McLeod, who lives near Charleston, South Carolina, is still paying off chemotherapy bills that followed her 2017 diagnosis. She also now faces an onslaught of out-of-pocket costs for follow-up monitoring and care, including regular visits to a pulmonologist and allergist.
McLeod, 45, said she had already spent $2,500 in the first two months of the year and owes an additional $1,300 from a January colonoscopy. That’s on top of the $895 monthly premium for a health insurance plan that covers her family of six.
Those costs have led McLeod to ration her other care. Despite feeling intense chest pain since February, for example, she is putting off a CT scan and a visit to a heart specialist.
“You’re forced to pick and choose as to where your priorities really need to be,” said McLeod, director of strategic programs and partnerships at the Cancer Hope Network, a nonprofit that supports cancer patients. Even in that role, she struggles to navigate the financial aftermath of surviving the disease.
The cost of postcancer care often “keeps us hostage,” she said.
McLeod is one of nearly 19 million U.S. cancer survivors, many of whom continue to need prescriptions, doctor visits, and procedures to monitor their condition and manage posttreatment side effects. Of more than 1,200 cancer patients and survivors , about 47% said they had carried medical debt, with nearly half having owed more than $5,000, according to the American Cancer Society Cancer Action Network.

Yet health policy researchers and patient advocates said the experiences of cancer survivors reveal the limits of the Trump administration’s proposals to lower premiums, which may not help patients who accumulate large medical bills year after year. The proposals center on increasing the availability of high-deductible health plans, which have lower monthly payments but require patients to pay thousands of dollars out-of-pocket before coverage kicks in.
In addition, the administration has supported allowing insurers more leeway to sell plans that are not compliant with the Affordable Care Act. Such plans could bar people who have preexisting health conditions, like a cancer diagnosis, and exclude that ACA plans are required to cover.
The administration did not answer a request for comment on how its proposals would affect cancer survivors. But its supporters say, in general, people would have more flexibility to personalize coverage and more options for plans with lower monthly fees.
Michael Cannon, director of health policy studies at the Cato Institute, a libertarian think tank, believes patients would have better control over spending, and the option to choose what kind of care gets covered, if health plans were exempted from the ACA’s regulations. A person could opt for a plan that includes cancer treatment but not maternity care, for example.
History proves insurance coverage is not that simple, especially for people with preexisting conditions, said Jennifer Hoque, an associate policy principal with the American Cancer Society Cancer Action Network. When health plans could “pick and choose” enrollees based on preexisting conditions prior to the ACA, people needing the costliest care often struggled to find coverage, she said.
“They’re not going to choose a cancer survivor,” Hoque said of health insurers.
That was the case for Veronika Panagiotou, who said private insurers refused her coverage back in September 2013 because she had a high body mass index. Two months later, as a 25-year-old uninsured graduate student, she was diagnosed with non-Hodgkin lymphoma. The hospital treated her, she recalled, “and sent me all the bills.”
In January 2014, Panagiotou was able to buy one of the first ACA plans that went into effect. It covered chemotherapy and immunotherapy treatment, imaging, medications, hospital stays, weekly blood draws, a blood transfusion, and emergency room visits.
Now Panagiotou, 37, is cancer-free and works as director of advocacy and programs at Cancer Nation, a nonprofit advocacy group. Even though she is covered through her employer, Panagiotou said treatment-related expenses weigh heavily on her life decisions.
“Every choice I make, I think about cancer,” she said.

