And CEO Brad Meyer fears times will soon get worse for the clinic and its 21,000 patients. That’s because Nebraska is set to become the first state to require certain Medicaid enrollees to work or lose their coverage under new rules in President Donald Trump’s One Big Beautiful Bill Act.
“This will have a huge financial impact on us,” Meyer said. On May 1, seven months before the law requires, the state will begin imposing work requirements on eligible adult Medicaid enrollees.
Most of Bluestem’s patients are covered by the government program for people with low incomes or disabilities. Meyer estimates up to 15% of them may be kicked off Medicaid, which could cost his center about $600,000 a year. That could mean cutting services or staff.
Nationwide, about 17,000 federally funded community health centers like Bluestem . They’re bracing for fallout from the law Trump signed last year, which could cost the nonprofit health centers $32 billion collectively over five years, according to the Commonwealth Fund, a health research foundation.
Health centers receive annual federal grants but depend on Medicaid reimbursements for patient care as their largest source of revenue. The government insurance program covered about half of their roughly 33 million patients in 2024.
Commonwealth estimates that 5.6 million patients of health centers will lose Medicaid coverage over the next decade as most states enact work requirements ‚Äî a provision of Trump’s law that requires nondisabled enrollees to work, volunteer, or perform another approved activity for at least 80 hours a month.
Most are expected to lose coverage not because they don’t work but because of paperwork errors, like failing to document their hours or verify that they qualify for an exemption.
Health center officials say there’s no easy way to make up for the lost revenue other than cutting staff or services, which would affect all their patients. The cuts will coincide with an expected increase in patients, as people who lose coverage turn to the clinics for low-cost care.
By law, health centers are required to treat all patients regardless of their ability to pay.
A Double Whammy
Overall, about 10 million fewer Americans will have insurance by 2034, the Congressional Budget Office estimates, both because of Trump’s law and congressional Republicans’ decision to scale back premium subsidies for Affordable Care Act health plans.
“We are incredibly worried,” said Jeffrey McKee, CEO of Community Health Centers of Burlington in Vermont. His clinics treat about 35,000 patients a year, nearly a third covered by Medicaid.
He predicts a surge in uninsured patients will cost another $3 million in lost revenue. That revenue crash could imperil street medicine programs and home care for patients 65 and older, he said.
In 2024, community health centers because of rising costs and the expiration of covid pandemic-era relief funds, according to a KFF analysis.
Centers with high rates of uninsured patients typically struggle more financially, while some centers are sustained through private donations.
People without insurance — who made up about 18% of all health center patients in 2024 — pay on a sliding scale. Those amounts are a fraction of what insurers pay.
The new Medicaid work requirements apply to Washington, D.C., and 40 states that expanded Medicaid eligibility under the ACA, and to adults with incomes up to 138% of the federal poverty level — $22,025 for a single person this year.
Republicans say the work requirements will nudge people into the workforce and help preserve Medicaid for children and people who are pregnant or have disabilities. Studies by KFF and others show most enrollees already work, go to school, or have a health condition that prevents them from working.
Nebraska Is First Up
The Trump administration approved Nebraska’s early launch of its work requirement program, which could affect about . State Medicaid officials say they plan to use state and national databases to check whether people are already working or meeting an exemption so that most won’t have to do anything to keep coverage. But thousands will need to prove they satisfy the requirements.
At Bluestem in Lincoln, Meyer worries many of his Medicaid patients won’t take the steps needed to keep coverage.
Angelisa Corum, 57, said she loves the care she has gotten from her regular doctor at Bluestem Health over the past dozen years, particularly in dealing with breast cancer. “I am cancer-free, and they helped me get through that,” she said.
She said the care was the same when she was covered by her husband’s commercial insurance through his employer and when she was on Medicaid while he wasn’t working.
The work requirements are just one part of the Republican law passed last year that could hurt the health centers. It also requires more frequent eligibility checks for adults enrolled under Medicaid expansion, which advocates say could also lead people to lose coverage. Many states now require eligibility checks only once a year.
The law also reduces overall federal Medicaid funding to states, which may prompt them to cut reimbursements to centers and other health providers.
The National Association of Community Health Centers, the largest advocacy group for the clinics, has tried to walk a tightrope, warning about impending cuts from the law while still working with the Trump administration. The group praised Congress for increasing base grant funding for health centers in the federal budget approved in January.
Kyu Rhee, CEO of the national association, said the clinics enjoy strong bipartisan support in Washington despite the Medicaid cuts.
He has met with Trump administration officials to discuss how health centers can play a role in keeping people from losing coverage due to work requirements. He said they can help meet other priorities of the administration’s, like improving American diets, expanding primary care, and focusing on chronic diseases ‚Äî though it’s unclear how any of that would result in more funding.
To further show the reach of health centers, the association recently funded a study that found 52 million people visited the clinics over a three-year-period. “It makes a statement we serve a lot more Americans than those from just a single year,” Rhee said.
Health center officials are hopeful they will get some of the funding from the included in the GOP-passed law. States will begin spending the first tranche of that money this spring.
Rhee said he is encouraged that states will have technology to help tap into databases to verify many enrollees’ work status or health conditions to meet “medical frailty” rules that could help them avoid being disenrolled.
Others are less optimistic.
“Health centers are bracing for a major financial impact,” said Sara Rosenbaum, a health law and policy professor at George Washington University and Medicaid expert who co-authored the Commonwealth Fund study. “The way they cope is the same way health systems usually cope as they go through mass layoffs, site closures, and service reductions.”
Amanda Pears Kelly, CEO of Advocates for Community Health, a trade group representing 52 health centers, said health centers are also worried about rising costs, especially for prescription drugs. The impending financial challenges will make it more difficult to hire staff both in rural areas where doctors and nurses are scarce and in more populated areas, where competition for workers is more acute, she told ∫⁄¡œ≥‘πœÕ¯ News.
“The challenge is health centers are being hit from every direction,” Pears Kelly said.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/federal-funded-community-health-centers-revenue-loss-under-trump/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2173906&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But seven months later, findings from five states shared with ∫⁄¡œ≥‘πœÕ¯ News show that the reviews have uncovered little evidence of a widespread problem.
Only U.S. citizens and some lawfully present immigrants are eligible for Medicaid, which covers health care costs for people with low incomes and disabilities, and the closely related Children’s Health Insurance Program. Both programs are administered by states.
Spokespeople from Pennsylvania’s and Colorado’s Medicaid agencies said, as of March, the states had found no one who needed to be terminated from Medicaid. That was after checking a combined 79,000 names.
Texas has reviewed records of more than 28,000 Medicaid enrollees at the Trump administration’s request and terminated coverage for 77 of them, according to Jennifer Ruffcorn, a spokesperson for the Texas Department of Human Services.
Ohio has checked 65,000 Medicaid enrollees, of which 260 people were disenrolled from the program, said Stephanie O’Grady, a spokesperson for the Ohio Department of Medicaid.
In Utah, 42 of the 8,000 enrollees identified by the Trump administration had their Medicaid coverage terminated, said Becky Wickstrom, a spokesperson for the state’s Department of Workforce Services.
In announcing the reviews, Health and Human Services Secretary Robert F. Kennedy Jr. said: “We are tightening oversight of enrollment to safeguard taxpayer dollars and guarantee that these vital programs serve only those who are truly eligible under the law.”
Leonardo Cuello, a research professor at Georgetown University’s Center for Children and Families, said the reviews ordered by the federal Centers for Medicare & Medicaid Services were unneeded because states check immigration status when people sign up.
“It is entirely predictable that all of these burdensome reviews that the federal government is forcing upon states would yield no pay dirt,” Cuello said. “The states had already done the reviews once, and CMS was just making them reverify the same information they had already checked. Making states go through the same bureaucratic process twice is incredibly wasteful and inefficient.”
CMS spokesperson Chris Krepich said in a statement to ∫⁄¡œ≥‘πœÕ¯ News that the ongoing checks are verifying eligibility “for certain enrollees whose status could not be confirmed through federal data sources.”
“CMS provides states with regular reports for follow-up review, and states are responsible for independently verifying eligibility and taking appropriate action consistent with federal requirements,” he said.
