
An elementary school teacher chose a low-price health insurance plan but soon realized she wasn’t clear about what it would mean for her family’s finances.
“Once I got the insurance card, I compared our old plan to our new plan, and that’s when I really got worried, because I didn’t really understand what a deductible was. It got me thinking, how do I use this insurance?”
— Madison Burgess, 31, of San Diego
When enhanced federal subsidies expired at the end of 2025, a lot of people buying their own health insurance on the state and federal exchanges saw their expected monthly rates jump. To keep costs down, many switched to a high-deductible health plan. These plans offer lower monthly payments, but in exchange patients can face steep out-of-pocket costs when they need care.
The plans are pretty common. In 2023, 30% of people who got insurance through their employer had a high-deductible plan, up from only 4% in 2006.
Madison Burgess, a teacher in San Diego, gets health insurance through her teaching job. But when she investigated adding her husband to her plan, it was just too expensive, so she started shopping on the exchange for a cheaper option for him.
The longer she scrolled through the plan options, the more overwhelming it felt. Insurance jargon made it hard to tell what her family would owe if her husband got sick.
“I didn’t know what a deductible was, so I just went with what was cheap, and now I have regret,” she said.
In exchange for that lower monthly premium payment, her husband’s coverage won’t kick in for most care until they’ve paid $5,800 in medical bills. Burgess didn’t know that the deductible must be met before insurance picks up part of the tab.
Deductible:
The amount you as the patient have to pay before insurance picks up part of the tab

Premium:
The monthly bill for your policy, paid to the insurance company

How do you prepare for thousands of dollars in upfront costs? One option is a health savings account, or HSA, which lets you save pretax money and is now available to people enrolled in lower-tier state and federal exchange plans, including bronze and catastrophic coverage. These plans generally have the lowest premiums on the exchange but the highest out-of-pocket costs when you need care.
Burgess had chosen a bronze plan and didn’t know HSAs were an option.
“I’ve never thought about having to put money away for a deductible,” she said.
Burgess and others are often more worried about socking away money for unexpected car and house repairs or vet bills.
If, like Burgess, you chose cheaper health coverage for this year only to discover you’re on the hook for meeting a high deductible, these tips can help you prepare.
1. You might qualify for an HSA and not know it.

If you’re enrolled in a bronze or catastrophic plan, you qualify to open a health savings account. Think of it as a medical piggy bank with tax perks. You put in pretax money, which lowers your taxable income. The money grows tax-free, and when you spend it on , those transactions are also tax-free. That’s what people call a “triple tax advantage.”
These accounts build a cushion for future health costs, such as doctor visits, prescriptions, and even products like over-the-counter medicine, tampons, and sunscreen.
The money typically can’t be used for monthly premiums, but the account is yours to use for qualified medical expenses for yourself, your spouse, or your dependents anytime in the future. The money in the account is yours, even if you change jobs or health plans.
An HSA is not the same as a flexible spending account, or FSA. FSAs are tax-advantaged too but are offered only through employers. The money expires annually and you lose any remaining money when you leave that job.
2. HSA-curious? Here’s how to open one.
You open a health savings account through a bank or other financial institution. The institution will issue you a debit card so you can make purchases from the HSA.
You can at any point during the year as long as you’re covered by an eligible plan. You can choose where to open the account, but be sure to check for any fees financial institutions charge and shop around.
If you get insurance through your job, your employer may require you to use a specific IRS-approved company.

Many people decide they can’t afford to contribute to an HSA. For some households, the desire to set aside money for medical expenses competes with the need to pay rent and buy groceries.
But there’s a detail that can make it feel more manageable. Contributions don’t have to be large. Just a few dollars a month can get you started.
There is, however, a limit. The IRS sets an annual cap on how much you’re allowed to contribute to an HSA. In 2026, an individual is limited to $4,400, or $8,750 for a family plan. Under that ceiling, the amount is up to you.
3. Preventive services should be covered at no cost to you.
All plans sold on marketplaces must cover at no cost to the patient as long as the care is provided in-network. Those services include routine immunizations and cancer screenings.
Beyond preventive care, understanding what different services cost can help you decide which type of medical appointment works best for your health needs and your wallet. For example, some plans charge less for a telehealth visit than to see your primary care doctor in person.
Check out your for more details.
4. Seek care early in the year.
Most deductibles reset on Jan. 1. Scheduling appointments or surgeries early in the year can be strategic if you discover a condition that requires ongoing care. If you can afford it, meeting your deductible sooner can make the rest of the year significantly cheaper, said Caitlin Donovan, a senior director at the Patient Advocate Foundation.
5. Consider paying cash instead of spending down your deductible.
Some hospitals, clinics, or other providers offer cheaper prices if you pay cash. You have the and explanation of how much a health service would cost if you paid out-of-pocket. Ask for the estimate before you get care. Then, compare that price with what your insurance company tells you it would cost if you used your insurance. If you decide to go with a cash payment, you’ll need to pay while you’re still at the doctor’s office, before charges get submitted to your insurance company.
Paying cash may save you money, but the amount you pay generally won’t count toward your deductible or out-of-pocket maximum.
“If you don’t think you’re ever going to hit your deductible ‚Äî you’re that young invincible, and your deductible is $10,000 ‚Äî negotiate the cash price,” Donovan said.
6. On an ACA plan? Update your income and use an HSA to avoid a tax surprise.

If you’re on an ACA plan and you’re eligible for subsidies, be aware: If your and you don’t update your marketplace application, you could owe thousands of dollars at tax time. The . Report raises, new jobs, or side gigs as they happen. If your income goes up, stashing money in an HSA can help because the money you put in the account doesn’t count toward your taxable income.
As soon as you report an increase in your income, that could mean higher premiums (if you no longer qualify for the same subsidy), but experts say it’s better to pay now than owe a big bill that you have to pay all at once.
“One of the biggest problems I see is someone is newly unemployed and they sign up for coverage, they say that they’re not making any money, and then eventually they get a job and don’t report it, and then they have this huge tax bill at the end,” Donovan said.
She advises updating your marketplace profile as soon as your income changes, which could newly qualify you for Medicaid or a plan that contributes more toward your medical bills.
Taylor Cook contributed to this report.
Health Care Helpline helps you navigate the health system hurdles between you and good care. Send us your tricky question and we may tap a policy sleuth to puzzle it out. Share your story. The crowdsourced project is a joint production of NPR and ∫⁄¡œ≥‘πœÕ¯ News.
This <a target="_blank" href="/health-care-costs/health-care-helpline-npr-hsa-savings-account-high-deductible-plan-tips/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2171426&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Still, 69% of those enrolled last year signed up again this year, often for less generous coverage. About 9% said they had to forgo insurance, according to the survey by KFF, a health information nonprofit that includes ∫⁄¡œ≥‘πœÕ¯ News.
The KFF poll revisited the people who responded to of Affordable Care Act enrollees during open enrollment for ACA plans.
Steve Davis, a 64-year-old retired car salesman in Rogersville, Tennessee, who participated in both polls, said he was looking at an annual premium of about $14,000 to renew his ACA coverage this year. He didn’t qualify for enough of a tax credit to defray the cost, he said, after Congress gridlocked on an extension of more-generous subsidies put in place under President Joe Biden.
But things worked out for Davis. He landed a job at a convenience store that came with insurance, with his share costing about $100 more a month than the $300 he paid for an ACA plan last year, before the enhanced tax credits expired.
“As it happened, the Lord provided and my insurance kicked in through my employer,” he told ∫⁄¡œ≥‘πœÕ¯ News.
In the November survey, many respondents were not sure what they would do for their health insurance in the coming year.
Some were waiting to see whether Congress would extend the enhanced premium subsidies, which had helped many people get lower-cost — or even zero-cost — health premiums.
Congress’ inaction left some consumers in a bind.
Now, the new poll found, affordability issues are hitting home as the midterm election approaches. And that might play a role in competitive districts, creating headwinds for Republicans.
Midterm Signals
Across all respondents who were registered to vote, the poll found more than half place “a lot” of blame for rising costs on Republicans in Congress (54%), with a similar share putting the same level of blame on President Donald Trump (53%). A smaller group placed a lot of the blame on congressional Democrats (34%). Among independents, a group expected to be a key factor in many districts, the percentages putting a lot of the blame on the GOP (56%) and Trump (58%) were higher.
Among Republicans, 60% placed a lot of the blame on Democrats in Congress.
“Those who have marketplace coverage, who remained on it, they’re really struggling with health care costs,” said Lunna Lopes, senior survey manager for KFF.
