The CDC withheld the data for months as a team hit hard by mass layoffs and resignations sorted through the information. But now that scientists at the agency have posted their first batch of whole measles genomes ‚Äî the genetic blueprint of the viruses ‚Äî the rest should “start flowing more smoothly at a more rapid cadence,” said Kristian Andersen, an evolutionary virologist at the Scripps Research Institute who isn’t involved with the CDC’s effort but is following it.
The CDC did not answer queries from ∫⁄¡œ≥‘πœÕ¯ News on its timeline for publishing measles data or analyses. However, once all the data is public, researchers can run that will signal whether outbreaks across the U.S. last year resulted from the continuous spread of the disease between states, rather than separate introductions from abroad. If there was continuous transmission for a year, that means the U.S. has lost its status as a country that has eliminated measles. That status, which the U.S. has held since 2000, reflects a country’s vaccination rates: Two doses of the measles-mumps-rubella vaccine prevent most infections and so stop outbreaks from growing.
More careful analyses take weeks.
“We should see a report in April,” Andersen said, “assuming no political interference.”
This is the first time that the U.S. has applied sophisticated genomic techniques to measles, which largely disappeared from the country a quarter-century ago because of broad vaccine uptake.
Declining , misinformation, and the Trump administration’s to outbreaks have fueled a resurgence of the disease. With at least 2,285 cases in 44 states, 2025 was the worst year for measles in more than three decades. This year is on track to surpass that, with 1,575 cases as of late March.
While welcoming the science, researchers say the government’s top priority should be to stop the virus from spreading.
“I think it’s incredibly important to do whole genome sequencing for outbreaks,” Andersen said, “but we shouldn’t need to do this for measles in the first place, because we have an extremely effective and safe vaccine.”
“That we’re even talking about this is nuts,” he added.
Health and Human Services Secretary Robert F. Kennedy Jr. and other government officials should sound an alarm about measles’ comeback and launch nationwide vaccine campaigns, said Rekha Lakshmanan, executive director of , a nonprofit in Houston that advocates for vaccine access.
“I applaud the science,” she said, “but the more urgent need is to get measles under control as quickly as possible.”

Top officials have instead , and false notions about vaccines have been granted new life in Kennedy’s CDC. This includes abrupt changes to vaccine information on CDC websites that say aren’t based on evidence and endanger lives.
Kennedy continues to promote unproven remedies that could mislead parents into believing that they can avoid vaccines without consequence. On the podcast in late February, Kennedy spoke at length about measures to improve America’s health but didn’t mention vaccines. He said preventive measures could entail “holistic medicine, or take vitamins, or take vitamin D, which is, as you know, it’s kind of miraculous.”
“The risk of measles remains low for most of the United States,” HHS spokesperson Emily Hilliard wrote. “CDC has made $8.5 million available to address measles response activities in 7 jurisdictions experiencing outbreaks,” she wrote. “The CDC, HHS principles, and the Secretary have been vocal that the MMR vaccine is the best way to protect yourself against measles.”
1,000 Genomes
In December, the CDC enlisted the help of one of the country’s leading centers for virus sequencing, the Broad Institute in Cambridge, Massachusetts. Major outbreaks in Texas, Utah, and South Carolina had been fueled by the same type of measles virus, labeled D8-9171. But since that type also circulates in Canada and Mexico, researchers need more data to discern whether it spread among states or entered the U.S. multiple times.
Whole genome sequencing provides that information because viruses evolve over time. The measles virus acquires a mutation every two to four transmissions between people, said Bronwyn MacInnis, director of pathogen surveillance at the Broad.
“There is enough signal in this data to tease apart questions at hand,” MacInnis said, “the main one being sustained transmission within this country.”
MacInnis’ team worked overtime to sequence the entire genomes of inactivated measles viruses that had been collected from states in 2025 and 2026.
“We’ve done about 1,000 samples and delivered the genome data back to the CDC,” sending it on a rolling basis since December, MacInnis said. “This is the CDC’s data to publish.”
The CDC didn’t post a single one of those genomes until late March, when eight appeared on a public database hosted by the National Center for Biotechnology Information. By April 1, an additional 154 had gone online.
“It should be on NCBI within a couple of weeks of being produced,” Andersen said, “and certainly not take longer than a month when you have an active outbreak.”
Genomic data holds clues about how outbreaks start and spread. It allows researchers to develop tests, treatments, and vaccines — and detect variants that might evade them.
Such data was critical in the covid pandemic. Chinese and Australian scientists online on Jan. 10, 2020, of sequencing it. “It definitely shouldn’t take the CDC months,” said Eddie Holmes, the Australian virologist who helped publish the first coronavirus sequence.


One reason for the delay is that the CDC’s measles lab has been sorely understaffed amid mass layoffs and other turmoil at the agency over the past year, a CDC scientist told ∫⁄¡œ≥‘πœÕ¯ News. Another reason, the researcher added, is a learning curve: The CDC and health departments haven’t needed to sequence hundreds of whole measles genomes before now. (∫⁄¡œ≥‘πœÕ¯ News agreed not to identify the scientist, who feared retaliation.)
In contrast with the CDC, the Utah Public Health Lab has shared measles genomes rapidly. Most of some 970 measles genomes posted online since Jan. 1, 2025, were sequenced by the state, hailing from Utah, Arizona, South Carolina, and other states willing to share them.
“We’ve only got a handful of samples from Texas that were collected kind of in the middle of their outbreak,” said Kelly Oakeson, a genomics researcher at the Utah Department of Health and Human Services. The genomes of the Texas and Utah measles viruses are similar but distinct, Oakeson said, meaning that intermediate versions of the virus are missing.
If the genetic code of viruses collected late in the Texas outbreak are a closer match to those from Utah’s, that will suggest that spread was continuous and the country has lost its measles-free status. The hundreds of genome sequences still sitting at the CDC probably hold the answer.
Waiting on the CDC
The CDC expected to finish its analysis before April, said Daniel Salas, executive manager of the immunization program at the Pan American Health Organization, which works with the World Health Organization. That’s when PAHO was slated to evaluate the United States’ measles status.
He said PAHO delayed its evaluation until the organization’s annual meeting in November, partly because the CDC needed more time to do the genomic analysis and partly because the measles status of Mexico, Bolivia, and other countries is also under review, and holding staggered meetings for each country is inefficient.
The U.S. is the only country using whole genome sequencing to answer the elimination question, Salas said. Typically, countries classify measles viruses according to a tiny snippet of genes, then assume that large outbreaks caused by the same type are linked. Whole genomes provide a more accurate view.
“If the U.S. can fill in the blanks with genomic data, that’s a sort of breakthrough,” Salas said. “That doesn’t mean other countries are going to be able to pull off this kind of analysis,” he added. “It takes a lot of specialized knowledge and resources.”
Equipment to sequence and analyze genomes costs upward of $100,000, and the cost to process each sample, including paying the researchers involved, typically ranges from $100 to $500 per sequence.
“I’m pro-science, but we shouldn’t have to do this,” said Theresa McCarthy Flynn, president of the North Carolina Pediatrics Society. “We don’t have to have a measles epidemic.”

Flynn said she regularly fields questions from parents concerned by misinformation spread by Kennedy and anti-vaccine groups, including the one he founded before joining the Trump administration. Parents have also pointed to changes in the CDC’s recommendations and to its websites that are at odds with the scientific consensus.
Before Kennedy took the helm, a said “Vaccines do not cause autism” in prominent type, and listed in premier scientific journals that refuted a link between vaccines and developmental disorders.
Last year, shifted to saying, “Studies supporting a link have been ignored by health authorities.” The high-quality studies were replaced with a report from a single investigator who has ties to anti-vaccine groups. In an email to ∫⁄¡œ≥‘πœÕ¯ News, HHS spokesperson Hilliard echoed the altered website’s claims about vaccines, disregarding extensive studies on the topic.
Flynn, of the pediatrics association, said, “The CDC itself is spreading misinformation about vaccines. I cannot overstate the seriousness of this.”
Although the acting director of the CDC, Jay Bhattacharya, says vaccines are the best way to prevent measles, he too has undermined vaccine policy. He said the controversial to reduce the number of vaccines recommended to children was based on “gold standard science.” In fact, the new schedule makes the among peer nations. Hilliard wrote that the updated schedule was “aligning U.S. guidance with international norms.”
A federal court temporarily invalidated the change last month in a lawsuit brought by the American Academy of Pediatrics and other groups.
