State governments rely on such companies to design and operate computer systems that assess whether low-income people qualify for Medicaid or food aid through the Supplemental Nutrition Assistance Program, commonly referred to as food stamps. Those state systems have a that can , a ║┌┴╧│╘╣╧═Ї News .
These benefits, provided to the poorest Americans, can mean the difference between someone obtaining medical care and having enough to eat тАФ or going without.
States are now racing to update their eligibility systems to adhere to President Donald Trump’s sweeping tax and domestic spending law. The changes will add red tape and restrictions. They are coming at a steep price тАФ both in the cost to taxpayers and coverage losses тАФ according to state documents obtained by ║┌┴╧│╘╣╧═Ї News and interviews.
The documents show government agencies will spend millions to save considerably more by removing people from health benefits. While states sign eligibility system contracts with companies and work with them to manage updates, the federal government foots most of the bill.
The law’s Medicaid policies will cause to become uninsured by 2034, according to the nonpartisan Congressional Budget Office. Roughly will lose access to monthly cash assistance for food, including those with children.
In five states alone, for state officials and reviewed by ║┌┴╧│╘╣╧═Ї News show that changes will cost at least $45.6 million combined.
“This is a pretty big payday,” said Adrianna McIntyre, an assistant professor of health policy and politics at Harvard’s T.H. Chan School of Public Health.
The law, which grants tax breaks to the nation’s wealthiest people, requires most states to tie Medicaid coverage for some adults to having a job, and imposes other restrictions that will make it harder for people with low incomes to stay enrolled. SNAP restrictions began to take effect in 2025. Major Medicaid provisions begin later this year.
Documents prepared by consulting company Deloitte estimate that a pair of computer system changes for Medicaid work requirements in Wisconsin will . Two other changes related to the state’s SNAP program will cost an additional $4.2 million, according to the documents, which for the Wisconsin Department of Health Services.
In Iowa, changes to its Medicaid system are expected to cost at least $20 million, , a consulting company that operates the state’s eligibility system.
Optum тАФ which operates the platform Vermont residents use for Medicaid and marketplace health plans under the Affordable Care Act тАФ to evaluate and incorporate new health coverage restrictions.
Initial changes in Kentucky, which has had a contract with Deloitte since 2012, . And in Illinois, will cost at least $12 million.
A Historic Mandate
For six decades after President Lyndon Johnson created the government insurance program in 1965, Congress had never mandated that Medicaid enrollees have a job, volunteer, or go to school.
That will change next year. The tax and spending law enacted by Trump and congressional Republicans requires millions of Medicaid enrollees in 42 states and the District of Columbia to prove they’re working or participating in a similar activity for 80 hours a month, unless they qualify for an exemption. The CBO projected, based on an early version of the bill, that 18.5 million adults would be subject to the new rules тАФ .
Vermont Medicaid officials expect it will cost $5 million in fiscal 2027 to implement changes in response to the federal law, said Adaline Strumolo, deputy commissioner of the Department of Vermont Health Access. About $1.8 million is for Optum to make eligibility system adjustments. Optum is a subsidiary of UnitedHealth Group.
The One Big Beautiful Bill Act will subject nearly 55,000 Vermont Medicaid recipients to work requirements тАФ about a third of the state’s enrollees.
The law forced the state “to essentially drop everything else we were doing,” Strumolo said in an interview. “This is a big, big lift.”
Optum’s contract with the state was as of October.
of adult Medicaid enrollees nationally are already working, according to KFF. Advocacy groups for Medicaid recipients say work requirements will nonetheless cause significant coverage losses. Enrollees will face added red tape to prove they’re complying. And eligibility systems already prone to error will have to account for employment, job-related activities, and any exemptions.
An estimated 5.3 million enrollees will become uninsured by 2034 due to work requirements, the .
In Wisconsin, state officials estimate could lose coverage after work requirements take effect. Not covering those people would in Medicaid spending for one year.
Wisconsin’s eligibility system for Medicaid and SNAP тАФ known as CARES тАФ in 1994, and initially was a transfer system from Florida, according to a 2016 state document.
Deloitte submitted its cost estimates for Medicaid and SNAP changes to the state in September and December. Elizabeth Goodsitt, a spokesperson for the Wisconsin Department of Health Services, declined to answer questions about whether additional changes will be needed, how much it will cost to make all eligibility system changes to comply with the new federal law, and whether the state negotiated prices with Deloitte.
Bobby Peterson, executive director of the public interest law firm ABC for Health, said Wisconsin has invested “very little” to help people navigate the Medicaid eligibility process, which soon will become more difficult.
“But they’re very willing to throw $6 million to their contractors to create the bells and whistles,” Peterson said. “That’s where I feel a sense of frustration.”
New Hurdles for Vets and Homeless People
Medicaid work requirements are only one change required by Trump’s tax law that will make it harder to obtain safety-net benefits.
Starting in October, the law prohibits several immigrant populations from accessing Medicaid and ACA coverage, including people who have been granted asylum, refugees, and certain survivors of domestic violence or human trafficking. Beginning Dec. 31, states must verify eligibility twice a year for millions of adults тАФ doubling state officials’ workload. And the law restricts SNAP benefits by requiring more adult recipients to work and by removing work exemptions for veterans, homeless people, and former foster youth.
Days after Trump signed the bill in July, Kentucky health officials raced to make changes to the state’s integrated eligibility system, which verifies eligibility for Medicaid, SNAP, and other programs. Deloitte operates the system under a five-year . , initial changes costing $1.6 million were labeled a “high priority” and approved on an “emergency” basis, with some of the changes to the nation’s largest food aid program going into effect almost immediately.
Officials with Kentucky’s Cabinet for Health and Family Services declined to answer a detailed list of questions, including how much it will cost to make all the modifications needed.
Deloitte spokesperson Karen Walsh said the company is working with states to implement new requirements but declined to answer questions about cost estimates in several states. “We are delivering the value and investments we committed to,” Walsh said.
In most states, government agencies rely on contractors to build and run the systems that determine eligibility for Medicaid. Many of those states also use such computer systems for SNAP. But the federal government тАФ that is, taxpayers тАФ to develop and implement state Medicaid eligibility systems and pays 75% of ongoing maintenance and operations expenses, according to federal regulations.
“Five, 10 years ago, I’m not sure if you would hear much mention of SNAP from a Medicaid director,” Melisa Byrd, Washington, D.C.’s Medicaid director, said in November at an annual conference of Medicaid officials. “And particularly for those with integrated eligibility systems тАФ as D.C. is тАФ┬н I’m learning more about SNAP than I ever thought.”
The federal law was the topic du jour at last year’s gathering in Maryland, held at the Gaylord National Resort and Convention Center, the largest hotel between New Jersey and Florida.
Consulting companies had taken notice. Gainwell, an eligibility contractor and one of the conference’s corporate sponsors, emblazoned its logo on hotel escalators. Companies set up booths with materials promoting how they could help states and handed out snacks and swag.
“Conduent helps agencies work smarter by simplifying operations, cutting costs and driving better outcomes through intelligent automation, analytics, and innovation in fraud prevention,” read one such handout from another contractor. “Together, we can better serve residents at every step of their health journeys.” Conduent holds Medicaid eligibility and enrollment contracts in Mississippi and New Jersey, their Medicaid agencies confirmed to ║┌┴╧│╘╣╧═Ї News.
In handouts, Deloitte touted its role in “building a new era in state health care” and as “a national leader in Medicaid program and technology transformation, building a strong track record across the federal, state, and commercial health care ecosystem.” ║┌┴╧│╘╣╧═Ї News found that Deloitte, a global consultancy that generated in revenue in fiscal 2025, dominates this slice of government business.
“With Medicaid Community Engagement (CE) requirements, states are tasked with adding a new condition of Medicaid eligibility to support state and federal objectives,” added another brochure. “Deloitte offers strategic outreach and responsive support to help states engage communities, lower barriers, and address access to coverage.”
A $20.3 Million Bill in Iowa
Before Trump signed the One Big Beautiful Bill Act, Iowa lawmakers wanted to impose their own version of work requirements. They would have applied to 183,000 people before any exemptions. The new law would necessitate a change to Iowa’s Medicaid eligibility system, according to documents prepared by Accenture, which operates Iowa’s system through a .
Adding the ability to verify work status would cost up to $7 million, . By July, the cost to implement the One Big Beautiful Bill Act’s work requirements and other Medicaid provisions . Accenture’s analysis said the federal law necessitated . Making employment a condition of Medicaid benefits could cause an estimated 32,000 Iowans to lose coverage, according to a
Cutting 32,000 people from coverage in one year, a fraction of the Iowa and the federal government spend on Medicaid in a given year.
In Cedar Rapids, most of Eastern Iowa Health Center’s patients rely on Medicaid, CEO Joe Lock said. He questioned the government’s logic of spending tens of millions of dollars on a policy to remove Iowans from Medicaid.
Most of the health center’s patients live at or below the federal poverty level тАФ currently .
“There is no benefit to this population,” Lock said.

Danielle Sample, a spokesperson for Iowa’s Department of Health and Human Services, did not answer questions about how much it will cost to implement changes to the state’s separate SNAP eligibility system.
In Illinois, the state’s work this year is largely focused on meeting major provisions of the One Big Beautiful Bill Act. The state estimates that as many as 360,000 residents could lose Medicaid, largely due to the work requirements, said Melissa Kula, a spokesperson for the Illinois Department of Healthcare and Family Services.
