Jillian Broomstein starts to cry when she talks about the day her newborn son Jeremy was taken from her by New Hampshire’s child welfare agency. He was 2 weeks old.
“They came into the house and said they would have to place him in foster care and I would get a call and we would set up visits,” she said. “It was scary.”
Broomstein, who was 26 at the time, had not used heroin for months and was on methadone treatment, trying to do what was safest for her child. The clinic social worker told her that since Jeremy would test positive for methadone when he was born, she would need to find safe housing or risk losing custody.
Broomstein moved in with a friend and her kids ã but it turned out that friend had her own legal battles with the state’s Division of Children, Youth and Families, known as DCYF. The friend’s home would not pass muster as “safe housing” because of that.
Since Broomstein grew up in foster care and had no family to take her in, Jeremy was taken from her. She had 12 months to try to get her son back or lose her parental rights permanently.
To get their children back from the foster care system in New Hampshire, parents struggling with addiction are required to be compliant in drug treatment and have a safe place to live. If they can’t find housing or if they relapse, the clock does not stop ticking.
“I cannot stress enough that 12 months is a really short window for somebody who’s in early recovery,” said Courtney Tanner, who runs Hope On Haven Hill, one of the few places in New Hampshire where pregnant women and new mothers can live with their children and get treated for addiction. But with just eight beds here, the waitlists can be long.
There are more than 430,000 children in foster care in the U.S., according to the . The opioid crisis is definitely a factor in an increasing trend of more children being removed from the home, but the scope of the problem is .
New Hampshire has some of the highest rates of opioid abuse in the country. One of the fastest-growing groups of heroin users is women of childbearing age. In the past few years the number of children taken into state custody has more than doubled, according to DCYF. Last year, New Hampshire spent $36 million for foster care.
“Here in New Hampshire, what I have seen is a mom can be enrolled in this program and compliant in treatment and they are giving birth to a child and that child is still being removed and put into foster care,” said Tanner.
In 2012 state legislators made major budget cuts to DCYF ã and those dollars have not been restored. Child welfare workers in New Hampshire have more than triple the caseloads than in many other states, according to the agency’s director Joseph Ripsam. Also as a result of the budget cuts, DCYF can only engage a family once case workers have opened a legal case of abuse and neglect. There’s little money to support parents before that happens.
“The result of that is … that more children coming into the foster care system that otherwise might not if we had the capacity to serve families more holistically up front,” said Ripsam.
After her son Jeremy was placed into foster care, Jillian Broomstein continued her methadone treatment and her parenting classes.
She was determined to get her son back. She finally got off a waiting list and got a bed at one of the residential treatment centers for young mothers. After a few months she was reunited with Jeremy. But she was told that her case was unusual.
“They said in court that it was an odd case that they gave me my child back so quickly,” Broomstein said. “It made me want to cry.”
“I knew it was going to be hard,” she said. “Not everybody tries to get their children back. A lot of people I’ve known just give up; they just resort back to drugs again.”
This story is part of a reporting partnership that includes and Kaiser Health News.
¤Öêü°å¿üë½ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFãan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/mental-health/in-new-hampshire-even-mothers-in-treatment-for-opioids-struggle-to-keep-children/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=847890&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>For years, Eileen Shea says her former partner Eddie Sawyer struggled with a heroin addiction. But after losing his job and time with his daughter, he was ready to get help. He was on the waiting list for a bed at the Friendship House, northern New Hampshire’s only residential treatment facility.
He never made it to treatment. Instead, Sawyer was one of 428 people in New Hampshire who died last year from a drug overdose. When the police found him in his apartment, there was list of rehab facilities on the table next to his bed. It was a list Shea had given to him a month earlier, and there were check marks next to the name of each one. Sawyer had called every place on the list.
New Hampshire has the second-lowest level of access to substance abuse treatment in the U.S., right above Texas, according to the Substance Abuse and Mental Health Services Administration (SAMHSA). At the same time, New Hampshire isô ô with the highest rateô of drug overdose deaths per capita.
“It’s typically four to six weeks that they’re on [the] waiting list,” said Kristy Letendre, director of the Friendship House in Bethlehem, New Hampshire. The facility has 18 beds and transitional housing where people recovering from addiction can live after they finish a 28-day program. “A lot of our admissions come from Manchester and Nashua, which is the southern part of the state, because they have six-month waitlists to get into their programs, so they’re coming up north.”

