Hunt died five days later. Her death certificate said the foot injury was a “significant” factor. Genesis denied wrongdoing but agreed to pay $3.5 million in a settlement Hunt’s son signed in August 2024.
Yet Genesis hasn’t paid most of that debt, court records show. It may never have to.
Once the nation’s largest nursing home chain, it was spending $8 million a month defending and settling lawsuits over resident injuries and deaths in recent years. But the company is now poised to wipe the liability slate clean by seeking refuge in the most protective corner of the legal system for the nursing home industry: bankruptcy court.
The Genesis case, one of 11 large senior care bankruptcies this year, illustrates how health care companies can dodge public and financial accountability for alleged negligence through delays, confidentiality clauses, and bankruptcy maneuvers, a ║┌┴╧│╘╣╧═Ї News investigation found.
When it filed for bankruptcy in Dallas in July, Genesis estimated its total liability for nearly a thousand settled and pending lawsuits at $259 million. A ║┌┴╧│╘╣╧═Ї News review of the terms of 155 settlement agreements and shows Genesis officials knew insolvency was possible yet included provisions in its settlement agreements allowing it to defer payment, often for a year or more.
As a result, Genesis paid nothing in 85 cases and only a portion in the other 70, according to civil court records and bankruptcy claims made available through people with access to them. It still owes $41 million of the $58 million it had agreed to pay in those cases, the records show.

“It just feels like they killed my mom and got away with it,” said Vanessa Betancourt, whose mother, Nellie Betancourt, a retired nurse, fractured her hip at a Genesis home in Albuquerque, New Mexico — an injury the medical examiner’s report said led to her death. Genesis agreed to a $650,000 settlement with Betancourt’s family in April under the condition it would not need to pay the first of seven installments for another year, according to the settlement document.

Genesis denied wrongdoing in all lawsuits and settlements. In a written statement, the company did not answer questions about individual personal injury cases. The statement said Genesis remained “focused on delivering high-quality, compassionate care to our patients and residents without disruption” during bankruptcy.
One lawsuit Genesis settled for nearly $1 million alleged nursing home managers ignored repeated warnings about a male resident’s behavior before he sexually assaulted a female Alzheimer’s patient, according to court records. In a case the company resolved for $500,000, a Genesis nursing home was accused of delaying the hospitalization of a resident who had vomited brown mucus. He died of a bowel obstruction. Genesis has paid nothing for either settlement, according to bankruptcy claims.
Creditors, including families of the deceased, are expected to salvage a fraction of what they were promised, if anything. On Dec. 10, the company’s owners were scheduled to seek approval by the U.S. Bankruptcy Court for the Northern District of Texas to sell its nursing homes and other assets to its largest investor, a private equity firm. In court papers, lawyers for residents and other creditors say the complex plan will from pursuing Genesis’ new ownership and other companies the company’s collapse.
John Anthony, a bankruptcy attorney representing 340 personal injury claims against Genesis, said, “They never had any intention to honor these deals.”
Low Ratings and Fines
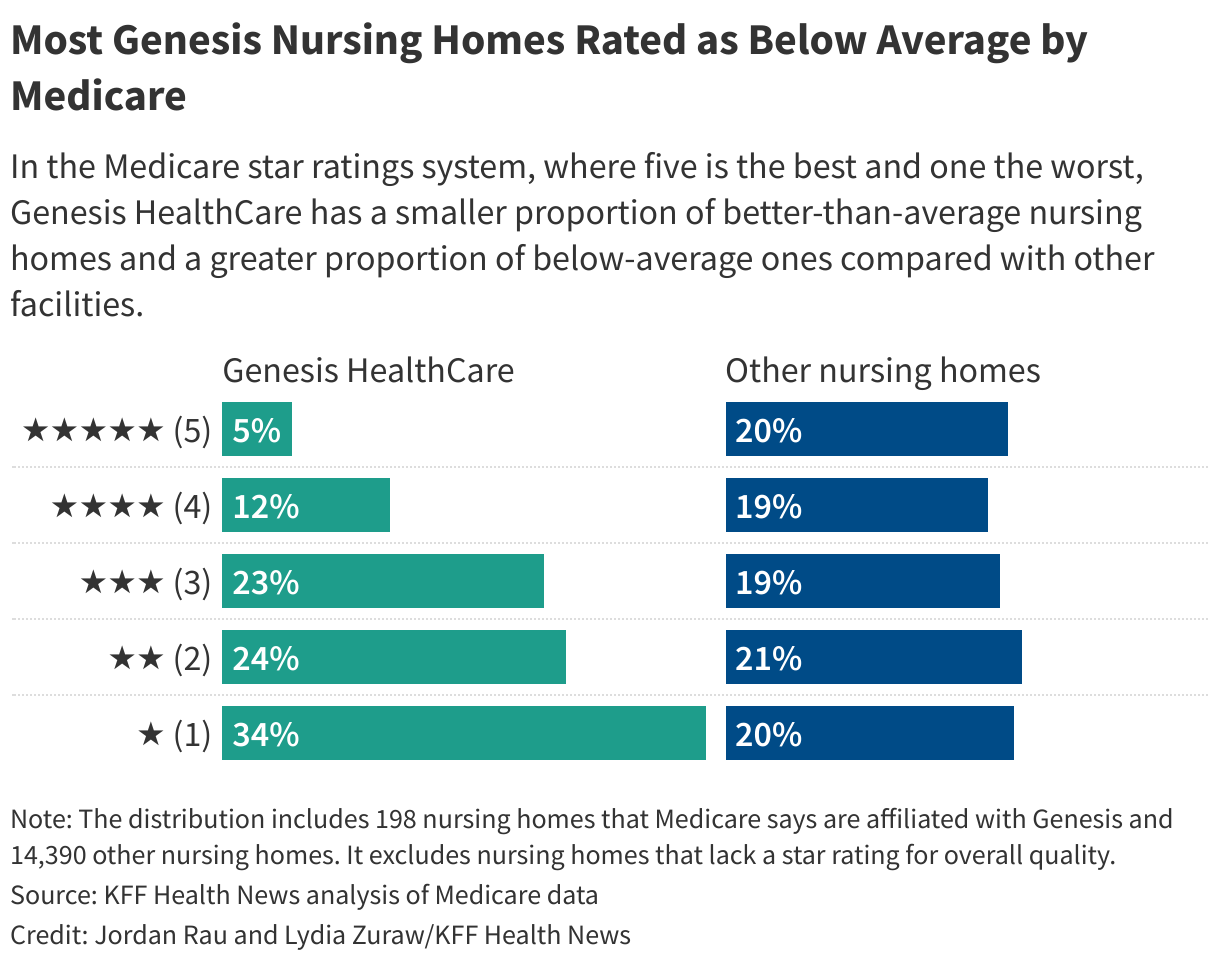
During years of financial turmoil, Genesis has frequently struggled to provide top-notch care, federal records show. Using its five-star system, the Centers for Medicare & Medicaid Services affiliated with Genesis as below average or much below average. CMS Genesis homes $10 million for violating federal health standards over the past three years.
In 2022, a Genesis home after two deaths and multiple violations. The company this year after residents twice were evacuated over safety concerns.
In its filing, Genesis said it cared for about 15,000 residents in 165 nursing homes and 10 assisted living facilities in 18 states. They are centered in Pennsylvania, West Virginia, New Mexico, New Hampshire, New Jersey, Maine, Alabama, Maryland, and North Carolina, according to the bankruptcy filing.
The company said it owed $709 million in secured debt to lenders and the IRS. Under bankruptcy rules, those debts, backed by Genesis collateral, take precedence over the $1.6 billion in unsecured debt Genesis said it owes. Unsecured creditors include a pension fund; contractors that provided health services and equipment; Pennsylvania, New Mexico, and West Virginia for unpaid provider taxes; and former residents and their families who sued.
