It’s one of the many parts of the 25-bed rural hospital that need updating, former CEO Ron Wiens said.
He said the hospital, an essential service in its namesake town of nearly 800 residents in the state’s sprawling north-central high plains, needs at least $1 million for deferred maintenance, including a failing HVAC system. But the facility has struggled to make payroll each month and can’t afford to make all the fixes, Wiens said.
Built by farmers and ranchers in 1965, Big Sandy Medical Center began with nine beds. Today, a similar community effort тАФ donations and grants to plug financial holes each year тАФ keeps it afloat.
Wiens, who recently left his position at the hospital, said he wishes Big Sandy could get funding from Montana’s share of the $50 billion federal Rural Health Transformation Program to renovate the hospital and direct payments to help secure its future. The state received more than $233 million in its first-year award.
But the hospital may not get the kind of help he sought.
That’s because the five-year program focuses on new, creative ways to improve access to rural health care, not on directly funding services and renovations. And Montana is one of at least 10 states whose leaders say projects launched under the federal program could lead rural hospitals to cut services so they can continue to afford to offer emergency and other essential care.

Congressional Republicans created the fund as a last-minute sweetener to their One Big Beautiful Bill Act, signed into law last summer. The funding was intended to offset disproportionate fallout anticipated in rural communities from the law, which is expected to slash Medicaid spending .
includes programs to make it easier for rural residents to get medical care and live a healthy lifestyle. For example, it says funding can be used to start community gardens, train paramedics to make home visits, open school-based clinics, or bring mobile clinics to rural areas.
rural Montana hospitals can receive payments for implementing recommendations, “including right-sizing select inpatient services” to match demand. In some cases, it says, right-sizing might mean “downsizing.” The state says hospitals will have input and recommendations will be specific to each facility.
“That’s what has all the hospitals on pins and needles, words like restructuring, reducing inpatient beds. Everybody is going, тАШWhat is this going to look like?’” Wiens said.
The Montana Department of Public Health and Human Services declined to answer questions about how it will carry out its right-sizing efforts.
A Lifeline of Care
Big Sandy cattle rancher Shane Chauvet doesn’t want any services cut.
He credits Big Sandy Medical Center with saving his life after a flying piece of metal nearly cut off his arm during a windstorm a few years back.
“I looked over, saw it coming, and whack!” Chauvet recalled.
His wife drove him to the hospital, where they frantically pounded on the ER door while Chauvet’s blood pooled on the ground.
Because of the storm, staffers worked on Chauvet with no power and no ability to summon a helicopter. He was then taken by ambulance 80 miles through intense rain and hail to a larger hospital.
Chauvet understands the state’s plan doesn’t call for eliminating emergency care, but he worries that reducing other services would set off a downward spiral for the hospital and his town.

In Oklahoma, realigning clinical services could mean “shutting down service lines,” to the federal program. And in Wyoming, any facility that receives funding must agree to “reduce unprofitable, duplicative or nonessential service lines,” .
Monique McBride, business operations administrator at the Wyoming Department of Health, said the department interprets right-sizing as helping rural hospitals provide essential services тАФ such as emergency departments, ambulance services, and labor and delivery units тАФ while maintaining long-term, financial stability.
“This might involve limiting some elective procedures that could be done at lower cost in higher-volume facilities. The main distinction here is time-sensitive emergencies vs. тАШshoppable’ services,” she said.
A New Lease on Life?
Seven of the 10 states тАФ Nebraska, North Dakota, Tennessee, Kansas, Nevada, South Carolina, and Washington тАФ where rural hospital service cuts are on the table say they’ll help pay for hospitals to convert to Rural Emergency Hospitals. The recently created federal designation requires hospitals to halt inpatient services and offers enhanced payments to help them maintain emergency and outpatient care.
At least 15 additional states wrote that they’ll use the federal funding to right-size, evaluate, or adjust services тАФ which could mean adding or taking away services, or transitioning them to a telehealth or outpatient setting.
Brock Slabach, chief operations officer of the National Rural Health Association, said, “There’s a proper concern from rural hospital administrators that this funding is not going to where it was intended.”
He said cutting services that lose money could backfire in the long run. For example, he said, halting labor and delivery care might drive more people out of small towns, further reducing hospitals’ patient numbers and revenue.
The type of hospital services that states will assess matters, said Tony Shih, a senior adviser at the Commonwealth Fund, a nonprofit focused on making health care more equitable.
“If the end result is that high-margin services are taken away from local hospitals with nothing given back in return, it can be financially harmful,” he said.
Shih noted that states’ plans to add more outpatient care could prove beneficial for patients. It’ll take time to know which states help stabilize rural hospitals, he said.
Rural hospital leaders say they know which changes would keep their facilities open and that states shouldn’t suggest or mandate service cuts and other changes on their behalf.

Josh Hannes, who oversees rural health policy at the Colorado Hospital Association, said “top-down” directives won’t work.
He said the association’s members believe they can find efficiencies and are eager to collaborate. But “a state agency shouldn’t be making those determinations,” he said.
Hannes said members are worried Colorado’s plan to classify rural health facilities as a “hub, spoke, or telehealth node” will compel service reductions. The classification will help determine “which services are sustainable locally and which are best provided regionally or through telehealth,” .
Spokespeople for the Colorado and Oklahoma health departments said no facility will be forced to end services. But Oklahoma spokesperson Rachel Klein said some facilities might choose to do so as part of a broader effort to make sure they’re meeting community needs while remaining financially stable.
“A hospital might shift certain services to a nearby regional provider with higher patient volume and specialized staff while expanding other local services,” such as primary, outpatient, or community-based care, she said.
Wiens and Darrell Messersmith, CEO of Dahl Memorial Hospital in the southeastern Montana town of Ekalaka, said they worry the only way hospitals will get their share of funding is to cut services or become Rural Emergency Hospitals that don’t offer inpatient services.
“I would hate to see things shift toward a pack-and-ship facility,” Messersmith said. “Right now, we function quite well as an inpatient facility.”
Not all Montana health leaders are worried.
Ed Buttrey, president and CEO of the Montana Hospital Association, said he thinks his state’s plan could help rural hospitals become financially sustainable and survive Medicaid cuts. Buttrey is also a Republican state lawmaker.
Chauvet, the Big Sandy rancher, said his perspective on whether remote towns like his should have a hospital is forever changed because of his accident.
“I always would say, тАШOh, they’re nice to have,’ but now I look at the hospital and say, тАШThat’s essential to our community,’” he said.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/rural-emergency-hospitals-montana-rightsize-downsize-services-transformation-fund/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2172028&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The legislation would prohibit state and local governments from requiring crisis pregnancy centers to perform abortions, provide referrals for abortion services, or inform patients about such services or contraception options. It also would allow crisis pregnancy centers to sue the violating government entity.
Wyoming lawmakers of the Center Autonomy and Rights of Expression Act, or , on March 4. Other versions have advanced in and this year. One was in 2025. The CARE Act is “model legislation” created by the , an anti-abortion, conservative Christian legal advocacy group.
A similar proposal, the , was introduced in Congress last year but hasn’t moved out of the House Energy and Commerce Committee.
The Wyoming bill says that pregnancy centers, many of which are affiliated with religious organizations, need legal protection after facing “unprecedented attacks” following the Supreme Court’s overturning of Roe v. Wade. It says that several state legislatures have introduced bills that . Opponents of these centers say they falsely present themselves to consumers as medical clinics, though they are not subject to state and federal laws that protect patients in medical facilities.
“Across the country, government officials are increasingly, increasingly targeting pregnancy care centers,” Valerie Berry, executive director of the in Cheyenne, said at a February legislative hearing on the Wyoming bill. “This legislation is not about creating division. It’s about protecting constitutional freedoms, freedom of speech, and freedom of conscience.”
Wyoming state , a Republican, expressed concern at the hearing about granting protections to pregnancy centers that other private businesses do not have.
“They have protections in place,” he said. “My issue with this is giving extra special protections.”
In 2022, Wellspring Health Access, the only clinic in Wyoming that provides abortions, in an arson attack.
“We are the ones providing the accurate information on reproductive health care, and we suffer the consequences for that,” Julie Burkhart, the president and founder of Wellspring Health Access, told ║┌┴╧│╘╣╧═Ї News.
, a professor at the University of California-Davis School of Law, said the proposed legislation would insulate crisis pregnancy centers from having to meet the standards that medical organizations face. It would blur the line between advocacy and medical practice, she said. And such legislation provides Republicans with a potentially useful campaign message ahead of midterm elections.
“The GOP needs a messaging strategy as for how it cares about women even if it bans abortion and even if it doesn’t want to commit state resources to helping people before and after pregnancy,” Ziegler said. “The strategy is to outsource that to pregnancy counseling centers, which of course increases the incentive to protect them.”
Model Legislation
The Alliance Defending Freedom is the same group that , the 1973 court ruling that protected the right to abortion nationwide. The group drafted model legislation to establish a 15-week abortion ban that was the basis of a 2018 Mississippi law. That led to the Dobbs v. Jackson Women’s Health Organization Supreme Court case that overturned Roe.
The alliance said its attorneys were unavailable to comment on the organization’s strategy for the CARE Act. In for the bill, the group said federal, state, and local efforts are targeting pregnancy care centers in a “clear attempt to undermine and impede” their work and shut them down.
In recent years, have been targeted with vandalism and threats.
But the attacks the model legislation primarily aims to address are the legal and regulatory efforts by some states seeking more oversight of the crisis pregnancy centers, including a California law requiring centers to clearly inform patients about their services. That law was overturned when the Supreme Court ruled in favor of crisis pregnancy centers’ argument that it violated their First Amendment rights.
