And CEO Brad Meyer fears times will soon get worse for the clinic and its 21,000 patients. That’s because Nebraska is set to become the first state to require certain Medicaid enrollees to work or lose their coverage under new rules in President Donald Trump’s One Big Beautiful Bill Act.
“This will have a huge financial impact on us,” Meyer said. On May 1, seven months before the law requires, the state will begin imposing work requirements on eligible adult Medicaid enrollees.
Most of Bluestem’s patients are covered by the government program for people with low incomes or disabilities. Meyer estimates up to 15% of them may be kicked off Medicaid, which could cost his center about $600,000 a year. That could mean cutting services or staff.
Nationwide, about 17,000 federally funded community health centers like Bluestem . They’re bracing for fallout from the law Trump signed last year, which could cost the nonprofit health centers $32 billion collectively over five years, according to the Commonwealth Fund, a health research foundation.
Health centers receive annual federal grants but depend on Medicaid reimbursements for patient care as their largest source of revenue. The government insurance program covered about half of their roughly 33 million patients in 2024.
Commonwealth estimates that 5.6 million patients of health centers will lose Medicaid coverage over the next decade as most states enact work requirements тАФ a provision of Trump’s law that requires nondisabled enrollees to work, volunteer, or perform another approved activity for at least 80 hours a month.
Most are expected to lose coverage not because they don’t work but because of paperwork errors, like failing to document their hours or verify that they qualify for an exemption.
Health center officials say there’s no easy way to make up for the lost revenue other than cutting staff or services, which would affect all their patients. The cuts will coincide with an expected increase in patients, as people who lose coverage turn to the clinics for low-cost care.
By law, health centers are required to treat all patients regardless of their ability to pay.
A Double Whammy
Overall, about 10 million fewer Americans will have insurance by 2034, the Congressional Budget Office estimates, both because of Trump’s law and congressional Republicans’ decision to scale back premium subsidies for Affordable Care Act health plans.
“We are incredibly worried,” said Jeffrey McKee, CEO of Community Health Centers of Burlington in Vermont. His clinics treat about 35,000 patients a year, nearly a third covered by Medicaid.
He predicts a surge in uninsured patients will cost another $3 million in lost revenue. That revenue crash could imperil street medicine programs and home care for patients 65 and older, he said.
In 2024, community health centers because of rising costs and the expiration of covid pandemic-era relief funds, according to a KFF analysis.
Centers with high rates of uninsured patients typically struggle more financially, while some centers are sustained through private donations.
People without insurance тАФ who made up about 18% of all health center patients in 2024 тАФ pay on a sliding scale. Those amounts are a fraction of what insurers pay.
The new Medicaid work requirements apply to Washington, D.C., and 40 states that expanded Medicaid eligibility under the ACA, and to adults with incomes up to 138% of the federal poverty level тАФ $22,025 for a single person this year.
Republicans say the work requirements will nudge people into the workforce and help preserve Medicaid for children and people who are pregnant or have disabilities. Studies by KFF and others show most enrollees already work, go to school, or have a health condition that prevents them from working.
Nebraska Is First Up
The Trump administration approved Nebraska’s early launch of its work requirement program, which could affect about . State Medicaid officials say they plan to use state and national databases to check whether people are already working or meeting an exemption so that most won’t have to do anything to keep coverage. But thousands will need to prove they satisfy the requirements.
At Bluestem in Lincoln, Meyer worries many of his Medicaid patients won’t take the steps needed to keep coverage.
Angelisa Corum, 57, said she loves the care she has gotten from her regular doctor at Bluestem Health over the past dozen years, particularly in dealing with breast cancer. “I am cancer-free, and they helped me get through that,” she said.
She said the care was the same when she was covered by her husband’s commercial insurance through his employer and when she was on Medicaid while he wasn’t working.
The work requirements are just one part of the Republican law passed last year that could hurt the health centers. It also requires more frequent eligibility checks for adults enrolled under Medicaid expansion, which advocates say could also lead people to lose coverage. Many states now require eligibility checks only once a year.
The law also reduces overall federal Medicaid funding to states, which may prompt them to cut reimbursements to centers and other health providers.
The National Association of Community Health Centers, the largest advocacy group for the clinics, has tried to walk a tightrope, warning about impending cuts from the law while still working with the Trump administration. The group praised Congress for increasing base grant funding for health centers in the federal budget approved in January.
Kyu Rhee, CEO of the national association, said the clinics enjoy strong bipartisan support in Washington despite the Medicaid cuts.
He has met with Trump administration officials to discuss how health centers can play a role in keeping people from losing coverage due to work requirements. He said they can help meet other priorities of the administration’s, like improving American diets, expanding primary care, and focusing on chronic diseases тАФ though it’s unclear how any of that would result in more funding.
To further show the reach of health centers, the association recently funded a study that found 52 million people visited the clinics over a three-year-period. “It makes a statement we serve a lot more Americans than those from just a single year,” Rhee said.
Health center officials are hopeful they will get some of the funding from the included in the GOP-passed law. States will begin spending the first tranche of that money this spring.
Rhee said he is encouraged that states will have technology to help tap into databases to verify many enrollees’ work status or health conditions to meet “medical frailty” rules that could help them avoid being disenrolled.
Others are less optimistic.
“Health centers are bracing for a major financial impact,” said Sara Rosenbaum, a health law and policy professor at George Washington University and Medicaid expert who co-authored the Commonwealth Fund study. “The way they cope is the same way health systems usually cope as they go through mass layoffs, site closures, and service reductions.”
Amanda Pears Kelly, CEO of Advocates for Community Health, a trade group representing 52 health centers, said health centers are also worried about rising costs, especially for prescription drugs. The impending financial challenges will make it more difficult to hire staff both in rural areas where doctors and nurses are scarce and in more populated areas, where competition for workers is more acute, she told ║┌┴╧│╘╣╧═Ї News.
“The challenge is health centers are being hit from every direction,” Pears Kelly said.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/federal-funded-community-health-centers-revenue-loss-under-trump/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2173906&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>State governments rely on such companies to design and operate computer systems that assess whether low-income people qualify for Medicaid or food aid through the Supplemental Nutrition Assistance Program, commonly referred to as food stamps. Those state systems have a that can , a ║┌┴╧│╘╣╧═Ї News .
These benefits, provided to the poorest Americans, can mean the difference between someone obtaining medical care and having enough to eat тАФ or going without.
States are now racing to update their eligibility systems to adhere to President Donald Trump’s sweeping tax and domestic spending law. The changes will add red tape and restrictions. They are coming at a steep price тАФ both in the cost to taxpayers and coverage losses тАФ according to state documents obtained by ║┌┴╧│╘╣╧═Ї News and interviews.
The documents show government agencies will spend millions to save considerably more by removing people from health benefits. While states sign eligibility system contracts with companies and work with them to manage updates, the federal government foots most of the bill.
The law’s Medicaid policies will cause to become uninsured by 2034, according to the nonpartisan Congressional Budget Office. Roughly will lose access to monthly cash assistance for food, including those with children.
In five states alone, for state officials and reviewed by ║┌┴╧│╘╣╧═Ї News show that changes will cost at least $45.6 million combined.
“This is a pretty big payday,” said Adrianna McIntyre, an assistant professor of health policy and politics at Harvard’s T.H. Chan School of Public Health.
The law, which grants tax breaks to the nation’s wealthiest people, requires most states to tie Medicaid coverage for some adults to having a job, and imposes other restrictions that will make it harder for people with low incomes to stay enrolled. SNAP restrictions began to take effect in 2025. Major Medicaid provisions begin later this year.
Documents prepared by consulting company Deloitte estimate that a pair of computer system changes for Medicaid work requirements in Wisconsin will . Two other changes related to the state’s SNAP program will cost an additional $4.2 million, according to the documents, which for the Wisconsin Department of Health Services.
In Iowa, changes to its Medicaid system are expected to cost at least $20 million, , a consulting company that operates the state’s eligibility system.
Optum тАФ which operates the platform Vermont residents use for Medicaid and marketplace health plans under the Affordable Care Act тАФ to evaluate and incorporate new health coverage restrictions.