Kula confirmed that тАФ priced at $12 million тАФ is related to Trump’s law. The estimate also mentions other work. Kula said Deloitte is charging the state a $2 million fixed fee related to work requirements.
The Trump administration has acknowledged that the work is coming at a cost. In January, top officials for the Centers for Medicare & Medicaid Services said government contractors, including Deloitte, Accenture, and Optum, have and reduced rates through 2028 to help states incorporate system changes.
“The companies were extremely excited to do this,” , the top CMS Medicaid official. “Everyone’s really focused on getting to work.”
CMS spokesperson Catherine Howden declined to answer questions about the discounts.
Goodsitt, the Wisconsin Medicaid spokesperson, declined to answer questions about whether Deloitte has discounted its rates. Officials with Kentucky’s Cabinet for Health and Family Services did not answer a detailed list of questions, including whether Deloitte extended discounts to make these changes.
It’s unclear what discounts, if any, Deloitte and Accenture have offered to individual states. Walsh, the Deloitte spokesperson, declined to answer detailed questions about the discounts the Trump administration announced this year. Accenture did not respond to repeated requests for comment.
Strumolo, the Vermont health official, said state officials discussed the announcement with Optum “in detail.”
Optum for a specific module related to Medicaid work requirements. That product is unworkable for Vermont because it would mean “moving to a new system when we don’t have to.” When asked about whether the company offered discounts, Strumolo said “not explicitly.”
In a statement, UnitedHealth Group spokesperson Tyler Mason said Optum supports state implementation of new federal requirements “with a range of options to meet their unique cost and policy needs.”
He declined to specify whether Optum discounted Vermont’s rates and how it calculated the costs of doing its work. “Optum is helping mitigate upfront implementation expenses so states can focus on approaches that reduce duplication, accelerate implementation, and manage costs over time тАФ supporting better outcomes for individuals covered by Medicaid,” Mason said.
Strumolo said Optum’s initial changes in Vermont cover items that take effect this year and in 2027 тАФ Medicaid work requirements, checking eligibility every six months, and prohibiting certain immigrants from qualifying for health programs.
“There’s a lot more that could come,” she said.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/state-medicaid-work-requirements-eligibility-systems-deloitte-accenture-optum/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2174991&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Sam Walker, 35, has severe autism and other disabilities. He is deaf and cannot speak. Sometimes when he’s frustrated, he hits himself or others.
Medicaid provides about $8,500 a month for health workers who visit his apartment in the basement of his parents’ home. The staffers help him with everyday tasks, including dressing, bathing, and eating. They also take Walker on outings, such as dining at restaurants, volunteering at Goodwill, and exercising at a recreation center or on park trails. They stick to a strict routine, which soothes him.
His parents say that without the in-home services, their son would need to move to a specialized residential facility in another state. Sending him away would break their hearts and cost taxpayers much more money. They strive to keep him home because they know change makes him anxious.
“The last thing I want is to put him into some kind of care facility, where he’ll just get kicked out,” said his mother, Leisa. The Iowa Department of Health and Human Services did not respond to ║┌┴╧│╘╣╧═Ї News’ questions about the Walkers’ case.
Federal Cuts Raise Pressure
Patient advocates say state administrators in Iowa appear to be reining in Medicaid spending by cutting what are known as home and community-based services for people with disabilities, and they’ve heard of multiple families facing battles like the Walkers’.
Disability rights advocates expect the pressure to intensify as states respond to reductions in federal Medicaid funding called for under the Trump administration’s signature tax and spending law, which passed last year.
June Klein-Bacon, CEO of the Brain Injury Association of Iowa, said the cuts and proposed rule changes appear to be part of a quiet attempt to save money in response to the state’s budget deficit and expected reductions in federal Medicaid funding.
Medicaid, jointly financed by the federal and state governments, covers people with low incomes or disabilities. Walker is one of served by “Medicaid waiver” programs, which pay for care that allows people with disabilities or who are at least 65 to live at home.
Unlike most parts of Medicaid, waiver programs are optional for states. Idaho’s governor noted that fact in January, when he suggested legislators consider cutting them. Disability rights groups fear other states will do the same. Leaders in , , and have considered such cuts this year.
Leisa Walker has heard Trump administration officials claim the national Medicaid cuts are intended to reduce waste, fraud, and abuse. That’s not how it will play out, she said. “These are real people, real families, and this causes real suffering when you do this to people,” she said. “It’s a very scary time.”
a private insurance company that manages Sam Walker’s Medicaid benefits, intends to cut his in-home care coverage by about $3,200 per month, his mother said. Company leaders told a judge they are following state officials’ direction, but they did not dispute Leisa Walker’s math.
Walker has been on the waiver program for three decades. It covers assistance from workers known as “direct service providers” тАФ one of whom has been with him for 25 years. His parents receive no pay for the hours they spend caring for him when the aides aren’t working.
On a February morning, Leisa and Kent Walker drove an hour and a half to Des Moines for an appeal hearing. An administrative law judge sat behind a wooden desk in a conference room as the Walkers and their lawyer faced off against three representatives from Iowa Total Care, a subsidiary of the national insurer Centene Corp.
Leisa testified that her son is 6 feet tall and weighs 230 pounds. Although he knows some sign language, he has trouble communicating, she said. When he becomes frustrated or his routine is interrupted, he sometimes wails and hits himself or other people. “It’s devastating to watch,” she testified.
He’s not a bad person, she said. “He doesn’t understand how strong he is.”
She said her family would try to keep his main caregiver employed under the planned Medicaid reduction but would have to drop others who cover nights and weekends. She said no residential facility near their southern Iowa home could address her son’s complicated needs. She said a case manager told her that a Florida facility might be the closest one that could safely handle him.
Leisa Walker testified that the state’s Medicaid program would pay about $22,000 per month to put him in an institution, more than double what the program spends on his home care.
Sam Walker’s longtime psychiatrist, Christopher Okiishi, testified that Walker’s family and their support staff spent years developing a “fragile” but stable existence for him.
Lori Palm, a senior manager for Iowa Total Care, testified that Sam Walker gets about 16 hours of daily assistance financed by Medicaid. Palm said much of that time amounts to “supervision.” She said state officials recently advised her company that the program should pay mainly for “skill-building” time, not supervision.
The Walkers showed the judge a 2018 document in which a previous Iowa Medicaid director stipulated that supervision of people with disabilities is an allowable service for workers paid under the program.

Judge Rachel Morgan asked the Iowa Total Care representatives if the recent policy change was made in writing by the state Department of Health and Human Services. They said it was not and that they couldn’t specify who at the department had given them the new guidance.
The judge suggested during the hearing that for someone like Sam Walker, learning to regulate emotions could be an important form of skill-building. Three days later, the judge ruled in the Walkers’ favor, writing that the insurer’s attempt to cut care hours was improper. The insurer appealed the decision to the director of the Iowa Department of Health Human Services, who could overrule it. The dispute could eventually wind up in district court.
Iowa Total Care and the state Department of Health and Human Services did not respond to questions about the reports that many other Iowans with disabilities face reductions in care hours covered by Medicaid. Department spokesperson Danielle Sample said in an email that the agency supports home and community-based services, which, she noted, help “states save money by avoiding expensive long-term facility care.”
Spokespeople for the federal Department of Health and Human Services, which oversees Medicaid nationally, did not respond to a request for comment on the issue.
Medicaid waiver programs started in the 1980s, after President Ronald Reagan heard about an Iowa girl with a disability who was forced to live in a hospital for months because Medicaid wouldn’t pay for home care. The Republican president thought it was outrageous that the girl, had to live that way, even though home care would have been cheaper.
Members of Congress approved allowing states to use their Medicaid programs to pay for in-home care. But they made the change optional, to offer states flexibility and encourage innovation.
Designating such spending as optional “waiver programs” also made the change more politically palatable, said Kim Musheno, senior director of Medicaid policy for , which represents people with intellectual and developmental disabilities.
Prospects were much different for babies born with serious disabilities before the change, Musheno said. “Doctors instructed families to forget they existed, and to put them in an institution.”
Waivers Have Been Cut Before
All states have Medicaid waiver programs, but benefits and the number of people covered vary significantly. Applicants often wait months or years to get into the programs because of limited funding. More than 600,000 Americans were on waiting lists or “interest lists” for waiver services in 2025, , a health information nonprofit that includes ║┌┴╧│╘╣╧═Ї News.
Disability rights advocates and care providers have fought for decades to maintain funding for the programs, but a national leader said the threat feels especially severe now.
“When Medicaid is cut, people with disabilities are at the center of the impact,” said Barbara Merrill, CEO of the American Network of Community Outcomes and Resources, which represents agencies that care for people with intellectual disabilities or autism.
That’s what happened after Congress reduced Medicaid funding in 2011, according to a recent paper published by .
States could again rein in waiver programs by limiting enrollment, reducing covered services, or cutting pay for caregivers, who already are in short supply.
However, states that try to cut the in-home care programs could face legal challenges, Musheno said. The U.S. Supreme Court declared in 1999 that people with disabilities have a right to live outside of institutions if possible. The decision, in the case of , has been cited in lawsuits against states that fail to provide care options apart from nursing homes and similar facilities.
Several Iowans who belong to a Facebook group for Medicaid participants have posted in recent weeks that their families were notified of impending cuts in coverage of home care services for people with disabilities.