The Supreme Court is that will decide whether states can subpoena the organizations for donor and internal information.
It’s unlikely that crisis pregnancy centers would face such regulatory measures in the conservative states where the legislation is under consideration. One Wyoming lawmaker acknowledged that in the February committee hearing.
Differing Services
During that hearing, state , a Republican who heads the committee sponsoring the bill, presented the measure as “so important, especially with our maternity desert,” referring to a lack of access to maternity health care services.
Some crisis pregnancy centers may have a few licensed clinicians, but many do not. Many offer free resources, such as diapers, baby clothing, and other items, sometimes in exchange for participation in counseling or parenting classes.
Planned Parenthood clinics, by contrast, provide a range of health services, such as testing and treatment for sexually transmitted infections, primary care, and screenings for cervical cancer. They also are regulated as medically licensed organizations.
Since Roe was overturned, the abortion rights movement has faced significant challenges. Congressional Republicans’ One Big Beautiful Bill Act, which President Donald Trump signed into law last summer, to abortion providers. The move contributed to Planned Parenthood closing last year.
As of 2024, operated nationwide, according to a map created by researchers at the University of Georgia, compared with providing abortions at the end of 2025.
a research organization affiliated with the anti-abortion nonprofit SBA Pro-Life America, has suggested that pregnancy centers could help fill the gap left by the Planned Parenthood closures.
Ziegler said that would leave patients vulnerable to medical risks.
Centers’ Growing Power
Previous efforts in , Colorado, and Vermont to regulate crisis pregnancy centers arose from concerns over allegations of and questions about .
In 2024, in five states to investigate whether centers were misleading patients into believing that their personal information was protected under the Health Insurance Portability and Accountability Act, known as HIPAA, and to find out how the centers were using patients’ information.
Courts, including the Supreme Court, have regularly that argue the attempts at regulation are violations of their First Amendment rights to free speech and religious expression.
Crisis pregnancy centers also have seen a flood of funding since Roe was overturned.
At least , including crisis pregnancy centers, according to the Lozier Institute.
Six states distribute a portion of their federal Temporary Assistance for Needy Families funding тАФ cash payments meant for low-income families with children тАФ to crisis pregnancy centers. Texas, Florida, Tennessee, and Oklahoma have provided tens of millions of dollars for the organizations.
One analysis found that crisis pregnancy centers also received from 2017 to 2023, including from the 2020 relief package signed into law during Trump’s first term amid the covid pandemic.
Despite the challenges clinics that provide abortions face, Burkhart, the head of the Wellspring facility in Wyoming, said it’s important to continue offering access to people who need it. She’s helped open clinics in rural parts of other conservative states and said those clinics continue to see people walking through their doors.
“That proves to me, regardless of your religion, political party, there are times in people’s lives that people need access to qualified reproductive health care,” she said. “That includes abortion.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/courts/abortion-bans-clinics-crisis-pregnancy-centers-maternity-care-wyoming/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2166071&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The 59-year-old, who lives in Harrisburg, North Carolina, closed her nonprofit circus arts school last year because she could no longer see well enough to complete paperwork. She then worked making dough at a pizza shop for a bit. Currently, she sorts recyclable materials, including cans and bottles, at a local concert venue. It is her main source of income ― but the work isn’t year-round.
“This place knows me, and this place loves me,” Kelley said of her employer. “I don’t have to explain to this place why I can’t read.”
Kelley, who lives in a camper, survives on less than $10,000 a year. She says that’s possible, in part, because of her Medicaid health coverage, which pays for arthritis and anxiety medications and has enabled doctor visits to manage high blood pressure.
But she worries about losing that coverage next year, when rules take effect requiring millions of people like Kelley to work, volunteer, attend school, or perform other qualifying activities for at least 80 hours a month.
“I’m scared right now,” she said.


Before the coverage changes were signed into law, Republican lawmakers suggested that young, unemployed men were taking advantage of the government health insurance program that provides coverage to millions of low-income or disabled people. Medicaid is not intended for “29-year-old males sitting on their couches playing video games,” House .
But, in reality, adults ages 50 to 64, particularly women, are likely to be , said Jennifer Tolbert, deputy director of the Program on Medicaid and the Uninsured at KFF, a health information nonprofit that includes ║┌┴╧│╘╣╧═Ї News. For Kelley and others, the work requirements will create barriers to keeping their coverage, Tolbert said. Many could lose Medicaid as a result, putting their physical and financial health at risk.
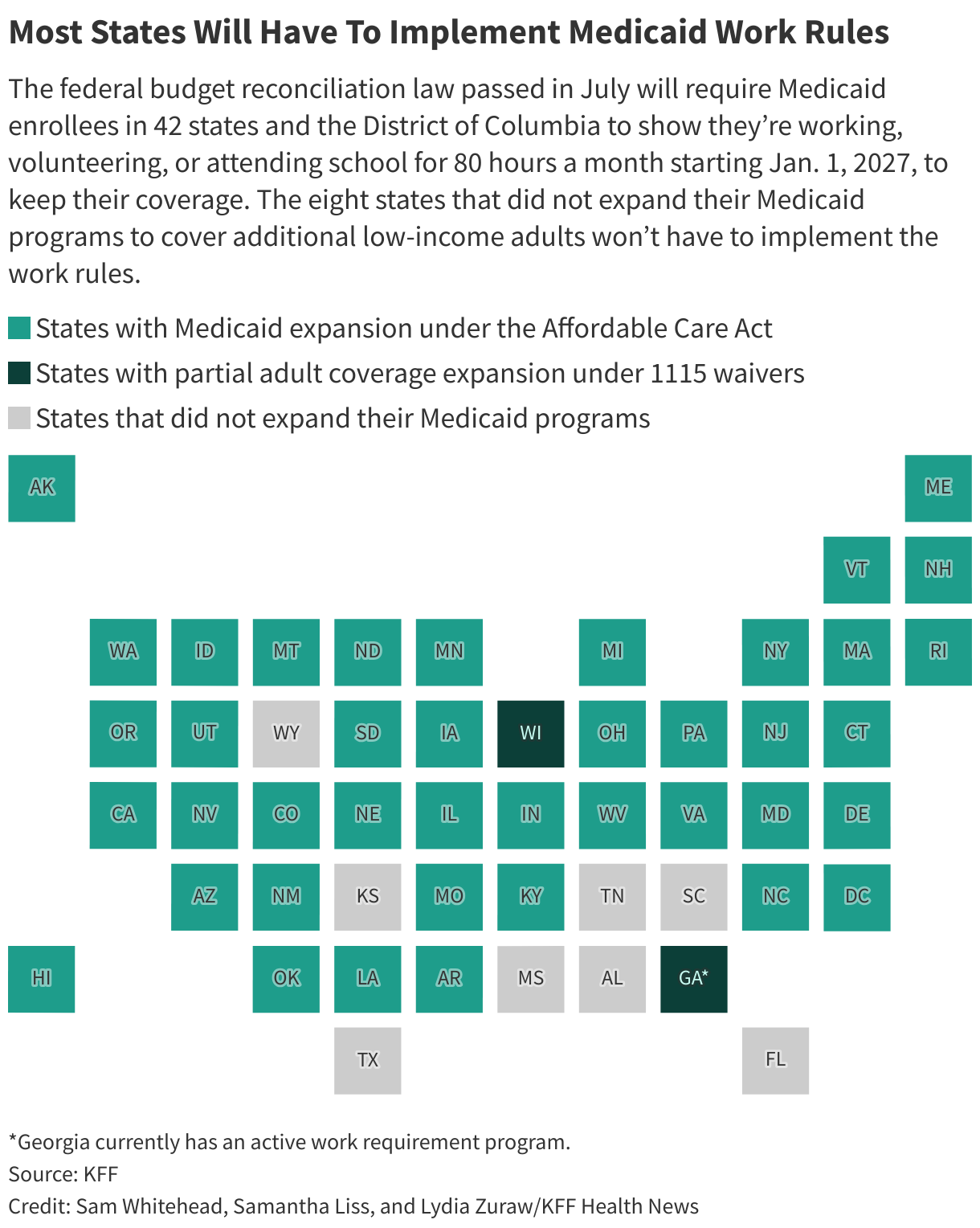
Starting next January, some 20 million low-income Americans in 42 states and Washington, D.C., will need to meet the activity requirements to gain or keep Medicaid health coverage.
Alabama, Florida, Kansas, Mississippi, South Carolina, Tennessee, Texas, and Wyoming didn’t expand their Medicaid programs to cover additional low-income adults under the Affordable Care Act, so they won’t have to implement the work rules.
The nonpartisan Congressional Budget Office predicts the work rules will result in at least 5 million fewer people with Medicaid coverage over the next decade. Work rules are the largest driver of coverage losses in the GOP budget law, which slashes nearly $1 trillion to offset the costs of tax breaks that mainly benefit the rich and increase border security, .
“We’re talking about saving money at the expense of people’s lives,” said Jane Tavares, a gerontology researcher at the University of Massachusetts Boston. “The work requirement is just a tool to do that.”
Department of Health and Human Services spokesperson Andrew Nixon said requiring “able-bodied adults” to work ensures Medicaid’s “long-term sustainability” while safeguarding it for the vulnerable. Exempt are people with disabilities, caregivers, pregnant and postpartum individuals, veterans with total disabilities, and others facing medical or personal hardship, Nixon told ║┌┴╧│╘╣╧═Ї News.