Initial changes in Kentucky, which has had a contract with Deloitte since 2012, . And in Illinois, will cost at least $12 million.
A Historic Mandate
For six decades after President Lyndon Johnson created the government insurance program in 1965, Congress had never mandated that Medicaid enrollees have a job, volunteer, or go to school.
That will change next year. The tax and spending law enacted by Trump and congressional Republicans requires millions of Medicaid enrollees in 42 states and the District of Columbia to prove they’re working or participating in a similar activity for 80 hours a month, unless they qualify for an exemption. The CBO projected, based on an early version of the bill, that 18.5 million adults would be subject to the new rules тАФ .
Vermont Medicaid officials expect it will cost $5 million in fiscal 2027 to implement changes in response to the federal law, said Adaline Strumolo, deputy commissioner of the Department of Vermont Health Access. About $1.8 million is for Optum to make eligibility system adjustments. Optum is a subsidiary of UnitedHealth Group.
The One Big Beautiful Bill Act will subject nearly 55,000 Vermont Medicaid recipients to work requirements тАФ about a third of the state’s enrollees.
The law forced the state “to essentially drop everything else we were doing,” Strumolo said in an interview. “This is a big, big lift.”
Optum’s contract with the state was as of October.
of adult Medicaid enrollees nationally are already working, according to KFF. Advocacy groups for Medicaid recipients say work requirements will nonetheless cause significant coverage losses. Enrollees will face added red tape to prove they’re complying. And eligibility systems already prone to error will have to account for employment, job-related activities, and any exemptions.
An estimated 5.3 million enrollees will become uninsured by 2034 due to work requirements, the .
In Wisconsin, state officials estimate could lose coverage after work requirements take effect. Not covering those people would in Medicaid spending for one year.
Wisconsin’s eligibility system for Medicaid and SNAP тАФ known as CARES тАФ in 1994, and initially was a transfer system from Florida, according to a 2016 state document.
Deloitte submitted its cost estimates for Medicaid and SNAP changes to the state in September and December. Elizabeth Goodsitt, a spokesperson for the Wisconsin Department of Health Services, declined to answer questions about whether additional changes will be needed, how much it will cost to make all eligibility system changes to comply with the new federal law, and whether the state negotiated prices with Deloitte.
Bobby Peterson, executive director of the public interest law firm ABC for Health, said Wisconsin has invested “very little” to help people navigate the Medicaid eligibility process, which soon will become more difficult.
“But they’re very willing to throw $6 million to their contractors to create the bells and whistles,” Peterson said. “That’s where I feel a sense of frustration.”
New Hurdles for Vets and Homeless People
Medicaid work requirements are only one change required by Trump’s tax law that will make it harder to obtain safety-net benefits.
Starting in October, the law prohibits several immigrant populations from accessing Medicaid and ACA coverage, including people who have been granted asylum, refugees, and certain survivors of domestic violence or human trafficking. Beginning Dec. 31, states must verify eligibility twice a year for millions of adults тАФ doubling state officials’ workload. And the law restricts SNAP benefits by requiring more adult recipients to work and by removing work exemptions for veterans, homeless people, and former foster youth.
Days after Trump signed the bill in July, Kentucky health officials raced to make changes to the state’s integrated eligibility system, which verifies eligibility for Medicaid, SNAP, and other programs. Deloitte operates the system under a five-year . , initial changes costing $1.6 million were labeled a “high priority” and approved on an “emergency” basis, with some of the changes to the nation’s largest food aid program going into effect almost immediately.
Officials with Kentucky’s Cabinet for Health and Family Services declined to answer a detailed list of questions, including how much it will cost to make all the modifications needed.
Deloitte spokesperson Karen Walsh said the company is working with states to implement new requirements but declined to answer questions about cost estimates in several states. “We are delivering the value and investments we committed to,” Walsh said.
In most states, government agencies rely on contractors to build and run the systems that determine eligibility for Medicaid. Many of those states also use such computer systems for SNAP. But the federal government тАФ that is, taxpayers тАФ to develop and implement state Medicaid eligibility systems and pays 75% of ongoing maintenance and operations expenses, according to federal regulations.
“Five, 10 years ago, I’m not sure if you would hear much mention of SNAP from a Medicaid director,” Melisa Byrd, Washington, D.C.’s Medicaid director, said in November at an annual conference of Medicaid officials. “And particularly for those with integrated eligibility systems тАФ as D.C. is тАФ┬н I’m learning more about SNAP than I ever thought.”
The federal law was the topic du jour at last year’s gathering in Maryland, held at the Gaylord National Resort and Convention Center, the largest hotel between New Jersey and Florida.
Consulting companies had taken notice. Gainwell, an eligibility contractor and one of the conference’s corporate sponsors, emblazoned its logo on hotel escalators. Companies set up booths with materials promoting how they could help states and handed out snacks and swag.
“Conduent helps agencies work smarter by simplifying operations, cutting costs and driving better outcomes through intelligent automation, analytics, and innovation in fraud prevention,” read one such handout from another contractor. “Together, we can better serve residents at every step of their health journeys.” Conduent holds Medicaid eligibility and enrollment contracts in Mississippi and New Jersey, their Medicaid agencies confirmed to ║┌┴╧│╘╣╧═Ї News.
In handouts, Deloitte touted its role in “building a new era in state health care” and as “a national leader in Medicaid program and technology transformation, building a strong track record across the federal, state, and commercial health care ecosystem.” ║┌┴╧│╘╣╧═Ї News found that Deloitte, a global consultancy that generated in revenue in fiscal 2025, dominates this slice of government business.
“With Medicaid Community Engagement (CE) requirements, states are tasked with adding a new condition of Medicaid eligibility to support state and federal objectives,” added another brochure. “Deloitte offers strategic outreach and responsive support to help states engage communities, lower barriers, and address access to coverage.”
A $20.3 Million Bill in Iowa
Before Trump signed the One Big Beautiful Bill Act, Iowa lawmakers wanted to impose their own version of work requirements. They would have applied to 183,000 people before any exemptions. The new law would necessitate a change to Iowa’s Medicaid eligibility system, according to documents prepared by Accenture, which operates Iowa’s system through a .
Adding the ability to verify work status would cost up to $7 million, . By July, the cost to implement the One Big Beautiful Bill Act’s work requirements and other Medicaid provisions . Accenture’s analysis said the federal law necessitated . Making employment a condition of Medicaid benefits could cause an estimated 32,000 Iowans to lose coverage, according to a
Cutting 32,000 people from coverage in one year, a fraction of the Iowa and the federal government spend on Medicaid in a given year.
In Cedar Rapids, most of Eastern Iowa Health Center’s patients rely on Medicaid, CEO Joe Lock said. He questioned the government’s logic of spending tens of millions of dollars on a policy to remove Iowans from Medicaid.
Most of the health center’s patients live at or below the federal poverty level тАФ currently .
“There is no benefit to this population,” Lock said.

Danielle Sample, a spokesperson for Iowa’s Department of Health and Human Services, did not answer questions about how much it will cost to implement changes to the state’s separate SNAP eligibility system.
In Illinois, the state’s work this year is largely focused on meeting major provisions of the One Big Beautiful Bill Act. The state estimates that as many as 360,000 residents could lose Medicaid, largely due to the work requirements, said Melissa Kula, a spokesperson for the Illinois Department of Healthcare and Family Services.
Kula confirmed that тАФ priced at $12 million тАФ is related to Trump’s law. The estimate also mentions other work. Kula said Deloitte is charging the state a $2 million fixed fee related to work requirements.
The Trump administration has acknowledged that the work is coming at a cost. In January, top officials for the Centers for Medicare & Medicaid Services said government contractors, including Deloitte, Accenture, and Optum, have and reduced rates through 2028 to help states incorporate system changes.
“The companies were extremely excited to do this,” , the top CMS Medicaid official. “Everyone’s really focused on getting to work.”
CMS spokesperson Catherine Howden declined to answer questions about the discounts.