Sam Walker’s main caregiver, Andy Koettel, has worked with him since Walker was in fourth grade. Koettel, who works full-time, knows how to keep Walker calm in most situations and soothe him during a blowup. Their relationship took years to build, and it is a key reason Walker can continue to live at home with his parents, Koettel said.
“If I was not there, it would be incredibly difficult for all of them,” he said.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/medicaid-cuts-disabilities-home-community-based-services-iowa/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2162736&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
Last year was a tough one for farmers. Amid such as corn and soybeans, for supplies like , as well as the Trump tariffs and the , many farms weren’t profitable last year.
And now, the enhanced Affordable Care Act subsidies that many Americans, including farmers, relied on to purchase health insurance are gone, having .
James Davis, 55, who grows cotton, soybeans, and corn in northern Louisiana, said he didn’t know how he and his wife would afford coverage. Their share of their insurance premium quadrupled for 2026, jumping to about $2,700 a month.
“You can’t afford it,” Davis said. “Bottom line. There’s nothing to discuss. You can’t afford it without the subsidies.”
More than a quarter of the agricultural workforce purchases health insurance through the individual marketplace, according to , a health information nonprofit that includes ║┌┴╧│╘╣╧═Ї News.
That 27% rate is much higher than the overall population’s тАФ only .
Farmers are used to facing challenges such as unpredictable weather and fluctuating commodity prices. But the loss of the enhanced subsidies, coupled with challenging economic conditions, will make coverage unaffordable for many.
Without major intervention from Washington, farmers say they’ll have to choose between being uninsured or leaving the farm work behind for a job that offers health insurance.
A Gamble for Farmers
Farming is dangerous work. Agricultural workers spend much of their time outside and exposed to the elements. Many of their duties can lead to injury or illness. They drive and operate heavy machinery, work with toxic chemicals, and handle large animals.
The rate of work-related deaths for farmers is .

The financial toll of non-fatal farm injuries is also significant. from the University of Nebraska Medical Center found that the average cost of a farming injury was $10,878 in medical care and $4,735 in lost work.
It’s essential that farmers can purchase comprehensive insurance, said , a rural sociologist and associate professor of agricultural health and safety at Pennsylvania State University, where she studies the social and economic needs of farm households.
In a , Becot found that more than 20% of U.S. farm households had medical debt exceeding $1,000 and that more than half were not confident they could cover the costs of a major illness or injury.
“That shows you the level of vulnerability and concerns that farmers are facing,” she said.
Mental health is also a concern. as likely to die by suicide compared with the general population. Mental health hotlines that serve rural communities have an in calls.
These concerns around farmers’ , coupled with a , conjures memories of the farm crisis of the 1980s, said , a vice president at the industry group . During that decade, there was a raft of foreclosures, and .
“We’re really afraid of what’s going to happen,” Klein said.
Farmers can be reluctant to acknowledge that they rely on government-subsidized insurance, said Meghan Palmer, 43, who runs a dairy farm in northeastern Iowa with her husband, John, 45.
“We’re not handout-takers,” Palmer said.
More than 40% of dairy farmers lack health insurance тАФ among all agricultural sectors.
But going uninsured is not an option for the Palmers.
During their first year of marriage, the couple recalled, they were uninsured and had to pay out-of-pocket for two unexpected health crises: Palmer had an appendectomy, and her husband needed stitches after getting kicked in the face by one of his cows.
“It was stupid of us,” Palmer said of the decision to forgo coverage.
But this year, the combined out-of-pocket monthly cost of their plans is increasing by more than 90%, to $368.18. Their total 2026 deductible is $7,200.

Palmer is a registered nurse who picks up shifts on an as-needed basis, allowing her the flexibility to prioritize her work on the farm. She’s now searching for a job with health benefits. But she worries a job that doesn’t allow her to keep up with the farm work will create a greater burden for her husband.
“John is working exhausted most of the time,” she said. “That’s when mistakes get made and you end up in the ER.”
Political Consequences
Even after the enhanced subsidies expired at the end of 2025, the Palmers estimate their income will still be low enough that they’ll qualify for some tax credits to purchase coverage.
However, under the GOP’s One Big Beautiful Bill Act, , so if the Palmers have a surprisingly profitable 2026, they’ll be forced to pay some, or even all, of that subsidy back at tax time.
A farmer’s income can vary drastically year to year, Becot said, partly because commodity prices can fluctuate rapidly.
Some farmers might deliberately choose to not expand their businesses, because too much profit might mean they lose access to health care subsidies.

Farmers who are insured through Medicaid have similar concerns, Becot said. But prioritizing health care affordability by suppressing operational growth can have long-term consequences for a farm’s success.
Palmer, in Iowa, and Davis, in Louisiana, are both upset that lawmakers aren’t more sensitive to the economic demands of farming and how those have coincided with rising health costs.
President Donald Trump recently pledged $12 billion in one-time to row crop farmers, but that’s not going to stop health care costs from ballooning.
Republicans are aware that health care affordability is a problem and have put forth proposals, said , a political scientist at the University of Northern Iowa. But most don’t support extending the enhanced ACA subsidies, because they don’t see them as a good solution to the problem of rising health care costs.
This article is from a partnership that includes the , , and ║┌┴╧│╘╣╧═Ї News.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/farmers-health-insurance-costs-aca-obamacare-subsidies/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2145414&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Jonna Quinn was initially thrilled when she got her first job after her medical residency, working as an OB-GYN in Mason City, Iowa. It was less than two hours down the road from West Bend, where she grew up on a farm.
But the hospital started restricting certain birth control options and fertility treatments based on with the Roman Catholic Church, she said. At the same time, her unit was as other obstetricians left and retired.
At one point, Quinn said, she was seeing up to 50 patients a day.
“That is twice what a normal OB-GYN will see in a day,” she said. “I knew I was going to miss something, because there’s no way somebody can function at that level.”
In spring 2024, Quinn decided to leave тАФ not just Mason City, but Iowa entirely.
At the time, the state Supreme Court banning abortion as early as six weeks of pregnancy, with very few exceptions.
It was the last straw for Quinn, who in Minnesota and moved her family there. Minnesota has for abortion.
“I could either stay and ruin myself and my career and my mental health and my relationship with my children, or I could go and continue to practice OB, which had always been my dream,” she said.
A few months after Quinn moved away, Iowa’s abortion ban went into effect on July 29, 2024.
A Severe Shortage
After the Supreme Court overturned Roe v. Wade in 2022, multiple states, including Iowa, .
Coupled with existing OB-GYN shortages, the laws have put doctors under increasing strain and surveillance, for miscarriage, ectopic pregnancy, premature membrane rupture, and other pregnancy problems. Some physicians fear these laws could drive these much-needed doctors from certain states and dissuade other OB-GYNs from moving in and establishing a practice.
Iowa has the among states, according to a KFF analysis of 2021-22 from the .
Studies show that insufficient maternity care is linked to and increased infant and .

Stress on Those Who Remain
Rural hospitals in Iowa have been struggling to find more OB-GYNs.
The , a 49-bed hospital in a rural college town, has been trying to recruit an OB-GYN, and a family practice doctor with obstetrical training, for more than a year.
The hospital has seen a dramatic jump in deliveries after a neighboring hospital in 2024. The additional deliveries have been stressful for its two existing obstetrical-unit doctors, said , an executive with the center.
Back when patient volume was lower, it was easier for doctors to be on call over the weekend, he explained.
“You just kind of had to hang out at home, be by the phone,” he said. But recently, the on-call doctors have been delivering “five babies on Saturday, six babies on Sunday,” Cavazos said. “It becomes more stressful.”
An enacted last May increased Medicaid reimbursement rates for maternity care, so OB-GYNs could be paid more for caring for pregnant patients. The new law also directs federal funding toward a project to set up additional medical residency slots, including OB-GYN residency slots, in the state. Medical residents tend to stay and in states where they complete their residency.
These things could help, said , chair of the Iowa section of the American College of Obstetricians and Gynecologists. But the state’s abortion restrictions are still a red flag for some OB-GYNs when deciding whether to practice in Iowa, she said.
“They understandably do not want to put their licenses and their livelihood at risk when it comes to taking care of patients,” Solheim said.
At her previous job in Quad Cities, Solheim performed an abortion on a patient who had life-threatening complications, she said. It spurred many phone calls from hospital administrators.
They peppered her with questions about her decision, Solheim recalled. “Did I have enough evidence? Was her blood count low enough that her life was in danger? Should we have waited until her blood pressure got lower?”
Solheim recently stopped delivering babies to focus on gynecology and outpatient care, saying she had become exhausted working in Iowa hospital units that didn’t have enough obstetricians.
Recent data on residency applications shows that state abortion bans may be influencing the next generation of doctors.
Fewer medical students to OB-GYN residency programs in states that restrict or ban abortion, according to from the Association of American Medical Colleges.
For E., a fourth-year medical student in Iowa, the law weighs heavily on her decision of where to apply for OB-GYN residency, and, ultimately, practice. She worries about how Iowa’s law will affect her ability to practice evidence-based care.
E. is her middle initial тАФ ║┌┴╧│╘╣╧═Ї News and NPR are identifying her that way to prevent her comments from jeopardizing future job opportunities.
“I’m seriously questioning whether Iowa is a state that I want to practice in, in the long term, and it breaks my heart because I know that there is such a need,” she said.

A Mixed Picture
It’s still unclear whether abortion bans are driving doctors out of state.
