EUTAW, Ala. ŌĆö Leroy Walker arrived at the county hospital short of breath. Walker, 65 and with chronic high blood pressure, was brought in by one of rural Greene CountyŌĆÖs two working ambulances.
Nurses checked his heart activity with a portable electrocardiogram machine, took X-rays, and tucked him into Room 122 with an IV pump pushing magnesium into his arm.
ŌĆ£I feel better,ŌĆØ Walker said. Then: Beep. Beep. Beep.
The Greene County Health System, with only three doctors, has no intensive care unit or surgical services. The 20-bed hospital averages a few patients each night, many of them, like Walker, with chronic illnesses.
Greene County residents are some of the sickest in the nation, ranking near the top for rates of stroke, obesity, and high blood pressure, according to data from the federal Centers for Disease Control and Prevention.
Patients entering the hospital waiting area encounter floor tiles that are chipped and stained from years of use. A circular reception desk is abandoned, littered with flyers and advertisements.
But a less visible, more critical inequity is working against high-quality care for Walker and other patients: The hospitalŌĆÖs internet connection is a fraction of what experts say is sufficient. High-speed broadband is the new backbone of AmericaŌĆÖs health care system, which depends on electronic health records, high-tech wireless equipment, and telehealth access.

Greene is one of more than 200 counties with some of the nationŌĆÖs worst access to not only reliable internet, but also primary care providers and behavioral health specialists, according to a ║┌┴Ž│į╣Ž═° News analysis. Despite repeated federal promises to support telehealth, these places remain disconnected.
During his first term, President Donald Trump signed promising to improve ŌĆ£the financial economics of rural healthcareŌĆØ and touted ŌĆ£access to high-quality careŌĆØ through telehealth. In 2021, President Joe Biden committed billions to broadband expansion.
║┌┴Ž│į╣Ž═° News found that counties without fast, reliable internet and with shortages of health care providers are mostly rural. Nearly 60% of them have no hospital, and hospitals closed in nine of the counties in the past two decades, according to data collected by the Cecil G. Sheps Center for Health Services Research at the University of North Carolina-Chapel Hill.
Residents in these ŌĆ£dead zoneŌĆØ counties tend to live sicker and die younger than people in the rest of the United States, according to ║┌┴Ž│į╣Ž═° NewsŌĆÖ analysis. They are places where systemic poverty and historical underinvestment are commonplace, including the remote West, Appalachia, and the rural South.
ŌĆ£It will always be rural areas with low population density and high poverty that are going to get attended to last,ŌĆØ said Stephen Katsinas, director of the Education Policy Center at the University of Alabama. ŌĆ£ItŌĆÖs vital that the money we do spend be well deployed with a thoughtful plan.ŌĆØ
Now, after years of federal and state planning, BidenŌĆÖs $42 billion Broadband Equity Access and Deployment, or BEAD, program, which was approved with bipartisan support in 2021, is being held up, just as states ŌĆö such as Delaware ŌĆö were prepared to begin construction. TrumpŌĆÖs new Department of Commerce secretary, Howard Lutnick, has demanded ŌĆ£a rigorous reviewŌĆØ of the program and called for the elimination of regulations.
TrumpŌĆÖs nominee to lead the federal agency overseeing the broadband program, Arielle Roth, repeatedly said during her nomination hearing in late March that she would work to get all Americans broadband ŌĆ£expeditiously.ŌĆØ But when pressed by senators, Roth declined to provide a timeline for the broadband program or confirm that states would receive promised money.
Instead, Roth said, ŌĆ£I look forward to reviewing those allocations and ensuring the program is compliant with the law.ŌĆØ
Sen. Maria Cantwell (D-Wash.), the Senate commerce committeeŌĆÖs ranking minority member, said she wished Roth had been more committed to delivering money the program promised.
The political wrangling in Washington is unfolding hundreds of miles from Greene County, where only about half of homes have high-speed internet and 36% of the population lives below the poverty line, according to the U.S. Census Bureau.
Walker has lived his life in AlabamaŌĆÖs Black Belt and once worked as a truck driver. He said his high blood pressure emerged when he was younger, but he didnŌĆÖt take the medicine doctors prescribed. About 11 years ago, his kidneys failed. He now needs dialysis three times a week, he said.
While lying in the hospital bed, Walker talked about his dialysis session the day before, on his birthday. As he talked, the white sheet covering his arm slipped and revealed where the skin around his dialysis port had swollen to the size of a small grapefruit.