Goodsitt, the Wisconsin Medicaid spokesperson, declined to answer questions about whether Deloitte has discounted its rates. Officials with Kentucky’s Cabinet for Health and Family Services did not answer a detailed list of questions, including whether Deloitte extended discounts to make these changes.
It’s unclear what discounts, if any, Deloitte and Accenture have offered to individual states. Walsh, the Deloitte spokesperson, declined to answer detailed questions about the discounts the Trump administration announced this year. Accenture did not respond to repeated requests for comment.
Strumolo, the Vermont health official, said state officials discussed the announcement with Optum “in detail.”
Optum for a specific module related to Medicaid work requirements. That product is unworkable for Vermont because it would mean “moving to a new system when we don’t have to.” When asked about whether the company offered discounts, Strumolo said “not explicitly.”
In a statement, UnitedHealth Group spokesperson Tyler Mason said Optum supports state implementation of new federal requirements “with a range of options to meet their unique cost and policy needs.”
He declined to specify whether Optum discounted Vermont’s rates and how it calculated the costs of doing its work. “Optum is helping mitigate upfront implementation expenses so states can focus on approaches that reduce duplication, accelerate implementation, and manage costs over time тАФ supporting better outcomes for individuals covered by Medicaid,” Mason said.
Strumolo said Optum’s initial changes in Vermont cover items that take effect this year and in 2027 тАФ Medicaid work requirements, checking eligibility every six months, and prohibiting certain immigrants from qualifying for health programs.
“There’s a lot more that could come,” she said.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/state-medicaid-work-requirements-eligibility-systems-deloitte-accenture-optum/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2174991&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The legislation would prohibit state and local governments from requiring crisis pregnancy centers to perform abortions, provide referrals for abortion services, or inform patients about such services or contraception options. It also would allow crisis pregnancy centers to sue the violating government entity.
Wyoming lawmakers of the Center Autonomy and Rights of Expression Act, or , on March 4. Other versions have advanced in and this year. One was in 2025. The CARE Act is “model legislation” created by the , an anti-abortion, conservative Christian legal advocacy group.
A similar proposal, the , was introduced in Congress last year but hasn’t moved out of the House Energy and Commerce Committee.
The Wyoming bill says that pregnancy centers, many of which are affiliated with religious organizations, need legal protection after facing “unprecedented attacks” following the Supreme Court’s overturning of Roe v. Wade. It says that several state legislatures have introduced bills that . Opponents of these centers say they falsely present themselves to consumers as medical clinics, though they are not subject to state and federal laws that protect patients in medical facilities.
“Across the country, government officials are increasingly, increasingly targeting pregnancy care centers,” Valerie Berry, executive director of the in Cheyenne, said at a February legislative hearing on the Wyoming bill. “This legislation is not about creating division. It’s about protecting constitutional freedoms, freedom of speech, and freedom of conscience.”
Wyoming state , a Republican, expressed concern at the hearing about granting protections to pregnancy centers that other private businesses do not have.
“They have protections in place,” he said. “My issue with this is giving extra special protections.”
In 2022, Wellspring Health Access, the only clinic in Wyoming that provides abortions, in an arson attack.
“We are the ones providing the accurate information on reproductive health care, and we suffer the consequences for that,” Julie Burkhart, the president and founder of Wellspring Health Access, told ║┌┴╧│╘╣╧═Ї News.
, a professor at the University of California-Davis School of Law, said the proposed legislation would insulate crisis pregnancy centers from having to meet the standards that medical organizations face. It would blur the line between advocacy and medical practice, she said. And such legislation provides Republicans with a potentially useful campaign message ahead of midterm elections.
“The GOP needs a messaging strategy as for how it cares about women even if it bans abortion and even if it doesn’t want to commit state resources to helping people before and after pregnancy,” Ziegler said. “The strategy is to outsource that to pregnancy counseling centers, which of course increases the incentive to protect them.”
Model Legislation
The Alliance Defending Freedom is the same group that , the 1973 court ruling that protected the right to abortion nationwide. The group drafted model legislation to establish a 15-week abortion ban that was the basis of a 2018 Mississippi law. That led to the Dobbs v. Jackson Women’s Health Organization Supreme Court case that overturned Roe.
The alliance said its attorneys were unavailable to comment on the organization’s strategy for the CARE Act. In for the bill, the group said federal, state, and local efforts are targeting pregnancy care centers in a “clear attempt to undermine and impede” their work and shut them down.
In recent years, have been targeted with vandalism and threats.
But the attacks the model legislation primarily aims to address are the legal and regulatory efforts by some states seeking more oversight of the crisis pregnancy centers, including a California law requiring centers to clearly inform patients about their services. That law was overturned when the Supreme Court ruled in favor of crisis pregnancy centers’ argument that it violated their First Amendment rights.
The Supreme Court is that will decide whether states can subpoena the organizations for donor and internal information.
It’s unlikely that crisis pregnancy centers would face such regulatory measures in the conservative states where the legislation is under consideration. One Wyoming lawmaker acknowledged that in the February committee hearing.
Differing Services
During that hearing, state , a Republican who heads the committee sponsoring the bill, presented the measure as “so important, especially with our maternity desert,” referring to a lack of access to maternity health care services.
Some crisis pregnancy centers may have a few licensed clinicians, but many do not. Many offer free resources, such as diapers, baby clothing, and other items, sometimes in exchange for participation in counseling or parenting classes.
Planned Parenthood clinics, by contrast, provide a range of health services, such as testing and treatment for sexually transmitted infections, primary care, and screenings for cervical cancer. They also are regulated as medically licensed organizations.
Since Roe was overturned, the abortion rights movement has faced significant challenges. Congressional Republicans’ One Big Beautiful Bill Act, which President Donald Trump signed into law last summer, to abortion providers. The move contributed to Planned Parenthood closing last year.
As of 2024, operated nationwide, according to a map created by researchers at the University of Georgia, compared with providing abortions at the end of 2025.
a research organization affiliated with the anti-abortion nonprofit SBA Pro-Life America, has suggested that pregnancy centers could help fill the gap left by the Planned Parenthood closures.
Ziegler said that would leave patients vulnerable to medical risks.
Centers’ Growing Power
Previous efforts in , Colorado, and Vermont to regulate crisis pregnancy centers arose from concerns over allegations of and questions about .
In 2024, in five states to investigate whether centers were misleading patients into believing that their personal information was protected under the Health Insurance Portability and Accountability Act, known as HIPAA, and to find out how the centers were using patients’ information.
Courts, including the Supreme Court, have regularly that argue the attempts at regulation are violations of their First Amendment rights to free speech and religious expression.
Crisis pregnancy centers also have seen a flood of funding since Roe was overturned.
At least , including crisis pregnancy centers, according to the Lozier Institute.
Six states distribute a portion of their federal Temporary Assistance for Needy Families funding тАФ cash payments meant for low-income families with children тАФ to crisis pregnancy centers. Texas, Florida, Tennessee, and Oklahoma have provided tens of millions of dollars for the organizations.
One analysis found that crisis pregnancy centers also received from 2017 to 2023, including from the 2020 relief package signed into law during Trump’s first term amid the covid pandemic.
Despite the challenges clinics that provide abortions face, Burkhart, the head of the Wellspring facility in Wyoming, said it’s important to continue offering access to people who need it. She’s helped open clinics in rural parts of other conservative states and said those clinics continue to see people walking through their doors.
“That proves to me, regardless of your religion, political party, there are times in people’s lives that people need access to qualified reproductive health care,” she said. “That includes abortion.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/courts/abortion-bans-clinics-crisis-pregnancy-centers-maternity-care-wyoming/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2166071&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Sylvia Chou, 51, Maryland
Program director, National Cancer Institute

This <a target="_blank" href="/health-industry/nih-national-institutes-of-health-resignation-scientist-profiles-brain-drain/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2162351&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>More than three-quarters of American adults didn’t get a covid shot last season, a figure that health care experts warn could rise this year amid new U.S. government recommendations.
