
The first sign came when Deepanwita Dasgupta was 5 and started stumbling more while playing at her home in Bangalore in southern India. The girl was always up to something, so her parents figured extra bumps and bruises were just symptoms of an active childhood. Maybe, they thought, it was ill-fitting shoes.
Relatives described the unicorn-loving child as smart, affectionate, and occasionally rascally. Before she learned the alphabet, she had figured out how to find her favorite show, Blippi, on a phone. She was known to sneak butter from the fridge to enjoy a few finger licks.
But then her limbs started jerking. A spinal tap revealed measles in her cerebrospinal fluid. The virus she probably had as an infant had secretly made its way to her brain. Now 8 years old, Deepanwita is paralyzed, unable to talk.
Measles causes complications тАФ ranging from diarrhea to death тАФ in , according to the Infectious Diseases Society of America. Some are immediate, while others take weeks or months to appear. The one Deepanwita is experiencing, subacute sclerosing panencephalitis, or SSPE, typically takes years to rear its head.
“People think, тАШOh, you know, if we get measles, then we’ll be fine, because I know my neighbor had it and they’re fine,’” said , who leads the national Child Neurology Society but spoke to ║┌┴╧│╘╣╧═Ї News in her capacity as a New York City doctor with expertise in neurologic conditions.
Measles, though, can be dangerous: A will have to relearn how to walk after enduring one of the more immediate complications, brain swelling. And every so often, the virus plants a ticking time bomb in the nervous system. A person can recover from measles and continue life as usual, no longer contagious and without any identifiable symptoms тАФ sometimes for a decade or more тАФ before problems appear. While some patients end up severely disabled for a while, Khakoo said, the condition is almost always fatal.
Before the advent of widespread and effective vaccines, the complication occurred enough in the U.S. that in the 1960s a doctor created of SSPE patients. Researchers about 1 in 10,000 people who get measles will develop SSPE, but the risk is significantly higher for those who contract measles before age 5. Populous nations where the virus is endemic, including India, see cases routinely.
Now, doctors and researchers fear that as vaccination rates drop and measles spreads in the U.S., cases of this debilitating complication will also rise here. Since the start of 2025, the over 3,500 measles cases тАФ more than in the entire preceding decade тАФ mostly people who were unvaccinated. Many were children. Last year, Connecticut doctors with SSPE, and in California, a school-age child who’d had measles as an infant .
“We are likely to see SSPE cases going forward, especially if we don’t get this under control,” said , a member of the American Academy of Pediatrics’ Committee on Infectious Diseases and author of the book .
Concern about SSPE was great enough that in January, the Child Neurology Society to educate U.S. clinicians about the condition, and doctors who have seen such cases are warning their peers.
“We don’t have a way of knowing who’s going to get it, and we don’t have a way of very effectively treating it,” said , a professor of neurology with the New York University Grossman School of Medicine. “The one best thing that we can do, ideally, is to prevent children from having to go through it in the first place.”
The recommended two-dose measles vaccine slashes an exposed person’s risk of getting the contagious virus from тАФ and thus reduces the chance of SSPE. The vaccines carry small risks of and a , but measles itself has a higher risk of causing both.

Cases in the U.S.
A of California children who developed SSPE after a measles outbreak there years ago determined that 1 case is diagnosed for about every 1,400 known cases of measles in children under age 5, and 1 for every 600 infected babies.
The researchers also found that, over the years, doctors had missed some cases among patients who had died with undiagnosed neurologic illness.
The possibility that future cases could go undiagnosed spurred and her colleagues to publish a news release in September when a Los Angeles County child .
“We’ve had very few cases of measles in the last 25 years in this country,” said Yeganeh, who is the medical director with the Vaccine Preventable Disease Control Program at the Los Angeles County public health department and has had two patients with SSPE. “Unfortunately, that’s changing, and so we wanted to make sure that everyone was aware of this long-term complication.”
The California child who died had gotten measles as an infant, Yeganeh said, before the child could receive the vaccine. Measles is highly contagious, so at least 95% of the population must be immune to it to protect vulnerable people тАФ including babies too young to vaccinate and people who are immunocompromised тАФ from infection.
“This is an example of someone who did everything right, wanted to protect their child against this infection, and unfortunately ended up losing their child because we didn’t have herd immunity for them,” Yeganeh said.
Shortly after Yeganeh’s group published the news release in California, Nelson was working to get the word out, too.
He had recently seen a 5-year-old whose family had traveled to the U.S. for medical care after the child started stumbling, jerking, hallucinating about bugs and animals, and having seizures. The child had contracted measles as an infant and had been too young to be vaccinated. Nelson diagnosed the child with SSPE.
“Imagine that: Having a child who is healthy and happy, moving to talking less and less, eventually not able to walk,” Nelson said. “It’s a very sad thing.”
He thought he would encounter the condition only in medical school textbooks, as a relic of the past. Instead, in October he found himself presenting the case at the Child Neurology Society’s national conference and participating in the society’s video about the condition. “I’ve now seen something I shouldn’t have ideally seen ever in my career,” he said.
Warning Signs From India
Globally, the number of measles outbreaks in recent years, and physicians in places including and have recently seen clusters of SSPE.
The high human cost of measles’ spread is especially evident in India. While total cases aren’t tracked, about 200 families caring for people with SSPE, including Deepanwita’s, are in a single chat group in the Bangalore area.
In New Delhi, Sheffali Gulati and sees about 10 new patients a year with the condition, what she calls the “delayed echo” of measles outbreaks. The youngest she has seen was 3 years old.
“The ages are , and a death or a vegetative state can develop as soon as in six months to five years of onset,” said Gulati, who leads the pediatric neurology program at the and until recently led India’s .
Gulati hasn’t found any treatments that reverse SSPE’s course, only some that slow its progress. She’s found herself counseling parents: It’s catastrophic, it’s not their fault, and they can do nothing but accept it.
Deepanwita’s relatives try to find joy where they can. They think they noticed the girl smiling when her favorite cousin called recently. Anindita Dasgupta, her mother, said Deepanwita moves her hands and feet on her own and sometimes turns her head, especially when her father enters the room. The girl communicates with her parents through her eyes and a few sounds.
But it’s far from where she was in 2022: At a cousin’s birthday, a few months before noticeable symptoms started, Deepanwita started the birthday song and sang the loudest.
At her own 8th-birthday gathering last year, Deepanwita, wearing a pink eyelet dress and a nasal tube, could only blink and move her eyes as she sat propped up before two cakes that she would not be able to eat. She can no longer swallow, so her mom dabbed a bit of icing on her tongue.
Research That Shouldn’t Be Needed
, a molecular biologist at the Mayo Clinic in Rochester, Minnesota, has been for years. He recently used postmortem brain tissue to map how the measles virus can spread from the frontal cortex to colonize the entire brain. Still, he said it’s a “black box” what exactly measles is doing in those dormant years between the initial infection and when the symptoms of neurologic damage crop up.
It’s possible the virus replicates in the brain that whole time, undetected, killing off neurons. But with so many neurons in the human brain тАФ 10 times as many as people living on the planet тАФ the brain may find a way to adjust, Cattaneo said, until finally it can’t anymore.
He’s applying for funding to continue research on the disease and possible treatments, though ultimately, he wishes he didn’t have to. The tools to obliterate the condition already exist.
“The problem could be solved with vaccination,” Cattaneo said. The U.S. should have no cases of SSPE, he said. “It’s just painful.”
This <a target="_blank" href="/public-health/measles-outbreaks-long-term-complications-sspe-subacute-sclerosing-panencephalitis/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2166663&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The legislation introduced in , , , , , , , and builds on efforts made in other states in past years. This latest push for patient protections comes as the Trump administration has backed away from federal debt protections, health care has become , and more people are expected to go without medical coverage or but riskier high-deductible insurance plans that could lead them into debt.
“In the wealthiest country on Earth, people are going bankrupt, suffering wage garnishment, just because they get sick,” said Colorado state Rep. , a Democrat who introduced legislation on Feb. 19 that would, among other measures, ban wage garnishment for medical debt.
That legislation is under consideration after a ║┌┴╧│╘╣╧═Ї News investigation found that courts approved wage garnishment requests in an estimated 14,000 medical debt cases a year in Colorado. The investigation also showed that it isn’t just urban hospitals or big health care chains allowing their patients’ wages to be garnished. It’s also small rural hospitals, physician groups, and public ambulance services, among other medical care providers. And the reporting showed that wage garnishment can erroneously target patients. For example, one family lost wages тАФ and subsequently power to their home, because they couldn’t pay their electric bill тАФ after an ambulance company incorrectly billed the family instead of Medicaid.
Wage garnishment is one tool creditors can use in most states to recoup money from people with unpaid bills. In many states, they can garnish someone’s bank account or put a lien on their home, too. To garnish a person’s wages, a creditor must typically get permission from a court to make the person’s employer hand over a piece of the debtor’s earnings.
“The creditor is taking the money directly out of somebody’s paycheck, and so it doesn’t leave people with any choice to say, тАШI need to prioritize food for my children,’” said , legal and policy director for the National Center for Access to Justice. The center, based at Fordham Law School, and the District of Columbia on how fair their laws are to consumers who get sued over debt.
It is legal to garnish patients’ wages for medical debt in all but a , according to the Commonwealth Fund, a nonprofit foundation based in New York focused on health care.
Now, lawmakers in additional states seek to ban the practice entirely. Others want to limit it by exempting debtors whose household income falls under a certain threshold or by upping the amount of earnings immune from garnishment.
Such policies on wage garnishment fit into a larger push around the country to address the effect of medical debt on people’s lives and finances. Those efforts include barring medical debt from credit reports, prohibiting liens on people’s homes, capping interest rates, and limiting the ability to file lawsuits against people with low incomes over unpaid medical bills.
Debt collectors have fought against such measures, arguing they don’t solve the problem of health care affordability and hurt the ability of medical providers to continue to provide care.
“The wage garnishment process is already highly regulated at the federal and state level and includes many consumer protection measures,” said Scott Purcell, chief executive of , an association of credit and collection professionals.
Even before the Colorado legislation was introduced, BC Services warning its clients that the legislation “poses an existential threat,” especially to rural health providers. And Bridget Frazier, a spokesperson for the , said Feb. 20 that the bill “could drive up costs and financial risk for health care providers, making it harder to keep hospitals sustainable and ensuring Coloradans have access to care when they need it most.”
The pending Colorado measure would ban wage garnishment for all patients. It also would limit bank garnishments, in which a patient’s financial institution must hand over a chunk of the money in the person’s account. Additionally, among other things, it would prevent payment plans from exceeding 4% of weekly net income, require creditors to check whether uninsured patients are eligible for public health insurance before collecting, bar creditors from collecting on bills that are more than three years old, and leave medical care providers liable to the patient for at least $3,000 if collectors don’t comply.
“No one is saying, тАШDon’t get paid for your services.’ We’re saying getting health care should not lead to financial ruin for people,” said Dana Kennedy, co-executive director at the Denver-based , a health advocacy group that has been working with lawmakers on the Colorado measure.
Kennedy said that ║┌┴╧│╘╣╧═Ї News’ investigation drove home how many kinds of Colorado health care facilities are willing to let this collection practice happen to their patients, and that the people whose wages are being garnished are often working at Family Dollar, Walmart, Amazon, or gas stations and restaurants.
“Medical debt is typically different from other forms of indebtedness,” said Colorado state Sen. , a Democrat co-sponsoring the legislation. “You could choose to keep driving your old car or buy a new one and take on debt for that. You could upgrade your home. You could buy consumer appliances. There’s not usually that voluntary element in a health care context.”
, a senior attorney with the National Consumer Law Center, said broad laws that don’t require patients to jump through hoops to access protections are the most likely to be effective. Because of that, she and other consumer advocates prefer state policies that get rid of wage garnishment for all debtors and all types of debt.
“It can be hard to identify medical debt as medical debt,” Carter said. “For example, if you have a medical debt and you put it on your credit card, it’s not going to be easy for a court system to identify that debt as medical debt.”