Medicaid expansion has provided a lifeline for middle-aged adults who otherwise would lack insurance, according to . Medicaid covers 1 in 5 Americans ages 50 to 64, giving them access to health coverage before they qualify for Medicare at age 65.
Among women on Medicaid, those ages 50 through 64 are more likely to face challenges keeping their coverage than their younger female peers and are likely to have a greater need for health care services, Tolbert said.
These middle-aged women are less likely to be working the required number of hours because many serve as family caregivers or have illnesses that limit their ability to work, Tolbert said.
Tavares and other researchers found that of the total Medicaid population is considered “able-bodied” and not working. This group consists largely of women who are very poor and have left the workforce to become caretakers. Among this group, 1 in 4 are 50 or older.
“They are not healthy young adults just hanging out,” the researchers stated.
Plus, making it harder for people to maintain Medicaid coverage “may actually undermine their ability to work” because their health problems go untreated, Tolbert said. Regardless, if this group loses coverage, their chronic health conditions will still need to be managed, she said.
Adults often start wrestling with health issues before they’re eligible for Medicare.
If older adults don’t have the means to pay to address health issues before age 65, they’ll ultimately be sicker when they qualify for Medicare, costing the program more money, health policy researchers said.
Many adults in their 50s or early 60s are no longer working because they’re full-time caregivers for children or older family members, said caregiver advocates, who refer to people in the group as “the sandwich generation.”


The GOP budget law does allow some caregivers to be exempted from the Medicaid work rules, but the carve-outs are “very narrow,” said Nicole Jorwic, chief program officer for the group Caring Across Generations.
She worries that people who should qualify for an exemption will fall through the cracks.
“You’re going to see family caregivers getting sicker, continuing to forgo their own care, and then you’re going to see more and more families in crisis situations,” Jorwic said.
Paula Wallace, 63, of Chidester, Arkansas, said she worked most of her adult life and now spends her days helping her husband manage his advanced cirrhosis.
After years of being uninsured, she recently gained coverage through her state’s Medicaid expansion, which means she’ll have to comply with the new work requirements to keep it. But she’s having a hard time seeing how that will be possible.
“With me being his only caregiver, I can’t go out and work away from home,” she said.
Wallace’s husband receives Social Security Disability Insurance, she said, and the law says she should be exempt from the work rules as a full-time caregiver for someone with a disability.
But federal officials have yet to issue specific guidance on how to define that exemption. And ― the only states to have run Medicaid work programs ― shows that many enrollees struggle to navigate complicated benefits systems.
“I’m very concerned,” Wallace said.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/medicaid-work-requirements-middle-aged-adults-women/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2151346&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Then 25 years old and six months pregnant, she drove herself to the emergency room in Ronan, Montana, on the Flathead Indian Reservation, where an ambulance transferred her to a larger hospital 60 miles away in Missoula. Once she arrived, the staff couldn’t detect her baby’s heartbeat. Swaney began to bleed heavily. She delivered a stillborn baby and was hospitalized for several days. At one point, doctors told her to call her family. They didn’t expect her to survive.
“It certainly changed my life тАФ the experience тАФ but my life has not been a bad life,” she told ║┌┴╧│╘╣╧═Ї News.
Though her experiences were nearly 50 years ago, Swaney, a member of the Confederated Salish and Kootenai Tribes, said Native Americans continue to receive inadequate maternal care. The data appears to support that belief.
In 2024, the most recent year for which data for the population is available, Native American and Alaska Native people had the among major demographic groups, according to the Centers for Disease Control and Prevention.
In response to this disparity, Native organizations, the CDC, and some states are working to boost tribal participation in state maternal mortality review committees to better track and address pregnancy-related deaths in their communities. Native organizations are also considering ways tribes could create their own committees.
State maternal mortality review committees investigate deaths that occur during pregnancy or within a year after pregnancy, analyze data, and issue policy recommendations to lower death rates.
According to 2021 CDC data, compiled from 46 maternal mortality review committees, 87% of maternal deaths in the U.S. were deemed preventable. Committees reported that , deaths among Native American and Alaska Native people were considered preventable.
Our matriarchs, our moms, are what carries a nation forward.
Kim Moore-Salas
State committees have received federal money through the Preventing Maternal Deaths Act, which President Donald Trump signed in 2018.
But the money is scheduled to dry up on Jan. 31, when the short-term spending bill that ended the government shutdown expires.
Funding for the committees is included in the Labor, Health and Human Services, Education, and Related Agencies for fiscal year 2026. That bill must be approved by the House, Senate, and president to take effect.
Native American leaders said including members of their communities in maternal mortality review committee activities is an important step in addressing mortality disparities.
In 2023, tribal leaders and federal officials met to discuss four models: a mortality review committee for each tribe, a committee for each of the 12 Indian Health Service administrative regions, a national committee to review all Native American maternal deaths, and the addition of Native American subcommittees to state committees.
Whatever the model, tribal sovereignty, experience, and traditional knowledge are important factors, said Kim Moore-Salas, a co-chair of the Arizona Maternal Mortality Review Committee. She’s also the chairperson of the panel’s American Indian/Alaska Native mortality review subcommittee and a member of the Navajo Nation.
“Our matriarchs, our moms, are what carries a nation forward,” she said.
Mental health conditions and infection were the leading underlying causes of pregnancy-related death among Native American and Alaska Native women as of 2021, according to the CDC report analyzing data from 46 states.
The CDC found an estimated 68% of pregnancy-related deaths among Native American and Alaska Native people happened within a week of delivery to a year postpartum. The majority of those happened between 43 days and a year after birth.
The federal government has a responsibility under signed treaties to provide health care to the 575 federally recognized tribes in the U.S. through the Indian Health Service. Tribal members can receive limited services at no cost, but the agency is .
A that analyzed data from 2016 to 2020 found that approximately 75% of Native American and Alaska Native pregnant people didn’t have access to care through the Indian Health Service around the time of giving birth, meaning many likely sought care elsewhere. More than 90% of Native American and Alaska Native births occur outside of IHS facilities, . For those who did deliver at IHS facilities, a from the Department of Health and Human Services’ Office of Inspector General found that 56% of labor and delivery patients received care that did not follow national clinical guidelines.
The 2024 study’s authors also found that members of the population were less likely to have stable insurance coverage and more likely to have a lapse in coverage during the period close to birth than non-Hispanic white people.
Cindy Gamble, who is Tlingit and a tribal community health consultant for the American Indian Health Commission in Washington, has been a member of the state’s maternal mortality review panel for about eight years. In the time she’s been on the state panel, she said, its composition has broadened to include more people of color and community members.
The panel also began to include suicide, overdose, and homicide deaths in its data analysis and added racism and discrimination to the risk factors considered during its case review process.
Solutions need to be tailored to the tribe’s identity and needs, Gamble said.
“It’s not a one-size-fits-all,” Gamble said, “because of all the beliefs and different cultures and languages that different tribes have.”
Gamble’s tenure on the state committee is distinctive. Few states have tribal representation on maternal mortality review committees, according to the National Indian Health Board, a nonprofit organization that advocates for tribal health.
The National Council of Urban Indian Health is also the participation of Urban Indian health organizations, which provide care for Native American people who live outside of reservations, in state maternal mortality review processes. As of 2025, the council had connected Urban Indian health organizations to state review committees in California, Kansas, Oklahoma, and South Dakota.
Native leaders such as Moore-Salas find the current efforts encouraging.
“It shows that state and tribes can work together,” she said.
In March 2024, Moore-Salas became the first Native American co-chair of Arizona’s Maternal Mortality Review Committee. In 2025 she and other Native American members of the committee developed guidelines for the American Indian/Alaska Native subcommittee and reviewed the group’s first cases.
The subcommittee is exploring ways to make the data collection and analysis process more culturally relevant to their population, Moore-Salas said.
But it takes time for policy changes to create widespread change in the health of a population, Gamble said. Despite efforts around the country, other factors may hinder the pace of progress. For example, maternity care deserts are growing nationally, caused by rapid hospital and labor and delivery unit closures. Health experts have that upcoming cuts to Medicaid will hasten these closures.
Despite her experience and the ongoing crisis among Native American and Alaska Native people, Swaney hopes for change.
She had a second complicated pregnancy soon after her stillbirth. She went into labor about three months early, and the doctors said her son wouldn’t live to the next morning. But he did, and he was transferred about 525 miles away from Missoula to the nearest advanced neonatal unit, in Salt Lake City.
Her son, Kelly Camel, is now 48. He has severe cerebral palsy and profound deafness. He lives alone but has caregivers to help with cooking and other tasks, said Swaney, 73.
He “has a good sense of humor. He’s kind to other people. We couldn’t ask for a more complete child.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/native-american-pregnancy-maternal-mortality-mothers-deaths-tribes/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2137280&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>“That’s what I’m trying to avoid,” said Ferguson, who still calls Quincy Jackson III her baby. She remembers a boy who dressed himself in three-piece suits, donated his allowance, and graduated high school at 16 with an academic scholarship and plans to join the military or start a business.
Instead, Ferguson watched as her once bright-eyed, handsome son sank into disheveled psychosis, bouncing between family members’ homes, homeless shelters, jails, clinics, emergency rooms, and Ohio’s regional psychiatric hospitals.
Over the past year, The Marshall Project – Cleveland and ║┌┴╧│╘╣╧═Ї News interviewed Jackson, other patients and families, current and former state hospital employees, advocates, lawyers, judges, jail administrators, and national behavioral health experts. All echoed Ferguson, who said the mental health system makes it “easier to criminalize somebody than to get them help.”