The covid vaccine was initially popular. About 75% of Americans had received of the first versions of the vaccine by early 2022, Centers for Disease Control and Prevention data shows. But only about 23% of American adults got a covid shot during the 2024-25 virus season, well below the 47% of American adults who got a flu shot. The vaccination rates for , , and tetanus are also going down.
Yet covid remains a serious, potentially deadly health risk, listed as the primary cause of death on roughly 31,400 death certificates last year. By comparison, flu killed people and pneumonia, a common complication of the flu, killed , .
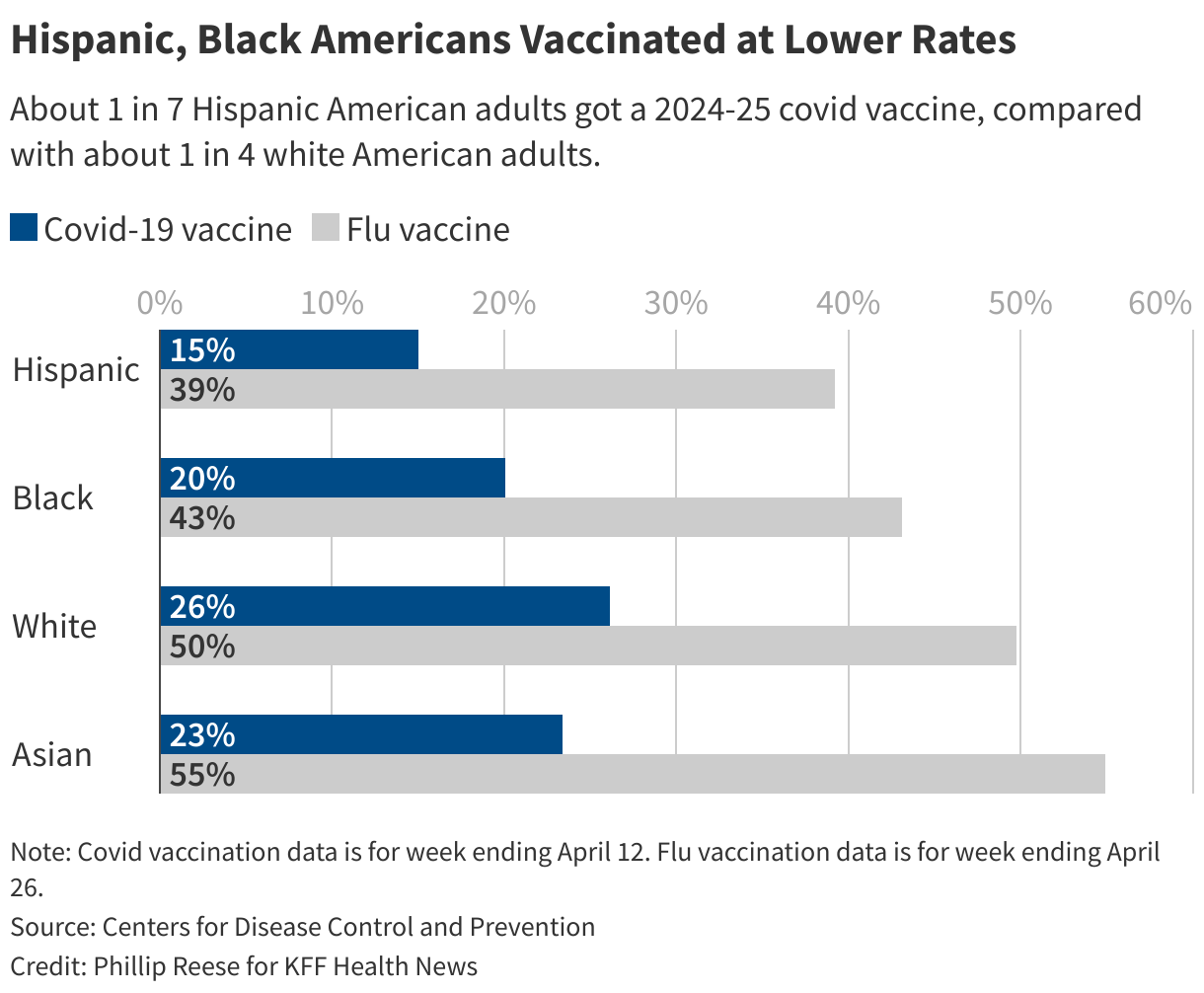
As millions of Americans decide whether to get a covid shot this season, public health researchers worry vaccination rates will slide further, especially because Hispanic and Black Americans and those under 30 have lower rates, exposing them to serious complications such as long covid. Under the Trump administration and Health and Human Services Secretary Robert F. Kennedy Jr., the federal government has narrowed its recommendations on the covid vaccine, leading to a hodgepodge of rules on pharmacy access, with Americans living in Republican states often facing more barriers to getting a shot.
“A lot of misinformation is going around regarding covid,” said , an assistant professor of health, society, and behavior at the University of California-Irvine. “Vaccine hesitancy is going to increase.”
In August, the FDA for covid vaccines to those 65 or older and to adults and children with at least one underlying condition that puts them at high risk for serious complications from covid.
A month later, the CDC’s Advisory Committee on Immunization Practices “shared clinical decision-making” on the vaccine, pulling back from advising all adults to get vaccinated. The committee advised doctors to emphasize to adults under 65 and children that the benefits of the vaccine are greatest for those with underlying health conditions.
The guidance is rebutted by infectious disease experts who say most adults and children should get both the flu and covid vaccines, which are safe, effective, and prevent serious illness. Several independent medical organizations like the American Academy of Family Physicians and the American Academy of Pediatrics have reiterated their support for broad adoption of covid vaccines.
More than two dozen states have taken steps to ensure most people can get a covid shot at the pharmacy without a prescription, with many states tying their policies to the advice given by medical organizations. And many of those states require insurers to cover vaccines at no cost, according to . In several other states, predominantly Republican-led, pharmacy access to vaccines may require a prescription.
Among the most commonly cited reasons for covid vaccine hesitation are fears about side effects, long-term health consequences, and the effectiveness of the vaccine, and mistrust of pharmaceutical corporations and government officials, according to of multiple studies, published in the journal Vaccines.
Covid vaccine hesitancy in the 2024-25 virus season was higher among Latinos, African Americans, men, uninsured people, and people living in Republican-leaning states, CDC data shows.
Latino adults were significantly less likely than adults from most other racial and ethnic groups to get a covid shot last season, with a vaccination rate around 15%.
Some of that may be due to age: A of Latinos are young. But public policy actions may also be a factor. The first Trump administration, for example, tied Medicaid to “public charge,” a rule allowing the federal government to deny an immigrant a green card or visa based on their dependence on taxpayer-funded programs. Some Latinos may be afraid to sign up for social services even after the Biden administration reversed those first-term Trump actions.
Haro-Ramos co-authored published in 2024 that found many Latinos were hesitant to get vaccinated because of fears about their immigration status, and that experiencing health discrimination, like care denials or delays, increased their vaccine hesitancy.
“Do you trust the health care system, broadly speaking? Do you want to provide your information — your name, your address?” Haro-Ramos said. “Trust is critical.”
Haro-Ramos said the problem has likely worsened since her study was published. The Trump administration that it would give the personal information of Medicaid enrollees to Immigration and Customs Enforcement. Many Latinos are canceling doctor appointments to head off possible confrontation with immigration enforcement officials.
“People are avoiding leaving their homes at all costs,” Haro-Ramos said.
, an associate professor at the University of Georgia College of Public Health, recently of covid vaccination among nearly 1,500 African Americans living in south Georgia. The study found that participants were more likely to listen to their health care providers than faith leaders or co-workers when seeking advice on getting vaccinated.
More than 90% of those studied had received at least one dose of the vaccine, but those who were unvaccinated were more likely to agree with false statements that tied vaccines to miscarriages, to components’ remaining in the body for a long time, or even to the conspiracy that they implant a computer chip in the body.
“It’s the clinicians who can take the messages about vaccination — that these are myths,” Rajbhandari-Thapa said.