She said another reason is that complexity is the enemy of effectiveness. Carter pointed to a showing that even though people in the state can keep $10,000 in their bank accounts safe from garnishment, few consumers take advantage of the protection. They must know the protection exists, know where to find the relevant form, get the form notarized, file it, and mail copies to creditors. The same report found that garnishments can also be burdensome for employers, who must process garnishments and can find themselves in court if they make an error.
Jones, at the National Center for Access to Justice, said outlawing wage garnishment fully, rather than limiting it, has other benefits. “It’s also to protect people’s jobs, because in most states, if somebody has two or more orders of garnishment, they can lose their job for it,” she said.
Still, some lawmakers are pushing for the intermediate route. In Washington state, Democratic state Sen. is spearheading legislation to rope off a larger portion of low-wage earnings from garnishment. So, for example, a person making $1,000 a week would be able to keep their whole paycheck, as opposed to the $800 that the law would currently protect.
Mindy Chumbley, owner of a Washington-based collections company and an ACA International board member, testified against the bill on Feb. 2. “Washington has made sweeping changes to medical debt policy year after year without pausing to study the cumulative impact,” she told lawmakers. “Our clients are reporting clinic closures, urgent care centers shutting down, staffing shortages, and rural facilities struggling to stay open.”
The Washington State Hospital Association said it is neutral on the legislation. The American Hospital Association said it does not take positions on state policies.
Liias told ║┌┴╧│╘╣╧═Ї News that lawmakers need to ensure health care providers can recoup their costs while also protecting patients. “We don’t want families either to be driven into bankruptcy or to be driven into under-the-table work to avoid these garnishment thresholds,” he said.
Liias said his measure follows the lead of Arizona, which passed similar consumer protections in 2022. “Obviously, the health care system is still functioning in Arizona, and folks are able to make it work.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/medical-debt-wage-garnishment-state-legislation-patient-protection/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2154960&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>In Alaska and Michigan, legislators are nonetheless advancing bills to keep medical debt off consumer credit reports.
The attorneys general of California and Colorado said they would stand behind credit reporting laws enacted in those states in recent years, even as Colorado faces a lawsuit from debt collectors contesting such laws.
Indiana and Ohio lawmakers have dropped proposals to remove medical debt from credit reports but are pushing legislation that would extend other protections to patients who cannot pay their medical bills.
“ of Alaska voters don’t think credit reports should include medical debt,” said state Rep. , a Democrat there. “I’m not going to wait on the courts on the medical debt issue.”
An estimated 100 million Americans are saddled with health care debt. And a growing number of red and blue states have enacted laws to protect patients.
But federal policy on such debt boomeranged this year when President Donald Trump’s administration chose not to defend federal regulations that would have removed medical debt from all Americans’ credit scores. And in October, Trump’s Consumer Financial Protection Bureau do not have the authority to regulate consumer credit reports.
“It’s sort of a head-spinning, 180-degree reversal,” said , an attorney with the National Consumer Law Center, which advocates for people with low incomes. She called the Consumer Financial Protection Bureau, now led by Project 2025 architect , the “evil twin” of its predecessor under President Joe Biden.
The bureau did not respond to requests for comment.
Eight days after the new federal guidance, debt collectors filed a lawsuit contesting Colorado’s 2023 medical debt credit reporting law, the first to require removal of some or all medical debt from credit reports.
Scott Purcell, CEO of , which is a debt collection trade group and a plaintiff in the Colorado suit, said removing the debt makes it harder to gauge creditworthiness, which he said would lead creditors to assume everyone is a riskier bet.
His also argues the Colorado law violates the First Amendment by suppressing “truthful commercial speech.”
Colorado Attorney General Phil Weiser, a Democrat, called the lawsuit outrageous in a statement to ║┌┴╧│╘╣╧═Ї News. His office, he said, “will strongly oppose all efforts to strip away critical medical debt protections.”
In California, Attorney General Rob Bonta, too, is standing firm on his state’s law regardless of how federal officials now interpret state rights. The Democrat told constituents in a : “Let me be clear: This remains the law in California.”
In other states still contemplating credit reporting laws, legislators are adjusting their strategy to account for the lawsuit and the Trump administration’s moves, by either ditching the plan to remove medical debt from credit reports or modifying such legislation.
Wu said her organization saw the federal change coming and had already urged state lawmakers to make pending legislation on credit reporting more lawsuit-proof by looking upstream and downstream of the credit reporting agencies. For example, Wu said, states can tell landlords, employers, or other credit report perusers that they cannot use a person’s medical debt history in their decision-making. And states can require health providers to include, in their contracts with debt collectors, limits on what they can tell credit reporting agencies about the bills they’re collecting.
“You’ll often hear providers say, тАШOh, well, we don’t want to hurt our patients’ credit,’” she said. “Tell the debt collectors, тАШDon’t report this.’”
Alaska’s legislation has both elements: It bars landlords from making decisions about potential renters based on their medical debt history, and it bars providers and collectors from telling credit reporting agencies about patient debt.
Elsewhere, state lawmakers have opted out of trying to pass credit reporting provisions in proposed legislation. Indiana state Sen. , a Democrat, that tries to, among other things, cap interest rates, limit wage garnishment, and keep people from losing their homes over unpaid bills from medically necessary procedures. But he and his colleagues made a tactical decision to leave out credit reporting, after unsuccessfully including it in a similar bill last year.
“It’s out of legislative pragmatism,” Qaddoura said. “We want to be sure that you don’t get a piece of legislation killed with many benefits to tens of thousands of families just because one provision can’t go in.”
In Ohio, Democratic state Rep. made a similar calculation. She has been working on to ban wage garnishment over medical debt, cap interest rates for such debt at 3%, and scratch it from credit reports. She said she and other lawmakers recently removed the credit reporting portion.
“It’s better to pass something than nothing at all,” Grim said. “It still bans wage garnishment, which is a very aggressive, more-common-than-you-think practice. And it caps the interest rate.”
A recent investigation by ║┌┴╧│╘╣╧═Ї News found that, in Colorado alone, thousands of people each year have their wages garnished to pay back medical bills, and some people taken to court for medical debts never actually owed the money.
Legislative efforts to protect people from the effects of medical debt are often bipartisan, but that doesn’t mean they pass easily. Even before the Consumer Financial Protection Bureau reversed its stance on credit reports, several measures hit obstacles in conservative states this year, and legislation failed in Wyoming and South Dakota that aimed to take medical debt off credit reports.
Americans are largely protected from having their credit scores dinged by small medical debts. In 2023, the three big credit bureaus тАФ TransUnion, Equifax, and Experian тАФ to remove medical debts under $500 from their credit reports, and the Consumer Data Industry Association, a trade group for the companies, confirmed they are still doing so.
Even so, lawmakers in several states said they are deciding whether and how to get ahead of the federal guidance with legislation that tackles additional, larger medical debt on credit reports.
“We know that this will need to get beefed up,” said , a Democratic state senator in Michigan, of . She isn’t sure what that will look like, though consumer advocates including Libby Benton hope to see the measure follow Wu’s strategy.
“These aren’t debts that people choose to take on. People might choose to buy a huge pickup truck and that’s a bad financial decision,” said Benton, director of the Michigan Poverty Law Program. “People don’t choose to have emergency heart bypass surgery.”
Yet both can end up on a credit report.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/courts/credit-reports-medical-debt-state-legislation-cfpb-trump-reversal/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2130361&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The texts were part of a pilot run to test technology the Trump administration says will make it easier for some Medicaid enrollees to prove they meet new requirements тАФ working, studying, job training, or volunteering at least 80 hours a month тАФ set to take effect in just over a year.
But only 894 people completed the quarterly wage check, or just under 7% of enrollees who got the text, according to Drew Maranto, undersecretary for the Louisiana Department of Health.
“We’re hoping to get more to opt in,” Maranto said. “We plan to raise awareness.”
The clock is ticking for officials in 42 states тАФ excluding those that did not expand Medicaid at all тАФ and Washington, D.C., to figure out how to verify that an estimated 18.5 million Medicaid enrollees meet rules included in President Donald Trump’s tax and spending law. They have until the end of next year, and federal officials are giving those jurisdictions a total of $200 million to do so.
The policy change is one of several to free up money for Trump’s priorities, such as increased border security and tax breaks that mainly benefit the wealthy.
The nonpartisan Congressional Budget Office has said the millions of people won’t be able to access health insurance over the next decade. It estimates changes to the Medicaid program will result in 10 million fewer Americans covered by 2034 тАФ more than half of them because of the eligibility rules.
For now, state officials, health policy researchers, and consumer advocates are watching the pilot program in Louisiana and another in Arizona. , director of the Centers for Medicare & Medicaid Services, has touted those test-drives and said they will allow people to verify their incomes “within seven minutes.”
“There have been efforts to do this in the past, but they haven’t been able to achieve what we can achieve because we have technologies now,” said Oz, in August.
Brian Blase, the president of the conservative Paragon Health Institute and a key architect of Medicaid changes in the new law, has chimed in, saying during a that with today’s artificial intelligence “people should be able to seamlessly enter how they are spending their time.”
║┌┴╧│╘╣╧═Ї News found scant evidence to support such claims. Federal and state officials have offered little insight into what new technology the two pilots have tested. They do say, however, that it connects directly with the websites of Medicaid enrollees’ payroll providers, rather than using artificial intelligence to draw conclusions about their activities.
Oz said the Trump administration’s efforts started “as soon as the bill was signed” in July. But work on the pilot programs .
And Medicaid is a state-federal program: The federal government contributes most of the funds, but it is up to the states to administer them, not the federal government.
“Oz can say, тАШOh no, we’re going to fix this. We’re going to do this.’ Well, they don’t actually run the program,” said , a health policy researcher at Georgetown’s Center for Children and Families.
Officials have also offered few details about the pilots’ effectiveness in assisting enrollees in Medicaid or other public benefit programs.
The shortage of information has some state officials and health policy researchers worried that the Trump administration lacks viable solutions to help states implement the work rules. As a result, they say, people with a legal right to Medicaid benefits could lose access to them.
“What actually keeps me up at night is the fear that members that are eligible for Medicaid and are trying to get health care services would fall through the cracks and lose coverage,” said Emma Sandoe, Oregon’s Medicaid director.
Officials involved in the Louisiana and Arizona projects declined to answer many specific questions about their efforts, instead directing ║┌┴╧│╘╣╧═Ї News to federal officials.
Spokespeople for Arizona’s Medicaid and Economic Security departments тАФ Johnny Córdoba and Brett Bezio, respectively тАФ did not share data on how many people participated in the state’s pilot test nor describe the outcome. They said the pilot had been used to verify eligibility only for the federal Supplemental Nutrition Assistance Program, a smaller program than Medicaid.
The , a nonprofit that helps people sign up for such SNAP benefits, hadn’t heard of the pilot program.
State officials and health policy researchers said neither pilot program could confirm whether a person meets other qualifying activities тАФ such as community service тАФ or any of the numerous exemptions. The tools being tested can verify only income.
Andrew Nixon, director of communications for the U.S. Department of Health and Human Services, which oversees Oz’s agency, wrote in a statement that the digital tools officials aim to share with states “are largely under development.”
One person is Michael Burstein, who until recently worked at the U.S. Digital Service, which later became known as the Department of Government Efficiency.
As the U.S. Digital Service was turned into DOGE, Burstein and other staffers left and started a nonprofit called to finish supporting the technology to make it easier for people to verify their incomes for Medicaid enrollment.
But without permission from state officials, Burstein would not describe the tool in development, aside from saying that it’s mobile-first, can quickly verify income for a new or returning client, “and we’re pretty happy with it.”
The state agencies that manage benefit programs, such as Medicaid and SNAP, are understaffed, and they use different eligibility systems, , which makes improving them “a challenging task,” he said.
The $200 million in start-up costs the federal government has earmarked for systems to track work requirements equals to administer Georgia’s Medicaid work requirement program alone.
That state, which has the nation’s only active work requirement program, called Georgia Pathways to Coverage, in September was granted a , despite a from a federal watchdog saying it hadn’t received enough federal oversight. A has kept enrollment in the program far below Georgia’s own projections.
Trump’s tax and spending law allows states to ask for extra time тАФ until the end of 2028 тАФ to start enforcing the rules, but only with the approval of HHS Secretary Robert F. Kennedy Jr. It also allows counties with , but states must apply for that exemption.
