In one notable example, three dozen nursing home residents in San Luis Obispo County were informed on the same day that their Medi-Cal managed care plan was cutting off payment for nursing home care, said Karen Jones, the county’s long-term care ombudsman.
The residents included a 68-year-old amputee with diabetes, memory loss and kidney disease who required dialysis three times a week, and an 82-year-old man with congestive heart failure and diabetes who wasn’t strong enough to transfer himself from his bed to a wheelchair, Jones said.
“It just felt like we were tossing our seniors and disabled adults,” Jones said of the letters, which arrived in September 2018 and sparked a year-long dispute. “‚ÄòSorry, we’re going to save some money here.’ That’s exactly what it felt like.”
The California Department of Health Care Services, which administers Medi-Cal, the state’s Medicaid program for low-income people, said the terminations by the managed care plan, CenCal Health, were isolated, a perspective some long-term care advocates share. CenCal said it was just following protocol, examining the books to make sure members still met the qualifications for long-term care under Medi-Cal.
But California Healthline interviewed multiple long-term care advocates and legal aid attorneys on the Central Coast and other parts of the state who said they have witnessed an increase in coverage denials for nursing home residents covered by Medi-Cal managed care plans. They worry such denials may soon become more commonplace: Medi-Cal nursing home care in all 58 counties will be placed under managed care beginning in January 2021, the state announced recently — up from 29 counties currently.
Under , the state pays plans a monthly rate for each recipient to provide all of the medically necessary services that person needs. By comparison, under traditional “fee-for-service” Medi-Cal, the state compensates medical providers directly for each service they render.
California and other states increasingly are moving their Medicaid patients into managed care, arguing that the model saves money and also improves members’ health by coordinating care. More than 80% of the on Medi-Cal are covered by managed care.
Long-term care advocates fear that the trend means more frail people will be forced out of nursing homes as managed care plans look to their bottom lines.
“We’re looking at multiplying this problem across the state,” said Leza Coleman, executive director of the California Long-Term Care Ombudsman Association.
The typical nursing home population in California is about two-thirds Medi-Cal, and many have given up everything ‚Äî their apartments or mobile homes, their furniture, their burial insurance ‚Äî to qualify, said Lonnie Golick, ombudsman for Shasta, Trinity, Siskiyou, Modoc and Lassen Counties in Northern California. Golick said she’s received a number of complaints against Partnership HealthPlan of California about coverage terminations. “They gave up their whole life,” she said. “And then they’re told, ‚ÄòIt’s time to go.’”
Exacerbating the problem, Coleman added, is a shortage of assisted living facilities willing to serve Medi-Cal patients who no longer qualify for nursing home care.
To be eligible for nursing home coverage under Medi-Cal, individuals must have medical needs that require continual, around-the-clock care to prevent significant illness or disability, or alleviate severe pain.
CenCal sent the termination letters to the San Luis Obispo County nursing home residents as part of the process of reviewing their eligibility, said Bob Freeman, CenCal’s CEO. Normally that process is spread out over the year, he said, but the plan got “backed up” on evaluations, which is why so many patients were notified at once.
“We don’t like to do this,” he said. “It’s destabilizing; we don’t want to disrupt people’s lives. We do have state regulations that we have to follow.”
Last month, the Department of Health Care Services sent Medi-Cal managed care plans a notice clarifying that federal law allows residents to stay in nursing homes to receive “intermediate care”; in essence, plans should pay for lower levels of care rather than terminating coverage.
Freeman said the plan is reconsidering some residents’ eligibility, given the clarification. And Jones, the San Luis Obispo ombudsman, said CenCal recently hired a new nurse who has begun restoring eligibility for some residents in certain homes.
But residents of other homes — and in other regions — are still facing denials.
David Green, 60, a registered nurse in Santa Barbara County, said his 90-year-old mother received a letter last year telling her CenCal would no longer pay for her care at Marian Extended Care Center in Santa Maria.
She’d landed in a nursing home in 2016 after a bout of sepsis, he said. At first, she was so weak, she couldn’t walk. By the time she got the letter, her strength had improved, but she still had diabetes, kidney disease, hypertension, atrial fibrillation, breast cancer, memory loss and pain in her artificial knees, Green said.
Green sought out the Santa Barbara County ombudsman and, later, a lawyer. Eventually, he prevailed ‚Äî but he’s always on alert for another letter.
“It’s very nerve-racking,” he said.
Tessa Hammer, the attorney from Legal Services of Northern California who helped Green, said she has worked on seven such cases out of Santa Barbara County, as well as a handful in the state’s rural northern counties. She’s concerned about residents who don’t have family advocating for them.
“I’m not sure where those folks might end up,” she said.
Golick, the ombudsman for several northern counties, said a man in his 80s in Trinity County received a notice from Partnership HealthPlan earlier this year that he was no longer covered for nursing care he’d depended on for a decade. Like many elderly residents, she said, he felt he had no choice but to comply. He told her he might sleep on someone’s couch, or in his brother’s car.
“Rural areas are really scary,” she said. “Where the hell do you go?”
Dustin Lyda, a spokesman for Partnership, said the plan doesn’t track data on these kind of coverage denials, but anecdotally hasn’t noticed an upsurge. Lyda said the plan works with facilities, doctors and family members to determine a patient’s needs. If Partnership determines skilled nursing is no longer medically necessary, it works for 60 days to find an alternative solution, he said.
In the meantime, nursing homes find themselves in a difficult situation. They cannot legally who don’t have a safe place to go, but they are no longer paid to keep them. In some cases, including in San Luis Obispo, nursing homes have kept residents without pay.
“We’re all watching this closely,” said Craig Cornett, CEO of the California Association of Health Facilities.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/aging/california-nursing-home-residents-told-to-find-new-homes/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1013467&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>For the better part of a year, Baker-Ajene pushed Savitri — who has cerebral palsy, spastic quadriplegia and epilepsy — in a child-sized chair that was too small for her. Baker-Ajene said she also has run into problems getting an appropriate shower chair for 17-year-old Savitri. Because of that, she mostly gives her daughter sponge baths in bed.
“It’s ridiculously difficult to get what you need for your child,” said the 62-year-old Clovis, Calif., resident and graphic designer. “I’m tired now. I try not to argue with people anymore, because I need my energy for her.”

Many California children with serious health care needs often wait months, or even years, before they receive essential medical equipment like custom wheelchairs, shower chairs and hospital beds, according to .
For some children, these long waits aggravate existing health problems, cause pain and pressure sores, or exacerbate developmental delays, said the report, published in May by the Lucile Packard Foundation for Children’s Health.
“It’s a big bureaucratic mess, and kids are suffering,” said Maryann O’Sullivan, an independent health policy consultant and author of the report.
In one case Sullivan documented, a boy with muscular dystrophy started kindergarten in a stroller because his parents could not get him an appropriate wheelchair in time, in part due to the slow insurance approval process. In another case, a 7-year-old with a serious bone disorder has remained in diapers for years while waiting for a state public health program for children to find a vendor to supply him with a modified commode.
A variety of factors lead to the delays. Families say they are often bounced between private health insurance companies and publicly funded programs such as Medicare, Medi-Cal and California Children’s Services (CCS), which provides coverage for 200,000 children with special health care needs. Once families have navigated that bureaucratic maze to obtain approval for equipment, low reimbursement rates paid by some of the public insurers can make it difficult to find vendors willing to provide the equipment.
