Urgent Care Stepping Up or Michigan Legislature Falling Short?
Kate Wells’ report on Michigan’s Upper Peninsula reveals an important gap between constitutional protections and real-world access to care (“Urgent Care Clinics Move To Fill Abortion Care Gaps in Rural Areas,” April 8). But the story leaves a critical question unanswered: Can urgent care centers bear this weight?
Rural communities were already stretched thin before clinics, such as Planned Parenthood, closed amid ongoing funding cuts and shifting political landscapes. By 2030, the National Rural Health Association anticipates a reduction in rural physicians by nearly 25%, and rural doctors already report burnout at far higher rates than other occupations. Rural patients also travel farther distances to reach care, a burden that’s only growing as clinics disappear.
Urgent care centers absorb whomever shows up, often patients who have fewer nearby options. The addition of abortion services to an already strained, under-resourced setting risks inflating patient volume and shortchanging people who need more time and specialized support than a quick appointment allows.
Marquette Medical Urgent Care deserves credit for stepping up. But individual clinics should not be expected to fix a systemic failure alone.
Michigan’s constitutional amendment protecting abortion rights means little if it cannot be exercised in full across the entire state. The Michigan Legislature must commission a formal audit to ensure equitable provision and funding of reproductive health services across counties.
A right that exists on paper but not in practice is not a right at all.
тАФ Cecily Jones; Baltimore
I just finished listening (twice!) to Kate Wells’ excellent segment on NPR Morning Edition regarding the urgent care facility in Michigan taking on the role of reproductive health clinic after other clinics in the area had closed. Thank you for putting a spotlight on the very real consequences of the decisions being made regarding reproductive health and abortion and the overall issue of access to medicine for rural communities.
I live in an area that has total access to all medicine, so I do not think people understand how these decisions impact other parts of the country. Your story did a great job of highlighting the disparity. I appreciated the doctor who spoke candidly about her personal beliefs versus her medical doctor obligations. And special thanks to the brave woman who allowed you to follow her journey through that clinic. Both of their comments were powerful and meaningful additions that demonstrate the complexity of each issue you touched on.
Thank you so much for this important and impactful segment. I appreciated it so much that I tracked you down to say so!
тАФ Denise Minuti; Centreville, Delaware
Silicosis Hits Close to Home
Silicosis is not just an occupational hazard (“As Lung Disease Threatens Workers, Lawmakers Seek Protections for Countertop Manufacturers,” March 12). My husband and I live next door to a now-completed (we think) sand-mining operation, where the property owner digs sand to sell. There are numerous sand mine operations going on here in Carver, Massachusetts, as well as in Wareham and Plymouth.
Every day, from 2011 to 2024, our property was covered in silica sand and/or sand. If we opened our door to go out, we’d end up with a coating of silica dust on everything in our home. We could not comprehend how dangerous breathing in the dust was. Well, my husband was diagnosed with silicosis recently. I, too, have the silica dust and nodules in my lungs and have received a preliminary diagnosis of “restrictive lung disease consistent with silicosis.”
I have been referred to a specialist, as I also have severe rheumatoid arthritis, which may have been caused by breathing in the silica dust (according to an ).
Our hometown has the best sand in the world. The property owners are making millions from selling it.
тАФ Josephine Beadling; Carver, Massachusetts
The Tangled Web of Medical Debt
This responds to the recent ║┌┴╧│╘╣╧═Ї News-CT Mirror article on medical debt lawsuits filed by physicians and other non-hospital providers in Connecticut (“In Connecticut, Doctors Now Sue Patients Most Over Medical Bills, Surpassing Hospitals,” April 20). The patient stories are difficult and deserve attention. No physician wants to see patients struggle financially, nor does anyone enter medicine intending to take legal action against them.
What’s missing is how we got here.
Over the past decade, insurers have expanded high-deductible health plans, shifting thousands of dollars in upfront costs onto patients. As a result, physicians provide care, incur real costs, and must increasingly collect payment directly from patients rather than insurers тАФ effectively becoming bill collectors for costs that insurers defer.
This dynamic strains the physician-patient relationship. Patients delay care due to cost, and clinical time is diverted to payment issues. Trust erodes when financial concerns intertwine with care.
Meanwhile, physician practices face rising overhead тАФ staffing, technology, compliance, and high malpractice premiums. Government reimbursement compounds the strain: Connecticut Medicaid rates are among the lowest in the region, and Medicare payments have not kept pace with inflation. Practices rely heavily on commercial insurance to remain viable.
At the same time, large insurers report substantial profits while promoting plans that shift more financial responsibility onto patients and physicians.
When bills go unpaid, practices have limited options. Care has already been delivered, and costs incurred. Financial viability is essential to maintaining access to care.
Medical debt is a serious problem, but focusing blame on physicians misses the root cause. Policymakers should address high-deductible plan design, restore meaningful coverage at the point of care, and return responsibility for cost structures to insurers. Until then, both patients and physicians will continue to bear the consequences.
тАФ Mariam Hakim-Zargar, president of the Connecticut State Medical Society; Avon, Connecticut
How Organ Donor Registration Really Works
The article “Lost in Transmission: Changes in Organ Donor Status Can Fall Through Cracks in the System” (March 17) misrepresents the United States’ opt-in organ donation system, thereby undermining public trust in donation and ultimately reducing the number of lives donation and transplant professionals can save.
The article is based on an inaccurate premise: When someone who has previously registered as a donor moves to a new state and does not register as an organ donor, that should be treated as a revocation of their intent to donate. This does not align with how the system is designed or governed.
The U.S. framework for organ donation is designed to respect each person’s right to decide whether they want to donate their organs and tissues once they pass away. It operates on express consent, meaning a person must take affirmative action to opt in. In the same vein, a person would have to take action to remove that authorization. It is never presumed.
The decision to donate is legally binding тАФ just like a will or advance directive тАФ and protected by the .
By proposing a non-response equals a revocation, the article could also be interpreted to suggest organ procurement organizations, or OPOs, have overruled the individual autonomies of organ donors and their families. That is not true either. As nonprofits overseen by the federal government, OPOs must uphold the UAGA and act in accordance with each donor’s legal decision.
Journalists play an in any system built on public trust, especially the organ donation system. When news outlets publish inaccurate or incomplete information, it can discourage Americans from considering donation. Conversely, clear and accurate representation of organ donation helps drive system improvements and encourages more people to save lives as donors.
тАФ Jeffrey Trageser, president of the Association of Organ Procurement Organizations; San Diego
Clamp Down on the Use of Chatbots
On April 17, you reported on the growing use of artificial intelligence chatbots as substitutes for mental health care (“Your New Therapist: Chatty, Leaky, and Hardly Human”). This trend is deeply concerning because these tools are being marketed as “therapy” despite lacking clinical evidence, regulation, and accountability.
As a public health student, I see this not just as a technological issue, but as a public health risk. Many individuals turn to these platforms because they are more accessible and affordable than traditional care. However, what people don’t realize is that these apps can provide misleading, unverified, and even harmful advice while collecting highly sensitive personal data with little oversight.
One thing that would really make a difference is stronger federal regulation of AI-based mental health tools. Clear standards for safety, transparency, and data privacy are urgently needed to ensure that vulnerable users are not misled into believing they are receiving legitimate care.
Without action, these tools risk worsening the very mental health crisis they claim to address.
тАФ Joyce Truong; San Francisco
Reporting on Long Covid Holds Up
Your reporting captured what long-covid patients have been telling Congress for years: $1.15 billion in federal research dollars has not produced a single approved treatment (“Long-Covid Patients Are Frustrated That Federal Research Hasn’t Found New Treatments,” Jan. 22, 2025). What the piece left room to explore is the cost of that inaction, and what the alternative looks like on paper.
The National Institutes of Health’s Researching COVID to Enhance Recovery (RECOVER) Initiative , engaging over 33,000 participants across 400-plus study sites and producing 131 peer-reviewed papers that established long covid as a measurable, multisystem condition with immune dysfunction and viral persistence. While clinical trials have shown mixed results тАФ modest cognitive improvements from brain training but no benefit from heart rate medications тАФ this prevents ineffective treatments from reaching patients and focuses resources on promising pathways. The challenge is translating this scientific foundation into approved therapies.
On March 15, 2026, Long Covid Awareness Day, I delivered a to the Senate HELP (Health, Education, Labor & Pensions) Committee. The model is built on 112 peer-reviewed sources and complies with the Office of Management and Budget’s guidelines. Against a $5.19 billion federal investment over three years, it projects a 4.59-to-1 federal fiscal benefit-cost ratio and an 8.38-to-1 social welfare benefit-cost ratio.
In April 2026, the independently validated the model architecture in its of long covid’s economic burden through 2035. Both analyses, developed separately, : Productivity and workforce losses are the dominant economic burden, and that burden is persistent, not temporary. The OECD projects $135 billion annually across OECD nations; mine provides the U.S. specific measurement that the OECD acknowledged it could not produce for this country.
These figures are not advocacy. They are what standard federal economic analysis returns when the inputs include 19.4 million disabled adults, lost labor force participation, cascading Medicaid and Social Security Disability Insurance costs, and the cardiovascular, cognitive, and autonomic sequelae your reporting has documented elsewhere. The provides the implementation road map.