One in Idaho found that two years after the state enacted its highly restrictive abortion law, 35% of the state’s 268 OB-GYNs had stopped practicing obstetrics.
But , analyzing federal data two years after the 2022 Dobbs decision, failed to find significant departures of OB-GYNs from states with abortion bans.
“We were surprised, and we cut the data in every possible way that we could,” said , an assistant professor at the University of California-Berkeley’s School of Public Health, and the study’s lead author.
While numbers don’t show a systemic exit, it’s possible some OB-GYNs are adapting how they practice so they can stay with their patients, she said.
“We’ve heard anecdotally, and through qualitative research, that they’re really highly committed to those patients,” Staiger said.
She said how OB-GYNs feel about .
“What we can’t observe is anything about the quality of care that the providers are able to provide, about provider satisfaction with job, about provider safety,” Staiger said.
This article is from a partnership with and .
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/courts/iowa-obgyn-shortage-abortion-ban-reproductive-care/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2125190&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Most of the lawyers work either for the Department of Justice or for disability rights agencies that Congress set up in every state decades ago. Many of the Justice Department lawyers quit in 2025 after being reassigned to other duties, their supporters say. And Trump budget officials proposed deep cuts to federal grants supporting the state-based legal groups.
People with disabilities have the right to live in their communities if possible. Federal laws and court decisions say they may attend school, work jobs, and go to restaurants, movie theaters, and other public places. If they can find lawyers, they can file legal challenges when those rights are denied.
The federally funded attorneys quietly work to ensure the U.S. lives up to promises made by the Americans with Disabilities Act and other laws, said Alison Barkoff, a health law professor at George Washington University.
“I think many families of people with disabilities, or even many people with disabilities themselves, don’t hear about it until they Google, тАШWhere can I get help?’” said Barkoff, who helped lead such efforts under Presidents Joe Biden and Barack Obama.
The attorneys’ goals include ensuring that people with disabilities have the services they need to live in their own homes, instead of having to move into nursing homes or other types of institutions, Barkoff said.
“These are people who, if these supports are ripped away, are going to have to leave their communities and their families, at a higher cost for taxpayers,” she said.
The state-based disability rights groups are known as “protection and advocacy” organizations. Most of them are nonprofit groups.
Congress approved the federally financed system in the 1970s after TV journalist Geraldo Rivera in a New York institution for people with mental and intellectual disabilities, revelations that ignited a national outcry.
President Donald Trump proposed cutting the system’s federal funding from $148 million to $69 million for fiscal year 2026, according to the National Disability Rights Network, which represents the state-based groups.
Appropriations committees in the U.S. House and Senate have recommended Congress maintain funding at the previous level. But advocates for the agencies worry that even if Congress maintains current support, the administration will try again to slash their support in future years. “It definitely would put people in our communities in harm’s way,” said Marlene Sallo, the national network’s executive director.
White House officials declined to comment on why the Trump administration proposed the deep cuts.
Isaac Schreier’s family can attest to the value of the state-based legal groups.
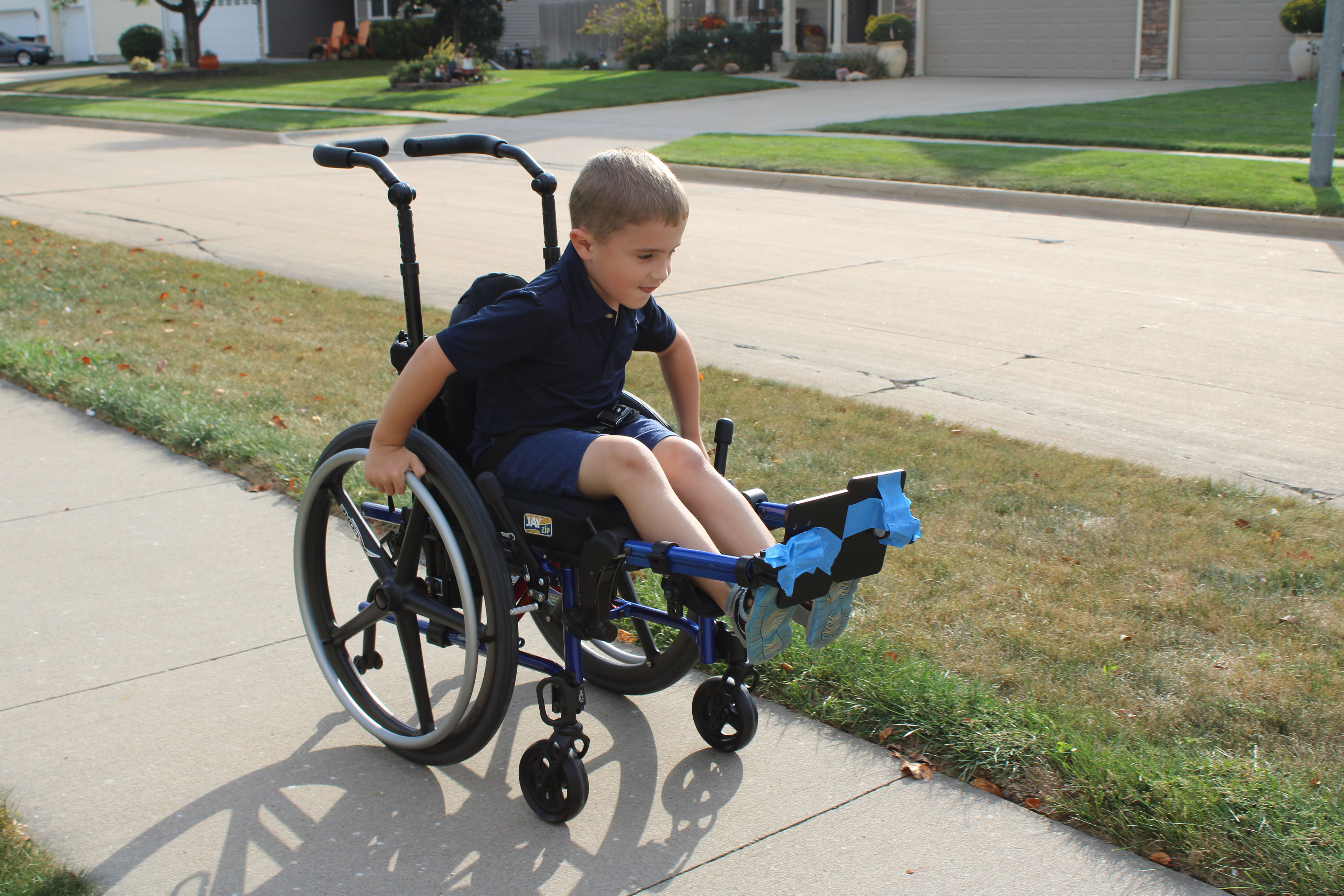
Isaac, 7, lives in Ankeny, Iowa. He has a rare condition called osteogenesis imperfecta, also known as brittle bone disease. The condition has caused about 60 bone fractures, including in his limbs, spine, and skull. It can cause intense pain and leave him unable to walk.
At times, Isaac’s disability is practically invisible, said his father, Jake Schreier. Unless he has recently suffered a broken leg bone, he walks well. “But he tires much more quickly than you or I would.”
Isaac’s doctor said he needed a special wheelchair that could be adjusted to put him in different positions depending on which bones were broken. But the private insurer that manages his Medicaid coverage declined to pay for the $3,500 wheelchair. “They required proof that it was a permanent and long-standing condition,” Jake Schreier said. “We were very frustrated.”
Schreier appealed the denial but lost. A nurse at a specialty clinic then recommended he reach out to Disability Rights Iowa, a federally funded protection and advocacy group that had helped other families in similar straits.
The group linked Schreier with two of its attorneys, who filed a new appeal. The lawyers wrote a detailed letter explaining why Isaac was legally entitled to the new wheelchair, and they cited specific Iowa codes and court precedents.
The insurer wound up paying for Isaac’s special wheelchair.
The chair allows Isaac to participate in school and community activities even when he has broken bones. “It’s absolutely night and day. I can’t imagine a world where we didn’t have it,” his father said.
Isaac may again need people like the disability rights lawyers to fight for him, so he won’t be shunted away from society, Schreier said. “We’re really trying to keep as many doors open as possible for him.”
The threat to the state-based groups’ funding comes as the more people with mental illness or addictions into institutions.
David Hutt, deputy executive director for legal services at the National Disability Rights Network, noted that the groups have legal authority to go into facilities where people with disabilities live, to check conditions and treatment. Those facilities include state institutions and privately owned nursing homes.
More Americans could wind up living in such settings if Trump succeeds in his quest to institutionalize people with mental illness who are living on the streets, Hutt said.
At the same time, in federal contributions to Medicaid, the public health coverage program for people with low incomes or disabilities. In response, they may be tempted to reduce Medicaid coverage of , many of which are considered optional under federal law, Hutt said. If that happens, “you’re going to get increased institutionalization, which actually costs more,” he said.
Disability rights organizations often have stepped in when states failed to provide care and services that people with disabilities are entitled to. So have lawyers from the Justice Department’s civil rights division.
For example, Disability Rights Iowa filed a lawsuit in 2023 alleging the state failed to provide proper mental health resources for children on the Medicaid program. The state that advocates said could bring “radical change” to the system.
In 2021, the Justice Department that their lack of support for community services meant too many people with intellectual disabilities had to live in facilities. State officials vowed to do better.
