More changes lie ahead that make it important for those getting subsidies in 2026 to track their income and take steps to protect against that kind of financial hit.
First, the basics of how the subsidies work.
Enrollees pay a percentage of their household income toward their health insurance premiums based on a sliding scale, ranging in 2025 from nothing for very low-income people to 8.5% at higher income levels. Subsidies, usually paid directly to insurers, cover the rest.
The income calculation done during open enrollment is an estimate of what a household thinks it will earn in the coming year. At tax time, ACA enrollees must reconcile what they received in subsidies with what they actually earned. If their income rose, they might owe some of the subsidies back.
But don’t skip filing! People who get ACA subsidies must file tax returns no matter their income, and that is becoming even more important: The Trump administration people from subsidy eligibility if they have gone two consecutive years without filing, and it is proposing lowering that to one year.
Beware Surprise Tax Bills
All enrollees who received subsidies for ACA coverage in 2025 ‚Äî ‚Äî need to include a special form, the , with their tax filings. That form is used to reconcile a person’s actual income with the amount of subsidies they received, information the IRS mails them on a separate, . Subsidy amounts are based in part on the income projections they made when they enrolled in their ACA plans.
And that can lead to surprises. Some may find they get money back if their income was less than they estimated. But, if their income went above their initial or updated estimates, they probably qualify for less in assistance and will have to pay money back.
Groups that help people file their taxes say it’s not always easy for people to accurately estimate their income for the year ahead, especially those who run their own businesses, work multiple jobs, or have work that comes with varying hours.
Clients will say, “I can make anywhere between $20,000 and $45,000 next year. I just don’t know,” said Katie Alexander, director of training and volunteers for the health and economic opportunity program at Pisgah Legal Services, a western North Carolina nonprofit that provides free tax and health insurance help to people with low incomes.
Still, for taxes being filed now for the 2025 tax year, on what many people must repay.
That cap is $375 for a single individual who earned less than $31,300 in 2025, or . The maximum owed under that sliding scale for people whose income is on the higher end of the range is $1,625 for an individual and $3,250 for a family.
There is no repayment cap for people earning more than four times the federal poverty level — totaling $62,600 in 2025 for an individual or $106,600 for a family of three — so they could owe back all amounts that exceeded their eligibility.
“The amount is just so staggering for folks,” Alexander said.
One woman whom Pisgah staff helped with pulling together her taxes for 2025 made just above $50,000, which was more than she initially estimated. Her repayment was capped at $1,625, Alexander said. Without that cap, she would have owed $4,000, a substantial chunk of her annual income.
Plan Ahead: The Rules Will Be Tougher Next Tax Season
Congressional Republicans’ One Big Beautiful Bill Act, signed into law by President Donald Trump last summer, . That means come next year’s tax season, there will be no sliding-scale limit to how much people could owe back in subsidies for 2026 if their income exceeds their projections.
“That’s just going to be absolutely devastating,” Alexander said.
There are at least two other things to keep in mind, both stemming from covid-era enhanced tax credits, which expired at the end of last year because Congress did not extend them. One is that the amount of household income people must pay toward their premiums this year before subsidies kick in has risen to just over 2% on the low end of the income scale and up to nearly 10% for higher-income earners.
The second is that households earning over four times the federal poverty level no longer qualify for ACA subsidies.
The biggest financial hit could be felt by enrollees whose income rises enough during the year to exceed four times the poverty level. In that case, they would owe back all the subsidies they receive in 2026.
And that could be a lot.
In 2025, for example, the average monthly premium for ACA coverage was $619, but the average enrollee received subsidies worth enough to offset all but $74 of that, according to the .
There’s another twist for some. Because the enhanced credits were not extended, people are paying, on average, double the amount toward their premiums this year, so they may be looking to add to their incomes to cover the cost. A found that 43% of people who remained enrolled in coverage this year are planning to work more hours or get additional work to cover those costs.
“That makes sense, but it can also present a risk of being eligible for less subsidy money than they thought, or even mean they would have to repay the entire tax credit,” said Cynthia Cox, senior vice president and director of the Program on the ACA at KFF, a health information nonprofit that includes ∫⁄¡œ≥‘πœÕ¯ News.
People can update their projected income at the marketplace website as it changes during the year.
Pisgah staff are calling people they’ve worked with and saying, “Please, please, please, if your income changes, call us so we can adjust your income through the marketplace,” Alexander said.
As much as possible, keep track of income during the year. This isn’t easy, especially for workers who don’t have a job with regular paychecks.
“If you’re meeting with a CPA to talk about taxes, have a conversation to make sure you’re making enough money to afford your costs, but not too much to lose eligibility for a subsidy,” Cox said. “Contributing toward a retirement plan or a health savings account can lower part of your income that counts toward subsidy eligibility.”
Others might choose to dial back their work hours or forgo a new client contract.
“If taking that extra shift means putting you over the line of 400% of the federal poverty level and that’s going to cost you $10,000 in repayments, maybe don’t take that shift,” said Jason Levitis, a senior fellow at the Urban Institute who follows ACA and tax policy issues.
Are you struggling to afford your health insurance? Have you decided to forgo coverage? Click here to contact ∫⁄¡œ≥‘πœÕ¯ News and share your story.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/tax-tips-aca-affordable-care-act-obamacare-subsidies-income-owing/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2174385&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Ollie’s parents, who adopted her in 2020, tried to sign her up for a clinical trial using ‚Äî which genetically reprograms a patient’s white blood cells to help them fight cancer ‚Äî at UNC Health in Chapel Hill, North Carolina, an hour-and-a-half drive from their home in Eden.
Her mother, Britany Super, described it as Ollie’s “last option.”
But in early March, Super recalled, UNC Health’s financial office told them the bad news: The state’s new insurance for kids in foster care wasn’t going to pay for the treatment.
In December, Ollie became one of hundreds of thousands of kids nationwide enrolled in a special kind of public health insurance for people served by the foster care system. That insurance, known as a specialized managed care plan, is part of Medicaid, the federal-state program that covers health costs for people with low incomes or disabilities.
North Carolina is one of 14 states with such specialized foster care plans, according to the National Academy for State Health Policy. The plans differ by state, but each is meant to expand coverage for children in the foster care system — and for kids who were adopted out of it, such as Ollie and her siblings.
Yet, as in other states that have struggled when adding such plans, North Carolina families have faced hurdles obtaining care. Thousands of doctors whose services were covered under Medicaid were not included in the specialized plan — which is costing the state $3.1 billion over four years — when it rolled out on Dec. 1. That left guardians and parents of kids adopted out of the system scrambling to figure out whether they would have to find new health care providers or new insurance.



In North Carolina, the insurance plan’s stumbles have added another layer of complication around health care issues. The state ‚Äî like many others ‚Äî is already over expected Medicaid cuts in the wake of congressional Republicans’ One Big Beautiful Bill Act. A separate Medicaid funding shortfall also prompted a push to cut care providers’ reimbursement rates.
Texas, which established its plan 18 years ago, that its foster families also had a hard time finding doctors on the insurance. In , researchers for the state reported as early as 2016 that there was .
Illinois’ plan by the Centers for Medicare & Medicaid Services over a lack of access to care. Research concluded that California’s plan children with adequate mental health services. Georgia’s alarmed state officials enough to calling for children to be removed from the plan and put back on other Medicaid plans.
But such specialized plans for kids in foster care continue to gain traction. Four states have started their own plans in the past five years, said , the senior director of children and family health at the National Academy for State Health Policy, and she said it’s likely more will adopt them soon.
showing how these programs are faring, Medicaid policy analysts said. It’s therefore difficult to know why they’ve run into rollout problems or whether they’ve improved access to care. That makes the plans risky, said , a research professor at Georgetown University’s Center for Children and Families.
