The federal government doesn’t track how many children have entered foster care because of immigration enforcement actions, leaving it unclear how often it happens. In Oregon, as of February two children had been placed in foster care after being separated from their parents in immigration detention cases, according to Jake Sunderland, a spokesperson for the Oregon Department of Human Services.
“Before fall 2025, this simply had never happened before,” Sunderland said.
As of mid-February, nearly by Immigration and Customs Enforcement. The record 73,000 people in detention in January represented an compared with one year before. According to , parents of 11,000 children who are U.S. citizens were detained from the beginning of Trump’s term through August.
The news outlet NOTUS that at least 32 children of detained or deported parents had been placed in foster care in seven states.
Sandy Santana, executive director of Children’s Rights, a legal advocacy organization, said he thinks the actual number is much higher.
“That, to us, seems really, really low,” he said.
Separation from a parent is deeply traumatic for children and can lead to , including post-traumatic stress disorder. Prolonged, intense stress can lead to more-frequent infections in children and developmental issues. That “toxic stress” is also associated with responsible for learning and memory, according to KFF.
, and amended existing laws during Trump’s first term to allow guardians to be granted temporary parental rights for immigration enforcement reasons. Now the enforcement surge that began after Trump returned to office last year has prompted a new wave of state responses.
In New Jersey, lawmakers are considering to amend a state law that allows parents to nominate standby, or temporary, guardians in the cases of death, incapacity, or debilitation. The bill would add separation due to federal immigration enforcement as another allowable reason.
Nevada and California passed laws last year to protect families separated by immigration enforcement actions. California’s law, called the , allows parents to nominate guardians and share custodial rights, instead of having them suspended, while they’re detained. They regain their full parental rights if they are released and are able to reunite with their children.
There are significant legal barriers to reunification once a child is placed in state custody, said Juan Guzman, director of children’s court and guardianship at the Alliance for Children’s Rights, a legal advocacy organization in Los Angeles.
If a parent’s child is placed in foster care and the parent cannot participate in required court proceedings because they are in detention or have been deported, it’s less likely they will be able to reunite with their child, Guzman said.
are U.S. citizens who live with a parent or family member who does not have legal immigration status, according to research from the Brookings Institution, a Washington, D.C.-based think tank. Within that group, 2.6 million children have two parents lacking legal status.
Santana said he expects the number of family separation cases to grow as the Trump administration continues its immigration enforcement campaign, putting more children at risk of being placed in foster care.
the agency to make efforts to facilitate detained parents’ participation in family court, child welfare, or guardianship proceedings, but Santana said it’s uncertain whether ICE is complying with those rules.
ICE officials did not respond to requests for comment for this report.
Before the change in California’s law, the only way a parent could share custodial rights with another guardian was if the parent was terminally ill, Guzman said.
If parents create a preparedness plan and identify an individual to assume guardianship of their children, the state child welfare agency can begin the process of placing the children with that individual without opening a formal foster care case, he added.
While Nevada lawmakers expanded an existing guardianship law last year to include immigration enforcement, the measure requires the parents to take the additional step of filing notarized paperwork with the secretary of state’s office, said Cristian Gonzalez-Perez, an attorney at Make the Road Nevada, a nonprofit that provides resources to immigrant communities.
Gonzalez-Perez said some immigrants are still hesitant to fill out government forms, out of fear that ICE might access their information and target them. He reassures community members that the state forms are secure and can be accessed only by hospitals and courts.
The Trump administration has taken through the Centers for Medicare & Medicaid Services, the IRS, the Supplemental Nutrition Assistance Program, the Department of Housing and Urban Development, and other entities.
Gonzalez-Perez and Guzman said that not enough immigrant parents know their rights. Nominating a temporary guardian and creating a plan for their families is one way they can prevent feelings of helplessness, Gonzalez-Perez said.
“Folks don’t want to talk about it, right?” Guzman said. “The parent having to speak to a child about the possibility of separation, it’s scary. It’s not something anybody wants to do.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/courts/immigrants-ice-arrests-family-separation-children-foster-care/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2178906&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
Six months after a West Virginia man died following a protracted battle with his health insurer over doctor-recommended cancer care, the state’s Republican governor signed a bill intended to curb the harm of insurance denials.
West Virginia’s Public Employees Insurance Agency enrolls nearly 215,000 people — state workers, as well as their spouses and dependents. The new law, which will take effect June 10, will allow plan members who have been approved for a course of treatment to pursue an alternative, medically appropriate treatment of equal or lesser value without the need for another approval from the state-based health plan.
“This legislation is rooted in a simple principle: if a treatment has already been approved, patients should be able to pursue a medically appropriate alternative without being forced to start the process over again — especially when it does not cost more,” Gov. Patrick Morrisey said in a statement after signing the bill into law on March 31.
“This is about common sense, compassion, and trusting patients and their doctors to make the best decisions for their care,” he said.

Delegate Laura Kimble, the Republican from Harrison County who introduced the legislation, told ∫⁄¡œ≥‘πœÕ¯ News the measure offers “a rational solution” for patients facing “the most irrational and chaotic time of their lives.”
From Arizona to Rhode Island, at least half of all state legislatures have taken up bills this year related to prior authorization, a process that requires patients or their medical team to seek approval from an insurer before proceeding with care. These state efforts come as patients across the country await relief from prior authorization hurdles, as promised by dozens of major health insurers in a pledge announced by the Trump administration last year.
The West Virginia law was inspired by Eric Tennant, a coal-mining safety instructor from Bridgeport who died on Sept. 17 at age 58. In early 2025, the Public Employees Insurance Agency of a $50,000 noninvasive cancer treatment, called histotripsy, that would have used ultrasound waves to target, and potentially shrink, the largest tumor in his liver. His family didn’t expect the procedure to eradicate the cancer, but they hoped it would buy him more time and improve his quality of life. The insurer said the procedure wasn’t medically necessary and that it was considered “experimental and investigational.”
Becky Tennant, Eric’s widow, told members of a West Virginia House committee in late February that she submitted medical records, expert opinions, and data as part of several attempts to appeal the denial. She also reached out to “almost every one of our state representatives,” asking for help.
Nothing worked, she told lawmakers, until ∫⁄¡œ≥‘πœÕ¯ News and NBC News got involved and posed questions to the Public Employees Insurance Agency about Eric’s case. Only then did the insurer reverse its decision and approve histotripsy, Tennant said.
“But by then, the delay had already done its damage,” she said.
Within one week of the reversal in late May, Eric Tennant was hospitalized. His health continued to decline, and by midsummer he was no longer considered a suitable candidate for the procedure. “The insurance company’s decision did not simply delay care. It closed doors,” his wife said.
Had the new law been in effect, Kimble said, Tennant could have undergone histotripsy without preapproval, because it was a less expensive alternative to chemotherapy, which his insurer had already authorized. The bill was passed unanimously by the state legislature in March.

U.S. health insurers argue that most prior authorization requests are quickly, if not instantly, approved. AHIP, the health insurance industry trade group, says prior authorization in preventing potential harm to patients and reducing unnecessary health care costs. But denials and delays tend to affect patients who need expensive, time-sensitive care, .
The practice has come under intense scrutiny in recent years, particularly after the in New York City in late 2024. Americans rank prior authorization as their biggest burden when it comes to getting health care, according to a by KFF, a health information nonprofit that includes ∫⁄¡œ≥‘πœÕ¯ News.
Samantha Knapp, a spokesperson for the West Virginia Department of Administration, would not answer questions about the law’s financial impact on the state. “We prefer to avoid any speculation at this time regarding potential impact or actions,” Knapp said.
In a fiscal note attached to the bill, Jason Haught, the Public Employees Insurance Agency’s chief financial officer, said the law would cost the agency an estimated $13 million annually and “cause member disruption.”
West Virginia isn’t an outlier in targeting prior authorization. By late 2025, 48 other states, in addition to the District of Columbia and Puerto Rico, already had some form of a prior authorization law — or laws — on the books, according to a by the National Association of Insurance Commissioners.
Many states have set up “gold carding” programs, which allow physicians with a track record of approvals to bypass prior authorization requirements. Some states establish a maximum number of days insurance companies are allowed to respond to requests, while others prohibit insurance companies from issuing retrospective denials after a service has already been preauthorized. There are also a crop of new state laws seeking to regulate the use of artificial intelligence in prior authorization decision-making.
Meanwhile, prior authorization bills introduced this year across the country, including in Kentucky, Missouri, and New Jersey, have been supported by politicians from both parties.
“Republicans in conservative states see health care as a vulnerability for the midterm elections, and so, unsurprisingly, you’ll see some action on this,” said Robert Hartwig, a clinical associate professor of risk management, insurance, and finance at the University of South Carolina. “They realize that they’re not really going to get much action at the federal level given the degree of gridlock we’ve already seen.”

Last summer, the Trump administration announced a pledge signed by dozens of health insurers vowing to reform prior authorization. The insurers promised to reduce the scope of claims that require preapproval, decrease wait times, and communicate with patients in clear language when denying a request.
Consumers, patient advocates, and medical providers that companies will follow through on their promises.
Becky Tennant is skeptical, too. That’s why she advocated for the West Virginia bill.
“Families should not have to beg, appeal, or go public just to access time-sensitive care,” she told lawmakers. Tennant, who sees the bill’s passage as bittersweet, said she thought her husband would have been proud.