Patients like Erica Hayes, profiled in your piece, are not a rounding error. They are a fiscal signal the federal government has chosen not to read. ║┌┴╧│╘╣╧═Ї News is positioned to cover what a fully scored federal response would cost, and what it would return. The numbers are on the table.
тАФ Marty Pack; Spokane, Washington
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/letter-to-the-editor/urgent-care-abortion-organ-donors-chatbots-medical-debt-april-2026/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2228677&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
║┌┴╧│╘╣╧═Ї News Michigan correspondent Kate Wells discussed urgent care clinics offering abortions on Apple News Today on April 15.
║┌┴╧│╘╣╧═Ї News Montana correspondent Katheryn Houghton discussed doula Medicaid reimbursements on Montana Public Radio on April 9.
- Read Houghton’s “This Northern Cheyenne Doula Was About To Start Getting Paid тАФ Then Medicaid Cuts Hit.”
║┌┴╧│╘╣╧═Ї News contributor Michelle Andrews discussed farm bureau health plans on The Yonder Report on April 8.
- Read Andrews’ “Farm Bureau Health Plans Beat the ACA on Prices With an Age-Old Tactic: Rejecting Sick People.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .
This <a target="_blank" href="/on-air/on-air-april-18-2026-urgent-care-abortion-doulas-farm-bureau-health-plans/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2183401&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>MARQUETTE, Mich. тАФ Providing abortions was the last thing Shawn Brown thought she’d be doing when she opened an urgent care clinic in this remote town in Michigan’s Upper Peninsula.
But she also wasn’t expecting the Planned Parenthood in Marquette to shut down last spring. Roughly 1,100 patients relied on that clinic each year for cancer screenings, IUD insertions, and medication abortions. Now the area has no other in-person resource for abortions. “It’s a 500-mile stretch of no access,” Brown said.
So the doctor, who describes herself as “individually pro-life,” added medication abortions to Marquette Medical Urgent Care’s already busy practice, which treats a steady flow of kids with the flu, college students with migraines, and tourists with skiing injuries.
At least 38 abortion clinics shut down last year in states where they’re still legal, according to data collected by , a project supported by a number of nonprofits that helps people find abortion options. Even states that recently protecting abortion rights, such as Michigan, have had clinics close since the U.S. Supreme Court overturned Roe v. Wade in 2022. And as shutter , patients are losing access to pregnancy care. “You cannot have a high-risk pregnancy up here,” Brown said. “It’s a scary place.”
Now communities are coming up with alternatives, such as Brown’s urgent care.
The idea that urgent cares “could be an untapped solution to closures for abortion clinics across the country is really exciting,” said Kimi Chernoby, the chief operating and legal officer at , a national nonprofit that works to improve professional training and patient outcomes for women in emergency medicine.
One patient at the Marquette urgent care on a recent day was a woman whom ║┌┴╧│╘╣╧═Ї News agreed to identify by only her first initial, “A,” to protect her medical privacy. She drove more than an hour on snowy backroads while her kids were in day care to get to her appointment.
Her youngest is still a baby, A said, and she got pregnant again while taking the progestin-only birth control pill, which is less likely to interfere with breast milk production but slightly less effective than the regular pill.
“Financials, housing, vehicles тАФ it’s a lot,” she said. And another baby is “just not something that we could really do even at this time.”
She said she was making the long round trip because receiving abortion care in an office felt more secure than being treated by “someone that I’ve never met, or receiving meds that were just shipped to me.”

Face-to-Face Care
In one of the urgent care’s exam rooms, A sat in a chair against the wall, waiting quietly for the doctor. Viktoria Koskenoja, an emergency medicine physician, knocked on the door and then greeted her warmly, pulling up a stool across from her.
“Are you confident in your decision that you want to go ahead? Or do you want to talk about options?” she said.
“No, I’m pretty set on it,” A said.
Koskenoja previously worked at Planned Parenthood. When she learned its Marquette clinic was closing, she started crying and making calls. She recalled asking everyone she knew in health care in Marquette: “What are we going to do?”
One of her first calls was to Brown, a friend and fellow emergency medicine doctor. Their families harvest maple syrup together each spring.
In the wake of the Planned Parenthood closure, Koskenoja convened a community meeting downtown at the Women’s Federated Clubhouse, an 1880s-era building where guests sip from gold-rimmed china teacups on lace tablecloths. The goal: brainstorm new ways to provide abortion access in the Upper Peninsula.
officials said that growing financial challenges and the Trump administration’s cuts to funding, including for the public insurance program Medicaid, had prompted the closures of some brick-and-mortar clinics in the state.
Plus, the availability of pills by mail exploded after the 2022 Dobbs v. Jackson Women’s Health Organization decision overturned Roe. As abortion became illegal in many states, telehealth abortions went from 5% of all abortions provided to 25% by the end of 2024, , a national reporting project that tracks shifts in abortion volume.
Planned Parenthood of Michigan’s telehealth appointments increased 13% for patients in the Upper Peninsula after the Marquette location closed, said Paula Thornton Greear, president and CEO of Planned Parenthood in the state.
All the abortion patients Koskenoja sees at the urgent care have one thing in common: They want to talk to someone in person.
“I had a patient order the pills online and then get scared to use them because they felt like they were going to screw it up, or they weren’t sure they could rely on the pills,” she said. “So they literally came in here with the pills in their hand.”
Others have medical complications or need an ultrasound to determine how far along they are with the pregnancy.
“It annoys me that telehealth is considered an acceptable thing in rural areas,” Koskenoja said. “As though we’re not the human beings that like talking to human beings and looking someone in the eye, especially when something serious is going on.”


The Urgent Care Option
The options presented at that community clubhouse meeting were limited. The few family medicine doctors and OB-GYNs in the area were either already putting patients on months-long waitlists or were too “rightward leaning,” Brown said.
But urgent cares are designed to fill gaps in the system, she said, ready to take walk-ins who aren’t already patients.
Brown knew from her years in the emergency room that medication abortions aren’t that complicated. The for first-trimester and are essentially the same: one dose of mifepristone, followed by misoprostol after 24 to 48 hours.
“Clinically, I was never worried about it,” she said.
The biggest hurdle was getting medical malpractice insurance, Brown said. At first, insurers balked, demanding “onerous and unrealistic” documentation and additional training, she said. Then they quoted a $60,000 annual premium for medication abortions тАФ about three times the cost of insuring the entire urgent care. Ultimately, Brown said, the urgent care’s broker pushed back, providing data that medication abortions didn’t add “significant liability.”
The company agreed to a premium of about $6,000 per year, she said.
The community pitched in, too. A local donor covered an ultrasound machine. And supporters started a nonprofit to help pay for the costs of the medication and additional staffing, bringing the price for patients down from about $450 to an average of about $225, based on a sliding scale.
Word spread quickly once Marquette Medical began offering medication abortions, Brown said. Now the office provides as many as four per week, with patients traveling from as far away as Louisiana. The clinic is on track to match the volume of abortion patients treated at the local Planned Parenthood office before its closure, Brown said.
As pills by mail become the next major target for abortion opponents, Chernoby said, it will be critical to offer more care in more brick-and-mortar places. Brown said the Marquette clinic has already fielded questions from a large academic medical center that plans to start providing medication abortion at its own urgent cares later this year.
“It’s a wonderful idea, but it’s potentially got major pitfalls,” said David Cohen, a professor at the Drexel University Kline School of Law who studies abortion access.
Urgent cares that provide medication abortion would have to abide by state-specific laws тАФ some mandate 24-hour waiting periods or facility structural requirements тАФ and federal regulations, such as the FDA’s requirement that mifepristone prescribers be certified by the drug’s distributors and obtain signed patient agreements.
If abortion access isn’t a core part of a health organization’s mission, “do you want to be on that list? I don’t know if you do,” Cohen said. “There’s just a very particular regulatory environment” around abortion.

Making a Choice
In the exam room, Koskenoja listened as A talked about why she decided to seek an abortion. She has four kids at home, including the baby.
“You OK if we do an ultrasound, just confirm how far along you are, make sure it’s not an ectopic pregnancy?” Koskenoja asked.
“Yeah,” A said.
Koskenoja noted A’s reaction to the question. “OK. You’re making a face?”
“Yeah, I just don’t тАФ yeah, it’s fine. I just don’t want to see it.”
“Oh, you don’t have to see it,” Koskenoja said.
“I just don’t want to hear a heartbeat or anything like that,” A said.
“Definitely not,” Koskenoja said.
After the ultrasound, Koskenoja stepped out into the hall to give A time to call her partner.
When A said she was ready, Koskenoja stepped in and asked her how she was feeling. A had made up her mind. She said that her partner would be supportive of whatever she decided and that she didn’t want to have another baby right now.
“As much as I know this baby would be loved no matter what, it’s just not a good time,” A said quietly, her hands in her lap.
“Most people who get abortions love babies,” Koskenoja said. And you can still have more in the future, she assured A.
This kicked off a long conversation about the mental load of parenting and the pros and cons of various birth control options. A said she wanted to get her tubes tied, but Koskenoja suggested her partner consider a vasectomy instead. It’s a much less invasive procedure, she said. “You’ve had a lot of kids. I feel like it could be his turn to take some responsibility.”
