The federal government doesn’t track how many children have entered foster care because of immigration enforcement actions, leaving it unclear how often it happens. In Oregon, as of February two children had been placed in foster care after being separated from their parents in immigration detention cases, according to Jake Sunderland, a spokesperson for the Oregon Department of Human Services.
“Before fall 2025, this simply had never happened before,” Sunderland said.
As of mid-February, nearly by Immigration and Customs Enforcement. The record 73,000 people in detention in January represented an compared with one year before. According to , parents of 11,000 children who are U.S. citizens were detained from the beginning of Trump’s term through August.
The news outlet NOTUS that at least 32 children of detained or deported parents had been placed in foster care in seven states.
Sandy Santana, executive director of Children’s Rights, a legal advocacy organization, said he thinks the actual number is much higher.
“That, to us, seems really, really low,” he said.
Separation from a parent is deeply traumatic for children and can lead to , including post-traumatic stress disorder. Prolonged, intense stress can lead to more-frequent infections in children and developmental issues. That “toxic stress” is also associated with responsible for learning and memory, according to KFF.
, and amended existing laws during Trump’s first term to allow guardians to be granted temporary parental rights for immigration enforcement reasons. Now the enforcement surge that began after Trump returned to office last year has prompted a new wave of state responses.
In New Jersey, lawmakers are considering to amend a state law that allows parents to nominate standby, or temporary, guardians in the cases of death, incapacity, or debilitation. The bill would add separation due to federal immigration enforcement as another allowable reason.
Nevada and California passed laws last year to protect families separated by immigration enforcement actions. California’s law, called the , allows parents to nominate guardians and share custodial rights, instead of having them suspended, while they’re detained. They regain their full parental rights if they are released and are able to reunite with their children.
There are significant legal barriers to reunification once a child is placed in state custody, said Juan Guzman, director of children’s court and guardianship at the Alliance for Children’s Rights, a legal advocacy organization in Los Angeles.
If a parent’s child is placed in foster care and the parent cannot participate in required court proceedings because they are in detention or have been deported, it’s less likely they will be able to reunite with their child, Guzman said.
are U.S. citizens who live with a parent or family member who does not have legal immigration status, according to research from the Brookings Institution, a Washington, D.C.-based think tank. Within that group, 2.6 million children have two parents lacking legal status.
Santana said he expects the number of family separation cases to grow as the Trump administration continues its immigration enforcement campaign, putting more children at risk of being placed in foster care.
the agency to make efforts to facilitate detained parents’ participation in family court, child welfare, or guardianship proceedings, but Santana said it’s uncertain whether ICE is complying with those rules.
ICE officials did not respond to requests for comment for this report.
Before the change in California’s law, the only way a parent could share custodial rights with another guardian was if the parent was terminally ill, Guzman said.
If parents create a preparedness plan and identify an individual to assume guardianship of their children, the state child welfare agency can begin the process of placing the children with that individual without opening a formal foster care case, he added.
While Nevada lawmakers expanded an existing guardianship law last year to include immigration enforcement, the measure requires the parents to take the additional step of filing notarized paperwork with the secretary of state’s office, said Cristian Gonzalez-Perez, an attorney at Make the Road Nevada, a nonprofit that provides resources to immigrant communities.
Gonzalez-Perez said some immigrants are still hesitant to fill out government forms, out of fear that ICE might access their information and target them. He reassures community members that the state forms are secure and can be accessed only by hospitals and courts.
The Trump administration has taken through the Centers for Medicare & Medicaid Services, the IRS, the Supplemental Nutrition Assistance Program, the Department of Housing and Urban Development, and other entities.
Gonzalez-Perez and Guzman said that not enough immigrant parents know their rights. Nominating a temporary guardian and creating a plan for their families is one way they can prevent feelings of helplessness, Gonzalez-Perez said.
“Folks don’t want to talk about it, right?” Guzman said. “The parent having to speak to a child about the possibility of separation, it’s scary. It’s not something anybody wants to do.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/courts/immigrants-ice-arrests-family-separation-children-foster-care/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2178906&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Raven’s case reveals a little-known gap in the U.S. donation system: There is no clear, nationally binding way to opt out ‚Äî or to ensure a later “no” overrides an earlier “yes” in a different state.
This gap, along with a range of other issues related to the organ procurement system, has become a point of bipartisan congressional concern. Late last year, the House Ways and Means subcommittee on oversight examining what members described as shortcomings, including alleged consent failures.
The panel’s scrutiny of organ procurement organizations, or OPOs, and their consent practices is a first step toward a more meaningful accountability plan that could help maintain trust across the system, according to some committee staff members.
The trust in our organ procurement and transplant system “has been eroded,” said Rep. Terri Sewell of Alabama, the panel’s senior Democrat, calling for stronger transparency and oversight to rebuild public confidence.
“Respect for autonomy ‚Äî our ability to make our own decisions (self-determination) ‚Äî allows for both ‚Äòyes’ and ‚Äòno’ decisions and for changing one’s mind,” Margaret McLean, a bioethicist at Santa Clara University, said in an email.
“Medical decision-making is not well served in a context of ambiguity,” she said.
And if a donor revokes consent, she added, “revocation by that person should carry the same ethical and procedural weight as the initial authorization, perhaps more.”
Raven Kinser Changed Her Mind
Raven was 25 when she died. Her parents, Jeff and Jaime Kinser, were at home in Michigan when they received the phone call that shattered their world. They drove through the night to the Newport News hospital, where they learned Raven’s disposition had been referred to LifeNet Health, the region’s federally designated OPO. LifeNet a failing OPO by the Centers for Medicare & Medicaid Services, meaning it doesn’t meet the government’s standards for how well it finds donors and recovers usable organs for transplant compared with other organizations.
Under federal law, hospitals are required to refer deaths and imminent deaths to OPOs, which take responsibility for donation-related decisions and discussions.
OPOs occupy a hybrid position in the health care system, as private nonprofit entities that hold exclusive, federally authorized contracts to recover organs within defined regions. They are regulated by CMS and overseen by the Health Resources and Services Administration, but that oversight occurs primarily through certification standards, performance metrics, and periodic audits rather than routine public disclosure requirements. With donor registries largely managed at the state level and no unified federal reporting requirement for removals, comprehensive national data on revocations is elusive.
OPOs are meant to separate bedside care from organ procurement decisions ‚Äî to help prevent conflicts of interest and preserve the trust that decisions about life-sustaining treatment are made solely in the dying patient’s interest. But the , leaving families unsure who is in control if and when conflicts arise.
The Kinsers, for instance, felt their daughter would not have wanted to go through the donation process, but, at the time, had no evidence. Jaime remembers telling her husband that Raven would have been mad at them for letting it happen. In an effort to stop it, Jaime inquired about whether she would be asked to sign a consent form. But a LifeNet staff member told her that wasn’t an option because donation was Raven’s “living will,” Jaime said. Meanwhile, Raven’s parents said, her personal effects, including her Virginia driver’s license, which bore no donor designation, had not yet been turned over to the family, leaving them no meaningful way to challenge LifeNet’s determination in real time.
Jaime struggled with this outcome, even mentioning in Raven’s obituary that she was an organ donor. “How would you try to make peace with something that you felt was so wrong but had no proof?” Jaime said.
Two months passed before the Kinsers gained possession of the license, which, as they had expected, showed that Raven had not opted to be an organ donor.
According to the Kinsers, LifeNet staff told them that Raven’s status as a registered donor was established by her designation on her older Michigan license.
An emailed statement attributed to Douglas Wilson, LifeNet executive vice president, said the OPO follows federal law on organ donation, the , and queries applicable state donor registries, relying on time stamps and governing law to determine the , legally valid expression of intent. Under that framework, a prior donor authorization remains enforceable unless a valid revocation is recorded in the regional OPO’s donor registry.
Because of privacy laws, Wilson said, LifeNet could not comment on the specifics of any individual case.
Raven Kinser’s choice not to be a donor when she applied for a Virginia license in July 2024 was not reflected in the registry LifeNet consulted, according to her parents, who said that is what the organization told them. According to Lara Malbon, executive director of Donate Life Virginia, which manages the state’s organ donor registry, if someone changes their donor status while completing a Virginia driver’s license or ID transaction, “that information is sent to our registry, and the registry is updated daily to reflect those changes.” Malbon also said Virginia’s registry includes only people who have “affirmatively said ‚Äòyes’ to becoming an organ, eye, and tissue donor, and it retains records solely for those who have made that decision.”
The Kinsers said they were never told why Raven’s Virginia DMV record was insufficient, or how an older yes from Michigan could outweigh a newer no in Virginia.
In December, the Kinsers filed a complaint with the Health Resources and Services Administration, urging federal regulators to investigate LifeNet’s actions and require OPOs to provide families with documented proof of the donor’s current status at the time of referral. They also called for OPOs, which operate as federally designated regional monopolies but are structured as private nonprofits, to be made subject to public records laws.
When Opting Out Doesn’t Stick
Such confusion is not unique to the Kinser family. It is a consequence of the organ donation consent process in the United States.
“I have also wondered that: why there’s not just one” registry for organ donation, Jaime said. If you go to get a firearm, you have one federal registry, she said.
Here’s how the system works: Americans typically register their organ donation intentions when they apply for driver’s licenses through state DMVs, and that decision remains governed largely by state law. That has led to 50 different sets of rules and very little federal regulation of what has become an in the U.S.
In some states, a donor checkbox is a binding legal document. In other states, the same choice may have different rules about when it takes effect, what it covers, and how it can be revoked.
Those differences can be big. State rules determine whether a person’s “gift” is limited to transplantation or also includes research and education. They determine whether the donation authorization includes tissue. And they can determine what counts as a valid revocation and when it is legally recognized.
Because of the system’s fragmentation, though, signals can cross when someone changes their mind, like Raven; it’s not always reflected from one state system to another.
Under state versions of the Uniform Anatomical Gift Act, a donor’s most recent legally valid expression of intent is meant to control.
“Personal autonomy is paramount to everything,” said Adam Schiavi, a neurointensivist who studies end-of-life decision-making. “If I say I want to be a donor, or if I say I don’t want to be a donor, that has to take precedence over everything else.”
But states differ in how revocation must be recorded and which registry is considered authoritative if someone has lived in more than one state. Those inconsistencies can create uncertainty when records conflict across jurisdictions.
“It has to be the most recent expression, not the most recent yes,” Schiavi said.
In Michigan, a change to someone’s donor status is reflected immediately in the secretary of state’s system, but only affirmative “yes” registrations appear in the registry. Removal information remains in internal motor vehicle records. In Virginia, the state registry includes only those who have affirmatively said “yes,” retaining records solely of donors, creating potential gaps if someone believes a DMV change alone is sufficient.
Elsewhere, processes and volumes differ sharply. New Mexico updates driver records in real time but does not transmit status changes to its donor registry. Instead, donor services receive restricted search access. The state logged nearly 15,000 removals in late 2021 and almost 30,000 in 2022. Florida, which maintains formal removal records through weekly DMV data files, reported 356,161 removals in 2020, more than 1.5 million in 2023, and over 1.2 million in 2025. Kentucky processed 847,371 donor registrations from 2020 to 2025, but only 16,043 icon removals, with registry withdrawal handled separately. In 2025, more than 570,000 Texans opted into the registry, while over 31,000 individuals requested removal.
According to a federal official who asked not to be identified for fear of professional repercussions, OPOs have been highly effective at lobbying states to broaden the definition of consent and authorization — shaping how those terms are applied, whether those statuses must be renewed, and how easy or difficult it is for someone to opt out.
In subsequent correspondence with federal officials, the Kinsers have urged reforms to prevent OPOs from relying on older registry entries when a more recent state DMV record exists, and they have called for criminal penalties in cases in which consent is knowingly misrepresented. Federal regulators have not indicated whether such proposals are under consideration.
Congress Takes a Closer Look
Ethicists have long cautioned that consent must be more than a checkbox and must remain grounded in respect for the donor-patient. In an October on organ transplantation, the American College of Physicians emphasized that clinicians’ primary duty is to the patient in their care, and that maintaining trust requires transparency and safeguards to prevent conflicts of interest from blurring that “bright line.”
Advocates say those steps leave unresolved the core problem raised by the Kinser family: the lack of a clear, legally binding way for people to say “no” and for that decision to follow them across state lines.
The said it “supports strengthening donor registries and enhancing registry interoperability to ensure that an individual’s documented donation decision is honored.” But OPOs have also argued that current policies protect donation as a legally enforceable gift and prevent families from overriding a loved one’s “yes” in the midst of grief. They argue that stronger, more durable consent helps reduce missed donations and saves lives.
Congress and federal regulators are considering changes to the nation’s organ donation system, including how consent is recorded and what should happen when a donor changes their mind.
Sen. Ron Wyden (D-Ore.) last year to create new federal standards for patient safety, transparency, and oversight of organ transplants, including a formal authorization for hospital or OPO staff to pause harvesting if there is any “clinical sign of life.”
HHS press secretary Emily Hilliard said the agency is “committed to holding organ procurement organizations accountable” and to “restoring integrity and transparency” to organ donation policy, calling reforms essential to informed consent and protecting donor rights. CMS issued related March 11, but it does not address the problems highlighted by the Kinsers’ case.
Critics of the organ transplant system say it is difficult for families to obtain documentation or independently verify how consent determinations were made in disputed cases.
HRSA has launched a sweeping modernization of the Organ Procurement and Transplantation Network, the national system that oversees organ allocation and transplant policy. Federal officials have described the overhaul as the most significant restructuring of the transplant system in decades, aimed at breaking up a long-standing contractor monopoly, strengthening patient safety oversight, and replacing aging technology infrastructure.
Central to that effort is modernizing the OPTN’s data systems: improving interoperability, audit trails, and transparency in how decisions are documented and reviewed. A more modern federal data architecture could make it easier to trace which registry was queried, what time stamp controlled, and how a consent determination was reached in disputed donations that span multiple states. But the modernization effort would not change the underlying state-by-state legal framework for donor authorization and what counts as a valid “no.”
Meanwhile, Donate Life America, a national nonprofit that supports state donor registries, also runs the , a central database that allows people to sign up as organ donors directly. Unlike many DMV systems, the national registry lets people log in at any time to view, update, or remove their registration and print proof of their decision. The group is also starting a project to let participating states send registrations directly into the national system, creating one place to track donor sign-ups and removals across state lines.
Each of the proposals comes with trade-offs, and both advocates and OPOs have raised concerns about how they would work in practice.
“Just doing a dump truck dump of information is not going to do much unless you really apply it through checking and auditing,” said Arthur Caplan, a professor of bioethics at New York University’s Grossman School of Medicine. “It could be like the IRS. They don’t have to audit everybody. Just do a spot audit once in a while.”
The Kinsers aren’t opposed to organ donation itself. They celebrated Raven’s donation in her obituary, and in their complaint to federal regulators, they wrote, “We are NOT anti-organ donation, and we will never take away the gift of life our oldest daughter gave to others. However, that was not LifeNet’s choice to make.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/organ-donor-state-registries-consent-authorization-optn-opo-raven-kinser-virginia/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2167503&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>After Health and Human Services Secretary Robert F. Kennedy Jr. fired Centers for Disease Control and Prevention Director Susan Monarez for refusing what her lawyers called “,” Newsom to help modernize California’s public health system. He also gave a job to Debra Houry, the agency’s former chief science and medical officer, who had resigned in protest hours after Monarez’s firing.
Newsom also teamed up with fellow Democratic governors Tina Kotek of Oregon, Bob Ferguson of Washington, and Josh Green of Hawaii to form the , a regional public health agency, whose guidance would “uphold scientific integrity in public health as Trump destroys” the CDC’s credibility. Newsom argued establishing the independent alliance was vital as Kennedy leads the Trump administration’s rollback of national vaccine recommendations.
More recently, California became the a global outbreak response network coordinated by the World Health Organization, followed by Illinois and New York. Colorado and Wisconsin signaled they plan to join. They did so after President Donald Trump officially from the agency on the grounds that it had “strayed from its core mission and has acted contrary to the U.S. interests in protecting the U.S. public on multiple occasions.” Newsom said joining the WHO-led consortium would enable California to respond faster to communicable disease outbreaks and other public health threats.
Although other Democratic governors and public health leaders have openly criticized the federal government, few have been as outspoken as Newsom, who is considering a run for president in 2028 and is in his second and final term as governor. Members of the scientific community have praised his effort to build a public health bulwark against the Trump administration’s slashing of funding and scaling back of vaccine recommendations.
What Newsom is doing “is a great idea,” said Paul Offit, an outspoken critic of Kennedy and a vaccine expert who formerly served on the Food and Drug Administration’s vaccine advisory committee but was removed under Trump in 2025.
“Public health has been turned on its head,” Offit said. “We have an anti-vaccine activist and science denialist as the head of U.S. Health and Human Services. It’s dangerous.”
The White House did not respond to questions about Newsom’s stance and HHS declined requests to interview Kennedy. Instead, federal health officials criticized Democrats broadly, arguing that blue states are participating in fraud and mismanagement of federal funds in public health programs.
HHS spokesperson Emily Hilliard said the administration is going after “Democrat-run states that pushed unscientific lockdowns, toddler mask mandates, and draconian vaccine passports during the covid era.” She said those moves have “completely eroded the American people’s trust in public health agencies.”
Public Health Guided by Science
Since Trump returned to office, Newsom has criticized the president and his administration for engineering policies that he sees as an affront to public health and safety, labeling federal leaders as “extremists” trying to “weaponize the CDC and spread misinformation.” He has for erroneously linking vaccines to autism, the administration is endangering the lives of infants and young children in scaling back childhood vaccine recommendations. And he argued that the White House is unleashing “chaos” on America’s public health system in backing out of the WHO.
The governor declined an interview request. Newsom spokesperson Marissa Saldivar said it’s a priority of the governor “to protect public health and provide communities with guidance rooted in science and evidence, not politics and conspiracies.”
The Trump administration’s moves have triggered financial uncertainty that local officials said has reduced morale within public health departments and left states unprepared for disease outbreaks and . The White House last year proposed cutting HHS spending , including . Congress largely rejected those cuts last month, although funding for programs focusing on social drivers of health, such as access to food, housing, and education, .
The Trump administration announced that it would claw back in public health funds from California, Colorado, Illinois, and Minnesota, arguing that the Democratic-led states were funding “woke” initiatives that didn’t reflect White House priorities. Within days, and a judge the cut.
“They keep suddenly canceling grants and then it gets overturned in court,” said Kat DeBurgh, executive director of the Health Officers Association of California. “A lot of the damage is already done because counties already stopped doing the work.”
Federal funding has accounted for of state and local health department budgets nationwide, with money going toward fighting HIV and other sexually transmitted infections, preventing chronic diseases, and boosting public health preparedness and communicable disease response, according to a 2025 analysis by KFF, a health information nonprofit that includes ∫⁄¡œ≥‘πœÕ¯ News.
Federal funds account for $2.4 billion of California’s $5.3 billion public health budget, making it difficult for Newsom and state lawmakers to backfill potential cuts. That money helps fund state operations and is vital for local health departments.
Funding Cuts Hurt All
Los Angeles County public health director Barbara Ferrer said if the federal government is allowed to cut that $600 million, the county of nearly 10 million residents would lose an estimated $84 million over the next two years, in addition to other grants for prevention of HIV and other sexually transmitted infections. Ferrer said the county depends on nearly $1 billion in federal funding annually to track and prevent communicable diseases and combat chronic health conditions, including diabetes and high blood pressure. Already, the the closure of that provided vaccinations and disease testing, largely because of funding losses tied to federal grant cuts.
“It’s an ill-informed strategy,” Ferrer said. “Public health doesn’t care whether your political affiliation is Republican or Democrat. It doesn’t care about your immigration status or sexual orientation. Public health has to be available for everyone.”
A single case of measles requires public health workers to track down 200 potential contacts, Ferrer said.
The U.S. but is close to losing that status as a result of vaccine skepticism and misinformation spread by vaccine critics. The U.S. had , the most since 1991, with 93% in people who were unvaccinated or whose vaccination status was unknown. This year, the highly contagious disease has been reported at , , and .
Public health officials hope the West Coast Health Alliance can help counteract Trump by building trust through evidence-based public health guidance.
“What we’re seeing from the federal government is partisan politics at its worst and retaliation for policy differences, and it puts at extraordinary risk the health and well-being of the American people,” said Georges Benjamin, executive director of the American Public Health Association, a coalition of public health professionals.
Robust Vaccine Schedule
Erica Pan, California’s top public health officer and director of the state Department of Public Health, said the West Coast Health Alliance is defending science by recommending a vaccine schedule than the federal government. California is part of a coalition over its decision to rescind recommendations for seven childhood vaccines, including for hepatitis A, hepatitis B, influenza, and covid-19.
Pan expressed deep concern about the state of public health, particularly the uptick in measles. “We’re sliding backwards,” Pan said of immunizations.
Sarah Kemble, Hawaii’s state epidemiologist, said Hawaii joined the alliance after hearing from pro-vaccine residents who wanted assurance that they would have access to vaccines.
“We were getting a lot of questions and anxiety from people who did understand science-based recommendations but were wondering, ‚ÄòAm I still going to be able to go get my shot?’” Kemble said.
Other states led mostly by Democrats have also formed alliances, with Pennsylvania, New York, New Jersey, Massachusetts, and several other East Coast states banding together to create the .
HHS’ Hilliard said that even as Democratic governors establish vaccine advisory coalitions, the federal “remains the scientific body guiding immunization recommendations in this country, and HHS will ensure policy is based on rigorous evidence and gold standard science, not the failed politics of the pandemic.”
Influencing Red States
Newsom, for his part, has approved a recurring annual infusion of nearly $300 million to support the state Department of Public Health, as well as the 61 local public health agencies across California, and last year authorizing the state to issue its own immunization guidance. It requires health insurers in California to provide patient coverage for vaccinations the state recommends even if the federal government doesn’t.
Jeffrey Singer, a doctor and senior fellow at the libertarian Cato Institute, said decentralization can be beneficial. That’s because local media campaigns that reflect different political ideologies and community priorities may have a better chance of influencing the public.
A KFF analysis found some red states are joining blue states in decoupling their vaccine recommendations from the federal government’s. Singer said some doctors in his home state of Arizona are looking to more liberal California for vaccine recommendations.
“Science is never settled, and there are a lot of areas of this country where there are differences of opinion,” Singer said. “This can help us challenge our assumptions and learn.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/gavin-newsom-california-public-health-fight-west-coast-alliance-trump-hhs-rfk/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2164665&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The city’s mobile crisis team had just gotten a call about a man walking around outside without shoes. The man’s family told the team he was having a mental health crisis and wouldn’t come inside.
As they drove down the highway toward the city’s outskirts, team member Evan Thiessen spoke with the relative who had reached out.
“You’re doing the right thing, and we’re going to make sure he gets help today, OK?” he said.
They pulled up the man’s police record on a laptop and saw that he did have a record of some previous encounters with police, including some that had turned violent.
, a licensed therapist, had that in mind as they pulled into a neighborhood of single-family homes. He stepped out of the Ford Bronco and headed toward the front door.
A Funding Problem
Many communities around the country send out teams like this one to help people in psychiatric crisis, rather than dispatching regular police.
A found there were at least 1,800 mobile teams nationwide in 2023. But financial support for them is often inadequate and inconsistent, leaving many communities struggling to keep the teams operating.
Two programs — one in Great Falls, in central Montana, and one in Billings, in south-central Montana — recently shut down. Six units remain in Montana.
The strategy in Eugene, Oregon, but gained momentum nationally over the past 10 years.
Recent about police killing people who are experiencing a psychiatric crisis have sparked conversations about how to safely and effectively respond. Most police officers are not trained to deal with people experiencing delusions or hallucinations, nor to de-escalate situations involving threatening behaviors to themselves or others.
An across 27 states found that about a third of the victims showed signs of being in crisis. Another study found that people with a serious mental illness were at least to experience use of force by police as those without.
By contrast, crisis response teams have been trained to de-escalate such situations and provide appropriate therapeutic care.
When the team arrived at the house in Bozeman, the man had already gone back inside. The team then talked with the man’s family for about half an hour and helped them devise a plan to keep him at home ‚Äî and safe. Before they left, team members determined the man wasn’t a threat to himself or others.
Also, they planned to follow up within a few days to connect him with ongoing mental health care. After an encounter with the team, some clients might need follow-up therapy, assistance with psychiatric medications, or help finding treatment for substance abuse.
The Bozeman team is available 12 hours a day, seven days a week, and costs roughly $1 million a year to run.
Police departments are generally funded by local taxpayers. Mobile crisis teams don’t have a single, reliable source of funding.
Some, despite successful operations and , are or have closed entirely. One that shuttered was Oregon’s .
Most crisis calls end with people staying where they are, avoiding a trip to the emergency room or going to jail, according to , which runs the mobile crisis program in Bozeman.
Beyond police and firefighters, members of the public can call the team directly.
“I’ve been out on calls where individuals have barricaded themselves in residences or in their vehicles with a firearm. So, helping to assist not only law enforcement, the negotiators, but consulting on the behavioral health side of that,” said Ryan Mattson, who leads the Bozeman crisis team.

