It’s one of the many parts of the 25-bed rural hospital that need updating, former CEO Ron Wiens said.
He said the hospital, an essential service in its namesake town of nearly 800 residents in the state’s sprawling north-central high plains, needs at least $1 million for deferred maintenance, including a failing HVAC system. But the facility has struggled to make payroll each month and can’t afford to make all the fixes, Wiens said.
Built by farmers and ranchers in 1965, Big Sandy Medical Center began with nine beds. Today, a similar community effort тАФ donations and grants to plug financial holes each year тАФ keeps it afloat.
Wiens, who recently left his position at the hospital, said he wishes Big Sandy could get funding from Montana’s share of the $50 billion federal Rural Health Transformation Program to renovate the hospital and direct payments to help secure its future. The state received more than $233 million in its first-year award.
But the hospital may not get the kind of help he sought.
That’s because the five-year program focuses on new, creative ways to improve access to rural health care, not on directly funding services and renovations. And Montana is one of at least 10 states whose leaders say projects launched under the federal program could lead rural hospitals to cut services so they can continue to afford to offer emergency and other essential care.

Congressional Republicans created the fund as a last-minute sweetener to their One Big Beautiful Bill Act, signed into law last summer. The funding was intended to offset disproportionate fallout anticipated in rural communities from the law, which is expected to slash Medicaid spending .
includes programs to make it easier for rural residents to get medical care and live a healthy lifestyle. For example, it says funding can be used to start community gardens, train paramedics to make home visits, open school-based clinics, or bring mobile clinics to rural areas.
rural Montana hospitals can receive payments for implementing recommendations, “including right-sizing select inpatient services” to match demand. In some cases, it says, right-sizing might mean “downsizing.” The state says hospitals will have input and recommendations will be specific to each facility.
“That’s what has all the hospitals on pins and needles, words like restructuring, reducing inpatient beds. Everybody is going, тАШWhat is this going to look like?’” Wiens said.
The Montana Department of Public Health and Human Services declined to answer questions about how it will carry out its right-sizing efforts.
A Lifeline of Care
Big Sandy cattle rancher Shane Chauvet doesn’t want any services cut.
He credits Big Sandy Medical Center with saving his life after a flying piece of metal nearly cut off his arm during a windstorm a few years back.
“I looked over, saw it coming, and whack!” Chauvet recalled.
His wife drove him to the hospital, where they frantically pounded on the ER door while Chauvet’s blood pooled on the ground.
Because of the storm, staffers worked on Chauvet with no power and no ability to summon a helicopter. He was then taken by ambulance 80 miles through intense rain and hail to a larger hospital.
Chauvet understands the state’s plan doesn’t call for eliminating emergency care, but he worries that reducing other services would set off a downward spiral for the hospital and his town.

In Oklahoma, realigning clinical services could mean “shutting down service lines,” to the federal program. And in Wyoming, any facility that receives funding must agree to “reduce unprofitable, duplicative or nonessential service lines,” .
Monique McBride, business operations administrator at the Wyoming Department of Health, said the department interprets right-sizing as helping rural hospitals provide essential services тАФ such as emergency departments, ambulance services, and labor and delivery units тАФ while maintaining long-term, financial stability.
“This might involve limiting some elective procedures that could be done at lower cost in higher-volume facilities. The main distinction here is time-sensitive emergencies vs. тАШshoppable’ services,” she said.
A New Lease on Life?
Seven of the 10 states тАФ Nebraska, North Dakota, Tennessee, Kansas, Nevada, South Carolina, and Washington тАФ where rural hospital service cuts are on the table say they’ll help pay for hospitals to convert to Rural Emergency Hospitals. The recently created federal designation requires hospitals to halt inpatient services and offers enhanced payments to help them maintain emergency and outpatient care.
At least 15 additional states wrote that they’ll use the federal funding to right-size, evaluate, or adjust services тАФ which could mean adding or taking away services, or transitioning them to a telehealth or outpatient setting.
Brock Slabach, chief operations officer of the National Rural Health Association, said, “There’s a proper concern from rural hospital administrators that this funding is not going to where it was intended.”
He said cutting services that lose money could backfire in the long run. For example, he said, halting labor and delivery care might drive more people out of small towns, further reducing hospitals’ patient numbers and revenue.
The type of hospital services that states will assess matters, said Tony Shih, a senior adviser at the Commonwealth Fund, a nonprofit focused on making health care more equitable.
“If the end result is that high-margin services are taken away from local hospitals with nothing given back in return, it can be financially harmful,” he said.
Shih noted that states’ plans to add more outpatient care could prove beneficial for patients. It’ll take time to know which states help stabilize rural hospitals, he said.
Rural hospital leaders say they know which changes would keep their facilities open and that states shouldn’t suggest or mandate service cuts and other changes on their behalf.

Josh Hannes, who oversees rural health policy at the Colorado Hospital Association, said “top-down” directives won’t work.
He said the association’s members believe they can find efficiencies and are eager to collaborate. But “a state agency shouldn’t be making those determinations,” he said.
Hannes said members are worried Colorado’s plan to classify rural health facilities as a “hub, spoke, or telehealth node” will compel service reductions. The classification will help determine “which services are sustainable locally and which are best provided regionally or through telehealth,” .
Spokespeople for the Colorado and Oklahoma health departments said no facility will be forced to end services. But Oklahoma spokesperson Rachel Klein said some facilities might choose to do so as part of a broader effort to make sure they’re meeting community needs while remaining financially stable.
“A hospital might shift certain services to a nearby regional provider with higher patient volume and specialized staff while expanding other local services,” such as primary, outpatient, or community-based care, she said.
Wiens and Darrell Messersmith, CEO of Dahl Memorial Hospital in the southeastern Montana town of Ekalaka, said they worry the only way hospitals will get their share of funding is to cut services or become Rural Emergency Hospitals that don’t offer inpatient services.
“I would hate to see things shift toward a pack-and-ship facility,” Messersmith said. “Right now, we function quite well as an inpatient facility.”
Not all Montana health leaders are worried.
Ed Buttrey, president and CEO of the Montana Hospital Association, said he thinks his state’s plan could help rural hospitals become financially sustainable and survive Medicaid cuts. Buttrey is also a Republican state lawmaker.
Chauvet, the Big Sandy rancher, said his perspective on whether remote towns like his should have a hospital is forever changed because of his accident.
“I always would say, тАШOh, they’re nice to have,’ but now I look at the hospital and say, тАШThat’s essential to our community,’” he said.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/rural-emergency-hospitals-montana-rightsize-downsize-services-transformation-fund/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2172028&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But plans to spend those nine-digit awards aren’t all warmly received.
At least one group of Republican state lawmakers appears to have scuttled an initiative preapproved by federal officials. And at least one hospital association persuaded its state health leaders to alter who greenlights spending. Other critics are taking a more cautious approach.
That’s because the Centers for Medicare & Medicaid Services, which manages the five-year Rural Health Transformation Program, says states could lose money if they make major changes to the plans approved in their applications. Changes could also delay states’ ability to get projects rolling in time to show the agency that they’re meeting progress deadlines.
“During the application period, states were advised to only propose initiatives and state policy actions that the state deemed feasible,” said CMS spokesperson Catherine Howden, who noted that the agency will work with states case by case.
The recent pushback reflects “tension” over state plans тАФ which were approved by the federal government тАФ from state lawmakers and health leaders who want more input amid tight deadlines, said Carrie Cochran-McClain, chief policy officer of the National Rural Health Association, the largest organization representing rural hospitals and clinics.
Cochran-McClain said many states must pass a bill to allow federal dollars to be spent and added that because the program rolled out so quickly “there’s important work that still needs to be done in some states between the legislatures and the governors.”
State lawmakers want to have a say, she said, in “how the funding is being allocated тАФ how the implementation will go.”
Congressional Republicans created the program as a last-minute sweetener to include in their One Big Beautiful Bill Act, signed into law last summer. The funding was intended to offset concerns about the anticipated in rural communities from the law, which is expected to slash Medicaid spending by nearly $1 trillion over a decade.
CMS officials announced first-year funding тАФ ranging from $147 million for New Jersey to $281 million for Texas тАФ on Dec. 29, after scoring applications. Federal officials will begin evaluating progress in late summer and announce 2027 allocations at the end of October.
A chorus of critics say the program won’t make up for harm caused by Medicaid cuts.
The program is “a complete sham,” Sen. Ron Wyden (D-Ore.) said at a rural policy conference in February.
Medicaid, a joint federal-state program for low-income and disabled Americans, serves nearly , and many rural hospitals depend on it to stay afloat.
But the rural health program tilts toward seeding innovative projects and technologies, not shoring up rural hospital finances. States can use only up to 15% of their funding to pay providers for patient care.
That hasn’t stopped some federal officials and lawmakers from framing the program as a rural hospital rescue.
For example, the White House , “President Trump secured $50 billion in funding for rural hospitals.”
Now that applications have been approved, some state Republican lawmakers тАФ who are than Democrats are тАФ and hospital associations are upset that the political rhetoric doesn’t match what they see.
They’re also lobbing criticisms at specific aspects of their states’ plans, including the proposed projects, what’s not included, and the spending approval process.
In Wyoming, lawmakers didn’t just criticize an initiative from their state’s application. They moved to kill it.