Juno Duenas, the executive director of the San Francisco-based Support for Families of Children With Disabilities, said appropriate equipment can be essential to a child’s independence, future job prospects and ability to contribute to society.
Many parents say they struggle to get equipment, in part, because they don’t understand the system. Yuki Baba, a 54-year-old translator who lives in Berkeley, Calif., waited a year to get a hospital bed for her son, Nate, who has cerebral palsy. At 5, Nate was still sleeping in a crib he’d outgrown. Nate is insured by both California Children’s Services and Medi-Cal, the state’s health insurance program for low-income people, and Baba kept calling the wrong program for help.
“Because I didn’t know the system very well, I wasted a lot of energy and time,” she said.
Even when the approval process is smooth, low rates paid by the government-funded programs California Children’s Services and Medi-Cal can mean there are sometimes no outside vendors willing to provide equipment.
California Children’s Services covers treatments and therapies for children under 21 who meet income guidelines and have a range of eligible serious medical conditions, including cerebral palsy, traumatic injuries and cancer. Many of these children also are insured by Medi-Cal. Others have some private insurance coverage combined with CCS.
Dave Kramer-Urner, CCS administrator for Santa Cruz County, says he has a hard time finding vendors to provide padded bath benches, bidets and certain crutches because reimbursements from the program are low.
CCS rates haven’t changed in 10 years, he said. And the disappearance of small “mom and pop” vendors has exacerbated the problem. The last such vendor in Santa Cruz shut its doors three years ago, he said.
“The big companies have the capacity to say ‚Äòno’ more easily,” he said.
O’Sullivan’s research relied on three existing surveys of parents, advocates and health care providers. She also interviewed dozens of medical therapists, nurses, physicians, vendors, advocates, parents and staff from Medi-Cal managed-care health plans.
O’Sullivan notes in her report that the California Department of Health Care Services, which administers both Medi-Cal and California Children’s Services, doesn’t track wait times for medical equipment and hasn’t set a minimum time frame for the delivery of such equipment.
Tony Cava, a spokesman for the department, said in an emailed statement that it “has been working for several years to improve health care and to emphasize quality and coordination of care for children and youth with special health care needs.”
The department will roll out a program in 21 counties in the coming months to coordinate health care under California Children’s Services and Medi-Cal, Cava said. The program should address many of the issues outlined in O’Sullivan’s report because it will reduce bureaucratic back-and-forth, he added.
However, the majority of children in the CCS program don’t live in those counties, so the changes won’t affect them.
Health Plan of San Mateo, which piloted the integration of Medi-Cal and CCS five years ago, has addressed many of the administrative hurdles detailed in the report, said Sophie Scheidlinger, the plan’s pediatric health manager. However, she continues to see delays due to a shortage of vendors willing to work with the public programs.
In the meantime, many parents fight to find workarounds — or just pay for things themselves.
Alison Beier’s son, Evan, was born two months early with renal failure, a malformed urinary tract and multiple congenital anomalies. While still an infant, Evan was stuck in the hospital for several days after doctors insisted that he needed an automated blood pressure monitor with an infant-sized cuff before they would release him. Neither his public nor private insurers would pay for one.
“Insurance wouldn’t pay for the monitor, we couldn’t afford the monitor, and we didn’t know how to get the monitor,” Beier said.
Eventually, Beier posted her problem on Facebook. A friend of a friend worked at the company that manufactured the monitor and was able to help her.
She feels blessed to have her son, who has gone through 50 surgeries and has battled rejection of his two transplanted kidneys since 2012. She describes him as a brilliant 8-year-old and “the happiest guy on the planet.” Still, advocating for his needs can be overwhelming.
“It’s like I’m always fighting for somebody to cover something,” she said.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/children-with-disabilities-endure-long-waits-for-life-changing-medical-equipment/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=856829&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Ayala, an Oakland-based AIDS advocate, does not want the conference in his own city — or anywhere else in the United States, for that matter.
His statement of opposition and a second one drafted by colleagues at other AIDS organizations have been co-signed by hundreds of organizations and individuals in the United States and around the world.
Their biggest concern: long-standing U.S. visa policies will prevent many of the people most affected by AIDS and HIV, including who live in other countries, from attending the conference. They also worry about new restrictions affecting travel from Muslim countries.

“In this day and age, I have to wonder why we support big international AIDS conferences happening in places that bar anyone,” said Ayala, executive director of the Global Forum on MSM [Men who have Sex with Men] & HIV.
HIV/AIDS is far more prevalent in many countries, , than in the United States. Almost 19 percent of people ages 15 to 49 in South Africa are infected with HIV, as are more than 20 percent in some neighboring countries.
In the U.S., prevalence among the same demographic group hovers — although that masks some stark disparities. Last year, the Centers for Disease Control and Prevention projected that in the U.S. who have sex with men were at risk of contracting HIV. Globally, people are living with HIV.
Ayala and other critics of the Bay Area location raise broader questions about the cost and frequency of a biennial event they say is enormously expensive and often excludes the very people it purports to represent.
The organizers of the conference and others who support the decision to bring it to the Bay Area say they understand these worries.
“Travel restrictions to the U.S. remain a significant concern for us,” said Mandy Sugrue, spokeswoman for the International AIDS Society, which organizes the conference.
However, Sugrue and other proponents of a San Francisco-Oakland conference venue argue that the politically liberal Bay Area offers a perfect platform for rebuking the Trump administration’s exclusionary immigration policies and its perceived retreat from leadership on AIDS policy.
In December, the administration of the Presidential Advisory Council on HIV/AIDS, six months after a half-dozen others had resigned in protest. Trump officials have also proposed cutting national HIV/AIDS spending by more than $100 million and reducing the U.S. contribution to global funding by more than $1 billion.
“If there is any place in the U.S. where people can come and protest and rise up and have their voices heard ‚Ķ Oakland is it,” said Cynthia Carey-Grant, executive director of the Oakland-based group Women Organized to Respond to Life-Threatening Disease. She penned of the conference location that has been signed by nearly a dozen individuals and groups.
Carey-Grant believes the contrast between upscale, predominantly white San Francisco and its decidedly poorer neighbor across the Bay offers a window on the disparities that pervade AIDS treatment and funding around the world – to the detriment of low-income communities of color.

Sofia Tobar, a 50-year-old transgender woman from Oakland who was diagnosed with HIV in 1998, said the conference is an opportunity “for Oakland’s diverse humans to embrace people from other countries ‚Ķ and to also highlight what we’re lacking.” She is especially interested in speaking out against federal cuts to AIDS services and violence targeting the transgender community, she said.
Others say they are eager to honor San Francisco’s long history of battling AIDS.
Joe Hollendoner, CEO of , noted that the conference organizers have secured use of the Moscone Center, the central conference venue, free of charge. They will use the money they save to help more people attend, he said. His foundation, along with the San Francisco Travel Association, led the committee that submitted the successful conference bid.
The planners of the International AIDS Conference usually try to alternate venues between affluent and lower-income countries. The conference was last held in the United States in 2012 in Washington, D.C. In 2014, it was in Melbourne, Australia, and in 2016, in Durban, South Africa. This year, the conference will be in Amsterdam.
Conference organizers said they reached out to a number of lower-income countries to host the 2020 conference, but . As many as 20,000 people, perhaps more, are expected to attend the conference — and many cities cannot accommodate such a large gathering, they said. Sugrue, the International AIDS Society spokeswoman, said they are not considering changing the venue.
