But physicians, dentists, ambulance companies, and other health care providers are still taking their patients to court, a Connecticut Mirror-║┌┴╧│╘╣╧═Ї News investigation of state legal records shows.
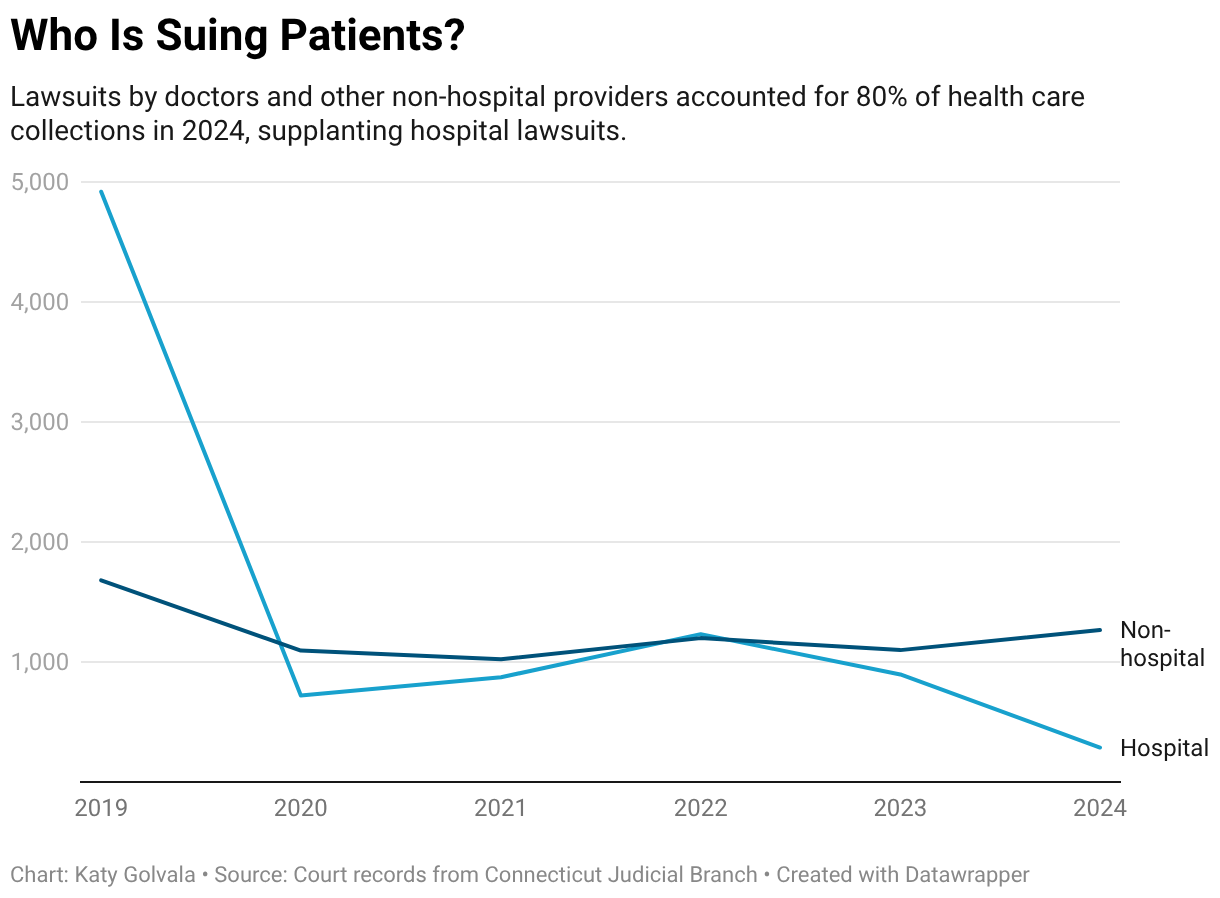
Lawsuits by doctors and other nonhospital providers now dominate health care collections in Connecticut, the records show, accounting for more than 80% of cases filed against patients and their families in 2024.
That’s a major reversal from just five years earlier, when hospital system lawsuits made up three-quarters of health-related collection cases in the state’s courts.
The shift is moving medical debt collections into a less regulated realm. Most hospitals, because they are tax-exempt nonprofits, must make financial aid available to low-income patients and follow federal regulations that limit aggressive collection activities. Other medical providers, such as private medical groups, are generally exempt from these rules.
The lawsuits are typically over bills of less than $3,000, but the impact on patients can be devastating. Lawsuits are among the most ruinous byproducts of a health care debt problem that burdens an estimated 100 million people in the U.S.
Lawsuits can lead to garnished wages, liens on homes, and hundreds of dollars of added debt from interest and court fees. They also pile additional financial strains on struggling families, prevent patients from getting needed care, and sap trust in medical providers.
“It’s really messed up,” said Allie Cass-Wilson, a nurse in Bristol, Connecticut, who was sued over a $1,972 debt by an OB-GYN practice where she’d been a patient years earlier. “How can they do that to people?” She did not contest the lawsuit, court records show.
Cass-Wilson, who is 36 and lives in a small apartment just off an expressway on-ramp, said she learned of the outstanding debt only when she was sued. When she tried making an appointment, she said, she was told her doctor wouldn’t see her. “They said I was blacklisted,” Cass-Wilson said. “I was so confused. I couldn’t believe that my medical provider let my care be interrupted like this.”
Cass-Wilson ultimately sought medical care elsewhere.
Radiologists, Dentists, Ambulances
Overall, CT Mirror and ║┌┴╧│╘╣╧═Ї News identified more than 16,000 health care-related debt cases in Connecticut courts from 2019 to 2024. The database was assembled from online court records with the help of January Advisors, a data science consulting firm that helped extract and sort the data.
Over the six-year period, most of Connecticut’s more than 25,000 did not pursue patients in court for outstanding balances.
But records show that more than 400 medical providers, including several hospital systems, sued their patients. Among those filing lawsuits were radiologists, anesthesiologists, eye doctors, podiatrists, allergists, and pediatricians.