State psychiatric hospitals nationwide have largely lost the ability to treat patients before their mental health deteriorates and they are charged with crimes. Driving the problem is a meteoric rise in the share of patients with criminal cases who stay significantly longer, generally by court order.
Patients Wait or Are Turned Away
Across the nation, psychiatric hospitals are short-staffed and consistently turn away patients or leave them waiting with few or no treatment options. Those who do receive beds are often sent there by court order after serious criminal offenses.
In Ohio, the share of state hospital patients with criminal charges jumped from about half in 2002 to .
The surge has coincided with a steep decline in total state psychiatric hospital patients served, down 50% in Ohio in the past decade, from 6,809 to 3,421, according to the . During that time, total patients served nationwide dropped about 17%, from 139,434 to 116,320, with state approaches varying widely, from adding community services and building more beds to closing hospitals.
Ohio Department of Behavioral Health officials declined multiple interview requests for this article.
The decline in capacity at state facilities unfurled as a spate of local hospitals across the country shuttered their psychiatric units, which disproportionately serve patients with Medicaid or who are uninsured. And the financial stability of is likely to deteriorate further after Congress passed President Donald Trump’s One Big Beautiful Bill Act, which slashes nearly $1 trillion from the federal Medicaid budget over the next decade.
The constricted flow of new patients through state hospitals is “absolutely” a crisis and “a huge deal in Ohio and everywhere,” said retired Ohio Supreme Court Justice Evelyn Lundberg Stratton. As co-chair of the state attorney general’s , Lundberg Stratton has spent decades searching for solutions.
“It hurts everybody who has someone who needs to get a hospital bed that’s not in the criminal justice system,” she said.


тАШIt’s Heartbreaking’
Quincy Jackson III’s white socks stuck out of the end of a hospital bed as police officers stood watch.
At 5 feet, 7 inches tall, Jackson has a stocky build and robotic stare. Staff at Blanchard Valley Hospital in Findlay, Ohio, had called for help, alleging Jackson had assaulted a security guard.
“I’m sick; I take medication,” Jackson said to the officers, according to law enforcement body camera footage. His hands were cuffed behind his back as he lay on the bed, a loose hospital gown covering him.
Ferguson called it one of his “episodes” and said her son experienced severe psychosis frequently. In one incident, she said, Jackson “went for a knife” at her home.
From December 2023 through this July, Jackson was arrested or cited in police reports on at least 17 occasions. He was jailed at least five times and treated more than 10 times at hospitals, including three state-run psychiatric facilities. A recent psychiatric evaluation noted that Jackson has been in and out of community and state facilities since 2015.
Jackson is among a glut of people nationwide with severe mental illness who overwhelm community hospitals, courtrooms, and jails, eventually leading to backlogs at state hospitals.
High-Profile Incidents
That dearth of care is often cited by families, law enforcement authorities, and mental health advocates after people struggling with severe mental illness harm others. In the past six months, at least four incidents made national headlines.
In August, a homeless reportedly diagnosed with schizophrenia fatally stabbed a woman on a train. Also in August, police said a with a history of mental health issues killed three people, including a child, at a Target store. In July, a homeless who family members said had needed treatment for decades attacked 11 people at a Walmart store with a knife. In June, police shot and killed a reportedly diagnosed with schizophrenia after authorities said he attacked law enforcement.
Mark Mihok, a longtime municipal judge near Cleveland, told a spring that he had never seen so many people with serious mental illnesses living on the streets and “now punted into the criminal justice system.”
37-Day Wait for a Bed
At Blanchard Valley Hospital, sheriff’s deputies had taken Jackson from jail for a mental health check. But Jackson’s actions raised concerns.
In the body camera video, a nurse said Jackson was “going to be here all weekend. And we’re going to be calling you guys every 10 minutes.”
The officer responded: “Yeah, well, if he keeps acting like that, he’s going to go right back” to the county jail.
Within minutes, Jackson was taken back to jail, yelling at the officers: “Kill me, motherf—–. Yeah, shoot them, shoot them. Pop!”
Statewide, Ohio has about 1,100 beds in its six regional psychiatric hospitals. In May, the median wait time to get a state bed was 37 days.
That’s “a long time to be waiting in jail for a bed without meaningful access to mental health treatment,” said Shanti Silver, a senior research adviser at the national nonprofit Treatment Advocacy Center.
Long waits, often leaving people who need care lingering in jails, have drawn lawsuits in several states, including , , and , where a large 2014 class action case forced systemic changes such as expansion of crisis intervention training and residential treatment beds.
Ohio officials noticed bed shortages as early as 2018. State leaders assembled task forces and . They launched community programs, crisis units, and a statewide emergency hotline.
Yet backlogs at the Ohio hospitals mounted.
Ohio Department of Behavioral Health Director LeeAnne Cornyn, who left the agency in October, wrote in a May emailed statement that the agency “works diligently to ensure a therapeutic environment for our patients, while also protecting patient, staff, and public safety.”
Eric Wandersleben, director of media relations and outreach for the department, declined to respond to detailed questions submitted before publication and, instead, noted that responses could be publicly found in a governor’s working group report .
Elizabeth Tady, a hospital liaison who also spoke to judges and lawyers at the May gathering, said 45 patients were waiting for beds at Northcoast Behavioral Healthcare, the state psychiatric hospital serving the Cleveland region.
“It’s heartbreaking for me and for all of us to know that there are things that need to be done to help the criminal justice system, to help our communities, but we’re stuck,” she said.
Ohio officials added 30 state psychiatric beds by in Columbus and are planning in southwestern Ohio.
Still, Ohio Director of Forensic Services Lisa Gordish told the gathering in Cleveland that adding capacity alone won’t work.
“If you build beds тАФ and what we’ve seen in other states is that’s what they’ve done тАФ those beds get filled up, and we continue to have a waitlist,” she said.
This year, Jackson waited 100 days in the and Montgomery County jail for a bed at a state hospital, according to jail records.
Ferguson said she was afraid to leave him there but could not bail him out, in part, she said, because her son cannot survive on his own.
“There’s no place for my son to experience symptoms in the state of Ohio safely,” Ferguson said.

Sick System
Patrick Heltzel got the extended treatment Ferguson has long sought for her son, but he stabbed a 71-year-old man to death before getting it.
The 32-year-old is one of more than receiving treatment in Ohio’s psychiatric hospitals.
“People need long-term care,” Heltzel said in October, calling from inside Heartland Behavioral Healthcare, near Canton, where he has lived for more than a decade after being found not guilty by reason of insanity of aggravated murder. Inpatient care, he said, helps patients figure out what medication regimen will work and deliver the therapy needed “to develop insight.”
As he spoke, the sound of an open room and patients chatting filled the background.
“You have to know, тАШOK, I have this chronic condition, and this is what I have to do to treat it,’” Heltzel said.

As the ranks of criminally charged patients in Ohio’s hospitals have increased over the past decade, the shift has had an impact on patient care: The hospitals have endangered patients, have become more restrictive, and are understaffed, according to interviews with Heltzel, other patients, and former staff members, as well as documents obtained through public records requests.
Escapes and a Lockdown
Katie Jenkins, executive director of the National Alliance on Mental Illness Greater Cleveland, said the shift from mostly civil patients, who haven’t been charged with a crime, to criminally charged patients has changed the hospitals.
“It’s hard in our state hospitals right now,” she said. Unfortunately, she said, patients who have been in jail bring that culture to the hospitals.
In the first 10 months of 2024, at least nine patients escaped from Ohio’s regional psychiatric hospitals тАФ compared with three total in the previous four years, according to .
, two female patients at Summit Behavioral Healthcare near Cincinnati escaped after one lunged at a staff member. In another, a man broke a window and climbed out.
Most of the escapes, though, were not violent. Days after a patient at Northcoast during a trip to the dentist in a Cleveland suburb, state officials stopped allowing patients to leave any of the six regional hospitals.
to leaders at the hospitals said officials had seen “similarities across multiple facilities,” raising significant concern about “ensuring patient and public safety.”
For Heltzel, the inability to go on outings or to his mother’s house on the weekends was a setback for his treatment. In 2024, when the lockdown began, he had more freedom than most patients at the psychiatric hospitals, regularly leaving to go to the local gym and attend off-site group therapy.
His mother signed him out each Friday to go home for the weekend, where he drove a car and played with his 2-year-old German shepherd, Violet. On Sundays, Heltzel was part of the “dream team” at church, volunteering to operate the audio and slides.
Federal records reveal that, at Ohio’s larger state-run psychiatric hospitals, including Summit and Northcoast, patients and staff have faced imminent danger.
In 2019 and 2020, federal investigators responded to patient deaths, including two suicides in six months at Northcoast. One hospital employee told federal inspectors, “The facility has been understaffed for a while and it’s getting worse,” according to . “It is very dangerous out here.”
Disability Rights Ohio, which has a federal mandate to monitor the facilities, in October against the department. The advocacy group, alleging abuse and neglect, asked for records of staff’s response to a Northcoast patient who suffocated from a plastic bag over their head. At the end of October, the court docket showed the parties had settled the case.
Retired sheriff’s deputy Louella Reynolds worked as a police officer at Northcoast for about five years before leaving in 2022. She said the increase in criminally charged patients meant the hospitals “absolutely” became less safe. Her hip still hurts from a patient who threw her against a cement wall.
Reynolds said officers should be able to carry weapons, which they don’t, and that more staff are needed to handle the patients. Mandatory overtime was common, she said, and often staff would report to work and not “know when we would get off.”
A Disaster That Wasn’t Averted
Back at Heartland, Heltzel requested conditional release. The judge denied the release request.
