But plans to spend those nine-digit awards aren’t all warmly received.
At least one group of Republican state lawmakers appears to have scuttled an initiative preapproved by federal officials. And at least one hospital association persuaded its state health leaders to alter who greenlights spending. Other critics are taking a more cautious approach.
That’s because the Centers for Medicare & Medicaid Services, which manages the five-year Rural Health Transformation Program, says states could lose money if they make major changes to the plans approved in their applications. Changes could also delay states’ ability to get projects rolling in time to show the agency that they’re meeting progress deadlines.
“During the application period, states were advised to only propose initiatives and state policy actions that the state deemed feasible,” said CMS spokesperson Catherine Howden, who noted that the agency will work with states case by case.
The recent pushback reflects “tension” over state plans ‚Äî which were approved by the federal government ‚Äî from state lawmakers and health leaders who want more input amid tight deadlines, said Carrie Cochran-McClain, chief policy officer of the National Rural Health Association, the largest organization representing rural hospitals and clinics.
Cochran-McClain said many states must pass a bill to allow federal dollars to be spent and added that because the program rolled out so quickly “there’s important work that still needs to be done in some states between the legislatures and the governors.”
State lawmakers want to have a say, she said, in “how the funding is being allocated ‚Äî how the implementation will go.”
Congressional Republicans created the program as a last-minute sweetener to include in their One Big Beautiful Bill Act, signed into law last summer. The funding was intended to offset concerns about the anticipated in rural communities from the law, which is expected to slash Medicaid spending by nearly $1 trillion over a decade.
CMS officials announced first-year funding — ranging from $147 million for New Jersey to $281 million for Texas — on Dec. 29, after scoring applications. Federal officials will begin evaluating progress in late summer and announce 2027 allocations at the end of October.
A chorus of critics say the program won’t make up for harm caused by Medicaid cuts.
The program is “a complete sham,” Sen. Ron Wyden (D-Ore.) said at a rural policy conference in February.
Medicaid, a joint federal-state program for low-income and disabled Americans, serves nearly , and many rural hospitals depend on it to stay afloat.
But the rural health program tilts toward seeding innovative projects and technologies, not shoring up rural hospital finances. States can use only up to 15% of their funding to pay providers for patient care.
That hasn’t stopped some federal officials and lawmakers from framing the program as a rural hospital rescue.
For example, the White House , “President Trump secured $50 billion in funding for rural hospitals.”
Now that applications have been approved, some state Republican lawmakers ‚Äî who are than Democrats are ‚Äî and hospital associations are upset that the political rhetoric doesn’t match what they see.
They’re also lobbing criticisms at specific aspects of their states’ plans, including the proposed projects, what’s not included, and the spending approval process.
In Wyoming, lawmakers didn’t just criticize an initiative from their state’s application. They moved to kill it.
State Rep. John Bear, a Republican, said he and other lawmakers declined to fund “BearCare,” a proposed state-sponsored health insurance plan that patients could use only after medical emergencies. But they did approve other aspects of the rural health program.
The Wyoming Department of Health won’t “proceed with BearCare without express legislative authority to do so,” said spokesperson Lindsay Mills.
While Wyoming lawmakers removed an initiative from their state’s rural health plan, a group in Ohio wants to add something.
Ohio Rep. Kellie Deeter and other Republican lawmakers to use the maximum allowed funding for provider payments — 15% — to support 13 independent, rural hospitals.
“We understand that the rural transformation fund is not designed to be given directly to prop up hospitals,” Deeter said. “We just want to capitalize on the mechanism of the fund that can be utilized for that purpose.”
Those hospitals “operate with very, very narrow margins, and it’s just difficult and, frankly, unsustainable,” she added.
Ken Gordon, a press secretary responding for the governor’s office and the state health department, said, “It’s still very early in this process, and many details are being worked out.”
State lawmakers around the country are also trying to ensure the federal program’s dollars benefit rural areas.
In North Dakota, Rep. Bill Tveit, a Republican who lives in a town with about 2,000 residents, that would have required the state to reserve its funding for programs located more than 35 miles from urban areas and small cities.
During a hearing, lawmakers appeared sympathetic to Tveit’s concerns but quickly shot down his idea.
State Sen. Brad Bekkedahl said the North Dakota health department already committed to prioritizing funding for the most pressing rural health needs. He also said he’s concerned any significant changes could cause the state to lose funding because CMS already reviewed and approved the plan.
Meanwhile, Republican lawmakers in Michigan and North Carolina have criticized their states’ definitions of “partially rural” or “rural,” saying that counties that include urban population centers could take money from lower-density counties, according to and .
Lawmakers aren’t the only ones speaking out.
The Colorado Hospital Association to state lawmakers denouncing how the state created its plan and two of its proposed initiatives.
“Not only were Colorado’s rural hospitals’ recommendations disregarded,” president and CEO Jeff Tieman wrote, but the plan includes ideas “they actively oppose and believe will harm the communities they serve.”
The department responded to one of the association’s concerns by adding rural health leaders to the .
Meanwhile, and Nebraska, some health groups are upset that their states’ plans lack specific funding streams for rural hospitals.
Lauren LaPine-Ray, who oversees rural health policy at the Michigan Health & Hospital Association, predicted the state’s rural hospitals will compete with other organizations, such as academic centers and health clinics, for funding. She said about 65% of the group’s rural members have never applied for a state grant before.
“The rural hospitals, the ones that really need the funding the most, will not be well equipped to apply for and pull down these dollars,” LaPine-Ray said.
Jed Hansen, executive director of the Nebraska Rural Health Association, said the federal funding won’t go to “rural hospitals, rural clinics, and rural providers in a meaningful way.”
“Rural Health Transformation will not save a single hospital in our state,” he said. “I don’t think it will save a hospital nationally.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/rural-transformation-fund-lawmakers-health-groups-resist-state-spending-plans/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2161929&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>During a January White House roundtable touting the first grants to states under a new $50 billion rural health fund, Centers for Medicare & Medicaid Services Administrator Mehmet Oz called the idea “pretty cool.” Later that day, Sen. Bernie Sanders, the independent from Vermont, said it is decidedly . And obstetricians and others chimed in on social media to express alarm, with one political activist calling it a “.”
The disparate responses highlight how excitement over the tech-heavy ideas states pitched in their applications for the federal Rural Health Transformation Program conflicts with the reality that there simply aren’t enough health workers to serve patients in many rural communities. Now, as states prepare to spend their first-year awards, tension is mounting, and nowhere is that strain more visible than in Alabama.
Oz has lauded the state’s proposal to invest in the relatively new technology of robotic ultrasounds.
“Alabama has no OB-GYNs in many of their counties,” Oz said, sitting with President Donald Trump and Cabinet members. The dearth of care, , prompted the proposal to use robots for ultrasounds on pregnant women.
Britta Cedergren directs the and has a firm grip on reality: “No one is using autonomous robots.”
While robotic ultrasounds are a “really neat technology,” she said, they are not yet being used in the state. Instead, clinicians providing obstetric care lean on phone consultations and ‚Äî when equipment and internet are available ‚Äî telehealth.
The goal, she said, is to “support places where there is no care.”
Cedergren is part of multiple state maternal and fetal health groups and works daily with doctors, hospitals, and first responders. While enhanced technology is vital for patient care, it’s not a replacement for a well-trained workforce and a coordinated care and data system, she said.
In 2024, the most recent year for which data is available, Alabama’s infant mortality rate was per 1,000 live births. The nationwide rate was 5.5 per 1,000 live births, according to released by the Centers for Disease Control and Prevention.
Hospital-based obstetric unit closures, which often lead to a loss of health care providers who can care for expectant mothers and their babies, are a long-standing, ongoing trend in rural America. But Alabama’s loss of services has been particularly profound.
In 1980, 45 of the state’s 55 rural counties had hospital-based obstetric services. By 2025, , according to state data. And the losses aren’t slowing. Five hospital obstetric units closed in 2023 and 2024, including in three rural counties: Monroe, Marengo, and Clarke.

, a professor at the University of Minnesota School of Public Health, found that closures in remote areas in preterm births, a leading cause of infant mortality.
“People will be pregnant and give birth in communities all over the place,” she said. “You have to be able to get to a place where you can be cared for.”
Nearly all 50 states’ applications for the Rural Health Transformation Program declared workforce shortages and maternal health needs as priorities, but only Alabama proposed using robots to fill the gap. The rural fund, which Congress created as a last-minute sweetener in Trump’s One Big Beautiful Bill Act last summer, encouraged states to be creative, be innovative, and pitch tech solutions.
Alabama was awarded $203 million for the first of the program’s five years. Among nearly a dozen , the state’s application included bolstering its rural workforce as well as improving maternal and fetal health.
Mike Presley, a spokesperson for the , which is overseeing the plan, said no one was available for an interview about telerobotic ultrasounds.
LoRissia Autery, an obstetrics and gynecology specialist in rural Alabama northwest of Birmingham, said the robots won’t decrease maternal and infant mortality. There are nuances, she said, to doing ultrasounds.
Many of her patients have high-risk pregnancies with diabetes, high blood pressure, and hepatitis C, she said. She said she worries about the kind of care that will be given to her patients, many of whom drive an hour or more to get to her, if robots are used instead of a trained specialist.
“It takes away just the care that we need to have for women,” said Autery, who co-founded . The clinic includes three doctors, draws patients from five counties, and could use an additional physician to meet the demand, Autery said.
“Probably for the past six or seven years, we’ve been putting out feelers trying to find a fourth partner,” Autery said. “It’s difficult for a variety of reasons.”
In his social media remarks to Oz, Vermont’s Sanders called the lack of rural health care providers in the U.S. an “international embarrassment.”
“In the richest country on earth, we need more doctors, nurses, dentists and mental health counselors, not more robots,” Sanders wrote on the social platform X.
At least one country is using robots paired with trained workers to decrease deaths.
In the remote Canadian village of La Loche, Julie Fontaine operates an ultrasound robot at a clinic with two on-site nurse practitioners and rotating doctors. She said patients like the robot because it saves them the time and expense of traveling to a bigger regional health care facility six to seven hours away.