Chris Bond, a spokesperson for AHIP, the main health insurance trade association, said its members are working to improve access to coverage. But that can be a challenge when doctors and drugmakers are hiking prices, he said. Health plans are trying to “shield Americans from the full impact of those rising costs,” Bond said.
The Lymphoma Research Foundation has seen a 10% increase in applications to its patient aid fund this year, CEO Meghan Gutierrez said. “This trajectory suggests that financial safety nets, when they exist, are straining,” she said.
Rising prices are affecting everyone, regardless of the kind of health insurance they have, if any, said Brian Blase, president of Paragon Health Institute, a Republican-aligned think tank. “The biggest challenge for cancer patients isn’t the type of coverage,” he said. “It’s the underlying cost of care.”
Blase pointed to President Donald Trump’s as potentially helpful to cancer survivors. The Medicare Drug Price Negotiation Program, established by the Inflation Reduction Act of 2022, required the Department of Health and Human Services to negotiate prices for certain high-cost drugs, to lower prices for the federal health insurance program for people ages 65 and older. Drugs for breast, prostate, and kidney cancers are already on that list, .
Yet Hoque fears efforts to weaken ACA protections and financial support for marketplace plans will give cancer survivors тАФ who she said tend to “hang on to insurance for dear life” тАФ fewer options, especially between jobs or during career changes.
Erin Jones, a 31-year-old food policy researcher living in Fort Collins, Colorado, who was diagnosed with Hodgkin lymphoma as a young adult, is now cancer-free but still sees two oncologists, visits a high-risk breast clinic, and gets a breast MRI annually. Jones gets health insurance through the university where she works, and said she recently deferred acceptance to a PhD program partly due to uncertainty over affordable coverage.
“I don’t have the freedom to do the things I want to do as easily,” she said, “because I am constantly worried about health insurance.”
Costs related to surviving cancer, including monitoring for recurrence and treatment of side effects, were expected to reach $246 billion by 2030, up from $183 billion in 2015, according to .
Advancements in both detecting and curing cancer have resulted in a higher percentage of people surviving five years or more after diagnosis, according to the American Cancer Society. The number of survivors is expected to grow to more than 22 million people by 2035, .
Despite these advancements, the cost of treatment can steal the spotlight, said Ezekiel Emanuel, a co-director of the Healthcare Transformation Institute at the University of Pennsylvania and a onetime health policy adviser to former President Barack Obama.
An oncologist, Emanuel said he had observed patients make the difficult decision to delay or skip postcancer care as a result.
“Even when we triumph,” he said, “we don’t seem to be able to have a celebration.”
Are you struggling to afford your health insurance? Have you decided to forgo coverage? Click hereтАпto contact ║┌┴╧│╘╣╧═Ї News and share your story.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/cancer-survival-costs-testing-treatment-premiums-deductibles-trump/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2229400&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>“I feel like I’m suffocating inside this shelter, trapped with no way out,” Carlos’ son said, according to one of the teens’ attorneys, when asked to describe how he felt after months at the Houston-area facility. “Every day, the same routine. Every day, feeling stuck. It makes me feel hopeless and terrified.”
During daily video calls, Carlos, who had temporary protected status, urged the siblings to be patient, to trust the process. Federal officials had vetted Carlos before he could be granted custody and told him his case was complete. He believed he would soon be back with his children, who, like him, had sought refuge from political violence in Venezuela.
An immigration officer called Carlos on a Friday and asked him to attend a meeting at an ICE office the following Monday to discuss reunification with his children. Once Carlos arrived, officers tried to force him to sign documents he said he didn’t understand. When he refused, they stripped off his clothes, seized his ID and belongings, and chained him by the neck, waist, and legs.
“They tricked me,” Carlos said in a phone call from an immigration detention center in El Paso, Texas, where he was held for several months. “They used my children to grab me,” he said.
In reporting on the family’s story, ║┌┴╧│╘╣╧═Ї News reviewed court documents, spoke with the family’s immigration attorneys, interviewed Carlos, and reviewed statements from his children, translated from Spanish. Carlos is a pseudonym, being used at the request of attorneys concerned that speaking out could jeopardize Carlos’ immigration case or further delay his reunion with his family.
Using Children to Arrest Parents
Since 2003, the Department of Health and Human Services’ Office of Refugee Resettlement has cared for immigrant children under 18 who arrive in the country without their parents, often fleeing violence, abuse, or trafficking. The office, which in February had more than 2,300 children in shelters or with foster families across the country, is supposed to promptly release them to vetted caregivers, typically parents or other family members already living in the country.
Congress placed this responsibility with the health agency over 20 years ago to prioritize the well-being of unaccompanied children and separate their care from immigration enforcement priorities.
Now the second Trump administration is using migrant children held by the resettlement office to lure their parents, such as Carlos, whether or not they have a criminal record. A ║┌┴╧│╘╣╧═Ї News investigation found the resettlement office, , coordinates with the Department of Homeland Security to arrest people seeking custody of migrant children.
Arrest documents show Homeland Security Investigations, the arm of the agency that normally focuses on organized criminals and traffickers, will interview parents or other caregivers then arrest them if they are in the country illegally. Before Donald Trump returned to the White House, the resettlement office prohibited data sharing and collaboration with immigration enforcement, and it did not deny caregivers custody of children solely because of their immigration status. Those last year.
It’s unclear exactly how many caregivers have been baited into arrest. LAist indicating more than 100 have been arrested while trying to get their kids out of detention, but ║┌┴╧│╘╣╧═Ї News could not independently verify that number with federal agencies.
Since February, the Department of Health and Human Services, Department of Homeland Security, and Justice Department have not responded to questions about caregiver arrests. Prior to leaving DHS last month, Assistant Secretary Tricia McLaughlin said the administration protects children from being released to people who shouldn’t care for them. Andrew Nixon, an HHS spokesperson, referred questions related to immigration enforcement to DHS.
At the same time, the resettlement office has that make it harder for caregivers to gain custody of unaccompanied children. These include narrowing the range of accepted documents, requiring fingerprint-based background checks for every adult in the home and backup caregivers, and requiring in-person appointments to verify identification documents, sometimes with ICE agents present. The requirements keep “children safe from traffickers and other bad, dangerous people,” Nixon said.
As of January, the agency had detained at least 300 children already placed with vetted sponsors and asked their caregivers to reapply, according to the National Center for Youth Law and the Democracy Forward Foundation. The advocacy groups filed calling these actions “a quieter, new form of family separation.”
Reverse Separation
Dulce, a Guatemalan mother in Virginia, said her 8-year-old son was sent to a government shelter after he was detained during a traffic stop last summer while visiting family members in a different state.
At first, Dulce expected to get her son back within days — she had passed the government’s sponsorship requirements in 2024 and was reunited with him three weeks after he first crossed the border. But resettlement agency officials asked her to repeat the entire process and resubmit documents, Dulce said. It took eight months to get him back.
Dulce is a pseudonym being used at her request because she fears speaking out could get her deported.
At one point, Dulce was told to attend an interview at an ICE office to show her identification as part of the process of reuniting with her son. She refused out of fear that she too might be detained, because she doesn’t have legal status. She believes ICE agents visited her home at one point.
“I stopped going home,” Dulce said. “I lived with some of my friends for days.”
Even though she lived just 45 minutes away, Dulce was allowed to visit her son only twice a month.
Until recently, most unaccompanied children landed in government custody after being detained at the border. But border crossings started to fall in 2024, and the number of people coming to the U.S. has dropped precipitously in President Trump’s second term.
Now, hundreds of kids have been taken to government shelters after being swept up inside the country, often during immigration raids or traffic stops, according to the advocates’ lawsuit. Many were already living with relatives, including guardians already vetted by the resettlement agency.
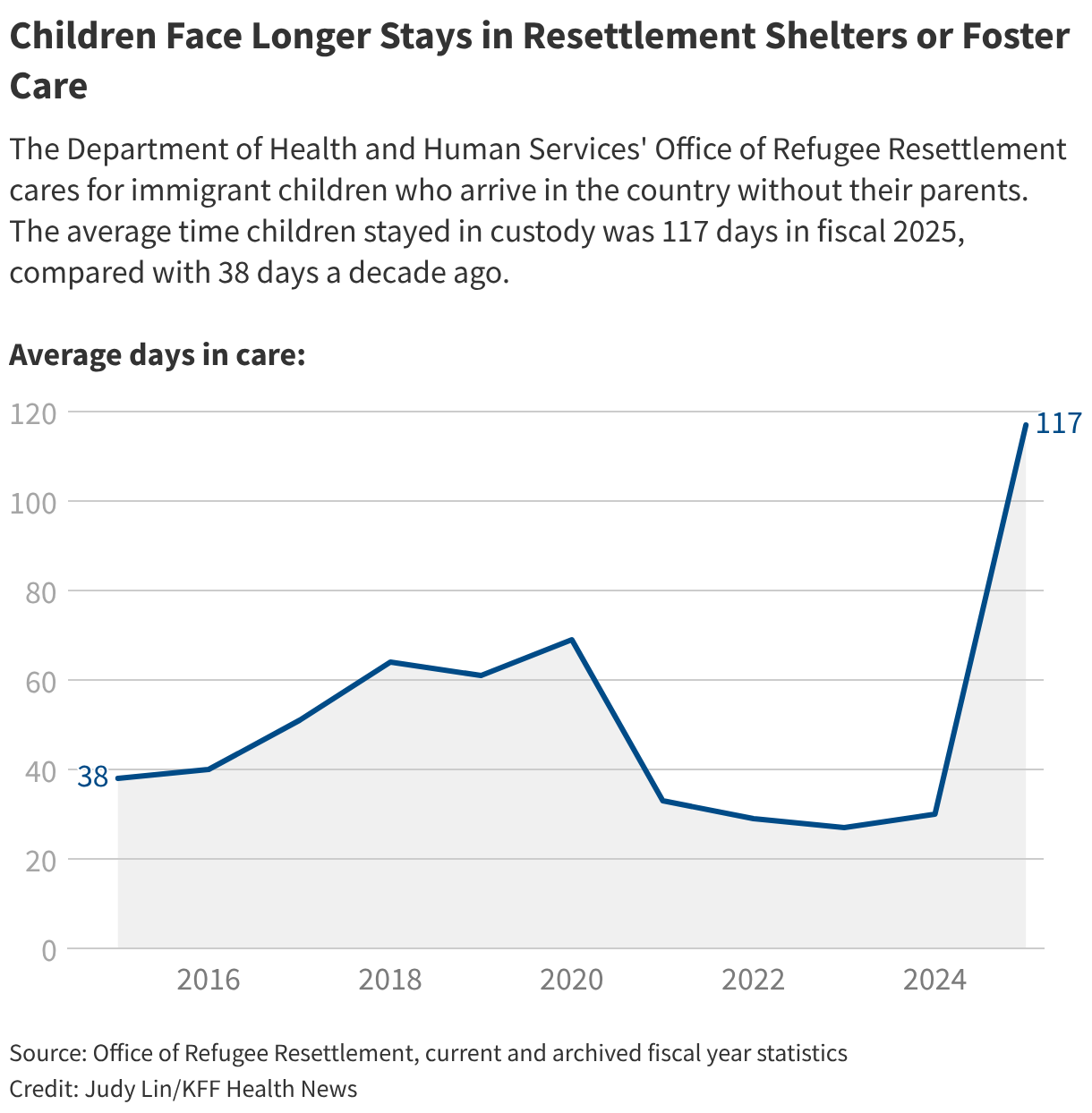
Releases have grinded nearly to a halt. According to the resettlement office, children in its custody stayed in government shelters or foster care for an average of one month in 2024. As of February, that had jumped to more than half a year.
When children do get released, it’s often only after their attorneys file a lawsuit in federal court challenging their detention as unconstitutional.
Authorities released Dulce’s son to her in February after the boy’s attorneys filed such a petition. Dulce said she’s relieved to have him back but still anxious that ICE could show up at their house.
Immigrants at Risk
During Trump’s first term, his administration was criticized for of children who had been released from custody. President Joe Biden was blamed for how his administration processed a surge of unaccompanied children that peaked in 2021 with about 22,000 in the resettlement office’s custody. Though most children were placed with legitimate sponsors, some were placed with people who hadn’t cleared , putting them at risk of .
The Trump administration says it is checking on those , and the Justice Department has prosecuted . On March 1, Homeland Security Secretary Kristi Noem, who is set to leave her role at the , touted a , including the resettlement office, that DHS said had tracked down 145,000 unaccompanied children who had been placed with caregivers during Biden’s term.
Yet internal HHS reports about that initiative obtained by ║┌┴╧│╘╣╧═Ї News show that nearly 11,800 of those migrant children and nearly 500 of their caregivers were arrested as of Jan. 29. Only 125 of those migrant children and 55 of those caregivers were arrested for alleged criminal activity, suggesting the majority were for immigration violations.
HHS referred questions about the figures in the reports to DHS, which did not respond to requests for comment about the data. However, Michelle Brané, who was a DHS official in the Biden administration, said the figures show that most of the arrests were to detain and deport migrants. Previously, the administration targeted parents and caregivers who had paid for children to cross the border, trying to levy smuggling charges against them.
“They have really dropped that pretense in a lot of ways, and they are going for anyone openly,” Brané said. “These numbers clearly reflect that this is not about public safety or about safety of the children.”
Case on Hold
Carlos left Venezuela in 2022 because of death threats and, like thousands of others fleeing that country, was granted what’s called temporary protected status under the Biden administration. That protection for most Venezuelans by the Trump administration.
In January 2025, days before Trump was sworn in for his second term, Carlos’ children crossed the border from Mexico to the U.S., turned themselves over to border authorities, and were immediately placed in the resettlement agency’s custody. Carlos spent months submitting paperwork to reunite with them. He said he’s their only parent, because their mother left when they were toddlers.
Officials visited his home twice and determined he was fit to care for them, according to court documents petitioning for his release from detention. He passed DNA testing, proving he’s the biological father, one of his attorneys said. His arrest documents show he has “no criminal history.” In July, Carlos was told his reunification case was complete and being sent for approval. But then, with little explanation, the case was put on hold.
Before his arrest by ICE, Carlos said, he drove 14 hours each way from his home to visit his children. Once there, he could see them for only one hour. When he was in detention, he said, he spoke to them about every two weeks in quick, monitored phone calls.
He’s trying to stay hopeful, but it’s hard.
According to documents completed by ICE officers during his arrest and submitted in his court case, Carlos was arrested under an initiative called Operation Guardian Trace, which requires immigration officers to detain potential caregivers if they are in the country without legal authorization and recommend that they be deported.
“This operation is designed to force parents to make an impossible choice between reuniting with their children and seeking safety,” said one of Carlos’ attorneys, Chiqui Sanchez Kennedy of the Galveston-Houston Immigrant Representation Project, a nonprofit that helps low-income immigrants.
‘I’m Going to Wait’
In March, a federal judge said officials had unlawfully detained Carlos and he was released on bond.
But his children still face an uncertain future for now. Government shelters often lack sufficient resources, , and social workers say lengthy stays in these facilities can result in additional trauma.
“Not only is it bad, full stop, but the longer you’re there, the worse it gets,” said Jonathan Beier, associate director of research and evaluation for the Acacia Center for Justice’s Unaccompanied Children Program, which coordinates legal services for unaccompanied minors.
Carlos’ children could also be sent back to the country they fled. Because of his detention, Carlos will have to redo much of the process to reunite with them, according to an attorney for the children, Alexa Sendukas, also with the Galveston-Houston Immigrant Representation Project.
In statements shared through Sendukas, Carlos’ daughter said she no longer wants to be around others and spends most of the time in her room. His son, now 15, described having panic attacks and feeling that he’s missing out on life, whether it’s the opportunities he longs for — to learn English, to study science — or watching basketball with his family.