Even with an app that states can use to prove people are eligible for Medicaid, enrollees would still need to know that app existed and how to use it тАФ neither of which is a given, Alker said. There is also no guarantee they’d have reliable cell service or internet access. As , millions of Americans live in rural areas without reliable internet.
Private vendors also have been working on such apps, said , who researches Medicaid eligibility and enrollment at the Center on Budget and Policy Priorities. Wagner said she has seen several vendors demonstrate products they plan to pitch to states for the work rules. Many are limited in scope, she said, like those in the pilot tests.
“Nobody has a magical solution that’ll make sure eligible people don’t lose coverage,” she said.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/medicaid-eligibility-tool-pilot-test-work-requirements-ai-louisiana-arizona-georgia/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2103530&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>So she was shocked when, three years after the trip to the hospital, her employer received court orders requiring it to start funneling a chunk of her paychecks to a debt collector for an — which had from interest and court fees.
The timing was terrible. After leaving a bad marriage and staying in a shelter, she had just gotten full custody of her three children, steady housing in Montrose, Colorado, and a job at a gas station.
“And that’s when I got that garnishment from the court,” she said. “It was really scary. I’d never been on my own or raised kids on my own.”
║┌┴╧│╘╣╧═Ї News reviewed 1,200 Colorado cases in which judges, over a two-year period from Feb. 1, 2022, through Feb. 1, 2024, gave permission to garnish wages over unpaid bills. At least 30% of the cases stemmed from medical care — even when patients’ bills should have been covered by Medicaid, the public insurance program for those with low incomes or disabilities. That 30% is likely an underestimate since medical debt is behind other types of debt, such as from credit cards or payday loans. But even that minimum would translate to roughly 14,000 cases a year in Colorado in which courts approved taking people’s wages because of unpaid medical bills.
Among the other findings:
- Patients were pursued for medical bills ranging from under $30 to over $30,000, with most of the bills amounting to less than $2,400. As the cases rolled through the legal system, accumulating interest and court fees, the amount that patients owed often grew by 25%. In one case, it snowballed by more than 400%.
- Cases trailed people for up to 14 years after they received medical care, with debt collectors reviving their cases even as they moved from job to job.
- Medical providers of all stripes are behind these bills — big health care chains, small rural hospitals, physician groups, public ambulance services, and more. In several cases, hospitals won permission to take the pay of their own employees who had unpaid bills from treatment at the facilities.
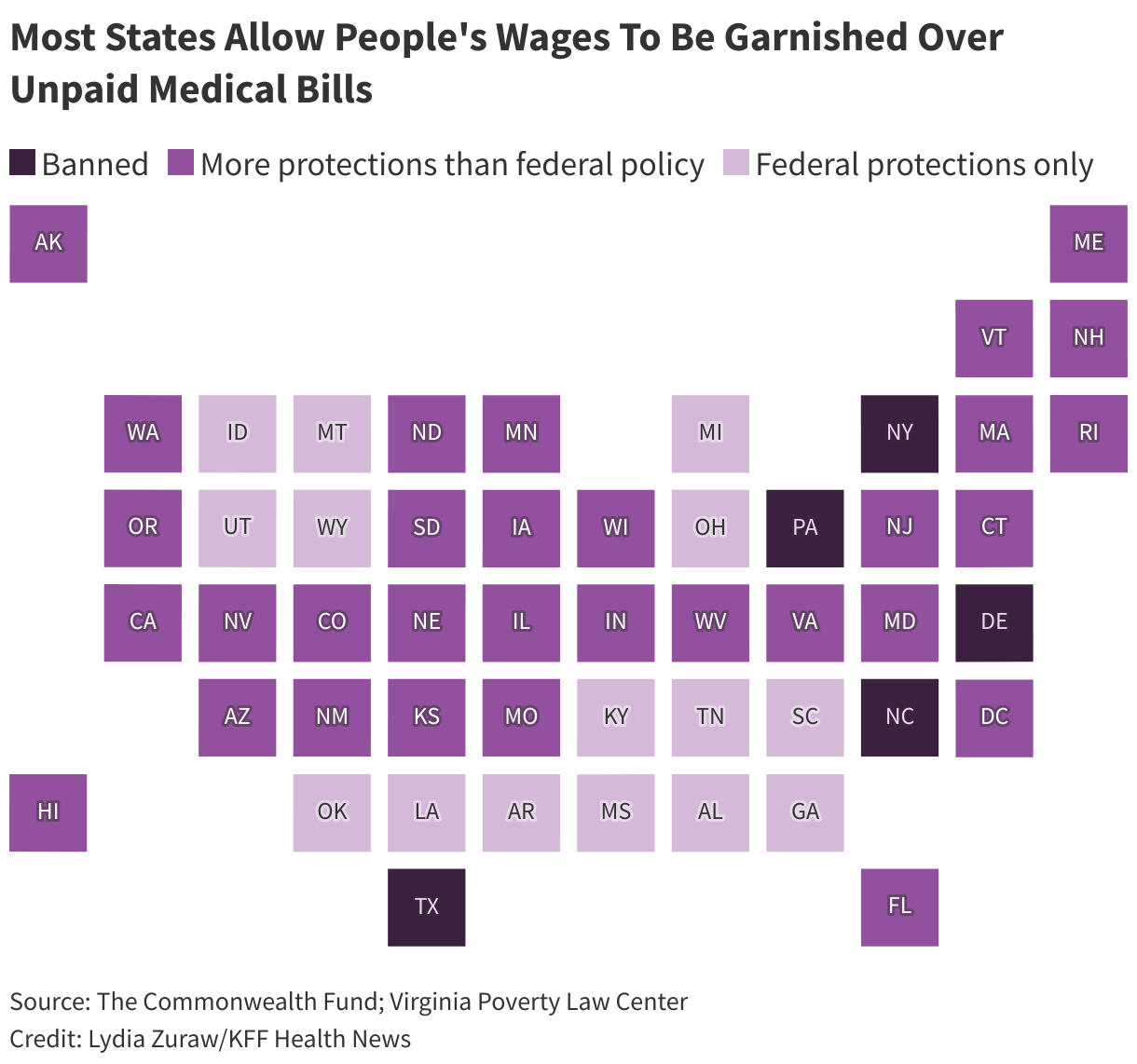
Colorado has company. It is one of 45 states that allow wage garnishment for unpaid medical bills. Only Delaware, New York, North Carolina, Pennsylvania, and Texas have banned wage garnishment for medical debt.
As ║┌┴╧│╘╣╧═Ї News has reported, medical debt is devastating for millions of people across the country. And now the problem is likely to grow more pressing nationwide. Millions of Americans are expected to lose health insurance in the coming years due to Medicaid changes in President Donald Trump’s tax and spending law and if Congress allows some Affordable Care Act subsidies to expire. That means health crises for the newly uninsured could lead them, too, into a spiral of medical debt.
And the hurt will linger: Large unpaid medical bills are staying on credit reports in most states after a July reversed a new rule aimed at protecting consumers.
“If you can’t maintain your health, how are you going to work to pay back a debt?” said , deputy director of the Colorado Consumer Health Initiative, a nonprofit aimed at lowering health costs. “And if you fundamentally can’t pay the bill, wage garnishment isn’t going to help you do that. It’s going to put you in more financial distress.”
Flying Blind on Medical Debt
When someone fails to pay a bill, the creditor that provided the service — whether for a garage door repair, a car loan, or medical care — can take the debtor to court. Creditors can also pass the debt to a debt collector or debt buyer, who can do the same.
“At any given point, about 1% of working adults are being garnished for some reason,” said , an economist at the University of Wisconsin-Madison, who studied paycheck data from ADP, a payroll processor that distributes paychecks to about a fifth of private sector U.S. workers. “That’s a big chunk of the population.”
But specific research into the practice of garnishing wages over medical debt is scant. Studies in , , and have found that nonprofit hospitals commonly garnish wages from indebted patients, with some studies finding those patients tend to work in low-wage occupations.
Marty Makary, who led research on medical debt wage garnishment in Virginia at Johns Hopkins University before joining Trump’s cabinet as Food and Drug Administration commissioner, has He co-authored a study that found 36% of Virginia hospitals, mostly nonprofit and mostly in urban areas, were using garnishment to collect unpaid debts in 2017, affecting thousands of patients.
The Colorado findings from ║┌┴╧│╘╣╧═Ї News show that hospitals are far from the only medical providers going after patients’ paychecks, though.
Researchers and advocates say that, in addition to a dearth of court case data, another phenomenon tends to obscure how often this happens. “People find debt shameful,” said Lester Bird, a senior manager at the who specializes in courts. “A lot of this exists in the shadows.”
Without data on how often this tactic is employed, lawmakers are flying blind — even as a 2024 about 4 in 5 U.S. adults believe it’s important for the federal government to provide medical debt relief.
‘Blood From a Turnip’
Colorado was of to scratch medical debt from credit reports. Debt buyers in the state aren’t allowed to foreclose on a patient’s home. If qualified patients opt to pay in monthly installments, those payments shouldn’t exceed 6% of their household income — and the remaining debt gets wiped after about three years of paying.
But if they don’t agree to a payment plan, Coloradans can have of their disposable earnings garnished. The National Consumer Law Center gave the state a for state protections of family finances.
Consumer advocates said they aren’t sure how well even those Colorado requirements are being followed. And people wrote letters to the courts saying wage garnishment would exacerbate their already dire financial situations.
“I have begun to fall behind on my electricity, my gas, my water my credit cards,” wrote a man in western Colorado to a judge that ║┌┴╧│╘╣╧═Ї News obtained in the court filings. Court records show he was working in construction and at a rent-to-own store, with about $8,000 in medical debt. He wrote to the judge that he was paying close to $1,000 a month. “The way things are going now I will lose everything.”
The people being sued in ║┌┴╧│╘╣╧═Ї News’ Colorado review worked in a wide array of jobs. They worked in school districts, ranching, mining, construction, local government, even health care. Several worked at stores such as Walmart and Family Dollar, or at gas stations, restaurants, or grocery stores.

“You’re really kicking people when they’re down,” said Lois Lupica, a former attorney working with the Denver-based and the Debt Collection Lab at Princeton. “They’re basically suing the you-can’t-get-blood-from-a-turnip population.”
In 2022, court records show, Valley View health system based in Glenwood Springs was allowed to garnish the wages of one of its patients over a $400 medical bill. The patient was working at a local organization that the as part of the community benefits it provides to keep its tax-exempt status. Nonprofit hospitals like Valley View are required to provide community benefits, which can also include charity care that covers patients’ bills.
, the health system’s chief community relations officer, said it offers options such as interest-free payment plans and care at reduced or no cost to families with incomes up to 500% of the federal poverty level.
“As our rural region’s largest healthcare provider, it is imperative to the health and well-being of our community that Valley View remains a financially viable organization,” she said. “Most of our patients work with us to develop a payment plan or pursue financial assistance.”
The collection agency that took the employee to court, A-1 Collection Agency, as empathetic: “We understand times are tough and money is tight.”
, who oversees operations at A-1’s parent company, Healthcare Management, said it accepts payment plans as small as $50 a month and that most of the hospitals it works with allow it to offer a discount if patients pay all at once.
“Suing a patient is the absolute last resort,” she said. “We try everything we can to work with the patient.”
If you can’t maintain your health, how are you going to work to pay back a debt?
Adam Fox, deputy director of the Colorado Consumer Health Initiative
Hospitals sometimes also garnish wages from their own employees for care they provided them. In one case, a hospital employee worked her way up from housekeeper to registrar to quality analyst. She even participated in public events representing her employer and appeared on the hospital’s website as a featured employee — while the court issued writs of garnishment until her $10,000 in medical bills from the hospital was paid off.
“Hospital care costs money to deliver,” said Colorado Hospital Association spokesperson Julie Lonborg about hospitals’ garnishing their own employees’ wages. “In some ways, I think it’s funny to be asked the question. I would understand if someone said, ‘Why aren’t you garnishing their wages?’”
Studies show that hospital debt collection efforts through wage garnishment bring in only about 0.2% of hospital revenues, said , a senior attorney with the National Consumer Law Center, which advocates for people with low incomes.