Room 122, where Walker rested, is sparse with a single hospital bed, a chair, and a TV mounted on the wall. He was connected to the IV pump, but no other tubes or wires were attached to him. The IV machineŌĆÖs beeping echoed through the hallway outside. Staffers say they must listen for the high-pitched chirps because the internet connection at the hospital is too slow to support a modern monitoring system that would display alerts on computers at the nursesŌĆÖ station.

Aaron Brooks, the hospitalŌĆÖs technology consultant, said financial challenges keep Greene County from buying monitoring equipment. The hospital on patient care in its most recent federal filing. Even if Greene could afford a system, it does not have the thousands of dollars to install a high-speed fiber-optic internet connection necessary to operate it, he said.
Lacking central monitoring, registered nurse Teresa Kendrick carries a portable pulse oximeter device, she said ŌĆö like ones sold at drugstores that surged in popularity during the covid-19 pandemic.
Doing her job means a ŌĆ£continuous spot-check,ŌĆØ Kendrick said. Another longtime nurse described her job as ŌĆ£a lot of watching and checking.ŌĆØ
Beep. Beep.
The beeping in Room 122 persisted for more than two minutes as Walker talked. He wasnŌĆÖt in pain ŌĆö he was just worried about the beeping.
About 50 paces down the hall ŌĆö past the pharmacy, an office, and another patient room ŌĆö registered nurse Jittaun Williams sat at her station behind plexiglass. She was nearly 20 minutes past the end of her 12-hour shift and handing off to the three night-shift nurses.
They discussed plans for patientsŌĆÖ care, reviewing electronic records and flipping through paper charts. The nurses said the hospitalŌĆÖs internal and external computer systems are slow. They handwrite notes on paper charts in a patientŌĆÖs room and duplicate records electronically. ŌĆ£Our system isnŌĆÖt strong enough. There are many days you kind of sit here and wait,ŌĆØ Williams said.

Broadband dead zones like Greene County persist despite decades of efforts by federal lawmakers that have created a patchwork of more than 133 funding programs across 15 agencies, .
AlabamaŌĆÖs leaders, like others around the U.S., are actively spending federal funds from the Biden-era American Rescue Plan Act, according to public records. And Greene County Hospital is on the list of places waiting for ARPA construction, according to by the Alabama Department of Economic and Community Affairs.
ŌĆ£It is taking too long, but I am patient,ŌĆØ said Alabama state Sen. Bobby Singleton, a Democrat who represents the district that includes Greene County Hospital and two others he said lack fast-enough connectivity. Speed bumps such as a need to meet federal requirements and a ŌĆ£big fightŌĆØ to get internet service providers to come into his rural district slowed the release of funds, Singleton said.
Alabama received its first portion of ARPA funds in June 2021, which Singleton said included money for building fiber-optic cables to anchor institutions like the hospital. AlabamaŌĆÖs the projects to be completed by February 2026 ŌĆö nearly five years after money initially flowed to the state.
Singleton said he now sees fiber lines being built in his district every day and knows the hospital is ŌĆ£on the mapŌĆØ to be connected. ŌĆ£This doesnŌĆÖt just happen overnight,ŌĆØ he said.
Alabama Fiber Network, a consortium of electric cooperatives, won a total of $45.7 million in ARPA funding specifically for construction to anchor institutions in Greene and surrounding counties. James Hoffman, vice president of external affairs for AFN, said the company is ahead of schedule. It plans to offer the hospital a monthly service plan that uses fiber-optic lines by yearŌĆÖs end, he said.
Greene County Health System chief executive Marcia Pugh confirmed that she had talked with multiple companies but said she wasnŌĆÖt sure the work would be complete in the time frame the companies predicted.
"You know, you want to believe," Pugh said.

Beep. Beep.
Nurse Williams had finished the night-shift handoff when she heard beeps from WalkerŌĆÖs room.
She rushed toward the sound, accidentally ducking into Room 121 before realizing her mistake.
Once in WalkerŌĆÖs room, Williams pressed buttons on the IV pump. The magnesium flowing in the tube had stopped.
ŌĆ£You had a little bit more left in the bag, so I just turned it back on,ŌĆØ Williams told Walker. She smiled gently and asked if he was warm enough. Then she hand-checked his heart rate and adjusted his sheets. At the bottom of the bed, WalkerŌĆÖs feet hung off the mattress and Williams gently moved them and made sure they were covered.