But waiting for treatment doesn’t work for a lot of people addicted to heroin and other opioid drugs such as fentanyl and OxyContin. There’s a small window of time, Letendre says, when people are ready for help. If they don’t get help in that window, the risk of relapse and overdose is very high because withdrawal sickness is so miserable it drives people to use again.
“Lately we’ve lost people who have reached out and were at the beginnings stages of accessing a bed and then you get a call or hear on the news that that person overdosed and their chance is gone,” Letendre said.
Nobody knows this better than Sean Warren.
“In 2015, I had seven friends die of heroin addiction,” said Warren, 23, who had been struggling with heroin for more than two years. He wanted to get off the drug, but he says he couldn’t do it on his own. When he called around to find a rehab bed, he was told it would be nine weeks before he could get one.

“I needed to be in a safe place,” Warren said. “I called everywhere crying and begging to get in, and no one had room for me, so my addiction led me to do more crime.”
Warren ended up stealing his sister’s credit cards to get money to buy drugs. And that’s when Warren said he got lucky — he was arrested. With no access to heroin, Warren went through withdrawal sickness alone in his cell. From jail he was admitted to the Friendship House.
“You have to survive for X amount of time,” Warren said. “If I stayed out there for nine weeks, I can guarantee you I wouldn’t be alive right now.”
Most rehab programs in New Hampshire will not take people unless they are free from drugs for at least three days.ô But finding a place to detox safely is not easy — there are only a handful in the state. There’s also a who can prescribe medications to help people detox at home. (President Obama proposed on Monday.)
Many of the people trying to detox on their own show up at Littleton Regional Healthcare, a 25-bed hospital not far from the Friendship house.
Dr. Randy Knight, an emergency room physician, says every shift he works he sees two to three patients struggling with a drug addiction. Sometimes these are people who have overdosed and are dumped unconscious at the hospital entrance.

“It’s worse than it’s ever been,” Knight said. “We’re burying way too many young people from this disease, and we risk losing an entire generation from New Hampshire because we haven’t committed the necessary human resources, hospital beds or treatments beds to help patients kick this habit.”
Knight says when people show up at the emergency room desperate to detox from opioids there is very little he can do for them. It is different from detoxing from severe alcohol abuse, where people can be admitted to the hospital because they can have life-threatening seizures.
Coming off heroin and other opioids is often a brutal experience — which can include hallucinations, vomiting, chills and diarrhea — but it is not considered a medical emergency.
“When I meet a patient and their family requesting help getting off of heroin or opiates, I have to tell them a hospital is not going to be able to provide the services that they need because the patient is not unstable from a medical point of view,” Knight said. “That doesn’t mean they’re not going to use again. And they tell me that, ãIf you send me out there, I’m going to use again.’ But I just can’t offer them a hospital bed in that situation.”
Knight usually gives these patients a blood pressure drug that may ease some of their withdrawal symptoms — but then he can only refer them to rehab — and hope that they don’t have to wait too long for a bed.

Eileen Shea will mark the first anniversary of Eddie Sawyer’s death April 7. She replays what could have been done differently for her daughter’s father.
Shea offered to take Sawyer to a nearby hospital to help him detox. But she knew there were no guarantees he would be admitted.
“I told him when we go to the hospital, you’re either gonna have to drink a bunch of booze and they’ll admit you that way because they take alcoholics, or we’re going to go in there and you’re going to have to say you’re suicidal,” she said. “That was the only thing I could think of to help him, because they would not let him in because he was just a drug addict.”
But they never made it to the hospital.
“I wish I could have said, ãEddie I’m gonna come pick you up. We’re going to go to the hospital. They’re going to admit you. They’re going take care of you,’” Shea said. “But that’s not what happened. Eddie did not want to continue to do drugs, he just could not stop and he reached out for people to help him stop, and nobody took him.”
This year New Hampshire has doubled its funding for substance abuse treatment, and has made 43,000 residents eligible for treatment under expanded Medicaid.
This story is a collaboration between Kaiser Health News and .
¤Öêü°å¿üë½ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFãan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/mental-health/the-wait-for-opioid-treatment-can-mean-life-or-death-in-new-hampshire/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=610926&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
Those with severe pain were more likely to have worse health status, use more health care and suffer from more disability than those with less severe pain.