“When people come in, they’re like, ‚ÄòWow, like, technology these days,’” said Fontaine, a member of the in northern Saskatchewan. “It’s something they’ve never seen before or even used.”

When working with patients, Fontaine connects the robotic ultrasound machine to a tele-sonographer at a control station in Saskatoon. The sonographer then remotely operates a robotic arm on the machine. A radiologist, who can be anywhere, reads the scan’s report and sends it back to the family doctor in La Loche, said Ivar Mendez, a neurosurgeon and the director of Canada’s . Most babies in Canada, he said, are delivered by family doctors or midwives, not specialists.
“The most important thing is the identification of a high-risk pregnancy early enough so you can intervene,” said Mendez, who added that the robotic ultrasound is “as good as the in-person ultrasound” but can’t be used when a patient needs a more invasive vaginal ultrasound. The mortality rate for mothers and newborns in the north, site of the La Loche clinic, is 20 to 25 times greater than in the rest of the nation, he said.
“One of the reasons is that there’s no availability of prenatal ultrasonography in those communities, so pregnant women have to travel to cities and they’re put up at hotels,” he said.
In a , Mendez and his team at the University of Saskatchewan examined 87 telerobotic ultrasounds and found that 70% of the time, the robotic ultrasound made travel for care unnecessary. Nearly all the patients said they would use the robot again.
The same robotic ultrasound technology was in the U.S.
Nicolas Lefebvre, chairman and chief executive of the robot’s creator and manufacturer, AdEchoTech, said the company has “U.S. maternity-specific projects that are currently under preparation.” The average price of a robot will be $250,000 to $350,000, according to AdEchoTech’s U.S.-based business development consultant.
Using robotic ultrasounds is one part of Alabama’s proposed maternal and fetal health initiative, according to the . Acknowledging loss of hospital obstetric units, officials said they planned to connect smaller rural providers and health care facilities that lack “high-quality maternal and fetal health services” to regional care hubs that can provide the services digitally, including through telerobotic ultrasound.
For their workforce initiative, state officials proposed training programs for doctors, emergency services, and nurse-midwives.
The estimated required funding for the maternal and fetal health initiative is . Alabama officials proposed for their workforce initiative over five years.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/alabama-robot-ultrasounds-maternity-care-rural-health-oz/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2150215&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But there are strings attached.
In late December, President Donald Trump’s administration announced how much all 50 states would get under its new Rural Health Transformation Program, assigning them to use the money to fix systemic problems that leave rural Americans without access to good health care. Now, the clock is ticking.
Within eight months, states must submit revised budgets, begin spending, and show the money is going to good use. Federal officials will begin reviewing state progress in late summer and announce 2027 funding levels by the end of October.
The money — divided into unique allocations for each state, ranging from $147 million for New Jersey to $281 million for Texas — represents the first $10 billion installment from the five-year, $50 billion program. Congress created the fund as a last-minute sweetener in Trump’s One Big Beautiful Bill Act last summer to offset the anticipated in rural communities from the statute’s nearly $1 trillion in Medicaid spending cuts over the next decade.
Federal officials crafted the fund to give states “space to be creative,” Mehmet Oz, administrator of the Centers for Medicare & Medicaid Services, said on a call with reporters after announcing the funding Dec. 29. “Some states will fail, and we will learn from that.”
The money was divided according to a complicated formula.
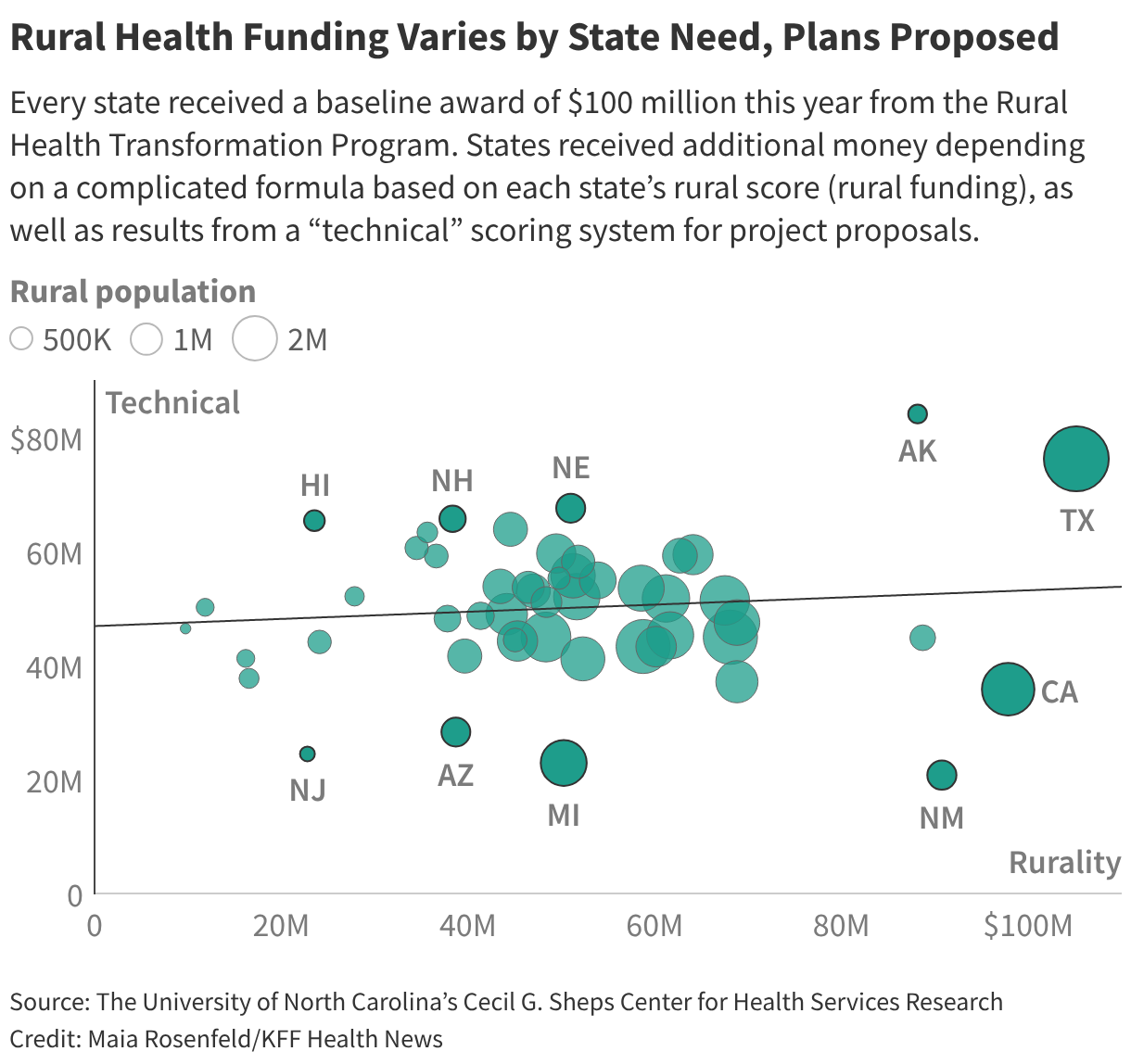
In 2026, each state will receive an equal $100 million share for the first half of the money, plus additional funding from the second half. Oz’s staff steered payouts from the second portion based on each state’s rural score, as well as results from a “technical” scoring system for project proposals.
Within hours of the announcement, academics and researchers began to parse the awards to better understand why some states received more than others, including whether the awards reflected any partisanship or political favoritism.
At first glance, total awards do not appear to favor states governed by either Republicans or Democrats. But teased out the amount awarded for each state’s technical score, which is the part determined by the discretion of agency officials.
The analysis was performed at the University of North Carolina’s Cecil G. Sheps Center for Health Services Research, which specializes in rural health. A ∫⁄¡œ≥‘πœÕ¯ News review of the Sheps Center data found that states with Republican governors tended to receive more money for the parts of their application based on the technical score. Democratic-controlled states crowded the bottom quarter of those technical score awards.
Overall, though, the state awards reveal wild variation in how much money each state will get per rural resident, almost a hundredfold difference between the top and bottom.
In an emailed statement to , a spokesperson for Arizona’s Democratic Gov. Katie Hobbs accused the administration of shortchanging rural residents in the state, which was awarded $167 million this year from the program.
CMS spokesperson Chris Krepich said in an emailed statement to ∫⁄¡œ≥‘πœÕ¯ News that “politics played no role in funding decisions.”
On the December call, Oz pushed states to start working on policy actions championed by the administration — such as approving presidential fitness tests and restricting food benefits — that could require legislative approval.
Half of states promised to mandate the presidential fitness test, Oz said. Many states also proposed food waivers under the Supplemental Nutrition Assistance Program, known as SNAP, which would limit low-nutrition items such as soda. He also said some states promised to teach health care professionals about nutrition. And others confirmed they will repeal certificate-of-need laws, which require companies to prove that new health facilities they want to open are necessary.
Krepich said CMS’ new Office of Rural Health Transformation is hiring program officers to serve as point people for three or four states. Many states are setting up their own offices to oversee the new funding.
Oz highlighted Alabama’s “big maternity initiative with robotics doing ultrasounds” and said states are tackling issues ranging from behavioral health to obesity.
A ∫⁄¡œ≥‘πœÕ¯ News review of state “” and “” released by CMS shows that many states plan to address the workforce challenges in rural areas. Delaware, for example, plans to use its funding to create the state’s first four-year medical school with a rural primary care track.
A third of states said they want to improve electronic health records, and every state mentioned telehealth.
Many state legislatures to distribute the funding to their state offices. Meanwhile, state officials are hiring staff, , and .
“I’m excited about what’s next,” said Terry Scoggin, former interim chief executive of the Texas Organization of Rural & Community Hospitals, or TORCH. Texas was awarded the biggest allocation. The money will bolster a rural hospital funding bill Republican Texas Gov. Greg Abbott signed last year, Scoggin said.
More than two dozen cash-strapped rural hospitals in Texas to clinics since 2005, a nationwide trend that hit the Lone Star State particularly hard. The state has the largest rural population in the United States. Texas’ allocation amounts to about $66 per rural resident, . By contrast, Rhode Island was granted about $6,300 per rural resident.