Bhattacharya hasn’t held briefings with the public or the press on the surge of measles this year or activated the CDC’s emergency capabilities.
“Normally, we’d have a big push to get vaccination rates up in areas where it’s low. We’d do a big social media push, put out ads on getting vaccinated,” said another CDC scientist whom ∫⁄¡œ≥‘πœÕ¯ News agreed not to identify, because of fears of retaliation. “People at the CDC want to do this, but political leadership at the agency has not allowed the CDC to do it.”
Further, the Trump administration’s to public health funds have made it hard for local health officials to protect communities. Philip Huang, director at Dallas County Health and Human Services in Texas, said the department lost over $4 million when the administration clawed back about $11 billion from health departments early last year as a measles outbreak surged in the state.
“We lost 27 staff and had to cancel over 20 of our community vaccination efforts, including to schools identified as having low vaccination rates,” he said. “There are simultaneous attacks on immunizations that are making our jobs harder.”
This <a target="_blank" href="/public-health/measles-genome-cdc-data-elimination-status-outbreaks-rfk/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2177574&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But seven months later, findings from five states shared with ∫⁄¡œ≥‘πœÕ¯ News show that the reviews have uncovered little evidence of a widespread problem.
Only U.S. citizens and some lawfully present immigrants are eligible for Medicaid, which covers health care costs for people with low incomes and disabilities, and the closely related Children’s Health Insurance Program. Both programs are administered by states.
Spokespeople from Pennsylvania’s and Colorado’s Medicaid agencies said, as of March, the states had found no one who needed to be terminated from Medicaid. That was after checking a combined 79,000 names.
Texas has reviewed records of more than 28,000 Medicaid enrollees at the Trump administration’s request and terminated coverage for 77 of them, according to Jennifer Ruffcorn, a spokesperson for the Texas Department of Human Services.
Ohio has checked 65,000 Medicaid enrollees, of which 260 people were disenrolled from the program, said Stephanie O’Grady, a spokesperson for the Ohio Department of Medicaid.
In Utah, 42 of the 8,000 enrollees identified by the Trump administration had their Medicaid coverage terminated, said Becky Wickstrom, a spokesperson for the state’s Department of Workforce Services.
In announcing the reviews, Health and Human Services Secretary Robert F. Kennedy Jr. said: “We are tightening oversight of enrollment to safeguard taxpayer dollars and guarantee that these vital programs serve only those who are truly eligible under the law.”
Leonardo Cuello, a research professor at Georgetown University’s Center for Children and Families, said the reviews ordered by the federal Centers for Medicare & Medicaid Services were unneeded because states check immigration status when people sign up.
“It is entirely predictable that all of these burdensome reviews that the federal government is forcing upon states would yield no pay dirt,” Cuello said. “The states had already done the reviews once, and CMS was just making them reverify the same information they had already checked. Making states go through the same bureaucratic process twice is incredibly wasteful and inefficient.”
CMS spokesperson Chris Krepich said in a statement to ∫⁄¡œ≥‘πœÕ¯ News that the ongoing checks are verifying eligibility “for certain enrollees whose status could not be confirmed through federal data sources.”
“CMS provides states with regular reports for follow-up review, and states are responsible for independently verifying eligibility and taking appropriate action consistent with federal requirements,” he said.
But the findings shared with ∫⁄¡œ≥‘πœÕ¯ News also suggest that many of the enrollees whose eligibility the Trump administration said it could not confirm are indeed U.S. citizens. O’Grady said Ohio found that, of the 65,000 names referred by the federal government, the state already had information on 53,000 confirming them as citizens and an additional 11,000 showing appropriate immigration status for Medicaid.
Caseworkers then worked on the remaining 1,000 names to review their information or reach out for more details, she said.
CMS did not answer questions about the findings from the states sampled by ∫⁄¡œ≥‘πœÕ¯ News or provide information about responses it received from all 50 states and the District of Columbia, which were instructed to perform verification checks.
The agency also did not respond to a question about whether it’s forwarding the names of those whose Medicaid coverage was terminated to federal immigration officials.
In June, advisers to Kennedy ordered CMS to share information about Medicaid enrollees with the Department of Homeland Security, prompting a lawsuit by some states alarmed that the administration would use the information for its deportation campaign against residents living in the U.S. without authorization.
A federal judge that Immigration and Customs Enforcement workers could access information only about people in the country unlawfully in the Medicaid databases of the states that sued.
CMS continues to send states lists of names at least every few months, though state officials say the numbers have declined since the first batch last summer.
People without legal status are ineligible for federally funded health coverage, including Medicaid, Medicare, and plans through the Affordable Care Act marketplaces. Medicaid does reimburse hospitals for providing emergency care to people without legal status if they meet income and other program requirements.
Seven states and the District of Columbia provide health coverage regardless of immigration status, funding the programs with their own money.
In March 2025, CMS began financial reviews of those programs. “CMS has identified over $1.8 billion in federal funds that are being recouped through voluntary returns and deferrals of future federal Medicaid payments,” Krepich said. He did not answer how much has been collected so far or from which states.
Medicaid’s overall spending topped $900 billion in fiscal year 2024.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/medicaid-undocumented-enrollees-review-few-violators/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2174376&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>While taking her history and vital signs, Supiano, a geriatrician at the University of Utah, saw one disturbing signal: Her blood pressure was 148/86, above normal despite her taking two medications intended to lower it. “Clearly that was too high,” he said recently.
Several factors could have contributed to the high reading, including the anti-inflammatory drug the 78-year-old woman took for arthritis pain, a high-sodium diet, and a lack of regular exercise. She had also told Supiano that she typically drank a couple of glasses of wine each evening.
After Supiano discussed ways to lower her risk, the woman and her husband joined a gym. She stopped taking the anti-inflammatory and cut back on salt and alcohol, bringing her systolic blood pressure readings into the 130-to-140 range — still hypertension, according to issued by the American Heart Association and the American College of Cardiology later that year, but more acceptable. (Systolic is the top number in the blood pressure ratio and the more clinically important number.)
By 2019, though, the patient had a diagnosis of mild cognitive impairment, and medical evidence was emerging about a connection between hypertension (the medical term for high blood pressure) and dementia. “I was not as aggressive as I should have been,” Supiano recalled. He added a third drug for high blood pressure to the woman’s regimen, and her readings fell to 120 or lower.
The shifting guidelines for blood pressure control may remind those at advanced ages of a dance fad from their youth, the limbo. As Chubby Checker once intoned, “How low can you go?”
For more than 25 years, a reading of 140/90 or below was considered normal, according to the AHA/ACC guidelines. But the 2017 update introduced major changes, backed by results from the , which enrolled adults over 50 who were at high cardiovascular risk.
The SPRINT trial found that intensive treatment aimed at bringing the systolic number below 120 reduced the risk of heart attacks, strokes, other cardiovascular illnesses, and overall mortality so substantially that the investigators .
It was unethical, they decided, to deny half the trial participants the benefits of intensive treatment. The 2017 guidelines, therefore, recommended medication for those with a systolic blood pressure over 130.
∞’≥Û±Ã˝, issued last year, encourage still tighter control. They call for patients at cardiovascular risk to strive for systolic readings below 120, and they also call that target “reasonable” even for those who are not at high risk. Readings considered normal not so long ago are now defined as hypertension.
Blood pressure normally rises with age because “with stiffening of the arteries, the heart has to pump harder,” said Erica Spatz, the director of the preventive cardiovascular health program at the Yale School of Medicine. From 2021 to 2023, about had hypertension, according to the operative definition at the time.
But recent revisions could “define a lot more people as having high blood pressure,” said Rita Redberg, a cardiologist at the University of California-San Francisco.
To Supiano, recent and that show cognitive benefit for the lower readings “have tipped the scales” for older adults. “What’s good for the heart is good for the brain,” he said, calling those findings “a lever to get people to pay more attention to their blood pressure. They may not want to live longer, but they want to hold on to their cognition longer.”
Nearly all major medical associations, including the American Geriatrics Society (Supiano is the chair of the organization’s board), have endorsed the latest guidelines.
“I used to be lenient in many of my older patients,” said John Dodson, a cardiologist and researcher at NYU Langone Health. “If I overtreated high blood pressure, bad things were going to happen.”
Blood pressure that drops too low — hypotension — can cause dizziness and fainting or injuries from falls.
Now, Dodson said, “I’m treating my older patients more aggressively.” Studies have shown that treating high blood pressure¬Ý. And while older adults in the SPRINT trial had more fall injuries, the rate wasn’t higher¬Ý¬Ýthan in those undergoing standard treatment. Among those over 75, it was¬Ý¬Ýfor both groups.