“The states that are going in this direction, unless they have data to support it, are experimenting,” Schneider said. “They’re putting all their eggs in one basket, so they need to pay close attention.”
Rough Rollout
North Carolina’s specialized insurance plan for foster kids experienced problems the day it rolled out.
The state automatically enrolled Ollie and about 32,000 other people in , called . North Carolina officials had said the program would improve health care access for foster children, who often have medically complex needs and move frequently.
But foster families quickly began hearing that their health care providers were not taking the insurance, according to several families who recounted their experiences fighting to get their children’s procedures covered under the plan.
UNC Health, a state-run health system that is , with nearly 4,400 physicians, initially, which is why it told Super that Ollie’s CAR T-cell treatment wouldn’t be covered.
After more than two months of limbo for families, UNC Health ultimately in mid-March with Blue Cross Blue Shield of North Carolina, which runs the plan.
But some North Carolina doctors still don’t accept Healthy Blue insurance.
, interim deputy secretary for North Carolina’s Medicaid program, said her office to expand its network, even though it already has what she called an “adequate” number of providers. North Carolina’s health department and Blue Cross Blue Shield did not answer ∫⁄¡œ≥‘πœÕ¯ News’ questions about how many providers are covered by the new insurance.
“We welcome qualified providers who want to join,” said Blue Cross Blue Shield of North Carolina spokesperson Sara Lang.
Other problems . As thousands of health care records move over to a statewide database managed by Healthy Blue, children’s doctors are struggling to track their patients’ medical histories, said foster care advocates and pediatricians. Parents reported problems seeing health records, finding themselves locked out of online portals. Others couldn’t access prescriptions. Surgeries got delayed. Appointments were canceled.
“Network management for any plan is an ongoing process,” Lang said.
All this meant added red tape and heartache for the caregivers of children like Ollie with complex medical needs — those the .


Gearing Up
Cancer has been part of Ollie’s life since she was 2. She was in the process of getting adopted out of foster care when she began chemotherapy and radiation treatments, then received two stem cell transplants, Super recalled.
Surgeons installed temporary tubes in a vein near her heart and a feeding tube in her abdomen. Her hair fell out as the treatment intensified, and a thin layer of skin peeled off, forcing her new family to wear surgical gowns and gloves when they wanted to be close.
“She doesn’t remember life outside of going to doctors and being in a hospital,” Super said.
Ollie still has a port in her chest ready for whenever she needs intravenous medicine, and her monthly doctor appointments are about to become weekly. During an emergency room visit in mid-March, doctors told Super her daughter’s cancer had spread. Ollie will need more chemotherapy before her body is ready for the more advanced treatment.
But the Supers, thrown into uncertainty for more than two months, still feel some relief. They’re preparing for back-and-forth drives for the CAR T-cell therapy treatments in Chapel Hill. And they’re grateful, even if it means Ollie will spend at least five more weeks in and out of a hospital.
Reliable health insurance will be vital for Ollie, and Healthy Blue leaders said they are talking with doctors, parents, and others to make sure the plan is working. Her procedures carry multimillion-dollar price tags, her mother said, but having her bills seamlessly covered allows the family to focus on Ollie’s treatment.
“The biggest challenges for her will be in the first few months of the study,” said Super, who knows the therapy’s side effects include fever, fatigue, and confusion. “But I’m hoping that after that, the CAR T-cells will do their job and fight the cancer and she can continue to have a playful, active life.”
That means, they hope, the girl could be at home more often with her five siblings and the three family dogs, including Remy, a border collie mix who is Ollie’s favorite.
Super relishes those precious moments for her daughter ‚Äî “being a kid and doing kid things.”

This <a target="_blank" href="/health-care-costs/foster-children-insurance-specialized-medicaid-healthy-blue-north-carolina/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2174002&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But plans to spend those nine-digit awards aren’t all warmly received.
At least one group of Republican state lawmakers appears to have scuttled an initiative preapproved by federal officials. And at least one hospital association persuaded its state health leaders to alter who greenlights spending. Other critics are taking a more cautious approach.
That’s because the Centers for Medicare & Medicaid Services, which manages the five-year Rural Health Transformation Program, says states could lose money if they make major changes to the plans approved in their applications. Changes could also delay states’ ability to get projects rolling in time to show the agency that they’re meeting progress deadlines.
“During the application period, states were advised to only propose initiatives and state policy actions that the state deemed feasible,” said CMS spokesperson Catherine Howden, who noted that the agency will work with states case by case.
The recent pushback reflects “tension” over state plans ‚Äî which were approved by the federal government ‚Äî from state lawmakers and health leaders who want more input amid tight deadlines, said Carrie Cochran-McClain, chief policy officer of the National Rural Health Association, the largest organization representing rural hospitals and clinics.
Cochran-McClain said many states must pass a bill to allow federal dollars to be spent and added that because the program rolled out so quickly “there’s important work that still needs to be done in some states between the legislatures and the governors.”
State lawmakers want to have a say, she said, in “how the funding is being allocated ‚Äî how the implementation will go.”
Congressional Republicans created the program as a last-minute sweetener to include in their One Big Beautiful Bill Act, signed into law last summer. The funding was intended to offset concerns about the anticipated in rural communities from the law, which is expected to slash Medicaid spending by nearly $1 trillion over a decade.
CMS officials announced first-year funding — ranging from $147 million for New Jersey to $281 million for Texas — on Dec. 29, after scoring applications. Federal officials will begin evaluating progress in late summer and announce 2027 allocations at the end of October.
A chorus of critics say the program won’t make up for harm caused by Medicaid cuts.
The program is “a complete sham,” Sen. Ron Wyden (D-Ore.) said at a rural policy conference in February.
Medicaid, a joint federal-state program for low-income and disabled Americans, serves nearly , and many rural hospitals depend on it to stay afloat.
But the rural health program tilts toward seeding innovative projects and technologies, not shoring up rural hospital finances. States can use only up to 15% of their funding to pay providers for patient care.
That hasn’t stopped some federal officials and lawmakers from framing the program as a rural hospital rescue.
For example, the White House , “President Trump secured $50 billion in funding for rural hospitals.”
Now that applications have been approved, some state Republican lawmakers ‚Äî who are than Democrats are ‚Äî and hospital associations are upset that the political rhetoric doesn’t match what they see.
They’re also lobbing criticisms at specific aspects of their states’ plans, including the proposed projects, what’s not included, and the spending approval process.
In Wyoming, lawmakers didn’t just criticize an initiative from their state’s application. They moved to kill it.
State Rep. John Bear, a Republican, said he and other lawmakers declined to fund “BearCare,” a proposed state-sponsored health insurance plan that patients could use only after medical emergencies. But they did approve other aspects of the rural health program.
The Wyoming Department of Health won’t “proceed with BearCare without express legislative authority to do so,” said spokesperson Lindsay Mills.
While Wyoming lawmakers removed an initiative from their state’s rural health plan, a group in Ohio wants to add something.
Ohio Rep. Kellie Deeter and other Republican lawmakers to use the maximum allowed funding for provider payments — 15% — to support 13 independent, rural hospitals.
“We understand that the rural transformation fund is not designed to be given directly to prop up hospitals,” Deeter said. “We just want to capitalize on the mechanism of the fund that can be utilized for that purpose.”
Those hospitals “operate with very, very narrow margins, and it’s just difficult and, frankly, unsustainable,” she added.
Ken Gordon, a press secretary responding for the governor’s office and the state health department, said, “It’s still very early in this process, and many details are being worked out.”
State lawmakers around the country are also trying to ensure the federal program’s dollars benefit rural areas.
In North Dakota, Rep. Bill Tveit, a Republican who lives in a town with about 2,000 residents, that would have required the state to reserve its funding for programs located more than 35 miles from urban areas and small cities.
During a hearing, lawmakers appeared sympathetic to Tveit’s concerns but quickly shot down his idea.