The program has reduced the time that Bozeman police officers must spend on mental health calls by nearly 80%, according to Mattson, and prevented unnecessary ER visits.
Residents and political leaders see that value, he said, but finding a way to pay for the service has been difficult.
“I’m confident we’ll be here through next fiscal year. That’s about as confident as I am at this point,” Mattson said.
Mobile crisis programs in Montana, which began operating about five years ago, have cost more than the state originally projected.
Health insurance is sometimes a revenue source for mobile crisis teams. That’s because a crisis call is a type of mental health service, provided by trained professionals such as therapists or crisis intervention specialists. Still, many private insurance companies don’t reimburse for mobile crisis services.
What Medicaid Pays For ‚Äî And Doesn’t
Medicaid, the government-funded insurance program for low-income and disabled Americans, is another funding source. Two-thirds of states allow Medicaid reimbursement for such calls, but rates vary.
In Montana, Medicaid reimburses the team only for the time they spend responding to a call in the field. Additional time spent on a case ‚Äî documenting the encounters, or waiting for the next call ‚Äî isn’t reimbursed.
“You need to pay for the capacity to be at the ready, just like we do with fire or police, regardless of whether somebody is going to be called out,” said of Inseparable, a nonprofit that advocates for mental health policy reform.
It’s not feasible for mobile crisis teams to rely solely on reimbursement from insurance companies, she said.
To deal with the shortfalls, many mobile teams rely on a patchwork of grants and other funding, according to , who studies Medicaid policy at KFF, a health information nonprofit that includes ∫⁄¡œ≥‘πœÕ¯ News.
Some state governments have stepped in to help.
Eight states, including New Jersey, California, and Washington, mandate that private insurers cover the cost of mobile crisis calls for people on their plans, according to Kimball. At least 10 states have implemented fees on cellphone bills to help pay for service.
Montana hasn’t followed suit.
The state provides about $2 million annually in supplemental funds to help the mobile teams pay for service calls that aren’t reimbursed through Medicaid, according to an emailed statement from Jon Ebelt, a state health department spokesperson.
But program managers counter that the paperwork to access that funding is complicated and often isn’t worth the staff time.
Will Montana Step In?
Despite this state support, mobile teams are still struggling to stay afloat, Ebelt acknowledged. He said Montana officials are considering boosting what Medicaid reimburses for each service call.
In Missoula, the mobile crisis team turned to local taxpayers for additional help. Their annual expenditure is $1.4 million, but Medicaid reimbursements were covering only about 20% of the cost, according to program manager John LaRocque. Even with local tax dollars, the program faces a $250,000 shortfall, so LaRocque is looking for grants.