She said the location of major conference donors was not a factor in the 2020 venue decision.
In this day and age, I have to wonder why we support big international AIDS conferences happening in places that bar anyone.
George Ayala, Global Forum on MSM & HIV
Gilead Sciences Inc., which is based 20 miles from San Francisco and makes the HIV prevention drug Truvada, is one of the , as it was in 2016. Other big industry donors are not located in the Bay Area, including Johnson & Johnson, Merck and ViiV Healthcare, which specializes in HIV drugs. Funding for the 2020 conference has not yet been confirmed, Sugrue said.
Naina Khanna, the executive director of the Oakland-based Positive Women’s Network, said the fact that no developing countries submitted a bid isn’t enough to assuage her concern for the people who will likely be excluded. Khanna helped draft demanding that the conference be relocated outside the U.S. More than 100 organizations and nearly as many individuals have signed the statement.
“Where is our commitment to actually holding the conference where the most people are impacted?” asked Ruth Morgan Thomas, global coordinator of the , which includes 305 organizations representing sex workers in 85 countries.
Prior to the Washington, D.C., conference, the U.S. had lifted a ban on people with HIV entering the country, and many were hopeful that similar prohibitions against sex workers and drug users would also end. But they didn’t, and sex workers scrambled to organize a parallel conference in Kolkata, India, Morgan Thomas said. Drug users convened one in Kiev.
Khanna, of the Positive Women’s Network, said that the high cost of accommodations in the Bay Area will also make the conference inaccessible to many people within the United States ‚Äî especially low-income African-Americans in the South, who are disproportionately burdened with the virus.
Marsha Martin, coordinating director of the Global Network of Black People Working in HIV, said she would have been happy had Bangkok or South America or even Atlanta been chosen to host the conference. “But if venues don’t submit bids, there’s nothing to do about it,” she said. So she’s treating the Bay Area conference as an opportunity to grapple with the big disparities in AIDS funding and to reinvigorate efforts in the U.S. to combat the disease.
“If we do bring it [to the Bay Area] and make it the best conference we can make it, then we win,” Martin said. “We show the world we are not giving up.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/choice-of-bay-area-for-aids-conference-exposes-tension-among-activists/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=832858&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>A published last month in the journal Tobacco Control suggests the new law is already working. Seven months after it took effect, preliminary data show, the percentage of state retailers selling tobacco to kids under age 18 dropped significantly — from 10.3 percent before the law took effect, to 5.7 percent afterward. The rates are based on surveys in which teenaged decoys attempted to purchase tobacco from retailers.
By raising the minimum age to 21, experts had predicted teenagers would no longer have such easy access to tobacco through their slightly older friends.
Survey data also showed that almost 99 percent of tobacco retailers were aware of the new law, and that the majority supported it.
April Roeseler, chief of the California Tobacco Control Program and co-author of the report, said she was “pleasantly surprised” at how well tobacco retailers had responded to the increased age of purchase.
“We know that they’re the front line in helping make this law be successful,” she said. “I think we expected that this would be a tough law to implement and get compliance with, but I think it’s just indicative of the groundwork we’ve been doing in California for nearly three decades.”
Larry Cohen, executive director of the Oakland-based Prevention Institute, said he, too, was surprised that most retailers support the law.
“It’s a sign that there’s real momentum over the past couple of decades in recognizing that tobacco is harmful and that protections are appropriate,” he said.
Sen. Ed Hernandez (D-West Covina), chair of the Senate Health Committee, said he first proposed legislation to increase the state’s minimum tobacco sales age after reading a magazine article about teen smoking in 2015. Soon after, the Institute of Medicine published a report saying that 90 percent of adults who became daily smokers first used tobacco by the time they were 19.
The following year, Hernandez introduced the law, and his colleagues in the California legislature passed it. The law does permit active-duty military members to purchase tobacco even if they are not yet 21, a concession Hernandez said he made in order to get needed votes. He said he received pushback from people in the military who believed “if you are old enough to go to war, you are old enough to smoke.” Hernandez notes that the law still requires members of the military to be 21 to buy alcohol.
The new report shows that how well retailers comply with the new age limits also varies geographically: Retailers in Los Angeles sold to underage buyers much more frequently than did those in the Bay Area.
“There are always kids that come around,” said an employee of Sana Market and Liquor on Telegraph Avenue in Oakland, who did not want his name published so he could speak freely.
He said the market — which carries snacks and alcohol in addition to cigarettes — is very strict about checking IDs.
They also refuse to sell to adults when it is clear they are trying to buy for someone under legal purchasing age. So-called shoulder-tap buys continue to be a problem, according to the study.
Still, said the employee, there is only so much the law can do: “Whoever is going to smoke is going to smoke.”
Nearby, just off upscale Piedmont Avenue, Stephen Richman, the longtime owner of The Piedmont Tobacconist, said he supports the increased age of sale. Even before the new law, he said, teenagers rarely tried to buy from his shop, with its wood-paneled walls, leather lounge chairs and background jazz.
He pointed to a big, yellow sticker on the cash register that read: “The Sale of Tobacco Products to Persons Under 21 Years of Age is Prohibited by Law and Subject to Penalties.”
“This discourages them,” he said.
Occasionally, he said, a young person comes in hoping to buy a cigar to hollow out and fill with marijuana. When they hear the price, he added, they usually leave.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/after-raising-age-for-tobacco-purchases-state-sees-decreased-sales-to-minors/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=820265&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Now, California nursing home advocates are calling on the state to take it down, saying the new site is incomplete, inaccurate and “a huge step in the wrong direction.”
The state describes the website as a user-friendly replacement for its previous tool . Among other things, state officials say the new site allows consumers to compare up to three facilities at a time, improves compliance with the Americans with Disabilities Act and offers language translation tools.
But the nonprofit organization California Advocates for Nursing Home Reform says those extras are of ¬Ýlittle use because the content itself is wrong. The group complains of inaccurate complaint counts for problematic nursing homes and missing links to inspection reports filed before 2016.
“Choosing the right nursing homes can be a life-and-death decision,” said Michael Connors, an advocate with the organization. “This site should help them avoid places that are likely to neglect them. Right now, it will do the opposite.”
State officials argue that the site is a work in progress that is being refined, with updates to complaint counts coming this week. The new site cost about $437,000 to build and operate, officials said.
“The department has acknowledged and identified the source of the problem [with complaint counts]¬Ýand has already implemented a correction plan,” Corey Egel, a spokesman for the California Department of Public Health, said in a written statement. “The department believes Cal Health Find improves the user experience. ‚Ķ We find no reason to remove the site while we correct errors.”
Deborah Pacyna, a spokeswoman for the California Association of Health Facilities, which represents nursing homes, said her organization also has shared some concerns about the data with the state, but she declined to give further details. She added that some nursing homes were complaining that pictures from Google Earth did not accurately reflect their facilities, instead showing only the street or a back parking lot. She repeated the state’s assertion that the site is a work in progress.
Connors said she remains skeptical that the state is taking the problems seriously.
The state’s old website is still up, although it refers people to the new site. A comparison of its data with that available on Cal Health Find showed marked discrepancies.
For example, the state’s old website shows that 90 complaints were made against Lake Merritt Healthcare Center in Oakland in 2017. The new website shows only 34 for the same year. Similarly, while the old website lists 49 complaints against San Diego Healthcare Center in 2017, the new website lists only 13.
