
April 16
Katheryn Houghton reads the week’s news: Many Americans say it’s hard to pay for the dentist, but putting off care also has its costs. Plus, for some patients, Medicare will start covering GLP-1 drugs for weight loss this year.
April 9
Zach Dyer reads the week’s news: Rising health costs have some middle-aged adults skipping the doctor until Medicare will pick up the tab. Plus, there’s little evidence that immigrants without legal status are using Medicaid, despite White House claims.
April 2
Arielle Zionts reads the week’s news: Scientists say staff losses at the National Institutes of Health could lead to fewer medical breakthroughs. Plus, doctors worry they’ll see more kids with potentially deadly complications from measles, as cases surge.
March 26
Jackie Fortiér reads the week’s news: Consumers know which party they blame after Congress failed to extend enhanced Obamacare subsidies. Plus, updated standards say seniors should aim for even lower blood pressure readings.
March 19
Sam Whitehead reads the week’s news: Amid federal spending cuts and suspicion of fluoride, tooth problems are sending more kids to the ER. Plus, patients look to health savings accounts to deal with rising medical costs.
March 12
Katheryn Houghton reads the week’s news: Looming Medicaid cuts could mean states stop covering dental care for adults, and a growing number of U.S. nurses are moving to Canada.
March 5
Zach Dyer reads the week’s news: The Trump administration is calling for sharp restrictions on direct-to-consumer drug ads, and for some people facing skyrocketing health insurance costs, becoming eligible for Medicare because of a new diagnosis is a terrible irony.
Feb. 26
Sam Whitehead reads the week’s news: Some places are bringing back house calls to try to fight maternal and infant mortality, and almost all Americans benefit from health care subsidies in different forms.
Feb. 19
Arielle Zionts reads the week’s news: Some health systems are using AI tools to help patients get primary care, and the Trump administration’s new data-sharing rules make going to the hospital more dangerous for people without legal status.
Feb. 12
Jackie Fortiér reads the week’s news: Moves by the Trump administration have slowed cancer research, and more of America’s doctors are working into their golden years.
Feb. 5
Katheryn Houghton reads the week’s news: American farmers are being hit hard by the end of extra Obamacare subsidies, and hospitals are starting their own Medicare Advantage plans.
Jan. 29
Zach Dyer reads this week’s news: An expensive new gene therapy that can potentially cure people with sickle cell disease will be covered by Medicaid, but only when it works for patients. Plus, community health centers are preparing to help care for millions more uninsured people.
Jan. 22
Arielle Zionts reads the week’s news: Some states are cutting public funding for a type of autism therapy, and older adults are more likely than younger ones to stop taking GLP-1 drugs such as Ozempic.
Jan. 15
Jackie Fortiér reads the week’s news: Parents are confused by an overhaul of U.S. childhood immunization guidelines, and while people 65 and older make up the fastest-growing homeless population in the country, traditional homeless shelters often can’t accommodate them.
Jan. 8
Zach Dyer reads the week’s news: Instead of extending extra Affordable Care Act subsidies that would keep monthly premiums more affordable, some Republicans are pushing health savings accounts. Plus, people seeking cheaper health insurance options outside the ACA marketplaces may find some, but they come with downsides.
Jan. 1
Katheryn Houghton reads the week’s news: AI voices can help patients who have had their voice boxes removed sound like themselves again, and many state-run psychiatric hospitals don’t have enough beds to treat patients unless they’ve been charged with a crime.
The ║┌┴╧│╘╣╧═Ї News Minute is available every Thursday on CBS News Radio.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/news/listen-to-the-latest-kff-health-news-minute-2026/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2138213&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>After some federal financial aid expired, many Americans found that high-deductible health plans were the only option they could afford.
In a new episode of NPR’s Life Kit podcast, ║┌┴╧│╘╣╧═Ї News reporter Jackie Fortiér and podcast host Marielle Segarra discuss what these plans are, and why they can feel so confusing. Imagine paying $100 out-of-pocket for a routine doctor visit that used to cost you $20. Imagine shouldering thousands of dollars in bills before your insurance pays a cent.
Still, for some people тАФ especially those who rarely need medical care тАФ high-deductible plans work. Listen to the episode to explore how timing your care and taking advantage of free preventive services can help you make the most of your coverage.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/listen-health-care-helpline-life-kit-high-deductible-plans-out-of-pocket-costs/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2228954&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>An Arm and a Leg host Dan Weissmann traces Engelberg’s story back more than 50 years, from a scrappy childhood on the Atlantic City boardwalk to watching President Ronald Reagan sign his bill into law at the . Today, Engelberg advocates for policy changes he believes will enable more generic drugs to reach the market faster.
Credits
Note: “An Arm and a Leg” uses speech-recognition software to generate transcripts, which may contain errors. Please use the transcript as a tool but check the corresponding audio before quoting the podcast.
Dan: Hey thereтАУ
We are kicking off a new series here тАФ We’re calling it An Arm and a Leg 101.
We’ve spent years of reporting on two huge questions: Why does health care cost so freaking much? And what can we maybe do about it?
We’ve been chasing answers one story, one question at a time.
Now, we’re pulling together some of what we’ve learned. Digging a little deeper, going a little broader.
Starting with why so many drugs cost so much.
One of the first questions I ever asked тАФ one of our first stories тАФ was: How can insulin be so expensive? Wasn’t it discovered in the early 20th century? Shouldn’t it be a generic drug by now?
You know, cheap?
And part of the answer I got was: Insulin has been transformed since the early 20th century. A lot.
A medical researcher named Jing Luo told me: Today’s insulins are a long way from what we had a hundred years ago.
Jing Luo: They’ve been really modified at a molecular level. It’s cool stuff. It’s super cool stuff. And you know, there are multiple Nobel prizes in physiology and medicine that have made this happen.
Dan: And all that super-cool stuff, those amazing discoveries, got patented.
Meaning: The patent-holdersтАУ the pharma companies тАФ got a monopoly on those amazing discoveries.
The pharma companies claimed patents тАФ and monopoliesтАУ on a bunch of other things too. Not all of them amazing.
But each new patent can mean another delay for a generic version coming to market.
Jing Luo: Companies can stack dozens of patents on top of each other to try to thwart generic competition because they can say, look, we’ve got three patents on the active ingredient. We’ve got patents on the medical uses of the active ingredient. We’ve got patents on the non-active excipient associated with this ingredient. We’ve got multiple patents on the devices, and so you who are trying to enter this space will sue you for patent infringement on all of them.
Dan: A patent guarantees you at least a 20-year monopoly. Drugs can generally get an extra five.
And these extra patents тАФ secondary patents тАУcan keep you protected LONGER. If you don’t file them at the same time as the original:
To talk about a drug that’s in the news right now. The original patent on the active ingredient in Wegovy and Ozempic actually expired this year.. The extra five years extends it to the early 2030s.
But dozens of extra patents тАФ secondary patents, filed later тАФ mean that here in the U.S., we might not see cheaper generic versions until 2042. Or later.
And as Jing Luo told me: This strategy isn’t a secret. It’s an industry cornerstone.
Jing Luo: When you listen to these like CEOs of pharma companies being interviewed at CNBC, you know, they’d be like, well, what about generic competition for this product? And they’ll just keep saying, no, no, no. We’ve got this really robust patent portfolio. We can withstand any challenge. We’re gonna tie this up in courts forever and don’t worry about it.We’re gonna continue this gravy boat for a long, long time. That’s the way they reinsure investors.
Dan: A robust patent portfolio. ?Or what researchers and advocates call a patent thicket.
They say quality matters less than quantity.
The numbers are wild.
, the 10 best-selling drugs for 2021 тАФ drugs for cancer, HIV, arthritis тАФ were protected by a combined total of seven hundred and forty-two patents. With hundreds more “pending.”
When these add-on patents get challenged in court, they actually get tossed out more often than primary patents..
But lawsuits cost money. A robust patent portfolio тАФ a patent thicket тАФ means generic companies would need to be ready to file a LOT of them.
So, we wanted to know: How did all this happen? How did these games get started?
It turns out, there is one guy who can tell you the story from the beginning, for better and for worse. Who helped shape it. Made millions of dollars from it. Saw its flaws. And has spent most of the last 30 years trying to fix them. Hie’s a lawyer named Al Engelberg, and he’s 86 years old.
Alfred Engelberg: I tell people all the time, I live in a world, a pharma world where half the people think I’m dead and the other half wish I was.
Dan: Al Engelberg’s story is the story of generic drugs in America. And it’s a wild ride.
This is An Arm and a Leg тАФ a show about why health care costs so freaking much, and what we can maybe do about it. I’m Dan Weissmann. I’m a reporter, and I like a challenge. So the job we’ve chosen here is to take one of the most enraging, terrifying, depressing parts of American life, and bring you something entertaining, empowering, and useful.
?Al Engelberg’s parents fled Nazi Germany in the late 1930s.
He was born here, less than a year after they arrived. They had nothing.
And here’s where they made their new life.
Retro news reel: We are flying over a well-known eastern city. That is remarkable because manufacturing is almost non-existent. A city whose principle business is the entertainment of millions. Atlantic city, often called the vacation capital of the nation
Dan: Al likes to say he learned most of what he knows about practicing law on the Atlantic City boardwalk, by the time he was 16.
Alfred Engelberg: We grew up very, very fast there. I started working when I was about nine or 10 and, and there were lots of opportunities on the boardwalk.
Dan: His first “job” was crawling around under the boardwalk, looking for loose change.
Alfred Engelberg: But I went on to work at hotdog stands and at an illegal bingo game for the local mob.
Dan: And in every job, Atlantic City drove home its major lesson: Cheating тАФ hustling тАФ is something you’ve gotta expect.
At this illegal bingo parlor, Al’s job was walking between tables, doling out bingo cards for a dime apiece. The bosses hired college kids to walk behind kids like Al, to keep him honest.
Alfred Engelberg: I mean, these guys are running an illegal game, but they still need to count, and they still inherently don’t trust anybody.
Dan: Which was correct. Al says the college kids had their own hustle: They’d have him set aside a dollar or two before turning in his dimes тАФ split that dollar with him fifty-fifty тАФ and tell the bosses Al’s count was fine.
Alfred Engelberg: And everybody knowing that the counts were wildly inaccurate anyway тАШcause the little old ladies were, were stealing cards. Everybody in the room had their own thing going, you know, from the customers on.
Dan: After Al made it out of Atlantic City, his unique on-the-job education continued. He studied chemical engineering at Drexel, then took a job as a patent examiner while going to law school at night.
And at that job, he learned: The patent system was ripe for hustling.
Partly because most of his colleagues weren’t necessarily giving the job their all.
Like him, most patent examiners were working their way through law school. And they were sneaking time to study on the job.
Alfred Engelberg: We used to be able to cut our notes down so they fit in these file drawers with the patents. And we would be reading your notes and if your boss came by, you would just drop a patent on top of the notes.
Dan: You could say it was Atlantic City all over again. Everybody in the job is sneaking something for themselves тАФ in this case, time.
And Al Engelberg could see that, even if his colleagues gave it their all, they were too green to do their job well.
A patent examiner’s job тАФ deciding whether a proposed invention deserves a monopoly (which at that time was 17 years) тАФ means deciding whether the idea for that invention would be obvious to “a person of ordinary skill in that field.”
Alfred Engelberg: And most of the examiners had never worked in that field and had absolutely no idea. And this is the big leagues. You’re granting somebody a monopoly for 17 years, and it seemed ridiculous on its face.
Dan: Al cut his own path at the patent office. He’d worked his way through engineering school, in manufacturing plants, he saw what people of ordinary skill in that field solve problems every day. So he specialized in examining patents he actually knew something about.
That got him promoted, then it got him recruited by a corporate lawyer.. After the company paid his way through the rest of law school, he jumped to the Justice Department.
He was ambitiousтАУ he wanted experience junior lawyers don’t usually get тАФ like trying cases of his own.
After a few years doing just that, he took a job with a small law firm in New York City in 1968.
Alfred Engelberg: I came to New York to private practice at the age of 30 and I was ready to go. I mean, I was ready to, to tear the world apart and I did.
Dan: Patents were still a specialty. Then, in 1973, he gets a call that leads to his first generic drug case.
Generic drugs were not a hot market at the time.
Alfred Engelberg: ?The generic drug industry in 1970s was essentially, a half a dozen, privately owned family businesses, mostly in the metropolitan New York area. And most of the drugs that they were selling were drugs that were approved before 1962.
Dan: Yeah. 1962 is when the FDA made it harder to get a new drug approved тАФ you had to go through long clinical trials to show that your drug was safe and effective.
Even if your drug was a generic version of an existing drug. Those little companies didn’t have the capital to run those trials, so they were stuck selling those old drugs.
Not much of a business. Maybe 20 percent of prescriptions were for generic drugs.
So when Al Engelberg got a call for his first generic drug case, that was the context. And the case itself did not sound promising. For one thing:
Alfred Engelberg: The call wasn’t even from the client. It was from a bank. The client was bankrupt.
Dan: The client was bankrupt. This bankrupt client, Premo Pharmaceuticals, was getting sued for patent infringement. The bank was willing to put up ten thousand dollars for a defense. Nowhere near enough to actually try a case. Oh, andтАж
Alfred Engelberg: From what they told me, the information they gave me, we didn’t have a very good defense.
Dan: But Al Engelberg saw an opening. He could see that his opponents have weaknesses too.
Alfred Engelberg: The patent owners were in a very strange position. If they won, they got nothing because we were already bankrupt. Two, they were gonna have to spend the legal fees to win.
Dan: Win against a young lawyer named Al Engelberg who already had a rep as a tough opponent. So they could lose.
Alfred Engelberg: And if they lost, they would lose millions and millions of dollars in business because there wouldn’t be a patent. And they’d have competition from generic drugs.
Dan: And meanwhile, Al Engelberg is also sizing up the judge. He knows the guy doesn’t love patents.
So Al shows up to the first conference and he bluffs.
Alfred Engelberg: I said to the judge, oh, your Honor, you know, it’s another one of those patents. They’re all invalid. And I said, we don’t need very much discovery. We’re, we’ll be ready to go to trial in a few months. Just set a trial date.
Dan: The other side walks out beside themselves.
And within a couple of weeks they call Al to say: Hey, how about this? You guys just acknowledge our patent is OK, and we’ll give you the money we would’ve spent litigating. Call it 400,000 bucks?
Alfred Engelberg: I called the client and said, how’s $400,000? He said, are you kidding?
Dan: They didn’t just get out of trouble тАФ they got out of bankruptcy, with $400,000 in their pockets. Because Al Engelberg knew how to size up a situation.
Alfred Engelberg: You don’t learn that in law school. That’s not what they teach.
Dan: Word gets around about that case, and pretty soon everybody in the generic drug world is calling him.
It’s a small world, but by the end of the 1970s, there may be room for it to start getting bigger.
People are starting to notice: Drugs are expensive. Maybe there should be more cheap generics.
Some generic drug companies form an association and start lobbying: Make it easier to get generic drugs to market without having to go through all those trials.
The brand-name drugmakers push back: They say it takes so long to run the trials and get their drugs approved, they don’t get enough time to make money before those patents expire.
In 1983, Democratic Representative Henry Waxman steps in to broker a compromise, with Republican Senator Orrin Hatch.
And Mr. Engelberg goes to Washington. To run strategy for the generic drugmakers.
Alfred Engelberg: In a lot of ways , that’s where my Atlantic City training really helped me at the end of the day
Dan: There were a lot of people, with a lot of interests. A lot of angles. ?He starts commuting from New York to Washington DC a couple times a week тАФ for months and months, more than a year.
And Al Engelberg says: This time, it wasn’t just about winning a case.
Alfred Engelberg: I was in the back of a cab the way I remember, with the senior partner of the law firm. And he says to me, why are you breaking your ass going to Washington two or three times? Why don’t you send an associate? You know, it’s just like, it’s just another case. And I said. I said, are you kidding? I said, you know, how many lawyers ever get to do what I’m doing right now? To be at the table influencing what may be a major law that’s gonna have major consequences is, is like something I never thought my whole life I’d be doing.
Dan: A kid from Atlantic City was exactly the right person to try to balance all the angles, negotiate a compromise. It took more than a year. It almost didn’t happen. But then it did. Congress passed the bill, and President Ronald Reagan got in front of cameras to sign it.
Ronald Reagan: Let me turn my attention to the real reason we’re here this afternoon, signing into law the Drug Price Competition and Patent Term Restoration Act of 1984.
Dan: better known as Hatch-Waxman.
Hatch Waxman had three basic components:
One: Brand drugmakers got a few extra years on their patents.
Two: Generic drugmakers got a pathway to get FDA approval.
And three тАУThe new law laid out rules for a generic drugmaker when they wanted to CHALLENGE an existing patent.
Negotiating that third part was the part where Al Engelberg’s education on the Atlantic City boardwalk, and the U.S. patent office, and the generic drug industry came together: The result would make him millions and millions of dollars тАФ and blow a giant hole into the grand bargain he had worked so hard to bring about.