Mobile crisis is still a relatively new concept, and growing pains are to be expected, said Sierra Riesberg, director of the .
Still, abrupt closures create instability and lead some patients to the ER, placing financial pressure on another distressed part of the local health system.
“A much-needed service is available and then not available, available and then not available. These things need to be taken into consideration when developing programs in communities,” she said.
If more mobile crisis teams shut down, that might interfere with Montana’s recent efforts to overhaul an outdated and underfunded mental health system. The state’s only psychiatric hospital hasn’t kept up with the to the facility.
Later this year, Montana hopes to join a federal pilot program to open a new type of clinic: , or CCBHCs. Those clinics will receive boosted levels of federal funding, but they are required to offer round-the-clock mobile crisis services as well as other crisis care.
That could be a tall order for rural communities, said , an executive at in Great Falls.
Alluvion used to operate the mobile crisis team in Great Falls before it shuttered the service. One major reason it closed was that the expected Medicaid payments covered less than anticipated. Before Alluvion would consider getting involved again, the state would need to “completely revamp” the way the service is funded, Schreiner said.
“Is it a priority for our state or not?” he asked.
This article is from a partnership with and .
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/police-mental-health-calls-988-911-mobile-crisis-teams-funding/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2159605&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The Millers resettled on Vancouver Island, their scenic refuge accessible only by ferry or plane. Justin went to work in the emergency room at Nanaimo Regional General Hospital, where he became one of at least 20 U.S.-trained nurses hired since April.
Fear of Trump, some of the nurses said, was why they left.
“There are so many like-minded people out there,” said Justin, who now works elbow to elbow with Americans in Canada. “You aren’t trapped. You don’t have to stay. Health care workers are welcomed with open arms around the world.”
The Millers are part of a new surge of American nurses, doctors, and other health care workers moving to Canada, and specifically British Columbia, where more than 1,000 U.S.-trained nurses have been approved to work since April. As the Trump administration enacts increasingly authoritarian policies and decimates funding for , insurance, and medical research, many nurses have felt the draw of Canada’s progressive politics, friendly reputation, and universal health care system.
Additionally, some nurses were incensed last year when the Trump administration said it would reclassify nursing as a , which would impose strict federal limits on the loans nursing students could receive.
Canada is poised to capitalize. Two of its most populous provinces, Ontario and British Columbia, have streamlined the licensing process for American nurses since Trump returned to the White House. British Columbia also launched a last year to recruit nurses from California, Oregon, and Washington state.
“With the chaos and uncertainty happening in the U.S., we are seizing the opportunity to attract the talent we need,” Josie Osborne, the province’s health minister, said in a statement announcing the campaign.
Fears Realized
Amy Miller, a nurse practitioner, said she and her husband were determined to move their children out of the country because they felt Trump’s second term would inevitably spiral into violence.
First, the Millers got nursing licenses in New Zealand, but when the job search took too long, they pivoted to Canada.
Justin was offered a job within weeks.
Amy found one within three months.
So they moved. And just a few days later, the Millers watched with horror from afar as their fears came true.
As federal immigration forces clashed with protesters in Minneapolis on Jan. 24, federal agents fatally shot an ICU nurse, Alex Pretti, as he filmed a confrontation and appeared to be trying to shield a woman who was knocked down. Video of the killing showed border agents pinning Pretti to the ground before seizing his concealed, licensed handgun and opening fire on him.
The Trump administration quickly called Pretti a “domestic terrorist” who intended to kill federal agents. That allegation was disputed by eyewitness videos that circulated on social media and spurred widespread outrage, including from nurses and nursing organizations, some of whom invoked the profession’s duty to care for the vulnerable.
“I don’t want to say it was expected, but that’s why we are here,” Amy Miller said. “Even our oldest kid, she was like: ‚ÄòIt’s OK, Mom, because we are not there anymore. We are safe here.’ So she recognizes that, and she’s not even in middle school yet.”
Both the U.S. and Canada have a severe need for nurses. The U.S. is projected to be short about 270,000 registered nurses, plus at least 120,000 licensed practical nurses, by 2028, according to from the Health Resources and Services Administration. In Canada, nursing job vacancies tripled from 2018 to 2023, when they reached nearly 42,000, according to from the Montreal Economic Institute, a Canadian think tank.
When asked to comment, the White House noted that shows the number of nurses licensed in the U.S. increased in 2025. It dismissed accounts of nurses moving to Canada as “anecdotes of individuals with severe cases of Trump derangement syndrome.”
“The American health care workforce is the finest in the world, and it continues to expand under President Trump,” White House spokesperson Kush Desai said. “Employment opportunities in the American health care system remain robust, with career advancement and pay that far exceed that of other developed nations.”