But the findings shared with ∫⁄¡œ≥‘πœÕ¯ News also suggest that many of the enrollees whose eligibility the Trump administration said it could not confirm are indeed U.S. citizens. O’Grady said Ohio found that, of the 65,000 names referred by the federal government, the state already had information on 53,000 confirming them as citizens and an additional 11,000 showing appropriate immigration status for Medicaid.
Caseworkers then worked on the remaining 1,000 names to review their information or reach out for more details, she said.
CMS did not answer questions about the findings from the states sampled by ∫⁄¡œ≥‘πœÕ¯ News or provide information about responses it received from all 50 states and the District of Columbia, which were instructed to perform verification checks.
The agency also did not respond to a question about whether it’s forwarding the names of those whose Medicaid coverage was terminated to federal immigration officials.
In June, advisers to Kennedy ordered CMS to share information about Medicaid enrollees with the Department of Homeland Security, prompting a lawsuit by some states alarmed that the administration would use the information for its deportation campaign against residents living in the U.S. without authorization.
A federal judge that Immigration and Customs Enforcement workers could access information only about people in the country unlawfully in the Medicaid databases of the states that sued.
CMS continues to send states lists of names at least every few months, though state officials say the numbers have declined since the first batch last summer.
People without legal status are ineligible for federally funded health coverage, including Medicaid, Medicare, and plans through the Affordable Care Act marketplaces. Medicaid does reimburse hospitals for providing emergency care to people without legal status if they meet income and other program requirements.
Seven states and the District of Columbia provide health coverage regardless of immigration status, funding the programs with their own money.
In March 2025, CMS began financial reviews of those programs. “CMS has identified over $1.8 billion in federal funds that are being recouped through voluntary returns and deferrals of future federal Medicaid payments,” Krepich said. He did not answer how much has been collected so far or from which states.
Medicaid’s overall spending topped $900 billion in fiscal year 2024.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/medicaid-undocumented-enrollees-review-few-violators/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2174376&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But when Quinn chipped a tooth and it became infected, she could not find a dentist near her home who would accept her government health coverage and was taking new patients.
She went to an emergency room, receiving painkillers and antibiotics, but she remained in agonizing pain weeks later and paid a dentist $200 to extract the tooth.
Years later, it still hurts to chew on that side, she said, but Quinn ‚Äî a 34-year-old who has four children and, with her husband, earns about $30,000 a year ‚Äî still can’t find a dentist nearby.
“You should be able to get dental care,” she said, “because at the end of the day dental care is health care.”
The federal government has long required states to offer dental coverage for children enrolled in Medicaid, the joint state-federal health program for people who are low-income or disabled. Paying for adults’ dental care, though, is optional for states.
In recent years, several states have opted to expand the coverage offered by their Medicaid programs, seeking to boost access in recognition of its importance to overall health. So far, increasing adult dental care is a work in progress: In a sampling of six of those states by ∫⁄¡œ≥‘πœÕ¯ News, fewer than 1 in 4 adults on Medicaid see a dentist at least once a year.
But under congressional Republicans’ One Big Beautiful Bill Act, which President Donald Trump signed into law last year, the federal government is expected to reduce Medicaid spending by more than $900 billion over the next decade. The range from about $184 million for Wyoming to about $150 billion for California.
State Medicaid programs typically expand or reduce benefits depending on their finances, and such massive federal cuts could force some to shrink or eliminate what they offer, including dental benefits.
“We will lose all the gains we have made,” said Shillpa Naavaal, a dental policy researcher at Virginia Commonwealth University in Richmond.
Tennessee’s Medicaid program, for instance, spent nearly $64 million on its dental coverage in 2024 and saw a 20% decrease in dental-related ER visits, said Amy Lawrence, the program’s spokesperson.
But under the new law, Tennessee is projected to lose about $7 billion in federal funding over the next decade.
As of last year, 38 states and the District of Columbia offered enhanced dental benefits for adult Medicaid beneficiaries, according to the American Dental Association. Most of the others offer limited or emergency-only care. Alabama is the only state that offers no dental coverage for adult beneficiaries.
Since 2021, 18 states have enhanced their coverage to include checkups, X-rays, fillings, crowns, and dentures, while loosening annual dollar caps for benefits.
Use of dental benefits in states with the enhanced benefits is greater than in states with only limited or emergency coverage, though still low overall, according to with the latest data as of December. No more than a third of adult Medicaid recipients saw a dentist in 2022 in any state.
To review more recent progress, ∫⁄¡œ≥‘πœÕ¯ News asked one-third of the states that have expanded their benefits in the past five years for their most recent data on the percentage of adults on Medicaid who visit a dentist at least once a year:
- Maryland — 22% (in 2024)
- Oklahoma — 16% (in 2025)
- Maine — 13% (in 2025)
- New Hampshire — 19% (in 2025)
- Tennessee — 16% (in 2024)
- Virginia — 21% (in 2025)
In comparison, about 50% to 60% of adults with private dental coverage see a dentist at least once a year, according to the ADA.
Nationwide, 41% of dentists reported participating in Medicaid in 2024, a share that has remained stable over the past decade despite the dental benefit expansions in many states, the ADA says. Many participating dentists, though, limit the number of Medicaid enrollees they treat, and some will not accept new patients on Medicaid.
Reimbursement rates have not kept up with costs, deterring dentists from accepting Medicaid, said Marko Vujicic, chief economist and vice president at the ADA Health Policy Institute.
Because of a lack of dentists who take Medicaid in southwestern Virginia, the Appalachian Highlands Community Dental Center in Abingdon sees patients who travel more than two hours for care — and must turn many away, said Elaine Smith, its executive director.
The center’s seven residents treated about 5,000 patients last year, most of them on Medicaid. About 3,000 people are on its waitlist, waiting up to a year to be seen.
“It’s sad because they have the means now to see a dentist, but they still don’t have a dental home,” Smith said.
Low-income adults face other barriers to dental care, including a lack of transportation, child care, or time off work, she said.
The inability to see a dentist has consequences broader than tooth pain. Poor dental health can contribute to a host of other significant health problems, such as heart disease . It can also make it harder to do things like apply for jobs and generally lead a healthy life.
Robin Mullins, 49, who has been off and on Medicaid since 2013, said a lack of regular dental visits contributed to her losing her bottom teeth. Unable to find a dentist near her home in rural Clintwood, Virginia, she drives almost 90 minutes to Smith’s clinic ‚Äî that is, when she can afford to get time away from driving for DoorDash or find help watching her daughter, who has special needs.
She gets by with partial dentures but misses her natural teeth, she said. “It’s absolutely horrible, as you can’t chew your food properly.”
In New Hampshire, though, the challenges have more to do with low demand than a low supply of dentists, said Tom Raffio, chief executive of Northeast Delta Dental, which manages the state’s Medicaid dental program. The company has added new dentists to its list of participating providers, along with two mobile dental units that traverse the state, he said.
Raffio said Northeast Delta Dental also has publicized the state benefits using radio advertising and social media, among other efforts.
Until 2023, New Hampshire Medicaid covered only dental emergencies.
“Culturally, it’s going to take a while,” he said, “as people just are used to not going to the dentist, or going to the ER when have dental pain.”
Brooks Woodward, dental director at Baltimore-based Chase Brexton Health Care, called Maryland’s rate of roughly 1 in 5 adults on Medicaid seeing a dentist in 2024 “pretty good” considering the benefits had been enhanced only since 2023.
Woodward said many adults on Medicaid believe that you go to a dentist only when you’re in pain. “They’ve always just not gone to the dentist, and that’s just the way they had it in their life,” he said.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/medicaid-cuts-dental-coverage-republicans-big-beautiful-bill/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2161478&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Warning patients could deter them from signing up for a program called Emergency Medicaid, through which the government reimburses hospitals for the cost of emergency treatment for immigrants who are ineligible for standard Medicaid coverage.
But if hospitals don’t disclose that the patients’ information is shared with federal law enforcement, they might not know that their medical coverage puts them at risk of being located by Immigration and Customs Enforcement.