During Eric’s final hospital stay, Tennant recalled, right before he was discharged to home hospice care, she asked him whether he wanted her to keep fighting to change the state agency’s prior authorization process.
“‘Well, you need to at least try to change it,’” she recalled her husband saying. “‘Because it’s not fair.’”
“I told him I would keep trying,” she said, “at least for a while. And so I am keeping that promise to him.”
NBC News health and medical unit producer Jason Kane and correspondent Erin McLaughlin contributed to this report.
Do you have an experience with prior authorization you’d like to share? to tell ∫⁄¡œ≥‘πœÕ¯ News your story.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/prior-authorization-insurance-delays-coverage-denials-state-laws-west-virginia/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2172747&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>State governments rely on such companies to design and operate computer systems that assess whether low-income people qualify for Medicaid or food aid through the Supplemental Nutrition Assistance Program, commonly referred to as food stamps. Those state systems have a history of errors that can cut off benefits to eligible people, a ∫⁄¡œ≥‘πœÕ¯ News investigation showed.
These benefits, provided to the poorest Americans, can mean the difference between someone obtaining medical care and having enough to eat — or going without.
States are now racing to update their eligibility systems to adhere to President Donald Trump’s sweeping tax and domestic spending law. The changes will add red tape and restrictions. They are coming at a steep price ‚Äî both in the cost to taxpayers and coverage losses ‚Äî according to state documents obtained by ∫⁄¡œ≥‘πœÕ¯ News and interviews.
The documents show government agencies will spend millions to save considerably more by removing people from health benefits. While states sign eligibility system contracts with companies and work with them to manage updates, the federal government foots most of the bill.
The law’s Medicaid policies will cause to become uninsured by 2034, according to the nonpartisan Congressional Budget Office. Roughly will lose access to monthly cash assistance for food, including those with children.
In five states alone, for state officials and reviewed by ∫⁄¡œ≥‘πœÕ¯ News show that changes will cost at least $45.6 million combined.
“This is a pretty big payday,” said Adrianna McIntyre, an assistant professor of health policy and politics at Harvard’s T.H. Chan School of Public Health.
The law, which grants tax breaks to the nation’s wealthiest people, requires most states to tie Medicaid coverage for some adults to having a job, and imposes other restrictions that will make it harder for people with low incomes to stay enrolled. SNAP restrictions began to take effect in 2025. Major Medicaid provisions begin later this year.
Documents prepared by consulting company Deloitte estimate that a pair of computer system changes for Medicaid work requirements in Wisconsin will . Two other changes related to the state’s SNAP program will cost an additional $4.2 million, according to the documents, which for the Wisconsin Department of Health Services.
In Iowa, changes to its Medicaid system are expected to cost at least $20 million, , a consulting company that operates the state’s eligibility system.
Optum — which operates the platform Vermont residents use for Medicaid and marketplace health plans under the Affordable Care Act — to evaluate and incorporate new health coverage restrictions.
Initial changes in Kentucky, which has had a contract with Deloitte since 2012, . And in Illinois, will cost at least $12 million.
A Historic Mandate
For six decades after President Lyndon Johnson created the government insurance program in 1965, Congress had never mandated that Medicaid enrollees have a job, volunteer, or go to school.
That will change next year. The tax and spending law enacted by Trump and congressional Republicans requires millions of Medicaid enrollees in 42 states and the District of Columbia to prove they’re working or participating in a similar activity for 80 hours a month, unless they qualify for an exemption. The CBO projected, based on an early version of the bill, that 18.5 million adults would be subject to the new rules ‚Äî .
Vermont Medicaid officials expect it will cost $5 million in fiscal 2027 to implement changes in response to the federal law, said Adaline Strumolo, deputy commissioner of the Department of Vermont Health Access. About $1.8 million is for Optum to make eligibility system adjustments. Optum is a subsidiary of UnitedHealth Group.
The One Big Beautiful Bill Act will subject nearly 55,000 Vermont Medicaid recipients to work requirements ‚Äî about a third of the state’s enrollees.
The law forced the state “to essentially drop everything else we were doing,” Strumolo said in an interview. “This is a big, big lift.”
Optum’s contract with the state was as of October.
of adult Medicaid enrollees nationally are already working, according to KFF. Advocacy groups for Medicaid recipients say work requirements will nonetheless cause significant coverage losses. Enrollees will face added red tape to prove they’re complying. And eligibility systems already prone to error will have to account for employment, job-related activities, and any exemptions.
An estimated 5.3 million enrollees will become uninsured by 2034 due to work requirements, the .
In Wisconsin, state officials estimate could lose coverage after work requirements take effect. Not covering those people would in Medicaid spending for one year.
Wisconsin’s eligibility system for Medicaid and SNAP ‚Äî known as CARES ‚Äî in 1994, and initially was a transfer system from Florida, according to a 2016 state document.
Deloitte submitted its cost estimates for Medicaid and SNAP changes to the state in September and December. Elizabeth Goodsitt, a spokesperson for the Wisconsin Department of Health Services, declined to answer questions about whether additional changes will be needed, how much it will cost to make all eligibility system changes to comply with the new federal law, and whether the state negotiated prices with Deloitte.
Bobby Peterson, executive director of the public interest law firm ABC for Health, said Wisconsin has invested “very little” to help people navigate the Medicaid eligibility process, which soon will become more difficult.
“But they’re very willing to throw $6 million to their contractors to create the bells and whistles,” Peterson said. “That’s where I feel a sense of frustration.”
New Hurdles for Vets and Homeless People
Medicaid work requirements are only one change required by Trump’s tax law that will make it harder to obtain safety-net benefits.
Starting in October, the law prohibits several immigrant populations from accessing Medicaid and ACA coverage, including people who have been granted asylum, refugees, and certain survivors of domestic violence or human trafficking. Beginning Dec. 31, states must verify eligibility twice a year for millions of adults ‚Äî doubling state officials’ workload. And the law restricts SNAP benefits by requiring more adult recipients to work and by removing work exemptions for veterans, homeless people, and former foster youth.
Days after Trump signed the bill in July, Kentucky health officials raced to make changes to the state’s integrated eligibility system, which verifies eligibility for Medicaid, SNAP, and other programs. Deloitte operates the system under a five-year . , initial changes costing $1.6 million were labeled a “high priority” and approved on an “emergency” basis, with some of the changes to the nation’s largest food aid program going into effect almost immediately.
Officials with Kentucky’s Cabinet for Health and Family Services declined to answer a detailed list of questions, including how much it will cost to make all the modifications needed.
Deloitte spokesperson Karen Walsh said the company is working with states to implement new requirements but declined to answer questions about cost estimates in several states. “We are delivering the value and investments we committed to,” Walsh said.
In most states, government agencies rely on contractors to build and run the systems that determine eligibility for Medicaid. Many of those states also use such computer systems for SNAP. But the federal government — that is, taxpayers — to develop and implement state Medicaid eligibility systems and pays 75% of ongoing maintenance and operations expenses, according to federal regulations.
“Five, 10 years ago, I’m not sure if you would hear much mention of SNAP from a Medicaid director,” Melisa Byrd, Washington, D.C.’s Medicaid director, said in November at an annual conference of Medicaid officials. “And particularly for those with integrated eligibility systems ‚Äî as D.C. is ‚Äî¬≠ I’m learning more about SNAP than I ever thought.”
The federal law was the topic du jour at last year’s gathering in Maryland, held at the Gaylord National Resort and Convention Center, the largest hotel between New Jersey and Florida.
Consulting companies had taken notice. Gainwell, an eligibility contractor and one of the conference’s corporate sponsors, emblazoned its logo on hotel escalators. Companies set up booths with materials promoting how they could help states and handed out snacks and swag.
“Conduent helps agencies work smarter by simplifying operations, cutting costs and driving better outcomes through intelligent automation, analytics, and innovation in fraud prevention,” read one such handout from another contractor. “Together, we can better serve residents at every step of their health journeys.” Conduent holds Medicaid eligibility and enrollment contracts in Mississippi and New Jersey, their Medicaid agencies confirmed to ∫⁄¡œ≥‘πœÕ¯ News.
In handouts, Deloitte touted its role in “building a new era in state health care” and as “a national leader in Medicaid program and technology transformation, building a strong track record across the federal, state, and commercial health care ecosystem.” ∫⁄¡œ≥‘πœÕ¯ News found that Deloitte, a global consultancy that generated in revenue in fiscal 2025, dominates this slice of government business.
“With Medicaid Community Engagement (CE) requirements, states are tasked with adding a new condition of Medicaid eligibility to support state and federal objectives,” added another brochure. “Deloitte offers strategic outreach and responsive support to help states engage communities, lower barriers, and address access to coverage.”
A $20.3 Million Bill in Iowa
Before Trump signed the One Big Beautiful Bill Act, Iowa lawmakers wanted to impose their own version of work requirements. They would have applied to 183,000 people before any exemptions. The new law would necessitate a change to Iowa’s Medicaid eligibility system, according to documents prepared by Accenture, which operates Iowa’s system through a .
Adding the ability to verify work status would cost up to $7 million, . By July, the cost to implement the One Big Beautiful Bill Act’s work requirements and other Medicaid provisions . Accenture’s analysis said the federal law necessitated . Making employment a condition of Medicaid benefits could cause an estimated 32,000 Iowans to lose coverage, according to a
Cutting 32,000 people from coverage in one year, a fraction of the Iowa and the federal government spend on Medicaid in a given year.