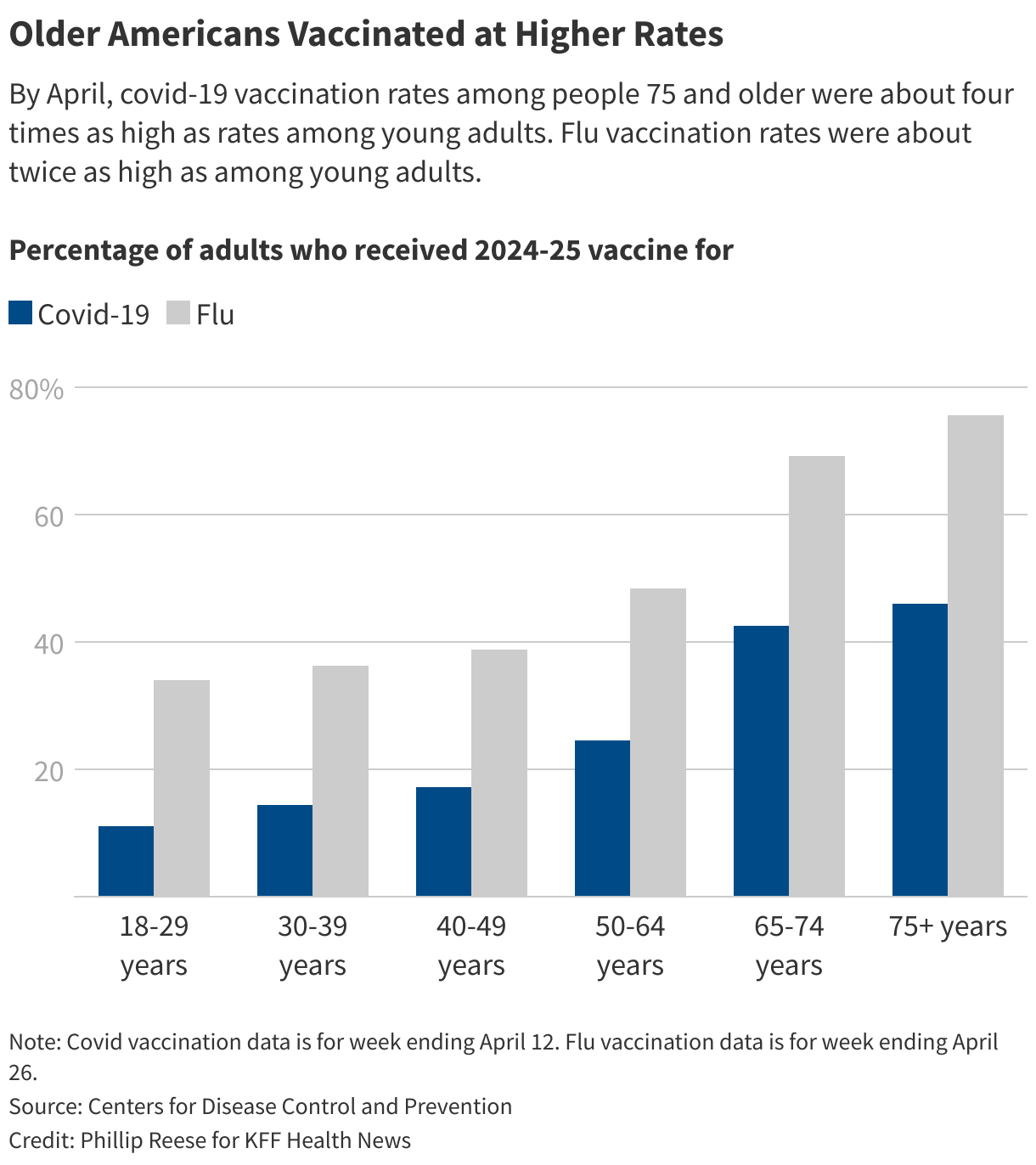
Even though covid hospitalization and death rates have fallen dramatically since the worst days of the pandemic, fatal complications related to covid remain most common among older people. of U.S. covid deaths last year were among people 65 and older, compared with of flu and pneumonia deaths.
As the pandemic falls into the rearview, young people have developed a sense of invincibility. Only 11% of Americans ages 18 to 29 received a vaccine during the 2024-25 virus season, the lowest vaccination rate among adult age groups. That’s far below the who got at least one dose of the initial covid vaccines by November 2023.
While many people get covid after receiving a covid shot, because the vaccine’s ability to prevent infection wears off pretty fast, some misunderstand the purpose of the shot, said , an infectious disease specialist at UCLA Health.
“They think, ‘Well, the vaccine didn’t prevent me from getting covid, so the vaccine didn’t work,’” Yang said. “And what they’re not seeing is that the vaccine prevented them from getting severely ill, which is ultimately the most important thing.”
And the vaccine can help prevent long covid, which is a problem for all ages, Yang said. A recent Northwestern University study younger adults suffer worse symptoms of long covid than older adults.
Ultimately, Yang said, it is not a consistent choice to get a flu vaccine but forgo a covid vaccine, since both are safe, effective, and prevent serious illness. It is clear, he added, that people with compromised immune systems and those at higher risk should get a covid shot. The decision is “a little bit less clear” for others, but “probably most adults should be getting vaccinated, just like it’s recommended for the flu vaccine, as well as most children.”
Phillip Reese is a data reporting specialist and an associate professor of journalism at California State University-Sacramento.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/covid-flu-vaccination-rates-virus-season-conflicting-guidance-immigration/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2110742&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Fast-forward to the congressional stalemate that has closed the federal government for more than a month. Democrats, entrenched on one side of the legislative battle, staked their political future on merely preserving parts of the Affordable Care Act тАФ a far cry from the systemic health policy changes that party members once described as crucial for tackling the high price of care.
Democrats succeeded in focusing national attention on rising health insurance costs, vowing to hold up funding for the federal government until a deal could be made to extend the more generous tax subsidies that have cut premiums for Obamacare plans. Their doggedness could help them win votes in midterm elections next year.
But health care prices are rocketing, costly high-deductible plans are proliferating, and 4 in 10 adults have some form of health care debt. As health costs reach a crisis point, a yawning gulf exists between voters’ desire for more aggressive action and the political urgency in Washington for sweeping change.
“There isn’t a lot of eagerness among politicians,” said , an economist who played a key role in drafting the ACA. “Why aren’t they being more bold? Probably scars from the ACA fights. But health care is a winning issue. The truth is we need universal coverage and price regulation.”
Voters rank lowering health care costs as a top priority, above housing, jobs, immigration, and crime, according to a by Hart Research Associates for Families USA, a consumer health advocacy group.
And costs are climbing. Premiums for job-based health insurance rose 6% in 2025 to an average of $26,993 a year for family coverage, according to an annual survey of employers released Oct. 22 by KFF, a health information nonprofit that includes ║┌┴╧│╘╣╧═Ї News. For all the attention given to grocery, gas, and energy prices, health premiums and deductibles in recent years have risen and wages.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/elections/shutdown-health-care-costs-obamacare-democrats-public-option/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2108528&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Despite progress in some mostly blue states this year, however, recent setbacks in more conservative legislatures underscore the persistent challenges in strengthening patient protections.
Bills to shield patients from medical debt failed this year in Indiana, Montana, Nevada, South Dakota, and Wyoming in the face of industry opposition. And advocates warn that states need to step up as millions of Americans are expected to lose insurance coverage because of President Donald Trump’s tax and spending law.
“This is an issue that had been top of mind even before the change of administrations in Washington,” said Kate Ende, policy director of Maine-based Consumers for Affordable Health Care. “The pullback at the federal level made it that much more important that we do something.”
This year, Maine joined a growing list of states that have barred medical debt from residents’ credit reports, a key protection that can make it easier for consumers to get a home, a car, or sometimes a job. The with bipartisan support.
An in the U.S. have some form of health care debt.
The federal government was poised to bar medical debt from credit reports under in the waning days of former President Joe Biden’s administration. That would have helped an estimated 15 million people nationwide.