State Rep. John Bear, a Republican, said he and other lawmakers declined to fund “BearCare,” a proposed state-sponsored health insurance plan that patients could use only after medical emergencies. But they did approve other aspects of the rural health program.
The Wyoming Department of Health won’t “proceed with BearCare without express legislative authority to do so,” said spokesperson Lindsay Mills.
While Wyoming lawmakers removed an initiative from their state’s rural health plan, a group in Ohio wants to add something.
Ohio Rep. Kellie Deeter and other Republican lawmakers to use the maximum allowed funding for provider payments тАФ 15% тАФ to support 13 independent, rural hospitals.
“We understand that the rural transformation fund is not designed to be given directly to prop up hospitals,” Deeter said. “We just want to capitalize on the mechanism of the fund that can be utilized for that purpose.”
Those hospitals “operate with very, very narrow margins, and it’s just difficult and, frankly, unsustainable,” she added.
Ken Gordon, a press secretary responding for the governor’s office and the state health department, said, “It’s still very early in this process, and many details are being worked out.”
State lawmakers around the country are also trying to ensure the federal program’s dollars benefit rural areas.
In North Dakota, Rep. Bill Tveit, a Republican who lives in a town with about 2,000 residents, that would have required the state to reserve its funding for programs located more than 35 miles from urban areas and small cities.
During a hearing, lawmakers appeared sympathetic to Tveit’s concerns but quickly shot down his idea.
State Sen. Brad Bekkedahl said the North Dakota health department already committed to prioritizing funding for the most pressing rural health needs. He also said he’s concerned any significant changes could cause the state to lose funding because CMS already reviewed and approved the plan.
Meanwhile, Republican lawmakers in Michigan and North Carolina have criticized their states’ definitions of “partially rural” or “rural,” saying that counties that include urban population centers could take money from lower-density counties, according to and .
Lawmakers aren’t the only ones speaking out.
The Colorado Hospital Association to state lawmakers denouncing how the state created its plan and two of its proposed initiatives.
“Not only were Colorado’s rural hospitals’ recommendations disregarded,” president and CEO Jeff Tieman wrote, but the plan includes ideas “they actively oppose and believe will harm the communities they serve.”
The department responded to one of the association’s concerns by adding rural health leaders to the .
Meanwhile, and Nebraska, some health groups are upset that their states’ plans lack specific funding streams for rural hospitals.
Lauren LaPine-Ray, who oversees rural health policy at the Michigan Health & Hospital Association, predicted the state’s rural hospitals will compete with other organizations, such as academic centers and health clinics, for funding. She said about 65% of the group’s rural members have never applied for a state grant before.
“The rural hospitals, the ones that really need the funding the most, will not be well equipped to apply for and pull down these dollars,” LaPine-Ray said.
Jed Hansen, executive director of the Nebraska Rural Health Association, said the federal funding won’t go to “rural hospitals, rural clinics, and rural providers in a meaningful way.”
“Rural Health Transformation will not save a single hospital in our state,” he said. “I don’t think it will save a hospital nationally.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/rural-transformation-fund-lawmakers-health-groups-resist-state-spending-plans/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2161929&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Because they aren’t U.S. citizens, they would each need a visa.
West River and other companies used to pay up to $5,000 in fees to sponsor each H-1B visa for such workers.
The nonprofit hospital now has to pay $100,000 if it wants to hire one of the new applicants, who are all from the Philippines or Nigeria. Or it could spend money on an attorney to petition the government for an exemption from the new fee.
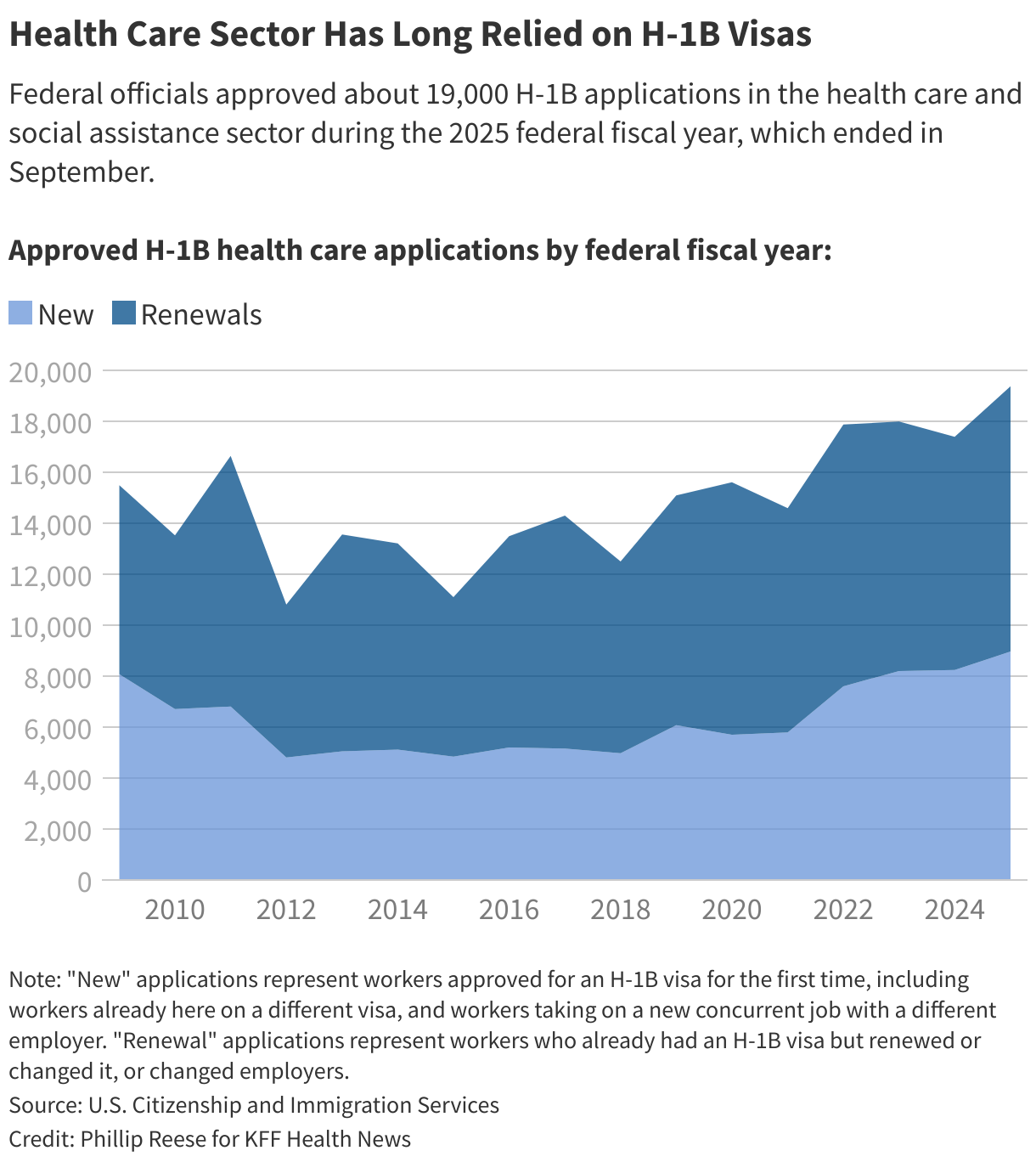
H-1B visas are for highly skilled foreign workers in fields тАФ such as the chronically understaffed rural health system тАФ that struggle to find enough American employees.
In September, President Donald Trump increased the visa fee to $100,000 for workers living outside the U.S. It doesn’t apply to foreign workers or students who were already in the U.S. on a visa.
His proclamation rails against the tech world’s use of H-1B workers, but the new fee applies to all fields.
“The health care industry wasn’t even considered. They’re going to be collateral damage, and to such an extreme degree that it was clearly not thought about at all,” said Eram Alam, a Harvard associate professor whose examines the history of foreign doctors in the U.S.
H-1B applicants will receive a fee exemption only in an “extraordinarily rare circumstance.”
The , two , and asked Homeland Security Secretary Kristi Noem to grant categorical exemptions for the health care industry. The new cost will disproportionally harm rural communities that already struggle to afford and recruit enough providers, the groups argued.
DHS officials directed inquiries to the White House, which did not answer questions about individual waiver timelines or the possibility of an exemption for the health care industry.
Instead, White House spokesperson Taylor Rogers sent a statement defending the new fee, saying it will “put American workers first.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/the-week-in-brief-rural-health-h1b-visa-fee/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2130398&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Not one U.S. citizen has applied.
West River Health Services in Hettinger, a town of about 1,000 residents in the southwestern part of the state, has four options, and none is good.
The hospital could fork over $100,000 for the Trump administration’s new H-1B visa fee and hire one of the more than 30 applicants from the Philippines or Nigeria. The fee is the equivalent of what some rural hospitals would pay two lab techs in a year, said Holzkamm, who is West River’s lab manager.
West River could ask the Department of Homeland Security to waive the fee. But it’s unclear how long the waiver process would take and if the government would grant one. The hospital could continue trying to recruit someone inside the U.S. for the job. Or, Holzkamm said, it could leave the position unfilled, adding to the workload of the current “skeleton crew.”
The U.S. health care system depends on foreign-born professionals to fill its ranks of doctors, nurses, technicians, and other health providers, particularly in chronically understaffed facilities in rural America.