Since Trump returned to office, many of the Justice Department’s most experienced disability rights lawyers have taken buyouts or been reassigned to other areas, said Jennifer Mathis, a former top administrator at the Justice Department under Biden. “There’s really skeleton staffing at this point,” said Mathis, now deputy director of , which advocates for rights of people with mental disabilities.
The overall civil rights division is down to about 300 people, fewer than half the number it had under Biden, Mathis said.
The civil rights division’s new director, Harmeet Dhillon, in April that more than 100 attorneys had left the division, but that they didn’t support Trump’s priorities. “The job here is to enforce the federal civil rights laws, not woke ideology,” she told Beck.
In a statement to ║┌┴╧│╘╣╧═Ї News, Dhillon said the division continues to be “a vocal and active advocate for Americans with disabilities.”
Dhillon noted the department recently over complaints that the ride-hailing service was turning away customers with service dogs or wheelchairs; has secured agreements with and to improve treatment of imprisoned people with disabilities; and over allegations of failing to provide proper accommodations for people with disabilities.
The department declined to comment on the record about the number of attorneys it has working on disability rights issues. However, “civil rights warriors,” including lawyers, to join the civil rights division.
Jake Schreier, the Iowa parent, hopes the issue will be worked out nationally. “I really can’t believe this is anything that would be partisan,” he said.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/courts/disability-lawyers-doj-civil-rights-division-protection-advocacy-organizations-iowa/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2127593&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The Trump administration, which has promised “radical transparency,” that it plans to publish the “project summary” for states that win awards. Following the lead of federal regulators, many states are withholding their complete applications, and some have refused to release any details.
“Let’s be clear,” said Alan Morgan, chief executive of the National Rural Health Association. “The hospital CEOs, the clinic administrators, the community leaders: They’re going to want to know what their states are doing.” The NRHA’s members include struggling rural hospitals and clinics, which would benefit from the Trump administration’s Rural Health Transformation Program.
Morgan said his members are interested in what states propose, which of their ideas are approved or rejected, and their budget narratives, which detail how the money could be spent.
Improving rural health care is an “insanely complicated and difficult task,” Morgan said.
The five-year Rural Health Transformation Program was approved by Congress in a law — the One Big Beautiful Bill Act — that also drastically cuts Medicaid spending, on which rural providers heavily depend. It’s being watched closely because it’s a much-needed influx of funds — with a caveat from the Trump administration that the money be spent on transformational ideas, not just to prop up ailing rural hospitals.
The law says half of the $50 billion will be divided equally among all states with an approved application. The rest will be distributed through a points-based system. Of , $12.5 billion will be allotted based on each state’s rurality. The remaining $12.5 billion will go to states that on initiatives and policies that, in part, mirror the Trump administration’s “” objectives.
Health and Human Services Secretary Robert F. Kennedy Jr. has repeatedly promised to open the government to the American people. His agency has devoted to “radical transparency.”
“We’re working to make this the most transparent HHS in its 70-year history,” in written testimony to lawmakers in September.
Lawrence Gostin, a professor of public health law at Georgetown University, said HHS is “acting in a way that utterly lacks transparency” and that the public has the right to demand “greater openness and clarity.” Without transparency, the public cannot hold HHS accountable, he said.
Centers for Medicare & Medicaid Services spokesperson Catherine Howden said the agency will follow the federal regulations when releasing information about the rural health program.
Grant applications are “not released to the public during the merit review process,” Howden said, adding, “The purpose of this policy is to protect the integrity of evaluations, applicant confidentiality, and the competitive nature of the process.”
Democrats and many health care advocates are concerned politics will affect how much money states get.
“I am very concerned about retaliation,” said Rep. Nikki Budzinski (D-Ill.). Because Democrats control her state’s politics, “our application might not be as seriously considered as other states that have Republican leadership,” she added.
Illinois’ Democratic members of the U.S. House to CMS Administrator Mehmet Oz in November asking for “full and fair consideration” of their state application. Illinois officials have not yet released their state’s proposal to ║┌┴╧│╘╣╧═Ї News, which has a pending public records request.
Heather Howard, a professor of the practice at Princeton University, said she is “pleasantly surprised at how transparent the states have been.”
Howard directs the university’s State Health and Value Strategies program, which the rural health fund, and praised most states for publicly posting their project summaries.
“To me, it speaks to the intense interest in this program,” Howard said. Her team, reviewing about two dozen state summaries, found themes including expansion of home-based and mobile services, increased use of technology, and workforce development initiatives like scholarships, signing bonuses, and child care assistance for high-demand positions.
“I think it’s exciting,” Howard said. “What’s great here is the experimentation we’re going to learn from.”
Telerobotics appeared in Georgia’s and Alabama’s applications, she said, including a proposal to use robotic equipment for remote ultrasounds.
Another theme that “warms my heart,” Howard said, was the effort among states to create advisory groups or committees, including in Idaho, where work groups are expected to focus on technology, workforce development, tribal collaboration, and behavioral health.
All 50 states submitted applications to federal regulators by the Nov. 5 deadline and awards will be announced by the end of the year, according to CMS.
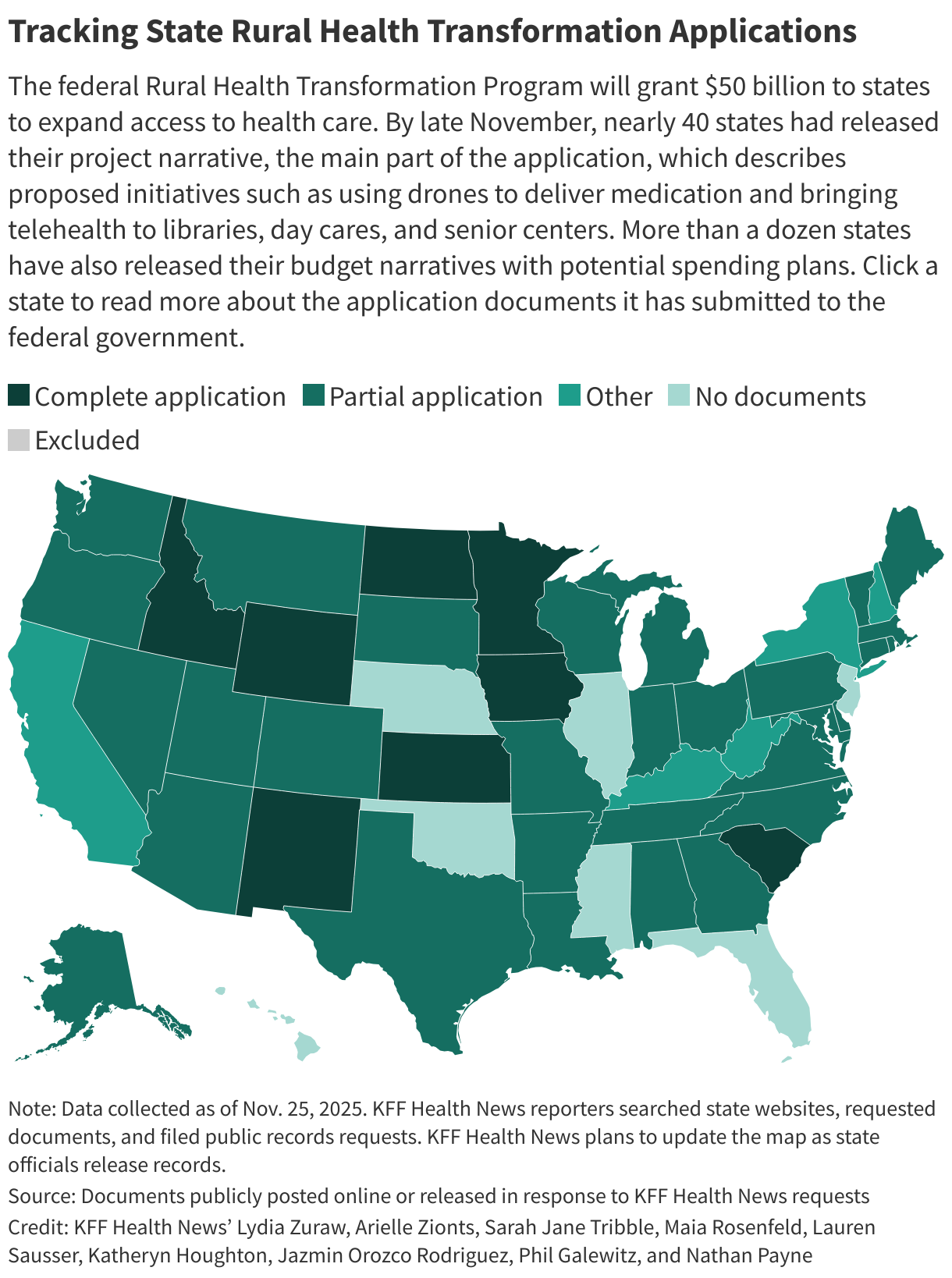
As of late November, nearly 40 states had released their project narrative, the main part of the application, which describes proposed initiatives, according to ║┌┴╧│╘╣╧═Ї News tracking. More than a dozen states have also released their budget narratives.
Also as of late November, only a handful of states — Idaho, Iowa, Kansas, Minnesota, New Mexico, North Dakota, South Carolina, and Wyoming — had released all parts of the application.
║┌┴╧│╘╣╧═Ї News filed public records requests for states’ complete applications. Some states have refused to release any of their application materials.