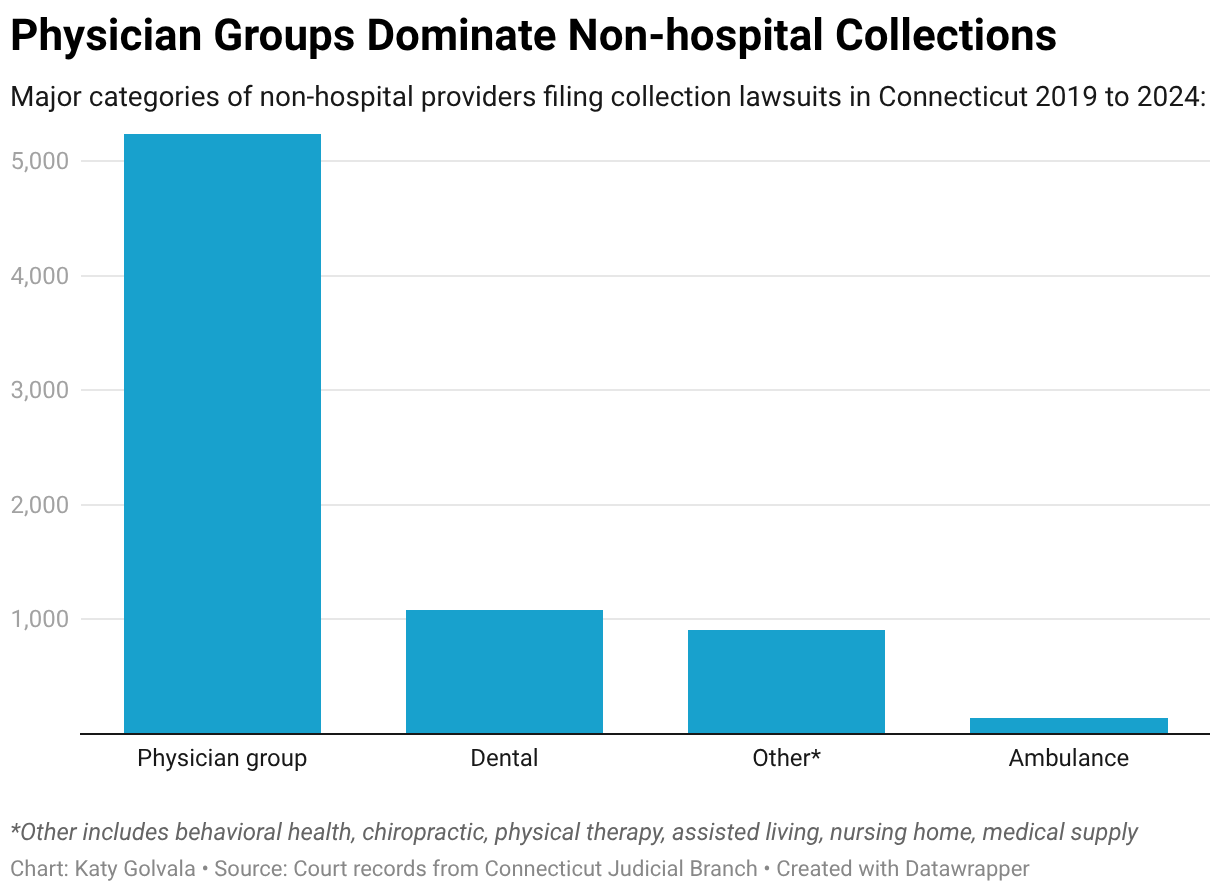
Dentists, periodontists, and other dental providers filed more than 1,000 lawsuits against patients. And ambulance companies sued more than 140 people.
Med-Aid, a company based outside New Haven, Connecticut, that provides orthopedic braces and other medical supplies to patients, sued more than 400 people, the court records show. The company’s president, Frank Dilieto, did not respond to repeated interview requests.
Cass-Wilson was sued by Briar Rose Network in Bristol, Connecticut, a member of a large network of OB-GYN practices across Connecticut called Physicians for Women’s Health. The network’s members sued close to 100 patients in 2024, records show.
Paula Greenberg, CEO of Women’s Health Connecticut, a private equity-backed company affiliated with Physicians for Women’s Health that manages business operations for the network, said the lawsuits represent a small fraction of the more than 300,000 patients the network sees every year.
“This is an organization committed to patients,” Greenberg said. She noted that the group offers options to help patients pay, including installment plans and financial aid.
Geoffrey Manton, president of Naugatuck Valley Radiological Associates, said his practice also will work with people who say they can’t pay. But, he said, patients sometimes stop responding to their bills.
“Hiding from your problems isn’t going to solve them,” Manton said. “If we didn’t take any action, there could be that person that is in that late-model Mercedes that just chooses not to pay any bills.” The group sued more than 125 patients from 2019 to 2024, according to the court records.
Many medical providers say that aggressive collections stem from the growing prevalence of high-deductible health plans that leave patients with thousands of dollars of bills before their coverage kicks in.
Greenberg and Manton said each of their physician groups must collect. “This is a business,” Greenberg said. “We have to look at our operating costs.”
Critics of medical collection lawsuits note that the patients are typically sued over relatively small debts that are likely to have little impact on multimillion-dollar medical practices.
The average patient debt that members of Physicians for Women’s Health sued over in 2024 was less than $1,100, court records show. The physician group’s annual revenues are typically in the tens of millions of dollars, according to Greenberg.
Even relatively small debts — which often include interest — can place substantial burdens on families struggling to keep up with their bills, especially while dealing with a serious illness, patient advocates say.
“We don’t have a realistic choice in using health care,” said Lisa Freeman, who heads the Connecticut Center for Patient Safety and has advocated for patients struggling with medical bills. “To then get sued for it, when people have less and less funds available for anything extra, that’s very disheartening.”
A Stroke, Then a Lawsuit

Matthew Millman, 54, lost his job as an IT support worker after having a stroke. Then Meriden Imaging Center sued him over an $1,891 bill.
Millman and his wife said they tried to explain their financial situation to the center, which is affiliated with Midstate Radiology Associates, a large physician group that operates imaging centers and doctors’ offices across Connecticut.
“It was very frustrating,” said Millman, who lives in an aging apartment owned by his wife’s family in New Britain. Millman, his wife, and their teenage daughter are barely getting by on his two part-time jobs — one bagging groceries, the other helping homebound seniors. Together, the jobs pay about $1,500 a month, he said.
The imaging center, after winning the collection case against Millman, tried to garnish his wages, though that was unsuccessful because Millman had lost his IT job.
“It’s all about money,” Millman said, shaking his head. “If you are trained in helping somebody with their health, it shouldn’t be about the money first. It should be about their health.”
Court records show that Midstate Radiology, Meriden Imaging Center and affiliates filed more than 1,000 collection lawsuits against patients from 2019 to 2024, making them the most litigious nonhospital providers in the state. As is common in medical debt lawsuits, the plaintiffs prevailed in most cases, records show.
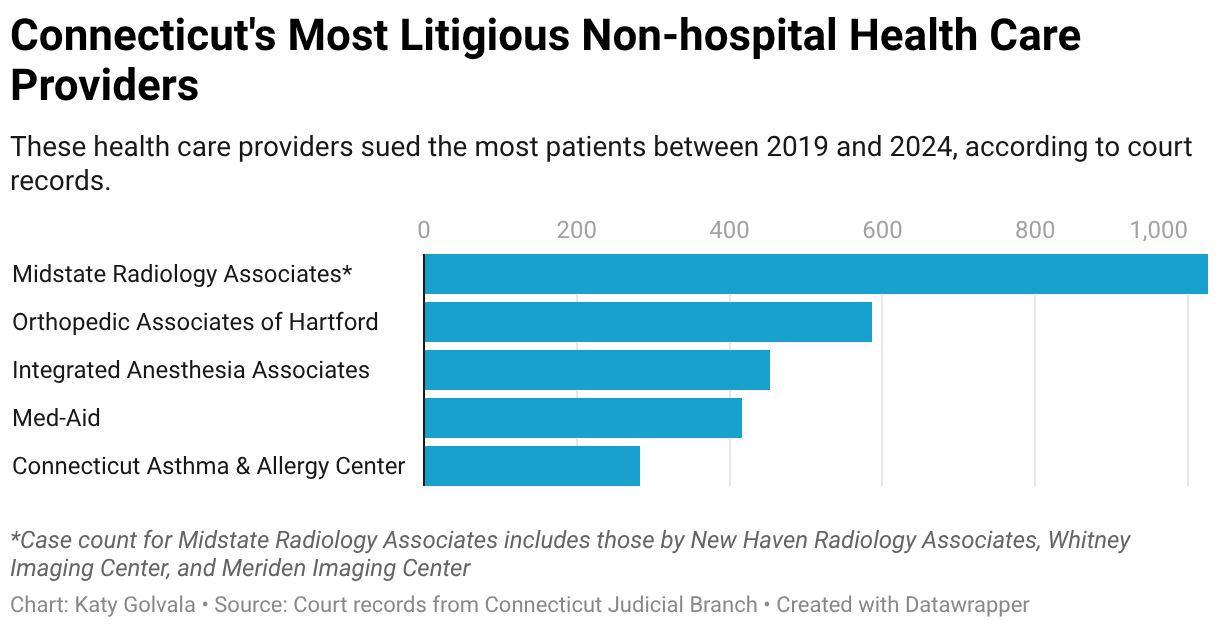
Midstate president Gary Dee, a radiologist, didn’t respond to emails and messages left at his West Hartford office.