Officials offered a complex explanation for the discrepancies, including that the new site contained more records so that it was updating more slowly than the old one. Also, they said, the old site erroneously counted some deficiencies more than once.
People searching the new website will find no links next to individual nursing homes for citations made before 2016 – those links are still there but, according to the patient advocates, buried on the new site.
So, the advocates say, an individual considering Oakpark Healthcare Center in Tujunga, for example, may miss the serious Class AA citation from September 2015 that was more readily evident on the old website. That citation determined that the nursing home failed to identify and treat a gangrenous wound on a resident’s heel, leading to her death.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/user-friendly-or-error-ridden-debate-swirls-around-website-comparing-nursing-homes/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=819449&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>That depends on the hospital.
According to data from the California Department of Public Health, flu vaccination rates among health care staffers at the state’s acute care hospitals range from a low of 37 percent to 100 percent.
Overall, flu vaccination rates among hospital workers climbed significantly in the past several years ‚Äî from an average of 63 percent during the 2010-11 influenza season to 83 percent during the 2016-17 season, . Vaccination rates for the current season won’t be determined until later this year.
But that general increase masks some big variations. Monrovia Memorial Hospital in Los Angeles, Los Robles Hospital and Medical Center, East Campus and Thousand Oaks Surgical Center in Ventura each reported that fewer than 40 percent of their health care workers received the flu vaccine last year. Representatives from those hospitals did not return repeated calls for comment.
On the other end of the spectrum, Rady Children’s Hospital in San Diego reported that every single person working there got the vaccine.
California’s flu vaccination policies for hospital workers, and those of many other states, are far from uniform or ironclad. In various states, health care workers have legally challenged hospital requirements for vaccination on and grounds. And some unions in California and elsewhere oppose a legal mandate, partly for civil rights reasons.
Public health officials themselves have different takes on the legal requirements for hospital workers. The Centers for Disease Control and Prevention lists California and Massachusetts among the handful of states where the flu vaccination is mandated for health care workers. But the states’ laws allow health care workers to opt out by signing a form declining the vaccine. For that reason, officials from those two states said they do not actually consider the vaccine mandatory.
Colorado law requires hospital health care workers to provide proof of immunization or a doctor’s note providing for a medical exemption, and requires that non-immunized workers wear masks. Hospitals that achieve a 90 percent or higher flu vaccination rate are exempt from these rules, however.
In California, state law requires that hospitals offer the vaccine free of charge. Many hospitals offer vaccines to personnel in the cafeteria, and during day and night shifts. “The key to getting more people vaccinated is to make it more easily accessible for people,” said Lynn Janssen, chief of the California Department of Public Health’s associated infections branch.
She also said many California counties and hospitals have required health care workers to either get the flu vaccine or wear a mask, which can help prevent spreading illness to others.
Partly as a result, nearly a third of the state’s hospitals now have flu vaccination rates above 90 percent.
Vaccination rates vary significantly among different categories of hospital workers, however. Hospital employees had an average vaccination rate of 87 percent statewide in 2016-17, while licensed independent practitioners — including some physicians, advance practice nurses and physician assistants who do not receive paychecks from the hospital — had a rate of just 67 percent.
The CDC recommends that health workers get one dose of influenza vaccine annually, and cites data showing the vaccine in recent years — though it was far less so this year. Dr. Bill Schaffner, an infectious diseases professor at Vanderbilt University School of Medicine in Nashville, Tenn., says there are three principal reasons to get vaccinated: to prevent workers from infecting patients, to keep them healthy in order to care for patients and to spare them a bout with the flu.
, however, suggests that the benefits of health care worker vaccinations have been overstated.
In any case, just because experts say health care personnel should get the vaccine doesn’t mean they will choose to do so.
“In the studies, and also in our experience, it turns out ‚Äî to everyone’s great surprise ‚Äî that health care workers are human beings,” Schaffner said. “Some are too busy, some don’t think the flu vaccine is worth it, some don’t like shots. Some are not convinced they can’t get flu from the flu vaccine.”
Because of this, Schaffner said, it’s up to hospital leadership to push staffers to get vaccinated. At Vanderbilt University Medical Center, vaccination rates increased from 70 percent to 90 percent once leaders there effectively made the flu vaccine “mandatory,” he said, requiring noncompliant hospital personnel to present vaccine exemption requests to a hospital committee.
Health officials also encourage patients to ask whether their caregivers are vaccinated.
Jan Emerson-Shea, spokeswoman for the California Hospital Association, said her organization would like the flu vaccine to be mandatory for all health care personnel. Independent physicians have proven an especially challenging group to motivate, she said, since hospitals hold little sway over them.
“I, for the life of me, can’t imagine why a physician wouldn’t want to be vaccinated,” she said. “But they make that choice.”
Yet the California Nurses Association strongly opposes making flu vaccines mandatory, said Gerard Brogan, a registered nurse and spokesman for the union.
He said the union does recommend that providers get the vaccine, but it objects to making vaccination a condition of employment. He said some employees have religious issues or safety concerns about the vaccines and “we think that should be respected as a civil rights issue,” he said.
He also called rules requiring unvaccinated providers to wear a face mask “punitive.”
“It’s almost like the scarlet letter to shame you,” he said.
He said the masks can frighten patients¬Ý‚Äî . In any case, he said, wearing the masks is not especially effective in stopping the spread of flu (although some researchers ). Instead, he said, employees should be encouraged to wash hands and to stay home when they are sick.
Too often, he said, nurses are asked to come in to work when they are ill. He said he was not able to find any nurses willing to discuss their decision not to get the flu shot.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/at-some-california-hospitals-fewer-than-half-of-workers-get-the-flu-shot/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=817955&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>She had until midnight to decide.
Willis’ Medicaid managed-care plan had told the home that it was cutting off payment because she no longer qualified for such a high level of care. If Willis, 58, stayed and paid the daily rate, her Social Security disability money would run out in three days. But if she left, she had nowhere to go. She’d recently become homeless after a breakup and said she couldn’t even afford a room-and-board setting.
In tears, she said, she agreed to leave. Thus began a months-long odyssey from budget motels to acquaintances’ couches to hospital ERs ‚Äî at least five emergency visits in all, she said. Sometimes, her 25-year-old daughter drove down from Sacramento, and Willis slept in her daughter’s car.
“They kicked me out in the cold,” said Willis, a former Head Start teacher.
Complaints about allegedly improper evictions and discharges from nursing homes are on the rise in California, Illinois and other states, according to government data. These concerns are echoed in lawsuits and by ombudsmen and consumer advocates.
In California alone, such complaints have jumped 70 percent in five years, reaching 1,504 last year, said Joseph Rodrigues, the state-employed Long-Term Care Ombudsman, who for 15 years has overseen local ombudsman programs, which are responsible for resolving consumer complaints.
Around the country, ombudsmen say many patients like Willis end up with no permanent housing or regular medical care after being discharged. Even when the discharges are deemed legal, these ombudsmen say, they often are unethical.
“Absolutely, it’s a growing problem,” said Leza Coleman, executive director of the California Long-Term Care Ombudsman Association. Coleman says the practice stems from skilled nursing facilities’ desire for better compensation for their services and from the shortage of other affordable long-term care options that might absorb less severe cases.