Nebraska, for example, rejected a public records request, saying its application materials are “proprietary or commercial information” that “would give advantage to business competitors.”
Kentucky shared its application summary but said the remainder of the application is a “preliminary draft” not subject to release under state laws.
Erika Engle, a spokesperson for Hawaii Gov. Josh Green, said the governor “is committed to transparency” but declined to share any of the state’s proposal.
Hawaii and other states are still processing formal public records requests.
The rural health program is part of the July law projected to reduce federal Medicaid spending in rural areas by 10 years.
Those cuts are expected to affect rural health facilities’ bottom lines, threatening their ability to stay open. A recent Commonwealth Fund report found that rural areas continue to to primary care. But the guidelines for the rural health program say states can use only 15% of their new funding to pay providers for patient care.
Between the Medicaid cuts and funding boost from the new program, “there’s real opportunity for national policy to impact rural, both in the negative and the positive potentially,” said Celli Horstman, a senior research associate at the New York-based policy think tank who co-authored the report.
Among the publicly available rural health transformation proposals, Democratic-leaning states show support, or are willing to adopt, some of the administration’s goals but will lose out on points from eschewing others.
For example, New Mexico said it would introduce legislation requiring students to take the Presidential Fitness Test and physicians to complete continuing education courses on nutrition. But it won’t prevent people from using their Supplemental Nutrition Assistance Program benefits to buy “non-nutritious” foods such as soda and candy.
Many states want to invest in technology, including telehealth, cybersecurity, and remote patient monitoring equipment. Other themes include increasing access to healthy food, improving emergency services, preventing and managing chronic illnesses, and enlisting community health workers and paramedics for home visits.
Specific proposals include:
- Arkansas wants to spend $5 million through its “FAITH” program — Faith-based Access, Interventions, Transportation, & Health — to enlist rural religious institutions to host education and preventive screening events. Congregations could also install walking circuits and fitness equipment.
- Alaska, which historically relied on dogsled teams to bring medication to remote areas, is looking to test the use of “unmanned aerial systems” to speed up pharmacy deliveries to such communities.
- Tennessee wants to increase access to healthy activities by spending money on parks, trails, and farmers markets.
- Maryland wants to start mobile markets and install refrigerators and freezers to improve access to fresh, healthy food that often spoils in rural areas with few grocery stores.
State Sen. Stephen Meredith, a Republican who represents part of western Kentucky, said he still expects rural hospitals to close despite his state’s rural health transformation program.
“I think we’re treating symptoms without curing the disease,” he said after listening to a presentation on Kentucky’s proposal at .
Morgan, whose organization represents rural hospitals likely to close, said the state’s ideas may sound good.
“You can craft a narrative that sounds wonderful,” he said. “But then translating the aspirational goals to a functioning program? That’s difficult.”
║┌┴╧│╘╣╧═Ї News staffers Phil Galewitz, Katheryn Houghton, Tony Leys, Jazmin Orozco Rodriguez, Maia Rosenfeld, Bram Sable-Smith, and Lauren Sausser contributed to this report.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/rural-health-transformation-program-cms-state-applications-transparency/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2123985&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The investigators allege that some insurers effectively set up “ghost networks” of psychologists, psychiatrists, and other mental health professionals who purportedly have agreed to treat patients covered by the publicly financed Medicare and Medicaid plans. In fact, many of those professionals do not have contracts with the plans, do not work at the locations listed, or are retired, the investigators said.
The Office of Inspector General for the Department of Health and Human Services, which oversees the giant Medicare and Medicaid health programs, released its findings
The report focuses on insurers the government pays to cover people in Medicare Advantage plans and in privately managed Medicaid plans. About 30% of all Americans are covered by such insurance, the report says. The government pays the insurers hundreds of billions of dollars annually.
The companies are paid set rates per person they cover and are allowed to keep whatever money they don’t spend on patient care. The insurers are required to have adequate numbers of health care professionals under contract to serve patients in each region they cover.
But the new report found that 55% of mental health professionals listed as in-network by Medicare Advantage plans were not providing such care to any of the plans’ members. The figure was 28% for Medicaid managed care plans.
Some mental health professionals told investigators they shouldn’t have been listed as in-network care providers for the insurers’ members, because they no longer worked at the locations listed or because they didn’t participate in the Medicare Advantage or Medicaid managed care plans. Others said they were working as administrators and no longer providing patient care.
In one case, the report says, a private Medicaid plan listed a mental health professional as providing care in 19 practice locations. But when the investigators checked, a receptionist at one of the clinics said the person had retired a few years ago.
Jeanine Simpkins of Mesa, Arizona, learned how skimpy the networks can be when a 40-year-old family member was in crisis this fall. Simpkins struggled to find a drug rehabilitation program that would accept the Medicare Advantage insurance the relative is on because of a disability.
Simpkins said she contacted about 20 rehab programs, none of which would take the Medicare insurance plan. “You feel kind of dropped,” she said. “I was pretty surprised, because I thought we had something good in place for her.”
Simpkins’ relative eventually enrolled in part-time hospital care instead of an inpatient rehabilitation center.
It can be challenging for patients to find timely, nearby care, for all kinds of health problems, from colds to cancer.
But Jodi Nudelman, a regional inspector general who helped write the federal report, said in an interview that the stakes can be especially high for patients seeking mental health care.
“They can be particularly vulnerable,” she said. It can be daunting for people to acknowledge they need such care, and any roadblock can discourage them from trying to find help, she said.
She added that taxpayers aren’t getting their money’s worth if insurers fail to meet obligations to provide sufficient care options for Medicare and Medicaid participants in the plans.
The federal report focused on a sample of 10 counties in five states: Arizona, Iowa, Ohio, Oregon, and Tennessee. It included urban and rural areas. It did not identify the insurers whose networks were checked.
Susan Reilly, vice president of communications for the Better Medicare Alliance, a trade group representing Medicare Advantage plans, said managed care companies support federal efforts to improve access to mental health services. “While this report looks at a small sample of plans, we agree there’s more work to do and are committed to continuing that progress together with policymakers,” she said in a statement.
The report’s authors said their sample was a good representation of the national situation. It looked at 40 Medicare Advantage plans and 20 Medicaid managed care plans.
The report recommends government administrators make more use of medical billing data to confirm whether health professionals listed as in-network are providing care to patients covered by private Medicare and Medicaid insurance plans.
The watchdogs also recommend that federal regulators create a national, searchable directory of mental health providers, listing which Medicare and Medicaid insurance plans each one accepts. Such a directory would help patients find care and would make it easier to double-check the accuracy of plans’ listings of in-network providers, they said.
Federal administrators overseeing Medicare and Medicaid have taken steps toward creating such a directory, the authors said. Reilly, the industry representative, said managed care companies support the effort.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/medicare-medicaid-private-plans-networks-mental-health-providers/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2102833&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>“They have health care needs, but they don’t have the digital skills,” said Waiters, who is a digital navigator for an Alabama nonprofit. Her work has involved giving away computers and tablets while also teaching classes on how to use the internet for work and personal needs, like banking and health. “It’s like a foreign space.”
Those stories are now bittersweet.
Waiters is part of a network of digital navigators across the country whose work to bring others into the digital world was, at least in part, propped up by a $2.75 billion federal program that abruptly canceled funding this spring. The halt came after President Donald Trump platform that the Digital Equity Act was unconstitutional and pledged “no more woke handouts based on race!”
The act the money should benefit, including low-income households, older residents, some incarcerated people, rural Americans, veterans, and members of racial or ethnic minority groups. Politicians, researchers, librarians, and advocates said defunding the program, along with other changes in federal broadband initiatives, jeopardizes efforts to help rural and underserved residents participate in the modern economy and lead healthier lives.
“You could see lives change,” said Sam Helmick, president of the American Library Association, recalling how they helped grandpas in Iowa check prescriptions online or laid-off factory workers fill out job applications.
The Digital Equity Act is part of the sweeping 2021 infrastructure law, which included $65 billion to build high-speed internet infrastructure and connect millions without access to the internet.
This year, Congress once again pushed for a modern approach to help Americans, mandating that state leaders prioritize new and emerging technologies through its $50 billion Rural Health Transformation Program.
A found that nearly 3 million people in America live in areas with shortages of medical professionals and where modern telehealth services are often inaccessible because of poor internet connections. The analysis found that in about 200 mostly rural counties where dead zones persist, on average than people in the rest of the country. Access to high-speed internet is among a host of social factors, like food and safe housing, that help people lead healthier lives.
“The internet provides this extra layer of resilience,” said Christina Filipovic, who leads the research for an initiative of the Institute for Business in the Global Context at Tufts University. The research group that access to high-speed internet correlated with fewer covid deaths, particularly in metro areas.
During the covid-19 pandemic, federal lawmakers launched a subsidy program paid for by the infrastructure law. That aid, called the Affordable Connectivity Program, aimed to connect more people to their jobs, schools, and doctors. In 2024, Congress did not renew funding for the subsidy program, which had enrolled about .
This year, U.S. Commerce Secretary Howard Lutnick the infrastructure law’s construction initiative тАФ known as the Broadband Equity, Access, and Deployment Program, or BEAD тАФ after announcing plans to . More than 40 states and territories have submitted final proposals to extend high-speed internet to underserved areas under the administration’s new guidelines, according to a .
In May, the Digital Equity Act’s funding was terminated within days of Trump’s Truth Social post. While many states in 2022 had received money to plan their programs, the next round of funding, designated for states and agencies to implement the plans, had largely been awarded but not distributed.