“I remember when I first arrived at this shelter, I was so hopeful and had faith that I would be reunited with my dad soon,” he said.
Carlos’ daughter spent the day crying in bed when the siblings learned their father had been detained. For days, they didn’t know where he was. Now, they fear the only way out is through adoption or foster care.
“I am afraid,” she said. “I’m going to wait for my dad forever.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/courts/trump-deportation-immigration-unaccompanied-children-bait-parent-arrests-hhs/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2171527&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Loretta Forbes realized she would have to drop her plan after her monthly ACA marketplace premiums jumped tenfold in 2026. So the 56-year-old, who lives outside Nashville, Tennessee, started rationing her rheumatoid arthritis medications. Her husband, Jim, gave up on his fledgling handyman business and started looking for a job with insurance coverage.
And when Nicole Wipp learned the monthly premium for her family’s ACA plan would be more than their mortgage payment, she and her husband decided to drop their family plan and buy coverage only for their 15-year-old son.
After crunching the numbers, Wipp, 54, a self-employed lawyer in Aiken, South Carolina, said she and her family made the tough call.
“We decided that, ultimately, it would be better for us to gamble.”
Despite a contentious back-and-forth and the longest government shutdown in history last fall, the GOP-led Congress allowed enhanced ACA subsidies, which had helped millions of Americans cover all or part of their marketplace premiums since 2021, to expire on Dec. 31. With the loss of the subsidies and health care costs already surging, face tough decisions about their health coverage this year.

Hulsman, Forbes, and Wipp don’t qualify for Medicaid, the public insurance program for those with low incomes or disabilities. But like many others, they are being squeezed by the increasing costs of groceries, housing, and other necessities. Rising monthly health insurance premiums, along with copayments, high deductibles, and other out-of-pocket medical costs, can often push families like these to the brink.
More than 80% of Americans said their cost of living has increased in the past year, according to from that includes ║┌┴╧│╘╣╧═Ї News. Health care costs ranked at the top of their concerns, with about two-thirds saying that they are somewhat or very worried about affording health care тАФ more than said the same about other necessities, such as food and housing, the poll found.
“Premiums are getting quite unaffordable for a lot of people. The cost of both health care and other basic needs is rising,” said , director of private coverage at the health consumer group Families USA. “This is an especially critical time for Congress to do something.”
Most Republican lawmakers have refused to renew the enhanced subsidies. Most of the public says that inaction by Congress was the “wrong thing,” according to the KFF poll. Instead, GOP lawmakers have advocated for an expansion of and for more plans with lower premiums and steeper deductibles and copays that don’t reduce overall costs.
President Donald Trump released in January with few details about how to lower out-of-pocket costs for millions of Americans. The One Big Beautiful Bill Act, which he signed in July, is expected to leave millions uninsured over the next decade as it reduces federal health spending by nearly $1 trillion, mostly from Medicaid.
Already about 1.2 million fewer people have signed up for plans for this year under the ACA, also known as Obamacare, according to . Health policy analysts expect more people to stop making payments and drop coverage in the coming months. ACA marketplace insurers have said that they are charging 4 percentage points more in 2026 because they expect healthier people to drop plans as enhanced tax credits expire, leaving more sick and high-cost patients.
Rising costs and lack of congressional action are forcing many to make “untenable choices,” said , executive director and co-founder of the Center for Children and Families at Georgetown University.
“People are faced with absorbing this huge financial and health risk,” she said.
Forbes, the woman with rheumatoid arthritis near Nashville, had been on an ACA marketplace plan since 2018. But this year she and her husband, Jim, dropped their coverage after learning the monthly premium would jump from $250 to $2,500 because the enhanced subsidies expired. Jim, 59, gave up his handyman business and began searching for a job with health insurance.
“We were like: тАШOK, we can’t breathe. We’re gonna tap out,’” said Forbes, who was diagnosed with cervical cancer in 2021. Last year she lost her job at a retirement facility because she couldn’t work after she had a hysterectomy.
A day before their ACA coverage lapsed, her husband got a job offer at a property management company that provides health coverage. In January, they learned that Forbes was approved for Medicare because of her disability. The $155 monthly premium is automatically deducted from her disability check, she said.
Forbes’ Medicare plan starts in February, just in time for her next cancer screening.
“You cannot imagine what a relief it is to know I will have care,” Forbes said.
Even those who are insured face drastically higher out-of-pocket costs. This year, health insurers’ premiums for ACA marketplace plans , the result of higher hospital costs, the popularity of pricey GLP-1 drugs for obesity and diabetes, and the threat of tariffs, according to KFF. Nearly 4 in 10 adults said they were skipping or postponing necessary care because of costs, showed.
Hulsman, the Louisville shop owner, said he takes home about $33,000 a year from his business. Last year he paid about $105 a month for a gold plan on the marketplace, with a $750 deductible. This year, with the loss of the enhanced subsidy, Hulsman is paying the same monthly premium for a “bronze” plan, but with a deductible of $8,450, which he must pay out-of-pocket before his insurer starts paying for care. On average, deductibles for bronze plans are more than four times those of gold plans, according to .
Hulsman didn’t consider dropping health insurance, because Kentucky has limited . But he said he’ll try to get an estimate if he needs to go to a doctor. And he’s worried that a major accident could wipe out his skate shop. He won’t be able to buy inventory or pay shop bills if he has to meet his full deductible, he said.
“I’m just riding the line right now,” the skateboarder said. “One slip and it’s gonna be uncomfortable.”