Across town from Millman’s apartment in New Britain, Joseph Lentz lives in a cramped apartment with his wife and daughter. He used to oversee operations at a Boy Scout camp but is now unemployed. Lentz lost his job during the pandemic. The family home went into foreclosure, he said.
In 2023, Orthopedic Associates of Hartford sued Lentz over a $3,644 bill the practice said he owed after having shoulder surgery in 2018.
“I’d pay it if I could, I guess,” said Lentz, 59. “But I don’t even know where next month’s rent is coming from. I’m trying to climb out as best I can. I guess this is just one more thing to shovel in.”
The orthopedic group filed more than 580 lawsuits against patients from 2019 to 2024, prevailing in most, records show.
The medical group declined interview requests. But chief executive David Mudano said in a statement: “As an independent physician practice, we strive to balance compassion for patients with the financial responsibility required to sustain our practice.”
Old Debts and Disputed Claims
Lentz, who did not contest the lawsuit, said he has no reason to doubt he owes the debt. But in many cases reviewed by CT Mirror and ║┌┴╧│╘╣╧═Ї News and in interviews, patients being sued questioned the accuracy of their medical bills, citing care they thought health insurance should have covered or, in some cases, bills for services they never received.
This reflects with aggressive collection tactics like lawsuits when disputes over the accuracy of medical bills and delayed or denied insurance claims are so widespread in American health care.
A by the federal Consumer Financial Protection Bureau found that nearly half of the medical debt complaints fielded by the agency involved bills that consumers said were erroneous in some way or that consumers said they’d already paid.
“We know people are billed incorrectly,” said Lester Bird, who studies debt collection lawsuits at the nonprofit Pew Charitable Trusts. Bird noted that courts are ill equipped to sort through disputed medical charges or insurance claims, especially when there is little documentation in most debt collection lawsuits.
“It’s complicated before it gets to the courts,” Bird said, “and it’s very complicated when it gets into the courts.”
This can create headaches for physicians and other providers. But billing problems ultimately affect patients and their families most, said Connecticut state Sen. Saud Anwar, a Democrat who is also a physician. “Patients are left to deal with it.”
Andrew Skolnick, an attorney in Milford, outside New Haven, was sued in 2023 by an imaging center where his wife had received services in 2020.
Skolnick said that when the couple, who were covered through his job-based insurance, originally received the bill from Diagnostic Imaging of Milford, he tried to tell the imaging center it had submitted the claim to the wrong insurance plan, but he said they wouldn’t speak with him.
The center later filed the lawsuit, alleging he owed more than $2,000, plus almost $300 in interest.
Despite interview requests, officials at Diagnostic Imaging of Milford did not comment for this article.
Unlike most patients who are sued, Skolnick had the resources and expertise to contest the suit. He said he offered to pay what would have been his responsibility under the plan if the imaging center had filed his claim correctly. He ultimately settled for $1,700, court records show.
“It wasn’t a tremendous amount, but I knew that they had made a mistake,” Skolnick said. “The system is not working.”
More Protections?
Anwar, the state lawmaker and physician, expressed concern that lawsuits undermine patients’ faith in their doctors.
“It’s a sacred relationship,” he said. “If your physician, who is taking care of you, is suing you for money, that’s a problem.
Many hospitals, facing bad publicity from suing patients, have stopped taking patients to court over unpaid bills. Hospital collection lawsuits identified by CT Mirror and ║┌┴╧│╘╣╧═Ї News in Connecticut court records plunged from more than 4,900 in 2019 to fewer than 300 in 2024.
Also, in recent years, several states, including Connecticut, have expanded protections for patients with bills they can’t pay.
Connecticut now from consumer credit reports, and legislators are pushing to get hospitals to provide more financial aid to patients. Other states have restricted the use of wage garnishment and property liens to collect medical debt.
But state efforts to rein in aggressive medical debt collections have mostly focused on hospitals. That may need to change, said Connecticut state Sen. Matt Lesser, a Democrat who co-chairs the legislature’s Human Services Committee.
He is a key backer of a bill that would bar hospitals from billing patients who receive public benefits like food assistance or who make less than twice the federal poverty level, about $32,000 for an individual.
The restriction would not apply to bills from physicians and other nonhospital providers, however. “We may have to go bigger if that’s where the heart of the matter is,” Lesser said.
Connecticut Gov. Ned Lamont, a Democrat who spearheaded an initiative to for more than 150,000 state residents, also expressed concern about physicians suing the people in their care.
“Everyone should do the right thing by patients,” he said.
This article was produced in partnership with , a statewide nonprofit newsroom that covers public policy and politics.
How We Did It: Analyzing Connecticut Health Care Debt Collection Lawsuits
How often do health care providers sue patients over unpaid bills?
In most states, that’s nearly impossible to answer because courts don’t typically identify which debt collection lawsuits involve a medical debt versus other kinds of debt, such as rent, credit cards, or cellphone bills.
But Connecticut is different. Debt collection cases filed in small-claims court for unpaid medical or dental bills must be classified as health care debt. We worked with the data science consulting firm January Advisors to pull these cases from the Connecticut court database and analyze them. (January Advisors has worked with nonprofits and researchers across the country to collect debt collection data from state courts. The firm did not have any editorial input in our project.)
We started with health care collection cases filed in small-claims court from 2019 to 2024. But this covered only cases involving debts smaller than $5,000. We also wanted to know about cases in which providers sued for bills exceeding $5,000. Connecticut courts don’t assign a “medical” category for large-claim cases. So we pulled all large-claim records for any plaintiff — hospital or nonhospital provider — that appeared in medical small-claims cases. We also included cases with plaintiffs that didn’t appear in that dataset but had common medical terminology in their names, like “hospital” or “DDS.”
We then went through each case manually to confirm that the plaintiff was a medical or dental provider. We determined whether the provider was part of a larger hospital or physician group. And we categorized each plaintiff by a provider type (e.g., hospital system, dental, physician group).