“If hospitals tell people that their Emergency Medicaid information will be shared with ICE, it is foreseeable that many immigrants would simply stop getting emergency medical treatment,” said , a research professor at Georgetown University’s Center for Children and Families. “Half of the Emergency Medicaid cases are for the delivery of U.S. citizen babies. Do we want these mothers avoiding the hospital when they go into labor?”
For more than a decade, hospitals and states have assured patients that their personal information, including their home addresses and immigration status, would not be shared with immigration enforcement officials when they apply for federal health care coverage. guaranteed the agency would not use information from health coverage applications for enforcement activities.
But that changed last year, after President Donald Trump returned to the White House and ordered one of the most aggressive immigration crackdowns in recent history. His administration began funneling data from a variety of government agencies to the Department of Homeland Security, including filed with the IRS.
The Centers for Medicare & Medicaid Services, part of the Department of Health and Human Services, agreed last spring to give ICE officials direct access to a Medicaid database that includes enrollees’ addresses and citizenship status.
Twenty-two states, all but one led by Democratic governors, the Medicaid data-sharing agreement, which the administration did not formally announce until a federal judge ordered it to do so last summer. The judge that in those states, ICE could access information in the Medicaid database only about people in the country unlawfully. ∫⁄¡œ≥‘πœÕ¯ News contacted more than a dozen hospitals and hospital associations in states and cities that have been targets of ICE sweeps. Many declined to comment on whether they’ve updated their disclosure policies after the ruling.
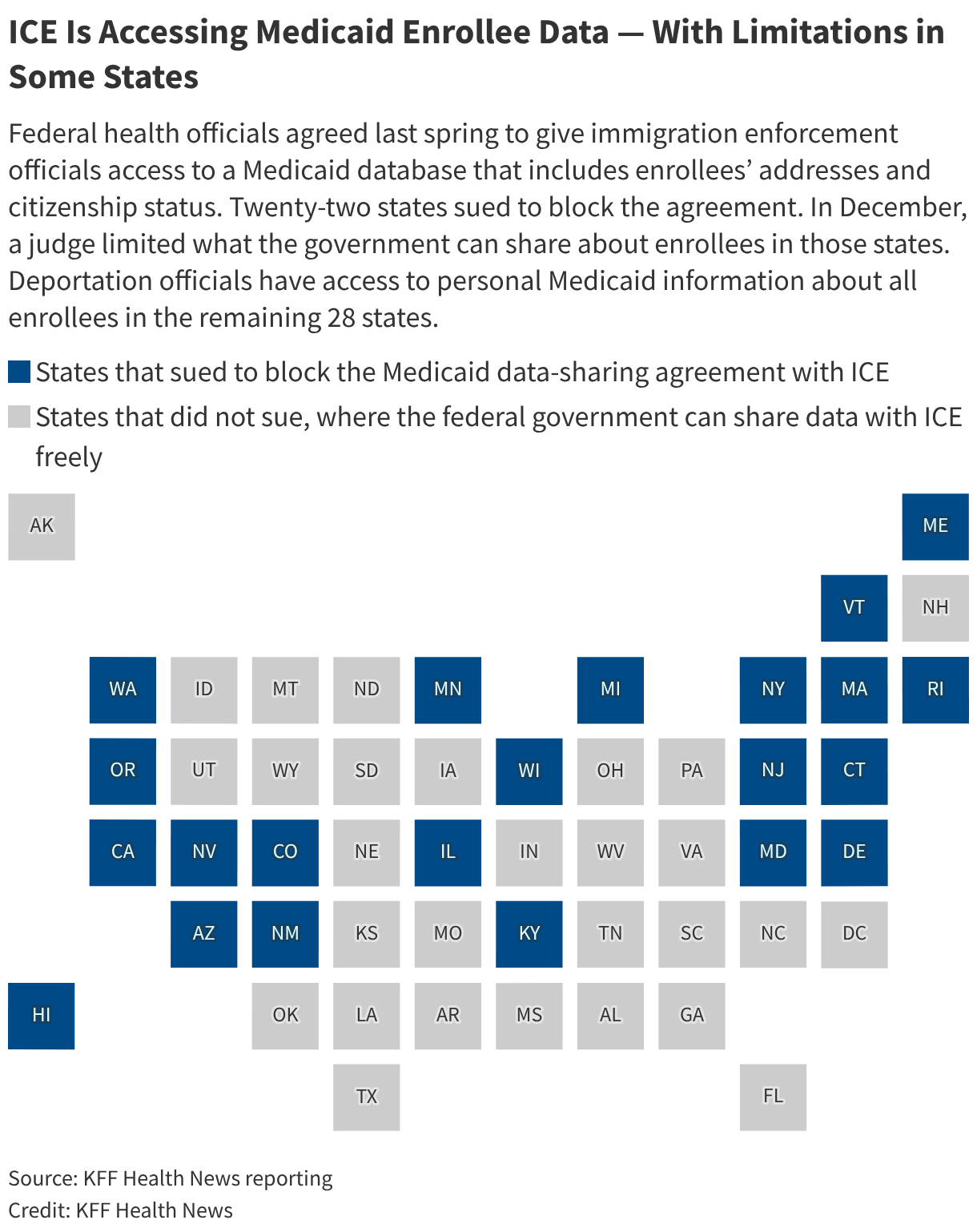
Of those that responded, none said they are directly warning patients that their personal information may be shared with ICE when they apply for Medicaid coverage.
“We do not provide legal advice about federal government data-sharing between agencies,” Aimee Jordon, a spokesperson for M Health Fairview, a Minneapolis-based hospital system, said in an email to ∫⁄¡œ≥‘πœÕ¯ News. “We encourage patients with questions about benefits or immigration-related concerns to seek guidance from appropriate state resources and qualified legal counsel.”
Information on Applications
Some states’ Emergency Medicaid applications specifically ask for a patient’s immigration status — and still assure people that their information will be kept secure and out of the hands of immigration enforcement officials.
For example, as of Feb. 3, California’s application still included language advising applicants that their immigration information is “confidential.”
“We only use it to see if you qualify for health insurance,” states the 44-page form, which the state’s Medicaid program, known as Medi-Cal, in January.
California Department of Health Care Services spokesperson Anthony Cava said in a statement that the agency, which oversees Medi-Cal, will “ensure that Californians have accurate information on the privacy of their data, including by revising additional publications as necessary.”
Until late January, Utah’s Medicaid website also claimed its Emergency Medicaid program did not share its information with immigration officials. After ∫⁄¡œ≥‘πœÕ¯ News contacted the state agency, Kolbi Young, a spokesperson, said Jan. 23 that the language would be taken down immediately. It was removed that day.
Oregon Health & Science University, a hospital system based in Portland, offers immigrant patients developed by the state Medicaid program for those with concerns about how their information might be used. The document does not directly say that Medicaid enrollees’ information is shared with ICE officials.
Hospitals rely on Emergency Medicaid to reimburse them for treating people who would qualify for Medicaid if not for their citizenship status — those in the country illegally and lawfully present immigrants, such as those with a student or work visa. The coverage pays only for emergency medical and pregnancy care. Typically, hospital representatives help patients apply while they are still in the medical facility.
The main Medicaid program, which covers a much broader range of services for over 77 million low-income and disabled people, does not cover people living in the country illegally.
Examining Emergency Medicaid enrollment is the most obvious way, then, for deportation officials to identify immigrants, including those who might not reside in the U.S. lawfully.
HHS spokesperson Rich Danker said in an email that CMS — which oversees Medicaid, a joint state-federal program — is sharing data with ICE after the judge’s ruling. But he would not answer how the agency is ensuring it is sharing information only on people who are not lawfully present, as the judge required.
With ICE now getting direct access to the personal information of millions of Medicaid enrollees, hospitals — while “definitely in a tough position” — should be up-front about the changes, said Sarah Grusin, at the National Health Law Program, an advocacy group.
“They need to be telling people that the judge has permitted sharing of information, including their address, for people who are not lawfully residing,” she said. “Once this information is submitted, you can’t protect it from disclosure at this point.”
Grusin said she advises families to weigh the importance of seeking medical care against the risk of having their information shared with ICE.
“We want to give candid, honest information even if it means the decision people have to make is really hard,” she said.
Those who have previously enrolled in Medicaid or can easily search their address online should assume that immigration officials already have their information, she added.