Instead, federal regulators тАФ including the National Telecommunications and Information Administration, the federal agency overseeing implementation of the Digital Equity Act тАФ that the grants would be terminated. The grants were created and administered with “unconstitutional racial preferences,” according to the letter.
In Phoenix, officials learned in January that the city was slated to get $11.8 million to increase internet access and teach digital literacy, but they received an email May 20 stating that all grants, “except for grants to Native Entities,” had been terminated. “It’s a shame,” said Phoenix Mayor Kate Gallego, a Democrat. The money, she said, would have helped 37,000 residents get internet access.
Georgia’s Democratic leaders in July to Lutnick and NTIA’s then-acting administrator, Adam Cassady, urging reinstatement of the money, noting that the federal cut ignores congressional intent and violates public trust.
The act’s creator, Sen. Patty Murray (D-Wash.), said in May that Republican governors in 2024 supported the law and its funding when each state touted completing its required digital equity plans and asked for resources.
“I cannot believe there aren’t Republican governors out there that are going to join with us to fight back on this,” Murray said, adding “the other way is through courts.”
All 50 states developed digital equity plans after months of focus groups, surveys, and public comment periods. NTIA Digital Equity Director Angela Thi Bennett, during an August 2024 interview with ║┌┴╧│╘╣╧═Ї News, said the “intentional community engagement” by federal and state leaders to deliver broadband to unserved communities was “the greatest demonstration of participatory democracy our country has ever seen.”
Thi Bennett could not be reached for comment on this article. NTIA spokesperson Stephen Yusko said the agency “will not be able to accommodate” a request for an interview with Thi Bennett and did not respond to questions for this article.
Caroline Stratton, a research director at the Benton Institute for Broadband & Society, said the act’s funding allowed states to staff offices; identify existing high-speed internet programs, including those operating within other state agencies; and create plans to fill the gaps.
“This sent folks out looking,” Stratton said, to see whether agencies in the state were already working on health improvement plans and to ask whether the broadband work could contribute and “actively help move the needle.”
State grant applications included goals . In Mississippi, the of the state university and another agency’s health improvement plan, Stratton said.
While states were required to create programs that would help specific covered populations, some states modified the language or added subcategories to include other populations. included immigrants and “individuals experiencing homelessness.”
“In every state, there’s a loss,” said Angela Siefer, executive director of the National Digital Inclusion Alliance. The nonprofit, which was awarded to work with organizations nationwide but did not receive any funds, filed a lawsuit Oct. 7 seeking to force Trump and the administration to distribute the money.
“The digital divide is not over,” Siefer said.
The nonprofit’s grant had been planned to support digital navigators in 11 states and territories, including Waiters. Her employer, the nonprofit Community Service Programs of West Alabama, expected to receive a $1.4 million grant.
In the past two years, Waiters spent hours driving the roads of rural Alabama to reach residents. She has distributed 648 devices тАФ laptops, tablets, and SIM cards тАФ and helped hundreds of clients through 117 two-hour digital skills classes at libraries, senior centers, and workplace development programs in and around Tuscaloosa, Alabama.
People of “all races, of all ages, of all financial backgrounds” who did not “fit into our typical minority category” were helped through her work, Waiters said. Trump and his administration should know, she said, “what it actually looks like for the people I serve.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/race-and-health/digital-equity-act-bead-trump-cuts-health-care-access-rural/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2098549&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Sager, a Marine Corps and Army veteran, uses his VA coverage for non-VA treatment of back injuries stemming from his military service. But he said he sometimes must make several phone calls to obtain approval to see a local chiropractor. “It seems like it takes entirely too long,” he said.
Many veterans live hours from VA facilities, or they need health services that aren’t readily available from the VA. In such cases, the department is supposed to provide a referral and pay for private care. Critics say it often hesitates to do so.
Republicans controlling Congress aim to streamline the process of obtaining what is known as community care.
Two Republican senators have that would make it easier for rural veterans to seek care at local hospitals and clinics. The proposals would build on VA community care programs that started under Democratic President Barack Obama and were expanded in Trump’s first term.
Critics worry that steering veterans to private care facilities drains federal money from the VA hospital and clinic system. But supporters say veterans shouldn’t be forced to travel long distances or wait months for the treatment they could obtain at local hospitals and clinics.
“My main concern is for veterans, not for the VA,” Sen. Kevin Cramer (R-N.D.) told ║┌┴╧│╘╣╧═Ї News. “I don’t believe we have an obligation to sustain the bureaucracy.”
About 9 million veterans are enrolled in the VA health system. Last year, about 3 million of them тАФ including 1.2 million rural veterans тАФ used their benefits to cover care at non-VA facilities, according to data provided by the department.
Cramer that would allow veterans who live within 35 miles of a rural, “critical access” hospital to use VA benefits to cover care there or at affiliated clinics without referrals from VA staff.
Cramer, who serves on the Senate Veterans’ Affairs Committee, noted his state has just one VA hospital. It’s in Fargo, on the state’s eastern border, which is more than 400 miles by car from parts of western North Dakota.
Many North Dakota veterans drive past multiple community hospitals to get to the VA hospital for treatment, he said. Meanwhile, many rural hospitals are desperate for more patients and income. “I kept thinking to myself, тАШThis doesn’t make any sense at all,’” Cramer said.
Cramer said previous laws, including the , made it easier for veterans to use their benefits to cover care at community hospitals and clinics.
But he said veterans still must fill out too much paperwork and obtain approval from VA staffers to use non-VA facilities.

“We can’t let the VA itself determine whether a veteran is qualified to receive local care,” he said.
U.S. Rep. Mark Takano of California, who is the top Democrat on the House Veterans’ Affairs Committee, said he sees the need for outside care for some veterans. But he contends Republicans are going overboard in shifting the department’s money to support private health care facilities.
The VA provides specialized care that responds to veterans’ needs and experiences, he argues.
“We must prevent funds from being siphoned away from veterans’ hospitals and clinics, or VA will crumble,” Takano said in a statement released by his office. “Veterans cannot afford for us to dismantle VA direct care in favor of shifting more care to the community.”
Some veterans’ advocacy groups have also expressed concerns.
Jon Retzer, deputy national legislative director for the Disabled American Veterans, said the group wants to make it easier for veterans to find care. Rural and female veterans can have a particularly tough time finding appropriate, timely services at VA hospitals and clinics, he said. But the Disabled American Veterans doesn’t want to see VA facilities weakened by having too much federal money diverted to private hospitals and clinics.
Retzer said it’s true that patients sometimes wait for VA care, but so do patients at many private hospitals and clinics. Most delays stem from staff shortages, he said, which afflict many health facilities. “This is a national crisis.”
Retzer said the Disabled American Veterans favors continuing to require referrals from VA physicians before veterans can seek VA-financed care elsewhere. “We want to ensure that the VA is the primary provider of that care,” he said.
Veterans Affairs Secretary Doug Collins to improve the community care program while maintaining the strength of the department’s hospitals and clinics. The department declined a ║┌┴╧│╘╣╧═Ї News request to interview Collins.
Marcus Lewis, CEO of First Care Health Center, which includes a hospital in Park River, North Dakota, supports Cramer’s bill. Lewis is a Navy veteran who uses the VA’s community care option to pay for treatment of a back injury stemming from his military service.
Overall, Lewis said, the community care program has become easier to use. But the application process remains complicated, and participants must repeatedly obtain VA referrals for treatment of chronic issues, he said. “It’s frustrating.”
Park River is a 1,400-person town about 50 miles south of the Canadian border. Its 14-bed hospital offers an array of services, including surgery, cancer care, and mental health treatment. But Lewis regularly sees a VA van picking up local veterans, some of whom travel 140 miles to Fargo for care they’re entitled to receive locally.
“I think a lot of folks just don’t want to fight the system,” he said. “They don’t want to go through the extra hoops, and so they’ll jump in the van, and they’ll ride along.”
Rep. Mike Bost (R-Ill.), chairman of the House Veterans’ Affairs Committee, said veterans in some areas of the country have had more trouble than others in getting VA approval for care from private clinics and hospitals.
Bost helped gain for Trump’s request for $34.7 billion for the community care program in 2026. Although spending on the program has gone up and down in recent years, the appropriation represents an increase of about 50% from what it was in 2025 and 2022. The Senate included similar figures for next year in its version of a military spending budget that
Bost also co-sponsored that would spell out requirements for the VA to pay for community care.