“There are so many people in the severe pain category that something has to be done,” said Richard Nahin, the lead author of the analysis and lead epidemiologist for the National Center for Complementary and Integrative Health, the arm of the NIH that funded the study. “If people are in the most severe category of pain, whatever treatment they are getting may be inadequate.”
Published in The Journal of Pain earlier this month, the of 2012 data from the National Health Interview Survey. It follows a comprehensive 2011 Institute of Medicine .
The analysis examined pain differences among ethnic groups. For example, Hispanics and Asians are less likely to report pain.
“If you are dealing with a minority group that doesn’t speak English, you need to pay greater attention to eliciting what they mean when they say they have mild pain or severe pain,” Nahin said.
The authors of the analysis hope their work will help inform greater research and better treatment options for people in pain.
“We’re doing a lot of research on the mechanism of pain and potential medications. The problem is there is no silver bullet,” said David Shurtleff, deputy director of NCCIH. “These data are giving us a better understanding of the pain conditions in the United States. We now can understand how sub-populations across age and across ethnic groups are experiencing pain.”

Shurtleff said that pain is a challenge to treat because it is not just about what happens to a person physically. Emotional and cognitive factors come into play as well. “Our major focus is on symptom management for pain,” he said. “It’s not necessarily [one] medication or behavioral intervention. It’s likely to be an integrative approach using multiple strategies to help patients alleviate their pain.”
Paul Gileno, who has had chronic pain since he broke his back 12 years ago, is doing just that. Gileno, who founded the advocacy group, uses acupuncture, meditation and changes to his diet to manage his pain. He is now able to take fewer painkillers, he said.
“You need to keep trying these different modalities because you never want to give up hoping that your pain can be reduced or go away,” he says.
Gileno endured multiple surgeries and has tried many different pain medicines, but he still lives with pain every day.
“After I saw the last neurologist and the last doctor and they said, ãListen we’ve done everything we can do and I don’t think your pain is going to go away,’ I had to come to terms that I would have chronic pain for the rest of my life,” said Gileno. “Pain comes with a lot of baggage. It comes with depression. It comes with feeling judged and you feel less of a person. You become very isolated.”
Untreated pain is something Dr. Sean Morrison sees in many of his patients. He is a geriatrician and director of Palliative Care at Mount Sinai Hospital in New York.
“Pain causes a tremendous amount of suffering,” said Morrison. “It has huge economic costs, because of people who cannot work ãÎ And it has a significant impact on caregivers who are caring for people who have pain.”
As more effective treatments are developed for a greater number of diseases, a growing number of people will suffer from pain as a side-effect, he said.
“Many of the cancer drugs we use now result in permanent nerve injury and resulting neuropathic pain which is very difficult to treat,” he said.
Another of Morrison’s frustrations is the growing level of scrutiny physicians and pharmacists are under as they treat pain. The law enforcement crackdown on prescription drug abuse appears to be to get the medicines they need.
“What’s happening is that the same drug is being used appropriately by group of patients and inappropriately in a large segment of the population,” Morrison said. “What we’ve seen is people in pain are the unintended victims of the war of drugs.”
NIH is in the process of finalizing a to coordinate efforts among different agencies to prevent, treat, manage and study pain.
¤Öêü°å¿üë½ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFãan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/pain-by-the-numbers/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=563022&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The accident happened 10 years ago when Chris Young was 35. He owned a salvage yard in Maui, Hawaii, and his employee had hoisted a junker on a machine called an excavator when the hydraulics gave out. The car fell on him from above his head, smashing his spine.
“He was crushed accordion-style,” says his wife Lesley.
The accident left Young with a condition known as “partial paraplegia.” He can’t walk and he needs a wheelchair, but he does have some sensation in his legs. Unfortunately for Young, that sensation is often excruciating pain.

“It feels like electric shocks, like lightning bolts going down my legs. And when it gets down to the bottom, it feels like someone is driving a big metal spike up my legs,” says Young.
To control the pain, Young, who has since moved to Florida, needs high doses of narcotic painkillers, but he can’t always fill his doctor’s prescription. He is not alone. In what may be an unintended side effect of a crackdown on prescription drug abuse, Young and other legitimate chronic pain patients are having increasing trouble getting the medicine that allows them to function on a daily basis.
Young’s pharmacy runs out every month.
“They just do not have the medications because they have run out of their allocation within the first week,” he says. “It’s just that bad, where I know I am going to end up in the E.R. because of not having my medications. We don’t know what to do. We’ve tried everything.”