Walker beamed. At this hospital, he said, ŌĆ£they care.ŌĆØ
As rural hospitals like GreeneŌĆÖs wait for fast-enough internet, nurses like Williams are ŌĆ£heroes every single day,ŌĆØ said Aaron Miri, an executive vice president and the chief digital and information officer for Baptist Health in Jacksonville, Florida.
Miri, who served under both Democratic and Republican administrations on Department of Health and Human Services technology advisory committees, said hospitals need at least a gigabit of speed ŌĆö which is 1,000 megabits per second ŌĆö to support electronic health records, video consultations, the transfer of scans and images, and continuous remote monitoring of patientsŌĆÖ heartbeats and other vital signs.
But GreeneŌĆÖs is less than 10% of that level, recorded on the nursesŌĆÖ station computer as nearly 90 megabits per second for upload and download speeds.
ItŌĆÖs a ŌĆ£heartbreakingŌĆØ situation, Miri said, ŌĆ£but thatŌĆÖs the reality of rural America.ŌĆØ
The Beeping Stopped
Michael Gordon, one of the hospital's three doctors, arrived the next morning for his 24-hour shift. He paused in Room 122. Walker had been released overnight.
Not being able to monitor a cardiovascular patientŌĆÖs heart rhythm, well, ŌĆ£thatŌĆÖs a problem,ŌĆØ Gordon said. ŌĆ£You want to know, ŌĆśDid something really change or is that just a crazy IV machine just beeping loud and proud and nobody can hear it?ŌĆÖŌĆØ

Despite the lack of modern technology tools, staffers do what they can to take care of patients, Pugh said. ŌĆ£We show the community that we care,ŌĆØ she said.
Pugh, who started her career as a registered nurse, arrived at the hospital in 2017. It was ŌĆ£a mess,ŌĆØ she said. The hospital was dinged four years in a row, starting in 2016, with reduced Medicare payments for readmitting patients. Pugh said that at times the hospital had not made payroll. Staff morale was low.
In 2021, federal inspectors notified Pugh of an ŌĆö grounds for regulators to shut off federal payments ŌĆö because of an Emergency Medical Treatment and Labor Act complaint. Among seven deficiencies inspectors cited, the hospital failed to provide a medical screening exam or stabilizing treatment and did not arrange appropriate transfer for a 23-year-old woman who arrived at the hospital in labor, according to .
Inspectors also said the hospital failed to ensure a doctor was on duty and failed to create and maintain medical records. An ambulance took the woman to another hospital, where the baby was ŌĆ£pronounced ,ŌĆØ according to the report.
Federal inspectors required the hospital to take corrective actions and in July 2021 found the hospital to be in compliance.
In 2023, federal inspectors again cited the hospitalŌĆÖs failure to maintain records and noted it had the ŌĆ£.ŌĆØ
Inspectors that year found that medical records for four discharged patients had been lost. The ŌĆ£physical recordŌĆØ included consent forms, physician orders, and treatment plans and was , where it had been left for two months.
Pugh declined to comment on the immediate jeopardy case. She confirmed that a lack of internet connectivity and use of paper charts played a role in federal findings, though she emphasized the charts were discharge papers rather than for patients being treated.
She said she understands why federal regulators require electronic health records but ŌĆ£our hospitals just arenŌĆÖt the same.ŌĆØ Larger facilities that can ŌĆ£get the latest and greatestŌĆØ compared with ŌĆ£our facilities that just donŌĆÖt have the manpower or the financials to purchase it,ŌĆØ she said, ŌĆ£itŌĆÖs two different things.ŌĆØ

Walker, like many rural Americans, relies on Medicaid, a joint state and federal insurance program for people with low incomes and disabilities. Rural hospitals in states such as Alabama that have not expanded Medicaid coverage to a wider pool of residents fare worse financially, .
During WalkerŌĆÖs stay, because the hospital canŌĆÖt afford to modernize its systems, nurses dealt with what Pugh later called an ŌĆ£astronomicalŌĆØ number of paper forms.