Dangers in Memory Care
Sandia Ridge Center, a Genesis home in Albuquerque, was repeatedly faulted by health regulators for not preventing sexual misbehavior in its memory care unit. In November 2021, CMS for lacking enough nurses to prevent sexual abuse among residents. An inspection report the following August inappropriate sexual contact. Police were called to investigate sexual assault allegations in and of 2023, police reports show; neither resulted in criminal charges.
Then in April 2023, a 61-year-old male resident with alcohol-related dementia sexually assaulted a female resident with Alzheimer’s in the dining room, according to a and an . When the resident screamed for him to stop and that he was hurting her, he responded “shut up bitch I know you like this,” according to a lawsuit brought on behalf of the woman, identified in court papers as R.S.
Sandia Ridge management had been aware of the male resident’s behavioral issues for months, according to employee depositions in the case. Police had investigated a against him the previous year without bringing charges. In one deposition, a former activities assistant testified he hit her and twice pushed her into a bathroom while announcing, “I want to have sex with you.” When she reported him to a senior Genesis manager, she said in the deposition, the manager put his finger over his lips and said, “Shhh.”
The activities worker testified that R.S. used to happily sing along with Elvis Presley songs. After the assault, the worker said, R.S. “don’t sing anymore.”
Inspectors cited the home for failing to protect R.S. The same report said the home didn’t provide a therapist for another female resident who was being sexually harassed. Medicare fined Sandia Ridge Center $91,247. Genesis denied liability but settled R.S.’ lawsuit for $925,000 in May, according to the bankruptcy claim.
“We just felt we have to hold them accountable,” R.S.’ daughter said in an interview, speaking on the condition that she and her mother not be identified, because of the nature of the assault. “Maybe I’m wrong, maybe I’m naive, but the only way to do that is to sue someone, right?”
Genesis has not paid any of the settlement, according to the family’s claim filing.

Growth and Debt
Genesis’ downfall can be , when affiliates of two private equity firms acquired the company in a $1.5 billion leveraged buyout, taking on substantial debt, according to its bankruptcy filing. Private equity also has been involved in other health care bankruptcies, including those of the nursing home chain, the prison health care contractor , and two for-profit hospital systems, and .
In 2011, Genesis raised $2.4 billion by transferring substantially all its nursing home buildings and other real estate to Welltower, a publicly traded real estate investment trust, according to Genesis’ bankruptcy filing. Genesis then rented the buildings back from Welltower, which made leasing costs a significant expense.
Genesis went on a nationwide buying spree. At its peak in 2016, it had grown to more than 500 nursing homes. In a court declaration, Louis Robichaux IV, a consultant overseeing Genesis’ bankruptcy restructuring, wrote that as the company expanded, it became harder to manage and “mired in corporate inefficiencies.” Robichaux wrote that Genesis’ financial woes were exacerbated by rapidly increasing labor costs and lawsuits, including some predating the covid pandemic.
Starting in 2021, Genesis avoided bankruptcy after from a founded by Joel Landau, the owner of a , according to Robichaux’s filing.
But Genesis continued to teeter on the edge of insolvency. In for 2022 and 2023 submitted to a California oversight agency, management and auditors said rent and debt obligations raised “substantial doubt about the company’s ability to continue as a going concern.”
In a court filing, a committee appointed by the U.S. Trustee’s Office to represent the unsecured creditors in the bankruptcy accused Landau and Welltower of that allowed Welltower to keep getting its rents while Landau could run the company and “siphon value to himself.” The committee alleged their efforts forced the company into insolvency while “staffing levels and patient care declined precipitously.” Landau and Welltower did not respond to requests for comment.
Drawn-Out Lawsuits
Erin Pearson sued Genesis over the death of her father, James Sanderson, a retired mining company executive who died in 2018 after spending less than a month at Bear Canyon Rehabilitation Center in Albuquerque. In the memory care unit, Sanderson fell repeatedly, suffered medication errors made by nursing home staff, and developed a bowel obstruction and sepsis, according to the lawsuit, filed in 2019. Pearson’s lawyers said he was not hospitalized until eight days after nurses noticed he was vomiting brown mucus.

After the judge rejected Genesis’ request to force Pearson into arbitration, Genesis appealed. It took 2½ years before an appeals court affirmed the original decision to let the case go forward in court, records show.
This past May, more than five years after suing, Pearson reached a $500,000 settlement, with the first payment required by November, according to a copy of the agreement. Nothing was paid, according to the bankruptcy claim.
“It was so drawn out and for so long,” Pearson said in an interview, calling Genesis’ bankruptcy “despicable.”
Payouts Postponed
Jennifer Foote, an Albuquerque attorney who represents clients in multiple lawsuits against Genesis, including Pearson’s, said the company frequently filed appeals. “They did not usually win them on these issues,” she said, “and our sense was that they were doing it as a delay tactic.”
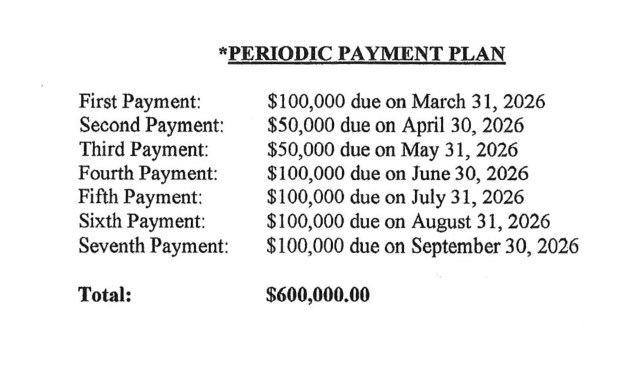

Genesis started using installment payments around 2018, said Dusti Harvey, Foote’s law partner. “The payments wouldn’t start for several months out,” Harvey said. Foote said Genesis’ lawyers often wanted to time the payments to start the month the trial in the case was scheduled to occur.
Families had to wait even when comparatively small amounts of money were involved, settlement agreements show. Genesis’ settlement agreements also included a confidentiality clause prohibiting discussion of the incidents.
Genesis agreed to pay $42,000 in a November 2024 settlement, but the first payment was not due until nine months later. It was not paid, according to the bankruptcy claim.
A $250,000 settlement signed in October 2023 did not start paying out until the following September. When Genesis declared bankruptcy — 21 months after the case was resolved — it still owed $100,000, according to the family’s claim.
‘We Never Found Out the Truth’
Settling cases allowed Genesis to avoid the expense and publicity of a trial, at which details of how its nursing homes functioned might have been revealed. In October 2020, Margarett Johnson, a retired school bus driver, fell out of her wheelchair at a Genesis nursing home in Waldorf, Maryland, fracturing her jawbone, nose, and neck, according to a lawsuit brought by her family. Johnson was sent to a trauma center and placed on a ventilator. She died three months later, at age 76, from ventilator-associated pneumonia, the lawsuit said.
“It looked like she was hit by a truck,” Angelina Harley, one of her daughters, said in an interview. “I knew my mom was not going to come home. I knew the Lord was not going to punish her more.”

The company denied negligence and blamed the accident on Johnson’s jacket getting tangled in the wheel of her wheelchair, according to the lawsuit. Harley and her sister Angela Swann were dubious.
“We never found out the truth,” Harley said. “They wanted to settle out of court.”
The company denied liability but agreed to a $950,000 settlement in October 2024. It never paid the final $112,500 installment, according to a letter Johnson’s five children sent to the bankruptcy judge.
“If you settle out of court, you know doggone well you did something wrong,” Harley said.
Maddening Judges
By summer 2025, judges in some civil cases had run out of patience.
Alma Brown, a retired day care manager and accordion teacher living in a Genesis nursing home in Clovis, New Mexico, suffered falls, infections, bedsores, and other neglect that hastened her death in 2023, according to her estate’s lawsuit. In Santa Fe District Court, Judge Kathleen McGarry Ellenwood castigated Genesis after it failed to pay $2 million of the $3 million settlement to Brown’s estate or explain the delay.