Koskenoja handed her a small, handsewn “comfort bag” that all medication abortion patients receive. It was filled with the pills, reminders about when to take them, a handwritten note of support from local community members, pain meds, comfortable socks, and a heating pad.
“Call us if you need anything,” she told A. “Any questions?”
“No,” A said.
“OK. Good luck,” Koskenoja said before A walked out past the waiting room, filled with sick babies and other patients, to drive back to her kids.
This <a target="_blank" href="/health-care-costs/abortion-providers-clinics-closing-urgent-care-michigan-upper-peninsula/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2174428&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Raven’s case reveals a little-known gap in the U.S. donation system: There is no clear, nationally binding way to opt out тАФ or to ensure a later “no” overrides an earlier “yes” in a different state.
This gap, along with a range of other issues related to the organ procurement system, has become a point of bipartisan congressional concern. Late last year, the House Ways and Means subcommittee on oversight examining what members described as shortcomings, including alleged consent failures.
The panel’s scrutiny of organ procurement organizations, or OPOs, and their consent practices is a first step toward a more meaningful accountability plan that could help maintain trust across the system, according to some committee staff members.
The trust in our organ procurement and transplant system “has been eroded,” said Rep. Terri Sewell of Alabama, the panel’s senior Democrat, calling for stronger transparency and oversight to rebuild public confidence.
“Respect for autonomy тАФ our ability to make our own decisions (self-determination) тАФ allows for both тАШyes’ and тАШno’ decisions and for changing one’s mind,” Margaret McLean, a bioethicist at Santa Clara University, said in an email.
“Medical decision-making is not well served in a context of ambiguity,” she said.
And if a donor revokes consent, she added, “revocation by that person should carry the same ethical and procedural weight as the initial authorization, perhaps more.”
Raven Kinser Changed Her Mind
Raven was 25 when she died. Her parents, Jeff and Jaime Kinser, were at home in Michigan when they received the phone call that shattered their world. They drove through the night to the Newport News hospital, where they learned Raven’s disposition had been referred to LifeNet Health, the region’s federally designated OPO. LifeNet a failing OPO by the Centers for Medicare & Medicaid Services, meaning it doesn’t meet the government’s standards for how well it finds donors and recovers usable organs for transplant compared with other organizations.
Under federal law, hospitals are required to refer deaths and imminent deaths to OPOs, which take responsibility for donation-related decisions and discussions.
OPOs occupy a hybrid position in the health care system, as private nonprofit entities that hold exclusive, federally authorized contracts to recover organs within defined regions. They are regulated by CMS and overseen by the Health Resources and Services Administration, but that oversight occurs primarily through certification standards, performance metrics, and periodic audits rather than routine public disclosure requirements. With donor registries largely managed at the state level and no unified federal reporting requirement for removals, comprehensive national data on revocations is elusive.
OPOs are meant to separate bedside care from organ procurement decisions тАФ to help prevent conflicts of interest and preserve the trust that decisions about life-sustaining treatment are made solely in the dying patient’s interest. But the , leaving families unsure who is in control if and when conflicts arise.
The Kinsers, for instance, felt their daughter would not have wanted to go through the donation process, but, at the time, had no evidence. Jaime remembers telling her husband that Raven would have been mad at them for letting it happen. In an effort to stop it, Jaime inquired about whether she would be asked to sign a consent form. But a LifeNet staff member told her that wasn’t an option because donation was Raven’s “living will,” Jaime said. Meanwhile, Raven’s parents said, her personal effects, including her Virginia driver’s license, which bore no donor designation, had not yet been turned over to the family, leaving them no meaningful way to challenge LifeNet’s determination in real time.
Jaime struggled with this outcome, even mentioning in Raven’s obituary that she was an organ donor. “How would you try to make peace with something that you felt was so wrong but had no proof?” Jaime said.
Two months passed before the Kinsers gained possession of the license, which, as they had expected, showed that Raven had not opted to be an organ donor.
According to the Kinsers, LifeNet staff told them that Raven’s status as a registered donor was established by her designation on her older Michigan license.
An emailed statement attributed to Douglas Wilson, LifeNet executive vice president, said the OPO follows federal law on organ donation, the , and queries applicable state donor registries, relying on time stamps and governing law to determine the , legally valid expression of intent. Under that framework, a prior donor authorization remains enforceable unless a valid revocation is recorded in the regional OPO’s donor registry.
Because of privacy laws, Wilson said, LifeNet could not comment on the specifics of any individual case.
Raven Kinser’s choice not to be a donor when she applied for a Virginia license in July 2024 was not reflected in the registry LifeNet consulted, according to her parents, who said that is what the organization told them. According to Lara Malbon, executive director of Donate Life Virginia, which manages the state’s organ donor registry, if someone changes their donor status while completing a Virginia driver’s license or ID transaction, “that information is sent to our registry, and the registry is updated daily to reflect those changes.” Malbon also said Virginia’s registry includes only people who have “affirmatively said тАШyes’ to becoming an organ, eye, and tissue donor, and it retains records solely for those who have made that decision.”
The Kinsers said they were never told why Raven’s Virginia DMV record was insufficient, or how an older yes from Michigan could outweigh a newer no in Virginia.
In December, the Kinsers filed a complaint with the Health Resources and Services Administration, urging federal regulators to investigate LifeNet’s actions and require OPOs to provide families with documented proof of the donor’s current status at the time of referral. They also called for OPOs, which operate as federally designated regional monopolies but are structured as private nonprofits, to be made subject to public records laws.
When Opting Out Doesn’t Stick
Such confusion is not unique to the Kinser family. It is a consequence of the organ donation consent process in the United States.
“I have also wondered that: why there’s not just one” registry for organ donation, Jaime said. If you go to get a firearm, you have one federal registry, she said.
Here’s how the system works: Americans typically register their organ donation intentions when they apply for driver’s licenses through state DMVs, and that decision remains governed largely by state law. That has led to 50 different sets of rules and very little federal regulation of what has become an in the U.S.
In some states, a donor checkbox is a binding legal document. In other states, the same choice may have different rules about when it takes effect, what it covers, and how it can be revoked.
Those differences can be big. State rules determine whether a person’s “gift” is limited to transplantation or also includes research and education. They determine whether the donation authorization includes tissue. And they can determine what counts as a valid revocation and when it is legally recognized.
Because of the system’s fragmentation, though, signals can cross when someone changes their mind, like Raven; it’s not always reflected from one state system to another.
Under state versions of the Uniform Anatomical Gift Act, a donor’s most recent legally valid expression of intent is meant to control.
“Personal autonomy is paramount to everything,” said Adam Schiavi, a neurointensivist who studies end-of-life decision-making. “If I say I want to be a donor, or if I say I don’t want to be a donor, that has to take precedence over everything else.”
But states differ in how revocation must be recorded and which registry is considered authoritative if someone has lived in more than one state. Those inconsistencies can create uncertainty when records conflict across jurisdictions.
“It has to be the most recent expression, not the most recent yes,” Schiavi said.
In Michigan, a change to someone’s donor status is reflected immediately in the secretary of state’s system, but only affirmative “yes” registrations appear in the registry. Removal information remains in internal motor vehicle records. In Virginia, the state registry includes only those who have affirmatively said “yes,” retaining records solely of donors, creating potential gaps if someone believes a DMV change alone is sufficient.
Elsewhere, processes and volumes differ sharply. New Mexico updates driver records in real time but does not transmit status changes to its donor registry. Instead, donor services receive restricted search access. The state logged nearly 15,000 removals in late 2021 and almost 30,000 in 2022. Florida, which maintains formal removal records through weekly DMV data files, reported 356,161 removals in 2020, more than 1.5 million in 2023, and over 1.2 million in 2025. Kentucky processed 847,371 donor registrations from 2020 to 2025, but only 16,043 icon removals, with registry withdrawal handled separately. In 2025, more than 570,000 Texans opted into the registry, while over 31,000 individuals requested removal.
According to a federal official who asked not to be identified for fear of professional repercussions, OPOs have been highly effective at lobbying states to broaden the definition of consent and authorization тАФ shaping how those terms are applied, whether those statuses must be renewed, and how easy or difficult it is for someone to opt out.
In subsequent correspondence with federal officials, the Kinsers have urged reforms to prevent OPOs from relying on older registry entries when a more recent state DMV record exists, and they have called for criminal penalties in cases in which consent is knowingly misrepresented. Federal regulators have not indicated whether such proposals are under consideration.
Congress Takes a Closer Look
Ethicists have long cautioned that consent must be more than a checkbox and must remain grounded in respect for the donor-patient. In an October on organ transplantation, the American College of Physicians emphasized that clinicians’ primary duty is to the patient in their care, and that maintaining trust requires transparency and safeguards to prevent conflicts of interest from blurring that “bright line.”
Advocates say those steps leave unresolved the core problem raised by the Kinser family: the lack of a clear, legally binding way for people to say “no” and for that decision to follow them across state lines.
The said it “supports strengthening donor registries and enhancing registry interoperability to ensure that an individual’s documented donation decision is honored.” But OPOs have also argued that current policies protect donation as a legally enforceable gift and prevent families from overriding a loved one’s “yes” in the midst of grief. They argue that stronger, more durable consent helps reduce missed donations and saves lives.