That’s coming right up.
This episode of An arm and a Leg is produced in partnership with ║┌┴╧│╘╣╧═Ї News. That’s a nonprofit newsroom covering health issues in America. The folks at ║┌┴╧│╘╣╧═Ї News are amazing journalists тАФ their work wins all kinds of awards, every year. We are honored to work with them.
So. The brand-name drug makers and the generic drug makers struck a deal. That deal was good for them. Both sides got something big out of it. The public was supposed to get something out of it too.
And, to be fair, we did: Remember, back then, maybe one out of five prescriptions was for a generic drug. Now it’s nine out of ten.
But we pay more than ever for drugs. Mostly for branded, patent-protected drugs. And the biggest, most-important, most profitable drugs get locked behind patent thickets.
How did that happen?
Well, to understand that, it helps to know what Al Engelberg got out of the whole bargain.
Al had been there at the bargaining table, on behalf of the generics.
One day, during those negotiations, he was in the office with Henry Waxman’s lead counsel, a guy named Bill Corr, when Corr got a call from someone on the other side.
Corr starts pointing at the phone, pointing to Al тАФ indicating: This guy is talking about you.
When Corr gets off the phone he says: That guy’s not sure about this deal where bad patents could be challenged. He’s suspicious about where you might take this. Like, are you just gonna set up a bounty-hunting operation, to get patents declared invalid?
And Corr said, Al, would you do that?
Alfred Engelberg: And I said, you know, Bill, until this moment, I’ve never given it any thought, but it’s a hell of a good idea. Maybe I’ll look at it.
Dan: And he did. Starting almost as soon as Hatch-Waxman became law.
Alfred Engelberg: And we sat in the rose garden, September 23rd, 1984, watched Reagan sign the bill. And in December of that year, I sat down at my kitchen table with a yellow pad and I laid out a strategy.
Dan: If you were gonna set up a bounty-hunting operation, how would you do it?
Al Engelberg knew a lot of patents were garbage. Knew it from his time in the patent office, knew it from practicing law. And he knew how much money a successful patent challenge could be worth.
The way Hatch-Waxman worked: If a generic drug company challenged a patent and won, they would get six months before any OTHER generic drugmakers could get a crack at the market.
So their only competition would be the brand. If a pill cost two cents to make, and the brand was selling for a dollar a pill тАФ that’s 98 cents of profit for every pill.
You’re the only competitor? You could charge 75 cents a pill and get 73 cents of profit. On a hit drug, you could make millions and millions тАФ just in those six months.
Al’s idea was this: Partner up with a generic drugmaker. Go find casesтАУ drugs with weak patents. Win ’em.
And split those millions in potential profits fifty-fifty.
Al pitched a generic drugmaker тАФ they were ready to go тАФ and brought the deal to his law firm. .
Alfred Engelberg: As it turned out, my partners weren’t interested in having me do this. They tried to talk me out of it.
Dan: But they couldn’t. So he left. Went out on his own. All on his own.
Alfred Engelberg: I never hired a single soul, not even a secretary. And I couldn’t type. I still can’t type.
Dan: But he hunted and pecked his way through brief after brief. He bought an early portable computer тАФ it weighed thirty pounds тАФ and lugged it around in the back of his car. For ten years.
Alfred Engelberg: It was stupid. I almost killed myself. But, it worked out okay.
Dan: Yeah. Turns out Al was really good at finding the problems with drug patents.
In one of his first cases, Al Engelberg personally made more than 70 million dollars. Others settled: A few million here, a few million thereтАУ it adds up.
And thenтАж
Alfred Engelberg: It got to be the mid nineties, and I was working on a case called Buspar.
Dan: The Buspar case ended up a big winner for Al Engelberg and his generic drug partners.
But it had consequences that went way beyond a single case. And led to big losses for the public.. Here’s how it went.
Alfred Engelberg: Buspar was an anti-anxiety drug. And by all accounts not a very good one.
Dan: But Bristol Meyers Squibb invested in big advertising and marketing campaigns.
Speaker 5: I feel anxious. I can’t concentrate.
Speaker 6: I’m so irritable. If you. You suffer from excessive worry. It can feel like a mountain of anxiety.
Speaker 5: I’ll never get it all done. I’m overwhelmed.
Speaker 6: But a prescription medication called buspar can help.
Dan: And all that marketing did its job. By the mid-1990s, Buspar was making more than 200 million dollars a year for Bristol.
Alfred Engelberg: The only problem for them was that the drug was not new.
Dan: The active ingredient was well-known in medical literature as a tranquilizer. Nobody had bothered to market it.
So Bristol Myers Squibb filed a patent on it, claiming it had discovered a new use for this well-known tranquilizer: Treating anxiety.
Al Engelberg says when he read the patent application, he could barely believe it: What do tranquilizers do if notтАж treat anxiety?
It’s like saying: There’s this stuff called sugar. We’re gonna take out a patent on using it as a sweetener.
This looked like a case for a guy from Atlantic City.
Alfred Engelberg: I did something that lawyers don’t. That’s just the way I was built.
I filed a motion with the court and basically said, we don’t need any evidence.
You just have to read the patent. If you believe it’s true, the patent’s invalid. Just, you know, all you need is a dictionary basically.
Dan: Al says Bristol was eager to settle.
Alfred Engelberg: We get into a settlement discussion and we keep saying, no, no, no, no.
Dan: Al’s partners had done the math: They figured they stood to make a hundred million dollars or more once they won. So when the other side offered 25 million, no was the easy answer.
Alfred Engelberg: We said, why are we gonna take this? You know, it’s crazy. There’s a reward here we know what it is. We’re gonna get it eventually.
Dan: Al sits down with a lawyer from the other side, a guy he knows, explains how he sees the math.
And soon the other side comes through with a much bigger offer: 72 million dollars тАУ almost three times as much.
Alfred Engelberg: And I’m sitting there like, what are you crazy? But then think about it from their point of view.
Dan: Paying 72 million dollars is nothing, compared to what Bristol stands to gain if this lawsuit goes away.
With their monopoly, Bristol Meyer Squibb is making more than 200 million dollars a year on Buspar. And unless somebody else lines up to do what Al Engelberg had done, expect to keep that monopoly for years.
Charging whatever they want. Two dollars a pill, three dollars a pill. Which Al Engelberg says is exactly what happened.
In fact, they kept that monopoly for like five years.
Alfred Engelberg: As it turned out, nobody came behind us. And so, they had that monopoly until 2000. So they got five years of 2 billion, in gross profits.
Dan: They made out.
Alfred Engelberg: For the cost of $75 million. And you know, the public got screwed ’cause they are continuing to pay, you know, $2 a pill or $3 a pill for a drug that eventually ends up being available for 20 or 30 cents. Um, so that’s, that’s how it works.
Dan: That’s how it works. The branded company and the generic company both make out great. Cheaper generic versions of a drug get delayed.
That amazing payday for Al Engelberg and his partners at the generic drug company turned into a model a template for the kind of deal that every generic drug company would want in on.
It got a nickname: Pay for delay.
Alfred Engelberg: That spread through the industry like wildfire, those numbers, you know, you don’t make those numbers half a cent at a time on, on pills,
Dan: Lawsuits were way more profitable.
But Al Engelberg wasn’t filing them.
A year or so after the Buspar case settled, sparking the Pay for Delay gold rush, he retired. He had plenty of money and nothing to prove.
And in retirement, he started evaluating what he’d accomplished, for better and for worse.
For better, generic drugs had more than doubled their share of the market since Hatch-Waxman took effect.
For worse, he could see two places where тАФ despite all of his Atlantic City training тАФ he had missed a couple of angles in negotiating Hatch-Waxman.
One was: this whole pay-for-delay scheme. Turned out, in balancing incentives for brands and generic makers, he’d left open this perverse incentive that left the public out.
And the second was a loophole that Hatch-Waxman had left open.:
It created a process where players like Al and his generic partners could challenge patents on drugs like Buspar, that they thought didn’t deserve protected monopolies. It removed some friction for those attacks.
The drug companies developed a way to add more friction: stacking extra patents тАФ secondary patents тАФ on every drug.
Developing patent thickets.
Even if a secondary patent is trivial тАФ and lots of them do get tossed out тАФ challenging it means a court fight. And that costs money.
Alfred Engelberg: It caused the big drug companies to just get more and more patents. Because why not? You know, there was nothing standing in the way.
Dan: I mean, nobody knows better than Al Engelberg: Patent examiners don’t exactly stand in the way.
And those patent thickets and pay for delay, they feed on each other.
Alfred Engelberg: The economics of the business, caused these kinds of settlements to reach epic proportions. So the generic companies would, challenge these secondary patents and, the drug companies would pay them off.
Dan: In 1999 he published an article in a scholarly journal arguing that Hatch-Waxman needed a reboot. Even the six-month head start for a successful challenge could probably go.
And ever since тАФ for more than twenty-five years тАФ he’s poured millions of dollars into efforts to tighten the rules. Funding research. A public-information campaign from Consumer Reports. Even a center for IP law at his alma mater, NYU.
It hasn’t always gone his way.
Pay for delay has gotten much bigger since Al Engelberg wrote his first article calling for reform: He wrote in 1999 that about two dozen patent challenges had been filed.
Now he estimates that number at twelve thousand.
Alfred Engelberg: I can’t tell you how many tens of billions of dollars in legal fees that is. It’s one of the fastest growing and and steadiest industries for big law.
Dan: A Hatch-Waxman litigation forum on LinkedIn has more than fourteen thousand members.
And Hatch-Waxman doesn’t cover many of today’s the top-selling drugsтАУ the biggest moneymakers. They belong to a class called “biologics.”
That includes famously-expensive rheumatoid arthritis drugs like Humira and Enbrel тАФ and insulin.
Biologics weren’t a category forty years ago when Hatch-Waxman got negotiated. Congress passed a new law to deal with them in 2010 тАФ ?the Biologics Price Competition and Innovation Act.
Al Engelberg is not a fan of that law.
Alfred Engelberg: Whatever mistakes were made in Hatch Waxman, they were multiplied by 10 and deliberately in the biologics law
Dan: He says the all but encourages patent thickets. And doesn’t provide a pathway to challenge them.
He says it reminds him of some of his early days practicing law.
Alfred Engelberg: Back in the seventies, we used to have small startup clients in the computer field, and they would get letters from IBM. It says, we are ready to inform you that you may be infringing one or more of the following patents. And there was a 10 page list of patents attached. And the startup would come to us and say, you know, what should we do? And we would say, find another line of work, you know, what are you gonna do?
Dan: But he has not given up. In 2025, he published a book: Breaking the Medicine Monopolies.
It tells the story of his career тАФ and lays out his prescriptions for fixing the problem.
He doesn’t JUST focus on plugging the holes in Hatch-Waxman and the biologics law.
Alfred Engelberg: You know, we don’t actually need a generic drug industry. We need generic drug pricing.
Dan: He’s got proposals for an increased government role in negotiating and regulating prices тАФ and more than that.
He argues that a 1980 law allows the government to commisssion generic versions of drugs that were developed using public research dollars.
He also says the FDA rules that protect secondary patents on drugs тАФ that allow patent thicketing тАФ are based on a completely wrong interpretation of Hatch-Waxman.
And tells us he’s working up a challenge, with help from AI tools like Claude.
He’s 86 years old. And he doesn’t seem inclined to stop.
Alfred Engelberg: It so changed my life and I did so well by it, I thought, how can I not take on this problem? Who’s gonna do it if I don’t do it?
Dan: He’s got the time. Money’s no object. And he knows the territory as well as anybody. He helped create it.
Alfred Engelberg: So it’s, it’s my obligation really. It’s that sort of Jewish guilt. What can I tell you? I’m paying back for the bingo game.
Dan: So we’ve gone back more than fifty years on the question: Why aren’t there more generic drugs? We’ve learned why we’ve got the ones we have, and what stands in the way of getting more.
And that is just in time. Because this spring the U.S. Supreme Court will hear arguments in a case that could restrict the generic drug pipeline even further. It could have major implications.
And understanding what they are requires all of the 101 we’ve covered here. We’ll have that story for you in a few weeks. Til then, take care of yourself.
This episode of An Arm and a Leg was produced by Emily Pisacreta, with help from Dan WeissmannтАФ and edited by Ellen Weiss.
Adam Raymonda is our audio wizard.
Our music is by Dave Weiner and Blue Dot Sessions.
Claire Davenport is our engagement producer.
Sarah Ballema is our Operations Manager. Bea Bosco is our consulting director of operations.
This series тАФ An Arm and a Leg 101 тАФ is made possible in part by support from Arnold Ventures.
An Arm and a Leg is produced in partnership with ║┌┴╧│╘╣╧═Ї News. That’s a national newsroom producing in-depth journalism about health issues in America and a core program at KFF, an independent source of health policy research, polling, and journalism.
Zach Dyer is senior audio producer at ║┌┴╧│╘╣╧═Ї News. He’s editorial liaison to this show.
An Arm and a Leg is distributed by KUOW, Seattle’s NPR news station.
And thanks to the Institute for Nonprofit News for serving as our fiscal sponsor.
They allow us to accept tax-exempt donations. You can learn more about INN at INN.org.
Finally, thank you to everybody who supports this show financially.
You can join in any time at arm and a leg show, dot com, slash: support.
“An Arm and a Leg” is a co-production of ║┌┴╧│╘╣╧═Ї News and Public Road Productions.
For more from the team at “An Arm and a Leg,” subscribe to its weekly newsletter, . You can also follow the show on , , , and . And if you’ve got stories to tell about the health care system, the producers would love to .
To hear all ║┌┴╧│╘╣╧═Ї News podcasts, click here.
And subscribe to “An Arm and a Leg” on , , , or wherever you listen to podcasts.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/podcast/an-arm-and-a-leg-alfred-engelberg-accidental-architect-drug-patent-thicket/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2228494&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>But physicians, dentists, ambulance companies, and other health care providers are still taking their patients to court, a Connecticut Mirror-║┌┴╧│╘╣╧═Ї News investigation of state legal records shows.
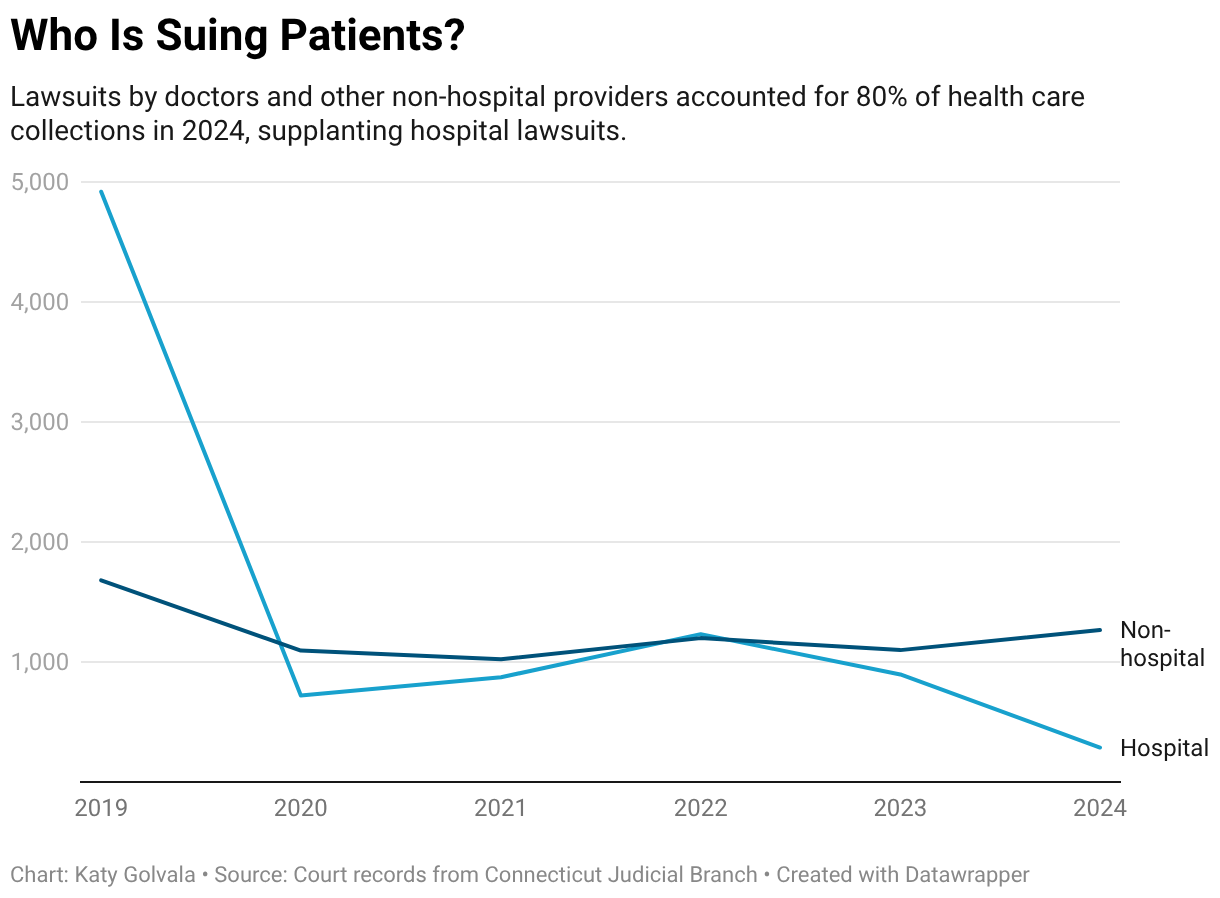
Lawsuits by doctors and other nonhospital providers now dominate health care collections in Connecticut, the records show, accounting for more than 80% of cases filed against patients and their families in 2024.