Emergency Medicaid
Emergency Medicaid coverage was established in the mid-1980s, when a federal law began requiring hospitals to treat and stabilize all patients who show up at their doors with a life-threatening condition.
Federal government spending on Emergency Medicaid accounted for nearly $4 billion in 2023, or of total federal spending on Medicaid.
States send monthly reports to the federal government with detailed information about who enrolls in Medicaid and what services they receive. The judge’s ruling in December limited what CMS can share with ICE to only basic information, including addresses, about Medicaid enrollees in the 22 states that sued over the data-sharing arrangement. ICE officials are not supposed to access information about the medical services people receive, per the judge’s order.
The judge also prohibited the agency from sharing the data of U.S. citizens or lawfully present immigrants from those states.
Deportation officials have access to personal Medicaid information of all enrollees in the remaining 28 states.
The federal health agency has not clarified how it is ensuring that certain states’ information on citizens and legal residents is not shared with ICE. But Medicaid experts say it would be nearly impossible for the agency to separate the data, raising questions about whether the Trump administration is complying with the judge’s order.
The Trump administration’s efforts to deport immigrants living in the country illegally have had implications on immigrant families seeking care. About a third of adult immigrants reported skipping or postponing health care in the past year, according to a released in November. (KFF is a health information nonprofit that includes ∫⁄¡œ≥‘πœÕ¯ News.)
Bethany Pray, the chief legal and policy officer at the Colorado Center on Law and Policy, warned that sharing Medicaid data directly with deportation officials will force even tougher decisions upon some families.
“This is very concerning,” Pray said. “People should not have to choose between giving birth in a hospital and wondering if that means they risk deportation.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/ice-immigrants-medicaid-data-sharing-hospitals-states-deportation/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2151281&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>It was a contrast to how Cole, 18, spent part of the 2024 holiday season. She was in the hospital — a frequent occurrence with sickle cell disease, a genetic condition that damages oxygen-carrying red blood cells and for years caused debilitating pain in her arms and legs. Flare-ups often would force her to cancel plans or miss school.
“With sickle cell it hurts every day,” she said. “It might be more tolerable some days, but it’s a constant thing.”
In May, Cole completed a several-months-long that helps reprogram the body’s stem cells to produce healthy red blood cells.
She was one of the first Medicaid enrollees nationally to benefit from a in which the federal government negotiates the cost of a cell or gene therapy with pharmaceutical companies on behalf of state Medicaid programs ‚Äî and then holds them accountable for the treatment’s success.
Under the agreement, participating states will receive “discounts and rebates” from the drugmakers if the treatments don’t work as promised, according to the Centers for Medicare & Medicaid Services.
That’s a stark difference from how Medicaid and other health plans typically pay for drugs and therapies ‚Äî the bill usually gets paid regardless of the treatments’ benefits for patients. But CMS has not disclosed the full terms of the contract, including how much the drug companies will repay if the therapy doesn’t work.
The treatment Cole received offers a potential cure for many of the 100,000 primarily Black Americans with sickle cell disease, which is estimated to shorten lifespans by more than two decades. But the treatment’s cost presents a steep financial challenge for Medicaid, the joint state-federal government insurer for people with low incomes or disabilities. Medicaid covers roughly half of Americans with the condition.
There are two gene therapies approved by the Food and Drug Administration on the market, one costing $2.2 million per patient and the other $3.1 million, with neither cost including the expense of the long hospital stay.
The CMS program is one of the rare health initiatives started under President Joe Biden and continued during the Trump administration. The Biden administration with the two manufacturers, Vertex Pharmaceuticals and Bluebird Bio, in December 2024, opening the door for states to join voluntarily.
“This model is a game changer,” Mehmet Oz, the CMS administrator, said announcing that 33 states, Washington, D.C., and Puerto Rico had signed onto the initiative.
Asked for further details on the contracts, Catherine Howden, a CMS spokesperson, said in a statement that the terms of the agreements are “confidential and have only been disclosed to state Medicaid agencies.”
“Tackling the high cost of drugs in the United States is a priority of the current administration,” the statement said.
Citing confidentiality, two state Medicaid directors and the two manufacturers declined to reveal the financial terms of agreements.


New Therapies
The gene therapies, approved for people 12 or older with sickle cell disease, offer a chance to live without pain and complications, which can include strokes and organ damage, and avoid hospitalizations, emergency room visits, and other costly care. The Biden administration estimated that sickle cell care already costs the health system almost $3 billion a year.
With many more expensive gene therapies on the horizon, the cost of the sickle cell therapies presages financial challenges for Medicaid. Hundreds of cell and gene therapies are in clinical trials, and dozens could get federal approval in the next few years.
If the sickle cell payment model works, it will probably lead to similar arrangements for other pricey therapies, particularly for those that treat rare diseases, said Sarah Emond, president and CEO of the Institute for Clinical and Economic Review, an independent research institute that evaluates new medical treatments. “This is a worthy experiment,” she said.
Setting up payment for drugs based on outcomes makes sense when dealing with high treatment costs and uncertainty about their long-term benefits, Emond said.
“The juice has to be worth the squeeze,” she said.
Clinical trials for the gene therapies included fewer than 100 patients and followed them for only two years, leaving some state Medicaid officials eager for reassurance they were getting a good deal.
“What we care about is whether services actually improve health,” said Djinge Lindsay, chief medical officer for the Maryland Department of Health, which runs the state’s Medicaid program. Maryland is expected to begin accepting patients for the new sickle cell program this month.
Medicaid is already required to cover almost all FDA-approved drugs and therapies, but states have leeway to limit access by restricting which patients are eligible, setting up a lengthy prior authorization process, or requiring enrollees to first undergo other treatments.
While the gene therapy treatments are limited to certain hospitals around the country, state Medicaid officials say the federal model means more enrollees will have access to the therapies without other restrictions.
The manufacturers also pay for fertility preservation such as freezing reproductive cells, which could be damaged by chemotherapy during the treatment. Typically, Medicaid doesn’t cover that cost, said Margaret Scott, a principal with the consulting firm Avalere Health.
Emond said pharmaceutical companies were interested in the federal deal because it could lead to quicker acceptance of the therapy by Medicaid, compared with signing individual contracts with each state.
States are attracted to the federal program because it offers help monitoring patients in addition to negotiating the cost, she said. Despite some secrecy around the new model, Emond said she expects a federally funded evaluation will track the number of patients in the program and their results, allowing states to seek rebates if the treatment is not working.
The program could run for as long as 11 years, according to CMS.
“This therapy can benefit many sickle cell patients,” said Edward Donnell Ivy, chief medical officer for the Sickle Cell Disease Association of America.
He said the federal model will help more patients access the treatment, though he noted utilization will depend in part on the limited number of hospitals that offer the multimonth therapy.
Hope for Sickle Cell Patients
Before gene therapy, the only potential cure for sickle cell patients was a bone marrow transplant ‚Äî an option available only to those who could find a suitable donor, about 25% of patients, Ivy said. For others, lifelong management includes medications to reduce the disease’s effects and manage pain, as well as blood transfusions.
About 30 of Missouri’s 1,000 Medicaid enrollees with sickle cell disease will get the therapy in the first three years, said Josh Moore, director of the state’s Medicaid program. So far, fewer than 10 enrollees have received it since the state began offering it in 2025, he said.
Less than a year into the federal program, Moore said it’s too early to tell its rate of success ‚Äî defined as an absence of painful episodes that lead to a hospital visit. But he hopes it will be close to the 90% rate seen over the course of a couple of years in clinical trials.
Moore said the federal program based on how well the treatment works was preferred over cutting fees for a new and promising therapy, which would put the manufacturers’ ability to develop new drugs at risk. “We want to be good stewards of taxpayer dollars,” he said.
He declined to comment on how much the state may save from the arrangement or disclose other details, such as how much the drug companies might have to pay back, citing confidentiality of the contracts.
Lately Cole, who underwent gene therapy at St. Louis Children’s Hospital, has been able to focus on her hobbies ‚Äî playing video games, drawing, and painting ‚Äì and earning her high school diploma.