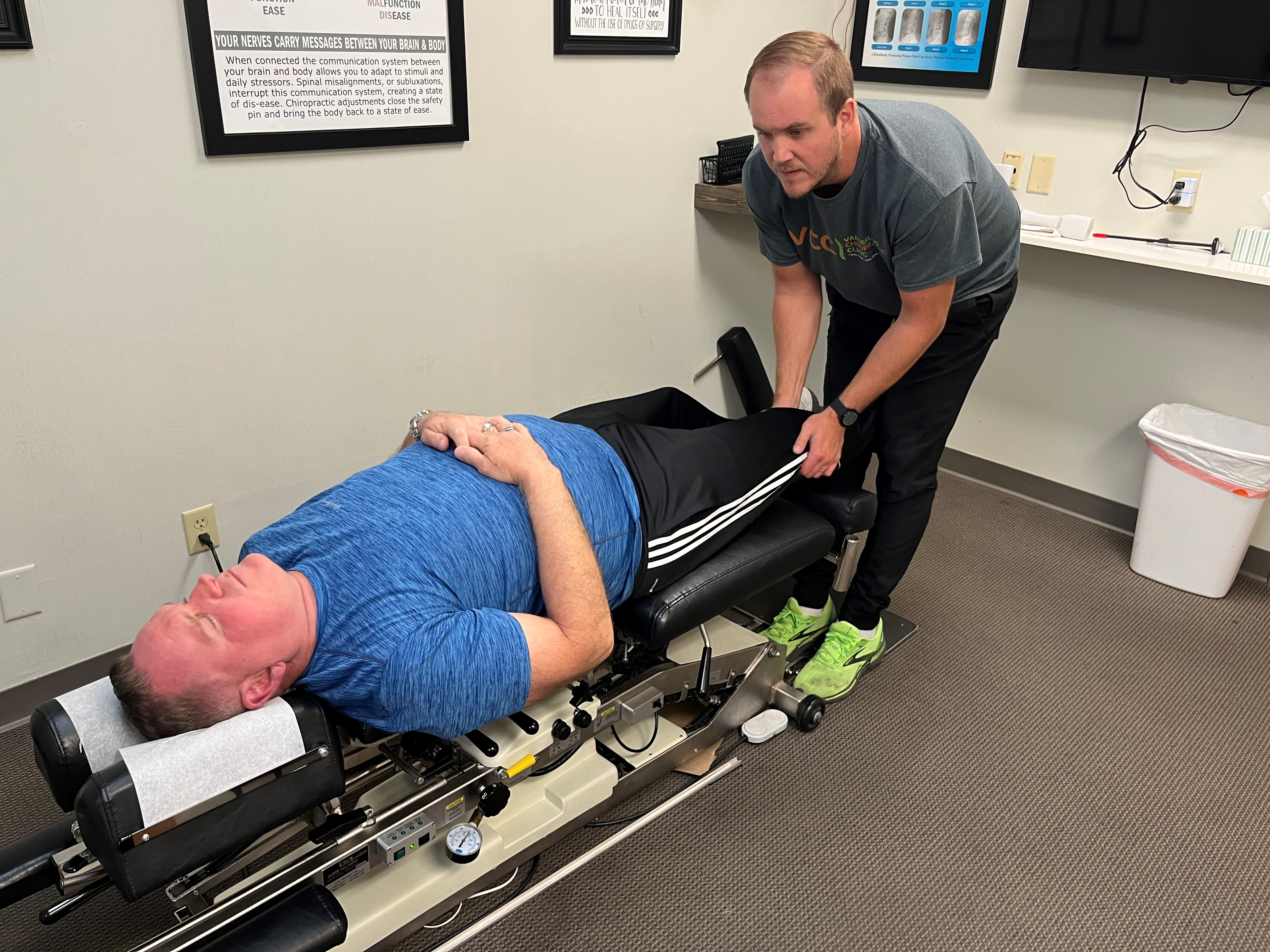
Sager hopes the new proposals make life easier for veterans. The Gulf War veteran lives in the northeastern Iowa town of Denver. He travels about 15 miles to Waterloo to see a chiropractor, who treats him for back and shoulder pain from injuries he suffered while training Saudi troops in hand-to-hand combat.
Sager, who remains active in the Army Reserve, also visits a Waterloo outpatient clinic run by the VA, where his primary care doctor practices. He appreciates the agency’s mission, including its employment of many veterans. “You just feel like you’re being taken care of by your own,” he said.
He believes the VA can run a strong hospital and clinic system while offering alternatives for veterans who live far from those facilities or who need care the VA can’t promptly provide.
The local VA doesn’t offer chiropractic care, so it pays for Sager to visit the private clinic. But every few months, he needs to obtain fresh approval from the VA. That often requires several phone calls, he said.
Sager is one of about a dozen veterans who use the community care program to pay for visits at Vanderloo Chiropractic Clinic, office manager Linda Gill said.
Gill said the VA program pays about $34 for a typical visit, which is comparable to private insurance, but the paperwork is more burdensome. She said leaders of the chiropractic practice considered pulling out of the VA program but decided to put up with the hassles for a good cause. She wishes veterans didn’t have to jump through so many hoops to obtain convenient care.
“After what they’ve done for us? Please,” she said.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/veterans-rural-care-private-facilities-legislation/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2068256&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Georgia is the only state with a work requirement in place for Medicaid, but several states have been pursuing such a policy for years, only to be blocked by courts or, most recently, the Biden administration. Some seek state-specific touches to the new rules. Others aim to implement work requirements before the federal law takes effect at the end of 2026.
These states’ moves and Trump’s massive tax-and-spending law share one demand: To keep their Medicaid health coverage, adults who can work must prove they’re logging a minimum number of hours at a job or school, or else qualify for one of the few exemptions.
But now, states that jumped ahead need to ensure their proposals, which require federal approval, don’t stray too far from Trump’s law.
“The statute sets both the floor and ceiling” for work requirements, said Sara Rosenbaum, a health law and policy professor with George Washington University.
South Dakota, for example, an application for work requirements as previously planned amid concerns that the state’s laxer rules would not be allowed under the new federal law. The state’s Department of Social Services secretary had warned that working on a state proposal while the federal rules are being hashed out could be “.”
Arkansas’ plan, on the other hand, is more stringent than the federal law. There are no exemptions to its work requirements , which is pending with the Centers for Medicare & Medicaid Services.
Arizona’s proposal also includes something that’s not in the federal law: a ban on “able-bodied adults” receiving Medicaid benefits for longer than five years total in their lives.
Arkansas and Arizona government officials said they were working with federal officials to square their plans with the new standards.
Andrew Nixon, a spokesperson for the U.S. Department of Health and Human Services, said the department is analyzing how the new federal standards interact with state waivers.
The federal health department must release rules by next June that outline how states are to implement work requirements, according to , who has been tracking such waivers as part of the Program on Medicaid and the Uninsured at KFF, a health information nonprofit that includes ║┌┴╧│╘╣╧═Ї News.
“We don’t exactly know what that will cover,” Hinton said.
It’s unclear how federal officials will respond to the states’ requests, she added, but “we are aware that some folks think there is no wiggle room here.”
States can tweak their Medicaid programs through what are known as demonstration waivers, which are subject to federal approval. The waivers are designed to test new ideas in policy gray areas.
The states that have filed or plan to file such applications with work requirements include Arizona, Arkansas, Georgia, Idaho, Indiana, Iowa, Kentucky, Montana, New Hampshire, North Carolina, Ohio, South Carolina, South Dakota, and Utah.
Congressional Republicans who passed the budget reconciliation bill left room for states to use waivers to fast-track the national standards. Tara Sklar, a professor leading the University of Arizona’s Health Law & Policy Program, said she expects states seeking certain stricter requirements to have a chance of approval, while more lenient ones may face denials.
Federal officials may look favorably on Arizona’s plan, Sklar said, as a five-year lifetime Medicaid limit is different from work requirements. Even if the federal government greenlights stricter work requirements than the federal law calls for, those programs are likely to face legal challenges, she added.
The federal law includes an 80-hour-per-month minimum for work or education, with exemptions for certain adults, including people who are medically frail and parents with young, dependent children.
Montana is the first state to draft a waiver application since Congress finalized national work requirements. State lawmakers first approved work requirements — called “community engagement” standards under the state plan — in 2019, but the state’s application stalled through the end of the first Trump term and the Biden administration.
After Trump was elected again, Montana lawmakers lifted the 2025 expiration date of its Medicaid expansion program, making permanent the program that covered more than 76,000 adults in April, with the expectation that the Trump administration would approve work requirements. In mid-July, state officials to make that a reality “as soon as is practicable.”
The Montana plan largely aligns with the federal law, but it would create additional exemptions, including for people who are homeless or fleeing domestic violence.
Republican state Sen. Gayle Lammers said work requirements that also protect such people who need Medicaid were a big part of persuading legislators to keep the expansion program. At the time, officials didn’t know where the federal government would land on work requirements. And now, Lammers said, it makes sense for Montana to stick to its plan.
“The state should have a say,” Lammers said. “We’re very independent, and everyone is different.”
In South Carolina, state officials are seeking to roll out work requirements for a limited number of newly eligible Medicaid beneficiaries. South Carolina is one of 10 states that has not expanded Medicaid eligibility under the Affordable Care Act, and yet the state submitted a request with the federal government in June for a partial Medicaid expansion that includes a work requirement component that largely reflects the new federal standards.
In to Health and Human Services Secretary Robert F. Kennedy Jr., South Carolina Gov. Henry McMaster, a Republican, called South Carolina’s proposal “a state-specific solution.”
The only state with an active work requirement program now wants to scale it back and awaits federal approval to do so. “Georgia Pathways to Coverage” expires at the end of September unless CMS greenlights an extension of the program with a key change: requiring enrollees to document once a year that they’re working, not monthly. That’s a pivot away from the program’s initial design but also differs from the new federal rules, which call for checks every six months.
Fiona Roberts, a spokesperson for Georgia’s Medicaid agency, said the state is still waiting to hear whether it needs to alter its plan.
So Georgia is among the states in limbo, awaiting guidance from the federal government.
║┌┴╧│╘╣╧═Ї News correspondents Sam Whitehead and Lauren Sausser contributed to this report.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/medicaid-federal-work-requirements-less-leeway-for-states/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2067611&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>