‚ÄòA Sense of Relief’
It is unknown precisely how many American nurses have moved north since Trump returned to office, because some Canadian provinces do not track or release such statistics.
British Columbia, which has done the most to recruit Americans, approved the licensing applications of 1,028 U.S.-trained nurses from when the province’s streamlined application process took effect in April 2025 through January, according to the British Columbia College of Nurses and Midwives. In all of 2023, only 112 applicants from the U.S. were approved, the agency said. In 2024, it was 127.
Increased interest from American nurses was also confirmed by nursing associations in Ontario and Alberta, as well as by the nationwide Canadian Nurses Association.
Angela Wignall, CEO of Nurses and Nurse Practitioners of British Columbia, said American nurses used to move north because they had fallen in love with Canada (or a Canadian). But more recently, she said, she had met nurses who feared the White House would spur violence and vigilantism, particularly against families that included same-sex couples.
“Some of them were living in fear of the administration, and they shared a sense of relief when crossing the border,” Wignall said. “As a Canadian, it’s heartbreaking. And also a joy to welcome them.”
Vancouver Island, which has a population of about 860,000, has gained 64 U.S.-trained nurses since April, including those at Nanaimo Regional, said Andrew Leyne, a spokesperson for the island’s health agency.
One of the nurses was Susan Fleishman, a Canadian who moved to the U.S. as a child, then worked for 23 years in American emergency rooms before leaving the country in November.
Fleishman said hateful rhetoric from Trump has fueled an angry division that has permeated and soured American life.
“It wasn’t an easy move ‚Äî that’s for sure. But I think it’s definitely worth it,” she said, happily back in Canada. “I find there is a lot more kindness here. And I think that will keep me here.”
Brandy Frye, who also worked for decades in American ERs, said she moved to Vancouver Island last year after waiting to see whether Mark Carney would become Canada’s prime minister. Carney’s rise was widely viewed as a rejection of Trumpism.
Meanwhile, Frye said, the California hospital where she worked had been stripping words associated with diversity and equity out of its paperwork to appease the Trump administration. She couldn’t stand it.
“It felt like a step against everything I believe in,” Frye said. “And I didn’t feel like I belonged there anymore.”