In Cedar Rapids, most of Eastern Iowa Health Center’s patients rely on Medicaid, CEO Joe Lock said. He questioned the government’s logic of spending tens of millions of dollars on a policy to remove Iowans from Medicaid.
Most of the health center’s patients live at or below the federal poverty level ‚Äî currently .
“There is no benefit to this population,” Lock said.

Danielle Sample, a spokesperson for Iowa’s Department of Health and Human Services, did not answer questions about how much it will cost to implement changes to the state’s separate SNAP eligibility system.
In Illinois, the state’s work this year is largely focused on meeting major provisions of the One Big Beautiful Bill Act. The state estimates that as many as 360,000 residents could lose Medicaid, largely due to the work requirements, said Melissa Kula, a spokesperson for the Illinois Department of Healthcare and Family Services.
Kula confirmed that ‚Äî priced at $12 million ‚Äî is related to Trump’s law. The estimate also mentions other work. Kula said Deloitte is charging the state a $2 million fixed fee related to work requirements.
The Trump administration has acknowledged that the work is coming at a cost. In January, top officials for the Centers for Medicare & Medicaid Services said government contractors, including Deloitte, Accenture, and Optum, have and reduced rates through 2028 to help states incorporate system changes.
“The companies were extremely excited to do this,” , the top CMS Medicaid official. “Everyone’s really focused on getting to work.”
CMS spokesperson Catherine Howden declined to answer questions about the discounts.
Goodsitt, the Wisconsin Medicaid spokesperson, declined to answer questions about whether Deloitte has discounted its rates. Officials with Kentucky’s Cabinet for Health and Family Services did not answer a detailed list of questions, including whether Deloitte extended discounts to make these changes.
It’s unclear what discounts, if any, Deloitte and Accenture have offered to individual states. Walsh, the Deloitte spokesperson, declined to answer detailed questions about the discounts the Trump administration announced this year. Accenture did not respond to repeated requests for comment.
Strumolo, the Vermont health official, said state officials discussed the announcement with Optum “in detail.”
Optum for a specific module related to Medicaid work requirements. That product is unworkable for Vermont because it would mean “moving to a new system when we don’t have to.” When asked about whether the company offered discounts, Strumolo said “not explicitly.”
In a statement, UnitedHealth Group spokesperson Tyler Mason said Optum supports state implementation of new federal requirements “with a range of options to meet their unique cost and policy needs.”
He declined to specify whether Optum discounted Vermont’s rates and how it calculated the costs of doing its work. “Optum is helping mitigate upfront implementation expenses so states can focus on approaches that reduce duplication, accelerate implementation, and manage costs over time ‚Äî supporting better outcomes for individuals covered by Medicaid,” Mason said.
Strumolo said Optum’s initial changes in Vermont cover items that take effect this year and in 2027 ‚Äî Medicaid work requirements, checking eligibility every six months, and prohibiting certain immigrants from qualifying for health programs.
“There’s a lot more that could come,” she said.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/state-medicaid-work-requirements-eligibility-systems-deloitte-accenture-optum/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2174991&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>“I call it the unaffordable care act,” he said. He reprised the line in his address, blaming “the crushing cost of health care” on Obamacare.
Trump’s words also play off an ongoing congressional debate that began late last year with the expiration of the enhanced tax subsidies that had lowered the cost of ACA insurance for millions of Americans ‚Äî and thrust the issue of ACA-related costs back to center stage.
Without those enhanced subsidies, the amount people pay toward monthly Obamacare premiums doubled, on average. The number of people enrolled in ACA coverage for this year has dropped by more than a million, and experts say more people could abandon coverage once premiums come due. Democrats are using this development to crank up the heat on Republicans ahead of the November elections and steer the conversation on the affordability issue.
Republicans fault the law itself for driving up these costs. For instance, Rep. Mike Lawler (R-N.Y.) that premiums “skyrocketed across the country since it took effect.”
Critics routinely point to several provisions within the ACA as the culprits — among them, essential health benefits, or EHBs. Under the law, Obamacare plans must cover certain essential services, including emergency care, hospitalization, maternity, and prescription drugs, without annual or lifetime dollar limits. But connecting EHBs to the premium increases felt by consumers is not straightforward.
Here’s a primer on key issues involved.
Checking the Numbers
It’s clear that Obamacare premiums have increased.
An analysis by the right-leaning Paragon Health Institute shows that the average premium for a 50-year-old with Obamacare since 2014. The average premium for employer-based plans grew 68% during that same time.
Paragon’s president, , told ∫⁄¡œ≥‘πœÕ¯ News that this shows the ACA has made health care on the individual market more expensive.
Still, the comparison overlooks a couple of points. Pre-ACA, employer plans generally offered more generous coverage than individual market plans, so work-based coverage cost more. And individual plans were cheaper in part because they could bar applicants with health problems. Beginning in 2014, the ACA forced individual policies to look more like employer plans, covering a broader range of benefits and accepting both healthy and unhealthy applicants. As a result, premiums rose that first year. In the years that followed, ACA plans often experienced faster growth in premiums than job-based plans. Some policy analysts say this isn’t surprising because ACA plans started at a lower dollar base and had more room to rise.
States that saw less dramatic post-ACA premium increases, such as Massachusetts and New York, already mandated that individual-market plans provide EHB-like coverage, noted , a senior research fellow at the Heritage Foundation, a conservative think tank. These states also had higher premiums due to that and other provisions, such as not allowing plans to exclude people with preexisting conditions.
“It was a combination of things,” he said.
Blase acknowledges that the two types of insurance started at different price points. But he said the percentage change over time shows that the ACA faces “underlying inflationary pressures” ‚Äî including the now-expired, more generous, covid pandemic-era subsidies ‚Äî that affect its policyholders more so than employer plans.
Aside from that point, however, were on the rise even before the ACA took effect.
An analysis by Jonathan Gruber at the Massachusetts Institute of Technology found that between 2008 and 2010, premiums grew by at least 10% a year and were highly variable across states and insurers.
Consumers’ Other Costs
Over time, ACA deductibles ‚Äî the amounts policyholders must satisfy in a given year before insurance kicks in ‚Äî have seen large increases, with “bronze” plans now averaging $7,476 annually, up from $5,113 in 2014, according to KFF, a health information nonprofit that includes ∫⁄¡œ≥‘πœÕ¯ News. Bronze plans tend to have lower premiums than the other metal-level categories ‚Äî “silver,” “gold,” and “platinum” ‚Äî in part because of their higher deductibles.
The Trump administration is doubling down on high-deductible plans as part of its emphasis on affordability, making it easier this year for people age 30 and up to qualify for what are called “catastrophic plans.” These come with even larger deductibles than bronze plans.
The administration to cement those changes, saying it was designed to lower premiums and expand choices. It would raise next year’s deductibles for catastrophic plans to $15,600 a year for an individual or around $30,000 for a family. It isn’t clear how popular such plans would be. Detailed enrollment figures for this year are not yet available, but estimates indicate chose catastrophic plans in 2025, and consumers can’t use federal subsidies to purchase them.
Before this Trump proposal, though, recent data showed that the rising rate of ACA plan deductibles had not outpaced deductibles for employer plans.
The weighted average ‚Äî a calculation that gives more weight to ACA plans with the most people enrolled ‚Äî shows in annual deductible amounts since 2014, from $1,881 to $2,912. During that same period, deductibles in plans offered by 59%, from $1,186 to $1,886, according to KFF’s annual employer survey.
Essential What?
To be clear, the ACA’s catastrophic and bronze plans must cover essential health benefits, as do all Obamacare plans. These EHBs fall into 10 categories of medical services and were included in the ACA to ensure individual policies meet a minimum standard of coverage and are comparable to employer-based health insurance.
Preventive services, such as annual checkups, vaccines, and certain cancer screenings, must be covered at no additional cost to patients. All plans must completely cover the cost of specific vaccines, including the annual flu shot. And insurers cannot refuse to pay for emergency care provided at an out-of-network hospital. Other EHBs are subject to out-of-pocket costs, such as copays at the doctor’s office or pharmacy counter.
In some ways, EHBs save money because they’ve increased access to preventive care, said , a professor of health policy and management at Johns Hopkins University’s Bloomberg School of Public Health.
Services such as cancer screenings and lab tests can lead to earlier detection of serious conditions, when treatment is less costly, and positive outcomes are more likely.
“If you look down the list of essential health benefits, I think most people would reach the judgment that those are health care services that people should have access to,” said Larry Levitt, KFF’s executive vice president for health policy.
Joseph Antos, a senior fellow emeritus at the conservative American Enterprise Institute, said ACA requirements ‚Äî such as requiring insurers to accept anyone, regardless of their health status, and limiting insurers’ ability to charge older people more for coverage ‚Äî also have played roles in boosting premiums.
“Really, it’s practically impossible to tease any one thing out,” Antos said.
States do have latitude to add benefits that fall under the EHB umbrella. For example, bariatric surgery is covered as an EHB in , but not in . Pennsylvania’s EHBs also don’t include hearing aids, but do.