Congress and federal regulators are considering changes to the nation’s organ donation system, including how consent is recorded and what should happen when a donor changes their mind.
Sen. Ron Wyden (D-Ore.) last year to create new federal standards for patient safety, transparency, and oversight of organ transplants, including a formal authorization for hospital or OPO staff to pause harvesting if there is any “clinical sign of life.”
HHS press secretary Emily Hilliard said the agency is “committed to holding organ procurement organizations accountable” and to “restoring integrity and transparency” to organ donation policy, calling reforms essential to informed consent and protecting donor rights. CMS issued related March 11, but it does not address the problems highlighted by the Kinsers’ case.
Critics of the organ transplant system say it is difficult for families to obtain documentation or independently verify how consent determinations were made in disputed cases.
HRSA has launched a sweeping modernization of the Organ Procurement and Transplantation Network, the national system that oversees organ allocation and transplant policy. Federal officials have described the overhaul as the most significant restructuring of the transplant system in decades, aimed at breaking up a long-standing contractor monopoly, strengthening patient safety oversight, and replacing aging technology infrastructure.
Central to that effort is modernizing the OPTN’s data systems: improving interoperability, audit trails, and transparency in how decisions are documented and reviewed. A more modern federal data architecture could make it easier to trace which registry was queried, what time stamp controlled, and how a consent determination was reached in disputed donations that span multiple states. But the modernization effort would not change the underlying state-by-state legal framework for donor authorization and what counts as a valid “no.”
Meanwhile, Donate Life America, a national nonprofit that supports state donor registries, also runs the , a central database that allows people to sign up as organ donors directly. Unlike many DMV systems, the national registry lets people log in at any time to view, update, or remove their registration and print proof of their decision. The group is also starting a project to let participating states send registrations directly into the national system, creating one place to track donor sign-ups and removals across state lines.
Each of the proposals comes with trade-offs, and both advocates and OPOs have raised concerns about how they would work in practice.
“Just doing a dump truck dump of information is not going to do much unless you really apply it through checking and auditing,” said Arthur Caplan, a professor of bioethics at New York University’s Grossman School of Medicine. “It could be like the IRS. They don’t have to audit everybody. Just do a spot audit once in a while.”
The Kinsers aren’t opposed to organ donation itself. They celebrated Raven’s donation in her obituary, and in their complaint to federal regulators, they wrote, “We are NOT anti-organ donation, and we will never take away the gift of life our oldest daughter gave to others. However, that was not LifeNet’s choice to make.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/organ-donor-state-registries-consent-authorization-optn-opo-raven-kinser-virginia/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2167503&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Lingering pain from a car crash two months ago, on top of an already hardscrabble life, has Angulo worried about her pregnancy. So, she was relieved when a mobile street medicine van from St. John’s Community Health pulled up near her encampment last month.
“Thank God that we have them,” she said.
, which operates 28 clinics, mostly in L.A. County, is part of the nation’s network of nonprofit community clinics that care for the poorest Americans. Around 80% of its 144,000 patients, including Angulo, have Medi-Cal, California’s version of the Medicaid program for people with low incomes or disabilities.
But federal cuts to Medicaid spending under the Republican-passed One Big Beautiful Bill Act, compounded by in Sacramento, could cost St. John’s up to one-third of its $240 million annual revenue, requiring cuts to services that might include street medicine, said Jim Mangia, the president and CEO.
Smaller, more cash-strapped clinics in L.A. County could face harsher consequences, including closure, if the lost funding is not replaced.
That’s why Mangia, along with a coalition of community clinics, health care workers, and advocates, is pushing for a five-year, in the nation’s most populous county to help backfill the projected loss of federal and state dollars. St. John’s has contributed at least $2 million to the campaign so far.

Louise McCarthy, president and CEO of the Community Clinic Association of Los Angeles County, said there aren’t a lot of options to save the health care system from disaster.
“Our backs are up against the wall,” she said. “This has the potential to be a game changer. It will be an absolutely significant offset to the losses.”
The L.A. County Board of Supervisors last month for inclusion on the June 2 primary ballot, over the objection of some cities within the county. Their leaders argued the tax would put a strain on consumers and business owners. Most of an in annual revenue generated would be used to protect safety-net health care at community clinics, hospitals, and schools.
Scrambling To Stay Afloat
Nationally, the GOP budget law is expected to cut federal Medicaid spending by over 10 years, and it could lead to an increase of in the number of people left uninsured. The L.A. ballot proposal is among many local and state initiatives nationwide, as clinics, hospitals, health care workers, advocates, and legislators scramble for new money to help offset the spending cuts.
In Michigan, where the federal law is projected to cost the state , Democratic Gov. Gretchen Whitmer’s office has proposed on tobacco, vape products, online gambling, sports betting, and digital advertising, which it projects would raise hundreds of millions of dollars annually.
In Rhode Island, a group of state legislators hopes to ease some of the pain caused by the federal cuts with a that includes a tax on digital ads and a 3% surcharge on taxable incomes above roughly $640,000.
“The goal is not to replace the revenue; it’s to mitigate the damage,” said Democratic state Rep. Brandon Potter, one of the legislators involved.
In Washington, Democratic state Rep. Shaun Scott recently introduced legislation to address the loss of federal dollars with on large companies, applied to employee salaries exceeding $125,000 a year.
In California, the GOP law will slash the to Medi-Cal by an a year, or 25%. Enrollment in Medi-Cal could by 2028 as a result of the federal and state spending cuts, according to an analysis by the UCLA Center for Health Policy Research and the University of California-Berkeley Labor Center.
In July, California will slash Medi-Cal payments that community clinics receive for certain services provided to patients with “unsatisfactory” immigration status by about . Those patients include permanent residents in the country for less than five years, refugees, asylees, and other lawfully present people.

Bracing for a тАШNew Reality’?
Advocates and health care experts say finding new revenue is the only way to avoid a crisis in California’s health care system.
“Are we going to let the gaps created by federal policies and state budget cuts leave millions of people uninsured?” said Laurel Lucia, deputy executive director of programs at the UC Berkeley Labor Center. “I think a lot of that question comes down to revenues.”
Some medical professionals say that new revenue is needed in the short term but that the country needs to address its notoriously expensive health care system.
“This new reality is that we have to do our work with less money going into the future,” said Hector Flores, of the Los Angeles County Medical Association. “So, this is an opportunity for us to look at how we can do things better.”
In the meantime, efforts to raise taxes for health care abound.
Voters in Santa Clara County, home to Silicon Valley, last November approved a five-year 0.625% to offset federal Medicaid cuts. A will be on the June ballot in Contra Costa County.
The best-known initiative, and a hotly contested one, is a union-sponsored ballot proposal in California for a on the state’s . Democratic Gov. Gavin Newsom strongly opposes it; Sen. Bernie Sanders (I-Vt.) stumped for it in California recently and has a national version in Congress.
Proponents of the temporary wealth tax say it would raise , which would mostly be used to backfill lost federal and state dollars in Medi-Cal and other safety-net programs. Proponents are trying to collect nearly 875,000 signatures needed to get it on the November ballot.
“We are on the precipice of a collapse of our health care system. So the most fortunate among us pay a modest tax that will hold us over and allow us to figure out a long-term solution,” said Suzanne Jimenez, chief of staff for Service Employees International Union-United Healthcare Workers West, the measure’s chief sponsor. “They would still be incredibly wealthy after that.”
Billionaires Push Back
The plan has stirred considerable controversy, not just in the Golden State but nationwide, and has generated strong and others.
Critics argue the measure could prompt billionaires to leave California, putting a damper on innovation, jobs, and tax receipts. And, some warn, the measure could end up in a legal quagmire, as those deemed liable to pony up challenge it on multiple fronts.
“If this passed, you would expect it to be tied up in court for some time,” said Jared Walczak, a visiting fellow at the California Tax Foundation. “It is fairly plausible that no revenue could come in for a number of years, if there’s ever any revenue at all.”
The prospect of such complications has led some health care advocates to focus instead on local initiatives that could start generating revenue more quickly, such as the proposed sales tax in L.A. County.
That one has critics too, including leaders of multiple cities within the county who to reject a proposal they argued would add to the affordability worries of consumers and put a strain on businesses.
Kathryn Barger, a Republican and the only L.A. County supervisor to oppose putting the measure on the June ballot, said in a statement that the proposed tax would make the county “less affordable for families and less appealing for consumers to shop and businesses to operate.”
But supporters say safety-net health care is already feeling the impact of diminished funding. Last month, for example, L.A. County’s Department of Public Health announced it was due to $50 million in federal, state, and local funding cuts.
Medi-Cal enrollees are worried, too. “We get a lot of calls from panicked patients afraid they’re going to lose their Medi-Cal. Dozens of calls a day, hundreds of calls a week,” said St. John’s Mangia.
“We tell them that we’re working on a solution and hopefully we’ll have that solution come June.”

This <a target="_blank" href="/health-industry/federal-cuts-state-tax-increases-budget-shortfalls-health-clinics-los-angeles-california/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2166003&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But plans to spend those nine-digit awards aren’t all warmly received.
