based strategies of transparency, choice and competition.” Perry wants states to be given flexibility and incentives to foster competition in the insurance market, to design solutions for patients with pre-existing conditions, to lower costs for small businesses and to implement Texas-style tort reform, Miner said.Â
Candidates on both sides of the aisle have a history of getting into trouble with voters when they unveil too much too soon. When it looked like Arizona Sen. John McCain’s presidential bid might fold in 2007, the candidate produced highly detailed positions on policy issues, said Douglas Holtz-Eakin, president of the American Action Forum and one of McCain’s top advisers in 2008. The result? “Barack Obama spent a lot of time shooting at our health care plan while saying nothing specific himself,” Holtz-Eakin said.
Still, a look at Perry’s legislative history provides surefire clues as to what some of his specifics could be. Policy experts expect a President Perry would seek to allow more state control over the Food and Drug Administration to blast through what he sees as road blocks that prevent medical industries from taking off. And they think he’d shift far more responsibility for running Medicaid — the joint state-federal health insurer that predominantly covers long-term care and poor children — to the states, as evidenced by his requests for more flexibility (and control of the purse strings) from Washington.
At least on the campaign trail, Medicare would probably be excluded from that conversation, because talk of changing the federal health insurance program for the disabled and elderly could frighten seniors — a key voting group, particularly in primaries. Â
“He’s going to have to use the bully pulpit to really explain how states have to take the leadership role and how people have to assume responsibility for themselves,” said Arlene Wohlgemuth, executive director of the conservative Texas Public Policy Foundation, which has guided many of Perry’s key legislative initiatives. “That’s not going to be easy.”
Perry will also have to avoid getting hit too hard by Tea Party loyalists on one of his highest profile health care stumbles: his failed effort in 2007 to make vaccines for the human papillomavirus mandatory for school age girls. Perry has acknowledged that his effort, which he argues was firmly rooted in preventing cervical cancer in a generation of young women, was misguided because he didn’t seek more public input on it. Because the virus can be transmitted sexually, conservatives insist that the vaccine might encourage promiscuity. Health care experts suggest Perry might be able to make up for it with the Tea Party by redoubling efforts to protect patient privacy and requiring consent for virtually everything in the electronic records age.
But state Rep. John Zerwas, R-Simonton, who is an anesthesiologist, said Perry’s best bet will simply be to stay on high alert for any health care policies that could bleed into an individual’s private domain. “You have to be very, very respectful all of the time not to step into the living room of every family out there,” Zerwas said.
Strategists say the fact that Perry doesn’t have an extensive health care record as governor can only help him. Candidates are much more likely to get in trouble for what they’ve done than what they haven’t.
“Talk to [Massachusetts] Gov. [Mitt] Romney,” said Gail Wilensky, a senior fellow at Project Hope, a global health care organization, who advised McCain in 2008. Indeed, Wilensky and others say Perry’s best approach in the primary is to continue attacking the federal health law, not only because polls show that GOP voters overwhelmingly oppose it but because many associate it with his Republican foe, who instituted a similar health insurance mandate in Massachusetts as governor.
“Candidates are trying to distance themselves from Romney,” said Kavita Patel, a fellow at the Brookings Institution who was a health care adviser to Obama during the health reform debate. “Perry has a leg up because he has no Perrycare.”
But if Perry makes it to the general election, he’ll have to show his health care hand. “Usually,” Wilensky said, “Democrats want to talk about it.”
Democrats say if the time comes, they’ve got ammunition. Of all 50 states, Texas has the worst rate of health insurance coverage and mental health spending, and the second worst rate of low-income people covered by Medicaid and per capita spending on Medicaid. It has the lowest percentage of pregnant women receiving prenatal care. It ranks 44th in health care expenditures per capita.Â
Miner suggested Perry’s got his own success stories to offer. Texas has a strong health care industry, he said; Houston’s Texas Medical Center is the largest in the world, and MD Anderson is the no. 1 cancer center in the world. And he argued that the Texas health insurance market is healthy: 133 companies provide coverage, he said, and Texas premiums are lower than the national average.
“Texas continues to pursue measures that will increase access and availability of health care coverage,” he said.Â
şÚÁĎłÔąĎÍř News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/rick-perry-health-care/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=28568&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story comes from
An unlikely battlefield in Texas’ budget war is a hushed pink-and-blue hospital nursery, where 1- and 2-pound babies bleat like lambs under heating lamps and neonatal nurses use tiny rulers to measure limbs no bigger than fingers.
State health officials, searching for solutions to Texas’ multibillion-dollar budget shortfall, have set their sights on these neonatal intensive care units, or NICUs, which they fear are being overbuilt and overused by hospitals eager to profit from the high-cost care – and by doctors too quick to offer pregnant mothers elective inductions and Caesarean sections before their babies are full term.
The Texas Health and Human Services Commission (HHSC), under the gun to find cost savings in the state’s huge Medicaid program, suggested last month it could save $36.5 million over the next biennium by better managing which babies end up in NICUs, curbing so-called convenience C-sections and refusing to finance elective inductions before the 39th week of pregnancy.