While more than half (55%) of returning ACA enrollees said they will have to pare back on other household expenses to cover health care costs, about 17% said they might not be able to continue paying insurance premiums throughout the year.
Overall, 80% of those who reenrolled for 2026 said their premiums, deductibles, or other costs are higher this year than last, with 51% saying they are “a lot higher.”
About three-quarters of ACA enrollees in the survey who were registered voters said the cost of health care will have an impact on their decision to vote ‚Äî and on which party’s candidate they support.
Democrats were more than twice as likely as Republicans to say those costs will have a major impact on their decision.
“Democrats seem particularly more energized by health care costs than their Republican counterparts,” Lopes said.
Enrollment Tally Down
Data released Jan. 28 by federal officials showed that about 23 million people enrolled in Obamacare plans across the federal healthcare.gov marketplace and those run by states, about 1.2 million fewer than in 2025.
But it isn’t yet known how many are paying their monthly premiums on time, and many analysts expect overall enrollment numbers to fall as that data becomes available in the coming months.
For most people, having to pay more for premiums this year was mainly due to the expiration of the enhanced tax cuts, pollsters noted. Because the subsidies that remain are less generous, households have to pay more of their income toward coverage. Congressional inaction also meant the restoration of an income cap for subsidies at four times the poverty level, or $62,600 for an individual, sticking people like Davis with higher bills.
Not everyone saw increases.
Matthew Rutledge, a 32-year-old substitute teacher in Apple Valley, California, who participated in both KFF polls, said he qualified as low-income and his subsidies fully offset his monthly premium payment, just as they did last year. He does have copayments when he sees a doctor or accesses other medical care, but he told ∫⁄¡œ≥‘πœÕ¯ News that “as long as the premium doesn’t go up, I’m fine with it.”
Rising premiums are fueled by a variety of factors, including hospital costs, doctors’ services, and the prices of drugs.
To lower premiums, insurers offer plans with higher deductibles or copayments. In the ACA, plans with lower premiums but higher deductibles are called “catastrophic” or “bronze” plans. “Silver” plans generally balance premiums and out-of-pocket spending, while the highest-premium plans with lower deductibles are “gold” or “platinum.”
About 28% of those who stayed in the ACA marketplaces switched plans, the pollsters noted.
One 56-year-old Texas man told pollsters that his family’s income exceeded the cap for subsidies, so they switched down from a gold plan to a bronze. “Even doing that, our premiums are three times what they were in 2025, with lower plan features and a higher deductible,” he said, according to a KFF poll news release.
For some, reenrolling was not a viable option.
In addition to the 9% who said they are now uninsured, about 5% said they switched to some type of non-ACA coverage.
Some people, like Davis, landed job-based coverage, while others found they qualified for Medicaid, the joint state-federal program for low-income residents.
Such churn in and out of ACA coverage is not unusual, Lopes noted. “People get a job. They get married. They age into Medicare,” the program for older or disabled people, she said.
The poll highlighted that many people dropping coverage were younger, between 18 and 29. About 14% of people in that range now say they are uninsured.
That’s not surprising, given that younger people tend to use health coverage less. ACA insurers said one reason they raised premiums this year was because they expected more young or healthy people to drop out, leaving them with a higher share of older, more costly enrollees. Among those 50 or older, the poll found that only 7% are now uninsured.
GOP critics of the now-expired enhanced subsidies say they were always meant to be temporary. Extending them would have cost about $350 billion from 2026 to 2035, .
But not extending them means more people will become uninsured. The CBO said the extension would have meant 3.8 million more people having insurance coverage in 2035.
KFF pollsters, in February and early March, surveyed 1,117 U.S. adults, more than 80% of the ACA enrollees originally polled in November, online and by telephone. The margin of error is plus or minus four percentage points for the full sample.
Are you struggling to afford your health insurance? Have you decided to forgo coverage? to contact ∫⁄¡œ≥‘πœÕ¯ News and share your story.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/kff-poll-aca-obamacare-higher-premiums-blame-trump-gop/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2171015&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>“I call it the unaffordable care act,” he said. He reprised the line in his address, blaming “the crushing cost of health care” on Obamacare.
Trump’s words also play off an ongoing congressional debate that began late last year with the expiration of the enhanced tax subsidies that had lowered the cost of ACA insurance for millions of Americans ‚Äî and thrust the issue of ACA-related costs back to center stage.
Without those enhanced subsidies, the amount people pay toward monthly Obamacare premiums doubled, on average. The number of people enrolled in ACA coverage for this year has dropped by more than a million, and experts say more people could abandon coverage once premiums come due. Democrats are using this development to crank up the heat on Republicans ahead of the November elections and steer the conversation on the affordability issue.
Republicans fault the law itself for driving up these costs. For instance, Rep. Mike Lawler (R-N.Y.) that premiums “skyrocketed across the country since it took effect.”
Critics routinely point to several provisions within the ACA as the culprits — among them, essential health benefits, or EHBs. Under the law, Obamacare plans must cover certain essential services, including emergency care, hospitalization, maternity, and prescription drugs, without annual or lifetime dollar limits. But connecting EHBs to the premium increases felt by consumers is not straightforward.
Here’s a primer on key issues involved.
Checking the Numbers
It’s clear that Obamacare premiums have increased.
An analysis by the right-leaning Paragon Health Institute shows that the average premium for a 50-year-old with Obamacare since 2014. The average premium for employer-based plans grew 68% during that same time.
Paragon’s president, , told ∫⁄¡œ≥‘πœÕ¯ News that this shows the ACA has made health care on the individual market more expensive.
Still, the comparison overlooks a couple of points. Pre-ACA, employer plans generally offered more generous coverage than individual market plans, so work-based coverage cost more. And individual plans were cheaper in part because they could bar applicants with health problems. Beginning in 2014, the ACA forced individual policies to look more like employer plans, covering a broader range of benefits and accepting both healthy and unhealthy applicants. As a result, premiums rose that first year. In the years that followed, ACA plans often experienced faster growth in premiums than job-based plans. Some policy analysts say this isn’t surprising because ACA plans started at a lower dollar base and had more room to rise.
States that saw less dramatic post-ACA premium increases, such as Massachusetts and New York, already mandated that individual-market plans provide EHB-like coverage, noted , a senior research fellow at the Heritage Foundation, a conservative think tank. These states also had higher premiums due to that and other provisions, such as not allowing plans to exclude people with preexisting conditions.
“It was a combination of things,” he said.
Blase acknowledges that the two types of insurance started at different price points. But he said the percentage change over time shows that the ACA faces “underlying inflationary pressures” ‚Äî including the now-expired, more generous, covid pandemic-era subsidies ‚Äî that affect its policyholders more so than employer plans.
Aside from that point, however, were on the rise even before the ACA took effect.
An analysis by Jonathan Gruber at the Massachusetts Institute of Technology found that between 2008 and 2010, premiums grew by at least 10% a year and were highly variable across states and insurers.
Consumers’ Other Costs
Over time, ACA deductibles ‚Äî the amounts policyholders must satisfy in a given year before insurance kicks in ‚Äî have seen large increases, with “bronze” plans now averaging $7,476 annually, up from $5,113 in 2014, according to KFF, a health information nonprofit that includes ∫⁄¡œ≥‘πœÕ¯ News. Bronze plans tend to have lower premiums than the other metal-level categories ‚Äî “silver,” “gold,” and “platinum” ‚Äî in part because of their higher deductibles.
The Trump administration is doubling down on high-deductible plans as part of its emphasis on affordability, making it easier this year for people age 30 and up to qualify for what are called “catastrophic plans.” These come with even larger deductibles than bronze plans.
The administration to cement those changes, saying it was designed to lower premiums and expand choices. It would raise next year’s deductibles for catastrophic plans to $15,600 a year for an individual or around $30,000 for a family. It isn’t clear how popular such plans would be. Detailed enrollment figures for this year are not yet available, but estimates indicate chose catastrophic plans in 2025, and consumers can’t use federal subsidies to purchase them.
Before this Trump proposal, though, recent data showed that the rising rate of ACA plan deductibles had not outpaced deductibles for employer plans.
The weighted average ‚Äî a calculation that gives more weight to ACA plans with the most people enrolled ‚Äî shows in annual deductible amounts since 2014, from $1,881 to $2,912. During that same period, deductibles in plans offered by 59%, from $1,186 to $1,886, according to KFF’s annual employer survey.
Essential What?
To be clear, the ACA’s catastrophic and bronze plans must cover essential health benefits, as do all Obamacare plans. These EHBs fall into 10 categories of medical services and were included in the ACA to ensure individual policies meet a minimum standard of coverage and are comparable to employer-based health insurance.