Another significant change: The new guidelines recommend at-home monitoring.
“Blood pressure is tricky,” Spatz pointed out. “It varies throughout the day, depending on whether a person is just waking up or just ate or it’s hot outside.” Systolic readings can bounce around by 30 points or more in a single day.
And they’re almost always higher in a doctor’s office. “I don’t want to put much stock in one reading,” Spatz said.
“Maybe the patient has white-coat syndrome,” she added, referring to anxiety about doctors and testing, “or they had a fight with the parking attendant” on the way in.
She asks patients to record their blood pressure twice a day for a week or two before their appointments. Some doctors prescribe a 24-hour home monitor.
Will patients adopt home monitoring and more aggressive treatment? Cardiologists argue that high blood pressure, almost always asymptomatic, remains undertreated despite the newer guidelines.
Price is not likely to present an obstacle. Most patients need two or three drugs to lower blood pressure, but as generics they’re “dirt cheap, about $5 a month,” and rarely interact with the other drugs that are often prescribed for older people, Supiano said. A blood pressure monitor for home use , or more for those that digitally transmit data.
Although some side effects are serious ‚Äî a fall can be life-altering ‚Äî most complications “thankfully are transient and reversible and rather mild,” he said.
Yet the guidelines have skeptics, too. Redberg, for example, counsels older patients about diet, exercise, and weight loss but does not urge them to start medication to reduce a 135 systolic reading to below 120.
They already seem overanxious about their blood pressure, she said, adding, “I encourage them to go out and enjoy themselves.”
“Take a class! Go to a museum!” she said. “You can’t do that if you’re at home taking your blood pressure five times a day.”
While trials and guidelines address benefits for the population as a whole — even small reductions in dementia would have an enormous impact — they are not useful for predicting individual outcomes. The , used to gauge whether someone would see cardiovascular benefit from hypertension treatment, has not been validated for people over 79 and does not factor in cognitive benefits, Supiano noted.
For people with other serious illnesses — cancer patients or frail nursing home residents with dementia, for instance — controlling blood pressure may be far down the list of concerns.
Time is also a factor in weighing risks versus benefits. A meta-analysis of older patients by Sei Lee, a geriatrician at UCSF, and colleagues found that for 200 patients in intensive treatment for hypertension, it would .
Reducing very high blood pressure is simpler and more important than trying to lower a 130 reading to below 120, Lee added. “You’d have to work a lot harder, add a third or fourth medication, and the risk of side effects is higher.”
Supiano’s 78-year-old patient did hit that target and did well for six or seven years. Then, as happens with many patients with mild cognitive impairment, she began to decline and eventually received an Alzheimer’s diagnosis.
Given what researchers are reporting about the cognitive benefits of treating high blood pressure, “maybe it gave her another couple of good years,” he mused. “Maybe it delayed the progression.” Or maybe, he added, he should have started intensive treatment earlier.
The New Old Age is produced through a partnership with .
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/aging/high-blood-pressure-hypertension-dementia-risks-new-old-age/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2169388&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Within a few days, Reynolds became so desperate that she and her husband had to physically restrain Jonah, dumping pain medication down his throat as he screamed in pain.
“It broke our hearts,” said Reynolds, who lived in Georgetown, Kentucky, at the time. “And I remember just thinking that it shouldn’t have to come to that.”
Reynolds couldn’t find a dentist with an opening who could treat Jonah, who is autistic and often resists dental exams due to hypersensitivity and anxiety. Over the course of five days, Reynolds took Jonah twice to a nearby emergency room as he struggled with persistent pain and a fever due to a likely infected tooth with an exposed nerve. The ER had no dentists; both times, the family was sent home with only pain medication and an ice pack.
Across the nation, more children are entering ERs for preventable tooth problems. Dentists, hygienists, and researchers attributed that trend to a shortage of pediatric dental care professionals in and worsening oral hygiene since the covid-19 pandemic. Tens of thousands of kids end up in the hospital for dental emergencies each year, according to Melissa Burroughs, senior director of policy and advocacy at the national health nonprofit CareQuest Institute for Oral Health.
ER visits for tooth problems unrelated to physical injuries for children under 15 years old from 2019 to 2022, according to a report released late last year by CareQuest. And local data reflects that national trend: At Children’s Hospital Colorado in the Denver area, nontraumatic dental cases, such as cavities or gum infections, in its ER increased 175% from 2010 to 2025, according to hospital spokesperson Sarah Bonar. In Kentucky, where Jonah lives, children’s visits to the ER for dental problems rose 72% from 2020 to 2024, according to the state.
Policy changes under the Trump administration are poised to worsen the trend. President Donald Trump’s 2025 federal budget reconciliation law, known as the One Big Beautiful Bill Act, called for billions in cuts from Medicaid, which may force states to limit or drop dental coverage from the public insurance program for those with low incomes or disabilities. New eligibility requirements for Medicaid in some states could affect kids’ access to dental care, even though children are guaranteed dental coverage under the program. Research shows that when parents lose Medicaid, even kids with coverage are more likely to have and to go to a dentist.
The Trump administration has also promoted skepticism about fluoride. show that fluoride in drinking water and topical fluoride treatments dramatically reduce tooth decay and prevent cavities. In recent months, the Food and Drug Administration against the use of fluoride supplements and the Environmental Protection Agency of “potential health risks of fluoride in drinking water.” Health and Human Services Secretary Robert F. Kennedy Jr. has called fluoride a “” and “.” A 2025 study in JAMA Pediatrics linked high levels of fluoride with lower IQ in children ‚Äî but only at concentrations the recommended level in public drinking water.
, a pediatric dentist at the University of Washington who studies fluoride hesitancy, worries that these anti-fluoride stances will further erode trust in fluoride treatment. Since the start of 2026, lawmakers in at least 15 states have introduced bills prohibiting or limiting fluoride in public drinking water. Utah and Florida in 2025 became the first states to enact fluoride bans.
“Will that have an effect on cavity rates?” Chi asked. “Absolutely.”
Severe Dental Cases Rise
Pediatric dentists Katherine Chin and Chaitanya Puranik said they are treating more patients like Jonah at Children’s Hospital Colorado. More severe cases have become more common, too. Puranik said he used to typically see patients with only one cavity, but now his patients are often coming in with tooth decay throughout their mouth.
During the pandemic, many dental offices , and studies show children also increased , a major risk factor for cavities. Severe cavities that lead to tooth extraction can affect , sometimes causing long-term problems with or .
Millions of people live in in the U.S., with scant dentists within driving distance. On top of that, only treat Medicaid patients, due to low reimbursement rates, which are on average of their typical dental charges, according to the American Dental Association.
Children with intellectual or developmental disabilities may especially struggle to access quality dental care. Few general dentists have sufficient pediatric training to care for kids with disabilities such as Jonah, who are easily overwhelmed or need to be sedated for an exam, , a health information nonprofit that includes ∫⁄¡œ≥‘πœÕ¯ News. Over have special health care needs, and those children are to have unmet dental needs. Their parents are also to finding a dentist.
When he was younger, Jonah would not let his parents brush his teeth, which led to cavities in his baby teeth, his mother said. After Jonah’s first visit to the ER, Reynolds found a general dentist with an opening. But unlike a trained pediatric dentist, she said, the dentist did not know how to examine Jonah in a way he could tolerate and wasn’t prepared to provide sedation. Jonah left without treatment and was soon back in the ER when his fever returned.
ERs Rarely Provide Solutions
, a pediatrician in Washington County, Maine, said he is fielding “the most horrifying cavities” at Down East Community Hospital.
ERs are often ill-equipped to treat dental concerns, Weitz said. Similar to the ER Jonah went to in Kentucky, Down East has no dentists on staff. Weitz often finds himself prescribing antibiotics as a temporary measure.
“But a month later, they’re back again because it’s flaring up again,” Weitz said.
As a potential solution, states such as Maine and Alaska are proposing to use money from the $50 billion to develop the oral health workforce or to create specialized dental care centers, which can better serve children with special health care needs on short notice. But those initiatives won’t address the loss of coverage anticipated from Medicaid cuts. California last year in state grants to develop or expand over 120 dental facilities to serve patients with special health care needs.
Jonah’s dental emergency cost Reynolds a week of work from her job as a dog groomer and Jonah three days of third grade, plus hundreds of dollars in out-of-pocket costs.


