That’s not stopping Florida lawmakers from trying to adopt Medicaid work requirements anyway. It’s the only legislative body in a nonexpansion state to even consider it so far.
“You need to go to work if you want your friends and neighbors to pay for your health care,” said , the Republican sponsor of a Medicaid work requirement proposal making its way through the legislature.
The move baffles health care advocates and Medicaid experts. Some doubt it’s even legal under President Donald Trump’s signature domestic policy law.
“You cannot change the terms of the work requirement,” said , an attorney and a professor at Georgetown University’s McCourt School of Public Policy, issued by the Centers for Medicare & Medicaid Services. For Cuello, the answer is clear: “It’s a pretty easy no.”
Medicaid work requirements affect Washington, D.C., and the 40 states that have expanded Medicaid eligibility to all nondisabled adults ages 19 through 64 with incomes up to 138% of the federal poverty level, as prescribed under the Affordable Care Act. That’s an income of $22,025 a year for a single person.
Starting next January, those states must require people in their expansion groups to report at least 80 hours a month of work, education, or community service to qualify for and maintain Medicaid coverage.
About 4 million people are enrolled in Florida’s program, and Gaetz estimates that about 147,000 of them are adults who “could work and should work.”
They “are able-bodied and they don’t have small children at home, and they aren’t taking care of an elderly person or a disabled person,” he said. “Yet they receive Medicaid benefits.”
People affected by would primarily be parents of children 14 and older, and some 19- and 20-year-olds, he said. A in the Florida House would apply Medicaid work requirements to parents of children ages 6 and older.
To qualify for Medicaid in Florida, a working-age adult without a disability must generally be caring for a child or an older or disabled family member and cannot earn more than 26% of the federal poverty level, or about $592 a month for a family of three.
Most adults who are not disabled and receive Medicaid already work, and many people in low-paying jobs do not receive health insurance through an employer, , a health information nonprofit that includes ∫⁄¡œ≥‘πœÕ¯ News. Among single adults ages 19 to 64 in Florida who made under $15,000 a year in 2024, through work.
Critics say Florida’s proposal would likely force some people to become uninsured, even if they meet the work requirement. That’s because the state’s Medicaid income limit is so low that working the mandated 80 hours a month would likely cause those individuals to exceed the income eligibility limit but also leave them earning too little to qualify for subsidized coverage on the Affordable Care Act marketplace.
Michelle Mastrototaro said she lost her Medicaid coverage in November after taking a part-time job as a teaching assistant at a Tampa elementary school last year. Mastrototaro, 47, cares for a disabled teenage son and likely would not need to meet Florida’s proposed work requirement.
But she said her biweekly wages from working about 17 hours a week pushed her past the Medicaid income limit. She has struggled to afford her prescription medications since.
“What I’m making is nothing,” Mastrototaro said. “I am scavenging just to make ends meet.”

The Gaetz-led proposal ignores “the hard realities of what it takes to be qualifying for Medicaid in Florida,” said , executive director of Florida Voices for Health, a nonprofit that advocates for Medicaid expansion. “On its face,” he said, “it doesn’t make sense.”
Medicaid experts say the holds that nonexpansion states cannot adopt work requirements.
A state that hasn’t added more low-income adults to its Medicaid program can’t impose work requirements on those who are already covered, Cuello said. States must cover specific categories of low-income people ‚Äî such as children, pregnant women, some parents, older adults, and people with disabilities ‚Äî to receive federal funding for their programs.
States that have expanded Medicaid eligibility to a limited group of low-income adults, namely Georgia and Wisconsin, will be required to impose work requirements on those enrollees.
, launched in July 2023, already includes a requirement that newly eligible adults report at least 80 hours of work or community engagement. Federal approval for the program expires at the end of December, and the state . will have to implement a work requirement by Jan. 1.
South Carolina applied in June for federal approval to to nondisabled parents and caregivers ages 19 to 64 who earn 67-100% of the federal poverty level. That’s about $18,300 to $27,300 a year for a family of three. The state’s application is pending with CMS, and if approved would implement work requirements for those newly eligible adults.
Gaetz said if the Florida legislation were approved, the state would develop a “business plan” for implementing work requirements and seek CMS approval.
It is unclear how much it would cost, but experience in states with Medicaid work requirements suggests that implementation would be expensive. States must upgrade their eligibility and enrollment systems, hire additional staff, and inform the public of the new mandate.
For its program, Georgia spent about $54.2 million on administrative changes out of $80.3 million in total spending for the program from October 2020 to March 2025, according to from the U.S. Government Accountability Office. Most of the administrative spending — about $47.4 million, or 88% — came from the federal government.
Georgia’s experience echoes others’, according to a 2019 of states that received approval to implement Medicaid work requirements during the first Trump administration. That report focused on five states ‚Äî Arkansas, Indiana, Kentucky, New Hampshire, and Wisconsin ‚Äî and estimated costs would total $408 million. They ranged from $6 million in New Hampshire to more than $270 million in Kentucky, though those figures did not reflect all the state costs.
Florida’s computer infrastructure for collecting and verifying information and determining eligibility is more than 30 years old and is being replaced. That is anticipated to be completed in 2028 and cost more than $180 million.
A legislative analysis of Gaetz’s bill estimated that if 1 in 4 people affected by the proposed work requirement were to lose Medicaid coverage, the state could save about $80 million a year.
Darius, with Florida Voices for Health, said those potential savings hardly seem worth the effort.
“It requires the state to build this giant regulatory-like framework and to rebuild systems, and to employ a whole set of people to chase down the very small number of folks who would ultimately be touched by this,” he said.
Are you struggling to afford your health insurance? Have you decided to forgo coverage? to contact ∫⁄¡œ≥‘πœÕ¯ News and share your story.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/florida-medicaid-work-requirements-expansion-one-big-beautiful-bill-act/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2162808&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But when Quinn chipped a tooth and it became infected, she could not find a dentist near her home who would accept her government health coverage and was taking new patients.
She went to an emergency room, receiving painkillers and antibiotics, but she remained in agonizing pain weeks later and paid a dentist $200 to extract the tooth.
Years later, it still hurts to chew on that side, she said, but Quinn ‚Äî a 34-year-old who has four children and, with her husband, earns about $30,000 a year ‚Äî still can’t find a dentist nearby.
“You should be able to get dental care,” she said, “because at the end of the day dental care is health care.”
The federal government has long required states to offer dental coverage for children enrolled in Medicaid, the joint state-federal health program for people who are low-income or disabled. Paying for adults’ dental care, though, is optional for states.
In recent years, several states have opted to expand the coverage offered by their Medicaid programs, seeking to boost access in recognition of its importance to overall health. So far, increasing adult dental care is a work in progress: In a sampling of six of those states by ∫⁄¡œ≥‘πœÕ¯ News, fewer than 1 in 4 adults on Medicaid see a dentist at least once a year.
But under congressional Republicans’ One Big Beautiful Bill Act, which President Donald Trump signed into law last year, the federal government is expected to reduce Medicaid spending by more than $900 billion over the next decade. The range from about $184 million for Wyoming to about $150 billion for California.
State Medicaid programs typically expand or reduce benefits depending on their finances, and such massive federal cuts could force some to shrink or eliminate what they offer, including dental benefits.
“We will lose all the gains we have made,” said Shillpa Naavaal, a dental policy researcher at Virginia Commonwealth University in Richmond.
Tennessee’s Medicaid program, for instance, spent nearly $64 million on its dental coverage in 2024 and saw a 20% decrease in dental-related ER visits, said Amy Lawrence, the program’s spokesperson.
But under the new law, Tennessee is projected to lose about $7 billion in federal funding over the next decade.
As of last year, 38 states and the District of Columbia offered enhanced dental benefits for adult Medicaid beneficiaries, according to the American Dental Association. Most of the others offer limited or emergency-only care. Alabama is the only state that offers no dental coverage for adult beneficiaries.
Since 2021, 18 states have enhanced their coverage to include checkups, X-rays, fillings, crowns, and dentures, while loosening annual dollar caps for benefits.
Use of dental benefits in states with the enhanced benefits is greater than in states with only limited or emergency coverage, though still low overall, according to with the latest data as of December. No more than a third of adult Medicaid recipients saw a dentist in 2022 in any state.
To review more recent progress, ∫⁄¡œ≥‘πœÕ¯ News asked one-third of the states that have expanded their benefits in the past five years for their most recent data on the percentage of adults on Medicaid who visit a dentist at least once a year:
- Maryland — 22% (in 2024)
- Oklahoma — 16% (in 2025)
- Maine — 13% (in 2025)
- New Hampshire — 19% (in 2025)
- Tennessee — 16% (in 2024)
- Virginia — 21% (in 2025)
In comparison, about 50% to 60% of adults with private dental coverage see a dentist at least once a year, according to the ADA.
Nationwide, 41% of dentists reported participating in Medicaid in 2024, a share that has remained stable over the past decade despite the dental benefit expansions in many states, the ADA says. Many participating dentists, though, limit the number of Medicaid enrollees they treat, and some will not accept new patients on Medicaid.
Reimbursement rates have not kept up with costs, deterring dentists from accepting Medicaid, said Marko Vujicic, chief economist and vice president at the ADA Health Policy Institute.
Because of a lack of dentists who take Medicaid in southwestern Virginia, the Appalachian Highlands Community Dental Center in Abingdon sees patients who travel more than two hours for care — and must turn many away, said Elaine Smith, its executive director.
The center’s seven residents treated about 5,000 patients last year, most of them on Medicaid. About 3,000 people are on its waitlist, waiting up to a year to be seen.
“It’s sad because they have the means now to see a dentist, but they still don’t have a dental home,” Smith said.
Low-income adults face other barriers to dental care, including a lack of transportation, child care, or time off work, she said.
The inability to see a dentist has consequences broader than tooth pain. Poor dental health can contribute to a host of other significant health problems, such as heart disease . It can also make it harder to do things like apply for jobs and generally lead a healthy life.
Robin Mullins, 49, who has been off and on Medicaid since 2013, said a lack of regular dental visits contributed to her losing her bottom teeth. Unable to find a dentist near her home in rural Clintwood, Virginia, she drives almost 90 minutes to Smith’s clinic ‚Äî that is, when she can afford to get time away from driving for DoorDash or find help watching her daughter, who has special needs.