That’s a major reversal from just five years earlier, when hospital system lawsuits made up three-quarters of health-related collection cases in the state’s courts.
The shift is moving medical debt collections into a less regulated realm. Most hospitals, because they are tax-exempt nonprofits, must make financial aid available to low-income patients and follow federal regulations that limit aggressive collection activities. Other medical providers, such as private medical groups, are generally exempt from these rules.
The lawsuits are typically over bills of less than $3,000, but the impact on patients can be devastating. Lawsuits are among the most ruinous byproducts of a health care debt problem that burdens an estimated 100 million people in the U.S.
Lawsuits can lead to garnished wages, liens on homes, and hundreds of dollars of added debt from interest and court fees. They also pile additional financial strains on struggling families, prevent patients from getting needed care, and sap trust in medical providers.
“It’s really messed up,” said Allie Cass-Wilson, a nurse in Bristol, Connecticut, who was sued over a $1,972 debt by an OB-GYN practice where she’d been a patient years earlier. “How can they do that to people?” She did not contest the lawsuit, court records show.
Cass-Wilson, who is 36 and lives in a small apartment just off an expressway on-ramp, said she learned of the outstanding debt only when she was sued. When she tried making an appointment, she said, she was told her doctor wouldn’t see her. “They said I was blacklisted,” Cass-Wilson said. “I was so confused. I couldn’t believe that my medical provider let my care be interrupted like this.”
Cass-Wilson ultimately sought medical care elsewhere.
Radiologists, Dentists, Ambulances
Overall, CT Mirror and ║┌┴╧│╘╣╧═Ї News identified more than 16,000 health care-related debt cases in Connecticut courts from 2019 to 2024. The database was assembled from online court records with the help of January Advisors, a data science consulting firm that helped extract and sort the data.
Over the six-year period, most of Connecticut’s more than 25,000 did not pursue patients in court for outstanding balances.
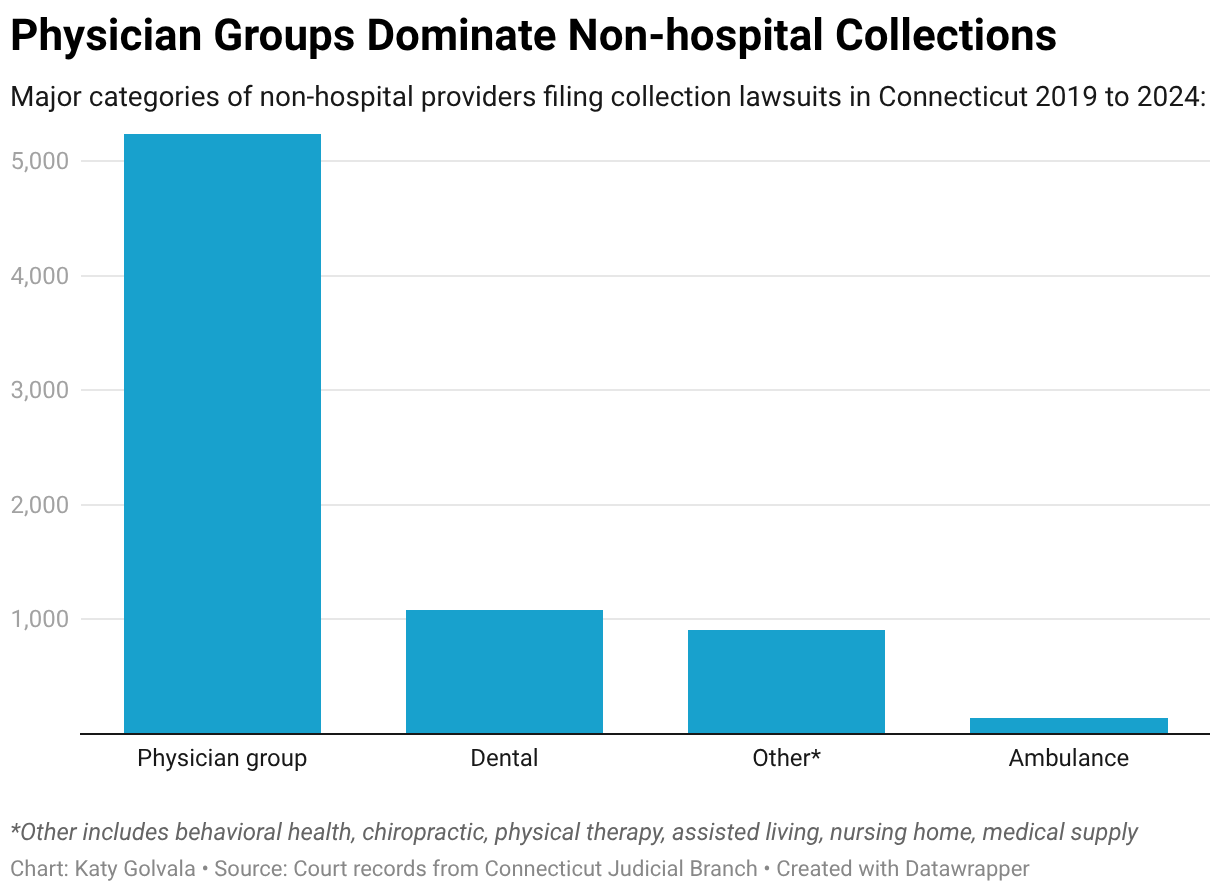
But records show that more than 400 medical providers, including several hospital systems, sued their patients. Among those filing lawsuits were radiologists, anesthesiologists, eye doctors, podiatrists, allergists, and pediatricians.
Dentists, periodontists, and other dental providers filed more than 1,000 lawsuits against patients. And ambulance companies sued more than 140 people.
Med-Aid, a company based outside New Haven, Connecticut, that provides orthopedic braces and other medical supplies to patients, sued more than 400 people, the court records show. The company’s president, Frank Dilieto, did not respond to repeated interview requests.
Cass-Wilson was sued by Briar Rose Network in Bristol, Connecticut, a member of a large network of OB-GYN practices across Connecticut called Physicians for Women’s Health. The network’s members sued close to 100 patients in 2024, records show.
Paula Greenberg, CEO of Women’s Health Connecticut, a private equity-backed company affiliated with Physicians for Women’s Health that manages business operations for the network, said the lawsuits represent a small fraction of the more than 300,000 patients the network sees every year.
“This is an organization committed to patients,” Greenberg said. She noted that the group offers options to help patients pay, including installment plans and financial aid.
Geoffrey Manton, president of Naugatuck Valley Radiological Associates, said his practice also will work with people who say they can’t pay. But, he said, patients sometimes stop responding to their bills.
“Hiding from your problems isn’t going to solve them,” Manton said. “If we didn’t take any action, there could be that person that is in that late-model Mercedes that just chooses not to pay any bills.” The group sued more than 125 patients from 2019 to 2024, according to the court records.
Many medical providers say that aggressive collections stem from the growing prevalence of high-deductible health plans that leave patients with thousands of dollars of bills before their coverage kicks in.
Greenberg and Manton said each of their physician groups must collect. “This is a business,” Greenberg said. “We have to look at our operating costs.”
Critics of medical collection lawsuits note that the patients are typically sued over relatively small debts that are likely to have little impact on multimillion-dollar medical practices.
The average patient debt that members of Physicians for Women’s Health sued over in 2024 was less than $1,100, court records show. The physician group’s annual revenues are typically in the tens of millions of dollars, according to Greenberg.
Even relatively small debts — which often include interest — can place substantial burdens on families struggling to keep up with their bills, especially while dealing with a serious illness, patient advocates say.
“We don’t have a realistic choice in using health care,” said Lisa Freeman, who heads the Connecticut Center for Patient Safety and has advocated for patients struggling with medical bills. “To then get sued for it, when people have less and less funds available for anything extra, that’s very disheartening.”
A Stroke, Then a Lawsuit

Matthew Millman, 54, lost his job as an IT support worker after having a stroke. Then Meriden Imaging Center sued him over an $1,891 bill.
Millman and his wife said they tried to explain their financial situation to the center, which is affiliated with Midstate Radiology Associates, a large physician group that operates imaging centers and doctors’ offices across Connecticut.
“It was very frustrating,” said Millman, who lives in an aging apartment owned by his wife’s family in New Britain. Millman, his wife, and their teenage daughter are barely getting by on his two part-time jobs — one bagging groceries, the other helping homebound seniors. Together, the jobs pay about $1,500 a month, he said.
The imaging center, after winning the collection case against Millman, tried to garnish his wages, though that was unsuccessful because Millman had lost his IT job.
“It’s all about money,” Millman said, shaking his head. “If you are trained in helping somebody with their health, it shouldn’t be about the money first. It should be about their health.”
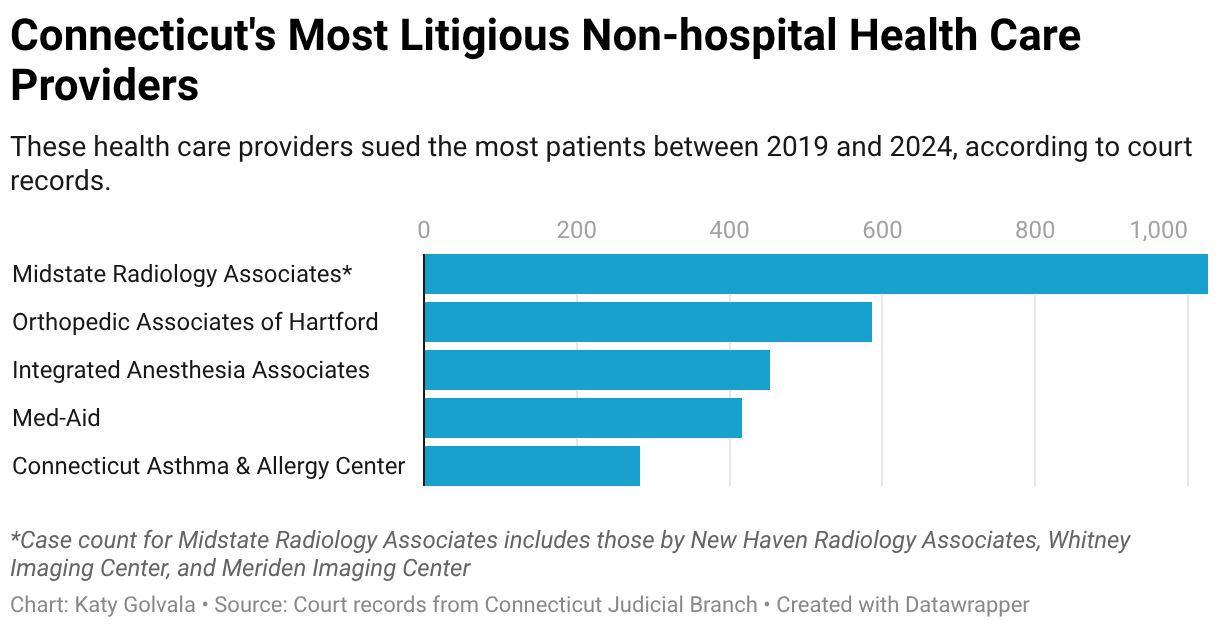
Court records show that Midstate Radiology, Meriden Imaging Center and affiliates filed more than 1,000 collection lawsuits against patients from 2019 to 2024, making them the most litigious nonhospital providers in the state. As is common in medical debt lawsuits, the plaintiffs prevailed in most cases, records show.
Midstate president Gary Dee, a radiologist, didn’t respond to emails and messages left at his West Hartford office.
Across town from Millman’s apartment in New Britain, Joseph Lentz lives in a cramped apartment with his wife and daughter. He used to oversee operations at a Boy Scout camp but is now unemployed. Lentz lost his job during the pandemic. The family home went into foreclosure, he said.
In 2023, Orthopedic Associates of Hartford sued Lentz over a $3,644 bill the practice said he owed after having shoulder surgery in 2018.
“I’d pay it if I could, I guess,” said Lentz, 59. “But I don’t even know where next month’s rent is coming from. I’m trying to climb out as best I can. I guess this is just one more thing to shovel in.”
The orthopedic group filed more than 580 lawsuits against patients from 2019 to 2024, prevailing in most, records show.
The medical group declined interview requests. But chief executive David Mudano said in a statement: “As an independent physician practice, we strive to balance compassion for patients with the financial responsibility required to sustain our practice.”
Old Debts and Disputed Claims
Lentz, who did not contest the lawsuit, said he has no reason to doubt he owes the debt. But in many cases reviewed by CT Mirror and ║┌┴╧│╘╣╧═Ї News and in interviews, patients being sued questioned the accuracy of their medical bills, citing care they thought health insurance should have covered or, in some cases, bills for services they never received.
This reflects with aggressive collection tactics like lawsuits when disputes over the accuracy of medical bills and delayed or denied insurance claims are so widespread in American health care.
A by the federal Consumer Financial Protection Bureau found that nearly half of the medical debt complaints fielded by the agency involved bills that consumers said were erroneous in some way or that consumers said they’d already paid.
“We know people are billed incorrectly,” said Lester Bird, who studies debt collection lawsuits at the nonprofit Pew Charitable Trusts. Bird noted that courts are ill equipped to sort through disputed medical charges or insurance claims, especially when there is little documentation in most debt collection lawsuits.
“It’s complicated before it gets to the courts,” Bird said, “and it’s very complicated when it gets into the courts.”
This can create headaches for physicians and other providers. But billing problems ultimately affect patients and their families most, said Connecticut state Sen. Saud Anwar, a Democrat who is also a physician. “Patients are left to deal with it.”
Andrew Skolnick, an attorney in Milford, outside New Haven, was sued in 2023 by an imaging center where his wife had received services in 2020.
Skolnick said that when the couple, who were covered through his job-based insurance, originally received the bill from Diagnostic Imaging of Milford, he tried to tell the imaging center it had submitted the claim to the wrong insurance plan, but he said they wouldn’t speak with him.
The center later filed the lawsuit, alleging he owed more than $2,000, plus almost $300 in interest.
Despite interview requests, officials at Diagnostic Imaging of Milford did not comment for this article.
Unlike most patients who are sued, Skolnick had the resources and expertise to contest the suit. He said he offered to pay what would have been his responsibility under the plan if the imaging center had filed his claim correctly. He ultimately settled for $1,700, court records show.
“It wasn’t a tremendous amount, but I knew that they had made a mistake,” Skolnick said. “The system is not working.”
More Protections?
Anwar, the state lawmaker and physician, expressed concern that lawsuits undermine patients’ faith in their doctors.
“It’s a sacred relationship,” he said. “If your physician, who is taking care of you, is suing you for money, that’s a problem.
Many hospitals, facing bad publicity from suing patients, have stopped taking patients to court over unpaid bills. Hospital collection lawsuits identified by CT Mirror and ║┌┴╧│╘╣╧═Ї News in Connecticut court records plunged from more than 4,900 in 2019 to fewer than 300 in 2024.
Also, in recent years, several states, including Connecticut, have expanded protections for patients with bills they can’t pay.
Connecticut now from consumer credit reports, and legislators are pushing to get hospitals to provide more financial aid to patients. Other states have restricted the use of wage garnishment and property liens to collect medical debt.
But state efforts to rein in aggressive medical debt collections have mostly focused on hospitals. That may need to change, said Connecticut state Sen. Matt Lesser, a Democrat who co-chairs the legislature’s Human Services Committee.
He is a key backer of a bill that would bar hospitals from billing patients who receive public benefits like food assistance or who make less than twice the federal poverty level, about $32,000 for an individual.
The restriction would not apply to bills from physicians and other nonhospital providers, however. “We may have to go bigger if that’s where the heart of the matter is,” Lesser said.
Connecticut Gov. Ned Lamont, a Democrat who spearheaded an initiative to for more than 150,000 state residents, also expressed concern about physicians suing the people in their care.
“Everyone should do the right thing by patients,” he said.
This article was produced in partnership with , a statewide nonprofit newsroom that covers public policy and politics.
How We Did It: Analyzing Connecticut Health Care Debt Collection Lawsuits
How often do health care providers sue patients over unpaid bills?
In most states, that’s nearly impossible to answer because courts don’t typically identify which debt collection lawsuits involve a medical debt versus other kinds of debt, such as rent, credit cards, or cellphone bills.