Scoggin said he has “a ton of concerns” about companies taking the money instead of it helping rural hospitals and residents. “I was blown away about how many for-profit companies reached out.” The companies have also called rural hospitals and asked to work with them to apply for state money, he said.
The awards should be judged on how they benefit rural residents because “the stated goal of the program is to improve rural health,” said Paula Chatterjee, an assistant professor of medicine at the University of Pennsylvania who co-authored on the transformation fund.
Researchers at the Sheps Center conducted the analysis to estimate how much money states received from the technical score, which is the portion of funding based on the quality of their proposals and state policy actions that align with “Make America Healthy Again” priorities.
New Mexico won the least amount of technical funding, with less than 10% of its award based on the discretionary metrics. Alaska won the largest technical award, according to the Sheps Center data.
Texas, Nebraska, New Hampshire, and Hawaii rounded out the top five recipients of technical funding. In addition to New Mexico, the other lowest technical awards went to Michigan, New Jersey, Arizona, and California.
Mark Holmes, director of the Sheps Center, declined to comment on whether he saw any political bias in the awards but said the nuance in the final portion of discretionary awards based on technical scores is important because those dollars can be redistributed and potentially clawed back in future years.
“We can be fairly certain that every state will get at least a slightly, if not a vastly, different amount next year based on this re-pooling and reallocation piece,” Holmes said.
States now have a limited time to show they’re using the money effectively to secure future funding.
But they can’t start spending yet. CMS followed standard grant procedures and is requiring each state to submit revised budgets before they can draw down money, Krepich said.
States have until Jan. 30 to resubmit their budgets, and CMS then has 30 days to respond, according to the standard . Under that timing, some states may not have cash in hand until March.
“CMS is working closely with states to complete this process as efficiently as possible,” Krepich said.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/rural-health-transformation-state-distribution-technical-scores-variation-deadlines/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2141942&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>“That’s what I’m trying to avoid,” said Ferguson, who still calls Quincy Jackson III her baby. She remembers a boy who dressed himself in three-piece suits, donated his allowance, and graduated high school at 16 with an academic scholarship and plans to join the military or start a business.
Instead, Ferguson watched as her once bright-eyed, handsome son sank into disheveled psychosis, bouncing between family members’ homes, homeless shelters, jails, clinics, emergency rooms, and Ohio’s regional psychiatric hospitals.
Over the past year, The Marshall Project – Cleveland and ∫⁄¡œ≥‘πœÕ¯ News interviewed Jackson, other patients and families, current and former state hospital employees, advocates, lawyers, judges, jail administrators, and national behavioral health experts. All echoed Ferguson, who said the mental health system makes it “easier to criminalize somebody than to get them help.”
State psychiatric hospitals nationwide have largely lost the ability to treat patients before their mental health deteriorates and they are charged with crimes. Driving the problem is a meteoric rise in the share of patients with criminal cases who stay significantly longer, generally by court order.
Patients Wait or Are Turned Away
Across the nation, psychiatric hospitals are short-staffed and consistently turn away patients or leave them waiting with few or no treatment options. Those who do receive beds are often sent there by court order after serious criminal offenses.
In Ohio, the share of state hospital patients with criminal charges jumped from about half in 2002 to .
The surge has coincided with a steep decline in total state psychiatric hospital patients served, down 50% in Ohio in the past decade, from 6,809 to 3,421, according to the . During that time, total patients served nationwide dropped about 17%, from 139,434 to 116,320, with state approaches varying widely, from adding community services and building more beds to closing hospitals.
Ohio Department of Behavioral Health officials declined multiple interview requests for this article.
The decline in capacity at state facilities unfurled as a spate of local hospitals across the country shuttered their psychiatric units, which disproportionately serve patients with Medicaid or who are uninsured. And the financial stability of is likely to deteriorate further after Congress passed President Donald Trump’s One Big Beautiful Bill Act, which slashes nearly $1 trillion from the federal Medicaid budget over the next decade.
The constricted flow of new patients through state hospitals is “absolutely” a crisis and “a huge deal in Ohio and everywhere,” said retired Ohio Supreme Court Justice Evelyn Lundberg Stratton. As co-chair of the state attorney general’s , Lundberg Stratton has spent decades searching for solutions.
“It hurts everybody who has someone who needs to get a hospital bed that’s not in the criminal justice system,” she said.


‚ÄòIt’s Heartbreaking’
Quincy Jackson III’s white socks stuck out of the end of a hospital bed as police officers stood watch.
At 5 feet, 7 inches tall, Jackson has a stocky build and robotic stare. Staff at Blanchard Valley Hospital in Findlay, Ohio, had called for help, alleging Jackson had assaulted a security guard.
“I’m sick; I take medication,” Jackson said to the officers, according to law enforcement body camera footage. His hands were cuffed behind his back as he lay on the bed, a loose hospital gown covering him.
Ferguson called it one of his “episodes” and said her son experienced severe psychosis frequently. In one incident, she said, Jackson “went for a knife” at her home.
From December 2023 through this July, Jackson was arrested or cited in police reports on at least 17 occasions. He was jailed at least five times and treated more than 10 times at hospitals, including three state-run psychiatric facilities. A recent psychiatric evaluation noted that Jackson has been in and out of community and state facilities since 2015.
Jackson is among a glut of people nationwide with severe mental illness who overwhelm community hospitals, courtrooms, and jails, eventually leading to backlogs at state hospitals.
High-Profile Incidents
That dearth of care is often cited by families, law enforcement authorities, and mental health advocates after people struggling with severe mental illness harm others. In the past six months, at least four incidents made national headlines.
In August, a homeless reportedly diagnosed with schizophrenia fatally stabbed a woman on a train. Also in August, police said a with a history of mental health issues killed three people, including a child, at a Target store. In July, a homeless who family members said had needed treatment for decades attacked 11 people at a Walmart store with a knife. In June, police shot and killed a reportedly diagnosed with schizophrenia after authorities said he attacked law enforcement.
Mark Mihok, a longtime municipal judge near Cleveland, told a spring that he had never seen so many people with serious mental illnesses living on the streets and “now punted into the criminal justice system.”
37-Day Wait for a Bed
At Blanchard Valley Hospital, sheriff’s deputies had taken Jackson from jail for a mental health check. But Jackson’s actions raised concerns.
In the body camera video, a nurse said Jackson was “going to be here all weekend. And we’re going to be calling you guys every 10 minutes.”
The officer responded: “Yeah, well, if he keeps acting like that, he’s going to go right back” to the county jail.
Within minutes, Jackson was taken back to jail, yelling at the officers: “Kill me, motherf—–. Yeah, shoot them, shoot them. Pop!”
Statewide, Ohio has about 1,100 beds in its six regional psychiatric hospitals. In May, the median wait time to get a state bed was 37 days.
That’s “a long time to be waiting in jail for a bed without meaningful access to mental health treatment,” said Shanti Silver, a senior research adviser at the national nonprofit Treatment Advocacy Center.
Long waits, often leaving people who need care lingering in jails, have drawn lawsuits in several states, including , , and , where a large 2014 class action case forced systemic changes such as expansion of crisis intervention training and residential treatment beds.
Ohio officials noticed bed shortages as early as 2018. State leaders assembled task forces and . They launched community programs, crisis units, and a statewide emergency hotline.
Yet backlogs at the Ohio hospitals mounted.
Ohio Department of Behavioral Health Director LeeAnne Cornyn, who left the agency in October, wrote in a May emailed statement that the agency “works diligently to ensure a therapeutic environment for our patients, while also protecting patient, staff, and public safety.”
Eric Wandersleben, director of media relations and outreach for the department, declined to respond to detailed questions submitted before publication and, instead, noted that responses could be publicly found in a governor’s working group report .
Elizabeth Tady, a hospital liaison who also spoke to judges and lawyers at the May gathering, said 45 patients were waiting for beds at Northcoast Behavioral Healthcare, the state psychiatric hospital serving the Cleveland region.
“It’s heartbreaking for me and for all of us to know that there are things that need to be done to help the criminal justice system, to help our communities, but we’re stuck,” she said.
Ohio officials added 30 state psychiatric beds by in Columbus and are planning in southwestern Ohio.
Still, Ohio Director of Forensic Services Lisa Gordish told the gathering in Cleveland that adding capacity alone won’t work.
“If you build beds ‚Äî and what we’ve seen in other states is that’s what they’ve done ‚Äî those beds get filled up, and we continue to have a waitlist,” she said.
This year, Jackson waited 100 days in the and Montgomery County jail for a bed at a state hospital, according to jail records.
Ferguson said she was afraid to leave him there but could not bail him out, in part, she said, because her son cannot survive on his own.
“There’s no place for my son to experience symptoms in the state of Ohio safely,” Ferguson said.

Sick System
Patrick Heltzel got the extended treatment Ferguson has long sought for her son, but he stabbed a 71-year-old man to death before getting it.
The 32-year-old is one of more than receiving treatment in Ohio’s psychiatric hospitals.
“People need long-term care,” Heltzel said in October, calling from inside Heartland Behavioral Healthcare, near Canton, where he has lived for more than a decade after being found not guilty by reason of insanity of aggravated murder. Inpatient care, he said, helps patients figure out what medication regimen will work and deliver the therapy needed “to develop insight.”
As he spoke, the sound of an open room and patients chatting filled the background.
“You have to know, ‚ÄòOK, I have this chronic condition, and this is what I have to do to treat it,’” Heltzel said.

As the ranks of criminally charged patients in Ohio’s hospitals have increased over the past decade, the shift has had an impact on patient care: The hospitals have endangered patients, have become more restrictive, and are understaffed, according to interviews with Heltzel, other patients, and former staff members, as well as documents obtained through public records requests.
Escapes and a Lockdown
Katie Jenkins, executive director of the National Alliance on Mental Illness Greater Cleveland, said the shift from mostly civil patients, who haven’t been charged with a crime, to criminally charged patients has changed the hospitals.
“It’s hard in our state hospitals right now,” she said. Unfortunately, she said, patients who have been in jail bring that culture to the hospitals.
In the first 10 months of 2024, at least nine patients escaped from Ohio’s regional psychiatric hospitals ‚Äî compared with three total in the previous four years, according to .