She gets by with partial dentures but misses her natural teeth, she said. “It’s absolutely horrible, as you can’t chew your food properly.”
In New Hampshire, though, the challenges have more to do with low demand than a low supply of dentists, said Tom Raffio, chief executive of Northeast Delta Dental, which manages the state’s Medicaid dental program. The company has added new dentists to its list of participating providers, along with two mobile dental units that traverse the state, he said.
Raffio said Northeast Delta Dental also has publicized the state benefits using radio advertising and social media, among other efforts.
Until 2023, New Hampshire Medicaid covered only dental emergencies.
“Culturally, it’s going to take a while,” he said, “as people just are used to not going to the dentist, or going to the ER when have dental pain.”
Brooks Woodward, dental director at Baltimore-based Chase Brexton Health Care, called Maryland’s rate of roughly 1 in 5 adults on Medicaid seeing a dentist in 2024 “pretty good” considering the benefits had been enhanced only since 2023.
Woodward said many adults on Medicaid believe that you go to a dentist only when you’re in pain. “They’ve always just not gone to the dentist, and that’s just the way they had it in their life,” he said.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/medicaid-cuts-dental-coverage-republicans-big-beautiful-bill/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2161478&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But there are strings attached.
In late December, President Donald Trump’s administration announced how much all 50 states would get under its new Rural Health Transformation Program, assigning them to use the money to fix systemic problems that leave rural Americans without access to good health care. Now, the clock is ticking.
Within eight months, states must submit revised budgets, begin spending, and show the money is going to good use. Federal officials will begin reviewing state progress in late summer and announce 2027 funding levels by the end of October.
The money — divided into unique allocations for each state, ranging from $147 million for New Jersey to $281 million for Texas — represents the first $10 billion installment from the five-year, $50 billion program. Congress created the fund as a last-minute sweetener in Trump’s One Big Beautiful Bill Act last summer to offset the anticipated in rural communities from the statute’s nearly $1 trillion in Medicaid spending cuts over the next decade.
Federal officials crafted the fund to give states “space to be creative,” Mehmet Oz, administrator of the Centers for Medicare & Medicaid Services, said on a call with reporters after announcing the funding Dec. 29. “Some states will fail, and we will learn from that.”
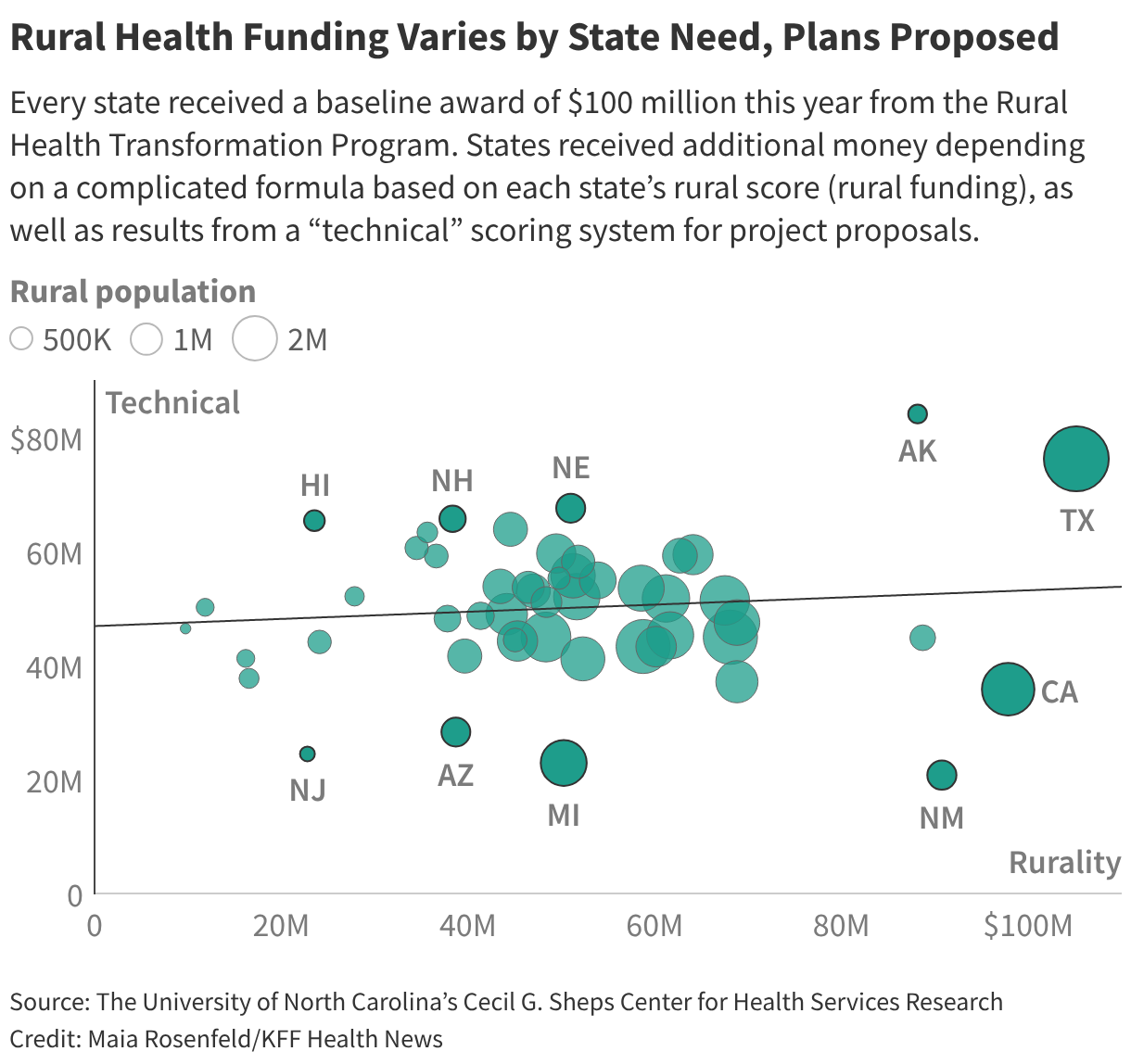
The money was divided according to a complicated formula.
In 2026, each state will receive an equal $100 million share for the first half of the money, plus additional funding from the second half. Oz’s staff steered payouts from the second portion based on each state’s rural score, as well as results from a “technical” scoring system for project proposals.
Within hours of the announcement, academics and researchers began to parse the awards to better understand why some states received more than others, including whether the awards reflected any partisanship or political favoritism.
At first glance, total awards do not appear to favor states governed by either Republicans or Democrats. But teased out the amount awarded for each state’s technical score, which is the part determined by the discretion of agency officials.
The analysis was performed at the University of North Carolina’s Cecil G. Sheps Center for Health Services Research, which specializes in rural health. A ∫⁄¡œ≥‘πœÕ¯ News review of the Sheps Center data found that states with Republican governors tended to receive more money for the parts of their application based on the technical score. Democratic-controlled states crowded the bottom quarter of those technical score awards.
Overall, though, the state awards reveal wild variation in how much money each state will get per rural resident, almost a hundredfold difference between the top and bottom.
In an emailed statement to , a spokesperson for Arizona’s Democratic Gov. Katie Hobbs accused the administration of shortchanging rural residents in the state, which was awarded $167 million this year from the program.
CMS spokesperson Chris Krepich said in an emailed statement to ∫⁄¡œ≥‘πœÕ¯ News that “politics played no role in funding decisions.”
On the December call, Oz pushed states to start working on policy actions championed by the administration — such as approving presidential fitness tests and restricting food benefits — that could require legislative approval.
Half of states promised to mandate the presidential fitness test, Oz said. Many states also proposed food waivers under the Supplemental Nutrition Assistance Program, known as SNAP, which would limit low-nutrition items such as soda. He also said some states promised to teach health care professionals about nutrition. And others confirmed they will repeal certificate-of-need laws, which require companies to prove that new health facilities they want to open are necessary.
Krepich said CMS’ new Office of Rural Health Transformation is hiring program officers to serve as point people for three or four states. Many states are setting up their own offices to oversee the new funding.
Oz highlighted Alabama’s “big maternity initiative with robotics doing ultrasounds” and said states are tackling issues ranging from behavioral health to obesity.
A ∫⁄¡œ≥‘πœÕ¯ News review of state “” and “” released by CMS shows that many states plan to address the workforce challenges in rural areas. Delaware, for example, plans to use its funding to create the state’s first four-year medical school with a rural primary care track.
A third of states said they want to improve electronic health records, and every state mentioned telehealth.
Many state legislatures to distribute the funding to their state offices. Meanwhile, state officials are hiring staff, , and .
“I’m excited about what’s next,” said Terry Scoggin, former interim chief executive of the Texas Organization of Rural & Community Hospitals, or TORCH. Texas was awarded the biggest allocation. The money will bolster a rural hospital funding bill Republican Texas Gov. Greg Abbott signed last year, Scoggin said.
More than two dozen cash-strapped rural hospitals in Texas to clinics since 2005, a nationwide trend that hit the Lone Star State particularly hard. The state has the largest rural population in the United States. Texas’ allocation amounts to about $66 per rural resident, . By contrast, Rhode Island was granted about $6,300 per rural resident.
Scoggin said he has “a ton of concerns” about companies taking the money instead of it helping rural hospitals and residents. “I was blown away about how many for-profit companies reached out.” The companies have also called rural hospitals and asked to work with them to apply for state money, he said.
The awards should be judged on how they benefit rural residents because “the stated goal of the program is to improve rural health,” said Paula Chatterjee, an assistant professor of medicine at the University of Pennsylvania who co-authored on the transformation fund.
Researchers at the Sheps Center conducted the analysis to estimate how much money states received from the technical score, which is the portion of funding based on the quality of their proposals and state policy actions that align with “Make America Healthy Again” priorities.
New Mexico won the least amount of technical funding, with less than 10% of its award based on the discretionary metrics. Alaska won the largest technical award, according to the Sheps Center data.
Texas, Nebraska, New Hampshire, and Hawaii rounded out the top five recipients of technical funding. In addition to New Mexico, the other lowest technical awards went to Michigan, New Jersey, Arizona, and California.