Like many of the American nurses who have moved to Vancouver Island, Frye was first wooed to the area by a that was meant to attract tourist dollars but ended up doing much more.
About a year ago, Tod Maffin, a and former CBC Radio host, invited Americans to the port city of Nanaimo for a weekend event designed to offset the impact of Trump’s tariffs on the local economy.
Maffin said about the April event.
“A lot of them were health care workers looking for an escape route,” Maffin said. “They were there to help support our economy but also to look into Canada.”
Maffin saw an opportunity. He repurposed the event website into a recruiting tool and launched a Discord chatroom to help Americans relocate.
Maffin said he believes the campaign helped about 35 health care workers move to Vancouver Island. Volunteers in have since duplicated his website in an effort to attract their own American nurses and doctors.
“There are communities across Canada where the emergency room closes at night because one nurse is out. That’s how thin staffing is,” Maffin said.
“One new nurse in a small town, or in a midsized city like Nanaimo,” he said, “makes a difference.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/us-nurses-move-to-canada-trump-policies-care-shortages/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2158443&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Warning patients could deter them from signing up for a program called Emergency Medicaid, through which the for the cost of emergency treatment for immigrants who are ineligible for standard Medicaid coverage.
But if hospitals don’t disclose that the patients’ information is shared with federal law enforcement, they might not know that their medical coverage puts them at risk of being located by Immigration and Customs Enforcement.
“If hospitals tell people that their Emergency Medicaid information will be shared with ICE, it is foreseeable that many immigrants would simply stop getting emergency medical treatment,” said , a research professor at Georgetown University’s Center for Children and Families. “Half of the Emergency Medicaid cases are for the delivery of U.S. citizen babies. Do we want these mothers avoiding the hospital when they go into labor?”
For more than a decade, hospitals and states have assured patients that their personal information, including their home addresses and immigration status, would not be shared with immigration enforcement officials when they apply for federal health care coverage. guaranteed the agency would not use information from health coverage applications for enforcement activities.
But that changed last year, after President Donald Trump returned to the White House and ordered one of the most aggressive immigration crackdowns in recent history. His administration began funneling data from a variety of government agencies to the Department of Homeland Security, including filed with the IRS.
The Centers for Medicare & Medicaid Services, part of the Department of Health and Human Services, agreed last spring to give ICE officials direct access to a Medicaid database that includes enrollees’ addresses and citizenship status.
Twenty-two states, all but one led by Democratic governors, the Medicaid data-sharing agreement, which the administration did not formally announce until a federal judge ordered it to do so last summer. The judge that in those states, ICE could access information in the Medicaid database only about people in the country unlawfully. ∫⁄¡œ≥‘πœÕ¯ News contacted more than a dozen hospitals and hospital associations in states and cities that have been targets of ICE sweeps. Many declined to comment on whether they’ve updated their disclosure policies after the ruling.
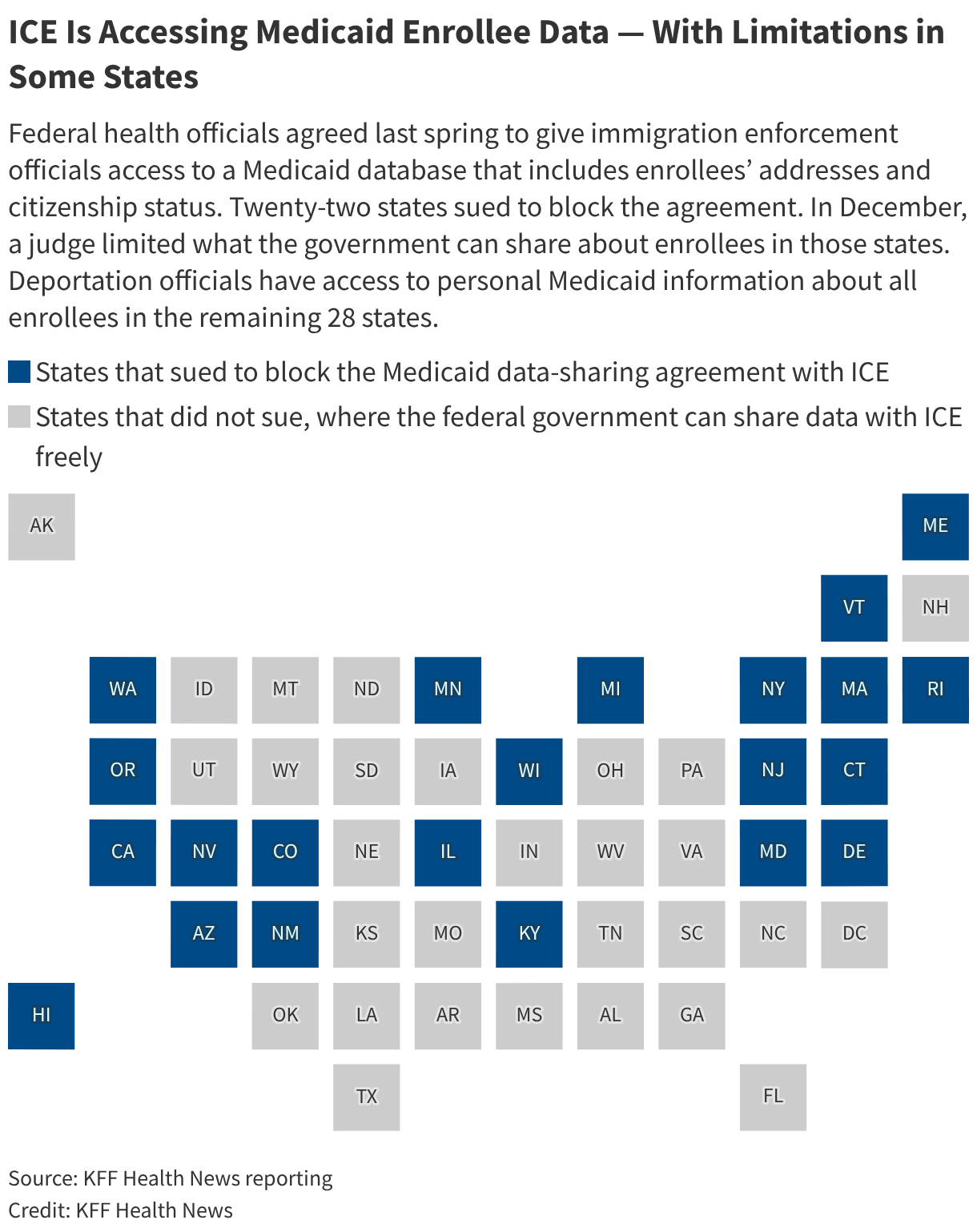
Of those that responded, none said they are directly warning patients that their personal information may be shared with ICE when they apply for Medicaid coverage.
“We do not provide legal advice about federal government data-sharing between agencies,” Aimee Jordon, a spokesperson for M Health Fairview, a Minneapolis-based hospital system, said in an email to ∫⁄¡œ≥‘πœÕ¯ News. “We encourage patients with questions about benefits or immigration-related concerns to seek guidance from appropriate state resources and qualified legal counsel.”
Information on Applications
Some states’ Emergency Medicaid applications specifically ask for a patient’s immigration status — and still assure people that their information will be kept secure and out of the hands of immigration enforcement officials.
For example, as of Feb. 3, California’s application still included language advising applicants that their immigration information is “confidential.”
“We only use it to see if you qualify for health insurance,” states the 44-page form, which the state’s Medicaid program, known as Medi-Cal, in January.
California Department of Health Care Services spokesperson Anthony Cava said in a statement that the agency, which oversees Medi-Cal, will “ensure that Californians have accurate information on the privacy of their data, including by revising additional publications as necessary.”
Until late January, Utah’s Medicaid website also claimed its Emergency Medicaid program did not share its information with immigration officials. After ∫⁄¡œ≥‘πœÕ¯ News contacted the state agency, Kolbi Young, a spokesperson, said Jan. 23 that the language would be taken down immediately. It was removed that day.
Oregon Health & Science University, a hospital system based in Portland, offers immigrant patients developed by the state Medicaid program for those with concerns about how their information might be used. The document does not directly say that Medicaid enrollees’ information is shared with ICE officials.
Hospitals rely on Emergency Medicaid to reimburse them for treating people who would qualify for Medicaid if not for their citizenship status — those in the country illegally and lawfully present immigrants, such as those with a student or work visa. The coverage pays only for emergency medical and pregnancy care. Typically, hospital representatives help patients apply while they are still in the medical facility.
The main Medicaid program, which covers a much broader range of services for over 77 million low-income and disabled people, does not cover people living in the country illegally.
Examining Emergency Medicaid enrollment is the most obvious way, then, for deportation officials to identify immigrants, including those who might not reside in the U.S. lawfully.
HHS spokesperson Rich Danker said in an email that CMS — which oversees Medicaid, a joint state-federal program — is sharing data with ICE after the judge’s ruling. But he would not answer how the agency is ensuring it is sharing information only on people who are not lawfully present, as the judge required.
With ICE now getting direct access to the personal information of millions of Medicaid enrollees, hospitals — while “definitely in a tough position” — should be up-front about the changes, said Sarah Grusin, at the National Health Law Program, an advocacy group.
“They need to be telling people that the judge has permitted sharing of information, including their address, for people who are not lawfully residing,” she said. “Once this information is submitted, you can’t protect it from disclosure at this point.”
Grusin said she advises families to weigh the importance of seeking medical care against the risk of having their information shared with ICE.
“We want to give candid, honest information even if it means the decision people have to make is really hard,” she said.
Those who have previously enrolled in Medicaid or can easily search their address online should assume that immigration officials already have their information, she added.
Emergency Medicaid
Emergency Medicaid coverage was established in the mid-1980s, when a federal law began requiring hospitals to treat and stabilize all patients who show up at their doors with a life-threatening condition.
Federal government spending on Emergency Medicaid accounted for nearly $4 billion in 2023, or of total federal spending on Medicaid.
States send monthly reports to the federal government with detailed information about who enrolls in Medicaid and what services they receive. The judge’s ruling in December limited what CMS can share with ICE to only basic information, including addresses, about Medicaid enrollees in the 22 states that sued over the data-sharing arrangement. ICE officials are not supposed to access information about the medical services people receive, per the judge’s order.
The judge also prohibited the agency from sharing the data of U.S. citizens or lawfully present immigrants from those states.
Deportation officials have access to personal Medicaid information of all enrollees in the remaining 28 states.
The federal health agency has not clarified how it is ensuring that certain states’ information on citizens and legal residents is not shared with ICE. But Medicaid experts say it would be nearly impossible for the agency to separate the data, raising questions about whether the Trump administration is complying with the judge’s order.
The Trump administration’s efforts to deport immigrants living in the country illegally have had implications on immigrant families seeking care. About a third of adult immigrants reported skipping or postponing health care in the past year, according to a released in November. (KFF is a health information nonprofit that includes ∫⁄¡œ≥‘πœÕ¯ News.)
Bethany Pray, the chief legal and policy officer at the Colorado Center on Law and Policy, warned that sharing Medicaid data directly with deportation officials will force even tougher decisions upon some families.
“This is very concerning,” Pray said. “People should not have to choose between giving birth in a hospital and wondering if that means they risk deportation.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/ice-immigrants-medicaid-data-sharing-hospitals-states-deportation/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2151281&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>A week earlier, immigration agents had grabbed Julio César Peña from his front yard in Glendale, California. Now, he was in a hospital after suffering a ministroke. He was shackled to the bed by his hand and foot, he told Romero, and agents were in the room, listening to the call. He was scared he would die and wanted his wife there.
“What hospital are you at?” Romero asked.
“I can’t tell you,” he replied.
Viridiana Chabolla, Peña’s attorney, couldn’t get an answer to that question, either. Peña’s deportation officer and the medical contractor at the Adelanto ICE Processing Center refused to tell her. Exasperated, she tried calling a nearby hospital, Providence St. Mary Medical Center.
“They said even if they had a person in ICE custody under their care, they wouldn’t be able to confirm whether he’s there or not, that only ICE can give me the information,” Chabolla said. The hospital confirmed this policy to ∫⁄¡œ≥‘πœÕ¯ News.
Family members and attorneys for patients hospitalized after being detained by federal immigration officials said they are facing extreme difficulty trying to locate patients, get information about their well-being, and provide them emotional and legal support. They say many hospitals refuse to provide information or allow contact with these patients. Instead, hospitals allow immigration officers to call the shots on how much — if any — contact is allowed, which can deprive patients of their constitutional right to seek legal advice and leave them vulnerable to abuse, attorneys said.
Hospitals say they are trying to protect the safety and privacy of patients, staff, and law enforcement officials, even while hospital employees in , , and , cities where Immigration and Customs Enforcement has conducted immigration raids, say it’s made their jobs difficult. Hospitals have used what are sometimes called blackout procedures, which can include registering a patient under a pseudonym, removing their name from the hospital directory, or prohibiting staff from even confirming that a patient is in the hospital.
“We’ve heard incidences of this blackout process being used at multiple hospitals across the state, and it’s very concerning,” said Shiu-Ming Cheer, the deputy director of immigrant and racial justice at the California Immigrant Policy Center, an advocacy group.
Some Democratic-led states, , have enacted legislation that seeks to protect patients from immigration enforcement in hospitals. However, those policies do not address protections for people already in ICE custody.
More Detainees Hospitalized
Peña is among arrested by federal immigration authorities since President Donald Trump returned to the White House. As arrests and detentions have climbed, so too have reports of people taken to hospitals by immigration agents because of illness or injury ‚Äî due to preexisting conditions or problems stemming from their arrest or detention.
ICE has for using and tactics, as well as for and at its facilities. Sen. Adam Schiff (D-Calif.) told reporters at a Jan. 20 news conference outside a detention center he visited in California City that he spoke to a diabetic woman held there who had not received treatment in .
While there are no publicly available statistics on the number of people sick or injured in ICE detention, the agency’s news releases point to who died in immigration custody in 2025. Six more have died this year.
The Department of Homeland Security, which oversees ICE, did not respond to a request for information about its policies or Peña’s case.
According to , people in custody should be given access to a telephone, visits from family and friends, and private consultation with legal counsel. The agency can make administrative decisions, including about visitation, when a patient is in the hospital, but should defer to hospital policies on contacting next of kin when a patient is seriously ill, the guidelines state.
Asked in detail about hospital practices related to patients in immigration custody and whether there are best practices that hospitals should follow, Ben Teicher, a spokesperson for the American Hospital Association, declined to comment.
David Simon, a spokesperson for the California Hospital Association, said that “there are times when hospitals will ‚Äî at the request of law enforcement ‚Äî maintain confidentiality of patients’ names and other identifying characteristics.”
Although policies vary, members of the public can typically call a hospital and ask for a patient by name to find out whether they’re there, and often be transferred to the patient’s room, said William Weber, an emergency physician in Minneapolis and medical director for the Medical Justice Alliance, which advocates for the medical needs of people in law enforcement custody. Family members and others authorized by the patient can visit. And medical staff routinely call relatives to let them know a loved one is in the hospital, or to ask for information that could help with their care.
But when a patient is in law enforcement custody, hospitals frequently agree to restrict this kind of information sharing and access, Weber said. The rationale is that these measures prevent unauthorized outsiders from threatening the patient or law enforcement personnel, given that hospitals lack the security infrastructure of a prison or detention center. High-profile patients such as celebrities sometimes also request this type of protection.
Several attorneys and health care providers questioned the need for such restrictions. Immigration detention is civil, not criminal, detention. The Trump administration says it’s focused on , yet most of those arrested have no criminal conviction, according to data compiled by the and several news outlets.