Genesis “obviously benefited by not having to go to trial,” McGarry Ellenwood said in one hearing, according to a court transcript. “They assure me that they’re not trying to renege on their contract, but it certainly seems like they haven’t lived up to what the bargain was.”
Genesis declared bankruptcy the day McGarry Ellenwood announced she would impose more than $100,000 in fines, plus $10,000 more each day until the settlement was paid.
In Pennsylvania, Greg Hunt petitioned a judge to punish Genesis after it stopped payments of the $3.5 million settlement after the death of his mother, Nancy, the resident with the gangrenous foot. She had spent eight months in 2019 at Brandywine Hall, a Genesis facility in West Chester that was later sold and renamed.
In a filing with the Common Pleas Court of Montgomery County, Genesis admitted it was in arrears but asked the judge for more time, citing “unforeseen and exigent financial challenges.” Genesis said care for patients at its nursing homes would suffer if it had to pay immediately.
Unswayed, Judge Richard Haaz in June ordered Genesis to pay up, along with punitive interest. But the bankruptcy court stayed that order. Genesis still owes $1.4 million of the $2 million it was supposed to pay, according to Hunt’s claim. (The rest of the $3.5 million settlement is supposed to be paid by an insurer in January 2026.) Ian Norris, Hunt’s lawyer, declined to comment, citing confidentiality provisions in the settlement.
Court records indicate Genesis lawyers never disclosed in either case that it was preparing to declare bankruptcy.
‘Bankruptcy as a Tool’
In the first nine months of 2025, 10 other senior living companies with liabilities over $10 million entered Chapter 11 bankruptcy, according to , a consulting firm.
Hamid Rafatjoo, a bankruptcy lawyer representing nursing homes who is not involved in the Genesis bankruptcy case, said filings may increase as the industry has become costlier to run and class action lawsuits have become a fixture.
“Nursing homes get sued all the time for everything,” Rafatjoo said. “A lot of operators wait too long to use bankruptcy as a tool.”
On Dec. 1, Genesis announced the , saying it had elected to to a private equity firm controlled by Landau. In a court filing, Anthony, the attorney for the personal injury claimants, in Landau’s favor despite an “objectively better and higher competing bid” from another private equity investor that would have provided more money to creditors. Genesis said in its statement that Landau’s group had increased its bid during the auction.
Sen. Elizabeth Warren (D-Mass.) and two other senators last month to intervene in the case, out of concern that “individuals who already own or control Genesis are trying to sell it to themselves, wiping away legal and other creditor debts in the process.” Lawyers representing those in charge of the auction did not respond to a request for comment.
Families of former Genesis residents said they fear the capacity to purge lawsuits through bankruptcy emboldens nursing home owners who provide deficient care.
“They can file bankruptcy again,” said Gabe Betancourt, whose wife, Nellie, died after her stay at Uptown Rehabilitation Center in Albuquerque. “And we’re the ones that will pay for it, with our memories, our lives.”

This <a target="_blank" href="/aging/nursing-homes-genesis-bankruptcy-liability-settlements-dallas-new-mexico/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2129309&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>║┌┴╧│╘╣╧═Ї News chief Washington correspondent Julie Rovner appeared Oct. 6 on the podcast “” to discuss TrumpRx, President Donald Trump’s proposal for a direct-to-consumer website aimed at lowering prescription drug costs.
While few details were made public when the program was announced on Sept. 30, Rovner explains that consumers who are enrolled in health plans through their employers or government programs may save more money on drugs using their insurance or drugmakers’ patient discount programs.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/julie-rovner-today-explained-podcast-trumprx-announcement-prescription-drug-costs/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2098911&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
The number of people receiving treatment at the National Institutes of Health Clinical Center тАФ the renowned research hospital that cares for patients with rare or life-threatening diseases тАФ has tumbled under the second Trump administration, according to government documents and interviews with current and former NIH employees.
NIH documents viewed by ║┌┴╧│╘╣╧═Ї News show a pronounced decline in patients at the 200-bed hospital from February through April, a time that coincides with the Department of Health and Human Services’ mass firings of government employees, the gutting of scientific research, and the administration’s broad crackdown on immigration. The average number of patients being treated daily during that time hovered between 60 and 80, with the April numbers falling to the lower end of that range. By contrast, in October, about 80 patients a day on average were at the hospital.
The number of cancer clinical trial participants at the hospital as of July was down about 20% from last year, one NIH cancer scientist said. ║┌┴╧│╘╣╧═Ї News agreed not to identify the scientist and others who participated in this article who were not authorized to speak to the press and feared retaliation.
The numbers “really don’t look too good,” Pius Aiyelawo, acting CEO of the clinical center, said during a May 23 meeting of the NIH Clinical Center Research Hospital Board.
As of April 30, the average number of patients in the hospital per day had declined by 5.7% from the same period a year ago.

Adults and children with cancer, people who need bone marrow transplants, and people with rare diseases or infections are among the patients who receive care at no charge at the NIH hospital, according to former officials. Clinicians there provide potentially lifesaving treatments as part of clinical trials, often to people who have run out of options.
Research at the hospital has also led to breakthroughs about cancer, traumatic brain injury, and AIDS, among other ailments. James Gilman, a physician who was CEO of the clinical center from 2017 until retiring in January, said the center has driven important advances against disease “that couldn’t have happened anywhere else.”
Former officials said the drop in patients this year is a consequence of the upheaval the Trump administration has caused at the NIH, the world’s largest public funder of scientific research.
Current and former employees say an exodus of clinicians, scientists, and other staffers has limited how many patients can be treated. Morale has tanked because of widespread firings and the administration’s cancellation of grants that funded research into health disparities, vaccines, the health of LGBTQ+ people, and more. Contracts have been cut, and scientists have seen delays in getting essential supplies for clinical research.
“Every day seems to be some type of breaking point,” one NIH worker said.
During the May board meeting, a video of which ║┌┴╧│╘╣╧═Ї News viewed, Aiyelawo attributed the decrease in patients coming to the hospital to the departure of NIH investigators тАФ the researchers on studies тАФ and less patient recruitment. He also noted 11 recent departures of clinical center staffers. They included Christine Grady, a nurse who led the center’s bioethics department and the wife of Anthony Fauci, the former head of the NIH’s infectious diseases institute who became a lightning rod for conservatives during the covid pandemic.
HHS has fired more than 1,200 NIH employees this year as part of its purge of the federal workforce, but the true number of departures is almost certainly higher. Others have opted for early retirement or quit because they opposed the Trump administration’s orders.
Gilman said the NIH hospital relies on a “very complex ecosystem and network to find patients who are not too sick” to potentially be enrolled in a clinical trial. When researchers leave, “those patients are lost,” he said.
The clinical center’s 2025 said there were roughly 1,500 research studies underway in 2024, including studies focused on cancer, infectious disease, heart and lung conditions, and blood disorders. Clinical trials accounted for about half.
The National Cancer Institute тАФ which is the largest of the NIH’s 27 institutes and has been crippled by cuts and chaos this year тАФ typically has the most patients needing inpatient care, Gilman said.
“What has happened here since January has been a pretty traumatic time for that ecosystem,” he said, “and there are pieces of it that will take a long time to rebuild, if indeed they get a chance to rebuild.”
During the May board meeting, Aiyelawo said NIH Director Jay Bhattacharya “is very aware” that fewer people are getting treated at the hospital “and we’re doing everything we can to be able to get those numbers up.”
The drop in patients this year isn’t isolated to people needing inpatient care, NIH documents show. As of the end of April, outpatient visits were down 8.5% from the same period in the prior fiscal year. The number of new patients overall had declined by 6.7%, to about 3,370 people.