“We also know that there are states that don’t allow this at all,” she said. “Hospitals are continuing to provide medical care to consumers.”
Smooth Sailing for Collectors — But Not for Patients
Health care providers appeared as the plaintiffs in only 2% of the medical debt cases. Instead, cases were filed almost entirely by third-party debt collectors and buyers, with BC Services and Professional Finance Company behind more than half of the cases, followed by A-1 Collection Agency and Wakefield & Associates.
Debt buyers make money by buying debt from providers who’ve given up on getting paid then collecting what they can of the money owed, plus interest. Debt collectors get paid a percentage of what they recover. Some companies do a bit of both.
BC Services declined to comment, and Wakefield & Associates did not respond to questions.
Charlie Shoop, president of Professional Finance Company, said his company initiates wage garnishment on less than 1% of all accounts placed with it for collection.
Health care providers in Colorado can no longer hide behind debt collectors’ names when they sue people, according to a prompted by a in partnership with a .
In many states, the path for filing a case against a debtor and garnishing their wages is relatively smooth — especially if the debtor doesn’t appear in court.
“It’s unbelievably easy,” said Dan Vedra, a lawyer in Colorado who often represents consumers in debt cases. “If you have a word processor and a spreadsheet, you can mass-produce thousands of lawsuits in a matter of hours or minutes.”
Within ║┌┴╧│╘╣╧═Ї News’ sample, nearly all the medical debt cases were default judgments, meaning the patient did not in court or in writing. Missing a court date can happen for a variety of reasons, such as not receiving the notice in the mail, assuming it was a scam, knowingly ignoring it, or not having the time to take off from work.
Vedra and other debt law experts said a high rate of default judgments indicates a system that favors the pursuers over the pursued — and increases the chances someone will be harmed by an erroneous bill.
But in New Hampshire, creditors now have to keep going to court for each paycheck they want to garnish, because to garnish only wages that have already been earned, said an associate research professor at the Center on Health Insurance Reforms at Georgetown University.
“It might not look like much on paper,” she said. “It’s just not worth it if they have to keep going back to court.”
If you have a word processor and a spreadsheet, you can mass-produce thousands of lawsuits in a matter of hours or minutes.
Dan Vedra
Wrongly Pursued for Bills
The nation’s medical billing setup is already prone to errors due to its complexity, according to , a law professor at George Washington University and a senior scholar at Stanford Medicine who has in several states. “Bills are not only noncomprehensible, but often wrong,” Richman said.
Indeed, Colorado’s Health Care Policy & Financing Department, which runs Medicaid in the state, said it sent out nearly 11,000 letters in the past fiscal year to health providers and collectors that erroneously went after patients on Medicaid. Bills for Medicaid recipients are supposed to be sent to Medicaid, not the patients, who typically pay a nominal amount, if anything, for their care.
Shoop said his industry has pushed Colorado, without success, for access to a database that would allow them to confirm if patients had Medicaid coverage.
Colorado’s Medicaid program declined to comment.
Patricia DeHerrera in Rifle, Colorado, had to prove that she and her children had Medicaid when they received care at Grand River Health — but only after A-1 contacted her employer at the time, the gas station chain Kum & Go, with court-approved paperwork to take a portion of her paychecks.
She contacted the state, which to the hospital and the collector notifying them they were engaging in “illegal billing action” and telling the collector to stop. The companies did.
Theresa Wagenman, controller for Grand River Health, said if a patient can present a letter from a Medicaid caseworker saying they’re eligible, then their bills get removed from the collections pipeline. Wagenman also said patients get at least eight letters in the mail and several phone calls before Grand River gives the go-ahead for the collector to send them to court.
DeHerrera’s main advice to others in this situation: “Know your rights. Otherwise, they’re going to take advantage of you.”
Yet isn’t easy.

Nicole Silva, who lives in the 900-person town of Sanford in south-central Colorado, said she and her family were all on Medicaid when her daughter was in a car crash. Still, court records show, her wages were garnished for a $2,181.60 ambulance ride, which grew to from court fees and interest.
She the bill was wrong, contacting her county’s social services office, but Silva said it wasn’t helpful and she wasn’t able to reach the right person at a state office. The state Medicaid program confirmed to ║┌┴╧│╘╣╧═Ї News that her daughter was covered at the time of the wreck.
Fighting the bill felt like too much for Silva and her husband to handle while parenting a growing number of kids, one of them severely disabled, and working — she as a preschool teacher and he as a rancher.
Not receiving the roughly $500 a month that she said came out of her pay was enough to affect their ability to pay other bills. “It was deciding to buy groceries or pay the electric bill,” Silva said.
When their electricity got shut off, she said, they had to scramble to borrow money from colleagues and friends to get it turned back on — with an extra fee.
She said the saga makes her hesitant to call an ambulance in the future.
Fox, of the Colorado Consumer Health Initiative, said consumers often think they cannot do anything to stop their wages from being garnished, but they can contest it in court, for example by pointing out they should have qualified for discounted — or charity — care if the hospital that provided the treatment is a nonprofit.
DeFusco, the economist, believes filing for is an underused option for debtors. It halts garnishment in its tracks, though not always permanently, and it comes with other consequences. But he understands it’s a Catch-22: It’s a and typically necessitates hiring a lawyer.
“To get rid of your debt, you need money,” he said. “And the whole reason you’re in this situation is because you don’t have money.”
Methodology
We wanted to know how often Coloradans get their wages garnished due to medical debt. Courts don’t compile this information, and researchers and advocates haven’t tracked it systematically.
So we created our own database. We requested a list of all civil cases across the state in which judges gave permission for a person’s earnings to be garnished — known as writs of garnishment in court lingo — from Feb. 1, 2022, through Feb. 1, 2024. The provided a list from all courts except for Denver County Court, which provided its own records. The combined list comprised nearly 90,000 unique court cases. We split up the cases by county population — small (fewer than 10,000 people), medium (10,000 to 100,000 people), and large (more than 100,000 people) — then generated a random sample of 400 cases from each group to ensure we evaluated medical debt across counties of all sizes.
To identify medical debt cases, we looked at the original creditors named in court records, primarily the complaints or affidavits of indebtedness. Often, this information was available through . When it wasn’t available online, we asked county courthouses to send us supporting documents. We counted dentists as medical providers. We excluded 14 cases in which the debt wasn’t exclusively medical.
We looked only at cases in which courts approved money to be garnished from someone’s paycheck, as opposed to from other sources such as their bank accounts. We did not review garnishment cases involving child support, taxes, or federal student loans.
║┌┴╧│╘╣╧═Ї News intern Henry Larweh, data editor Holly K. Hacker, Mountain States editor Matt Volz, and web editor Lydia Zuraw contributed to this report.
This <a target="_blank" href="/courts/colorado-wage-garnishment-health-care-medical-debt-collections-medicaid/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2092949&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The Department of Health and Human Services in late March canceled nearly 700 Centers for Disease Control and Prevention grants nationwide — together worth about $11 billion. Awarded during the covid-19 pandemic, they supported efforts to vaccinate people, reduce health disparities among demographic groups, upgrade antiquated systems for detecting infectious disease outbreaks, and hire community health workers.
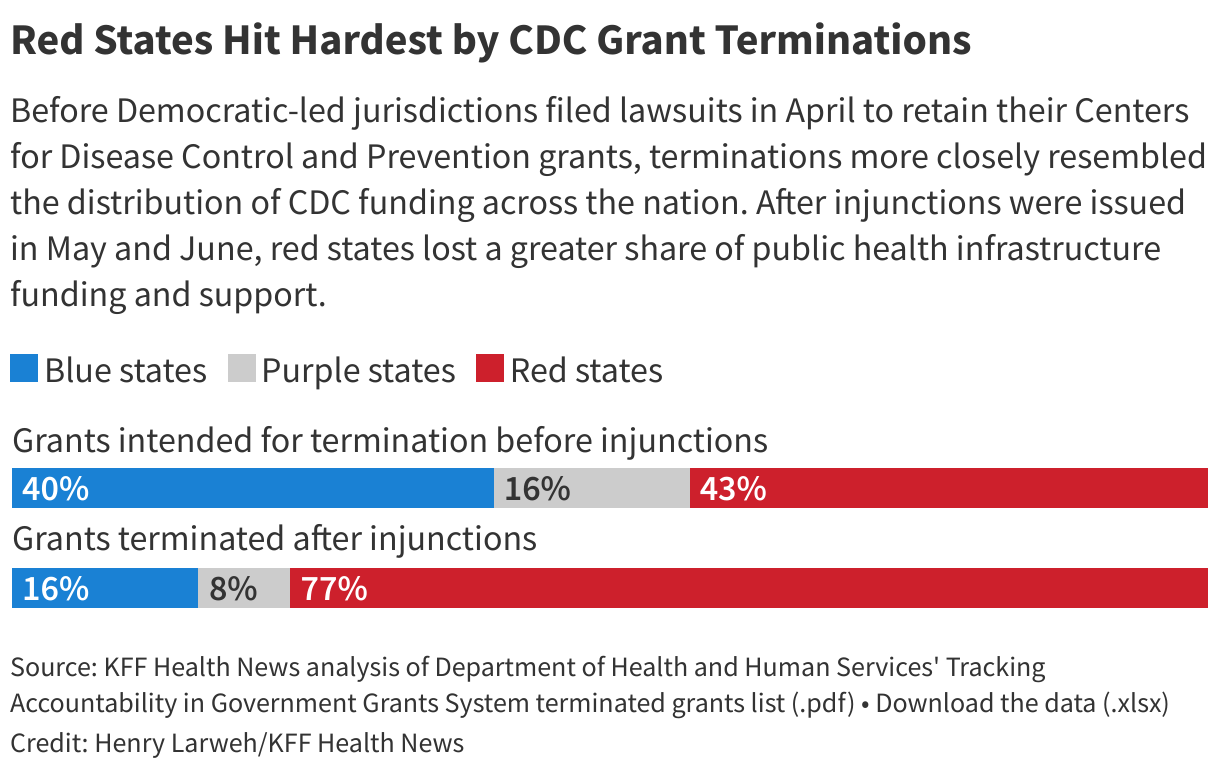
Initially, grant cancellations hit blue and red states roughly evenly. Four of the five jurisdictions with the largest number of terminated grants were led by Democrats: California, the District of Columbia, Illinois, and Massachusetts.
But after attorneys general and governors from about two dozen blue states sued in federal court and won an injunction, the balance flipped. Of the five states with the most canceled grants, four are led by Republicans: Texas, Georgia, Oklahoma, and Ohio.
In blue states, nearly 80% of the CDC grant cuts have been restored, compared with fewer than 5% in red states, according to the ║┌┴╧│╘╣╧═Ї News analysis. Grant amounts reported in an HHS database known as the Tracking Accountability in Government Grants System, or TAGGS, often don’t match what states confirmed. Instead, this analysis focused on the number of grants.