Mark Holmes, director of the Sheps Center, declined to comment on whether he saw any political bias in the awards but said the nuance in the final portion of discretionary awards based on technical scores is important because those dollars can be redistributed and potentially clawed back in future years.
“We can be fairly certain that every state will get at least a slightly, if not a vastly, different amount next year based on this re-pooling and reallocation piece,” Holmes said.
States now have a limited time to show they’re using the money effectively to secure future funding.
But they can’t start spending yet. CMS followed standard grant procedures and is requiring each state to submit revised budgets before they can draw down money, Krepich said.
States have until Jan. 30 to resubmit their budgets, and CMS then has 30 days to respond, according to the standard . Under that timing, some states may not have cash in hand until March.
“CMS is working closely with states to complete this process as efficiently as possible,” Krepich said.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/rural-health-transformation-state-distribution-technical-scores-variation-deadlines/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2141942&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Health officials are recommending diet and exercise as alternatives to heavily advertised weight loss drugs like Wegovy and Zepbound, advice experts say is unrealistic.
“Of course he tried eating well and everything, but now with the medications, it’s better ‚Äî a 100% change,” said Wilmer Cardenas of Santa Clara, who said his husband lost about 100 pounds over about two years using GLP-1s covered by Medi-Cal, California’s version of Medicaid.
California joined several other states in restricting an option they say is no longer affordable as they confront soaring pharmaceutical costs and under the Trump administration, among . Despite negotiated price reductions announced in November that would make the drugs available at a “dramatically lower cost to taxpayers” and enable Medicaid to cover them, states are going ahead with the cuts, which providers say may undermine patients’ health.
“It will be quite negative for our patients” because data shows people typically regain weight after stopping the drugs, said , medical director of the University of California-San Francisco Weight Management Program.
While California, , , and stopped covering adult GLP-1 prescriptions for obesity on Jan. 1, they continue to cover the drugs for other health issues, such as Type 2 diabetes, cardiovascular disease, and chronic kidney disease.
, , and Wisconsin are planning or considering restrictions, according to KFF’s .
That reverses a trend that saw 16 states covering the medications for obesity as of Oct. 1. Interest in providing the coverage “appears to be waning,” the survey found, likely due to the drugs’ cost and other state budget pressures. North Carolina pulled back GLP-1 coverage in October, but reinstated it in December, bowing to court orders despite a lingering budget shortfall.
Catherine Ferguson, vice president of federal advocacy for the American Diabetes Association and its affiliated Obesity Association, said it’s not clear how states will adjust to the White House plan to lower the cost of several of the most popular GLP-1s through TrumpRx, an online portal for discounted prescription drugs. The price of Wegovy, for example, will be $350 per month for consumers, versus the current list price of nearly $1,350, and Medicare and Medicaid programs will pay $245, according to the plan.
“Many states are facing budgetary challenges, such as deficits, and are working to address the impacts of the changes to Medicaid and SNAP,” Ferguson wrote, referring to the Supplemental Nutrition Assistance Program. “As more details become available for the Administration’s agreements, we will see how state Medicaid responds.”
The Department of Health and Human Services referred questions to the White House, which did not respond to requests for comment on states’ termination of Medicaid coverage for the weight loss drugs.
California projected its costs to cover GLP-1s for weight loss would have more than quadrupled over four years to if it didn’t end Medi-Cal coverage for that use. Medi-Cal has covered weight loss drugs since 2006, but use of GLP-1s soared only in recent years. By 2024, more than 645,000 prescriptions were covered by Medi-Cal across all uses of the medications. The California Department of Health Care Services could not readily provide a breakdown of whether the drugs were for weight loss or other conditions.
When asked whether the state would reconsider its plans in light of the announced price cuts, Department of Finance spokesperson H.D. Palmer said it had no plans to do so. California’s cut is written into .
California officials would not say how much it could save under the TrumpRx plan, citing federal and state restrictions on disclosing rebate information.
Health providers don’t expect the Trump administration’s negotiated price cuts to make much difference to consumers, because pharmaceutical companies already offer some discounts.
“The out-of-pocket costs will still be very cost-prohibitive for most, especially individuals with Medicaid insurance,” Thiara said.
is among the other states that ended their coverage Jan. 1. Officials with the New Hampshire Department of Health and Human Services did not respond to requests for comment.
About 1 in 8 adults are now taking a GLP-1 drug for obesity, disease, or both, up 6 percentage points from May 2024, according to released in November. Over half of users said their GLP-1s were difficult to afford, and many who had stopped the treatment cited the cost.
Public and private payers have been trying to to save costs. California health officials said Medi-Cal members and their health care providers “other treatment options that can support weight loss, such as diet changes, increased activity or exercise, and counseling.” That echoes advice from the New Hampshire Medicaid program.
California Department of Health Care Services spokesperson Tessa Outhyse said in an email that the official advice to try those other approaches now “is not meant to dismiss any past efforts, but to encourage Medi-Cal members to take a renewed, proactive, and medically supported approach with their healthcare provider that may appropriately include these additional options.”
But that may be unrealistic, said , founding director of the Center for Clinical Nutrition at Keck School of Medicine of the University of Southern California.
“We definitely want patients to do their part with the diet and exercise, but unfortunately, and from a practical standpoint, that itself frequently is not enough,” Hong said, adding that usually by the time patients see doctors they have already failed at achieving results through those means.
Hong understands why Medicaid programs, as well as private providers, want to cut back on covering the drugs, which can cost per patient per year. However, they can produce twice the weight loss as the medications typically used previously, he said.
A school of medical thought supports patients’ gradually ending their use, but Hong said obesity is generally considered a chronic condition that requires indefinite treatment.
“Once they reach their target weight, a lot of people will try to see whether or not they can wean off,” Hong said. “We do see a lot of patients ‚Äî when they try to get off, unfortunately, then the weight comes back.”
Medi-Cal members under age 21 for purposes including weight loss, California officials said, citing a federal requirement.
Medi-Cal members are able to keep their GLP-1 coverage if they can demonstrate it is medically necessary for purposes other than weight loss, the department said. Members who are denied coverage can seek a hearing, the department said in to members.
Members will still be able to pay for the prescriptions and may be able to use various discounts to lower costs. Another option is new pills to treat obesity, which will be cheaper than their injectable counterparts. The a pill version of Wegovy on Dec. 22, which will likely run $149 per month for the lowest dosage, and similar weight loss pills are expected to be available in the first half of the year.
While Cardenas said his husband, Jeffer Jimenez, 37, uses GLP-1s primarily for weight loss, Jimenez’s prescription is for his diabetes, so the couple hoped to continue receiving coverage through Medi-Cal.
“He tried a thousand medications, pills, natural teas, exercise program, but it doesn’t work like the injections,” Cardenas said. “You need both.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/california-medicaid-medi-cal-glp1-weight-loss-drugs-ends-coverage-cost/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2135528&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Hunt died five days later. Her death certificate said the foot injury was a “significant” factor. Genesis denied wrongdoing but agreed to pay $3.5 million in a settlement Hunt’s son signed in August 2024.
Yet Genesis hasn’t paid most of that debt, court records show. It may never have to.
Once the nation’s largest nursing home chain, it was spending $8 million a month defending and settling lawsuits over resident injuries and deaths in recent years. But the company is now poised to wipe the liability slate clean by seeking refuge in the most protective corner of the legal system for the nursing home industry: bankruptcy court.
The Genesis case, one of 11 large senior care bankruptcies this year, illustrates how health care companies can dodge public and financial accountability for alleged negligence through delays, confidentiality clauses, and bankruptcy maneuvers, a ∫⁄¡œ≥‘πœÕ¯ News investigation found.
When it filed for bankruptcy in Dallas in July, Genesis estimated its total liability for nearly a thousand settled and pending lawsuits at $259 million. A ∫⁄¡œ≥‘πœÕ¯ News review of the terms of 155 settlement agreements and shows Genesis officials knew insolvency was possible yet included provisions in its settlement agreements allowing it to defer payment, often for a year or more.
As a result, Genesis paid nothing in 85 cases and only a portion in the other 70, according to civil court records and bankruptcy claims made available through people with access to them. It still owes $41 million of the $58 million it had agreed to pay in those cases, the records show.

“It just feels like they killed my mom and got away with it,” said Vanessa Betancourt, whose mother, Nellie Betancourt, a retired nurse, fractured her hip at a Genesis home in Albuquerque, New Mexico — an injury the medical examiner’s report said led to her death. Genesis agreed to a $650,000 settlement with Betancourt’s family in April under the condition it would not need to pay the first of seven installments for another year, according to the settlement document.

Genesis denied wrongdoing in all lawsuits and settlements. In a written statement, the company did not answer questions about individual personal injury cases. The statement said Genesis remained “focused on delivering high-quality, compassionate care to our patients and residents without disruption” during bankruptcy.
One lawsuit Genesis settled for nearly $1 million alleged nursing home managers ignored repeated warnings about a male resident’s behavior before he sexually assaulted a female Alzheimer’s patient, according to court records. In a case the company resolved for $500,000, a Genesis nursing home was accused of delaying the hospitalization of a resident who had vomited brown mucus. He died of a bowel obstruction. Genesis has paid nothing for either settlement, according to bankruptcy claims.
Creditors, including families of the deceased, are expected to salvage a fraction of what they were promised, if anything. On Dec. 10, the company’s owners were scheduled to seek approval by the U.S. Bankruptcy Court for the Northern District of Texas to sell its nursing homes and other assets to its largest investor, a private equity firm. In court papers, lawyers for residents and other creditors say the complex plan will from pursuing Genesis’ new ownership and other companies the company’s collapse.
John Anthony, a bankruptcy attorney representing 340 personal injury claims against Genesis, said, “They never had any intention to honor these deals.”