Eventually, Reynolds found an oral surgeon who extracted the tooth. But even that went poorly, she said. When Jonah became upset over a needle stick, the surgeon threatened to hold him down, Reynolds said. She said the surgeon left quickly after the procedure and never gave her a clear diagnosis of what caused Jonah’s pain. The procedure did resolve his toothache, but Reynolds said more professionals should know how to handle cases like Jonah’s, with sensitivity to the families. Four years later, forcing Jonah to take his pain meds still lives fresh in her memory.
“That will never leave my mind,” Reynolds said.
This <a target="_blank" href="/public-health/dental-care-emergency-rooms-special-needs-medicaid-shortage-areas/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2162392&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The boys sat in one waiting room and then another. Two hours and 20 minutes passed before the two were isolated, according to obtained by ∫⁄¡œ≥‘πœÕ¯ News. Then two more hours ticked by.
As the sun rose, an emergency room doctor called the state epidemiologist and described the symptoms. The public health official told him to keep the kids in the hospital and quarantine them. Shortly after that call, the patients were diagnosed.
It was measles.
Hospital staff gave the father instructions on how to quarantine the family and sent them home.
The virus exposed at least 26 other people in the hospital that January day, federal investigators determined. Health inspectors for CMS investigated the measles infections and other failures in care and concluded that the twins’ symptoms should have triggered an isolation procedure for which Mission Hospital staffers had trained seven months earlier. CMS designated Mission in “” for the exposures and other unrelated issues, one of the most severe sanctions a hospital can face, threatening to pull federal funding unless it remedied the problems.
A spokesperson for Mission said its staff was trained to manage airborne sickness and is following federal rules.
As U.S. hospitals face an increasing risk of encountering measles, and pressure to immediately spot it, health care workers face an unusual barrier: Many don’t know what it looks like.
“There’s a word, ‚Äòmorbilliform’ ‚Äî it means measles-like, and there are lots of viruses that can cause a rash that looks like a measles rash in children,” said Theresa Flynn, a pediatrician in Raleigh and the president of the North Carolina Pediatric Society. In 30 years in health care, she’s never seen a measles case, she said.
North Carolina has reported more than 20 cases since mid-December, and more than 3,000 people nationwide have been infected since the beginning of 2025.
Children in areas with low immunization rates to outbreaks, triggering public health campaigns to promote the measles vaccine. CMS Administrator Mehmet Oz encouraged vaccination in a .
, mumps, and rubella vaccine, a person has a 3% chance of getting the virus after exposure. If exposed, an unvaccinated person has a 90% chance of being infected, according to the CDC. It can take a week or two before someone infected with measles shows symptoms.
But for the past year, the Trump administration has . Health and Human Services Secretary Robert F. Kennedy Jr. was a longtime anti-vaccine activist before taking office, and under his leadership the Centers for Disease Control and Prevention has reduced the number of shots recommended to children.
After measles erupted in West Texas last year, Kennedy publicly for the virus, including steroids, antibiotics, and cod liver oil.
Infectious disease experts and doctors said federal policies have left health care workers to lean on their own experience or guidance from their state public health systems to fight a disease that many are preparing to see for the first time and that initially may behave like the common cold.
“As measles becomes more common, all of us are leveling up in our ability to recognize and immediately respond to suspected measles,” Flynn said.
Three C’s
Officially, the U.S. has maintained “measles elimination status” since 2000, meaning the U.S. has avoided significant spread of the virus. After outbreaks in Texas, Arizona, Utah, and now South Carolina, the nation is on track to lose that designation before the year is out. tie elimination status to a lack of a continuous viral spread persisting for 12 months.
One county in South Carolina, an hour’s drive from Asheville, has had in the current outbreak ‚Äî more than Texas reported in all of 2025.
Symptoms of measles, a virus that , can include fever, cough, a blotchy rash, and red, watery eyes. Researchers consider measles among the most contagious diseases, and the virus may remain active for up to two hours after an infected person leaves a room.
It can be lethal, with .
In 2025, two children in Texas and one adult in New Mexico died of measles.
Along with tracking data, the CDC on its website for diagnosing measles. State public health agencies and some counties have developed dashboards tracing the disease as it surfaces in such places as hospitals, schools, grocery stores, and airports. Large hospital systems developed staff training protocols last year and shared them with area clinics.
Look for the three C’s, : cough, coryza (cold symptoms), and conjunctivitis (pink eye). According to CMS inspection records, HCA Healthcare, which owns Mission Hospital, trained Mission staff on the three C’s early last year. On top of failing to isolate the twin patients right away, Mission staff didn’t have a designated area for patients with respiratory symptoms, federal inspectors found.
The CDC advises health workers to immediately place patients with measles or suspicious symptoms in a special isolation room, where airflow is controlled inward. The Mission patients were separated from other patients only by plastic partitions, according to the CMS records.
Mission spokesperson Nancy Lindell said the hospital was equipped and staffed to manage airborne illnesses like measles.
“Our hospital has been working with state and federal health officials on proactive preparedness, and we are following guidance provided by the CDC,” Lindell said.
(Dogwood Health Trust, a private foundation established as part of HCA’s purchase of Mission Health, helps fund ∫⁄¡œ≥‘πœÕ¯ News coverage.)
Most U.S. clinics and hospitals have never experienced measles cases, said Patsy Stinchfield, a former president of the National Foundation for Infectious Diseases and a nurse practitioner. She called CMS’ Immediate Jeopardy penalty for Mission “extreme,” given the virus can be so difficult to identify.
“In the middle of winter right now, measles looks like every other viral respiratory infection that kids come in with,” Stinchfield said.
The CDC has been less communicative in the past year with clinics about their response to outbreaks, said health workers and infectious disease experts. This disconnect began soon after Trump took office, according to a ∫⁄¡œ≥‘πœÕ¯ News investigation finding that health officials in West Texas were unable to talk with CDC scientists as measles surged last February and March.
“We certainly do not feel the support or guidance from the CDC right now,” said Brigette Fogleman, a pediatrician at Asheville Children’s Medical Center, where staff members have come up with their own method of staving off the virus: screening patients over the phone and in their cars before a visit.
In response to questions about how the CDC is supporting health care organizations during the measles resurgence, spokesperson Andrew Nixon said that “state and local health departments have the lead in investigating measles cases and outbreaks” and that the CDC provides support “as requested.” He pointed to numerous guides and simulation tools the agency has developed as the virus has spread.
Jennifer Nuzzo, an epidemiologist and director of the Pandemic Center at Brown University, acknowledged that diagnosing measles is a major challenge, emphasizing that coordination among public health agencies is critical in overcoming that challenge.
Stinchfield attributed the spread of measles to CDC leaders’ lack of communication to clinics and to the public ‚Äî no ads on buses, no social media campaigns, no sense of urgency. “When you are at the highest level of measles cases in 30 years, we should be seeing lots more from our federal government,” Stinchfield said. “And I think it’s harming kids and causing an inordinate amount of work and expense that really doesn’t belong in health care right now.”
State Prepares for More Measles Cases
In North Carolina’s Buncombe County, home to Asheville and Mission Hospital, health officials had counted seven measles cases by mid-February and anticipated many more, according to state epidemiologist Zack Moore. It’s unclear how many of those are connected to the Mission exposure.
“We are preparing for a future in which we follow a trajectory like South Carolina,” Moore said, “where we see sort of a gradual accumulation of cases, and then all of a sudden it reaches kind of a tipping point, and we see a more explosive growth in the outbreak and spread across the state.”
Fogleman, who is also a pediatrician, and Buncombe health department director Jennifer Mullendore spoke during a hosted by the county, urging families to get their children vaccinated, debunking vaccine misinformation, and updating parents on local case numbers.
Days before, a local private school had quarantined about 100 students after an exposure. were immunized, according to state data.
At Fogleman’s clinic, parents are asked to wait in their vehicles with their children, and staffers come out to screen them there. Some parents resist vaccination and note recently weakened federal recommendations around measles vaccines , she said.
Kennedy handpicked the committee members who made those recommendations, with several members having spread medical misinformation in the past.
One parent recently told a nurse, “It’s only measles. It doesn’t kill anybody,” Fogleman said.
That’s not true, her team must explain.
As the clinic holds families in the parking lot, trying to figure out whether symptoms point to the dangerous virus, it’s difficult to get the message across, Fogleman said, especially when the nation’s top disease agency hasn’t conducted a widespread information campaign about the risks from measles ‚Äî or the vaccine’s ability to almost entirely prevent it.