But a new presidential proclamation aimed at the tech industry’s use of H-1B visas is making it harder for West River and other rural providers to hire those staffers.
“The health care industry wasn’t even considered. They’re going to be collateral damage, and to such an extreme degree that it was clearly not thought about at all,” said Eram Alam, a Harvard associate professor whose new book examines the history of foreign doctors in the U.S.
Elissa Taub, a Memphis, Tennessee-based attorney who assists hospitals with the H-1B application process, has been hearing concerns from her clients.
“It’s not like there’s a surplus of American physicians or nurses waiting in the wings to fill in those positions,” she said.
Until recently, West River and other employers paid up to $5,000 each time they applied to sponsor an H-1B worker. The visas are reserved for highly skilled foreign workers.
The new $100,000 fee — part of a by President Donald Trump — applies to workers living outside the U.S. but not those who were already in the U.S. on a visa.
West River lab tech Kathrine Abelita is one of nine employees — six technicians and three nurses — at the hospital who are current or former H-1B visa holders. Abelita is from the Philippines and has worked at West River since 2018. She’s now a permanent U.S. resident.
“It’s going to be a big problem for rural health care,” she said of the new fee. She said most younger American workers want to live in urban areas.
Sixteen percent of registered nurses, 14% of physician assistants, and 14% of nurse practitioners and midwives who work in U.S. hospitals are immigrants, according to a . Nearly a quarter of physicians in the U.S. went to medical school outside the U.S. or Canada, according to .
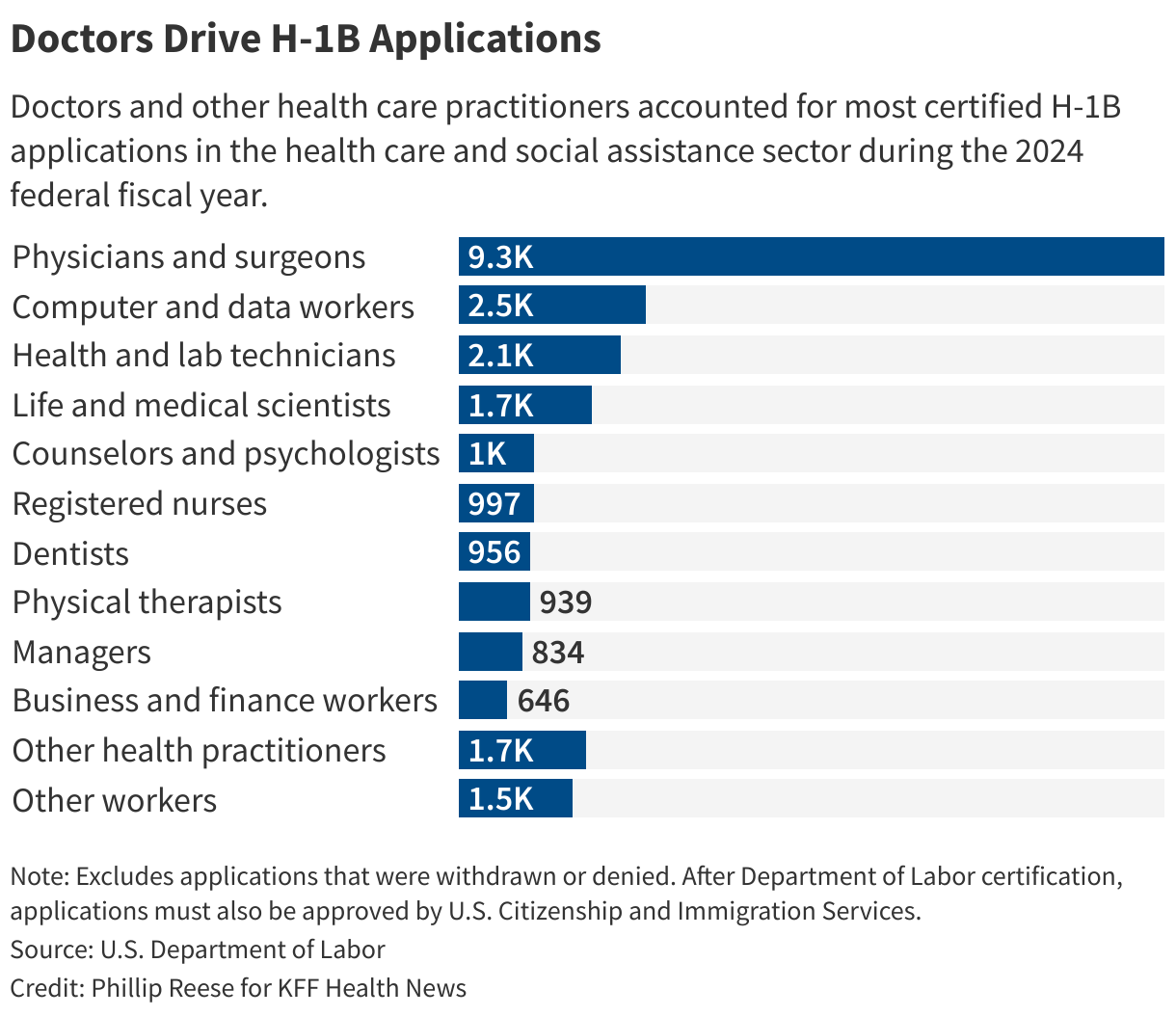
The , two , and have asked the administration to give the health care industry exemptions from the new fee. The new cost will disproportionally harm rural communities that already struggle to afford and recruit enough providers, the groups argue.
“A blanket exception for healthcare providers is the simplest path forward,” the National Rural Health Association and National Association of Rural Health Clinics wrote in a joint letter.
The proclamation allows fee exemptions for individuals, workers at specific companies, and those in entire industries when “in the national interest.” says the fee will be waived only in an “extraordinarily rare circumstance.” That includes showing that there is “no American worker” available for the position and that requiring a company to spend $100,000 would “significantly undermine” U.S. interests.
Taub called those standards “exceptionally high.”
Representatives of the NRHA and the American Medical Association, which organized a letter from the medical societies, said they’ve received no response after sending requests to Homeland Security Secretary Kristi Noem in late September and early October. The AHA declined to say whether it had heard back.
Homeland Security officials directed ║┌┴╧│╘╣╧═Ї News’ inquiries to the White House, which did not answer questions about individual waiver timelines or the possibility of a categorical exemption for the health care industry.
Instead, White House spokesperson Taylor Rogers sent a statement defending the new fee, saying it will “put American workers first.” Her comments echo Trump’s proclamation, which focuses on accusations that the tech industry is abusing the H-1B program by replacing American workers with lower-paid foreign ones. But the order applies to all trades.
Alam, the Harvard professor, said the U.S.’ reliance on international providers does raise legitimate concerns, such as about how it takes professionals away from lower-income countries facing even greater health concerns and staffing shortages than the U.S.
This decades-long dependency, she said, stems from population booms, medical schools’ historical exclusion of nonwhite men, and the “much, much cheaper” cost of importing providers trained abroad than expanding health education in the U.S.
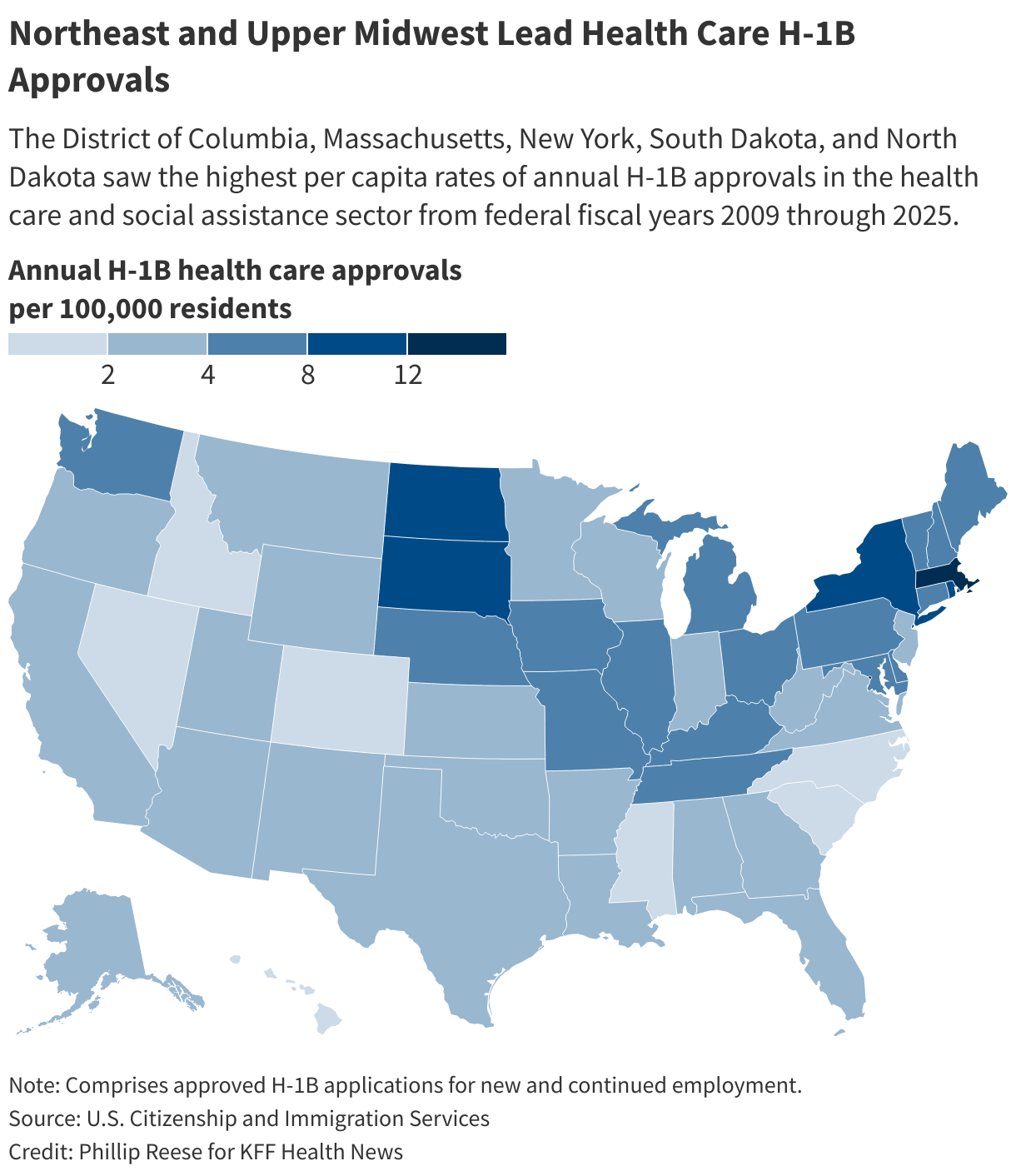
Internationally trained doctors tend to work in rural and urban areas that are poor and underserved, according to and .