At least one group of Republican state lawmakers appears to have scuttled an initiative preapproved by federal officials. And at least one hospital association persuaded its state health leaders to alter who greenlights spending. Other critics are taking a more cautious approach.
That’s because the Centers for Medicare & Medicaid Services, which manages the five-year Rural Health Transformation Program, says states could lose money if they make major changes to the plans approved in their applications. Changes could also delay states’ ability to get projects rolling in time to show the agency that they’re meeting progress deadlines.
“During the application period, states were advised to only propose initiatives and state policy actions that the state deemed feasible,” said CMS spokesperson Catherine Howden, who noted that the agency will work with states case by case.
The recent pushback reflects “tension” over state plans тАФ which were approved by the federal government тАФ from state lawmakers and health leaders who want more input amid tight deadlines, said Carrie Cochran-McClain, chief policy officer of the National Rural Health Association, the largest organization representing rural hospitals and clinics.
Cochran-McClain said many states must pass a bill to allow federal dollars to be spent and added that because the program rolled out so quickly “there’s important work that still needs to be done in some states between the legislatures and the governors.”
State lawmakers want to have a say, she said, in “how the funding is being allocated тАФ how the implementation will go.”
Congressional Republicans created the program as a last-minute sweetener to include in their One Big Beautiful Bill Act, signed into law last summer. The funding was intended to offset concerns about the anticipated in rural communities from the law, which is expected to slash Medicaid spending by nearly $1 trillion over a decade.
CMS officials announced first-year funding тАФ ranging from $147 million for New Jersey to $281 million for Texas тАФ on Dec. 29, after scoring applications. Federal officials will begin evaluating progress in late summer and announce 2027 allocations at the end of October.
A chorus of critics say the program won’t make up for harm caused by Medicaid cuts.
The program is “a complete sham,” Sen. Ron Wyden (D-Ore.) said at a rural policy conference in February.
Medicaid, a joint federal-state program for low-income and disabled Americans, serves nearly , and many rural hospitals depend on it to stay afloat.
But the rural health program tilts toward seeding innovative projects and technologies, not shoring up rural hospital finances. States can use only up to 15% of their funding to pay providers for patient care.
That hasn’t stopped some federal officials and lawmakers from framing the program as a rural hospital rescue.
For example, the White House , “President Trump secured $50 billion in funding for rural hospitals.”
Now that applications have been approved, some state Republican lawmakers тАФ who are than Democrats are тАФ and hospital associations are upset that the political rhetoric doesn’t match what they see.
They’re also lobbing criticisms at specific aspects of their states’ plans, including the proposed projects, what’s not included, and the spending approval process.
In Wyoming, lawmakers didn’t just criticize an initiative from their state’s application. They moved to kill it.
State Rep. John Bear, a Republican, said he and other lawmakers declined to fund “BearCare,” a proposed state-sponsored health insurance plan that patients could use only after medical emergencies. But they did approve other aspects of the rural health program.
The Wyoming Department of Health won’t “proceed with BearCare without express legislative authority to do so,” said spokesperson Lindsay Mills.
While Wyoming lawmakers removed an initiative from their state’s rural health plan, a group in Ohio wants to add something.
Ohio Rep. Kellie Deeter and other Republican lawmakers to use the maximum allowed funding for provider payments тАФ 15% тАФ to support 13 independent, rural hospitals.
“We understand that the rural transformation fund is not designed to be given directly to prop up hospitals,” Deeter said. “We just want to capitalize on the mechanism of the fund that can be utilized for that purpose.”
Those hospitals “operate with very, very narrow margins, and it’s just difficult and, frankly, unsustainable,” she added.
Ken Gordon, a press secretary responding for the governor’s office and the state health department, said, “It’s still very early in this process, and many details are being worked out.”
State lawmakers around the country are also trying to ensure the federal program’s dollars benefit rural areas.
In North Dakota, Rep. Bill Tveit, a Republican who lives in a town with about 2,000 residents, that would have required the state to reserve its funding for programs located more than 35 miles from urban areas and small cities.
During a hearing, lawmakers appeared sympathetic to Tveit’s concerns but quickly shot down his idea.
State Sen. Brad Bekkedahl said the North Dakota health department already committed to prioritizing funding for the most pressing rural health needs. He also said he’s concerned any significant changes could cause the state to lose funding because CMS already reviewed and approved the plan.
Meanwhile, Republican lawmakers in Michigan and North Carolina have criticized their states’ definitions of “partially rural” or “rural,” saying that counties that include urban population centers could take money from lower-density counties, according to and .
Lawmakers aren’t the only ones speaking out.
The Colorado Hospital Association to state lawmakers denouncing how the state created its plan and two of its proposed initiatives.
“Not only were Colorado’s rural hospitals’ recommendations disregarded,” president and CEO Jeff Tieman wrote, but the plan includes ideas “they actively oppose and believe will harm the communities they serve.”
The department responded to one of the association’s concerns by adding rural health leaders to the .
Meanwhile, and Nebraska, some health groups are upset that their states’ plans lack specific funding streams for rural hospitals.
Lauren LaPine-Ray, who oversees rural health policy at the Michigan Health & Hospital Association, predicted the state’s rural hospitals will compete with other organizations, such as academic centers and health clinics, for funding. She said about 65% of the group’s rural members have never applied for a state grant before.
“The rural hospitals, the ones that really need the funding the most, will not be well equipped to apply for and pull down these dollars,” LaPine-Ray said.
Jed Hansen, executive director of the Nebraska Rural Health Association, said the federal funding won’t go to “rural hospitals, rural clinics, and rural providers in a meaningful way.”
“Rural Health Transformation will not save a single hospital in our state,” he said. “I don’t think it will save a hospital nationally.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/rural-transformation-fund-lawmakers-health-groups-resist-state-spending-plans/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2161929&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>That’s the case in New Orleans, where an investigation by Verite News found high lead levels in about half of the playgrounds on city property and found in most homes that tested their drinking water in a voluntary program.
No level of lead exposure is safe, according to federal environmental officials, but undertaking a comprehensive cleanup can be financially prohibitive. New Orleans is facing a $220 million budget deficit that has led to city employee furloughs and layoffs.
Congress allocated $15 billion over five years to lead pipe replacement under the Bipartisan Infrastructure Law, a Biden-era measure set to expire at the end of this year. In 2024, the Environmental Protection Agency also tightened the standards for lead-contaminated soil for the first time in 30 years and mandated that water systems by late 2037.
But passed by Congress and signed by President Donald Trump in January redirected $125 million of that lead remediation money to wildfire prevention. And since October, the EPA has partially rolled back protections against soil contamination, raising the federal hazard level in urban areas and the threshold for removing contaminated soil.
Tom Neltner, the national director of the nonprofit advocacy group Unleaded Kids, said it was the first time an administration had loosened the limits on lead in soil.
“тАКWe’ve seen the Trump administration say positive things about its commitment to lead but then take actions that undermine that,” Neltner said.
But, he added, progress is still being made in some communities.
EPA press secretary Brigit Hirsch said the changes made under the Trump administration have reduced confusion and uncertainty that could hamper cleanup efforts.
“The Trump EPA’s record on protecting Americans тАФ especially American children тАФ from lead is unmatched,” Hirsch said in an emailed statement. “In just the last year, the Trump EPA backed up its commitment to reducing lead exposure in children with BILLIONS of dollars and historic action.”
She cited a of $3 billion available to pay for water pipe replacement. That money is from the passed during the Biden administration.
Verite News spoke with people in Michigan, Indiana, and Rhode Island to learn how they addressed their lead pollution, with the aim of finding options that could be applied in New Orleans and other cities.
“тАКWe don’t need to do research on lead anymore,” said Tulane University professor Felicia Rabito, an epidemiologist who researches the toxic metal and its sources. “What we need are policies to get the lead out of the environment.”

Benton Harbor, Michigan: Lead Pipes Begone
Benton Harbor, a predominantly Black beach town of about 9,000 people on the southeastern shore of Lake Michigan, spent three years out of compliance with federal drinking water standards. The concentration of lead in the water remained dangerously high until residents and organizations petitioned the EPA in 2021, drawing responses from state and federal officials.
“Nobody should be drinking lead in their water for this long,” said Elin Betanzo, an engineer who provided the petitioning residents with technical support.
That year, federal officials issued an for the Michigan city to bring its water supply into compliance, and the state required Benton Harbor to replace all its lead pipes within 18 months. Gov. Gretchen Whitmer, a Democrat, committed to securing funding in the state budget for the $35 million effort, which included bottled water distribution and paying outstanding water bills for low-income residents. The state, alongside the city, allocated money from its general fund, secured regional water loans, and cobbled together grants from several federal programs to cover the total.
By the end of 2023, city officials had completed the project. Now it’s one of 21 municipalities in Michigan that have replaced all their lead pipes. Benton Harbor had more than 4,500 pipes to replace.
The Trump administration has said it would defend the Biden-era mandate for lead pipe replacement by 2037 against a lawsuit challenging it.
Betanzo recommended that utilities in other cities reduce barriers to line replacement to increase efficiency, as Benton Harbor’s water system did.