She said she was glad to get the treatment. The worst part was the chemotherapy, she said, which left her unable to talk or eat — and entailed getting stuck with needles.
She said that her condition is “way better” and that she has had no pain episodes leading to a hospital stay since completing the therapy last spring. “I’m just grateful I was able to get it.”

This <a target="_blank" href="/medicaid/sickle-cell-disease-gene-therapy-medicaid-vertex-bluebird-bio/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2141959&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Humphreys, 68, feels betrayed by the Federal Employees Health Benefits Program. “As federal employees, we sacrificed good salaries in the private sector because we thought the benefits from government would be better now, in retirement,” he said.
As the nation’s largest employer-sponsored health insurance program, the covers more than 8.2 million federal government employees and retirees, and it was once celebrated as a national model for controlling costs while giving enrollees many health plan options.
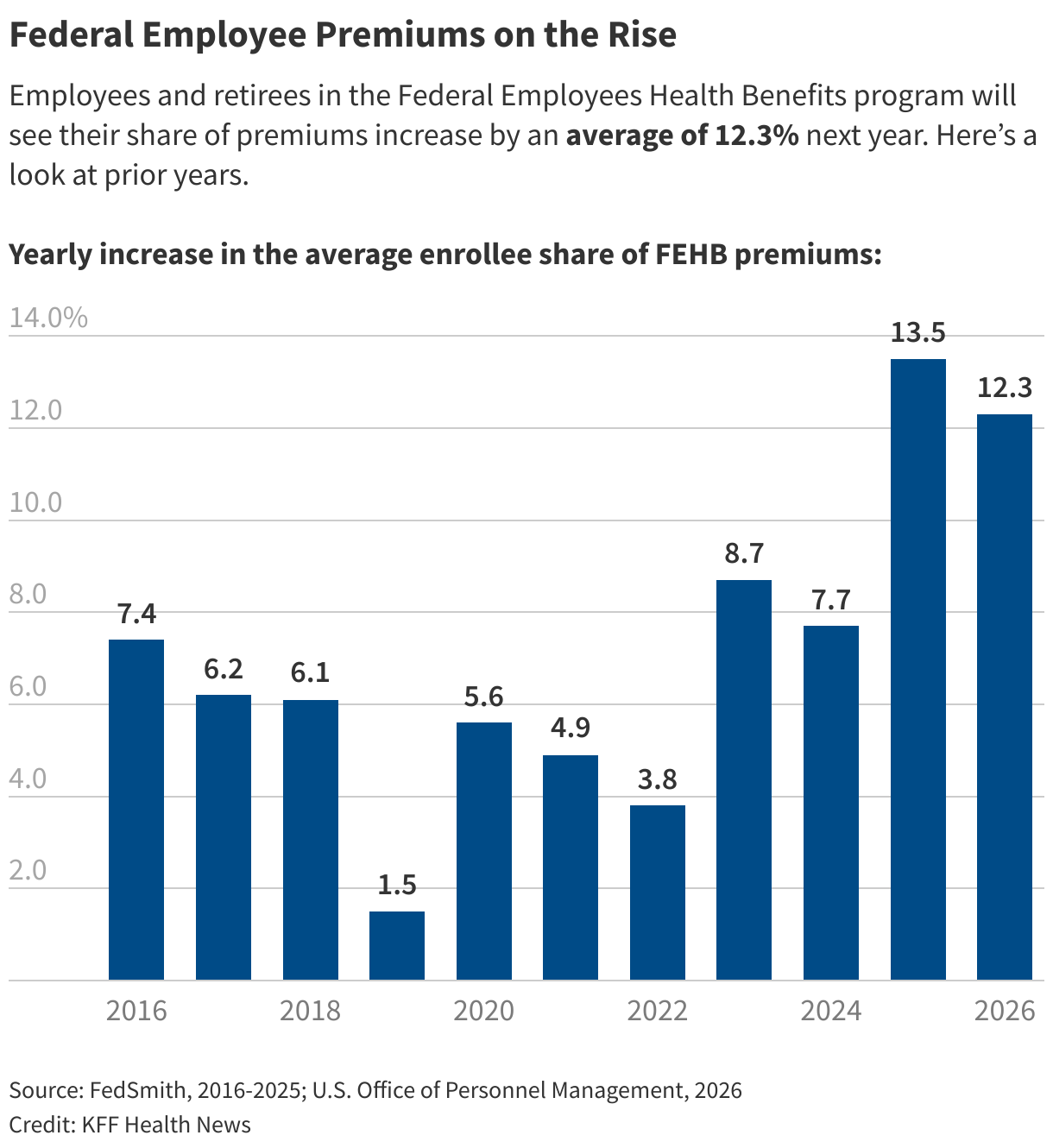
But next year, average enrollee premium payments in the system are set to jump more than 12%, on top of a 13.5% hike in 2025. The two-year increase is higher than what many private employers and their workers are experiencing.
The FEHB rate hikes are similar to those for plans sold on the Affordable Care Act exchanges — excluding the government subsidies most enrollees get, a major point of contention on Capitol Hill. The premiums insurers charge for Obamacare plans are rising 26% on average for 2026, following a 4% increase this year.
What’s making the latest hike in FEHB premium payments even harder to stomach for millions of federal employees is its timing: The 2026 increase was announced in October, when many federal workers were on unpaid furlough during the 43-day government shutdown.
Unlike most private employers, the FEHB Program gives its enrollees numerous health plans to choose from. That allows some people to lower their monthly premium payments by switching to plans with higher deductibles or copayments. But each year of enrollees switch plans, according to the Office of Personnel Management, which oversees the program.
Humphreys, who has stayed with the same health plan for decades despite steadily higher prices, said it’s difficult determining which plan is best based on their health conditions. He has glaucoma and diabetes, and his wife, Julianne, has faced heart issues.
Their FEHB plan covers costs for their care not covered by Medicare, which typically pays 80% of their health bills.
“There’s a fear that if you do something and change plans and it’s wrong, you could be in a bad spot,” he said.
Open enrollment for federal employees and retirees runs through Dec. 8.
Among the factors causing premiums to increase, according to OPM, are an aging federal workforce with more chronic conditions, as well as prescription drug use, including pricey GLP-1 medications for weight loss.
About 42% of federal employees are over the age of 50, compared with 33% in the general workforce, OPM says. About 7% of federal employees are under the age of 30, compared with about 20% of workers overall.
OPM officials said the Trump administration’s policies aimed at lowering drug costs and focused on prevention of costly medical conditions will hopefully help it control premiums in the future.
“None of these initiatives of course will happen overnight – turning a $79 billion ship takes slow and steady progress,” Shane Stevens, OPM’s associate director for health care and insurance, . “But, we are committed to improving the quality of life and quality of care for our members while also ensuring that healthcare remains accessible and affordable for those who work (or have worked) for the American people.”
OPM didn’t respond to requests for comment.
John Holahan, a health policy fellow at the nonpartisan Urban Institute, said OPM’s explanation left out a key reason for rising premiums: hospital consolidation. While the FEHB Program is a collection of health plans, in many markets — including the Washington, D.C., area — those insurers must negotiate with a handful of powerful health systems that have bought up other hospitals and doctors. That market power enables them to drive prices higher on FEHB plans, he said.
Jacqueline D. Bowens, president and CEO of the D.C. Hospital Association, said in a statement that “the costs borne by patients are not determined solely by the care they receive, but by how insurance companies choose to price, reimburse, and restrict access to that care.”
Holahan said it’s surprising that FEHB premiums are rising even faster than those of other, smaller employers. But he is not surprised federal employees don’t switch plans more often, even when it may be in their financial interest.
“It’s that people find the health care world so complicated,” he said. Holahan, a noted health economist, said he, too, finds it daunting to switch Medicare health plans.
Mike Lindquist, a scientific review officer for the National Institutes of Health, said he’s not happy with the rise in his premium payments the past two years. “It’s tough, as it’s a big expense.”
Lindquist, 43, who lives in Brunswick, Maryland, has been on the same Blue Cross and Blue Shield plan through the FEHB Program the past few years even though he evaluates his options each fall.
“By not switching, you don’t have to worry about choosing a new plan that might not take your practitioners,” he said.