“We can’t change the past,” Fogleman said. “All we can do is try to educate and move forward.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/measles-outbreak-cdc-carolina-sc-nc-vaccines/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2159986&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Warning patients could deter them from signing up for a program called Emergency Medicaid, through which the government reimburses hospitals for the cost of emergency treatment for immigrants who are ineligible for standard Medicaid coverage.
But if hospitals don’t disclose that the patients’ information is shared with federal law enforcement, they might not know that their medical coverage puts them at risk of being located by Immigration and Customs Enforcement.
“If hospitals tell people that their Emergency Medicaid information will be shared with ICE, it is foreseeable that many immigrants would simply stop getting emergency medical treatment,” said , a research professor at Georgetown University’s Center for Children and Families. “Half of the Emergency Medicaid cases are for the delivery of U.S. citizen babies. Do we want these mothers avoiding the hospital when they go into labor?”
For more than a decade, hospitals and states have assured patients that their personal information, including their home addresses and immigration status, would not be shared with immigration enforcement officials when they apply for federal health care coverage. guaranteed the agency would not use information from health coverage applications for enforcement activities.
But that changed last year, after President Donald Trump returned to the White House and ordered one of the most aggressive immigration crackdowns in recent history. His administration began funneling data from a variety of government agencies to the Department of Homeland Security, including filed with the IRS.
The Centers for Medicare & Medicaid Services, part of the Department of Health and Human Services, agreed last spring to give ICE officials direct access to a Medicaid database that includes enrollees’ addresses and citizenship status.
Twenty-two states, all but one led by Democratic governors, the Medicaid data-sharing agreement, which the administration did not formally announce until a federal judge ordered it to do so last summer. The judge that in those states, ICE could access information in the Medicaid database only about people in the country unlawfully. ∫⁄¡œ≥‘πœÕ¯ News contacted more than a dozen hospitals and hospital associations in states and cities that have been targets of ICE sweeps. Many declined to comment on whether they’ve updated their disclosure policies after the ruling.
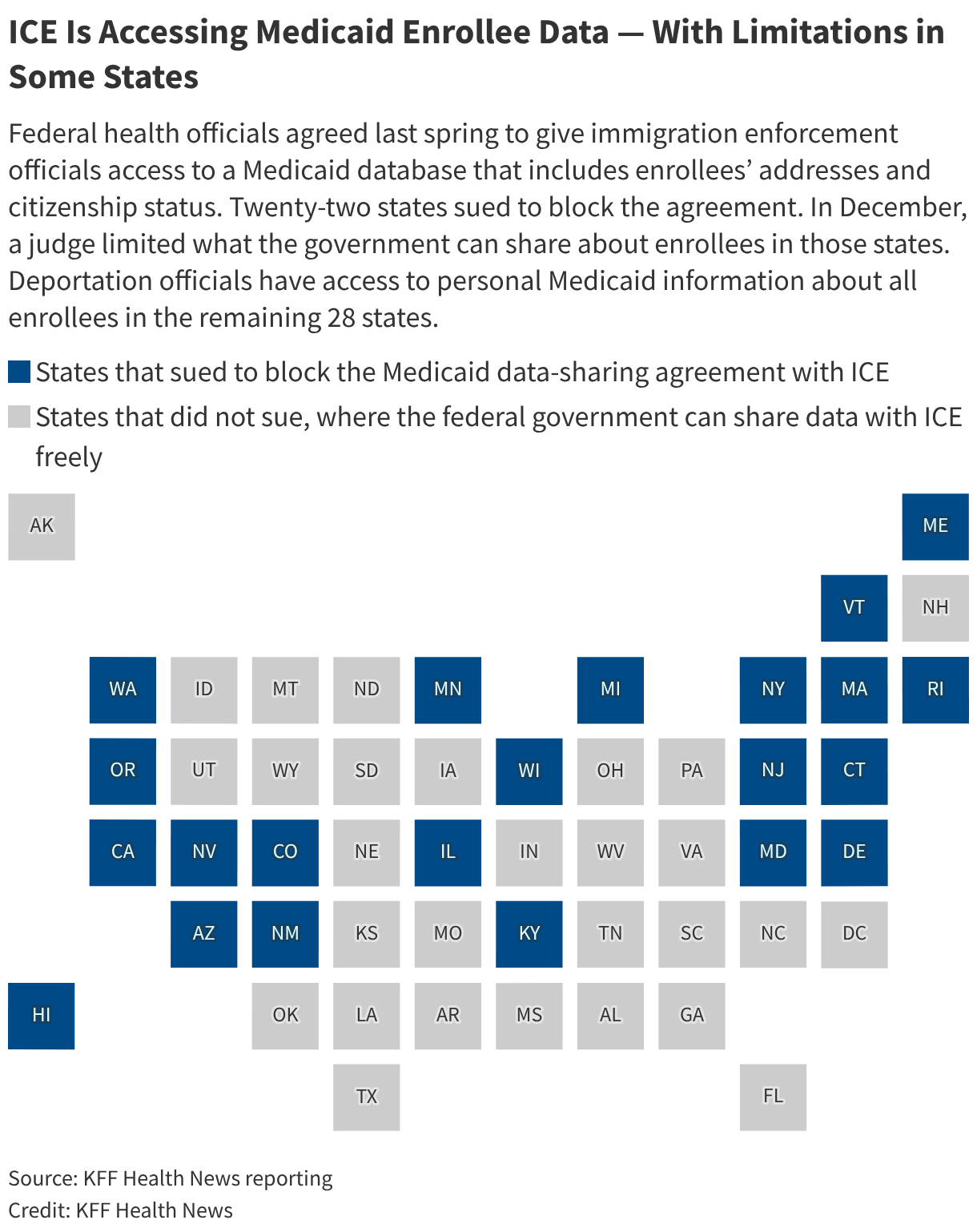
Of those that responded, none said they are directly warning patients that their personal information may be shared with ICE when they apply for Medicaid coverage.
“We do not provide legal advice about federal government data-sharing between agencies,” Aimee Jordon, a spokesperson for M Health Fairview, a Minneapolis-based hospital system, said in an email to ∫⁄¡œ≥‘πœÕ¯ News. “We encourage patients with questions about benefits or immigration-related concerns to seek guidance from appropriate state resources and qualified legal counsel.”
Information on Applications
Some states’ Emergency Medicaid applications specifically ask for a patient’s immigration status — and still assure people that their information will be kept secure and out of the hands of immigration enforcement officials.
For example, as of Feb. 3, California’s application still included language advising applicants that their immigration information is “confidential.”
“We only use it to see if you qualify for health insurance,” states the 44-page form, which the state’s Medicaid program, known as Medi-Cal, in January.
California Department of Health Care Services spokesperson Anthony Cava said in a statement that the agency, which oversees Medi-Cal, will “ensure that Californians have accurate information on the privacy of their data, including by revising additional publications as necessary.”
Until late January, Utah’s Medicaid website also claimed its Emergency Medicaid program did not share its information with immigration officials. After ∫⁄¡œ≥‘πœÕ¯ News contacted the state agency, Kolbi Young, a spokesperson, said Jan. 23 that the language would be taken down immediately. It was removed that day.
Oregon Health & Science University, a hospital system based in Portland, offers immigrant patients developed by the state Medicaid program for those with concerns about how their information might be used. The document does not directly say that Medicaid enrollees’ information is shared with ICE officials.
Hospitals rely on Emergency Medicaid to reimburse them for treating people who would qualify for Medicaid if not for their citizenship status — those in the country illegally and lawfully present immigrants, such as those with a student or work visa. The coverage pays only for emergency medical and pregnancy care. Typically, hospital representatives help patients apply while they are still in the medical facility.
The main Medicaid program, which covers a much broader range of services for over 77 million low-income and disabled people, does not cover people living in the country illegally.
Examining Emergency Medicaid enrollment is the most obvious way, then, for deportation officials to identify immigrants, including those who might not reside in the U.S. lawfully.
HHS spokesperson Rich Danker said in an email that CMS — which oversees Medicaid, a joint state-federal program — is sharing data with ICE after the judge’s ruling. But he would not answer how the agency is ensuring it is sharing information only on people who are not lawfully present, as the judge required.
With ICE now getting direct access to the personal information of millions of Medicaid enrollees, hospitals — while “definitely in a tough position” — should be up-front about the changes, said Sarah Grusin, at the National Health Law Program, an advocacy group.