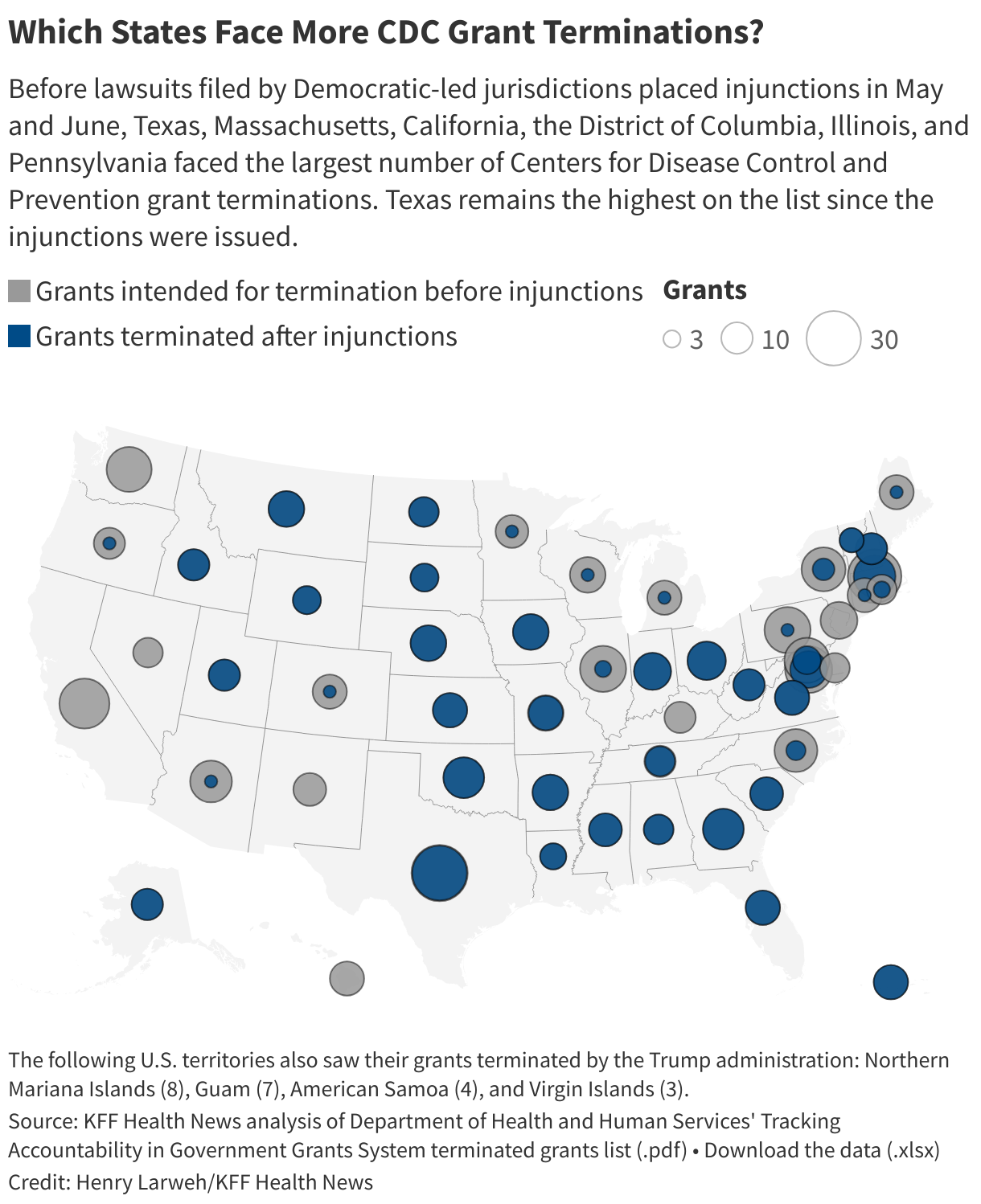
The divide is an example of the polarization that permeates health care issues, in which access to safety-net health programs, abortion rights, and the ability of public health officials to respond to disease threats diverge significantly depending on the political party in power.
In an emailed statement, HHS spokesperson Andrew Nixon said the agency “is committed to protecting the health of every American, regardless of politics or geography. These funds were provided in response to the COVID pandemic, which is long over. We will continue working with states to strengthen public health infrastructure and ensure communities have the tools they need to respond to outbreaks and keep people safe.”
The money in question wasn’t spent solely on covid-related activities, public health experts say; it was also used to bolster public health infrastructure and help contain many types of viruses and diseases, including the flu, measles, and RSV, or respiratory syncytial virus.
“It really supported infrastructure across the board, particularly in how states respond to public health threats,” said Susan Kansagra, chief medical officer of the Association of State and Territorial Health Officials.
The Trump cutbacks came as the U.S. recorded its largest measles outbreak in over three decades and 266 pediatric deaths during the most recent flu season — the outside of a pandemic since 2004. Public health departments canceled vaccine clinics, laid off staff, and put contracts on hold, health officials said in interviews.
After its funding cuts were blocked in court, California retained every grant the Trump administration attempted to claw back, while Texas remains the state with the most grants terminated, with at least 30. As the CDC slashed grants in Texas, its measles outbreak spread across the U.S. and Mexico, sickening at least 4,500 people and killing at least 16.
Colorado, which joined the lawsuit, had 11 grant terminations at first, but then 10 were retained. Meanwhile, its neighboring states that didn’t sue — Wyoming, Utah, Kansas, Nebraska, and Oklahoma — collectively lost 55 grants, with none retained.
In Jackson, Ohio, a half-dozen community health workers came to work one day in March to find the Trump administration had canceled their grant five months early, leaving the Jackson County Health Department half a million dollars short — and them without jobs.
“I had to lay off three employees in a single day, and I haven’t had to do that before. We don’t have those people doing outreach in Jackson County anymore,” Health Commissioner Kevin Aston said.
At one point, he said, the funding helped 11 Appalachian Ohio counties. Now it supports one.
Marsha Radabaugh, one employee who was reassigned, has scaled back her community health efforts: She’d been helping serve hot meals to homeless people and realized that many clients couldn’t read or write, so she brought forms for services such as Medicaid and the Supplemental Nutrition Assistance Program to their encampment in a local park and helped fill them out.
“We would find them rehab places. We’d get out hygiene kits, blankets, tents, zero-degree sleeping bags, things like that,” she said. As a counselor, she’d also remind people “that they’re cared for, that they’re worthy of being a human — because, a lot of the time, they’re not treated that way.”
Sasha Johnson, who led the community health worker program, said people like Radabaugh “were basically a walking human 411,” offering aid to those in need.
Radabaugh also partnered with a food bank to deliver meals to homebound residents.
Aston said the abrupt way they lost the funds — which meant the county unexpectedly had to pay unemployment for more people — could have ruined the health district financially. Canceling funding midcycle, he said, “was really scary.”
HHS Secretary Robert F. Kennedy Jr., a longtime anti-vaccine activist and promoter of vaccine misinformation, a “cesspool of corruption.” At HHS, he has taken steps to undermine vaccination in the U.S. and abroad.
Federal CDC funding accounts for of state and local health department budgets, according to KFF, a health information nonprofit that includes ║┌┴╧│╘╣╧═Ї News. States that President Donald Trump won in the 2024 election received a higher share of the in fiscal 2023 than those that Democrat Kamala Harris won, according to KFF.
The Trump administration’s nationwide CDC grant terminations reflect this. More than half were in states that Trump won in 2024, totaling at least 370 terminations before the court action, according to ║┌┴╧│╘╣╧═Ї News’ analysis.
The Columbus, Ohio, health department had received $6.2 million in CDC grants, but roughly half of it — $3 million — disappeared with the Trump cuts. The city laid off 11 people who worked on investigating infectious disease outbreaks in such places as schools and nursing homes, Columbus Health Commissioner Mysheika Roberts said.
She also said the city had planned to buy a new electronic health record system for easier access to patients’ hospital records — which could improve disease detection and provide better treatment for those infected — but that was put on ice.
“We’ve never had a grant midcycle just get pulled from us for no reason,” Roberts said. “This sense of uncertainty is stressful.”
Columbus did not receive its money directly from the CDC. Rather, the state gave the city some funds it received from the federal government. Ohio, led by Republican Gov. Mike DeWine and a Republican attorney general, did not sue to block the funding cuts.
Columbus to keep its money, along with other Democratic-led municipalities in Republican-governed states: Harris County, Texas, home to Houston; the Metropolitan Government of Nashville and Davidson County in Tennessee; and Kansas City, Missouri. A federal judge in June blocked those cuts.
As of mid-August, Columbus was awaiting the funds. Roberts said the city won’t rehire staff because the federal funding was expected to end in December.
Joe Grogan, a senior scholar at the University of Southern California’s Schaeffer Institute and former director of the White House Domestic Policy Council in Trump’s first term, said state and local agencies “are not entitled” to the federal money, which was awarded “to deal with an emergency” that has ended.
“We were throwing money out the door the last five years,” Grogan said of the federal government. “I don’t understand why there would ever be a controversy in unspent covid money coming back.”
Ken Gordon, Ohio Department of Health spokesperson, wrote in an email that the $250 million in grants lost had helped with, among other things, upgrading the disease reporting system and boosting public health laboratory testing.
Some of the canceled HHS funding wasn’t slated to end for years, including four grants to strengthen public health in Indian Country, a grant to a Minnesota nonprofit focused on reducing substance use disorders, and a few to universities about occupational safety, HIV, tuberculosis, and more.
Brent Ewig, chief policy and government relations officer for the Association of Immunization Managers, said the cuts were “the predictable result of ‘boom, bust, panic, neglect’ funding” for public health.
The association represents 64 state, local, and territorial immunization programs, which Ewig said will be less prepared to respond to disease outbreaks, including measles.
“The system is blinking red,” Ewig said.
Methodology
║┌┴╧│╘╣╧═Ї News’ analysis of Centers for Disease Control and Prevention grants sought to answer four questions: 1) How many grants have been terminated in the U.S. under the Trump administration since March? 2) Which states saw the most grants cut? 3) What were the grants for? and 4) Did the grant terminations affect blue, red, and purple states differently? This follows a similar analysis by ║┌┴╧│╘╣╧═Ї News for an article on nationwide NIH grant terminations.
Our primary data source was a Department of Health and Human Services website showing grant terminations. We compared an initial list of grant terminations from April 3 with one from July 11 to determine how many grants had been restored. The USAspending.gov database helped us track grants by state.
To classify states politically, we followed the same steps from our April coverage of National Institutes of Health grant terminations. States were “blue” if Democrats had complete control of the state government or if the majority of voters favored Democratic presidential candidates in the last three elections (2016, 2020, 2024). “Red” states were classified similarly with respect to the Republican Party. “Purple” states had politically split state governments and/or were generally considered to be presidential election battleground states. The result was 25 red states, 17 blue states, and eight purple states. The District of Columbia was classified as blue using similar methods.
This analysis does not account for potential grant reinstatements in local jurisdictions where the funds were awarded indirectly rather than directly from the CDC; it accounts only for the recipients’ location, and excludes grants terminated from Compacts of Free Association states and other foreign entities that received grants directly from the CDC. At least 40 CDC grants were terminated that were meant for global health efforts or assisting public health activities in other nations following the for the CDC to withdraw support for the World Health Organization.
This <a target="_blank" href="/courts/cdc-grant-trump-clawbacks-blue-red-state-comparison/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2078985&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Silva’s daughter was on Medicaid, which was supposed to cover the cost of the ambulances. But one of the three ambulance companies, Northglenn Ambulance, a public company since , sent Silva’s bill to a debt collector. It was for $2,181.60, which grew to more than $3,000 with court fees and interest, court records show. The preschool teacher couldn’t pay, and the collector garnished Silva’s wages.
“It put us so behind on bills тАФ our house payment, electric, phone bills, food for the kids,” said Silva, whose daughter recovered fully from the 2015 crash. “It took away from everything.”
Some state legislators are looking to curb bills like the one she received тАФ surprise bills for ground ambulance rides.
When an ambulance company charges more than an insurer is willing to pay, patients can be left with a big bill they probably had no choice in.
States are trying to fill a gap left by the federal , which covers air ambulances but not ground services, including ambulances that travel by road and water. This year, Utah and North Dakota joined that have passed protections against surprise billing for such rides.
Those protections often include setting a minimum for insurers to pay out if someone they cover needs a ride. But the sticking point is where to set that bar. Legislation in Colorado and Montana stalled this year because policymakers worried that forcing insurers to pay more would lead to higher health coverage costs for everyone.
Surprise ambulance bills are one piece of a health care system that Americans with medical debt, straining their finances, preventing them from accessing care, and increasing racial disparities, as ║┌┴╧│╘╣╧═Ї News has reported.
“If people are hesitating to call the ambulance because they’re worried about putting a huge financial burden on their family, it means we’re going to get stroke victims who don’t get to the hospital on time,” said , who directs health care campaigns at PIRG, a national consumer advocacy group. “It means that person who’s worried it might be a heart attack won’t call.”
The No Surprises Act, signed into law by President Donald Trump in 2020, says that for most emergency services, patients can be billed for out-of-network care only for the same amount they would have been billed if it were in-network. Like doctors or hospitals, ambulance companies can contract with insurers, making them in-network. Those that don’t remain out-of-network.
But unlike when making an appointment with a doctor or planning a surgery, a patient generally can’t choose the ambulance company that will respond to their 911 call. This means they can get hit with large out-of-network bills.