“When we look at the data, it indicates that, yes, there is overutilization of NICUs – more babies are being put in NICUs than need to be in NICUs,” said HHSC Commissioner Tom Suehs, adding that two of his own grandchildren were put in Texas hospital NICUs in the last two years, even though they were healthy and their deliveries were uncomplicated.
Lawmakers are not ready to say with certainty that Texas has a NICU overutilization problem, though their comments suggest it. “We are seeing some trends that are a bit troubling,” said State Rep. Lois Kolkhorst, R-Brenham, who has filed legislation to create a commission to study NICU use. Added Sen. Jane Nelson, R-Flower Mound: “We don’t want to reduce services, but we need to combat inefficient, unnecessary use.”
Nor will most hospitals admit to a NICU problem. Couple Texas’ high birth rate, low health insurance coverage and limited prenatal care with the growth of in vitro fertilization, multiple-baby births and so-called geriatric – or past the age of 35 – pregnancies, hospital administrators say, and you have a full NICU. “The services exist because they fill a need,” said Amanda Engler, spokeswoman for the Texas Hospital Association.Â
A need that Natasha and Mark Rosen felt acutely when their son Matthew was born at 1 pound, 14 ounces at Austin’s Seton Medical Center in January, after Natasha had complications with her placenta and started contracting three months before her delivery date. “He only had a 35 percent chance of survival,” she said, holding Matthew, still tethered to plastic tubes and no bigger than a kitten, against her chest, in a daily break from his incubator. “We were so lucky to be here.”
The data suggests NICU beds may not be proliferating due to natural demand alone. Births in Texas are up nearly 18 percent since 1998, according to state health statistics. Meanwhile, the number of NICU beds in Texas hospitals has surged roughly 84 percent, to 2,510 in 2009 from 1,365 in 1998.
State health officials are not shy in suggesting there is a profit motive at play for hospitals. The average routine delivery costs Medicaid $2,500, according to state records; the average NICU stay costs $45,000.
Elective procedures like inducing labor prior to 39 weeks of gestation or delivering a baby via C-section at the mother’s request are only contributing to complications that send babies to the NICU, these health officials say. In 1998, C-sections made up 23.8 percent of Medicaid births, state data shows; more than a decade later, they made up 35 percent. In 2009 alone, 137 Medicaid-covered newborns suffered complications resulting from elective inductions, according to state health officials, costing the Texas Medicaid program $1.6 million.
Dr. Charles T. Hankins, a longtime neonatologist at Texas Children’s Hospital in Houston and an associate professor of pediatrics at the Baylor College of Medicine, suggested there is a far more nuanced motive than pure profit. Hospitals – hard hit by low reimbursement rates and high malpractice costs for routine obstetric care – are simply looking for ways to make up the difference. “A lot of facilities realize if they had a Level 3 nursery, they could help offset their costs,” he said.
He thinks the NICU boom is often driven less by hospitals than by obstetricians, who do their residency training in facilities with NICUs and cannot imagine not having one available for their patients. “The doctors want their patients to be happy, and the hospital administrators want to keep the doctors happy,” he said.
The problem is that diagnosing the need for neonatal care can be subjective, Hankins said. If a hospital wants to increase its NICU census, providers can admit more infants or lengthen their stays – and parents generally trust those assessments. And he said there is no state oversight, either of admission and discharge best practices, or of how NICUs advertise themselves. Some hospitals convert Level 2 NICU beds to Level 3 NICU beds with little to no increase in infrastructure or technology, he said, and no one challenges the designation.
State health officials acknowledge that the NICU designation is up to the hospital and is not reviewed by the state. “Hospitals are willing to work together to accomplish the optimal care for these babies,” Hankins said, but added that they need proper guidance to do so.
Some state lawmakers question what Texas’ Medicaid program has been doing, if not offering this guidance. The growth in NICU beds – much of it along the Texas-Mexico border, which has the youngest population in the state, and in suburban hospitals outside of Houston, Dallas and San Antonio – comes despite years of improvements in prenatal care for mothers on Medicaid, the joint state-federal health program that covers more than half of Texas births.
“One of the tenets of Medicaid has long been better prenatal care, and less babies needing NICUs,” said Sen. Bob Deuell, R-Greenville, a family practice doctor who, in a recent Senate hearing, suggested the cost savings health officials are looking for may not be ample in the delivery room.  Â
But Dr. Frank Mazza, vice president and chief patient safety officer for the Seton Family of Hospitals, said state health officials are on the right path in considering birth inefficiencies. When Seton made the almost unheard-of move in 2005 of prohibiting elective inductions before 39 weeks – part of a system-wide effort to improve perinatal safety – the number of babies admitted to the NICU fell off dramatically. The hospital’s revenue from them also dropped by 95 percent, to $186,000 per year from roughly $4.5 million per year.
“We should have in Texas the safest health care and the most cost-effective health care,” Mazza said. “By keeping babies out of the NICU, you accomplish both.”
Still, even Mazza acknowledged that if his own wife were having a baby today, he would choose a hospital with all the bells and whistles. “Of course I’d want her in a hospital with a NICU,” he said, “with the latest and greatest technology.”