“They need to be telling people that the judge has permitted sharing of information, including their address, for people who are not lawfully residing,” she said. “Once this information is submitted, you can’t protect it from disclosure at this point.”
Grusin said she advises families to weigh the importance of seeking medical care against the risk of having their information shared with ICE.
“We want to give candid, honest information even if it means the decision people have to make is really hard,” she said.
Those who have previously enrolled in Medicaid or can easily search their address online should assume that immigration officials already have their information, she added.
Emergency Medicaid
Emergency Medicaid coverage was established in the mid-1980s, when a federal law began requiring hospitals to treat and stabilize all patients who show up at their doors with a life-threatening condition.
Federal government spending on Emergency Medicaid accounted for nearly $4 billion in 2023, or of total federal spending on Medicaid.
States send monthly reports to the federal government with detailed information about who enrolls in Medicaid and what services they receive. The judge’s ruling in December limited what CMS can share with ICE to only basic information, including addresses, about Medicaid enrollees in the 22 states that sued over the data-sharing arrangement. ICE officials are not supposed to access information about the medical services people receive, per the judge’s order.
The judge also prohibited the agency from sharing the data of U.S. citizens or lawfully present immigrants from those states.
Deportation officials have access to personal Medicaid information of all enrollees in the remaining 28 states.
The federal health agency has not clarified how it is ensuring that certain states’ information on citizens and legal residents is not shared with ICE. But Medicaid experts say it would be nearly impossible for the agency to separate the data, raising questions about whether the Trump administration is complying with the judge’s order.
The Trump administration’s efforts to deport immigrants living in the country illegally have had implications on immigrant families seeking care. About a third of adult immigrants reported skipping or postponing health care in the past year, according to a released in November. (KFF is a health information nonprofit that includes ∫⁄¡œ≥‘πœÕ¯ News.)
Bethany Pray, the chief legal and policy officer at the Colorado Center on Law and Policy, warned that sharing Medicaid data directly with deportation officials will force even tougher decisions upon some families.
“This is very concerning,” Pray said. “People should not have to choose between giving birth in a hospital and wondering if that means they risk deportation.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/ice-immigrants-medicaid-data-sharing-hospitals-states-deportation/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2151281&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>“It’s just the cost of doing business with our borders being somewhat porous for global and international travel,” Abraham said. “We have these communities that choose to be unvaccinated. That’s their personal freedom.”
Infections from other countries, however, accounted for only of measles cases detected since Jan. 20, 2025, the official start of the deadly measles outbreak in West Texas, which spread to other states and Mexico. The rest were acquired domestically. This marks a change since the U.S. eliminated measles in 2000. Measles occasionally popped up in the U.S. from people infected abroad, but the cases rarely sparked outbreaks, because of extremely high rates of vaccination. Two doses of the measles, mumps, and rubella vaccine strongly prevent infection and halt the virus’s spread.
To maintain its measles elimination status, the U.S. must prove that the virus has not circulated continuously in the nation for a year, between Jan. 20, 2025, and Jan. 20, 2026. To answer the question, scientists are examining whether the major outbreaks in South Carolina, Utah, Arizona, and Texas were linked.
Health officials confirmed that the main measles virus strain in each of these outbreaks is D8-9171. But because this strain also occurs in Canada and Mexico, CDC scientists are now analyzing the entire genomes of measles viruses — about 16,000 genetic letters long — to see whether those in the United States are more closely related to one another than to those in other countries.
The CDC expects to complete its studies within a couple of months and make the data public. Then the Pan American Health Organization, which oversees the Americas in partnership with the World Health Organization, will decide whether the U.S. will lose its measles elimination status. And that would mean that potentially deadly, and preventable measles outbreaks could become common again.
“When you hear somebody like Abraham say ‚Äòthe cost of doing business,’ how can you be more callous,” said pediatrician and vaccine specialist Paul Offit, in an hosted by the health blog on Jan. 20. “Three people died of measles last year in this country,” Offit added. “We eliminated this virus in the year 2000 ‚Äî eliminated it. Eliminated circulation of the most contagious human infection. That was something to be proud of.”
Abraham said vaccination remains the most effective way to prevent measles but that parents must have the freedom to decide whether to vaccinate their children. Several states have loosened school vaccine requirements since 2020, and vaccine rates . A record rate of kindergartners, representing about obtained vaccine exemptions for the 2024-25 school year.
Information on vaccines has been muddied by Health and Human Services Secretary Robert F. Kennedy Jr., who previously founded an anti-vaccine organization. He has undermined vaccines throughout his tenure. On national television, he has repeated scientifically debunked rumors that vaccines may cause autism, .
Jennifer Nuzzo, director of the Pandemic Center at Brown University, disparaged the Trump administration’s focus on finding genetic technicalities that may spare the country’s measles-free status. “This is the wrong thing to pay attention to. Our attention has to be on stopping the outbreaks,” she said.
“If we keep our status, it should be because we have stopped the spread of measles,” she said. “It’s like they’re trying to be graded on a curve.”
The Trump administration impeded the CDC’s ability to assist West Texas during the first critical weeks of its outbreak and slowed the release of federal emergency funds, according to ∫⁄¡œ≥‘πœÕ¯ News investigations. However, the agency stepped up its activity last year, providing local health departments with measles vaccines, communication materials, and testing. Abraham said HHS would give South Carolina $1.5 million to respond to its outbreak, which began nearly four months ago and had reached 646 cases as of Jan. 20.
If the CDC’s genomic analyses show that last year’s outbreaks resulted from separate introductions from abroad, political appointees will probably credit Kennedy for saving the country’s status, said Demetre Daskalakis, a former director of the CDC’s national immunization center, who resigned in protest of Kennedy’s actions in August.
And if studies suggest the outbreaks are linked, Daskalakis predicted, the administration will cast doubt on the findings and downplay the reversal of the country’s status: “They’ll say, who cares.”
Indeed, at the briefing, Abraham told a that a reversal in the nation’s status would not be significant: “Losing elimination status does not mean that the measles would be widespread.”
Data shows otherwise. Case counts last year were the highest since 1991, before the government enacted vaccine policies to ensure that all children could be protected with measles immunization.
Lauren Sausser contributed reporting.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/measles-free-status-us-cdc-ralph-abraham-paho-who-outbreaks-vaccines/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2145407&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Then 25 years old and six months pregnant, she drove herself to the emergency room in Ronan, Montana, on the Flathead Indian Reservation, where an ambulance transferred her to a larger hospital 60 miles away in Missoula. Once she arrived, the staff couldn’t detect her baby’s heartbeat. Swaney began to bleed heavily. She delivered a stillborn baby and was hospitalized for several days. At one point, doctors told her to call her family. They didn’t expect her to survive.
“It certainly changed my life ‚Äî the experience ‚Äî but my life has not been a bad life,” she told ∫⁄¡œ≥‘πœÕ¯ News.
Though her experiences were nearly 50 years ago, Swaney, a member of the Confederated Salish and Kootenai Tribes, said Native Americans continue to receive inadequate maternal care. The data appears to support that belief.
In 2024, the most recent year for which data for the population is available, Native American and Alaska Native people had the among major demographic groups, according to the Centers for Disease Control and Prevention.
In response to this disparity, Native organizations, the CDC, and some states are working to boost tribal participation in state maternal mortality review committees to better track and address pregnancy-related deaths in their communities. Native organizations are also considering ways tribes could create their own committees.
State maternal mortality review committees investigate deaths that occur during pregnancy or within a year after pregnancy, analyze data, and issue policy recommendations to lower death rates.
According to 2021 CDC data, compiled from 46 maternal mortality review committees, 87% of maternal deaths in the U.S. were deemed preventable. Committees reported that , deaths among Native American and Alaska Native people were considered preventable.
Our matriarchs, our moms, are what carries a nation forward.
Kim Moore-Salas
State committees have received federal money through the Preventing Maternal Deaths Act, which President Donald Trump signed in 2018.
But the money is scheduled to dry up on Jan. 31, when the short-term spending bill that ended the government shutdown expires.
Funding for the committees is included in the Labor, Health and Human Services, Education, and Related Agencies for fiscal year 2026. That bill must be approved by the House, Senate, and president to take effect.
Native American leaders said including members of their communities in maternal mortality review committee activities is an important step in addressing mortality disparities.
In 2023, tribal leaders and federal officials met to discuss four models: a mortality review committee for each tribe, a committee for each of the 12 Indian Health Service administrative regions, a national committee to review all Native American maternal deaths, and the addition of Native American subcommittees to state committees.