In South Carolina, Wipp dragged her family to get routine vaccinations on New Year’s Eve тАФ the last day that she and her husband had health coverage.
This year’s monthly premium for a bare-bones bronze family plan would have cost them $1,400, up from $900 last year. They would still have faced high copays for doctor visits and need to meet a deductible of more than $10,000. Instead, they’re paying around $200 to cover just her son.
Wipp, who has a rare condition that causes cysts and other growths to form in the lungs, said she and her husband plan to pay out-of-pocket this year for any initial preventive care. Their second source of money, for larger medical expenses, is an old health savings account. But she said that account doesn’t have enough to cover a major accident or illness. And Wipp can’t add to the account while she is uninsured.
“The third source would be, I don’t know,” Wipp said. “The fourth is bankruptcy.”
Are you struggling to afford your health insurance? Have you decided to forgo coverage? to contact ║┌┴╧│╘╣╧═Ї News and share your story.
This <a target="_blank" href="/health-care-costs/priced-out-health-insurance-costs-kentucky-tennessee-south-carolina/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2149295&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
Health policy changes in Washington will ripple through the country, resulting in millions of Americans losing their Medicaid or Affordable Care Act coverage. But there are still ways to find care.
Over the next decade, the GOP’s One Big Beautiful Bill Act is expected to slash nearly $1 trillion in spending from Medicaid, the state-federal program for people with low incomes and disabilities. The implementation of new work rules will cause some beneficiaries to lose their Medicaid coverage.
Millions of Americans are facing enormous increases in their out-of-pocket costs for ACA coverage. So far, 1.2 million fewer people have signed up for Obamacare plans compared with last year, and health policy analysts estimate more will lose coverage as they fail to pay their premiums.
Health costs are a top concern for Americans. Two-thirds of the public say they are somewhat or very worried about affording health care, more than express the same worries about utilities, food, housing, or gas, according to a , a health information nonprofit that includes ║┌┴╧│╘╣╧═Ї News.
“All of this pain just doesn’t have to be there,” said Cheryl Fish-Parcham, director of private coverage at the health consumer group Families USA.
Doctors and health policy researchers say health coverage, of any kind, is the best protection against major medical debt.
Caitlin Donovan, a senior director at the Patient Advocate Foundation, recommends exhausting every available option for health coverage before going uninsured.
Even a high-deductible plan can protect patients from medical bankruptcy “if the absolute worst-case scenario happens,” she said.
Here are five ways that the uninsured can find affordable care.
1. Don’t be afraid to talk with your doctor about money
Patients can be hesitant to tell their doctors they’re uninsured or be wary of expressing concern about being able to afford care.
But some hospitals, physicians, and other providers offer cheaper cash pay options, said Cynthia Cox, a senior vice president and the director of the Program on the ACA at KFF.
Often prices are negotiable. “Always ask,” she said.
Health care providers can make adjustments if they know patients are worried about money, said Ateev Mehrotra, a doctor and researcher at Brown University.
“If my patient tells me, тАШDoc, I’m gonna have to pay for this out-of-pocket,’ I’m gonna make a different risk calculus,” Mehrotra said.
That doesn’t mean a patient won’t get the care they need, he said. A doctor, for instance, might order an ultrasound instead of an MRI, which is more expensive.
2. Search for providers that specifically work with uninsured patients
If your usual provider won’t budge on prices, then search for providers that cater to patients without insurance.
Federally qualified health centers, or FQHCs, and other community clinics offer routine and non-emergency care, such as treatment for flu or infection, for low-income residents and the uninsured. Community health centers charge based on a sliding scale and see annually in some of the country’s most underserved areas, according to the National Association of Community Health Centers.
The Trump administration has made funding cuts that might lead some of the country’s approximately 1,500 FQHCs to close or cut services. But the administration still maintains .
Planned Parenthood also accepts uninsured patients. Its centers test for sexually transmitted diseases, provide birth control options, and offer postpartum and gender-affirming care .
And the National Association of Free & Charitable Clinics also offers to help people find free or low-cost care.
Most community clinics don’t offer specialty care, but they can usually refer patients who need more intensive services to providers willing to work with uninsured patients.
And academic medical centers tend to have more charity care programs that help uninsured patients lower their bills.
“If you’re uninsured or even underinsured, you might be able to qualify for a significant discount on the cost of your care,” Cox said.
Still, be wary of heading to the emergency room, which is the most expensive place to get care. While ERs are federally required to stabilize all patients regardless of their ability to pay, they can still leave you with a big bill тАФ and often do.
3. Call your local health department
Health services vary widely from county to county, but many offer free vaccinations, family planning services, and testing for sexually transmitted infections, as well as for flu, covid, and tuberculosis.
Some county health departments also offer more advanced care, such as dental services and mental health or substance abuse programs. And some states have consumer assistance programs that can guide residents in finding care, Fish-Parcham said.
In addition, the Centers for Disease Control and Prevention’s makes free or low-cost breast and cervical cancer screenings available to low-income women in all states and territories. And some states cover screenings for other types of cancer as well.
4. It’s easier to shop around for drugs than doctors
Don’t just fill your prescription at the closest pharmacy. Instead, research generic drug options and look around for the best price on brand names.
A handful of sites such as and offer comparison shopping tools and information on other ways to get drug discounts.
And some retailers offer low-cost access to common prescription drugs тАФ at prices cheaper than you would find if you had insurance. Walmart, for instance, sells 90-day prescriptions of of drugs for $10. As do , , and a new site called the .
Many drugmakers also offer patient assistance programs, coupons, and rebates on some medications. Check their websites for details on how to apply.
States also offer drug assistance programs. The steps to qualify and types of drugs vary, but has a list of programs and how they work.
Joining a clinical trial is another way to access treatment. The and its have lists, but patients must first meet the criteria. Clinical trials aren’t necessarily free, even with insurance, Donovan said, so be sure to ask about any associated costs.
5. Your diagnosis might lead you to specialized resources
Patients with a specific diagnosis might have additional options for specialty treatment.
For example, someone with breast cancer should check with the and the nonprofit , Cox said.
The Patient Advocate Foundation hosts that can help offset the cost of medical bills and provide other resources such as transportation and lodging, Donovan said. Just type in basic information such as age, location, and diagnosis to see what is available.
Disorder-specific foundations, such as those for lupus or irritable bowel syndrome, can also steer patients to free or low-cost resources or cover some costs of care, Donovan said.
“Everything is out there,” she said.
As you research affordable care options, don’t be tricked by plans that look like health insurance but don’t offer guaranteed protection against big bills.
Some short-term plans and health care sharing ministries might seem like good deals, but read the fine print. Some red flags to look for: too-good-to-be-true monthly payments; no coverage for preexisting conditions; morality clauses such as those prohibiting the use of alcohol or drugs; or a lack of coverage for benefits such as mental health counseling that are required in ACA plans.
║┌┴╧│╘╣╧═Ї News correspondent Sam Whitehead contributed to this report.
Are you struggling to afford your health insurance? Have you decided to forgo coverage? Click here to contact ║┌┴╧│╘╣╧═Ї News and share your story.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/uninsured-health-care-low-cost-discounts-options-advice-5-things/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2149311&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The effort, part of Baltimore’s more than $100 million gun violence prevention plan, relies on staffers like Fitzgerald to build trust with people at risk of such violence and offer them resources like housing or food. Researchers believe these programs reduce gun deaths.
Yet one morning in 2019, Fitzgerald said, his oldest son, Deshawn McCoy, then 26, was shot just outside of the neighborhood he patrolled at the time. Fitzgerald said McCoy was a “really beautiful soul,” who fixed dirt bikes at a local garage. McCoy became the city’s , one of 348 that year, among the city’s deadliest. He left behind three daughters.
“This is our zone,” said Fitzgerald, pointing toward McElderry Park. “My son got cooked over here.”
For years, violence intervention was the work of loosely organized, underfunded groups. Then gun violence spiked during the covid pandemic and the Biden administration and Congress poured in money to better integrate such programs within cities. It appeared to help: In Baltimore and beyond, gun violence has plummeted.
The number of homicides in the city dropped 41%, from more than 300 a year in 2021 to 201 in 2024, according to the U.S. attorney’s office in Maryland.
“Gun violence is a sticky, hard problem to solve,” said Daniel Webster, a researcher at the Johns Hopkins Center for Gun Violence Solutions in Baltimore. “We’re getting it right finally.”
Now President Donald Trump’s administration has gutted funding for that work.
Webster said it could take years to untangle what led to the city’s gun violence drop. Among the factors, he said: the pandemic’s end, investments in violence intervention, improvements that have given police more legitimacy in neighborhoods, targeted prosecutions, and an aggressive effort to remove untraceable ghost guns.
“You need all of these systems working well to have systemic reductions in gun violence,” he said.
The Trump administration has slashed funding for and research, cutting about $500 million in grants to organizations that support public safety.
At the same time, Trump has loosened gun laws the Bureau of Alcohol, Tobacco, Firearms and Explosives, which oversees gun dealers. He has also sent federal troops into the Democratic-led cities of Chicago; Los Angeles; Memphis, Tennessee; Portland, Oregon; and Washington, D.C.
Webster said cities are still benefiting from pandemic-era efforts to address gun deaths. But given the Trump policy changes, if violence escalates, city leaders could have a hard time keeping it from spiraling out of control.
Trying Something Different
Safe Streets is among the promising violence prevention programs that could lose funding. Staffers in the city’s most violent neighborhoods operate like community health workers.

During the pandemic, the Biden administration provided billions of dollars to local governments through the American Rescue Plan Act. Biden urged them to deploy money to community violence intervention programs, which have been shown to by as much as 60%. His administration to spend Medicaid dollars on such programs. The goal: Stop gun deaths.
Few cities seized the opportunity.
Analyzing federal data, professors Philip Rocco of Marquette University and Amanda Kass of DePaul University found local governments used the ARPA money for 132,451 projects. Yet only 231, less than 0.2%, involved community violence intervention, they said.
In Baltimore, then-newly elected mayor Brandon Scott was ready for the federal influx.
Baltimore’s homicide rate had been high since 2015, when a 25-year-old Black man named Freddie Gray died in police custody. Protests erupted and fractures between residents and police deepened. Baltimore ended the year with 342 homicides, the first time since 1999 that more than 300 were recorded in the city.
“We got really good at our jobs” in the years after Gray’s death, said James Gannon, trauma program manager at Sinai Hospital of Baltimore.

Gun deaths tracked what public health researcher Lawrence T. Brown called the : racially segregated areas that fanned out across Baltimore’s eastern and western neighborhoods around a wealthy central strip. People who faced years of forced displacement and disinvestment , which fueled the cycle.
Every year from 2015 to 2022, the city recorded at least 300 homicides.
“We had to try something different,” said Stefanie Mavronis, director of the Mayor’s Office of Neighborhood Safety and Engagement. Scott created the agency weeks after he was sworn into office in 2020, later with $50 million in ARPA money and $20 million annually from the city’s budget.
Containing an Outbreak
The office’s budget тАФ $22 million in fiscal year 2026 тАФ is a fraction of the city’s .
Still, the money allowed Baltimore’s leaders to scale up a new approach: addressing gun violence the way public health officials might handle an infectious disease outbreak, Mavronis said.
City staffers identified the small subset of people most at risk of being shot or becoming the next shooter through crime data and referrals from social service workers, hospitals, and violence intervention staff, she said. Mavronis said that gangs, friends willing to engage in violence for each other, and retaliation had been driving gun deaths in the city.
“This never-ending cycle of violence and loss and trauma,” Mavronis said, “comes from that.”
The city convened hospital presidents to connect gunshot victims and their friends and family to counseling, crisis support, and city services.
It offered people help finding therapy, a job, or emergency relocation тАФ and threatened arrest and prosecution if they retaliated.
“We decided that we were no longer going to subscribe to the belief that one thing, one agency, one part of government, one program was going to help cure Baltimore of this disease of gun violence that has had a stranglehold on this city for the entirety of my life,” Scott said.
The Coming Cliff
Baltimore is on pace this year to post its fewest gun deaths since Richard Nixon was president.
“Some of it is the national zeitgeist of the moment,” said Adam Rosenberg, executive director of Center for Hope at LifeBridge Health, which operates Safe Streets sites and the Violence Response Team at Sinai Hospital. He credits mainly the infusion of funding that allowed more resources and hands-on engagement with high-risk communities.
“We typically talk about how poverty affects homicides, but it works in reverse too,” Webster said. “People don’t invest in homes and businesses or, frankly, in people, where people get shot regularly.”
Fitzgerald, who grew up in East Baltimore, said he started working for Safe Streets in 2010 for the paycheck.
He’s been on both sides of gun violence, he said, as someone hit more than a dozen times in shootings тАФ first when he was 12. At 13, Fitzgerald said, he shot a cousin in the leg. Over years, he was in and out of the criminal justice system, including for charges of attempted murder, which helped him understand the people he now works with every day, he said.
No college “can certify you in my experiences in violence,” he said. “That’s what allows me to identify and detect potentially violent situations.”
Today, Fitzgerald, 49, believes that teaching kids trauma coping mechanisms can drive culture change and stop shootings.
“Our kids see more death than soldiers,” he said.
But federal funding is drying up. Anthony Smith, executive director of , which supports local leaders on gun violence reduction, estimates that about 65 groups have lost funding this year. And Trump’s signature legislation slashes nearly $1 trillion in anticipated federal Medicaid spending over the next decade.
Center for Hope lost $1.2 million from federal cuts.