But the Trump administration did not defend the regulations from lawsuits brought by debt collectors and the credit bureaus, who argued that the Consumer Financial Protection Bureau exceeded its authority in issuing the rules. A federal judge in Texas appointed by Trump ruled that the regulation should be scrapped.
Now, only patients in states that have enacted their own credit reporting rules will benefit from such protections. More than a dozen have such limits, including California, Colorado, Connecticut, Minnesota, New York, and Vermont, which, like Maine, enacted a ban this year.
Still more states have passed in recent years, including caps on how much interest can be charged on such debt and limits on the use of wage garnishments and property liens to collect unpaid medical bills.
In many cases, the medical debt rules won bipartisan support, reflecting the overwhelming popularity of these consumer protections. In Virginia, the state’s conservative Republican governor this year restricting wage garnishment and capping interest rates.
And several GOP lawmakers in California joined Democrats to make it easier for patients to access financial assistance from hospitals for big bills.
“This is the kind of commonsense, pocketbook issue that appeals to Republicans and Democrats,” said Eva Stahl, a vice president at Undue Medical Debt, a nonprofit that buys up and retires patients’ debts and has pushed for expanded patient protections.
But in several statehouses, the drive for more safeguards hit walls.
Bills to ban medical debts from appearing on credit reports failed in and , despite support from some GOP lawmakers. And measures to limit aggressive collections against residents with medical debt were derailed in , , and .
In some states, the measures faced stiff opposition from debt collectors, the credit reporting industry, and banks, who told legislators that without information about medical debts, they might end up offering consumers risky loans.
In Maine, the Consumer Data Industry Association, which represents credit bureaus, that regulating medical debt should be left to the federal government. “Only national, uniform standards can achieve the dual goals of protecting consumers and maintaining accurate credit reports,” warned Zachary Taylor, the group’s government relations director.
In South Dakota, state Rep. Lana Greenfield, a Republican, echoed industry objections in urging her colleagues to vote against a credit reporting ban. “Small-town banks could not receive information on a mega, mega medical bill. And so, they would in good faith perhaps loan money to somebody without knowing what their credit was,” Greenfield said on the House floor.
Under the Biden administration, that medical debt, unlike other debt, was not a good predictor of creditworthiness.
But South Dakota state Rep. Brian Mulder, a Republican who chairs the health committee and authored the legislation, noted the power of the banking industry in South Dakota, where favorable regulations have made the state a magnet for financial institutions.
In Montana, legislation to shield a portion of debtors’ assets from garnishment easily passed a committee. Supporters hoped the measure would be particularly helpful to Native American patients, who are by medical debt.
But when the bill reached the House floor, opponents “showed up en masse,” talking one-on-one with Republican lawmakers an hour before the vote, said Rep. Ed Stafman, a Democrat who authored the bill. “They lassoed just enough votes to narrowly defeat the bill,” he said.
Advocates for patients and legislators who backed some of these measures said they’re optimistic they’ll be able to overcome industry opposition in the future.
And there are signs that legislation to expand patient protections may make headway in other conservative states, including Ohio and Texas. A to force nonprofit hospitals to expand aid to patients facing large bills picked up support from leading conservative organizations.
“These things can sometimes take time,” said Lucy Culp, who oversees state lobbying efforts by Blood Cancer United, formerly known as the Leukemia & Lymphoma Society. The patients’ group has been pushing for state medical debt protections in recent years, including in Montana and South Dakota.
More concerning, Culp said, is the wave of uninsured patients expected as millions of Americans lose health coverage due to cutbacks in the recently passed GOP tax law. That will almost certainly make the nation’s medical debt problem more dire.
“States are not ready for that,” Culp said.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/courts/medical-debt-battle-patient-protections-states-trump-policy-credit-reports/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2091514&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>There never is.
Dahl Memorial’s three-bed emergency department тАФ a two-hour drive from the closest hospital with more advanced services тАФ instead depends on physician assistants and nurse practitioners.
Physician assistant Carla Dowdy realized the patient needed treatment beyond what the ER could provide, even if it had had a doctor. So, she made a call for a medical plane to fly the patient to treatment at Montana’s most advanced hospital. Dowdy also called out medications and doses needed to stabilize the patient as a paramedic and nurses administered the drugs, inserted IV lines, and measured vital signs.
Emergency medicine researchers and providers believe ERs, especially in rural areas, increasingly operate with few or no physicians amid a nationwide shortage of doctors.
A found that in 2022, at least 7.4% of emergency departments across the U.S. did not have an attending physician on-site 24/7. Like Dahl Memorial, more than 90% were in low-volume or critical access hospitals тАФ a federal designation for small, rural hospitals.
The results come from the 82% of hospitals that responded to a survey sent to all emergency departments in the country, except those operated by the federal government. The study is the first of its kind so there isn’t proof that such staffing arrangements are increasing, said Carlos Camargo, the lead author and a professor of emergency medicine at Harvard Medical School. But Camargo and other experts suspect ERs running without doctors present are becoming more common.
Placing ERs in the hands of nondoctors isn’t without controversy. Some doctors and their professional associations say physicians’ extensive training leads to better care, and that some hospitals are just trying to save money by not employing them.
The , open to all medical students and physicians, and the both support state and federal laws or regulations that would require ERs to staff a doctor around the clock. Indiana, Virginia, and South Carolina recently passed such legislation.
Rural ERs may see fewer patients, but they still treat serious cases, said Alison Haddock, president of ACEP.
“It’s important that folks in those areas have equal access to high-quality emergency care to the greatest extent possible,” Haddock said.
Other health care providers and organizations say advanced-practice providers with the right experience and support are capable of overseeing ERs. And they say mandating that a physician be on-site could drive some rural hospitals to close because they can’t afford or recruit enough тАФ or any тАФ doctors.
“In an environment, especially a rural environment, if you have an experienced PA who knows what they know, and knows the boundaries of their knowledge and when to involve consultants, it works well,” said Paul Amiott, a board member of the Society of Emergency Medicine PAs.
“I’m not practicing independently” despite working 12-hour night shifts without physicians on-site at critical access hospitals in three states, he said.

Amiott said he calls specialists for consultation often and about once a month asks the physician covering the day shift at his hospital to come help him with more challenging cases such as emergency childbirth and complicated trauma. Amiott said this isn’t unique to PAs тАФ ER doctors seek similar consultations and backup.
The proportion of ERs without an attending physician always on-site varies wildly by state. The 2022 survey found that 15 states тАФ including substantially rural ones, such as New Mexico, Nevada, and West Virginia тАФ had no such emergency departments.
But in the Dakotas, more than half of emergency departments were running without 24/7 attending physician staffing. In Montana it was 46%, the third-highest rate.
None of those three states have a program to train physicians as ER specialists. Neither does Wyoming or Idaho.
But Sanford Health, which bills itself as “the largest rural health system in the United States,” is launching an emergency medicine residency in the region. The Sioux Falls, South Dakota-based program is intended to boost the ranks of rural emergency doctors in those states, the residency director said in .
Leon Adelman is an emergency medicine physician in Gillette, Wyoming, which, at around 33,800 residents, is the largest city in the state’s northeast. Working in such a rural area has given him nuanced views on whether states should require 24/7 on-site physician coverage in ERs.
Adelman said he supports such laws only where it’s feasible, like in Virginia. He said the state’s emergency physicians’ organization pushed for the law only after doing research that made it confident that the requirement wouldn’t shutter any rural hospitals.
Camargo said some doctors say that if lawmakers are going to require 24/7 on-site physician coverage in ERs, they need to pay to help hospitals implement it.
Adelman said when instituting staffing requirements isn’t possible, states should create other regulations. For example, he said, lawmakers should make sure hospitals not hiring physicians aren’t refraining just to save money.
He pointed to Vermont, where recommended that several of the state’s hospitals cut physicians from their ERs. The report was part of a mandated process to improve the state’s .
Adelman said states should also require PAs and NPs without on-site physician supervision to have extensive emergency experience and the ability to consult with remote physicians.