Whatever the model, tribal sovereignty, experience, and traditional knowledge are important factors, said Kim Moore-Salas, a co-chair of the Arizona Maternal Mortality Review Committee. She’s also the chairperson of the panel’s American Indian/Alaska Native mortality review subcommittee and a member of the Navajo Nation.
“Our matriarchs, our moms, are what carries a nation forward,” she said.
Mental health conditions and infection were the leading underlying causes of pregnancy-related death among Native American and Alaska Native women as of 2021, according to the CDC report analyzing data from 46 states.
The CDC found an estimated 68% of pregnancy-related deaths among Native American and Alaska Native people happened within a week of delivery to a year postpartum. The majority of those happened between 43 days and a year after birth.
The federal government has a responsibility under signed treaties to provide health care to the 575 federally recognized tribes in the U.S. through the Indian Health Service. Tribal members can receive limited services at no cost, but the agency is underfunded and understaffed.
A that analyzed data from 2016 to 2020 found that approximately 75% of Native American and Alaska Native pregnant people didn’t have access to care through the Indian Health Service around the time of giving birth, meaning many likely sought care elsewhere. More than 90% of Native American and Alaska Native births occur outside of IHS facilities, . For those who did deliver at IHS facilities, a from the Department of Health and Human Services’ Office of Inspector General found that 56% of labor and delivery patients received care that did not follow national clinical guidelines.
The 2024 study’s authors also found that members of the population were less likely to have stable insurance coverage and more likely to have a lapse in coverage during the period close to birth than non-Hispanic white people.
Cindy Gamble, who is Tlingit and a tribal community health consultant for the American Indian Health Commission in Washington, has been a member of the state’s maternal mortality review panel for about eight years. In the time she’s been on the state panel, she said, its composition has broadened to include more people of color and community members.
The panel also began to include suicide, overdose, and homicide deaths in its data analysis and added racism and discrimination to the risk factors considered during its case review process.
Solutions need to be tailored to the tribe’s identity and needs, Gamble said.
“It’s not a one-size-fits-all,” Gamble said, “because of all the beliefs and different cultures and languages that different tribes have.”
Gamble’s tenure on the state committee is distinctive. Few states have tribal representation on maternal mortality review committees, according to the National Indian Health Board, a nonprofit organization that advocates for tribal health.
The National Council of Urban Indian Health is also the participation of Urban Indian health organizations, which provide care for Native American people who live outside of reservations, in state maternal mortality review processes. As of 2025, the council had connected Urban Indian health organizations to state review committees in California, Kansas, Oklahoma, and South Dakota.
Native leaders such as Moore-Salas find the current efforts encouraging.
“It shows that state and tribes can work together,” she said.
In March 2024, Moore-Salas became the first Native American co-chair of Arizona’s Maternal Mortality Review Committee. In 2025 she and other Native American members of the committee developed guidelines for the American Indian/Alaska Native subcommittee and reviewed the group’s first cases.
The subcommittee is exploring ways to make the data collection and analysis process more culturally relevant to their population, Moore-Salas said.
But it takes time for policy changes to create widespread change in the health of a population, Gamble said. Despite efforts around the country, other factors may hinder the pace of progress. For example, maternity care deserts are growing nationally, caused by rapid hospital and labor and delivery unit closures. Health experts have raised concerns that upcoming cuts to Medicaid will hasten these closures.
Despite her experience and the ongoing crisis among Native American and Alaska Native people, Swaney hopes for change.
She had a second complicated pregnancy soon after her stillbirth. She went into labor about three months early, and the doctors said her son wouldn’t live to the next morning. But he did, and he was transferred about 525 miles away from Missoula to the nearest advanced neonatal unit, in Salt Lake City.
Her son, Kelly Camel, is now 48. He has severe cerebral palsy and profound deafness. He lives alone but has caregivers to help with cooking and other tasks, said Swaney, 73.
He “has a good sense of humor. He’s kind to other people. We couldn’t ask for a more complete child.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/native-american-pregnancy-maternal-mortality-mothers-deaths-tribes/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2137280&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Residents share rooms designed to be accessible to those with mobility issues. There are also private bathrooms, which are a big deal for seniors struggling with incontinence.
Unlike the MVP, most homeless shelters aren’t equipped to help seniors, especially those 65 and older. They are the fastest-growing homeless population nationwide, according to , a researcher at the University of Pennsylvania. Not only are people who struggle with chronic homelessness aging, but many seniors are becoming homeless for the first time in their lives.
Getting in and out of bunks, managing medications, and making it to a shared bathroom in time are among the major challenges of shelter life for older adults. Staff at traditional shelters sometimes ask seniors to leave if they’re unable to care for themselves.
The MVP is unusual among shelters because it provides on-site medical care to better serve its residents as they age.
Last spring, Jamie Mangum, who is in her 50s and has lung cancer, tripped and fell in her room. To visit with an emergency medical technician, she needed only to make it downstairs. Her swollen wrist was quickly wrapped, and she returned to her room. She said that wouldn’t have been possible at other shelters she’s stayed in.
“There, I’d have to wait hours as opposed to come in here, be seen,” Mangum said.
Mangum said that in other shelters she’d likely have had to find her own way to an urgent care office or get an ambulance ride. Specialized case managers at the MVP have helped her get treatment for lung cancer as well.
“We have clients that need memory care. Maybe they were living independently before, but they were unable to maintain that and got evicted due to dementia or different things like that,” said Baleigh Dellos, who manages the MVP shelter for , a local nonprofit.
Specialized medical case managers work at the shelter. Primary care doctors and therapists visit weekly. Residents can even receive physical therapy in private spaces on-site.

A Path to Stability
The MVP partnered with the to offer medical care.
The first thing most new residents need help with is medication, said Matt Haroldsen with the Fourth Street Clinic, which provides health services at the shelter.
For people living on the streets, just keeping hold of regular medications is a challenge. “Their medications get jacked when they’re in their camps,” he said.
Diabetes patients without homes often bury their insulin to keep it cold. Haroldsen said they might forget where they buried it, or the vials might get too warm and spoil.
Helping residents at the shelter get those medications can stabilize their conditions, allowing them to focus on other priorities, such as getting an ID and other documents they need to apply for disability, Social Security, and various programs that can help them secure housing.
Nonprofits and local governments have opened similar shelters in Florida, California, and Arizona to meet the needs of older unhoused adults.
Having access to specialized shelters can be the difference between life and death, said , assistant director of the National Health Care for the Homeless Council.
In cold-weather states, denying seniors a bed because of mobility and other health issues can be especially risky. In 2022, a Bozeman, Montana, after he was asked to leave a shelter because of incontinence.
Complex medical needs can pose a danger to other residents that most shelters aren’t prepared to manage.
“A typical shelter doesn’t allow somebody on oxygen to come in because that’s such a fire hazard and risk,” she said.
Synovec said giving seniors better access to health care inside shelters is the best way to help them succeed once they get housing. Health issues are a common reason seniors can’t afford or maintain housing, she said.
A Growing Model
The MVP model is showing promise, both in Utah and elsewhere.
“Over 80% of the people who’ve stayed in our program this past year have moved into stable or permanent housing,” said , vice president of programs for the TaskForce for Ending Homelessness in Fort Lauderdale, Florida. The nonprofit runs a shelter called .
The MVP shelter near Salt Lake City is also marking success. It was able to permanently house 36 seniors as of late last year.
Still, there are more seniors in need of shelter than it can accommodate. Dellos, the shelter’s manager, said the MVP’s waitlist hovers around 200 people. She said the shelter prioritizes people based on medical need, not time spent on the waitlist.
For residents who do get a room, it’s life-changing.
Last spring, 62-year-old Jeff Gregg was playing fetch with his dog, Ruffy, just beyond the lawn in front of the MVP.
An old back injury forced Gregg to hunch over as he threw the ball. It also fueled a decades-long addiction to opioids. That cycle was hard to escape, he said.

“Fighting that, having a job, insurance, then losing the job, not having insurance, going out to the streets and being back in that crap, and I’d be back in the same position,” he said.
Gregg said sobriety took a back seat to more immediate needs like finding food and a bed in a shelter. He said the MVP was the first place where he could relax and focus on recovery.
“I was able to get clean. It took me a couple months, but I just kept plucking away,” he said.
He said the experience paved the way for him to get back surgery. He hopes that with less back pain, he can eventually get a job to help him afford an apartment.
This article is part of a partnership with and .