Jonathan Foley, a health consultant who worked as a senior adviser at OPM during the Biden administration, said premium increases will be a hardship for many enrollees. While the FEHB Program offers 200 health plans in total, with about 10 to 20 in each geographic market, enrollment is concentrated in just a handful of Blue Cross and Blue Shield plans.
“This concentration reduces competition and gives outsize influence” to rate increases by Blue Cross and Blue Shield, Foley said in an email.
He said the FEHB Program also faces higher costs because it requires its health plans to cover GLP-1 medications, such as Wegovy and Ozempic. Nationally, fewer than half of large employers offer this benefit, according to . KFF is a health information nonprofit that includes ∫⁄¡œ≥‘πœÕ¯ News.
Another cost pressure has been more members using behavioral health benefits to treat depression and anxiety since the start of the covid pandemic, Foley said.
The Trump administration’s federal workforce reductions also have contributed to cost increases, Foley said. OPM has lost about a third of its employees in the past year, leaving fewer workers to oversee the FEHB Program and negotiate with dozens of health insurers, he said.
“The workforce reductions and the unpredictable nature of policymaking in the Trump administration has created considerable uncertainty among health insurance carriers,” Foley said. “The response of actuaries to increased uncertainty is to raise rates.”
A this year found that recent OPM staffing vacancies led to a suspension of fraud risk assessments in the FEHB Program.
John Hatton, staff vice president for policy and programs at an advocacy group called the National Active and Retired Federal Employees Association, said higher prices mean it’s critical for FEHB members to shop and compare plans for next year. “The program was designed to promote competition to mitigate and drive down costs,” he said.
Hatton said OPM surveys show the main reasons people don’t change plans is they are overwhelmed by their options and worried about making a mistake. Switching to a plan with even a slightly higher deductible, he said, could save people a few hundred dollars a month on premiums.
But Humphreys, the Georgia retiree, said he likes that his current plan comes with low out-of-pocket costs for him and his wife. They owed little money when his wife suffered a kidney stone infection and sepsis, which put her in the hospital for 12 days.
That reassurance will soon come at a higher cost: Their FEHB and Medicare premiums will take up more than half of his pension check next year after accounting for taxes.
“I can take a lower-premium plan, but it’s a gamble I am not willing to take,” he said.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/news/federal-worker-health-insurance-fehb-premiums-increases/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2123855&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Advocates say the push burdens states with duplicative verification checks and could lead people to lose coverage just for missing paperwork deadlines. But the administrator of the Centers for Medicare & Medicaid Services, Mehmet Oz, said in a post on the social platform X on Oct. 31 that more than $1 billion “of federal taxpayer dollars were being spent on funding Medicaid for illegal immigrants” in five states and Washington, D.C.
Medicaid’s overall spending topped $900 billion in fiscal year 2024.
It wasn’t clear from Oz’s statement or an accompanying video over what period the spending happened, and CMS spokespeople did not immediately respond to questions, either for an earlier version of this article or after Oz’s statement was posted.
Only U.S. citizens and some lawfully present immigrants are eligible for Medicaid, which covers low-income and disabled people, and the closely related Children’s Health Insurance Program. Those without legal status are ineligible for federally funded health coverage, including Medicaid, Medicare, and plans through the Affordable Care Act marketplaces.
Several states disputed Oz’s comments.
“Our payments for coverage of undocumented individuals are in accordance with state and federal laws,” said Marc Williams, a spokesperson for Colorado’s Department of Health Care Policy & Financing, which administers the state’s Medicaid program. “The $1.5 million number referenced by federal leaders today is based on an incorrect preliminary finding, and has been refuted with supporting data by our Department experts.”
He added: “It is disappointing that the administration is announcing this number as final when it is clearly overstated and the conversations are very much in the education and discussion phase.”
Illinois Medicaid officials blasted Oz’s comments.
“Once again, the Trump administration is spreading misinformation about standard uses of Medicaid dollars,” said Illinois Medicaid spokesperson Melissa Kula. “This is not a reality show, and there is no conspiracy to circumvent federal law and provide ineligible individuals with Medicaid coverage. Dr. Oz should stop pushing conspiracy theories and focus on improving health care for the American people.”
The Washington State Health Care Authority, which runs the state’s Medicaid program, was also blunt.
“The numbers Dr. Oz posted on social media today are inaccurate,” said spokesperson Rachelle Alongi. “We were very surprised to see Dr. Oz’s post, especially considering we continue to work with CMS in good faith to answer their questions and clear up any confusion.”
In August, CMS began sending states the names of people enrolled in Medicaid that the agency suspected might not be eligible, demanding state Medicaid agencies check their immigration status.
∫⁄¡œ≥‘πœÕ¯ News in October reached out to Medicaid agencies in 10 states. Five provided the approximate number of names they had received from the Trump administration, with expectations of more to come: Colorado had been given about 45,000 names, Ohio 61,000, Pennsylvania 34,000, Texas 28,000, and Utah 8,000. More than 70 million people are enrolled in Medicaid.
Most of those states declined to comment further. Medicaid agencies in California, Florida, Georgia, New York, and South Carolina refused to say how many names they were ordered to review or did not respond.
Oz said in his X post that California had misspent $1.3 billion on care for people not eligible for Medicaid, while Illinois spent $30 million, Oregon $5.4 million, Washington state $2.4 million, Washington, D.C., $2.1 million, and Colorado $1.5 million.
“We notified the states, and many have begun refunding the money,” he said. “But what if we had never asked?”
Washington, D.C.’s Medicaid director, Melisa Byrd, said CMS had identified administrative expenses for the district program that covers people regardless of immigration status that should not have been billed to the federal government and her agency has already fixed some of those areas. “We run a big program that is very complex and when mistakes or errors happen, we fix them,” she said.
The program plans to pay $654,014 back to CMS by mid-November.
All five states, plus Washington, D.C., are led by Democrats, and President Donald Trump didn’t win any of them in the 2024 election.
In recent days, Deputy Health and Human Services Secretary Jim O’Neill on X of people he said are convicted criminals living in the U.S. without authorization who had received Medicaid benefits.
O’Neill could not be reached for comment.
“We are very concerned because this seems, frankly, to be a waste of state resources and furthers the administration’s anti-immigrant agenda,” said Ben D’Avanzo, senior health advocacy strategist with the National Immigration Law Center, an advocacy group. “This duplicates what states already do,” he said.
As part of the administration’s crackdown on people in the U.S. without authorization, President Donald Trump in February directed federal agencies to take action to ensure they are not obtaining benefits in violation of federal law.
In June, advisers to Health and Human Services Secretary Robert F. Kennedy Jr. ordered CMS to share information about Medicaid enrollees with the Department of Homeland Security, drawing a lawsuit by some states alarmed that the administration would use the information for its deportation campaign against unauthorized residents.
In August, a federal judge ordered HHS to with immigration authorities.
State Medicaid agencies use databases maintained by the Social Security Administration and Department of Homeland Security to verify enrollees’ immigration status.
If states need to go back to individuals to reverify their citizenship or immigration status, it could lead some to fall off the rolls unnecessarily ‚Äî for example, if they don’t see a letter requesting paperwork or fail to meet a deadline to respond.
“I am not sure that evidence suggests there really is a need for this” extra verification, said Marian Jarlenski, a health policy professor at the University of Pittsburgh School of Public Health.
Oz made clear that the Trump administration disagrees.
“Whether willful or not, the states’ conduct highlights a terrifying reality: American taxpayers have been footing the bill for illegal immigrants’ Medicaid coverage, despite many Democrats and the media insisting otherwise,” Oz said in his X post.
In an August press release, CMS said it would ask states to verify eligibility for enrollees whose immigration status could not be confirmed via federal databases. “We expect states to take quick action and will monitor progress on a monthly basis,” the agency said.
Leonardo Cuello, a research professor at Georgetown University’s Center for Children and Families, called the CMS order to states “unprecedented” in the Medicaid program’s 60-year history.
He said the federal government may have been unable to verify certain individuals’ immigration status because names were misspelled or outdated, such as when a beneficiary is identified by their maiden instead of married name. The names may also include people helped by Emergency Medicaid, a program that covers the cost of hospital emergency services, including labor and delivery, for people regardless of immigration status.