But Connecticut is different. Debt collection cases filed in small-claims court for unpaid medical or dental bills must be classified as health care debt. We worked with the data science consulting firm January Advisors to pull these cases from the Connecticut court database and analyze them. (January Advisors has worked with nonprofits and researchers across the country to collect debt collection data from state courts. The firm did not have any editorial input in our project.)
We started with health care collection cases filed in small-claims court from 2019 to 2024. But this covered only cases involving debts smaller than $5,000. We also wanted to know about cases in which providers sued for bills exceeding $5,000. Connecticut courts don’t assign a “medical” category for large-claim cases. So we pulled all large-claim records for any plaintiff — hospital or nonhospital provider — that appeared in medical small-claims cases. We also included cases with plaintiffs that didn’t appear in that dataset but had common medical terminology in their names, like “hospital” or “DDS.”
We then went through each case manually to confirm that the plaintiff was a medical or dental provider. We determined whether the provider was part of a larger hospital or physician group. And we categorized each plaintiff by a provider type (e.g., hospital system, dental, physician group).
In some cases, the data we pulled was incomplete, so we looked up the court records online and manually entered the information into our database. The Connecticut Judicial Department purges case records from its online portal after a certain amount of time. In those cases, we asked the agency to provide summonses and claims so we could manually enter the case information into our database.
We removed cases with out-of-state defendants or out-of-state plaintiffs and any cases in which missing records made it difficult to confirm information about the provider.
This <a target="_blank" href="/news/medical-debt-connecticut-doctors-sue-patients/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2228622&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
President Donald Trump this week nominated a former deputy surgeon general who has expressed support for vaccines to lead the Centers for Disease Control and Prevention. Considered a more traditional fit for the job, Erica Schwartz would be the agency’s fourth leader in roughly a year, should she be confirmed by the Senate.
And Health and Human Services Secretary Robert F. Kennedy Jr. appeared on Capitol Hill this week in the first of several hearings discussing Trump’s budget request for the department. But the topics up for discussion deviated quite a bit from the subject of federal funding, with lawmakers raising issues of Medicaid fraud, measles outbreaks, the hepatitis B vaccine, peptides, unaccompanied minors, and much, much more.
This week’s panelists are Mary Agnes Carey of ║┌┴╧│╘╣╧═Ї News, Anna Edney of Bloomberg News, Emmarie Huetteman of ║┌┴╧│╘╣╧═Ї News, and Joanne Kenen of the Johns Hopkins University Bloomberg School of Public Health and Politico Magazine.
Panelists



Among the takeaways from this week’s episode:
- Trump on Thursday named four officials to the CDC’s leadership team. Schwartz, whom he picked as director, is a physician and Navy officer who served as a deputy surgeon general during Trump’s first term. She has voiced support for vaccines and played a key role in the covid-19 pandemic response.
- RFK Jr. testified before three committees of the House of Representatives this week on the president’s budget request for HHS. While the hearings touched on a wide variety of topics, notable moments included a slight softening of Kennedy’s stance on the measles vaccine, including the acknowledgment that being immunized is safer than having measles тАФ although he also stood by the decision to remove the recommendation for the newborn dose of the hepatitis B vaccine.
- New studies on the use of acetaminophen during pregnancy and the effects of water fluoridation on cognitive function refute Trump administration claims. And a White House meeting that brought together Trump, Kennedy, and other leaders of the Make America Healthy Again movement aimed to soothe concerns among supporters тАФ yet there’s reason to believe the overture won’t completely mend fences between the Trump administration and the MAHA constituency ahead of the midterm elections.
Also this week, ║┌┴╧│╘╣╧═Ї News’ Julie Rovner interviews Michelle Canero, an immigration attorney, about how the Trump administration’s policies affect the medical workforce.
Plus, for “extra credit,” the panelists suggest health policy stories they read (or wrote) this week that they think you should read, too:
тАпMary Agnes Carey: Politico’s “,” by Alice Miranda Ollstein.
Joanne Kenen: The New York Times’ “,” by Teddy Rosenbluth.
Anna Edney: Bloomberg’s “,” by Anna Edney.
Emmarie Huetteman: ║┌┴╧│╘╣╧═Ї News’ “Your New Therapist: Chatty, Leaky, and Hardly Human,” by Darius Tahir.
Also mentioned in this week’s podcast:
- JAMA Pediatrics’ “,” by Kira Philipsen Prahm, Pingnan Chen, Line Rode, et al.
- Proceedings of the National Academy of Sciences’ “,” by John Robert Warren, Gina Rumore, Kamil Sicinski, and Michal Engelman.
- ║┌┴╧│╘╣╧═Ї News’ “Pennsylvania Town Faces Fallout From Trump’s Environmental Rule Rollback,” by Stephanie Armour and Maia Rosenfeld.
- The New York Times’ “,” by Sheryl Gay Stolberg.
- Wakely Consulting Group’s “,” by Michelle Anderson, Chia Yi Chin, and Michael Cohen.
[Editor’s note: This transcript was generated using both transcription software and a human’s light touch. It has been edited for style and clarity.]
Mary Agnes Carey: Hello from ║┌┴╧│╘╣╧═Ї News and WAMU radio in Washington, D.C. Welcome to What the Health? I’m Mary Agnes Carey, managing editor of ║┌┴╧│╘╣╧═Ї News, filling in for Julie Rovner this week. And as always, I’m joined by some of the best and smartest health reporters covering Washington. We’re taping this week on Friday, April 17, at 10 a.m. As always, news happens fast and things might have changed by the time you hear this. So here we go.
Today we’re joined via videoconference by Anna Edney of Bloomberg News.
Anna Edney: Hi, everybody.
Carey: Joanne Kenen of the Johns Hopkins Bloomberg School of Public Health and Politico Magazine.
Joanne Kenen: Hi, everybody.
Carey: And my ║┌┴╧│╘╣╧═Ї News colleague Emmarie Huetteman.
Emmarie Huetteman: Hey there.
Carey: Later in this episode, we’ll play Julie’s interview with immigration attorney Michelle Canero about the impact the Trump administration’s immigration policies are having on the medical workforce. But first, this week’s news тАФ and there is plenty of it.
On Thursday, President [Donald] Trump nominated Dr. Erica Schwartz to lead the Centers for Disease Control and Prevention. Schwartz, a vaccine supporter, served as a deputy surgeon general in President Trump’s first term, and during the coronavirus pandemic she ran the federal government’s drive-through testing program. She’s also a Navy officer and a retired rear admiral in the Commissioned Corps of the U.S. Public Health Service. Her appointment requires Senate confirmation. President Trump also announced other changes to the agency’s top leadership: Sean Slovenski, a health care industry executive, as the agency’s deputy director and chief operating officer; Dr. Jennifer Shuford, health commissioner for Texas, as deputy director and chief medical officer, and Dr. Sara Brenner, who briefly served as acting commissioner of the FDA [Food and Drug Administration], as a senior counselor to Department of Health and Human Services Secretary Robert F Kennedy Jr. So we’ve discussed previously on the podcast several times that the CDC has lacked a permanent director for most of the president’s second term. Will Dr. Schwartz, if confirmed, and the other members of this new leadership team make the difference?
Huetteman: I think that we’ve seen a CDC that’s been in a protracted period of turmoil, and this is going to be an opportunity for maybe a shift in that. Dr. Schwartz would actually be the agency’s fourth leader in a little more than a year, and we’ve talked on the podcast about how naming someone who could fit the bill to lead the CDC was a difficult task facing the Trump administration. They needed someone who could support the MAHA [Make America Healthy Again] agenda while not embracing some of the more anti-vaccine views, and that person needed to be able to win Senate confirmation, which isn’t a given, even with this Republican-controlled Senate.
Edney: And I think we’ve seen that there have been some people already in the MAHA coalition that have come out and been upset about this pick. So I think what that shows is a calculated decision by the administration to, kind of, as they’ve been doing for this year, is kind of not focus on the vaccine part of Secretary Kennedy’s agenda and to, as Emmarie said, try to get someone that can get through Senate confirmation. We’ve already seen the surgeon general nominee be held up in the Senate because she was not as strong on vaccines as I think some would have liked to see when she had her confirmation hearing.
Kenen: So this happened late yesterday, and I’ve been traveling this week, but I did have a chance to talk to some public health people about her, and there was sort of this audible sigh of relief. The Senate is a very unpredictable place, and we live in very unpredictable times. At this point, my initial gut reaction is she’s got a pretty good chance of confirmation. The other thing, I think some of the other appointees, there’s a little bit more concern about, but what really matters is who is the face of the CDC, and she would be the face of the CDC. She would be in charge, and people like her. Also, this is an administration that has not had a lot of minorities, and she will be, she’s a Black woman. respected in her field. And that also is going to тАФ she needs to be able to speak to all Americans about their health, and I think that people welcome that as well, both her credentials and her life experience. So, yeah, I think that MAHA is sort of in this funny moment now, because clearly Kennedy isn’t doing everything that people wanted or expected. And so we’ll sort of see how the тАФ I think if he had his ideal CDC director, this, we can probably surmise that this would not, she would not be the first on his list. But there’s a certain amount of adaptation going on at the moment. So I think many, many people will be relieved to see somebody get through, confirmed pretty quickly. People can get held up for things that have absolutely nothing to do with the CDC or public health. The Senate has all sorts of peculiarities. But I think there’s probably going to be a desire to get this done pretty quickly.
Carey: All right. Well, we’ll see what happens, and we will go back to the MAHA folks a little bit later in the podcast. But right now I want to shift to Capitol Hill. Thursday was a very big day on the Hill for HHS Secretary Kennedy. He kicked off a series of appearances before Congress. This week he’s testifying before three House committees before he heads over to the Senate next week. This is the first time that the secretary has visited some of these House panels, and while the purpose of the latest congressional visit is to talk about President Trump’s HHS budget request, this also was the first time that a lot of lawmakers ever had an opportunity to talk to Kennedy, and what they asked him sometimes deviated, maybe quite a bit, from that subject of federal funding. The topics included Medicaid fraud, measles outbreaks, the birth-dose recommendation for the hepatitis B vaccine, peptides, unaccompanied minors, and more тАФ actually, much more when you look at the hearings from yesterday, and I’m sure that will also happen with today’s session. What stood out to you about Kennedy’s testimony this week?
Edney: I think it was the mix of questions, and you sort of alluded to this, but they wanted, the members of Congress wanted to talk about so many things. And I feel like in the earlier hearing, which was in the House Ways and Means Committee, that it was, there was a lot of focus in the beginning on fraud, and that sort of surprised me, and then we saw maybe one or two questions on vaccines. And so I thought the mix of questions, the things that members were interested in, were really interesting. And it did тАФ there were some fiery moments, but for his first time on the Hill in a while, for such a controversial Cabinet member, I thought they were pretty tame.
Kenen: Yeah, I watched a fair amount of the morning. I did not see the afternoon, but I read about the afternoon, and I totally agree with Anna’s take. This administration and Kennedy did what this administration has been doing. They blame all problems on [former president Joe] Biden and the prior administration. And to be fair, Democrats, when they’re in power, they, I don’t think they do it quite to this extreme, but Democrats spend, when they have the chance, they blame things on Republicans. So that’s sort of Washington as usual. The emphasis on fraud has been a hallmark of this administration, particularly in health and social services. And you’ve seen, of course, in the way they’ve gone after blue states in particular. And a lot of their justification for the changes in Medicaid that are coming in the coming year are supposedly because of massive fraud and they’re cracking down. It was not dominated by vaccines, and I was watching Kennedy’s face really carefully. When he was asked about the first child to die of measles in Texas last year, and a Democrat asked him could the vaccine have saved her life, and you could sort of see him just, you just sort of watch his facial expressions, and he knew he had to say this, and he came out with the word “possibly,” and, which is a change. And then in the afternoon тАФ where I did not, as I said, I did not watch the afternoon, but I read about it тАФ he was much more certain. He was much stronger about the measles vaccine and said it’s, the measles vaccine, is safer than measles, which is a big signal shift there.
Huetteman: It’s true, although I will point out, though, that he did stand by the decision to remove the recommendation for the birth dose of the hepatitis B vaccine when he was pressed on that. So it was, I agree it was a softening, I’d say. At least it wasn’t a dramatic turnaround from what he’d said or not said in the past. But for him, it was at least a softening.
Kenen: In the hepatitis B recommendation, he said that the biggest threat to infection was at, through birth, at, through the mother, and if you test the mother, the baby is not at risk. And that’s partially true, and that is a significant factor to eliminate risk. It doesn’t тАФ it minimizes risk. It does not eliminate risk. Babies can and have been infected in the first weeks of life in other ways. The recommendation was not to totally eliminate that vaccine. It was to postpone it. But there’s, public health, still believe that, in general, many public health leaders would still say that the vaccine at birth is the better way of doing it.
Carey: The focus was, theoretically, on the budget request from the administration. Did the secretary shed any light on those priorities or their impacts? I was taken, I think in the afternoon hearing I read about various lawmakers, including Rosa DeLauro from Connecticut, who sort of just said: A CDC cut of 30%? We’re not gonna do that. And there were also some Republican members who jumped in to sort of say, I don’t think we’re going to do the cuts you envision. But did the secretary defend them? Did he bring any new clarity to them?
Edney: I don’t feel like I gained any new clarity on it. I think to bring it back to Budget 101, I guess, is like when the president, when the administration, sends down their budget, I think a lot of people already assume it’s dead on arrival. And maybe even though Kennedy is there to talk about the budget, it does become this broader hearing, because they don’t get him on the Hill that often and people go there to talk about all kinds of things, and I think that he probably knew that he didn’t have to defend it in the same way, because it’s not going to happen.
Carey: Sure. As they say, the president proposes and Congress disposes. But Joanne, you want to jump in?
Kenen: Yeah, there’s something significant about this administration, which is Congress has repeatedly authorized more money for various health programs and science programs, and the administration doesn’t spend it, so that there’s a different dynamic. Traditionally, yes, Congress тАФ the president proposes, Congress legislates, and then people go off and spend money. That’s what people like to do. And in this case, when Congress has, in a bipartisan way, differed with the administration and restored funding, it hasn’t all gone, those dollars haven’t gone out the door. So the entire sort of checks-and-balances system has been askew in terms of funding. I agree with everybody here. I do not think that Congress is going to accept these extreme cuts across the board in health care and health policy, in public health and science and NIH [the National Institutes of Health] and everything, but I don’t know what they’re actually going to spend at the end of the day.
Carey: Emmarie, you wanted to jump in.
Huetteman: Yeah, there was one striking exchange to me where the secretary acknowledged he wasn’t happy with the cuts that were proposed. I think those were his words. But he pretty quickly added, and neither is President Trump, and he framed it as a matter of making hard decisions when faced with federal budget shortfalls.
Carey: All right. Well, we’ll keep watching this as it moves through Congress. Also during yesterday’s House Ways and Means hearing, some Democrats took issue with past statements from Secretary Kennedy and President Trump that linked Tylenol use during pregnancy to autism in children. released this week in JAMA Pediatrics found that the use of Tylenol by women during pregnancy was not associated with autism in their children. This nationwide study from Denmark followed more than one and a half million kids born between 1997 and 2002, including more than 31,000 who were exposed to Tylenol in the womb. in another medical journal examining community water fluoridation exposure from childhood to age 80 found no impact on IQ or brain function. Kennedy has claimed that fluoride in water has led to IQ loss in children. These studies clearly debunk medical claims that have gotten a lot of attention. Will these findings have an impact now?
Kenen: I think we’ve seen over and over and over again that there are people who are very deeply wedded to certain beliefs, and new science, new research, does not deter them from those beliefs. We also see some people who are sort of in the middle, who are uncertain, and new findings can shift their beliefs, right? And then, of course, there’s a lot of тАФ these are not new studies. I mean these are new studies but they are not the first of their kind. The reason we’ve been using fluoride for, what, 60 years now in the water. Tylenol has been around a long time. So is it going to change everybody’s belief? No. Is it going to perhaps slow the push to ban fluoridation? Perhaps. But I just don’t think we know, because we’re sort of on these dual-reality tracks regarding a lot of science in this country, where once people sort of buy into disinformation, they’re very, it’s very hard to change тАФ or misinformation тАФ it’s hard to change people’s minds.
Edney: I do think, on the Tylenol front тАФ I absolutely agree with what Joanne said overall. And I think on the Tylenol front that it’s possible that this study will give pediatricians something to give and talk about with parents that are asking. I think there still is some confusion among some people. It’s not a huge, I don’t think, widespread thing, but I think there are some new parents who are wondering. And if you are able to take this study that is published in 2026 тАФ it just happened, it was after Trump made his statements тАФ I think maybe that would give them something to talk about with their patients.