But the Trump administration’s 2027 regulatory proposal : When “states enact benefit mandates, plan premiums must generally increase to account for the additional coverage,” it reads. It also signals that added benefits can raise consumer costs and proposes that states be required to use their own funds to offset some of those costs.
Paragon’s Blase echoed this take in his bottom line. Mandating that plans cover EHBs without annual or lifetime caps, as required under the ACA law, encourages clinicians to overbill and overprescribe, he said. That drives up premiums and means a bigger check for insurers and medical providers at the expense of taxpayers. “You just turn patients into money factories,” he said.
, a senior research fellow at Georgetown University’s Center on Health Insurance Reforms, disagrees, saying that whatever EHBs’ role, they aren’t to blame for the year-over-year premium hikes.
People aren’t consuming medical care at exponential rates just because certain services are now covered: “Me not paying anything for that colonoscopy doesn’t make me want to get more of them,” she said.
Are you struggling to afford your health insurance? Have you decided to forgo coverage? to contact ∫⁄¡œ≥‘πœÕ¯ News and share your story.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/obamacare-essential-health-benefits-premium-costs-debate/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2164137&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>After Health and Human Services Secretary Robert F. Kennedy Jr. fired Centers for Disease Control and Prevention Director Susan Monarez for refusing what her lawyers called “,” Newsom to help modernize California’s public health system. He also gave a job to Debra Houry, the agency’s former chief science and medical officer, who had resigned in protest hours after Monarez’s firing.
Newsom also teamed up with fellow Democratic governors Tina Kotek of Oregon, Bob Ferguson of Washington, and Josh Green of Hawaii to form the , a regional public health agency, whose guidance would “uphold scientific integrity in public health as Trump destroys” the CDC’s credibility. Newsom argued establishing the independent alliance was vital as Kennedy leads the Trump administration’s rollback of national vaccine recommendations.
More recently, California became the a global outbreak response network coordinated by the World Health Organization, followed by Illinois and New York. Colorado and Wisconsin signaled they plan to join. They did so after President Donald Trump officially from the agency on the grounds that it had “strayed from its core mission and has acted contrary to the U.S. interests in protecting the U.S. public on multiple occasions.” Newsom said joining the WHO-led consortium would enable California to respond faster to communicable disease outbreaks and other public health threats.
Although other Democratic governors and public health leaders have openly criticized the federal government, few have been as outspoken as Newsom, who is considering a run for president in 2028 and is in his second and final term as governor. Members of the scientific community have praised his effort to build a public health bulwark against the Trump administration’s slashing of funding and scaling back of vaccine recommendations.
What Newsom is doing “is a great idea,” said Paul Offit, an outspoken critic of Kennedy and a vaccine expert who formerly served on the Food and Drug Administration’s vaccine advisory committee but was removed under Trump in 2025.
“Public health has been turned on its head,” Offit said. “We have an anti-vaccine activist and science denialist as the head of U.S. Health and Human Services. It’s dangerous.”
The White House did not respond to questions about Newsom’s stance and HHS declined requests to interview Kennedy. Instead, federal health officials criticized Democrats broadly, arguing that blue states are participating in fraud and mismanagement of federal funds in public health programs.
HHS spokesperson Emily Hilliard said the administration is going after “Democrat-run states that pushed unscientific lockdowns, toddler mask mandates, and draconian vaccine passports during the covid era.” She said those moves have “completely eroded the American people’s trust in public health agencies.”
Public Health Guided by Science
Since Trump returned to office, Newsom has criticized the president and his administration for engineering policies that he sees as an affront to public health and safety, labeling federal leaders as “extremists” trying to “weaponize the CDC and spread misinformation.” He has for erroneously linking vaccines to autism, the administration is endangering the lives of infants and young children in scaling back childhood vaccine recommendations. And he argued that the White House is unleashing “chaos” on America’s public health system in backing out of the WHO.
The governor declined an interview request. Newsom spokesperson Marissa Saldivar said it’s a priority of the governor “to protect public health and provide communities with guidance rooted in science and evidence, not politics and conspiracies.”
The Trump administration’s moves have triggered financial uncertainty that local officials said has reduced morale within public health departments and left states unprepared for disease outbreaks and . The White House last year proposed cutting HHS spending , including . Congress largely rejected those cuts last month, although funding for programs focusing on social drivers of health, such as access to food, housing, and education, .
The Trump administration announced that it would claw back in public health funds from California, Colorado, Illinois, and Minnesota, arguing that the Democratic-led states were funding “woke” initiatives that didn’t reflect White House priorities. Within days, and a judge the cut.
“They keep suddenly canceling grants and then it gets overturned in court,” said Kat DeBurgh, executive director of the Health Officers Association of California. “A lot of the damage is already done because counties already stopped doing the work.”
Federal funding has accounted for of state and local health department budgets nationwide, with money going toward fighting HIV and other sexually transmitted infections, preventing chronic diseases, and boosting public health preparedness and communicable disease response, according to a 2025 analysis by KFF, a health information nonprofit that includes ∫⁄¡œ≥‘πœÕ¯ News.
Federal funds account for $2.4 billion of California’s $5.3 billion public health budget, making it difficult for Newsom and state lawmakers to backfill potential cuts. That money helps fund state operations and is vital for local health departments.
Funding Cuts Hurt All
Los Angeles County public health director Barbara Ferrer said if the federal government is allowed to cut that $600 million, the county of nearly 10 million residents would lose an estimated $84 million over the next two years, in addition to other grants for prevention of HIV and other sexually transmitted infections. Ferrer said the county depends on nearly $1 billion in federal funding annually to track and prevent communicable diseases and combat chronic health conditions, including diabetes and high blood pressure. Already, the the closure of that provided vaccinations and disease testing, largely because of funding losses tied to federal grant cuts.
“It’s an ill-informed strategy,” Ferrer said. “Public health doesn’t care whether your political affiliation is Republican or Democrat. It doesn’t care about your immigration status or sexual orientation. Public health has to be available for everyone.”
A single case of measles requires public health workers to track down 200 potential contacts, Ferrer said.
The U.S. but is close to losing that status as a result of vaccine skepticism and misinformation spread by vaccine critics. The U.S. had , the most since 1991, with 93% in people who were unvaccinated or whose vaccination status was unknown. This year, the highly contagious disease has been reported at , , and .
Public health officials hope the West Coast Health Alliance can help counteract Trump by building trust through evidence-based public health guidance.
“What we’re seeing from the federal government is partisan politics at its worst and retaliation for policy differences, and it puts at extraordinary risk the health and well-being of the American people,” said Georges Benjamin, executive director of the American Public Health Association, a coalition of public health professionals.
Robust Vaccine Schedule
Erica Pan, California’s top public health officer and director of the state Department of Public Health, said the West Coast Health Alliance is defending science by recommending a vaccine schedule than the federal government. California is part of a coalition over its decision to rescind recommendations for seven childhood vaccines, including for hepatitis A, hepatitis B, influenza, and covid-19.
Pan expressed deep concern about the state of public health, particularly the uptick in measles. “We’re sliding backwards,” Pan said of immunizations.
Sarah Kemble, Hawaii’s state epidemiologist, said Hawaii joined the alliance after hearing from pro-vaccine residents who wanted assurance that they would have access to vaccines.
“We were getting a lot of questions and anxiety from people who did understand science-based recommendations but were wondering, ‚ÄòAm I still going to be able to go get my shot?’” Kemble said.
Other states led mostly by Democrats have also formed alliances, with Pennsylvania, New York, New Jersey, Massachusetts, and several other East Coast states banding together to create the .
HHS’ Hilliard said that even as Democratic governors establish vaccine advisory coalitions, the federal “remains the scientific body guiding immunization recommendations in this country, and HHS will ensure policy is based on rigorous evidence and gold standard science, not the failed politics of the pandemic.”
Influencing Red States
Newsom, for his part, has approved a recurring annual infusion of nearly $300 million to support the state Department of Public Health, as well as the 61 local public health agencies across California, and last year authorizing the state to issue its own immunization guidance. It requires health insurers in California to provide patient coverage for vaccinations the state recommends even if the federal government doesn’t.
Jeffrey Singer, a doctor and senior fellow at the libertarian Cato Institute, said decentralization can be beneficial. That’s because local media campaigns that reflect different political ideologies and community priorities may have a better chance of influencing the public.
A KFF analysis found some red states are joining blue states in decoupling their vaccine recommendations from the federal government’s. Singer said some doctors in his home state of Arizona are looking to more liberal California for vaccine recommendations.
“Science is never settled, and there are a lot of areas of this country where there are differences of opinion,” Singer said. “This can help us challenge our assumptions and learn.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/gavin-newsom-california-public-health-fight-west-coast-alliance-trump-hhs-rfk/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2164665&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The city’s mobile crisis team had just gotten a call about a man walking around outside without shoes. The man’s family told the team he was having a mental health crisis and wouldn’t come inside.
As they drove down the highway toward the city’s outskirts, team member Evan Thiessen spoke with the relative who had reached out.
“You’re doing the right thing, and we’re going to make sure he gets help today, OK?” he said.
They pulled up the man’s police record on a laptop and saw that he did have a record of some previous encounters with police, including some that had turned violent.
, a licensed therapist, had that in mind as they pulled into a neighborhood of single-family homes. He stepped out of the Ford Bronco and headed toward the front door.