şÚÁĎłÔąĎÍř News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/maternity-wards-nicu-budget-texas-tribune/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=29001&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story, which appeared in , was produced in partnership with

Just a few months ago, Gov. Rick Perry led a group of Texas lawmakers who were threatening to drop out of Medicaid, the state-federal health care program for the poor. A state analysis showing that Texas would lose billions of dollars in financing put an end to talk of opting out.
Now, the debate has shifted, as Texas and other struggling states ask Washington for permission to operate the program as they see fit. Their approach – finding savings by curbing mandatory benefits or limiting eligibility among Medicaid populations – is unlikely to be approved by the Obama administration, which is intent on expanding Medicaid, not shrinking it. And while pressing for a waiver is a far cry from threatening to drop out, it may have the same result: fueling the fire behind Texas’ anti-Washington, state-sovereignty rhetoric.
Texas is hardly the only state pursuing this course; governors across the country are preparing to flood the Department of Health and Human Services with waiver requests. “The feds hold all the power and all the cards here,” said Gov. Mitch Daniels of Indiana, a Republican. “You can expect a whole lot more of this.”
The Obama administration took a small step toward the states’ position this week when it advised Arizona that it would not need a waiver to exclude about 250,000 adults from its Medicaid program – people who were added under special conditions years ago and are not part of the state’s regularly covered Medicaid group.
While many states have received permission to add people to Medicaid over the years, most have not added large numbers, limiting the effect they would see by cutting them. Texas covers slightly more people under Medicaid than federal law requires, meaning that without a waiver, the state could do little to change how it administers the program.
In Texas, Medicaid covers 3.6 million poor, disabled and elderly people, including children, and costs roughly $40 billion per biennium, of which the federal government pays 60 percent.
Texas has pursued a waiver before. In 2008, officials petitioned the Bush administration to redirect some federal hospital money into a Texas pool to help low-income people buy private insurance. The proposal, which was never approved, would have allowed Texas to change Medicaid eligibility levels and start using enrollment caps based on available financing, according to the request.
The difficulty, said Michael Leavitt, who was the secretary of health and human services at the time and is now a health care consultant, was that Texas wanted federal money more than it wanted flexibility.
“At that time,” Mr. Leavitt said, “we were running up against budget constraints, and the administration was not inclined to approve waivers that would increase substantially the outflow from the U.S. Treasury.”
With the state now facing a large budget shortfall, Texas officials want a waiver that gives the state greater flexibility with Medicaid. They want to be able to choose which services to offer, to design eligibility packages tailored to different types of patients, to require Medicaid patients to pay co-pays in emergency rooms so they will see a primary-care doctor instead, and to consolidate Medicaid financing streams now divided by type of care provider. Some are taking an even tougher tack: seeking a federal block grant, effectively a lump sum, to operate Medicaid as Texas sees fit.
“The state puts up almost half of the funding for Medicaid,” said Thomas M. Suehs, executive commissioner of the Texas Health and Human Services Commission. “But we don’t have an equal say in program decisions.”
Ron Pollack, executive director of the consumer group Families USA, said the Obama administration should not allow states to cut enrollment or benefits that are required by federal law. Mr. Pollack said it makes no sense to reduce eligibility leading up to 2014, when an additional 16 million Americans are expected to enroll in Medicaid under the terms of the federal health care overhaul.
The immediate concern for many states is a so-called maintenance of effort provision in the health care law that requires them to maintain current eligibility levels until 2014 or risk losing federal matching money. To complicate matters, federal stimulus financing for Medicaid runs out at the end of June, further cramping states that face a collective budget shortfall of $175 billion through 2013, according to the National Governors Association.
In a recent letter to governors, Kathleen Sebelius, the United States secretary of health and human services, pointed out that the health care law allows states with budget shortfalls to cut adults who are not disabled or pregnant and whose incomes are above 133 percent of the federal poverty level, which is $14,500 for an individual. Ms. Sebelius promised to “expedite review of state ideas” and offered examples of how states could find cost savings in the Medicaid program.
But health care advocates say Texas has few options to save money, because Medicaid benefits here are already so bare-bones that the “optional” services Ms. Sebelius says states could cut are not even offered. And Texas has long since carried out many of the efficiency measures Ms. Sebelius recommends.
Texas officials, who have been strategizing with counterparts in other states on ways to obtain waivers, said they think the Department of Health and Human Services is waiting for direction from Congress before authorizing waivers. Richard Sorian, Ms. Sebelius’s assistant secretary for public affairs, said his boss is planning to announce within the next few weeks new ways for states to get waivers.
But, Mr. Leavitt said, what the agency is talking about is unlikely to provide enough relief to states. The new process would most likely give states fill-in-the-blank templates to make specified changes that are acceptable to the administration, he said.
What states really need, Mr. Leavitt said, is statutory relief from the maintenance of effort requirements, which he expects will be a priority for governors when they meet in Washington the last week in February.
Indeed, Mr. Perry has called on Congress to eliminate those requirements. But Texas wants even more substantive changes in how Medicaid is administered, his office said, including revising the federal formula for financing Medicaid, which is currently built around per capita income. If the formula was based on the percent of the population living in poverty, state officials said, Texas would gain almost $6 billion in federal money a year.