Kenen: I agree with Anna. I think the Tylenol one is easier to change than some of the fluoridation stuff going on, partly because so many of us тАФ and we should just say, it’s not just the Tylenol, the brand. It’s acetaminophen, which I’ve never pronounced right. I think those of us who have been pregnant, we’ve taken that in our life before and we don’t think of it as a big, dangerous, heavy prescription drug. I think we’ve, it’s something we feel comfortable with. And I think there’s also the counterinformation, which is, a fever in a pregnant woman can, a pregnant person can be dangerous to the fetus. So I think that one’s a little тАФ and I don’t, also, I don’t think it’s as deep-rooted. The fluoridation stuff goes back decades, and the Tylenol thing is sort of new. And it might be, I’m not sure that the course of these arguments тАФ I think that Tylenol is easier to counter than some other things, because partly just we do feel safe with it.
Carey: All right. We’re going to take a quick break. We’ll be right back.
We’re back and talking about how the Trump administration is managing the voters behind the Make America Healthy Again, or MAHA, movement, which helped President Trump win the 2024 election. My colleagues Stephanie Armour and Maia Rosenfeld wrote about the administration’s recent decision to give coke oven plants in the U.S. a one-year exemption from tougher environmental standards. And that was a move that angered some MAHA activists who wondered if the GOP is more beholden to industry than the MAHA agenda. President Trump, HHS Secretary Kennedy, and other top administration officials met recently at the White House with a group of MAHA leaders to calm concerns that the administration is moving too slowly on food policy changes, and they are concerned about the president’s recent support of the pesticide glyphosate. According to press reports, the MAHA folks seem to feel their concerns were heard during that session. But is this ongoing conflict between the president and this key political constituency, will it be one that keeps brewing as the midterm elections approach?
Edney: Yes, 100%. I think it will continue to brew. I think that meeting was thrown together so quickly that some members of the MAHA movement who were invited couldn’t even make it. So it wasn’t exactly a long-planned, seemingly deep desire to fix everything. But it was, as you’ve said, an effort to kind of hear them out and make them feel heard. No one that I’ve talked to has said everything is fixed now. It’s more of a to-be-determined We will see what the administration will do moving forward, if they will listen to any of our plans тАФ which we will not share with you, by the way тАФ to make us happy. And I think that that’s going to continue. There’s a rally planned in front of the Supreme Court on glyphosate later this month where a lot of those people will be, and so I think that they’re upset and they’re stirring up, that concern is only going to get stirred up more.
Carey: Emmarie.
Huetteman: It’s a small thing, but our fellow podcast panelist Sheryl Stolberg at The New York Times during this White House meeting where President Trump was meeting with MAHA leaders, one of the leaders made a joke about how this is not a group that’s going to be, quote, “Team Diet Coke,” and the president apparently took that as a cue to press that Diet Coke button he famously has on his desk and summon a server who apparently brought him a Diet Coke. Supporters of MAHA have been clear that they want not just for the Trump administration to promote policies supporting priorities like healthy eating and removing food dyes, but also they want them to rein in or end policies they don’t support. And that weed-killer executive order, that really was a big example of that. The MAHA constituency made it clear that they felt betrayed by that order, and they’re going to have to do some work to walk that back.
Carey: We’ll also see how, with their concerns about the new CDC director nominee, which they’re already voicing, we’ll see how that plays out.
Kenen: No, I just think that we are, as we mentioned at the beginning, we’re seeing cracks, right? We’re seeing тАФ none of us are privy to any conversations that President Trump has had privately with Secretary Kennedy. But his, Secretary Kennedy’s, public statements have been a little different than they were a few months ago. There’s certainly been reports that he’s been told to soft-pedal vaccines and talk about some of the things that there’s more unanimity across ideological and party lines. Healthier food тАФ there’s debate about how to, whether, there’s debate about how Kennedy defines healthier food. But in general, should we eat healthier? Yes, we should eat healthier. Should our kids get more exercise? Yes, our kids should get more exercise. Do we have too much chronic disease? Yes, we have too much chronic disease. So they’re sort of this, trying to move a little bit more, sort of this sort of top line, very hazier agreement. But at the same time, the people who are sort of really the core of MAHA, as Kennedy has sort of created it or led it, there’s cracks there.
Carey: All right, we’ll see. We’ll see where that goes. But let’s go ahead and move on to ACA enrollment. A found that 1 in 7 people who signed up for an Affordable Care Act plan failed to pay their first month’s premium. The analysis from Wakely consulting group found that nationally around 14% of those who enrolled in ACA plans didn’t pay their first bill for January coverage. Now we know the elimination of the enhanced ACA tax credits and higher premium costs led to lower enrollment in the ACA exchanges, with sign-ups for 2026 falling to 23 million from 24 million a year ago. But how do you interpret this finding that 14% of enrollees didn’t pay their January premium? Is it a sign of more trouble ahead?
Edney: I think it could be a sign of more trouble ahead. Some тАФ what we’re seeing is sticker shock. And there may be some people who are trying to deal with that and won’t be able to as the months go on. And so, yeah, I think it could mean that even more drop out, and that means more people lose coverage and are uninsured.
Kenen: I think there was sort of a general, initial, misleading sigh of relief when in December, when the enrollment figures, the drop wasn’t as bad as some feared. But at the same time, people said: Wait a minute. This doesn’t really count. Signing up isn’t the same thing as staying covered. The drop in January was significant, we now know. And I agree with Anna. I think we don’t know how many more people will decide they can’t afford it. Or we don’t know whether the big drop is January. Probably a lot of it is, because you get that first bill. But can, will more people drop? Probably. We have no way of knowing how many. And it also depends on the economy, right? If more people lose jobs, right now it’s still pretty, kind of still pretty stable, but we don’t know what’s ahead. We don’t know what’s going to happen with the war. We don’t know many, many, many тАФ we don’t know anything. So the future is mysterious. I would expect it to drop more. I don’t think, I don’t know whether this is the big drop or February will be just as bad. I suspect January will be the biggest. But who knows? It depends on other outside factors.
Huetteman: We’re also seeing a drop-off in the kind of coverage that people are choosing. That analysis that you referenced, Mac, showed that there was a 17% drop in silver plan membership, with most of those folks switching to bronze plans, which, in other words, that means they switch to plans that have lower monthly premiums but they have higher deductibles. And that means that when you get sick, you owe more, in some cases much more, before your insurance starts picking up the tab. And I think really what this means is people are more exposed to the high charges for medical services, bigger bills when you get sick. I think that
Kenen: I think that the Republicans were seen as having pushed back a lot of the health impacts of the so-called One Big Beautiful Bill and that it would be after the election. And I and others wrote: No, no, no, no, no. We’re going to see this playing out before the election. This is a really big political red flag, right? This is a lot more people becoming uninsured, which makes other people worried about their insurance and stability. So I think this is definitely going to тАФ it may not be. There are other things going on in the world. Health care may not be the dominant theme in this year’s election. But yes, this is going to be, the off-year elections are going to be health care elections, like almost every one else has been forтАФ
Carey: Oh yeah.
Kenen: тАФsince the Garden of Eden, right?
Carey: Absolutely, it’s a perennial. All right, we’ll keep our eye on that. That’s this week’s news. Now we’re going to play Julie’s interview with immigration attorney Michelle can arrow, and then we’ll be back with our extra credits.
Julie Rovner: I am pleased to welcome to the podcast Michelle Canero. Michelle is an immigration attorney from Miami and a member of the board of Immigrants’ List, a bipartisan political action committee focused on immigration reform. Michelle, thanks for joining us.
Michelle Canero: Thank you for having me.
Rovner: So, we’ve talked a lot about immigration policy on this podcast over the past year, but I want to look at the big picture. How important to the U.S. health care system are people who originally come from other countries?
Canero: I think the statistics speak for themselves. One in three residency positions can’t be filled by American graduates alone. That means 33% of these residency positions are being filled by immigrant workers. Twenty-seven percent of physicians are foreign-born. Twenty percent of hospital workers are immigrants. And, at least in Florida, a large percentage of our home health care workers happen to be immigrants. And we depend on this population heavily in the health care sector.
Rovner: Now, we talk a lot about the Trump administration’s crackdown on illegal immigration, but we talk a little bit less about their sort of messing with the legal immigration system. And there’s a lot going on there, isn’t there?
Canero: There is. And I think that the campaign talking points were illegal immigration but what we’re actually seeing is a little more sinister. I think that the goal of leadership at the head of DHS [the Department of Homeland Security] and DOS [the State Department], or really Stephen Miller, is pushing something called reverse migration, which is really not about limiting illegal immigration but reducing the immigrant population in the United States. And I think that’s where the real concern is and why you’re seeing these policies that directly affect legal immigrants.
Rovner: We talk a lot about doctors and nurses and skilled, the top skilled, medical professionals who make up a large chunk of the United States health care workforce. We don’t talk as much about the sort of midlevel professional workers and the support staff. They’re also overwhelmingly immigrant, aren’t they?
Canero: Yeah, and whether it’s your IT- and technical-knowledge-based workers in hospitals who facilitate all the technology тАФ we rely on an immigrant workforce for a lot of the technology sector. And then you’ve got research professionals. A lot of clinical researchers, medical researchers, are foreign-born. So it’s not just about the doctors. It’s also the critical staff that keep the hospitals operating. And I’m from Florida. For us, it’s the home health care workers. We have an aging population, and a large percentage of the home health care workers, particularly in Florida, happen to be Haitians on TPS [temporary protected status] or people with asylum work authorizations. And when we lose that, our aging population is left with no resources, because that’s not something AI or technology can fix. You can’t turn someone over in a bed with a robot yet, and we’re probably decades away from that.
Rovner: So what’s the last year been like for you and your clients?
Canero: I think it’s a lot of uncertainty. A lot of these policies are percolating, and we’re assuming that they’ll be resolved in litigation, but the damage is being done in real time. So we’re seeing hospitals turning away from hiring foreign workers, because of the H-1B penalty now. The suspension of J-1 processing created backlogs. These visa bans that affect 75 countries on certain visas and 39 countries on others. You’ve got thousands of health care workers that are stuck outside the U.S. So what’s happening, really, is that hospitals and medical providers are just shutting down, and they’re cutting back services, and that means that there are less available services and resources for the same population and the same demand. People are waiting longer for doctor’s appointments. People are finding that they’re not able to get to the specialist that they need to get to in time. And so for us as practitioners, I think, we’re trying to navigate as best we can, but we’re just seeing a lot of people, employers that traditionally would rely on our services, give up and foreign workers looking to go elsewhere.
Rovner: I noticed during the annual residency match in March that it worked out, I think, fairly well for most graduating medical students. But the big sort of sore thumb that stuck out were international medical graduates. That’s going to impact the pipeline going forward, isn’t it?
Canero: From what I understand, it takes like seven to 15 years to get to that level, and we just don’t have the student body to meet the demand of residency positions. From my understanding, there’s a gap between American graduates and the demand for residents that’s usually filled by foreign workers. And if we don’t have those foreign workers, those residency positions just don’t get filled. And that becomes more expensive for hospitals, and that transfers to our medical bills.
Rovner: And people assume that, Oh well this doesn’t impact me. But it really impacts all patients, doesn’t it? And I would think particularly those in rural areas, which are less desirable for U.S.-born and -trained medical professionals and tend to be overrepresented by immigrants.
Canero: Yeah, I think a lot of the J-1 doctors and H-1B doctors are what facilitate, are working at, our veterans hospitals and our rural medical facilities. And what’s ending up happening is the very same people that this administration touts to support their interests are being forced to travel farther for specialists, right? If there isn’t an endocrinologist in your area, you may have to drive 100 miles to go see that specialist, and you may forgo necessary medical care because of the inconvenience or the cost. And I think that’s hitting at our health.
Rovner: So you’re on the board of Immigrants’ List, which is working to change things politically. What’s one change that could really make a big difference in what we’re starting to see in terms of immigration and the health care workforce?
Canero: Well, asking Congress to actually do something. It’s been a problem for decades. So I don’t really know, but I think there’s a couple of things, whether it’s just policymakers supporting our fight against some of these illegal policy changes in courts, organizations supporting us with amicus briefs. For example, there’s a lot of lawsuits challenging these visa bans and these adjudicative holds and the H-1B fine. The more support that the plaintiffs in the litigation get, the more likely we are to resolve that through the court system. And then I hope that there’s enough pressure from hospitals and organizations that have real dollars that impact these elected officials to get them to start seeing, Hey, we need to pass reasonable immigration reform to address some of the loopholes that this administration is using to cause chaos in the system, right? They’re able to do this because we have a gap. We allow them to terminate TPS. We don’t have a structure to ensure that a community that’s been on TPS for 20 years gets grandfathered into some sort of more stable visa. We don’t have a system that precludes the administration from just putting a hold or a visa ban on nationalities. So it’s something that Congress is going to have to step up and do something about.
Rovner: What worries you most about sort of what’s going on with the immigration system and health care? What keeps you up at night? Obviously you, I know you work on more than just health care.
Canero: I think my concern is that the American people aren’t seeing what’s happening, or they’re sort of turning a blind eye to it, and by the time it starts to actually impact them and they start asking, Wait, wait, wait. Why is this happening? I don’t understand, it’s going to be too late. Because it’s not hitting their pocket, because it’s not their suffering at this point, they’re not standing up and saying, Hey, this needs to stop, at the level that we need, opposition, to make it stop. And by the time it does hit their pocket and it does affect them directly, I think, it’ll be a little too late. I think people will be scared off from coming here, people that we needed will be gone, and to reverse the system is going to take decades.
Rovner: Michelle Canero, thanks again.
Canero: No, you’re very welcome. Thank you for your time.
Carey: OK, we’re back. Now it’s time for our extra-credit segment, and that’s where we each recognize a story we read this week and we think that you should read it, too. Don’t worry if you miss it. We’ll post the links in our show notes. Joanne, why don’t you start us off this week?
Kenen: Well, this is by Teddy Rosenbluth in The New York Times. The headline is “” This is one of those stories where you know exactly how it’s going to end in the first paragraph, and yet it was so compellingly and beautifully written that you kept reading until the last word. It is, as the headline suggested, a young man who is an expert on AI and cognitive science named Ben Riley discovered that his father had been lying about a controllable, treatable form of leukemia. He had denied treatment, he’d refused treatment, he had ignored his oncologist because he was relying on AI. And as we all know, AI has its up moments and its down moments. And he was getting incorrect information, distrusted the diagnosis, refused treatment, getting sicker and sicker and sicker as the oncologist and the family got increasingly desperate. And the son, Ben Riley, had, like, skills. He knew how to find scientific evidence, and his father just would not believe it. And by the time his father finally consented to treatment, it was too late, and he did die. And his father was a neuroscientist, a retired neuroscientist, but he found a neuroscience rabbit hole.
Carey: That’s amazing. Anna, what’s your extra credit?
Edney: Mine, I’m highlighting a story that I wrote in Bloomberg called “.” And this is, I wanted to dive into this policy that the FDA had implemented. The commissioner has long talked about and felt that perimenopausal and menopausal women were not getting access to the treatments that maybe they really needed, because there had been sort of this two-decade-old study that had showed there were some safety issues regarding breast cancer and cardiovascular disease, but the issue being that those studies had looked at older forms of the medication and also at women who were much older than those who might benefit from taking it. And so they, the agency, asked the companies to remove those warning labels, at least the strongest ones. And what we’ve seen, why тАФ I wanted to dive into the numbers specifically. Bloomberg has some prescription data that was able to help me out here and just look at when this started rising. You could see that the prescriptions started going up around 2021. I feel like a lot of influencers, a lot of celebrities, were talking about this. And then in 2024 to 2025 when the FDA started talking about this, it really just goes, the prescription numbers just go straight up on the scale. And so there were about 32 million prescriptions written last year, which is a huge increase. And I just dove into some of this, some of the companies, what kind of drugs there are out there, and talked to some women who are benefiting but also, because of this pop, experiencing shortages, because the companies aren’t quite keeping up with the products.
Carey: Wow, that sounds like an outstanding deep dive. Thank you. Emmarie.
Huetteman: Yeah, my extra credit is from my colleague at ║┌┴╧│╘╣╧═Ї News who covers health technology. That’s Darius Tahir. The headline is “Your New Therapist: Chatty, Leaky, and Hardly Human.” The story looks at the proliferation of AI chatbot apps that offer mental health and emotional support, particularly the ones that market themselves as, quote-unquote, “therapy apps.” Darius counted 45 such apps in Apple’s App Store last month, and he uncovered in some cases that safety and privacy concerns existed, such as minimal age protections. Fifteen of the apps that he looked at said they could be downloaded by users who were only 4 years old. His story also explored the tension between the risks of sharing sensitive data and the interests of app developers and collecting that data for business purposes. It’s a good read. All right,
Carey: All right. Thanks so much. My extra credit is from Politico, and it’s written by Alice Miranda Olstein, and she’s a frequent guest here on What the Health? The headline is, quote, “,” close quote. The headline kind of says it all. Alice writes that Nebraska is racing to implement Medicaid work requirements by May 1, and that’s eight months ahead of the national deadline that was set by the One Big Beautiful Bill Act. Nebraska state officials plan to do this without hiring additional staff, even as other health departments in other states prepare to bring in dozens, if not hundreds, of new employees. Alice writes that advocates for people on Medicaid fear that this rush timeline and lack of new staff will cause many problems for Medicaid beneficiaries who are just trying to meet those new work requirements.