Heltzel said it was devastating. He grew up Catholic and said, “I was kind of looking for absolution.”
Now, Heltzel said he is practicing acceptance. “Acceptance is all the more important to practice when you don’t agree with something,” Heltzel said, adding, “I’m a ward of the state.”
He still hopes to be released: “I just do what I can to move forward.”
Heltzel, like Jackson, had been hospitalized before and released.
In early 2013, Heltzel said, he asked his dad to kill him. “And he refused and I did smack him,” he said. Heltzel was sent to Heartland for a short stay тАФ about 10 days, according to his mother, Jan Dyer. She recalled “begging” the hospital staff to keep him.
Heltzel said he remembers not being ready to leave: “I was still sick, and I was still delusional.” Back at home, he said, he had a “sense of existential dread, like that all this horrible stuff was going to happen.” He stopped taking his medication.
Within weeks, Heltzel killed 71-year-old Milton A. Grumbling III at his home, placing him in a chokehold and stabbing him repeatedly, according to . He beat him with a remote control and then left, taking a Bible from the home, as well as a ring. Delusional with schizophrenia, Heltzel believed that Grumbling had sexually abused him in another life, according to the records.
A family member of the man he killed told the judge in 2023 that Heltzel should “stay in prison,” according to .
In denying his conditional release, judges cited Heltzel’s failure to take medication before killing Grumbling.
Jenkins, who said she worked at a state hospital for nine years before becoming the lead advocate for NAMI Greater Cleveland, said psychiatric medications can take as long as six weeks to become fully effective.
“So clients aren’t even getting stabilized when they’re being hospitalized,” Jenkins said.
тАШHe’s Not a Throwaway Child’
In a July interview, Jackson said inconsistent care or unmedicated time in jail “worsens my symptoms.” Jackson was on the phone during a stay at a state psychiatric hospital.
Without medicine, “my head hurts, to be honest,” Jackson said, before asking to get off the phone because he was hungry. It was lunchtime. “Can you get the information from my mom?” Jackson said. “She has the records.”
After Jackson hung up the phone, Ferguson explained that “he says the food is excellent, so he does not want to miss it.” And, she added, the hospital staff had not yet seen the explosive side of her son.
In early September, after 45 days at Summit тАФ his longest stay yet at a state psychiatric hospital тАФ Jackson returned to the Montgomery County jail facing misdemeanor charges because of with staff at a Dayton behavioral health hospital. In court, Ferguson said, her son struggled to explain to the judge why he was there. On a video call from the jail days later, she saw him playing with his hair and ears.
“That tells me he’s not OK,” Ferguson said.
Before Jackson’s diagnosis more than a decade ago, Ferguson said, her son wasn’t a troublemaker. He had goals and dreams. And he’s still “loved and liked by a lot of people.”
“He’s not a throwaway child,” she said.
is a nonprofit news team covering Ohio’s criminal justice systems.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/race-and-health/criminally-ill-state-mental-psychiatric-hospitals-prisons-waitlists-ohio/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2122343&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The Trump administration, which has promised “radical transparency,” that it plans to publish the “project summary” for states that win awards. Following the lead of federal regulators, many states are withholding their complete applications, and some have refused to release any details.
“Let’s be clear,” said Alan Morgan, chief executive of the National Rural Health Association. “The hospital CEOs, the clinic administrators, the community leaders: They’re going to want to know what their states are doing.” The NRHA’s members include struggling rural hospitals and clinics, which would benefit from the Trump administration’s Rural Health Transformation Program.
Morgan said his members are interested in what states propose, which of their ideas are approved or rejected, and their budget narratives, which detail how the money could be spent.
Improving rural health care is an “insanely complicated and difficult task,” Morgan said.
The five-year Rural Health Transformation Program was approved by Congress in a law — the One Big Beautiful Bill Act — that also drastically cuts Medicaid spending, on which rural providers heavily depend. It’s being watched closely because it’s a much-needed influx of funds — with a caveat from the Trump administration that the money be spent on transformational ideas, not just to prop up ailing rural hospitals.
The law says half of the $50 billion will be divided equally among all states with an approved application. The rest will be distributed through a points-based system. Of , $12.5 billion will be allotted based on each state’s rurality. The remaining $12.5 billion will go to states that on initiatives and policies that, in part, mirror the Trump administration’s “” objectives.
Health and Human Services Secretary Robert F. Kennedy Jr. has repeatedly promised to open the government to the American people. His agency has devoted to “radical transparency.”
“We’re working to make this the most transparent HHS in its 70-year history,” in written testimony to lawmakers in September.
Lawrence Gostin, a professor of public health law at Georgetown University, said HHS is “acting in a way that utterly lacks transparency” and that the public has the right to demand “greater openness and clarity.” Without transparency, the public cannot hold HHS accountable, he said.
Centers for Medicare & Medicaid Services spokesperson Catherine Howden said the agency will follow the federal regulations when releasing information about the rural health program.
Grant applications are “not released to the public during the merit review process,” Howden said, adding, “The purpose of this policy is to protect the integrity of evaluations, applicant confidentiality, and the competitive nature of the process.”
Democrats and many health care advocates are concerned politics will affect how much money states get.
“I am very concerned about retaliation,” said Rep. Nikki Budzinski (D-Ill.). Because Democrats control her state’s politics, “our application might not be as seriously considered as other states that have Republican leadership,” she added.
Illinois’ Democratic members of the U.S. House to CMS Administrator Mehmet Oz in November asking for “full and fair consideration” of their state application. Illinois officials have not yet released their state’s proposal to ║┌┴╧│╘╣╧═Ї News, which has a pending public records request.
Heather Howard, a professor of the practice at Princeton University, said she is “pleasantly surprised at how transparent the states have been.”
Howard directs the university’s State Health and Value Strategies program, which the rural health fund, and praised most states for publicly posting their project summaries.
“To me, it speaks to the intense interest in this program,” Howard said. Her team, reviewing about two dozen state summaries, found themes including expansion of home-based and mobile services, increased use of technology, and workforce development initiatives like scholarships, signing bonuses, and child care assistance for high-demand positions.
“I think it’s exciting,” Howard said. “What’s great here is the experimentation we’re going to learn from.”
Telerobotics appeared in Georgia’s and Alabama’s applications, she said, including a proposal to use robotic equipment for remote ultrasounds.
Another theme that “warms my heart,” Howard said, was the effort among states to create advisory groups or committees, including in Idaho, where work groups are expected to focus on technology, workforce development, tribal collaboration, and behavioral health.
All 50 states submitted applications to federal regulators by the Nov. 5 deadline and awards will be announced by the end of the year, according to CMS.
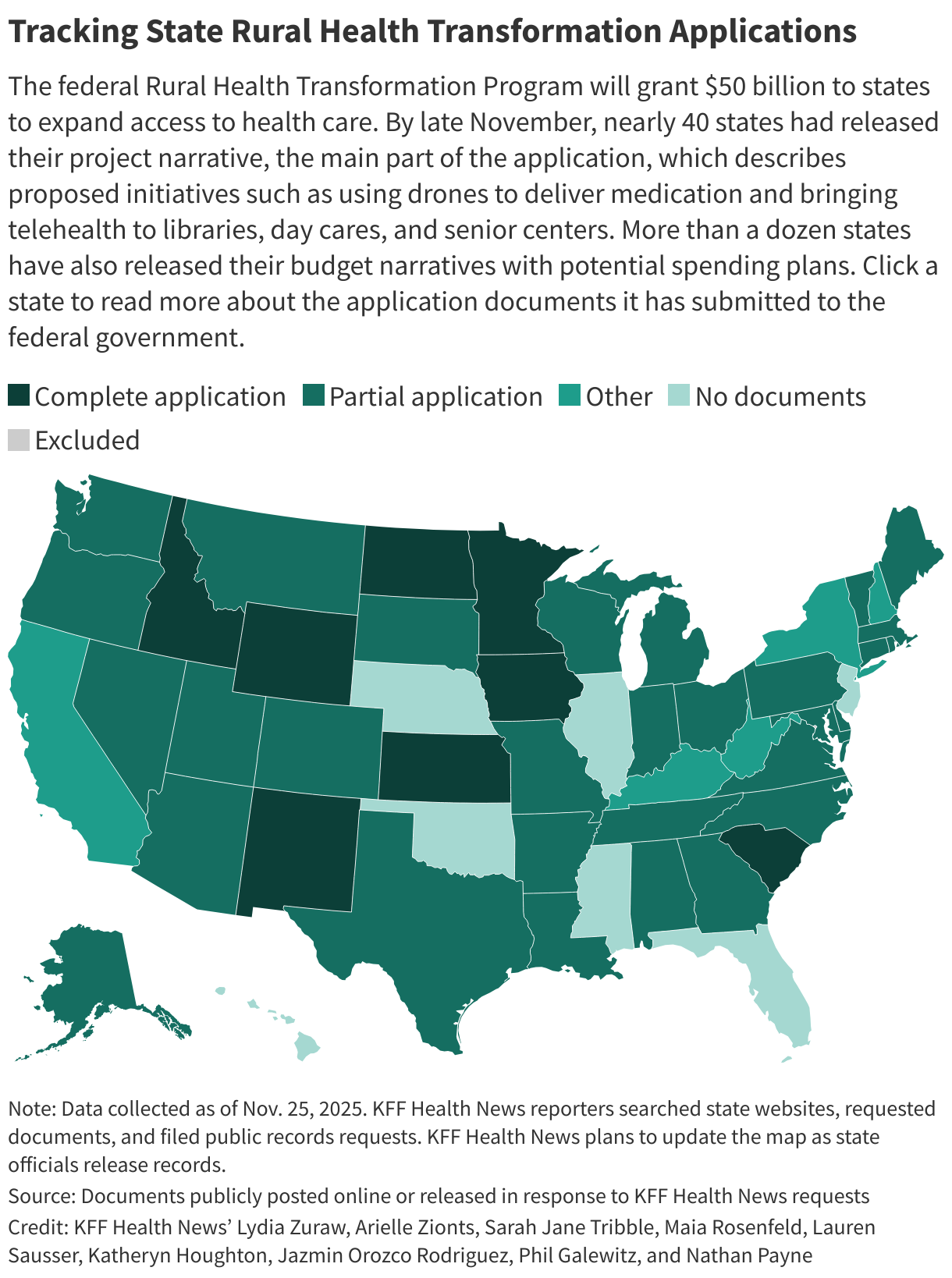
As of late November, nearly 40 states had released their project narrative, the main part of the application, which describes proposed initiatives, according to ║┌┴╧│╘╣╧═Ї News tracking. More than a dozen states have also released their budget narratives.