“We need a system that provides for a more market-based health care delivery model that emphasizes individuals sharing in their health care decisions and responsibilities,” said Lucy Nashed, a spokeswoman for Mr. Perry.
And if that help does not come soon? Mr. Leavitt predicts that many states will violate the law and cut eligibility levels anyway. That would place the Obama administration in the tough political position of having to decide how to respond, including whether to withhold federal money from the offending state.
şÚÁĎłÔąĎÍř News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/texas-medicaid-waiver/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=27778&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story was produced in collaboration with
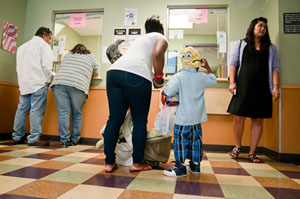
Patients check out at the People’s Community Clinic in Austin, a safety-net clinic that serves Medicaid recipients and the under-insured. The federal government is preparing to reduce the percentage of Texas Medicaid expenses that it currently pays, adding to the state’s fiscal problems. (Callie Richmond/Texas Tribune)
The biggest culprit in Texas’ growing debate over escalating Medicaid costs? A mathematical formula that calculates how much the federal government pays and what’s left over for the state.
Already facing a record budget shortfall, Texas’ (FMAP) will drop more than 2 percentage points in late 2011, equivalent to a $1.2 billion hit. Only two states –Â Louisiana and North Dakota – will face a bigger percentage drop. And that’s after federal stimulus funds that have been artificially enhancing this match dry up in the spring, another blow to cash-strapped state Medicaid programs in Texas and across the nation.
The problems with the Medicaid matching formula “have been talked about for the last 15 years,” says , the state’s Health and Human Services Commissioner. “But the magnitude of the problem and the growth rate of health care spending in general is going to make this a front-line issue.”
Texas’ Medicaid costs have grown a staggering 170 percent in the last 11 years and now account for a quarter of the state’s biennial $182 billion budget –Â a spike that has far exceeded the growth in state tax revenue, inflation and population.
Texas health officials, embroiled in a debate over or , argue the FMAP formula’s determining factor – how a state’s per-capita personal income compares to the national average – is unfair and punitive. They say it strips funding from states that improve their fiscal health but ignores rates of poverty and the uninsured.
Right now, under Texas’ FMAP match, the federal government should be paying 60 percent of the state’s Medicaid costs. Instead, the number is closer to 70 percent, reflecting a boost from federal stimulus dollars that were supposed to run out this month but have been extended through June. Democratic governors, meeting in Washington, D.C., last week, said they doubted Congress would extend the enhanced Medicaid funding again when it runs out this summer.
Texas health officials have already asked for an additional $7 billion in the upcoming budget to make up the difference when Texas’ FMAP match drops back down to 60 percent in July and to maintain current Medicaid and Children’s Health Insurance Program services hard hit by growing enrollment and rising health care costs. But the federal match is projected to drop another 2 points in October, from 60.6 percent to 58.2 percent, a $1.2 billion loss state leaders hadn’t accounted for.
“Virtually every state is struggling to pay for Medicaid,” says Stacey Mazer, a senior staff associate for the . For those that are also watching their match rates decline, she says, “it makes their Medicaid problem even worse.”
The problem with the FMAP formula, Suehs says, is that it creates winners and losers. States with the highest per-capita personal incomes, like New York, get more than their fair share of federal dollars, he says, because of a congressional mandate that caps a state’s FMAP contribution at 50 percent. Meanwhile, Texas is home to 10 percent of the nation’s population living below the poverty line and 14 percent of the nation’s uninsured but receives just under 7 percent of federal Medicaid dollars.
“The current way Medicaid dollars flow is fundamentally flawed,” says Suehs, who predicts Texas will be down to the minimum – a 50 percent federal match rate – in six to eight years, dumping billions more dollars onto the state’s shoulders. “And some states aren’t getting their fair share back.”
Another problem with the formula, critics argue, is that the data on per-capita income lags a few years. For example, the fiscal year 2012 Medicaid match is based on states’ per-capita income average from 2007 to 2009. During that time, per-capita income across the U.S. rose only 0.4 percent; in Texas, it jumped 4.1 percent, reflecting the early part of that period, before the full impact of the economic recession hit. But the state’s per-capita income dropped 3.2 percent from 2008 to 2009; nationally, the per-capita income level dropped 2.6 percent.
Meanwhile, Congress has not tinkered with the formula in recent years out of concern it would lead to higher federal costs for the program, says , who chairs the health policy department at George Washington University. “This goes to the fundamental question of whether the federal Medicaid participation formula is realistic,” Rosenbaum says.
Texas won’t see the biggest percentage drop of any state in fiscal year 2012;Â that unfortunate superlative goes to North Dakota, whose 4.5 percentage point decrease is the state Medicaid program’s biggest in more than 25 years. The drop will cost North Dakota about $105 million in the next budget cycle –Â chump change for Texas but a big deal for a state with a tiny fraction of Texas’ population.
“With this amount of general fund dollars that need to be infused in the program, it is certainly a big budget discussion,” says Maggie Anderson, North Dakota’s Medicaid director.