In some cases, the data we pulled was incomplete, so we looked up the court records online and manually entered the information into our database. The Connecticut Judicial Department purges case records from its online portal after a certain amount of time. In those cases, we asked the agency to provide summonses and claims so we could manually enter the case information into our database.
We removed cases with out-of-state defendants or out-of-state plaintiffs and any cases in which missing records made it difficult to confirm information about the provider.
This <a target="_blank" href="/news/medical-debt-connecticut-doctors-sue-patients/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2228622&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>She and her family lived in a neatly landscaped neighborhood near Cleveland. They had a six-figure income and health insurance. Then, four years ago, when Monroe was pregnant with twin girls, something started to feel off.
“I kept having to come into the emergency room for fainting and other symptoms,” recalled Monroe, 43, who works for an insurance company.
The babies were fine. But after months of tests and hospital trips, Monroe was diagnosed with a potentially dangerous heart condition.
It would be costly. Within a year, as she juggled a serious illness and a pair of newborns, Monroe was buried under more than $13,000 in medical debt.
Part of the reason: Like tens of millions of Americans, she had a high-deductible health plan. People with these plans typically pay thousands of dollars out of their own pockets before coverage kicks in.
The plans, which have over the past two decades, are getting renewed attention thanks to President Donald Trump and his GOP allies in Congress.
Many Republicans are reluctant to extend government subsidies that help cover patients’ medical bills and insurance premiums through the Affordable Care Act.
And although GOP leaders have yet to coalesce around an alternative, several leading Republican lawmakers have said Americans who don’t get insurance through an employer should get cash in a special health care account, paired with a high-deductible health plan. In such an arrangement, someone could choose a plan on an ACA marketplace that costs less per month but comes with that can top $7,000.
“A patient makes the decision,” Sen. Bill Cassidy (R-La.) said . “It empowers the patient to lower the cost.”
In a last month, Trump said, “The only healthcare I will support or approve is sending the money directly back to the people.”
Conservative economists and GOP lawmakers have been making since high-deductible health plans started to catch on two decades ago.
Back then, a backlash against the limitations of HMOs, or health maintenance organizations, propelled many employers to move workers into these plans, which were supposed to empower patients and control costs. A change in tax law allowed patients in these plans to put away money in tax-free health savings accounts to cover medical bills.
“The notion was that if a consumer has тАШskin in the game,’ they will be more likely to seek higher-quality, lower-cost care,” said Shawn Gremminger, who leads the National Alliance of Healthcare Purchaser Coalitions, a nonprofit that works with employers that offer their workers health benefits.
“The unfortunate reality is that largely has not been the case,” Gremminger said.
Today, deductibles are almost ubiquitous, with the with job-based coverage approaching $1,700, up from around $300 in 2006.
But even as high deductibles became widespread, medical prices in the U.S. skyrocketed. The average price of a knee replacement, for example, from 2003 to 2016, more than double the rate of overall inflation.
At the same time, patients have been left with thousands of dollars of medical bills they can’t pay, despite having health insurance.
About 100 million people in the U.S. have some form of health care debt, showed.
Most, like Monroe, are insured.
Although Monroe had a health savings account paired with her high-deductible plan, she was never able to save more than a few thousand dollars, she said. That wasn’t nearly enough to cover the big bills when her twins were born and when she got really ill.
“It’s impossible, I will tell you, impossible to pay medical bills,” she said.
There was another problem with her high-deductible plan. Although these plans are supposed to encourage patients to shop around for medical care to find the lowest prices, Monroe found this impractical when she had a complex pregnancy and heart troubles.
Instead, Monroe chose the largest health system in her area.
“I went with that one as far as medical risk,” she said. “If anything were to happen, I could then be transferred within that system.”
Federal rules that require hospitals to post more of their prices can make comparing institutions easier than it used to be.
But unlike a car or a computer, most medical services remain difficult to shop for, in part because they stem from an emergency or are complex and can stretch over numerous years.
Researchers at the nonprofit Health Care Cost Institute, for example, estimated that of total health care spending for Americans with job-based coverage was for services that realistically could be shopped for.
Fumiko Chino, an oncologist at the MD Anderson Cancer Center in Houston, said it makes no sense to expect patients with cancer or another chronic disease to go out and compare prices for complicated medical care such as surgeries, radiation, or chemotherapy after they’ve been diagnosed with a potentially deadly illness.
“You’re not going be able to actually do that effectively,” Chino said, “and certainly not within the time frame that you would need to when facing a cancer diagnosis and the imminent need to start treatment.”
Chino said patients with high deductibles are often instead slammed with a flood of huge medical bills that lead to debt and a cascade of other problems.
She and other researchers found in presented last year that cancer patients who had high-deductible health insurance were more likely to die than similar patients without that kind of coverage.
For her part, Monroe and her family were forced to move out of their house and into a 1,100-square-foot apartment.
She drained her savings. Her credit score sank. And her car was repossessed.
There have been other sacrifices, too. “When families get to have nice Christmases or get to go on spring break,” Monroe said, hers often does not.
She is thankful that her children are healthy. And she continues to have a job. But Monroe said she can’t imagine why anyone would want to double down on the high-deductible model for health care.
“We owe it to ourselves to do it a different way,” she said. “We can’t treat people like this.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/trump-health-accounts-hsa-cash-patient-debt-high-deductible-insurance/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2126215&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>LISTEN: Bad credit can keep you from getting a job, a car loan, or an apartment to rent. For many Americans, health care debt is to blame. ║┌┴╧│╘╣╧═Ї News senior correspondent Noam N. Levey appeared on WAMU’s “Health Hub” on Nov. 12 to explain why new federal guidelines on health care debt and credit reports worry some consumer protection advocates.
More than 100 million Americans are estimated to have health care debt. In response, more than a dozen states have instituted laws to keep these unpaid bills off consumer credit reports.
The Trump administration has been .
The Consumer Financial Protection Bureau, headed by President Donald Trump’s budget director, issued new guidance that challenges state laws, saying only the federal government can decide what can go in a credit report. Consumer advocates say that move could undercut state-level protections and worsen the financial strain on Americans burdened by medical bills.
║┌┴╧│╘╣╧═Ї News senior correspondent Noam N. Levey appeared on WAMU’s “Health Hub” on Nov. 12 to explain why state laws like these could be especially important in the wake of the One Big Beautiful Bill Act, set to kick millions off Medicaid, and the potential lapsing of enhanced tax credits for people buying health insurance through the Affordable Care Act marketplaces.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/wamu-health-hub-medical-debt-credit-reports-cfpb-vought-new-rule/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2114479&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>More than a dozen states, including Washington, Oregon, California, Colorado, Minnesota, Maryland, New York, and most of New England, have enacted laws in recent years to keep medical debt from affecting consumers’ credit.
And more states тАФ including several in conservative regions of the Midwest and Mountain West тАФ have been considering similar protections, spurred by bipartisan concerns that medical debt on a credit report can make it harder for people to get a home, a car, or a job.
Nationwide, about 100 million people have some form of health care debt, with millions burdened by $10,000 or more in unpaid bills.
But , the Consumer Financial Protection Bureau asserts that federal law bars states from restricting medical debts from credit reports, arguing that only the federal government has this authority.