In Willis’ case, she ultimately lost her appeal to return to the nursing home, Courtyard Care Center. A state hearing judge determined that she had left the home voluntarily because she refused the opportunity to pay to remain there.
Top administrators at Sava Senior Care, which owns Courtyard, did not return repeated calls for comment.
Among other recent cases of allegedly improper discharges:
- In October, California’s attorney general moved to prevent a Bakersfield nursing home administrator from working with elderly and disabled people, while he awaits trial on charges of elder abuse and wrongful discharge. State prosecutors said one patient was falsely informed that she owed the home money, then sent to an independent living center even though she could not “walk or toilet on her own.” The administrator did not return messages left at the nursing home.
- alleges a nursing home chain, Neiswanger Management Services (NMS), illegally evicted residents, sending them to homeless shelters or other inadequate facilities to free up bed space for higher-paying patients. NMS countersued state regulators, alleging they are trying to drive the chain out of business.
- Last month, a 73-year-old woman with diabetes and heart failure for allegedly in front of a relative’s home. The suit said conditions in the residence were unsafe and a family member refused to allow her inside. The state cited the home in July and issued a $20,000 fine.
Of course, not all complaints or lawsuits are well-founded. Federal law allows a nursing home to discharge or evict a patient when it cannot meet the resident’s needs or the person no longer requires services; if the resident endangers the health and safety of other individuals; or if the patient has failed, after reasonable and appropriate notice, to pay.
The law also generally requires a home to provide 30 days’ notice before discharging a patient involuntarily and requires all discharges be safe and orderly.
Deborah Pacyna, spokeswoman for the California Association of Health Facilities, a trade organization that represents nursing homes, questions why nursing homes should be responsible for providing a safety net for the indigent and homeless.
“Nursing home residents reflect society,” she said in a written statement.¬Ý“Some nursing home residents live in homeless shelters or hotels. They may request that they go back ‚Äòhome,’ or to their local shelter or hotel upon discharge. We must honor their choices as long as their needs are met.”
Pacyna also noted that eviction and discharge complaints represent a tiny fraction of the hundreds of thousands of residents released from the state’s nursing homes each year.
Nationally, discharge and eviction complaints have remained more or less steady in recent years after rising significantly between 2000 and 2007, according to data collected by the federal government. Still, these complaints remain the top grievance reported to nursing home ombudsmen as the number of overall complaints about everything from abuse to access to information has dropped in the past decade.
The rate of complaints can vary considerably by state. Jamie Freschi, the Illinois state ombudsman, says discharge and eviction complaints have more than doubled in her state since 2011.
She recalled one wheelchair-bound nursing resident who was in severe pain from osteoarthritis, scoliosis and fibromyalgia when she was discharged from a nursing home and sent to a homeless shelter. After the shelter rejected her because it could not accommodate her wheelchair, the resident went to a motel, which kicked her out when she ran out of money. She has since cycled between the emergency room and the streets, Freschi said.
“It’s an example of a really, really broken system, all the way around,” Freschi said.
Advocates say such decisions are often money-driven: Medicare covers patients for just a short time after they are released from hospitals. After that, these critics say, many nursing homes don’t want to accept the lower rates paid by Medicaid, the public insurance program for low-income residents.
Even when they appeal and win, advocates say, it doesn’t always help the patient. The Centers for Medicare & Medicaid Services has advised California on two occasions ‚Äî including this past summer ‚Äî that it must enforce decisions from appeals hearings. (The state contends that it uses a variety of strategies to enforce the law.)
Last month, the California Long-Term Care Ombudsman Association joined with the legal wing of the AARP Foundation to , alleging it had improperly discharged an 83-year-old woman with Alzheimer’s ‚Äî requiring the nursing home to readmit her.
“The facilities are getting the message that they don’t have to follow the rules here, so they’re emboldened,” said Matt Borden, a San Francisco attorney helping with the lawsuit.
Willis and her advocates were convinced that Courtyard Care Center broke the rules in her case.
Willis “did not leave Courtyard ‚Äòvoluntarily’ in just about any sense of the word,” said Tony Chicotel, a staff attorney with California Advocates for Nursing Home Reform.
At a hearing in April, held at the nursing home and attended by a reporter, Chicotel and an ombudsman argued that Willis’ discharge violated legal requirements, including lack of written notice. They asked that she be immediately readmitted.
According to hearing documents, Willis’ documented medical problems were many: an aneurysm, an ulcer, difficulty walking, muscle weakness, gastritis, anemia and heart and kidney disease. During her stay at the nursing home, she said, she’d fallen and hit her head while visiting the doctor, resulting in a severe concussion.
For their part, Courtyard staffers explained that Medicaid wouldn’t cover Willis anymore based on their assessment of her condition. They said she had “almost returned to her prior level of functioning.”
During the hearing, Willis repeatedly told those in attendance that she felt dizzy and nauseated. Her head pounded. “I’m not good,” she said. Afterward, she begged for a ride to the emergency room, where she was admitted with a torn aorta and bleeding ulcer.
She was still in the hospital when the hearing officer issued her decision a few days later. Eventually, she was released to another nursing home, which also discharged her after a month, she said. Then she resumed sleeping on friends’ couches. She chose not to file another appeal.
“This time in my life,” Willis said, “it’s very discouraging.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/courts/when-nursing-homes-push-out-poor-and-disabled-patients/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=799233&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>She failed to find one, so she started one herself.
Norman said her company, , along with a handful of other Silicon Valley start-ups, is attempting to usher medical billing technology into the 21st century. Banking, transportation, furniture and grocery shopping can all be managed with some fancy finger work on smartphone screens. She and other entrepreneurs wondered: Why not medical bills?
Today, Norman’s clients submit digital copies of their out-of-network bills through an app on their phones. Better’s employees navigate the bureaucratic thicket to track down reimbursements ‚Äî and keep 10 percent of the money they recover from insurers.
The company has processed millions of dollars in claims, for everything from psychiatry to acupuncture to contact lenses, Norman said. The majority of Better’s customers have (PPOs) or other types of insurance policies with out-of-network benefits. Unlike visiting in-network doctors, patients using out-of-network services often must pay upfront, then ask for reimbursement from their insurer later.
“For a lot of people, it becomes magic that we’re able to solve those problems and get them the money they are owed from insurance,” said Norman, who founded Oakland-based Better about a year and a half ago.
Better is among a new breed of start-ups trying to lead customers through the labyrinth of medical billing. Each has taken on a different aspect of billing — helping patients file claims, scanning bills for errors or making charges easier to understand.
But in their quest to revolutionize an industry, these start-ups face a variety of obstacles, including trouble getting access to medical records and difficulty cracking complex insurance policies. Some of the young companies are flourishing. Others are folding.
Pairing a technological solution with an industry that still uses faxes, distant call centers and snail-mailed bills can prove challenging. “You can’t automate repeated phone calls to a guy in a basement who doesn’t want to do his job,” said Victor Echevarria, whose company,¬Ý,¬Ýfolded two years after he founded it.
The emergence of these businesses reflects the fact that medical billing is a complicated, often byzantine process that can mystify even the savviest consumers. Adding insult, these bills often start to pile up while — either dealing with serious medical issues, or just beginning to recover.
Kristin-Leigh Brezinski, who works for a small tech company in Seattle, said she started using Better to address a pile of therapy bills she’d been meaning to submit for reimbursement. She had put off the task partly because she knew it would be a headache to spend hours on interminable phone calls, she said.