In addition to Texas and North Dakota, the other states that will see a drop in their federal base match rate next year will be Arkansas, Hawaii, Illinois, Iowa, Kansas, Kentucky, Louisiana, Maine, Mississippi, Montana, Nebraska, New Mexico, Oklahoma, Pennsylvania, Rhode Island, South Dakota, Utah, Vermont and West Virginia, according to Health Management Associates, a consulting firm.
şÚÁĎłÔąĎÍř News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/feds-slated-to-reduce-texas-medicaid-match/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=30855&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story comes from
For years, the state paid private providers who care for people with disabilities to help the clients decide how many services they need and how intensive they should be.
But an 11th-hour change state lawmakers inserted into the budget last session stripped the private providers of this case management responsibility, giving it instead to local, quasi-governmental Mental Retardation Authorities, who administer publicly funded services to people with disabilities.
The goal, lawmakers said, was to avoid conflicts of interest – to ensure the 19,000 people receiving Medicaid waiver services at home and in the community had case managers who were advocating in their best interests and were not motivated by their employer’s bottom line.
The reality, the providers allege, is just the opposite.
Nearly all of the state’s MRAs provide some care services – including operating group homes – in addition to their case management role. Private providers, some of whom say they are losing hundreds of thousands of dollars a year under the new arrangement, argue that if they cannot be case managers, MRAs should not be allowed to provide care services.
“There’s an underlying feeling that they’re cherry-picking, that they’re filling up their homes first,” said Mickey Atkins, chief executive of D&S Residential, a private provider that operates group homes across Texas. “Any time you’re competing with somebody, you want it on a fair playing field.”
MRAs aren’t exactly in the expansion business. Lawmakers passed a bill in 2003 designating them “providers of last resort,” and in 2007, they capped the number of clients to whom they can provide services. Thirty-eight of the state’s 39 MRAs provide some care services, but private providers care for the overwhelming majority – more than 80 percent – of Texans who qualify for the services.
Allison Lowery, a spokeswoman with the Department of Aging and Disability Services, said the goal of last session’s change, which took effect in June, was for people with disabilities to have their care coordinated by someone “who is separate and independent from the service provider.” The shift was part of a larger set of reforms designed to increase the local oversight and monitoring of people receiving care services, said Danette Castle, the CEO of the Texas Council of Community Mental Health and Mental Retardation Centers.
Private providers say that while they understand the intent of the change, it has resulted in more gaps in coordination and, in some regions, a lack of trust. Though the MRA case managers are required to objectively offer clients a complete list of care providers, the private providers say they have no proof that it is happening. Some are asking state health officials and lawmakers to push for a return to the old way in the upcoming legislative session.
MRA officials agree that the debate is one for the Legislature. But they caution that, for years, private providers had to be begged and pleaded to provide community-based care – and even today, some private providers do not operate in remote corners of the state.
“The state has created a situation where future growth is primarily in the private sector,” Castle said, “but they’re still allowing a public sector option for consumers who feel more comfortable there.”
şÚÁĎłÔąĎÍř News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/texas-private-providers-fight-back-over-service-change-tt/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=30787&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story, which appeared in , was produced in partnership with

Patients wait to be seen at the People’s Community Clinic in Austin. (Callie Richmond/The Texas Tribune)
A week after newly emboldened Republicans in the Texas Legislature floated a radical cost-saving proposal – opting out of the federal Medicaid program – health care experts, economists and think tanks are trying to determine just how serious they are, and if it would even be possible.
The answer? It is complicated. But that is not stopping some conservative lawmakers in nearly a dozen other states, frantic over budget shortfalls and anticipating new costs from the federal health care overhaul, from exploring it.
“States feel like their backs are against the wall, so this is the nuclear option for them,” said Christie Herrera, director of the health and human services task force for the , an association for conservative state lawmakers. “I’m hearing below-the-radar chatter from legislators around the country from states considering this option.”
In Texas, some Republicans – bolstered by their expanded majority in the State House – say the strings attached to Medicaid and the Children’s Health Insurance Program (CHIP) are bankrupting the state, which is staring down a budget hole that some have estimated as high as $25 billion. They argue that states could provide more efficient and cost-effective care for children, the disabled and the impoverished by either giving up federal matching money altogether or getting federal officials to grant states waivers to provide health care as they see fit.
Jobless parents in Texas only qualify for Medicaid if their income is below 12 percent of poverty ($22,050 for a family of four), and working parents only qualify if their income is below 26 percent of poverty. Gov. Rick Perry “understands the frustrations of legislators as they deal with a program that consumes 20 percent of the state budget,” said Katherine Cesinger, his spokeswoman. “Their options are severely limited by a federal government that continues to tie their hands when it comes to administering Medicaid.”
Opponents argue that dropping Medicaid would have such a devastating effect on the state’s economy – not to mention the health of 3.6 million Texans currently enrolled in the program – that the idea is pure anti-Washington grandstanding.

Regina Rogoff, executive director of the safety-net People’s Community Clinic in Austin. (Callie Richmond/The Texas Tribune)
The federal government covers 60 percent of Texas’ $45 billion biennial Medicaid budget. Without that money, critics say, any health care the state could provide would be so limited that undercovered patients would flood emergency rooms, and Texans would end up paying the costs through local property taxes or higher insurance premiums.