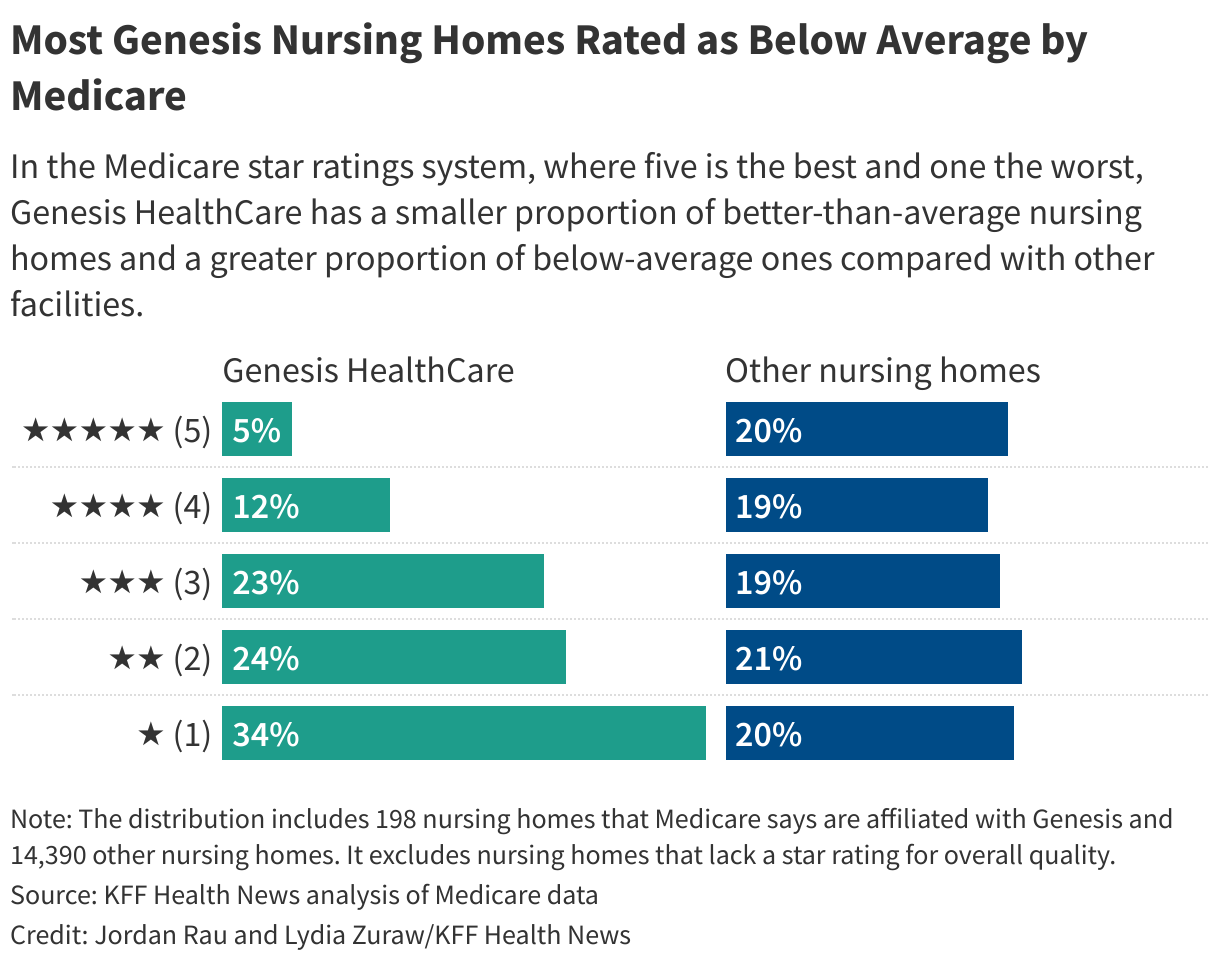
Low Ratings and Fines
During years of financial turmoil, Genesis has frequently struggled to provide top-notch care, federal records show. Using its five-star system, the Centers for Medicare & Medicaid Services affiliated with Genesis as below average or much below average. CMS Genesis homes $10 million for violating federal health standards over the past three years.
In 2022, a Genesis home after two deaths and multiple violations. The company this year after residents twice were evacuated over safety concerns.
In its filing, Genesis said it cared for about 15,000 residents in 165 nursing homes and 10 assisted living facilities in 18 states. They are centered in Pennsylvania, West Virginia, New Mexico, New Hampshire, New Jersey, Maine, Alabama, Maryland, and North Carolina, according to the bankruptcy filing.
The company said it owed $709 million in secured debt to lenders and the IRS. Under bankruptcy rules, those debts, backed by Genesis collateral, take precedence over the $1.6 billion in unsecured debt Genesis said it owes. Unsecured creditors include a pension fund; contractors that provided health services and equipment; Pennsylvania, New Mexico, and West Virginia for unpaid provider taxes; and former residents and their families who sued.
Dangers in Memory Care
Sandia Ridge Center, a Genesis home in Albuquerque, was repeatedly faulted by health regulators for not preventing sexual misbehavior in its memory care unit. In November 2021, CMS for lacking enough nurses to prevent sexual abuse among residents. An inspection report the following August inappropriate sexual contact. Police were called to investigate sexual assault allegations in and of 2023, police reports show; neither resulted in criminal charges.
Then in April 2023, a 61-year-old male resident with alcohol-related dementia sexually assaulted a female resident with Alzheimer’s in the dining room, according to a and an . When the resident screamed for him to stop and that he was hurting her, he responded “shut up bitch I know you like this,” according to a lawsuit brought on behalf of the woman, identified in court papers as R.S.
Sandia Ridge management had been aware of the male resident’s behavioral issues for months, according to employee depositions in the case. Police had investigated a against him the previous year without bringing charges. In one deposition, a former activities assistant testified he hit her and twice pushed her into a bathroom while announcing, “I want to have sex with you.” When she reported him to a senior Genesis manager, she said in the deposition, the manager put his finger over his lips and said, “Shhh.”
The activities worker testified that R.S. used to happily sing along with Elvis Presley songs. After the assault, the worker said, R.S. “don’t sing anymore.”
Inspectors cited the home for failing to protect R.S. The same report said the home didn’t provide a therapist for another female resident who was being sexually harassed. Medicare fined Sandia Ridge Center $91,247. Genesis denied liability but settled R.S.’ lawsuit for $925,000 in May, according to the bankruptcy claim.
“We just felt we have to hold them accountable,” R.S.’ daughter said in an interview, speaking on the condition that she and her mother not be identified, because of the nature of the assault. “Maybe I’m wrong, maybe I’m naive, but the only way to do that is to sue someone, right?”
Genesis has not paid any of the settlement, according to the family’s claim filing.

Growth and Debt
Genesis’ downfall can be , when affiliates of two private equity firms acquired the company in a $1.5 billion leveraged buyout, taking on substantial debt, according to its bankruptcy filing. Private equity also has been involved in other health care bankruptcies, including those of the nursing home chain, the prison health care contractor , and two for-profit hospital systems, and .
In 2011, Genesis raised $2.4 billion by transferring substantially all its nursing home buildings and other real estate to Welltower, a publicly traded real estate investment trust, according to Genesis’ bankruptcy filing. Genesis then rented the buildings back from Welltower, which made leasing costs a significant expense.
Genesis went on a nationwide buying spree. At its peak in 2016, it had grown to more than 500 nursing homes. In a court declaration, Louis Robichaux IV, a consultant overseeing Genesis’ bankruptcy restructuring, wrote that as the company expanded, it became harder to manage and “mired in corporate inefficiencies.” Robichaux wrote that Genesis’ financial woes were exacerbated by rapidly increasing labor costs and lawsuits, including some predating the covid pandemic.
Starting in 2021, Genesis avoided bankruptcy after from a founded by Joel Landau, the owner of a , according to Robichaux’s filing.
But Genesis continued to teeter on the edge of insolvency. In for 2022 and 2023 submitted to a California oversight agency, management and auditors said rent and debt obligations raised “substantial doubt about the company’s ability to continue as a going concern.”
In a court filing, a committee appointed by the U.S. Trustee’s Office to represent the unsecured creditors in the bankruptcy accused Landau and Welltower of that allowed Welltower to keep getting its rents while Landau could run the company and “siphon value to himself.” The committee alleged their efforts forced the company into insolvency while “staffing levels and patient care declined precipitously.” Landau and Welltower did not respond to requests for comment.
Drawn-Out Lawsuits
Erin Pearson sued Genesis over the death of her father, James Sanderson, a retired mining company executive who died in 2018 after spending less than a month at Bear Canyon Rehabilitation Center in Albuquerque. In the memory care unit, Sanderson fell repeatedly, suffered medication errors made by nursing home staff, and developed a bowel obstruction and sepsis, according to the lawsuit, filed in 2019. Pearson’s lawyers said he was not hospitalized until eight days after nurses noticed he was vomiting brown mucus.

After the judge rejected Genesis’ request to force Pearson into arbitration, Genesis appealed. It took 2½ years before an appeals court affirmed the original decision to let the case go forward in court, records show.
This past May, more than five years after suing, Pearson reached a $500,000 settlement, with the first payment required by November, according to a copy of the agreement. Nothing was paid, according to the bankruptcy claim.
“It was so drawn out and for so long,” Pearson said in an interview, calling Genesis’ bankruptcy “despicable.”
Payouts Postponed
Jennifer Foote, an Albuquerque attorney who represents clients in multiple lawsuits against Genesis, including Pearson’s, said the company frequently filed appeals. “They did not usually win them on these issues,” she said, “and our sense was that they were doing it as a delay tactic.”
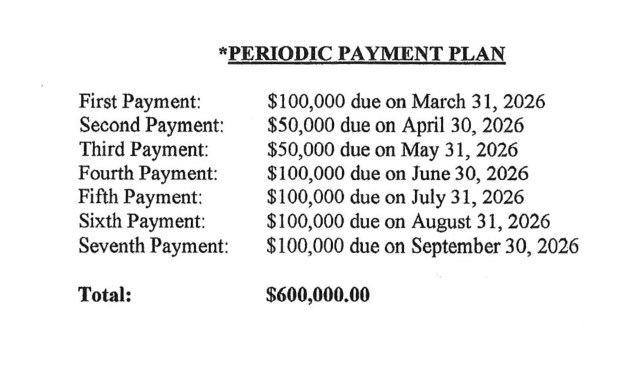

Genesis started using installment payments around 2018, said Dusti Harvey, Foote’s law partner. “The payments wouldn’t start for several months out,” Harvey said. Foote said Genesis’ lawyers often wanted to time the payments to start the month the trial in the case was scheduled to occur.