Federal lawmakers punted on including ground ambulances, in part because of the variety of business models тАФ from private companies to volunteer fire departments тАФ and a lack of data on how much rides cost.
Instead, Congress created an that issued recommendations last year. Its overarching conclusion тАФ that patients shouldn’t be stuck in the crossfire between providers and payers тАФ was not controversial or partisan. In Colorado, aimed at expanding protections from surprise ambulance bills got a unanimous thumbs-up in both legislative chambers.
Colorado had previously protecting people from surprise bills from private ambulance companies. This new measure was aimed at providing similar protections against bills from public ambulance services and for transfers between hospitals.
“We knew it had bipartisan support, but there are some people that vote no on everything,” said a pleasantly surprised , a Democratic state representative.
A less pleasant surprise came later, when Gov. Jared Polis, who is also a Democrat, vetoed it, citing the fear of rising premiums.
States can do only so much on this issue, because state laws apply only to state-regulated health plans. That leaves out a lot of workers. According to a by KFF, a health information nonprofit that includes ║┌┴╧│╘╣╧═Ї News, 63% of people who work for private employers and get health insurance through their jobs have , which aren’t state-regulated.
“It’s why we need a federal ambulance protection law, even if we passed 50 state laws,” Kelmar said.
According to data from the Colorado secretary of state’s office, the only lobbying groups the bill were Anthem and UnitedHealth Group, plus UnitedHealth subsidiaries Optum and UnitedHealthcare.
As soon as the legislative session ended in May, , executive director of the Colorado Association of Health Plans, a trade group representing health insurance companies in the state, sent a requesting a veto, with an estimate that the legislation would result in premiums rising 0.4%.
The Colorado bill said local governments тАФ such as cities, counties, or special districts тАФ would set rates.
“We are in a much better place by not having local entities set their own rates,” McFatridge told ║┌┴╧│╘╣╧═Ї News. “That’s almost like the fox managing the henhouse.”
, an emeritus research professor with Georgetown University’s McCourt School of Public Policy, said it isn’t clear whether state laws approved elsewhere are raising premiums, or if so by how much. Hoadley said Washington state is expected to come out with an impact analysis of its law in a couple of years.
The national trade association for insurance companies declined to provide a comment for this article. Instead, AHIP forwarded letters that its leaders submitted to lawmakers , , and this year opposing measures in each state to set base ambulance rates. AHIP leadership described the proposals as inflated, government-mandated pricing that would reduce insurers’ chance to negotiate fair prices. Ultimately, the association warned, the proposed minimums would increase health care costs.
In Montana, legislators a minimum reimbursement for ground ambulances of 400% of what Medicare pays, or at a set local rate if one exists. The proposal was sponsored by two Republicans and backed by ambulance companies. Health insurers successfully lobbied against it, arguing that the price was too steep.
Sarah Clerget, a lobbyist representing AHIP, told Montana lawmakers in a legislative hearing that it’s already hard to get ambulance companies to go in-network with insurers, “because folks are going to need ambulance care regardless of whether their insurance company will cover it.” She said the state’s proposal would leave those paying for health coverage with the burden of the new price.
“None of us like our insurance rates to move,” Republican state Sen. said during a legislative meeting as a committee tabled the bill. He equated the proposed minimum to a mandate that could lead to people having to pay more for health coverage for an important but nonetheless niche service.
Colorado’s governor was similarly focused on premiums. Polis said in his that the legislation would have raised premiums between 73 cents and $2.15 per member per month.
“I agree that filling this gap in enforcement is crucial to saving people money on health care,” he wrote. “However, those cost savings are outweighed in my view by the premium increases.”
, policy director at the Colorado Consumer Health Initiative, which supported the bill, said that even if premiums did rise, Coloradans might be OK with the change. After all, she said, they’d be trading the threat of a big ambulance bill for the price of half a cup of coffee per month.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/ground-ambulance-surprise-billing-colorado-montana-insurer-pushback-premiums/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2055593&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>LISTEN: Some scientists say the Trump administration’s decision to cancel hundreds of National Institutes of Health grants will set back efforts to tackle public health challenges like HIV. On June 11, WAMU’s “Health Hub” featured ║┌┴╧│╘╣╧═Ї News correspondent Rae Ellen Bichell to explain how the spending cuts are being felt across the country.
An analysis by ║┌┴╧│╘╣╧═Ї News found that the Trump administration’s cuts to the National Institutes of Health have been felt in both red and blue states, across political and geographic lines. Scientists warn these cuts will stall progress on urgent health issues and could set back care for vulnerable communities.
More reductions in health research spending could be ahead. The Trump administration’s for next year calls on Congress to slash the NIH budget more than 40%.
║┌┴╧│╘╣╧═Ї News correspondent Rae Ellen Bichell appeared on WAMU’s “Health Hub” on June 11 to explain how these cuts could set back research for years to come.
║┌┴╧│╘╣╧═Ї News audio producer Taylor Cook contributed reporting to this segment.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/news/wamu-health-hub-nih-research-grants-canceled-federal-cuts/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2048334&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>A ║┌┴╧│╘╣╧═Ї News analysis underscores that the terminations are sparing no part of the country, politically or geographically. About 40% of organizations whose grants the NIH cut in its first month of slashing, which started Feb. 28, are in states Trump won in November.
The Trump administration has singled out Ivy League universities including Columbia and Harvard for broad federal funding cuts. But the spending reductions at the NIH, the nation’s foremost source of funding for biomedical research, go much further: Of about 220 organizations that had grants terminated, at least 94 were public universities, including flagship state schools in places such as Florida, Georgia, Ohio, Nebraska, and Texas.
The Trump administration has canceled hundreds of grants supporting research on topics such as vaccination; diversity, equity, and inclusion; and the health of LGBTQ+ populations. Some of the terminations are a result of Trump’s executive orders to abandon federal work on diversity and equity issues. Others followed the Senate confirmation of anti-vaccine activist Robert F. Kennedy Jr. to lead the Department of Health and Human Services, which oversees the NIH. Many mirror the ambitions laid out in Project 2025’s “Mandate for Leadership,” for Trump’s second term.
Affected researchers say Trump administration officials are taking a cudgel to efforts to improve the lives of people who often experience worse health outcomes — ignoring a scientific reality that diseases and other conditions do not affect all Americans equally.
║┌┴╧│╘╣╧═Ї News found that the NIH terminated about 780 grants or parts of grants between Feb. 28 and March 28, published by the Department of Health and Human Services and a . Some grants were canceled in full, while in other cases, only supplements — extra funding related to the main grant, usually for a shorter-term, related project — were terminated.
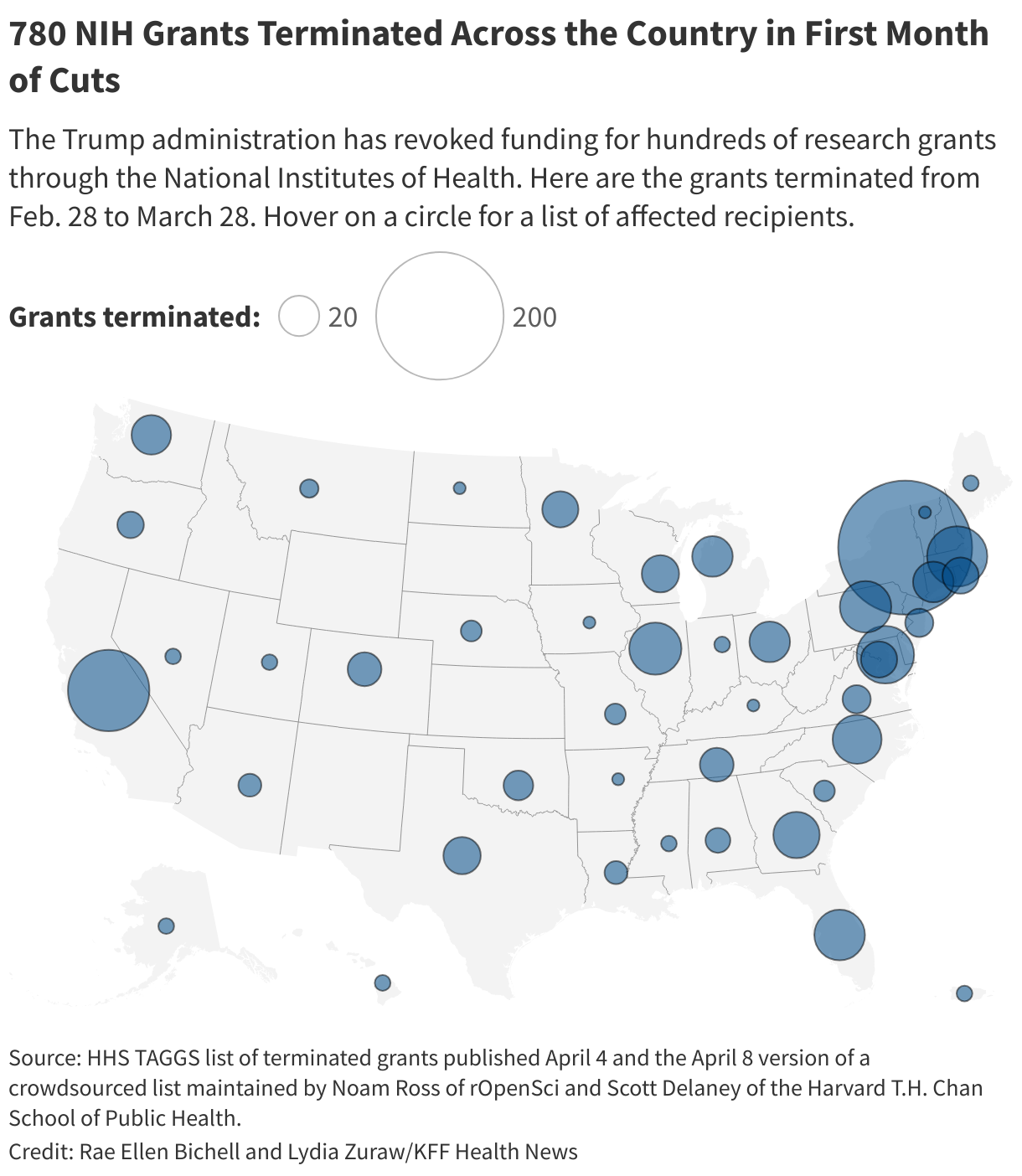
Among U.S. recipients, 96 of the institutions that lost grants in the first month are in politically conservative states including Florida, Ohio, and Indiana, where Republicans control the state government or voters reliably support the GOP in presidential campaigns, or in purple states such as North Carolina, Michigan, and Pennsylvania that were presidential battleground states. An additional 124 institutions are in blue states.
Sybil Hosek, a research professor at the University of Illinois-Chicago, helps run a network that focuses on improving care for people 13 to 24 years old who are living with or at risk for HIV. The NIH $73 million to lead the HIV project.
“We never thought they would destroy an entire network dedicated to young Americans,” said Hosek, one of the principal investigators of the Adolescent Medicine Trials Network for HIV/AIDS Interventions. The termination “doesn’t make sense to us.”
is director of the Office of Policy for Extramural Research Administration, which oversees grants policy and compliance across NIH institutes. In terminating the grant March 21, Bulls wrote that research “based primarily on artificial and nonscientific categories, including amorphous equity objectives, are antithetical to the scientific inquiry, do nothing to expand our knowledge of living systems, provide low returns on investment, and ultimately do not enhance health, lengthen life, or reduce illness.”
Adolescents and young adults ages 13 to 24 accounted for new HIV infections in the U.S. in 2022, according to the Centers for Disease Control and Prevention.
“It’s science in its highest form,” said Lisa Hightow-Weidman, a professor at Florida State University who co-leads the network. “I don’t think we can make America healthy again if we leave youth behind.”
HHS spokesperson Emily Hilliard said in an emailed statement that “NIH is taking action to terminate research funding that is not aligned with NIH and HHS priorities.” The NIH and the White House didn’t respond to requests for comment.
“As we begin to Make America Healthy Again, it’s important to prioritize research that directly affects the health of Americans. We will leave no stone unturned in identifying the root causes of the chronic disease epidemic as part of our mission to Make America Healthy Again,” Hilliard said.