“The real benefit of Medicaid is it’s a shared expense, with the feds taking up a larger portion,” said Regina Rogoff, executive director of the safety-net in Austin. Speaking of a withdrawal from the program, Ms. Rogoff said: “This will raise local property taxes, because hospital emergency rooms can’t turn away patients. And it has the implication of us paying, through federal taxes, to subsidize care in other states, leaving people who live in our state without care.”
Such fears notwithstanding, the idea of dropping out of Medicaid is on the table in Texas and roughly a dozen other states, including Alabama, Mississippi, Washington and Wyoming. Options include remaking Medicaid with only state financing to give states broad flexibility in benefit and cost design, and, two, seeking federal waivers to allow states to change parts of their Medicaid programs.
“If people are in superbad poverty, that’s one thing,” said State Representative Warren Chisum, Republican of Pampa, the state’s most vocal supporter of dropping out of Medicaid and a candidate for speaker of the House. “It breaks my heart when there’s someone who smokes, and who stays drunk half the time, and we’re supposed to provide their health care.”
Starting in 2014, the new health law extends Medicaid to those with incomes up to 133 percent of the federal poverty level, which is $29,327 for a family of four in 2010. Some conservatives believe that if states dropped Medicaid, many low-income people could instead receive federal subsidies to buy private insurance coverage through state exchanges, another piece of federal health care overhaul that takes effect in 2014. States would then become totally responsible for Medicaid beneficiaries who require nursing homes and other long-term care, for premiums and other Medicaid costs for Medicare beneficiaries – but everyone else would go into the exchange.
Edmund Haislmaier, senior research fellow at , a conservative research organization, estimates that Texas would save $46.5 billion from 2014 to 2019 under this model. In all, Mr. Haislmaier said, 40 states would come out ahead financially.
Others dispute that and note that switching millions of people from Medicaid to subsidized private insurance would be costly to the federal government, and may not be legal.
“The subsidies are explicitly not available for those with incomes below the poverty level,” said Jennifer Sullivan, senior health policy analyst at the consumer group .
Judith Solomon, co-director of health policy at the nonprofit , said the new health care law explicitly stated that only “applicable taxpayers” were eligible for subsidies, ruling out anyone whose income is less than 100 percent of poverty, except for legal immigrants.
Cindy Mann, director of the federal Center for Medicaid and State Operations, said the Department of Health and Human Services was trying to determine whether Medicaid recipients dropped by their home states would qualify for subsidies.

Founded in 1970, the People’s Community Clinic is a primary care center for the medically under served and uninsured. (Callie Richmond/The Texas Tribune)
Critics say dropping out of Medicaid would be a devastating blow to the state’s medically underserved. Seven of 10 Texas nursing home residents rely on Medicaid, which also pays for more than half of all deliveries of babies in the state.
The state’s share of these expenses would not shift to the federal government, said Jose Camacho, executive director of the , but to counties and local taxpayers.
Others fear that cutting off the flow of federal Medicaid dollars could cripple the state’s economy: About a million Texans work in health care, and from 2005 to 2009, a quarter of the new jobs created in the state were in that field.
Tom Banning, chief executive of the , said that without Medicaid, or with a less-extensive replacement program, health care providers would be forced to shift their costs to the private market, driving up insurance premiums and prompting more people to forgo coverage. “From a practical standpoint,” Mr. Banning said, “the downstream economic implications for Texas’ health care infrastructure would be decimating.”
Opponents also say that the theory that a Democratic administration would offer Texas a no- or few-strings-attached Medicaid waiver is a pipe dream. “A state’s choice to get out of Medicaid is to get all the way out, not to pick and choose,” said Anne Dunkelberg, associate director of the , a nonprofit group in Austin.
In the end, said Robert Reischauer, a former director of the Congressional Budget Office, the debate over Medicaid alternatives may be more about states’ leveraging additional federal financing than dropping the program.
“Some states will toy with it, think about it, and reject it from the state perspective,” Mr. Reischauer said. “To the extent they don’t, I would hope Congress and the president work together to create very strong incentives against it.”
Marilyn Werber Serafini is the Kaiser Family Foundation’s Robin Toner Distinguished Fellow based at Kaiser Health News. The fellowship honors the late Robin Toner, The New York Times’ long-time health and politics reporter whose work often framed the public debate on health issues. KHN is an editorially independent news service of the foundation.
şÚÁĎłÔąĎÍř News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/medicaid-drop-out/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=31382&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story comes from
Barbara Cullison waited eight years and eight months to get community-based care for her profoundly autistic daughter Audrey through a popular Medicaid waiver program designed to keep people with disabilities out of institutions. Now, Audrey and thousands of other Texans with disabilities fear losing their services because of budget cuts demanded of state agencies.
Advocates say the Texas Department of Aging and Disability Services’ baseline budget request eliminates financing for more than 13,000 people – the majority of them waiting to receive so-called Medicaid waiver services in private homes, group homes or other community settings. Agency officials say an “unknown number” of people already receiving the services could lose them.