Families had to wait even when comparatively small amounts of money were involved, settlement agreements show. Genesis’ settlement agreements also included a confidentiality clause prohibiting discussion of the incidents.
Genesis agreed to pay $42,000 in a November 2024 settlement, but the first payment was not due until nine months later. It was not paid, according to the bankruptcy claim.
A $250,000 settlement signed in October 2023 did not start paying out until the following September. When Genesis declared bankruptcy — 21 months after the case was resolved — it still owed $100,000, according to the family’s claim.
‘We Never Found Out the Truth’
Settling cases allowed Genesis to avoid the expense and publicity of a trial, at which details of how its nursing homes functioned might have been revealed. In October 2020, Margarett Johnson, a retired school bus driver, fell out of her wheelchair at a Genesis nursing home in Waldorf, Maryland, fracturing her jawbone, nose, and neck, according to a lawsuit brought by her family. Johnson was sent to a trauma center and placed on a ventilator. She died three months later, at age 76, from ventilator-associated pneumonia, the lawsuit said.
“It looked like she was hit by a truck,” Angelina Harley, one of her daughters, said in an interview. “I knew my mom was not going to come home. I knew the Lord was not going to punish her more.”

The company denied negligence and blamed the accident on Johnson’s jacket getting tangled in the wheel of her wheelchair, according to the lawsuit. Harley and her sister Angela Swann were dubious.
“We never found out the truth,” Harley said. “They wanted to settle out of court.”
The company denied liability but agreed to a $950,000 settlement in October 2024. It never paid the final $112,500 installment, according to a letter Johnson’s five children sent to the bankruptcy judge.
“If you settle out of court, you know doggone well you did something wrong,” Harley said.
Maddening Judges
By summer 2025, judges in some civil cases had run out of patience.
Alma Brown, a retired day care manager and accordion teacher living in a Genesis nursing home in Clovis, New Mexico, suffered falls, infections, bedsores, and other neglect that hastened her death in 2023, according to her estate’s lawsuit. In Santa Fe District Court, Judge Kathleen McGarry Ellenwood castigated Genesis after it failed to pay $2 million of the $3 million settlement to Brown’s estate or explain the delay.
Genesis “obviously benefited by not having to go to trial,” McGarry Ellenwood said in one hearing, according to a court transcript. “They assure me that they’re not trying to renege on their contract, but it certainly seems like they haven’t lived up to what the bargain was.”
Genesis declared bankruptcy the day McGarry Ellenwood announced she would impose more than $100,000 in fines, plus $10,000 more each day until the settlement was paid.
In Pennsylvania, Greg Hunt petitioned a judge to punish Genesis after it stopped payments of the $3.5 million settlement after the death of his mother, Nancy, the resident with the gangrenous foot. She had spent eight months in 2019 at Brandywine Hall, a Genesis facility in West Chester that was later sold and renamed.
In a filing with the Common Pleas Court of Montgomery County, Genesis admitted it was in arrears but asked the judge for more time, citing “unforeseen and exigent financial challenges.” Genesis said care for patients at its nursing homes would suffer if it had to pay immediately.
Unswayed, Judge Richard Haaz in June ordered Genesis to pay up, along with punitive interest. But the bankruptcy court stayed that order. Genesis still owes $1.4 million of the $2 million it was supposed to pay, according to Hunt’s claim. (The rest of the $3.5 million settlement is supposed to be paid by an insurer in January 2026.) Ian Norris, Hunt’s lawyer, declined to comment, citing confidentiality provisions in the settlement.
Court records indicate Genesis lawyers never disclosed in either case that it was preparing to declare bankruptcy.
‘Bankruptcy as a Tool’
In the first nine months of 2025, 10 other senior living companies with liabilities over $10 million entered Chapter 11 bankruptcy, according to , a consulting firm.
Hamid Rafatjoo, a bankruptcy lawyer representing nursing homes who is not involved in the Genesis bankruptcy case, said filings may increase as the industry has become costlier to run and class action lawsuits have become a fixture.
“Nursing homes get sued all the time for everything,” Rafatjoo said. “A lot of operators wait too long to use bankruptcy as a tool.”
On Dec. 1, Genesis announced the , saying it had elected to to a private equity firm controlled by Landau. In a court filing, Anthony, the attorney for the personal injury claimants, in Landau’s favor despite an “objectively better and higher competing bid” from another private equity investor that would have provided more money to creditors. Genesis said in its statement that Landau’s group had increased its bid during the auction.
Sen. Elizabeth Warren (D-Mass.) and two other senators last month to intervene in the case, out of concern that “individuals who already own or control Genesis are trying to sell it to themselves, wiping away legal and other creditor debts in the process.” Lawyers representing those in charge of the auction did not respond to a request for comment.
Families of former Genesis residents said they fear the capacity to purge lawsuits through bankruptcy emboldens nursing home owners who provide deficient care.
“They can file bankruptcy again,” said Gabe Betancourt, whose wife, Nellie, died after her stay at Uptown Rehabilitation Center in Albuquerque. “And we’re the ones that will pay for it, with our memories, our lives.”

This <a target="_blank" href="/aging/nursing-homes-genesis-bankruptcy-liability-settlements-dallas-new-mexico/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2129309&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>On vacation in Mexico last year, Michael DiPlacido passed out twice while scuba diving and again in his hotel. Back in St. Louis, doctors diagnosed him with amyotrophic lateral sclerosis, or ALS, an incurable disease that often requires mechanical ventilation.
When his son Adam DiPlacido tried to find a permanent place to care for his father, who now needed a ventilator to breathe through a tracheostomy tube, he discovered none of Missouri’s nearly 500 nursing homes could take him.
“I never thought it would be easy, but I never thought it would be this hard,” Adam said.
A ∫⁄¡œ≥‘πœÕ¯ News investigation found widespread flaws and gaps in care for some of the country’s most debilitated people: those who cannot breathe on their own.
Spinal cord injuries, strokes, chronic obstructive pulmonary disease, and neurological diseases such as multiple sclerosis have left tens of thousands of Americans permanently dependent on ventilators. The barriers these patients face offer a stark example of how the United States’ disjointed health care system makes dealing with severe illness so much harder.
The investigation found patients are frequently stymied in efforts to get their insurers to provide appropriate home ventilators. They can end up spending hundreds of thousands of dollars for private nurses to make sure they don’t die overnight. Those who need to be in a nursing home or other health facility sometimes must move to another state, far from their families.
“There are not a lot of institutions that can manage these people,” said Jonathon Schwartz, acting chief medical officer for the Spaulding Rehabilitation Network in Boston.
Only 347 of the nation’s roughly 14,750 nursing homes have specialized units dedicated to people on ventilators, a ∫⁄¡œ≥‘πœÕ¯ News analysis of federal data shows. Fifteen states, including Missouri, have no nursing homes with a specialized unit for ventilator care.
While nursing homes can care for residents on ventilators on their regular floors, in practice few do. From April through June, fewer than 10% of nursing homes had long-stay residents breathing with the assistance of invasive mechanical ventilators, which deliver air through a tube down the airway or via a tracheostomy, the analysis found. Fewer than 15% of nursing homes had short-stay patients on ventilators.
Many patients in nursing homes can be weaned off ventilators, but those who can’t because of their condition often spend years in hospitals, which are not designed for residency. Innovative alternatives to traditional nursing homes exist in some areas of the country, but they haven’t been widely replicated and now are at risk from steep reductions in Medicaid enacted by President Donald Trump and the Republican-controlled Congress.
“It could create a terrible scenario,” said Gene Gantt, a respiratory care consultant to states and insurers.
Many people permanently on ventilators prefer to live at home as long as they can. But care there can be perilous and pricey. Some state health programs pay for ventilator care for low-income patients, but getting enrolled can take months amid bureaucratic hurdles and waitlists.
Some insurers balk at providing advanced home ventilators — which sound alerts for collapsed lungs, airway leaks, or malfunctions and can cost more than $10,000 — until patients have lost much of their ability to breathe.
“Feeling you’re suffocating is a horrific feeling, and that feeling can go on for months and months” as ALS patients decline while sparring with insurers, said Tyler Rehbein, an assistant professor of neurology at the University of Rochester who treats ALS patients.

‚ÄòOut of Money’
David Goldstein’s first symptom of ALS was a limp that appeared in the fall of 2022. It took six months for doctors to diagnose him with the neuromuscular disorder, also known as Lou Gehrig’s Disease. ALS afflicts about 34,000 Americans, destroying the nerve cells in the brain and spinal cord that control muscles, including those for breathing. It eventually results in complete paralysis, while most people remain mentally alert. Patients usually end up on ventilators if they do not die first, and respiratory failure is the most common cause of death.
Now 69 and on a ventilator, David cannot move anything except his eyes and mouth, said his ex-wife, Janis Goldstein, who has power of attorney. He requires someone around all the time in his Houston apartment to feed and bathe him, give him medication, and remove mucus blocking his airway. The settings on the ventilator require frequent monitoring and adjustments.
In spring of 2023, David got on the waiting list for Texas’ Medicaid home health program for disabled adults. More than a year later, Texas authorized 12 hours of home care a day. Still, Janis said, the state’s designated administrator sometimes has trouble getting workers for those shifts, and she and her ex-husband must pay for nurses to cover the rest of the day or night.
She said they have spent around a half-million dollars, largely on nurses and aides. They raised much of it through online campaigns and a fundraiser headlined by the country singer Larry Gatlin.
“The point that we’re at now, with the 24-hour help, is we’re pretty much out of money,” Janis said.
She is planning to move David into one of the few nursing homes in the region that take patients on ventilators, she said, but is concerned it will be difficult to arrange for someone to stay with David overnight in his room. She fears that if David’s position shifts even half an inch, he won’t be able to call for help through the machine that tracks his eye movements.
“I don’t know that he’ll be able to handle the stress and the anxiety of knowing that he could suffocate, even in a facility, because he doesn’t have someone by his side,” she said.