Preventive services, such as annual checkups, vaccines, and certain cancer screenings, must be covered at no additional cost to patients. All plans must completely cover the cost of specific vaccines, including the annual flu shot. And insurers cannot refuse to pay for emergency care provided at an out-of-network hospital. Other EHBs are subject to out-of-pocket costs, such as copays at the doctor’s office or pharmacy counter.
In some ways, EHBs save money because they’ve increased access to preventive care, said , a professor of health policy and management at Johns Hopkins University’s Bloomberg School of Public Health.
Services such as cancer screenings and lab tests can lead to earlier detection of serious conditions, when treatment is less costly, and positive outcomes are more likely.
“If you look down the list of essential health benefits, I think most people would reach the judgment that those are health care services that people should have access to,” said Larry Levitt, KFF’s executive vice president for health policy.
Joseph Antos, a senior fellow emeritus at the conservative American Enterprise Institute, said ACA requirements ‚Äî such as requiring insurers to accept anyone, regardless of their health status, and limiting insurers’ ability to charge older people more for coverage ‚Äî also have played roles in boosting premiums.
“Really, it’s practically impossible to tease any one thing out,” Antos said.
States do have latitude to add benefits that fall under the EHB umbrella. For example, bariatric surgery is covered as an EHB in , but not in . Pennsylvania’s EHBs also don’t include hearing aids, but do.
But the Trump administration’s 2027 regulatory proposal : When “states enact benefit mandates, plan premiums must generally increase to account for the additional coverage,” it reads. It also signals that added benefits can raise consumer costs and proposes that states be required to use their own funds to offset some of those costs.
Paragon’s Blase echoed this take in his bottom line. Mandating that plans cover EHBs without annual or lifetime caps, as required under the ACA law, encourages clinicians to overbill and overprescribe, he said. That drives up premiums and means a bigger check for insurers and medical providers at the expense of taxpayers. “You just turn patients into money factories,” he said.
, a senior research fellow at Georgetown University’s Center on Health Insurance Reforms, disagrees, saying that whatever EHBs’ role, they aren’t to blame for the year-over-year premium hikes.
People aren’t consuming medical care at exponential rates just because certain services are now covered: “Me not paying anything for that colonoscopy doesn’t make me want to get more of them,” she said.
Are you struggling to afford your health insurance? Have you decided to forgo coverage? to contact ∫⁄¡œ≥‘πœÕ¯ News and share your story.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/obamacare-essential-health-benefits-premium-costs-debate/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2164137&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The changes come as affordability is a key concern for many Americans, some of whom are struggling to pay their ACA premiums since enhanced subsidies expired at the end of last year. Initial enrollment numbers for this year .
Health care coverage and affordability have in the run-up to November’s midterm elections.
The proposed changes are part of a lengthy rule that addresses a broad swath of standards, including benefit packages, out-of-pocket costs, and health care provider networks. Insurers refer to these standards when setting premium rates for the coming year.
After a comment period, the rule will be finalized this spring.
It “puts patients, taxpayers, and states first by lowering costs and reinforcing accountability for taxpayer dollars,” said Centers for Medicare & Medicaid Services Administrator Mehmet Oz .
One way it would do so focuses heavily on a type of coverage — — that last year attracted only about 20,000 policyholders, , although put it closer to 54,000.
“To me, this proposal reads like the administration has found their next big thing in the catastrophic plans,” said Katie Keith, director of the Health Policy and the Law Initiative at the O’Neill Institute for National and Global Health Law at Georgetown University Law Center.
Such plans have very high annual out-of-pocket costs for the policyholder but often lower premiums than other ACA coverage options. Formerly restricted to those under age 30 or facing certain hardships, the Trump administration allowed older people who lost subsidy eligibility to enroll in them for this year. It is not yet known how many people chose to do so.
The payment rule cements this move by making eligible anyone whose income is below the poverty line ($15,650 for this year) and those earning more than 2.5 times that amount who lost access to an ACA subsidy that lowered their out-of-pocket costs. It also notes that a person meeting these standards would be eligible in any state — an important point because this coverage is in only 36 states and the District of Columbia.
In addition, the proposal would require out-of-pocket maximums on such plans to hit $15,600 a year for an individual and $27,600 for a family, Health Affairs. (The current out-of-pocket max for catastrophic plans is $10,600 for an individual plan and $21,200 for family coverage.) Not counting preventive care and three covered primary care doctor visits, that spending target must be met before a policy’s other coverage kicks in.
In the rule, the administration wrote that the proposed changes would help differentiate catastrophic from “bronze” plans, the next level up, and, possibly, spur more enrollment in the former. Currently, the proposal said, there may not be a significant difference if premiums are similar. Raising the out-of-pocket maximum for catastrophic plans to those levels would create that difference, the proposal said.
“When there is such a clear difference, the healthier consumers that are generally eligible and best suited to enroll in catastrophic plans are more motivated to select a catastrophic plan in lieu of a bronze plan,” the proposal noted.
However, ACA subsidies cannot be used toward catastrophic premiums, which could limit shoppers’ interest.
Enrollment in bronze plans, which currently have an average annual deductible of $7,500, has doubled since 2018 to about 5.4 million last year. This year, that number will likely be higher. Some states’ sign-up data indicates a shift toward bronze as consumers left higher-premium “silver,” “gold,” or “platinum” plans following the expiration of more generous subsidies at the end of last year.
The proposal also would allow insurers to offer bronze plans with cost-sharing rates that exceed what the ACA law currently allows, but only if that insurer also sells other bronze plans with lower cost-sharing levels.
In what it calls a “novel” approach, the proposal would allow insurers to offer multiyear catastrophic plans, in which people could stay enrolled for up to 10 years, and their out-of-pocket maximums would vary over that time. Costs might be higher, for example, in the early years, then fall the longer the policy is in place. The proposal specifically asks for comments on how such a plan could be structured and what effect multiyear plans might have on the overall market.
“As we understand it thus far, insurers could offer the policy for one year or for consecutive years, up to 10 years,” said Zach Sherman, managing director for coverage policy and program design at HMA, also known as Health Management Associates, a health policy consulting firm that does work for states and insurance plans. “But the details on how that would work, we are still unpacking.”
Matthew Fiedler, senior fellow with the Center on Health Policy at the Brookings Institution, said the proposed rule included a lot of provisions that could “expose enrollees to much higher out-of-pocket costs.”
In addition to the planned changes to bronze and catastrophic plans, he points to another provision that would allow plans to be sold on the ACA exchange that have no set health care provider networks. In other words, the insurer has not contracted with specific doctors and hospitals to accept their coverage. Instead, such plans would pay medical providers a set amount toward medical services, possibly a flat fee or a percentage of what Medicare pays, for example. The rule says insurers would need to ensure “access to a range of providers” willing to accept such amounts as payment in full. Policyholders might be on the hook for unexpected expenses, however, if a clinician or facility doesn’t agree and charges the patient the difference.
Because the rule is so sweeping — with many other parts — it is expected to draw hundreds, if not thousands, of comments between now and early March.
Pennsylvania insurance broker Joshua Brooker said one change he would like to see is requiring insurers that sell the very high out-of-pocket catastrophic plans to offer other catastrophic plans with lower annual maximums.
Overall, though, a wider range of options might appeal to people on both ends of the income scale, he said.
Some wealthier enrollees, especially those who no longer qualify for any ACA premium subsidies, would prefer a lower premium like those expected in catastrophic plans, and could just pay the bills up to that max, he said.
“They’re more worried about the half-million-dollar heart attack,” Brooker said. It’s tougher for people below the poverty level, who don’t qualify for ACA subsidies and, in . So they’re likely to go uninsured. At least a catastrophic plan, he said, might let them get some preventive care coverage and cap their exposure if they end up in a hospital. From there, they might qualify for charity care at the hospital to cover out-of-pocket costs.
Overall, “putting more options on the market doesn’t hurt, as long as it is disclosed properly and the consumer understands it,” he said.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/aca-trump-proposal-catastrophic-coverage-premiums-care-networks/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2155711&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>It’s all part of a drama that roiled the ACA’s 2026 open enrollment period. Congressional debate over whether to extend more generous subsidies made available under the Biden administration led to and focused public attention on rising health care costs and the affordability issue.
The enhanced subsidies, which expanded eligibility both by lowering the percentage of household income people had to pay toward their care and removing an income cap, expired at the end of last year. As a result, just about everyone buying ACA coverage saw their costs increase. For some, what they paid toward premiums doubled or more, even though less generous subsidies remain in place.