Also as of late November, only a handful of states — Idaho, Iowa, Kansas, Minnesota, New Mexico, North Dakota, South Carolina, and Wyoming — had released all parts of the application.
║┌┴╧│╘╣╧═Ї News filed public records requests for states’ complete applications. Some states have refused to release any of their application materials.
Nebraska, for example, rejected a public records request, saying its application materials are “proprietary or commercial information” that “would give advantage to business competitors.”
Kentucky shared its application summary but said the remainder of the application is a “preliminary draft” not subject to release under state laws.
Erika Engle, a spokesperson for Hawaii Gov. Josh Green, said the governor “is committed to transparency” but declined to share any of the state’s proposal.
Hawaii and other states are still processing formal public records requests.
The rural health program is part of the July law projected to reduce federal Medicaid spending in rural areas by 10 years.
Those cuts are expected to affect rural health facilities’ bottom lines, threatening their ability to stay open. A recent Commonwealth Fund report found that rural areas continue to to primary care. But the guidelines for the rural health program say states can use only 15% of their new funding to pay providers for patient care.
Between the Medicaid cuts and funding boost from the new program, “there’s real opportunity for national policy to impact rural, both in the negative and the positive potentially,” said Celli Horstman, a senior research associate at the New York-based policy think tank who co-authored the report.
Among the publicly available rural health transformation proposals, Democratic-leaning states show support, or are willing to adopt, some of the administration’s goals but will lose out on points from eschewing others.
For example, New Mexico said it would introduce legislation requiring students to take the Presidential Fitness Test and physicians to complete continuing education courses on nutrition. But it won’t prevent people from using their Supplemental Nutrition Assistance Program benefits to buy “non-nutritious” foods such as soda and candy.
Many states want to invest in technology, including telehealth, cybersecurity, and remote patient monitoring equipment. Other themes include increasing access to healthy food, improving emergency services, preventing and managing chronic illnesses, and enlisting community health workers and paramedics for home visits.
Specific proposals include:
- Arkansas wants to spend $5 million through its “FAITH” program — Faith-based Access, Interventions, Transportation, & Health — to enlist rural religious institutions to host education and preventive screening events. Congregations could also install walking circuits and fitness equipment.
- Alaska, which historically relied on dogsled teams to bring medication to remote areas, is looking to test the use of “unmanned aerial systems” to speed up pharmacy deliveries to such communities.
- Tennessee wants to increase access to healthy activities by spending money on parks, trails, and farmers markets.
- Maryland wants to start mobile markets and install refrigerators and freezers to improve access to fresh, healthy food that often spoils in rural areas with few grocery stores.
State Sen. Stephen Meredith, a Republican who represents part of western Kentucky, said he still expects rural hospitals to close despite his state’s rural health transformation program.
“I think we’re treating symptoms without curing the disease,” he said after listening to a presentation on Kentucky’s proposal at .
Morgan, whose organization represents rural hospitals likely to close, said the state’s ideas may sound good.
“You can craft a narrative that sounds wonderful,” he said. “But then translating the aspirational goals to a functioning program? That’s difficult.”
║┌┴╧│╘╣╧═Ї News staffers Phil Galewitz, Katheryn Houghton, Tony Leys, Jazmin Orozco Rodriguez, Maia Rosenfeld, Bram Sable-Smith, and Lauren Sausser contributed to this report.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/rural-health-transformation-program-cms-state-applications-transparency/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2123985&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The 27-year-old resident of Bloomington, Indiana, has a pacemaker and a painful joint disease. She also has fused vertebrae in her neck from a spinal injury, preventing her from turning her head.
Indiana’s Medicaid agency currently considers Brader “medically frail,” giving her access to an expanded set of benefits, such as physical therapy.
New federal rules will require more than 18 million Medicaid enrollees nationwide to show they’re working, volunteering, or going to school for 80 hours a month starting in 2027 to keep their coverage. Brader is exempt as long as she’s deemed medically frail.
But lacking sufficient federal guidance, states are wrestling with how to define medical frailty — a consequential decision that could cut Medicaid coverage for many people, said state officials, consumer advocates, and health policy researchers.
“It’s terrifying,” Brader said. “I already have fought so hard to get my health care.”
‘Incredibly High’ Stakes
President Donald Trump’s One Big Beautiful Bill Act slashes nearly $1 trillion from Medicaid over the next decade, with much of the savings projected to come from no longer covering those who don’t qualify under the new work rules. Those spending cuts help offset the costs of GOP priorities, such as extra border security and tax cuts that mainly benefit the wealthy.
Conservative lawmakers have argued that Medicaid, the government health insurance program for people with low incomes or with disabilities, has grown too large and expensive, especially in the wake of its expansion to more low-income adults under the Affordable Care Act. They also say that requiring participants to work is common sense.
The work rules in Trump’s tax-and-spending law offer exemptions for several groups who might struggle to meet them, including people deemed “medically frail.” The law spells out certain “medically frail” conditions such as blindness, disability, and substance use disorder. But it does not list many others.
Instead, the law exempts those with a “serious or complex medical condition,” a term whose interpretation could vary by state.
State officials say they need more clarity to ensure that people who cannot work for health reasons retain rightful access to Medicaid. They also worry that, even with a clear definition, people will face the onerous task of having to regularly vouch for being medically frail, which is a challenge without reliable access to medical care.
“The stakes are incredibly high,” said Kinda Serafi, a partner at consulting firm Manatt Health.
The new work requirements will affect Medicaid recipients in 42 states and Washington, D.C. Eight states — Alabama, Florida, Kansas, Mississippi, South Carolina, Tennessee, Texas, and Wyoming — did not expand their Medicaid programs to cover additional low-income adults, so they won’t have to implement the work rules.
The Medicaid work rules are expected to be the over the next decade, according to the nonpartisan Congressional Budget Office.
Forty-four percent of all adults covered by states’ expanded Medicaid programs , according to KFF.

A Challenge for States
State Medicaid agencies are scrambling to implement the rules with little direction from the U.S. Department of Health and Human Services, which has yet to issue specific guidance. Federal officials will clarify the “medically frail” definition next year, said Andrew Nixon, an agency spokesperson.
Ultimately, states will have to decide who is unhealthy enough to be exempt from work rules. And it won’t be easy for state workers and their computer systems to track.
Every year, state eligibility systems screen millions of applicants to check if they qualify for Medicaid and other government programs. Now, these same systems must screen applicants and existing enrollees to determine whether they meet the new work rules.
Jessica Kahn, a partner at consulting firm McKinsey & Co., has urged states to start planning how to adapt eligibility systems to verify work status. States can do a “tremendous amount” of work without direction from the federal government, said Kahn, a former federal Medicaid systems official, who spoke during a recent Medicaid advisory panel hearing. “Time is a-wasting already.”
State Medicaid directors are pondering the challenge.
“Medical frailty gets so complex,” Emma Sandoe, Oregon’s Medicaid director, said during a recent panel discussion. Conditions that can keep people from working, such as mental health disorders, can be hard to prove, she said.
A state might try to use data pulled from a person’s health records, for instance, to determine medical frailty. But information from a patient’s chart may not paint a clear picture of someone’s health, especially if they lack regular access to medical care.
It’s a tall order for eligibility systems that historically have not had to scrape medical records to screen applicants, said Serafi of Manatt Health.
“That is an incredibly new thing that eligibility enrollment systems are just not fluent in at all,” Serafi said.
Lobbying groups for the private health insurance companies that help run Medicaid in many states also have urged federal regulators to clearly define medical frailty so it can be applied uniformly.
In a to federal officials, the Medicaid Health Plans of America and the Association for Community Affiliated Plans advocated for allowing enrollees to qualify for the exemption by saying on their applications that they have conditions that make them medically frail. Successfully implementing exemptions for the medically frail will be “crucial” given the “severe health risks of coverage loss for these populations,” the groups said.
Some state officials worry about unintended consequences of the work rules for people with chronic conditions.

Jennifer Strohecker, who recently resigned as Utah’s Medicaid director, reiterated the high stakes, especially for those with diabetes on Medicaid. They may be very healthy and functional with insulin, but if they fail to complete the work requirements, that may change, Strohecker said during a recent Medicaid advisory hearing.
Whether someone is deemed medically frail already depends heavily on where they live.
For example, in Arkansas, people indicate on their Medicaid applications that they’re disabled, blind, or need help with daily living activities.