A Funding Problem
Many communities around the country send out teams like this one to help people in psychiatric crisis, rather than dispatching regular police.
A found there were at least 1,800 mobile teams nationwide in 2023. But financial support for them is often inadequate and inconsistent, leaving many communities struggling to keep the teams operating.
Two programs — one in Great Falls, in central Montana, and one in Billings, in south-central Montana — recently shut down. Six units remain in Montana.
The strategy in Eugene, Oregon, but gained momentum nationally over the past 10 years.
Recent about police killing people who are experiencing a psychiatric crisis have sparked conversations about how to safely and effectively respond. Most police officers are not trained to deal with people experiencing delusions or hallucinations, nor to de-escalate situations involving threatening behaviors to themselves or others.
An across 27 states found that about a third of the victims showed signs of being in crisis. Another study found that people with a serious mental illness were at least to experience use of force by police as those without.
By contrast, crisis response teams have been trained to de-escalate such situations and provide appropriate therapeutic care.
When the team arrived at the house in Bozeman, the man had already gone back inside. The team then talked with the man’s family for about half an hour and helped them devise a plan to keep him at home ‚Äî and safe. Before they left, team members determined the man wasn’t a threat to himself or others.
Also, they planned to follow up within a few days to connect him with ongoing mental health care. After an encounter with the team, some clients might need follow-up therapy, assistance with psychiatric medications, or help finding treatment for substance abuse.
The Bozeman team is available 12 hours a day, seven days a week, and costs roughly $1 million a year to run.
Police departments are generally funded by local taxpayers. Mobile crisis teams don’t have a single, reliable source of funding.
Some, despite successful operations and , are or have closed entirely. One that shuttered was Oregon’s .
Most crisis calls end with people staying where they are, avoiding a trip to the emergency room or going to jail, according to , which runs the mobile crisis program in Bozeman.
Beyond police and firefighters, members of the public can call the team directly.
“I’ve been out on calls where individuals have barricaded themselves in residences or in their vehicles with a firearm. So, helping to assist not only law enforcement, the negotiators, but consulting on the behavioral health side of that,” said Ryan Mattson, who leads the Bozeman crisis team.

The program has reduced the time that Bozeman police officers must spend on mental health calls by nearly 80%, according to Mattson, and prevented unnecessary ER visits.
Residents and political leaders see that value, he said, but finding a way to pay for the service has been difficult.
“I’m confident we’ll be here through next fiscal year. That’s about as confident as I am at this point,” Mattson said.
Mobile crisis programs in Montana, which began operating about five years ago, have cost more than the state originally projected.
Health insurance is sometimes a revenue source for mobile crisis teams. That’s because a crisis call is a type of mental health service, provided by trained professionals such as therapists or crisis intervention specialists. Still, many private insurance companies don’t reimburse for mobile crisis services.
What Medicaid Pays For ‚Äî And Doesn’t
Medicaid, the government-funded insurance program for low-income and disabled Americans, is another funding source. Two-thirds of states allow Medicaid reimbursement for such calls, but rates vary.
In Montana, Medicaid reimburses the team only for the time they spend responding to a call in the field. Additional time spent on a case ‚Äî documenting the encounters, or waiting for the next call ‚Äî isn’t reimbursed.
“You need to pay for the capacity to be at the ready, just like we do with fire or police, regardless of whether somebody is going to be called out,” said of Inseparable, a nonprofit that advocates for mental health policy reform.
It’s not feasible for mobile crisis teams to rely solely on reimbursement from insurance companies, she said.
To deal with the shortfalls, many mobile teams rely on a patchwork of grants and other funding, according to , who studies Medicaid policy at KFF, a health information nonprofit that includes ∫⁄¡œ≥‘πœÕ¯ News.
Some state governments have stepped in to help.
Eight states, including New Jersey, California, and Washington, mandate that private insurers cover the cost of mobile crisis calls for people on their plans, according to Kimball. At least 10 states have implemented fees on cellphone bills to help pay for service.
Montana hasn’t followed suit.
The state provides about $2 million annually in supplemental funds to help the mobile teams pay for service calls that aren’t reimbursed through Medicaid, according to an emailed statement from Jon Ebelt, a state health department spokesperson.
But program managers counter that the paperwork to access that funding is complicated and often isn’t worth the staff time.
Will Montana Step In?
Despite this state support, mobile teams are still struggling to stay afloat, Ebelt acknowledged. He said Montana officials are considering boosting what Medicaid reimburses for each service call.
In Missoula, the mobile crisis team turned to local taxpayers for additional help. Their annual expenditure is $1.4 million, but Medicaid reimbursements were covering only about 20% of the cost, according to program manager John LaRocque. Even with local tax dollars, the program faces a $250,000 shortfall, so LaRocque is looking for grants.

Mobile crisis is still a relatively new concept, and growing pains are to be expected, said Sierra Riesberg, director of the .
Still, abrupt closures create instability and lead some patients to the ER, placing financial pressure on another distressed part of the local health system.
“A much-needed service is available and then not available, available and then not available. These things need to be taken into consideration when developing programs in communities,” she said.
If more mobile crisis teams shut down, that might interfere with Montana’s recent efforts to overhaul an outdated and underfunded mental health system. The state’s only psychiatric hospital hasn’t kept up with the to the facility.
Later this year, Montana hopes to join a federal pilot program to open a new type of clinic: , or CCBHCs. Those clinics will receive boosted levels of federal funding, but they are required to offer round-the-clock mobile crisis services as well as other crisis care.
That could be a tall order for rural communities, said , an executive at in Great Falls.
Alluvion used to operate the mobile crisis team in Great Falls before it shuttered the service. One major reason it closed was that the expected Medicaid payments covered less than anticipated. Before Alluvion would consider getting involved again, the state would need to “completely revamp” the way the service is funded, Schreiner said.
“Is it a priority for our state or not?” he asked.
This article is from a partnership with and .
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/police-mental-health-calls-988-911-mobile-crisis-teams-funding/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2159605&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But plans to spend those nine-digit awards aren’t all warmly received.
At least one group of Republican state lawmakers appears to have scuttled an initiative preapproved by federal officials. And at least one hospital association persuaded its state health leaders to alter who greenlights spending. Other critics are taking a more cautious approach.
That’s because the Centers for Medicare & Medicaid Services, which manages the five-year Rural Health Transformation Program, says states could lose money if they make major changes to the plans approved in their applications. Changes could also delay states’ ability to get projects rolling in time to show the agency that they’re meeting progress deadlines.
“During the application period, states were advised to only propose initiatives and state policy actions that the state deemed feasible,” said CMS spokesperson Catherine Howden, who noted that the agency will work with states case by case.
The recent pushback reflects “tension” over state plans ‚Äî which were approved by the federal government ‚Äî from state lawmakers and health leaders who want more input amid tight deadlines, said Carrie Cochran-McClain, chief policy officer of the National Rural Health Association, the largest organization representing rural hospitals and clinics.
Cochran-McClain said many states must pass a bill to allow federal dollars to be spent and added that because the program rolled out so quickly “there’s important work that still needs to be done in some states between the legislatures and the governors.”
State lawmakers want to have a say, she said, in “how the funding is being allocated ‚Äî how the implementation will go.”
Congressional Republicans created the program as a last-minute sweetener to include in their One Big Beautiful Bill Act, signed into law last summer. The funding was intended to offset concerns about the anticipated in rural communities from the law, which is expected to slash Medicaid spending by nearly $1 trillion over a decade.
CMS officials announced first-year funding — ranging from $147 million for New Jersey to $281 million for Texas — on Dec. 29, after scoring applications. Federal officials will begin evaluating progress in late summer and announce 2027 allocations at the end of October.
A chorus of critics say the program won’t make up for harm caused by Medicaid cuts.
The program is “a complete sham,” Sen. Ron Wyden (D-Ore.) said at a rural policy conference in February.
Medicaid, a joint federal-state program for low-income and disabled Americans, serves nearly , and many rural hospitals depend on it to stay afloat.
But the rural health program tilts toward seeding innovative projects and technologies, not shoring up rural hospital finances. States can use only up to 15% of their funding to pay providers for patient care.
That hasn’t stopped some federal officials and lawmakers from framing the program as a rural hospital rescue.
For example, the White House , “President Trump secured $50 billion in funding for rural hospitals.”
Now that applications have been approved, some state Republican lawmakers ‚Äî who are than Democrats are ‚Äî and hospital associations are upset that the political rhetoric doesn’t match what they see.
They’re also lobbing criticisms at specific aspects of their states’ plans, including the proposed projects, what’s not included, and the spending approval process.
In Wyoming, lawmakers didn’t just criticize an initiative from their state’s application. They moved to kill it.
State Rep. John Bear, a Republican, said he and other lawmakers declined to fund “BearCare,” a proposed state-sponsored health insurance plan that patients could use only after medical emergencies. But they did approve other aspects of the rural health program.
The Wyoming Department of Health won’t “proceed with BearCare without express legislative authority to do so,” said spokesperson Lindsay Mills.
While Wyoming lawmakers removed an initiative from their state’s rural health plan, a group in Ohio wants to add something.
Ohio Rep. Kellie Deeter and other Republican lawmakers to use the maximum allowed funding for provider payments — 15% — to support 13 independent, rural hospitals.
“We understand that the rural transformation fund is not designed to be given directly to prop up hospitals,” Deeter said. “We just want to capitalize on the mechanism of the fund that can be utilized for that purpose.”