City officials saved time after assuming most pipes would be lead. They decided to go street by street, digging up, inspecting, and replacing nearly every pipe. If the pipe wasn’t lead, it wasn’t replaced, but nearly all were, Betanzo said.
Concentrating the mass replacement in one zone at a time made the contracts more cost-effective, Betanzo added. Contractors bid on zones in the city, and multiple contractors worked in different neighborhoods simultaneously. For transparency, progress was published on a public database.
The city also passed a law requiring lead lines be replaced, including those on customers’ side of the water meter. All residents had to allow the contractors onto their property or face disconnection. The residents didn’t pay for the line replacements.
“тАКThe health benefits of lead service line replacement are greatest the sooner you get it done,” Betanzo noted, referencing a she co-authored. “If you do it wrong, you can absolutely increase exposure to lead through a lead service line replacement.”
Completion of full pipe replacement is rare in the U.S., because of the cost, poor service line tracking, the time it takes, and the prioritization of other issues. In New Orleans, the process could require up to $1 billion of investment over 10 years, according to the city’s Sewerage and Water Board.

Indianapolis: Safe Dirt for Kids
It’s not just lead pipes that are problematic. In 2024, a in the academic journal GeoHealth estimated that nearly a quarter of homes in the U.S. have unsafe levels of lead in the soil on their properties.
To that end, Indianapolis has taken some actions that other cities can learn from, said Gabriel Filippelli, a professor at the Indiana University-Indianapolis School of Science who led the study and has researched the risk of lead exposure through soil for years.
The Indy Parks & Recreation department partnered with Filippelli’s team to test a dozen parks relatively close to the contaminated site of a shuttered lead smelter.
Out of all the parks tested, Filippelli’s team found only one hot spot, beneath an old bench from which lead-based paint had flaked off into the surrounding soil.
The parks department followed Filippelli’s suggestion to replace the bench and add concrete and a thick layer of mulch and plants on the ground, so kids wouldn’t be able to play directly in the contaminated dirt.
“It was a relatively low-cost intervention,” he said, estimating it cost a few thousand dollars. The ground wasn’t excavated, and new dirt wasn’t brought in. “If you deal with it by dilution and by capping, remove the source, you’re solving the problem for today and probably many, many years to come.”
The contaminated dirt may need to be removed in some cases and replaced with clean soil, such as after severe, widespread pollution from industrial sources. But Filippelli said such extensive remediation can be impractical and too expensive for cities to undertake on their own.
Where full remediation is cost-prohibitive, Filippelli said, there are more creative solutions, like landscaping, covering the area with new dirt, or mulching. These methods won’t eliminate the lead entirely, but they will significantly reduce exposure risk.
“You can eliminate the hazard at a fraction of the cost,” he said.
Cities could also look to New York City’s , which places uncontaminated soil left over from construction projects in neighborhood-level banks for volunteers to distribute, he said.
Rhode Island: Stopping Lead at the Source
New England, home to some of the nation’s oldest homes, has led the U.S. in mitigating one of the largest ongoing sources of lead contamination: paint.
In 2023, the state legislature in Rhode Island, where most of the homes were built before lead paint was banned in 1978, passed strengthening the state’s ability to enforce tenant protections.
Prior to 2023, the state had long required most landlords to have their property inspected to ensure it met “lead safe” guidelines, said DeeAnn Guo, a community organizer for the . Although no level of lead is considered safe, replacing windows and doors that have lead paint, painting over all interior and exterior walls, and mitigating contaminated soil significantly reduce the risk of exposure.
But for years “there was no incentive to do it,” Guo said, “aside from it being the right thing to do.”
Now, landlords can be fined if they don’t have an active lead certificate on file for homes built before 1978, and the property has to be inspected every two years to remain in compliance. Before the new law, less than 15% of rentals were certified. In late 2025, that had increased to 40%, Guo said.
The state has also seen a steady decline in the in children’s blood.
Guo said it helps that the state has federal funding from the Department of Housing and Urban Development to subsidize its If a homeowner or landlord owns an old house, they can apply for the state to send an inspector. If lead is found, the state will then send a certified contractor to address the problem at little to no cost to the property owner.
Rhode Island prioritizes low-income households and homes with pregnant women or children under 6 years old, because of the heightened health risk. It can also help pay to remediate homes if a child living there has elevated levels of lead in their blood.
States and communities looking to start a successful lead paint abatement program using HUD money should combine strong enforcement, public education, and offers of subsidies, Guo said. It also helps to include community members in the planning process, she said.
Under the Trump administration, however, it might become harder for more communities like New Orleans to receive money for a “lead safe” program. Last year, HUD asked Congress to eliminate new funding for its lead hazards program, stating it would be restored in 2027. But advocates for more lead protections argue that once funding is lost, it is unlikely to be approved again.
“It shows the White House’s hypocrisy, where they talk about lead as being important and then propose eliminating the funds that are essential to cleaning up affordable housing,” said Neltner, the Unleaded Kids director. “This administration talks about the importance of children and then seems to be careless about children’s brains.”
This article was produced in collaboration with . The four-month investigation was supported by a Kozik Environmental Justice Reporting grant funded by the National Press Foundation and the National Press Club Journalism Institute. It was also produced as a project for the USC Annenberg Center for Health Journalism’s National Fellowship fund and Dennis A. Hunt Fund for Health Journalism.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/lead-pipes-soil-cleanup-new-orleans-benton-harbor-michigan-indianapolis-rhode-island/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2162403&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The legislation introduced in , , , , , , , and builds on efforts made in other states in past years. This latest push for patient protections comes as the Trump administration has backed away from federal debt protections, health care has become , and more people are expected to go without medical coverage or but riskier high-deductible insurance plans that could lead them into debt.
“In the wealthiest country on Earth, people are going bankrupt, suffering wage garnishment, just because they get sick,” said Colorado state Rep. , a Democrat who introduced legislation on Feb. 19 that would, among other measures, ban wage garnishment for medical debt.
That legislation is under consideration after a ║┌┴╧│╘╣╧═Ї News investigation found that courts approved wage garnishment requests in an estimated 14,000 medical debt cases a year in Colorado. The investigation also showed that it isn’t just urban hospitals or big health care chains allowing their patients’ wages to be garnished. It’s also small rural hospitals, physician groups, and public ambulance services, among other medical care providers. And the reporting showed that wage garnishment can erroneously target patients. For example, one family lost wages тАФ and subsequently power to their home, because they couldn’t pay their electric bill тАФ after an ambulance company incorrectly billed the family instead of Medicaid.
Wage garnishment is one tool creditors can use in most states to recoup money from people with unpaid bills. In many states, they can garnish someone’s bank account or put a lien on their home, too. To garnish a person’s wages, a creditor must typically get permission from a court to make the person’s employer hand over a piece of the debtor’s earnings.
“The creditor is taking the money directly out of somebody’s paycheck, and so it doesn’t leave people with any choice to say, тАШI need to prioritize food for my children,’” said , legal and policy director for the National Center for Access to Justice. The center, based at Fordham Law School, and the District of Columbia on how fair their laws are to consumers who get sued over debt.
It is legal to garnish patients’ wages for medical debt in all but a , according to the Commonwealth Fund, a nonprofit foundation based in New York focused on health care.
Now, lawmakers in additional states seek to ban the practice entirely. Others want to limit it by exempting debtors whose household income falls under a certain threshold or by upping the amount of earnings immune from garnishment.
Such policies on wage garnishment fit into a larger push around the country to address the effect of medical debt on people’s lives and finances. Those efforts include barring medical debt from credit reports, prohibiting liens on people’s homes, capping interest rates, and limiting the ability to file lawsuits against people with low incomes over unpaid medical bills.
Debt collectors have fought against such measures, arguing they don’t solve the problem of health care affordability and hurt the ability of medical providers to continue to provide care.
“The wage garnishment process is already highly regulated at the federal and state level and includes many consumer protection measures,” said Scott Purcell, chief executive of , an association of credit and collection professionals.
Even before the Colorado legislation was introduced, BC Services warning its clients that the legislation “poses an existential threat,” especially to rural health providers. And Bridget Frazier, a spokesperson for the , said Feb. 20 that the bill “could drive up costs and financial risk for health care providers, making it harder to keep hospitals sustainable and ensuring Coloradans have access to care when they need it most.”
The pending Colorado measure would ban wage garnishment for all patients. It also would limit bank garnishments, in which a patient’s financial institution must hand over a chunk of the money in the person’s account. Additionally, among other things, it would prevent payment plans from exceeding 4% of weekly net income, require creditors to check whether uninsured patients are eligible for public health insurance before collecting, bar creditors from collecting on bills that are more than three years old, and leave medical care providers liable to the patient for at least $3,000 if collectors don’t comply.
“No one is saying, тАШDon’t get paid for your services.’ We’re saying getting health care should not lead to financial ruin for people,” said Dana Kennedy, co-executive director at the Denver-based , a health advocacy group that has been working with lawmakers on the Colorado measure.
Kennedy said that ║┌┴╧│╘╣╧═Ї News’ investigation drove home how many kinds of Colorado health care facilities are willing to let this collection practice happen to their patients, and that the people whose wages are being garnished are often working at Family Dollar, Walmart, Amazon, or gas stations and restaurants.