Harm to HIV, Vaccine Studies
The NIH, with its nearly $48 billion annual budget, is the largest public funder of biomedical research in the world, awarding nearly 59,000 grants in the 2023 fiscal year. The Trump administration has upended funding for projects that were already underway, stymied money for new applications, and sought to reduce how much recipients can spend on overhead expenses.
Those changes — plus the firing of 1,200 agency employees as part of mass layoffs across the government — are alarming scientists and NIH workers, who warn that they will undermine progress in combating diseases and other threats to the nation’s public health. On April 2, the American Public Health Association, Ibis Reproductive Health, and affected researchers, among others, in federal court against the NIH and HHS to halt the grant cancellations.
Two National Cancer Institute employees, who were granted anonymity because they were not authorized to speak to the press and feared retaliation, said its staff receives batches of grants to terminate almost daily. On Feb. 27, the cancer institute had more than 10,800 active projects, the highest share of the NIH’s roughly two dozen institutes and centers, according to the NIH’s website. At least 47 grants that NCI awarded were terminated in the first month.
Kennedy has said the NIH should take a years-long pause from funding infectious disease research. In November 2023, he told an anti-vaccine group, “I’m gonna say to NIH scientists, ‘God bless you all. Thank you for public service. We’re going to give infectious disease a break for about eight years,’” .
For years, Kennedy has peddled falsehoods about vaccines — including that “” is “safe and effective,” and that “” showing a connection between vaccines and autism, a link that has repeatedly been debunked — and that HIV is not the only cause of AIDS.
║┌┴╧│╘╣╧═Ї News found that grants in blue states were disproportionately affected, making up roughly two-thirds of terminated grants, many of them at Columbia University. The university had more grants terminated than all organizations in politically red states combined. On April 4, Democratic attorneys general in 16 states to block the agency from canceling funds.
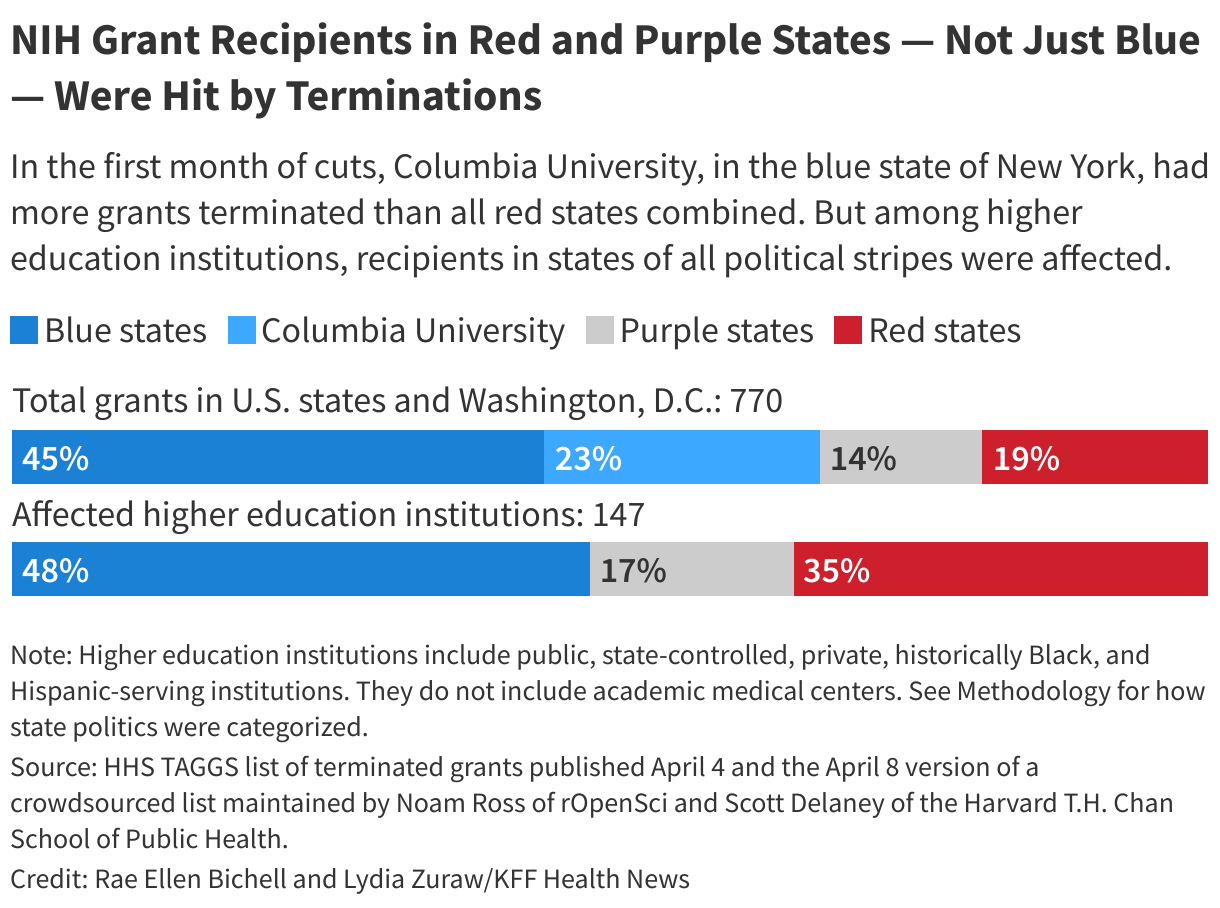
Researchers whose funding was stripped said they stopped clinical trials and other work on improving care for people with HIV, reducing vaping and smoking rates among LGBTQ+ teens and young adults, and increasing vaccination rates for young children. NIH grants routinely span several years.
For example, Hosek said that when the youth HIV/AIDS network’s funding was terminated, she and her colleagues were preparing to launch a clinical trial examining whether a particular antibiotic that is effective for men to prevent sexually transmitted infections would also work for women.
“This is a critically important health initiative focused on young women in the United States,” she said. “Without that study, women don’t have access to something that men have.”
Other scientists said they were testing how to improve health outcomes among newborns in rural areas with genetic abnormalities, or researching how to improve flu vaccination rates among Black children, who are to be hospitalized and die from the virus than non-Hispanic white children.
“It’s important for people to know that — if, you know, they are wondering if this is just a waste of time and money. No, no. It was a beautiful and rare thing that we did,” said Joshua Williams, a pediatric primary care doctor at Denver Health in Colorado who was researching whether about harm experienced due to vaccine-preventable diseases — from missed birthdays to hospitalizations and job loss — might inspire caregivers to get their children vaccinated against the flu.
He and his colleagues had recruited 200 families, assembled a community advisory board to understand which vaccinations were top priorities, created short videos with people who had experienced vaccine-preventable illness, and texted those videos to half of the caregivers participating in the study.
They were just about to crack open the medical records and see if it had worked: Were the group who received the videos more likely to follow through on vaccinations for their children? That’s when he got the notice from the NIH.
“It is the policy of NIH not to prioritize research activities that focuses gaining scientific knowledge on why individuals are hesitant to be vaccinated and/or explore ways to improve vaccine interest and commitment,” the notice read.
Williams said the work was already having an impact as other institutions were using the idea to start projects related to cancer and dialysis.
A Hit to Rural Health
Congress previously tried to ensure that NIH grants also went to states that historically have had less success obtaining biomedical research funding from the government. Now those places aren’t immune to the NIH’s terminations.
Sophia Newcomer, an associate professor of public health at the University of Montana, said she had 18 months of work left on a study examining undervaccination among infants, which means they were late in receiving recommended childhood vaccines or didn’t receive the vaccines at all. Newcomer had been analyzing 10 years of CDC data about children’s vaccinations and that most U.S. infants from 0 to 19 months old were not adequately vaccinated.
Her grant was terminated March 10, with the NIH letter stating the project “no longer effectuates agency priorities,” a phrase replicated in other termination letters ║┌┴╧│╘╣╧═Ї News has reviewed.
“States like Montana don’t get a lot of funding for health research, and health researchers in rural areas of the country are working on solutions to improve rural health care,” Newcomer said. “And so cuts like this really have an impact on the work we’re able to do.”
Montana is one of 23 states, along with Puerto Rico, that are eligible for the NIH’s , meant to bolster NIH funding in states that historically have received less investment. Congress established the program in 1993.
The NIH’s grant terminations hit institutions in 15 of those states, more than half that qualify, plus Puerto Rico.
Researchers Can’t ‘Just Do It Again Later’
The NIH’s research funds are deeply entrenched in the U.S. health care system and academia. Rarely does an awarded grant stay within the four walls of a university that received it. One grant’s money is divvied up among other universities, hospitals, community nonprofits, and other government agencies, researchers said.
Erin Kahle, an infectious disease epidemiologist at the University of Michigan, said she was working with Emory University in Georgia and the CDC as part of her study. She was researching the impact of intimate partner violence on HIV treatment among men living with the virus. “They are relying on our funds, too,” she said.
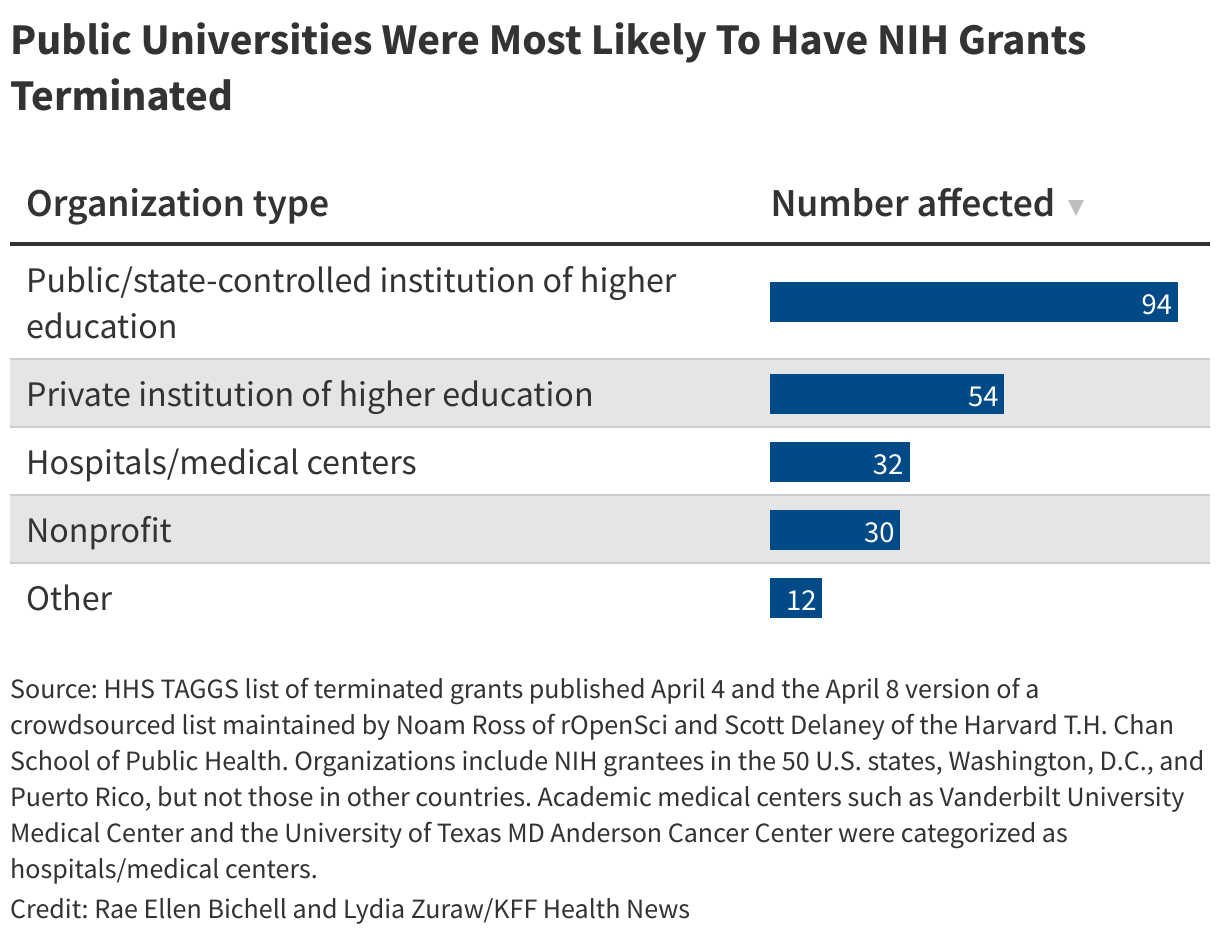
Kahle said her top priority was to ethically and safely wind down her nationwide study, which included 418 people, half of whom were still participating when her grant was terminated in late March. Kahle said that includes providing resources to participants for whom sharing experiences of intimate partner violence may cause trauma or mental health distress.