“It’s like a car racing along, and you see the cliff coming,” Rosenberg said. “I don’t know if the resources are there anymore, but the need certainly is.”
Rosenberg said that, because of their experiences, staffers such as Fitzgerald are “incredible messengers” for people involved in gun violence, and he noted that they are thoroughly vetted.
Fitzgerald put it this way: “I’m trying to save my kids, the community. The people we’re trying to save is our friends and our family, and ourselves.”
║┌┴╧│╘╣╧═Ї News senior correspondent Fred Clasen-Kelly contributed to this report.
If you or someone you know have experienced the pain of a gunshot wound, and are willing to talk about the medical experience, please fill out our form .
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/race-and-health/baltimore-guns-community-violence-intervention-homicide-decline-arpa-federal-funds/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2131266&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The Supplemental Nutrition Assistance Program тАФ commonly referred to as food stamps, or SNAP тАФ helps feed 42 million low-income people in the United States. Now, because of changes included in the One Big Beautiful Bill Act, to keep his food benefits Santillan-Garcia might soon have to prove to officials that he’s working.
He said he lost his last job for taking time off to go to the doctor for recurrent stomach infections. He doesn’t have a car and said he has applied to a grocery store, Walmart, Dollar General, “any place you can think of” that he could walk or ride his bike to.
“No job has hired me.”
Under the new federal budget law, to be eligible for SNAP benefits, more people are required to show that they are working, volunteering, or studying. Those who don’t file paperwork in time risk losing food aid for up to three years. States were initially instructed to start counting strikes against participants on Nov. 1, the same day that millions of people saw their SNAP benefits dry up because of the Trump administration’s refusal to fund the program during the government shutdown. But federal officials backtracked partway through the month, instead giving states until December to enforce the new rules.
The new law further limits when states and counties with high unemployment can waive recipients from requirements. But a legal battle over that provision means that the deadline for people to comply with the new rules varies depending on where recipients live, even within a state in some cases.
The U.S. Department of Agriculture did not respond to a detailed list of questions about how the new rules around SNAP will be implemented, and the White House did not respond to a request for comment about whether the rules could kick off people who rely on the program. The law did extend exemptions to many Native Americans.
Still, states must comply with new rules or accrue penalties that could force them to pay a bigger share of the program’s cost, which was about $100 billion last year.

President Donald Trump signed the massive budget bill, along with the new SNAP rules, into law on July 4. States initially predicted they would need at least 12 months to implement such significant changes, said Chloe Green, an assistant director at the American Public Human Services Association who advises states on federal programs.
Under the law, “able-bodied” people subject to work requirements can lose access to benefits for three years if they go three months without documenting working hours.
Depending on when states implement the rules, many people could start being dropped from SNAP early next year, said Lauren Bauer, a fellow in economic studies at the Brookings Institution, a policy think tank. The changes are expected to knock at least 2.4 million people off SNAP within the next decade, according .
“It’s really hard to work if you are hungry,” Bauer said.
Many adult SNAP recipients under 55 already needed to meet work requirements before the One Big Beautiful Bill Act became law. Now, for the first time, adults ages 55 to 64 and parents whose children are all 14 or older must document 80 hours of work or other qualifying activities per month. The new law also removes exemptions for veterans, homeless people, and former foster care youths, like Santillan-Garcia, that had been in place since 2023.
Republican policymakers said the new rules are part of a broader effort to eliminate waste, fraud, and abuse in public assistance programs.
Agriculture Secretary Brooke Rollins said in November that in addition to the law, she will require millions to reapply for benefits to curb fraud, though she did not provide more details. Rollins she wants to ensure that SNAP benefits are going only to those who “are vulnerable” and “can’t survive without it.”
States are required to notify people that they are subject to changes to their SNAP benefits before they’re cut off, Green said. Some states have announced the changes on websites or by mailing recipients, but many aren’t giving enrollees much time to comply.
Anti-hunger advocates fear the changes, and confusion about them, will increase the number of people in the U.S. experiencing hunger. Food pantries have reported record numbers of people seeking help this year.
Even when adhering to the work rules, people often report challenges uploading documents and getting their benefits processed by overwhelmed state systems. In a survey of SNAP participants, about 1 in 8 adults reported having lost food benefits because they had problems filing their paperwork, according to . Some enrollees have been dropped from aid as a result of state errors and staffing shortfalls.
Pat Scott, a community health worker for the Beaverhead Resource Assistance Center in rural Dillon, Montana, is the only person within at least an hour’s drive who is helping people access public assistance, including seniors without reliable transportation. But the center is open only once a week, and Scott says she has seen people lose coverage because of problems with the state’s online portal.
Jon Ebelt, a spokesperson with the Montana health department, said the state is always working to improve its programs. He added that while some of the rules have changed, a system is already in place for reporting work requirements.
In Missoula, Montana, Jill Bonny, head of the Poverello Center, said the homeless shelter’s clients already struggle to apply for aid, because they often lose documentation amid the daily challenge of carrying everything they own. She said she’s also worried the federal changes could push more older people into homelessness if they lose SNAP benefits and are forced to pick between paying rent or buying food.
In the U.S., are the fastest-growing group experiencing homelessness, according to federal data.
Sharon Cornu is the executive director at St. Mary’s Center, which helps support homeless seniors in Oakland, California. She said the rule changes are sowing distrust. “This is not normal. We are not playing by the regular rules,” Cornu said, referring to the federal changes. “This is punitive and mean-spirited.”
In early November, a federal judge in Rhode Island ordered the Trump administration to deliver full SNAP payments during the government shutdown, which ended Nov. 12. That same judge sought to buffer some of the incoming work requirements. He ordered the government to respect existing agreements that waive work requirements in some states and counties until each agreement is set to end. In total, and the District of Columbia had such exemptions, with different end dates.
Adding to the confusion, some states, including New Mexico, have waivers that mean people in different counties will be subject to the rules at different times.
If states don’t accurately document SNAP enrollees’ work status, they will be forced to pay later on, Green said. Under the new law, states must cover a portion of the food costs for the first time тАФ and the amount depends on how accurately they calculate benefits.
During the government shutdown, when no one received SNAP benefits, Santillan-Garcia and his girlfriend relied on grocery gift cards they received from a nonprofit to prioritize feeding his girlfriend’s baby. They went to a food pantry for themselves, even though many foods, including dairy, make Santillan-Garcia sick.
He’s worried that he’ll be in that position again in February when he must renew his benefits тАФ without the exemption for former foster care youths. Texas officials have yet to inform him about what he will need to do to stay on SNAP.
Santillan-Garcia said he’s praying that, if he is unable to find a job, he can figure out another way to ensure he qualifies for SNAP long-term.
“They’ll probably take it away from me,” he said.

What You Should Know
Changes to SNAP removed work-requirement exemptions for:
- People ages 55 to 64.
- Caretakers of dependent children 14 or older
- Veterans
- People without housing
- People 24 or younger who aged out of foster care
What SNAP Participants Should Do:
- Check with public assistance organizations to find out when the new rules go into effect in your region. Your benefits may be checked at recertification, but you may be required to meet the monthly work reporting rules long before that.
- Let your state know if you’re responsible for a dependent child younger than 14 who lives in your home; pregnant; a student at least half the time; attending a drug or alcohol treatment program; physically or mentally unable to work; a Native American; or a caretaker of an incapacitated household member. If so, you may still be exempt.
This <a target="_blank" href="/health-care-costs/snap-food-stamps-hunger-work-requirements-one-big-beautiful-bill/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2122381&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Permanent changes to the Supplemental Nutrition Assistance Program are coming regardless of the outcome of at least two federal lawsuits that seek to prevent the government from cutting off November SNAP benefits. The lawsuits challenge the Trump administration’s refusal to release emergency funds to keep the program operating during the government shutdown.
A federal judge in Rhode Island ordered the government to use those funds to keep SNAP going. A Massachusetts judge in a separate lawsuit also said the government must use its food aid contingency funds to pay for SNAP, but gave the Trump administration until Nov. 3 to come up with a plan.
Amid that uncertainty, food banks across the U.S. braced for a surge in demand, with the possibility that millions of people will be cut off from the food program that helps them buy groceries.
On Oct. 28, a vanload of SpaghettiOs, tuna, and other groceries arrived at Gateway Food Pantry in Arnold, Missouri. It may be Gateway’s last shipment for a while. The food pantry south of St. Louis largely serves families with school-age children, but it has already exhausted its yearly food budget because of the surge in demand, said Executive Director Patrick McKelvey.