Many experts expected ACA enrollment, which hit a record 24 million in 2025, to fall this time around.
“If you raise the price of something a whole lot, economics tell us that a lot of people will buy less of it or not buy at all,” said Katherine Hempstead, a senior policy officer with the Robert Wood Johnson Foundation.
Here are things to watch now:
Initial Numbers Aren’t Final
The in December 2024 that not extending the enhanced subsidies would cause 2.2 million people to lose insurance in 2026, with further increases in following years. Analysts with the Wakely Consulting Group would opt out of insurance for this year.
Data released Jan. 28 by federal officials showed a year-over-year enrollments across the federal healthcare.gov marketplace and those run by states. Overall, there were 23 million enrollees, including 3.4 million new to ACA coverage.
At about the same time last year, there were , with 3.9 million new to the marketplaces.
But there’s more to it than those initial numbers.
For one thing, both years’ data was pegged to Jan. 15 for the federal marketplace, which closed its open enrollment period that day. But, the data for the states that run their own marketplaces included sign-ups in most cases only through Jan. 10 or 11, even though some held open enrollment until the . Thus, the numbers don’t reflect what might have happened in those last days. Was there a surge in state sign-ups? Or, conversely, did the marketplaces see more enrollees cancel their coverage?
Additionally, those initial numbers are a mix of newly minted ACA enrollees and existing customers, many of whom were auto-reenrolled for 2026 — which raises other issues.
For existing, reenrolled policyholders, the real figures won’t be known for weeks or months, when it becomes clear how many actually pay their premiums. Some consumers may not have focused on their reenrollment costs or may have hoped Congress would extend the subsidies.
That’s an important factor to keep in mind because the CBO and Wakely estimates of millions losing insurance were based on projections for full-year coverage, not initial sign-ups.
In the coming weeks, “consumers may find they really can’t afford the premiums and cancel their plans, while carriers may also cancel coverage for nonpayment,” said Pat Kelly, executive director of Your Health Idaho, a state-based ACA marketplace, during a Jan. 22 call with reporters.
Sharp Differences in State Enrollment Patterns
Changes are also afoot in the 19 other states (and the District of Columbia) that , some of which have issued more detailed data about enrollment than the federal marketplace.
Most states saw lower enrollment for 2026 than the prior year, with the biggest drop in North Carolina, where sign-ups fell by nearly 22%, federal data shows.
In a few states — including New Mexico, Texas, California, and Maryland, as well as the District of Columbia — the number of people selecting ACA plans increased.
The jump was largest in New Mexico, with its initial number of people selecting plans up by nearly 14%. Increases were in the single digits in the other states and Washington, D.C.
New Mexico — uniquely — used its own tax dollars to fully offset the loss of the more generous federal tax subsidies for all consumers. , including California, Colorado, Maryland, and Washington, used state money to help some enrollees.
The , a collective of 22 state marketplaces supported by the National Academy for State Health Policy, said initial enrollment figures . Compared with the same time last year, outright plan cancellations are up 83% in Colorado, disenrollments are four times what they were in Idaho, and Virginia has seen cancellations double.
New enrollments are from the same period last year, according to data from the state. In Pennsylvania, people ages 55 to 64, the group with the highest premiums, and young people 26 to 34 in higher numbers than other age groups, state data shows.
“We have drastically higher rates of people dropping their coverage,” said Devon Trolley, executive director of the Pennsylvania Health Insurance Exchange Authority. “We had 70,000 drop in the last two months, from early retirees to small-business owners to farmers not knowing how to make ends meet.”
On Feb. 9, Pennsylvania released , showing enrollment dropped by about 2% from last year, although that figure masks some of the effects. The state says nearly 18% of enrollees dropped coverage altogether, with older and rural residents being the most likely to fall out.
Some Republicans credited Trump-administration-backed anti-fraud measures, which included a range of , for tightening the system. Although some of those actions were paused by a federal court and have not taken effect, those ACA critics, some of whom have produced that millions may have been improperly enrolled, say that’s behind the decline. They have previously for unauthorized enrollments or ACA plan-switching by commission-seeking brokers.
States that run their own ACA marketplaces, however, reported little or no such unauthorized switching. Relative to the federal marketplace, the state-based ACA platforms employ additional safeguards to prevent brokers from accessing consumers’ coverage without authorization.
Among consumers not returning to the marketplace, the main reason is cost, said Mila Kofman, executive director of the DC Health Benefit Exchange Authority, which runs the district’s ACA marketplace.
“When we looked at who these folks are, half are small-business owners,” Kofman said. “They are not folks committing fraud.”
Lower Premiums, Higher Deductibles
Rather than sticking with automatic reenrollment, existing customers in many states shifted sharply into lower-priced “bronze” plans that come with higher deductibles than silver, gold, and platinum plans.
California saw 73% of renewing members who switched plans move to a bronze plan, up from 27% at the same time last year, the State Marketplace Network reported. In Maine, bronze enrollment now represents almost 60% of all plans purchased.
People are “looking at what works in their monthly budget, looking for that lower premium,” said Stacey Pogue, a senior research fellow at the Center on Health Insurance Reforms at Georgetown University. “Some might be crossing their fingers that they won’t need to meet their deductible.”
On average, bronze plans have an . All ACA plans are required to cover certain preventive services — such as some vaccinations, cancer screenings, and other tests — without a copayment or deductible, but most everything else is covered only after an annual deductible is met.
High deductibles can lead some patients to avoid seeking medical care, Hempstead said.
“People are terrified to use their care,” she said. “They may delay something until it’s more serious.”
She added that medical providers, including hospitals and doctors, are bracing for an increase in the number of insured patients who can’t afford to pay their deductibles.
“Everyone is anticipating that hospitals will have to give out more charity care, which will hurt their bottom lines and might lead them to have to lay off people or close or reduce services,” she said.
Are you struggling to afford your health insurance? Have you decided to forgo coverage? Click here‚ÄØto contact ∫⁄¡œ≥‘πœÕ¯ News and share your story.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/affordable-care-act-aca-obamacare-sign-ups-subsidies-higher-premiums/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2150584&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>His monthly premium payment of $435 for family coverage is roughly the same as the insurance at his previous job. But the policy at his current job carries an annual deductible of $4,000, which he must pay out-of-pocket for his family’s care until he reaches that amount each year.
“Now everything is full price,” said the 53-year-old, who works at a warehouse just south of Dallas-Fort Worth. “That’s been a little bit of a struggle.”
To reduce his costs, Garza switched to a lower-cost diabetes medication, and he no longer wears a continuous glucose monitor to check his blood sugar. Since he started his job nearly two years ago, he said, his blood sugar levels have inched upward from an A1c of 7% or less, the target goal, to as high as 14% at his most recent doctor visit in November.
“My A1c is through the roof because I’m not on, technically, the right medication like before,” Garza said. “I’m having to take something that I can afford.”
Plans with high deductibles — the amount that patients must pay for most medical care before insurance starts pitching in — have become increasingly common. In 2024, participating in medical care plans were offered this type of insurance, up from 38% in 2015, according to federal data. Such plans are also offered through the Affordable Care Act marketplace.
With and many of the subsidies to help people pay for them poised to expire at year’s end, more people face tough choices as they weigh monthly premium costs against deductibles. To afford insurance at all, people may opt for a plan with low premium payments but with a high deductible, gambling that they won’t have any medical crises.
But high-deductible plans pose a particular challenge for those with chronic conditions, such as the who live with Type 1 or Type 2 diabetes. Adults with diabetes who are involuntarily switched to a high-deductible plan, compared with adults on other types of insurance, face an 11% higher risk of being hospitalized with a heart attack, a 15% higher risk of hospitalization for a stroke, and that they’ll go blind or develop end-stage kidney disease, according to a study published in 2024.
“All of these complications are preventable,” said , the study’s lead author.
Care vs. Cost
The initial rationale behind such high-deductible plans was to encourage people to become wiser health care shoppers, said McCoy, an associate professor of medicine at the University of Maryland School of Medicine in Baltimore. And they can be a good fit, proponents say, for people who don’t use a lot of medical care or who have cash on hand for a health crisis.
But while people with an excruciating earache will seek care, McCoy said, those with unhealthy blood sugar levels might not feel as urgent a need to seek treatment — despite the potential long-term damage — given the acute financial pain.
“You have no symptoms until it’s too late,” she said. “At that point, the damage is irreversible.”