“I didn’t really want to sit on hold for the rest of my life,” said Brezinski, 28. She liked Better’s service so much that she continues to use it and has recommended it to others.
Experts agree that consumers need help tackling costly and complicated medical bills.
“Medical problems and medical bills are very likely to be the straw that breaks the camel’s back of a family’s finances,” said Anthony Wright, executive director of , a health care consumer advocacy organization.
Wright said the Affordable Care Act provided some protection for people, such as banning annual and lifetime limits on coverage and capping out-of-pocket maximums.
Many states, including California, have also adopted consumer protections against surprise medical bills. These are the often costly charges consumers receive from out-of-network providers, even though they went to an in-network facility.
Despite those advances, Wright said many aspects of medical billing remain a major problem for consumers. He thinks apps might help patients navigate certain issues, but policy fixes could be even more effective.
For example, an app could notify consumers when they’ve hit their annual out-of-pocket maximum, but the state could simply require insurers to provide that notice, negating the need for the app.
“I would love to put in place some laws and consumer protections that make some of these apps obsolete,” Wright said.
The landscape isn’t necessarily friendly to medical billing start-ups, as Echevarria discovered after he founded San Francisco-based two years ago.
He was inspired to tackle the problem of medical overbilling after his infant son had to go to the emergency room for a fever-related seizure and his family incurred about $12,000 dollars in medical bills, many of them laced with errors.
Co-founder Marija Ringwelski had looked at her own bills and found errors about 80 percent of the time. The two decided to build a platform similar to , the popular credit and financial management platform that offers a free credit score and free credit monitoring. Only this one would be for medical bills.
“Everybody wanted that product,” Echevarria said. “They wanted the medical bill version of identity protection.”
Using new technology and a team of experts that scrutinized clients’ medical bills in search of errors, Remedy eventually figured out how to operate efficiently in all ways but one, Echevarria said: While patients had a legal right to their own medical information, many billing offices refused to hand it over to third parties.
“The industry operates in a way that is decades old,” he said. While a lot of the operation could be automated, some of it remains frustratingly hands-on and time-intensive, he said.
The problem proved insurmountable, and the company went out of business this past summer.
Even if companies manage to get their hands on required medical records, insurance policies are extremely complicated and can be difficult to navigate, said Betsy Imholz, special projects director for .
Rules vary among companies, and regulations among states, she said. To help an individual, companies must comb through piles of documents and figure out each customer’s specific situation. As Remedy’s experience illustrates, that process can’t always be accomplished with simple technology.
There’s also a marketing problem: Many consumers “don’t realize there’s help to be had,” said Mark Hall, director of the Health Law and Policy Program at Wake Forest University’s School of Law.
Palo Alto-based addressed some of these challenges by shifting its business model.
Rather than directly serving consumers — as it did when it was a new start-up seven years ago — Simplee now markets its software to hospitals. Its clients currently include more than 400 hospitals and more than 2,000 clinics.
The software gives patients access to all of their bills in one place and attempts to make charges easier for them to understand. It also allows patients to see detailed explanations of charges and to create payment plans when necessary, said John Adractas, the company’s chief commercial officer.
“It’s not like there’s one formula for how to tackle health care problems,” Adractas said.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/news/can-apps-slay-the-medical-bill-dragon/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=790235&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Dozens of times a day, her parents, Rafael and Sonia, use a special machine to suction out saliva and phlegm from their oldest daughter’s mouth. Because choking and seizures can strike Abril anytime, a parent is always by her side.
Rafael and Sonia, both from Mexico, have lived in this country without permission for more than a decade. But only since the recent presidential election has a question haunted them: If they are deported, what will happen to Abril?
As the Trump administration promises to deport a broader range of people, parents like Rafael and Sonia increasingly are seeking help to stay in the country so they can tend to very sick children, according to interviews with doctors, lawyers and others who work with immigrants. And these professionals say they are struggling to come up with sound advice.
Rafael and Sonia know that many neighbors in their crowded mobile home park — along with millions of other immigrants living in the country without permission — are keeping to the shadows to avoid detection by federal authorities.
But Abril depends on her parents to stay alive.

The couple, along with other families in this story, spoke to California Healthline on the condition that their surnames be withheld, because they fear deportation. Abril and her younger¬Ýsister are U.S. citizens.
Dr. Salem Magarian, pediatric director of the Santa Cruz Community Health Centers, said immigrant parents of his sickest patients are asking for letters documenting their children’s health care requirements. Some parents say they hope such letters will help them stay in the country if they are picked up by authorities.
“Some people are freaked out,” Magarian said. “Most people are concerned. Almost no one says ‚Äòit’s not a big deal.’”
One of Magarian’s patients, a toddler named Leonardo, has had multiple surgeries for serious heart defects. The boy’s mother, Karla, has been in the country without papers for 23 years, having been brought to the United States at age 5. Karla is terrified by the prospect of leaving her children and being sent back to Mexico, a country she doesn’t remember.
Another child suffers from a life-threatening genetic condition that leaves him unable to speak or eat, Magarian said. Richey, 8, lost his father to cancer four years ago. His mother, Sugay, has been in the country illegally for 16 years.
“I try not to go anywhere,” Sugay said. “If I go anywhere, I’m very afraid. ‚Ķ I know this is not my country, I know this is not my place, but I’ve never done anything bad and I have a special baby who needs his mother.”
Such fears are reinforced by news accounts. The Salt Lake Tribune recently that the single mother and sole caretaker of an 18-year-old with cerebral palsy and epilepsy was deported to Colombia.
In , an Ohio mother of four children ‚Äî including one with a history of seizures ‚Äî was deported to Mexico. A spokesman for Immigration and Customs Enforcement (ICE) told The Guardian that the woman’s case had been reviewed several times by the courts.
“For parents who are ordered removed, it is their decision whether or not to relocate their children with them,” the spokesman said.
Immigration officials say they continue, as under the previous administration, to target for deportation people who have committed crimes — but they also say the new administration has changed policies to no longer support the practice of selective enforcement.
“Basically, there’s no exempted class for arrest,” said James Schwab, spokesman for the ICE field office in San Francisco.
Jessica Vaughan, director of policy studies at the Center for Immigration Studies, a pro-enforcement think tank that favors reduced immigration, says she sees plenty of benefits to enforcing immigration laws more rigorously — particularly increasing access to low-wage jobs for U.S. citizens and legal residents.
But she also says she “absolutely” believes exceptions should ‚Äî and will ‚Äî be made in cases where deporting parents would cause “undue hardship” for a young U.S. citizen.
“That’s why Congress created these forms of relief,” she said. “I think most Americans would support that.”