State Sen. Brad Bekkedahl said the North Dakota health department already committed to prioritizing funding for the most pressing rural health needs. He also said he’s concerned any significant changes could cause the state to lose funding because CMS already reviewed and approved the plan.
Meanwhile, Republican lawmakers in Michigan and North Carolina have criticized their states’ definitions of “partially rural” or “rural,” saying that counties that include urban population centers could take money from lower-density counties, according to and .
Lawmakers aren’t the only ones speaking out.
The Colorado Hospital Association to state lawmakers denouncing how the state created its plan and two of its proposed initiatives.
“Not only were Colorado’s rural hospitals’ recommendations disregarded,” president and CEO Jeff Tieman wrote, but the plan includes ideas “they actively oppose and believe will harm the communities they serve.”
The department responded to one of the association’s concerns by adding rural health leaders to the .
Meanwhile, and Nebraska, some health groups are upset that their states’ plans lack specific funding streams for rural hospitals.
Lauren LaPine-Ray, who oversees rural health policy at the Michigan Health & Hospital Association, predicted the state’s rural hospitals will compete with other organizations, such as academic centers and health clinics, for funding. She said about 65% of the group’s rural members have never applied for a state grant before.
“The rural hospitals, the ones that really need the funding the most, will not be well equipped to apply for and pull down these dollars,” LaPine-Ray said.
Jed Hansen, executive director of the Nebraska Rural Health Association, said the federal funding won’t go to “rural hospitals, rural clinics, and rural providers in a meaningful way.”
“Rural Health Transformation will not save a single hospital in our state,” he said. “I don’t think it will save a hospital nationally.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/rural-transformation-fund-lawmakers-health-groups-resist-state-spending-plans/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2161929&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The boys sat in one waiting room and then another. Two hours and 20 minutes passed before the two were isolated, according to obtained by ∫⁄¡œ≥‘πœÕ¯ News. Then two more hours ticked by.
As the sun rose, an emergency room doctor called the state epidemiologist and described the symptoms. The public health official told him to keep the kids in the hospital and quarantine them. Shortly after that call, the patients were diagnosed.
It was measles.
Hospital staff gave the father instructions on how to quarantine the family and sent them home.
The virus exposed at least 26 other people in the hospital that January day, federal investigators determined. Health inspectors for CMS investigated the measles infections and other failures in care and concluded that the twins’ symptoms should have triggered an isolation procedure for which Mission Hospital staffers had trained seven months earlier. CMS designated Mission in “” for the exposures and other unrelated issues, one of the most severe sanctions a hospital can face, threatening to pull federal funding unless it remedied the problems.
A spokesperson for Mission said its staff was trained to manage airborne sickness and is following federal rules.
As U.S. hospitals face an increasing risk of encountering measles, and pressure to immediately spot it, health care workers face an unusual barrier: Many don’t know what it looks like.
“There’s a word, ‚Äòmorbilliform’ ‚Äî it means measles-like, and there are lots of viruses that can cause a rash that looks like a measles rash in children,” said Theresa Flynn, a pediatrician in Raleigh and the president of the North Carolina Pediatric Society. In 30 years in health care, she’s never seen a measles case, she said.
North Carolina has reported more than 20 cases since mid-December, and more than 3,000 people nationwide have been infected since the beginning of 2025.
Children in areas with low immunization rates to outbreaks, triggering public health campaigns to promote the measles vaccine. CMS Administrator Mehmet Oz encouraged vaccination in a .
, mumps, and rubella vaccine, a person has a 3% chance of getting the virus after exposure. If exposed, an unvaccinated person has a 90% chance of being infected, according to the CDC. It can take a week or two before someone infected with measles shows symptoms.
But for the past year, the Trump administration has . Health and Human Services Secretary Robert F. Kennedy Jr. was a longtime anti-vaccine activist before taking office, and under his leadership the Centers for Disease Control and Prevention has reduced the number of shots recommended to children.
After measles erupted in West Texas last year, Kennedy publicly for the virus, including steroids, antibiotics, and cod liver oil.
Infectious disease experts and doctors said federal policies have left health care workers to lean on their own experience or guidance from their state public health systems to fight a disease that many are preparing to see for the first time and that initially may behave like the common cold.
“As measles becomes more common, all of us are leveling up in our ability to recognize and immediately respond to suspected measles,” Flynn said.
Three C’s
Officially, the U.S. has maintained “measles elimination status” since 2000, meaning the U.S. has avoided significant spread of the virus. After outbreaks in Texas, Arizona, Utah, and now South Carolina, the nation is on track to lose that designation before the year is out. tie elimination status to a lack of a continuous viral spread persisting for 12 months.
One county in South Carolina, an hour’s drive from Asheville, has had in the current outbreak ‚Äî more than Texas reported in all of 2025.
Symptoms of measles, a virus that , can include fever, cough, a blotchy rash, and red, watery eyes. Researchers consider measles among the most contagious diseases, and the virus may remain active for up to two hours after an infected person leaves a room.
It can be lethal, with .
In 2025, two children in Texas and one adult in New Mexico died of measles.
Along with tracking data, the CDC on its website for diagnosing measles. State public health agencies and some counties have developed dashboards tracing the disease as it surfaces in such places as hospitals, schools, grocery stores, and airports. Large hospital systems developed staff training protocols last year and shared them with area clinics.
Look for the three C’s, : cough, coryza (cold symptoms), and conjunctivitis (pink eye). According to CMS inspection records, HCA Healthcare, which owns Mission Hospital, trained Mission staff on the three C’s early last year. On top of failing to isolate the twin patients right away, Mission staff didn’t have a designated area for patients with respiratory symptoms, federal inspectors found.
The CDC advises health workers to immediately place patients with measles or suspicious symptoms in a special isolation room, where airflow is controlled inward. The Mission patients were separated from other patients only by plastic partitions, according to the CMS records.
Mission spokesperson Nancy Lindell said the hospital was equipped and staffed to manage airborne illnesses like measles.
“Our hospital has been working with state and federal health officials on proactive preparedness, and we are following guidance provided by the CDC,” Lindell said.
(Dogwood Health Trust, a private foundation established as part of HCA’s purchase of Mission Health, helps fund ∫⁄¡œ≥‘πœÕ¯ News coverage.)
Most U.S. clinics and hospitals have never experienced measles cases, said Patsy Stinchfield, a former president of the National Foundation for Infectious Diseases and a nurse practitioner. She called CMS’ Immediate Jeopardy penalty for Mission “extreme,” given the virus can be so difficult to identify.
“In the middle of winter right now, measles looks like every other viral respiratory infection that kids come in with,” Stinchfield said.
The CDC has been less communicative in the past year with clinics about their response to outbreaks, said health workers and infectious disease experts. This disconnect began soon after Trump took office, according to a ∫⁄¡œ≥‘πœÕ¯ News investigation finding that health officials in West Texas were unable to talk with CDC scientists as measles surged last February and March.
“We certainly do not feel the support or guidance from the CDC right now,” said Brigette Fogleman, a pediatrician at Asheville Children’s Medical Center, where staff members have come up with their own method of staving off the virus: screening patients over the phone and in their cars before a visit.
In response to questions about how the CDC is supporting health care organizations during the measles resurgence, spokesperson Andrew Nixon said that “state and local health departments have the lead in investigating measles cases and outbreaks” and that the CDC provides support “as requested.” He pointed to numerous guides and simulation tools the agency has developed as the virus has spread.
Jennifer Nuzzo, an epidemiologist and director of the Pandemic Center at Brown University, acknowledged that diagnosing measles is a major challenge, emphasizing that coordination among public health agencies is critical in overcoming that challenge.
Stinchfield attributed the spread of measles to CDC leaders’ lack of communication to clinics and to the public ‚Äî no ads on buses, no social media campaigns, no sense of urgency. “When you are at the highest level of measles cases in 30 years, we should be seeing lots more from our federal government,” Stinchfield said. “And I think it’s harming kids and causing an inordinate amount of work and expense that really doesn’t belong in health care right now.”