Nearly 1,000 H-1B providers were employed in rural areas this year, the two rural health organizations wrote in their letter to the Trump administration.
J-1 visas, the most common type held by foreign doctors during their residencies and other postgraduate training in the U.S., require them to return to their home country for two years before applying for an H-1B.
But a government program called the Conrad 30 Waiver Program allows up to 1,500 J-1 holders a year to remain in the U.S. and apply for an H-1B in exchange for working for three years in a provider shortage area, which includes many rural communities.
Trump’s proclamation says employers that sponsor H-1B workers already inside the U.S., such as doctors with these waivers, won’t have to pay the six-figure fee, a nuance clarified in guidance released about a month later.
But employers will have to pay the new fee when hiring doctors and others who apply while living outside the U.S.
Alyson Kornele, CEO of West River Health Services, said most of the foreign nurses and lab techs it hires are outside the U.S. when they apply.
Ivan Mitchell, CEO of Great Plains Health in North Platte, Nebraska, said most of his hospital’s H-1B physicians were inside the U.S. on other visas when they applied. But he said physical therapists, nurses, and lab techs typically apply from abroad.
Holzkamm said it took five to eight months to hire H-1B applicants at her lab before the new fee was introduced.

Bobby Mukkamala, a surgeon and the president of the American Medical Association, said Republican and Democratic lawmakers are concerned about the ramifications for rural health care.
They include Senate Majority Leader John Thune, who said he planned to reach out about possible exemptions.
“We want to make it easier, not harder, and less expensive, not more expensive, for people who need the workforce,” the Republican told ║┌┴╧│╘╣╧═Ї News in September.
Thune’s office did not respond to questions about whether the senator has heard from the administration regarding potential waivers for health workers.
The Trump administration is facing at least two lawsuits attempting to block the new fee. includes a company that recruits foreign nurses and a union that represents medical graduates. , by the U.S. Chamber of Commerce, mentions concerns about the physician shortage and health systems’ ability to afford the new fee.
Kornele said West River won’t be able to afford a $100,000 fee so it’s doubling down on local recruiting and retention.
But Holzkamm said she hasn’t been successful in finding lab techs from North Dakota colleges, even those who intern at the hospital. She said West River can’t compete with the salaries offered in bigger cities.
“It’s a bad cycle right now. We’re in a lot of trouble,” she said.
Phillip Reese is a data reporting specialist and an associate professor of journalism at California State University-Sacramento.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/h1b-visa-fee-rural-hospitals-foreign-worker-shortages-north-dakota/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2123805&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Federally recognized tribes can’t directly apply for a share of the rural health fund тАФ only states can. And states aren’t required to consider tribes’ needs. But state applications for the five-year payout show some states with significant Native American populations did so anyway.
Workforce development, technology upgrades, and traditional healing are a few of the initiatives specifically aimed at Native American communities that some states included in their applications, which were due to the Centers for Medicare & Medicaid Services on Nov. 5. The fund was a late addition to the One Big Beautiful Bill Act in response to worries about the harm the spending reductions in Republicans’ bill would have on rural hospitals’ finances.
Some states, , Nevada, , are also considering setting aside 3% to 10% of their federal payouts to distribute among tribes. Washington proposed setting aside $20 million per year.
Federally recognized tribes have direct relationships with the U.S. government, but state governments also allocate resources to tribes and can create policies that support tribal priorities. States and tribes share concerns about the effect that the massive GOP budget bill, which President Donald Trump signed into law in July, will have on the U.S. health system. The law is expected to reduce federal Medicaid spending by nearly $1 trillion and increase the number of uninsured by , according to KFF, a health information nonprofit that includes ║┌┴╧│╘╣╧═Ї News.
Catherine Howden, a CMS spokesperson, said that states are required to develop their applications in collaboration with key stakeholders, including the state governments’ tribal affairs offices or tribal liaisons, as well as “Indian health care providers, as applicable.” But these entities do not include tribal governments or official tribal representatives.
Tribes can apply for Rural Health Transformation Fund subgrants through their states. But during a recent call with federal health officials, tribal leaders expressed frustration about being regarded as just another stakeholder in the issue rather than sovereign nations. Tribal sovereignty guides most government-to-government consultations over proposed federal actions that would have a substantial effect on tribes.
“Even in a scenario where tribal consultation is required, the quality and quantity of that tribal consultation on a state-by-state basis is all over the place,” said Liz Malerba, director of policy and legislative affairs for the United South and Eastern Tribes Sovereignty Protection Fund, which advocates for tribal nations from Texas to Maine. Malerba is a citizen of the Mohegan Tribe.
Federal policy works better when tribal nations are directly eligible for funding that supports essential services in their communities, Malerba said, adding that tribal leaders are concerned that the reach of the program into their communities will vary considerably.
There are and Native American and Alaska Native people in the U.S. The population faces a lower life expectancy and when compared with other demographics. The Indian Health Service, the federal agency responsible for providing health care to Native Americans and Alaska Natives, has been by Congress.
║┌┴╧│╘╣╧═Ї News analyzed how 12 states with significant Native American populations took tribes into account as they developed plans for the pot of federal money.
, , , and were among the states that held tribal consultations or listening sessions ahead of the Nov. 5 application deadline.
In states that did not initiate input from tribes, some Native American leaders made sure their voices were heard in other public hearings. Jerilyn Church, CEO of the Great Plains Tribal Leaders’ Health Board, said she attended an October public meeting in South Dakota because she felt it was important for state leaders to consider how they could use the program’s resources on reservations. There are nine federally recognized tribes in the state, and Native American people make up 9% of the population.
“I felt like we needed to help be that advocate,” said Church, a citizen of the Cheyenne River Sioux Tribe.
In the proposed initiatives included in its rural fund application, South Dakota such as improved telehealth and funding for doula programs. It also said the state will continue meeting with the Great Plains tribal health board throughout the five-year funding cycle.
In Oklahoma тАФ where more than 14% of the population is Native American, a higher share than in most other states тАФ tribal representatives were invited to weigh in with the rest of the public when the state was gathering information for its application, the details of which have not been publicly released.
“We’ve welcomed input from any Oklahoman,” said state health department spokesperson Erica Rankin-Riley.
North Dakota in the Rural Health Transformation Program and included initiatives such as expanding physician residency slots with tribal-specific rotations and opportunities for farm-to-table food distributions. But that would have pledged 5% of its federal allotment to tribes. There are five federally recognized tribes in the state, and Native Americans make up nearly 5% of the population.
Some states did include proposals to fund high-priority initiatives for tribes.
for the rural fund included an initiative focused on improving health among Native American communities. Its goals include investing in workforce development for tribes, better care coordination between tribes and rural hospitals, and $2.4 million annually to support Washington State University’s rural health education programs, including its Indigenous health program.
included integrating Indigenous traditional healing in Alaska Native village clinics. It would include offering traditional-healing house calls, hands-on training for healers, and traditional-medicine training for health care providers and staff, according to the application.
One of would support the state’s nine federally recognized tribes in improving health outcomes. The state estimates the initiative would require $20 million per year, or 10% of the Rural Health Transformation Program award.
Whether or not states identified funding for tribes or included tribal priorities in their proposals, tribes will be eligible to apply to their states for subgrants of the Rural Health Transformation Program money. While larger tribes that have more resources, such as grant writers and staff to implement programs, could benefit, smaller tribes may struggle to produce competitive applications.
Church said that the Great Plains Tribal Leaders’ Health Board will know the fruits of its labor when states are notified of their rural health fund allotments by the end of the year.
“Hopefully the work that we did, the advocacy that we did, and the outreach,” Church said, “will result in resources getting to our tribes.”