Young’s pharmacist is Bill Napier, who owns the small, independent Panama Pharmacy in Jacksonville. Napier says he can’t serve customers who legitimately need painkillers because the wholesalers who supply his store will no longer distribute the amount of medications he needs.
“I turn away sometimes 20 people a day,” says Napier.
Last year Napier says federal Drug Enforcement Administration agents visited him to discuss the narcotics he dispensed.
“They showed me a number, and they said that if I wasn’t closer to the state average, they would come back. So I got pretty close to the state average,” Napier says. He says he made the adjustment “based on no science, but knowing where the number needed to be. We had to dismiss some patients in order to get to that number.”
According to Napier, DEA agents took all of his opioid prescriptions and held on to them for seven months. Napier hired a lawyer and paid for criminal background checks on his patients taking narcotics to help him decide which ones to drop.
“We’re being asked to act as quasi-law enforcement people to ration medications,” says Napier. “I have not had training in the rationing of medications.”
Until a few years ago, Florida was for the trafficking of illegal prescription narcotics. The DEA and local law enforcement shut down more than 250 so-called “pill mills” ô — clinics where doctors could sell narcotics directly to people for cash. Now Florida doctors can no longer dispense narcotics directly to patients. Wholesalers, who to claims for suspicious orders of drugs, now limit the amount they sell to pharmacies, Napier says.

Jack Riley, who is acting deputy administrator of the DEA, credits a in Florida with an upsurge in law enforcement activity. The problem of addiction and the drug trade is dire, he says.
“A hundred and twenty people a day die of drug abuse in this country,” Riley said. “If that doesn’t get your attention, I don’t think anything can.”
Riley also says cannot be blamed for any claim of rationing of painkillers.
“I’m not a doctor. We do not practice medicine. We’re not pharmacists. We obviously don’t get involved in that,” said Riley. “What we do do is make sure the people that have the licenses are as educated as possible as to what we’re seeing, and that they can make informed decisions as they do dispense.”
Doctors, too, say DEA enforcement actions have made it harder for them to prescribe narcotics. Last year, hydrocodone products, such as Vicodin, to , meaning they have a high potential for abuse and cannot be prescribed in large quantities.
“What we’ve seen is dramatic reductions in our ability to provide appropriate care for our patients in pain,” says Dr. R. Sean Morrison, director of the palliative care program at Mount Sinai Hospital in New York.
Morrison’s patient Ora Chaikin has been taking high levels of narcotics for years to control her pain. She has had multiple surgeries because her bones and ligaments disintegrate, a problem caused by rheumatoid arthritis and other autoimmune diseases. But Chaikin, who lives in Riverdale, N.Y., says her mail order pharmacy, CVS/caremark, has been denying her medications.
“Every month there’s a reason they won’t give me my medication,” says Chaikin. “Sometimes it’s ãWell, why are you taking this dose?’ ãMy doctor prescribed it.’ ãWell, why did your doctor prescribe so much?’ ãAsk my doctor,’” she recounts. “That’s the dose that works for me and you’re made to feel like a drug addict.”
The DEA investigated both CVS and Walgreens, and both pharmacy chains settled civil suits in 2013 for record-keeping violations of the Controlled Substances Act. Walgreens paid penalty, and CVS paid an .
Riley, of the DEA, says it would be wrong to draw a line between these actions and problems like those Chaikin is experiencing. “If there is a chilling effect, it’s clearly not at our direction,” Riley said. “We’re simply enforcing the law, taking bad people off the street and really trying to interrupt the supply of illegal prescriptions.”
In a statement, CVS/caremark said that the dosage of pain medication prescribed to Chaikin “exceeded the recommended manufacturer dosing.” It also said that she “continued to receive her controlled substance prescriptions from CVS/caremark without interruption.”
CVS/caremark said it has a legal obligation to make sure controlled substance prescriptions are for legitimate ailments and “that patients are receiving safe medication therapy, including appropriate dosing.”
Ora Chaikin’s wife, Roseanne Leipzig, who is a geriatrician and palliative care physician, says when it comes to narcotics, there is nothing in medical literature that says a dose is too high.
“There is no maximum dose for narcotics,” she says. “It’s the dose you need to take care of the pain.”