Overall, medical care for people with diabetes costs insurers and patients an average of the disease, according to an analysis. Type 2 diabetes, the more common form, is diagnosed when the body can no longer process or produce enough insulin to adequately regulate blood sugars. With Type 1, the body can’t produce insulin. Those with the disease may end up on the financial hook not just for insulin and other types of medication but for related equipment.
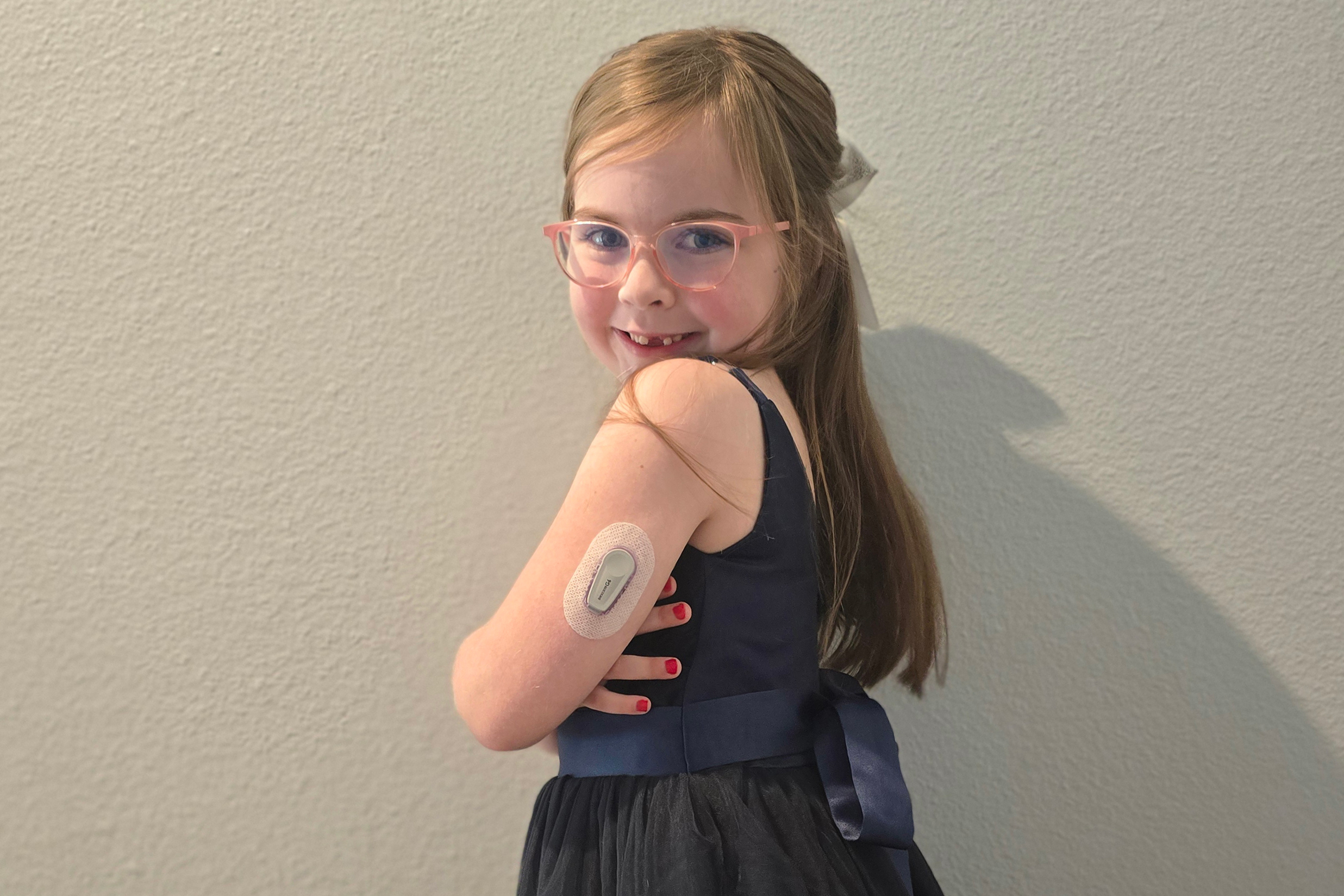
Mallory Rogers, whose 6-year-old daughter, Adeline, has Type 1, calculates that it costs roughly $1,200 a month for insulin, a pump, and a continuous glucose monitor. That figure doesn’t include the cost of emergency supplies needed in case Adeline’s technology malfunctions. Those include another type of insulin, blood-testing strips, and a nasal spray that’s nearly $600 for a two-pack of vials ‚Äî supplies that must be replaced once a year or more frequently.
“If she doesn’t have insulin, it would become an emergency situation within two hours,” said Rogers, a technology consultant who lives in Sanford, Florida. Rogers has been saving for the coming year when her daughter moves to the high-deductible health plan offered by Rogers’ employer, which has a $3,300 deductible for family coverage.
Taxing Decisions
Many insurance plans carry increasingly high deductibles. But to be defined as a high-deductible health plan ‚Äî and thus be eligible to offer a health savings account ‚Äî a plan’s deductible for 2026 must be , according to IRS rules.
Health savings accounts enable people to squirrel away money that can be rolled over from year to year to be used for eligible medical expenses, including prior to meeting a deductible. Such accounts, available through a plan or employer, can provide tax benefits. The contributions are limited to $4,400 individually and $8,750 for a family in 2026, and employers may contribute toward that total. Rogers’ employer pays $2,000 spread out over the year, and Garza’s contributes $1,200.
Rogers recognizes that she’s fortunate to have accumulated $7,000 so far in her health savings account to prepare for her daughter’s insurance shifting to Rogers’ plan.
“Adding a financial burden to an already very stressful medical condition, it hurts my heart,” she said, reflecting on those who can’t similarly stockpile. “Nobody asks to have diabetes, Type 1 or Type 2.”
The median deductible for employer health insurance plans was $2,750 in 2024, but deductibles can run $5,000 or higher, said George Huntley, CEO of both the and .
When deductibles are too high, Huntley said, routine maintenance is what patients skimp on: “You don’t take the drug that you’re supposed to take to maintain your blood glucose. You ration your insulin, if that’s your scenario. You take pills every other day.”
Garza knows he should do more to control his blood sugar, but financial realities complicate the equation. His previous health plan covered a newer class of diabetes medication, called a GLP-1 agonist, for $25 a month. He wasn’t charged for his remaining medications, which included blood pressure and cholesterol drugs, or his continuous glucose monitor.
With his new insurance, he pays $125 monthly for insulin and several other medications. He doesn’t see his endocrinologist for checkups more than twice a year.
“He wants to see me every three months,” Garza said. “But I told him it’s not possible at $150 a pop.”
Plus, he typically needs lab testing before each visit, an additional $111.
In 2026, the deductible for a “silver”-level plan on the marketplace will average $5,304 without cost-sharing reductions, according to an analysis from KFF, a health information nonprofit that includes ∫⁄¡œ≥‘πœÕ¯ News. For a . An annual visit and some preventive screenings, such as a mammogram, would be covered free of cost to the patient.
Moreover, people , whether through their employer or the marketplace, should figure out their annual out-of-pocket maximum, which still applies after the deductible is met, Huntley said.
Garza’s family policy requires him to pay 20% until he reaches $10,000, for example.
Given Garza’s high blood sugar levels, his doctor prescribed a fast-acting form of insulin to take as needed with meals, which costs an additional $79 monthly. He planned to fill it in December, when he’s responsible for only 20% of the cost after he has hit his deductible but not yet reached his out-of-pocket maximum.
Garza likes his job despite its health plan, saying he’s never missed a day of work, even recently when he had a stomach bug. As of late 2025, he remained conflicted about whether to sign up for health insurance when his company’s enrollment period rolls around in mid-2026.
He worries that dropping insurance would place his family too much at risk if a major medical crisis struck. Still, he pointed out, he could then use the money he now spends on monthly premiums to directly pay for care to better manage his diabetes.
“I’m just stuck, to be honest with you,” he said.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/high-deductible-plans-out-of-pocket-diabetes-care/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2124505&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>LISTEN: Obamacare. COBRA. Deductibles. Coinsurance. There’s a lot to figure out when you’re on your own looking for health insurance for the first time. ∫⁄¡œ≥‘πœÕ¯ News senior contributing editor Elisabeth Rosenthal appeared on WAMU’s “Health Hub” series on Sept. 24 to help young adults find a plan that meets their needs.