In response to questions, HHS spokesperson Andrew Nixon wrote in an emailed statement that the clinical center “remains fully operational and continues to provide world-class clinical research and patient care. Every day, patients from across the country and around the globe come here to participate in cutting-edge studies that drive scientific discovery and improve health outcomes.”
“As the crown jewel of research and discovery, the Clinical Center is a top priority” under Bhattacharya’s leadership, Nixon said. “We are committed to fully leveraging its capabilities as the nation’s hub for clinical research innovation. Our focus remains on empowering the research community and advancing the critical mission of making medical breakthroughs possible right here on the NIH campus.”

Even before President Donald Trump began his second term, the hospital had struggled with lagging patient numbers. Before the pandemic, it averaged more than 110 patients daily. Those numbers plummeted starting in 2020, government documents show. During the 2022 fiscal year, there were about 73 patients, on average, in the hospital per day.
While yearly figures have increased since then, they have not gone back to pre-pandemic levels. NIH documents show that the hospital saw an average of roughly 81 patients a day during fiscal 2024, which ended in September. Still, one NIH worker said: “This is a manufactured crisis. Covid was not.”
The federal government has also moved to tighten rules surrounding visitors from abroad, which likely limits how many people living in the U.S. without legal status would come to the NIH for care.
Before Trump, officials developed a new visitor policy for the NIH that required people who aren’t U.S. citizens or legal permanent residents to register online before arriving. But its implementation was delayed, Gilman said. It did not launch , after President Joe Biden was no longer in office and around the time the Trump administration began its deportation operation.
The Department of Homeland Security has carried out widespread raids and arrests and allowed immigration authorities unprecedented access to various federal data sources тАФ including tax information and Medicaid recipients’ personal data тАФ as part of its immigration enforcement efforts.
The clinical center’s most recent annual report said around 600 patients in 2024 were from abroad.
Now “international patients are terrified to come,” said one recently departed clinician. “They don’t know what will happen to them.”
Are you a cancer patient whose care at the National Institutes of Health Clinical Center in Maryland, or another hospital, has been affected by the Trump administration’s cuts? Are you a family member or caregiver of a cancer patient who has received care at the NIH? We’d like to hear about your experience. Tell us here.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/nih-clinical-center-patient-numbers-drop-under-trump-jeopardizing-care/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2071450&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>“A lot of times, health care comes with a job.”Sen. John Thune (R-S.D.), in an interview with KOTA on May 30, 2025

Millions of people are expected to lose access to Medicaid and Affordable Care Act marketplace health insurance plans if federal lawmakers approve the One Big Beautiful Bill Act, President Donald Trump’s domestic policy package, which is now moving through the Senate.
Senate Majority Leader John Thune discussed health care and the pending legislation in an , a South Dakota TV station. But he focused on a different kind of health insurance — employer-sponsored insurance.
“A lot of times, health care comes with a job,” Thune said.
Thune’s comments in the interview were made in the context of highlighting part of the GOP’s economic policy objective. “Creating those better-paying jobs that come with benefits is ultimately the goal here,” he said.
║┌┴╧│╘╣╧═Ї News reached out to Thune’s office to find out the basis for this comment. His communications director, Ryan Wrasse, responded by reiterating Thune’s message: “Getting a job has the potential to lead a worker to acquiring health care.”
Paul Fronstin, director of health benefits research at the Employee Benefit Research Institute, said Thune’s comment may also be alluding to discussions surrounding Medicaid work requirements. The One Big Beautiful Bill Act enroll in Medicaid only if they prove they’re volunteering, working, or searching or training for work.
Medicaid, funded by the federal government and states, is the country’s main health insurance program for people with low incomes. Some people with disabilities also qualify.
Some Republicans have built on the jobs talking point in defending the Medicaid cuts and work requirements. Sen. James Lankford (R-Okla.), for instance, the bill isn’t about “kicking people off Medicaid. It’s transitioning from Medicaid to employer-provided health care.”
But the health policy experts we checked with made clear that getting a job isn’t a guarantee for getting work-sponsored insurance.
Employer-Sponsored Health Insurance: The Basics
These experts said most jobs do offer health insurance. But they also said the link between employment and work-based coverage is not always straightforward.
“When I see this statement, I’m like, ‘I’ve got so much more to say about this.’ But I’m not arguing with the statement,” Fronstin said.
Matthew Rae, an associate director focused on researching private insurance at KFF, a health information nonprofit that includes ║┌┴╧│╘╣╧═Ї News, also weighed in.
“Employer-sponsored coverage remains the bedrock of how people get health insurance in the United States,” Rae said. “I would say that getting a job is not a guarantee you’re going to have health insurance. It just increases your chances of getting it.”
About 60% of Americans younger than 65 receive health insurance through their job or as the spouse, child, or other dependent of someone insured through their work,
Among workers ages 18 to 64 who were eligible but didn’t sign up for their workplace insurance, 28% said the reason they decided not to enroll was that the plans were too expensive, showed.
Most of these workers found health insurance elsewhere, such as through a relative’s workplace plan. But a small percentage of eligible employees, 3.7%, .
Health insurance has been “the most valued benefit in the workplace” since businesses to recruit employees in a tight labor market during World War II, Fronstin said.
Federal law also encourages companies to offer plans. Under the Affordable Care Act, employers with 50 or more full-time workers if they don’t offer most employees insurance that the federal government considers affordable.
As of last year, 54% of companies offered health insurance to at least some employees, .
But that’s not the main way the of people without health insurance, said Melissa Thomasson, a professor at Miami University in Ohio who specializes in the economic history of health insurance. “Nearly all of that” change, she said, came from the ACA creating private marketplace plans and allowing states to expand Medicaid eligibility.
Health policy analysts say the One Big Beautiful Bill would make it more difficult for people to qualify or afford marketplace plans, with proposals that would increase paperwork, shorten enrollment periods, and allow enhanced tax credits to fizzle out. Thomasson also noted that political rhetoric surrounding jobs and health insurance doesn’t always align.
“We often talk about small businesses being the engine of job creation,” but those are the businesses that often can’t afford to offer workplace insurance, she said.
So Who Isn’t Insured Through Workplace Insurance?
The most obvious category of people who don’t have workplace insurance are those who don’t have a job. This group includes children and retirees, people searching for work, people who choose not to work, and those who can’t work, because of a disability or illness.
Another group without employer-provided insurance is the 25% of people ages 18 to 64 who have a job but are unable to obtain such insurance, according to .
Some of these people work for companies that don’t offer health insurance. These employers tend to be small businesses or part of certain industries, such as farming and construction.
Others are part-time, temporary, or seasonal workers at companies that offer health insurance only to full-time employees. Workers with low incomes are significantly less likely than those with higher incomes to be eligible for workplace insurance,
People who aren’t employed or don’t get insurance through their job can get coverage in other ways. Some are insured through a relative’s workplace plan, while others purchase plans and may qualify for subsidies on the ACA marketplace.
Others get insurance through Medicaid or Medicare, the federal health insurance program for people 65 or older and some people with disabilities.
Cost and Quality — And Therefore Access to Care — Vary
Just because someone has health insurance doesn’t mean they’ll get the health care they need. People may skip or delay care if their plans are unaffordable or if they limit in-network providers.
“Health benefits come in all shapes and sizes,” Fronstin said. “Some employers offer very generous benefits, and others less so.”
KFF data shows that premiums and enrollees’ cost-sharing expenses grew faster than wages but have .
Whether workplace insurance is affordable significantly varies by income. , lower-income families insured through a full-time worker spent, on average, 10.4% of their income on premiums and out-of-pocket costs. That’s more than twice the rate when looking at families across all incomes.
Our Ruling
Thune said, “A lot of times, health care comes with a job.”
This statement is partially accurate. Most workers in the U.S. get health coverage through work. But it glosses over aspects of our nation’s job-based health insurance system — such as how costs and coverage, especially for those with lower incomes, can make an employer plan out of reach even if it is available.