“CMS is conducting pointless immigration status reviews for people whose hospital bills were paid by Emergency Medicaid,” Cuello said.
Oz noted in his post that federal law “does permit states to use Medicaid dollars for emergency treatment, regardless of patients’ citizenship or immigration status,” and that states can “legally build Medicaid programs for illegal immigrants using their own state tax dollars, so long as no federal tax dollars are used.”
The states Oz mentioned all such programs.
The verification checks create an added burden for state Medicaid agencies that are already busy preparing to implement the tax and policy law Trump signed in July. The measure, which Republicans call the One Big Beautiful Bill Act, makes many changes to Medicaid, including adding a work requirement in most states starting by 2027. The law also requires most states to more frequently check the eligibility of many adult Medicaid enrollees — at least twice a year.
“I fear states may do unnecessary checks that create a burden for some enrollees who will lose health coverage who should not,” Cuello said. “It’s going to be a whole lot of work for CMS and states for very little pay dirt.”
Cuello said the effort may have “greater political value than actual value.”
Brandon Cwalina, a spokesperson for the Pennsylvania Department of Human Services, which runs Medicaid in the state, said the state already requires every Medicaid applicant to verify their citizenship or, where applicable, their eligible immigration status.
However, he said, the directive issued by CMS “constitutes a new process, and DHS is carefully reviewing the list in order to take appropriate actions.”
Oz did not name Pennsylvania, which Trump won in 2024, in his post.
If a lawful resident does not have a Social Security number, the state confirms their legal status by checking a database from Homeland Security, as well as verifying specific immigration documents, he said.
Other state Medicaid agencies said they also needed to regroup before reaching out to enrollees.
“Our teams just received this notice and are working through a process by which we will perform these reviews,” Jennifer Strohecker, then Utah’s Medicaid director, told a state advisory board in August.
Renuka Rayasam and Rae Ellen Bichell contributed reporting.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/trump-hhs-medicaid-eligibility-reviews-states-cms-immigrants/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2106888&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Premiums for job-based health insurance rose 6% in 2025 to an average of $26,993 a year for family coverage, according to an annual survey of employers released Oct. 22 by KFF, a health information nonprofit that includes ∫⁄¡œ≥‘πœÕ¯ News.
It’s the first time in two decades that the cost of covering a family of four has risen by 6% or more for three consecutive years, data from KFF shows.
Over the last five years, the average premium for family coverage has increased by 26%, compared with a 29% increase in workers’ wages and nearly 24% growth in inflation. The average cost for family coverage is now about the same as
The average annual premium for an individual health plan provided by employers increased by 5% to $9,325 — nearly $3,000 higher than in 2016, according to the survey.
“It’s a concern as health costs just keep going up,” said Eric Trump, controller at Steve Reiff Inc., a small company in South Whitley, Indiana, that specializes in sandblasting and painting heavy equipment.
Trump, who is not related to President Donald Trump, said his company’s health insurance costs rose 8% for the 2026 fiscal year ‚Äî roughly the same as they have in the last few years.
Workers at Reiff pay about half the cost of their health coverage. About half of its 20 current employees decline the insurance because they get coverage through a family member or choose to go uninsured, he said. “There’s not a lot we can do as we don’t have enough employees to spread out the costs.”
Most people with job-based insurance contribute to the cost of their premiums, with the average worker this year contributing $1,440 for individual coverage or $6,850 for family coverage.
Over time, more workers have paid increasingly higher deductibles, the amount they must spend out-of-pocket on medical services before their insurer pitches in. More than one‚Äëthird of covered workers are enrolled in a plan with a deductible of $2,000 or more for an individual. The share of workers with such a plan has increased 32% over the last five years and 77% over the last 10 years, the report said.
Rising drug and hospital costs as major culprits for rising health insurance costs, and neither shows signs of ebbing.
“Early reports suggest that cost trends will be higher for 2026, potentially leading to higher premium increases unless employers and plans find ways to offset higher costs through changes to benefits, cost sharing, or plan design,” the KFF survey said.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/workplace-health-insurance-premiums-family-plans-kff-survey/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2103836&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But in the past couple of years, she’s fallen from 600 pounds to 385, and her blood pressure and blood sugar levels are down, too. “I’m not as fatigued as I used to be, and I’ve been able to go back to church,” she said.
Hines, 46, credits her weight loss to Trulicity, part of a new class of expensive weight loss drugs known as GLP-1s, and her Medicaid coverage for it. “It’s a blessing,” she said.
In a state where the obesity rate ranks among the highest in the country, many health providers were thrilled when Mississippi Medicaid in 2023 began covering GLP-1s for people 12 and older. Only 13 states cover the drugs for Medicaid enrollees for obesity, and Mississippi’s Medicaid program typically has some of the sparsest benefits and strictest eligibility rules.
Hines is one of relatively few enrollees to have used the new Medicaid benefit, which weight loss doctors in the state say has been hindered by national drug shortages, the state’s prior authorization process for the drugs, and a lack of marketing. Just 2% of adults on Mississippi Medicaid who meet the weight-related criteria had been prescribed a GLP-1 as of December 2024, according to to the state’s Medicaid Drug Utilization Review Board.
“It’s a little sad to have so many people out there not benefiting,” said William Rosenblatt, a family doctor in Columbus who treats Hines. “These drugs get to the root cause of so many health conditions.”

Already-scarce Medicaid coverage of the highly touted weight loss drugs could become more limited, with federal Medicaid funding cuts expected in the wake of the massive tax-and-spending bill President Donald Trump signed into law in July. The Congressional Budget Office estimated that the law would reduce Medicaid spending by about $911 billion over a decade.
“The law is going to create fairly intense pressure on states not to expand benefits,” said Michael Kolber, a partner in the health consulting firm Manatt. That may be especially true for these drugs, which often cost around $1,000 a month and could be used by a large percentage of Medicaid recipients, he said.
GLP-1s, which to treat Type 2 diabetes, have gained widespread attention as a way to lose weight and reduce obesity-related conditions and their long-term costs.
But states may remain reluctant to offer the expensive drugs for obesity, because Medicaid recipients frequently churn on and off the coverage as their income changes. And because the drugs’ health benefits may take years to materialize ‚Äî such as averting a future heart attack ‚Äî the long-term financial advantages could accrue to other insurers.
Even ahead of the federal cuts, which will largely take effect in 2027, states are already feeling the pinch. North Carolina’s Medicaid program of the drugs this month, citing their high cost.
Coverage for the weight loss drugs presents a dilemma for the Trump administration, which has identified as priorities attacking chronic health conditions and reducing federal spending. Health and Human Services Secretary Robert F. Kennedy Jr. has for the drugs and said more emphasis should be placed on eating better and exercising more.
In 2024, the Biden administration proposed that Medicare and Medicaid cover weight loss drugs to help tackle obesity as a public health crisis. In April, the Trump administration revoked the Biden-era proposal, saying the programs would not cover GLP-1 drugs for weight loss.
But in August, the Trump administration was considering a five-year pilot program for Medicare and Medicaid to cover the drugs after all. No details have been released. Asked for comment on the report, Centers for Medicare & Medicaid Services spokesman Alexx Pons told ∫⁄¡œ≥‘πœÕ¯ News that all decisions go through a cost-benefit review.
Meanwhile, the Trump administration has included the GLP-1 drugs Ozempic, Wegovy, and Rybelsus on its list of 15 medicines that will be subject to price negotiations with pharmaceutical manufacturers under its Medicare Part D program, a system created during the Biden administration amid opposition from Republicans. The results of those negotiations are expected to be announced this fall.
Most private insurers don’t cover GLP-1s for weight loss, which can make the drugs unaffordable for those paying out of pocket.

to Mississippi’s Medicaid drug review board shows that, in the first 15 months the drugs were covered, only about 2,900 Medicaid enrollees age 12 or older started treatment. Nearly 90% of them were female, and many had high blood pressure and high cholesterol.
The analysis also found most enrollees using the drugs lived in the southern, central, or northern parts of Mississippi — not along the Mississippi Delta on the western side of the state, where obesity rates are highest, at nearly 50%.