All right. That’s this week’s show. Thank you so much for listening. Thanks, as always, to our editor and panelist Emmarie Huetteman, to this week’s producer and engineer, Taylor Cook, and to my KFF colleague Richard Ho, who provided technical assistance. A reminder: What the Health? is now available on WAMU platforms, the NPR app, and wherever you get your podcasts, as well as, of course, kffhealthnews.org. Also, as always, you can email us with your comments or questions. We’re at whatthehealth@kff.org. Or you can find me on X, . Joanne, where can people find you these days?
Kenen: and , @joannekenen.
Carey: OK. Anna?
Edney: and and , @annaedney.
Carey: And Emmarie.
Huetteman: You can find me on .
Carey: We’ll be back in your feed next week. Until then, be healthy.
Credits
Click here to find all our podcasts.
And subscribe to “What the Health? From ║┌┴╧│╘╣╧═Ї News” on , , , , , or wherever you listen to podcasts.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/podcast/what-the-health-442-cdc-director-nominee-rfk-hearing-april-17-2026/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2182989&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>LISTEN: Quashing innovation or risking a patient’s health? Lauren Sausser told WAMU’s Health Hub on April 15 why the White House and some states are at odds over how to regulate AI in health care.
Speed, efficiency, and lower costs. Those are the traits artificial intelligence supporters celebrate. But the same qualities worry physicians who fear the technology could lead to insurance denials with humans left out of the loop.
With scant federal regulation, states are left to shape the rules on AI in health care. For residents in the Washington, D.C., metropolitan area, a divide is playing out on opposite sides of the Potomac River. Maryland and Virginia have taken very different approaches to regulating AI in health insurance.
║┌┴╧│╘╣╧═Ї News correspondent Lauren Sausser joined WAMU’s Health Hub on April 15 to explain why where you live may determine how much of a role AI plays in your coverage.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/wamu-health-hub-ai-state-regulation-april-15-2026/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2228242&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>HAY SPRINGS, Neb.тАФ The sun was just warming the horizon as Mark Pieper left his house near his cattle ranch on a crisp February morning.
It’s not unusual for the rancher to wake up early to tend to livestock, but at 5:45 a.m. this day his cattle wouldn’t come first. For the past 3┬╜ years, three days a week, Pieper has made an early-morning commute to get dialysis at the nearest hospital.
Pieper lives outside Hay Springs, which has 599 residents, according to a sign at the edge of town. He makes sure not to forget his chocolate-brown cowboy hat before starting up his pickup truck for the half-hour drive to Chadron.
That February morning was one of his last dialysis sessions there before the hospital shuttered the service at the end of March.
“I guess I’ll just bloat up and die in a month,” Pieper remembered thinking when he learned the center was closing, eliminating the only option near his home.
He needs dialysis to survive after cancer treatment damaged his kidneys.
Pieper and 16 other patients relied on Chadron Hospital for the life-sustaining therapy that filters waste and fluid from their blood тАФ a job their failing kidneys could no longer do. Treatment lasts about four hours.

The closure is just one example of the long decline of health care services in rural America, where people have higher rates of many chronic conditions but less access to care than elsewhere.
The Trump administration promised to address this problem, when it launched the $50 billion federal Rural Health Transformation Program in September. It may not be enough to stop the trend.
“[President Donald] Trump says he is going to help the rural health care,” Pieper said. Dialysis “is one thing that we really need here.”
Some patients have moved to live closer to care, including several nursing home residents. Their new facilities may be farther from their families.
Others are making long drives to dialysis centers. Pieper eventually found treatment in Scottsbluff, which, with about 14,000 residents, is the biggest city in the rural Panhandle region of western Nebraska. The hour-and-a-half drive will triple his time on the road to more than nine hours each week.
Jim Wright and his wife reduced their drive time тАФ but are spending more money тАФ by renting a small home near Rapid City, South Dakota, and living there on weekdays so he can get dialysis. Wright said he understands that rural hospitals face financial challenges.
“But we’re talking about something that’s lifesaving. It’s not a matter of, тАШOh, I would like to be there’” getting treatment, he said. “It’s a case that if you don’t, you die.”

An Influx of Money That’s Out of Reach
Jon Reiners, CEO of the independent, nonprofit Chadron Hospital, wrestled with the decision to end dialysis services. He and several patients said that the closure was announced as the $219 million the state will receive in first-year funding from the .
But the five-year program is aimed at exploring new, creative ways to improve rural health, not to help existing services stay afloat. States can use only up to 15% of their funding to pay providers for patient care.
At least 11 states тАФ Nebraska is not among them тАФ have mentioned using funding for rural dialysis programs, according to a ║┌┴╧│╘╣╧═Ї News review of applications. Their ideas include starting a mobile dialysis unit and helping people get treatment at home or in long-term care facilities.
Reiners said Chadron Hospital lost $1 million a year on its dialysis service due to low reimbursement rates that didn’t cover operational costs.

The facility is a critical access hospital, a designation that allows certain small, mostly rural hospitals to get increased reimbursement rates for their Medicare patients. While most of the affected patients were on Medicare, the critical access program doesn’t cover outpatient dialysis, Reiners said.
Reiners said the hospital worked for more than a year to find solutions, such as reaching out to four private companies to potentially take over the center. But he said they all passed after realizing they would lose money.
Nephrologist Mark Unruh said the dialysis closure in Chadron reflects a wider trend of staffing and funding challenges.
“You do end up in situations where you have people who are displaced like this, and it’s just sad,” said Unruh, chair of the Internal Medicine Department at the University of New Mexico.
People in rural America face significant disparities in kidney health and treatment, published in 2024 in the American Journal of Nephrology. They’re and face after diagnosis, according to data from the National Institutes of Health.
The best way to address this is to focus on prevention, Unruh said. He pointed to a that helps primary care doctors in rural and other underserved areas prevent end-stage renal failure.
Another idea, Unruh said, is boosting the rate of kidney transplantation for rural patients. He’s looking at whether it’s helpful to “fast-track” tests patients need to get approved for a transplant by scheduling all of them over a couple of days to limit travel time.
Unruh said the U.S. health system also needs to recruit more staff who can train patients and their caregivers to administer dialysis at home.
Exploring the Option of Home Dialysis
Rural dialysis patients are more likely than urban ones to get home dialysis, according to . In 2023, the rate was nearly 18% for rural patients and about 14% for urban ones.
One type of home dialysis requires surgery to get a catheter placed in the abdomen and . The other kind requires . The nearest facility to Chadron that offers training for the first option is in Scottsbluff. The nearest that offers training for the latter kind is three hours away in Cheyenne, Wyoming.
Pieper said doctors told him he’s not a candidate for home dialysis or a transplant. The Panhandle has a nonprofit, rural transit system, but its schedule won’t work for Pieper. He said that leaves him with no choice but to get treatment in Scottsbluff, a 200-mile round trip.
It takes Linda Simonson even longer тАФ more than four hours round trip тАФ to drive her husband, Alan, from their ranch to his treatment in Scottsbluff.
Linda sat in the waiting room with a yellow legal pad during one of Alan’s final treatments in Chadron. The paper was scrawled with phone numbers of politicians to call and driving distances to dialysis centers in the region. She said facilities closer to their ranch either don’t have room for new patients or lack good spots along the route to take a driving break in bad weather.
“It’s just unreal,” she said.
She said even if Alan took a bus, she’d have to ride along to support him during the trip and his treatment.
Jim and Carol Wright, the couple staying near Rapid City on weekdays, said they can’t afford to rent a second home forever. Their weekly commute is already taking a physical and emotional toll. They said they’ll eventually have to move to a bigger city, giving up the house they love in the scenic Nebraska National Forest.
Carol said she feels for the dialysis staffers in Chadron, who are wonderful.
“It just doesn’t seem right to sacrifice one unit that’s so vital,” she said while standing next to a pile of moving boxes stacked inside their rental.

The Wrights wrote letters to politicians and hospital leaders to share their concerns and ideas for keeping the unit open, including using the federal rural health funding.
Simonson said she spoke with aides for the governor and her state representatives but none of the leaders called her back.
“It feels like they don’t know that we exist at this end of the state,” she said.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/rural-health/dialysis-unit-closes-rural-transformation-health-fund-nebraska/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2178069&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
An elementary school teacher chose a low-price health insurance plan but soon realized she wasn’t clear about what it would mean for her family’s finances.
“Once I got the insurance card, I compared our old plan to our new plan, and that’s when I really got worried, because I didn’t really understand what a deductible was. It got me thinking, how do I use this insurance?”
тАФ Madison Burgess, 31, of San Diego
When enhanced federal subsidies expired at the end of 2025, a lot of people buying their own health insurance on the state and federal exchanges saw their expected monthly rates jump. To keep costs down, many switched to a high-deductible health plan. These plans offer lower monthly payments, but in exchange patients can face steep out-of-pocket costs when they need care.
The plans are pretty common. In 2023, 30% of people who got insurance through their employer had a high-deductible plan, up from only 4% in 2006.
Madison Burgess, a teacher in San Diego, gets health insurance through her teaching job. But when she investigated adding her husband to her plan, it was just too expensive, so she started shopping on the exchange for a cheaper option for him.
The longer she scrolled through the plan options, the more overwhelming it felt. Insurance jargon made it hard to tell what her family would owe if her husband got sick.
“I didn’t know what a deductible was, so I just went with what was cheap, and now I have regret,” she said.
In exchange for that lower monthly premium payment, her husband’s coverage won’t kick in for most care until they’ve paid $5,800 in medical bills. Burgess didn’t know that the deductible must be met before insurance picks up part of the tab.
Deductible:
The amount you as the patient have to pay before insurance picks up part of the tab

Premium:
The monthly bill for your policy, paid to the insurance company

How do you prepare for thousands of dollars in upfront costs? One option is a health savings account, or HSA, which lets you save pretax money and is now available to people enrolled in lower-tier state and federal exchange plans, including bronze and catastrophic coverage. These plans generally have the lowest premiums on the exchange but the highest out-of-pocket costs when you need care.
Burgess had chosen a bronze plan and didn’t know HSAs were an option.
“I’ve never thought about having to put money away for a deductible,” she said.
Burgess and others are often more worried about socking away money for unexpected car and house repairs or vet bills.
If, like Burgess, you chose cheaper health coverage for this year only to discover you’re on the hook for meeting a high deductible, these tips can help you prepare.
1. You might qualify for an HSA and not know it.

If you’re enrolled in a bronze or catastrophic plan, you qualify to open a health savings account. Think of it as a medical piggy bank with tax perks. You put in pretax money, which lowers your taxable income. The money grows tax-free, and when you spend it on , those transactions are also tax-free. That’s what people call a “triple tax advantage.”
These accounts build a cushion for future health costs, such as doctor visits, prescriptions, and even products like over-the-counter medicine, tampons, and sunscreen.
The money typically can’t be used for monthly premiums, but the account is yours to use for qualified medical expenses for yourself, your spouse, or your dependents anytime in the future. The money in the account is yours, even if you change jobs or health plans.
An HSA is not the same as a flexible spending account, or FSA. FSAs are tax-advantaged too but are offered only through employers. The money expires annually and you lose any remaining money when you leave that job.
2. HSA-curious? Here’s how to open one.
You open a health savings account through a bank or other financial institution. The institution will issue you a debit card so you can make purchases from the HSA.
You can at any point during the year as long as you’re covered by an eligible plan. You can choose where to open the account, but be sure to check for any fees financial institutions charge and shop around.
If you get insurance through your job, your employer may require you to use a specific IRS-approved company.

Many people decide they can’t afford to contribute to an HSA. For some households, the desire to set aside money for medical expenses competes with the need to pay rent and buy groceries.
But there’s a detail that can make it feel more manageable. Contributions don’t have to be large. Just a few dollars a month can get you started.
There is, however, a limit. The IRS sets an annual cap on how much you’re allowed to contribute to an HSA. In 2026, an individual is limited to $4,400, or $8,750 for a family plan. Under that ceiling, the amount is up to you.
3. Preventive services should be covered at no cost to you.
All plans sold on marketplaces must cover at no cost to the patient as long as the care is provided in-network. Those services include routine immunizations and cancer screenings.
Beyond preventive care, understanding what different services cost can help you decide which type of medical appointment works best for your health needs and your wallet. For example, some plans charge less for a telehealth visit than to see your primary care doctor in person.
Check out your for more details.
4. Seek care early in the year.
Most deductibles reset on Jan. 1. Scheduling appointments or surgeries early in the year can be strategic if you discover a condition that requires ongoing care. If you can afford it, meeting your deductible sooner can make the rest of the year significantly cheaper, said Caitlin Donovan, a senior director at the Patient Advocate Foundation.
5. Consider paying cash instead of spending down your deductible.
Some hospitals, clinics, or other providers offer cheaper prices if you pay cash. You have the and explanation of how much a health service would cost if you paid out-of-pocket. Ask for the estimate before you get care. Then, compare that price with what your insurance company tells you it would cost if you used your insurance. If you decide to go with a cash payment, you’ll need to pay while you’re still at the doctor’s office, before charges get submitted to your insurance company.
Paying cash may save you money, but the amount you pay generally won’t count toward your deductible or out-of-pocket maximum.
“If you don’t think you’re ever going to hit your deductible тАФ you’re that young invincible, and your deductible is $10,000 тАФ negotiate the cash price,” Donovan said.
6. On an ACA plan? Update your income and use an HSA to avoid a tax surprise.

If you’re on an ACA plan and you’re eligible for subsidies, be aware: If your and you don’t update your marketplace application, you could owe thousands of dollars at tax time. The . Report raises, new jobs, or side gigs as they happen. If your income goes up, stashing money in an HSA can help because the money you put in the account doesn’t count toward your taxable income.
As soon as you report an increase in your income, that could mean higher premiums (if you no longer qualify for the same subsidy), but experts say it’s better to pay now than owe a big bill that you have to pay all at once.
“One of the biggest problems I see is someone is newly unemployed and they sign up for coverage, they say that they’re not making any money, and then eventually they get a job and don’t report it, and then they have this huge tax bill at the end,” Donovan said.
She advises updating your marketplace profile as soon as your income changes, which could newly qualify you for Medicaid or a plan that contributes more toward your medical bills.
Taylor Cook contributed to this report.
Health Care Helpline helps you navigate the health system hurdles between you and good care. Send us your tricky question and we may tap a policy sleuth to puzzle it out. Share your story. The crowdsourced project is a joint production of NPR and ║┌┴╧│╘╣╧═Ї News.
This <a target="_blank" href="/health-care-costs/health-care-helpline-npr-hsa-savings-account-high-deductible-plan-tips/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2171426&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This year, executives from nearly every major health insurance company made the same declaration in calls with Wall Street analysts: Using artificial intelligence to make coverage decisions would help save them money.
Even the Trump administration is testing AI’s usefulness in managing the prior authorization process for the Medicare program, as well as seeking to override AI regulation by states.
But class action lawsuits have accused insurers of using AI to wrongfully withhold treatment. And outlines the risks of training AI on a current system rife with wrongful denials.
“There is a world in which using AI could make that worse, or at least replicate a bad human system, because the data that it would be training on is from that bad human system,” said Michelle Mello, a co-author of the study.
Although, Mello said, the research team found “real positives alongside the risks.”
In this video produced by ║┌┴╧│╘╣╧═Ї News’ Hannah Norman, Darius Tahir, a correspondent covering health technology, explains.
You can read Tahir’s recent coverage of AI’s use by health insurers below:
- “Red and Blue States Alike Want To Limit AI in Insurance. Trump Wants To Limit the States,” by Darius Tahir and Lauren Sausser.
- “AI Will Soon Have a Say in Approving or Denying Medicare Treatments,” by Lauren Sausser and Darius Tahir.
This <a target="_blank" href="/courts/watch-ai-artificial-intelligence-prior-authorization-insurance-coverage-decisions/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2181021&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
At the Trump administration’s request, a federal judge in Louisiana this week agreed to delay a ruling affecting the continued availability of the abortion drug mifepristone. That angered anti-abortion groups that want the drug, if not banned, at least more strictly controlled. But the administration clearly wants to avoid big abortion fights in the run-up to November’s midterm elections.
Meanwhile, the administration’s proposed budget for fiscal year 2027 calls for more than $15 billion in cuts to programs at the Department of Health and Human Services. It’s a significant number, but less drastic than cuts it proposed for fiscal 2026.
This week’s panelists are Julie Rovner of ║┌┴╧│╘╣╧═Ї News, Lauren Weber of The Washington Post, Alice Miranda Ollstein of Politico, and Maya Goldman of Axios.
Panelists



Among the takeaways from this week’s episode:
- The Trump administration says it is conducting a thorough scientific review of the abortion pill mifepristone at the Food and Drug Administration. Yet advocates on both sides of the abortion debate think the administration is just trying to buy time to avoid a controversial decision about medication abortion before November’s midterm elections.