Those hospitals “operate with very, very narrow margins, and it’s just difficult and, frankly, unsustainable,” she added.
Ken Gordon, a press secretary responding for the governor’s office and the state health department, said, “It’s still very early in this process, and many details are being worked out.”
State lawmakers around the country are also trying to ensure the federal program’s dollars benefit rural areas.
In North Dakota, Rep. Bill Tveit, a Republican who lives in a town with about 2,000 residents, that would have required the state to reserve its funding for programs located more than 35 miles from urban areas and small cities.
During a hearing, lawmakers appeared sympathetic to Tveit’s concerns but quickly shot down his idea.
State Sen. Brad Bekkedahl said the North Dakota health department already committed to prioritizing funding for the most pressing rural health needs. He also said he’s concerned any significant changes could cause the state to lose funding because CMS already reviewed and approved the plan.
Meanwhile, Republican lawmakers in Michigan and North Carolina have criticized their states’ definitions of “partially rural” or “rural,” saying that counties that include urban population centers could take money from lower-density counties, according to and .
Lawmakers aren’t the only ones speaking out.
The Colorado Hospital Association to state lawmakers denouncing how the state created its plan and two of its proposed initiatives.
“Not only were Colorado’s rural hospitals’ recommendations disregarded,” president and CEO Jeff Tieman wrote, but the plan includes ideas “they actively oppose and believe will harm the communities they serve.”
The department responded to one of the association’s concerns by adding rural health leaders to the .
Meanwhile, and Nebraska, some health groups are upset that their states’ plans lack specific funding streams for rural hospitals.
Lauren LaPine-Ray, who oversees rural health policy at the Michigan Health & Hospital Association, predicted the state’s rural hospitals will compete with other organizations, such as academic centers and health clinics, for funding. She said about 65% of the group’s rural members have never applied for a state grant before.
“The rural hospitals, the ones that really need the funding the most, will not be well equipped to apply for and pull down these dollars,” LaPine-Ray said.
Jed Hansen, executive director of the Nebraska Rural Health Association, said the federal funding won’t go to “rural hospitals, rural clinics, and rural providers in a meaningful way.”
“Rural Health Transformation will not save a single hospital in our state,” he said. “I don’t think it will save a hospital nationally.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/rural-transformation-fund-lawmakers-health-groups-resist-state-spending-plans/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2161929&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Finally, after decades of advocacy, the Biden administration in 2023 tackled the problem of perennial understaffing of long-term care facilities. Officials backed a Medicare regulation that would mandate at least 3.48 hours of care from nurses and aides per resident, per day, and would require a registered nurse on-site 24 hours a day, seven days a week.
The mandated hours were lower than supporters hoped for, said Hunter, who directs Washington state’s long-term care ombudsman program. But “I’m a pragmatic person, so I thought, this is a good start,” she said. “It would be helpful, for enforcement, to have a federal law.”
In 2024, when the Centers for Medicare & Medicaid Services adopted the standards, advocates celebrated. But industry lawsuits soon blocked most of the rule, with two federal district courts finding that Medicare had exceeded its regulatory authority.
And after the 2024 elections, Hunter said, “I was concerned about the changing of the guard.” Her concerns proved well founded.
In July, as part of Republicans’ One Big Beautiful Bill Act, Congress prohibited Medicare from implementing the staffing standards before 2034. Last month, CMS altogether. They never took effect.
“It was devastating,” Hunter said.
As with environmental law and consumer protections, the Trump administration’s enthusiasm for deregulation has undone long-sought rules to improve care for the aged. And it has introduced , now getting underway in six states, that has alarmed advocates, congressional Democrats, and a good number of older Americans.
Taken together, the moves will affect many of the facilities and workers providing care and introduce complications in health coverage in several states.
On the nursing home front, “it’s clear CMS has no interest in ensuring adequate staffing,” said Sam Brooks, the director of public policy for the National Consumer Voice for Quality Long-Term Care.
“They’re repealing a regulation that could have saved 13,000 lives a year,” he added, citing by University of Pennsylvania researchers.
Industry groups argued that nursing homes, with high rates of staff turnover, were already struggling to fill vacancies.
The staffing mandate “was requiring nursing homes to hire an additional 100,000 caregivers that simply don’t exist,” said Holly Harmon, a senior vice president at the American Health Care Association.
The organization had brought one of the suits that largely vacated the rule. “Facilities would have been forced to limit admissions or downsize to comply with the requirements, or close altogether,” Harmon said.
For supporters, the action is now likely to shift to updating requirements in 35 states, along with the District of Columbia, that have already established , and to developing them in those that haven’t.
Rules for Home Help
A second rescinded regulation, this one more unexpected, brought about upheaval in July, when the Labor Department announced a return to from the federal Fair Labor Standards Act.
Some history: Dating back to the New Deal, the FLSA mandated that workers receive the federal minimum wage (currently $7.25 an hour) and overtime pay. It exempted most “domestic service workers” until 1975, when a new Labor Department regulation included them ‚Äî with the exception of home care workers.
“There was a misinterpretation of home care work as being casual, nonprofessional, non-skilled,” the equivalent of teenage babysitting, said Kezia Scales, a vice president at PHI, a national research and advocacy organization. “Just someone popping into your mother’s house now and then and keeping her company.”
For almost 40 years, workers and their supporters lobbied to change the rule, seeing it as a contributor to the low wages and meager benefits of a swiftly growing workforce, one made up primarily of women and minority groups, with many immigrants.
In 2013, the Labor Department responded with a rule that , entitled to minimum wage, time and a half for overtime work, and payment for travel time between clients.
After industry lawsuits failed to overturn it, “everything settled down,” Scales said. “It was in place successfully for a decade.”
Home care workers brought hundreds of compliance complaints annually. In 87% of them, the Labor Department found , according to a 2020 Government Accountability Office report.
Since 2013, home care agencies have paid about , PHI has calculated.
Then in July, the Labor Department abruptly announced that it would return to the 1975 regulations and , which it said “had negative effects on the ground” and hindered consumer access to care.
The agencies employing most home care workers, primarily funded through Medicaid, would agree. “Many workers never got any benefit from this,” said Damon Terzaghi, a vice president at the National Alliance for Care at Home.
“States made a lot of moves to essentially absolve themselves of any responsibility,” he said. A 2020 federal report, for example, found that 16 states had at 40, thus averting overtime payment.
The alliance, which estimates that the number of impacted agencies and businesses has declined by 30% since 2013, supported the rescission. Scales, who hopes for congressional action, called it “a shocking step backward.”
Where they concur is that the United States has never really committed to sufficiently funding long-term care at home. With the July legislation setting the stage for a over the coming decade, that seems unlikely to change anytime soon.
Medicare’s AI Referee
Beyond rolling back policies for care of the aged, the Trump administration has established a pilot program to introduce one to traditional Medicare: prior authorization, using artificial intelligence and machine learning technologies.
Touting it as a boon to taxpayers, Medicare calls it WISeR — Wasteful and Inappropriate Service Reduction.
, in which private insurers review proposed treatments before agreeing to pay for them, is widely used in Medicare Advantage plans despite its unpopularity with patients, doctors, and health care organizations. It has rarely been used in traditional Medicare.
This month, however, in six states (Arizona, New Jersey, Ohio, Oklahoma, Texas, Washington) in a six-year trial to determine whether review by tech companies can reduce costs and improve efficiency, while maintaining or improving quality of care.
Initially, that CMS said “historically have had a higher risk of waste, fraud and abuse.” The list includes knee arthroscopy for arthritis, electrical nerve stimulation devices for several conditions, and treatment for impotence.
The pilot program excludes emergency services and inpatient hospital care, or care where delay poses “a substantial risk.” Algorithmic denials will trigger review by “an appropriately licensed human clinician.” The tech companies get “a share of averted expenditures.”
“It injects some of the worst of Medicare Advantage into traditional Medicare,” said David Lipschutz, co-director of the Center for Medicare Advocacy. The six vendors that approve or reject treatments “have a financial stake in the outcomes,” he said, and therefore “an incentive to deny care.”
Moreover, the CMS Innovation Center overseeing the pilot could theoretically bypass Congress and expand prior authorization to include more medical services in more states.
The agency did not respond to questions about what kind of human clinicians would review denials, except to say that they would have “relevant experience” and that tech companies would be “financially penalized for inappropriate denials, high appeal rates or poor performance.”
It plans an “independent, federally funded evaluation” and will release public reports annually.
Democrats in Congress have in both houses to repeal WISeR. “We should be reducing red tape in Medicare, not creating new hurdles that second-guess health care providers,” said Rep. Suzan DelBene of Washington, one of the bill’s sponsors.
For now, though, WISeR has opened for business, receiving prior authorization requests through its electronic portals.
“The New Old Age” is produced through a partnership with .
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/aging/long-term-care-nursing-homes-medicare-ai-prior-authorization/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2144663&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But there are strings attached.
In late December, President Donald Trump’s administration announced how much all 50 states would get under its new Rural Health Transformation Program, assigning them to use the money to fix systemic problems that leave rural Americans without access to good health care. Now, the clock is ticking.
Within eight months, states must submit revised budgets, begin spending, and show the money is going to good use. Federal officials will begin reviewing state progress in late summer and announce 2027 funding levels by the end of October.