║┌┴╧│╘╣╧═Ї News South Dakota correspondent Arielle Zionts contributed to this report.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/race-and-health/native-american-tribes-rural-health-transformation-program/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2124087&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The Trump administration, which has promised “radical transparency,” that it plans to publish the “project summary” for states that win awards. Following the lead of federal regulators, many states are withholding their complete applications, and some have refused to release any details.
“Let’s be clear,” said Alan Morgan, chief executive of the National Rural Health Association. “The hospital CEOs, the clinic administrators, the community leaders: They’re going to want to know what their states are doing.” The NRHA’s members include struggling rural hospitals and clinics, which would benefit from the Trump administration’s Rural Health Transformation Program.
Morgan said his members are interested in what states propose, which of their ideas are approved or rejected, and their budget narratives, which detail how the money could be spent.
Improving rural health care is an “insanely complicated and difficult task,” Morgan said.
The five-year Rural Health Transformation Program was approved by Congress in a law — the One Big Beautiful Bill Act — that also drastically cuts Medicaid spending, on which rural providers heavily depend. It’s being watched closely because it’s a much-needed influx of funds — with a caveat from the Trump administration that the money be spent on transformational ideas, not just to prop up ailing rural hospitals.
The law says half of the $50 billion will be divided equally among all states with an approved application. The rest will be distributed through a points-based system. Of , $12.5 billion will be allotted based on each state’s rurality. The remaining $12.5 billion will go to states that on initiatives and policies that, in part, mirror the Trump administration’s “” objectives.
Health and Human Services Secretary Robert F. Kennedy Jr. has repeatedly promised to open the government to the American people. His agency has devoted to “radical transparency.”
“We’re working to make this the most transparent HHS in its 70-year history,” in written testimony to lawmakers in September.
Lawrence Gostin, a professor of public health law at Georgetown University, said HHS is “acting in a way that utterly lacks transparency” and that the public has the right to demand “greater openness and clarity.” Without transparency, the public cannot hold HHS accountable, he said.
Centers for Medicare & Medicaid Services spokesperson Catherine Howden said the agency will follow the federal regulations when releasing information about the rural health program.
Grant applications are “not released to the public during the merit review process,” Howden said, adding, “The purpose of this policy is to protect the integrity of evaluations, applicant confidentiality, and the competitive nature of the process.”
Democrats and many health care advocates are concerned politics will affect how much money states get.
“I am very concerned about retaliation,” said Rep. Nikki Budzinski (D-Ill.). Because Democrats control her state’s politics, “our application might not be as seriously considered as other states that have Republican leadership,” she added.
Illinois’ Democratic members of the U.S. House to CMS Administrator Mehmet Oz in November asking for “full and fair consideration” of their state application. Illinois officials have not yet released their state’s proposal to ║┌┴╧│╘╣╧═Ї News, which has a pending public records request.
Heather Howard, a professor of the practice at Princeton University, said she is “pleasantly surprised at how transparent the states have been.”
Howard directs the university’s State Health and Value Strategies program, which the rural health fund, and praised most states for publicly posting their project summaries.
“To me, it speaks to the intense interest in this program,” Howard said. Her team, reviewing about two dozen state summaries, found themes including expansion of home-based and mobile services, increased use of technology, and workforce development initiatives like scholarships, signing bonuses, and child care assistance for high-demand positions.
“I think it’s exciting,” Howard said. “What’s great here is the experimentation we’re going to learn from.”
Telerobotics appeared in Georgia’s and Alabama’s applications, she said, including a proposal to use robotic equipment for remote ultrasounds.
Another theme that “warms my heart,” Howard said, was the effort among states to create advisory groups or committees, including in Idaho, where work groups are expected to focus on technology, workforce development, tribal collaboration, and behavioral health.
All 50 states submitted applications to federal regulators by the Nov. 5 deadline and awards will be announced by the end of the year, according to CMS.
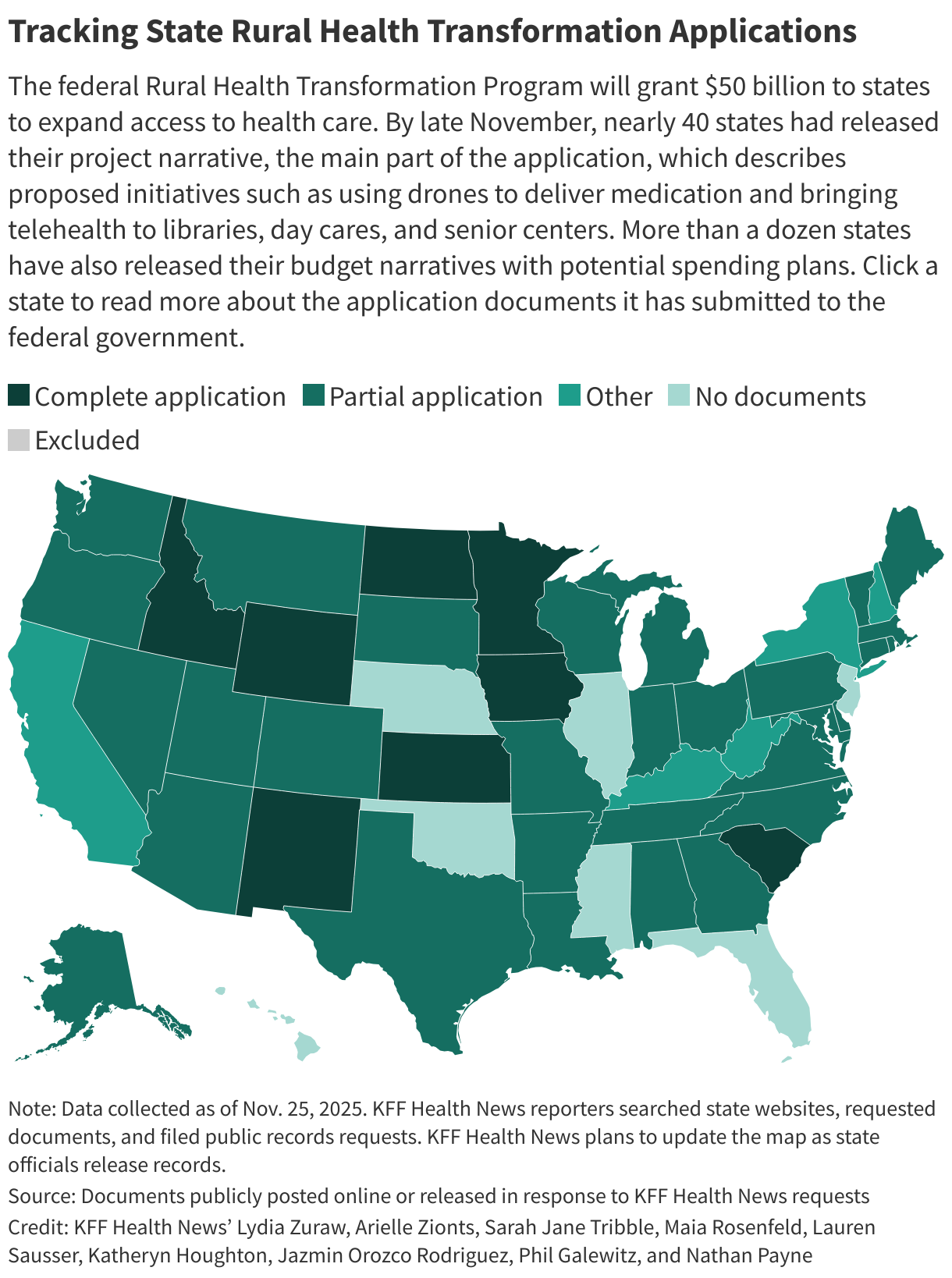
As of late November, nearly 40 states had released their project narrative, the main part of the application, which describes proposed initiatives, according to ║┌┴╧│╘╣╧═Ї News tracking. More than a dozen states have also released their budget narratives.
Also as of late November, only a handful of states — Idaho, Iowa, Kansas, Minnesota, New Mexico, North Dakota, South Carolina, and Wyoming — had released all parts of the application.
║┌┴╧│╘╣╧═Ї News filed public records requests for states’ complete applications. Some states have refused to release any of their application materials.
Nebraska, for example, rejected a public records request, saying its application materials are “proprietary or commercial information” that “would give advantage to business competitors.”
Kentucky shared its application summary but said the remainder of the application is a “preliminary draft” not subject to release under state laws.
Erika Engle, a spokesperson for Hawaii Gov. Josh Green, said the governor “is committed to transparency” but declined to share any of the state’s proposal.
Hawaii and other states are still processing formal public records requests.
The rural health program is part of the July law projected to reduce federal Medicaid spending in rural areas by 10 years.
Those cuts are expected to affect rural health facilities’ bottom lines, threatening their ability to stay open. A recent Commonwealth Fund report found that rural areas continue to to primary care. But the guidelines for the rural health program say states can use only 15% of their new funding to pay providers for patient care.
Between the Medicaid cuts and funding boost from the new program, “there’s real opportunity for national policy to impact rural, both in the negative and the positive potentially,” said Celli Horstman, a senior research associate at the New York-based policy think tank who co-authored the report.
Among the publicly available rural health transformation proposals, Democratic-leaning states show support, or are willing to adopt, some of the administration’s goals but will lose out on points from eschewing others.