Ventilator Deserts
When Michael DiPlacido’s son Adam spent weeks searching for a facility in Missouri that could take care of a patient on a ventilator with a trach tube, the only one that was even a possibility told him it couldn’t accept new patients, because its lone respiratory therapist had quit.
“It’s incredible to me there is not one single place in Missouri that can take a patient like my father,” Adam said.
Looking outside the state, Michael decided to move to a nursing home north of Chicago, about five hours by car from St. Louis. After three months, he left the facility because it was so far away from his family, Adam said.
Adam helped his father move into a long-term care hospital in suburban St. Louis for six weeks. But Michael’s insurer would not pay for hospital-level acute care, so Adam said Michael had to pay more than $47,000 out-of-pocket. Next, Adam helped him move to another Illinois nursing home, about an hour away, that his son had originally rejected because of online reviews, including a Medicare warning that abuse had occurred. Finding it deficient, Michael left after a week.
Adam found a private nursing home company that would care for Michael in his home, at a cost of $960 a day. “After 323 days, my father has finally made it back home,” Adam said in an email in September.
But with his health rapidly deteriorating, Michael was admitted to a hospice facility in October. He died later that month at 75.

Gantt, the respiratory care consultant, said that fewer than half of state Medicaid programs provide adequate reimbursement rates for ventilator patients. He said most state Medicaid payment formulas do not measure outcomes or reward nursing homes financially if they provide better care, such as weaning a patient off the ventilator or preventing infections. He said he has seen nursing homes accept patients with trach tubes even when nurses lack proper training, or when the facility doesn’t employ respiratory therapists.
“For the large part, these patients are stuck in bed,” Gantt said. “We should try to get them the best quality of life.”
David Gifford, the chief medical officer for the American Health Care Association, a nursing home trade group, said equipping a nursing home with ventilators and getting state approval is expensive, and outside of urban areas, many markets lack enough local patients who need ventilators to make it financially worthwhile.
“It’s not as simple as saying we’re going to pay more and have more respiratory therapists,” Gifford said. “This is a group that needs highly specialized care. You’re not going to have it everywhere.”
Flagging Breaths
Derek McManus’ weakening right hand and occasional twitching was the first sign something was wrong. In October 2023, doctors diagnosed Derek, a corporate executive who lives in Painted Post, New York, with ALS.
By August 2024, Derek’s lungs were operating at 78% of capacity, his medical records show. Because ALS progresses so quickly, doctors often prescribe advanced . These machines deliver high-pressure air through a mask (called non-invasive) or a tube down the airway or via a tracheostomy (called invasive). They can calibrate themselves based on a patient’s breathing and have alarms that detect leaks, airway blockages, and device malfunctions. They can run on portable power sources and backup batteries in case of a power failure. The machines can allow people to talk or eat.

But some insurers have what physicians call “fail first” policies that won’t pay for ventilators unless the patient has already tried a respiratory assist device without success (as defined by the company). These simpler machines, the kind sleep apnea patients use, are not as effective in removing carbon dioxide as ventilators and lack safety features. Commonly known by the acronyms or , they can cost $1,000 or more and need to be plugged into an electrical socket.
“It seems to be an expectation of insurance companies they should live the rest of their life attached to a wall outlet,” said Rehbein, the University of Rochester neurologist.
In November 2024, Derek’s insurer denied his physician’s request for a ventilator, writing that “you have not failed treatment” with the simpler device, according to the insurer’s letter, provided by his wife, Lesley McManus. By April, Derek’s breathing capacity had dropped to 60% of normal. Lesley said she worried he would suffocate overnight if his basic device stopped working, since it had no safety alert. “He couldn’t take the mask off, because he can’t move his hands,” she said.
The insurer denied a second request for a ventilator, reiterating that Derek had not shown the simpler machine hadn’t worked, according to another insurance letter. Derek, who is 56, appealed to an independent medical reviewer, who overturned the insurer’s decision and ordered it to provide a ventilator, according to a copy of the ruling. The doctor wrote that the machine’s alarm system and capacity to automatically clear away airway secretion by simulating a cough were “vital for patient safety” and would help protect Derek from developing pneumonia.
“This multi-faceted approach to respiratory care is essential for improving gas exchange, reducing the work of breathing, and ultimately enhancing the patient’s quality of life and extending survival,” the decision said.
Derek said that since he got the new machine, he’s breathing easier, literally and emotionally. “If I’m not breathing right, it will give it an alert, and it will let us know if I don’t have the mask on properly,” he said.
The McManus family requested ∫⁄¡œ≥‘πœÕ¯ News not publish their insurer’s name, out of fear of repercussions.

Insurance Rules
John Hansen-Flaschen, a pulmonologist who founded Penn Medicine’s , said some patients give up when an insurer denies their requests and don’t file appeals. “These are some of the most vulnerable people there are, and they don’t have energy to do this,” he said.
Doctors who treat patients with neuromuscular disorders said the most resistance to providing ventilators comes from some private Medicare Advantage plans, but they said it also has been an issue with some commercial policies.
Insurers dispute that they refuse ventilators for patients who need them. The of Excellus BlueCross BlueShield, which Rehbein said was one of the companies that covers his patients, requires simpler breathing machines to have failed before patients can get the more sophisticated ventilator. After a ∫⁄¡œ≥‘πœÕ¯ News inquiry, Excellus clarified its policy with a footnote saying it does consider mechanical ventilators as first-line therapy for certain situations, such as ALS, on a case-by-case basis.
UnitedHealthcare confirmed that some of its policies require that a less complex device be tried initially and found ineffective before a ventilator can be authorized. doesn’t mandate a stepped process and says it considers mechanical ventilators based on the severity of the condition and “where interruption or failure of respiratory support would lead to death,” with other patients eligible only for the simpler devices. Humana and Cigna did not respond to requests to provide their policies.
Chris Bond, a spokesperson for AHIP, the health insurance industry’s trade organization, said, “Health plans work to connect patients with safe, clinically appropriate care and welcome opportunities to work with policymakers and stakeholders across the health care system to continually improve access and precisely address any coverage-related issues.”
Melanie Lendnal, senior vice president for policy and advocacy at the ALS Association, said, “I haven’t met one person yet living with ALS, or a family member, who has not had to fight ‚Äî really fight ‚Äî to get a non-invasive ventilator.”
A Model in Massachusetts
In 2019, David Marion, a 36-year-old plumber, was hanging out with friends in Lowell, Massachusetts, when he tripped on the sidewalk and fractured his neck. The injury rendered him quadriplegic and paralyzed his abdominal and diaphragm muscles, requiring him to use a ventilator. Surgeons performed a tracheotomy, and over the next year and a half, Marion lived in two long-term acute care hospitals. “I didn’t get out of bed” at the second hospital, Marion, now 43, said in an interview.
His mother, Denise Valliere, who lives in New Hampshire, said she grew desperate trying to find a permanent home for him that was close enough that she could visit. “Some of those nursing homes are pretty sad places,” she said.
At the end of 2020, Marion’s luck turned. He was accepted by the Leonard Florence Center for Living in Chelsea, Massachusetts, which has created an alternative to the institutional life most nursing homes can offer people on ventilators. The center follows the philosophy, with small residences each serving 10 people, with private bedrooms, a common living room, and outdoor space. Residents set their own schedules, including when and what to eat. The center has 10 residences in its building; six are dedicated to people dependent on ventilators, including those with ALS or MS.
The center’s respiratory therapists helped Marion get to the point where he didn’t need a feeding tube and didn’t require his ventilator for portions of the day. The center provided a portable ventilator attached to his wheelchair and a computer tablet that Marion operates with his mouth. It allows him to summon the elevator, open doors, go outside, and adjust his bed, window shades, temperature, and television settings. Other residents who can’t use their hands or mouths can operate the devices through a camera that captures eye movement.
“This gives back independence to people who never thought they’d have independence again,” said Barry Berman, the chief executive officer of Chelsea Jewish Lifecare, the nonprofit that owns the Leonard Florence Center. “There are alternatives. It doesn’t have to be the way that it is.”

Most of the residents’ stays are paid for by Medicaid, which together with Medicare provides the bulk of the center’s revenue. Its finances are bolstered by the nonprofit’s endowment, something most nursing homes lack. Berman said that since the center opened in 2010, he has hosted dozens of visitors interested in replicating its model elsewhere in the country, but no one has.
Some states have licensed facilities that aren’t nursing homes to care for people on ventilators. In California, some people on ventilators live in “congregate living health facilities,” which are residential houses that for the terminally ill, people who are catastrophically or severely disabled, or people who are mentally alert but physically disabled.
Patients often must pay privately because Medicaid managed care programs don’t include these facilities as a benefit, said Mariam Voskanyan, who is president of the state association representing congregate living facilities and owns one in Los Angeles. California’s Medi-Cal program is authorized to pay these kinds of facilities through its waiver, but the program is at capacity and there is of more than 5,000 people.
Researchers expect to reduce or eliminate programs like these to make up for nearly $900 billion in coming Medicaid reductions, since the federal government does not require states to cover or .
Valliere, Marion’s mother, said she was baffled that there were not more places like Leonard Florence. “How can we be so behind in that kind of care and those kinds of facilities if we’re the best country in the world,” she asked. “Why is this?”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/ventilators-nursing-homes-insurers-medicaid-als-lou-gehrigs-disease-missouri/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2114481&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Georgia is the only state with a work requirement in place for Medicaid, but several states have been pursuing such a policy for years, only to be blocked by courts or, most recently, the Biden administration. Some seek state-specific touches to the new rules. Others aim to implement work requirements before the federal law takes effect at the end of 2026.
These states’ moves and Trump’s massive tax-and-spending law share one demand: To keep their Medicaid health coverage, adults who can work must prove they’re logging a minimum number of hours at a job or school, or else qualify for one of the few exemptions.
But now, states that jumped ahead need to ensure their proposals, which require federal approval, don’t stray too far from Trump’s law.
“The statute sets both the floor and ceiling” for work requirements, said Sara Rosenbaum, a health law and policy professor with George Washington University.
South Dakota, for example, an application for work requirements as previously planned amid concerns that the state’s laxer rules would not be allowed under the new federal law. The state’s Department of Social Services secretary had warned that working on a state proposal while the federal rules are being hashed out could be “.”