Bottom line: Not all jobs provide health insurance or offer plans to all their workers. When they do, cost and quality vary widely — making Thune’s statement an oversimplification.
We rate this statement Half True.
Sources
with Sen. John Thune, May 30, 2025.
with Sen. James Lankford, June 5, 2025.
KFF, “,” Oct. 9, 2024.
KFF, “,” Feb. 29, 2024.
KFF, “,” May 28, 2024.
Peterson-║┌┴╧│╘╣╧═Ї System Tracker, “” Dec. 22, 2023.
Peterson-║┌┴╧│╘╣╧═Ї System Tracker, “,”
March 10, 2022.
Peterson-║┌┴╧│╘╣╧═Ї System Tracker, “,” Aug. 14, 2019.
Manhattan Institute, “” May 22, 2025.
Brookings, “,” July 22, 2024.
Harvard Business Review, “?” March 15, 2019.
on the One Big Beautiful Bill Act increasing the number of uninsured people, June 4, 2025.
Phone interview with Paul Fronstin, director of health benefits research at the Employee Benefit Research Institute and a member of the Commonwealth Fund’s National Task Force on the Future Role of Employers in the U.S. Health System, June 6, 2025.
Phone interview with Melissa Thomasson, professor and health economist at Miami University, June 6, 2025.
Phone interview with Maanasa Kona, associate research professor at the Center on Health Insurance Reforms at Georgetown University, June 6, 2025.
Phone interview with Matthew Rae, associate director for the Health Care Marketplace Program at KFF, June 10, 2025.
Phone interview with Sally Pipes, president and CEO of the Pacific Research Institute, June 11, 2025.
Email correspondence with Ryan Wrasse, communications director for Sen. John Thune, June 10, 2025.
║┌┴╧│╘╣╧═Ї News, “Some Employers Test Arrangement To Give Workers Allowance for Coverage,” Oct. 2, 2024.
║┌┴╧│╘╣╧═Ї News, “Trump’s ‘One Big Beautiful Bill’ Continues Assault on Obamacare,” June 3, 2025.
This <a target="_blank" href="/medicaid/fact-check-thune-health-insurance-workplace-job-employers/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2053818&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>“You’d call and you’re talking about weeks to a month,” Andrews said.
That’s not surprising, as many workplace surveys show the supply of primary care doctors has fallen well below the demand, especially in rural areas such as western Massachusetts. But Andrews still wasn’t prepared for the letter that arrived last summer from her doctor, Christine Baker, at .
“We are writing to inform you of an exciting change we will be making in our Internal Medicine Practice,” the letter read. “As of September 1st, 2024, we will be switching to Concierge Membership Practice.”
Concierge medicine is a business model in which a doctor charges patients a monthly or annual membership fee тАФ even as the patients continue paying insurance premiums, copays, and deductibles. In exchange for the membership fee, doctors limit their number of patients.
Many physicians who’ve made the change said it resolved some of the pressures they faced in primary care, such as having too many patients to see in too short a time.
Andrews was floored when she got the letter. “The second paragraph tells me the yearly fee for joining will be $1,000 per year for existing patients. It’ll be $1,500 for new patients,” she said.
Although numbers are not tracked in any one place, the trade magazine Concierge Medicine Today estimates there are concierge physicians in the U.S. Membership fees range from $1,000 to as high as $50,000 a year.
Critics say concierge medicine helps only patients who have extra money to spend on health care, while shrinking the supply of more traditional primary care practices in a community. It can particularly affect rural communities already experiencing a shortage of primary care options.
Andrews and her husband had three months to either join and pay the fee or leave the practice. They left.
“I’m insulted and I’m offended,” Andrews said. “I would never, never expect to have to pay more out of my pocket to get the kind of care that I should be getting with my insurance premiums.”
Baker, Andrews’ former physician, said fewer than half her patients opted to stay тАФ shrinking her patient load from 1,700 to around 800, which she considers much more manageable. Baker said she had been feeling so stressed that she considered retiring.
“I knew some people would be very unhappy. I knew some would like it,” she said. “And a lot of people who didn’t sign up said, тАШI get why you’re doing it.’”
Patty Healey, another patient at Baker’s practice, said she didn’t consider leaving.
“I knew I had to pay,” Healey said. As a retired nurse, Healey knew about the shortages in primary care, and she was convinced that if she left, she’d have a very difficult time finding a new doctor. Healey was open to the idea that she might like the concierge model.
“It might be to my benefit, because maybe I’ll get earlier appointments and maybe I’ll be able to spend a longer period of time talking about my concerns,” she said.
This is the conundrum of concierge medicine, according to Michael Dill, director of workforce studies at the . The quality of care may go up for those who can and do pay the fees, Dill said. “But that means fewer people have access,” he said. “So each time any physician makes that switch, it exacerbates the shortage.”
the U.S. will face a shortage of within the next decade.
found that the percentage of residents in western Massachusetts who said they had a primary care provider was lower than in several other regions of the state.
Dill said the impact of concierge care is worse in rural areas, which often already experience physician shortages. “If even one or two make that switch, you’re going to feel it,” Dill said.
Rebecca Starr, an internist who specializes in geriatric care, recently started a concierge practice in Northampton.
For many years, she consulted for a medical group whose patients got only 15 minutes with a primary care doctor, “and that was hardly enough time to review medications, much less manage chronic conditions,” she said.
When Starr opened , she wanted to offer longer appointments тАФ but still bring in enough revenue to make the business work.
“I did feel a little torn,” Starr said. While it was her dream to offer high-quality care in a small practice, she said, “I have to do it in a way that I have to charge people, in addition to what insurance is paying for.”
Starr said her fee is $3,600 a year, and her patient load will be capped at 200, much lower than the 1,000 or even 2,000 patients that some doctors have. But she still hasn’t hit her limit.
“Certainly there’s some people that would love to join and can’t join because they have limited income,” Starr said.

Many doctors making the switch to concierge medicine say the membership model is the only way to have the kind of personal relationships with patients that attracted them to the profession in the first place.
“It’s a way to practice self-preservation in this field that is punishing patients and doctors alike,” said internal medicine physician Shayne Taylor, who recently opened offering “direct primary care” in Northampton. The direct primary care model is similar to concierge care in that it involves charging a recurring fee to patients, but bypasses insurance companies altogether.
Taylor’s patients, capped at 300, pay her $225 a month for basic primary care visits тАФ and they must have health insurance to cover care such as X-rays and medications, which her practice does not provide. But Taylor doesn’t accept insurance for any of her services, which saves her administrative costs.
“We get a lot of pushback because people are saying, тАШOh, this is elitist, and this is only going to be accessible to people that have money,’” Taylor said.
But she said the traditional primary care model doesn’t work. “We cannot spend so much time seeing so many patients and documenting in such a way to get an extra $17 from the insurance company.”
While much of the pushback on the membership model comes from patients and policy experts, some of the resistance comes from physicians.
, a primary care doctor who runs in western Massachusetts, said his practice is more stretched than ever. One reason is that the group’s clinics are absorbing some of the patients who have lost their doctor to concierge medicine.
“We all contribute through our tax dollars, which fund these training programs,” Carlan said.
“And so, to some degree, the folks who practice health care in our country are a public good,” Carlan said. “We should be worried when folks are making decisions about how to practice in ways that reduce their capacity to deliver that good back to the public.”
But Taylor, who has the direct primary care practice, said it’s not fair to demand that individual doctors take on the task of fixing a dysfunctional health care system.
“It’s either we do something like this,” Taylor said, “or we quit.”
This article is from a partnership that includes , , and ║┌┴╧│╘╣╧═Ї News.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/concierge-medicine-direct-primary-care-doctor-shortage-rural-western-massachusetts/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2013349&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>“Tell them she’s on Eliquis!” said Martin, a nurse who lived an hour’s drive away in Winston-Salem. She knew the blood thinner could lead to life-threatening blood loss.