Taken Outside His Home
According to Peña’s wife, Romero, he has no criminal record. Peña came to the United States from Mexico in sixth grade and has an adult son in the U.S. military. The 43-year-old has terminal kidney disease and survived a heart attack in November. He has trouble walking and is partially blind, his wife said. He was detained Dec. 8 while resting outside after coming home from dialysis treatment.
Initially, Romero was able to find her husband through the . She visited him at a temporary holding facility in downtown Los Angeles, bringing him his medicines and a sweater. She then saw he’d been moved to the Adelanto detention center. But the locator did not show where he was after he was hospitalized.
When she and other relatives drove to the detention facility to find him, they were turned away, she said. Romero received occasional calls from her husband in the hospital but said they were less than 10 minutes long and took place under ICE surveillance. She wanted to know where he was so she could be at the hospital to hold his hand, make sure he was well cared for, and encourage him to stay strong, she said.
Shackling him and preventing him from seeing his family was unfair and unnecessary, she said.
“He’s weak,” Romero said. “It’s not like he’s going to run away.”
say contact and visits from family and friends should be allowed “within security and operational constraints.” Detainees have to speak confidentially with an attorney. Weber said immigration authorities should tell attorneys where their clients are and allow them to talk in person or use an unmonitored phone line.
Hospitals, though, fall into a gray area on enforcing these rights, since they are primarily focused on treating medical needs, Weber said. Still, he added, hospitals should ensure their policies align with the law.
Family Denied Access
Numerous immigration attorneys have spent weeks trying to locate clients detained by ICE, with their efforts sometimes thwarted by hospitals.
Nicolas Thompson-Lleras, a Los Angeles attorney who counsels immigrants facing deportation, said two of his clients were registered under aliases at different hospitals in Los Angeles County last year. Initially, the hospitals denied the clients were there and refused to let Thompson-Lleras meet with them, he said. Family members were also denied access, he said.
One of his clients was , a car wash worker injured during a raid in August. Immigration agents surveilled him for over a month at Harbor-UCLA Medical Center, a county-run facility, without charging him.
In November, the Los Angeles County Board of Supervisors voted to of blackout policies for patients under civil immigration custody at county-run hospitals. In a statement, Arun Patel, the chief patient safety and clinical risk management officer for the Los Angeles County Department of Health Services, said the policies are designed to reduce safety risks for patients, doctors, nurses, and custody officers.
“In some situations, there may be concerns about threats to the patient, attempts to interfere with medical care, unauthorized visitors, or the introduction of contraband,” Patel said. “Our goal is not to restrict care but to allow care to happen safely and without disruption.”
Leaving Patients Vulnerable
Thompson-Lleras said he’s concerned that hospitals are cooperating with federal immigration authorities at the expense of patients and their families and leaving patients vulnerable to abuse.
“It allows people to be treated suboptimally,” Thompson-Lleras said. “It allows people to be treated on abbreviated timelines, without supervision, without family intervention or advocacy. These people are alone, disoriented, being interrogated, at least in Bayron’s case, under pain and influence of medication.”
Such incidents are alarming to hospital workers. In Los Angeles, two health care professionals who asked not to be identified by ∫⁄¡œ≥‘πœÕ¯ News, out of concern for their livelihoods, said that ICE and hospital administrators, at public and private hospitals, frequently block staff from contacting family members for people in custody, even to find out about their health conditions or what medications they’re on. That violates medical ethics, they said.
Blackout procedures are another concern.
“They help facilitate, whether intentionally or not, the disappearance of patients,” said one worker, a physician for the county’s Department of Health Services and part of a coalition of concerned health workers from across the region.
At Legacy Emanuel Medical Center in Portland, nurses publicly expressed outrage over what they saw as hospital cooperation with ICE and the flouting of patient rights. Legacy Health has to the nurses’ union, accusing it of making “false or misleading statements.”
“I was really disgusted,” said Blaire Glennon, a nurse who quit her job at the hospital in December. She said numerous patients were brought to the hospital by ICE with serious injuries they sustained while being detained. “I felt like Legacy was doing massive human rights violations.”

Handcuffed While Unconscious
Two days before Christmas, Chabolla, Peña’s attorney, received a call from ICE with the answer she and Romero had been waiting for. Peña was at Victor Valley Global Medical Center, about 10 miles from Adelanto, and about to be released.
Excited, Romero and her family made the two-hour-plus drive from Glendale to the hospital to take him home.
When they got there, they found Peña intubated and unconscious, his arm and leg still handcuffed to the hospital bed. He’d had a severe seizure on Dec. 20, but no one had told his family or legal team, his attorney said.
Tim Lineberger, a spokesperson for Victor Valley Global Medical Center’s parent company, KPC Health, said he could not comment on specific patient cases, because of privacy protections. He said the hospital’s policies on patient information disclosure comply with state and federal law.
Peña was finally cleared to go home on Jan. 5. No court date has been set, and his family is filing a petition to adjust his legal status based on his son’s military service. For now, he still faces deportation proceedings.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/courts/ice-immigrants-hospitals-detainees-patients-rights-family-blackout-policies-california/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2149325&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Or, you’ve completed a couple of weeks in rehab. Can you handle your complicated medication regimen, along with shopping and cooking?
Perhaps you fell in the shower, and now your family wants you to arrange help with bathing and getting dressed.
There are facilities that provide such help, of course, but most older people don’t want to go there. They want to stay at home; that’s the problem.
When older people struggle with daily activities because they have grown frail, because their chronic illnesses have mounted, or because they have lost a spouse or companion, most don’t want to move. For decades, surveys have shown that for as long as possible.
That means they need home care, either from family and friends, paid caregivers, or both. But paid home care represents an especially strained sector of the long-term care system, which is experiencing an intensifying labor shortage even as an aging population creates surging demand.
“It’s a crisis,” said Madeline Sterling, a primary care doctor at Weill Cornell Medicine and the director of Cornell University’s . “It’s not really working for the people involved,” whether they are patients (who can also be younger people with disabilities), family members, or home care workers.
“This is not about what’s going to happen a decade from now,” said Steven Landers, chief executive of the National Alliance for Care at Home, an industry organization. “Do an Indeed.com search in Anytown, USA, for home care aides, and you’ll see so many listings for aides that your eyes will pop out.”
Against this grim backdrop, however, some alternatives show promise in upgrading home care jobs and in improving patient care. And they’re growing.
Some background: Researchers and elder care administrators have warned about this approaching calamity for years. Home care is already among the nation’s fastest-growing occupations, with 3.2 million home health aides and personal care aides on the job in 2024, up from 1.4 million a decade earlier, , a research and advocacy group.
But the nation will need about 740,000 additional home care workers over the next decade, , and recruiting them won’t be easy. Costs to consumers are high ‚Äî the median hourly rate for a home health aide in 2024 was $34, shows, with big geographic variations. But an aide’s median hourly wage .
These remain unstable, low-paying jobs. Of the largely female workforce, about a third of whom are immigrants, 40% live in low-income households and most receive some sort of public assistance.
Even if the agencies that employ them offer health insurance and they work enough hours to qualify, many cannot afford their premium payments.
Unsurprisingly, the turnover rate approaches 80% annually, according to , a nonprofit organization that promotes co-ops.
But not everywhere. One innovation, still small but expanding: home care cooperatives owned by the workers themselves. The first and largest, Cooperative Home Care Associates in the Bronx borough of New York City, began in 1985 and now employs about 1,600 home care aides. The ICA Group now counts 26 such worker-owned home care businesses nationwide.
“These co-ops are getting exceptional results,” said Geoffrey Gusoff, a family medicine doctor and health services researcher at UCLA. “They have half the turnover of traditional agencies, they hold onto clients twice as long, and they’re paying $2 more an hour” to their owner-employees.
When Gusoff and his co-authors interviewed co-op members for in JAMA Network Open, “we were expecting to hear more about compensation,” he said. “But the biggest single response was, ‚ÄòI have more say’” over working conditions, patient care, and the administration of the co-op itself.
“Workers say they feel more respected,” Gusoff said.
Through an initiative to provide financing, business coaching, and technical assistance, the ICA Group intends to boost the national total to 50 co-ops within five years and to 100 by 2040.
Another approach gaining ground: registries that allow home care workers and clients who need care to connect directly, often without involving agencies that provide supervision and background checks but also absorb roughly half the fee consumers pay.
One of the largest registries, . Established through agreements with the Service Employees International Union, the nation’s largest health care union, it serves 40,000 providers and 25,000 clients. (About 10% of home care workers are unionized, according to PHI’s analysis.)
Carina functions as a free, “digital hiring hall,” said Nidhi Mirani, its chief executive. Except in the Seattle area, it serves only clients who receive care through Medicaid, the largest funder of care at home. State agencies handle the paperwork and oversee background checks.
Hourly rates paid to independent providers found on Carina, which are set by union contracts, are usually lower than what agencies charge, while workers’ wages start at $20, and they receive health insurance, paid time off, and, in some cases, retirement benefits.
may be operated by states, as in Massachusetts and Wisconsin, or by platforms like , available in four states. “People are seeking a fit in who’s coming into their homes,” Mirani said. “And individual providers can choose their clients. It’s a two-way street.”
Finally, recent studies indicate ways that additional training for home care workers can pay off.
“These patients have complex conditions,” Sterling said of the aides. Home care workers, who take blood pressure readings, prepare meals, and help clients stay mobile, can spot troubling symptoms as they emerge.
Her team’s recent clinical trial of home health ‚Äî “the No. 1 cause of hospitalization among Medicare beneficiaries,” Sterling pointed out ‚Äî measured the effects of a 90-minute virtual training module about its symptoms and management.
“Leg swelling. Shortness of breath. They’re the first signs that the disease is not being controlled,” Sterling said.
In the study, involving 102 aides working for VNS Health, a large nonprofit agency in New York, the training was shown to enhance their knowledge and confidence in caring for clients with heart failure.
Moreover, when aides were given a mobile health app that allowed them to message their supervisors, they made fewer 911 calls and their patients made fewer emergency room visits.
Small-scale efforts like registries, co-ops, and training programs do not directly address home care’s most central problem: cost.
Medicaid underwrites home care for low-income older adults who have few assets, though the Trump administration’s new budget by more than $900 billion over the next decade. The well-off theoretically can pay out-of-pocket.
But “middle-class retired families either spend all their resources and essentially bankrupt themselves to become eligible for Medicaid, or they go without,” Landers said. Options like assisted living and nursing homes are even more expensive.
The United States has never committed to paying for long-term care for the middle class, and it seems unlikely to do so under this administration. Still, savings from innovations like these can reduce costs and might help expand home care through federal or state programs. Several tests and pilots are underway.
Home care workers “have a lot of insight into patients’ conditions,” Sterling said. “Training them and giving them technological tools shows that if we’re trying to keep patients at home, here’s a way to do that with the workforce that’s already there.”
The New Old Age is produced through a partnership with .
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/aging/new-old-age-home-care-alternatives-cooperatives-registries-training/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2125124&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>For those in or near Columbia Memorial, the city’s only hospital, there will soon be a different plan: Shelter in place. The hospital is building a new facility next door with an on-site tsunami shelter — an elevated refuge atop columns deeply anchored in the ground, where nearly 2,000 people can safely wait out a flood.
Oregon needs more shelters like the one that Columbia Memorial is building, emergency managers say. Hospitals in the region are likely to incur serious damage, if not ruin, and could take more than three years to fully recover in the event of a major earthquake and tsunami, according to .
Columbia Memorial’s current facility is a single-story building, a half-century ago, that would likely collapse and sink into the ground or be swallowed by a landslide after a major earthquake or a tsunami, said Erik Thorsen, the hospital’s chief executive.
“It is just not built to survive either one of those natural disaster events,” Thorsen said.
At least 10 other hospitals along the Oregon coast are in danger as well. So Columbia Memorial leaders proposed building a hospital capable of withstanding an earthquake and landslide, with a tsunami shelter, instead of relocating the facility to higher ground. Residents and state officials supported the plans, and the federal government awarded a $14 million grant from the Federal Emergency Management Agency to help pay for the tsunami shelter.
The project broke ground in October 2024. Within six months, the Trump administration had , known as Building Resilient Infrastructure and Communities, or BRIC, calling it “yet another example of a wasteful and ineffective FEMA program … more concerned with political agendas than helping Americans affected by natural disasters.”
Molly Wing, director of the expansion project, said losing the BRIC grant felt like “a punch to the gut.”
“We really didn’t see that coming,” she said.