Lawmakers would have to approve another $317 million off of the agency’s budget wish list – called “exceptional items” – to keep the services intact, a pipe dream when the state is facing an estimated $21 billion shortfall and has asked agencies to submit options for cutting their budgets another 10 percent.
“If this goes away, what are we going to do?” asked Cullison, whose daughter just came off of the waiting list for community services in September. “I need that safety net, need to know [that] when I can’t take care of her anymore, there’s a place for her that’s set, that’s paid for. After nine years, I thought I didn’t have to worry about this anymore.”
Agency officials acknowledge their hands are tied. Their current budget proposal means thousands of people sitting on lengthy waiting lists for community-based care likely won’t get it – and some people who already get services will probably lose them.
The community cuts aren’t the only threatened services at the disability agency. Officials there already approved cutting reimbursement rates paid to care providers in the community and at private institutional settings, saving tens of millions of dollars. They’re saving another $2 million through “utilization review”: revisiting high-cost community care plans to “make sure that all recipients are receiving the services they need,” agency spokeswoman Cecilia Fedorov said, “not more or less.”
“We’ve got some lawmakers telling us there will be some services lost, but we’ll end up okay. There are others telling us that nothing’s safe,” said Amy Mizcles, director of governmental affairs for the Arc of Texas. “The reality is, if funding is not restored for those exceptional items, 13,000 people will lose their waivers.”
What’s not clear is if lawmakers can make these service cuts without risking losing federal funding. Federal health care reform requires states to maintain coverage at the same level it was when the Affordable Care Act became law in late March. Stephanie Goodman, spokeswoman for the Health and Human Services Commission, said the agency is asking the Centers for Medicare and Medicaid Services how that requirement will be interpreted, especially when it comes to people who have Medicaid waivers to receive care in the community.
Meanwhile, parents who rely on these community-based services for their disabled children are hoping their families won’t be called up for utilization review. Joe Nester, who has a 29-year-old daughter and a 27-year-old son who receive Medicaid waiver care at home, said his kids have undergone the review process twice – and have narrowly avoided cuts in services both times.
“For the kids, it would’ve been a significant backward step, not to mention our quality of life would’ve become so much worse,” said Nester, of San Antonio. “They need to try to find revenue somewhere else, and not cut services to families who need it.”
şÚÁĎłÔąĎÍř News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/diasbled-medicaid-tt/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=31998&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story comes from
Does a broken hospital bed constitute a medical mistake?
As a federal judge considers the  – and Gov. Ěý–ĚýłŮłó±đ has narrowly ruled that hospital injuries seemingly unrelated to doctor error can still fall under the state’s stringent medical malpractice caps.
The case centers on Irving Marks, who fell while recuperating from back surgery at Houston’s in 2000. Marks alleged that a broken footboard on his hospital bed led to his fall and that he should be entitled to sue St. Luke’s for unlimited damages with a so-called “premises liability” claim. The hospital argued the Marks incident involved medical care and should fall under Texas’ medical malpractice law –Â which requires a timely expert report and caps damages for pain and suffering at $250,000.
The 5-4 high court ruling late last month reversed a 2009 high court decision that Marks’ claims did not fall under medical malpractice law because the bed was not integral to his medical care. Under the new ruling, the court disqualified Marks for damages because he did not get a timely expert report, required in a medical malpractice case, on the broken bed.Â
Texas’ medical lawsuit rules define a health care liability claim as a “cause of action against a health care provider or physician for treatment, lack of treatment” or other medical shortfalls that lead to injury or death. When lawmakers capped damages in 2003, they did it to fix a medical malpractice insurance “crisis,” one they said negatively affected health care delivery in Texas.
The Marks ruling comes at a welcome time for advocates of Texas’ tort reform, including Perry, who is campaigning on a pledge to pass more extensive legislation against what tort reformers call frivolous litigation. Last week, a federal magistrate recommended upholding the constitutionality of the 2003 legislation’s cap on medical liability damages, which is being challenged by several alleged victims of medical malpractice in federal court in the Eastern District of Texas. A judge is expected to rule on the case within the next few weeks.
“The Supreme Court’s prior opinion [in the Marks case] could have opened a huge loophole in Texas’ health care liability reforms, allowing plaintiffs to dodge the expert report requirement and sidestep the noneconomic damage cap,” said Jon Opelt, executive director of the Texas Alliance For Patient Access, which advocates for medical malpractice reform. “Had the court not reversed its earlier decision, plaintiffs might have tried to artfully plead medical malpractice lawsuits as simple negligence cases.”
But trial lawyers say the case could have dangerous repercussions for patients. “The implication for all patients is, regardless of what happens to them in the hospital –Â whether it’s due to a wet floor or the way a bed is put together or an electricity failure –Â this court has found a way to cap the damages,” said Jay Harvey, a medical malpractice attorney based in Austin.
Some legal observers say the Marks decision is a perversion of the intent of the Legislature’s health care liability reform. “If the Legislature had wanted to immunize doctors and hospitals from all tort liability, it could have done so,” said , a professor at the . “But it didn’t.”