Approximately 6% of the roughly 221,000 people enrolled in Arkansas’ Medicaid expansion program are deemed medically frail, according to Gavin Lesnick, a spokesperson for the Arkansas Department of Human Services.
In West Virginia, the state accepts a medical frailty designation when an applicant self-reports it.
The burden of proof is higher in North Dakota. Applicants there must answer a questionnaire about their health and submit additional documentation, which may include medical chart notes and treatment plans. More than half of applicants were denied last year, according to Health and Human Services Department spokesperson Mindy Michaels.
Indiana’s Family and Social Services Administration, which runs its Medicaid program, declined an interview and said it could not comment on individual cases, like Brader’s.
Brader worries the additional red tape will cause her to lose Medicaid again. She said she was temporarily kicked off the program in 2019 for failing to meet the state’s work rules when Indiana said her work-study job didn’t count as employment.
“Anytime I have tried to receive help from the state of Indiana, it has been a bureaucratic nightmare,” she said.
As states await federal guidance, Kristi Putnam, a senior fellow at the conservative Cicero Institute and former secretary of the Arkansas Department of Human Services, which oversees the state Medicaid program, said even if a state creates an extensive list of qualifying “medically frail” conditions, the line must be drawn somewhere.
“You can’t possibly create a policy for exemptions that will catch everything,” she said.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/medicaid-work-rules-exempt-medically-frail-who-qualifies/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2120581&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Spartanburg County, in South Carolina’s Upstate region, has been fighting a measles outbreak since early October, with more than 50 cases identified. Health officials have encouraged people who are unvaccinated to get a shot by visiting its mobile vaccine clinic at any of its several stops throughout the county.
But on a Monday afternoon in Boiling Springs, only one person showed up.
“It’s progress. That progress is slow,” Linda Bell, the state epidemiologist with the Department of Public Health, said during a recent press briefing. “We had hoped to see a more robust uptake than that in our mobile health units.”
As South Carolina tries to contain its measles outbreak, public health officials across the nation are concerned that the highly contagious virus is making a major comeback. The Centers for Disease Control and Prevention has tallied and 45 outbreaks in 2025. The largest started in Texas, where hundreds of people were infected and two children died.
For the first time in more than two decades, the United States is poised to lose its measles , a designation indicating that outbreaks are rare and rapidly contained.
South Carolina’s measles outbreak isn’t yet as large as those in other states, such as , , and . But it shows how a confluence of larger national trends тАФ including historically low vaccination rates, skepticism fueled by the pandemic, misinformation, and “health freedom” ideologies proliferated by conservative politicians тАФ have put some communities at risk for the reemergence of a preventable, potentially deadly virus.
“Everyone talks about it being the canary in the coal mine because it’s the most contagious infectious disease out there,” said Josh Michaud, associate director for global and public health policy at KFF, a health information nonprofit that includes ║┌┴╧│╘╣╧═Ї News. “The logic is indisputable that we’re likely to see more outbreaks.”
Schools and тАШSmall Brush Fires’
Spartanburg’s vaccination rate is among the lowest of South Carolina’s 46 counties. And that was true “even before covid,” said Chris Lombardozzi, a senior vice president with the Spartanburg Regional Healthcare System.
Nearly 6,000 children in Spartanburg County schools last year тАФ 10% of the total enrollment тАФ either received an exemption allowing them to forgo required vaccinations or did not meet vaccine requirements, according to data published by the state.
Lombardozzi said the county’s low vaccination rate is tied to misinformation not only published on social media but also spread by “a variety of nonmedical leaders over the years.”
The pandemic made things worse. Michaud said that fear and misinformation surrounding covid vaccines “threw gasoline on the fire of people’s vaccine skepticism.” In some cases, that skepticism transferred to childhood vaccines, which historically have been less controversial, he said.
This made communities like Spartanburg County with low vaccination rates more vulnerable. “Which is why we’re seeing constant, small brush fires of measles outbreaks,” Michaud said.
In Spartanburg, the overall percentage of students with required immunizations fell from 95.1% to 90% between the 2020-21 and 2024-25 academic years. Public health officials say a minimum of 95% is required to prevent significant spread of measles.
Children who attend public and private schools in South Carolina are required to show that they’ve received some vaccinations, including the measles, mumps, and rubella vaccine, but religious exemptions are relatively easy to obtain. The exemption form must be notarized, but it does not require a doctor’s note or any disclosure about the family’s religious beliefs.
The number of students in South Carolina who have been granted religious exemptions has increased dramatically over the past decade. That’s particularly true in the Upstate region, where religious exemptions have increased sixfold from a decade ago. During the 2013-14 school year, 2,044 students in the Upstate were granted a religious exemption to the vaccine requirements, according to . By fall 2024, that number had jumped to more than 13,000.
Some schools are more exposed than others. The beginning of the South Carolina outbreak was largely linked to one public charter school, Global Academy of South Carolina, where only 17% of the 605 students enrolled during the 2024-25 school year provided documentation showing they had received their required vaccinations, according to data published by the Department of Public Health.
No one from Global Academy responded to interview requests.
тАШHealth Freedom’
In April, after visiting a Texas family whose daughter had died from measles, Health and Human Services Secretary Robert F. Kennedy Jr. wrote on social media that the “most effective way to prevent the spread of measles is the MMR vaccine.” He made a similar statement during an interview on “Dr. Phil” later that month.
But these endorsements stand at odds with other statements Kennedy has made that cast doubt on vaccine safety and have falsely linked vaccines with autism. The CDC, under his authority, now claims such links “have been ignored by health authorities.”
“What would I do if I could go back in time and I could avoid giving my children the vaccines that I gave them?” he said on a podcast in 2020. “I would do anything for that. I would pay anything to be able to do that.”
Throughout 2025, he has made other . During a congressional hearing in September, Kennedy defended his past claims that he was not anti-vaccine but affirmed his stated position that no vaccines are safe or effective.
Emily Hilliard, a spokesperson for the Department of Health and Human Services, told ║┌┴╧│╘╣╧═Ї News that Kennedy is “pro-safety, pro-transparency, and pro-accountability.” Hilliard said HHS is working with “state and local partners in South Carolina” and in other states to provide support during the measles outbreaks.
Meanwhile, Kennedy has frequently championed the idea of health freedom, or freedom of choice, regarding vaccines, a talking point that has taken root among Republicans.
That has had a “chilling effect all the way down through state and local lawmakers,” Michaud said, making some leaders hesitant to talk about the threat that the ongoing measles outbreaks poses or the effectiveness and safety of the MMR vaccine.
Brandon Charochak, a spokesperson for South Carolina Gov. Henry McMaster, said the governor was not available to be interviewed for this article but referenced McMaster’s comment from October that measles “is a dangerous disease, but in terms of diseases, it’s not one that we should panic about.”
On a separate occasion that month, the Republican governor said he does not support vaccine mandates. “We’re not going to have mandates,” he said, “and I think we are responding properly.”
Even though the South Carolina Department of Public Health has repeatedly encouraged measles vaccines, the push has been notably quieter than the agency’s covid vaccine outreach efforts.
In 2021, for example, the agency partnered with breweries throughout the state for a campaign called “Shot and a Chaser,” which rewarded people who got a covid vaccine with a free beer or soda. By contrast, the pop-up measles vaccine clinic at the Boiling Springs Library featured no flashy signage, no freebies, and wasn’t visible from the library’s main entrance.
Edward Simmer, interim director of the Department of Public Health, would not speak to ║┌┴╧│╘╣╧═Ї News about the measles outbreak. During a legislative hearing in April, Republican state lawmakers voted against his permanent confirmation because of his past support for covid vaccines and masking. One lawmaker specifically criticized the agency during that hearing for the Shot and a Chaser campaign.
Public health officials in other states also have been blocked from new roles because of their covid response. In Missouri, where among kindergartners since 2020 and measles cases have been reported this year, Republican lawmakers in 2022 after vaccine opponents protested his appointment.
In South Carolina, Simmer, lacking lawmakers’ confirmation, leads the public health agency in an interim capacity.
South Carolina Sen. Tom Davis of Beaufort was the only Republican on the Senate Medical Affairs Committee who voted to confirm Simmer in April. He told ║┌┴╧│╘╣╧═Ї News that his Republican colleagues raised valid questions about Simmer’s past support for covid vaccines.
But, Davis said, it would be “tremendously unfortunate and not beneficial from a public health perspective” if the Republican Party just took a stance against vaccines “as a matter of policy.”
The Department of Public Health had administered 44 doses of the MMR vaccine through its mobile health unit from October to mid-November. The last mobile vaccine clinic was scheduled for Nov. 24. But health officials are encouraged that patients are seeking vaccines elsewhere. The agency’s tracking system shows that providers across Spartanburg County administered more than twice as many measles vaccines in October as they did a year ago.
As of mid-November, more than 130 people remained in quarantine, most of them students at local elementary and middle schools. Cases have also been linked to a church and Greenville-Spartanburg International Airport.
“We’re reminding people that travel for the upcoming holidays increases the risk of exposures greatly,” said Bell, the state epidemiologist. “Due to that risk, we’re encouraging people to consider getting vaccinated now.”
║┌┴╧│╘╣╧═Ї News correspondent Amy Maxmen contributed to this report.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/news/measles-outbreak-south-carolina-vaccine-misinformation-kennedy-rfk/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2122955&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Kopplin, a physician assistant who works with seniors, low-income people, and mental health patients in the rural Black Hills, shared her thoughts at a meeting hosted by state officials.
South Dakota’s leaders did a “good job of diving in” and asking questions to get “deeper at the root of the problem,” she said.