The Florida Board of Pharmacy, which is responsible for licensing pharmacists and educating them on safe practice, has heard enough complaints from pain patients that it is addressing the issue in public meetings. In June, Lesley Young testified before the board on behalf of her husband. She said she has driven more than 100 miles trying to find a pharmacy that would fill her husband’s prescriptions for painkillers.
“I’ve had to do the pharmacy crawl like many of us here,” Lesley told the board. “I’ve been the one who had to go in and beg, crying, with stacks of his medical records, with stacks of imaging, only to get turned away, often rudely, saying ãWe don’t deal with those kinds of patients.’”
The next Florida Board of Pharmacy hearing is set for Monday. A representative of the DEA has been invited to attend.
This story was produced in a collaboration between NPR’s Here & Now and Kaiser Health News.
¤Öêü°å¿üë½ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFãan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/pain-patients-say-they-cant-get-medicine-after-crackdown-on-illegal-rx-drug-trade/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=559354&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>In her Manhattan apartment, Josephina Deltejo is trying to coax her 84-year-old mother Brunhilda Ortiz to get ready to leave the house. As she does most nights, Deltejo makes up a story to get her mother, who has dementia, to cooperate.
In Spanish, Deltejo asks her mother if she would rather go to Miami or the Dominican Republic. “She says she wants to go to the Dominican Republic,” Deltejo translates, and then she helps the older woman gather her things and go downstairs to a waiting van. The driver will bring her mother to the Elderserve At Night program at the Hebrew Home At Riverdale in the Bronx.ô It’s a kind of day campãbut at night, for people like Ortiz who suffer from Alzheimer’s disease.

Deltejo says her mother was once a proud, hard-working immigrant who raised four children on her own, but she has changed. “Her memory has been totally lost. She’s very disoriented,” Deltejo says. “She doesn’t communicate at all.”
For months, Ortiz would sleep during the day and be up much of the night wandering around the apartment. Her daughter was too afraid to sleepãafraid her mother might fall and hurt herself or even try to leave the apartment.
“She wanted to sweep the floor. She wanted to watch TV. She wanted to clean the bathroom,” Deltejo remembers. “She wanted to go out. This is at one, two o’clock in the morning.”
But now Deltejo is finally getting some sleep ã and her mother is being well cared for along with about 40 other clients seven nights a week. Activities may include arts and crafts, cooking, yoga or Zumba, and even live performances. On the night we visited, Juan Ortega played American and Spanish favorites on his synthesizer.
Though it looks like entertainment, each activity has a therapeutic benefit for memory-compromised people, says Deborah Messina, who runs the overnight program. She described a common problem among dementia patients known as “sundowning.” It is thought to affect about 20 percent of Alzheimer’s patients.
“Their day is our night and vice versa, and they are confused about it,” Messina says. “It is usually at dusk where an agitation comes, a confusion comes.”
Many people with dementia are more alert at night than they are all day ã just when their caregivers need to sleep. Rather than try to alter this mismatch, Elderserve At Night embraces it.
The program is the brainchild of David Pomeranz, the executive director of the Hebrew Home, who opened the program in 1996. He says the idea came to him after hearing heartbreaking stories from struggling families.
“People were sleeping in front of doorways because they were concerned that mom or dad would wander out of the house,” Pomeranz says.
Those families desperately needed a safe place for their loved ones at night — and a decent night’s sleep. And the Hebrew Home set out to meet that need.
It’s a similar philosophy ã to meet clients’ needs wherever they may be ã held by the therapists and social workers who staff Elderserve now. “Here, their behaviors are normalized,” Pomeranz explains. “Everything is OK. Activities are structured for them to be successful. Theyô eat, they relax — they can be themselves. To us is this is who they are. We’re not the family members who are dealing with that incredible loss of seeing someone who was and isn’t any more.”
The program is covered by some private insurers and by New York Medicaid, the federal-state program for poor and disabled people. To the extent that it can keep people out of nursing homes, it can save money.
Medicaid pays a typical nursing home in New York about $320 per day versus $200 for the overnight program. But so far, few if any other overnight programs exist solely for people with dementia. Pomeranz thinks the idea hasn’t caught on with other nursing homes because it is difficult to find staff who are willing to work the overnight shift. It was also important to get Medicaid and other insurers to reimburse for the program, and that funding has not been pursued in every state.