, two female patients at Summit Behavioral Healthcare near Cincinnati escaped after one lunged at a staff member. In another, a man broke a window and climbed out.
Most of the escapes, though, were not violent. Days after a patient at Northcoast during a trip to the dentist in a Cleveland suburb, state officials stopped allowing patients to leave any of the six regional hospitals.
to leaders at the hospitals said officials had seen “similarities across multiple facilities,” raising significant concern about “ensuring patient and public safety.”
For Heltzel, the inability to go on outings or to his mother’s house on the weekends was a setback for his treatment. In 2024, when the lockdown began, he had more freedom than most patients at the psychiatric hospitals, regularly leaving to go to the local gym and attend off-site group therapy.
His mother signed him out each Friday to go home for the weekend, where he drove a car and played with his 2-year-old German shepherd, Violet. On Sundays, Heltzel was part of the “dream team” at church, volunteering to operate the audio and slides.
Federal records reveal that, at Ohio’s larger state-run psychiatric hospitals, including Summit and Northcoast, patients and staff have faced imminent danger.
In 2019 and 2020, federal investigators responded to patient deaths, including two suicides in six months at Northcoast. One hospital employee told federal inspectors, “The facility has been understaffed for a while and it’s getting worse,” according to . “It is very dangerous out here.”
Disability Rights Ohio, which has a federal mandate to monitor the facilities, in October against the department. The advocacy group, alleging abuse and neglect, asked for records of staff’s response to a Northcoast patient who suffocated from a plastic bag over their head. At the end of October, the court docket showed the parties had settled the case.
Retired sheriff’s deputy Louella Reynolds worked as a police officer at Northcoast for about five years before leaving in 2022. She said the increase in criminally charged patients meant the hospitals “absolutely” became less safe. Her hip still hurts from a patient who threw her against a cement wall.
Reynolds said officers should be able to carry weapons, which they don’t, and that more staff are needed to handle the patients. Mandatory overtime was common, she said, and often staff would report to work and not “know when we would get off.”
A Disaster That Wasn’t Averted
Back at Heartland, Heltzel requested conditional release. The judge denied the release request.
Heltzel said it was devastating. He grew up Catholic and said, “I was kind of looking for absolution.”
Now, Heltzel said he is practicing acceptance. “Acceptance is all the more important to practice when you don’t agree with something,” Heltzel said, adding, “I’m a ward of the state.”
He still hopes to be released: “I just do what I can to move forward.”
Heltzel, like Jackson, had been hospitalized before and released.
In early 2013, Heltzel said, he asked his dad to kill him. “And he refused and I did smack him,” he said. Heltzel was sent to Heartland for a short stay ‚Äî about 10 days, according to his mother, Jan Dyer. She recalled “begging” the hospital staff to keep him.
Heltzel said he remembers not being ready to leave: “I was still sick, and I was still delusional.” Back at home, he said, he had a “sense of existential dread, like that all this horrible stuff was going to happen.” He stopped taking his medication.
Within weeks, Heltzel killed 71-year-old Milton A. Grumbling III at his home, placing him in a chokehold and stabbing him repeatedly, according to . He beat him with a remote control and then left, taking a Bible from the home, as well as a ring. Delusional with schizophrenia, Heltzel believed that Grumbling had sexually abused him in another life, according to the records.
A family member of the man he killed told the judge in 2023 that Heltzel should “stay in prison,” according to .
In denying his conditional release, judges cited Heltzel’s failure to take medication before killing Grumbling.
Jenkins, who said she worked at a state hospital for nine years before becoming the lead advocate for NAMI Greater Cleveland, said psychiatric medications can take as long as six weeks to become fully effective.
“So clients aren’t even getting stabilized when they’re being hospitalized,” Jenkins said.
‚ÄòHe’s Not a Throwaway Child’
In a July interview, Jackson said inconsistent care or unmedicated time in jail “worsens my symptoms.” Jackson was on the phone during a stay at a state psychiatric hospital.
Without medicine, “my head hurts, to be honest,” Jackson said, before asking to get off the phone because he was hungry. It was lunchtime. “Can you get the information from my mom?” Jackson said. “She has the records.”
After Jackson hung up the phone, Ferguson explained that “he says the food is excellent, so he does not want to miss it.” And, she added, the hospital staff had not yet seen the explosive side of her son.
In early September, after 45 days at Summit — his longest stay yet at a state psychiatric hospital — Jackson returned to the Montgomery County jail facing misdemeanor charges because of with staff at a Dayton behavioral health hospital. In court, Ferguson said, her son struggled to explain to the judge why he was there. On a video call from the jail days later, she saw him playing with his hair and ears.
“That tells me he’s not OK,” Ferguson said.
Before Jackson’s diagnosis more than a decade ago, Ferguson said, her son wasn’t a troublemaker. He had goals and dreams. And he’s still “loved and liked by a lot of people.”
“He’s not a throwaway child,” she said.
is a nonprofit news team covering Ohio’s criminal justice systems.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/race-and-health/criminally-ill-state-mental-psychiatric-hospitals-prisons-waitlists-ohio/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2122343&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The April wind was chilly at one of the tribes’ highest vistas in remote southeastern Idaho.
“Our goal is to bring fiber out here,” Goli said, sweeping one hand across the horizon. The landscape below is scattered with homes, bordered in the east by snowcapped mountain peaks and to the west by “The Bottoms,” where tribal bison graze along the Snake River.

In between, on any given day, a cancer patient drives to the reservation’s casino to call doctors. A young mother asks one child not to play video games so another can do homework. Tribal field nurses update charts in paper notebooks at patients’ homes, then drive back to the clinic to pull up records, send orders, or check prescriptions.
Three years ago, the Shoshone-Bannock Tribes were awarded more than $22 million during the first round of the federal Tribal Broadband Connectivity Program. But tribes that were awarded millions in a second round of funding saw their payments held up under the Trump administration. Last month, federal leaders to tribal broadband programs as part of a larger effort to “reduce red tape.” The National Telecommunications and Information Administration said it plans to “promote flexibility” and launch a new grant in the spring.
Federal regulators declined to provide details. The announcement comes after a year of upheaval for federal broadband programs, including the elimination of Digital Equity Act funding, which President Donald Trump has and a restructured $42 billion Broadband, Equity, Access, and Deployment program, which U.S. Commerce Secretary Howard Lutnick said was influenced by “.”
Across Indian Country and on the Fort Hall Reservation, high-speed despite billions set aside for tribes. In early November, U.S. Sens. Maria Cantwell (D-Wash.) and Brian Schatz (D-Hawaii) why funds already awarded had not been released to tribes and whether federal regulators were providing adequate technical assistance.
So far, the $3 billion tribal program has announced $2.24 billion in awards for 275 projects nationwide. But tribes that won awards have drawn down only about $500 million, according to a from the Commerce Department’s Office of Inspector General.
The agency on the broadband programs, offering tribal leaders two dates in January for online meetings.
The Shoshone-Bannock Tribes have drawn down less than 2% of their awarded funding and the program has not yet connected a single household, Goli said. NTIA spokesperson Stephen Yusko said the Shoshone-Bannock Tribes are still slated to get their full grant award and, he confirmed, future spending will not be subject to the administration’s recalibrations.
Gaps in high-speed internet can be profound and urgent on tribal lands. Tribal members are historically underserved and, on average, live with the highest rates of chronic illnesses and die than the average U.S. resident.
Diabetes and high suicide rates are among the most pernicious tribal health challenges — and federal research confirms telehealth . A showed that people tend to live sicker and die younger in America when they live in dead zones, or places where poor internet access intersects with shortages of health care providers, leaving patients who need it most unable to use telehealth.
“We’re in survival mode,” said Nancy Eschief Murillo, a longtime Shoshone-Bannock leader. The tribes, which have an on-site clinic, need more health care both in person and with telehealth, she said. “Right now, our reservation? We don’t have accessibility.”

‘Not 100% Accurate’
Inside a trailer that serves as the temporary headquarters for Fort Hall’s tribal broadband office, Goli sat at a desk in June and scanned the Federal Communications Commission’s most recent online map of the reservation.
As the tribes’ broadband project manager, Goli didn’t like what she saw on the map. Blue hexagons highlighted varying rates of high-speed coverage and signified that high-speed internet is available on much of the reservation. Companies have told federal regulators they provide fast transmission speeds to homes there.
“These are untrue,” Goli said. Fort Hall has about 2,400 households, and nearly all of them live without high-speed internet, she said.
When it comes to tracking who on a reservation has high-speed internet, “everybody acknowledges, including the FCC, that the map is not 100% accurate,” said Robert Griffin, co-chair of the Fiber Broadband Association Tribal Committee, an industry trade group. He is also the broadband director for the Choctaw Nation of Oklahoma.
Attempting to correct the maps is one of the many tasks Goli has taken on since becoming the Shoshone-Bannock Tribes’ broadband project manager in January 2023 — seven months after the tribes won the award.
A series of hurdles, including flaws in the plan initially approved by the federal government and a cyberattack, have delayed the project, she said. The attack hit in August 2024 and for months shut down nearly all phones and computers on the reservation.
“We didn’t have access to any of our information,” Goli told ∫⁄¡œ≥‘πœÕ¯ News this month, adding that the tribes are still “in recovery mode” from the attack.
Goli, who grew up on the reservation and still plays basketball at the tribal gym, left her job as a data analyst in Seattle to return home to be with family and to work. For two years, and with no broadband industry experience, Goli has overseen the multimillion-dollar grant without a staff.
Her first task, she said, was to collect data that could help create a realistic plan to deliver broadband to every home on the reservation. “Data tells a story,” Goli said.