New Disabled South, a Georgia-based nonprofit that advocates for people with disabilities, announced that it was offering one-time payments of $100 to $250 to individuals and families who were expected to lose SNAP benefits in the 14 states it serves.
Less than 48 hours later, the nonprofit had received more than 16,000 requests totaling $3.6 million, largely from families, far more than the organization had funding for.
“It’s unreal,” co-founder Dom Kelly said.
The threat of a SNAP funding lapse is a preview of what’s to come when changes to the program that were included in the One Big Beautiful Bill Act that President Donald Trump signed in July take effect.
The domestic tax-and-spending law cuts $187 billion within the next decade from SNAP. That’s a nearly 20% decrease from current funding levels, according to the Congressional Budget Office.
The new rules shift many food and administrative costs to states, which may lead some to consider withdrawing from the program, which helped about 42 million people buy groceries last year. Separate from the new law, the administration is also pushing states to limit SNAP purchases by barring such things as candy and soda.
All that “puts us in uncharted territory for SNAP,” said Cindy Long, a former deputy undersecretary at the Department of Agriculture who is now a national adviser at the law firm Manatt, Phelps & Phillips.
The country’s first food stamps were issued at the end of the Great Depression, when the poverty-stricken population couldn’t afford farmers’ products. Today, instead of stamps, recipients use debit cards. But the program still buoys farmers and food retailers and prevents hunger during economic downturns.
The CBO estimates that will lose food assistance as a result of in the budget law, including applying work requirements to more people and shifting more costs to states. Trump administration leaders have backed the changes as a way to limit waste, to , and to .
This is the biggest cut to SNAP in its history, and it is coming against the backdrop of rising food prices and a fragile labor market.
The exact toll of the cuts will be difficult to measure, because the Trump administration that measures food insecurity.
Here are five big changes that are coming to SNAP and what they mean for Americans’ health:
1. Want food benefits? They will be harder to get.
Under the new law, people will have to file more paperwork to access SNAP benefits.
Many recipients are already required to work, volunteer, or participate in other eligible activities for 80 hours a month to get money on their benefit cards. The new law to previously exempted groups, including homeless people, veterans, and young people who were in foster care when they turned 18. The expanded work requirements also apply to parents with children 14 or older and adults ages 55 to 64.
, if recipients fail to document each month that they meet the requirements, they will be limited to three months of SNAP benefits in a .
“That is draconian,” said Elaine Waxman, a senior fellow at the Urban Institute, a nonprofit research group. About 1 in 8 adults reported having lost SNAP benefits because they had problems filing their paperwork, according to .
Certain refugees, asylum-seekers, and other lawful immigrants are cut out of SNAP entirely under the new law.

2. States will have to chip in more money and resources.
The federal law drastically increases what each state will have to pay to keep the program.
Until now, states have needed to pay for only half the administrative costs and none of the food costs, with the rest covered by the federal government.
Under the new law, states are on the hook for 75% of the administrative costs and must cover a portion of the food costs. That amounts to an estimated median cost increase for states of more than 200%, according to by the Georgetown Center on Poverty and Inequality.
A ║┌┴╧│╘╣╧═Ї News analysis shows that a single funding shift related to the cost of food could put states on the hook for an additional $11 billion.
All states participate in the SNAP program, but they could opt out. In June, nearly wrote to congressional leaders warning that some states wouldn’t be able to come up with the money to continue the program.
“If states are forced to end their SNAP programs, hunger and poverty will increase, children and adults will get sicker, grocery stores in rural areas will struggle to stay open, people in agriculture and the food industry will lose jobs, and state and local economies will suffer,” the governors wrote.
3. Will the changes lead to more healthy eating?
The Trump administration, through its “Make America Healthy Again” platform, has made healthy eating a priority.
Health and Human Services Secretary Robert F. Kennedy Jr. has championed the restrictions on soda and candy purchases within the food aid program. To date, to limit what people can buy with SNAP dollars.
Federal officials previously blocked such restrictions, because they were difficult for states and stores to implement and they boost stigma around SNAP, according to . In 2018, the first Trump administration to ban sugar-sweetened drinks and candy.
A store may decide that hassle isn’t worth participating in the program and drop out of it, leaving SNAP recipients fewer places to shop.
People who receive SNAP are no more likely to buy sweets or salty snacks than people who shop without the benefits, . Research shows that encouraging healthy food choices is than regulating purchases.
When people have less money to spend on food, they often resort to cheaper, unhealthier alternatives that keep them sated longer rather than paying for more expensive food that is healthy and fresh but quick to perish.

4. How will SNAP cuts affect health?
Advocacy organizations working to end hunger in the nation say the cuts will have long-term health effects.
Research has found that kids in households with limited access to food to have a mental disorder. Similarly, food insecurity is linked to .
Working-age people with food insecurity to experience chronic disease. That high blood pressure, arthritis, diabetes, asthma, and chronic obstructive pulmonary disease.
Those health issues come with costs for individuals. Low-income adults who aren’t on SNAP more a year on health care than those who are.
lived in households with limited or uncertain access to food in 2023.
5. What does this mean for the nation’s food supply chain?
SNAP spending directly boosts grocery stores, their suppliers, and the transportation and farming industries. Additionally, when low-income households have help accessing food, they’re more likely to spend money on other needs, such as prescriptions or car repairs. All that means that every dollar spent through SNAP generates at least $1.50 in economic activity, .
A report by associations representing convenience stores, grocers, and the food industry estimated it to comply with the new SNAP restrictions.
Advocates warn stores may pass the costs on to shoppers, or they may close.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/snap-food-stamps-cuts-shutdown-states-lawsuits-groceries-healthy-eating/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2108057&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Separated from her adult children and grieving her husband’s death in the war, she started a job packing boxes in a warehouse, making just enough to cover rent for her own apartment and bills.
Antoinette has been relying on the Supplemental Nutrition Assistance Program, formerly known as food stamps, for her weekly grocery trips.
But now, just as life is starting to stabilize, she will have to deal with a new setback.
President Donald Trump’s massive budget law, which Republicans call the One Big Beautiful Bill Act, тАФ or nearly 20% тАФ from the federal budget for SNAP through 2034. And separate from any , the law cuts off access completely for refugees and other immigrant groups in the country lawfully. The change was slated to take effect immediately when the law was signed in July, but states are still awaiting federal guidance on when to stop or phase it out.
For Antoinette, 51, who did not want her last name used for fear of deportation and likely persecution in her native country, the loss of food aid is dire.
“I would not have the means to buy food,” she said in French through a translator. “How am I going to manage?”
Throughout its history, the U.S. has admitted into the country refugees like Antoinette, people who have been persecuted, or fear persecution, in their homelands due to race, religion, nationality, political opinions, or membership in a particular social group. These legal immigrants typically face an in-depth vetting process that can start years before they set foot on U.S. soil.

Once they arrive тАФ often with little or no means тАФ the federal government provides resources such as financial assistance, Medicaid, and SNAP, outreach that has typically garnered bipartisan support. Now the Trump administration has pulled back the country’s decades-long support for refugee communities.
The budget law, which funds several of the president’s priorities, including tax cuts to wealthy Americans and border security, revokes refugees’ access to Medicaid, the state-federal health insurance program for people with low incomes or disabilities, starting in October 2026.
But one of the first provisions to take effect under the law removes SNAP eligibility for most refugees, asylum seekers, trafficking and domestic violence victims, and other legal immigrants. About 90,000 people will lose SNAP in an average month as a result of the new restrictions narrowing which noncitizens can access the program, .
“It doesn’t get much more basic than food,” said Matthew Soerens, vice president of advocacy and policy at World Relief, a Christian humanitarian organization that supports U.S. refugees.
“Our government invited these people to rebuild their lives in this country with minimum support,” Soerens said. “Taking food away from them is wrong.”
Not Just a Handout
The White House and officials at the United States Department of Agriculture did not respond to emails about support for the provision that ends SNAP for refugees in the One Big Beautiful Bill Act.
But Steven Camarota, director of research for the Center for Immigration Studies, which advocates for reduced levels of immigration to the U.S., said cuts to SNAP eligibility are reasonable because foreign-born people and their young children disproportionately use public benefits.
Still, Camarota said, the refugee population is different from other immigrant groups. “I don’t know that this would be the population I would start with,” Camarota said. “It’s a relatively small population of people that we generally accept have a lot of need.”
Federal, state, and local spending on refugees and asylum seekers, including food, health care, education, and other expenses, totaled $457.2 billion from 2005 to 2019, according to from the Department of Health and Human Services. During that time, 21% of refugees and asylum seekers received SNAP benefits, compared with 15% of all U.S. residents.
In addition to the budget law’s SNAP changes, given to people entering the U.S. by the Office of Refugee Resettlement, a part of HHS, has been cut from one year to four months.
The HHS report also found that despite the initial costs of caring for refugees and asylees, this community contributed $123.8 billion more to federal, state, and local governments through taxes than they received in public benefits over the 15 years.
It’s in the country’s best interest to continue to support them, said Krish O’Mara Vignarajah, president and CEO of Global Refuge, a nonprofit refugee resettlement agency.
“This is not what we should think about as a handout,” she said. “We know that when we support them initially, they go on to not just survive but thrive.”
Food Is Medicine
Food insecurity can have lifelong physical and mental health consequences for people who have already faced years of instability before coming to the U.S., said Andrew Kim, co-founder of Ethn─У Health, a community health clinic in Clarkston, an Atlanta suburb that is home to thousands of refugees.

Noncitizens affected by the new law would have received, on average, $210 a month within the next decade, according to the CBO. Without SNAP funds, many refugees and their families might skip meals and switch to lower-quality, inexpensive options, leading to chronic health concerns such as obesity and insulin resistance, and potentially worsening already serious mental health conditions, he said.
After her husband was killed in the Democratic Republic of Congo, Antoinette said, she became separated from all seven of her children. The youngest is 19. She still isn’t sure where they are. She misses them but is determined to build a new life for herself. For her, resources like SNAP are critical.
From the conference room of New American Pathways, the nonprofit that helped her enroll in benefits, Antoinette stared straight ahead, stone-faced, when asked about how the cuts would affect her.
Will she shop less? Will she eat fewer fruits and vegetables, and less meat? Will she skip meals?
“Oui,” she replied to each question, using the French for “yes.”
Since arriving in the U.S. last year from Ethiopia with his wife and two teen daughters, Lukas, 61, has been addressing diabetes-related complications, such as blurry vision, headaches, and trouble sleeping. SNAP benefits allow him and his family to afford fresh vegetables like spinach and broccoli, according to Lilly Tenaw, the nurse practitioner who treats Lukas and helped translate his interview.
His blood sugar is now at a safer level, he said proudly after a class at Mosaic Health Center, a community clinic in Clarkston, where he learned to make lentil soup and balance his diet.
“The assistance gives us hope and encourages us to see life in a positive way,” he said in Amharic through a translator. Lukas wanted to use only his family name because he had been jailed and faced persecution in Ethiopia, and now worries about jeopardizing his ability to get permanent residency in the U.S.