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/aging/homeless-shelters-older-adults-medical-care-utah-florida/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2131252&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But in the upside-down world of Health and Human Services Secretary Robert F. Kennedy Jr., vaccines are on the ropes. A vaccine committee dominated by skeptics he chose for the panel voted 8-to-3 Friday to end a 34-year recommendation to inoculate newborns against hepatitis B, a practice that helped reduce childhood infections of the virus by 99%, from around 16,000 in 1991 to only seven in 2023.
While the committee went about its deliberations, the peril of abandoning vaccines was plain to see. The country’s worst year since 1992 for measles ‚Äî an entirely vaccine-preventable illness ‚Äî continued with flare-ups in Utah, Arizona, and South Carolina. A two-year outbreak of whooping cough, which vaccines can also check, has caused about 60,000 reported cases ‚Äî including at least six infant deaths.
But neither of those diseases was discussed on the first day of the meeting by members of the Advisory Committee on Immunization Practices. The panel’s chartered purpose is to determine vaccination policies to counter such risks, but under Kennedy, it has focused on responding to doubts from vaccine skeptics and opponents.
Like previous gatherings of the committee, which was handpicked by Kennedy after he fired the panel’s 17 incumbent experts in June, the session was chaotically at odds with past practices of the Centers for Disease Control and Prevention. Kennedy has described the agency as a “cesspool of corruption.”
The committee’s chair, epidemiologist Martin Kulldorff, left three days before the meeting and was named to a senior HHS position. His successor, Kirk Milhoan, a pediatric cardiologist who that the mRNA technology used to make covid vaccines is “the biggest threat to humanity,” was on a plane or in Asia for most of the meeting, leaving Vice Chair Robert Malone holding the reins. Malone opposes vaccine mandates and became a darling of the anti-vaccine movement when he told podcast host Joe Rogan in 2021 that Americans were “basically being hypnotized” into taking the covid vaccine.
Typically, slides and data for the panel’s meetings are posted on the CDC’s website several days beforehand. This time they weren’t posted at all.
The committee’s working group that studied hepatitis B vaccines did not include recognized hepatitis experts. When a few panel members expressed reservations during the ACIP meeting, CDC hepatitis specialist Adam Langer was brought in to answer questions. He frowned on the proposed changes.
Surprising Choice of Experts
At 8 a.m. Dec. 4, the CDC finally listed the names of the meeting’s presenters. Aaron Siri, one of Kennedy’s former lawyers and a strident legal foe of vaccination, was set to headline Friday’s discussion of the pediatric immunization schedule.
Sen. Bill Cassidy, a Louisiana Republican and physician who cast a deciding vote for Kennedy to win confirmation to his job, said on the social platform X: “Aaron Siri is a trial attorney who makes his living suing vaccine manufacturers. He is presenting as if an expert on childhood vaccines. The ACIP is totally discredited. They are not protecting children.”
In replies to his post, some people demanded to know what Cassidy planned to do about it. While he has publicly criticized some of Kennedy’s moves on vaccines, the senator has made no visible effort to reverse them.
As the meeting began, Malone revealed that Vicky Pebsworth, a senior officer at the National Vaccine Information Center, a four-decade-old cornerstone of vaccine skepticism, was chairing a committee that is reviewing the entire childhood vaccine schedule. That’s the repository of ACIP recommendations that protect American children from measles, pertussis, influenza, tetanus, chickenpox, meningitis, and a host of other diseases.
Typically, seasoned CDC and FDA experts on vaccines and infectious disease present data about a disease and the options for its prevention before ACIP votes on a policy. Instead, Pebsworth, vaccine-skeptical climate scientist , and businessperson Mark Blaxill, who helped lead another anti-vaccine group, presented the case — a negative one — on the hepatitis B vaccine on Dec. 4.
Sports medicine doctor Tracy Beth Høeg, who parlayed a year working with University of California-San Francisco epidemiologist Vinay Prasad, now the FDA’s vaccine chief, into a leading role at the agency, frequently chimed in. Nevison and Blaxill were co-authors of a 2021 autism study retracted for data misrepresentation and other problems.
Unsurprisingly, the picture they painted Dec. 4 suggested that the hepatitis B birth dose wasn’t necessary, and might be dangerous, notwithstanding years of scientific consensus to the contrary.
The presentations stunned Cody Meissner, an infectious disease specialist and one of the only vaccinologists on the CDC panel. “There were so many statements that I don’t agree with that it’s hard to be succinct,” he said.
Yvonne Maldonado, a Stanford University infectious disease specialist and one of the former ACIP members ejected in June, said she found it horrifying to watch unvetted presentations by nonexpert nonphysicians.
“Almost every statement made by this committee was misinformation, disinformation, or outright lies,” she said. “They are cherry-picking data, pulling up fringe papers, misunderstanding good papers. They are not the right people to be making decisions.”
Pebsworth said the committee was taking up the birth dose issue because of “pressure coming from stakeholder groups” ‚Äî presumably including Kennedy and his allies. The U.S. is an “outlier” in its universal recommendation, she erroneously said.
In fact, the birth dose of the hepatitis B vaccine is given in 115 countries and is recommended by the World Health Organization. Many Western European countries limit the birth dose to targeted groups, however.
Arguments for the Birth Dose
Nevison said targeted measures to stop the virus in the 1980s, including promoting safer sex, increasing blood screening, and vaccinating the babies of hepatitis B-positive mothers, had achieved most of the reduction in cases since then. But most experts say the birth dose played a key role. And the virus remains a threat, with an in the U.S.
The birth dose “is a safety net,” Meissner said. “It’s really for chronically infected mothers who for one reason or another do not get tested.”
“Where is the evidence of harm?” asked another panelist, psychiatrist Joseph Hibbeln.
In the years since the birth dose of hepatitis B vaccine was recommended, it has caused vanishingly few confirmed major side effects.
Blaxill, who 25 years ago helped advance the since-disproven theory that traces of mercury in vaccines were causing an epidemic of autism, said that hepatitis B vaccines were inadequately studied. He pointed to a study that showed high fevers in some children after the shot, which he said suggested brain inflammation.
Maldonado said that’s wrong. “I’ve seen thousands of children with fevers,” she said. “It’s not the same as encephalitis.”
Nevison said that a small number of vaccine court awards proved at least some harm by hepatitis B vaccinations. Reed Grimes, director of the Division of Injury Compensation Programs at the Health Resources and Services Administration, explained that an award does not necessarily signify proof of injury, but rather that the government decided not to contest a claim.
Speculation bloomed. Panelist Evelyn Griffin, an obstetrician, posited that rising cases of inflammatory bowel disease might be related to a medium ‚Äî brewer’s yeast ‚Äî used in the production of the hepatitis B vaccine. She did not cite a source for the idea.
Babies born with hepatitis B infections have a 90% chance of chronic liver infection later in life, and 25% of those with a chronic infection will die prematurely with chronic liver disease.
Panel members pushing to end the universal birth dose argued that blood tests of pregnant women should show who needs the shot. But only 35% of women who test positive receive all recommended follow-up care, and the virus can spread easily through contacts as common as a toothbrush or a bath towel. Ending the birth dose could result in nearly 500 deaths a year, according to a recent study.
The meeting was preceded by a heavy round of briefings for journalists and from established medical experts who view the new ACIP as a sounding board for anti-vaccine views ‚Äî “inflating speculative risks while downplaying well-established vaccine benefits,” as three recent .
They noted that the hepatitis B birth dose is already optional, although doctors strongly recommend it. But recommending that it be a shared decision based on individual choice, as the ACIP voted Dec. 5, could add paperwork for doctors and introduce doubts in parents’ minds.
ACIP recommendations aren’t binding but have been used by health insurers in the past to establish coverage decisions. Federal agencies and private insurers will in most cases continue to pay for the hepatitis B vaccination if parents want it, said Andrew Johnson, who represented the Centers for Medicare & Medicaid Services during the meeting. But studies have shown that ambiguous advice leads to lower vaccination rates, said Kathryn Edwards, a Vanderbilt University vaccinologist.
Anti-vaccine activists have long targeted the hepatitis B birth dose. At one time they baselessly claimed it caused sudden infant death syndrome.
But within a decade of the universal dose implementation, the rate of SIDS had . That was thanks to an HHS-American Academy of Pediatrics’ “back to sleep” campaign, which urged parents to avoid suffocation risk by not letting their babies go to sleep on their stomachs.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/cdc-acip-hepatitis-b-birth-dose-reversal-recommendation-rfk/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2128206&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>