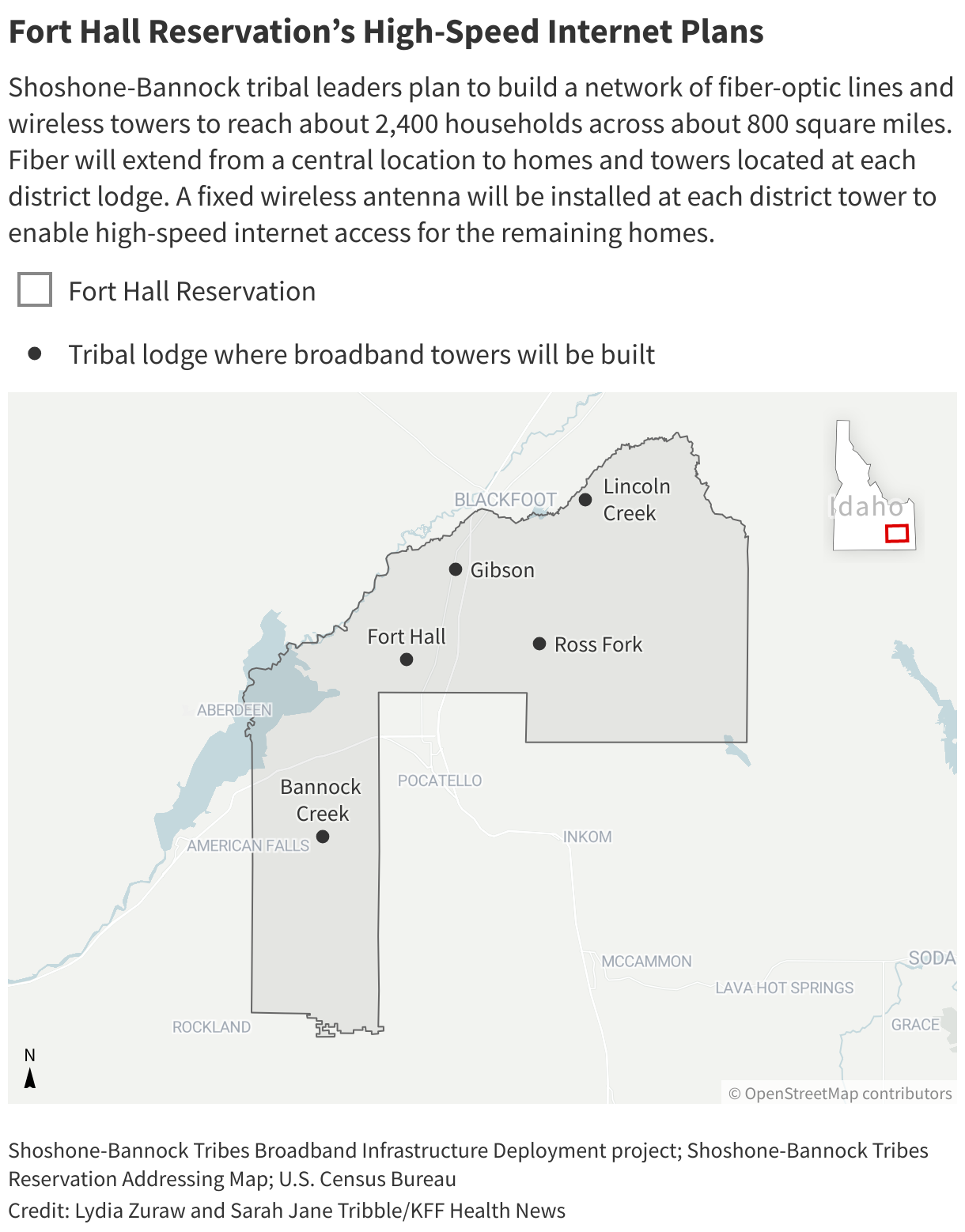
Fort Hall and many other tribal lands are remote with rugged, expansive terrain. To build fiber-optic cables underground, the tribes must navigate lava rock and work with the Bureau of Indian Affairs to get permits. To build communications towers, the tribes must ensure they follow migratory bird rules for American bald eagles. To provide wireless connections, the tribes must buy or license spectrum from federal regulators, Goli said.
When the federal tribal broadband program launched, more than — pitching projects totaling $5 billion — submitted requests to the NTIA. During a later round of funding, asked for more than $2.6 billion, even though only $980 million was available. There are 574 federally recognized tribes in the United States.
The tribal program funding was not enough to “build out Indian Country,” said Joe Valandra, chief executive and chairman of the broadband consulting firm Tribal Ready. Valandra is a member of the Rosebud Sioux Tribe of South Dakota.
Congress created the tribal program to be used in combination with funds from the larger $42 billion Broadband, Equity, Access, and Deployment, or BEAD, program, Valandra said.
But now, it seems “the administration has no appetite for expensive broadband infrastructure builds in rural areas,” said Jessica Auer, a senior researcher with the community broadband networks team at the Institute for Local Self-Reliance, a research and advocacy nonprofit.
Auer, who has of tribal programs, said the administration may think the money already given to states for BEAD, as well as the use of satellite internet connections, will be enough for tribal lands.
“They seem to have a strong interest in declaring this problem solved,” she said. Low-earth-orbit satellites, though, are costly for the consumer and do not always offer the consistent high speeds they should, she said.
Goli’s plan does not include the use of satellites. On Fort Hall, the few households that have fast speeds now buy Starlink, but tribal leaders say the $80 to $120 monthly subscription costs are too expensive for most members.
The newly revised plan will use a hybrid of fiber-optic cables and wireless internet to ensure that people can “live their lives, whether it be health, education, telehealth,” Goli said.

The Test
Ladd Edmo, a councilman for the Shoshone-Bannock Tribes, thinks the tribal broadband project is taking too long.
Goli “is doing the best she can,” Edmo said.
But when he thinks about the millions waiting to be spent, Edmo said, he worries federal regulators “can just grab it back.”
“I’m not afraid of the current administration,” said Edmo, who is in his fifth term on the tribes’ business council. “I just think that they’re looking for money everywhere they can.”
Edmo lives about half a mile from the Fort Hall townsite and said he can’t really use his internet because he “gets a tremendous amount of buffering.” When he travels to doctors for his prostate cancer treatment, Edmo has them print paper schedules to keep track of his treatment.
He said he is not a big fan of telehealth, “probably because I don’t know how to use it.”


For 53-year-old Carol Cervantes Osborne, who also lives on the reservation, having internet is a necessity. Osborne is in constant pain from severe rheumatoid arthritis.
“I’m just all broke down,” Osborne said as she stared at the open pasture last June. She talked about how she misses riding cattle roundups. At times, Osborne has been bed-bound because of her arthritis and bad knees. She said she tapped her credit line, which uses land and cattle as collateral, and signed up for Starlink so that she can connect with doctors remotely through telehealth appointments.
“I’m poor because of it, but we’ve got to have it,” Osborne said.
Meanwhile, nearly 15 months after the cyberattack, Goli said the tribes are beginning to hire vendors.
“Things happen very slow when it comes to processing things in the tribal government,” Goli said, adding there are a lot of “checks and balances.”
This month — as the holidays approached — Goli said she was excited.
“We’ve actually started our first segment of fiber,” Goli said. The engineering work is done, and they have begun issuing permits, she said. The fiber-optic lines, built by a private vendor, will cover a two-mile segment on the northern end of the reservation. The line will come from outside the reservation and connect to the tribes’ data hub, which is an old radio station still being converted into broadband offices.
“It’s our first segment, and we’re really using this as a test,” Goli said.

Eventually, the old radio station will be central to operations, with fiber-optic cable lines that web out over about 800 square miles to reach the reservation’s five district lodges. Each lodge will establish a communications tower, which will use the fiber line to power wireless antennas that will then provide high-speed internet to the reservation’s most remote homes.
Goli said the tribes are applying for another extension — and, she said, they would not be the only award winners of the Tribal Broadband Connectivity Program to ask for more time. Working with tribes, she said, takes time.
“It really saddens me that we’ve been left behind all these years,” Goli said, but “this is our opportunity. We want to do it right, slow and steady.”
Sarah Jane Tribble, ∫⁄¡œ≥‘πœÕ¯ News’ chief rural correspondent, spent more than a year interviewing Frances Goli through calls, texts, and emails. She traveled to Fort Hall Reservation twice, having received tribal approval to visit the land: in spring 2024 and again in summer 2025. Tribble also reviewed publicly requested copies of the tribal contract and interviewed dozens of industry and regulatory broadband experts.
This <a target="_blank" href="/rural-health/internet-broadband-digital-divide-tribal-health-disparities/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2131137&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>These are a few ideas proposed by states in their bids to win a portion of the new $50 billion federal Rural Health Transformation Program. Congress approved the five-year spending plan in the One Big Beautiful Bill Act, the same law that codified nearly $1 trillion in Medicaid spending reductions.
That law is expected to have an outsize effect on rural America, where the cuts are expected to slash health funding by over 10 years.
So, how the rural health fund money rolls out is being watched closely by people like Alan Morgan, chief executive of the National Rural Health Association. State applications were due in early November, and federal officials have promised to announce awards by Dec. 31.
“Let’s be clear,” Morgan said. “The hospital CEOs, the clinic administrators, the community leaders: They’re going to want to know what their states are doing.”