Later, at Home
Walker sat on the couch in the modest brick home he shares with his sister and nephew. In a pinch, Greene County Hospital, he said, is good ŌĆ£for us around here. You see what IŌĆÖm saying?ŌĆØ
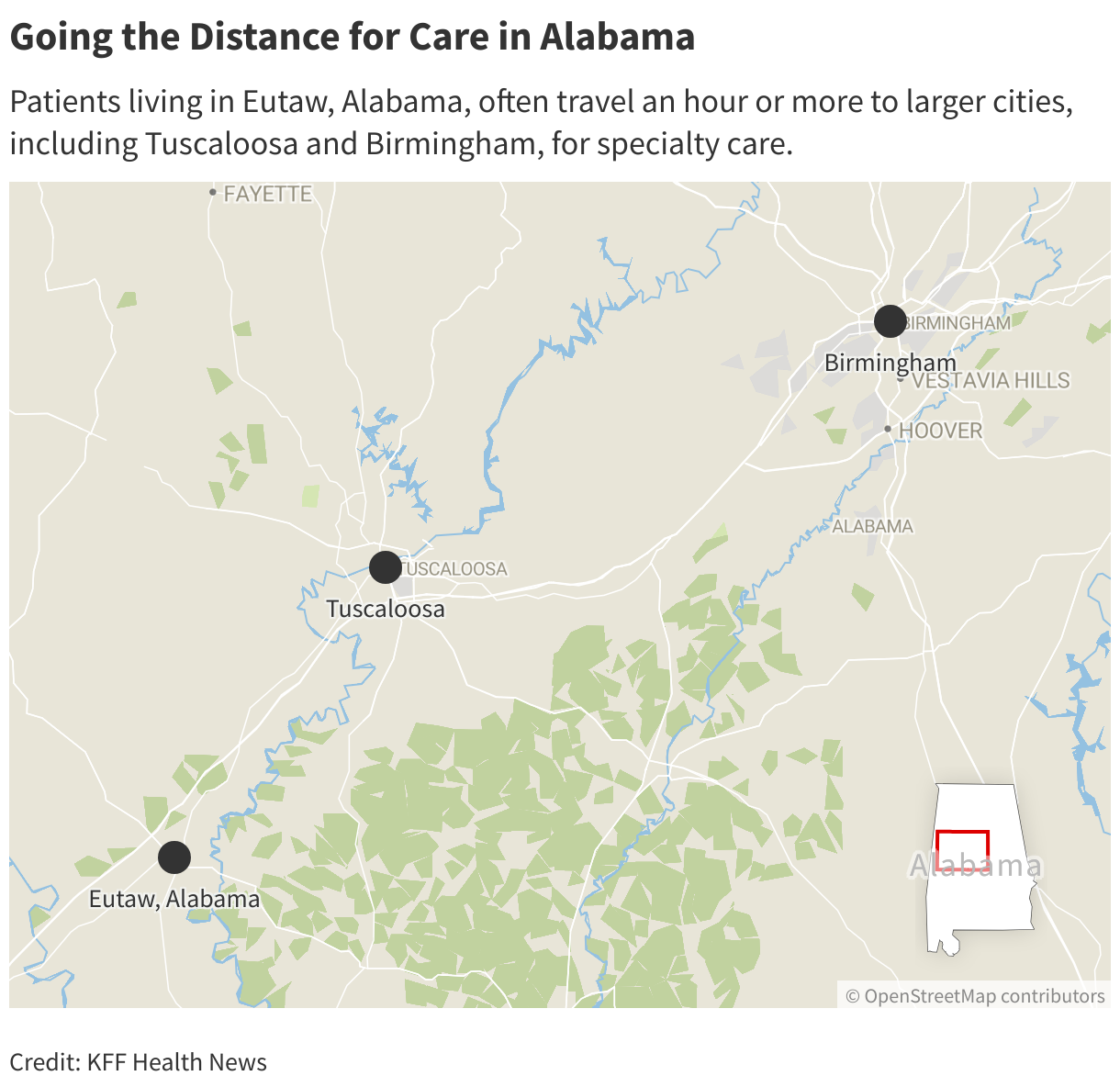
Still, Walker said, he often bypasses the county hospital and drives up the road to Tuscaloosa or Birmingham, where they have kidney specialists.
ŌĆ£We need better,ŌĆØ Walker said, speaking for the 7,600 county residents. He wondered aloud what might happen if he didnŌĆÖt make it to the city for specialty care.
Sometimes, Walker said, he feels ŌĆ£thrown away.ŌĆØ
ŌĆ£People done forgotten about me, it feels like,ŌĆØ he said. ŌĆ£They donŌĆÖt want to fool with no mess like me.ŌĆØ
Maybe Greene CountyŌĆÖs health care and internet will get better, Walker said, adding, ŌĆ£I hope so, for our sake out in a rural area.ŌĆØ
║┌┴Ž│į╣Ž═° News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFŌĆöan independent source of health policy research, polling, and journalism. Learn more about .