The Marks case hinged on the shifting views of Justice , a Republican who wrote the majority opinion in 2009 noting that the hospital bed was “unrelated to any professional judgment and is merely incidental to the patient’s case.” One year later, after the court granted St. Luke’s motion for a rehearing, Medina was the swing vote that led to the ruling’s reversal; he wrote that medical equipment such as Marks’ hospital bed “is an integral and inseparable part of the health care services provided.” In both cases, the vote was 5-4.Â
Medina did not return phone calls to explain his change of heart; a court spokesman said he couldn’t comment on it in the event it comes back for another rehearing. In the dissenting opinion, Chief Justice  expressed concern about the court’s inconsistency. “The Court must explain how a piece of wood at the end of a bed is integral to medical care,” he wrote.
Marks’ attorneys argued the hospital bed claim related to improper maintenance and unsafe conditions and should fall under a premises liability claim – which has no caps – not medical malpractice. The Supreme Court opinion acknowledges that “not every accidental injury to a patient in a health care setting would constitute a health care liability claim.” But a majority of justices said Marks’ case – and thus, a hospital bed –Â does qualify.Â
Harvey, the former president of the , said this means that whenever patients slip and fall in a hospital or trip over some broken equipment, they’ll have to “run and find a maintenance man to write an expert report” if they want to be entitled to any damages.Â
But Charles Bailey, general counsel for the , said that not every fall or injury will be a health care liability claim. He said the Supreme Court ruling offers good insight on one type of equipment in particular: beds. The Marks ruling “does not allow plaintiffs to be clever in how they plead a case to take it outside of healthcare liability,” he said. “This case helps draw some of those important lines.”
şÚÁĎłÔąĎÍř News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/news/tt-texas-malpractice-reform/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=30758&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story comes from
In the wake of high-profile abuse in Texas’ institutions for the disabled, state health officials want to boost payments to them – to the tune of $25,000 per patient per year. But the proposed Medicaid rate change has drawn the ire of Texas’ disability community, which wants to see the facilities shuttered rather than propped up.
The proposed rate increase could be “devastating” for the majority of disabled people who receive state support outside of the centers, says Amy Mizcles, director of governmental affairs with the Arc of Texas, who believes the increased funding at the centers will come at the expense of programs for people with disabilities living in the community.
Texas’ 13 state-supported living centers have been under intense monitoring since last year, when lawmakers agreed to a five-year, $112 million settlement with the U.S. Justice Department over widespread abuse and neglect at the state-run facilities. The proposed rate hike reflects the irony of that victory: The facilities advocates want closed are now protected from statewide Medicaid rate cuts by the settlement and in line for a new windfall.
Already about a third of state dollars for people with disabilities go to the state centers – which serve just 4,200 residents, or 9 percent of people receiving state services, Mizcles says. With the state facing a budget shortfall estimated at $18 billion, advocates believe the state will be forced to cut community-based programs because they can’t cut financing to the centers. “Public dollars can and must be used more effectively,” Mizcles says.
The abuse at Texas’ state-supported living centers in recent years has run the gamut from physical beatings and restraints to medical neglect; in some cases, advocates say, residents died or were permanently injured from their mistreatment. These types of incidents occur in community-based care, too, where people with disabilities receive services in their individual homes or small group settings for a fraction of the cost. Families of state-supported living center residents say the facilities – often on large campuses – provide safety and around-the-clock stimulation. Advocates for independent living say community care is less restrictive, more economical and far safer, because residents aren’t warehoused in a remote institution.
As part of the settlement agreement and reforms lawmakers passed last legislative session, the centers have added staff, implemented new security measures and moved residents into community settings – all at a cost. To meet these costs, and to qualify for a hefty federal match, state officials want to raise Medicaid reimbursement rates to the facilities by about 14 percent, from $470 per patient per day to $540. They say the costs, which were anticipated as part of the settlement agreement and would be shared with the federal government, are necessary to ensure “adequate funds will be available to serve individuals residing in those facilities.”
Even as the centers serve fewer people, the state has added staff and spent more money to comply with the Department of Justice agreement to improve state-supported living centers, which now serve mostly high-need residents, says Health and Human Services Commission spokeswoman Stephanie Goodman.
The rate change will be debated at an HHSC public hearing on Friday. Meanwhile, lawmakers on the Senate Finance Committee meet today to ensure all the terms of the Justice Department settlement are being followed, along with the emergency legislation passed last session. Despite many improvements, monitors stationed at state-supported living centers have in recent months found evidence of staffing shortages and “dehumanizing practices” – including giving women the exact same cropped haircut and leaving disabled residents with nothing to do for hours on end.
Cecilia Fedorov, a spokeswoman for the Department of Aging and Disability Services, says the agency has hired more workers, including night-shift supervisors, professional medical staff and facility ombudsmen. Video surveillance systems are being installed at all 13 centers. And the agency has implemented random drug testing and FBI fingerprinting for all state-supported living center employees.
Opponents of the state-supported living centers have worked for years to shutter them, lobbying lawmakers about abusive conditions as a way to move more people with disabilities into community-based services. But with the influx of money to facilities they consider failing, the advocates fear their efforts may have backfired. At this rate, they say, convincing lawmakers that they’re wasting their money is an uphill battle.
şÚÁĎłÔąĎÍř News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/texas-disability-medicaid-tt/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=30380&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>