Hunger and poor nutrition can lower productivity and make it hard for people to find and keep jobs, said Valerie Lacarte, a senior policy analyst at the Migration Policy Institute.
“It could affect the labor market,” she said. “It’s bleak.”
More SNAP Cuts To Come
While the Trump administration ended SNAP for refugees effective immediately, the change has created uncertainty for those who provide assistance.
State officials in Texas and California, which receive the most refugees among states, and in Georgia told ║┌┴╧│╘╣╧═Ї News that the USDA, which runs the program, has yet to issue guidance on whether they should stop providing SNAP on a specific date or phase it out.
And it’s not just refugees who are affected.
Nearly 42 million people receive SNAP benefits, . The nonpartisan Congressional Budget Office estimates that, within the next decade, more than 3 million people will lose monthly food dollars because of planned changes тАФ such as an extension of work requirements to more people and a shift in costs from the federal government to the states.
In September, the administration among all U.S. households, making it harder to assess the toll of the SNAP cuts.
The USDA also that no benefits would be issued for anyone starting Nov. 1 because of the federal shutdown, blaming Senate Democrats. The Trump administration has refused to release emergency funding тАФ as past administrations have done during shutdowns тАФ so that states can continue issuing benefits while congressional leaders work out a budget deal. A coalition of attorneys general and governors from 25 states and the District of Columbia contesting the administration’s decision.
Cuts to SNAP will ripple through local grocery stores and farms, stretching the resources of charity organizations and local governments, said Ted Terry, a DeKalb County commissioner and former mayor of Clarkston.
“It’s just the whole ecosystem that has been in place for 40 years completely being disrupted,” he said.
Muzhda Oriakhil, senior community engagement manager at Friends of Refugees, an Atlanta-area nonprofit that helps refugees resettle, said her group and others are scrambling to provide temporary food assistance for refugee families. But charity organizations, food banks, and other nonprofit groups cannot make up for the loss of billions of federal dollars that help families pay for food.
“A lot of families, they may starve,” she said.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/race-and-health/refugees-snap-benefits-food-aid-trump-law/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2105114&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But while the result seemed foretold, the debate was far from unanimous.
The Advisory Committee on Immunization Practices, or ACIP, met at a satellite campus of the Centers for Disease Control and Prevention because the agency’s headquarters were still smashed up from a deadly gun attack last month by a man who said the covid vaccine had made him depressed and suicidal.
Health and Human Services Secretary Robert F. Kennedy Jr. has made it clear he wants the panel to change the CDC’s childhood immunization schedule, which establishes, sometimes with legal authority, which vaccines are to be mandated, paid for, and administered by states, insurers, and doctors across the country.
Kennedy fired the 17-member panel in June and has so far restocked it with 12 people, including outspoken critics of vaccination. On Sept. 18, the new panel’s discussions reflected its thin expertise and ignorance of how the vaccination schedule came to be. Scientific questions answered decades ago were asked as if they were brand-new.
“We are rookies,” said biostatistician Martin Kulldorff, the committee’s chair, noting many “technical issues that we might not grasp as of yet.”
Paul Offit, director of the Vaccine Education Center at Children’s Hospital of Philadelphia, watched the telecast anxiously.
“It reminds me when as children we would have a mock United Nations meeting,” he said. “This would be like that, except we would have actually made decisions for the United Nations.”
Kennedy’s CDC accomplished what 30 years of public health attempts to fight anti-vaccine sentiment hadn’t: a head-to-head comparison of evidence and arguments. But while the winner was clear in the eyes of most experts, some doubted the result would be good.
“The whole purpose of the people on this committee is to circulate these old recycled anti-vax talking points,” said Sean O’Leary, a professor of pediatrics at the University of Colorado who previously was a liaison from the American Academy of Pediatrics to ACIP. On Friday morning, he said, a colleague had a mother in his practice who refused the measles, mumps, and rubella vaccine “because she heard something bad in the news about it last night.”
Until now, public health owned places like ACIP, while vaccine foes and skeptics dominated social media. At this meeting, the skeptics had moved onto public health’s turf тАФ where sometimes flimsy arguments and expertise were exposed.
Pharmacist Hillary Blackburn, for example, asked why children needed two measles, mumps, and rubella shots. ACIP began recommending a second shot in 1989 during a deadly measles outbreak. The two-shot regimen provided more than 95% immunity and led to the virtual elimination of measles from the United States. This year under the Trump administration more than 1,400 cases have been reported, mostly in unvaccinated people.
In one noteworthy gaffe, ACIP member Retsef Levi, a Massachusetts Institute of Technology operations management professor, misinterpreted data from a graph showing declines in hepatitis B in the United States since the 1980s. While rates had fallen in older groups, Levi said, cases in babies hadn’t declined substantially since 2005, when he inaccurately said a birth dose was first recommended.
“Where’s the argument to vaccinate even younger children at all,” he said. “Where is the benefit?”
In fact, the recommendation for a newborn shot began in 1991 and was reinforced and expanded in 2005. The first generation of hepatitis B-vaccinated babies are well into their 30s now.
“As time goes on,” CDC scientist Adam Langer patiently explained, “the people who benefited from the change in policy at the very beginning of the policy are moving into different age groups.”


Kulldorff, Levi, and committee member Evelyn Griffin, a gynecologist, also suggested that vaccines shouldn’t be recommended unless they are tested in placebo trials, which would require certain children not to be vaccinated тАФ a practice considered unethical.
Kulldorff began the meeting defiantly. He did not mention the CDC shooting, but disparaged former agency officials Kennedy had forced out and challenged nine former CDC directors to a debate.
He also asked if anyone in the audience would eat a hot dog laced with thimerosal, the mercury-containing preservative the committee banned from influenza vaccines at its last meeting. (No one has ever offered thimerosal as a condiment, but years of study showed the minuscule amounts in vaccines did no harm).
At the June meeting, HHS censored a CDC appraisal of thimerosal while inviting an anti-vaccine activist to present an error-filled criticism of the substance. But on Sept. 18 the panel got what looked like straight science from CDC professionals.
As the committee prepared to debate ending a 34-year-old ACIP recommendation for babies to get a dose of the hepatitis B vaccine at birth, CDC career scientists Langer and John Su presented evidence of the vaccine’s safety and benefits.
Langer also laid out the history of the fight against hepatitis B тАФ including the failed effort to control the disease by vaccinating people most at risk, including people who use drugs, sex workers, and pregnant women who tested positive for the virus. Years of trial and error showed that in the U.S., at least, it was necessary to vaccinate newborns to really knock down the disease.
Levi, who frequently mentions the vaccination status of his own six children, challenged the idea that a healthy baby from a “normal” household тАФ one with no history of drug use or prostitution тАФ needed the vaccine.
Cody Meissner, one of three panel members who put up a spirited defense of the status quo in the hepatitis debate, noted that when it comes to vaccination campaigns, “the more we try and define a target group to vaccinate, the less successful we are.” Meissner, a Dartmouth College professor, has published studies of vaccines and the diseases they fight since the 1970s.
Long-observed tropes of vaccine skepticism were abundant on the first day of the meeting. Levi praised a 2004 study from Guinea-Bissau, an outlier that suggested that babies, especially females, were more likely to die if they got a hepatitis B shot. Other panelists said the study, performed in a poor country with high infant mortality where children got an outdated vaccine, wasn’t relevant. But more studies were needed in general, Levi said. “We sit here with very lousy evidence,” he said.
Nurse Vicky Pebsworth of the National Vaccine Information Center, which opposes all vaccine mandates, frequently brought her own selective research into the meeting. She read off the names of studies other panelists hadn’t received to back her arguments that vaccines under discussion were not safe.
But while “too many, too soon” is a common anti-vaccine refrain, Judith Shlay from the National Association of County and City Health Officials, which had a nonvoting chair at the meeting, used it to support the current schedule. She pointed out that the panel’s debate over a combination measles, mumps, rubella, and varicella shot for children would result in a separate shot for the virus that causes chickenpox, adding to the number of inoculations on the childhood schedule.
“Some parents want to have fewer injections,” she said.