Many young adults are staring down an “insurance cliff” as they turn 26. That’s the age when many can no longer stay on their parents’ health insurance. If they can’t get coverage through their job, they’ll need to start looking for their own. The search can be nerve-racking and confusing. ∫⁄¡œ≥‘πœÕ¯ News senior contributing editor Elisabeth Rosenthal appeared on WAMU’s “Health Hub” on Sept. 24 to share some tips for finding the right plan.
Read her full article for more help starting your search.
Already have an Affordable Care Act insurance plan? Check out KFF’s to find out how much more you may have to pay next year if enhanced tax credits expire.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/listen-wamu-health-hub-rosenthal-turning-26-insurance-cliff-aca-subsidies/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2093507&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The agency that oversees the ACA that it would expand eligibility for “catastrophic” plans sold in Affordable Care Act online marketplaces. The plans require people to spend more than $10,000 a year on deductibles before the policies pay most medical costs but carry lower monthly premiums than other Obamacare policies.
The move reflects growing concern among Republicans about political backlash if Congress doesn’t extend larger tax credits put in place during the covid-19 public health emergency to help consumers pay their premiums. The extra subsidies are set to expire at the end of the year, resulting in an in the amount people pay for coverage, according to KFF, a health information nonprofit that includes ∫⁄¡œ≥‘πœÕ¯ News.
A small, bipartisan group of House lawmakers introduced legislation to extend the enhanced covid-era subsidies for one more year, which would keep them in place through midterm congressional elections in fall 2026.
But , with many Republicans opposed to extending the extra tax credits, with a permanent change costing . Without an extension, tax credit amounts would revert to pre-pandemic levels.
“They spent the last 15 years against the ACA, so a lot will be steadfast, but others are worried about the effect of massively spiked premiums on their constituents,” noted a Democratic Senate staffer who asked not to be identified because they weren’t authorized to speak to the media.
Republicans currently control Congress by slim margins, raising the stakes if voters who lose their ACA tax credits blame them at the ballot box.
Catastrophic plans are a little-known type of Obamacare policy that have previously been limited mainly to people under age 30. While they come with lower monthly premiums than other types of ACA plans, the coverage has higher annual deductibles, which are set at the out-of-pocket maximum for the year: $10,600 for individuals in 2026 or $21,200 for families.
A deductible is the amount patients must spend on health care before insurance plans pay for most services. Catastrophic plans do cover three primary care visits a year without having to pay the full deductible and, as with other ACA policies, policyholders pay nothing for preventive services such as some cancer screenings and vaccines.
The catastrophic plans will automatically show up on the federal marketplace, healthcare.gov, for consumers who lose tax credit coverage entirely next year due to their household income. Another category of consumers — people who continue to qualify for tax credits but not for subsidies that reduce out-of-pocket costs — may also be eligible but would have to send in paperwork.
“By expanding access to catastrophic plans, we are making sure hardworking people who face unexpected hardships can get affordable coverage that protects them from devastating medical costs,” Centers for Medicare & Medicaid Services Administrator Mehmet Oz .
It isn’t clear whether the policy changes will make the plans more attractive to consumers. Catastrophic plans aren’t available in all states, and the size of the deductibles can be off-putting.
“It’s a ton of money,” , a health insurance analyst and broker who writes regularly about the ACA. “A full-price catastrophic plan is still more expensive than some people can afford, but they’re doing this to offer a slightly more affordable option.”
Catastrophic plans have had limited appeal, with 24 million enrollees currently opting for the coverage, according to government data, Norris said.
“Uptake has always been quite low,” said Katie Keith, director of the O’Neill Institute’s Center for Health Policy and the Law at Georgetown University. “It’s not a bad option if it is the only option you have. I question whether consumers are looking for this kind of coverage.”
CMS plans to grant people a “hardship” designation to enroll in catastrophic plans if they lose eligibility for ACA tax credits next year. Most likely to qualify are people earning more than four times the federal poverty rate ($62,600 for an individual this year, or $106,600 for a family of three), who will lose access to all premium subsidies if Congress does not extend the current enhanced tax credits. It’s also unclear how much premiums will cost. Insurers, reacting to the new administration guidance, might seek to recalculate their rates based on what they estimate may be an influx of older people into the plans, Norris said.
AHIP, the insurance industry lobbying group, is pushing hard for the larger tax credits to be extended. It did not comment specifically on how the new guidance might affect catastrophic health plan premiums. Still, AHIP spokesperson Chris Bond said that “while catastrophic plans can provide important coverage for specific needs, they are not a replacement for affordable comprehensive coverage.”
There are other hurdles. Norris said insurers don’t offer plans at all in 10 states: Alaska, Arkansas, Indiana, Louisiana, Mississippi, New Mexico, Oregon, Rhode Island, Utah, and Wyoming. And where they are available, options are few. This year, for example, a 25-year-old in Orlando, Florida, had a choice of 61 “bronze” plans, the cheapest level of coverage available to all ACA shoppers, but just three catastrophic plans.
Policy experts say the expanded eligibility for catastrophic plans makes it more important than ever for consumers to consider all options when shopping for ACA coverage during the annual open enrollment period, which starts Nov. 1. In addition to the catastrophic and bronze plans, there are also “silver” and “gold” plans, each with varying premiums and deductibles.
Bronze plans have the lowest premiums but the highest deductibles; the , which is still lower than the catastrophic plans, according to KFF.
Catastrophic plan deductibles, while high, are comparable to some bronze plans, Norris noted. People who choose catastrophic plans are not eligible for any ACA tax subsidies to help pay monthly premiums.
A pending court battle may provide lawmakers concerned about voter pushback on Obamacare changes an unintended reprieve.
In late August, a federal judge in Maryland temporarily put on hold some changes the Trump administration had ordered for next year. Those changes, included by the administration, would have added additional verification paperwork requirements for some people enrolling in ACA plans, and were challenged by several cities, which cited government estimates that the changes could to lose their insurance in 2026.
The court ruling including income verification requirements that would affect people below the poverty level and those without tax return information. The move also paused verification requirements affecting people who apply outside the annual open enrollment period and blocked a $5 monthly charge for people who are automatically enrolled into plans in which subsidies cover the entire premium — unless they contact the marketplace and confirm their selection.
The Trump administration is appealing the decision, but the case may not be settled until next year, said Keith at Georgetown University.
That makes it likely that the pause of the new requirements will stay in place for this year’s open enrollment season.
Keith said the ruling was a “bigger deal” than expanding eligibility for catastrophic plans. “Consumers all across the country won’t have to deal with red tape the Trump administration rushed to put into place ahead of the new plan year,” and the ruling also “helps people keep their coverage.”
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/obamacare-catastrophic-plans-health-insurance-aca-trump/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2088212&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>When the Affordable Care Act was passed in March 2010, the goal was to help more Americans get health insurance. And, indeed, the establishment of online marketplaces and a broadening of the eligibility guidelines for Medicaid accomplished that.
Fifteen years later, however, that system is anything but user-friendly.
Young adults looking for health insurance will likely benefit from talking with so-called navigators who work for the online marketplaces. But if you want to go it alone, here are some tips about shopping for a plan, based on the advice of policy experts and people who have spent hundreds of hours helping others navigate this unwieldy set-up.
Buckle up.
Start Here
Begin your search at least two months before your 26th birthday. In some cases, you can sign up for a plan in advance so that it takes effect on your birthday.
First, find out if your family plan ends on your birthday or at the end of your birthday month. A few states allow young adults to stay on their family plan until they are 29, with certain conditions and, generally, higher costs. A navigator will know more.
You may have the option to stay, for a limited time, on your family’s plan under that allows those with group health plans to extend their coverage past age 26. Odds that you will be approved for an extension are even higher if you can claim a disability.
Be aware, though, that this option will involve a considerable expense, since you will be required to pay the entire premium (the employer will no longer pay what is usually a substantial share). Those who claim a disability can often stay on the family plan after age 26, depending on the type of insurance the family holds.
If you’re undergoing medical treatment and can’t change hospitals or doctors, paying this premium may be your best course. You don’t have this option, however, if your family is insured through an Obamacare plan.
Before you start your search, make a list of the medicines and physicians you rely on, and highlight those you can’t do without. Rank them, even.
It’s quite likely that you will have fewer choices on the marketplace than you had on a parent’s plan. Be prepared to make some switches and trade-offs.
Find the Right Marketplace
Thirty-two states have adopted the federal marketplace as the place residents can go to compare and buy insurance policies. The rest run their own online marketplaces. You can for insurance policies in your state.
Make sure you land at an official ACA website. There are many look-alikes run by private insurance brokers. The federal marketplace is found at and nowhere else.