State Prepares for More Measles Cases
In North Carolina’s Buncombe County, home to Asheville and Mission Hospital, health officials had counted seven measles cases by mid-February and anticipated many more, according to state epidemiologist Zack Moore. It’s unclear how many of those are connected to the Mission exposure.
“We are preparing for a future in which we follow a trajectory like South Carolina,” Moore said, “where we see sort of a gradual accumulation of cases, and then all of a sudden it reaches kind of a tipping point, and we see a more explosive growth in the outbreak and spread across the state.”
Fogleman, who is also a pediatrician, and Buncombe health department director Jennifer Mullendore spoke during a hosted by the county, urging families to get their children vaccinated, debunking vaccine misinformation, and updating parents on local case numbers.
Days before, a local private school had quarantined about 100 students after an exposure. were immunized, according to state data.
At Fogleman’s clinic, parents are asked to wait in their vehicles with their children, and staffers come out to screen them there. Some parents resist vaccination and note recently weakened federal recommendations around measles vaccines , she said.
Kennedy handpicked the committee members who made those recommendations, with several members having spread medical misinformation in the past.
One parent recently told a nurse, “It’s only measles. It doesn’t kill anybody,” Fogleman said.
That’s not true, her team must explain.
As the clinic holds families in the parking lot, trying to figure out whether symptoms point to the dangerous virus, it’s difficult to get the message across, Fogleman said, especially when the nation’s top disease agency hasn’t conducted a widespread information campaign about the risks from measles ‚Äî or the vaccine’s ability to almost entirely prevent it.
“We can’t change the past,” Fogleman said. “All we can do is try to educate and move forward.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/measles-outbreak-cdc-carolina-sc-nc-vaccines/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2159986&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But unlike parents in most of the U.S., she had extra help that was once much more common: house calls.
Adele was only a few weeks old when a registered nurse showed up at Bonfield’s door on Dec. 10 to check on them and offer hands-on help and advice.
As a city resident who had recently given birth, she was eligible for up to three home visits from , a program of the city health department.
She didn’t need to feed and change the baby before packing everything up for a car trip to the pediatrician or a clinic. It was a relief; Bonfield was exhausted and was still trying to figure out how to use the infant car seat.
“Everything is so abstract before you have a baby,” Bonfield said. “You are going to have questions you never even thought about.”
Louisiana is among the worst-performing states in maternal and infant health outcomes. So New Orleans is trying to catch health issues early — and get families off to an easier start — by adding health visits during the crucial first months of life.
The hope is that health outcomes can be improved by returning to the old-fashioned medical practice of house calls.
The Family Connects model has been tried in communities . It began in Durham, North Carolina, in 2008, as a partnership with Duke University. In 2023, New Orleans’ health director, , helped launch a local version of the program.
Avegno was concerned by Louisiana’s particularly grim statistics for maternal and infant health.
The state has some of the highest rates of preterm births, unnecessary cesarean sections, and maternal and infant deaths, according to the . A from the United Health Foundation found that Louisiana was the “least healthy” state for women and children.
“We got to do some real things real differently, unless you like being No. 50 all the time,” Avegno said.
The home visits are free and available to anyone who has just given birth in a New Orleans hospital, no matter their insurance status or income level.
Avegno describes the home visits as going “back to the future,” replicating a practice that was far more common a hundred years ago.
“There is no more critical time and vulnerable time than right at birth and in the few weeks to months following birth,” Avegno said.
The nurses arrive with diaper bags filled with newborn essentials, from diapers to nipple cream. They weigh, measure, and examine the babies, and check in with the mothers about their health and well-being. They offer referrals to other programs across the city.
They ask if the family has enough food, and whether there are guns in the house and how they’re stored, Avegno said.
In Bonfield’s case, the nurse stayed for over two hours. Bonfield especially liked their conversation about how to safely store breastmilk.
“I’ve never felt so well taken care of and listened to,” she said.
Broad Support
Louisiana has struggled a long time with poor maternal and infant health outcomes, but the problem has been complicated by the .
The 2022 law led to risky medical delays and in obstetrical care, and confusion among doctors about what’s allowed in ending dangerous pregnancies or .
Avegno opposes the state’s abortion policies, believing they are harmful to women’s health. But she says that Family Connects offers other ways to preserve and expand care for women. For example, the visiting nurse can check in with the mother about whether she needs help with birth control.
“We can’t give them abortion access,” she said. “That’s not the goal of this program, and that wouldn’t be possible anyway. But we can make sure they’re healthy and understand what their options are for reproductive health care.”
Abortion politics aside, the postpartum home visits seem to have bipartisan support in Louisiana, and state lawmakers want to expand their availability.
Last year, the Republican-dominated legislature requiring private insurance plans to cover the visits.
The new law is another way that Louisiana officials can be “pro-life,” said state , who, as a Republican and an abortion opponent, sponsored the legislation.
“One of the slings used against advocates against abortion is that we’re pro-birth, and not truly pro-life,” Bayham said. “And this bill is proof that we care about the overall well-being of our mothers and our newborns.”
Improving Health and Help for Postpartum Depression
Two years in, there are already promising signs that the program is improving health.
Early data analyzed by researchers at Tulane University showed that families who got the visits were more likely to stick to the recommended schedule of pediatric and postpartum checkups. Moms and babies were also less likely to need hospitalization, and overall health care spending was down among families insured by Medicaid.
Research on Family Connects programs elsewhere has found similar results. In North Carolina, one study showed that three to seven home visits in the year before a baby turned 1.
But the statistic that most excited Avegno related to the program’s role in screening mothers for postpartum depression.
The visiting nurses are helping spot more cases of postpartum depression — earlier — so that new moms can get treatment. About 10% of moms participating in the New Orleans program were eventually diagnosed with postpartum depression, compared with 6% of moms who did not get the visits.
Timely diagnosis is important to prevent depression symptoms from worsening, or leading to more , such as suicidal thoughts, thoughts of harming the baby, or problems bonding with their newborn.
Lizzie Frederick was one of the New Orleans mothers whose postpartum symptoms were caught early by a visiting nurse.
When she was pregnant, she and her husband took all the childbirth and newborn classes they could. They hired a doula to help with the birth. But Frederick still wasn’t prepared for the stresses of the postpartum period, she said.
“I don’t think there are enough classes out there to prepare you for all the different scenarios,” Frederick said.
When her son, James, was born in May, he had trouble breastfeeding. He was sleeping for only 90-minute stretches at night.
When the nurse arrived for the first visit a few weeks later, Frederick was busy trying to feed James. But the nurse reassured her that there was no rush. She could wait.
“I am here to support you and take care of you,” Frederick recalled the nurse saying.
The nurse weighed James, and Frederick was relieved to learn he was gaining weight. But for most of the visit, the nurse focused on Frederick’s needs. She was exhausted, anxious, and had started hearing what she called phantom cries.
The nurse walked her through a mental health questionnaire. Then she recommended that Frederick see a counselor and consider attending group therapy sessions for perinatal women.
Frederick followed up on these suggestions and was eventually diagnosed with postpartum depression.
“I think that I would have felt a lot more alone if I hadn’t had this visit, and struggled in other ways without the resources that the nurse provided,” Frederick said.
Home Visits Save Money
, an assistant professor at Tulane’s School of Public Health, helped interview over 90 families participating in the Family Connects New Orleans program.
“It was overwhelmingly positive experiences,” she said. “This is like a gold-standard public health project, in my opinion.”
To operate, Family Connects costs the city about $1.5 million a year, or $700 per birth, according to Avegno. But the program also has the potential to save money: Research on North Carolina’s program in the program saved $3.17 in health care billing before the child turned 2.