Some doctors have pointed to in which a 19-year-old woman died after being misdiagnosed by an NP who was certified in family medicine, not emergency care, and working alone at an Oklahoma ER. Few NPs have emergency certification, .


The Society of Emergency Medicine PAs PAs should have before practicing in rural areas or without on-site doctors.
Haddock said emergency physicians have seen cases of hospitals hiring inexperienced advanced-practice providers. She said ACEP is asking the federal government to require critical access and rural emergency hospitals to have physicians on-site or on call day and night.
Haddock said ACEP wouldn’t want such a requirement to close any hospital and noted that the organization has various efforts to keep rural hospitals staffed and funded.
Dahl Memorial Hospital has strict hiring requirements and robust oversight, said Dowdy, who previously worked for 14 years in high-volume, urban emergency rooms.
She said ER staffers can call physicians when they have questions and that a doctor who lives on the other side of Montana reviews all their patient treatment notes. The ER is working on getting virtual reality glasses that will let remote physicians help by seeing what the providers in Ekalaka see, Dowdy said.
She said patient numbers in the Ekalaka ER vary but average one or two a day, which isn’t enough for staff to maintain their knowledge and skills. To supplement those real-life cases, providers visit simulation labs, do monthly mock scenarios, and review advanced skills, such as using an ultrasound to help guide breathing tubes into patient airways.
Dowdy said Dahl Memorial hasn’t had a physician in at least 30 years, but CEO Darrell Messersmith said he would hire one if a doctor lived in the area. Messersmith said there’s a benefit to having advanced-practice providers with connections to the region and who stay at the hospital for several years. Other rural hospitals, he noted, may have physicians either as permanent staff who leave after a few years or contract workers who fly in for a few weeks at a time.
People eating at Ekalaka’s sole breakfast spot and attending appointments at the hospital’s clinic all told ║┌┴╧│╘╣╧═Ї News that they’ve been happy with the care they have received from Dowdy and her co-workers.
Ben Bruski had to visit the ER after a cow on his family ranch kicked a gate, smashing it against his hand. And he knows other people who’ve been treated for more serious problems.
“We’ve got to have this facility here because this facility saves a lot of lives,” Bruski said.

This <a target="_blank" href="/rural-health/rural-emergency-rooms-ers-no-doctors-pas-nps-south-dakota-wyoming-montana/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2071014&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>During a typical shift, she shows up at her clients’ home at 10 p.m. She answers questions they may have about basic infant care and keeps an eye out for signs of postpartum depression.
After bedtime, she may feed the baby a bottle or wake the mother to breastfeed. She soothes the infant back to sleep. Sometimes, she prepares meals for the family in a Crock-Pot or empties the dishwasher.
She leaves the following morning and returns, often nightly, for two or three weeks in a row.
“I’m certified to do all of it,” said Oliver, of Hardeeville, South Carolina, who runs Compassionate Care Doula Services. It takes a village to raise a child, as the adage goes, but “the village is not what it used to be,” Oliver said.
Doulas are trained to offer critical support for families тАФ before delivery, during childbirth, and in those daunting early days when parents are desperate for sleep and infants still wake up around the clock. While doulas typically don’t hold a medical or nursing degree, research shows they can improve health outcomes and reduce racial health disparities.
Yet their services remain out of reach for many families. Oliver charges $45 an hour overnight, and health insurance plans often don’t cover her fees. That’s partly why business “ebbs and flows,” Oliver said. Sometimes, she’s fully booked for months. Other times, she goes several weeks without a client.
That may soon change.
Two bipartisan bills, introduced in separate chambers of the South Carolina General Assembly, would require both Medicaid, which pays for more than half of all births in the state, and private insurers to cover the cost of doula services for patients who choose to use one.
South Carolina isn’t an outlier. Even as states in federal Medicaid funding over the next decade, legislatures across the country continue to pass laws that grant doula access to Medicaid beneficiaries. Some state laws already require private health insurers to do the same. Since the start of 2025, Vermont lawmakers, alongside Republican-controlled legislatures in Arkansas, Utah, Louisiana, and Montana, have passed laws to facilitate Medicaid coverage of doula services.
All told, more than 30 states are reimbursing doulas through Medicaid or are implementing laws to do so.
Notably, these coverage requirements align with one of the goals of Project 2025, whose “Mandate for Leadership” report, published in 2023 by the conservative Heritage Foundation, offered a blueprint for President Donald Trump’s second term. The document calls for increasing access to doulas “for all women whether they are giving birth in a traditional hospital, through midwifery, or at home,” citing concerns about maternal mortality and postpartum depression, which may be “worsened by poor birth experiences.” The report also recommends that federal money not be used to train doctors, nurses, or doulas to perform abortions.
The Heritage Foundation did not respond to an interview request.
Meanwhile, the idea that doulas can benefit babies, parents, and state Medicaid budgets by reducing costly cesarean sections and preterm birth complications is supported by a growing body of research and is gaining traction among conservatives.
published last year in the American Journal of Public Health found that women enrolled in Medicaid who used a doula faced a 47% lower risk of delivering by C-section and a 29% lower risk of preterm birth. They were also 46% more likely to attend a postpartum checkup.
“Why wouldn’t you want somebody to avail themselves of that type of care?” said Republican state Rep. Tommy Pope, who co-sponsored the doula reimbursement bill in the South Carolina House of Representatives. “I don’t see any reason we shouldn’t be doing that.”
Pope said his daughter-in-law gave birth with the assistance of a doula. “It opened my eyes to the positive aspects,” he said.
Amy Chen, a senior attorney with the National Health Law Program, which tracks doula reimbursement legislation around the country as part of its , said lawmakers tend to support these efforts when they have a personal connection to the issue.
“It’s something that a lot of people resonate with,” Chen said, “even if they, themselves, have never been pregnant.”
Conservative lawmakers who endorse state-level abortion bans, she said, often vote in favor of measures that support pregnancy, motherhood, and infant health, all of which these doula reimbursement bills are intended to do.
Some Republicans feel as if “they have to come out in favor of that,” Chen said.
Health care research also suggests that Black patients, who suffer maternal and infant mortality rates than white patients, may particularly benefit from doula care. In 2022, Black infants in South Carolina were more than twice as likely to die from all causes before their 1st birthday as white infants.
That holds true for women in where labor and delivery services have either closed or never existed.
That’s why Montana lawmakers passed a doula reimbursement bill this year тАФ to narrow health care gaps for rural and Indigenous communities. To that end, in 2023, the state enacted a bill that requires Medicaid to reimburse midwives for home births.
Montana state Sen. Mike Yakawich, a Republican who backed the Democratic-sponsored doula reimbursement bill, said pregnant women should have someone to call outside of a hospital, where health care services can be costly and intimidating.
“What help can we provide for moms who are expecting? My feeling is, it’s never enough,” Yakawich said.
Britney WolfVoice lives on the Northern Cheyenne Indian Reservation in southeastern Montana, about two hours from the closest birthing hospital. In early July, she was seven months pregnant with her fourth child, a son, and said she planned to have a doula by her side for the second time in the delivery room. During WolfVoice’s previous pregnancy, an Indigenous doula named Misty Pipe brought cedar oil and spray into the delivery room, rubbed WolfVoice’s back through contractions, and helped ensure WolfVoice’s husband was the first person their daughter saw.
“Being in a hospital, I felt heard for the very first time,” WolfVoice said. “I just can’t explain it any better than I felt at home. She was my safe place.”
Pipe said hospitals are still associated with the government forcibly removing children from Native American homes as a consequence of colonization. Her goal is to help give people a voice during their pregnancy and delivery.
Most of her clients can’t afford to pay for doula services out-of-pocket, Pipe said, so she doesn’t charge anything for her birth services, balancing her role as a doula with her day job at a post office.
“If a mom is vulnerable, she could miss a prenatal appointment or go alone, or I can take time off of work and take her myself,” Pipe said. “No mom should have to birth in fear.”
The new state law will allow her to get paid for her work as a doula for the first time.
In some states that have enacted such laws, initial participation by doulas was low because Medicaid reimbursement rates weren’t high enough. Nationally, doula reimbursement rates are improving, Chen said.