With an 8-3 vote at the end of the day, the committee nonetheless recommended separate vaccinations for MMR and chickenpox.
Everyone seemed puzzled about what had transpired with an ensuing vote on whether the Vaccines for Children Program, which pays for more than half of childhood vaccinations, should respond to ACIP’s new recommendation. The panel revoted on the issue on Sept. 19.
Nor could anyone provide a clear answer as to what prompted the committee’s discussion and planned vote on the birth dose of hepatitis B vaccine, since there was no new evidence suggesting any harm from it.
Two of Kennedy’s senior aides, both vaccine skeptics, pushed the hepatitis B discussion onto the ACIP schedule, according to testimony at a Sept. 17 Senate hearing by former CDC chief medical officer Debra Houry, who resigned to protest administration policies.
ACIP member Robert Malone, who has claimed that mRNA vaccines are dangerous, said hepatitis B was on the agenda because it is given to newborns at birth and of special concern to parents newly awakened to vaccine doubt. He appeared to nod off during a CDC staff presentation on the safety of the hepatitis B shot.
Vaccination of babies has always triggered parents. The 19th-century poet Alexander Hope Hume described evil vaccinators who turned “the rosy darling” who “crows with glee” into “a wailing infant” whose every vein “ferments with poison.”
The agenda item was not really about the merit of the hepatitis B vaccine, Malone acknowledged.
“The signal that is prompting this is not one of safety; it’s one of trust,” he said.
But in the end, the committee reconsidered what would have been its first drastic move to reverse a successful U.S. vaccination campaign. It postponed its vote on the hepatitis B birth dose.
This <a target="_blank" href="/health-industry/cdc-acip-meeting-mmrv-hepatitis-b-childhood-vaccine-schedule/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2091481&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>“We’re going to take care of the sickest patients first,” Margo, a family medicine physician, said.
It’s not like there was space on that June afternoon anyway. A small monitor on the wall pulsed with the vitals of current patients, who filled the ER. An ambulance idled outside in the South Texas heat with a patient waiting for a bed to open up.
“Everybody shows up here,” Margo said. “When you’re overwhelmed and you’re overrun, there’s only so much you can do.”
Starr County, a largely rural, Hispanic community on the southern U.S. border, when it voted Republican in a presidential election for the first time in more than a century. Immigration and the economy in this community, where roughly a third of the population falls below the poverty line.

Now, recent actions by the Trump administration and the GOP-controlled Congress have triggered a new concern: the inability of doctors, hospitals, and other health providers to continue to care for uninsured patients. It’s a fear not only in Starr County, which has one of the highest uninsured rates in the nation. Communities across the U.S. with similarly high proportions of uninsured people could struggle as additional residents lose health coverage.
About 14 million fewer Americans are expected to have health insurance in a decade due to President Donald Trump’s new tax-and-spending law, which Republicans dubbed the One Big Beautiful Bill Act, and the pending expiration of enhanced subsidies that slashed the price of Affordable Care Act plans for millions of people. The new law also that send billions of dollars to help those who care for uninsured people stay afloat.
“You can’t disinsure this many people and not have, in many communities, just a collapse of the health care system,” said Sara Rosenbaum, founding chair of the Department of Health Policy and Management at George Washington University’s Milken Institute School of Public Health.
“The future is South Texas,” she said.
║┌┴╧│╘╣╧═Ї News is examining the impact of national health care policy changes on uninsured people and their communities. Though the Trump administration told ║┌┴╧│╘╣╧═Ї News it is making “a historic investment in rural health care,” people who treat low-income patients, as well as researchers and consumer advocates, say recent policy decisions will make it harder for people to stay healthy. Doctors, hospitals, and clinics that make up the health care safety net could lose so much money they must close their doors, some of them warn.
“Because the patient’s bill is not going to get paid,” said Joseph Alpert, editor-in-chief of The American Journal of Medicine and a professor of medicine at the University of Arizona. “Uninsured patients stress the health care system.”
Starr County shows how this dynamic unfolds.
Primary care doctors in the county serve an average of each, nearly three times the U.S. average.
Margo, the family physician, said because so many people lack insurance and there are so few places to seek care, many residents treat the ER as their first stop when they’re sick.
In many cases, they have neglected their health, making them sicker and more expensive to treat. And requires ERs at hospitals in the Medicare program to stabilize or transfer patients, regardless of their ability to pay.
That leaves Margo and his team to practice what he described as “disaster medicine.”
“They come in with chest pain or they stop breathing. They collapse. They’ve never seen a doctor,” Margo said. “They’re literally dying.”
Health Systems in ‘Survival Mode’
When people are uninsured or on Medicaid, they tend to rely on a safety net of doctors, hospitals, clinics, and community health centers, which offer services free of charge or absorb getting reimbursed at lower rates than they do treating patients on commercial insurance.
Those providers’ financial situations can often be precarious, leading them to rely on myriad federal supports. The Trump administration’s cuts to health care and Medicaid in the name of eliminating “waste, fraud, and abuse” have many concerned they won’t weather the additional financial strain.
Trump’s new law funds his priorities, like extending tax cuts that mainly benefit wealthier Americans and expanding immigration enforcement. Those costs are covered in part by a nearly $1 trillion reduction in federal health spending for Medicaid within the next decade and changes to the ACA, such as requiring additional paperwork and shortening the time for people to sign up.
Many Republicans have argued Medicaid has gotten too large and strayed from the state-federal program’s core mission of covering those with low incomes and disabilities. And the GOP has fought to roll back the ACA since its passage.
Kush Desai, a spokesperson for the White House, said projections from the nonpartisan Congressional Budget Office about how many people could lose health insurance are an “overestimate.” He did not provide an estimate the administration sees as more accurate.
Supporters of the “One Big Beautiful Bill” say those who need health coverage can still get it if they meet new requirements such as working in exchange for Medicaid coverage.
And Michael Cannon, director of health policy studies at the Cato Institute, a libertarian think tank, said even with the legislation, Medicaid spending will grow, just not as quickly.
The budget law won’t cause “the sky to fall,” Cannon said. “The inefficient providers should be shutting down.”
from AMGA, formerly the American Medical Group Association, which represents health systems across the country, found nearly half of rural facilities could close or restructure due to Medicaid cuts. Nearly three-quarters of respondents said they anticipated layoffs or furloughs, including of front-line clinicians.
Public health departments, which often fill gaps in care, also face federal funding cuts that have reduced their capacity. In South Texas’ Cameron County, the health department has eliminated nearly a dozen positions, said agency head Esmer Guajardo. In neighboring Hidalgo County, the health department has laid off more than 30 people, said Ivan Melendez, who helps oversee its operations.
In July, the Texas Department of State Health Services , a massive annual event that last year provided free health services to nearly 6,000 South Texas residents.
Gateway Community Health Center in Laredo, a border city north of the Rio Grande Valley, is in “survival mode,” with about a third of patients already lacking insurance and even more who will struggle to afford health care if the ACA subsides aren’t renewed, said David Vasquez, its director of communications and public affairs. The center is looking for other forms of funding to avoid layoffs or cuts to services, and its expansion and hiring plans are on hold, Vasquez said.
That downsizing is happening as more people lose health insurance and need free or reduced-cost care.
Esther Rodriguez, 39, of McAllen has been out of work for two years and her husband makes $600 a week working in construction. Neither of them has health insurance.
Medicaid covered the bills for the births of her five children. Now, she depends on a mobile health clinic run by a local medical school, where she can pay out-of-pocket for routine checkups and drugs to control her Type 2 diabetes. If she needed more care, Rodriguez said, she would go to the ER.
“You have to adapt,” she said in Spanish.
‘Death by a Thousand Cuts’
People’s inability to pay results in uncompensated care, or services that hospitals, doctors, and clinics don’t get paid for, which, under an earlier version of the megabill, was projected to increase by $204 billion over the next decade, , a nonprofit think tank.
But the Trump administration is also cutting other support that helped offset the cost of care for people who can’t pay. The new law caps federal programs that many health providers for low-income people have come to depend on, especially in rural areas, to shore up their budgets. These include taxes on hospitals, health plans, and other providers that states use to help fund their Medicaid programs. Such provider taxes are a “financial gimmick,” Desai said.
While the law creates a temporary $50 billion fund to support rural doctors and hospitals, that’s a little over a third of estimated Medicaid funding losses in rural areas, , a health information nonprofit that includes ║┌┴╧│╘╣╧═Ї News. Desai called the analysis “flawed.”
Any loss in revenue could spell financial ruin, especially for small rural hospitals, said Quang Ngo, president of the Texas Organization of Rural & Community Hospitals Foundation.
“It’s kind of like death by a thousand cuts,” he said. “Some will probably not make it.”
And the hits could keep coming. The Trump administration’s budget request for the coming fiscal year calls for cuts to multiple rural health programs operated through the Health Resources and Services Administration. Desai said the spending law’s investment in rural health “dwarfs” the cuts.
In February, the Trump administration announced funding cuts of 90% to the ACA navigator program, which helps people find health insurance. That program has been “historically inefficient,” Desai said.
In December 2023, nearly 3 million of Texas’ uninsured were eligible for ACA subsidies, Medicaid, or the Children’s Health Insurance Program, , a public policy think tank.

Maria Salgado spends her workdays tabling at community events, dropping off flyers at doctors’ offices, and holding one-on-one meetings with clients of MHP Salud, a nonprofit that connects residents to Medicaid and ACA coverage.
She worried funding cuts would really set the organization’s efforts back: “A lot of community members here, they’re going to be left behind,” said Salgado, a community health worker, or promotora.
Chris Casso, a primary care physician who grew up in McAllen and now practices there, held back tears as she described treating patients who have put off seeing a doctor because of an inability to pay, only to have their preventable conditions deteriorate.
She worries about the future of her community as , potentially leaving few providers to treat uninsured people.
“It’s heartbreaking,” she said, sitting in a small back room in her office in a suburban strip mall, wedged between a Kohl’s and a Shoe Carnival. “These are hardworking people,” she said. “They try their best to take care of themselves.”
Casso said her own sister, who worked as a medical biller in a physician’s office, couldn’t afford health insurance. She delayed care and died at age 45 of complications from diabetes and heart disease. Casso worries the future will find more people in similar situations.
“Our population is going to suffer,” she said. “It’s going to be devastating.”

This <a target="_blank" href="/health-care-costs/uninsured-texas-rio-grande-valley-strain-local-health-systems-medicaid-aca/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2085435&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>