Elderserve At Night tries to serve its clients even as their conditions worsen. Next door to the room where Ortiz and others are dancing and enjoying the live music, it feels like another universe. The music is soft, the lights are low and a subtle scent of lavender is in the air. People with more advanced disease spend the evening here. Some are sitting around a table, each with a caseworker, who helps them work with blocks and basic puzzles.
Several other people are slumped in wheelchairs, getting hand massages from the social workers. Though their faces look expressionless, they seem calm. For people with advanced dementia who might otherwise become agitated at night, this room is a sanctuary, says Messina.
“We’re engaging them on their level. And being able to do that might be through touch, it might be through sound, it might be through smell,” she says. “It works for them. It gives them a sense of serenity.”

When the sun comes up tomorrow, all the clients will be given breakfast and everyone here will return home. Ortiz will take the van back to her apartment in upper Manhattan where she will be greeted by her daughter before she leaves for work. Deltejo says she doesn’t know exactly what happens during her mother’s nightly sojourns, but she is grateful.
“She was very weak when she started there. We had to carry her up and down [the stairs}. But now she walks up and down. She walks to Broadway,” Deltejo says. “She would not react to any of the conversation. Now she does. She’s a totally new person. I would say she’s 200 percent better.”
Deltejo says the program helped to improve her mother’s life and her own life as well. But Ortiz was battling congestive heart failure, and she succumbed to the disease a few months after we reported this story.
This story was produced in collaboration with and
KHN’s coverage of aging and long term care issues is supported in part by a grant from .
¤Öêü°å¿üë½ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFãan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/aging/awake-and-safe-all-night-despite-dementia/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=525823&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>“Patients coming to our hospital, getting what we believed was high quality care, were coming back at an alarmingly high rate,” says Yang.
The hospital was providing quality care to patients when they were in the hospital, but it turned out that focus was too narrow, says Yang.

Dr. Julius Yang runs a program that has helped Beth Israel Deaconess Medical Center improve its readmission rates. (Photo: James Derek Dwyer/BIDMC).
“In the hospital we provide a lot of structure, we provide a lot of staff. We provide a lot of expertise to manage every moment of their illness,” he says, “but as soon as they leave, the complexity of their situation probably explodes.”
Lila Gross, 84, is one of those complex patients, suffering from heart, lung and kidney problems. Gross frequently ended up in the hospital, and her daughter Geri Segel says the family always left with unanswered questions.
“She would check out of the hospital and there was no one who followed through,” says Segel. “We had a hundred questions and we had to wait for the next catastrophe to get her back in the hospitalô to find more answers.”
Now Lila Gross is one of 2,000 Medicare patients whoô is treated in Beth Israel Deaconess’ . The idea behind the program, which stands for Post-Acute Care Transitions, is to keep Medicare patients from bouncing in and out of the hospital. Studies show that about 30 percent of elderly patients return to the hospital within 30 days of being discharged.
With a $5 million federal grant, PACT nurses and pharmacists now track Medicare patients who are at high risk for readmission. Nurses call patients and their caregivers, communicate with a patient’s primary care provider and arrange for rehabilitation or visiting nurses. Pharmacists are also on hand to answer medication questions.
Siegel says having PACT nurse Susan Sorlien as an advocate for her mother means the family now knows when they should bring their mother into the hospital and when it can be avoided.
“Susan would keep touching base with my sister and myself to make sure that mom was taking everything and that we understood how to use everything and that mom was doing well,” says Segel. “When we had questions, Susan had an answer.”
So far Beth Israel Deaconess has reduced its readmission rate by 25 percent and its fines have also been reduced. According to Yang, who directs the PACT program, the hospital is now providing better care for its older patients.ô But there’s a catch, he says, because the hospital loses money for every bed it keeps empty.
“For a patient to come into the hospital, whether it’s a readmission or not, we collect revenue and yet we are being penalized for this,” he says.
The attempt to control costs under Obamacare focuses on hospitals because hospitals are expensive, says Ashish Jha, a professor at the Harvard School of Public Health. But the new readmissions policy alone is not enough to bring down those high hospital costs, he says.
“The problems with policies like these is that they are piecemeal, they are fragmented and they are little band aids,” says Jha. “I think we need a much more comprehensive approach to how we pay for healthcare.”
This story is part of a collaboration between Kaiser Health News and the WBUR-NPR show .