About 40% of adults in Mississippi are obese, just one percentage point behind top-ranked West Virginia, according to federal data.
Mississippi Medicaid spokesman Matt Westerfield told ∫⁄¡œ≥‘πœÕ¯ News that the state spent $12 million in the first 15 months, providing the weight loss drugs to 2,200 adult members. He said the state approved the new drugs on the logic that treating obesity would improve enrollees’ health and eventually could lead to cost savings by reducing diseases caused by obesity.
Westerfield said that while utilization has been below the state’s projections, such treatment decisions are up to patients and their doctors. He said the state has been “raising awareness” of the drugs among health care providers, but he declined to comment further.
Rosenblatt, who works for Baptist Medical Group, part of a large regional health system, said some doctors have less incentive to prescribe the medicine, because the state doesn’t pay them to counsel patients about necessary dietary changes when taking the new drugs.
He called the drugs “game changers,” adding that he has seen patients lose 50 pounds or more within a few months of starting the drugs and no longer need medications for diabetes or other conditions.
A published in 2021 found participants receiving GLP-1 drugs were more likely to show significant, sustained weight loss compared with those getting a placebo.
Other recent studies have shown the drugs help people with obesity lower their and reduce their odds of .
Mississippi is one of 10 states that have not expanded Medicaid eligibility under the 2010 Affordable Care Act to everyone with an income under 138% of federal poverty level, or $21,597 this year.
In Mississippi, Medicaid does not cover adults without dependent children. Parents qualify only if their income is below 22% of the federal poverty level, or $5,863 for a family of three this year.
The state’s prior authorization process requires doctors to document to the state that patients meet certain obesity levels and that a treatment plan is in place. Doctors must demonstrate that enrollees are losing weight every six months to renew their prescription.
At the Hattiesburg Clinic ‚Äî a large, multi-specialty group with a location in Hattiesburg, Mississippi ‚Äî Virginia Crawford, a physician who specializes in obesity, said she was surprised so few patients are getting the drugs. A year ago, there were shortages of the drugs that could have curtailed physicians prescribing them. And she said the state’s prior authorization requirements for the drug could discourage primary care doctors. Many common medications do not require progress reports or even prior authorization.
“We need to make patients more aware that this option is available for them,” she said.
Lauren Scott, 40, of Laurel, Mississippi, said that with the help of Medicaid coverage, she lost nearly 100 pounds taking Wegovy.
“It’s just been amazing,” she said of how the drug drastically cut her appetite. “I remember going to Outback with my husband, and we got the onion ring appetizer and 16-ounce ribeye and salad with extra ranch dressing. I had some onion rings and started on the salad and realized I could not eat any more of this.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/mississippi-medicaid-glp-1s-weight-loss-drugs-obesity/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2101025&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>By January 2027, President Donald Trump’s far-reaching will require many adult, nondisabled Medicaid enrollees in 42 states and Washington, D.C., to work or volunteer 80 hours a month or go to school.
But under the law, Medicaid enrollees in counties where unemployment is at least 8% or 1.5 times the national unemployment rate could be shielded from the work requirement, if their state applies for an exemption.
A shows that exemption in the GOP’s could offer a reprieve to potentially millions of Americans caught in a tough spot ‚Äî needing to work to secure health insurance but having trouble finding a job.
The Congressional Budget Office projected the work requirement would apply to 18.5 million Medicaid enrollees, causing about 5.3 million to lose their government health coverage by 2034. CBO spokesperson Caitlin Emma confirmed to ∫⁄¡œ≥‘πœÕ¯ News that analysts factored the unemployment rate exemption into their projections. Only states that expanded Medicaid under the 2010 Affordable Care Act or a special waiver must enact a work requirement, under the federal law.
But how many people could be exempt depends on how the Trump administration interprets the law, in addition to whether their states’ officials apply.
For example, if Trump officials exempt people in counties where the unemployment rate has been above the law’s thresholds for any month over a 12-month period, about 4.6 million Medicaid enrollees in 386 counties could qualify for an exemption today based on the latest unemployment data, according to KFF, a health information nonprofit that includes ∫⁄¡œ≥‘πœÕ¯ News.
That amounts to just under a quarter of all Medicaid enrollees subject to the work requirement.
Under that one-month threshold, “the impact could be fairly significant,” said Jennifer Tolbert, a co-author of the analysis and the deputy director of KFF’s Program on Medicaid and the Uninsured.
But, she said, the Trump administration is more likely to adopt a stricter threshold based on average unemployment over a 12-month period. That would align with work requirements under the federal Supplemental Nutrition Assistance Program, the food assistance commonly known as food stamps.
Only about 1.4 million Medicaid enrollees living in 158 counties could be exempted under that standard, or about 7% of the total subject to work requirements, KFF found. That’s about 7% of enrollees who live in expansion states who would otherwise need to meet the new requirement.
Based on the 12-month criteria, about 90% of Medicaid enrollees who could be exempted based on high unemployment reside in five states, according to KFF: California, New York, Michigan, Kentucky, and Ohio. California alone accounts for over half of those who could be exempted.
The unemployment rate exemption is one of several carve-outs from the Medicaid work requirement in the GOP’s law. The law also exempts parents with children under 14, people who are disabled or frail, and those who are pregnant, incarcerated, or in a substance use disorder program, among others. The high unemployment provision is different than most because it exempts people living in entire counties.
Two top Republicans key to the bill’s passage ‚Äî House Speaker Mike Johnson and Sen. Mike Crapo, chair of the Senate Finance Committee ‚Äî did not respond to requests for comment.
To qualify for the Medicaid exemption, states would have to apply to the federal government on behalf of individuals in eligible counties. And if a county earned an exemption, the government would determine how long it applies.
Even if the federal government grants exemptions broadly, health advocates fear some Republican-led states could balk at applying for exemptions in order to keep enrollment down, as they say has been the case with SNAP exemptions. As of 2023, 18 states did not have an exemption under the SNAP program, even though some of their residents might be eligible.
“It’s not a guarantee that people can rely on,” said Emily Beauregard, executive director of Kentucky Voices for Health, an advocacy group that intends to push for the broadest possible exemptions to help people maintain their coverage. Eastern Kentucky has several counties with perennially high unemployment.
In advocating for Trump’s bill, that most people who gained Medicaid benefits under the Affordable Care Act should be working to get off of government assistance.
But as have shown, Medicaid work requirements can be costly for states to run and . About 18,000 people in Arkansas, or nearly a quarter of the state’s adults who gained Medicaid coverage through the ACA expansion, lost coverage when the state had a work requirement in 2018 and 2019. A court ended the state’s work requirement program.
Critics point out that or have a disability or caregiving responsibilities, and they argue the reporting requirements merely serve as a bureaucratic hurdle to obtaining and keeping coverage. Under the GOP law, enrollees’ work status needs to be verified at least twice a year.
Most of the coverage losses due to work requirements occur among people who work or should qualify for an exemption but nevertheless lose coverage due to red tape, .
Not every state must implement a work requirement under Trump’s law, only those that chose to expand Medicaid coverage to more low-income people through the ACA or a federal waiver. The ACA has provided hundreds of billions in federal dollars to help states cover everyone making up to 138% of the federal poverty level ‚Äî $21,597 for an individual in 2025.
Forty states and Washington, D.C., took up the expansion. Georgia and Wisconsin partly expanded their Medicaid eligibility by getting a federal waiver, adding them to the list of states subject to the work requirement. These two states were not included in the KFF analysis because of a lack of county-level enrollment data.
Jennifer Wagner, director of Medicaid eligibility and enrollment at the left-leaning Center on Budget and Policy Priorities, said she is pleased the law makes some exceptions for places where jobs are scarce. It could limit how many people lose coverage because of the work requirement, she said.
Wagner said SNAP’s unemployment rate exemption has helped millions of people avoid losing their food assistance, but its impact also depends on whether a state seeks the waiver.
She is concerned the Trump administration may make it difficult for counties to get exempted under the Medicaid law.
“I’m glad it’s in there as it will certainly help people, but it’s still a terrible bill,” she said. “This will not really blunt the harm of the bill.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/medicaid-work-requirement-exemption-unemployment-jobs-waiver-counties/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2094229&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>