This summer, Oregon and 19 other states sued to restore the FEMA grants. On Dec. 11, a that the Trump administration had unlawfully ended the program without congressional approval.
The administration did not immediately indicate it would appeal the decision, but Department of Homeland Security spokesperson Tricia McLaughlin said by email: “DHS has not terminated BRIC. Any suggestion to the contrary is a lie. The Biden Administration abandoned true mitigation and used BRIC as a green new deal slush fund. It’s unfortunate that an activist judge either didn’t understand that or didn’t care.” FEMA is a subdivision of DHS.
Columbia Memorial was one of the few hospitals slated to receive grants from the BRIC program, which had announced more than $4.5 billion for nearly 2,000 building projects since 2022.
Hospital leaders have decided to keep building — with uncertain funding — because they say waiting is too dangerous. With the Trump administration reversing course on BRIC, fewer communities will receive help from FEMA to reduce their disaster risk, even places where catastrophes are likely.
More than three centuries have passed since a major earthquake caused the Pacific Northwest’s coastline to drop several feet and unleashed a tsunami that crashed onto the land in January 1700, according to scientists who study the evolution of the Oregon coast.
The greatest danger is an underwater fault line known as the , which lies 70 to 100 miles off the coast, from Northern California to British Columbia.
The Cascadia zone can produce a megathrust earthquake, with a magnitude of 9 or higher — the type capable of triggering a catastrophic tsunami — , according to the U.S. Geological Survey. Scientists predict a 10% to 15% chance of such an earthquake along the fault zone in the next 50 years.
“We can’t wait any longer,” Thorsen said. “The risk is high.”

Building for the Future
The BRIC program started in 2020, during the first Trump administration, to provide communities and institutions with funding and technical assistance to fortify their structures against natural disasters.
Joel Scata, a senior attorney with the environmental advocacy group Natural Resources Defense Council, said the program helped communities better prepare so they could reduce the cost of rebuilding after a flood, tornado, wildfire, or extreme weather event.
To qualify for a grant, a hospital had to show that the project’s benefits were greater than the future danger and cost. In some cases, that benefit might not be readily apparent.
“It prevents bad disasters from happening, and so you don’t necessarily see it in action,” Scata said.
Scata noted that the Trump administration has also stopped awarding grants through FEMA’s Hazard Mitigation Grant Program, which predates BRIC.
“There really is no money going out the door from the federal government to help communities reduce their disaster risk,” he said.
A recent ∫⁄¡œ≥‘πœÕ¯ News investigation using proprietary data from Fathom, a global leader in flood modeling, found that at least 170 U.S. hospitals are at risk of significant and potentially dangerous flooding from more intense and frequent storms. That count did not include Columbia Memorial, as Fathom’s data did not account for tsunamis. It models flooding from rivers, sea level rise, and extreme rainfall.
In recent days, an atmospheric river — a narrow storm band carrying significant amounts of moisture — dumped more than 15 inches of rain on parts of Oregon and Washington, causing catastrophic flooding along rivers and the coast. In the Washington town of Sedro-Woolley, which sits along the Skagit River, the PeaceHealth evacuated nonemergency patients.
High winds battered Astoria, leaving the city with some minor landslides, according to news reports. But flooding on the road to the nearby beach town of Seaside made the drive nearly impassable.
The Trump administration is leaning on states to take greater responsibility for recovering from natural disasters, Scata said, but most states are not financially prepared to do so.
“The disasters are just going to keep on piling up,” he said, “and the federal government’s going to have to keep stepping in.”

A Hospital at Risk
Columbia Memorial is blocks from the southern shore of the Columbia River, near the Washington border, where the include earthquakes, tsunamis, landslides, and floods. A critical access hospital with 25 beds, it opened in 1977 — before state building codes addressed tsunami protections.
Thorsen said the new facility and shelter would be a “model design” for other hospitals. Design plans show a five-level hospital built atop a foundation anchored to the bedrock and surrounded by concrete columns to shield it from tsunami debris.
The shelter will be on the roof of the second floor, above the projected maximum tsunami inundation. It will be accessible via an outdoor staircase and interior staircases and elevators, with enough room for up to 1,900 people, plus food, water, tents, and other supplies to sustain them for five days.


With most patient care provided on the second and third levels, generators on the fourth level, and utility lines underground, the hospital is expected to remain operational after a natural disaster.
Thorsen said an earthquake and tsunami threaten not only vast flooding , in which the ground loosens and causes structures above it to collapse. Deep foundations, thick slabs, and other structural supports are expected to protect the new hospital and tsunami structure against such failure.
Through the years, hospital administrators and civic leaders in Astoria have sought other locations for Columbia Memorial. But relocation wasn’t economical. Columbia Memorial committed to invest in a new hospital and tsunami shelter to protect not only patients and staff but also nearby residents.
“Your community should count on your hospital to be a safe haven in a natural disaster,” Thorsen said.

Fighting To Restore Funds
The estimated construction budget for Columbia Memorial’s expansion is $300 million, mostly financed through new debt from the hospital. The tsunami shelter is budgeted at about $20 million, for which FEMA’s BRIC program , with a $6 million matching grant from the state, which has maintained its support.
The shelter and the building’s structural protections — featuring reinforced steel, deeper foundations, and thicker slabs — are integral to the design and cannot be removed without compromising the rest of the structure, said Michelle Checkis, the project architect.
“We can’t pull the TVERS [tsunami vertical evacuation refuge structure] out without pulling the hospital back apart again,” she said. “It’s kind of like, if I was going to stack it up with Legos, I would have to take all those Legos apart and stack it up completely differently.”