- It’s budget time on Capitol Hill. With the unveiling of the president’s spending plan for fiscal 2027, Cabinet secretaries will make their annual tour of congressional committee hearings. HHS Secretary Robert F. Kennedy Jr., whose Hill appearances have been few during his tenure, is scheduled to testify before six separate House and Senate committees before the end of the month.
- Back at HHS, Kennedy appears to be trying to reconstitute the Advisory Committee on Immunization Practices in a way that will enable him to restock it with vaccine skeptics without running afoul of a March court ruling that he violated federal procedures with his replacements last year.
- Continuing his efforts to promote his Make America Healthy Again agenda, Kennedy announced this week that he will launch his own biweekly podcast. He also announced efforts to combat microplastics in the water supply and to get hospitals to stop serving ultraprocessed food to patients.
Plus, for “extra credit,” the panelists suggest health policy stories they read this week that they think you should read, too:
Julie Rovner: The Atlantic’s “,” by Katherine J. Wu.
Maya Goldman: ║┌┴╧│╘╣╧═Ї News’ “,” by Amanda Seitz and Maia Rosenfeld.
Lauren Weber: CNN’s “,” by Holly Yan.
Alice Miranda Ollstein: Politico’s “,” by Simon J. Levien.
Also mentioned in this week’s podcast:
- JAMA Internal Medicine’s “,” by Lauren J. Ralph, C. Finley Baba, Katherine Ehrenreich, et al.
- ║┌┴╧│╘╣╧═Ї News’ “,” by Vanessa G. Sánchez, El Tímpano.
- The New York Times’ “,” by Ellen Barry.
- Stateline’s “,” by Nada Hassanein.
- The Washington Post’s “,” by Lena H. Sun.
[Editor’s note: This transcript was generated using both transcription software and a human’s light touch. It has been edited for style and clarity.]
Julie Rovner: Hello, from ║┌┴╧│╘╣╧═Ї News and WAMU Public Radio in Washington, D.C. Welcome to What the Health? I’m Julie Rovner, chief Washington correspondent for ║┌┴╧│╘╣╧═Ї News, and I’m joined by some of the best and smartest health reporters covering Washington. We’re taping this week on Thursday, April 9, at 9:30 a.m. As always, news happens fast, and things might have changed by the time you hear this. So here we go.
Today, we are joined via video conference by Lauren Weber of The Washington Post.
Lauren Weber: Hello, hello.
Rovner: Alice Miranda Ollstein of Politico.
Alice Miranda Ollstein: Hi, everybody.
Rovner: And my fellow Michigan Wolverine this national championship week, Maya Goldman of Axios. Go, Blue!
Maya Goldman: Go, Blue.
Rovner: No interview this week, but plenty of news. So let’s get right to it. We’re going to start with reproductive health. On Tuesday, a federal judge in Louisiana ruled for the Trump administration and against anti-abortion forces in a lawsuit over the availability of the abortion pill mifepristone. Wait, what? Please explain, Alice, how the administration and anti-abortion groups ended up on opposite sides of an abortion pill lawsuit.
Ollstein: Yeah. So this has been building for a while, and it is not the only lawsuit of its kind out there. There are several. A bunch of different state attorneys general, who are very conservative and anti-abortion, have been suing the FDA in an attempt to either completely get rid of the availability of the abortion pill mifepristone or reimpose previous restrictions on it. So right now, at least according to federal rules, not according to every state’s rules, you can get it via telehealth. You can get it delivered by mail. You can pick it up at a retail pharmacy. You don’t have to get it in person handed to you from a doctor like you used to. So these lawsuits are attempting to bring back those restrictions or get the kind of national ban that a lot of groups want. And so you have other ones pending: Florida, Texas, Missouri, you have a bunch of ones. So this is the Louisiana version. And the Trump administration, it’s important to note, they are not defending the FDA or the abortion pill on the merits. They are saying, we don’t want this lawsuit and this court to force us to do something. We want to go through our own careful process and do our own internal review of the safety of mifepristone, and then we may decide to impose restrictions. But they’re asking courts to give them the time and space to complete that process and saying, you know, This is our power we should have in the executive branch. And so, in this case, the judge, in ruling for the Trump administration, basically just hit pause. This doesn’t get rid of the case. It just puts a stay on it for now, and that’s important. In some of these other cases, the Trump administration has asked the courts to throw out the case, but that was not the situation here. So this doesn’t mean that abortion pills are going to be available forever. This doesn’t mean nothing’s going to happen, and they’re going to be banned. This just means, you know, we’re kicking the can down the road.
Rovner: I was saying, just to be clear. I mean, we know that this FDA quote-unquote “study” тАФ whether it is or isn’t going on тАФ is part of, kind of, a delaying tactic by the administration, because they don’t want to really make abortion a big front-and-center issue in the midterms. So they’re trying to sort of run the clock out here. Is that not sort of the interpretation that’s going on right now?
Ollstein: That’s what people on both sides assume is going on. It’s really been fascinating how everyone is being kept in the dark about what’s happening inside the FDA тАФ and if this review is even happening, if it’s real, if it’s in good faith, what is it based on? And so it’s become this sort of Rorschach test, where people on the left are saying, you know, They’re laying the groundwork to do a national ban. This is just political cover. They just want to wait until after the midterms, and then they’re going to go for it. And people on the right are saying, you know, The administration is cowardly, and they aren’t really doing anything, and they’re just trying to get us to shut up and be patient. We don’t know if either of those interpretations or neither of them are true.
Rovner: Lauren, you want to add something?
Weber: I just think it’s pretty clear this is also just on a [Health and Human Services Secretary Robert F.] Kennedy [Jr.] priority. I mean, let’s go back. The man тАж comes from one of the top Democratic political families originally. You know, there’s obviously been a lot of chatter around his anti-abortion beliefs. Now, obviously, he’s on a Republican ticket. I think some of that plays into this as well. And he already has his hand on the stove on so many other hot issues that, [if] I had to guess, I don’t think that they’re trying to rock the boat on this one. тАж I think, some background context too, to some of what’s going on.
Rovner: We’ll get to some of those hotter issues. But, meanwhile, the Journal of the American Medical Association [Internal Medicine] has a suggesting that medication abortion is so safe that it could be provided over the counter тАФ that’s without any consultation with a medical professional, either in person or online. This doesn’t feel like it’s going to happen anytime soon, though, right? While we’re still debating the existence of medication abortion in general.
Ollstein: That’s right. I mean, there are a lot of people who can’t get this medication prescribed by a valid doctor right now, let alone over the counter. I will say it is common in a lot of parts of the world to get it over the counter, whereas in the United States, the most common way to have a medication abortion is with a two-pill combination, mifepristone and misoprostol. In a lot of parts of the world, people just use misoprostol alone, and it is effective and it is largely safe. It’s slightly less safe than using both pills together. And so I think there’s a lot of international data out there, and people point to that and advocate for this. And I will say there are activist groups in the United States who are setting up networks, underground networks, to get these pills to people with no doctor’s involvement. And so that is already going on. I think that a lot of people would prefer to get it from a doctor if they could. But because of bans and restrictions, they can’t. And so people are turning to these activist groups.
Rovner: I will point out, as a person who covered the entirety of the fight to have emergency contraception тАФ which is not the abortion pill тАФ made over the counter, it took like, 15 years. It shortened my life covering that story. Lauren, did you want to add something?
Weber: Yeah, I just wanted to say I find it really interesting. Obviously, reproductive issues end up taking 15 years, as you pointed out, to make it over the counter. But there are a lot of things that are considered potentially more dangerous that you can order up in a pretty basic telehealth visit or even just buy in not-so-sketchy ways that the administration is also even looking to deregulate. So I think the differences of access of this compared to other less studied, potentially more unsafe medication is quite striking.
Goldman: Part of [President Donald] Trump’s “Great Healthcare Plan” is making more medications available over the counter. So this is certainly something that they have said they want to do, in general. This is a political nightmare, though, to do that for abortion.
Ollstein: Yeah, and people have been pointing to this and a lot of other policies for a while to argue about something they call abortion exceptionalism, in which people apply a different standard to anything related to abortion, a different safety standard, a different standard of scrutiny than they do to medications for lots of other purposes. And you’ve seen that, and that comes up in lawsuits and political arguments about this. And I think, you know, people can point to this as another example.
Rovner: So last week, we talked about the federal family planning program Title X, which finally got funded after months of delays. But Alice, you warned us that the administration was planning to make some big changes to the program, and now those have finally been announced. Tell us what the plan is for a program that’s provided birth control and other types of primary and preventive care since the early 1970s.
Ollstein: Well, the changes have sort of been announced. They’ve more been teased. What we are still waiting for is an actual rule, like we saw in the first Trump administration, that would impose conditions on the program. And so what we saw recently, it was part of a wonky document called a “Notice of Funding Opportunity,” or NOFO, for those in the D.C. lingo. And basically it was signaling that when groups reapply тАФ they just got this year’s money, but when they reapply for next year’s money тАФ it sets up sort of new priorities and a new focus for the entire program. And what was really striking to me is, you know, this is a family planning program. It was created in the 1970s and it is primarily about delivering contraception to people who can’t afford it around the country, providing it to millions of people who depend on this program, and the word “contraception” did not appear in the entire 70-page document other than an assertion that it is overprescribed and has bad side effects. And instead, they signaled that they want to shift the program to focus on, quote, “family formation.” So this is really striking to me. I think we saw some signs that something like this was coming. You know, about a year ago, there was some Title X money approved to focus on helping people struggling with infertility. But that was sort of just a subset of the program, and now it looks like they want to make that, you know, an overriding focus of the program. So I think when the actual rule to this effect drops, and we don’t know when that will be тАФ will they wait till after the midterms to, you know, avoid blowback? Who knows? I think there will certainly be lawsuits then. But I think right now, this is just sort of a sign of where they want to go in the future. And it’s important to note that it came very quickly on the heels of a big backlash from the anti-abortion movement over the approval of this year’s funding going out to all of the clinics that got it before, including Planned Parenthood clinics. The anti-abortion groups were agitating for Planned Parenthood to be cut off at once, you know, not in the future, right now.
Rovner: Just to remind people that the ban on Planned Parenthood funding from last year was for Medicaid, not for the Title X program.
Ollstein: Right.
Rovner: And that’s why Planned Parenthood got money.
Ollstein: Yes, and Planned Parenthood is not allowed to use any Medicaid or Title X money for abortions, but the anti-abortion groups say it functions like a backdoor subsidy, and so they wanted it to be cut off. So they were very pissed that this money went out to Planned Parenthood. And so very quickly after, the administration put out this document, saying, Look, we are taking things in another direction, and it is not the direction of Planned Parenthood.
Rovner: Lauren, you want to add something?
Weber: Oh, I just wanted to say Alice has really been owning the beat on all the Title X coverage, so тАж
Rovner: Absolutely.
Weber: тАж glad we are able to have her explain it to us. But just wanted to throw out a kudos for breaking all the news on that front.
Goldman: Yeah, great coverage.
Rovner: Yes. Very happy to have you for this. Turning to the budget, which is normally the major activity for Congress in the spring, we finally got President Trump’s spending blueprint last week. It does propose cuts to discretionary spending at the Department of Health and Human Services to the tune of about $15 billion, but those cuts are far less deep than those proposed last year. And, as we have noted, Congress didn’t actually cut the HHS budget last year by much at all. And many programs, like the National Institutes of Health, actually got small increases. Is this budget a reflection of the fact that the administration is recognizing that cuts to Health and Human Services programs aren’t actually popular with the public or with Congress, for that matter, going into a midterm election?
Weber: I think it’s that last little piece you mentioned there, Julie. I think it’s the “going into the midterm election.” I think you hit the nail on the head there. Cuts are also not good economically for many Republicans. You know, we saw Katie Britt be one of the тАФ the Alabama Republican senator тАФ be one of the most outspoken senators in general about some of the cuts that were floated for the budget for HHS last year. So I think what you’re hinting at, and what we’re getting at, is that it’s not politically popular, it can be economically problematic, on top of the scientific advances that are not found. So I suspect you are right on that.
Ollstein: The administration knows that this is “hopes and dreams” and will not become reality. It did not become reality last year. It almost never becomes reality. And I think you can see the sort of acknowledgement that this is about sending a message more than actually making policy in things like Title X, because at the same time they put out this guidance from HHS about the future of Title X, moving away from contraception, in the president’s budget he proposed completely getting rid of Title X, completely defunding it, which he has in the past as well. And so why would they put out guidance for a program that doesn’t exist?
Goldman: I think, also, this is the second budget that they’re putting out in this administration, right? So now they are just a little more used to what’s going on, and they have more of their feet under them.
Weber: As a preview for listeners, too, I’m sure we will have Kennedy asked about this budget when he appears in a series of so many hearings next week and the week after. And there were a lot of fireworks last year with him and various members of Congress about the budget. So I am sure that we will hear a lot more on this front in the weeks to come.
Rovner: Yeah, I would say that’s one thing that the budget process does, is when the president finally puts out a budget, the Cabinet secretaries travel to all of the various committees on Capitol Hill to, quote, “defend the president’s budget,” which is sometimes or, I guess in the case of Kennedy, one of the few chances that they get to actually have him in person to ask him questions. But in the meantime, you know, we have the budget, then we have the president himself, who at an Easter lunch last week тАФ that was supposed to be private, but ended up being live-streamed тАФ said, and I quote, “It’s not possible for us to take care of day care, Medicare, Medicaid, all these individual things.” The president went on to say that states should take over all that social spending, and the only thing the federal government should fund is, quote, “military protection.” Did I just hear a thousand Democratic campaign ads bloom?
Goldman: I think this is a prime example of when you should take Trump seriously, but not literally. I don’t think that there’s any world, at least in the foreseeable future, where the federal government isn’t funding Medicare. But, you know, you certainly have to watch at the margins. It’s like, it’s not a secret that this is something that they’re interested in cutting back spending on. It’s super politically difficult to do that, and they know that, and that’s part of why, which I’m sure we’ll talk about in a little bit, they bumped up the payment rate for 2027 to Medicare Advantage plans.
Rovner: Which we will get to.
Goldman: Yeah, so I mean, it’s certainly an eye-opening statement, and you should remember it. But I don’t think that we’re in immediate jeopardy here.
Rovner: This is the president who ran in 2024, you know, saying that he was going to protect Medicare and Medicaid. I mean, it’s been, you know, against some of the recommendations of his own administration. I was just sort of shocked to see these words come out of his mouth. Lauren, you wanted to say something?
Weber: I mean, it’s not that surprising, though. I mean, look at what the One Big Beautiful Bill [Act] did to Medicaid. He’s already pushed through massive Medicaid cuts, which are essentially being offloaded to the states. So, I mean, I think this ideology has already borne out and will continue to bear out, and obviously it’s happening amid the backdrop of a war. So that plays into, obviously, the commentary as well.
Rovner: Well, meanwhile, Republicans are still talking about doing another budget reconciliation bill, the 2.0 version of last year’s Big Beautiful Bill, except this time it’s essentially just to fund the military and ICE [Immigration and Customs Enforcement] and border control, because Democrats won’t vote for those things, at least they won’t vote for additional military spending. What are the prospects for that to actually happen? And would Republicans really be able to do it if those programs are paid for with more cuts to Medicare and/or Medicaid, as some have suggested?
Goldman: You know, my co-worker Peter Sullivan wrote about this last week, and there was a lot of blowback from politicos, from advocates, from, you know, kind of across the spectrum of groups there. I think that it would be extremely politically unpopular, especially going into the midterms, to use health care as an offset. But I would say that Republicans are pretty good at rhetoric, right? That’s one of the things that they’re known for right now, and there’s always a way to spin it.
Rovner: Alice and I spoke to a group earlier this week, and I went out on a limb and predicted that I didn’t think Republicans could get the votes for another big budget reconciliation this year. I mean, look at how close it was last year. The idea of cutting any deeper seems to me unlikely, just given the margins that they have.
Goldman: And I think that is something that you do in between election years. That’s not something you do in an election year.
Rovner: That’s true, yes тАж you do tend to see these bigger bills in the odd-numbered years rather than the even-numbered years, but тАж
Ollstein: And I think it’s important to remember that the reason Republicans are in this bind and that they feel like they have to keep reconciliation nearly focused on funding immigration enforcement is because Democrats refuse to fund immigration enforcement. And so they feel pressured to put all their effort and political capital towards that, and don’t want to mess that up by adding a bunch of other health care things that could cause fights and lose them votes.
Goldman: The money has got to come from somewhere.
Rovner: And health care is where all the money is. Speaking of Medicare and Medicaid, where most of the money is, there is news on those fronts, too. Maya, as you hinted on Medicare, the administration is out with its payment rule for private Medicare Advantage plans for next year. And remember, we talked about how HHS was going to really go after overbilling in Medicare Advantage and cut reimbursement dramatically? Well, you can forget all that. The final rule will provide plans with a 2.48% pay bump next year. That’s compared to the less than 1% increase in the proposed rule. That’s a difference of about $13 billion. The final rule also eliminated many of the safeguards that were intended to prevent overbilling. What happened to the crackdown on Medicare Advantage? Are their lobbyists really that good?