“Congress meant to occupy the field of consumer reporting and displace state laws,” the bureau concluded in an “interpretive rule” signed by Russell Vought, the White House budget director and acting head of the CFPB.
The guidance, which offers a new interpretation of the Fair Credit Reporting Act, reverses policies advanced under former President Joe Biden that sought to empower states to expand protections for people with medical debt.
The Trump administration’s latest move will not immediately roll back existing state protections.
But advocates for patients and consumers warn that the new guidance may stall progress elsewhere, just as millions of Americans are poised to lose federal aid that helps them buy health insurance through the Affordable Care Act. The aid is tied up in the current budget showdown between congressional Republicans and Democrats.
“You’d be hard-pressed to find a crueler regulatory interpretation,” said Elisabeth Benjamin, a vice president for the Community Service Society of New York. The nonprofit has pushed for medical debt protections in that state.
Lucy Culp, who oversees state lobbying efforts by Blood Cancer United, formerly known as the Leukemia & Lymphoma Society, warned that the Trump administration’s guidance could reverberate across the country. “This rule will have a chilling effect on states’ willingness to pass these critical patient protections,” she said.
The CFPB did not respond to a request for comment.
The new CFPB guidance might spur more litigation challenging state restrictions on medical debt credit reporting.
Trade groups representing credit reporting agencies and debt collectors went to court early this year challenging regulations issued by the Biden administration that would have removed medical debt from credit reports nationwide. They argued that the administration exceeded its authority in issuing the credit reporting restrictions.
The federal restrictions would have helped an estimated 15 million people. But the Trump administration chose not to defend the new regulations, and a federal judge in Texas appointed by Trump ruled that the regulations should be scrapped. They never went into effect.
The Consumer Data Industry Association, which represents credit agencies and has argued that regulating medical debt should be left to the federal government, welcomed the new guidance from the Trump administration.
“There should be one national standard to govern how information is provided to consumer reporting agencies and what information can appear on a consumer’s credit report,” association president Dan Smith said in a statement.
Broader health insurance protections could prevent more Americans from sinking into debt and depressing their credit scores.
But millions of Americans to lose health coverage in the coming years as a result of the tax and spending bill signed by the president in July.
“Millions of Americans are avoiding medical care, putting off needed surgeries, skipping essential treatments,” said Allison Sesso, president and chief executive of Undue Medical Debt, a nonprofit that buys up and retires patients’ debts and advocates for broader patient protections.
“This isn’t just a health care issue,” Sesso added. “It’s an economic crisis that’s keeping families from building wealth and fully participating in the economy. When credit scores are dinged by medical bills, everyone loses.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/medical-debt-trump-consumer-financial-protection-bureau-reverses-credit-protections/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2106810&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>It came as Democrats and Republicans in Washington headed toward a budget impasse over extending the enhanced subsidies that help millions of people maintain Affordable Care Act coverage.
But these volunteers transcended politics.
Mary Catherine Johnson is a retired small-business owner from outside Rochester, New York. She voted for Donald Trump three times.
Lexy Mealing, who used to work in a physician’s office, is from Long Island. She’s a Democrat.
But the two women share a bond: They both survived breast cancer.
“Not one person here discussed if you’re a Democrat, if you’re a Republican,” said Mealing, one of 27 volunteers from New York. “Cancer doesn’t care.”
Every volunteer had been touched in some way by cancer, which is expected to kill people in the U.S. this year.
Johnson said each of her mother’s 10 siblings died from cancer. She said she’s worried about the state of politics today. “I think we’re probably the most divided that we’ve ever been,” she said. “That scares me. Scares me for my grandchildren.”
Americans are indeed split over many issues тАФ immigration, guns, President Trump.
Yet in , 7 in 10 voters said it’s very important for the federal government to fund medical research. That included majorities of Democrats and Republicans.
“Almost everybody in this country knows somebody who’s had cancer,” said Jarrett Lewis, a Republican pollster who conducted the survey for patient groups.
A recent found that three-quarters of U.S. adults, including most Republicans who align with the Make America Great Again movement, want Congress to extend subsidies that help Americans buy health insurance through Affordable Care Act marketplaces. KFF is a health information nonprofit that includes ║┌┴╧│╘╣╧═Ї News.
These subsidies, which are critical to people with chronic illnesses such as cancer, are a sticking point in the budget showdown in Congress.
The army of volunteers тАФ from every state тАФ hit 484 of the 535 Senate and House offices.
Not every visit was an unqualified victory. Many Republican lawmakers object to extending the insurance subsidies, arguing they’re too costly.
Lawmakers from both parties have backed increased research funding and support for more cancer screening.
When evening came, the volunteers met on the National Mall for a candlelight vigil.
John Manna, another New Yorker, is a self-described Reagan Republican whose father died from lung cancer. He reflected on lessons this day could offer a divided nation.
“Get to know each other as people,” he said, “and then you can understand somebody’s positions. тАКWe have little disagreements, but,┬аyou know, we┬аdon’t┬аattack each other. We talk.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/news/the-week-in-brief-cancer-lobbyists-bipartisanship/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2104594&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
Mary Catherine Johnson is a retired small-business owner from outside Rochester, New York. She voted for Donald Trump three times.
Lexy Mealing, who used to work in a physician’s office, is from Long Island. She’s a Democrat.
But the women share a common bond. They both survived breast cancer.
And when the American Cancer Society Cancer Action Network organized its annual citizen lobby day in Washington last month, Johnson and Mealing were among the more than 500 volunteers pushing Congress to keep cancer research and support for cancer patients at the top of the nation’s health care agenda.
The day is something of a ritual for groups like the cancer organization.


This year, it came as Democrats and Republicans in Washington slid toward a budget impasse that shut down the federal government. But these volunteers transcended their political differences and found common ground.
“Not one person here discussed if you’re a Democrat, if you’re a Republican,” said Mealing, one of 27 volunteers in the New York delegation. “Cancer doesn’t care.”
Every one of the volunteer lobbyists had been touched in some way by the deadly disease, which is expected to kill people in the U.S. this year.
Johnson said each of her mother’s 10 siblings died from cancer, as did a lifelong friend who died at age 57, leaving behind his wife and two young daughters.
Like many of the New York volunteers, Johnson also said she’s worried about the state of politics today.
“I think we’re probably the most divided that we’ve ever been,” she said. “That scares me. Scares me for my grandchildren.”
Katie Martin, a cancer volunteer from outside Buffalo, also worries. She and her daughter recently drove past political protesters screaming at one another on the street.
тАК“My daughter is silent and then starts asking, тАШWhat is this?’ And I don’t know how to explain it, because it doesn’t even make sense to me,” she said. “It’s very heartbreaking.”

Mealing said she can barely watch the news these days. “A lot of Americans are very stressed out. There’s a lot of things going on.”
Americans are indeed split over many issues тАФ immigration, guns, President Trump. But helping people with cancer and other serious illnesses retains broad bipartisan support, polls show.
In , 7 in 10 voters said it’s very important for the federal government to fund medical research. That included majorities of Democrats and Republicans.
“It’s rare in today’s environment to see numbers like that,” said Jarrett Lewis, a Republican pollster who conducted the survey for patient groups. “But almost everybody in this country knows somebody who’s had cancer.”