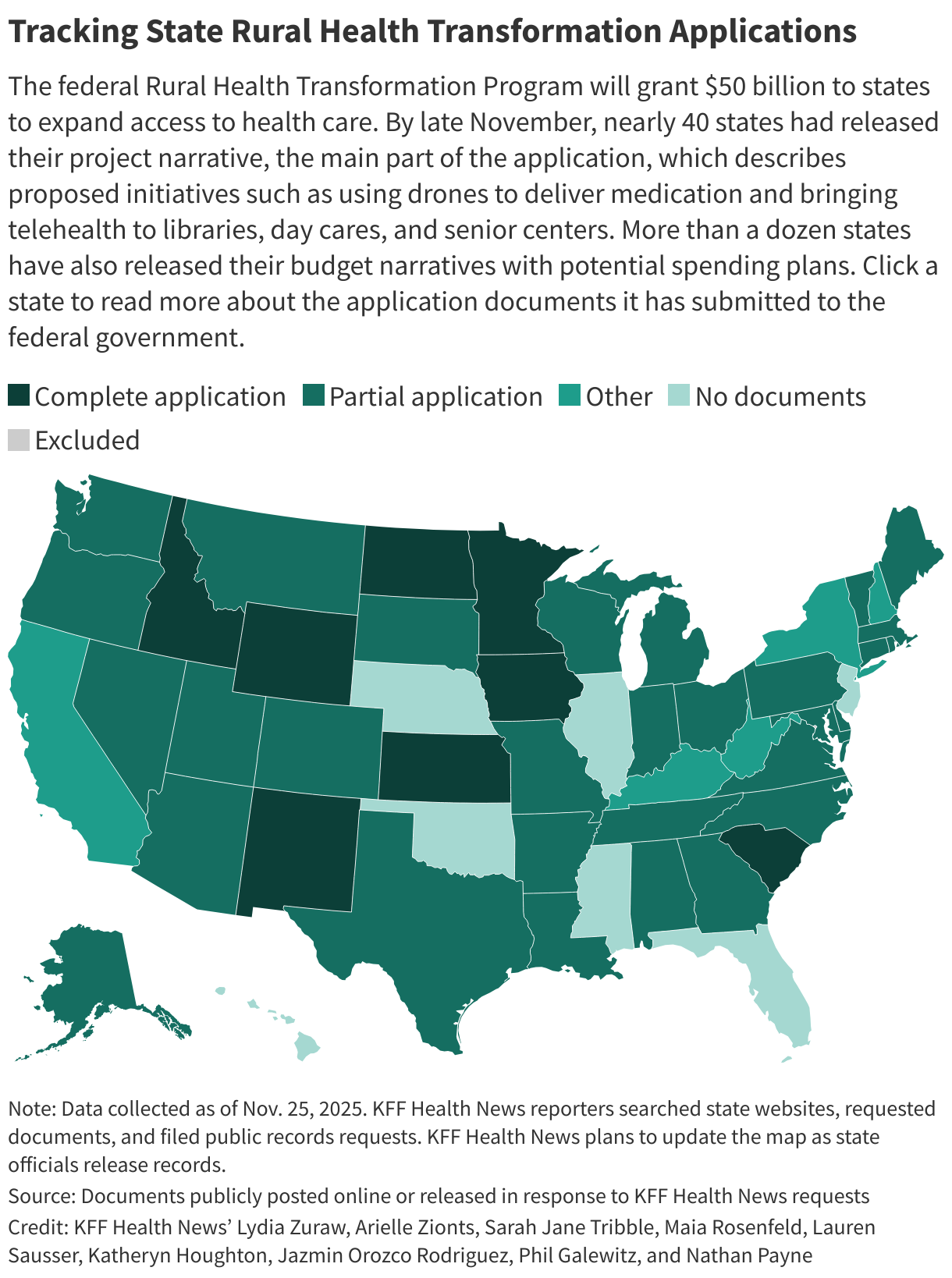
As of last week, nearly 40 states had released project narratives, the main part of the application, which describes their proposed initiatives. Those include Maryland’s plan to create demand for healthy foods in addition to increasing their supply.
“Many rural Maryland children and adults have low intake of fruits, vegetables, and water, and limited engagement in physically active behaviors,” the state said in its application. Among other initiatives, officials propose to start mobile markets and install refrigerators and freezers to improve access in rural areas with limited grocery stores.
More than a dozen states have also released their budget narratives. And a handful of states — Idaho, Iowa, Kansas, Maine, Minnesota, New Mexico, North Dakota, Pennsylvania, South Carolina, and Wyoming — have released their full applications.
∫⁄¡œ≥‘πœÕ¯ News collected application documents through both informal and formal public records requests and published them on a map.
Heather Howard, a professor of the practice at Princeton University, said she is “pleasantly surprised at how transparent the states have been.” Princeton’s State Health and Value Strategies program is also .
But others are not pleased with what federal regulators are (or are not) releasing. Centers for Medicare & Medicaid Services spokesperson Catherine Howden said applications will not be released while they are being reviewed.
CMS plans to follow the federal regulations when releasing information about the rural health program, Howden said.
In Illinois, where Democrats control state politics, Rep. Nikki Budzinski joined other Democratic members of the state’s U.S. House delegation in to CMS Administrator Mehmet Oz last month asking for “full and fair consideration” of their state’s application.
“I am very concerned about retaliation,” she said.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/the-week-in-brief-rural-health-transformation-program-fund-transparency/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2127581&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The Trump administration, which has promised “radical transparency,” that it plans to publish the “project summary” for states that win awards. Following the lead of federal regulators, many states are withholding their complete applications, and some have refused to release any details.
“Let’s be clear,” said Alan Morgan, chief executive of the National Rural Health Association. “The hospital CEOs, the clinic administrators, the community leaders: They’re going to want to know what their states are doing.” The NRHA’s members include struggling rural hospitals and clinics, which would benefit from the Trump administration’s Rural Health Transformation Program.
Morgan said his members are interested in what states propose, which of their ideas are approved or rejected, and their budget narratives, which detail how the money could be spent.
Improving rural health care is an “insanely complicated and difficult task,” Morgan said.
The five-year Rural Health Transformation Program was approved by Congress in a law — the One Big Beautiful Bill Act — that also drastically cuts Medicaid spending, on which rural providers heavily depend. It’s being watched closely because it’s a much-needed influx of funds — with a caveat from the Trump administration that the money be spent on transformational ideas, not just to prop up ailing rural hospitals.
The law says half of the $50 billion will be divided equally among all states with an approved application. The rest will be distributed through a points-based system. Of , $12.5 billion will be allotted based on each state’s rurality. The remaining $12.5 billion will go to states that on initiatives and policies that, in part, mirror the Trump administration’s “” objectives.
Health and Human Services Secretary Robert F. Kennedy Jr. has repeatedly promised to open the government to the American people. His agency has devoted to “radical transparency.”
“We’re working to make this the most transparent HHS in its 70-year history,” in written testimony to lawmakers in September.
Lawrence Gostin, a professor of public health law at Georgetown University, said HHS is “acting in a way that utterly lacks transparency” and that the public has the right to demand “greater openness and clarity.” Without transparency, the public cannot hold HHS accountable, he said.
Centers for Medicare & Medicaid Services spokesperson Catherine Howden said the agency will follow the federal regulations when releasing information about the rural health program.
Grant applications are “not released to the public during the merit review process,” Howden said, adding, “The purpose of this policy is to protect the integrity of evaluations, applicant confidentiality, and the competitive nature of the process.”
Democrats and many health care advocates are concerned politics will affect how much money states get.
“I am very concerned about retaliation,” said Rep. Nikki Budzinski (D-Ill.). Because Democrats control her state’s politics, “our application might not be as seriously considered as other states that have Republican leadership,” she added.
Illinois’ Democratic members of the U.S. House to CMS Administrator Mehmet Oz in November asking for “full and fair consideration” of their state application. Illinois officials have not yet released their state’s proposal to ∫⁄¡œ≥‘πœÕ¯ News, which has a pending public records request.
Heather Howard, a professor of the practice at Princeton University, said she is “pleasantly surprised at how transparent the states have been.”
Howard directs the university’s State Health and Value Strategies program, which the rural health fund, and praised most states for publicly posting their project summaries.
“To me, it speaks to the intense interest in this program,” Howard said. Her team, reviewing about two dozen state summaries, found themes including expansion of home-based and mobile services, increased use of technology, and workforce development initiatives like scholarships, signing bonuses, and child care assistance for high-demand positions.
“I think it’s exciting,” Howard said. “What’s great here is the experimentation we’re going to learn from.”
Telerobotics appeared in Georgia’s and Alabama’s applications, she said, including a proposal to use robotic equipment for remote ultrasounds.
Another theme that “warms my heart,” Howard said, was the effort among states to create advisory groups or committees, including in Idaho, where work groups are expected to focus on technology, workforce development, tribal collaboration, and behavioral health.
All 50 states submitted applications to federal regulators by the Nov. 5 deadline and awards will be announced by the end of the year, according to CMS.
As of late November, nearly 40 states had released their project narrative, the main part of the application, which describes proposed initiatives, according to ∫⁄¡œ≥‘πœÕ¯ News tracking. More than a dozen states have also released their budget narratives.
Also as of late November, only a handful of states — Idaho, Iowa, Kansas, Minnesota, New Mexico, North Dakota, South Carolina, and Wyoming — had released all parts of the application.
∫⁄¡œ≥‘πœÕ¯ News filed public records requests for states’ complete applications. Some states have refused to release any of their application materials.
Nebraska, for example, rejected a public records request, saying its application materials are “proprietary or commercial information” that “would give advantage to business competitors.”
Kentucky shared its application summary but said the remainder of the application is a “preliminary draft” not subject to release under state laws.
Erika Engle, a spokesperson for Hawaii Gov. Josh Green, said the governor “is committed to transparency” but declined to share any of the state’s proposal.
Hawaii and other states are still processing formal public records requests.
The rural health program is part of the July law projected to reduce federal Medicaid spending in rural areas by 10 years.
Those cuts are expected to affect rural health facilities’ bottom lines, threatening their ability to stay open. A recent Commonwealth Fund report found that rural areas continue to to primary care. But the guidelines for the rural health program say states can use only 15% of their new funding to pay providers for patient care.
Between the Medicaid cuts and funding boost from the new program, “there’s real opportunity for national policy to impact rural, both in the negative and the positive potentially,” said Celli Horstman, a senior research associate at the New York-based policy think tank who co-authored the report.
Among the publicly available rural health transformation proposals, Democratic-leaning states show support, or are willing to adopt, some of the administration’s goals but will lose out on points from eschewing others.
For example, New Mexico said it would introduce legislation requiring students to take the Presidential Fitness Test and physicians to complete continuing education courses on nutrition. But it won’t prevent people from using their Supplemental Nutrition Assistance Program benefits to buy “non-nutritious” foods such as soda and candy.
Many states want to invest in technology, including telehealth, cybersecurity, and remote patient monitoring equipment. Other themes include increasing access to healthy food, improving emergency services, preventing and managing chronic illnesses, and enlisting community health workers and paramedics for home visits.
Specific proposals include:
- Arkansas wants to spend $5 million through its “FAITH” program — Faith-based Access, Interventions, Transportation, & Health — to enlist rural religious institutions to host education and preventive screening events. Congregations could also install walking circuits and fitness equipment.
- Alaska, which historically relied on dogsled teams to bring medication to remote areas, is looking to test the use of “unmanned aerial systems” to speed up pharmacy deliveries to such communities.