That’s another reason to require the visits statewide, according to state Rep. Bayham.
“The nurses and medical practitioners will be able to monitor potential problems on the front end, so that they could be handled without a trip to the emergency room or something even more drastic,” he said.
Avegno is advocating that the program be included in Louisiana’s Medicaid program, since more than in the state are covered by Medicaid. A recent made the same recommendation.
This article is from a partnership that includes , , and ∫⁄¡œ≥‘πœÕ¯ News.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/new-orleans-postpartum-home-visits-newborn-maternal-health/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2158981&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Regulating artificial intelligence, especially its use by health insurers, is becoming a politically divisive topic, and it’s scrambling traditional partisan lines.
Boosters, led by Trump, are not only pushing its integration into government, as in Medicare’s experiment using AI in prior authorization, but also trying to stop others from building curbs and guardrails. A December seeks to preempt most state efforts to govern AI, describing “a race with adversaries for supremacy” in a new “technological revolution.”
“To win, United States AI companies must be free to innovate without cumbersome regulation,” Trump’s order said. “But excessive State regulation thwarts this imperative.”
Across the nation, states are in revolt. At least four — Arizona, Maryland, Nebraska, and Texas — enacted legislation last year reining in the use of AI in health insurance. Two others, Illinois and California, enacted bills the year before.
Legislators in Rhode Island plan to try again this year after a bill requiring regulators to collect data on technology use failed to clear both chambers last year. A bill in North Carolina requiring insurers not to use AI as the sole basis of a coverage decision attracted significant interest from Republican legislators last year.
DeSantis, a former GOP presidential candidate, has rolled out an “AI Bill of Rights,” include restrictions on its use in processing insurance claims and a requirement allowing a state regulatory body to inspect algorithms.
“We have a responsibility to ensure that new technologies develop in ways that are moral and ethical, in ways that reinforce our American values, not in ways that erode them,” DeSantis said during his State of the State address in January.
Ripe for Regulation
Polling shows Americans are skeptical of AI. A from Fox News found 63% of voters describe themselves as “very” or “extremely” concerned about artificial intelligence, including majorities across the political spectrum. Nearly two-thirds of Democrats and just over 3 in 5 Republicans said they had qualms about AI.
Health insurers’ tactics to hold down costs also trouble the public; from KFF found widespread discontent over issues like prior authorization. (KFF is a health information nonprofit that includes ∫⁄¡œ≥‘πœÕ¯ News.) Reporting and in recent years has highlighted the use of algorithms to rapidly deny insurance claims or prior authorization requests, apparently with little review by a doctor.
Last month, the House Ways and Means Committee hauled in executives from Cigna, UnitedHealth Group, and other major health insurers to address concerns about affordability. When pressed, the executives either denied or avoided talking about using the most advanced technology to reject authorization requests or toss out claims.
AI is “never used for a denial,” Cigna CEO David Cordani told lawmakers. Like others in the health insurance industry, the company is being sued for its methods of denying claims, as spotlighted by ProPublica. Cigna spokesperson Justine Sessions said the company’s claims-denial process “is not powered by AI.”
Indeed, companies are at pains to frame AI as a loyal servant. Optum, part of health giant UnitedHealth Group, announced Feb. 4 that it was rolling out tech-powered prior authorization, with plenty of mentions of speedier approvals.
“We’re transforming the prior authorization process to address the friction it causes,” John Kontor, a senior vice president at Optum,
Still, Alex Bores, a computer scientist and New York Assembly member prominent in the state’s legislative debate over AI, which culminated in a comprehensive bill governing the technology, said AI is a natural field to regulate.
“So many people already find the answers that they’re getting from their insurance companies to be inscrutable,” said Bores, a Democrat who is running for Congress. “Adding in a layer that cannot by its nature explain itself doesn’t seem like it’ll be helpful there.”
At least some people in medicine ‚Äî doctors, for example ‚Äî are cheering legislators and regulators on. The American Medical Association “supports state regulations seeking greater accountability and transparency from commercial health insurers that use AI and machine learning tools to review prior authorization requests,” said John Whyte, the organization’s CEO.
Whyte said insurers already use AI and “doctors still face delayed patient care, opaque insurer decisions, inconsistent authorization rules, and crushing administrative work.”
Insurers Push Back
With legislation approved or pending in at least nine states, it’s unclear how much of an effect the state laws will have, said University of Minnesota law professor Daniel Schwarcz. States can’t regulate “self-insured” plans, which are used by many employers; only the federal government has that power.
But there are deeper issues, Schwarcz said: Most of the state legislation he’s seen would require a human to sign off on any decision proposed by AI but doesn’t specify what that means.
The laws don’t offer a clear framework for understanding how much review is enough, and over time humans tend to become a little lazy and simply sign off on any suggestions by a computer, he said.
Still, insurers view the spate of bills as a problem. “Broadly speaking, regulatory burden is real,” said Dan Jones, senior vice president for federal affairs at the Alliance of Community Health Plans, a trade group for some nonprofit health insurers. If insurers spend more time working through a patchwork of state and federal laws, he continued, that means “less time that can be spent and invested into what we’re intended to be doing, which is focusing on making sure that patients are getting the right access to care.”
Linda Ujifusa, a Democratic state senator in Rhode Island, said insurers came out last year against the bill she sponsored to restrict AI use in coverage denials. It passed in one chamber, though not the other.
“There’s tremendous opposition” to anything that regulates tactics such as prior authorization, she said, and “tremendous opposition” to identifying intermediaries such as private insurers or pharmacy benefit managers “as a problem.”
In a , AHIP, an insurer trade group, advocated for “balanced policies that promote innovation while protecting patients.”
“Health plans recognize that AI has the potential to drive better health care outcomes ‚Äî enhancing patient experience, closing gaps in care, accelerating innovation, and reducing administrative burden and costs to improve the focus on patient care,” Chris Bond, an AHIP spokesperson, told ∫⁄¡œ≥‘πœÕ¯ News. And, he continued, they need a “consistent, national approach anchored in a comprehensive federal AI policy framework.”
Seeking Balance
In California, Newsom has signed some laws regulating AI, including one requiring health insurers to ensure their algorithms are fairly and equitably applied. But the Democratic governor has vetoed others with a broader approach, such as a bill including more mandates about how the technology must work and requirements to disclose its use to regulators, clinicians, and patients upon request.
Chris Micheli, a Sacramento-based lobbyist, said the governor likely wants to ensure the state budget — consistently powered by outsize stock market gains, especially from tech companies — stays flush. That necessitates balance.
Newsom is trying to “ensure that financial spigot continues, and at the same time ensure that there are some protections for California consumers,” he said. He added insurers believe they’re subject to a welter of regulations already.
The Trump administration seems persuaded. The president’s recent executive order proposed to sue and restrict certain federal funding for any state that enacts what it characterized as “excessive” state regulation ‚Äî with some exceptions, including for policies that protect children.
That order is possibly unconstitutional, said Carmel Shachar, a health policy scholar at Harvard Law School. The source of preemption authority is generally Congress, she said, and federal lawmakers twice took up, but ultimately declined to pass, a provision barring states from regulating AI.
“Based on our previous understanding of federalism and the balance of powers between Congress and the executive, a challenge here would be very likely to succeed,” Shachar said.
Some lawmakers view Trump’s order skeptically at best, noting the administration has been removing guardrails, and preventing others from erecting them, to an extreme degree.
“There isn’t really a question of, should it be federal or should it be state right now?” Bores said. “The question is, should it be state or not at all?”