Similarly, a recent found that three-quarters of U.S. adults, including most Republicans who align with the Make America Great Again, or MAGA, movement, want Congress to extend subsidies that help Americans buy health insurance through Affordable Care Act marketplaces.
These subsidies, which are critical to people with chronic illnesses such as cancer, are among the main sticking points in the current budget impasse in Congress.
As the cancer volunteers gathered in a conference hotel in Washington, they focused on their shared agenda: increasing funding for cancer research, retaining insurance subsidies, and expanding access to cancer screening.
“We may not see eye to eye politically. We might not even see eye to eye in social circumstances,” said Martin, the Buffalo-area volunteer. “But we can see beyond those differences because we’re here for one cause.”


The state delegations practiced the pitches they would make to their members of Congress. They ran through the personal stories they would share. And they swapped tips for how to deal with resistant staff and how to ask for a photo with a lawmaker.
On the morning of their lobby day, they reconvened in a cavernous ballroom, decked out in matching blue polo shirts and armed with red information folders to leave at each office they would visit.
They got a pep talk from a pair of college basketball coaches. Then they headed across town to Capitol Hill.
The army of volunteers тАФ from every state in the country тАФ hit 484 of the 535 Senate and House offices.
Not every visit was an unqualified victory. Many Republican lawmakers object to extending the insurance subsidies, arguing they’re too costly.
But lawmakers from both parties have backed increased research funding and support for more cancer screening.
And the New Yorkers felt good about the day. “It was amazing,” Mealing said as the day wrapped up. “You could just feel the sense of, тАШEverybody stronger together.’”
When evening came, the volunteers met on the National Mall for a candlelight vigil. It was raining. Bagpipes played.
Around a pond near the Lincoln Memorial, some 10,000 tea lights glimmered in little paper bags. Each luminary had a name on it тАФ a life touched by cancer.

John Manna, another New Yorker, is a self-described Reagan Republican whose father died from lung cancer. He reflected on the lessons this day could offer a divided nation.
“Talk to people,” he said. “Get to know each other as people, and then you can understand somebody’s positions. тАКWe have little disagreements, but, you know, we don’t attack each other. We talk and discuss it.”
Manna said he would be back next year.
This <a target="_blank" href="/public-health/cancer-common-ground-citizen-lobbyists-washington-dc/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2101966&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Despite progress in some mostly blue states this year, however, recent setbacks in more conservative legislatures underscore the persistent challenges in strengthening patient protections.
Bills to shield patients from medical debt failed this year in Indiana, Montana, Nevada, South Dakota, and Wyoming in the face of industry opposition. And advocates warn that states need to step up as millions of Americans are expected to lose insurance coverage because of President Donald Trump’s tax and spending law.
“This is an issue that had been top of mind even before the change of administrations in Washington,” said Kate Ende, policy director of Maine-based Consumers for Affordable Health Care. “The pullback at the federal level made it that much more important that we do something.”
This year, Maine joined a growing list of states that have barred medical debt from residents’ credit reports, a key protection that can make it easier for consumers to get a home, a car, or sometimes a job. The with bipartisan support.
An in the U.S. have some form of health care debt.
The federal government was poised to bar medical debt from credit reports under in the waning days of former President Joe Biden’s administration. That would have helped an estimated 15 million people nationwide.
But the Trump administration did not defend the regulations from lawsuits brought by debt collectors and the credit bureaus, who argued that the Consumer Financial Protection Bureau exceeded its authority in issuing the rules. A federal judge in Texas appointed by Trump ruled that the regulation should be scrapped.
Now, only patients in states that have enacted their own credit reporting rules will benefit from such protections. More than a dozen have such limits, including California, Colorado, Connecticut, Minnesota, New York, and Vermont, which, like Maine, enacted a ban this year.
Still more states have passed in recent years, including caps on how much interest can be charged on such debt and limits on the use of wage garnishments and property liens to collect unpaid medical bills.
In many cases, the medical debt rules won bipartisan support, reflecting the overwhelming popularity of these consumer protections. In Virginia, the state’s conservative Republican governor this year restricting wage garnishment and capping interest rates.
And several GOP lawmakers in California joined Democrats to make it easier for patients to access financial assistance from hospitals for big bills.
“This is the kind of commonsense, pocketbook issue that appeals to Republicans and Democrats,” said Eva Stahl, a vice president at Undue Medical Debt, a nonprofit that buys up and retires patients’ debts and has pushed for expanded patient protections.
But in several statehouses, the drive for more safeguards hit walls.
Bills to ban medical debts from appearing on credit reports failed in and , despite support from some GOP lawmakers. And measures to limit aggressive collections against residents with medical debt were derailed in , , and .
In some states, the measures faced stiff opposition from debt collectors, the credit reporting industry, and banks, who told legislators that without information about medical debts, they might end up offering consumers risky loans.
In Maine, the Consumer Data Industry Association, which represents credit bureaus, that regulating medical debt should be left to the federal government. “Only national, uniform standards can achieve the dual goals of protecting consumers and maintaining accurate credit reports,” warned Zachary Taylor, the group’s government relations director.
In South Dakota, state Rep. Lana Greenfield, a Republican, echoed industry objections in urging her colleagues to vote against a credit reporting ban. “Small-town banks could not receive information on a mega, mega medical bill. And so, they would in good faith perhaps loan money to somebody without knowing what their credit was,” Greenfield said on the House floor.
Under the Biden administration, that medical debt, unlike other debt, was not a good predictor of creditworthiness.
But South Dakota state Rep. Brian Mulder, a Republican who chairs the health committee and authored the legislation, noted the power of the banking industry in South Dakota, where favorable regulations have made the state a magnet for financial institutions.
In Montana, legislation to shield a portion of debtors’ assets from garnishment easily passed a committee. Supporters hoped the measure would be particularly helpful to Native American patients, who are by medical debt.
But when the bill reached the House floor, opponents “showed up en masse,” talking one-on-one with Republican lawmakers an hour before the vote, said Rep. Ed Stafman, a Democrat who authored the bill. “They lassoed just enough votes to narrowly defeat the bill,” he said.
Advocates for patients and legislators who backed some of these measures said they’re optimistic they’ll be able to overcome industry opposition in the future.
And there are signs that legislation to expand patient protections may make headway in other conservative states, including Ohio and Texas. A to force nonprofit hospitals to expand aid to patients facing large bills picked up support from leading conservative organizations.
“These things can sometimes take time,” said Lucy Culp, who oversees state lobbying efforts by Blood Cancer United, formerly known as the Leukemia & Lymphoma Society. The patients’ group has been pushing for state medical debt protections in recent years, including in Montana and South Dakota.
More concerning, Culp said, is the wave of uninsured patients expected as millions of Americans lose health coverage due to cutbacks in the recently passed GOP tax law. That will almost certainly make the nation’s medical debt problem more dire.
“States are not ready for that,” Culp said.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/courts/medical-debt-battle-patient-protections-states-trump-policy-credit-reports/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2091514&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Millions of people are expected to lose health insurance in the coming years as a result of the tax cut legislation Trump signed this month, leaving them with fewer protections from large bills if they get sick or suffer an accident.