When the ambulance arrived, the medics evaluated Martin’s aunt and then did something few emergency medical services crews do: They gave her a blood transfusion to replace what she’d lost, stabilizing her sinking blood pressure.
The ambulance took her to the local high school, and from there a medical helicopter flew her to the nearest trauma center, in Winston-Salem. She needed more units of blood in the helicopter and at the hospital but eventually recovered fully.
“The whole situation would have been different if they hadn’t given her blood right away,” Martin said. “She very well might have died.”
in the U.S. bleed to death every year from traumatic events like car crashes or gunshot wounds, or other emergencies, including those related to pregnancy or gastrointestinal hemorrhaging. It’s a leading cause of preventable death after a traumatic event.
But many of those people likely wouldn’t have died if they had received a blood transfusion promptly, trauma specialists say. At last fall, members of the American College of Surgeons estimated that 10,000 lives could be saved annually if more patients received blood before they arrived at the hospital.
“I don’t think that people understand that ambulances don’t carry blood,” said Jeffrey Kerby, who is chair of the ACS Committee on Trauma and directs trauma and acute care surgery at the University of Alabama-Birmingham Heersink School of Medicine. “They just assume they have it.”
Of the more than 11,000 EMS agencies in the U.S. that provide ground transport to acute care hospitals, only about 1% carry blood, .
The term “blood deserts” generally refers to a problem in rural areas where the nearest trauma center is dozens of miles away. But heavy traffic and other factors in suburban and urban areas can turn those areas into blood deserts, too. In recent years, several EMS agencies throughout the country have established “pre-hospital blood programs” aimed at getting blood to injured people who might not survive the ambulance ride to the trauma center.
With blood loss, . Blood helps move oxygen and nutrients to cells and keeps organs working. If the volume gets too low, it can no longer perform those essential functions.
If someone is catastrophically injured, sometimes nothing can save them. But in many serious bleeding situations, if emergency personnel can provide blood within 30 minutes, “it’s the best chance of survival for those patients,” said Leo Reardon, the Field Transfusion Paramedic Program director for the Canton, Massachusetts, fire department. “They’re in the early stages of shock where the blood will make the most difference.”
There are several roadblocks that prevent EMS agencies from providing blood. Several states don’t allow emergency services personnel to administer blood before they arrive at the hospital, said John Holcomb, a professor in the division of trauma and acute care surgery at UAB’s Heersink School.
“It’s mostly tradition,” Holcomb said. “They say: тАШIt’s dangerous. You’re not qualified.’ But both of those things are not true.”
On the battlefields in the Middle East, operators of military medical facilities would maintain that only nurses and doctors could do blood transfusions, said Randall Schaefer, a U.S. Army trauma nurse who was deployed there and now consults with states on implementing pre-hospital blood programs.
But in combat situations, “we didn’t have that luxury,” Schaefer said. Medical staff sometimes relied on medics who carried units of blood in their backpacks. “Medics can absolutely make the right decisions about doing blood transfusions,” she said.
A quick response made a difference: Soldiers who received blood within minutes of being injured were four times as likely to survive, .
Civilian emergency services are now incorporating lessons learned by the military into their own operations.
But they face another significant hurdle: compensation. are based on how far vehicles travel and the level of services they provide, with some adjustments. But the fee schedule doesn’t cover blood products. If EMS responders carry blood on calls, it’s usually low-titer O whole blood, which is generally safe for anyone to receive, or blood components тАФ liquid plasma and packed red blood cells. from $80 to $600 on average, according to Schaefer’s study. And payments don’t cover the blood coolers, fluid warming equipment, and other gear needed to provide blood at the scene.
, the Centers for Medicare & Medicaid Services began counting any administration of blood during ambulance pre-hospital transport as an “advanced life support, level 2” (ALS2) service, which will boost payment in some cases.
The higher reimbursement is welcome, but it’s not enough to cover the cost of providing blood to a patient, which can run to more than $1,000, Schaefer said. Agencies that run these programs are paying for them out of their own operating budgets or using grants or other sources.
Blood deserts exist in rural and urban areas. Last August, Herby Joseph was walking down the stairs at his cousin’s house in Brockton, Massachusetts, when he slipped and fell. The glass plate he was carrying shattered and sliced through the blood vessels in his right hand.
“I saw a flood of blood and called my cousin to call 911,” Joseph, 37, remembered.
The ambulance team arrived in just a few minutes, evaluated him, and called in the Canton-based Field Transfusion Paramedic Program team, which began administering a blood transfusion shortly thereafter. The program serves 30 towns in the Boston area. Since the transfusion program began last March, the team has responded to more than 40 calls, many of them related to car accidents along the ring of interstate highways surrounding the area, Reardon said.
Brockton has a Level 3 trauma center, but Joseph’s injuries required more intensive care. Boston Medical Center, the Level 1 trauma center where the EMS team was taking Joseph, is about 23 miles from Brockton, and depending on traffic it can take more than a half hour to get there.
Joseph was given more blood at the medical center, where he remained for nearly a week. He eventually underwent three surgeries to repair his hand and has now returned to his warehouse job.
Although Boston has several Level 1 trauma centers, the region south of the city is pretty much a trauma desert, said Crisanto Torres, one of the trauma surgeons who cared for Joseph.
Boston Medical Center partners with the Canton Fire Department to operate the field transfusion program. It’s an important service, Torres said.
“You can’t just put up a new Level 1 trauma center,” he said. “This is one way to blunt the inequity in access to care. It buys patients time.”
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/blood-deserts-transfusions-ems-ambulances-trauma-massachusetts/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1980274&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>“Patients who speak Spanish really prefer a Spanish-speaking provider,” Deem said. “I’ve gotten to know this community pretty well.”
Clemson doesn’t operate an academic medical center, nor does it run a medical school. Arguably, the public university is best known for its football program. Yet, with millions of dollars earmarked from the state legislature, it has expanded into delivering health care, with clinics in Walhalla and beyond. School leaders are attempting to address gaps in rural and underserved parts of a state where health outcomes routinely rank among the worst in the country.
“Some of these communities have such high need,” said , director of Clemson Rural Health, which operates four clinics and a fleet of mobile health units as part of the university’s College of Behavioral, Social and Health Sciences. “They have so many barriers that impact their ability to be healthy.”
Clemson Rural Health is one of several programs attempting to meet this need in the state.
“Rural health is trendy,” said Graham Adams, CEO of the .

State lawmakers nationwide are spending millions of dollars to address a rural health care crisis long in the making. For more than a decade, though, Republican-controlled legislatures in most have refused billions in federal funds that would provide public health insurance coverage to more low-income adults. These are the same states where racial health disparities and health outcomes are often worse than in other regions.
Nearly every state has extended Medicaid coverage for women in the months after they give birth. But haven’t fully expanded Medicaid coverage with federal money made available under the 2010 Affordable Care Act. Seven of these states тАФ Alabama, Florida, Georgia, Mississippi, South Carolina, Tennessee, and Texas тАФ are in the South. With few exceptions, adults without children in these states don’t qualify for Medicaid coverage, regardless of their income level.
Georgia Gov. Brian Kemp and South Carolina Gov. Henry McMaster, both Republicans, recently announced plans to expand Medicaid in limited ways to include some parents. The South Carolina plan would impose work requirements on some of these newly eligible Medicaid beneficiaries, while the Georgia plan would allow some parents of young children to skirt the state’s existing Medicaid work rules. Both plans require federal approval.
, a professor and health policy scholar at the University of North Carolina, said he doesn’t expect to see any of the remaining states rushing to fully expand Medicaid. Before Donald Trump took office on Jan. 20, Republicans in Washington had already expressed their intention to dramatically cut spending for Medicaid, which covers 72 million people at a cost of nearly $900 billion.
“There’s a large gray cloud hanging over Medicaid expansion right now, and that’s because there’s so much uncertainty about what the Trump administration and congressional Republicans are going to do,” Oberlander said.