Do you have an experience navigating prior authorization to get medical treatment that you’d like to share with us for our reporting? Share it with us here.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/artificial-intelligence-ai-health-insurance-companies-state-regulation-trump/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2154202&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>While more Americans enrolled than¬Ý, the number¬Ýwas¬Ý¬Ýwhat¬Ýit was¬Ýat the same time last year. And experts say¬Ýit will¬Ýbe¬Ýmonths¬Ýuntil¬Ýthe numbers¬Ýare final.¬ÝThe timing¬Ýwill depend on¬Ýhow many of those people¬Ýwho signed up for coverage¬Ýactually pay their premiums and remain enrolled.¬Ý
In coming weeks, “consumers may find they really can’t afford the premiums and cancel their plans, while carriers may also cancel coverage for nonpayment,” said Pat Kelly, executive director of Your Health Idaho, a state-based ACA marketplace, during a Jan. 22 call with reporters.
The drop comes after several years of record-breaking enrollment, with 24.2 million sign-ups for the 2025 enrollment year. Enrollment growth took off after enhanced subsidies — which lowered the amount most households had to pay out of their own income toward premiums and removed an upper-income cap — went into effect during the Biden administration. Lawmakers, in adopting the enhanced subsidies, set an expiration date of Dec. 31, 2025.
Congressional debate over extending those more generous subsidies was heated, even . Now, the subsidies are back to their original level, and people who earn more than four times the federal poverty rate (about $62,600 for an individual or $84,600 for a couple) can’t qualify for any at all.
in most states this year, with the biggest drop in North Carolina, where sign-ups fell by nearly 22%, .
In a few places ‚Äî including New Mexico, Texas, and Maryland, as well as the District of Columbia ‚Äî the number of people selecting ACA plans increased.¬Ý
The jump was largest in New Mexico, with its tally of people selecting plans up by nearly 18%. Increases were in the single digits in the other states and Washington, D.C.
New Mexico — uniquely — used its own tax dollars to fully offset the loss of the more generous federal tax subsidies for all consumers. , including California, Colorado, Maryland, and Washington, used state money to help some enrollees.
We’ll keep watching to see how this unfolds over the coming weeks.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/the-week-in-brief-obamacare-enrollment-affordable-care-act-enhanced-subsidies-fallout/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2155737&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>An older couple in flannel pajamas sat together in the waiting room. A toddler waved as Patricia Hall walked past him, a stethoscope draped over her neck. The family physician waved and smiled back.
But in the privacy of a conference room, her mood shifted. She is often bogged down with paperwork and can’t get patients timely appointments with specialists. She also fears that a health care affecting her clinic ‚Äî and many others across the nation ‚Äî will only get worse.
Hall’s clinic, the Celo Health Center, is one of seven locations that make up the , which was supposed to receive up to $10 million over the next decade through , a federal program to improve primary care, , by providing payments for physicians to address patient needs. Her organization planned to use the money to hire staff, build better connections with local specialists, and buy more vehicles to shuttle patients to appointments, according to its CEO, .
Then, in March, clinic administrators received an email during the Department of Government Efficiency’s whirlwind of federal cuts: The Centers for Medicare & Medicaid Services would soon shutter Making Care Primary, a year into what was supposed to be a 10-year program. Nearly 700 practices in eight states . North Carolina had 23 clinics and centers in the program, the most of any state, followed by Washington, New Mexico, and New York. Doctors who had signed up for it said they were stunned.
“I’m angry, but more than that, I am so very sad,” . “It’s heartbreaking ‚Äî to have an already inadequate health care system be made even more inadequate, to throw away opportunities to improve, even a little.”

Now, CMS’ Innovation Center, which created Making Care Primary, is set to launch a new 10-year program to boost primary care called the , known by its acronym LEAD. In that program, funding will be sent to health care organizations, often managed by companies, instead of directly to primary care doctors and clinics.
CMS wouldn’t say how much the programs cost. But it maintained that eliminating Making Care Primary reduced spending to improve quality of care. Nixing Making Care Primary and three other programs at the agency ‚Äî including another focused on primary care ‚Äî would , CMS said at the time.
Making Care Primary “was not on track to meet its intended savings goal,” CMS spokesperson Alexx Pons said. Innovation Center models to save money over time, in part by improving patients’ access to health care and helping them avoid costly hospital visits. Practices that signed up for Making Care Primary and want to join LEAD will have to apply for the program beginning in March.
Yet Making Care Primary’s elimination has created skepticism among doctors. The change exacerbated their fears about uncertain funding overseen by the Trump administration as covid-era Medicaid provisions , enhanced Affordable Care Act subsidies , and Congress passed more funding cuts in President Donald Trump’s One Big Beautiful Bill Act.
, a physician and the CEO of the Mountain Area Health Education Center in western North Carolina, which serves 16 mostly rural counties, questions how his organization is supposed to plan for the future “when the future can just go away so quickly.”
A Chance To Change Primary Care
The U.S. is facing a . In 2023, more than 100 million people in the U.S. to a primary care doctor in their area, the National Association of Community Health Centers reported. Some states, such as Colorado, have passed legislation more primary care funding at the state level.
The health care shortage where Hall works in western North Carolina is , she said she often makes personal calls to doctors to schedule appointments.
Hall said one of her patients is an uninsured woman who has been waiting six months for a colonoscopy. The patient has severe anemia and possibly gastrointestinal bleeding. Hall has been trying to get the patient somewhere that offers free or discounted care.
The additional funding through Making Care Primary would have allowed the network of clinics to improve its communication systems with specialists. Coordination of this kind of care is one of the challenges Making Care Primary was supposed to address.
“I’m still not sure what we’re going to do for her,” Hall said.

Making Care Primary sought to create an efficient payment system for primary care clinics and help them better track patients, allowing doctors to be less burdened by administrative duties and focus more on care.
It provided bonuses to primary care doctors for maintaining their patients’ health, as well as flexible funding that could be used to improve patients’ quality of life in numerous ways. That included patients’ transportation to health care facilities, food vouchers, moving expenses, or help with utility bills.
Spokespeople for health departments in the states that signed up for Making Care Primary said some doctors have since lost trust in federal support.
“It can be difficult for providers, especially smaller community base practitioners, to pool resources to invest in non-clinical development,” said Cadence Acquaviva, a spokesperson for New York’s health agency. “An abrupt change can damage the confidence in future programs’ sustainability.”
An Uncertain Future
The CMS Innovation Center tests health care models to find those that improve care and lower costs for the health system and patients. The center created Making Care Primary after testing it as one of those models. It’s unclear whether the models have ultimately saved money; a 2023 Congressional Budget Office report for increasing spending by nearly double the amount the CBO projected the center would save in taxpayer money over 10 years.
, who directed the center under President Joe Biden, said Making Care Primary ended so early that it could not have produced any meaningful data on whether the patients it served became healthier.
She acknowledged that the program didn’t draw in as many clinics as she hoped and lagged in enrollment. But if it were her decision to make, “I would have said, ‚ÄòIt’s not enough time,’” Fowler said. “It takes more than a year to get the numbers.”
Hathaway said his Mountain Area Health Education Center signed on to Making Care Primary believing it could change the profession: It promised to ensure practices received immediate, consistent federal money to enhance primary care. Other models made that funding more difficult to obtain.
It’s unclear whether LEAD will draw more enrollment than Making Care Primary, but Hathaway, who has years of experience with elements included in LEAD, is skeptical of the program.
“Anytime you put multiple layers of bureaucracy between us and the patients and the dollars, it just costs more,” he said.
Hall said doctors “see the suffering firsthand” but often feel helpless in a system that cuts people off from primary care. She has been frustrated with the nation’s health care system, she said, which she feels focuses on profits over patients.
“We should be rolling out the red carpet for everybody to come see their family doctor and keep them out of the emergency room,” Hall said. “That would keep costs lower for the whole system. I’m wearing rose-colored glasses now, but I really believe that.”

This <a target="_blank" href="/health-industry/cms-mcp-lead-primary-care-model-canceled-rural-health-north-carolina/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2151354&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The 59-year-old, who lives in Harrisburg, North Carolina, closed her nonprofit circus arts school last year because she could no longer see well enough to complete paperwork. She then worked making dough at a pizza shop for a bit. Currently, she sorts recyclable materials, including cans and bottles, at a local concert venue. It is her main source of income ― but the work isn’t year-round.