- Tennessee wants to increase access to healthy activities by spending money on parks, trails, and farmers markets.
- Maryland wants to start mobile markets and install refrigerators and freezers to improve access to fresh, healthy food that often spoils in rural areas with few grocery stores.
State Sen. Stephen Meredith, a Republican who represents part of western Kentucky, said he still expects rural hospitals to close despite his state’s rural health transformation program.
“I think we’re treating symptoms without curing the disease,” he said after listening to a presentation on Kentucky’s proposal at .
Morgan, whose organization represents rural hospitals likely to close, said the state’s ideas may sound good.
“You can craft a narrative that sounds wonderful,” he said. “But then translating the aspirational goals to a functioning program? That’s difficult.”
∫⁄¡œ≥‘πœÕ¯ News staffers Phil Galewitz, Katheryn Houghton, Tony Leys, Jazmin Orozco Rodriguez, Maia Rosenfeld, Bram Sable-Smith, and Lauren Sausser contributed to this report.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/rural-health-transformation-program-cms-state-applications-transparency/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2123985&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Kopplin, a physician assistant who works with seniors, low-income people, and mental health patients in the rural Black Hills, shared her thoughts at a meeting hosted by state officials.
South Dakota’s leaders did a “good job of diving in” and asking questions to get “deeper at the root of the problem,” she said.
Kopplin later told ∫⁄¡œ≥‘πœÕ¯ News how one of her rural patients recently missed two appointments because of a broken-down car and no access to public transportation.
Nationwide, health care workers like Kopplin and thousands of others — from patient advocates to technology executives — flocked to town halls or online portals during the seven weeks state leaders had to craft and submit their applications for the Rural Health Transformation Program to the federal Centers for Medicare & Medicaid Services. That deadline was Nov. 5.
“We will give $50 billion away by the end of the year,” CMS Administrator Mehmet Oz said Nov. 6 at a Milken Institute event in Washington. He said all 50 states had submitted applications.
The program will “allow us to right-size the health care system,” Oz said, adding that innovations from the rural work “will spill over to suburban and urban America as well.”
Among applications and summaries publicly shared by states, themes include workforce development, telehealth, and access to healthy food. In Kansas, leaders want to build a “Food is Medicine” program. Wyoming officials propose a new program called “BearCare,” a state-sponsored health insurance plan that patients could use only after medical emergencies.
But many health policy experts and Democrats are raising alarms that the Republican-backed program will become a “slush fund.” Critics worry it will fail to reach the small-town patients they say need it most, especially as states face nearly a trillion dollars in Medicaid spending reductions over the next decade. Medicaid, a joint federal-state program, serves nearly rural Americans.
“The status quo is tremendous distress in rural communities,” said Heather Howard, a professor of the practice at Princeton University and director of the university’s State Health and Value Strategies program, which is tracking the rural health fund. The new funding won’t be enough to offset the Medicaid losses, she said.
Congressional Republicans added the five-year, $50 billion Rural Health Transformation Program as a last-minute sweetener to President Donald Trump’s massive tax-and-spending legislation. The move helped win support for the One Big Beautiful Bill Act from conservative holdouts who worried that the Medicaid cuts in the bill would harm rural hospitals in their states.
In Montana, which hosted an online public forum before submitting its application, a nonprofit director pitched youth peer support as a way of battling high suicide rates. A registered nurse asked state leaders to “think maybe even bigger” and consider statewide universal health care.
And in Georgia, a technology-focused chain of primary care clinics that serves seniors proposed expanding its operations into that state in its online public comment. A rural grant writer asked for “safe and stable housing.”
The law says half of the $50 billion will be divided equally among all states with an approved application. The rest will be doled out according to a points-based system. Of , $12.5 billion will be allotted based on each state’s rurality. The remaining $12.5 billion will go to states that on initiatives and policies that, in part, mirror the Trump administration’s “” objectives.
Top Senate Democrats have raised alarms about the rural health program. They include Ron Wyden of Oregon and Tina Smith of Minnesota, who a federal watchdog agency to investigate the fairness and implementation of the fund. Taylor Harvey, a Wyden aide, said the Government Accountability Office has confirmed it will investigate.
According to , no less than a quarter of states with an approved application may share the second half of the funding each fiscal year, CMS spokesperson Catherine Howden said. The agency plans to publish summaries of approved state projects, .
A handful of conservative-leaning states ‚Äî including Texas, Arkansas, Louisiana, and Oklahoma ‚Äî have already instituted regulatory and legislative initiatives, such as prohibiting “non-nutritious” foods in benefit programs, that in the program application process.
Michael Chameides, a county supervisor in rural New York, said he fears the money could “be used in ways that would hurt certain states or reward certain states.” Chameides is also the communications and policy director with the Rural Democracy Initiative, a national advocacy organization that released last month.
Edwin Park, a research professor at Georgetown University’s Center for Children and Families, said federal lawmakers gave Oz and his agency “really excessive discretion” when awarding the money.
Federal administrators have added rules that aren’t within the statute that created the program, Park said. For example, its application guidelines say states cannot use more than 15% of their funding to pay providers for patient care ‚Äî payments that are expected to take a hit due to the Medicaid cuts.
Georgetown’s health policy experts and Democrats aren’t the only ones with concerns. and in Ohio worry the money will go to large health systems instead of smaller, independent hospitals that serve people within their rural communities.
CMS’ Oz repeated the idea of getting “big hospitals to adopt smaller institutions” at the Washington gathering after applications were filed. He used similar language at a rural health summit hosted by South Dakota-based Sanford Health. “How do we get big hospitals to adopt smaller hospitals? Not to take them over, but to keep them viable by giving them good telehealth services, specialty support, radiology support,” he said at the October event.
Sanford owns or manages dozens of hospitals and hundreds of clinics and long-term care centers, as well as a health insurance company. The system reported about $81 million in operating income during the first six months of fiscal year 2025, according to .
Last year, Sanford opened a “command center” for its systemwide telehealth initiative. It launched a telehealth expansion in 2021 and offers virtual care for 78 medical specialties, Sanford President and CEO Bill Gassen said.
“We’ve tried to imagine, what if that number doubles?” Gassen said. The startup costs for telehealth are high, he said, and the rural fund could be a unique opportunity “for us to make virtual care available to more patients, to more communities, to more hospitals and health systems across the country.”
Gassen, who is set to chair the American Hospital Association in 2027, said Sanford leaders have met with state and federal officials, including Oz, whom he’s known for years, and Chris Klomp, a top deputy at CMS and a senior adviser to Health and Human Services Secretary Robert F. Kennedy Jr.
The word “telehealth” appears 36 times in the rural health program’s 124-page application guidelines. But Don Robbins Jr., chief executive of a small hospital on the Illinois-Kentucky border, chuckled at the idea of using the funding for that purpose.
Robbins, whose 25-bed Massac Memorial Hospital averages five to seven patients in its beds each day, said his hospital does not regularly offer telehealth. Even if it did, he said, patients living more than a mile outside of town couldn’t use it because they don’t have a good internet connection.
The small hospital reported a $31,314 loss in September, Robbins said. “I think if we get anything out of it,” Robbins said of the rural health program, “we’ll be lucky.”
Kopplin, the physician assistant who attended the South Dakota meeting, is cautiously optimistic about the rural health fund. She views it as a wonderful chance for states to test out ideas and learn from what works and what doesn’t.
But “in a lot of ways this bill is going to be a band-aid approach” for rural health, she said. “It’s not really going to fix the problem.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/states-competing-rural-health-transformation-program-cms/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2113931&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
WASHINGTON — Nationwide, states are racing to win their share of a new $50 billion rural health fund. But helping rural hospitals, , is quickly becoming a quaint idea.
Rather, states should submit applications that “rebuild and reshape” how health care is delivered in rural communities, Centers for Medicare & Medicaid Services official Abe Sutton said late last month during a daylong meeting at Washington, D.C.’s Watergate Hotel. Simply changing the way government pays hospitals has been tried and has failed, Sutton told the audience of more than 40 governors’ office staffers and state health agency leaders ‚Äî some from as far away as Hawaii.
“This isn’t a backfill of operating budgets,” said Sutton, CMS’ innovation director. “We’ve been really clear on that.”
Rural hospitals and clinics nationwide face a looming financial catastrophe, with President Donald Trump’s massive tax-and-spending law expected to slash federal Medicaid spending on health care in rural areas by . Congressional Republicans added the one-time, five-year Rural Health Transformation Program as a last-minute sweetener to win the support of conservative holdouts who worried about the bill’s financial fallout for rural hospitals.
Yet, the words used by CMS Administrator Mehmet Oz and his agency’s leaders to describe the new pot of cash are generating tension between legacy hospital and clinic providers and new technology-focused companies stepping in to offer new ways to deliver health care.
It’s “what I would call incumbents versus insurgents in the rural space,” said Kody Kinsley, a senior policy adviser at the Institute for Policy Solutions at the Johns Hopkins School of Nursing.
Applications are due Nov. 5. The money will be awarded to states by the end of the year and distributed over five years.
Half of the $50 billion will be divided equally among all states with an approved application; the other half will go to states that win points. Of , $12.5 billion will be allotted based on a formula that calculates each state’s rurality. The remaining $12.5 billion will go to states that on initiatives and policies that mirror the Trump administration’s objectives.
The specific policy goals such as implementing the Presidential Fitness Test and restrictions to food assistance, as well as broader investment strategies around remote care services, data infrastructure, and consumer-facing technology tools, which CMS identified as “symptom checkers and AI chatbots.”
In September, after CMS officials released the application, Republican members of Congress from states with Democratic governors , concerned their states might direct the money to urban areas. In a letter to Oz and Health and Human Services Secretary Robert F. Kennedy Jr., they said the money “will serve as a lifeline for rural and at-risk hospitals in our communities that are already struggling to keep their doors open.”
Smaller hospitals fear they will get “a tiny little slice” of each state’s share, said Emily Felder, who leads the health care practice at Brownstein Hyatt Farber Schreck, a law firm whose clients include rural hospital systems.
“There’s a lot of frustration,” Felder said.
But Kinsley, who was previously North Carolina’s secretary of health and human services, said using this money only to shore up a balance sheet “is really just throwing good money after bad.” In contrast, he said, insurgents such as technology-driven startups can offer new strategies.