At the same time, in health plan premiums on state insurance marketplaces next year will likely push more Americans to either drop coverage or switch to higher-deductible plans that will require them to pay more out-of-pocket before their insurance kicks in.
Smaller changes to federal rules are poised to bump up patients’ bills, as well. New federal guidelines for covid-19 vaccines, for example, will to stop covering the shots for millions, so if patients want the protection, some may have to pay out-of-pocket.
The new tax cut legislation will also raise the cost of certain doctor visits, requiring copays of up to $35 for some Medicaid enrollees.
And for those who do end up in debt, there will be fewer protections. This month, the Trump administration secured permission from a federal court to that would have removed medical debt from consumer credit reports.
That puts Americans who cannot pay their medical bills at risk of lower credit scores, hindering their ability to get a loan or forcing them to pay higher interest rates.
“For tens of millions of Americans, balancing the budget is like walking a tightrope,” said Chi Chi Wu, a staff attorney at the National Consumer Law Center. “The Trump administration is just throwing them off.”
White House spokesperson Kush Desai did not respond to questions about how the administration’s health care policies will affect Americans’ medical bills.
The president and his Republican congressional allies have brushed off the health care cuts, including hundreds of billions of dollars in Medicaid retrenchment in the mammoth tax law. “You won’t even notice it,” at the White House after the bill signing July 4. “Just waste, fraud, and abuse.”
But consumer and patient advocates around the country warn that the erosion of federal health care protections since Trump took office in January threatens to significantly undermine Americans’ financial security.
“These changes will hit our communities hard,” said Arika Sánchez, who oversees health care policy at the nonprofit New Mexico Center on Law and Poverty.
Sánchez predicted many more people the center works with will end up with medical debt. “When families get stuck with medical debt, it hurts their credit scores, makes it harder to get a car, a home, or even a job,” she said. “Medical debt wrecks people’s lives.”
For Americans with serious illnesses such as cancer, weakened federal protections from medical debt pose yet one more risk, said Elizabeth Darnall, senior director of federal advocacy at the American Cancer Society’s Cancer Action Network. “People will not seek out the treatment they need,” she said.
Trump promised a rosier future while campaigning last year, and “expand access to new Affordable Healthcare.”
Polls suggest voters were looking for relief.
About 6 in 10 adults тАФ Democrats and Republicans тАФ say they are worried about being able to afford health care, according to , outpacing concerns about the cost of food or housing. And medical debt remains a widespread problem: As many as in the U.S. are burdened by some kind of health care debt.
Despite this, key tools that have helped prevent even more Americans from sinking into debt are now on the chopping block.
Medicaid and other government health insurance programs, in particular, have proved to be a powerful economic backstop for low-income patients and their families, said Kyle Caswell, an economist at the Urban Institute, a think tank in Washington, D.C.
Caswell and other , for example, that Medicaid expansion made possible by the 2010 Affordable Care Act led to measurable declines in medical debt and improvements in consumers’ credit scores in states that implemented the expansion.
“We’ve seen that these programs have a meaningful impact on people’s financial well-being,” Caswell said.
Trump’s tax law тАФ which will slash more than $1 trillion in federal health spending over the next decade, mostly through Medicaid cuts тАФ is expected to leave 10 million more people without health coverage by 2034, according to the from the nonpartisan Congressional Budget Office. The tax cuts, which primarily benefit wealthy Americans, will add $3.4 trillion to U.S. deficits over a decade, the office calculated.
The number of uninsured could spike further if Trump and his congressional allies don’t renew additional federal subsidies for low- and moderate-income Americans who buy health coverage on state insurance marketplaces.
This aid тАФ enacted under former President Joe Biden тАФ lowers insurance premiums and reduces medical bills enrollees face when they go to the doctor or the hospital. But unless congressional Republicans act, those subsidies will expire later this year, leaving many with bigger bills.
Federal developed by the Consumer Financial Protection Bureau under the Biden administration would have protected these people and others if they couldn’t pay their medical bills.
The agency issued rules in January that would have removed medical debts from consumer credit reports. That would have helped an estimated 15 million people.
But the Trump administration chose not to defend the new regulations when they were challenged in court by debt collectors and the credit bureaus, who argued the federal agency had exceeded its authority in issuing the rules. A federal judge in Texas appointed by Trump ruled that the regulation should be scrapped.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/medical-debt-trump-policies-little-relief/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2065016&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Cox, who is a property manager at a real estate company in Globe, has tenants who rely on the safety-net program. And at the domestic violence shelter where she volunteers as president of the board, Cox said, staff always look to enroll women and their children if they can.
But Cox, who is 65, has mixed feelings about Medicaid. “It’s not that I don’t see the need for it. I see the need for it literally on a weekly basis,” she said. “I also see a need for revamping it significantly because it’s been taken advantage of for so long.”
It wasn’t hard to find people in Globe like Cox with complicated views about Medicaid.
Gila County, where Globe is located, is a conservative place тАФ almost 70% of voters went for President Donald Trump in November. And concerns about government waste run deep.
Like many rural communities, it’s also a place where people have come to value government health insurance. The number of Gila County residents on Medicaid and the related Children’s Health Insurance Program has nearly doubled over the past 15 years, according to data from the Georgetown University Center for Children and Families. Today, almost 4 in 10 residents are on one of the plans for low- and moderate-income people or those with disabilities.
So as congressional Republicans consider plans to from Medicaid, the debate over the program hits close to home for many Globe residents, even as some welcome the prospect of tighter rules and less government spending.

For Heather Heisler, the stakes are high. Her husband has been on Medicaid for years.
“We’re ranchers, and there’s not much money in ranching,” said Heisler, who gets her own health care from the Indian Health Service. “Most people think there is, but there isn’t.”
Heisler was selling handicrafts outside the old county jail in Globe on a recent Friday night when the town hosted a downtown street fair with food trucks and live music.
She said Medicaid was especially helpful after her husband had an accident on the ranch. A forklift tipped over, and he had to have part of his left foot amputated. “If anything happens, he’s able to go to the doctor,” she said. “Go to the emergency room, get medicines.”
She shook her head when asked what would happen if he lost the coverage. “It would be very bad for him,” she said.
Among other things, proposed tax legislation written by House Republicans would require working-age Medicaid enrollees to prove they are employed or seeking work. The bill, which passed the House and has advanced to the Senate, would also mandate more paperwork from people to prove they’re eligible.
Difficult applications can dissuade many people from enrolling in Medicaid, even if they’re eligible, . And the nonpartisan more than 10 million people will likely lose Medicaid and CHIP insurance under the House Republican plan.
That would reverse big gains made possible by the 2010 Affordable Care Act, which has allowed millions of low-income, working-age adults in places like Globe to get health insurance.
Nationally, Medicaid and CHIP have expanded dramatically over the past two decades, with enrollment in the programs surging from about in 2005 to more than last year, according to federal data.
“Medicaid has always played an important role,” said Joan Alker, who runs the Georgetown University Center for Children and Families. “But its role has only grown over the last couple of decades. It really stepped in to address many of the shortcomings in our health care system.”
That’s particularly true in rural areas, where the share of is higher, residents have lower incomes, and communities are reliant on industries with skimpier health benefits such as agriculture and retail.
In Globe, former mayor Fernando Shipley said he’s seen this firsthand.