“This place knows me, and this place loves me,” Kelley said of her employer. “I don’t have to explain to this place why I can’t read.”
Kelley, who lives in a camper, survives on less than $10,000 a year. She says that’s possible, in part, because of her Medicaid health coverage, which pays for arthritis and anxiety medications and has enabled doctor visits to manage high blood pressure.
But she worries about losing that coverage next year, when rules take effect requiring millions of people like Kelley to work, volunteer, attend school, or perform other qualifying activities for at least 80 hours a month.
“I’m scared right now,” she said.


Before the coverage changes were signed into law, Republican lawmakers suggested that young, unemployed men were taking advantage of the government health insurance program that provides coverage to millions of low-income or disabled people. Medicaid is not intended for “29-year-old males sitting on their couches playing video games,” House .
But, in reality, adults ages 50 to 64, particularly women, are likely to be , said Jennifer Tolbert, deputy director of the Program on Medicaid and the Uninsured at KFF, a health information nonprofit that includes ∫⁄¡œ≥‘πœÕ¯ News. For Kelley and others, the work requirements will create barriers to keeping their coverage, Tolbert said. Many could lose Medicaid as a result, putting their physical and financial health at risk.
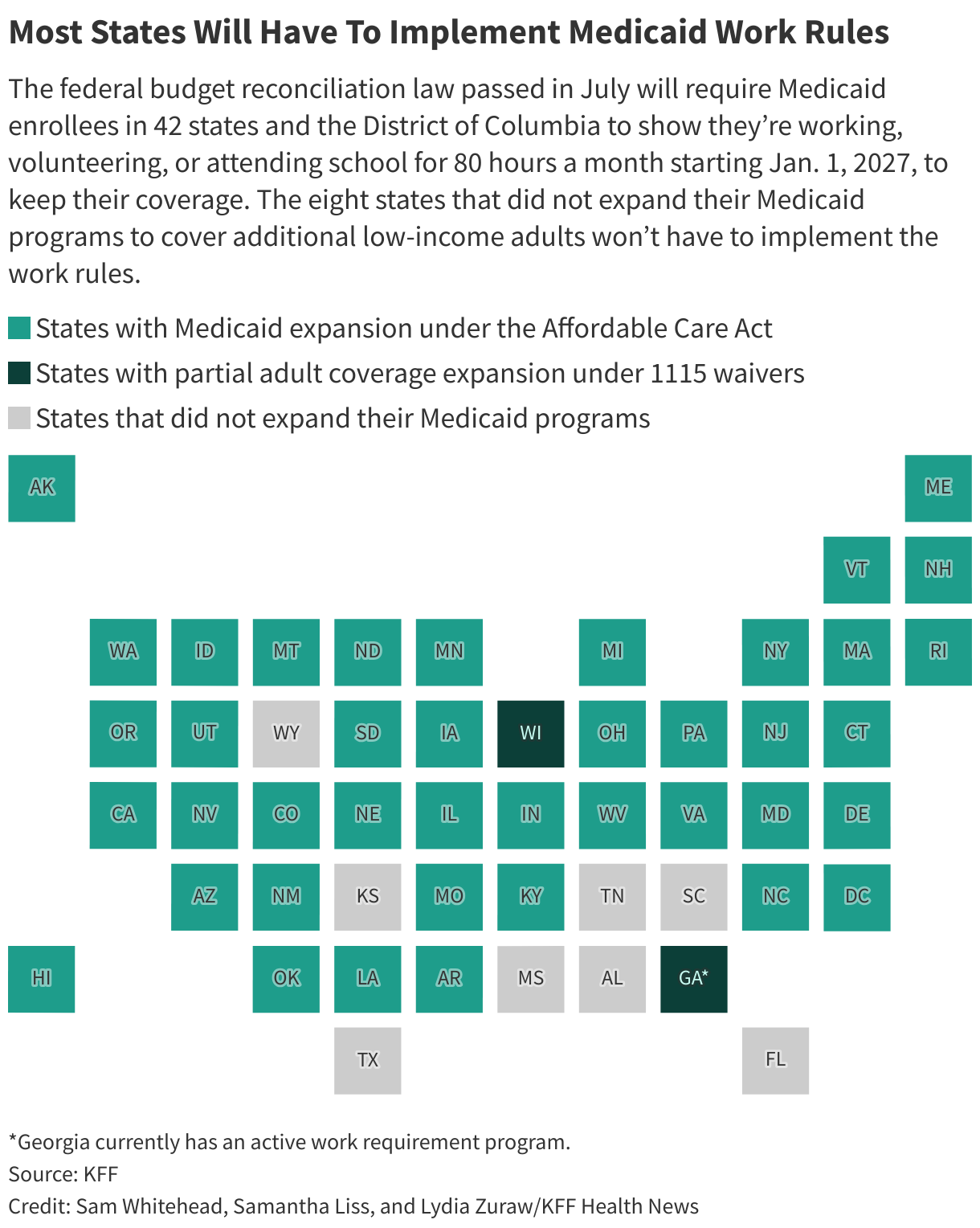
Starting next January, some 20 million low-income Americans in 42 states and Washington, D.C., will need to meet the activity requirements to gain or keep Medicaid health coverage.
Alabama, Florida, Kansas, Mississippi, South Carolina, Tennessee, Texas, and Wyoming didn’t expand their Medicaid programs to cover additional low-income adults under the Affordable Care Act, so they won’t have to implement the work rules.
The nonpartisan Congressional Budget Office predicts the work rules will result in at least 5 million fewer people with Medicaid coverage over the next decade. Work rules are the largest driver of coverage losses in the GOP budget law, which slashes nearly $1 trillion to offset the costs of tax breaks that mainly benefit the rich and increase border security, .
“We’re talking about saving money at the expense of people’s lives,” said Jane Tavares, a gerontology researcher at the University of Massachusetts Boston. “The work requirement is just a tool to do that.”
Department of Health and Human Services spokesperson Andrew Nixon said requiring “able-bodied adults” to work ensures Medicaid’s “long-term sustainability” while safeguarding it for the vulnerable. Exempt are people with disabilities, caregivers, pregnant and postpartum individuals, veterans with total disabilities, and others facing medical or personal hardship, Nixon told ∫⁄¡œ≥‘πœÕ¯ News.
Medicaid expansion has provided a lifeline for middle-aged adults who otherwise would lack insurance, according to . Medicaid covers 1 in 5 Americans ages 50 to 64, giving them access to health coverage before they qualify for Medicare at age 65.
Among women on Medicaid, those ages 50 through 64 are more likely to face challenges keeping their coverage than their younger female peers and are likely to have a greater need for health care services, Tolbert said.
These middle-aged women are less likely to be working the required number of hours because many serve as family caregivers or have illnesses that limit their ability to work, Tolbert said.
Tavares and other researchers found that of the total Medicaid population is considered “able-bodied” and not working. This group consists largely of women who are very poor and have left the workforce to become caretakers. Among this group, 1 in 4 are 50 or older.
“They are not healthy young adults just hanging out,” the researchers stated.
Plus, making it harder for people to maintain Medicaid coverage “may actually undermine their ability to work” because their health problems go untreated, Tolbert said. Regardless, if this group loses coverage, their chronic health conditions will still need to be managed, she said.
Adults often start wrestling with health issues before they’re eligible for Medicare.
If older adults don’t have the means to pay to address health issues before age 65, they’ll ultimately be sicker when they qualify for Medicare, costing the program more money, health policy researchers said.
Many adults in their 50s or early 60s are no longer working because they’re full-time caregivers for children or older family members, said caregiver advocates, who refer to people in the group as “the sandwich generation.”