Rachel Hess, the co-director of the Clinical & Translational Science Institute at the University of Utah, said the University of Nevada-Reno and Intermountain Health, one of the largest hospital systems in the West, had received funds that was awarded to the University of Utah and was terminated March 12.
The institute, which aims to make scientific research more efficient to speed up the availability of treatments for patients, supported over 5,000 projects last year, including 550 clinical trials with 7,000 participants. Hess said that, for example, the institute was helping design a multisite study involving people who have had heart attacks to figure out the ideal mix of medications “to keep them alive” before they get to the hospital, a challenge that’s more acute in rural communities.
After pushback from the university — the institute’s projects included work to reduce health care disparities between rural and urban areas — the NIH restored its grant March 29.
Among the people the Utah center about the reversal were the state’s congressional delegation, which consists entirely of Republican lawmakers. “We are grateful to University of Utah leadership, the University of Utah Board of Trustees, our legislative delegation, and the Utah community for their support,” it said.
Hilliard, of HHS, said that “some grants have been reinstated following the appeals process, and the agency will continue to carry out the remaining appeals as planned to determine their alignment.” She declined to say how many had been reinstated, or why the University of Utah grant was among them.
Other researchers haven’t had the same luck. Kahle, in Michigan, said projects like hers can take a dozen years from start to finish — applying for and receiving NIH funds, conducting the research, and completing follow-up work.
“Even if there are changes in the next administration, we’re looking at at least a decade of setting back the research,” Kahle said. “It’s not as easy as like, ‘OK, we’ll just do it again later.’ It doesn’t really work that way.”
Methodology
║┌┴╧│╘╣╧═Ї News analyzed National Institutes of Health grant data to determine the states and organizations most affected by the Trump administration’s cuts.
We tallied the number of terminated NIH grants using two sources: a Department of Health and Human Services list of published April 4; and maintained by Noam Ross of rOpenSci and Scott Delaney of the Harvard T.H. Chan School of Public Health, as of April 8. We focused on the first month of terminations: from Feb. 28 to March 28. We found that 780 awards were terminated in total, with 770 of them going to recipients based in U.S. states and two to recipients in Puerto Rico.
The analysis does not account for potential grant reinstatements, which we know happened in at least one instance.
Additional information on the recipients, such as location and business type, came from the USAspending.gov .
There were 222 U.S. recipients in total. At least 94 of them were public higher education institutions. Forty-one percent of organizations that had NIH grants cut in the first month were in states that President Donald Trump won in the 2024 election.
Some recipients, including the University of Texas MD Anderson Cancer Center and Vanderbilt University Medical Center, are medical facilities associated with higher education institutions. We classified these as hospitals/medical centers.
We also wanted to see whether the grant cuts affected states across the political spectrum. We generally classified states as blue if Democrats control the state government or Democratic candidates won them in the last three presidential elections, and red if they followed this pattern but for Republicans. Purple states are generally presidential battleground states or those where voters regularly split their support between the two parties: Arizona, Michigan, Nevada, New Hampshire, North Carolina, Pennsylvania, Virginia, and Wisconsin. The result was 25 red states, 17 blue states, and eight purple states. The District of Columbia was also blue.
We found that, of affected U.S. institutions, 96 were in red or purple states and 124 were in blue states.
║┌┴╧│╘╣╧═Ї News intern Henry Larweh contributed to this report.
This <a target="_blank" href="/health-industry/nih-grant-cuts-red-states-science-research-vaccines-hiv-trump-rfk/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2016404&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>In recent years, states across the Mountain West have passed laws that limit doctors from providing transgender children with certain kinds of gender-affirming care, from prohibitions on surgery to bans on puberty blockers and hormones. Colorado families say their state was a haven for those health services for a long time, but following executive orders from the Trump administration, even hospitals in Colorado limited the care they offer for trans patients under age 19. ║┌┴╧│╘╣╧═Ї News Colorado correspondent Rae Ellen Bichell spoke with youth and their families.
GRAND JUNCTION, Colo. тАФ On a Friday after school, 6-year-old Esa Rodrigues had unraveled a ball of yarn, spooked the pet cat, polled family members about their favorite colors, and tattled on a sibling for calling her a “butt-face mole rat.”
Next, she was laser-focused on prying open cherry-crisp-flavored lip gloss with her teeth.
“Yes!” she cried, twisting open the cap. Esa applied the gloopy, shimmery stuff in her bedroom, where a large transgender pride flag hung on the wall.
Esa said the flag makes her feel “important” and “happy.” She’d like to take it down from the wall and wear it as a cape.
Her parents questioned her identity at first, but not anymore. Before, their anxious child dreaded going to school, bawled at the barbershop when she got a boy’s haircut, and curled into a fetal position on the bathroom floor when she learned she would never get a period.
Now, that child is happily bounding up a hill, humming to herself, wondering aloud if fairies live in the little ceramic house she found perched on a stone.



Her mom, Brittni Packard Rodrigues, wants this joy and acceptance to stay. Depending on a combination of Esa’s desire, her doctors’ recommendations, and when puberty sets in, that might require puberty blockers, followed by estrogen, so that Esa can grow into the body that matches her being.
“In the long run, blockers help prevent all of those surgeries and procedures that could potentially become her reality if we don’t get that care,” Packard Rodrigues said.
The medications known as puberty blockers are for conditions that include prostate cancer, endometriosis, infertility, and puberty that sets in too early. Now, the Trump administration is seeking to limit their use specifically for transgender youth.
Esa’s home state of Colorado has long been known as a haven for gender-affirming care, which the state considers legally protected and an essential health insurance benefit. Medical exiles have for such treatment in the past few years. As early as the 1970s, the town of Trinidad became known as “the sex-change capital of the world” when a cowboy-hat-wearing former Army surgeon, , made his mark performing gender-affirming surgeries for adults.
On his first day in office, President Donald Trump signed an refuting the existence of transgender people by saying it is a “false claim that males can identify as and thus become women and vice versa.” The following week, he calling puberty blockers and hormones for anyone under age 19 a form of chemical “mutilation” and “a stain on our Nation’s history.” It directed agencies to take steps to ensure that recipients of federal research or education grants stop providing it.
Subsequently, health care organizations in Colorado; California; Washington, D.C.; and elsewhere announced they would preemptively comply. In Colorado, that included three major health care organizations: Children’s Hospital Colorado, Denver Health, and UCHealth. At the end of January and in early February, the three systems announced changes to the gender-affirming care they provide to patients under 19, effective immediately: no new hormone or puberty blocker prescriptions for patients who hadn’t had them before, limited or no prescription renewals for those who had, and no surgeries, though Children’s Hospital had never offered it, and such surgery is : For every 100,000 trans minors, fewer than three undergo surgery.
Children’s Hospital and Denver Health resumed offering puberty blockers and hormones on Feb. 24 and Feb. 19, respectively, after Colorado joined a U.S. District Court state. The court concluded that Trump’s orders relating to gender “discriminate on the basis of transgender status and sex.” It granted a preliminary injunction blocking them from taking effect in the four states involved in the lawsuit.
Surgeries, however, have not resumed. Denver Health said it will “continue its pause on gender-affirming surgeries for patients under 19 due to patient safety and given the uncertainty of the legal and regulatory landscape.”
UCHealth has resumed neither medication nor surgery for those under 19. “Our providers are awaiting a more permanent decision from federal courts that may resolve the uncertainty around providing this care,” spokesperson Kelli Christensen wrote.
Trans youth and their families said the court ruling and the two Colorado health systems’ decisions to resume treatments haven’t resolved matters. It has bought them time to stockpile prescriptions, to try to find private practice physicians with the right training to monitor blood work and adjust prescriptions accordingly, and, for some, to work out the logistics of moving to another state or country.
The Trump administration has continued to press health providers beyond the initial executive orders by threatening to withhold or cancel federal money awarded to them. In early March, the Health Resources and Services Administration funding for graduate medical education at children’s hospitals.
║┌┴╧│╘╣╧═Ї News requested comment from White House deputy press secretary Kush Desai but did not receive a response. HHS deputy press secretary Emily Hilliard responded with links to two prior .
Medical interventions are just one type of gender-affirming care, and the process to get treatment is . Researchers have found that, even among those with private insurance, to receive puberty blockers and hormones. Interestingly, most gender-affirming breast reduction surgeries performed on men and boys are done on cisgender тАФ not transgender тАФ patients.
Kai, 14, wishes he could have gone on puberty blockers. He lives in Centennial, a Denver suburb. ║┌┴╧│╘╣╧═Ї News is not using his full name because his family is worried about him being harassed or targeted.

Kai got his period when he was 8 years old. By the time he realized he was transgender, in middle school, it was too late to start puberty blockers.
His doctors prescribed birth control to , so he wouldn’t be reminded each month of his gender dysphoria. Then, once he turned 14, he started taking testosterone.
Kai said if he didn’t have hormone therapy now, he would be a danger to himself.
“Being able to say that I’m happy in my body, and I get to be happy out in public without thinking everyone’s staring at me, looking at me weird, is such a huge difference,” he said.
His mom, Sherry, said she is happy to see Kai relax into the person he is.
Sherry, who asked to use her middle name to prevent her family from being identified, said she started stockpiling testosterone the moment Trump got elected but hadn’t thought about what impact there would be on the availability of birth control. Yet after the executive orders, that prescription, too, became tenuous. Sherry said Kai’s doctor at UCHealth had to set up a special meeting to confirm the doctor could keep prescribing it.
So, for now, Kai has what he needs. But to Sherry, that is cold comfort.
“I don’t think that we are very safe,” she said. “These are just extensions.”
The family is coming up with a plan to leave the country. If Sherry and her husband can get jobs in New Zealand, they’ll move there. Sherry said such mobility is a privilege that many others don’t have.
For example, David, an 18-year-old student at Western Colorado University in the Rocky Mountain town of Gunnison. He asked to be identified only by his middle name because he worries he could be targeted in this conservative, rural town.



David doesn’t have a passport, but even if he did, he doesn’t want to leave Gunnison, he said. He is studying geology, is learning to play the bass, and has a good group of friends. He has plans to become a paleontologist.
His dorm room shelves are scattered with his essentials: fossils, Old Spice deodorant, microwave macaroni and cheese. But there are no mirrors. David said he got in the habit of avoiding them.
“For the longest time, I just had so much body dysphoria and dysmorphia that it can be kind of hard to look in the mirror,” David said. “But when I do, most of the time, I see something that I really like.”
He’s been taking testosterone for three years, and the hormone helped him grow a beard. In January, his doctor at Denver Health was told to stop prescribing it. His mom drove hours from her home to Gunnison to deliver the news in person.
That prescription is back on track now, but the mastectomy he’d planned for this summer isn’t. He’d hoped to have adequate recovery time before sophomore year. But he doesn’t know anyone in Colorado who would perform it until he is 19. He could easily get surgery to enhance his breasts, but he must seek surgical options in other states to reduce or remove them.
“Colorado as a state was supposed to be a safe haven,” said his mother, Louise, who asked to be identified by her middle name. “We have a law that makes it a right for trans people to have health care, and yet our health care systems are taking that away.”
It has taken eight years and about 10 medical providers and therapists to get David this close to the finish line. That’s a big deal after living through so many years of dysphoria and dysmorphia.
“I’m still going, and I’m going to keep going, and there’s almost nothing they can do to stop me тАФ because this is who I am,” David said. “There have always been trans people, and there always will be trans people.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/courts/transgender-youth-gender-affirming-care-colorado-trump-executive-order/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2009419&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>