¤Öêü°å¿üë½ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFãan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/aging/top-boston-hospital-tackles-readmissions/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=32927&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story was produced in collaboration with
It was her own experience with debilitating side effects after cancer treatment that led Dr. Julie Silver to realizeô there is a huge gap in care that keeps cancer patients from getting rehabilitation services.
ô was 38 in 2003 when she was diagnosed with breast cancer. Even though she is a physician, she was shocked at the toll chemotherapy and radiation took on her body. Silver was dealing with extreme fatigue, weakness and pain.

Julie Silver
“I was really, really sick, sicker than I ever imagined,” says Silver, who is an assistant professor at Harvard Medical School. “I did some exercise testing and I tested out as a woman in my 60s. So I had aged three decades in a matter of months through cancer treatment.”
Silver went to her oncology team for help. They told her to go home and heal. “The conversation should have been, ãWe’re going send you to cancer rehab to help you get stronger,’” she says. But that’s not what happened, and after Silver came to realize that her experience was typical, she set out to change the system for other patients.
In 2009 she startedô ô after treatment. It’s called STAR and is now offered in almost all 50 states.ô The program is growing, as isô ô and can be helped with rehab.
But even with the awareness of its benefits growing, there is still a disconnect for patients.
“Patients are getting stuck, and they don’t know where to go,” says Dr. Rebecca Lansky, a rehabilitation specialist at the University of Massachusetts Medical Center. She says the focus on cancer care is on treatment and that cancer patients suffering from major side effects often fall through the cracks. She recalls one patient who struggled with the side effects of tongue cancer treatment.
“He had radiation to the whole jaw and neck so he couldn’t open up his mouth for six months,” Lansky said. “He had a feeding tube, and he kept going to his oncologist saying, ãHow can I get better? What I can do? He finally got referred to me and we are now opening up his jaw six months after he has been unable to move.”
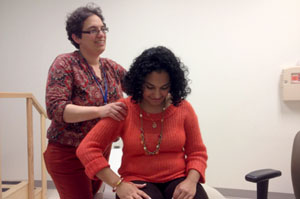
Dr. Rebecca Lansky examines a patient (Photo by Rachel Gotbaum/For KHN)
A in the Journal of Clinical Oncology found that 90 percent of the patients needed rehab but only about one third were getting the therapy.
“I’ve seen cases where someone has had a lot of pain, and they’ve done scans and it’s not a malignancy and maybe they have done exploratory surgery to see what is happening and not really finding much except a lot of scar tissue,” says physical therapist Jennifer Goyette, a STAR trained therapist who works with cancer patients in Worcester, Massachusetts. “I am able to get them a lot of relief and a lot of times patients don’t need to have further intervention. They don’t want to be on the narcotics for the pain management. They would rather come here.”
One of Goyette’s clients is 56-year-old cancer survivor Deborah Leonard. For two years after her treatment for early stage breast cancer, Leonard had swelling, pain and a large mass in her breast –which was not cancer.
“Clearly I didn’t have that before the surgery, because the tumor was so small and this was much bigger, and it just kept getting bigger,” says Leonard.ô “By nighttime my breast was extremely swollen and very painful.”
At first doctors thought Leonard might have an infection and gave her antibiotics. When that didn’t work they did another surgery to remove scar tissue. But the problem returned. Her doctors were suggesting a third surgery when Leonard finally found Goyette.
After three sessions with Goyette doing what is called lymphatic drainage, Leonard felt much better.ô Goyette uses manual pressure to clear Leonard’s lymphatic system, allowing the build up of fluid causing Leonard’s pain and swelling to subside.
“I had a 6-inch mass that is now down to half its size,” says Leonard.
“I’m sleeping at night, I have energy again. More people need to know about this because you don’t have to be a martyr and grin and bear it. This works.”
The issues are different for every type of cancer ã head and neck cancer patients may need swallowing and speech therapy; blood cancer patients may need therapy similar to cardiac rehab to rebuild their strength and stamina; and patients treated for colon cancer can get help from physical therapists with back pain and abdominal swelling.
Most insurers do cover rehab for cancer patients, but sometimes patients must battle to get more than the standard 9 to 12 sessions covered. Another barrier to care is that too few oncologists and cancer surgeons refer their patients to rehab.
The Commission on Cancer,ô the arm of the American College of Surgeonsô that accredits cancer programs in U.S. hospitals, recently announcedô ô including better access to rehabilitation therapy.
¤Öêü°å¿üë½ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFãan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/cancer-rehabilitation/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=25510&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>