Note that official state marketplaces sometimes have unusual names. The New York State of Health, Kynect (Kentucky), Covered California, and CoverMe (Maine) are examples.
In states that use the federal marketplace, shoppers can . On the state-based marketplaces, there is often a “find local help” button or a tab that directs you to a person who can help you find a good plan.
You will generally be asked to choose a broker, who is paid a commission if you sign up, or an “assister,” who provides the service at no cost. Assisters have received special training in the marketplace they serve, and, because they provide the service free, they have no financial incentive to steer you to a plan that pays a commission to the seller.
Assisters are often navigators who are funded by the marketplace, but in some cases they work for hospitals, health plans, or local nonprofits. You’ll have to ask.
While navigators are generally a surefire option for sound advice, they may become harder to find now that the Trump administration has cut funding for them in states that rely on the federal marketplace. (States that run their own marketplaces are unaffected.)
Many nonprofits and states run excellent programs that offer free assistance. And if, for example, you’re in the middle of cancer treatment, an assister affiliated with your hospital may offer better advice on picking a plan, since they will know which ones have contracts that may cover more of your expenses.
Ideally, these experts will walk you through the process and know which buttons to push to ensure you get the best coverage for your needs at the best rate for which you are eligible.
Sign Up
Once you’re on an official website that markets plans under the ACA, you will be asked to enter your personal information as well as an estimate of your income.
Forty states and the District of Columbia cover single young adults with no children under Medicaid if their income is low enough to qualify. If you’re eligible, you should be redirected to the Medicaid website to start the enrollment process, or you may enroll directly on the marketplace site.
But be aware that the Republicans’ recently passed domestic policy bill has increased the requirements and the paperwork required to get on, and stay on, Medicaid.
Medicaid, a joint federal and state program that provides health insurance to low-income Americans, does not charge its members a premium, and it covers medications at a nominal cost or free. The caveat is that those enrolled in the program have a smaller number of in-network doctors and hospitals to choose from.
If your income is above the threshold for Medicaid, you will need to shop on the marketplace for a policy.
On most sites, a search tool allows you to check whether your doctor or hospital is in a particular plan’s network. But beware: The directories on which this search relies are notoriously inaccurate, despite federal laws mandating otherwise.
So, before you select a plan, call the doctor or hospital to confirm they accept the insurance plan you’re considering purchasing.
Do the Math
When it comes to the math, it’s better to work on a computer than a phone. Generally, you can compare the costs of, and coverage offered by, only three plans at a time.
The following factors include premiums (taking account of any subsidy you get based on your income), as well as other expenses you’ll have to pay, called collective cost sharing:
- The deductible ‚Äî the amount you generally have to pay out-of-pocket before your insurance kicks in. (You may get a few “covered” visits with a primary care doctor; these won’t count against the deductible.)
- Copayments — a fixed payment that you owe for any visit to a doctor or emergency room.
- Coinsurance (this one can break the bank) — a percentage of the total bill, generally applied to hospital bills, that you have to pay. The plan may make it sound small, say, 10% to 30%. But if you have, for example, the common 80-20 split (in which the insurer pays 80% and you pay 20%), that can add up to a substantial sum. A single day in the hospital can cost tens or even hundreds of thousands of dollars, and 20% percent of that is a large amount.
- The out-of-pocket maximum ‚Äî the most you’ll have to pay out in a year, so long as you stay in network and pay the deductible.
Doing the math means looking at this holistically, balancing what you can pay in a premium against what you can afford for the above charges. If the deductible is over $3,000 and the out-of-pocket maximum allowed yearly is $9,200 — do you have that much money on hand?
Generally, the lower the monthly premium in a plan, the higher the share of costs you’ll have to pay should you need medical care. Note that an insurer may offer very different plans on the same marketplace, with different payment policies and networks.
People with incomes up to 2¬Ω times the poverty level may gain some relief from cost-sharing charges, but only if they sign up for silver plans. Plans are typically labeled bronze, silver, gold, and platinum; each tier reflects the percentage of your medical expenses that your plan pays overall. Bronze plans offer the least amount of coverage.
Choose Wisely
Once you’ve narrowed your choices to a few plans, study each closely.
A plan with a low deductible might require a $1,000 daily copayment, or 50% coinsurance (you pay 50%) for hospital stays. A plan that lists your desired hospital system as in-network may include only some of its locations, and not necessarily the ones close to you or that offer the type of care you need.
When looking at a plan’s details, make sure to scroll down and read its “summary of benefits and coverage” for examples of the plan’s coverage of common medical needs. Pay close attention to which services require preauthorization and, for example, how many physical therapy visits they’ll cover each year. Preauthorization can be a long and cumbersome process.
Generally, the lower the premium, the more preauthorization will be required and the more limited the coverage will be. And check what drugs the plan covers (called the formulary) to see if yours are included, as well as its network of providers, to see whether your doctors are in it.
Marketplace plans tend to have limited offerings compared with job-based insurance; there aren’t as many doctors and hospitals to choose from. Click on the “provider directory” to see if an insurer’s network includes doctors and specialists you’re most likely to need, and hospitals that are acceptable and accessible to you.
Check to see if the policy offers any coverage for out-of-network providers. Some will pay, say, 60% or 70% of approved charges. It’s a useful perk if you need to see an out-of-network specialist, or if the wait for an in-network appointment is too long.
One that patients with marketplace plans have access to only 40% of doctors near their home, on average, and in some areas that figure was as low as 25%. It’s quite likely even lower for mental health providers.
A Backstop
If you’ve tried to choose a plan and you’re still confused, look for one of the “easy pricing” or standard plans. These conform to certain basic standards laid out by the federal Centers for Medicare & Medicaid Services, which oversees the marketplaces for the federal government. These plans offer some primary care appointments before you have to start paying the deductible.
The government says these “easy pricing” on federal marketplace sites. But they may be identified differently on state-run marketplaces. In New York state, for example, they are simply marked with an ST (for standard).
Still, funding for premium subsidies is in place for this year at least, and free expert assistance is still out there, so don’t delay. There are good deals to be had, if only you put in the work.
Good luck.
∫⁄¡œ≥‘πœÕ¯ News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF‚Äîan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-care-costs/guide-find-insurance-at-age-26/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2066309&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>That is the age at which the Affordable Care Act declares that young adults generally must get off their family’s plan and figure out their coverage themselves.
When the ACA was voted into law in 2010, what’s known as its dependent coverage expansion was immediately effective, to millions of young Americans up to age 26 who would otherwise not have had coverage.
But for years, Republicans have whittled away at the infrastructure of the original ACA. Long gone is the requirement to buy insurance. Plans sold in the ACA’s online insurance marketplaces have no stringent quality standards. Costs keep rising, and eligibility requirements and subsidies are moving targets.
The erosion of the law has now created an “insurance cliff” for Americans who are turning 26 and don’t have a job that provides medical coverage.
Some, scared off by the complexity of picking a policy and by the price tags, tumble over the edge and go without insurance in a health system where the rate for an emergency room visit can be thousands, if not tens of thousands, of dollars.
Today, an estimated 15% of 26-year-olds go uninsured, which, according to a KFF analysis, is the highest rate among Americans of any age.
If they qualify, young adults can sign up for Medicaid, the federal-state program for Americans with low incomes or disabilities, in most but not all states.
Otherwise, many buy cheap subpar insurance that leaves them with insurmountable debt following a medical crisis. Others choose plans with extremely limited networks, losing access to longtime doctors and medicines.
They often find those policies online, in what has become a dizzyingly complicated system of government-regulated insurance marketplaces created by the ACA.
The marketplaces vary in quality from state to state; some are far better than others. But they generally offer few easily identifiable, affordable, and workable choices.
“The good news is that the ACA gave young people more options,” said Karen Pollitz, who directed consumer information and insurance oversight at the Department of Health and Human Services during the Obama administration.
“The bad news is the good stuff is hidden in a minefield of really bad options that’ll leave you broke if you get sick.”
Publicly funded counselors called “navigators” or “assisters” can help insurance seekers choose a plan. But those programs vary by state, and often customers don’t realize that the help is available. The Trump administration has cut funding to publicize and operate those navigator programs.
In addition, changes to Medicaid eligibility in the policy bill recently passed by Congress could mean that millions more ACA enrollees , according to the Congressional Budget Office.
Those changes threaten the very viability of the ACA marketplaces, which currently provide insurance to 24 million Americans.
In dozens of interviews, young adults described the unsettling and devastating consequences of having inadequate insurance, or no insurance at all.