One of those companies vying for funding is , a Silicon Valley-based company that contracts with Medicare managed care insurers. Using artificial intelligence analytics, Homeward helps patients get care in their home and with local providers.
The company manages the health of 100,000 rural Michigan patients enrolled in insurance, said Homeward co-founder and chief executive Jennifer Schneider. The company was a sponsor for the Watergate summit. It also has ongoing meetings with Oz and his team, Schneider said.
“They’re doing their job, and they’re talking to a lot of people in the ecosystem and really eager to learn from those of us that have been in the system,” Schneider said. “We’re one of many in that position.”
∫⁄¡œ≥‘πœÕ¯ News requested an interview with Alina Czekai, director of the Office of Rural Health Transformation. CMS spokesperson Alexx Pons said the agency was “unable to accommodate facilitation of any interview.”
Instead, CMS provided an emailed statement from Oz saying the program “will help states and communities reimagine what’s possible for rural healthcare.”
Brock Slabach, chief operations officer of the National Rural Health Association, the largest organization representing rural hospitals and clinics, said the money would best be used to help pay for transformation that isn’t “sexy” or “revolutionary.”
“If what we end up with is we have a wearable for every rural patient, I don’t think that’s transformational,” Slabach said, referring to digital health monitors such as fitness-tracking watches.
Slabach, a onetime small-hospital chief executive and an unofficial adviser to hundreds of rural facilities nationwide, named a few ideas for the money ‚Äî including paying for capital improvements such as electronic health records or equipment, loan repayment programs to aid workforce development, and creating “SWAT” teams that rescue rural hospitals on the brink of closure.
More than 150 rural hospitals nationwide since 2010 ‚Äî a statistic cited by CMS’ Sutton that is well known among industry watchers. The Sheps Center at the University of North Carolina, which compiles the closure data, also released to help states calculate how rural they are for their applications.
State applications will be reviewed by a panel, with some reviewers from within the government but others outside it, said Kate Sapra, acting deputy director of the Office of Rural Health Transformation, speaking at the Watergate.
“We will train them in the scoring criteria,” Sapra said, adding that the panelists will not be coming from “your state” and will need to fill out conflict-of-interest forms. A portion of money each state gets will be reevaluated annually based on the progress it makes on its goals and priorities, .
States are creating stakeholder groups, asking for public comment, and working with their health agencies. Some, such as and , are hiring consultants.
In Montana, a collection of health providers and associations proposed a list of ideas for the cash, including creating a loan repayment fund for rural clinicians to try to ease worker shortages.
“It’s one-time money, and it’s a little bit of money,” said David Mark, a doctor who is the CEO of One Health, which has clinics dotted across eastern Montana and Wyoming. A state could receive a minimum of $100 million a year for five years if all 50 states have applications approved.
“How do you accomplish goals of a health care system transformation with an infusion of money like that?” Mark said.
Neither Montana nor Wyoming — vast, rural states — sent leaders to the Watergate summit, according to a copy of the attendees list. In the afternoon, attendees could rotate among planning tables and meet with corporate sponsors such as the electronic health records behemoth Epic and the emergency services company Global Medical Response.
Wyoming Department of Health Deputy Director Franz Fuchs confirmed his state did not send representatives to the event, because they were “stretched with other commitments.” Montana, Wyoming, and other states submitted signaling they will apply for the funds. CMS did not respond to questions about how many and which states have submitted letters.
During the Watergate event, hints of brewing competition among states began to surface.
“I think Arkansas’ application is going to be better than yours,” seasoned political adviser Jack Sisson said with a smile during a morning panel.
The audience laughed. Sisson, who recently left his job as health adviser for Arkansas Gov. Sarah Sanders, had interrupted Michael Hendrix, policy adviser to another Republican governor, Tennessee’s Bill Lee.
“See, this is the kind of friendly competition that CMS is hoping for,” Hendrix said. He grinned, thanked Sisson, and added, “I look forward to us both winning.”
∫⁄¡œ≥‘πœÕ¯ News Montana correspondent Katheryn Houghton contributed to this report.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/rural-health-fund-medicaid-cuts-hospitals-cms-maha/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2101989&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>“They have health care needs, but they don’t have the digital skills,” said Waiters, who is a digital navigator for an Alabama nonprofit. Her work has involved giving away computers and tablets while also teaching classes on how to use the internet for work and personal needs, like banking and health. “It’s like a foreign space.”
Those stories are now bittersweet.
Waiters is part of a network of digital navigators across the country whose work to bring others into the digital world was, at least in part, propped up by a $2.75 billion federal program that abruptly canceled funding this spring. The halt came after President Donald Trump platform that the Digital Equity Act was unconstitutional and pledged “no more woke handouts based on race!”
The act the money should benefit, including low-income households, older residents, some incarcerated people, rural Americans, veterans, and members of racial or ethnic minority groups. Politicians, researchers, librarians, and advocates said defunding the program, along with other changes in federal broadband initiatives, jeopardizes efforts to help rural and underserved residents participate in the modern economy and lead healthier lives.
“You could see lives change,” said Sam Helmick, president of the American Library Association, recalling how they helped grandpas in Iowa check prescriptions online or laid-off factory workers fill out job applications.
The Digital Equity Act is part of the sweeping 2021 infrastructure law, which included $65 billion to build high-speed internet infrastructure and connect millions without access to the internet.
This year, Congress once again pushed for a modern approach to help Americans, mandating that state leaders prioritize new and emerging technologies through its $50 billion Rural Health Transformation Program.
A found that nearly 3 million people in America live in areas with shortages of medical professionals and where modern telehealth services are often inaccessible because of poor internet connections. The analysis found that in about 200 mostly rural counties where dead zones persist, on average than people in the rest of the country. Access to high-speed internet is among a host of social factors, like food and safe housing, that help people lead healthier lives.
“The internet provides this extra layer of resilience,” said Christina Filipovic, who leads the research for an initiative of the Institute for Business in the Global Context at Tufts University. The research group that access to high-speed internet correlated with fewer covid deaths, particularly in metro areas.
During the covid-19 pandemic, federal lawmakers launched a subsidy program paid for by the infrastructure law. That aid, called the Affordable Connectivity Program, aimed to connect more people to their jobs, schools, and doctors. In 2024, Congress did not renew funding for the subsidy program, which had enrolled about .
This year, U.S. Commerce Secretary Howard Lutnick the infrastructure law’s construction initiative ‚Äî known as the Broadband Equity, Access, and Deployment Program, or BEAD ‚Äî after announcing plans to . More than 40 states and territories have submitted final proposals to extend high-speed internet to underserved areas under the administration’s new guidelines, according to a .
In May, the Digital Equity Act’s funding was terminated within days of Trump’s Truth Social post. While many states in 2022 had received money to plan their programs, the next round of funding, designated for states and agencies to implement the plans, had largely been awarded but not distributed.
Instead, federal regulators ‚Äî including the National Telecommunications and Information Administration, the federal agency overseeing implementation of the Digital Equity Act ‚Äî that the grants would be terminated. The grants were created and administered with “unconstitutional racial preferences,” according to the letter.
In Phoenix, officials learned in January that the city was slated to get $11.8 million to increase internet access and teach digital literacy, but they received an email May 20 stating that all grants, “except for grants to Native Entities,” had been terminated. “It’s a shame,” said Phoenix Mayor Kate Gallego, a Democrat. The money, she said, would have helped 37,000 residents get internet access.
Georgia’s Democratic leaders in July to Lutnick and NTIA’s then-acting administrator, Adam Cassady, urging reinstatement of the money, noting that the federal cut ignores congressional intent and violates public trust.
The act’s creator, Sen. Patty Murray (D-Wash.), said in May that Republican governors in 2024 supported the law and its funding when each state touted completing its required digital equity plans and asked for resources.
“I cannot believe there aren’t Republican governors out there that are going to join with us to fight back on this,” Murray said, adding “the other way is through courts.”
All 50 states developed digital equity plans after months of focus groups, surveys, and public comment periods. NTIA Digital Equity Director Angela Thi Bennett, during an August 2024 interview with ∫⁄¡œ≥‘πœÕ¯ News, said the “intentional community engagement” by federal and state leaders to deliver broadband to unserved communities was “the greatest demonstration of participatory democracy our country has ever seen.”
Thi Bennett could not be reached for comment on this article. NTIA spokesperson Stephen Yusko said the agency “will not be able to accommodate” a request for an interview with Thi Bennett and did not respond to questions for this article.
Caroline Stratton, a research director at the Benton Institute for Broadband & Society, said the act’s funding allowed states to staff offices; identify existing high-speed internet programs, including those operating within other state agencies; and create plans to fill the gaps.
“This sent folks out looking,” Stratton said, to see whether agencies in the state were already working on health improvement plans and to ask whether the broadband work could contribute and “actively help move the needle.”
State grant applications included goals . In Mississippi, the of the state university and another agency’s health improvement plan, Stratton said.
While states were required to create programs that would help specific covered populations, some states modified the language or added subcategories to include other populations. included immigrants and “individuals experiencing homelessness.”
“In every state, there’s a loss,” said Angela Siefer, executive director of the National Digital Inclusion Alliance. The nonprofit, which was awarded to work with organizations nationwide but did not receive any funds, filed a lawsuit Oct. 7 seeking to force Trump and the administration to distribute the money.
“The digital divide is not over,” Siefer said.
The nonprofit’s grant had been planned to support digital navigators in 11 states and territories, including Waiters. Her employer, the nonprofit Community Service Programs of West Alabama, expected to receive a $1.4 million grant.
In the past two years, Waiters spent hours driving the roads of rural Alabama to reach residents. She has distributed 648 devices — laptops, tablets, and SIM cards — and helped hundreds of clients through 117 two-hour digital skills classes at libraries, senior centers, and workplace development programs in and around Tuscaloosa, Alabama.
People of “all races, of all ages, of all financial backgrounds” who did not “fit into our typical minority category” were helped through her work, Waiters said. Trump and his administration should know, she said, “what it actually looks like for the people I serve.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/race-and-health/digital-equity-act-bead-trump-cuts-health-care-access-rural/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2098549&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>