“Medical debt is typically different from other forms of indebtedness,” said Colorado state Sen. , a Democrat co-sponsoring the legislation. “You could choose to keep driving your old car or buy a new one and take on debt for that. You could upgrade your home. You could buy consumer appliances. There’s not usually that voluntary element in a health care context.”
, a senior attorney with the National Consumer Law Center, said broad laws that don’t require patients to jump through hoops to access protections are the most likely to be effective. Because of that, she and other consumer advocates prefer state policies that get rid of wage garnishment for all debtors and all types of debt.
“It can be hard to identify medical debt as medical debt,” Carter said. “For example, if you have a medical debt and you put it on your credit card, it’s not going to be easy for a court system to identify that debt as medical debt.”
She said another reason is that complexity is the enemy of effectiveness. Carter pointed to a showing that even though people in the state can keep $10,000 in their bank accounts safe from garnishment, few consumers take advantage of the protection. They must know the protection exists, know where to find the relevant form, get the form notarized, file it, and mail copies to creditors. The same report found that garnishments can also be burdensome for employers, who must process garnishments and can find themselves in court if they make an error.
Jones, at the National Center for Access to Justice, said outlawing wage garnishment fully, rather than limiting it, has other benefits. “It’s also to protect people’s jobs, because in most states, if somebody has two or more orders of garnishment, they can lose their job for it,” she said.
Still, some lawmakers are pushing for the intermediate route. In Washington state, Democratic state Sen. is spearheading legislation to rope off a larger portion of low-wage earnings from garnishment. So, for example, a person making $1,000 a week would be able to keep their whole paycheck, as opposed to the $800 that the law would currently protect.
Mindy Chumbley, owner of a Washington-based collections company and an ACA International board member, testified against the bill on Feb. 2. “Washington has made sweeping changes to medical debt policy year after year without pausing to study the cumulative impact,” she told lawmakers. “Our clients are reporting clinic closures, urgent care centers shutting down, staffing shortages, and rural facilities struggling to stay open.”
The Washington State Hospital Association said it is neutral on the legislation. The American Hospital Association said it does not take positions on state policies.
Liias told ║┌┴╧│╘╣╧═Ї News that lawmakers need to ensure health care providers can recoup their costs while also protecting patients. “We don’t want families either to be driven into bankruptcy or to be driven into under-the-table work to avoid these garnishment thresholds,” he said.
Liias said his measure follows the lead of Arizona, which passed similar consumer protections in 2022. “Obviously, the health care system is still functioning in Arizona, and folks are able to make it work.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/medical-debt-wage-garnishment-state-legislation-patient-protection/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2154960&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But there are strings attached.
In late December, President Donald Trump’s administration announced how much all 50 states would get under its new Rural Health Transformation Program, assigning them to use the money to fix systemic problems that leave rural Americans without access to good health care. Now, the clock is ticking.
Within eight months, states must submit revised budgets, begin spending, and show the money is going to good use. Federal officials will begin reviewing state progress in late summer and announce 2027 funding levels by the end of October.
The money — divided into unique allocations for each state, ranging from $147 million for New Jersey to $281 million for Texas — represents the first $10 billion installment from the five-year, $50 billion program. Congress created the fund as a last-minute sweetener in Trump’s One Big Beautiful Bill Act last summer to offset the anticipated in rural communities from the statute’s nearly $1 trillion in Medicaid spending cuts over the next decade.
Federal officials crafted the fund to give states “space to be creative,” Mehmet Oz, administrator of the Centers for Medicare & Medicaid Services, said on a call with reporters after announcing the funding Dec. 29. “Some states will fail, and we will learn from that.”
The money was divided according to a complicated formula.
In 2026, each state will receive an equal $100 million share for the first half of the money, plus additional funding from the second half. Oz’s staff steered payouts from the second portion based on each state’s rural score, as well as results from a “technical” scoring system for project proposals.
Within hours of the announcement, academics and researchers began to parse the awards to better understand why some states received more than others, including whether the awards reflected any partisanship or political favoritism.
At first glance, total awards do not appear to favor states governed by either Republicans or Democrats. But teased out the amount awarded for each state’s technical score, which is the part determined by the discretion of agency officials.
The analysis was performed at the University of North Carolina’s Cecil G. Sheps Center for Health Services Research, which specializes in rural health. A ║┌┴╧│╘╣╧═Ї News review of the Sheps Center data found that states with Republican governors tended to receive more money for the parts of their application based on the technical score. Democratic-controlled states crowded the bottom quarter of those technical score awards.
Overall, though, the state awards reveal wild variation in how much money each state will get per rural resident, almost a hundredfold difference between the top and bottom.
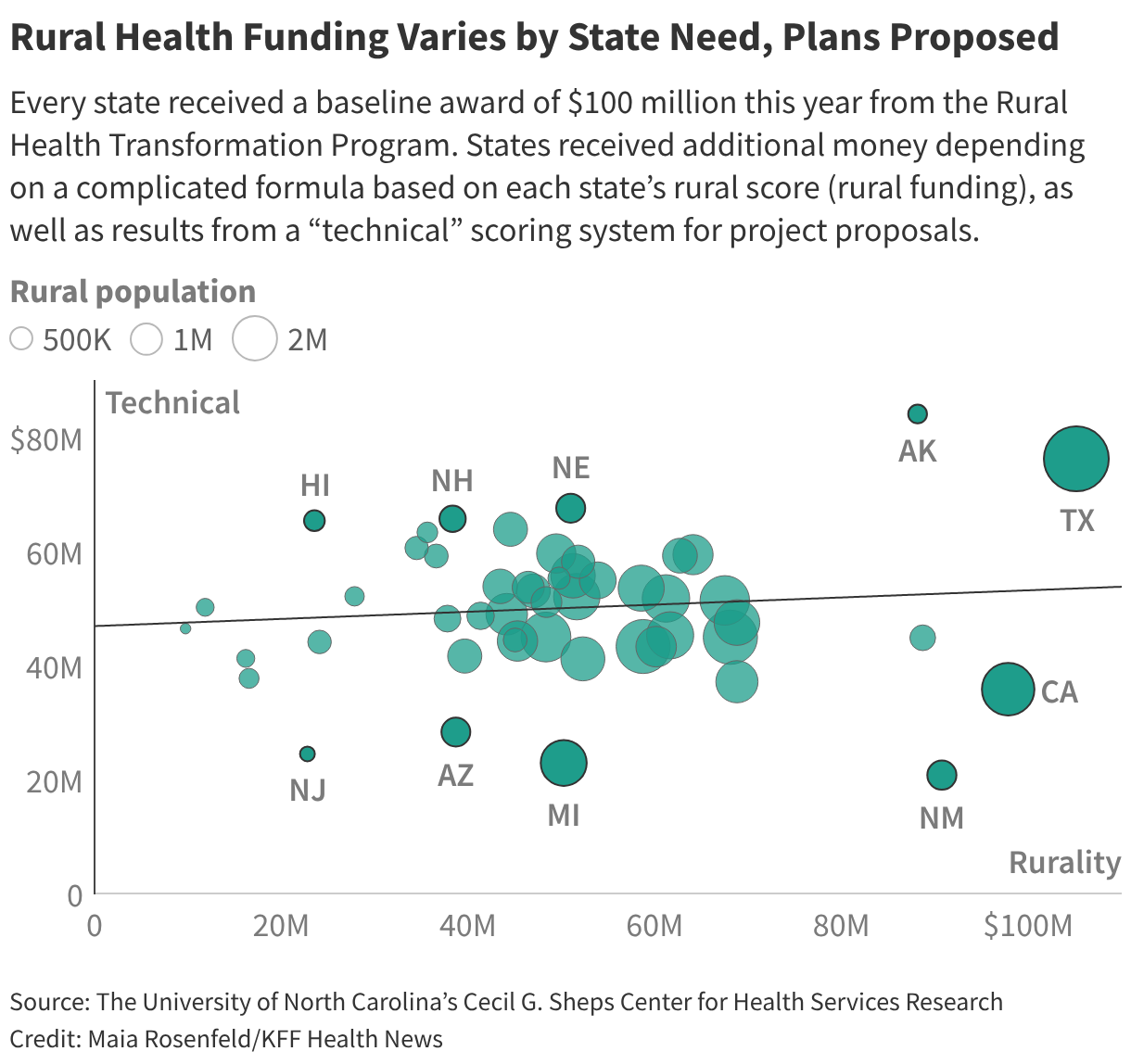
In an emailed statement to , a spokesperson for Arizona’s Democratic Gov. Katie Hobbs accused the administration of shortchanging rural residents in the state, which was awarded $167 million this year from the program.
CMS spokesperson Chris Krepich said in an emailed statement to ║┌┴╧│╘╣╧═Ї News that “politics played no role in funding decisions.”
On the December call, Oz pushed states to start working on policy actions championed by the administration — such as approving presidential fitness tests and restricting food benefits — that could require legislative approval.
Half of states promised to mandate the presidential fitness test, Oz said. Many states also proposed food waivers under the Supplemental Nutrition Assistance Program, known as SNAP, which would limit low-nutrition items such as soda. He also said some states promised to teach health care professionals about nutrition. And others confirmed they will repeal certificate-of-need laws, which require companies to prove that new health facilities they want to open are necessary.