Damian Phillips, 26, a reporter at a West Virginia newspaper, considered joining the Navy to get insurance as his 26th birthday approached. Instead, he felt he “didn’t make enough to justify having health insurance” and has reluctantly gone without it.
Ethan Evans, a 27-year-old aspiring actor in Chicago who works in retail, fell off his parents’ plan and temporarily signed up for Medicaid. But the diminished mental health coverage meant cutting back on visits to his longtime therapist.
Rep. Maxwell Frost, a Florida Democrat and the first Gen Z member of Congress, was able to quit his job and run for office at 25 only because he could stay on his mother’s plan until he turned 26, he said.
Now 28, he is insured through his federal job.
“The ACA was groundbreaking legislation, including the idea that every American needs health care,” he said. “But there are pitfalls, and one of them is that when young adults turn 26, they fall into this abyss.”
Why 26?
Back in 2010, the decision to make 26 the cutoff age for staying on a parent’s insurance was “kind of arbitrary,” recalled Nancy-Ann DeParle, deputy chief of staff for policy in the Obama White House.
“My kids were young , and I was trying to imagine when my child would be an adult.”
Before that time, children were often kicked off family plans at much younger ages, typically 18.
The Obama administration’s idea was that young adults were most likely settling into careers and jobs with insurance by 26. If they still didn’t have access to job-based insurance, Medicaid and the ACA marketplaces would offer alternatives, the thinking went.
But over the years, the courts, Congress, and the first Trump administration eviscerated provisions of the ACA. By 2022, a shopper on a federal government-run marketplace had more than 100 choices, many of which included expensive trade-offs, presented in a way that made comparisons difficult without spreadsheets.
Jack Galanty, 26, a freelance designer in Los Angeles, tried to plan for his 26th birthday by seeking coverage on the California insurance marketplace that would ensure treatment for his mild cerebral palsy and for HIV prevention.
“You’re scrolling for what feels like years, looking at 450 little slides, at the little bars, and trying to remember, ‚ÄòWas the one I liked No. 12 or 13?’” he recalled. “It feels like it’s nearly impossible to make a good choice in this scenario.”
Out-of-pocket expenses have soared. Complex plans in the lightly regulated marketplaces featured rising premiums, high deductibles, and requirements that patients pay a significant portion of the cost of care, often 20% — a charge known as coinsurance.
More than half of Americans ages 18 to 29 have incurred medical debt in the past five years, a ∫⁄¡œ≥‘πœÕ¯ News data investigation found. Few have the reserves to pay it off.
The networks of doctors to choose from in these plans are often so limited that an insured person struggles to get timely appointments. It can even be hard to find the official websites amid an explosion of look-alikes operated by commercial brokers.
Sharing her contact information with one site that appeared legitimate left Lydia Herne, a social media producer in Brooklyn, “drowning” in texts and phone calls offering plans of uncertain and unregulated quality. “It never ends,” said Herne, 27.
Young Invincibles, an advocacy group representing young adults, runs its own “navigator” program to help young people choose health insurance plans.
“We hear the frustration,” said Martha Sanchez, the group’s former director of health policy and advocacy. “Twenty-six-year-olds have had negative experiences in a process that’s become really complex. Many throw up their hands.”
Elizabeth Mathis, 29, and Evan Pack, 30, a married couple in Salt Lake City, turned to the marketplaces two years ago, after Pack went uninsured for a “really scary” year after he turned 26.
“Every time he got in the car, I thought, ‚ÄòWhat if?’” Mathis said.
The couple pays more than $200 a month for a high-deductible health plan backed by a federal subsidy (the kind set to expire next year). It’s a significant expense, but they wanted to be sure they had access to contraception and an antidepressant.
But last year, Pack suffered serious eye problems and underwent an emergency appendectomy. Their plan left them $9,000 in debt, for medical care billed at over $20,000.
“Technically, we gambled in the right direction,” Mathis said. “But I don’t feel like we’ve won.”
The Affordability Problem
The ACA was supposed to help consumers find affordable, high-quality plans online. The legislation also tried to expand Medicaid programs, which are administered by states, to provide health insurance to low-income Americans.
But the Supreme Court ruled in 2012 that states could not be forced to expand Medicaid. Ten states, led mostly by Republicans, have not done so, leaving up to 1.5 million Americans, who could have qualified for coverage, .
Even where Medicaid is available to 26-year-olds, the transition has often proved precarious.
Madeline Nelkin of New Jersey, who was studying social work, applied for Medicaid coverage before her 26th birthday in April 2024 because her university’s insurance premiums were more than $5,000 annually.
But it was September before her Medicaid coverage kicked in, leaving her uninsured while she fought a chest infection over the summer.
“People tell you to think ahead, but I didn’t think that meant six months,” she said.
When Megan Hughes, 27, of Hartland, Maine, hit the cliff, she went without. An aide for children with developmental delays, she has a thyroid condition and polycystic ovary syndrome.
She looked for a health care plan but found it hard to understand the marketplace. (She didn’t know there were navigators who could help.) Now she can’t afford her medicine or see her endocrinologist.
“I’m tired all the time,” Hughes said. “My cycles are not regular anymore at all. When I do get one, it’s debilitating.” She is hoping a new job will provide insurance later this year.
Traditionally, most Americans with private health insurance got it through their jobs. But the job market has changed dramatically since the ACA became law, particularly in the wake of the pandemic, with the rise of a gig economy.
Over said in recent surveys that they were working or have worked in short-term, part-time, or irregular jobs.
The ACA requires organizations with 50 or more employees to offer insurance to people working 30 hours per week. This has led to a growing number of contract employees who work up to, but not past, the hourly limit.
Many companies, which say they can’t afford the rising costs of traditional insurance, offer their employees only a modicum of help, perhaps around $200 per month toward buying a marketplace plan, or a bare-bones company plan.
Young people juggling part-time jobs and insurance options face bumpy, daunting transitions.
In Oklahoma, Daisy Creager, 29, has had three employers over the past three years. Insurance was important to her, not least because her former husband had Type 1 diabetes.
As she left the first of those jobs, her husband’s endocrinologist helped the couple stockpile less expensive insulin from Canada, since they would be uninsured.
After a few months, they bought a marketplace plan, but it was expensive and “didn’t cover a lot,” she said.
When she found a new job, she dropped that plan, only to discover that her new insurance coverage didn’t start until the end of her first month of employment. The couple would be uninsured for a few weeks.
A few days later, she came home to find her husband unconscious on the floor, in a diabetic coma. After hovering near death in an intensive care unit for four days, he woke up and began to recover.
“I think I’ve done everything right,” Creager said. “So why am I in a position where the health insurance available to me doesn’t cover what I need, or I can barely afford my premiums, or worse, at times I don’t even have it?”
Kathryn Russell, 27, developed excruciating back pain two months before her 26th birthday. After extensive testing, doctors determined she needed a complex surgery, which her surgeon couldn’t schedule until after she would be off her family’s insurance plan.
Forget the pain and the fear of the operation, she said, it was insurance that kept her up at night. “There’s this impending terror of, ‚ÄòWhat am I going to do?’” she recalled.
(One day before she turned 26, her father’s company agreed to keep her on his plan for six more months, if he paid higher premiums.)
The idea that the ACA would offer a variety of good options for people turning 26 has not worked as well as the legislation’s authors had hoped. The “job lock” tying insurance to employment has long plagued the United States workforce.
Young adults need guidance on their options beforehand, said Sanchez of Young Invincibles. None of those interviewed for this story, for example, knew there were navigators to help them find insurance on the online marketplaces.
Experts agree that the marketplaces need stronger regulation.
In 2023, for what plans in each tier of insurance should offer, such as better prescription drug benefits, defined copays for X-rays, or coverage for emergency room visits.
Certain types of basic care, such as primary care, should require just a small copay for at least a small number of initial visits. Each insurer must offer at least one plan that complies with these new standards for every level, known as an “” option or a “standard plan.”
Most plans on the marketplaces don’t meet these criteria. Federal and state regulators had long planned to cull such “noncompliant” plans, gradually ‚Äî fearing that doing so too quickly would scare insurers away from participating.
But with the priorities of the new Trump administration now in focus, and a Republican majority in Congress, it’s far from clear what course President Donald Trump, who sought to repeal the ACA outright in his first term, will take.
There are hints: Subsidies to help Americans buy insurance, adopted during the Biden administration, are set to expire at the end of 2025 unless the Republican-led Congress extends them.
If the subsidies expire, for plans sold on the marketplaces, leaving insurance out of reach for many more young adults.
This <a target="_blank" href="/health-care-costs/insurance-cliff-age-26-young-adults-chaos/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2066255&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>