“A lot of people think, тАШOh, those are the people that aren’t working.’ Not necessarily,” said Shipley, who operates a State Farm office across the road from the rusted remains of the Old Dominion copper mine. “If you’re a single parent with two kids and you’re making $20 an hour,” he added, “you’re not making ends meet. You’ve got to pay rent; you’ve got to feed those kids.”

Not far away, at the local hospital, some low-wage workers at the registration desk and in housekeeping get health care through Medicaid, chief financial officer Harold Dupper said. “As much as you’d like to pay everyone $75,000 or $80,000 a year, the hospital couldn’t stay in business if that was the payroll,” he said, noting the financial challenges faced by rural hospitals.
The growing importance of Medicaid in places like Globe helps explain why Republican efforts to cut the program face so much resistance, even among conservatives.
“There’s been a shift in the public’s attitude, and particularly voters on the right, that sometimes government plays a role in getting people health care. And that’s OK,” said pollster Bob Ward. “And if you take away that health care, people are going to be angry.” Ward’s Washington, D.C., firm, Fabrizio Ward, works for Trump. He also polls for a coalition trying to protect Medicaid.
At the same time, many of the communities where Medicaid has become more vital in recent years remain very conservative politically.
More than two-thirds of nearly 300 U.S. counties with the biggest growth in Medicaid and CHIP since 2008 backed Trump in the last election, according to a ║┌┴╧│╘╣╧═Ї News analysis of voting results and enrollment data from Georgetown. Many of these counties are in deep-red states such as Kentucky, Louisiana, and Montana.
Voters in places like these are more likely to be concerned about government waste, polls show. In one recent , 75% of Republicans said they think waste, fraud, and abuse in Medicaid is a major problem.
The actual scale of that waste is hotly debated, though relatively few enrollees are abusing the program.
Nevertheless, around Globe, Republican arguments that cuts will streamline Medicaid seemed to resonate.
Retiree Rick Uhl was stacking chairs and helping clean up after lunch at the senior center. “There’s a lot of waste, of money not being accounted for,” Uhl said. “I think that’s a shame.” Uhl said he’s been saddened by the political rancor, but he said he’s encouraged by the Trump administration’s aggressive efforts to cut government spending.
Back at the street fair downtown, David Sander, who is also retired, said he doubted Medicaid would really be trimmed at all.
“I’ve heard that they really aren’t cutting it,” Sander said. “That’s my understanding.”
Sander and his wife, Linda, were tending a stall selling embroidery that Linda makes. They also have a neighbor on Medicaid.
“She wouldn’t be able to live without it,” Linda Sander said. “Couldn’t afford to have an apartment, make her bills and survive.”

This <a target="_blank" href="/health-care-costs/medicaid-cuts-arizona-county-trump-voters-conflicted/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2039323&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Underscoring the massive scale of America’s medical debt problem, a New York-based nonprofit has struck a deal to pay off old medical bills for an estimated 20 million people.
, which buys patient debt, is retiring $30 billion worth of unpaid bills in a single transaction with Pendrick Capital Partners, a Virginia-based debt trading company. The average patient debt being retired is $1,100, according to the nonprofit, with some reaching the hundreds of thousands of dollars.
The deal will prevent the debt being sold and protect millions of people from being targeted by collectors. But even proponents of retiring patient debt acknowledge that these deals cannot solve a crisis that now touches around 100 million people in the U.S.
“We don’t think that the way we finance health care is sustainable,” Undue Medical Debt chief executive Allison Sesso said in an interview with ║┌┴╧│╘╣╧═Ї News. “Medical debt has unreasonable expectations,” she said. “The people who owe the debts can’t pay.”
In the past year alone, Americans borrowed an estimated $74 billion to pay for health care, a nationwide found. And even those who benefit from Undue’s debt relief may have other medical debt that won’t be relieved.
This large purchase also highlights the challenges that debt collectors, hospitals, and other health care providers face as patients rack up big bills that aren’t covered by their health insurance.
Pendrick’s chief executive, Chris Eastman, declined several requests to be interviewed about the debt sale, which has not been previously reported. But Eastman acknowledged in that collecting medical debts has grown more challenging as regulators have restricted how collectors can pursue patients.
Pendrick has now shuttered, which Sesso said provided strong motivation for this deal. “This was a really great opportunity to get a debt buyer out of the market,” she said.
Undue Medical Debt a decade ago, leveraging charitable donations to buy medical debt from debt trading companies at steeply discounted prices and then freeing patients from the obligation to pay.
The nonprofit now buys debts directly from hospitals, as well. And it is working with about two dozen state and local governments to leverage public money to relieve medical debt in communities from Los Angeles County to Cleveland to the state of Connecticut.
The approach has been controversial. And Undue Medical Debt’s record-setting purchase тАФ financed by a mix of philanthropy and taxpayer dollars тАФ is likely to stoke more debate over the value of paying collectors for medical debts.
“The approach is just treating the symptoms and not the disease,” said Elisabeth Benjamin, a vice president at the Community Service Society of New York, a nonprofit that has led efforts to restrict aggressive hospital collections. Benjamin and other advocates say systemic changes such as ensuring hospitals offer sufficient financial aid to patients and reining in high medical prices would be more valuable in preventing people from sinking into debt.
But many government officials see retiring people’s unpaid medical bills as part of a larger strategy to make it easier for patients to avoid debt in the first place.
“Turning off the tap is what’s really important in the long run,” said Naman Shah, a physician who directs medical affairs at the Los Angeles County Department of Public Health. The county is local hospital financial aid programs for patients. But Shah said debt relief is key, as well.
тАК“It’s easy to criticize band-aids when you’re not the one who’s cut,” he said. “As a physician, I take care of people who have cuts, and I know the importance of stitching them back up.”
Undue Medical Debt’s latest deal, which it is spending $36 million to close, will help patients nationwide, according to the nonprofit. But about half the estimated 20 million people whose debts Pendrick owned live in just two states: Texas or Florida.
Neither has expanded Medicaid coverage through the 2010 Affordable Care Act, a key tool that bolsters patients’ financial security by protecting them from big medical bills and debt.
The patients eligible for debt relief have incomes at or below four times the federal poverty level, about $63,000 for a single person, or debts that exceed 5% of their incomes.
About half the debts are also more than seven years old. These have been donated to Undue Medical Debt by Pendrick, the group reported.
The nonprofit plans to pay for the rest of the debts over the next year and a half, though all collections have stopped against patients. It also plans to spend an additional $40 million тАФ or $2 a person тАФ to process the debts, find patients, and inform them that their debts have been relieved.
Sesso, Undue’s chief executive, said she hopes the debt purchase will keep policymakers focused on enacting longer-term solutions to the nation’s medical debt crisis.
She applauded state leaders for taking steps to bar medical debts from their residents’ credit scores. But she said action is also needed in Washington, D.C. However, the Trump administration has suspended regulations enacted under former President Joe Biden that would have barred credit reporting of medical debt nationally, and congressional Republicans are now moving to revoke the new rules.
“There is a limit to what state and local governments can do to solve this problem,” Sesso said. “It’s really a national problem that has to be solved at the national level.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/undue-medical-debt-blockbuster-deal-relief-billions/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2009450&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>