The money — divided into unique allocations for each state, ranging from $147 million for New Jersey to $281 million for Texas — represents the first $10 billion installment from the five-year, $50 billion program. Congress created the fund as a last-minute sweetener in Trump’s One Big Beautiful Bill Act last summer to offset the anticipated in rural communities from the statute’s nearly $1 trillion in Medicaid spending cuts over the next decade.
Federal officials crafted the fund to give states “space to be creative,” Mehmet Oz, administrator of the Centers for Medicare & Medicaid Services, said on a call with reporters after announcing the funding Dec. 29. “Some states will fail, and we will learn from that.”
The money was divided according to a complicated formula.
In 2026, each state will receive an equal $100 million share for the first half of the money, plus additional funding from the second half. Oz’s staff steered payouts from the second portion based on each state’s rural score, as well as results from a “technical” scoring system for project proposals.
Within hours of the announcement, academics and researchers began to parse the awards to better understand why some states received more than others, including whether the awards reflected any partisanship or political favoritism.
At first glance, total awards do not appear to favor states governed by either Republicans or Democrats. But teased out the amount awarded for each state’s technical score, which is the part determined by the discretion of agency officials.
The analysis was performed at the University of North Carolina’s Cecil G. Sheps Center for Health Services Research, which specializes in rural health. A ∫⁄¡œ≥‘πœÕ¯ News review of the Sheps Center data found that states with Republican governors tended to receive more money for the parts of their application based on the technical score. Democratic-controlled states crowded the bottom quarter of those technical score awards.
Overall, though, the state awards reveal wild variation in how much money each state will get per rural resident, almost a hundredfold difference between the top and bottom.
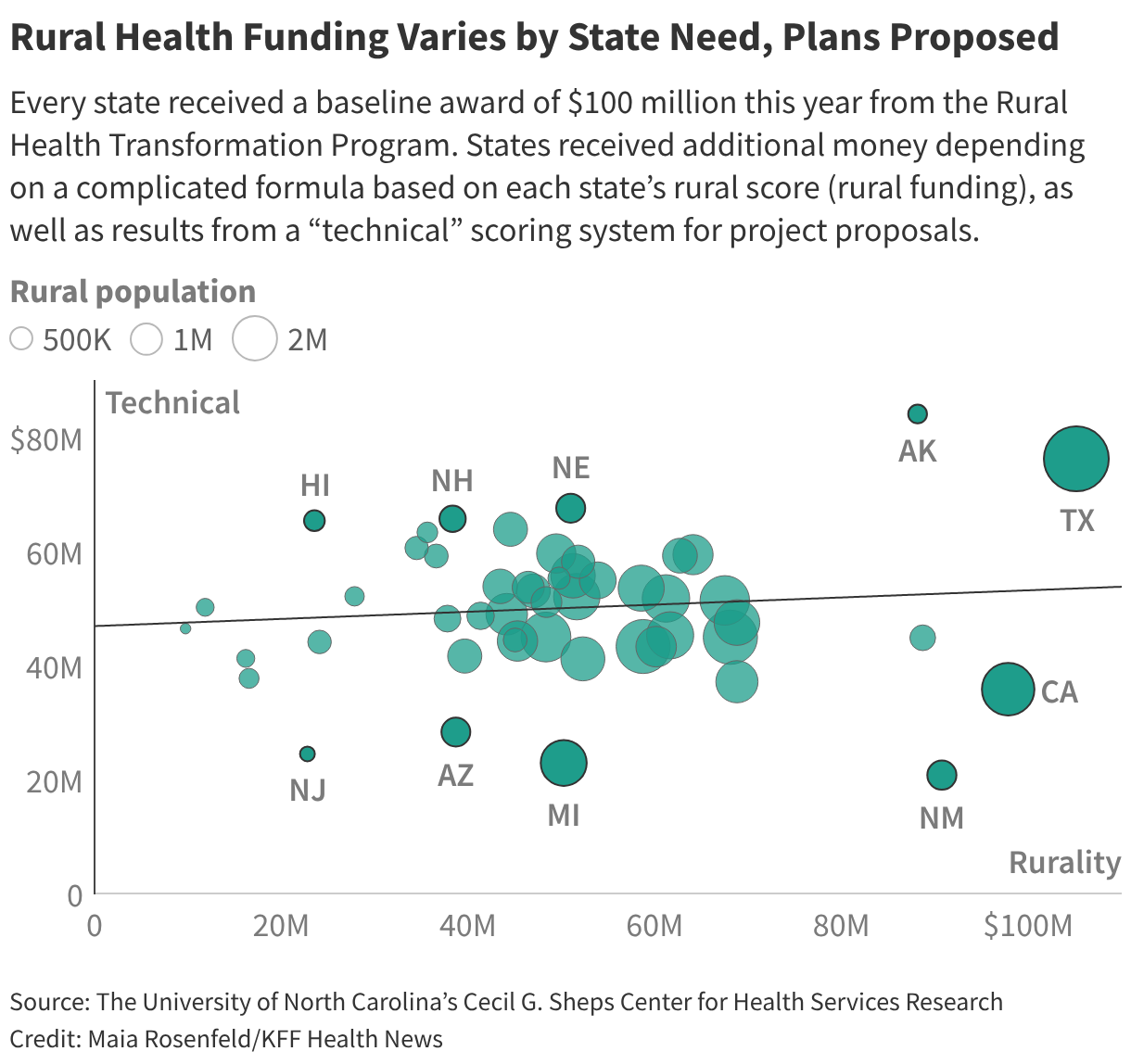
In an emailed statement to , a spokesperson for Arizona’s Democratic Gov. Katie Hobbs accused the administration of shortchanging rural residents in the state, which was awarded $167 million this year from the program.
CMS spokesperson Chris Krepich said in an emailed statement to ∫⁄¡œ≥‘πœÕ¯ News that “politics played no role in funding decisions.”
On the December call, Oz pushed states to start working on policy actions championed by the administration — such as approving presidential fitness tests and restricting food benefits — that could require legislative approval.
Half of states promised to mandate the presidential fitness test, Oz said. Many states also proposed food waivers under the Supplemental Nutrition Assistance Program, known as SNAP, which would limit low-nutrition items such as soda. He also said some states promised to teach health care professionals about nutrition. And others confirmed they will repeal certificate-of-need laws, which require companies to prove that new health facilities they want to open are necessary.
Krepich said CMS’ new Office of Rural Health Transformation is hiring program officers to serve as point people for three or four states. Many states are setting up their own offices to oversee the new funding.
Oz highlighted Alabama’s “big maternity initiative with robotics doing ultrasounds” and said states are tackling issues ranging from behavioral health to obesity.
A ∫⁄¡œ≥‘πœÕ¯ News review of state “” and “” released by CMS shows that many states plan to address the workforce challenges in rural areas. Delaware, for example, plans to use its funding to create the state’s first four-year medical school with a rural primary care track.
A third of states said they want to improve electronic health records, and every state mentioned telehealth.
Many state legislatures to distribute the funding to their state offices. Meanwhile, state officials are hiring staff, , and .
“I’m excited about what’s next,” said Terry Scoggin, former interim chief executive of the Texas Organization of Rural & Community Hospitals, or TORCH. Texas was awarded the biggest allocation. The money will bolster a rural hospital funding bill Republican Texas Gov. Greg Abbott signed last year, Scoggin said.
More than two dozen cash-strapped rural hospitals in Texas to clinics since 2005, a nationwide trend that hit the Lone Star State particularly hard. The state has the largest rural population in the United States. Texas’ allocation amounts to about $66 per rural resident, . By contrast, Rhode Island was granted about $6,300 per rural resident.
Scoggin said he has “a ton of concerns” about companies taking the money instead of it helping rural hospitals and residents. “I was blown away about how many for-profit companies reached out.” The companies have also called rural hospitals and asked to work with them to apply for state money, he said.
The awards should be judged on how they benefit rural residents because “the stated goal of the program is to improve rural health,” said Paula Chatterjee, an assistant professor of medicine at the University of Pennsylvania who co-authored on the transformation fund.
Researchers at the Sheps Center conducted the analysis to estimate how much money states received from the technical score, which is the portion of funding based on the quality of their proposals and state policy actions that align with “Make America Healthy Again” priorities.
New Mexico won the least amount of technical funding, with less than 10% of its award based on the discretionary metrics. Alaska won the largest technical award, according to the Sheps Center data.
Texas, Nebraska, New Hampshire, and Hawaii rounded out the top five recipients of technical funding. In addition to New Mexico, the other lowest technical awards went to Michigan, New Jersey, Arizona, and California.
Mark Holmes, director of the Sheps Center, declined to comment on whether he saw any political bias in the awards but said the nuance in the final portion of discretionary awards based on technical scores is important because those dollars can be redistributed and potentially clawed back in future years.
“We can be fairly certain that every state will get at least a slightly, if not a vastly, different amount next year based on this re-pooling and reallocation piece,” Holmes said.
States now have a limited time to show they’re using the money effectively to secure future funding.
But they can’t start spending yet. CMS followed standard grant procedures and is requiring each state to submit revised budgets before they can draw down money, Krepich said.
States have until Jan. 30 to resubmit their budgets, and CMS then has 30 days to respond, according to the standard . Under that timing, some states may not have cash in hand until March.