Even so, in South Carolina this year the plans to lobby the General Assembly to pass a bill to adopt Medicaid expansion, said Beth Johnson, regional government relations director for the American Cancer Society Cancer Action Network and a CoverSC board member. The state’s legislative session began Jan. 14.
If such a measure were approved, the federal government would cover 90% of the state’s Medicaid expansion costs and South Carolina would be expected to pay 10%, or an estimated $270 million during the first year, according to by the Milken Institute School of Public Health at George Washington University.
Across all 10 non-expansion states тАФ which, outside the South, also include Kansas, Wisconsin, and Wyoming тАФ about 1.5 million people fall into a coverage gap, according to , the health information nonprofit that includes ║┌┴╧│╘╣╧═Ї News. That means they do not qualify for Medicaid coverage or financial assistance to buy insurance through the federal marketplace.
Many of the people who would qualify for Medicaid if these states were to expand eligibility are gig workers, Johnson said. They play music, drive for Uber, or deliver pizza, and they typically don’t qualify for health insurance through their jobs.
“They are providing services that we all appreciate,” she said. “And they simply can’t afford health insurance.”

In some South Carolina communities, Clemson Rural Health attempts to fill this gap by providing primary care, cancer screenings, nutrition education, and diabetes management for uninsured patients free of charge or at reduced rates. Only about half of the patients seen by Clemson Rural Health have health insurance, Gimbel said, compared with 92% of the U.S. population.
During the current state fiscal year, Clemson Rural Health has been underwritten by a $2.5 million contract, its largest source of funding, from the state Department of Health and Human Services, which administers Medicaid in South Carolina and operates with a budget approved by state lawmakers.
That’s a relatively small amount of money compared with the $47.5 million the state legislature has given to the Medical University of South Carolina in recent years to move into rural communities. MUSC has served Charleston for most of its 200-year history, but since 2019 it has expanded across the state by purchasing, building, or partnering with seven rural hospitals тАФ some on the brink of closure тАФ and one freestanding emergency department. MUSC is set to open an additional rural hospital this year.
Other states have made similar investments. The University of Georgia, for example, has established a new medical school, partly to send more physicians into underserved and rural areas. The Georgia General Assembly kicked in half the cost of a new $100 million building for medical education and research in Athens.
Meanwhile, the Tennessee General Assembly passed a budget last year that included $81 million for a variety of rural health initiatives.
Outside the South, state legislatures in Colorado, Nevada, West Virginia, and elsewhere have made recent investments in rural health, in addition to expanding Medicaid eligibility.
Some of this spending has been prompted by a wave of rural hospital closures тАФ since 2010, according to the Cecil G. Sheps Center for Health Services Research at the University of North Carolina.
It’s not yet clear what long-term impact some of these initiatives will have тАФ for instance, whether the Clemson program will “reduce premature mortality, decrease preventable hospitalizations, and improve overall quality of life,” as it aims to do, according to . Some public health experts point out that bolstering the number of rural clinics, hospitals, and doctors in the South won’t matter much if patients can’t afford to make an appointment.
“Lack of ability to pay is one of the greatest barriers,” said Adams, the Office of Rural Health chief.
Oberlander said conservative lawmakers often consider projects such as building new rural clinics more politically palatable than expanding Medicaid coverage.
“The further away you get from the ACA, the less polarized the politics of health care,” he said.
South Carolina Senate President , a Republican who lives in Walhalla, said the General Assembly is willing to invest in some rural health initiatives to improve health care access.
“Just because you expand Medicaid doesn’t mean you’ve expanded access to the services,” Alexander said. “I want to focus on expanding access to the services.”
Gimbel would not comment on Medicaid expansion in South Carolina, and he said it’s too soon to know how federal Medicaid changes under the Trump administration might affect funding for Clemson Rural Health, which currently receives money from the state’s Medicaid agency. But making the Clemson program financially solvent might take several more years, he said.
“If rural health was profitable,” he said, “we wouldn’t have a rural health problem.”
This <a target="_blank" href="/rural-health/south-carolina-clemson-rural-health-medicaid-expansion-clinics/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1974623&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>One of his sponsors took advantage of the moment: the telehealth company Ro, which sells a variety of prescription medicines for erectile dysfunction and hair and weight loss. The company revved up a social media campaign on the social platform X for an ad in which Sharpe boasted about his experience with the company’s erectile dysfunction medications, a company spokesperson confirmed.
The ads were more than just a passing attempt to hitch a corporate caboose to a runaway social media locomotive. A group of direct-to-consumer telehealth companies have become omnipresent across just about all media formats, seeking patients interested in their low-stigma, low-fuss, low-touch, high-convenience health products.
They’re on your favorite podcasts and in the background on the cable TV in your gym. Thirteen telehealth entities in 2023 on television ads, more than double the sum in 2019, according to an analysis from , a television ad-tracking company, provided to ║┌┴╧│╘╣╧═Ї News.
The ads feature high-wattage celebrities such as Jennifer Lopez as well as lesser-known influencers who are paid four figures to post a snapshot or short video to Instagram, according to interviews with marketers. Three publicly traded telehealth companies spent a total of more than $1.4 billion on advertising, sales, and marketing in 2023, according to financial reports filed with the Securities and Exchange Commission, categories that reflect the extent of their online efforts.
The companies’ advertising typically emphasizes convenience in a health care system that’s often just the opposite. They promise judgment-free birth control or care for conditions like erectile dysfunction and hair loss that have traditionally been stigmatized. As the companies expand, they’re venturing into more complex kinds of medicine, such as care for mental health conditions and obesity.
Services that telehealth companies offer, critics warn, may shortchange patients in need of close, sensitive attention. Researchers differ on telehealth services’ quality, with some saying telehealth companies offer little follow-up and inconsistent care from a revolving cast of doctors.
Still, they agree the care is fundamentally different from the traditional style. A company’s model can “kind of flip what you’re taught at medical school on its head,” said Ateev Mehrotra, a Brown University professor of public health who studies telehealth.
Typically, he said, a patient goes to the doctor with a complaint; there, the parties figure out a diagnosis and, if appropriate, a medication. By contrast, he said, telehealth companies’ advertising invites patients to make their own diagnoses, while pairing them with clinicians who, if they confirm their conditions, prescribe medicines the patients already think they want.
Under this style of medicine, the clinician is “now a screener, and you just want to make sure that that medication is safe for that patient,” Mehrotra said.
The model may work for certain kinds of care, Mehrotra said, such as birth control. He and some colleagues conducted a study in which they recruited patients with standardized backstories to patronize startups offering contraceptive medicines over the internet. Generally, the study found, the services performed well.
Harley Diamond, a patient at Nurx, a startup offering birth control prescriptions and other services, offers an example of how these companies can work well in some circumstances. After she saw an Instagram ad, she signed up to get birth control. She lives in Tennessee, a red state where it can be difficult to access contraception: Local clinics have closed and an arsonist burned down a Planned Parenthood. (The facility .)
But when she turned to Nurx for her mental health, she found the service confounding and its convenience lacking.
The company’s app sends her frequent questionnaires about symptoms and reactions to drugs, she said. “There is no comforting face to validate you,” she wrote in an email to ║┌┴╧│╘╣╧═Ї News. The questions were the same each time, and she said she spoke with a new doctor in every interaction.
“It can feel like you’re having to start from scratch explaining yourself to someone new every month,” she said.
When she expressed concerns тАФ for example, about side effects of an antidepressant she was taking тАФ it would take “days, generally,” to hear back, with no change in her protocol, she said. Often, she said, her messages would get no response at all.
Rajani Rao, senior vice president at Nurx, said the company is “constantly working” to improve response times, “especially as we experience a high volume of patient care requests.” In mental health, the majority of Nurx’s patients experience elimination of symptoms after six months of treatment, she said.