Arkansas’ plan, on the other hand, is more stringent than the federal law. There are no exemptions to its work requirements , which is pending with the Centers for Medicare & Medicaid Services.
Arizona’s proposal also includes something that’s not in the federal law: a ban on “able-bodied adults” receiving Medicaid benefits for longer than five years total in their lives.
Arkansas and Arizona government officials said they were working with federal officials to square their plans with the new standards.
Andrew Nixon, a spokesperson for the U.S. Department of Health and Human Services, said the department is analyzing how the new federal standards interact with state waivers.
The federal health department must release rules by next June that outline how states are to implement work requirements, according to , who has been tracking such waivers as part of the Program on Medicaid and the Uninsured at KFF, a health information nonprofit that includes ∫⁄¡œ≥‘πœÕ¯ News.
“We don’t exactly know what that will cover,” Hinton said.
It’s unclear how federal officials will respond to the states’ requests, she added, but “we are aware that some folks think there is no wiggle room here.”
States can tweak their Medicaid programs through what are known as demonstration waivers, which are subject to federal approval. The waivers are designed to test new ideas in policy gray areas.
The states that have filed or plan to file such applications with work requirements include Arizona, Arkansas, Georgia, Idaho, Indiana, Iowa, Kentucky, Montana, New Hampshire, North Carolina, Ohio, South Carolina, South Dakota, and Utah.
Congressional Republicans who passed the budget reconciliation bill left room for states to use waivers to fast-track the national standards. Tara Sklar, a professor leading the University of Arizona’s Health Law & Policy Program, said she expects states seeking certain stricter requirements to have a chance of approval, while more lenient ones may face denials.
Federal officials may look favorably on Arizona’s plan, Sklar said, as a five-year lifetime Medicaid limit is different from work requirements. Even if the federal government greenlights stricter work requirements than the federal law calls for, those programs are likely to face legal challenges, she added.
The federal law includes an 80-hour-per-month minimum for work or education, with exemptions for certain adults, including people who are medically frail and parents with young, dependent children.
Montana is the first state to draft a waiver application since Congress finalized national work requirements. State lawmakers first approved work requirements — called “community engagement” standards under the state plan — in 2019, but the state’s application stalled through the end of the first Trump term and the Biden administration.
After Trump was elected again, Montana lawmakers lifted the 2025 expiration date of its Medicaid expansion program, making permanent the program that covered more than 76,000 adults in April, with the expectation that the Trump administration would approve work requirements. In mid-July, state officials to make that a reality “as soon as is practicable.”
The Montana plan largely aligns with the federal law, but it would create additional exemptions, including for people who are homeless or fleeing domestic violence.
Republican state Sen. Gayle Lammers said work requirements that also protect such people who need Medicaid were a big part of persuading legislators to keep the expansion program. At the time, officials didn’t know where the federal government would land on work requirements. And now, Lammers said, it makes sense for Montana to stick to its plan.
“The state should have a say,” Lammers said. “We’re very independent, and everyone is different.”
In South Carolina, state officials are seeking to roll out work requirements for a limited number of newly eligible Medicaid beneficiaries. South Carolina is one of 10 states that has not expanded Medicaid eligibility under the Affordable Care Act, and yet the state submitted a request with the federal government in June for a partial Medicaid expansion that includes a work requirement component that largely reflects the new federal standards.
In to Health and Human Services Secretary Robert F. Kennedy Jr., South Carolina Gov. Henry McMaster, a Republican, called South Carolina’s proposal “a state-specific solution.”
The only state with an active work requirement program now wants to scale it back and awaits federal approval to do so. “Georgia Pathways to Coverage” expires at the end of September unless CMS greenlights an extension of the program with a key change: requiring enrollees to document once a year that they’re working, not monthly. That’s a pivot away from the program’s initial design but also differs from the new federal rules, which call for checks every six months.
Fiona Roberts, a spokesperson for Georgia’s Medicaid agency, said the state is still waiting to hear whether it needs to alter its plan.
So Georgia is among the states in limbo, awaiting guidance from the federal government.
∫⁄¡œ≥‘πœÕ¯ News correspondents Sam Whitehead and Lauren Sausser contributed to this report.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/medicaid-federal-work-requirements-less-leeway-for-states/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2067611&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Now, as Congress steamrolls toward passing historic Medicaid cuts of about through Trump’s tax and spending legislation, red-state governors are saying little publicly about what it does to health care ‚Äî even as they face reductions that will punch multibillion-dollar holes in their states’ budgets.
Medicaid, a program jointly run by states and the federal government, covers more than 70 million low-income or disabled people, including nearly half of the nation’s children. Republicans say the $900 billion-a-year program was allowed to grow too large under Democrats Barack Obama and Joe Biden by adding nondisabled adults they say , and they have long sought to scale it back.
Some of the biggest health cuts in the legislation Trump calls the “One Big Beautiful Bill” are achieved through new policies that would reduce enrollment by imposing more paperwork demands on enrollees, including a requirement that many prove they’re working. Those policies would affect only states that expanded Medicaid to more low-income people under the Affordable Care Act.
Nineteen of those states are . Their silence on the bill’s health measures is giving political cover to GOP lawmakers from their states as they seek to cut Medicaid coverage for millions of people who gained it within the last decade.
∫⁄¡œ≥‘πœÕ¯ News contacted all 19 governors for comment on the legislation’s Medicaid cuts. Only six responded. Most said they backed imposing a work requirement on adult Medicaid enrollees.
“Implementing work requirements for able-bodied adults is a good and necessary reform so that Medicaid is being used for temporary assistance and not a permanent entitlement,” said Drew Galang, a spokesperson for Gov. Patrick Morrisey of West Virginia.
“Governor Rhoden supports workforce participation as a requirement of Medicaid expansion eligibility,” said Josie Harms, a spokesperson for South Dakota Gov. Larry Rhoden, adding that congressional lawmakers have the governor’s support: “South Dakota has an excellent federal delegation, and Governor Rhoden trusts them to fight for South Dakota’s priorities while delivering on President Trump’s promises.”
In a sign of how the political winds have changed, none of the governors said anything about another of the legislation’s significant cuts, to provider taxes ‚Äî a tool that nearly all of their states use to help pay their share of Medicaid and gain additional funds from the federal government. That change is expected to cost states billions.
No Longer a Bipartisan Issue
In contrast to the radio silence from GOP governors, Democratic governors have campaigned against the megabill for weeks.
Pennsylvania Gov. Josh Shapiro posted that Trump and congressional Republicans were misleading Americans by saying they were cutting only waste, fraud, and abuse in Medicaid.
“They’re rushing to kick hundreds of thousands of Pennsylvanians off their healthcare ‚Äî and lying about it,” he posted. “The damage this will do here in Pennsylvania and across America is staggering and will be felt for years to come.”
In New York, Gov. Kathy Hochul on July 1 charged that Trump’s legislation would devastate hospitals and could lead to more than 34,000 job cuts in her state.
“The collective impact of the GOP reconciliation bill in Washington, D.C., could force hospitals to curtail critically needed services such as maternity care and psychiatric treatment, not to mention to downsize operations, and even close entirely,” she said .
In 2017, the chorus was bipartisan, as Republican governors in , , and spoke out against cutting Medicaid. Trump’s bill to repeal much of the Affordable Care Act and roll back its Medicaid expansion narrowly failed in the Senate.
“It’s been surprising that red-state governors, particularly those in Medicaid expansion states, haven’t spoken out against Medicaid cuts,” said Larry Levitt, executive vice president for health policy at KFF, a health information nonprofit that includes ∫⁄¡œ≥‘πœÕ¯ News. “Republican governors were a potent political force in the failed 2017 effort to repeal and replace the ACA, including Medicaid expansion.”
What’s changed since 2017, policy experts say, is that there are fewer moderate Republican governors, and GOP state executives who advocated for Medicaid expansion over a decade ago are no longer in office.
Additionally, seven of the then-red states that expanded Medicaid , mostly over opposition from their governors.
In fact, the Medicaid work requirement is backed by many Republican governors, even if it means less federal Medicaid money and leads to fewer people covered.
Several states, including Arkansas and Ohio, have already passed state laws to implement a requirement that adults enrolled under the ACA’s Medicaid expansion work, volunteer, go to school, or participate in job training. Most states have yet to bring work requirement programs to fruition because they are waiting for federal government approval.
Charles “Chip” Kahn, president of the Federation of American Hospitals, a trade group of investor-owned hospitals, said that while fewer governors have engaged publicly in trying to block Medicaid cuts under the bill, federal lawmakers are hearing from legislators in their states.
A political dilemma for Republican governors is that, unlike in 2017, the bill before Congress is not legislation aimed expressly at repealing Obamacare. With a scope broader than health care, it would extend many of Trump’s tax cuts and direct billions in new spending toward border security, immigration enforcement, and the military, while also cutting health care spending.
“It’s like playing multidimensional chess rather than focusing on one issue,” Kahn said.
, director of the Center for the Study of Politics and Governance at the University of Minnesota, said some Republican governors may have expressed concerns privately to their states’ GOP senators but are not speaking out publicly for fear of drawing Trump’s wrath.
“Why are they being cagey? Trump and not wanting to be ‚ÄòLiz Cheney’d,’” Jacobs said, referring to the Republican former Wyoming lawmaker whom Trump helped oust after she served as vice chair of an inquiry into his attempts to overturn the results of the 2020 election.
Walking Political Tightropes
The political peril Republican lawmakers face in publicly challenging Trump remains explicit. On June 29, Sen. Thom Tillis (R-N.C.) announced he would not run for reelection after he voiced concerns about the bill and the president threatened to back a primary challenger. Tillis was one of three GOP senators to vote against it on July 1, though it still narrowly passed.
In addition to the work requirement, the biggest Medicaid cuts in the bill stem from its restrictions on provider taxes — levies that states impose on hospitals, nursing homes, and other health care institutions to help increase their federal reimbursement. Much of the additional money is then returned to the health care providers in the form of higher payments for their Medicaid patients.
The practice, which has been adopted in every state but Alaska, has been criticized by some Beltway Republicans as “money laundering” ‚Äî even though the taxes are approved by state lawmakers and the federal Centers for Medicare & Medicaid Services and have been allowed under federal law for decades.