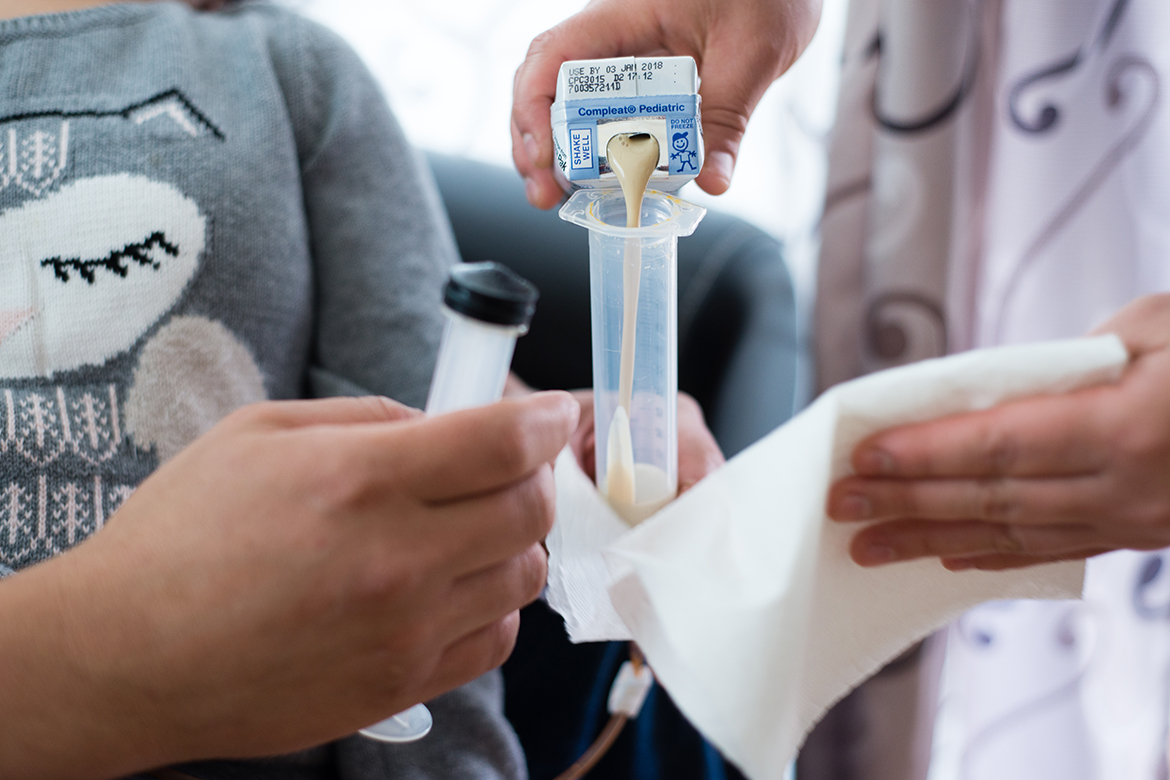
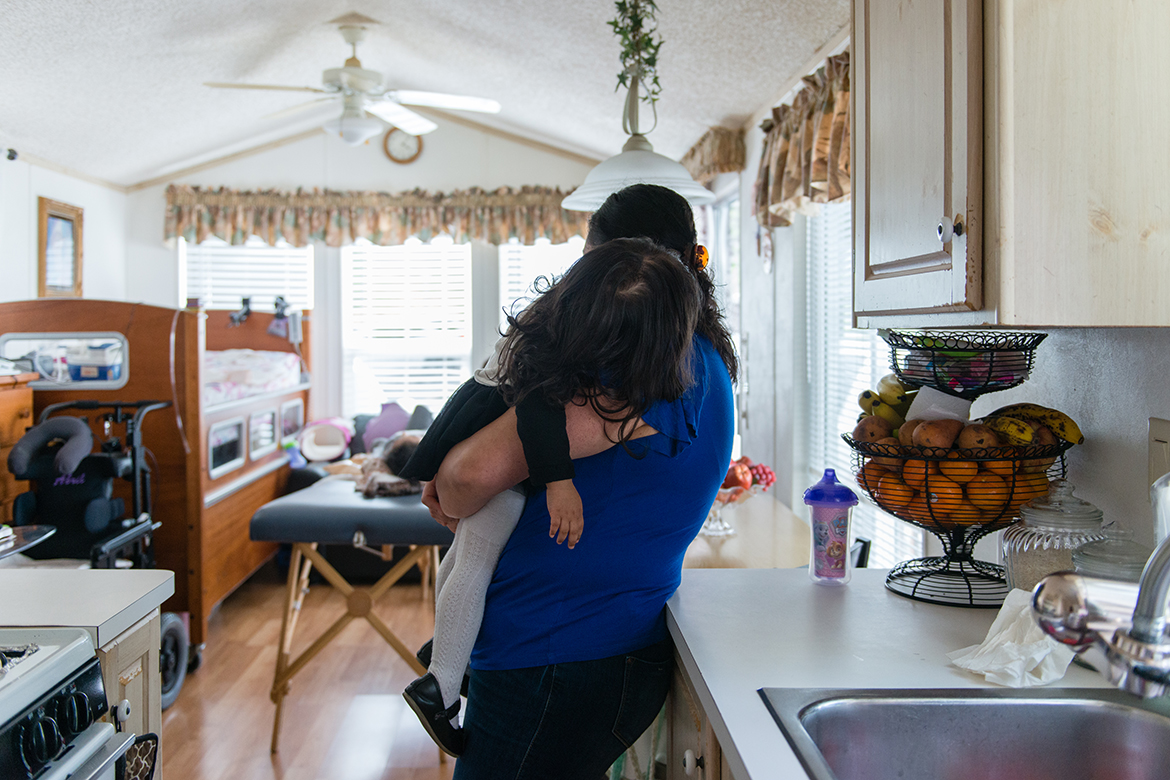
A Precarious Existence
Abril’s father, Rafael, arrived in Santa Cruz from Mexico as a teenager 19 years ago. His brothers are U.S. citizens and his mother is a legal permanent resident. In March 2001, before his 21st birthday, Rafael’s mother applied for a green card for him. He said he’s still waiting for the application to be processed.
After he’d been in California for nearly a decade, he fell in love with Sonia, who had arrived in the U.S. in 2006. She became pregnant. Everything seemed normal until she was 35 weeks along and stopped feeling the baby move. After an emergency cesarean section, Abril was rushed to Lucile Packard Children’s Hospital Stanford.
Magarian began caring for Abril when she came home at 6 weeks old. Given Abril’s serious brain damage and severe cerebral palsy, Magarian didn’t expect her to make it past six months.
Abril was in the hospital constantly at first. Her parents found great solace in their faith as they struggled to accept their new reality.
Over time, they learned the intricacies of caring for their daughter: how to suction her mouth, what to do if her gastrointestinal feeding tube gets blocked or she has a seizure, which of her grunts are normal and which require a call to 911.
Mostly because of her parents’ unwavering attention, Abril’s condition has stabilized over the years, Magarian said. Still, her health remains precarious, and she remains vulnerable to seizures and pneumonia. Many children in Abril’s situation end up hospitalized repeatedly, he said.

Even so, until recently, Rafael and Sonia had begun to feel they were living something of a normal life. Sonia watched their daughters. Rafael rode the bus each day to his job as a cook. A special-education teacher from the local school district came to the trailer twice a week to work with Abril.
Rafael and Sonia worried less about deportation during the Obama administration, which prioritized the removal of immigrants with criminal records. Donald Trump’s promises of a border wall and mass deportations made them nervous.
Their fear grew after helicopter flyovers in mid-February signaled federal immigration raids in Santa Cruz County.
Soon after, Rafael and Sonia hired an attorney to help them become legal residents.
Some advocates say they worry that desperate families with chronically ill or developmentally disabled children are unwittingly putting themselves at greater risk of deportation by seeking legal help.
Often the applicants get turned down, triggering deportation proceedings.