The GOP budget law does allow some caregivers to be exempted from the Medicaid work rules, but the carve-outs are “very narrow,” said Nicole Jorwic, chief program officer for the group Caring Across Generations.
She worries that people who should qualify for an exemption will fall through the cracks.
“You’re going to see family caregivers getting sicker, continuing to forgo their own care, and then you’re going to see more and more families in crisis situations,” Jorwic said.
Paula Wallace, 63, of Chidester, Arkansas, said she worked most of her adult life and now spends her days helping her husband manage his advanced cirrhosis.
After years of being uninsured, she recently gained coverage through her state’s Medicaid expansion, which means she’ll have to comply with the new work requirements to keep it. But she’s having a hard time seeing how that will be possible.
“With me being his only caregiver, I can’t go out and work away from home,” she said.
Wallace’s husband receives Social Security Disability Insurance, she said, and the law says she should be exempt from the work rules as a full-time caregiver for someone with a disability.
But federal officials have yet to issue specific guidance on how to define that exemption. And experience from Arkansas and Georgia ― the only states to have run Medicaid work programs ― shows that many enrollees struggle to navigate complicated benefits systems.
“I’m very concerned,” Wallace said.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/medicaid-work-requirements-middle-aged-adults-women/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2151346&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>It’s all part of a drama that roiled the ACA’s 2026 open enrollment period. Congressional debate over whether to extend more generous subsidies made available under the Biden administration led to and focused public attention on rising health care costs and the affordability issue.
The enhanced subsidies, which expanded eligibility both by lowering the percentage of household income people had to pay toward their care and removing an income cap, expired at the end of last year. As a result, just about everyone buying ACA coverage saw their costs increase. For some, what they paid toward premiums doubled or more, even though less generous subsidies remain in place.
Many experts expected ACA enrollment, which hit a record 24 million in 2025, to fall this time around.
“If you raise the price of something a whole lot, economics tell us that a lot of people will buy less of it or not buy at all,” said Katherine Hempstead, a senior policy officer with the Robert Wood Johnson Foundation.
Here are things to watch now:
Initial Numbers Aren’t Final
The in December 2024 that not extending the enhanced subsidies would cause 2.2 million people to lose insurance in 2026, with further increases in following years. Analysts with the Wakely Consulting Group would opt out of insurance for this year.
Data released Jan. 28 by federal officials showed a year-over-year enrollments across the federal healthcare.gov marketplace and those run by states. Overall, there were 23 million enrollees, including 3.4 million new to ACA coverage.
At about the same time last year, there were , with 3.9 million new to the marketplaces.
But there’s more to it than those initial numbers.
For one thing, both years’ data was pegged to Jan. 15 for the federal marketplace, which closed its open enrollment period that day. But, the data for the states that run their own marketplaces included sign-ups in most cases only through Jan. 10 or 11, even though some held open enrollment until the . Thus, the numbers don’t reflect what might have happened in those last days. Was there a surge in state sign-ups? Or, conversely, did the marketplaces see more enrollees cancel their coverage?
Additionally, those initial numbers are a mix of newly minted ACA enrollees and existing customers, many of whom were auto-reenrolled for 2026 — which raises other issues.
For existing, reenrolled policyholders, the real figures won’t be known for weeks or months, when it becomes clear how many actually pay their premiums. Some consumers may not have focused on their reenrollment costs or may have hoped Congress would extend the subsidies.
That’s an important factor to keep in mind because the CBO and Wakely estimates of millions losing insurance were based on projections for full-year coverage, not initial sign-ups.
In the coming weeks, “consumers may find they really can’t afford the premiums and cancel their plans, while carriers may also cancel coverage for nonpayment,” said Pat Kelly, executive director of Your Health Idaho, a state-based ACA marketplace, during a Jan. 22 call with reporters.
Sharp Differences in State Enrollment Patterns
Changes are also afoot in the 19 other states (and the District of Columbia) that , some of which have issued more detailed data about enrollment than the federal marketplace.
Most states saw lower enrollment for 2026 than the prior year, with the biggest drop in North Carolina, where sign-ups fell by nearly 22%, federal data shows.
In a few states — including New Mexico, Texas, California, and Maryland, as well as the District of Columbia — the number of people selecting ACA plans increased.
The jump was largest in New Mexico, with its initial number of people selecting plans up by nearly 14%. Increases were in the single digits in the other states and Washington, D.C.
New Mexico — uniquely — used its own tax dollars to fully offset the loss of the more generous federal tax subsidies for all consumers. , including California, Colorado, Maryland, and Washington, used state money to help some enrollees.
The , a collective of 22 state marketplaces supported by the National Academy for State Health Policy, said initial enrollment figures . Compared with the same time last year, outright plan cancellations are up 83% in Colorado, disenrollments are four times what they were in Idaho, and Virginia has seen cancellations double.
New enrollments are from the same period last year, according to data from the state. In Pennsylvania, people ages 55 to 64, the group with the highest premiums, and young people 26 to 34 in higher numbers than other age groups, state data shows.
“We have drastically higher rates of people dropping their coverage,” said Devon Trolley, executive director of the Pennsylvania Health Insurance Exchange Authority. “We had 70,000 drop in the last two months, from early retirees to small-business owners to farmers not knowing how to make ends meet.”
On Feb. 9, Pennsylvania released , showing enrollment dropped by about 2% from last year, although that figure masks some of the effects. The state says nearly 18% of enrollees dropped coverage altogether, with older and rural residents being the most likely to fall out.
Some Republicans credited Trump-administration-backed anti-fraud measures, which included a range of , for tightening the system. Although some of those actions were paused by a federal court and have not taken effect, those ACA critics, some of whom have produced that millions may have been improperly enrolled, say that’s behind the decline. They have previously for unauthorized enrollments or ACA plan-switching by commission-seeking brokers.
States that run their own ACA marketplaces, however, reported little or no such unauthorized switching. Relative to the federal marketplace, the state-based ACA platforms employ additional safeguards to prevent brokers from accessing consumers’ coverage without authorization.
Among consumers not returning to the marketplace, the main reason is cost, said Mila Kofman, executive director of the DC Health Benefit Exchange Authority, which runs the district’s ACA marketplace.
“When we looked at who these folks are, half are small-business owners,” Kofman said. “They are not folks committing fraud.”
Lower Premiums, Higher Deductibles
Rather than sticking with automatic reenrollment, existing customers in many states shifted sharply into lower-priced “bronze” plans that come with higher deductibles than silver, gold, and platinum plans.
California saw 73% of renewing members who switched plans move to a bronze plan, up from 27% at the same time last year, the State Marketplace Network reported. In Maine, bronze enrollment now represents almost 60% of all plans purchased.
People are “looking at what works in their monthly budget, looking for that lower premium,” said Stacey Pogue, a senior research fellow at the Center on Health Insurance Reforms at Georgetown University. “Some might be crossing their fingers that they won’t need to meet their deductible.”
On average, bronze plans have an . All ACA plans are required to cover certain preventive services — such as some vaccinations, cancer screenings, and other tests — without a copayment or deductible, but most everything else is covered only after an annual deductible is met.
High deductibles can lead some patients to avoid seeking medical care, Hempstead said.
“People are terrified to use their care,” she said. “They may delay something until it’s more serious.”
She added that medical providers, including hospitals and doctors, are bracing for an increase in the number of insured patients who can’t afford to pay their deductibles.
“Everyone is anticipating that hospitals will have to give out more charity care, which will hurt their bottom lines and might lead them to have to lay off people or close or reduce services,” she said.
Are you struggling to afford your health insurance? Have you decided to forgo coverage? Click here‚ÄØto contact ∫⁄¡œ≥‘πœÕ¯ News and share your story.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/affordable-care-act-aca-obamacare-sign-ups-subsidies-higher-premiums/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2150584&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>