For example, New Mexico said it would introduce legislation requiring students to take the Presidential Fitness Test and physicians to complete continuing education courses on nutrition. But it won’t prevent people from using their Supplemental Nutrition Assistance Program benefits to buy “non-nutritious” foods such as soda and candy.
Many states want to invest in technology, including telehealth, cybersecurity, and remote patient monitoring equipment. Other themes include increasing access to healthy food, improving emergency services, preventing and managing chronic illnesses, and enlisting community health workers and paramedics for home visits.
Specific proposals include:
- Arkansas wants to spend $5 million through its “FAITH” program — Faith-based Access, Interventions, Transportation, & Health — to enlist rural religious institutions to host education and preventive screening events. Congregations could also install walking circuits and fitness equipment.
- Alaska, which historically relied on dogsled teams to bring medication to remote areas, is looking to test the use of “unmanned aerial systems” to speed up pharmacy deliveries to such communities.
- Tennessee wants to increase access to healthy activities by spending money on parks, trails, and farmers markets.
- Maryland wants to start mobile markets and install refrigerators and freezers to improve access to fresh, healthy food that often spoils in rural areas with few grocery stores.
State Sen. Stephen Meredith, a Republican who represents part of western Kentucky, said he still expects rural hospitals to close despite his state’s rural health transformation program.
“I think we’re treating symptoms without curing the disease,” he said after listening to a presentation on Kentucky’s proposal at .
Morgan, whose organization represents rural hospitals likely to close, said the state’s ideas may sound good.
“You can craft a narrative that sounds wonderful,” he said. “But then translating the aspirational goals to a functioning program? That’s difficult.”
║┌┴╧│╘╣╧═Ї News staffers Phil Galewitz, Katheryn Houghton, Tony Leys, Jazmin Orozco Rodriguez, Maia Rosenfeld, Bram Sable-Smith, and Lauren Sausser contributed to this report.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/rural-health-transformation-program-cms-state-applications-transparency/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2123985&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The 27-year-old resident of Bloomington, Indiana, has a pacemaker and a painful joint disease. She also has fused vertebrae in her neck from a spinal injury, preventing her from turning her head.
Indiana’s Medicaid agency currently considers Brader “medically frail,” giving her access to an expanded set of benefits, such as physical therapy.
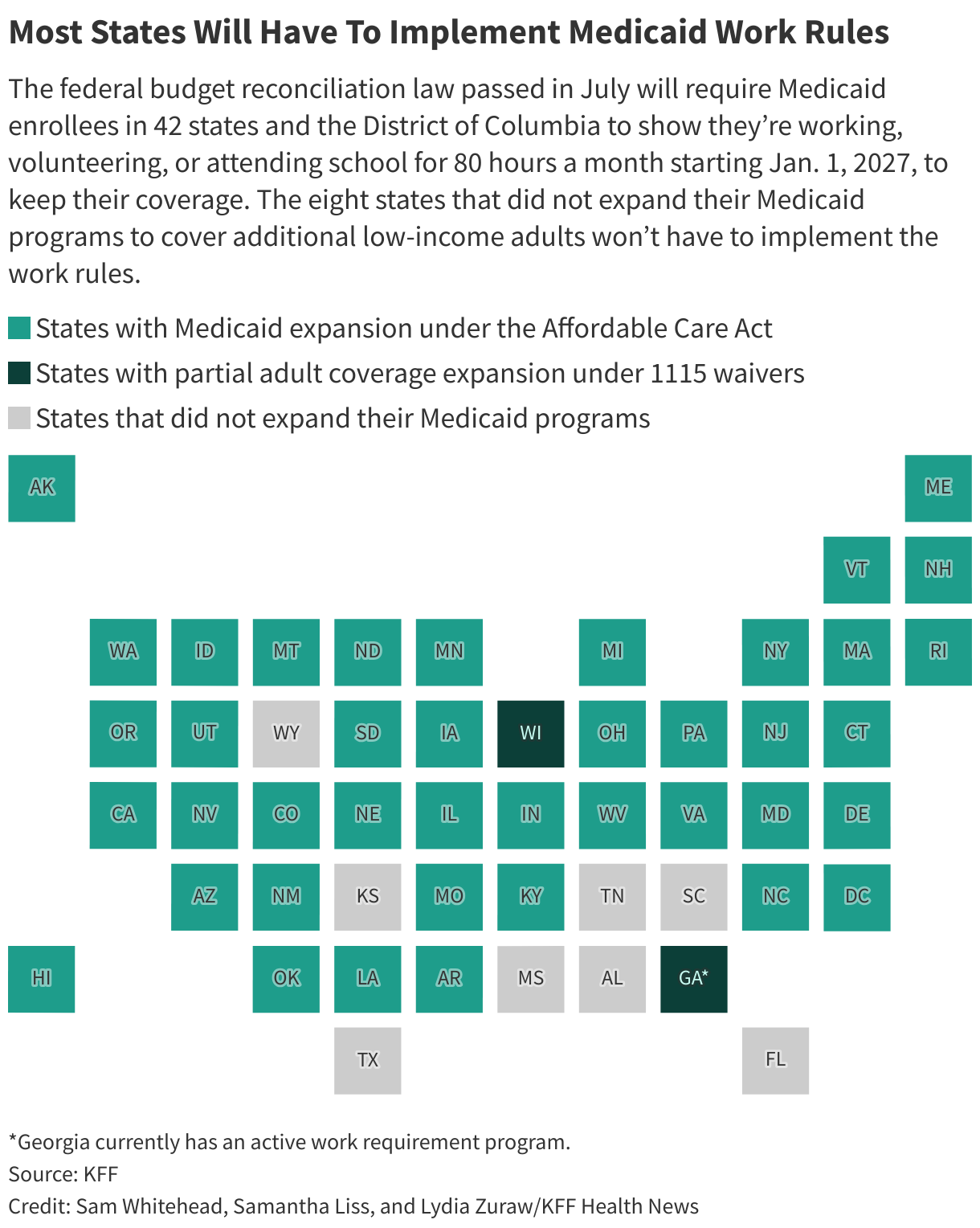
New federal rules will require more than 18 million Medicaid enrollees nationwide to show they’re working, volunteering, or going to school for 80 hours a month starting in 2027 to keep their coverage. Brader is exempt as long as she’s deemed medically frail.
But lacking sufficient federal guidance, states are wrestling with how to define medical frailty — a consequential decision that could cut Medicaid coverage for many people, said state officials, consumer advocates, and health policy researchers.
“It’s terrifying,” Brader said. “I already have fought so hard to get my health care.”
‘Incredibly High’ Stakes
President Donald Trump’s One Big Beautiful Bill Act slashes nearly $1 trillion from Medicaid over the next decade, with much of the savings projected to come from no longer covering those who don’t qualify under the new work rules. Those spending cuts help offset the costs of GOP priorities, such as extra border security and tax cuts that mainly benefit the wealthy.
Conservative lawmakers have argued that Medicaid, the government health insurance program for people with low incomes or with disabilities, has grown too large and expensive, especially in the wake of its expansion to more low-income adults under the Affordable Care Act. They also say that requiring participants to work is common sense.
The work rules in Trump’s tax-and-spending law offer exemptions for several groups who might struggle to meet them, including people deemed “medically frail.” The law spells out certain “medically frail” conditions such as blindness, disability, and substance use disorder. But it does not list many others.
Instead, the law exempts those with a “serious or complex medical condition,” a term whose interpretation could vary by state.
State officials say they need more clarity to ensure that people who cannot work for health reasons retain rightful access to Medicaid. They also worry that, even with a clear definition, people will face the onerous task of having to regularly vouch for being medically frail, which is a challenge without reliable access to medical care.
“The stakes are incredibly high,” said Kinda Serafi, a partner at consulting firm Manatt Health.
The new work requirements will affect Medicaid recipients in 42 states and Washington, D.C. Eight states — Alabama, Florida, Kansas, Mississippi, South Carolina, Tennessee, Texas, and Wyoming — did not expand their Medicaid programs to cover additional low-income adults, so they won’t have to implement the work rules.
The Medicaid work rules are expected to be the over the next decade, according to the nonpartisan Congressional Budget Office.
Forty-four percent of all adults covered by states’ expanded Medicaid programs , according to KFF.
A Challenge for States
State Medicaid agencies are scrambling to implement the rules with little direction from the U.S. Department of Health and Human Services, which has yet to issue specific guidance. Federal officials will clarify the “medically frail” definition next year, said Andrew Nixon, an agency spokesperson.
Ultimately, states will have to decide who is unhealthy enough to be exempt from work rules. And it won’t be easy for state workers and their computer systems to track.
Every year, state eligibility systems screen millions of applicants to check if they qualify for Medicaid and other government programs. Now, these same systems must screen applicants and existing enrollees to determine whether they meet the new work rules.
Jessica Kahn, a partner at consulting firm McKinsey & Co., has urged states to start planning how to adapt eligibility systems to verify work status. States can do a “tremendous amount” of work without direction from the federal government, said Kahn, a former federal Medicaid systems official, who spoke during a recent Medicaid advisory panel hearing. “Time is a-wasting already.”
State Medicaid directors are pondering the challenge.
“Medical frailty gets so complex,” Emma Sandoe, Oregon’s Medicaid director, said during a recent panel discussion. Conditions that can keep people from working, such as mental health disorders, can be hard to prove, she said.