Kopplin later told ║┌┴╧│╘╣╧═Ї News how one of her rural patients recently missed two appointments because of a broken-down car and no access to public transportation.
Nationwide, health care workers like Kopplin and thousands of others тАФ from patient advocates to technology executives тАФ flocked to town halls or online portals during the seven weeks state leaders had to craft and submit their applications for the Rural Health Transformation Program to the federal Centers for Medicare & Medicaid Services. That deadline was Nov. 5.
“We will give $50 billion away by the end of the year,” CMS Administrator Mehmet Oz said Nov. 6 at a Milken Institute event in Washington. He said all 50 states had submitted applications.
The program will “allow us to right-size the health care system,” Oz said, adding that innovations from the rural work “will spill over to suburban and urban America as well.”
Among applications and summaries publicly shared by states, themes include workforce development, telehealth, and access to healthy food. In Kansas, leaders want to build a “Food is Medicine” program. Wyoming officials propose a new program called “BearCare,” a state-sponsored health insurance plan that patients could use only after medical emergencies.
But many health policy experts and Democrats are raising alarms that the Republican-backed program will become a “slush fund.” Critics worry it will fail to reach the small-town patients they say need it most, especially as states face nearly a trillion dollars in Medicaid spending reductions over the next decade. Medicaid, a joint federal-state program, serves nearly rural Americans.
“The status quo is tremendous distress in rural communities,” said Heather Howard, a professor of the practice at Princeton University and director of the university’s State Health and Value Strategies program, which is tracking the rural health fund. The new funding won’t be enough to offset the Medicaid losses, she said.
Congressional Republicans added the five-year, $50 billion Rural Health Transformation Program as a last-minute sweetener to President Donald Trump’s massive tax-and-spending legislation. The move helped win support for the One Big Beautiful Bill Act from conservative holdouts who worried that the Medicaid cuts in the bill would harm rural hospitals in their states.
In Montana, which hosted an online public forum before submitting its application, a nonprofit director pitched youth peer support as a way of battling high suicide rates. A registered nurse asked state leaders to “think maybe even bigger” and consider statewide universal health care.
And in Georgia, a technology-focused chain of primary care clinics that serves seniors proposed expanding its operations into that state in its online public comment. A rural grant writer asked for “safe and stable housing.”
The law says half of the $50 billion will be divided equally among all states with an approved application. The rest will be doled out according to a points-based system. Of , $12.5 billion will be allotted based on each state’s rurality. The remaining $12.5 billion will go to states that on initiatives and policies that, in part, mirror the Trump administration’s “” objectives.
Top Senate Democrats have raised alarms about the rural health program. They include Ron Wyden of Oregon and Tina Smith of Minnesota, who a federal watchdog agency to investigate the fairness and implementation of the fund. Taylor Harvey, a Wyden aide, said the Government Accountability Office has confirmed it will investigate.
According to , no less than a quarter of states with an approved application may share the second half of the funding each fiscal year, CMS spokesperson Catherine Howden said. The agency plans to publish summaries of approved state projects, .
A handful of conservative-leaning states тАФ including Texas, Arkansas, Louisiana, and Oklahoma тАФ have already instituted regulatory and legislative initiatives, such as prohibiting “non-nutritious” foods in benefit programs, that in the program application process.
Michael Chameides, a county supervisor in rural New York, said he fears the money could “be used in ways that would hurt certain states or reward certain states.” Chameides is also the communications and policy director with the Rural Democracy Initiative, a national advocacy organization that released last month.
Edwin Park, a research professor at Georgetown University’s Center for Children and Families, said federal lawmakers gave Oz and his agency “really excessive discretion” when awarding the money.
Federal administrators have added rules that aren’t within the statute that created the program, Park said. For example, its application guidelines say states cannot use more than 15% of their funding to pay providers for patient care тАФ payments that are expected to take a hit due to the Medicaid cuts.
Georgetown’s health policy experts and Democrats aren’t the only ones with concerns. and in Ohio worry the money will go to large health systems instead of smaller, independent hospitals that serve people within their rural communities.
CMS’ Oz repeated the idea of getting “big hospitals to adopt smaller institutions” at the Washington gathering after applications were filed. He used similar language at a rural health summit hosted by South Dakota-based Sanford Health. “How do we get big hospitals to adopt smaller hospitals? Not to take them over, but to keep them viable by giving them good telehealth services, specialty support, radiology support,” he said at the October event.
Sanford owns or manages dozens of hospitals and hundreds of clinics and long-term care centers, as well as a health insurance company. The system reported about $81 million in operating income during the first six months of fiscal year 2025, according to .
Last year, Sanford opened a “command center” for its systemwide telehealth initiative. It launched a telehealth expansion in 2021 and offers virtual care for 78 medical specialties, Sanford President and CEO Bill Gassen said.
“We’ve tried to imagine, what if that number doubles?” Gassen said. The startup costs for telehealth are high, he said, and the rural fund could be a unique opportunity “for us to make virtual care available to more patients, to more communities, to more hospitals and health systems across the country.”
Gassen, who is set to chair the American Hospital Association in 2027, said Sanford leaders have met with state and federal officials, including Oz, whom he’s known for years, and Chris Klomp, a top deputy at CMS and a senior adviser to Health and Human Services Secretary Robert F. Kennedy Jr.
The word “telehealth” appears 36 times in the rural health program’s 124-page application guidelines. But Don Robbins Jr., chief executive of a small hospital on the Illinois-Kentucky border, chuckled at the idea of using the funding for that purpose.
Robbins, whose 25-bed Massac Memorial Hospital averages five to seven patients in its beds each day, said his hospital does not regularly offer telehealth. Even if it did, he said, patients living more than a mile outside of town couldn’t use it because they don’t have a good internet connection.
The small hospital reported a $31,314 loss in September, Robbins said. “I think if we get anything out of it,” Robbins said of the rural health program, “we’ll be lucky.”
Kopplin, the physician assistant who attended the South Dakota meeting, is cautiously optimistic about the rural health fund. She views it as a wonderful chance for states to test out ideas and learn from what works and what doesn’t.
But “in a lot of ways this bill is going to be a band-aid approach” for rural health, she said. “It’s not really going to fix the problem.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/states-competing-rural-health-transformation-program-cms/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2113931&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Bre Dolan, a 35-year-old resident of Hardy County, West Virginia, understands why. Throughout her childhood, when her dad had addiction and mental health crises, police officers were often the first ones to respond. Dolan calls them “good men and women” who “care about seeing their community recover.”
But she’s skeptical that they can mitigate the root causes of an addiction epidemic that has racked her home state for decades.
“Most of the busts that go down are addicts,” she said тАФ people who need treatment, not prison.
Dolan’s father was one of them. And so was she.
Now 14 years into recovery, she’s been surprised to see many local officials spending opioid settlement money тАФ an influx of cash from companies accused of fueling the overdose crisis тАФ on police Tasers, cruisers, night vision gear, and more.
“How is that really tackling an issue?” Dolan said. “How will it help families battling addiction?”

Nationwide, more than $61 million in opioid settlement funds were spent on law enforcement-related efforts in 2024, according to a yearlong investigation by ║┌┴╧│╘╣╧═Ї News and researchers at the Johns Hopkins Bloomberg School of Public Health and Shatterproof, a national nonprofit focused on addiction. That included initiatives that public health experts largely support, such as hiring social workers to accompany officers on overdose calls, as well as actions they’re more skeptical of, such as beefing up police arsenals.
Over nearly two decades, state and local governments are set to receive in opioid settlement money, which is intended to be used to fight addiction. The settlement agreements even and established other guardrails to limit unrelated uses of the funds тАФ as the Tobacco Master Settlement Agreement of the 1990s.
But there’s still significant flexibility with these dollars, and what constitutes a good use to one person can be deemed waste by another.
To , an addiction medicine doctor who was once addicted to opioids and has served as an expert in several opioid lawsuits, some law enforcement expenses fall into that second category.
and are not “in the spirit of what we wanted to use the money for when we were fighting for it,” Loyd said.
“People died for this money. Families were torn apart for this money. And to not spend it to try to make our system better, so that people don’t have to experience those losses going forward, to me, is unconscionable,” he said.
As part of this investigation, ║┌┴╧│╘╣╧═Ї News and its partners compiled the most comprehensive national database of opioid settlement spending to date, featuring more than 10,500 examples of how the money was used (or not) last year. The team filed public records requests, scoured government websites, and extracted expenditures, which were then , such as treatment or prevention. The findings include:
- Nearly $2.7 billion тАФ that’s the amount states and localities spent or committed in 2024, according to public records. The lion’s share went to investments addiction experts consider crucial, including about $615 million to treatment, $279 million to overdose reversal medications and related training, and $227 million to housing-related programs for people with substance use disorders.
- Smaller, though notable, amounts funded law enforcement initiatives тАФ such as creating a shooting range and tinting patrol car windows тАФ and prevention programs that experts called questionable, such as putting on a fishing tournament.
- Some jurisdictions paid for basic government services, such as firefighter salaries.
- The money is controlled by different entities in each state, and about 20% of it is untrackable through public records.
This year’s database, including the expenditures and untrackable percentages, should not be compared with the one ║┌┴╧│╘╣╧═Ї News and its partners , due to and state budget quirks. The database cannot present a full picture because some jurisdictions don’t publish reports or delineate spending by year. What’s shown is a snapshot of 2024 and does not account for decisions in 2025.
Still, the database helps counteract the in charge of settlement money among those .
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/opioid-settlements-law-enforcement-spending-states-towns-guns-narcan/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2102815&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