“CMS is working closely with states to complete this process as efficiently as possible,” Krepich said.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/rural-health-transformation-state-distribution-technical-scores-variation-deadlines/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2141942&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>“I was 18, healthy, in college,” she said. “And suddenly I had a chronic illness I didn’t even know about.”
Born in Florida in 1975, Wang grew up before the hepatitis B vaccine was routinely given to newborns. For years, she assumed she had been infected by her mother, only to discover later that both her parents were negative. “It turns out my grandparents, who cared for me after birth, probably passed it to me,” she said. “That’s how easy this virus spreads ‚Äî not from some exotic risk factor, just family.”
Today, Wang is the medical director for viral hepatitis programs at RWJBarnabas Health in New Jersey. Her story now sits at the center of a historic turning point in public health.
On Dec. 5, the Centers for Disease Control and Prevention’s Advisory Committee on Immunization Practices voted to end the universal U.S. recommendation for the newborn dose of the hepatitis B vaccine, instead adopting a policy urging individual-based decision-making.
Under the new approach, only infants born to mothers who test positive for hepatitis B will automatically receive a dose of the vaccine and hepatitis B antibodies shortly after birth. For everyone else, if the parents choose to vaccinate, the birth dose can be delayed until 2 months of age.
All the committee members were appointed by Health and Human Services Secretary Robert F. Kennedy Jr., a longtime anti-vaccine activist. In an 8-to-3 vote, the panel decided that since most pregnant women now receive hepatitis B testing, administering the vaccine at birth should be reserved for infants whose mothers test positive. They framed the shift as a way to reduce interventions deemed unnecessary, align vaccination with test results, and give parents more control over timing. Supporters of the decision described it as a move toward parental choice rather than a reflection of changing epidemiology.
But to many clinicians and epidemiologists, the change represents a dangerous rollback that could reverse three decades of progress toward eliminating a disease that still infects as many as 2.4 million Americans and kills tens of thousands each year. They see echoes of the 1980s, when risk-based vaccination left entire generations unprotected, and worry the country is about to repeat that mistake.
Moreover, the panel’s move on hepatitis B ‚Äî in the face of overwhelming data that shows the birth dose is effective and safe ‚Äî portends further upheaval for the nation’s childhood vaccine schedule, a cornerstone of public health.
“They’re not just trying to change one vaccine,” said Angela Rasmussen, a virologist and an editor of the scientific journal Vaccine. “They’re trying to dismantle how vaccine policy is made.”
Department of Health and Human Services spokesperson Emily Hilliard responded: “ACIP reviews all evidence presented and issues recommendations based on evidence and sound judgment to best protect America’s children.”
The authors of a by the Vaccine Integrity Project, which evaluated more than 400 studies and reports, warned in a that delaying the birth dose “would reduce protection for infants and increase the risk of avoidable HBV infections, undermining decades of progress” toward eliminating the hepatitis B virus. The review was led by researchers at the University of Minnesota’s Center for Infectious Disease Research and Policy, which created the Vaccine Integrity Project in response to what it regards as Trump administration actions that “,” and it was vetted by outside experts.
“We fought hard for that universal birth dose because targeted approaches missed too many babies,” Wang said. “We know what happens when you wait.”
What’s unfolding now is not just a technical policy update but a fundamental test of the systems meant to protect the most vulnerable. The debate turns on a few critical questions ‚Äî whether testing is reliable enough to replace universal safeguards, how infectious hepatitis B truly is, why past strategies failed, and what the CDC’s internal shake-ups mean for vaccine policy writ large.
The Limits of Testing
Hepatitis B testing sits at the center of the new ACIP recommendation, but even the CDC acknowledges that testing alone can’t guarantee protection. Pregnant women may test negative if the virus was acquired late in pregnancy or during the “window period,” before hepatitis B surface antigens become detectable. False negatives happen. No testing system, no matter how well designed, can catch every infection. That’s why universal vaccination was created in the first place.
If a mother’s status is unknown at delivery, hospitals are supposed to give the newborn a hepatitis B vaccine within 12 hours, adding hepatitis B antibodies for premature infants or if the mother later tests positive. But in real clinical settings, these safeguards routinely break down. Results take time. Nurses miss or misread labs. Pharmacies delay deliveries. Documentation gets lost.
“Every step you add increases the chance that something falls through the cracks,” Wang said. “Delaying the vaccine just adds another.”
ACIP’s vote shows how that logic is being challenged.
Some committee members suggested dropping the third hepatitis B shot if antibody levels look high after the second.
But Brian McMahon, a liver disease specialist who has spent decades treating hepatitis B, told the panelists that the data doesn’t support that idea. “Only maybe 20% to 30%” of infants have an adequate antibody level after the first dose, he said.
“You need two doses to really reach a high level of protection,” he said, with the third shot giving a stronger, longer-lasting response.
He said the overall message coming from the committee seemed designed to “discourage the birth dose.”
“They’re making it more and more difficult,” McMahon said.
In a second vote, ACIP also encouraged parents and clinicians to order post-vaccine serology tests — blood tests that measure protective antibody levels — after the second or third dose. The tests, ACIP said, should be covered by insurance.
More Infectious Than HIV or Hepatitis C
Hepatitis B can survive on toothbrushes, razors, and household surfaces for a week. It spreads not just from mother to child but also through ordinary family contact: shared items, open sores, small blood exposures. In the 1980s, researchers found that about half of infections in American children came not from mothers but from other household members.
That’s why state health departments continue to insist that every newborn be vaccinated within 24 hours of delivery, regardless of maternal status. “Delaying vaccination misses a crucial period of potential exposure,” warned this year. The vaccine, it noted, is 80% to 100% effective when given on time.

The Vaccine Integrity Project report underscores the stakes. Since the universal birth dose was introduced in 1991, pediatric hepatitis B infections in the U.S. have dropped by more than 99%. A estimated that the current schedule has prevented more than 6 million hepatitis B infections and nearly 1 million hospitalizations.
The benefits are lifelong. Infants vaccinated at birth are shielded not just from hepatitis B but also from the liver failure and cancer it can cause decades later. Yet because the disease unfolds slowly, the consequences of policy shifts may not surface for 20 or 30 years.
Trieu Pham, a California physician, doesn’t need to imagine those consequences. Born in Vietnam in 1976, he probably contracted the virus at birth. “If the vaccine had existed then, I wouldn’t have gone through what I did,” he said. Diagnosed in his 20s, he developed cirrhosis by 40. At 47, he was coughing blood from ruptured esophageal veins. Eventually, he required a liver transplant to survive.
“You live with this constant fatigue and fear,” he said. “And the saddest part is it was preventable.”
His three children, all vaccinated within hours of birth, are free of hepatitis B. “That’s the difference a day can make,” Pham said.
A Lesson Already Learned
In 1982, ACIP recommended the new hepatitis B vaccine only for adults at high risk: health care workers, injection drug users, and men who have sex with men. But by the late 1980s, it was clear that risk-based vaccination couldn’t contain transmission. Many newly infected adults didn’t fit any defined risk group. Identifying high-risk people proved imperfect, stigmatizing, and ultimately ineffective.
Meanwhile, infants infected during or shortly after birth had a of developing chronic infection, compared with in adults. Yet public health officials repeated the same targeted strategy, this time with newborns. In 1988, the CDC recommended universal prenatal screening and linked an infant’s vaccination to the mother’s test result, again basing protection on a risk marker instead of vaccinating all infants.
As before, it failed. Many infected mothers weren’t correctly identified. Some were never tested, some were tested too early, and others had results that were misread or never communicated. Too many infants slipped through the cracks, proof that another targeted approach couldn’t reliably protect them.
In 1991, the CDC issued its landmark guidance recommending that all infants, regardless of their mother’s infection status, receive a hepatitis B vaccine at birth, followed by two additional doses in infancy. By 2005, the policy was fully embedded in the routine immunization schedule, then reaffirmed in 2018. This evolution was based on data showing that a universal strategy, rather than a targeted one, was the most effective in preventing infections.
A Matter of Trust
The CDC’s new hepatitis B policy rests on the premise that moving the decision to parents will strengthen trust in the vaccine system. Supporters frame it as an empowerment shift ‚Äî a way to give families more control.
In 1999, when it was last recommended to postpone the first dose of hepatitis B vaccine for infants born to uninfected mothers, vaccination rates among infants born to those who were infected.
“Opt-in policies sound patient-centered,” Wang said, “but in practice they’re inequitable. They leave behind the very families who need protection most” ‚Äî the ones most likely to miss prenatal care and testing, have infections that go undetected or arise after testing, or slip through gaps in hospital care, as well as infants who can be exposed and infected by other caregivers and household members.
Those are often immigrant families, including from Asian and Pacific Islander communities in which hepatitis B remains endemic. “We already underdiagnose and undertreat these populations,” Wang said. “This change would deepen that gap.”
The United States is now the only country to abandon a universal hepatitis B birth dose recommendation. Though it will take decades to gather outcomes data, predict that delaying the first dose of hepatitis B vaccine to 2 months of age could result in over 1,400 preventable infections and about 300 cases of liver cancer per year.
“We don’t get to choose what we inherit,” Wang said. “But we do get to choose what we pass on.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/hepatitis-b-vaccine-acip-vote-birth-dose-policy-public-trust/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2131114&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>