A state might try to use data pulled from a person’s health records, for instance, to determine medical frailty. But information from a patient’s chart may not paint a clear picture of someone’s health, especially if they lack regular access to medical care.
It’s a tall order for eligibility systems that historically have not had to scrape medical records to screen applicants, said Serafi of Manatt Health.
“That is an incredibly new thing that eligibility enrollment systems are just not fluent in at all,” Serafi said.
Lobbying groups for the private health insurance companies that help run Medicaid in many states also have urged federal regulators to clearly define medical frailty so it can be applied uniformly.
In a to federal officials, the Medicaid Health Plans of America and the Association for Community Affiliated Plans advocated for allowing enrollees to qualify for the exemption by saying on their applications that they have conditions that make them medically frail. Successfully implementing exemptions for the medically frail will be “crucial” given the “severe health risks of coverage loss for these populations,” the groups said.
Some state officials worry about unintended consequences of the work rules for people with chronic conditions.

Jennifer Strohecker, who recently resigned as Utah’s Medicaid director, reiterated the high stakes, especially for those with diabetes on Medicaid. They may be very healthy and functional with insulin, but if they fail to complete the work requirements, that may change, Strohecker said during a recent Medicaid advisory hearing.
Whether someone is deemed medically frail already depends heavily on where they live.
For example, in Arkansas, people indicate on their Medicaid applications that they’re disabled, blind, or need help with daily living activities.
Approximately 6% of the roughly 221,000 people enrolled in Arkansas’ Medicaid expansion program are deemed medically frail, according to Gavin Lesnick, a spokesperson for the Arkansas Department of Human Services.
In West Virginia, the state accepts a medical frailty designation when an applicant self-reports it.
The burden of proof is higher in North Dakota. Applicants there must answer a questionnaire about their health and submit additional documentation, which may include medical chart notes and treatment plans. More than half of applicants were denied last year, according to Health and Human Services Department spokesperson Mindy Michaels.
Indiana’s Family and Social Services Administration, which runs its Medicaid program, declined an interview and said it could not comment on individual cases, like Brader’s.
Brader worries the additional red tape will cause her to lose Medicaid again. She said she was temporarily kicked off the program in 2019 for failing to meet the state’s work rules when Indiana said her work-study job didn’t count as employment.
“Anytime I have tried to receive help from the state of Indiana, it has been a bureaucratic nightmare,” she said.
As states await federal guidance, Kristi Putnam, a senior fellow at the conservative Cicero Institute and former secretary of the Arkansas Department of Human Services, which oversees the state Medicaid program, said even if a state creates an extensive list of qualifying “medically frail” conditions, the line must be drawn somewhere.
“You can’t possibly create a policy for exemptions that will catch everything,” she said.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/medicaid-work-rules-exempt-medically-frail-who-qualifies/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2120581&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Watts knew other missileers with similar cancers. But the connection really hit home later that same January day, when the results of a blood test revealed that Watts himself had chronic lymphocytic leukemia, a type of non-Hodgkin lymphoma.
“I don’t know if it was ironic or serendipitous or what the right word is, but there it was,” Watts said.
Within the community of U.S. service members who staff nuclear missile silos scattered across the Northern Rockies and Great Plains, suspicions had long been brewing that their workplaces were unsafe. Just months after Watts was diagnosed in 2022, Lt. Col. Danny Sebeck, a former Air Force missileer who had transferred to the U.S. Space Force, wrote a brief on a potential cancer cluster among people who served at Minuteman III launch control centers on Malmstrom Air Force Base in Montana.
Sebeck identified who served primarily from 1993 to 2011 and had been diagnosed with cancer, including himself. Of those, 11 had non-Hodgkin lymphoma; three had died. The Air Force responded swiftly to Sebeck’s findings, into cancer cases and the environment at three intercontinental ballistic missile bases and a California launch facility. The goal is to complete the research by the end of 2025.
The service has released portions of the studies as they conclude, holding online town halls and briefings to highlight its findings. But while former missileers say they are heartened by the rapid response, they remain concerned that the research, which crosses decades and includes thousands of ICBM personnel and administrative workers, may address too large a population or use statistical analyses that won’t show a connection between their illnesses and their military service.
They need that tie to expedite benefits from the Department of Veterans Affairs.
Historically, the Department of Defense has been slow to recognize potential environmental diseases. Veterans sickened by exposure to Agent Orange in Vietnam, Marines who drank contaminated water at Camp Lejeune, North Carolina, and service members who lived and worked near burn pits in Iraq and Afghanistan fought for years to have their illnesses acknowledged as related to military service.
In the case of the missileers, the Air Force already had studied potential contamination and cancer at Malmstrom in and . That research concluded that launch control centers were “safe and healthy working environments.” But with Sebeck’s presentation and the decision to pursue further investigation, Air Force Global Strike Command тАФ the unit responsible for managing nuclear missile silos and aircraft-based nuclear weapons тАФ said the earlier studies may not have included a large enough sampling of medical records to be comprehensive.
Sebeck, who serves as co-director of the Torchlight Initiative, an advocacy group that supports ICBM personnel and their families, told congressional Democrats that the Defense Department has not accurately tracked exposures to the community, making it difficult for veterans to prove a link and obtain VA health care and disability compensation.
“I had to go to a VA person and pull some papers,” Sebeck said, referring to the government system for recording service members’ environmental risks. “It says that I visited Poland once. It doesn’t mention that I pulled 148 alerts in a launch control center with polychlorinated biphenyls and with this contaminated air and water.”
PCBs тАФ And the Missileers Exposed to Them
PCBs are synthetic chemicals once used in industry, including missile control electrical components such as display screens, keyboards, and circuit breakers. They have been banned for manufacture since 1979, deemed toxic and a likely carcinogen by the Environmental Protection Agency.
The Air Force’s Missile Community Cancer Study compares 14 types of common cancers in the general U.S. population and the missile community and also studies the environments at Malmstrom Air Force Base in Montana, F.E. Warren Air Force Base in Wyoming, Minot Air Force Base in North Dakota, and Vandenberg Space Force Base in California to determine whether they may have contributed to the risk of developing cancer.
The Malmstrom, Warren, and Minot bases together field 400 Minuteman III missiles, the land-based leg of the U.S. nuclear triad, which also includes submarine- and aircraft-launched nuclear weapons. The missiles are housed in silos spread across parts of Montana, North Dakota, Wyoming, Colorado, and Nebraska, staffed around the clock by missileers operating from underground, bunkerlike launch control centers.

So far, the Air Force investigation has found from cancer in the missile community compared with the general population, and it found that the death rates for four types of common cancers тАФ non-Hodgkin lymphoma, lung, colon and rectum, and prostate cancer тАФ were significantly lower in missileers than in the general population.
Non-Hodgkin lymphoma accounted for roughly 5.8% of all cancer deaths among people who worked in launch control centers from January 1979 to December 2020.
Early results, derived from Defense Department medical records, found elevated rates of breast and prostate cancers in the missile community, but a later analysis incorporating additional data did not support those findings. The studies also did not find increased rates of non-Hodgkin lymphoma. Air Force officials noted during a June 4 online town hall, however, that these assessments are based on roughly half the data the service expects to review for its final epidemiological reports and cautioned against drawing conclusions given the limitations.
The final incidence report will include federal and state data, including information from civilian cancer registries, and delve into subgroups and exposures, which may “provide deeper insights into the complex relationship” between serving in the missile community and cancer risk, wrote Air Force Col. Richard Speakman in a September 2024 memo on the initial epidemiology results.
Gen. Thomas Bussiere, commander of Air Force Global Strike Command, said during the June town hall that only the final results will determine whether the missile community’s cancer rates are higher than the general population’s.
Some lawmakers share the concern of missileers about the Air Force study. Following the release of a of Torchlight Initiative data that showed higher rates of non-Hodgkin lymphoma тАФ at younger ages тАФ among Malmstrom missileers, Rep. Don Bacon (R-Neb.) to a defense policy bill calling for the National Academies of Sciences, Engineering, and Medicine to review health and safety conditions in the facilities.
“Let’s make sure that we have some outside experts working with the Air Force studying cancer rates with our ICBM missions,” Bacon posted July 30 on the social platform X. “We want to ensure credibility and that whatever results come out, we’ve done total due diligence.”
Regarding additional studies on the working environments at the installations and a possible relationship between exposures and cancer risk, Speakman, who commands the Air Force School of Aerospace Medicine, said Malmstrom had two types of PCBs that the other two missile wing bases did not.
He added that benzene, found in cigarette smoke, vehicle exhaust, and gasoline fumes, was the largest contributor to cancer risk in reviews of the bases.
The assessment concluded that health risks to missileers is “low, but it’s not zero,” Speakman said. He said it would be appropriate to monitor the health of launch control workers.
Next Steps
Watts, whose story has been highlighted by the Torchlight Initiative, has asked the Defense Department’s inspector general to investigate тАФ the watchdog agency referred his request to Global Strike Command тАФ and is closely watching the Air Force research. He said the bulk of the cancer cases reported to Torchlight occurred in the 2000s, when ICBM personnel still used technology that contained PCBs, burned classified material such as treated paper and plastic coding devices indoors, and possibly were exposed to contaminated water.