Krepich said CMS’ new Office of Rural Health Transformation is hiring program officers to serve as point people for three or four states. Many states are setting up their own offices to oversee the new funding.
Oz highlighted Alabama’s “big maternity initiative with robotics doing ultrasounds” and said states are tackling issues ranging from behavioral health to obesity.
A ║┌┴╧│╘╣╧═Ї News review of state “” and “” released by CMS shows that many states plan to address the workforce challenges in rural areas. Delaware, for example, plans to use its funding to create the state’s first four-year medical school with a rural primary care track.
A third of states said they want to improve electronic health records, and every state mentioned telehealth.
Many state legislatures to distribute the funding to their state offices. Meanwhile, state officials are hiring staff, , and .
“I’m excited about what’s next,” said Terry Scoggin, former interim chief executive of the Texas Organization of Rural & Community Hospitals, or TORCH. Texas was awarded the biggest allocation. The money will bolster a rural hospital funding bill Republican Texas Gov. Greg Abbott signed last year, Scoggin said.
More than two dozen cash-strapped rural hospitals in Texas to clinics since 2005, a nationwide trend that hit the Lone Star State particularly hard. The state has the largest rural population in the United States. Texas’ allocation amounts to about $66 per rural resident, . By contrast, Rhode Island was granted about $6,300 per rural resident.
Scoggin said he has “a ton of concerns” about companies taking the money instead of it helping rural hospitals and residents. “I was blown away about how many for-profit companies reached out.” The companies have also called rural hospitals and asked to work with them to apply for state money, he said.
The awards should be judged on how they benefit rural residents because “the stated goal of the program is to improve rural health,” said Paula Chatterjee, an assistant professor of medicine at the University of Pennsylvania who co-authored on the transformation fund.
Researchers at the Sheps Center conducted the analysis to estimate how much money states received from the technical score, which is the portion of funding based on the quality of their proposals and state policy actions that align with “Make America Healthy Again” priorities.
New Mexico won the least amount of technical funding, with less than 10% of its award based on the discretionary metrics. Alaska won the largest technical award, according to the Sheps Center data.
Texas, Nebraska, New Hampshire, and Hawaii rounded out the top five recipients of technical funding. In addition to New Mexico, the other lowest technical awards went to Michigan, New Jersey, Arizona, and California.
Mark Holmes, director of the Sheps Center, declined to comment on whether he saw any political bias in the awards but said the nuance in the final portion of discretionary awards based on technical scores is important because those dollars can be redistributed and potentially clawed back in future years.
“We can be fairly certain that every state will get at least a slightly, if not a vastly, different amount next year based on this re-pooling and reallocation piece,” Holmes said.
States now have a limited time to show they’re using the money effectively to secure future funding.
But they can’t start spending yet. CMS followed standard grant procedures and is requiring each state to submit revised budgets before they can draw down money, Krepich said.
States have until Jan. 30 to resubmit their budgets, and CMS then has 30 days to respond, according to the standard . Under that timing, some states may not have cash in hand until March.
“CMS is working closely with states to complete this process as efficiently as possible,” Krepich said.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/rural-health-transformation-state-distribution-technical-scores-variation-deadlines/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2141942&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Health officials are recommending diet and exercise as alternatives to heavily advertised weight loss drugs like Wegovy and Zepbound, advice experts say is unrealistic.
“Of course he tried eating well and everything, but now with the medications, it’s better тАФ a 100% change,” said Wilmer Cardenas of Santa Clara, who said his husband lost about 100 pounds over about two years using GLP-1s covered by Medi-Cal, California’s version of Medicaid.
California joined several other states in restricting an option they say is no longer affordable as they confront soaring pharmaceutical costs and under the Trump administration, among . Despite negotiated price reductions announced in November that would make the drugs available at a “dramatically lower cost to taxpayers” and enable Medicaid to cover them, states are going ahead with the cuts, which providers say may undermine patients’ health.
“It will be quite negative for our patients” because data shows people typically regain weight after stopping the drugs, said , medical director of the University of California-San Francisco Weight Management Program.
While California, , , and stopped covering adult GLP-1 prescriptions for obesity on Jan. 1, they continue to cover the drugs for other health issues, such as Type 2 diabetes, cardiovascular disease, and chronic kidney disease.
, , and Wisconsin are planning or considering restrictions, according to KFF’s .
That reverses a trend that saw 16 states covering the medications for obesity as of Oct. 1. Interest in providing the coverage “appears to be waning,” the survey found, likely due to the drugs’ cost and other state budget pressures. North Carolina pulled back GLP-1 coverage in October, but reinstated it in December, bowing to court orders despite a lingering budget shortfall.
Catherine Ferguson, vice president of federal advocacy for the American Diabetes Association and its affiliated Obesity Association, said it’s not clear how states will adjust to the White House plan to lower the cost of several of the most popular GLP-1s through TrumpRx, an online portal for discounted prescription drugs. The price of Wegovy, for example, will be $350 per month for consumers, versus the current list price of nearly $1,350, and Medicare and Medicaid programs will pay $245, according to the plan.
“Many states are facing budgetary challenges, such as deficits, and are working to address the impacts of the changes to Medicaid and SNAP,” Ferguson wrote, referring to the Supplemental Nutrition Assistance Program. “As more details become available for the Administration’s agreements, we will see how state Medicaid responds.”
The Department of Health and Human Services referred questions to the White House, which did not respond to requests for comment on states’ termination of Medicaid coverage for the weight loss drugs.
California projected its costs to cover GLP-1s for weight loss would have more than quadrupled over four years to if it didn’t end Medi-Cal coverage for that use. Medi-Cal has covered weight loss drugs since 2006, but use of GLP-1s soared only in recent years. By 2024, more than 645,000 prescriptions were covered by Medi-Cal across all uses of the medications. The California Department of Health Care Services could not readily provide a breakdown of whether the drugs were for weight loss or other conditions.
When asked whether the state would reconsider its plans in light of the announced price cuts, Department of Finance spokesperson H.D. Palmer said it had no plans to do so. California’s cut is written into .
California officials would not say how much it could save under the TrumpRx plan, citing federal and state restrictions on disclosing rebate information.
Health providers don’t expect the Trump administration’s negotiated price cuts to make much difference to consumers, because pharmaceutical companies already offer some discounts.
“The out-of-pocket costs will still be very cost-prohibitive for most, especially individuals with Medicaid insurance,” Thiara said.
is among the other states that ended their coverage Jan. 1. Officials with the New Hampshire Department of Health and Human Services did not respond to requests for comment.
About 1 in 8 adults are now taking a GLP-1 drug for obesity, disease, or both, up 6 percentage points from May 2024, according to released in November. Over half of users said their GLP-1s were difficult to afford, and many who had stopped the treatment cited the cost.
Public and private payers have been trying to to save costs. California health officials said Medi-Cal members and their health care providers “other treatment options that can support weight loss, such as diet changes, increased activity or exercise, and counseling.” That echoes advice from the New Hampshire Medicaid program.
California Department of Health Care Services spokesperson Tessa Outhyse said in an email that the official advice to try those other approaches now “is not meant to dismiss any past efforts, but to encourage Medi-Cal members to take a renewed, proactive, and medically supported approach with their healthcare provider that may appropriately include these additional options.”
But that may be unrealistic, said , founding director of the Center for Clinical Nutrition at Keck School of Medicine of the University of Southern California.
“We definitely want patients to do their part with the diet and exercise, but unfortunately, and from a practical standpoint, that itself frequently is not enough,” Hong said, adding that usually by the time patients see doctors they have already failed at achieving results through those means.
Hong understands why Medicaid programs, as well as private providers, want to cut back on covering the drugs, which can cost per patient per year. However, they can produce twice the weight loss as the medications typically used previously, he said.
A school of medical thought supports patients’ gradually ending their use, but Hong said obesity is generally considered a chronic condition that requires indefinite treatment.
“Once they reach their target weight, a lot of people will try to see whether or not they can wean off,” Hong said. “We do see a lot of patients тАФ when they try to get off, unfortunately, then the weight comes back.”
Medi-Cal members under age 21 for purposes including weight loss, California officials said, citing a federal requirement.
Medi-Cal members are able to keep their GLP-1 coverage if they can demonstrate it is medically necessary for purposes other than weight loss, the department said. Members who are denied coverage can seek a hearing, the department said in to members.
Members will still be able to pay for the prescriptions and may be able to use various discounts to lower costs. Another option is new pills to treat obesity, which will be cheaper than their injectable counterparts. The a pill version of Wegovy on Dec. 22, which will likely run $149 per month for the lowest dosage, and similar weight loss pills are expected to be available in the first half of the year.
While Cardenas said his husband, Jeffer Jimenez, 37, uses GLP-1s primarily for weight loss, Jimenez’s prescription is for his diabetes, so the couple hoped to continue receiving coverage through Medi-Cal.
“He tried a thousand medications, pills, natural teas, exercise program, but it doesn’t work like the injections,” Cardenas said. “You need both.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/california-medicaid-medi-cal-glp1-weight-loss-drugs-ends-coverage-cost/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2135528&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>