For example, in Minnesota, where in 2013 lawmakers passed one of the first doula reimbursement bills, Medicaid initially paid only $411 per client for their services. Ten years later, the state had raised the reimbursement rate to a maximum of $3,200 a client.
But Chen said it is unclear how might affect the fate of these state laws.
Some states that haven’t passed doula reimbursement bills, including South Carolina, might be hesitant to do so in this environment, she said. “It’s just a really uncertain time.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/doula-medicaid-state-laws-bipartisan-project-2025-south-carolina-montana/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2057015&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Now, as Congress steamrolls toward passing historic Medicaid cuts of about through Trump’s tax and spending legislation, red-state governors are saying little publicly about what it does to health care тАФ even as they face reductions that will punch multibillion-dollar holes in their states’ budgets.
Medicaid, a program jointly run by states and the federal government, covers more than 70 million low-income or disabled people, including nearly half of the nation’s children. Republicans say the $900 billion-a-year program was allowed to grow too large under Democrats Barack Obama and Joe Biden by adding nondisabled adults they say , and they have long sought to scale it back.
Some of the biggest health cuts in the legislation Trump calls the “One Big Beautiful Bill” are achieved through new policies that would reduce enrollment by imposing more paperwork demands on enrollees, including a requirement that many prove they’re working. Those policies would affect only states that expanded Medicaid to more low-income people under the Affordable Care Act.
Nineteen of those states are . Their silence on the bill’s health measures is giving political cover to GOP lawmakers from their states as they seek to cut Medicaid coverage for millions of people who gained it within the last decade.
║┌┴╧│╘╣╧═Ї News contacted all 19 governors for comment on the legislation’s Medicaid cuts. Only six responded. Most said they backed imposing a work requirement on adult Medicaid enrollees.
“Implementing work requirements for able-bodied adults is a good and necessary reform so that Medicaid is being used for temporary assistance and not a permanent entitlement,” said Drew Galang, a spokesperson for Gov. Patrick Morrisey of West Virginia.
“Governor Rhoden supports workforce participation as a requirement of Medicaid expansion eligibility,” said Josie Harms, a spokesperson for South Dakota Gov. Larry Rhoden, adding that congressional lawmakers have the governor’s support: “South Dakota has an excellent federal delegation, and Governor Rhoden trusts them to fight for South Dakota’s priorities while delivering on President Trump’s promises.”
In a sign of how the political winds have changed, none of the governors said anything about another of the legislation’s significant cuts, to provider taxes тАФ a tool that nearly all of their states use to help pay their share of Medicaid and gain additional funds from the federal government. That change is expected to cost states billions.
No Longer a Bipartisan Issue
In contrast to the radio silence from GOP governors, Democratic governors have campaigned against the megabill for weeks.
Pennsylvania Gov. Josh Shapiro posted that Trump and congressional Republicans were misleading Americans by saying they were cutting only waste, fraud, and abuse in Medicaid.
“They’re rushing to kick hundreds of thousands of Pennsylvanians off their healthcare тАФ and lying about it,” he posted. “The damage this will do here in Pennsylvania and across America is staggering and will be felt for years to come.”
In New York, Gov. Kathy Hochul on July 1 charged that Trump’s legislation would devastate hospitals and could lead to more than 34,000 job cuts in her state.
“The collective impact of the GOP reconciliation bill in Washington, D.C., could force hospitals to curtail critically needed services such as maternity care and psychiatric treatment, not to mention to downsize operations, and even close entirely,” she said .
In 2017, the chorus was bipartisan, as Republican governors in , , and spoke out against cutting Medicaid. Trump’s bill to repeal much of the Affordable Care Act and roll back its Medicaid expansion narrowly failed in the Senate.
“It’s been surprising that red-state governors, particularly those in Medicaid expansion states, haven’t spoken out against Medicaid cuts,” said Larry Levitt, executive vice president for health policy at KFF, a health information nonprofit that includes ║┌┴╧│╘╣╧═Ї News. “Republican governors were a potent political force in the failed 2017 effort to repeal and replace the ACA, including Medicaid expansion.”
What’s changed since 2017, policy experts say, is that there are fewer moderate Republican governors, and GOP state executives who advocated for Medicaid expansion over a decade ago are no longer in office.
Additionally, seven of the then-red states that expanded Medicaid , mostly over opposition from their governors.
In fact, the Medicaid work requirement is backed by many Republican governors, even if it means less federal Medicaid money and leads to fewer people covered.
Several states, including Arkansas and Ohio, have already passed state laws to implement a requirement that adults enrolled under the ACA’s Medicaid expansion work, volunteer, go to school, or participate in job training. Most states have yet to bring work requirement programs to fruition because they are waiting for federal government approval.
Charles “Chip” Kahn, president of the Federation of American Hospitals, a trade group of investor-owned hospitals, said that while fewer governors have engaged publicly in trying to block Medicaid cuts under the bill, federal lawmakers are hearing from legislators in their states.
A political dilemma for Republican governors is that, unlike in 2017, the bill before Congress is not legislation aimed expressly at repealing Obamacare. With a scope broader than health care, it would extend many of Trump’s tax cuts and direct billions in new spending toward border security, immigration enforcement, and the military, while also cutting health care spending.
“It’s like playing multidimensional chess rather than focusing on one issue,” Kahn said.
, director of the Center for the Study of Politics and Governance at the University of Minnesota, said some Republican governors may have expressed concerns privately to their states’ GOP senators but are not speaking out publicly for fear of drawing Trump’s wrath.
“Why are they being cagey? Trump and not wanting to be тАШLiz Cheney’d,’” Jacobs said, referring to the Republican former Wyoming lawmaker whom Trump helped oust after she served as vice chair of an inquiry into his attempts to overturn the results of the 2020 election.
Walking Political Tightropes
The political peril Republican lawmakers face in publicly challenging Trump remains explicit. On June 29, Sen. Thom Tillis (R-N.C.) announced he would not run for reelection after he voiced concerns about the bill and the president threatened to back a primary challenger. Tillis was one of three GOP senators to vote against it on July 1, though it still narrowly passed.
In addition to the work requirement, the biggest Medicaid cuts in the bill stem from its restrictions on provider taxes тАФ levies that states impose on hospitals, nursing homes, and other health care institutions to help increase their federal reimbursement. Much of the additional money is then returned to the health care providers in the form of higher payments for their Medicaid patients.
The practice, which has been adopted in every state but Alaska, has been criticized by some Beltway Republicans as “money laundering” тАФ even though the taxes are approved by state lawmakers and the federal Centers for Medicare & Medicaid Services and have been allowed under federal law for decades.
The Senate bill would limit the money states could raise тАФ a move that would mean billions in funding cuts to states and their hospitals.
The states with Republican governors that expanded Medicaid are Alaska, Arkansas, Idaho, Indiana, Iowa, Louisiana, Missouri, Montana, Nebraska, New Hampshire, Nevada, North Dakota, Ohio, Oklahoma, South Dakota, Vermont, Virginia, West Virginia, and Utah.
One of the governors who expressed concerns about repealing the Obamacare Medicaid expansion in 2017 was Jim Justice of West Virginia, a Democrat at the time.
In a to West Virginia Sen. Shelley Moore Capito, a Republican, Justice wrote: “Since so many of our people count on Medicaid, any cut to Medicaid would destroy families in West Virginia.” He added that “the consequences would be beyond catastrophic.”
On July 1, Justice тАФ elected to the Senate as a Republican last year тАФ voted for Trump’s megabill, including its Medicaid cuts.
“The Senator believes this bill strikes a good balance between protecting the most vulnerable and those who rely on the program while rooting out waste, fraud, and abuse to ensure the program is run efficiently for those deserving,” William O’Grady, a Justice spokesperson, said in an email July 2.
║┌┴╧│╘╣╧═Ї News correspondent Arielle Zionts contributed to this report.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/big-beautiful-bill-trump-medicaid-affordable-care-act-cuts-republican-gop-governors/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2056990&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>