“I open the door and there’s guys standing there in pressurized suits with sampling equipment,” Watts recalled. “They said, тАШWe’re here to check for contaminated water.’ I look at my crew commander, and we’re standing there in cotton uniforms. I said, тАШDo you see anything wrong with this?’”
Launch control operators no longer burn code tapes indoors and the Air Force has made improvements to air circulation in the centers. Sebeck wants Congress to consider including missileers and others sickened by exposure to base contamination in the PACT Act, landmark legislation that mandates health care and benefits for veterans sickened by burn pits and other pollutants.
“It’s documented that there is a large cancer cluster in Montana, probably also in Wyoming. People act surprised, but all they have to do is go to the oncology office in Denver. I can find my missileer buddies there. We are sitting in the same chairs getting chemotherapy,” Sebeck said.

Air Force Global Strike Command spokesperson Maj. Lauren Linscott said in response to Sebeck’s remarks that the unit understands the impact of cancer on its personnel and is committed to supporting them.
“While current findings are preliminary and no conclusions can yet be drawn, we are dedicated to a rigorous, peer-reviewed, data-driven process to better understand potential health risks because the safety of our airmen is our top priority,” Linscott said.
Bills introduced in the House and Senate would address the situation. In addition to Bacon’s amendment, the Senate version of an annual defense policy bill would require a “deep cleaning” of launch control centers every five years until the sites are decommissioned as a new ICBM, the Sentinel, replaces the Minuteman IIIs.
The Air Force aims to release its final epidemiological report by the end of the year.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/nuclear-missile-icbm-veterans-cancer-study-air-force-malmstrom-montana-colorado/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2089148&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The networks, which have cropped up in several states in recent years, offer small-town hospitals an alternative to selling to large hospital systems and forfeiting local autonomy.┬а
“We found that we could both have the power of negotiation as a larger entity but also be able to negotiate lower costs for services and equipment,” said Dennis Goebel, CEO of Southwest Healthcare Services, a Bowman hospital that is part of the 22-member Rough Rider Network in North Dakota.
Since 2010, 153 rural hospitals in the U.S. have either shuttered completely or cut inpatient services, according to the at the University of North Carolina. And 441 joined hospital chains between 2011 and 2021, commissioned by the Coalition to Strengthen America’s Healthcare, an advocacy group consisting of hospitals and health associations.
Proponents of the networks hope more collaborations will be fueled by the recently approved federal $50 billion Rural Health Transformation Program, which became law as part of the sweeping tax-and-spend measure backed by the Trump administration.
Many hospitals that join networks are motivated by the chance to combine their patient rolls for , a reimbursement model in which insurers pay providers based on the quality of care they provide and the health outcomes of their patients.
The hospitals can also pool staffers for health insurance plans, , and receive better rates on contracts for services ranging from prescription drug programs to mobile imaging.
Retta Jacobi recently took advantage of the latter service when a semitruck with an MRI machine inside its trailer parked outside the Bowman hospital in southwestern North Dakota, a sparsely populated region dotted with ranchland and Badlands rock formations. She hoped the scan would pinpoint what was causing pain in her shoulders.┬а
The mobile MRI operation visits one or two hospitals in the Rough Rider Network each day. Without it, Bowman residents would have to drive 40 minutes for similar scans.
Researchers haven’t yet examined whether the networks are working, according to a 2020 paper from the Rand Corp., a research nonprofit.
But leaders from network members say their programs are saving money and improving patient outcomes by, for example, increasing rates of preventive care and decreasing hospital admissions.
Jacobi, who provides speech therapy to children in the local school district, is doing physical therapy after a doctor examined her MRI results. She’s thankful she could get a diagnosis and treatment advice without having to travel far for the scan.
“Anytime we can maintain more local control, it’s a good thing for our small towns,” Jacobi said.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/the-week-in-brief-rural-hospitals-collaborative-networks/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2086662&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The mobile MRI unit visits Southwest Healthcare Services, the hospital in Bowman, North Dakota, each Wednesday. Without it, the community’s 1,400 residents would have to drive 40 minutes to get to an MRI machine, an expensive piece of medical equipment the hospital couldn’t afford on its own.
Southwest Healthcare Services and 21 other independent, rural North Dakota hospitals are part of the Rough Rider Network, which used its members’ combined patient rolls to negotiate better prices for the mobile imaging truck.
Independent rural hospitals are increasingly joining what are called clinically integrated networks, collaborative groups that allow them to avoid selling out to larger health systems while sharing resources to save money and improve patient care. Many are motivated by the chance to combine their patient rolls for , a growing reimbursement model in which insurers pay providers based on the quality of care they provide and the health outcomes of their patients.

Supporters of the networks are exploring whether funding from the $50 billion Rural Health Transformation Program тАФ part of President Donald Trump’s recent tax and spending bill тАФ can be used to help start or expand such organizations.
For independent, rural hospitals, the networks are an alternative to shutting down or reducing services, or to giving up local autonomy and joining a large hospital system.
“Anything that can help our rural hospitals and add services is awesome,” said Jacobi, who provides speech therapy to children in the local school district.
Since 2010, 153 rural hospitals in the U.S. have shuttered completely or stopped offering inpatient services, the Sheps Center for Health Services Research at the University of North Carolina. A far larger number, 441, merged with or were acquired by hospital systems between 2011 and 2021. That’s commissioned by the Coalition to Strengthen America’s Healthcare, an advocacy group comprising hospitals and health associations.
The Rough Rider Network provides negotiating leverage to its members, which serve about two-thirds of rural North Dakotans, said Dennis Goebel, CEO of the Bowman hospital.
Health care vendors “probably wouldn’t be talking to us if we’re by ourselves,” he said. “They’re not looking for the little, tiny crumbs. They want a big contract, and they’ll give you better pricing.”
Some rural networks share specialists who aren’t needed full time at any one hospital, according to , a nonprofit focused on improving the health care system. Some networks also invest in broadband, housing, and other community development projects that can help people stay healthy and access care.
Hospitals can pool staffers for a network-wide employee health insurance plan, said Nathan White, CEO of Cibolo Health, a company that helps launch and manage networks in rural areas. He said they can also enter shared contracts for telehealth, prescription drug programs, and other services.
White said he started Cibolo Health after a leader from an independent, rural North Dakota hospital asked him about collaborating with similar facilities. The Rough Rider Network launched in late 2023 with assistance from the company and $3.5 million from the North Dakota Legislature.
Since then, Cibolo Health has helped start networks in Minnesota, Nebraska, Montana, and Ohio. Once a sixth one opens in September, Cibolo-affiliated networks will represent more than 120 hospitals, with service areas covering 4.7 million people, White said.
The networks, which are nonprofits owned by the hospitals, pay an annual fee to Cibolo Health, a for-profit company, for management services. White said leaders from 10 other states are considering joining this model.
Similar networks have been around for more than 30 years but became more popular after the passage of the 2010 Affordable Care Act, by the Rand Corp., a research nonprofit.

Rural health care providers are increasingly interested in forming such networks, said Marnell Bradfield, executive director of the Community Care Alliance, a network of hospitals and independent primary care offices that launched in 2015 in rural western Colorado. About once a month, she said, she gets a call from health care leaders exploring similar networks and asking about her experience.
The Rand Corp. wrote in its 2020 paper that it didn’t find any academic studies that examined whether these networks do what its supporters claim тАФ save money and improve patient care.
“In theory, quality should improve with the alignment of health care organizations, but there is no evidence,” the report said. The paper also said such networks could end up increasing prices, something that can occur with traditional mergers and acquisitions.
Bradfield and White said they have the evidence, at least for their organizations.
Community Care Alliance members have reduced their insurance costs while improving patient outcomes, such as reducing their need for inpatient and emergency care, Bradfield said.
White said data from a pilot program between Caret Health, a care coordination company, and SMP Health-St. Kateri, one of Rough Rider’s hospitals, showed the program helped a significant number of patients catch up with preventive care.
Gabby Wilkie, finance director at the St. Kateri hospital, in Rolla near the Canadian border, said Caret Health staff called and texted patients who were behind on annual physicals, cancer screenings, vaccinations, and other visits. She said staffers explained to patients why this preventive care is important for their health before setting up a three-way call with St. Kateri staff to schedule an appointment. White said it took an average of 11 outreach attempts before patients came in for any visits.
“To be honest, we didn’t have the resources to reach out,” Wilkie said.
She said St. Kateri would have spent an estimated $300,000 to do that kind of outreach for 1,000 patients. Meanwhile, she said, the hospital estimates it will earn more than $100,000 when that many patients come in for their preventive care. Cibolo Health and the Rough Rider Network both contribute to the cost of the Caret Health service, which is now rolling out to other network hospitals.
Goebel said joining a network to remain independent is also beneficial for the economy of rural areas, where hospitals are often major employers. He said health systems sometimes cut services and staff at rural hospitals they acquire.
Jacobi is taking medication and doing physical therapy after a doctor examined her MRI results. If that doesn’t work, she may need to make a five-hour round trip to Bismarck to get an ultrasound-guided steroid shot. Jacobi was thankful she could get a diagnosis and treatment advice without having to travel far for the MRI.
“Anytime we can maintain more local control, it’s a good thing for our small towns,” she said.

This <a target="_blank" href="/rural-health/rural-hospitals-north-dakota-cins-rough-rider-network-closures/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2080068&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>