Rao also referred to Nurx as providing an “integrated care team,” using language echoed across the industry. Ro, for example, says its care is available in the time and format of its patient’s preference and that it audits the quality of its services.
Continuous care is crucial to make sure mental health patients are on the right doses of medications and that they’re not experiencing side effects, said Reshma Ramachandran, an assistant professor of medicine at Yale who has conducted her own secret-shopper study of telehealth sites.
What’s more, research shows many mental health medications are best paired with therapy, Ramachandran said.
Ramachandran thinks frustrations like Diamond’s might be widespread, based on her team’s research. She said she’s frustrated at the “very groovy, glossy” picture painted by telehealth ads.
Ramachandran said her study is still under consideration for publication in medical journals. But she provided preliminary results to congressional offices examining the telehealth sector.
Last year, Sen. Dick Durbin, an Illinois Democrat, and former Sen. Mike Braun, an Indiana Republican, introduced legislation to regulate some telehealth advertising practices. A spokesperson for Durbin said he intends to reintroduce the bill this year.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/telehealth-ads-marketing-birth-control-mental-health-obesity/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1971284&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The proposed merger between Union Health and Terre Haute Regional Hospital, the only acute care hospitals in Vigo County, Indiana, would have left Terre Haute’s 58,000 residents and those in the . Although federal laws prohibit monopolies, the hospitals sought the merger under a state provision known as a “Certificate of Public Advantage” law, or COPA.
“Recognizing the COPA process is a very complex, innovative approach to improving access and quality health care for area residents, we believe it is best to withdraw the current application,” Union Health posted on its website.
Union said it plans to submit a new application after working with Indiana regulators to “ensure the benefits” such as “improved access, quality” are included.
The withdrawal came nine days before a Dec. 4 deadline for state regulators to rule on whether to OK the merger. In recent months, the state health agency had from residents and the Federal Trade Commission opposed to the deal between Union Health, a nonprofit whose main hospital is licensed as a 341-bed facility, and the 278-bed Terre Haute Regional Hospital, owned by for-profit chain HCA Healthcare. The commenters cited concerns about longer travel times to get emergency care, higher prices, and fewer choices.
Union Health and HCA declined to answer questions about what prompted the decision to pull back the application.
“There could be any number of reasons why they pulled the application with the stated intention to refile,” said , a University of Missouri-Kansas City economist who has studied COPA mergers. Given the status of the application, he said, it’s unlikely the deal was headed toward an approval. “Either way, I think it’s clear that the state was not ready to approve the COPA with conditions similar to past COPAs.”
It was the latest setback against mergers under COPA laws. Indiana and 18 other states have such laws that shield hospital mergers from federal enforcement by the Federal Trade Commission.
As a condition of the deals, states typically agree to monitor hospital performance and quality while limiting price hikes. Supporters of COPAs argue that state oversight built into the agreements can mitigate the harms of a monopoly. But health economists and the FTC have said that oversight cannot replace competition and that these mergers ultimately harm patients.
“We know that COPAs generally benefit the merging hospitals, but not local residents,” said , a health economist and associate professor at Yale University.
His analysis of the Terre Haute deal suggested that it would have damaged the local economy and squeezed residents’ wallets. Cooper said he hopes that states faced with similar merger decisions will see Indiana’s waylaid case and the pushback against other COPA mergers as a cause for pause.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/copa-indiana-hospitals-pull-merger-application-pushback-monopoly/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1948552&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Union Health, a nonprofit whose main hospital is licensed as a 341-bed facility, would buy the county’s only other acute care hospital, the 278-bed Terre Haute Regional Hospital, owned by for-profit chain HCA Healthcare and located 5 miles south across the city’s downtown area. Union says the merger to create one larger nonprofit health system would improve the area’s poor public health rankings.
The Indiana Department of Health received hundreds of comments on the , according to documents ║┌┴╧│╘╣╧═Ї News obtained through a state public records request. Most people expressed opposition to the deal, citing concerns about longer travel times to get emergency care, higher prices, and fewer choices for Terre Haute’s 58,000 residents and those in Vigo County’s nearby rural communities.
“Monopoly should be just a board game. Not a healthcare system,” a commenter listed as H. Osborne wrote to the state health agency.
Doctors, health economists, and the Federal Trade Commission called on the Indiana Department of Health to deny Union Hospital’s merger application. Such mergers became possible after Indiana enacted a Certificate of Public Advantage law, or COPA, in 2021, shielding the deals from federal anti-monopoly laws.
Two dozen states have had COPA laws on their books at some point, despite FTC warnings that such mergers can become difficult to control and may decrease the overall quality of care. The trend has come amid a broader wave of hospital consolidation, which fuels price hikes and health care spending, driving up costs for families, employers, and taxpayers who foot the bill for Medicare and Medicaid.
Union Health said its proposed deal would improve care and increase access to services while “maintaining cost efficiency” for patients.
“This is not merely a business transaction; it is a strategic effort to improve healthcare delivery in our community,” .
John Collett, an executive with Garmong Construction who also serves on the board of the , wrote that the deal would help the region achieve its goal of boosting population and income levels. (Garmong Construction served as construction manager for Union on multiple projects, including one worth hundreds of millions of dollars, according to an of its past projects.)
“I firmly believe this to be a step in the right direction,” Collett wrote.
But the FTC тАФ using italics for emphasis тАФ said the deal is “unlikely to result in improved quality and access” and “would not lead to a healthier workforce or a stronger local economy,” according to to Indiana regulators.
, a health economist and associate professor at Yale University, said the merger would probably damage the local economy and squeeze residents’ wallets. estimates the price of care would rise by at least 10% for area residents and lead to 500 lost jobs, while nurses’ pay would drop by at least 7%. His research predicts the deal also would lead to unnecessary deaths from suicide or overdose, stemming from those job losses.
“I firmly believe this merger would harm members of the public in Terre Haute and Vigo County,” Cooper wrote.
As a condition of these types of mergers, state agencies typically agree to monitor hospital quality and prices to make up for the loss of competition. Union said monitoring would hold it accountable, according to to the FTC’s public comments opposing the deal.
The FTC pushed back, saying the oversight mechanism “would be insufficient to contain costs” and is a “poor substitute” for competition. Even though Union would face limits on raising prices in Vigo County, the FTC said, the system might be able to hike them elsewhere, including at its hospital in neighboring Vermillion County to the north.
Indiana has some of the highest hospital prices in the nation, according to ., a research organization.
In Terre Haute, some doctors worry the deal would exacerbate existing problems. Kathleen Stienstra, a physician in private practice, voiced her concerns about Union’s management style, saying it has led to an exodus of doctors.
“A monopoly will lead to further deterioration in services,” she wrote.
Separately, the FTC referenced ║┌┴╧│╘╣╧═Ї News’ reporting on Tennessee’s Ballad Health, a 20-hospital monopoly in Appalachia, as a cautionary tale against such mergers.
COPAs, such as the one that Ballad operates under, “have proven unwieldy,” are “difficult to manage,” and “have failed to protect local communities from the harmful effects of anticompetitive hospital mergers,” the FTC said in its comments on the Union-Regional merger.
Since Ballad launched in 2018 and became the nation’s largest state-approved hospital monopoly, it has , ║┌┴╧│╘╣╧═Ї News reported. It has fallen short on meeting quality and charity care goals, according to from Ballad and the Tennessee Department of Health. After years of problems and complaints from patients, the state is now trying for its quality of care.
Ballad declined to respond to ║┌┴╧│╘╣╧═Ї News inquiries regarding the FTC’s comments.
Now the Indiana Department of Health must consider the comments and decide by early December whether the proposed merger would improve health outcomes, access to services, and quality of care. Under the department’s standards, those benefits must “.”
║┌┴╧│╘╣╧═Ї News correspondent Brett Kelman contributed to this report.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/ftc-indiana-copa-effort-to-block-hospital-merger/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=1945933&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>