In the best-case scenario, a judge will cancel the parent’s removal because of the hardship it would cause for a medically dependent child. But judges don’t always do this. Barbara Pinto, a senior staff attorney at El Centro Legal de la Raza in Oakland, said more families have been asking her organization about this legal channel. She recommends against it.
“It’s seen as very irresponsible and unethical” for attorneys to suggest such a risky process, she said.
A Daunting Responsibility
Rafael and Sonia know they’re taking a risk. But they don’t know what else to do.
These days, they rarely venture out of their trailer. No more trips to the park. No more weekend strolls at the shopping mall.

In case they get picked up by immigration authorities, they have been writing down the details of Abril’s care. But those details could fill a book, they say, and they don’t even know who’d be willing to take her.
Her uncles feel so uncomfortable with her serious health problems they don’t visit anymore. Rafael’s mother is too frail to lift her 53-pound granddaughter. Certainly someone could care for Abril’s healthy younger¬Ýsister. But Abril?
“Nobody wants that big a responsibility,” Sonia said.
They think their best option might be a couple whom they barely know, whose own disabled child passed away. If that doesn’t work out, Abril could end up in foster care.
Rafael and Sonia say they wouldn’t be able to get the same financial support for Abril’s care in Mexico. Medi-Cal and California Children’s Services pay for the expensive equipment and medication that keep Abril alive ‚Äî but only here in the U.S. Together, Abril’s three seizure medications cost about $5,000 a month, an amount they say they cannot possibly afford on their own.
“If we go to Mexico and we have to bring her,” Sonia said, “it is certain she will not live much time.”
Priscila Rodríguez, associate director of Disability Rights International, said Sonia’s concerns are valid. Her organization has documented the condition of people with disabilities in Mexico, finding they often are .
Rafael and Sonia aren’t certain how much their daughter understands; her developmental delays are profound.
But, over time, they have learned to love things about her that other people don’t see: the peaceful expression that crosses her face when they hold her. The smile that started appearing much more often after her little sister was born. Her apparent affinity ‚Äî shared with little girls the world over ‚Äî for Anna and Elsa in the Disney movie “Frozen.”
Sonia smooths Abril’s hair and places her daughter gently on a bed made up with “Frozen” sheets.
“She gives us love how she can,” she says.
This story was produced by , which publishes , an editorially independent service of the .
KHN’s coverage of end-of-life and serious illness issues is supported by .
This <a target="_blank" href="/news/who-will-care-for-abril-parents-fear-for-their-disabled-child-if-they-are-deported/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=730937&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The authors of a published last month by the Cancer Prevention Institute of California believe they have a plausible explanation for the trend: People who lost their incomes or health insurance during that time were less likely to get routine screenings or visit the doctor.
The researchers’ analysis of data from the , published in the journal Cancer Causes &¬ÝControl, shows that in the state’s 30 largest counties, cancer diagnosis rates during the recession and subsequent recovery dropped by 3.3 percent annually for males and 1.4 percent for females ‚Äî¬Ýmuch faster than the average decline of 0.7 percent for males and 0.5 percent for females documented over the previous decade.
A ¬Ýin the Journal of Cancer covering the years from 1973 to 2008 found that the incidence and treatment of cancer in the United States dropped during recessions and with increased unemployment rates. During such periods, patients were perhaps more likely to forgo tests for early detection or ignore symptoms due to financial consideration, the researchers suggested.
The recent study from California buttresses that earlier finding.¬ÝThe largest drops were seen in the rates for prostate, lung and colorectal cancers. The declining rates of most cancers were especially noteworthy given the growing population of aging Baby Boomers, since cancer is more common later in life.
If people did delay getting screened for early-stage cancers during the recession, “might we then start seeing an uptick of late-stage cancers?” wondered Scarlett Lin Gomez, the study’s lead author and a researcher with the Cancer Prevention Institute of California.
Dr. Jennifer Hastings, who was not involved with the study, expects that to be the case. She is director of the transgender health care program for Planned Parenthood Mar Monte, which serves 29 counties in California and 13 in Nevada. The clinics screen for breast, cervical and colon cancer.
Hastings said doctors at her clinics started seeing more patients with advanced cancers and other serious illnesses starting in 2014, as previously uninsured people obtained coverage under the Affordable Care Act and began seeking care.
“There was great surprise about how sick people were,” she said. With the fate of the ACA now in limbo, Hastings said she’s very concerned about those people losing coverage.
Michelle Quiogue, a family doctor with Kaiser Permanente in Bakersfield and president-elect of the California Academy of Family Physicians, said she frequently sees patients make medical decisions based on the cost of care.
“Even when people have insurance, they will delay care if the cost share is too high,” Quiogue said.
During the recession, a number of her patients lost their job-based health insurance and stopped coming in for regular check-ups, she said. They didn’t return until they gained insurance under the ACA.
Lisa Schlager, vice president of community affairs and public policy for , a Tampa, Fla.-based nonprofit advocacy group focusing on hereditary ovarian and breast cancers, said it’s common for people to wait to seek treatment because they don’t have insurance or don’t have the money to pay medical bills or high deductibles.
Schlager recalled a woman who was between jobs when she felt a lump in her breast. The woman decided to wait until she found a new job ‚Äî¬Ýthen waited a few more months before her employer-sponsored insurance kicked in. By the time she went in for an exam, her cancer had advanced. She died of it.
“It’s sad, but it’s a reality in our country that money a lot of times drives the medical services that people receive or seek out,” Schlager said.
However, the state of the economy is not the only factor that can explain the drop in cancer diagnoses during the recession.
Dennis Deapen, director of the Los Angeles County Cancer Surveillance Program and a professor at the University of Southern California’s Keck School of Medicine, offered some alternative explanations for the declines in diagnoses of certain cancers, including prostate, lung and colorectal.
“It struck me that there’s good reason that those particular cancers would have been declining over that period, regardless of economic factors,” he said, noting that prostate cancer diagnosis rates, which dropped 6.3 percent annually during the study period, “have been plunging for years.”
That’s largely attributable to evolving guidelines for prostate cancer screening.
In 2008, the U.S. Preventive Services Task Force recommended against routine screening for prostate cancer among men over 75; in 2011, it recommended against the routine use of prostate-specific antigen screening in healthy men. Prior to that, Deapen said, prostate cancer was actually over-diagnosed.
Lung cancer diagnosis rates also have been dropping in recent years, at least partly due to a decrease in smoking, especially in California, he added. And colorectal cancer has declined because improved screening techniques have allowed for the removal of precancerous polyps.
Deapen said the diagnosis of some other cancers, including melanoma, is more likely to be influenced by economic factors. Melanoma often is discovered because a patient asks a doctor to check a mole, or the doctor independently notices it during a medical visit.
“If you’ve lost access, that doesn’t happen,” Deapen said. The incidence of melanoma flattened or showed slight declines during the recession years, compared with annual increases in the previous decade.
Deapen said he is interested to find out whether increased access to health care under the Affordable Care Act will have the opposite effect of the findings described in the study, allowing more people to get diagnosed ‚Äî¬Ýand treated ‚Äî¬Ýearlier.
He cited evidence that the ACA led to earlier diagnosis and saved lives. Without solid details about a replacement plan, he said he wasn’t ready to comment on whether that trend might be reversed if the law is repealed.
This story was produced by , which publishes , an editorially independent service of the .
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/cancer-rates-dropped-during-the-recession-thats-not-necessarily-a-good-thing/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=706074&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>