Goldman: Their lobbyists are pretty good. This was a year where there were тАФ I think CMS [the Centers for Medicare & Medicaid Services] said there were a record number of public comments on their proposed rate, flat rate increase, flat rate update. But I think it’s also not that surprising. Historically, the final rate announcement for Medicare Advantage is almost always a little higher than the proposed because they incorporate additional data from the end of the previous year that wasn’t available when first rate is proposed, the initial rate is proposed. But certainly they backed away from a big change to risk adjustment, or, like, the way to adjust payment based on how sick a plan’s enrollees are. You get more pay тАж
Rovner: Because that’s where the overbilling was happening, that we’d seen a lot of these wonderful stories that plans were basically, you know, inventing diagnoses for patients who didn’t necessarily have them or didn’t have a severe illness, and using that to get additional payments.
Goldman: Right. And they did move forward with a plan to prevent diagnoses that are not linked to information that’s in a patient’s medical chart from being used for risk adjustment. But a lot of plans had said, like, Yeah, this is, that’s the right thing to do, and it’s not going to be that impactful for us. You know, overall, this is a win for health insurance. I think one thing to note is that Chris Klomp, the director of Medicare, said, We’re still really focused on trying to right-size this program. That’s still a priority for us as an administration, but we also want to safeguard it. And so I think insurers are not off the hook entirely. There’s still going to be a lot of scrutiny, but their lobbyists are pretty good. And you know, no one wants to be seen as the candidate that cuts Medicare.
Rovner: And we have seen this before, that when Congress cuts “overfunding” for Medicare Advantage, the plans, seeing that they can’t make its big profits, drop out or they cut back on those extra benefits. And the beneficiaries complain because they’re losing their plans, or they’re losing their extra benefits, and they don’t really want to do that in an election year either, because there are a lot of people, many millions of people, who vote who are on these plans. So, in some ways, the plans have the administration over a political barrel, in addition to how good their lobbyists are.
Well, apparently, one group that HHS is still cracking down on are legal immigrants with Medicare. Most of the publicity around the health cuts in last year’s budget bill focused on the cuts to Medicaid. But about legal immigrants who’ve paid into the Medicare system with their payroll taxes for years and are now being cut off from their Medicare coverage. This is apparently the first time an entire category of beneficiaries are having their Medicare taken away. I’m surprised there hasn’t been more attention to this, or if it’s just too much all happening at once.
Ollstein: I mean, there’s a lot happening at once, and even just in the space of immigrants’ access to health care, there is so much happening at once. And so this is obviously having a huge impact on a lot of people, but so are 100 other things. And I think, you know, the zone has been flooded as promised. And really, state officials who are also dealing with a thousand other things, Medicaid cuts, you know, these federal changes, work requirements, are grappling with this as well.
Rovner: Lauren, you wanted to add something?
Weber: Yeah. I mean, I thought it was, there was a striking quote in the story from Michael Cannon, who basically said, The reason this isn’t resonating is because this won’t upset the Republican base. And I think that’s a striking quote to be considered.
Rovner: Michael Cannon, libertarian health policy expert, just kind of an observer to this one. But yeah, I think that’s true. I mean, or at least the perception is that these are not Republican voters, although, you know, as we’ve seen, you know, Congress has tried to take aim at people they think aren’t their voters, and it’s turned out that those are their voters. So we will see how this all plays out.
Well, at the same time that this is all going on, the folks over at the newsletter “Healthcare Dive” are reporting that the Centers for Medicare & Medicaid Services are trying to embark on all these new initiatives on fraud, and work requirements, and artificial intelligence with a diminished workforce. While CMS lost far fewer workers in the DOGE [Department of Government Efficiency] cuts last year than many other of the HHS agencies тАФ it was in the hundreds rather than the thousands тАФ CMS has long been understaffed, given the fact that it manages programs that provide health insurance to more than 160 million Americans through not just Medicare and Medicaid, but also the Children’s Health Insurance Program and the Affordable Care Act. I know last week, FDA Commissioner Marty Makary said he wants to hire more workers to replace the 3,000 who were RIF’ed or took early retirement there at the FDA. And CMS does have lots of job openings being advertised. But it’s hard to see how replacing trained and experienced workers with untrained, inexperienced ones are going to improve efficiency, right?
Goldman: Tangentially, I was talking to a health insurance executive yesterday who was saying that his team is so much bigger than CMS, and they cover a fraction of the market, and they’re often the ones coming to CMS and proposing ideas and working with CMS on it. I don’t, I think that is a dynamic that far predates this administration, but тАж
Rovner: Oh, absolutely.
Goldman: But it’s certainly interesting. And тАж CMS has very ambitious plans, and not that many people to carry them out. But, you know, I think one thing that I also want to note is that when I talk to trade associations and stakeholders about this CMS, they are generally like, pretty support- тАж like, they say that they think they’re being heard, and they think that CMS and the career staff are doing, you know, the same kind of caliber of work that they’ve been doing, which I think is notable.
Rovner: And as we have mentioned many times, you know, Dr. [Mehmet] Oz, the head of CMS, is very serious about his job and doing a lot of really interesting things. It’s just, it’s hard, you know, in the federal government, if you don’t have the resources that you want to тАж if you don’t have the resources to match your ambitions. Let’s put it that way.
Well, meanwhile, on the Medicaid front, we’re already seeing states cutting back, and some of the results of those cutbacks. on how psychiatric units are at risk of being shut down due to the Medicaid cuts, since they often serve a disproportionate number of low-income people and also tend to lose money. And The New York Times has a of an Idaho Medicaid cutback of a program that had provided home visits to people living in the community with severe mental illness, until those people who lost the services began to die or to end up back in more expensive institutional care. Now the state has resumed funding the program, but obviously will end up having to cut someplace else instead. I know when Republicans in Congress passed the cuts last year, they said that people on Medicaid who were not the able-bodied working-age populations wouldn’t see their services cut. But that’s not how this is playing out, right?
Weber: I just think the story by Ellen Barry, who you should always read on mental health issues in The New York Times, “,” is such an illustrative example of unintended consequences from these cuts. And the reason that they’re being reversed тАФ by Republican legislators, no less тАФ in Idaho, is because it’s more expensive to have cut the money from it than it is efficient. I mean, what they found was, is that after they cut the money to the schizophrenia program, they saw this massive uptick in law enforcement cases and hospitalizations, uninsured hospitalizations, that this avoided. And I think it’s a real canary in the coal mine situation, because we’re only starting to see these states cut these things off. And this was a pretty immediate multiple-death consequence. And I think we’re going to see a lot of stories like this, of a variety of programs that we all don’t even have any idea that exist in the safety net across the country that are being chipped away at.
Rovner: Well, turning to other news from the Department of Health and Human Services, we’re getting some more competition here at What the Health? Health secretary Kennedy has announced he’ll be unveiling his own podcast, called The Secretary Kennedy Podcast, next week. He promises to, according to the trailer posted online on Wednesday, quote, “name the names of the forces that obstruct the paths to public health.” OK then, we look forward to listening.
Meanwhile, in actual secretarial work, the secretary this week also unveiled changes to the charter of the Advisory Committee on [Immunization] Practices after a federal judge last month invalidated both the replacement members that he’d appointed last year and the changes made to the federally recommended vaccine schedule. So what’s going to happen here now? Will this get around the judge’s ruling by watering down the expertise that members of this advisory committee are supposed to have in vaccines? And why hasn’t the administration appealed the judge’s ruling yet?
Goldman: You know, I don’t have actual answers to this, but I do wonder and speculate that this is going to end up being some kind of legal whack-a-mole situation where the secretary and HHS says, OK, you don’t like it that way? We’ll do it this way, and then they’ll do it another way, and advocates will sue, and we’ll see how this plays out going forward in the courts. I think this is not the end of the story. Even though the judge’s decision was a big win for vaccine advocates, it’s just we’re in the midpoint, if that.
Rovner: And Lauren, speaking of vaccines, your colleague Lena H. Sun has on HHS and vaccine policy.
Weber: Yeah, Lena Sun is always delivering. She found out that the acting director of the CDC [Centers for Disease Control and Prevention] at the time delayed publication of a report showing that the covid-19 vaccine[s] cut the likelihood of emergency department visits and hospitalizations for healthy adults last winter by about half. So even though Kennedy is not talking more about vaccines, it appears that, based on this reporting, that some of his underlings are not necessarily touting the benefits of vaccine, so to speak. And I’m very curious, going back to Kennedy’s podcast, I found the rollout of that so interesting because the teaser was very leaning into the Kennedy that got elected, you know, someone who speaks about, you know, dark truths that are hidden from the public, and so on. And then the press team had these statements of, like, Kennedy will investigate the affordability of health costs and food and nutrition. And I think this dichotomy of who Kennedy is and who the White House and the press secretary and HHS want Kennedy to be before the midterms really could come to a head in this podcast. So I think we will all be listening to hear how that goes.
Rovner: Yeah, we keep hearing about how the secretary is being, you know, sort of put on a leash, if you will. And, you know, told to downplay some of his anti-vaccine views and things like this. And that seems quite at odds with him having his own podcast. Alice, do you want to тАж?
Weber: I guess, it depends on who’s editing the podcast and who they have on. I’m just very тАж you could even tell from the trailer to how his press secretary presented it, there was an interesting differential in framing, and I am curious how that plays out as we see guests on it.
Ollstein: I mean, it’s also worth noting that this is an administration of podcasters. I mean, you have Kash Patel, you have so many of these folks who have a history of podcasting, clearly have a passion for it, just can’t let it go while working a full-time, high-pressure government job.
Rovner: We shall see. Meanwhile, HHS, together with the Environmental Protection Agency, is waging war on microplastics, those nearly too impossible to detect bits of plastic that are getting into our lungs and stomachs and body tissues through air and water and food. The plan here seems to be to find ways to detect exactly how much microplastics we are all getting in our water and what the health impacts might be, since we don’t have enough information to regulate them yet. I would think this would be one of those things that pleases both MAHA [Make America Healthy Again] and the science community, right? Or is it just, as one MAHA supporter called it, theater?
Goldman: I think this is a great example of the, you know, part of the reason why MAHA is so interesting to such a wide swath of people. Like, there’s a lot of legitimate concern, not that other concerns aren’t necessarily legitimate, but there’s a lot of concern over, from the scientific community, over microplastics. I’m honestly surprised that we’re this far into the administration with this announcement. I would have thought that this is something they would have done sooner, but they obviously had other priorities as well.
Rovner: Well. Finally, this week, speaking of other priorities, HHS Secretary Kennedy and CMS Administrator Dr. Oz are declaring war on junk food in hospitals. Again, this seems like a popular and fairly harmless crusade; hospitals shouldn’t be serving their patients ultraprocessed food. Except, almost as soon as the announcement came out, I saw tons of pushback online from doctors and nurses who worried about patients for whom sugary food or drinks are actually medically indicated, or who, because of medications they’re taking, or illnesses they have, can only eat, or will only eat, highly palatable, often processed food. Nothing in health care is as simple as it seems, right?
Weber: I think what’s also interesting is one of my favorite examples in the memo they put out was they hope that every hospital, as an example, could serve quinoa and salmon. And I just am curious to see how fast that gets implemented. And it’s a very valid тАФ a lot of people complain about hospital food. It’s a very valid thing to push for better food. But I also question, as I understand it, this seems more like a carrot than a stick when it comes to the regulation they put out.
Rovner: As it were.
Weber: As it were. And so I’m curious to see how it gets implemented. That said, there are hospitals that have taken it upon themselves тАФ the Northwell [Health] example in New York is a good example тАФ to really improve their hospital food. And frankly, it’s a money maker. If your food’s better, people come to your hospital, especially in an urban area where there is hospital competition. So you know, like most MAHA topics, there’s a lot of interesting points in there, and then there’s a lot of what’s the reality and what’ actually going to happen. And so I’ very curious to see how this continues to play.
Rovner: I did a big story, like, 10 years ago on a hospital chain that had its own gardens, that literally grew its own healthy food. So this is not completely new but, again, interesting.
All right, that is this week’s news. Now it’s time for our extra-credit segment. That’s where we each recognize a story we read this week we think you should read, too. Don’t worry if you miss it. We will post the links in our show notes on your phone or other mobile device. Alice, why don’t you start us off this week?
Ollstein: I have a piece from my co-worker Simon [J.] Levien, and it is called “.” This is about thousands of doctors around the country who are from other countries that are placed on, you know, a list by the Trump administration of places where they want to scrutinize and limit the number of immigrants coming from there. And so these are people who are already here, already practicing, have poured years into their training, have been living here, and, in some cases, are the only folks willing to work in certain areas that have a lot of medical shortages, and they just can’t practice because their paperwork isn’t getting processed in time. And so they’re sort of in this scary limbo, and that’s putting these hospitals and clinics that they work in in a really tough bind. And so they’re hammering the Trump administration to give them answers about what their fate is. You know, they’re not trying to deport them yet, but they’re not allowing them to continue working either.
Rovner: For an administration that’s been pushing really hard to improve rural health care, this does not seem to be a way to improve rural health care. Maya.
Goldman: My extra credit this week is called “.” It’s a great KFF Health News scoop from Amanda Seitz and Maia Rosenfeld. It’s a really great example of the administration, you know, sort of moving in silence, doing these small regulatory announcements that could have big impact. Basically, the Office of Personnel Management is asking for personally identifiable medical information from health insurers, and its reasoning is to analyze costs and improve the health system, but they could get very detailed medical information from federal employees, including things like, did they get an abortion? Are they undergoing gender-affirming care? And, obviously, there is a strong concern that that could be used against them.
Rovner: Yeah тАж this was quite a scoop. Really, really interesting story. Lauren.
Weber: Mine was a pretty alarming story by Holly Yan at CNN: “.” And basically there’s this type of drug test that the scientists have found is not that effective, and it’s led to things like bird poop being scraped off a man’s car appearing on a drug test as cocaine, a great-grandmother’s medication testing positive for cocaine, and a toddler’s ashes registering as meth or ecstasy, and horrible legal and other consequences of this kind of misdiagnosis in the field. And the reason these drug tests are often done is because they’re cheaper. There’s a more expensive, more accurate version, but these are cheaper. They’re done in the field. But the potential side effects and horrible, wrongly accused effects are quite large, and so Colorado has passed this law to try and move away from this. And it’s curious to see if other states will follow suit.
Rovner: Yeah, this was something I knew nothing about until I read this story. My extra credit this week is from The Atlantic by Katherine [J.] Wu, and it’s called “.” And it’s about how some of the very top career officials from the NIH [National Institutes of Health], the CDC, and other agencies have, after having been put on leave more than a year ago, finally been reassigned to far-flung outposts of the Indian Health Service in the western United States. They got news of their proposed reassignments with little description of their new roles and only a couple of weeks to decide whether to move across the country or face termination. Now, if these officials’ skills matched those needed by the Indian Health Service, this all might make some sense. But what the IHS most needs are active clinicians: doctors and nurses and social workers and lab technicians. And those who are now being reassigned are largely managers, including тАФ and here I’m reading from the story, quote тАФ “the directors of several NIH institutes, leaders of several CDC centers, a top-ranking official from the FDA tobacco-products center, a bioethicist, a human-resources manager, a communications director, and a technology-information officer.” The Native populations who are ostensibly being helped here aren’t very happy about this, either. Former Biden administration Interior Secretary Deb Haaland, a Native American who’s now running for governor in New Mexico, called the reassignment proposals, quote, “shameful” and “disrespectful.” Also, and this is my addition, not a very efficient use of human capital.
OK, that’s this week’s show. Thanks this week to our fill-in editor, Mary-Ellen Deily, and our producer-engineer, Francis Ying. A reminder: What the Health? is now available on WAMU platforms, the NPR app, and wherever you get your podcasts тАФ as well as, of course, . Also, as always, you can email us your comments or questions. We’re at whatthehealth@kff.org. Or you can find me on X , or on Bluesky . Where do you guys hang these days? Maya.
Goldman: I am on LinkedIn under my first and last name, , and on X at .
Rovner: Alice.
Ollstein: I’m on Bluesky and on X .
Rovner: Lauren.
Weber: Still @LaurenWeberHP on both and .
╕щ┤╟▒╣▓╘▒Ё░ї:╠¤We will be back in your feed next week.┬аUntil then, be healthy.
Credits
And subscribe to “What the Health? From ║┌┴╧│╘╣╧═Ї News” on , , , , , or wherever you listen to podcasts.
║┌┴╧│╘╣╧═Ї News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFFтАФan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/podcast/what-the-health-441-mifepristone-trump-budget-request-hhs-april-9-2026/">article</a> first appeared on <a target="_blank" href="">KFF Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=2181013&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>