The Senate bill would limit the money states could raise — a move that would mean billions in funding cuts to states and their hospitals.
The states with Republican governors that expanded Medicaid are Alaska, Arkansas, Idaho, Indiana, Iowa, Louisiana, Missouri, Montana, Nebraska, New Hampshire, Nevada, North Dakota, Ohio, Oklahoma, South Dakota, Vermont, Virginia, West Virginia, and Utah.
One of the governors who expressed concerns about repealing the Obamacare Medicaid expansion in 2017 was Jim Justice of West Virginia, a Democrat at the time.
In a to West Virginia Sen. Shelley Moore Capito, a Republican, Justice wrote: “Since so many of our people count on Medicaid, any cut to Medicaid would destroy families in West Virginia.” He added that “the consequences would be beyond catastrophic.”
On July 1, Justice ‚Äî elected to the Senate as a Republican last year ‚Äî voted for Trump’s megabill, including its Medicaid cuts.
“The Senator believes this bill strikes a good balance between protecting the most vulnerable and those who rely on the program while rooting out waste, fraud, and abuse to ensure the program is run efficiently for those deserving,” William O’Grady, a Justice spokesperson, said in an email July 2.
∫⁄¡œ≥‘πœÕ¯ News correspondent Arielle Zionts contributed to this report.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/big-beautiful-bill-trump-medicaid-affordable-care-act-cuts-republican-gop-governors/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2056990&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Since taking office, President Donald Trump has issued a handful of executive orders aimed at terminating all diversity, equity, and inclusion, or DEI, initiatives in federally funded programs. And in his , he described the Supreme Court’s 2023 decision banning the consideration of race in college and university admissions as “brave and very powerful.”
Last month, the Education Department’s Office for Civil Rights ‚Äî which in mid-March ‚Äî directed schools, including postsecondary institutions, to end race-based programs or risk losing federal funding. The cited the Supreme Court’s decision.
Paulette Granberry Russell, president and CEO of the National Association of Diversity Officers in Higher Education, said that “every utterance of ‚Äòdiversity’ is now being viewed as a violation or considered unlawful or illegal.” Her organization filed a lawsuit .
While California and eight other states — Arizona, Florida, Idaho, Michigan, Nebraska, New Hampshire, Oklahoma, and Washington — had already of varying degrees on race-based admissions policies well before the Supreme Court decision, schools bolstered diversity in their ranks with equity initiatives such as targeted .
But the court’s decision and the subsequent state-level backlash ‚Äî 29 states have since introduced bills to curb diversity initiatives, according to data published by ‚Äî have tamped down these efforts and led to the recent declines in diversity numbers, education experts said.
After the Supreme Court’s ruling, the numbers of Black and Hispanic medical school enrollees fell by double-digit percentages in the 2024-25 school year compared with the previous year, according to the . Black enrollees declined 11.6%, while the number of new students of Hispanic origin fell 10.8%. The decline in enrollment of American Indian or Alaska Native students was even more dramatic, at 22.1%. New Native Hawaiian or other Pacific Islander enrollment declined 4.3%.
“We knew this would happen,” said Norma Poll-Hunter, AAMC’s senior director of workforce diversity. “But it was double digits ‚Äî much larger than what we anticipated.”
The fear among educators is the numbers will decline even more under the new administration.
At the end of February, the Education Department launched an encouraging people to “report illegal discriminatory practices at institutions of learning,” stating that students should have “learning free of divisive ideologies and indoctrination.” The agency later issued a “” document about its new policies, clarifying that it was acceptable to observe events like Black History Month but warning schools that they “must consider whether any school programming discourages members of all races from attending.”
“It definitely has a chilling effect,” Poll-Hunter said. “There is a lot of fear that could cause institutions to limit their efforts.”
Numerous requests for comment from medical schools about the impact of the anti-DEI actions went unreturned. University presidents are staying mum on the issue to protect their institutions, according to .
Utibe Essien, a physician and UCLA assistant professor, said he has heard from some students who fear they won’t be considered for admission under the new policies. Essien, who co-authored a study on the effect of on medical schools, also said students are worried medical schools will not be as supportive toward students of color as in the past.
“Both of these fears have the risk of limiting the options of schools folks apply to and potentially those who consider medicine as an option at all,” Essien said, adding that the “lawsuits around equity policies and just the climate of anti-diversity have brought institutions to this place where they feel uncomfortable.”
In early February, the Pacific Legal Foundation against the University of California-San Francisco’s Benioff Children’s Hospital Oakland over an internship program designed to introduce “underrepresented minority high school students to health professions.”
Attorney Andrew Quinio filed the suit, which argues that its plaintiff, a white teenager, was not accepted to the program after disclosing in an interview that she identified as white.
“From a legal standpoint, the issue that comes about from all this is: How do you choose diversity without running afoul of the Constitution?” Quinio said. “For those who want diversity as a goal, it cannot be a goal that is achieved with discrimination.”
UC Health spokesperson Heather Harper declined to comment on the suit on behalf of the hospital system.
Another lawsuit accuses the University of California of favoring Black and Latino students over Asian American and white applicants in its undergraduate admissions. Specifically, the complaint states that UC officials pushed campuses to use a “holistic” approach to admissions and “move away from objective criteria towards more subjective assessments of the overall appeal of individual candidates.”
The scrutiny of that approach to admissions could threaten diversity at the UC-Davis School of Medicine, which for years has employed a “race-neutral, holistic admissions model” that enrollment of Black, Latino, and Native American students.
“How do you define diversity? Does it now include the way we consider how someone’s lived experience may be influenced by how they grew up? The type of school, the income of their family? All of those are diversity,” said Granberry Russell, of the National Association of Diversity Officers in Higher Education. “What might they view as an unlawful proxy for diversity equity and inclusion? That’s what we’re confronted with.”
California Attorney General Rob Bonta, a Democrat, recently joined other state attorneys general urging that schools continue their DEI programs despite the federal messaging, saying that legal precedent allows for the activities. California is also among over its deep cuts to the Education Department.
If the recent decline in diversity among newly enrolled students holds or gets worse, it could have long-term consequences for patient care, academic experts said, pointing toward the vast racial disparities in health outcomes in the U.S., particularly for Black people.
A higher proportion of Black primary care doctors is associated with longer life expectancy and lower mortality rates among Black people, according to published by the JAMA Network.
Physicians of color are also more likely to build their careers in , studies have shown, which is increasingly important as the AAMC of up to 40,400 primary care doctors by 2036.
“The physician shortage persists, and it’s dire in rural communities,” Poll-Hunter said. “We know that diversity efforts are really about improving access for everyone. More diversity leads to greater access to care ‚Äî everyone is benefiting from it.”
This article was produced by ∫⁄¡œ≥‘πœÕ¯ News, which publishes , an editorially independent service of the .Ã˝
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/dei-crackdown-trump-diversity-medical-schools-universities-enrollment/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2002301&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Donald Trump’s election to a second term has cast uncertainty around the future of the health law. In addition, the Biden administration implemented to reduce fraudulent enrollment and is combating a lawsuit that aims to block immigrants who lack legal residency from buying insurance under the program.
So far, the number of new and returning enrollees using healthcare.gov ‚Äî the federal marketplace that ‚Äî is below last year’s. New enrollments in early December, at the same time last year.
To give consumers in federal marketplace states more time to enroll, the Centers for Medicare & Medicaid Services extended to Dec. 18 the deadline to sign up for coverage that starts Jan. 1. (The Jan. 15 deadline is for coverage that would begin Feb. 1.)
Also in flux is a rule issued by the Biden administration allowing ‚Äî ‚Äî enrollment in ACA coverage by people brought to the U.S. as children without immigration paperwork, known as “Dreamers.”
The Biden team was granted a by the U.S. Court of Appeals for the 8th Circuit regarding a Dec. 9 order by a federal judge in North Dakota. That district court judge had that sought to block the Biden administration’s Dreamers directive. Without a stay, the decision in that case, Kansas v. the United States, effectively bars those who have qualified for the Deferred Action for Childhood Arrivals program in the 19 states from enrolling in or getting subsidies for ACA plans. It does not appear to affect enrollment or coverage in other states, lawyers following the case have said.
A final decision on the temporary stay was expected any day now. If granted, it could allow Dreamers to continue enrolling while the ruling is heard, which is unlikely to occur before Trump takes office.
In its court filings, the Biden administration argues that not granting a stay would be very disruptive in the middle of open enrollment, causing the federal government to incur costs in retooling its marketplace to reflect the change, and notifying those who have already enrolled that their plans are canceled.
in August in the U.S. District Court for the District of North Dakota and is being heard by District Judge Daniel Traynor, who was nominated in 2019 by then-President Trump.
Previously, the federal government uninsured people out of a half-million DACA recipients might sign up for 2025 coverage. In its new filing, the government says 2,700 have enrolled in those states that brought the suit and use the federal marketplace.
The Biden administration rule, finalized in May, clarified that those who qualify for DACA would be considered “lawfully present” for the purposes of enrolling in plans under the ACA, which are open to citizens and those who are called “lawfully present” immigrants.
The federal lawyers argue that North Dakota has not proved it would be harmed by the rule, so it has no standing to bring the case. North Dakota argued that it incurs costs for approximately 130 DACA recipients who live in its state, and that it would not have those expenses if they were barred from enrolling in the ACA and thus decided to leave the country. An exodus is unlikely, the federal government argued. The legal brief also questioned North Dakota’s calculation that it incurs costs of $585 to issue driver’s licenses to the DACA recipients and about $14,000 annually to educate at least one DACA member or dependent.
All the states challenging the ACA rule say it will cause administrative and resource burdens as more people enroll, and that it will encourage additional people to remain in the U.S. when they don’t have permanent legal authorization. The plaintiff states are Alabama, Arkansas, Florida, Idaho, Indiana, Iowa, Kansas, Kentucky, Missouri, Montana, Nebraska, New Hampshire, North Dakota, Ohio, South Carolina, South Dakota, Tennessee, Texas, and Virginia.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/obamacare-enrollment-lag-trump-election-legal-challenges/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1961373&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>