Columbia Memorial has sought help from Oregon’s congressional delegation. In to Department of Homeland Security Secretary Kristi Noem and former FEMA acting administrator David Richardson, the lawmakers demanded that the agencies restore the hospital’s grant.
The hospital’s leadership is seeking other grants and philanthropic donations to make up for the loss. As a last resort, Thorsen said, the board will consider removing “nonessential features” from the building, though he added that there is little fat to trim from the project.
The in July alleged that FEMA lacks the authority to cancel the BRIC program or redirect its funding for other purposes.
The states argued that canceling the program and undermined projects underway.
In their response to the lawsuit, the Trump administration said repeatedly that the defendants “deny that the BRIC program has been terminated.”
The lawsuit cites examples of projects at risk in each state due to FEMA’s termination of the grants. Oregon’s first example is Columbia Memorial’s tsunami shelter. “Neither the County nor the State can afford to resume the project without federal funding,” the lawsuit states.
In response to questions about the impact of canceling the grant on Astoria and the surrounding community, DHS spokesperson Tricia McLaughlin said BRIC had “deviated from its statutory intent.”
“BRIC was more focused on climate change initiatives like bicycle lanes, shaded bus stops, and planting trees, rather than disaster relief or mitigation,” McLaughlin said. DHS and FEMA provided no further comment about BRIC or the Astoria hospital.


Preparing for a Tsunami Disaster
Located near the end of the Lewis & Clark National Historic Trail, Astoria sits on a peninsula that juts into the Columbia River near the Pacific Ocean.
Much of the city is not in the tsunami inundation area. But Astoria’s downtown commercial district — where gift shops, hotels, and seafood restaurants line the streets — is nearly all an evacuation zone.
Two hospitals — Ocean Beach Health in nearby Washington, and Providence Seaside Hospital in Oregon — are about 20 miles from Columbia Memorial. Both are 25-bed hospitals, and neither is designed to withstand a tsunami.
Ocean Beach Health regularly conducts drills for mass-casualty and natural disasters, said Brenda Sharkey, its chief nursing officer.
“We focus our planning and investments on areas where we can make a real difference for our community before, during, and after an event — such as maintaining continuity of care, ensuring rapid triage, and coordinating with regional emergency partners,” Sharkey said in an email.

Gary Walker, a spokesperson for Providence Seaside, said in a statement that the hospital has a “comprehensive emergency plan for earthquakes and tsunamis, including alternative sites and mobile resources.”
Walker added that Providence Seaside has hired “a team of consultants and experts to conduct a conceptual resilience study” that would evaluate the hospital’s vulnerabilities and recommend ways to address them.
Oregon’s emergency managers advise residents and visitors in coastal communities to immediately seek higher ground after a major earthquake — and not to rely on tsunami sirens, social media, or most technology.
“There may not even be cellphone towers operating after an event like this,” said Jonathan Allan, a coastal geomorphologist with the Oregon Department of Geology and Mineral Industries. “The earthquake shaking, its intensity, and particularly the length of time in which the shaking persists, is the warning message.”
The stronger the earthquake and the longer the shaking, he said, the more likely a tsunami will head to shore.
A tsunami triggered by a Cascadia zone earthquake could strike land in , according to state estimates.
Many of Oregon’s seaside communities are near high-enough ground to seek safety from a tsunami in a relatively short time, Allan said. But he estimated that, to save lives, Oregon would need about a dozen vertical tsunami evacuation shelters along the coast, including in seaside towns that attract tourists and where the nearest high ground is a mile or more away.
Willis Van Dusen’s family has lived in Astoria since the mid-19th century. A former mayor of Astoria, Van Dusen stressed that tsunamis are not a hypothetical danger. He recalled seeing one in Seaside in 1964. The wave was only about 18 inches high, he said, but it flooded a road and destroyed a bridge and some homes. The memory has stayed with him.
“It’s not like … ‘Oh, that’ll never happen,’” he said. “We have to be prepared for it.”


∫⁄¡œ≥‘πœÕ¯ News correspondent Brett Kelman contributed to this report.
This <a target="_blank" href="/health-industry/tsunami-shelter-oregon-hospital-fema-funding-cut-lawsuit/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2130169&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>California, Massachusetts, Connecticut, and have set caps on health care spending in a bid to rein in the intense financial pressure felt by many families, individuals, and employers who every year face increases in premiums, deductibles, and other health-related expenses.
Hospitals and other health care providers are citing Republicans’ One Big Beautiful Bill Act, signed by President Donald Trump in July, as one more reason to challenge those limits.
The law is expected to reduce federal Medicaid spending by over a decade, which mathematically should help the overall health care system meet the caps. But the law is also expected to increase the number of uninsured Americans, mostly Medicaid beneficiaries, by an estimated . Health care analysts predict hospitals and other providers will raise prices to cover the double whammy of lost Medicaid revenue and the cost of caring for an influx of newly uninsured patients.
Whether regulators in some states will allow providers to justify higher prices and exceed the spending caps is unclear. Only can penalize providers financially if they fail to meet targets.
“Are we going to say, ‚ÄòThat’s OK’? Or are we going to say, ‚ÄòWell, you exceeded the target. We’re still going to penalize you for that’?” said Richard Pan, a former state lawmaker and a member of the California Office of Health Care Affordability’s board. “That has not yet been decided.”
The California Hospital Association, the industry’s main state lobbying group, in October asking a state court to strike down the spending caps, which it argued fail to account for all the cost pressures hospitals face. Those pressures, it said, include an aging, sicker population; the of labor; expensive advances in medical technology; large capital outlays on required seismic retrofitting; and changes in federal policy, including the One Big Beautiful Bill Act. The hospital group’s lawsuit also asserted that the state affordability office, by hastily imposing ill-considered cost-cutting targets, was undermining its other key mission of improving health care access, quality, and equity.
California’s affordability office last year set a five-year target to cap statewide spending growth, starting at 3.5% in 2025 and declining to 3% by 2029. The annual caps apply to a wide range of health care entities, including hospitals, medical groups, insurers, and other payers.
Earlier this year, it imposed much lower spending growth caps — starting at 1.8% in 2026 and declining to 1.6% by 2029 — for .
“The spending caps set by politically appointed bureaucrats could force cuts that result in many Californians traveling farther for care, facing longer emergency room wait times, experiencing more overcrowding, and losing access to critical services,” Carmela Coyle, the hospital association’s president and CEO, said in an October press release.
The California attorney general’s office, which will represent the affordability agency, has not yet filed a response to the hospital group’s complaint and did not respond to a request for comment.
Hospitals’ Pushback
California is not the only state taking a close look at hospital prices, which are widely considered a of health care costs.
“States, armed with information that points to payments to hospitals as a driver of what is way beyond affordable commercial premiums, have begun to take increasingly targeted actions focused on commercial hospital prices,” said Michael Bailit, founder of the Needham, Massachusetts-based consultancy , which has advised multiple states, including California, on ways to tame health care spending. “It is not surprising that the hospital industry is going to oppose such state actions.”
In its lawsuit, the California Hospital Association said the affordability office’s own report showed that pharmaceutical and insurance companies are largely responsible for high costs.
Hospitals in some states with cost growth limits, including and , have expressed objections similar to the ones raised in the California lawsuit. They could follow their counterparts in California if their lawsuit succeeds, said Peter Lee, who led California’s Affordable Care Act marketplace, Covered California, for and is now a at Stanford Medicine’s Clinical Excellence Research Center.
Lee said the work of California’s affordability office and similar agencies in other states is just about the only systemwide effort being made to cut health care costs. They are basically saying, “‚ÄòLook, health care is taking money away from education, it is taking money away from the environment, it is taking money away from everything in the public sector, and in the private sector it is taking money away from wages,’” he said. “‚ÄòWe don’t know how you, the health system, are going to do it, but it is your job not just to provide quality but to lower costs. Here’s the target.’”
To be sure, achieving the cost savings that California and those other states are seeking is no easy lift. It will ultimately require persuading large, financially powerful players that compete fiercely for health care dollars to adopt a different mindset and begin cooperating to reduce costs instead. And that, in many cases, will mean lower revenue.
But the status quo, as many people know all too well, means continued financial pain for millions.
In early 2020, Estevan Rodriguez, a bartender at California’s Monterey Beach Hotel, had surgery for a staph infection in his leg. The bill came to nearly $168,000. His insurance paid most of it, but he still owed $5,665, which took him two years to pay, more than $200 every month. “It may not be a lot to some people, but it was a lot to me,” Rodriguez said.
He said he dropped his Hulu subscription, switched to a lower-cost cellphone, and got cheaper car insurance. He started going to food banks rather than the grocery store, he said, and had a lot less time with his kids, because he was constantly working to pay off the hospital bill.
, where Rodriguez had his surgery, is one of the seven hospitals identified by California’s affordability office as high-cost. A attributed high hospital prices in Monterey County to a lack of market competition “rather than higher operating costs or superior quality of care.”
The Monterey hospital referred a request for comment about its “high-cost” designation to the California Hospital Association. CHA spokesperson Jan Emerson-Shea declined to comment beyond the language of the lawsuit and Coyle’s press release statement.
Reduced Competition
Health care analysts worry the One Big Beautiful Bill Act will reduce market competition even further by stressing already weak hospitals, leading some to shut services, merge with larger health systems, or close. One study estimates are at risk of closing nationwide.
Less competition, in addition to fewer Medicaid dollars and an increase in uninsured patients, will only strengthen the incentive of health systems with the requisite market clout to raise their commercial prices, increasing premiums for employers and individuals.
“We think commercial prices will continue to increase as health care providers, and hospitals in particular, will seek to preserve or increase their revenue,” said Rachel Block, a program officer at the Milbank Memorial Fund, a foundation that focuses on health equity.
That in turn could pose a challenge to state affordability regulators tasked with overseeing compliance with growth targets for health care spending.
California’s affordability office is required to consider mitigating factors, including changes in federal and state laws. But some of its board members have expressed skepticism about letting hospitals offset Medicaid losses with higher commercial prices.
“There’s a lot of talk about using HR 1 and other federal policies as an excuse to raise prices on commercial payers,” Ian Lewis, an affordability office board member and policy director for UNITE HERE Local 2, a hospitality workers union in the Bay Area, said at the agency’s , referring to the One Big Beautiful Bill. “There’s no more blood to be squeezed from this stone.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/health-costs-spending-affordability-hospitals-california-one-big-beautiful-bill/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2131203&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>